Chapter 21 Fractures of the Upper Thoracic Spine: Approaches and Surgical Management
|
|
|
- Blaise Bradford
- 9 years ago
- Views:
Transcription
1 Chapter 21 Fractures of the Upper Thoracic Spine: Approaches and Surgical Management Sean D Christie, M.D., John Song, M.D., and Richard G Fessler, M.D., Ph.D. INTRODUCTION Fractures occurring in the thoracic region account for approximately 17 to 23% of all traumatic spinal fractures (1), with 22% of traumatic spinal fractures occurring between T1 and T4 (16). More than half of these fractures result in neurological injury, and almost three-quarters of those impaired suffer from complete paralysis. Obtaining surgical access to the anterior vertebral elements of the upper thoracic vertebrae (T1 T6) presents a unique anatomic challenge. The thoracic cage, which narrows significantly as it approaches the thoracic inlet, has an intimate association between the vertebral column and the superior mediastinal structures. The supraclavicular, transmanubrial, transthoracic, and lateral parascapular extrapleural approaches each provide access to the anterior vertebral elements of the upper thoracic vertebrae. However, each of these approaches has distinct advantages and disadvantages and their use should be tailored to each individual patient s situation. This chapter reviews these surgical approaches. Traditional posterior approaches are illustrated in Figure 21.1, but will not be discussed in depth here. ANATOMIC CONSIDERATIONS AND STABILITY The upper thoracic spine possesses unique anatomic and biomechanical properties. The anterior aspects of the vertebral bodies are smaller than the posterior aspects, which contribute to the physiological kyphosis present in this region of the spine. Furthermore, this orientation results in a ventrally positioned axis of rotation, predisposing this region to compression injuries. The combination and interaction of the vertebral bodies, ribs, and sternum increase the inherent biomechanical stability of this segment of the spine to 2 to 3 times that of the thoracolumbar junction. The costovertebral joints play an important role in this stability, forming a bony cylindrical shell (1, 15) that increases the rigidity of the upper thoracic spine. The enhanced stability in this region requires that greater forces be applied to the spine to generate significant fractures. Therefore, fracture dislocations occur less commonly in the upper thoracic spine; however, they are more likely to result in complete neurological injury because the size of the spinal cord approximates that of the spinal canal, and because this region of the spinal cord is thought to have a tenuous blood supply (6). SURGICAL CHALLENGES AND GOALS OF TREATMENT The unique anatomic relationships also create challenges for the surgeon approaching the upper thoracic spine. Other anatomic factors affecting surgical approaches include the narrow thoracic inlet, the contents of the mediastinum, the lungs, and the limitations related to the shoulder and scapular musculature. The nature of the fracture also plays a role in dictating the approach. Figures 21.2 and 21.3 outline a treatment algorithm for compression and burst fractures, respectively. Furthermore, one must be attentive to the goals of the procedure: to decompress the spinal cord, to realign and stabilize the spine, and to maximize physical function. These factors must
2 be considered when tailoring a surgical approach to an individual patient. SUPRACLAVICULAR APPROACH Brunig (4) and Jonnesco (10) independently described this approach in 1923, which initially found favor in the treatment of spastic paralysis (13), Raynaud s Disease (8), and thoracic sympathectomy (12). After adequate general endotracheal anesthesia, a transverse skin incision is made, approximately 2 cm above the clavicle, extending from the midline past the lateral border of the sternocleidomastoid (SCM) muscle. We use a leftsided approach to minimize the risk of injuring the recurrent laryngeal nerve. The superficial fascia and the platysma muscle are divided and undermined. The anterior and external jugular veins may be ligated and cut for exposure. The superficial layer of the deep cervical fascia is then opened along the anterior border of SCM. The SCM is isolated and transected, reflecting both heads rostrally. The medial third of the clavicle is cut and disarticulated from the manubrium, while preserving the subclavian vein. The omohyoid and sternohyoid muscles must be divided to reveal the anterior scalene muscle along with the associated phrenic nerve. The carotid artery is then palpated and retracted laterally. The standard cervical anatomic plane, between the trachea and esophagus medially and the carotid sheath laterally, is opened. Care must be taken to protect the recurrent laryngeal nerve, in the tracheo-esophageal groove; the phrenic nerve, along the anterior aspect of the anterior scalene muscle; and the thoracic duct, located laterally at the junction of the internal jugular and subclavian veins. After adequate exposure has been obtained, the prevertebral fascia is opened in the midline, and the anatomic level may be confirmed radiologically with the use of a 25-gauge needle. Dissecting and elevating the longus colli muscles enables the placement of retractors to complete the exposure. The operating microscope may then be brought in to facilitate decompression, if needed, before instrumentation. At the end of the case, the retractors are removed and the wound is irrigated copiously with Bacitracin solution. A Jackson-Pratt drain may be left in place if there is any doubt regarding hemostasis. The strap muscles are reapproximated and the SCM is sutured back to the clavicular periosteum. The platysma and skin are closed in separate layers. If necessary, an external orthosis may be applied. TRANSMANUBRIAL APPROACH The addition of a transmanubrial or sternal splitting approach to the transclavicular will enhance the exposure to the cervicothoracic junction and the upper thoracic vertebrae. This approach was initially described by Sundaresan et al. in 1984 (14) and then later modified by Birch et al. in 1990 (2). After induction of general endotracheal anesthesia and sterile draping, a T-shaped incision is fashioned, as illustrated in Figure 21.4, with the horizontal limb 1 to 2 cm above the clavicle. The vertical limb of the incision extends halfway down the sternum. The superficial dissection is the same as described above. The left SCM is identified and its muscular heads dissected from their osseous attachments and reflected superiorly and laterally (Fig. 21.5). The ipsilateral strap muscles are also identified and sectioned as described above. The suprasternal space of Burns is developed via blunt dissection. This facilitates the subperiosteal dissection of the manubrium and the medial third of the clavicle. The omohyoid muscle is then divided to reveal the carotid sheath and
