Bone Tissue Chapter 7
|
|
|
- Byron Walton
- 7 years ago
- Views:
Transcription
1 Bone Tissue Chapter 7 Tissues and organs of the skeletal system Histology of osseous tissue Bone development Physiology of osseous tissue Bone disorders
2 Bone Tissue Bone is alive and continuously changing. Bone tissue (osseous tissue) is a type of connective tissue with cells, vessels, nerves and a matrix hardened by minerals (mostly calcium phosphate) Bones are units of the skeletal system individual bones are made up of bone tissue, marrow, cartilage and periosteum Functions of the skeletal system include support, protection, movement, blood formation, calcium and phosphate reservoir, ph balance
3 Compact Bone and Spongy Bone Compact Bone does not have any spaces or hollows in the bone matrix that are visible to the eye. Compact bone forms the thick-walled tube of the shaft (or diaphysis) of long bones, which surrounds the marrow cavity (or medullary cavity). A thin layer of compact bone also covers the epiphyses of long bones. Spongy Bone (also called trabecular bone or cancellous bone) consists of a delicate network of trabeculae which branch and intersect to form a sponge-like tissue. The ends of long bones (or epiphyses) contain mainly spongy bone.
4 Compact Bone and Spongy Bone Spongy Bone Compact Bone
5 Features of Long Bones Diaphysis (shaft) is a cylinder of compact bone containing the marrow cavity (medullary cavity) Diaphysis covered with periosteum Marrow Cavity contains hematopoeitic tissue Epiphyses (enlarged ends) are spongy bone covered with a thin layer of compact bone enlarged ends strengthen joint and provide attachment of tendons and ligaments Joint Surface is covered with articular cartilage (smooth, low friction hyaline cartilage and synovial fluid)
6 Features of Long Bones
7 Periosteum is a layer of vascular, innervated, dense connective tissue surrounding the non-articular surfaces of bone. Perforating Fibers (also called Sharpey s fibers) are collagen fibers that connect the periosteum to the bone matrix. The endosteum is a thin layer of connective tissue that lines the inside of the marrow cavity and any canals passing through the compact bone. Both the periosteum and the endosteum membranes are osteogenic they contain cells that can produce bone. During growth or following injury, osteogenic cells can differentiate into bone-forming osteoblasts. Periosteum and Endosteum Endosteum Perforating Fibers
8 Structure of a Flat Bone External and internal surfaces of flat bone are composed of compact bone. Middle layer is spongy bone and it is also called the diploe. An impact to the skull may fracture the outer layer and crush the spongy bone, but not harm inner compact bone or the underlying brain.
9 Osteogenic Cells Osteogenic Cells are found in the endosteum and periosteum. arise from embryonic mesenchymal cells multiply continuously and differentiate into osteoblasts in response to stress or fractures Osteoblasts produce an extracellular matrix of about 35% collagen fibers and 65% mineral (mostly calcium phosphate). Osteocytes are osteoblasts that have completely surrounded themselves with the extracellular matrix they produce. Spicules are isolated, newly formed pieces of bone.
10 Osteocytes Osteocytes are completely surrounded by bone matrix. Lacunae are the pits in the matrix occupied by the cells. Filopods (also called pseudopods, cytoplasmic extensions, dendritic processes) are long thin extensions of the osteocytes that produce bone matrix around the cell. Filopods are inside tiny canals in the matrix called canaliculi.
11 Osteocytes Osteocytes are arranged in rings called lamellae that are around a central canal that contains blood vessels and nerves. Tips of filopods absorb nutrients from the central canal. Adjacent osteocytes are inter-connected with gap junctions at the tips of the filopods. Osteocytes transfer nutrients from one cell to another through gap junctions.
12 Osteoclasts Macrophages Some stem cells in bone marrow develop into macrophages white blood cells called macrophages. Some macrophages leave the blood and move into bone tissue. In the bone, 3-50 of these macrophages can merge into giant, multinucleated cells called osteoclasts. A single cell formed by the fusion of several cells is called a syncitium. The surface of an osteoclast facing bone is folded into a ruffled border that releases lysosomes that contain enzymes and acids that erode bone matrix and produce pits in the matrix called resorption bays (also called Howship s lacunae).
13 Osteoclasts Four multinucleated osteoclasts producing resorption bays ( Howship s lacunae) in the blue-stained bone matrix. The ruffled border of the osteoclasts is facing the the bone matrix. Dissolved components of the bone matrix (calcium and amino acids) accumulate in the interstitial space and are reabsorbed into the blood.
14 Bone Matrix Bone Matrix is about 35% organic and 65% inorganic Bone Organic matter consists of: collagen glycosaminoglycans (chondroitin sulfate) proteoglycans glycoproteins Bone Inorganic matter consists of: 85% hydroxyapatite (calcium phosphate crystals) 10% calcium carbonate 5% other minerals (fluoride, sulfate, potassium, magnesium) Combination of organic and inorganic materials makes bones both strong and resilient minerals resist compression collagen give some flexibility Bone matrix is similar to fiberglass that is composed of strong glass fibers embedded in a flexible polymer
15 Bone Matrix
16 Compact Bone Osteon (Haversian system) is the basic structural unit of bone. Osteons are cylinders of bone tissue formed from layers (concentric lamellae) of osteocytes and matrix arranged around a central (Haversian) canal. Central Canal is lined with endosteum and contains a neurovascular bundle. Neurovascular Bundles contain an artery, vein, nerve and lymphatic vessel Osteocytes are connected to each other and their blood supply by thin pseudopods within canaliculi. Perforating Canals (Volkmann s canals) are perpendicular branches of the central (Haversian) canal Circumferential lamellae ring the outer circumference and the marrow cavity. Bony trabeculae branch off the compact bone surrounding the marrow cavity, filling the cavity with spongy bone.
17 Osteon = Haversian System Circumferential lamellae
18 Histology of Compact Bone
19 Osteon = Haversian System Lacunae Canaliculi Haversian (central) Canal Concentric Lamellae
20 Perforating (Volkman s) Canal Central (Haversian) Canal
21 Development of an Osteon 5/student_view0/chapter 6/animation bone_gro wth_in_width.html
22 Spongy Bone Spongelike appearance formed by rods and plates of bone called trabeculae spaces among the trabeculae are filled with bone marrow Light weight but strong trabeculae develop along bone s lines of stress
23 Bone Marrow Bone Marrow is a soft tissue that occupies the medullary cavity of long bones and the spaces among the trabeculae of spongy bone Red Marrow looks like thick blood bone marrow is the adult hemopoietic tissue that produces blood cells and platelets found in vertebrae, ribs, sternum, pelvic girdle and proximal heads of femur and humerus in adults Yellow Marrow fatty marrow in shaft of long bones in adults Gelatinous Marrow reddish, jelly-like marrow in old individuals
24 Red Bone Marrow
25 Two types of Bone Development Intramembranous Ossification produces the flat bones of the skull. Endochondral Ossification produces most of the other bones of the skeleton including the long bones of the extremities (arms and legs). The principal difference between intramembranous bone formation and endochondral bone formation is what is replaced during development. The tissue replaced during development in intramembranous ossification is embryonic CT. The tissue replaced in endrochondral ossification is hyaline cartilage. The two processes can occur side by side, and do, in the case of fracture healing and in the development of the the mandible and the clavicle which develop partially from intramembranous ossification and partially from endochondral ossification.
26 Intramembranous Ossification Produces flat bones of skull Steps of the process: 1) Mesenchyme condenses into a sheet of vascular, soft tissue 2) Some mesenchymal cells develop into osteoblasts that form osteoid tissue (uncalcified bone matrix). Other mesencymal cells develop into fibroblasts that form the periosteum membrane. Calcium is deposited in the matrix and it hardens. Osteoblasts develop into osteocytes as they become surrounded by bone. 3) Bony trabeculae form spongy bone. 4) Spaces between trabeculae fill with bone in the surface layers forming compact bone that is covered with periosteum
27 Intramembranous Ossification of the Skull
28
29 Intramembranous Ossification periosteum bone periosteum This is a cross section of fetal skull bone developing by intramembranous ossification. The irregularly shaped pink areas are developing spicules of bone.
