Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
|
|
|
- Fay Griffith
- 10 years ago
- Views:
Transcription
1 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut Neck and Back specialists, LLC Mailing address: Connecticut Neck and Back Specialists, LLC 20 Germantown Rd Danbury, CT 06810
2 Introduction: Degenerative lumbar spinal stenosis is a common cause of low back and leg pain in individuals in their fifth and sixth decades of life. 1-4 The symptoms specific to intermittent neurogenic claudication include progressive back, buttock or leg pain, and lower extremity numbness or weakness with standing and walking. 2,5,6 In lumbar extension, as with standing, the diameter of the spinal canal is narrowed in the anteriorposterior dimension resulting in compression of the thecal sac and exiting nerve roots. 6 These symptoms are typically relieved by changing to a seated or forward flexed position, as this position increases sagittal spinal canal diameter. 4,6-9 Spinal stenosis is a dynamic process where the diameter of the spinal canal decreases below a critical threshold due to a combination of mechanical factors including degenerative disc disease with resultant disc protrusion, spondylolisthesis, ligamentum flavum hypertrophy, and facet joint arthropathy. 2,4,8 Lumbar spinal stenosis is a progressive disabling condition which compromises an individual s ability to perform their activities of daily living, reduces overall quality of life and ultimately threatens one s independence. 7 Analgesics, nonsteroidal anti-inflammatories, activity modification, physical therapy and epidural steroid injections are the mainstay of conservative care for spinal stenosis. 6, 7 Patients often fail conservative therapy because these treatment options do not alter the anatomic pathology that causes symptoms. 7 Since stenosis is a mechanical problem, surgical intervention in the form of mechanical decompression of the posterior spinal elements is indicated when a patient fails conservative management. 6 The conventional surgical treatment for spinal stenosis is a lumbar laminectomy. 10 The X- Stop is the first interspinous process decompression (IPD) device that provides an alternative surgical option for patients with spinal stenosis. 4 Interspinous process decompression using the X-Stop implant is a relatively new, FDA approved, minimally invasive procedure that increases spinal canal diameter while avoiding exposure of the spinal cord and neural elements. A titanium spacer is placed between adjacent spinous processes of the affected level maintaining distraction of the posterior elements of the vertebral bodies thereby indirectly reducing pressure on the neural elements. 2,4,8,10 The procedure may be performed under a general or local anesthetic in a lateral decubitus or prone position via a midline approach with a minimal hospital stay. 10
3 Surgical Technique: The patient is placed in the right lateral decubitus position and may be slightly sedated. Fluoroscopic imaging is used to localize the appropriate surgical level. Following the administration of a local anesthetic, the skin is incised and the lumbodorsal fascia overlying the adjacent spinous processes is exposed. Longitudinal incisions are then made on each side of the adjacent spinous processes with care taken to preserve the integrity of the supraspinous process ligament running between them. The lumbar paraspinal musculature is then subperiosteally dissected from the adjacent spinous processes out laterally to expose the facet joints. Care is taken to preserve the facet joint capsules. Once dissection is complete and exposure is adequate, attention is turned to the placement of the interspinous process distraction implant (X-STOP). Using lateral fluoroscopic imaging (to verify the correct level), the initial dilator tool is inserted and passed from the right side to the left side of the interspinous space with care taken to remain as anterior or ventral as possible. Then, sequential dilators are used to create maximal distraction and, in doing so, the appropriate size implant is determined. Maximal distraction between the spinous processes can be judged by palpating the tension within the overlying supraspinous process ligament. Once the appropriate implant is chosen, the device is affixed to its insertion tool and passed from the right side to the left side of the interspinous space. The left wing of the implant is then attached under direct visualization and a torque screwdriver is used to tighten the implant into its final position. AP and lateral fluoroscopic imaging is obtained to confirm appropriate positioning of the implant in both planes. The lumbodorsal fascia and skin is closed in the usual fashion. There is no need for placement of a drain as blood loss should be minimal. The procedure is usually performed in less than one hour. Bracing is not needed postoperatively. Materials and Methods: Following the Spine Center at Danbury Hospital X-Stop Protocol, the device was implanted at 35 levels in 26 patients (12 males and 14 females; age range years; mean, 77 years old) in a fifteen month period. Ten implants were placed at the L3/4 level and 25 implants were placed at the L4/5 level. Implants were single level in 16 patients