3 its contents. Caution is warranted to preserve the periosteum and the anterior aspect of the transthoracic fascia to prevent injury to the underlying innominate vessels and mediastinal structures. The medial third of the clavicle is removed using a high-speed drill or the Gigli saw, and the first costal cartilage is divided. The section of clavicle can then be disarticulated and removed. The high-speed drill is used to resect a rectangular portion of the manubrium. Alternatively, if an adequate subperiosteal dissection has been achieved beneath the manubrium and clavicle, these structures may be removed en bloc, with or without the SCM attachments (Fig. 21.6). The underlying vascular structures are identified and small venous tributaries of the innominate vein can be doubly ligated and sectioned. The thymus and any additional fat present in the superior mediastinum can be mobilized or resected. Working from the cephalad end of the exposure, the cervical fascia is opened as described above to reveal the prevertebral fascia. Attention must be paid to the numerous critical anatomic structures located in this region, particularly the carotid arteries, internal jugular vein, vagus nerve, subclavian artery, trachea, esophagus, the left recurrent laryngeal nerve, the thoracic duct, the thyrocervical trunk, the phrenic nerve, and the aortic arch and its branches, which limit the caudal exposure to approximately the level of the T3 vertebral body. After the prevertebral fascia is opened, the ventral aspect of the spine is identified and anatomic levels are confirmed with radiography or fluoroscopy. The longus colli muscles are dissected and elevated to facilitate placement of handheld or self-retaining retractors. At this point, the operating microscope may be brought into the field as necessary to aid in any decompression and realignment. After stabilization, the wound is irrigated copiously with Bacitracin irrigation. Should the pleura be violated, a chest tube is inserted through a separate stab wound and placed to suction or underwater seal. The manubrium and clavicle are replaced and fixed with mini-plates or stainless steel wires. The remainder of the closure proceeds as described above. When necessary, appropriate external immobilization is placed before extubation. Chapter 21, Fractures of the Upper Thoracic Spine:Approaches and Surgical Management (continued) TRANSTHORACIC APPROACH In detailing the management of a cohort of patients with Pott s disease, Hodgson et al. (9) were the first to describe the thoracotomy approach to the ventral spinal column. The spine may be either approached from the right or left side. Although the left side is generally favored for lesions in the lower thoracic spine and the thoracolumbar junction, a right-sided approach is often used for the upper thoracic spine because of the location of the great vessels. The patient is placed in the lateral decubitus position (Fig. 21.7). It is important to maintain the patient s orientation, keeping in mind the 3-D orientation of the spine. An axillary roll is placed to minimize the risk of brachial plexus injury. Fluoroscopy is used to confirm and mark the skin incision. The incision is made over the rib, one or two levels above the pathological vertebrae. A subperiosteal dissection is performed, protecting the inferior neurovascular bundle. The rib is then removed and the rib spreader is placed.
4 Either a retropleural or a transpleural approach to the spine may be used. The retropleural approach requires blunt dissection to mobilize the pleura off the posterior chest wall and vertebral bodies. This exposes the sympathetic chain, radicular vessels, rib, and the vertebral bodies. If the pleura is not violated, there is no need to place a chest tube at the conclusion of the case. The transpleural approach requires the lung to be retracted with a malleable or egg-beater retractor so that the spine can be visualized through the parietal pleura. This section of pleura must be incised and reflected back, thereby exposing the spine. Closure requires re-approximation of the parietal pleura and placement of a chest tube. Segmental vessels in the area of planned resection are removed early to minimize blood loss during the remainder of the procedure. The vessels are ligated close to the vertebral body to maintain the anastomoses more distally and minimize the risk of ischemic insult to the spinal cord. The proximal 2 to 3 cm of the head of the rib is sectioned using a high-speed drill or osteotome, and disarticulated. This reveals the intercostal nerve, which is an important landmark for the neural foramen and the pedicle. Identification of these structures facilitates an appreciation of the location of the thecal sac. Early identification of the thecal sac is imperative for safe resection of ventral pathology. The discs above and below the pathological vertebrae are incised and removal is in an anterior direction, away from the thecal sac. A high-speed drill with a cutting burr is used to remove the majority of the ventral aspect of the vertebral body. The anterior cortex and anterior longitudinal ligament are left intact, if possible. The posterior cortical margin is thinned down to an egg-shell thickness, and then can be fractured into the cavity created using curettes, thereby decompressing the spinal cord. An adequate decompression from pedicle to pedicle should be confirmed before beginning reconstruction. As noted, violation of the parietal pleura requires primary closure and placement of a chest tube. For the retropleural approach, the wound should be filled with saline to confirm that there are no occult leaks. Individual muscles are identified and closed in layers with either interrupted or running sutures. Early chest x-ray in the recovery room is warranted to exclude pneumothorax. LATERAL PARASCAPULAR EXTRAPLEURAL APPROACH The lateral parascapular extrapleural approach was first described in 1991 (7) as a modification of Capener s lateral rhachotomy approach (5) and the lateral extracavitary approach of Larson et al. (11), to deal with the limitations imposed by the shoulder girdle when these earlier approaches were used to approach the cervicothoracic junction. After induction of general, endotracheal anesthesia, the patient is placed in a prone position on the operating table with appropriate chest and hip padding. It is important to use a bed that allows free movement of the fluoroscope, not only in the region of interest but also either higher or lower to allow counting of vertebral bodies for localization. The arms can either be tucked at the patient s side or positioned abducted away from the body. By abducting the arm, the scapula is rotated forward and away from the midline spine, thus, providing more room for retraction of the paraspinal musculature. The incision must extend from three to four levels above the lesion to three to four levels below the lesion (Fig. 21.8). However, because of the relative tethering effect of the trapezius and levator scapulae muscles, a lesion located at T1 or T2 will require an incision that extends all the way up to approximately C3 or C4. Note that in the prone