30 Intramembranous Ossification Ob HC Oc T ECT T Ocl T HC Embryonic connective tissue (ECT) is gradually replaced by trabeculae (T) of bone that developes around blood vessels in Haversian canals (HC). Osteoblasts (Ob) cover the developing trabecular bone (T) and become osteocytes (Oc) once completely surrounded by matrix. Multinucleated osteoclasts (Ocl) demineralize and remodel the bone matrix.
31 Endochondral Ossification Long Bones form from endochondral ossification as a hyaline cartilage model that is gradually replaced by bone. Endochondral Ossification proceeds as follows: a primary ossification center forms in the cartilage model cartilage becomes hypertrophic (chondrocytes swell as they form the primary ossification center). hypertrophic cartilage is removed by macrophages primary marrow space is formed as cartilage is removed blood vessels and nerves grow into the marrow space osteogenic cells (mesenchymal-like fibroblasts) from the perichondrial/periosteal membrane invade the spaces created by the macrophages and transform into osteoblasts osteoblasts deposit osteoid tissue and calcified matrix
32 Ossification Centers The primary ossification center forms as cartilage in the center of the cartilage model becomes hypertrophic from a growing blood supply. Hypertrophic cartilage calcifies and dies. Osteoclasts remove of the dead hypertrophic cartilage and then blood vessels, nerves and osteoblasts grow into that space. The same process begins in each epiphysis forming secondary ossification centers that will develop into spongy bone.
33 Osteoblasts in the Primary ossification center Secondary ossification center Langman s
34 Perichondrium Ossification Centers
35 Zones of Ossification E Cartilage proliferates, becomes hypertrophic, calcifies, dies and is removed and is replaced with new bone tissue.
36 Zones of Ossification A) Zone of Reserve Cartilage is a layer of resting hyaline cartilage B) Zone of Cell Proliferation is a layer of chondrocytes that multiply forming columns of flattened lacunae C) Zone of Cell Hypertrophy is a region of swollen chondrocytes D) Zone of Calcification is where the cartilage matrix mineralizes and the chondrocytes die E) Zone of Bone Deposition is where mineralized cartilage matrix is replaced by bone. Voids are filled with osteoblasts and blood vessels forming Haversian canals and osteons
37 Secondary Ossification Centers develop in the Epiphyses Secondary Ossification Center Diaphysis Metaphysis Epiphysis Epiphyseal plate Metaphysis is cartilaginous tissue between the primary and secondary ossification centers. The epiphyseal plate (growth plate) is a temporary layer of cartilaginous tissue between the spongy bone of the medullary cavity (marrow cavity) and the spongy bone in the epiphyses that persists until growth of the bone is complete.
38 Secondary Ossification Centers Secondary ossification centers begin to form in the epiphyses near time of birth. Bone development does not proceed all the way to the end of the bone. Hyaline cartilage remains over epiphysis as the articular cartilage of the joint surface. The metaphysis is at the junction of the diaphysis and epiphysis and forms an epiphyseal plate (also called a growth plate) until growth ends.
39 epiphyseal plate
40 The Fetal Skeleton at 12 Weeks stained red for bone tissue. Cartilage is unstained.
41 Cranial ossification is incomplete at birth Soft regions of the skull called fontanels are regions of dense irregular connective tissue. There are usually 6 fontanels at birth Most fontanels close by 12 months and all are usually closed by 24 months.
42 Epiphyseal Plates
43 Bone Growth and Remodeling Bones grow and remodel throughout life exercise or manual labor increases density and mass of bone pulling of muscle on periosteum stimulates bone growth on that side of the bone osteoclasts are stimulated by increased pressure osteoblasts are stimulated by decreased pressure Dental braces reposition teeth by creating greater pressure on the bone on one side of the tooth socket and less pressure on the other side of the tooth socket which remodels the jaw bone as the tooth moves
44 Factors Affecting Bone Growth 20 or more hormones, vitamins and growth factors affect bone and not all the mechanisms are known. Bone growth is especially rapid at puberty growth hormones and sex hormones stimulate proliferation of osteogenic cells and chondrocytes in growth plate adolescent girls grow faster than boys and reach their full height earlier (estrogen has strong effect on bone growth) males grow for a longer time due to sustained high levels of testosterone resulting in larger average stature Growth ceases when epiphyseal plate closes anabolic steroids may cause premature closure of growth plate producing short adult stature
45 Achondroplastic Dwarfism Achondroplastic dwarfism is a genetic disorder resulting in short stature but normal-sized head and trunk Long bones of the limbs stop growing in childhood but other bones are unaffected.
46 Gigantism A pituitary giant can result from an excess of growth hormone during skeletal growth. 8 tall adult
47 Gigantism Robert Pershing Wadlow in 1938, at age 20 with actresses Maureen O Sullivan, left, and Ann Morris. Smithsonian August 2005 p. 76.
48 Robert Pershing Wadlow, with his mother at his side, had grown to a record height of 8 11 by the time of his death at age 22.
49 7 pounds at age 2 There are over 200 different types of dwarfism, all of which involve bone growth disorders (osteodysplasia) that result in short stature (adult height less than 4 ft. 10 in. tall). Primordial Dwarfism is a group of disorders in which growth is proportional but severely delayed, beginning in the womb. This results in some of the smallest people in the world. The individual pictured has Majewski osteodysplastic primordial dwarfism (MOPD) Type II. Only about 100 individuals worldwide have been identified as having MOPD type II. Both males and females of all ethnic backgrounds are affected. Some families have more than one child with MOPD Type II, which suggests that the disorder is inherited in an autosomal recessive manner. Majewski osteodysplastic primordial dwarfism type II (MOPD II): Natural History and Clinical Findings. Hall, Flora, Scott, Pauli, Tanaka, Am J. Med Genet A Sep 15 ; 130A(1):55-72.
50 Mineralization of Bone Matrix Mineralization is a process in which ions (mostly calcium and phosphate) are removed from blood plasma and are deposited in the matrix of bone tissue. Steps of the mineralization process: osteoblasts produce collagen fibers fibers become encrusted with minerals Image taken using a Scanning Electron Microscope showing collagen fibers produced by osteoblast cells on a polyurethane foam scaffold mimicking the bone matrix production and mineralization processes.
51 Mineral Resorption Bone is dissolved by the osteoclast ruffled border and dissolved calcium and phosphate are released into the blood pumps in the cell membrane secrete hydrogen ions into the space between the osteoclast and the bone and chloride ions follow forming hydrochloric acid (HCl) hydrochloric acid with a ph of 4 dissolves bone minerals an enzyme is also released that digests the collagen
52 Calcium Balance Calcium levels outside of normal values cause: hypocalcemia (deficiency of blood calcium) causes excessive excitability of nervous system by increasing the gradient for diffusion of cations out of the cell which leads to: muscle spasms, tremors or tetany laryngospasm may cause suffocation hypercalcemia (excessive of blood calcium) depresses nervous system activity by decreasing the ionic gradient across the neuron membrane Calcium phosphate homeostasis depends on a balance of calcitriol, calcitonin and parathyroid hormone (PTH)
53 Calcitriol (Activated Vitamin D) UV radiation of epidermal keratinocytes converts a cholesterol derivative into Vitamin D 3 (cholecalciferol) which is absorbed into the blood. Liver and kidney enzymes convert Vitamin D 3 into the hormone calcitriol. Actions of calcitriol include: stimulates the intestines to absorb calcium and phosphate stimulates the kidneys to retain calcium stimulates osteoclasts to release calcium from bone
54 Calcitriol Synthesis and Action
55 Calcitonin Secreted by C cells of the thyroid gland when calcium is abundant in the blood Functions: reduces blood calcium levels reduces osteoclast activity increases the number and activity of osteoblasts Calcitonin has a powerful effect in children, but it is less effective in adults calcitonin deficiency is not known to cause any disease in adults, but it may be useful in reducing bone loss in osteoporosis
56 Parathyroid Hormone (PTH) Secreted by the parathyroid glands when the calcium level is too low in the blood. Functions promotes calcitriol synthesis stimulates osteoclast multiplication and activity inhibits collagen and bone matrix synthesis by osteoblasts promotes calcium resorption by the kidneys promotes phosphate excretion by the kidneys
57
58 Osteoporosis Most common bone disease Bones lose mass and become brittle due to loss of both organic matrix and minerals increases risk of fracture of hip, wrist and vertebral column hump results from deformed spine Best treatment is prevention: exercise and a recommended calcium intake of 1000 mg/day between ages 25 and 40.
59 Effects of Osteoporosis
60 Healing of Fractures Normally healing takes 8-12 weeks (longer in elderly) Stages of healing: see next slide 1. fracture hematoma is a blood clot resulting from broken blood vessels 2. soft callus of collagen and fibrocartilage is formed by fibroblasts and infiltrated by capillaries at site of break 3. a soft callus is gradually replaced by a hard callus of spongy bone in about 6 weeks 4. remodeling occurs over 6 months as spongy bone is replaced with compact bone
61 Healing of Fractures
62 Fractures and Repairs
63 Fibrodysplasia Ossificans Progressiva
64 END
1. outer fibrous layer contains fibroblasts that secrete collagen
 I. cartilage A. perichondrium 1. outer fibrous layer contains fibroblasts that secrete collagen 2. inner chondrogenic layer contains cells that can proliferate and turn into chondroblasts B. cartilage
I. cartilage A. perichondrium 1. outer fibrous layer contains fibroblasts that secrete collagen 2. inner chondrogenic layer contains cells that can proliferate and turn into chondroblasts B. cartilage
Function of Bones. Bone Tissue and Bones BONE CLASSIFICATION. Long Bones Gross Anatomy. Lab Activity 1 - Gross Anatomy of a Long Bone
 Function of Bones Bone Tissue and Bones Bones form the framework of the skeleton. Anatomy and Physiology Text and Laboratory Workbook, Stephen G. Davenport, Copyright 2006, All Rights Reserved, no part
Function of Bones Bone Tissue and Bones Bones form the framework of the skeleton. Anatomy and Physiology Text and Laboratory Workbook, Stephen G. Davenport, Copyright 2006, All Rights Reserved, no part
Osseous Tissue & Structure. The skeletal system includes: Storage of minerals: calcium salts
 Chapter 15 Lecture The Skeletal System: Osseous Tissue & Skeletal Structure The Skeletal System The skeletal system includes: Bones, cartilages, ligaments Bone tissue = osseous tissue Includes living cells
Chapter 15 Lecture The Skeletal System: Osseous Tissue & Skeletal Structure The Skeletal System The skeletal system includes: Bones, cartilages, ligaments Bone tissue = osseous tissue Includes living cells
7. Skeletal System: Bone Structure and Function
 7. Skeletal System: Bone Structure and Function For the next two chapters (7 and 9) we will study the skeletal system. Although the major feature of this system is the bones, the skeletal system also consists
7. Skeletal System: Bone Structure and Function For the next two chapters (7 and 9) we will study the skeletal system. Although the major feature of this system is the bones, the skeletal system also consists
E. Blood cells production. Blood cells are produced within the cavities of bones.
 FUNCTIONS OF THE SKELETAL SYSTEM 1. The skeletal system consists of bone, cartilage, ligaments (attach bone to another bone), and tendons (attach muscle to bone). 2. Functions. A. Support. Bone helps to
FUNCTIONS OF THE SKELETAL SYSTEM 1. The skeletal system consists of bone, cartilage, ligaments (attach bone to another bone), and tendons (attach muscle to bone). 2. Functions. A. Support. Bone helps to
Chapter 6: The Skeletal System: Bone Tissue
 Chapter 6: The Skeletal System: Bone Tissue Chapter Objectives FUNCTIONS OF THE SKELETAL SYSTEM 1. Discuss the functions of support, protection, assistance in movement, mineral homeostasis, blood cell
Chapter 6: The Skeletal System: Bone Tissue Chapter Objectives FUNCTIONS OF THE SKELETAL SYSTEM 1. Discuss the functions of support, protection, assistance in movement, mineral homeostasis, blood cell
BONES AND BONE TISSUE
 BIO 2401 BONES & BONE TISSUE page 1 BONES AND BONE TISSUE Organization of the Skeletal System components: 1) bone 2) skeletal cartilage: surrounded by dense irregular connective tissue which acts to girdle
BIO 2401 BONES & BONE TISSUE page 1 BONES AND BONE TISSUE Organization of the Skeletal System components: 1) bone 2) skeletal cartilage: surrounded by dense irregular connective tissue which acts to girdle
CHS 06-07 BONES AND SKELETAL TISSUES
 CHS 06-07 BONES AND SKELETAL TISSUES This chapter provides a review of bone and skeletal tissue. The human skeleton is composed primarily of two connective tissues: (1) cartilage and (2) bone. CHARACTERISTICS
CHS 06-07 BONES AND SKELETAL TISSUES This chapter provides a review of bone and skeletal tissue. The human skeleton is composed primarily of two connective tissues: (1) cartilage and (2) bone. CHARACTERISTICS
10/12/2011. Classification of Bones Every adult skeleton contains 206 bones which can be arranged into six broad categories according to shape
 Primary Functions of Skeletal System 1. support 2. storage of minerals & lipids -calcium salts provide vital minerals -lipids are in stored yellow marrow 3. blood cell production -RBC s, WBC s, and other
Primary Functions of Skeletal System 1. support 2. storage of minerals & lipids -calcium salts provide vital minerals -lipids are in stored yellow marrow 3. blood cell production -RBC s, WBC s, and other
Chapter 11. What are the functions of the skeletal system? More detail on bone
 Skeletal System Chapter 11 11.1 Overview of the skeletal system What are the functions of the skeletal system? 1. Supports the body 2. Protects the soft body parts 3. Produces blood cells 4. Stores minerals
Skeletal System Chapter 11 11.1 Overview of the skeletal system What are the functions of the skeletal system? 1. Supports the body 2. Protects the soft body parts 3. Produces blood cells 4. Stores minerals
THE SKELETAL SYSTEM: BONE TISSUE. Chapter 6. Anatomy and Physiology Lecture
 Chapter 6 1 THE SKELETAL SYSTEM: BONE TISSUE Chapter 6 Anatomy and Physiology Lecture Chapter 6 2 THE SKELETAL SYSTEM: BONE TISSUE Bone (Osseous) Tissue forms most of the skeleton: Skeletal System - the
Chapter 6 1 THE SKELETAL SYSTEM: BONE TISSUE Chapter 6 Anatomy and Physiology Lecture Chapter 6 2 THE SKELETAL SYSTEM: BONE TISSUE Bone (Osseous) Tissue forms most of the skeleton: Skeletal System - the
Human Anatomy & Physiology I with Dr. Hubley. Practice Exam #2
 Human Anatomy & Physiology I with Dr. Hubley Practice Exam #2 For questions 1 through 3, select your answers from the following responses: a. stratified squamous epithelium b. reticular connective tissue
Human Anatomy & Physiology I with Dr. Hubley Practice Exam #2 For questions 1 through 3, select your answers from the following responses: a. stratified squamous epithelium b. reticular connective tissue
OBJECTIVE: List and describe the functions of the skeletal system. D. Storage depot for minerals and homeostasis
 Text Reference: Chapters 6 and 7 Pages 1-6 are mostly a review from lab Know this material before you come to lecture. Lecture will begin on page 7 Read text and complete packet before lecture. I. Introduction
Text Reference: Chapters 6 and 7 Pages 1-6 are mostly a review from lab Know this material before you come to lecture. Lecture will begin on page 7 Read text and complete packet before lecture. I. Introduction
Chapter 5 The Skeletal System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone
Ground substance is the component of connective tissue between the cells and the fibers