5 position, before takedown of the trapezius and rhomboid musculature, the scapula covers the lateral one-half of the posterior rib cage. This position makes mobilization of the trapezius and rhomboid musculature imperative to exposure of the upper thoracic spine. In the initial dissection for exposure of this region of the spine, the spinous process insertions of the trapezius, rhomboid, serratus posterior superior, splenius capitis, and splenius cervicis muscles are taken down, as a group, for lateral retraction (Fig. 21.9). As these muscles are taken down, the scapula is released from its attachments to the spinous processes and rotates anterolaterally out of the operative field. This exposes the posterior and posterolateral rib cage for the remainder of the procedure. During this rotation, all neurovascular structures rotate with the scapula and are not at risk of injury. The entire group of erector spinae muscles and transversospinalis muscles can be dissected off the spinous processes, laminae, facets, and transverse processes as a single muscular mass (Fig ). The insertions of the iliocostalis thoracis muscles are also taken down. Control of the musculature in this way exposes all of the vertebral elements from the tip of the spinous processes to the tip of the transverse processes, as well as the costotransverse ligaments, the joints, and the ribs. After blunt dissection to remove the intercostal muscles and the costotransverse and radiate ligaments, each rib can be resected. This resection should extend 6 to 8 cm lateral to the junction of the rib with the transverse process. In the course of this procedure, a strip of intercostal musculature is isolated between each rib. This strip of musculature will contain the intercostal nerve, artery, and vein as they pass laterally between the internal intercostal membrane and the pleura, and then between the internal and innermost intercostal muscles. Immediately ventral to the intercostal bundle and the intercostal muscles lays the pleura. With blunt dissection, the pleura can be separated from these structures to expose the lateral vertebral elements. Following the intercostal bundle medially will enable identification of the neural foramen. Within the neural foramen, the dorsal root ganglion can be identified along with the gray and white rami communicantes, which course ventrally to the sympathetic chain and ganglia. The sympathetic chain is contained within a fascial compartment over the costovertebral articulation. This compartment is formed by fusion of the mediastinal and prevertebral fascia. The major portion of the ventral ramus of the first thoracic nerve passes cephalad across the neck of the first rib to join the C8 nerve in the brachial plexus. A small intercostal branch runs across the inferior surface of the first rib to enter the first interspace close to the costal cartilage. The ventral ramus of the second thoracic nerve also usually sends a small branch to the brachial plexus. Occasionally, this branch will be very large, in which case, the lateral cutaneous branch of the second intercostal nerve is small or absent. Although the intercostal nerves below T1 can usually be sacrificed to facilitate exposure, the T1 and C7 intercostal nerves, which frequently are exposed during this procedure, cannot be sacrificed without causing a severe neurological deficit in hand function. Therefore, it is occasionally necessary to work around the inferior portion of the brachial plexus in this exposure. The phrenic nerve is located in the groove between the trachea and the vena cava on the right, and draping over the aorta and pulmonary arch on the left. The right vagus nerve courses dorsally over the trachea, under the azygous vein, to run in the groove between the trachea and esophagus. The left vagus nerve courses over the aortic arch and under the pulmonary artery to assume a similar position on the left. The thoracic duct is found on the left posterolateral aspect of the esophagus, cephalad to the aorta.
6 With these anatomic relationships in mind, decompression can proceed in a manner similar to that described above for the transthoracic approach. Again, it is imperative to identify the landmarks to conceptualize the location of the thecal sac at all times. After decompression and reconstruction, the individual muscles are reapproximated in layers and the skin closed with a running suture or staples. Again, an early chest x-ray in recovery is warranted to exclude the possibility of pneumothorax. MINIMALLY INVASIVE SURGICAL TECHNIQUE The senior author has recently experimented with a variant of the lateral parascapular approach requiring a less extensive skin incision and muscle dissection/retraction. This is made possible by newer, tubular retractors designed specifically for spinal surgery. The technique requires an approximately 30-mm paramedian incision placed either vertically or horizontally (depending on extent of pathology and surgeon preference), centered both at the level of interest vertically and the costovertebral junction (or farther) laterally. Soft tissue dissection is carried down to expose the lamina, facet, and ribs. The rib of the involved level is dissected from the pleura and neurovascular bundle and removed. The bone is saved for autologous grafting. After the rib has been removed, the retractor system can be placed. The remainder of the surgery can be carried out in standard fashion, albeit in a more confined surgical field. Anterior instrumentation can be successfully carried out by this method. SUMMARY Management of upper thoracic spinal fractures continues to be a challenging task for spinal surgeons. Appropriate treatment depends on a variety of factors, including the nature of the fracture, the need for neural decompression, and the need for spinal stabilization. A number of surgical approaches have been developed to address these lesions. Each approach carries its own inherent advantages and disadvantages and an understanding of each is required to optimize the treatment of any individual patient. As our surgical experience and expertise continues to grow in the field of minimally invasive surgery, these techniques and novel approaches will provide alternatives for our patients that will maintain the current quality of care but minimize surgical trauma and improve recovery times. Chapter 21, Fractures of the Upper Thoracic Spine:Approaches and Surgical Management (continued) TRANSTHORACIC APPROACH In detailing the management of a cohort of patients with Pott s disease, Hodgson et al. (9) were the first to describe the thoracotomy approach to the ventral spinal column. The spine may be either approached from the right or left side. Although the left side is generally favored for lesions in the lower thoracic spine and the thoracolumbar junction, a right-sided approach is often used for the upper thoracic spine because of the location of the great vessels. The patient is placed in the lateral decubitus position (Fig. 21.7). It is important to maintain the patient s orientation, keeping in mind the 3-D orientation of the spine. An axillary roll is placed to minimize the risk of brachial plexus injury.