 Connective Tissues Directions: Insert and install your Interactions: Foundations CD. a. Click the "Contents" button. b. Open the Tissue Level of Organization file. c. Click on Anatomy Overviews. d. Work
Connective Tissues Directions: Insert and install your Interactions: Foundations CD. a. Click the "Contents" button. b. Open the Tissue Level of Organization file. c. Click on Anatomy Overviews. d. Work
Unit 4: Skeletal System Test Review Test Review
 Name: Period: Unit 4: Skeletal System Test Review Test Review 1. List four functions of the skeletal system: a. b. c. d. 2. Define ossification and identify the roles of the osteoblasts, osteocytes, and
Name: Period: Unit 4: Skeletal System Test Review Test Review 1. List four functions of the skeletal system: a. b. c. d. 2. Define ossification and identify the roles of the osteoblasts, osteocytes, and
SAMPLE LECTURE EXAM 1 -- HUMAN ANATOMY
 SAMPLE LECTURE EXAM 1 -- HUMAN ANATOMY 1. The subcutaneous layer consists mostly of. a. smooth muscle c. areolar and adipose connective tissues d. melanin e. keratin 2. Which of the following statements
SAMPLE LECTURE EXAM 1 -- HUMAN ANATOMY 1. The subcutaneous layer consists mostly of. a. smooth muscle c. areolar and adipose connective tissues d. melanin e. keratin 2. Which of the following statements
Lab 5 Overview of the Skeleton: Classification and Structure of Bones and Cartilages Exercise 9 The Axial Skeleton Exercise 10
 Lab 5 Overview of the Skeleton: Classification and Structure of Bones and Cartilages Exercise 9 The Axial Skeleton Exercise 10 Overview of the Skeleton Locate the important cartilages in the human skeleton
Lab 5 Overview of the Skeleton: Classification and Structure of Bones and Cartilages Exercise 9 The Axial Skeleton Exercise 10 Overview of the Skeleton Locate the important cartilages in the human skeleton
THE SKELETAL SYSTEM FUNCTIONS OF THE SKELETAL SYSTEM
 THE SKELETAL SYSTEM The skeleton is the body s bony framework which consists of 206 bones. The bones are made up of water(45%), calcium and phosphorous(35%) and other organic materials(20%). The calcium
THE SKELETAL SYSTEM The skeleton is the body s bony framework which consists of 206 bones. The bones are made up of water(45%), calcium and phosphorous(35%) and other organic materials(20%). The calcium
Skeletal Development Multiple Cellular Origins
 Skeletal Development Multiple Cellular Origins 1 - Paraxial Mesoderm Somite, Sclerotome Axial Skeleton (e.g. vertebra) 2 - Lateral Plate Mesoderm Appendicular Skeleton (e.g. limb) 3 - Neural Crest Head
Skeletal Development Multiple Cellular Origins 1 - Paraxial Mesoderm Somite, Sclerotome Axial Skeleton (e.g. vertebra) 2 - Lateral Plate Mesoderm Appendicular Skeleton (e.g. limb) 3 - Neural Crest Head
Animal Tissues. I. Epithelial Tissue
 Animal Tissues There are four types of tissues found in animals: epithelial tissue, connective tissue, muscle tissue, and nervous tissue. In this lab you will learn the major characteristics of each tissue
Animal Tissues There are four types of tissues found in animals: epithelial tissue, connective tissue, muscle tissue, and nervous tissue. In this lab you will learn the major characteristics of each tissue
6 BONE TISSUE AND THE SKELETAL SYSTEM
 CHAPTER 6 BONE TISSUE AND THE SKELETAL SYSTEM 203 6 BONE TISSUE AND THE SKELETAL SYSTEM Figure 6.1 Child Looking at Bones Bone is a living tissue. Unlike the bones of a fossil made inert by a process of
CHAPTER 6 BONE TISSUE AND THE SKELETAL SYSTEM 203 6 BONE TISSUE AND THE SKELETAL SYSTEM Figure 6.1 Child Looking at Bones Bone is a living tissue. Unlike the bones of a fossil made inert by a process of
BIOL 4260 Human Evolu3onary Anatomy Lecture 5: Bone Development & Trunk Anatomy. Lecture 2: Fossil Record
 BIOL 4260 Human Evolu3onary Anatomy Lecture 5: Bone Development & Trunk Anatomy Lecture 2: Fossil Record Segmentation Cyclic genescreate segme ntation clock for somite production Final #s 4 occipital 8
BIOL 4260 Human Evolu3onary Anatomy Lecture 5: Bone Development & Trunk Anatomy Lecture 2: Fossil Record Segmentation Cyclic genescreate segme ntation clock for somite production Final #s 4 occipital 8
Module F SKELETAL SYSTEM & ARTICULATIONS
 Module F SKELETAL SYSTEM & ARTICULATIONS Topic from General functions of bone & the skeletal system Structural components microscopic anatomy Structural components gross anatomy Physiology of embryonic
Module F SKELETAL SYSTEM & ARTICULATIONS Topic from General functions of bone & the skeletal system Structural components microscopic anatomy Structural components gross anatomy Physiology of embryonic
Vertebrate Body Organization
 Vertebrate Body Organization Digestive tube suspended in coelom from mouth to anus Body supported by internal skeleton of jointed bones Vertebrae and Cranium protects nervous system Diaphragm divides coelom
Vertebrate Body Organization Digestive tube suspended in coelom from mouth to anus Body supported by internal skeleton of jointed bones Vertebrae and Cranium protects nervous system Diaphragm divides coelom
8/25/2014 JOINTS. The Skeletal System. Axial Skeleton STRUCTURE AND FUNCTION:
 STRUCTURE AND FUNCTION: JOINTS The Skeletal System Made up of the numerous bones of the human body Gives support and framework to the body Protects vital organs Manufactures blood cells Storage of calcium
STRUCTURE AND FUNCTION: JOINTS The Skeletal System Made up of the numerous bones of the human body Gives support and framework to the body Protects vital organs Manufactures blood cells Storage of calcium
Animal Systems: The Musculoskeletal System
 Animal Systems: The Musculoskeletal System Tissues, Organs, and Systems of Living Things Cells, Cell Division, and Animal Systems and Plant Systems Cell Specialization Human Systems The Digestive The Circulatory
Animal Systems: The Musculoskeletal System Tissues, Organs, and Systems of Living Things Cells, Cell Division, and Animal Systems and Plant Systems Cell Specialization Human Systems The Digestive The Circulatory
9/3/2013 JOINTS. Joints. Axial Skeleton STRUCTURE AND FUNCTION:
 STRUCTURE AND FUNCTION: JOINTS Joints A connection between 2 or more bones A pivot point for bony motion The features of the joint help determine The ROM freedom Functional potential of the joint Axial
STRUCTURE AND FUNCTION: JOINTS Joints A connection between 2 or more bones A pivot point for bony motion The features of the joint help determine The ROM freedom Functional potential of the joint Axial
UNIT 4 - SKELETAL SYSTEM LECTURE NOTES
 UNIT 4 - SKELETAL SYSTEM LECTURE NOTES 4.01 FUNCTIONS OF THE SKELETAL SYSTEM A. Support 1. Provides a framework for the body. 2. Supports soft tissue. 3. Serves as a point of attachment for ligaments,
UNIT 4 - SKELETAL SYSTEM LECTURE NOTES 4.01 FUNCTIONS OF THE SKELETAL SYSTEM A. Support 1. Provides a framework for the body. 2. Supports soft tissue. 3. Serves as a point of attachment for ligaments,
Section B: Epithelial Tissue 1. Where are epithelial tissues found within the body? 2. What are the functions of the epithelial tissues?