7 Fluoroscopy is used to confirm and mark the skin incision. The incision is made over the rib, one or two levels above the pathological vertebrae. A subperiosteal dissection is performed, protecting the inferior neurovascular bundle. The rib is then removed and the rib spreader is placed. Either a retropleural or a transpleural approach to the spine may be used. The retropleural approach requires blunt dissection to mobilize the pleura off the posterior chest wall and vertebral bodies. This exposes the sympathetic chain, radicular vessels, rib, and the vertebral bodies. If the pleura is not violated, there is no need to place a chest tube at the conclusion of the case. The transpleural approach requires the lung to be retracted with a malleable or egg-beater retractor so that the spine can be visualized through the parietal pleura. This section of pleura must be incised and reflected back, thereby exposing the spine. Closure requires re-approximation of the parietal pleura and placement of a chest tube. Segmental vessels in the area of planned resection are removed early to minimize blood loss during the remainder of the procedure. The vessels are ligated close to the vertebral body to maintain the anastomoses more distally and minimize the risk of ischemic insult to the spinal cord. The proximal 2 to 3 cm of the head of the rib is sectioned using a high-speed drill or osteotome, and disarticulated. This reveals the intercostal nerve, which is an important landmark for the neural foramen and the pedicle. Identification of these structures facilitates an appreciation of the location of the thecal sac. Early identification of the thecal sac is imperative for safe resection of ventral pathology. The discs above and below the pathological vertebrae are incised and removal is in an anterior direction, away from the thecal sac. A high-speed drill with a cutting burr is used to remove the majority of the ventral aspect of the vertebral body. The anterior cortex and anterior longitudinal ligament are left intact, if possible. The posterior cortical margin is thinned down to an egg-shell thickness, and then can be fractured into the cavity created using curettes, thereby decompressing the spinal cord. An adequate decompression from pedicle to pedicle should be confirmed before beginning reconstruction. As noted, violation of the parietal pleura requires primary closure and placement of a chest tube. For the retropleural approach, the wound should be filled with saline to confirm that there are no occult leaks. Individual muscles are identified and closed in layers with either interrupted or running sutures. Early chest x-ray in the recovery room is warranted to exclude pneumothorax. LATERAL PARASCAPULAR EXTRAPLEURAL APPROACH The lateral parascapular extrapleural approach was first described in 1991 (7) as a modification of Capener s lateral rhachotomy approach (5) and the lateral extracavitary approach of Larson et al. (11), to deal with the limitations imposed by the shoulder girdle when these earlier approaches were used to approach the cervicothoracic junction. After induction of general, endotracheal anesthesia, the patient is placed in a prone position on the operating table with appropriate chest and hip padding. It is important to use a bed that allows free movement of the fluoroscope, not only in the region of interest but also either higher or lower to allow counting of vertebral bodies for localization. The arms can either be tucked at the patient s side or positioned abducted away from the body. By abducting the arm, the scapula is rotated forward and away from the midline spine, thus, providing more room for retraction of the paraspinal musculature.
8 The incision must extend from three to four levels above the lesion to three to four levels below the lesion (Fig. 21.8). However, because of the relative tethering effect of the trapezius and levator scapulae muscles, a lesion located at T1 or T2 will require an incision that extends all the way up to approximately C3 or C4. Note that in the prone position, before takedown of the trapezius and rhomboid musculature, the scapula covers the lateral one-half of the posterior rib cage. This position makes mobilization of the trapezius and rhomboid musculature imperative to exposure of the upper thoracic spine. In the initial dissection for exposure of this region of the spine, the spinous process insertions of the trapezius, rhomboid, serratus posterior superior, splenius capitis, and splenius cervicis muscles are taken down, as a group, for lateral retraction (Fig. 21.9). As these muscles are taken down, the scapula is released from its attachments to the spinous processes and rotates anterolaterally out of the operative field. This exposes the posterior and posterolateral rib cage for the remainder of the procedure. During this rotation, all neurovascular structures rotate with the scapula and are not at risk of injury. The entire group of erector spinae muscles and transversospinalis muscles can be dissected off the spinous processes, laminae, facets, and transverse processes as a single muscular mass (Fig ). The insertions of the iliocostalis thoracis muscles are also taken down. Control of the musculature in this way exposes all of the vertebral elements from the tip of the spinous processes to the tip of the transverse processes, as well as the costotransverse ligaments, the joints, and the ribs. After blunt dissection to remove the intercostal muscles and the costotransverse and radiate ligaments, each rib can be resected. This resection should extend 6 to 8 cm lateral to the junction of the rib with the transverse process. In the course of this procedure, a strip of intercostal musculature is isolated between each rib. This strip of musculature will contain the intercostal nerve, artery, and vein as they pass laterally between the internal intercostal membrane and the pleura, and then between the internal and innermost intercostal muscles. Immediately ventral to the intercostal bundle and the intercostal muscles lays the pleura. With blunt dissection, the pleura can be separated from these structures to expose the lateral vertebral elements. Following the intercostal bundle medially will enable identification of the neural foramen. Within the neural foramen, the dorsal root ganglion can be identified along with the gray and white rami communicantes, which course ventrally to the sympathetic chain and ganglia. The sympathetic chain is contained within a fascial compartment over the costovertebral articulation. This compartment is formed by fusion of the mediastinal and prevertebral fascia. The major portion of the ventral ramus of the first thoracic nerve passes cephalad across the neck of the first rib to join the C8 nerve in the brachial plexus. A small intercostal branch runs across the inferior surface of the first rib to enter the first interspace close to the costal cartilage. The ventral ramus of the second thoracic nerve also usually sends a small branch to the brachial plexus. Occasionally, this branch will be very large, in which case, the lateral cutaneous branch of the second intercostal nerve is small or absent. Although the intercostal nerves below T1 can usually be sacrificed to facilitate exposure, the T1 and C7 intercostal nerves, which frequently are exposed during this procedure, cannot be sacrificed without causing a severe neurological deficit in hand function. Therefore, it is occasionally necessary to work around the inferior portion of the brachial plexus in this exposure. The phrenic nerve is located in the groove between the trachea and the vena cava on the right, and draping over the aorta and pulmonary arch on the left. The right vagus nerve courses dorsally over the trachea, under the azygous
9 vein, to run in the groove between the trachea and esophagus. The left vagus nerve courses over the aortic arch and under the pulmonary artery to assume a similar position on the left. The thoracic duct is found on the left posterolateral aspect of the esophagus, cephalad to the aorta. With these anatomic relationships in mind, decompression can proceed in a manner similar to that described above for the transthoracic approach. Again, it is imperative to identify the landmarks to conceptualize the location of the thecal sac at all times. After decompression and reconstruction, the individual muscles are reapproximated in layers and the skin closed with a running suture or staples. Again, an early chest x-ray in recovery is warranted to exclude the possibility of pneumothorax. MINIMALLY INVASIVE SURGICAL TECHNIQUE The senior author has recently experimented with a variant of the lateral parascapular approach requiring a less extensive skin incision and muscle dissection/retraction. This is made possible by newer, tubular retractors designed specifically for spinal surgery. The technique requires an approximately 30-mm paramedian incision placed either vertically or horizontally (depending on extent of pathology and surgeon preference), centered both at the level of interest vertically and the costovertebral junction (or farther) laterally. Soft tissue dissection is carried down to expose the lamina, facet, and ribs. The rib of the involved level is dissected from the pleura and neurovascular bundle and removed. The bone is saved for autologous grafting. After the rib has been removed, the retractor system can be placed. The remainder of the surgery can be carried out in standard fashion, albeit in a more confined surgical field. Anterior instrumentation can be successfully carried out by this method. SUMMARY Management of upper thoracic spinal fractures continues to be a challenging task for spinal surgeons. Appropriate treatment depends on a variety of factors, including the nature of the fracture, the need for neural decompression, and the need for spinal stabilization. A number of surgical approaches have been developed to address these lesions. Each approach carries its own inherent advantages and disadvantages and an understanding of each is required to optimize the treatment of any individual patient. As our surgical experience and expertise continues to grow in the field of minimally invasive surgery, these techniques and novel approaches will provide alternatives for our patients that will maintain the current quality of care but minimize surgical trauma and improve recovery times. References 1. Benzel EC: Biomechanics of Spine Stabilization. New York, Thieme, 2001, pp Birch R, Bonney G, Marshall RW: A surgical approach to the cervico-thoracic spine. J Bone Joint Surg Br 72: , Brown CVR, Antevil JL, Sise MJ, Sack DI: Spiral computed tomography for diagnosis of cervical, thoracic and
10 lumbar fractures: Its time has come. J Trauma 58: , Brunig F: Technik der kombinierten Resektionsmethode samtlicher sympathischen Nervenbaum am Halse [in German]. Zentralbl Chir 50: , Capener N: The evolution of lateral rhachotomy. J Bone Joint Surg 36: , Cook WA, Hardaker WT: Injuries to the thoracic and lumbar spine, in Wilkins RH, Rengachary SS (eds): Neurosurgery, 2nd Ed. McGraw-Hill, 1996, pp Fessler RG, Dietze DD, MacMillan M, Peace D: Lateral parascapular extrapleural approach to the upper thoracic spine. J Neurosurg 75: , Gask GE: The surgery of the sympathetic nervous system. Br J Surg 21: , Hodgson AR, Stock FE, Fang HSY: Anterior spinal fusion: The operative approach and pathological findings in 412 patients with Pott s disease of the spine. Br J Surg 48: , Jonnesco T: Le Sympathique Cervico-Thoracico [in French]. Paris, France, Masson, Larson SJ, Holst RA, Hemmy DC, Sances A: Lateral extracavitary approach to traumatic lesions of the thoracic and lumbar spine. J Neurosurg 45: , Ochsner A, DeBakey M: Peripheral vascular disease. Surg Gynecol Obstet 70: , Royle ND: Observations on the alteration of the circulation of the brain by surgical means in diseases of the central nervous system. BMJ 1: , Sundaresan N, Shah J, Foley KM, Rosen G: An anterior surgical approach to the upper thoracic vertebrae. J Neurosurg 61: , White AA, Panjabi MM: Clinical Biomechanics of the Spine, 2nd Ed. Philadelphia, Lippincott, 1990, pp Yue JJ, Sossan A, Selgrath C, Deutsch LS, Wilkens K, Testaiuti M, Gabriel JP: The treatment of unstable thoracic spine fractures with transpedicular screw instrumentation: A 3-year consecutive series. Spine 27: , 2002.
11 <DFIG> Fig Diagrammatic representation of the standard posterior approaches to the upper thoracic spine. Fig Treatment algorithm for compression fractures of the upper thoracic spine. Fig Treatment algorithm for burst fractures of the upper thoracic spine. Fig Illustration of the T-shaped incision used in the transmanubrial approach. Fig Illustration depicting the reflection of the sternocleidomastoid and strap muscles during the transmanubrial approach. Note the clavicular cut being performed with a Gigli saw. Fig Illustration of the ultimate spinal exposure after a transmanubrial approach. Fig Patient positioning and incision placement for the transthoracic approach. Fig External landmarks and incision placement for the lateral parascapular extrapleural approach. Fig Operative and diagrammatic representation of the initial myocutaneous flap that enables anterolateral scapular rotation. Fig Intraoperative photograph and illustration depicting the exposure of the ribs and posterior vertebral elements after elevation of the erector spinae complex.
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
by joseph e. muscolino, DO photography by yanik chauvin
 by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
Clarification of Terms
 Shoulder Girdle Clarification of Terms Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus What is the purpose (or function) of the shoulder and entire upper
Shoulder Girdle Clarification of Terms Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus What is the purpose (or function) of the shoulder and entire upper
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
PRACTICE GUIDELINE TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL
 PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
ANTERIOR LUMBAR INTERBODY FUSION (ALIF) Basic Anatomical Landmarks: Anterior Lumbar Spine
 (ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
(ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
MD 2016. Back Muscles & Movements Applied Anatomy. A/Prof Chris Briggs Anatomy & Neuroscience
 MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
Surgical Technique. coflex Surgical Technique
 Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Vertebral anatomy study guide. Human Structure Summer 2015. Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey.
 Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Thoracic Spine Anatomy
 A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: [email protected] DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: [email protected] DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Muscles of the Spinal Column. Chapter 12
 Muscles of the Spinal Column Chapter 12 Cervical Muscles Splenius Splenius (capitis and cervicis) Origin: Cervicis spinous process of T3-T6 Capitis - lower half of ligmentum nuchea & spinous process of
Muscles of the Spinal Column Chapter 12 Cervical Muscles Splenius Splenius (capitis and cervicis) Origin: Cervicis spinous process of T3-T6 Capitis - lower half of ligmentum nuchea & spinous process of
17 Forequarter Amputation
 Malawer Chapter 17 22/02/2001 08:32 Page 289 17 Forequarter Amputation Martin Malawer and Paul Sugarbaker OVERVIEW Forequarter amputation entails surgical removal of the entire upper extremity, scapula,
Malawer Chapter 17 22/02/2001 08:32 Page 289 17 Forequarter Amputation Martin Malawer and Paul Sugarbaker OVERVIEW Forequarter amputation entails surgical removal of the entire upper extremity, scapula,
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
ENT Emergencies. Injuries of the Neck. Registrar Dept Trauma and emergency Medicine Tygerberg Hospital
 ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Skeletal System. Axial Skeleton: Vertebral Column and Ribs
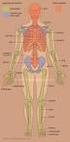 Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Chapter 4 The Shoulder Girdle
 Chapter 4 The Shoulder Girdle Key Manubrium Clavicle Coracoidprocess Acromionprocess bony landmarks Glenoid fossa Bones Lateral Inferior Medial border angle McGraw-Hill Higher Education. All rights reserved.