 Tissue worksheet Name Section A: Intro to Histology Cells are the smallest units of life. In complex organisms, cells group together with one another based on similar structure and function to form tissues.
Tissue worksheet Name Section A: Intro to Histology Cells are the smallest units of life. In complex organisms, cells group together with one another based on similar structure and function to form tissues.
THE SKELETAL & ARTICULAR SYSTEMS. The Bones & Joints
 THE SKELETAL & ARTICULAR SYSTEMS The Bones & Joints CLOSE YOUR POWERPOINT HANDOUTS!! Think-Pair-Share: Why do we need bones? Try to think of 3 reasons. THE SKELETAL SYSTEM Is made up of numerous bones
THE SKELETAL & ARTICULAR SYSTEMS The Bones & Joints CLOSE YOUR POWERPOINT HANDOUTS!! Think-Pair-Share: Why do we need bones? Try to think of 3 reasons. THE SKELETAL SYSTEM Is made up of numerous bones
Skeletal, Muscular, and Integumentary Systems
 Chapter 36 Skeletal, Muscular, and Integumentary Systems Section 36 1 The Skeletal System (pages 921 925) This section describes the skeletal system and its functions. Introduction (page 921) 1. What forms
Chapter 36 Skeletal, Muscular, and Integumentary Systems Section 36 1 The Skeletal System (pages 921 925) This section describes the skeletal system and its functions. Introduction (page 921) 1. What forms
STRUCTURE AND FUNCTION: JOINTS
 STRUCTURE AND FUNCTION: JOINTS Joints A connection between 2 or more bones A pivot point for bony motion The features of the joint help determine The ROM Degrees of freedom Functional potential of the
STRUCTURE AND FUNCTION: JOINTS Joints A connection between 2 or more bones A pivot point for bony motion The features of the joint help determine The ROM Degrees of freedom Functional potential of the
Human Anatomy & Physiology I with Dr. Hubley. Practice Exam 1
 Human Anatomy & Physiology I with Dr. Hubley Practice Exam 1 1. Which definition is the best definition of the term gross anatomy? a. The study of cells. b. The study of tissues. c. The study of structures
Human Anatomy & Physiology I with Dr. Hubley Practice Exam 1 1. Which definition is the best definition of the term gross anatomy? a. The study of cells. b. The study of tissues. c. The study of structures
The Tissue Level of Organization
 The Tissue Level of Organization Tissues A groups of similar cells, usually having similar embryonic origin and specialized function Histology: the study of tissues Four general types Epithelial Muscle
The Tissue Level of Organization Tissues A groups of similar cells, usually having similar embryonic origin and specialized function Histology: the study of tissues Four general types Epithelial Muscle
Chetek-Weyerhaeuser High School
 Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Skeletal system. 2012 Pearson Education, Inc.
 NURS1004 Week 6 Part I Prepared by Didy Button Skeletal system An Introduction to the Skeletal System The Skeletal System Includes: Bones of the skeleton Cartilages, ligaments, and connective tissues 6-1
NURS1004 Week 6 Part I Prepared by Didy Button Skeletal system An Introduction to the Skeletal System The Skeletal System Includes: Bones of the skeleton Cartilages, ligaments, and connective tissues 6-1
North Bergen School District Benchmarks
 Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
The Functions of the Skeletal System
 OpenStax-CNX module: m46341 1 The Functions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
OpenStax-CNX module: m46341 1 The Functions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
Anatomy and Physiology Warm up questions Fall 2013
 Anatomy and Physiology Warm up questions Fall 2013 QUESTION POSSIBLE ANSWERS : Chapter 1 Introduction and Regions Chapter 2 Chemistry I can name systems of the I can identify regions of the I can describe
Anatomy and Physiology Warm up questions Fall 2013 QUESTION POSSIBLE ANSWERS : Chapter 1 Introduction and Regions Chapter 2 Chemistry I can name systems of the I can identify regions of the I can describe
Biology 13A Lab #3: Cells and Tissues
 Biology 13A Lab #3: Cells and Tissues Lab #3 Table of Contents: Expected Learning Outcomes.... 28 Introduction...... 28 Activity 1: Eukaryotic Cell Structure... 29 Activity 2: Perspectives on Tissue Preparations.
Biology 13A Lab #3: Cells and Tissues Lab #3 Table of Contents: Expected Learning Outcomes.... 28 Introduction...... 28 Activity 1: Eukaryotic Cell Structure... 29 Activity 2: Perspectives on Tissue Preparations.
Skeletal System -Training Handout Karen L. Lancour National Rules Committee Chairman Life Science
 Skeletal System -Training Handout Karen L. Lancour National Rules Committee Chairman Life Science INTERACTION OF SKELETAL AND MUSCULAR SYSTEMS: Skeletal and Muscular systems works together to allow movement
Skeletal System -Training Handout Karen L. Lancour National Rules Committee Chairman Life Science INTERACTION OF SKELETAL AND MUSCULAR SYSTEMS: Skeletal and Muscular systems works together to allow movement
SKELETON AND JOINTS G.C.S.E. PHYSICAL EDUCATION. Unit 1. Factors Affecting Participation and Performance. G.C.S.E. P.E. Teacher:.
 G.C.S.E. PHYSICAL EDUCATION Unit 1 Factors Affecting Participation and Performance SKELETON AND JOINTS Name: G.C.S.E. P.E. Teacher:. By the end of this booklet you should be able to: Understand what the
G.C.S.E. PHYSICAL EDUCATION Unit 1 Factors Affecting Participation and Performance SKELETON AND JOINTS Name: G.C.S.E. P.E. Teacher:. By the end of this booklet you should be able to: Understand what the
Level 2 Certificate in Fitness Instructing Unit 1: Anatomy and Physiology
 Level 2 Certificate in Fitness Instructing Unit 1: Anatomy and Physiology These questions have been compiled based on the information available for the above qualification and unit. This mock should be
Level 2 Certificate in Fitness Instructing Unit 1: Anatomy and Physiology These questions have been compiled based on the information available for the above qualification and unit. This mock should be
Anatomy and Physiology of Domestic Animals
 Anatomy and Physiology of Domestic Animals 6 Bones and skeletal system Contents Bones Introduction Classification of Bones Bone Structure Gross Anatomy Microscopic Anatomy of Bone Chemical Composition
Anatomy and Physiology of Domestic Animals 6 Bones and skeletal system Contents Bones Introduction Classification of Bones Bone Structure Gross Anatomy Microscopic Anatomy of Bone Chemical Composition
X-Plain Vertebral Compression Fractures Reference Summary
 X-Plain Vertebral Compression Fractures Reference Summary Introduction Back pain caused by a vertebral compression fracture, or VCF, is a common condition that affects thousands of people every year. A
X-Plain Vertebral Compression Fractures Reference Summary Introduction Back pain caused by a vertebral compression fracture, or VCF, is a common condition that affects thousands of people every year. A
Human Body Vocabulary Words Week 1
 Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
Divisions of the Skeletal System
 OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
Definition: A joint or articulation is a place in the body where two bones come together.
 Definition: A joint or articulation is a place in the body where two bones come together. CLASSES OF JOINTS. 1. Joints are classified according to how the bones are held together. 2. The three types of
Definition: A joint or articulation is a place in the body where two bones come together. CLASSES OF JOINTS. 1. Joints are classified according to how the bones are held together. 2. The three types of
Skeletal Systems. General Properties of Skeletons. Molecular rope Pack closely together due to glycine content Not elastic so good for support
 Skeletal Systems General Properties of Skeletons Connective tissues important in support Collagen/tropocollagen molecules Molecular rope Pack closely together due to glycine content Not elastic so good
Skeletal Systems General Properties of Skeletons Connective tissues important in support Collagen/tropocollagen molecules Molecular rope Pack closely together due to glycine content Not elastic so good
Reavis High School Anatomy and Physiology Curriculum Snapshot
 Reavis High School Anatomy and Physiology Curriculum Snapshot Unit 1: Introduction to the Human Body 10 days As part of this unit, students will define anatomy, physiology, and pathology. They will identify
Reavis High School Anatomy and Physiology Curriculum Snapshot Unit 1: Introduction to the Human Body 10 days As part of this unit, students will define anatomy, physiology, and pathology. They will identify
Biology 141 Anatomy and Physiology I
 Fall 2016 Biology 141 Anatomy and Physiology I COURSE OUTLINE Faculty Name: Enter Faculty Name Here Program Head: Enter Program Head Here Dean s Review: Dean s Signature: Date Reviewed: / / Revised: Fall
Fall 2016 Biology 141 Anatomy and Physiology I COURSE OUTLINE Faculty Name: Enter Faculty Name Here Program Head: Enter Program Head Here Dean s Review: Dean s Signature: Date Reviewed: / / Revised: Fall
Introduction to Anatomy and Physiology: Tissues and Integumentary System. Biology 105 Lecture 7 Chapter 4
 Introduction to Anatomy and Physiology: Tissues and Integumentary System Biology 105 Lecture 7 Chapter 4 Outline I. Tissues A. Epithelial B. Connective C. Muscle D. Nervous tissues II. Cell-to-cell contact
Introduction to Anatomy and Physiology: Tissues and Integumentary System Biology 105 Lecture 7 Chapter 4 Outline I. Tissues A. Epithelial B. Connective C. Muscle D. Nervous tissues II. Cell-to-cell contact
To retain their shapes, all organisms need some type of structural
 36 1 The Skeletal System To retain their shapes, all organisms need some type of structural support. Unicellular organisms have a cytoskeleton that provides structural support. In multicellular animals,
36 1 The Skeletal System To retain their shapes, all organisms need some type of structural support. Unicellular organisms have a cytoskeleton that provides structural support. In multicellular animals,
Lesson Aim To explain the human body at a microscopic level, including the structure and function of cells, tissues and membranes.
 LESSON 1. CELLS & TISSUES Lesson Aim To explain the human body at a microscopic level, including the structure and function of cells, tissues and membranes. THE CELL All living matter is composed of functional
LESSON 1. CELLS & TISSUES Lesson Aim To explain the human body at a microscopic level, including the structure and function of cells, tissues and membranes. THE CELL All living matter is composed of functional
LOCOMOTION AND MOVEMENT
 UNIT - HUMAN PHYSIOLOGY Chapter 18 LOCOMOTION AND MOVEMENT Movement is an important feature of living organism. Both the microbes and macrobes show wide range of movements. The movements results in change
UNIT - HUMAN PHYSIOLOGY Chapter 18 LOCOMOTION AND MOVEMENT Movement is an important feature of living organism. Both the microbes and macrobes show wide range of movements. The movements results in change
Biology 105 Human Biology PRACTICE MIDTERM EXAM 1. Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 4 The Tissue Level of Organization
 Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 4 The Tissue Level of Organization Multiple-Choice Questions 1) The four main types of tissues include A) epithelium. B) muscle. C) nerve.
Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 4 The Tissue Level of Organization Multiple-Choice Questions 1) The four main types of tissues include A) epithelium. B) muscle. C) nerve.
DEVELOPMENT AND GROWTH OF THE MANDIBLE
 2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
Tissues (Histology) Ch. 3 Human Anatomy lecture
 I. Histology the study of tissues A. 4 basic tissue types epithelial connective muscle nervous Tissues (Histology) Ch. 3 Human Anatomy lecture B. Usually found in combinations to form organs. C. As you
I. Histology the study of tissues A. 4 basic tissue types epithelial connective muscle nervous Tissues (Histology) Ch. 3 Human Anatomy lecture B. Usually found in combinations to form organs. C. As you
Tissue Types. 1. Epithelial Tissue (or epithelium) is the lining, covering, and glandular tissue of the body
 Tissue Types A. Tissues 1. Tissues: groups of cells similar in structure and function 2. Four Types of Tissues: a. Epithelium: for covering b. Connective Tissue: for support c. Muscle: for movement d.
Tissue Types A. Tissues 1. Tissues: groups of cells similar in structure and function 2. Four Types of Tissues: a. Epithelium: for covering b. Connective Tissue: for support c. Muscle: for movement d.
Anatomy and Physiology
 Anatomy and Physiology UNIT I: Introduction to Anatomy and Physiology The student will demonstrate an understanding of the anatomic and physiological basis of life and the ability to explain the interdependence
Anatomy and Physiology UNIT I: Introduction to Anatomy and Physiology The student will demonstrate an understanding of the anatomic and physiological basis of life and the ability to explain the interdependence
Laboratory 3 Histology
 Laboratory 3 Histology Goals: For epithelial tissues: o discuss the major features; o classify based on simple/stratified and squamous/cubodial/columnar; o identify each type by microscopy; o identify
Laboratory 3 Histology Goals: For epithelial tissues: o discuss the major features; o classify based on simple/stratified and squamous/cubodial/columnar; o identify each type by microscopy; o identify
Paramedic Program Anatomy and Physiology Study Guide
 Paramedic Program Anatomy and Physiology Study Guide Define the terms anatomy and physiology. List and discuss in order of increasing complexity, the body from the cell to the whole organism. Define the
Paramedic Program Anatomy and Physiology Study Guide Define the terms anatomy and physiology. List and discuss in order of increasing complexity, the body from the cell to the whole organism. Define the
CENTRAL TEXAS COLLEGE BIOL 2401 ANATOMY AND PHYSIOLOGY I INSTRUCTOR: OFFICE HOURS:
 CENTRAL TEXAS COLLEGE BIOL 2401 ANATOMY AND PHYSIOLOGY I Semester Hours Credit: 4 INSTRUCTOR: OFFICE HOURS: I. INTRODUCTION A. Anatomy and Physiology I is the study of the parts of the living organisms
CENTRAL TEXAS COLLEGE BIOL 2401 ANATOMY AND PHYSIOLOGY I Semester Hours Credit: 4 INSTRUCTOR: OFFICE HOURS: I. INTRODUCTION A. Anatomy and Physiology I is the study of the parts of the living organisms
What are Minerals. Lecture 13: Minerals. Trace versus Major Minerals. Minerals are elements, can be found on the periodic table
 Lecture 13: Minerals What are Minerals Minerals are elements, can be found on the periodic table Inorganic (in chemical sense) Nutrition 150 Shallin Busch, Ph.D. Not broken down during digestion nor destroyed
Lecture 13: Minerals What are Minerals Minerals are elements, can be found on the periodic table Inorganic (in chemical sense) Nutrition 150 Shallin Busch, Ph.D. Not broken down during digestion nor destroyed
What Each Vitamin & Mineral Does In Your Body. Vitamin A
 What Each Vitamin & Mineral Does In Your Body Vitamin A Prevents skin disorders, such as acne, wrinkling and age spots. Enhances the immune system protects against colds, flu, and infections to kidney,
What Each Vitamin & Mineral Does In Your Body Vitamin A Prevents skin disorders, such as acne, wrinkling and age spots. Enhances the immune system protects against colds, flu, and infections to kidney,
Classification of bones Any bone may be classified into one of the following groups:
 Skeletal system This system is made up of hard tissues like bone and cartilages. This system gives form and shape to animal body The skeleton of a living animal is made up living structures of bones. The
Skeletal system This system is made up of hard tissues like bone and cartilages. This system gives form and shape to animal body The skeleton of a living animal is made up living structures of bones. The
Investigating the Human Body On-site student activities: Years 7-8 Investigating the Human Body On-site student activities Years 7 8
 Investigating the Human Body On-site student activities Years 7 8 Student activity (and record) sheets have been developed with alternative themes for students to use as guides and focus material during
Investigating the Human Body On-site student activities Years 7 8 Student activity (and record) sheets have been developed with alternative themes for students to use as guides and focus material during
Activity: Can You Identify the Age?