Chapter 4 The Shoulder Girdle Key Manubrium Clavicle Coracoidprocess Acromionprocess bony landmarks Glenoid fossa Bones Lateral Inferior Medial border angle McGraw-Hill Higher Education. All rights reserved.
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Level IA: Submental Group
 IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Fig. 1 The level system is used for describing the location of lymph nodes in the neck: Level I, submental and submandibular group; Level II, upper jugular
IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Fig. 1 The level system is used for describing the location of lymph nodes in the neck: Level I, submental and submandibular group; Level II, upper jugular
Lumbar Spine Anatomy. eorthopod.com 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.
 A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 [email protected] DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 [email protected] DISCLAIMER: The information in this booklet is compiled
SECTION 1 General Principles
 SECTION 1 General Principles Pierre-Alain Clavien Michael G. Sarr Introduction Pierre A. Clavien, Michael G. Sarr A competent surgeon must be aware of all the general aspects of a surgical procedure to
SECTION 1 General Principles Pierre-Alain Clavien Michael G. Sarr Introduction Pierre A. Clavien, Michael G. Sarr A competent surgeon must be aware of all the general aspects of a surgical procedure to
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Evaluation and Treatment of Spine Fractures. Lara C. Portmann, MSN, ACNP-BC
 Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Chapter 12 The Trunk and Spinal Column
 Chapter 12 The Trunk and Spinal Column Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Vertebral Abdominal 24 31 most column complex some intricate & complex articulating vertebrae do pairs
Chapter 12 The Trunk and Spinal Column Manual of Structural Kinesiology R.T. Floyd, EdD, ATC, CSCS Vertebral Abdominal 24 31 most column complex some intricate & complex articulating vertebrae do pairs
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Autonomic Nervous System of the Neck. Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW
 Autonomic Nervous System of the Neck Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW Autonomic nervous system sympathetic parasympathetic enteric Autonomic
Autonomic Nervous System of the Neck Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW Autonomic nervous system sympathetic parasympathetic enteric Autonomic
Chapter 15. Sympathetic Nervous System
 Chapter 15 Sympathetic Nervous System Somatic versus Autonomic Pathways Somatic efferent innervation ACh Myelinated fiber Somatic effectors (skeletal muscles) Autonomic efferent innervation ACh ACh or
Chapter 15 Sympathetic Nervous System Somatic versus Autonomic Pathways Somatic efferent innervation ACh Myelinated fiber Somatic effectors (skeletal muscles) Autonomic efferent innervation ACh ACh or
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S.
 Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Image-guided Spine Procedures for Relief of Severe Lower Back Pain:
 Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
MINIMAL ACCESS SPINE SURGERY
 MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
Divisions of the Skeletal System
 OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
Soft Tissue Neck CT Anatomy
 Soft Tissue Neck CT Anatomy Kris Cummings, M.D. Axial CT Unlabeled Labeled Deep s/lymph Node Chains s/lymph Nodes Temporalis Muscle Occipitalis Muscle s/lymph Nodes s/lymph Nodes s/lymph Nodes s/lymph
Soft Tissue Neck CT Anatomy Kris Cummings, M.D. Axial CT Unlabeled Labeled Deep s/lymph Node Chains s/lymph Nodes Temporalis Muscle Occipitalis Muscle s/lymph Nodes s/lymph Nodes s/lymph Nodes s/lymph
Upper Limb QUESTIONS UPPER LIMB: QUESTIONS
 1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
Chapter 5. The Shoulder Joint. The Shoulder Joint. Bones. Bones. Bones
 Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. Chapter 5 The Shoulder Joint Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Structural Kinesiology The Shoulder Joint 5-1 The Shoulder
Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. Chapter 5 The Shoulder Joint Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Structural Kinesiology The Shoulder Joint 5-1 The Shoulder
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord.
 Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Anatomical Consideration and Brachial Plexus Anesthesia. Anatomy
 Brachial Plexus Anesthesia There are four approaches to the brachial plexus. These include the interscalene, supraclavicular, infraclavicular, and axillary approach. For the purposes of this lecture we
Brachial Plexus Anesthesia There are four approaches to the brachial plexus. These include the interscalene, supraclavicular, infraclavicular, and axillary approach. For the purposes of this lecture we
Shoulder and Related Upper Extremity Radiating Pain
 Shoulder and Related Upper Extremity Radiating Pain ICD-9-CM codes: 723.3 Cervical brachial syndrome ICF codes: Activities and Participation Domain codes: d4301 Carrying in the hands (Taking or transporting
Shoulder and Related Upper Extremity Radiating Pain ICD-9-CM codes: 723.3 Cervical brachial syndrome ICF codes: Activities and Participation Domain codes: d4301 Carrying in the hands (Taking or transporting
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任
 Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
13 Adductor Muscle Group Excision
 Malawer Chapter 13 21/02/2001 15:36 Page 243 13 Adductor Muscle Group Excision Martin Malawer and Paul Sugarbaker OVERVIEW The adductor muscle group is the second most common site for high- and low-grade
Malawer Chapter 13 21/02/2001 15:36 Page 243 13 Adductor Muscle Group Excision Martin Malawer and Paul Sugarbaker OVERVIEW The adductor muscle group is the second most common site for high- and low-grade