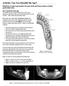 Activity: Can You Identify the Age? Skeletons are good age markers because teeth and bones mature at fairly predictable rates. How Teeth Reveal Age For toddler to age 21, teeth are the most accurate age
Activity: Can You Identify the Age? Skeletons are good age markers because teeth and bones mature at fairly predictable rates. How Teeth Reveal Age For toddler to age 21, teeth are the most accurate age
Pseudohypoparathyroidism: A Variation on the Theme of Hypoparathyroidism
 Pseudohypoparathyroidism: A Variation on the Theme of Hypoparathyroidism Amanda Tencza MS IV 1 and Michael A. Levine, MD 2 1 Cleveland Clinic Lerner College of Medicine of Case Western Reserve University
Pseudohypoparathyroidism: A Variation on the Theme of Hypoparathyroidism Amanda Tencza MS IV 1 and Michael A. Levine, MD 2 1 Cleveland Clinic Lerner College of Medicine of Case Western Reserve University
ANATOMY AND PHYSIOLOGY SYLLABUS FOR COMMUNITY COLLEGES. Leslie Dawn Schulz, B.S. Thesis Prepared for the Degree of MASTER OF SCIENCE
 ANATOMY AND PHYSIOLOGY SYLLABUS FOR COMMUNITY COLLEGES Leslie Dawn Schulz, B.S. Thesis Prepared for the Degree of MASTER OF SCIENCE UNIVERSITY OF NORTH TEXAS May 2000 APPROVED: Gerard A O Donovan, Major
ANATOMY AND PHYSIOLOGY SYLLABUS FOR COMMUNITY COLLEGES Leslie Dawn Schulz, B.S. Thesis Prepared for the Degree of MASTER OF SCIENCE UNIVERSITY OF NORTH TEXAS May 2000 APPROVED: Gerard A O Donovan, Major
Structure and Function of the Musculoskeletal System Professor Alan Hedge DEA 3250/6510
 Structure and Function of the Musculoskeletal System Professor Alan Hedge DEA 3250/6510 Functions of the Musculoskeletal System Support and protect the body and its organs. Provide motion. Musculoskeletal
Structure and Function of the Musculoskeletal System Professor Alan Hedge DEA 3250/6510 Functions of the Musculoskeletal System Support and protect the body and its organs. Provide motion. Musculoskeletal
RAD 223. Radiography physiology. Lecture Notes. First lecture: Cell and Tissue
 RAD 223 Radiography physiology Lecture Notes First lecture: Cell and Tissue Physiology: the word physiology derived from a Greek word for study of nature. It is the study of how the body and its part work
RAD 223 Radiography physiology Lecture Notes First lecture: Cell and Tissue Physiology: the word physiology derived from a Greek word for study of nature. It is the study of how the body and its part work
Human Bones BROWARD COUNTY ELEMENTARY SCIENCE BENCHMARK PLAN ACTIVITY ASSESSMENT OPPORTUNITIES. Grade 4 Quarter 3 Activity 21
 activity 21 Human Bones BROWARD COUNTY ELEMENTARY SCIENCE BENCHMARK PLAN Grade 4 Quarter 3 Activity 21 SC.F.1.2.1 The student knows that the human body is made of systems with structures and functions
activity 21 Human Bones BROWARD COUNTY ELEMENTARY SCIENCE BENCHMARK PLAN Grade 4 Quarter 3 Activity 21 SC.F.1.2.1 The student knows that the human body is made of systems with structures and functions
Essentials of Human Anatomy & Physiology. 7 th edition Marieb, Elaine, 2003. Chapters 10-11. Lab Manual, 2 nd edition and coloring book, 7 th edition
 Topic/Unit: Anatomy & Physiology Circulatory System Curricular Goals/ Learning Outcomes: Students will be able to identify the composition of blood and its function. Students will be able to differentiate
Topic/Unit: Anatomy & Physiology Circulatory System Curricular Goals/ Learning Outcomes: Students will be able to identify the composition of blood and its function. Students will be able to differentiate
BIO 201 ANATOMY AND PHYSIOLOGY I with LAB
 BIO 201 ANATOMY AND PHYSIOLOGY I with LAB (Title change ONLY Oct. 2013) Presented and Approved: January 12, 2012 Effective: 2012-13 FA Prefix & Number BIO 201 Course Title: Anatomy and Physiology I Purpose
BIO 201 ANATOMY AND PHYSIOLOGY I with LAB (Title change ONLY Oct. 2013) Presented and Approved: January 12, 2012 Effective: 2012-13 FA Prefix & Number BIO 201 Course Title: Anatomy and Physiology I Purpose
Anatomical Terminology: Planes Axes Direction (Text Pg 2 3)
 Anatomical Terminology: Planes Axes Direction (Text Pg 2 3) Anatomy: The structure and organization of the body and its organs. From Greek Origin: Anatome dissection Physiology: The function of the body
Anatomical Terminology: Planes Axes Direction (Text Pg 2 3) Anatomy: The structure and organization of the body and its organs. From Greek Origin: Anatome dissection Physiology: The function of the body
Our Human Body On-site student activities Years 5 6
 Our Human Body On-site student activities Years 5 6 Our Human Body On-site student activities: Years 5-6 Student activity (and record) sheets have been developed with alternative themes for students to
Our Human Body On-site student activities Years 5 6 Our Human Body On-site student activities: Years 5-6 Student activity (and record) sheets have been developed with alternative themes for students to
Introduction to Animal Systems
 Human Body Systems Introduction to Animal Systems Recurring Themes in Biology 1. Correlation between structure and function( seen at many levels) 2. Life is organized at many levels from Smallest ----
Human Body Systems Introduction to Animal Systems Recurring Themes in Biology 1. Correlation between structure and function( seen at many levels) 2. Life is organized at many levels from Smallest ----
Regulation of Metabolism. By Dr. Carmen Rexach Physiology Mt San Antonio College
 Regulation of Metabolism By Dr. Carmen Rexach Physiology Mt San Antonio College Energy Constant need in living cells Measured in kcal carbohydrates and proteins = 4kcal/g Fats = 9kcal/g Most diets are
Regulation of Metabolism By Dr. Carmen Rexach Physiology Mt San Antonio College Energy Constant need in living cells Measured in kcal carbohydrates and proteins = 4kcal/g Fats = 9kcal/g Most diets are
Development of Teeth
 Development of Teeth Dr. Khaldoun Darwich Specialist in Oral and Maxillo-Facial Surgery Hamburg University PhD Hamburg University Academic Teacher - Department of OMF Surgery in Damascus University Instructor
Development of Teeth Dr. Khaldoun Darwich Specialist in Oral and Maxillo-Facial Surgery Hamburg University PhD Hamburg University Academic Teacher - Department of OMF Surgery in Damascus University Instructor
Secondary dentition permanent teeth - 32. Primary dentition deciduous teeth - 20
 Department of Histology and Embryology, P. J. Šafárik University, Medical Faculty, Košice DEVELOPMENT OF TEETH: Sylabus for foreign students Dental medicine Author: doc. MVDr. Iveta Domoráková, PhD. Primary
Department of Histology and Embryology, P. J. Šafárik University, Medical Faculty, Košice DEVELOPMENT OF TEETH: Sylabus for foreign students Dental medicine Author: doc. MVDr. Iveta Domoráková, PhD. Primary
Lab Exercise 4. Epithelial Tissues. Connective Tissue Proper. What you need to be able to do on the exam after completing this lab exercise:
 Lab Exercise 4 Epithelial Tissues Connective Tissue Proper Textbook Reference: See Chapter 4 What you need to be able to do on the exam after completing this lab exercise: Be able to identify each type
Lab Exercise 4 Epithelial Tissues Connective Tissue Proper Textbook Reference: See Chapter 4 What you need to be able to do on the exam after completing this lab exercise: Be able to identify each type
The Search for the Missing Bones
 The Magic School Bus A Science Chapter Book #2 The Search for the Missing Bones Lapbook by Amy Yee. Yee Shall Know http:///www.yeeshallknow.com Lapbook Basics Follow the instructions in the following page(s)
The Magic School Bus A Science Chapter Book #2 The Search for the Missing Bones Lapbook by Amy Yee. Yee Shall Know http:///www.yeeshallknow.com Lapbook Basics Follow the instructions in the following page(s)
UNIT 2 - CHAPTER 7: SKELETAL SYSTEM. 1. Classify bones according to their shapes, and name an example from each group. (p. 200)
 LEARNING OUTCOMES: 7.1 Bone Shape and Structure UNIT 2 - CHAPTER 7: SKELETAL SYSTEM 1. Classify bones according to their shapes, and name an example from each group. (p. 200) 2. Describe the macroscopic
LEARNING OUTCOMES: 7.1 Bone Shape and Structure UNIT 2 - CHAPTER 7: SKELETAL SYSTEM 1. Classify bones according to their shapes, and name an example from each group. (p. 200) 2. Describe the macroscopic
67 The Human Skeleton
 67 The Human Skeleton Skull SCIENCE EXPLORER Focus on Life Science Prentice-Hall, Inc. Clavicle (collarbone) Scapula (shoulder blade) Carpals Metacarpals Phalanges Femur Tibia Humerus Ulna Sternum (breastbone)
67 The Human Skeleton Skull SCIENCE EXPLORER Focus on Life Science Prentice-Hall, Inc. Clavicle (collarbone) Scapula (shoulder blade) Carpals Metacarpals Phalanges Femur Tibia Humerus Ulna Sternum (breastbone)
Cardiovascular System. Blood Components
 Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
2161-1 - Page 1. Name: 1) Choose the disease that is most closely related to the given phrase. Questions 10 and 11 refer to the following:
 Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Integration and Coordination of the Human Body. Nervous System
 I. General Info Integration and Coordination of the Human Body A. Both the and system are responsible for maintaining 1. Homeostasis is the process by which organisms keep internal conditions despite changes
I. General Info Integration and Coordination of the Human Body A. Both the and system are responsible for maintaining 1. Homeostasis is the process by which organisms keep internal conditions despite changes
THE HUMAN BODY SYSTEMS
 Name Period Date THE HUMAN BODY SYSTEMS System Function Diagram Major Organs Digestive 1. take in food (ingestion) 2. digest food into smaller molecules and absorb nutrients 3. remove undigestable food
Name Period Date THE HUMAN BODY SYSTEMS System Function Diagram Major Organs Digestive 1. take in food (ingestion) 2. digest food into smaller molecules and absorb nutrients 3. remove undigestable food
ORGAN SYSTEMS OF THE BODY
 ORGAN SYSTEMS OF THE BODY DEFINITIONS AND CONCEPTS A. Organ a structure made up of two or more kinds of tissues organized in such a way that they can together perform a more complex function that can any
ORGAN SYSTEMS OF THE BODY DEFINITIONS AND CONCEPTS A. Organ a structure made up of two or more kinds of tissues organized in such a way that they can together perform a more complex function that can any
Histology. Epithelial Tissue
 Histology Epithelial Tissue Epithelial Tissue Lines internal and external body surfaces Forms glands Epithelial Tissue Little extracellular matrix Attached on one side Avascular Basement membrane Apical
Histology Epithelial Tissue Epithelial Tissue Lines internal and external body surfaces Forms glands Epithelial Tissue Little extracellular matrix Attached on one side Avascular Basement membrane Apical
12.1: The Function of Circulation page 478
 12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
Exploring Creation with Advanced Biology ~ Schedule for 2015-2016 Apologia ~ Exploring Creation with Biology ~ Module 1 (Week 1) Date:
 Apologia ~ Exploring Creation with Biology ~ Module 1 (Week 1) Mon., Aug. 31 Tue., Sep. 1 Wed., Sept. 2 Thurs., Sept. 3 Fri., Sept. 4 Reading Pgs. 1-4; Introduction, Heart of the matter, Pgs. 5-8; Organization
Apologia ~ Exploring Creation with Biology ~ Module 1 (Week 1) Mon., Aug. 31 Tue., Sep. 1 Wed., Sept. 2 Thurs., Sept. 3 Fri., Sept. 4 Reading Pgs. 1-4; Introduction, Heart of the matter, Pgs. 5-8; Organization
Week 30. Water Balance and Minerals
 Week 30 Water Balance and Minerals Water: more vital to life than food involved in almost every body function is not stored--excreted daily largest single constituent of the human body, averaging 60% of
Week 30 Water Balance and Minerals Water: more vital to life than food involved in almost every body function is not stored--excreted daily largest single constituent of the human body, averaging 60% of
CHAPTER 9 BODY ORGANIZATION
 CHAPTER 9 BODY ORGANIZATION Objectives Identify the meaning of 10 or more terms relating to the organization of the body Describe the properties of life Describe the function for the structures of the
CHAPTER 9 BODY ORGANIZATION Objectives Identify the meaning of 10 or more terms relating to the organization of the body Describe the properties of life Describe the function for the structures of the
Forensic Anthropology Forensic Science
 Forensic Anthropology Forensic Science A Closer Look At Bones Science Unit Years 9/10 Forensic Science Unit: Forensic Anthropology Years 9/10 6-8 weeks Forensic anthropology is about obtaining evidence
Forensic Anthropology Forensic Science A Closer Look At Bones Science Unit Years 9/10 Forensic Science Unit: Forensic Anthropology Years 9/10 6-8 weeks Forensic anthropology is about obtaining evidence
The Skeletal System. This Version Last Updated On Friday, March 27, 2009
 The Skeletal System This Version Last Updated On Friday, March 27, 2009 Note on vocabulary: Throughout the unit, useful vocabulary words, both technical and non-technical have been placed in BOLD print.
The Skeletal System This Version Last Updated On Friday, March 27, 2009 Note on vocabulary: Throughout the unit, useful vocabulary words, both technical and non-technical have been placed in BOLD print.
The Endocrine System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 9 The Endocrine System Slides 9.1 9.48 Lecture Slides in PowerPoint by Jerry L. Cook The Endocrine System Second messenger
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 9 The Endocrine System Slides 9.1 9.48 Lecture Slides in PowerPoint by Jerry L. Cook The Endocrine System Second messenger
Name Class Date Laboratory Investigation 24A Chapter 24A: Human Skin
 Name Class Date Laboratory Investigation 24A Chapter 24A: Human Skin Human Anatomy & Physiology: Integumentary System You may refer to pages 386-394 in your textbook for a general discussion of the integumentary
Name Class Date Laboratory Investigation 24A Chapter 24A: Human Skin Human Anatomy & Physiology: Integumentary System You may refer to pages 386-394 in your textbook for a general discussion of the integumentary