III./8.4.2: Spinal trauma. III./8.4.2.1 Injury of the spinal cord
 III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
BODY BODY PEDICLE PEDICLE TRANSVERSE TRANSVERSE PROCESS PROCESS
 Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
Learning Objective Radiology Anatomy of the Spine and Upper Extremity Identify anatomic structures of the spine and upper extremities on standard radiographic and cross-sectional images Timothy J. Mosher,
Lectures of Human Anatomy
 Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Instability concept. Symposium- Cervical Spine. Barcelona, February 2014
 Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Instability concept Guillem Saló Bru, MD, Phd AOSpine Principles Symposium- Cervical Spine Orthopaedic Depatment. Spine Unit. Hospital del Mar. Barcelona. Associated Professor UAB Barcelona, February 2014
Dr. Weyrich G04: Anterior Thoracic Wall, Breast and Lymphatic System
 Dr. Weyrich G04: Anterior Thoracic Wall, Breast and Lymphatic System Reading: 1. Gray s Anatomy for Students, Chapter 3 2. Dissection Guide for Human Anatomy, Lab 4 Objectives: 1. Osteocartilaginous thoracic
Dr. Weyrich G04: Anterior Thoracic Wall, Breast and Lymphatic System Reading: 1. Gray s Anatomy for Students, Chapter 3 2. Dissection Guide for Human Anatomy, Lab 4 Objectives: 1. Osteocartilaginous thoracic
Ken Ross BSc ST, Nat Dip ST
 Ken Ross BSc ST, Nat Dip ST Trunk Most people will suffer from back pain at some point in their lives. Good spinal posture places minimal strain on the muscles which maintain the natural curve of the spine
Ken Ross BSc ST, Nat Dip ST Trunk Most people will suffer from back pain at some point in their lives. Good spinal posture places minimal strain on the muscles which maintain the natural curve of the spine
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
THORACIC OUTLET SYNDROME
 THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called
THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called
Sign up to receive ATOTW weekly - email [email protected]
 THORACIC OUTLET SYNDROME ANAESTHESIA TUTORIAL OF THE WEEK 286 17 TH JUNE 2013 Dr Sandeep Kusre, Dr Richard Telford Royal Devon & Exeter Hospital, United Kingdom Correspondence to [email protected] QUESTIONS
THORACIC OUTLET SYNDROME ANAESTHESIA TUTORIAL OF THE WEEK 286 17 TH JUNE 2013 Dr Sandeep Kusre, Dr Richard Telford Royal Devon & Exeter Hospital, United Kingdom Correspondence to [email protected] QUESTIONS
MODIFIED STRAYER GASTROCNEMIUS RECESSION: A Technique Guide for the Supine Positioned Patient
 C H A P T E R 4 5 MODIFIED STRAYER GASTROCNEMIUS RECESSION: A Technique Guide for the Supine Positioned Patient M. Jay Groves, IV, DPM Gastrosoleal equinus is a common deforming force on the foot and ankle.
C H A P T E R 4 5 MODIFIED STRAYER GASTROCNEMIUS RECESSION: A Technique Guide for the Supine Positioned Patient M. Jay Groves, IV, DPM Gastrosoleal equinus is a common deforming force on the foot and ankle.
ICD-9-CM coding for patients with Spinal Cord Injury*
 ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis
 Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Basic techniques of pulmonary physical therapy (I) 100/04/24
 Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
Lesions, and Masses, and Tumors Oh My!!
 Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
Lesions, and Masses, and Tumors Oh My!! Presented by: Susan Ward, CPC, CPC-H, CPC-I, CPCD, CEMC, CPRC 1 1 CPT GUIDELINES Agenda CPT DEFINITIONS OP REPORT CASES 2 Definitions Cyst - a closed sac having
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
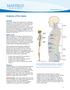 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
6. Histopathology of Alveoli 7. Surfactant 8. Blood supply of lungs 9. Lymphatics of Lungs 10. Nerve supply of Lungs 11. Pleura 12.
 ANATOMY OF LUNGS - 1. Gross Anatomy of Lungs 2. Surfaces and Borders of Lungs 3. Hilum and Root of Lungs 4. Fissures and Lobes of Lungs 5. Bronchopulmonary segments 6. Histopathology of Alveoli 7. Surfactant
ANATOMY OF LUNGS - 1. Gross Anatomy of Lungs 2. Surfaces and Borders of Lungs 3. Hilum and Root of Lungs 4. Fissures and Lobes of Lungs 5. Bronchopulmonary segments 6. Histopathology of Alveoli 7. Surfactant
Anatomy of Human Muscles
 Anatomy of Human Muscles PURPOSE: To develop skill in identifying muscle names and locations relative to other regional structures. To determine origin, insertion and principle action of muscles through
Anatomy of Human Muscles PURPOSE: To develop skill in identifying muscle names and locations relative to other regional structures. To determine origin, insertion and principle action of muscles through
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Minimally Invasive Transforaminal Lumbar Interbody Fusion: Technical Note
 8 The Open Neurosurgery Journal, 2009, 2, 8-13 Open Access Minimally Invasive Transforaminal Lumbar Interbody Fusion: Technical Note Gabriel C. Tender*,1 and John K. Ratliff 2 1 Department of Neurosurgery,
8 The Open Neurosurgery Journal, 2009, 2, 8-13 Open Access Minimally Invasive Transforaminal Lumbar Interbody Fusion: Technical Note Gabriel C. Tender*,1 and John K. Ratliff 2 1 Department of Neurosurgery,
SPINE. Postural Malalignments 4/9/2015. Cervical Spine Evaluation. Thoracic Spine Evaluation. Observations. Assess position of head and neck
 SPINE Observations Body type Postural alignments and asymmetries should be observed from all views Assess height differences between anatomical landmarks Figure 25-9 Figure 25-10 Figure 25-11 & 12 Postural
SPINE Observations Body type Postural alignments and asymmetries should be observed from all views Assess height differences between anatomical landmarks Figure 25-9 Figure 25-10 Figure 25-11 & 12 Postural
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Thoracic Spine. Anatomy, Kinesiology and Pathology of the Thoracic Spine. Thoracic Spine. Function of the Thoracic Spine.
 Anatomy, Kinesiology and Pathology of the Thoracic Spine Beth K. Deschenes, PT, MS, OCS Thoracic Spine Consists of thorax, rib cage and sternum 12 vertebrae and 12 ribs Function of the Thoracic Spine Support
Anatomy, Kinesiology and Pathology of the Thoracic Spine Beth K. Deschenes, PT, MS, OCS Thoracic Spine Consists of thorax, rib cage and sternum 12 vertebrae and 12 ribs Function of the Thoracic Spine Support
HOW TO CITE THIS ARTICLE:
 POST TRAUMATIC INSTABILITY OF SUB-AXIAL CERVICAL SPINE - REDUCTION AND INTERNAL FIXATION BY LATERAL MASS SCREWS A LONG TERM FOLLOW-UP STUDY Godagu Bhaskar 1, Ambarapu Mastan Reddy 2, Akyam Lakshman Rao
POST TRAUMATIC INSTABILITY OF SUB-AXIAL CERVICAL SPINE - REDUCTION AND INTERNAL FIXATION BY LATERAL MASS SCREWS A LONG TERM FOLLOW-UP STUDY Godagu Bhaskar 1, Ambarapu Mastan Reddy 2, Akyam Lakshman Rao
Vivian Gonzalez Gillian Lieberman, MD. January 2002. Lumbar Spine Trauma. Vivian Gonzalez, Harvard Medical School Year III Gillian Lieberman, MD
 January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis
 Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Administrative. Patient name Date compare with previous Position markers R-L, upright, supine Technical quality
 CHEST X-RAY Administrative Patient name Date compare with previous Position markers R-L, upright, supine Technical quality AP or PA ( with x-ray beam entering from back of patient, taken at 6 feet) Good
CHEST X-RAY Administrative Patient name Date compare with previous Position markers R-L, upright, supine Technical quality AP or PA ( with x-ray beam entering from back of patient, taken at 6 feet) Good
Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve,
 Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve, Larynx, Trachea, & Esophageal Management Robert C. Wang,
Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve, Larynx, Trachea, & Esophageal Management Robert C. Wang,
Anatomicalintroduction
 3rd INTERVENTIONAL HANDS-ON PAIN RELIEF & NEUROMODULATION CADAVER WORKSHOP Anatomicalintroduction Gdansk-Poland Programmeofthelecture Shortintroductionto theanatomyof: 1.Vertebralcolumn 2.Intervertebraldiscs
3rd INTERVENTIONAL HANDS-ON PAIN RELIEF & NEUROMODULATION CADAVER WORKSHOP Anatomicalintroduction Gdansk-Poland Programmeofthelecture Shortintroductionto theanatomyof: 1.Vertebralcolumn 2.Intervertebraldiscs
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria
 Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria MAY 2013 When paying the reasonable costs of medical services, the TAC and WorkSafe pay in
Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria MAY 2013 When paying the reasonable costs of medical services, the TAC and WorkSafe pay in
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
LABS 8 & 9: CAT MUSCULATURE
 ZOO 4377L - VERTEBRATE MORPHOLOGY LAB LABS 8 & 9: CAT MUSCULATURE Name: Name: SSN: SSN: ---------------------------------------------------------------------------------------------------------------------
ZOO 4377L - VERTEBRATE MORPHOLOGY LAB LABS 8 & 9: CAT MUSCULATURE Name: Name: SSN: SSN: ---------------------------------------------------------------------------------------------------------------------
Getting to the Backbone of Spinal Coding in ICD-10-PCS
 Getting to the Backbone of Spinal Coding in ICD-10-PCS Sponsored by 1915 N. Fine Ave #104 Fresno CA 93720-1565 Phone: (559) 251-5038 Fax: (559) 251-5836 www.californiahia.org Program Handouts Tuesday,
Getting to the Backbone of Spinal Coding in ICD-10-PCS Sponsored by 1915 N. Fine Ave #104 Fresno CA 93720-1565 Phone: (559) 251-5038 Fax: (559) 251-5836 www.californiahia.org Program Handouts Tuesday,
The Nervous System: The Spinal Cord and Spinal Nerves
 14 The Nervous System: The Spinal Cord and Spinal Nerves PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The Central Nervous System
14 The Nervous System: The Spinal Cord and Spinal Nerves PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The Central Nervous System
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
CeSpace Titanium / PEEK
 Aesculap Anterior Cervical Interbody Fusion System CeSpace Titanium / PEEK Aesculap Spine CeSpace Content A Foreword 3 B Implant Material 4 C Implant Features 6 D Surgical Technique 8 E Ordering Information
Aesculap Anterior Cervical Interbody Fusion System CeSpace Titanium / PEEK Aesculap Spine CeSpace Content A Foreword 3 B Implant Material 4 C Implant Features 6 D Surgical Technique 8 E Ordering Information
Femoral head and neck ostectomy (FHO) is a commonly
 P ro c e d u re s P ro O R T H O P E D I C S Peer Reviewed Laura E. Peycke, DVM, MS, Diplomate CVS Texas &M University Femoral Head & Neck Ostectomy Femoral head and neck ostectomy (FHO) is a commonly
P ro c e d u re s P ro O R T H O P E D I C S Peer Reviewed Laura E. Peycke, DVM, MS, Diplomate CVS Texas &M University Femoral Head & Neck Ostectomy Femoral head and neck ostectomy (FHO) is a commonly
Introduction. I. Objectives. II. Introduction. A. To become familiar with the terms of direction and location.
 E X E R C I S E Introduction I. Objectives A. To become familiar with the terms of direction and location. B. To become familiar with different types of planes and sections. C. To learn the names and locations
E X E R C I S E Introduction I. Objectives A. To become familiar with the terms of direction and location. B. To become familiar with different types of planes and sections. C. To learn the names and locations
Central Venous Access
 Central Venous Access Ian Rigby, Daniel Howes, Jason Lord, Ian Walker Resuscitation Education Consortium/Kingston Resuscitation Institute Introduction A great deal of this course is geared toward making
Central Venous Access Ian Rigby, Daniel Howes, Jason Lord, Ian Walker Resuscitation Education Consortium/Kingston Resuscitation Institute Introduction A great deal of this course is geared toward making
Spinal Anatomy. * MedX research contends that the lumbar region really starts at T-11, based upon the attributes of the vertebra.
 Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Completing the Loop: Management of the Adolescent Sports Injury. Adam Thomas, PT, DPT, ATC
 : Management of the Adolescent Sports Injury Adam Thomas, PT, DPT, ATC https://www.youtube.com/watch?v=vbufpo 8s3As On field assessment can be the most efficient when the health care provider has observed
: Management of the Adolescent Sports Injury Adam Thomas, PT, DPT, ATC https://www.youtube.com/watch?v=vbufpo 8s3As On field assessment can be the most efficient when the health care provider has observed
Anatomy and Terminology of the Spine. Bones of the Spine (Vertebrae)
 Anatomy and Terminology of the Spine The spine, also called the spinal column, vertebral column or backbone, consists of bones, intervertebral discs, ligaments, and joints. In addition, the spine serves
Anatomy and Terminology of the Spine The spine, also called the spinal column, vertebral column or backbone, consists of bones, intervertebral discs, ligaments, and joints. In addition, the spine serves
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Compression Fractures
 September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ)
 The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