4 and double level in 10 patients. All patients had the classic symptom complex associated with intermittent, neurogenic claudication secondary to spinal stenosis and had failed to respond to non-operative care including non-steroidal anti-inflammatories, physical therapy and the trial of at least one epidural steroid injection. Five patients underwent general endotracheal anesthesia and twenty-one patients received local anesthesia plus sedation. Five patients were operated upon in the prone position and the remainder in a lateral decubitus position. Seven patients had a single level L4/5 spondylolisthesis and one patient had a two-level L3/4 and L4/5 spondylolisthesis. A total of nine 10mm implants, seven 12mm implants and nineteen 14mm implants were placed. The average hospital length of stay was 1.75 days (range 1 to 6 days). Results: The data were analyzed for 26 X-Stop patients. As this case study is a retrospective chart and radiograph review, primary outcome is subjective and based on self reported improvement in symptoms and function at postoperative office visits. Twenty-four implantation procedures were successful. There were no treatment related deaths. Eleven patients (42%) were discharged from care by their six or twelve week follow-up visits with resolution of symptoms. There were two intra-operative related complications which represent treatment failures. One patient was noted to have an L4 spinous process fracture prior to closure requiring removal of the two adjacent implants prior to leaving the operating room. A second patient also sustained an L4 spinous process fracture and therefore, the procedure was aborted and no implant was placed. Two patients, each of which had a single level implant at L4/5 continued to have persistent symptoms postoperatively. Their cases are considered to reflect treatment failures as both patients ultimately required delayed implant removal and formal laminectomy less than one year from the initial procedure. No difficulties were noted when removing the implant when they subsequently underwent laminectomy. There was one device related adverse event. At a routine two week postop check, one patient (who underwent a two level implant) was noted to have a dislodged L4/5 implant detected on follow-up radiographic exam. Although she continues to be
5 symptomatic (persistent radicular left leg pain), she has an intact neurological exam and has refused additional treatment to date. Her case is also considered to represent a treatment failure. Postoperatively, one patient (who had received a local anesthetic) developed hypoxic respiratory failure, was found to have a right lower lobe infiltrate on radiograph and was presumed to have developed aspiration pneumonia. She received seven days of intravenous antibiotics along with an oral prednisone taper and was ultimately discharged home with home oxygen therapy. Her preoperative symptoms have resolved. Three patients in this series had stenosis at the L2/3 level that was not addressed as the device is not indicated for implantation at the L2/3 level. One patient was discharged to long-term pain management at twelve weeks post-operatively. One patient with an L4/5 implant developed recurrent radicular left leg pain with a new foot drop at ten months post-op at which time an L4/5 laminectomy was recommended. Although considered to be a minimally invasive procedure, five patients in our series required transfer to an extended care facility upon discharge from the hospital for additional rehabilitation. Discussion: As with any spinal procedure, peri and post-operative complications include the risk of cardiovascular and pulmonary complications related to a general anesthetic, infection, blood loss, iatrogenic instability and hardware failure. 10 Other considerations specific to the X-Stop include the risk of spinous process fracture which may result in failure to place the device, implant removal and or need to abort the procedure. Additional risks include device expulsion, migration or displacement and incomplete decompression resulting in inadequate pain relief and ultimate need for a subsequent laminectomy. The advantages of this minimally invasive procedure include the ability to perform it under a local rather than a general anesthetic 7 (although in our series 5 patients received general anesthesia). While the literature suggests that it can be performed on an out-patient basis that has not been our clinical experience. 4 There is minimal risk of dural tear or spinal cord injury since the neural elements are not exposed. Additionally, the supraspinous and interspinous ligaments are preserved so spinal stability is not sacrificed
6 and it may obviate the need for spinal fusion in some patients. In theory, length of stay should be shorter than that of patients who have undergone a conventional lumbar laminectomy and fewer patients should require nursing home care or rehabilitation. However, five patients in our series (19%) required transfer to short term rehabilitation facilities upon discharge from the hospital. Conclusion: Despite its limitations, this study shows that the X-Stop device can effectively treat spinal stenosis in approximately one-third of patients. The study by Hsu et al. demonstrated that treatment with the X-Stop device was superior to conservative care alone and comparable to the benefit of lumbar decompression. 1,8 This new technology offers an alternative, low risk, minimally invasive treatment option when compared to laminectomy with or without fusion. As with all new technology, clear indications need to be defined in order to have predictable surgical outcomes. While IPD may be superior to conservative care, conventional lumbar laminectomy still provides the most definitive treatment option. Long term data are still lacking and time will reveal how many patients will deteriorate and ultimately go on to require decompressive laminectomy. IPD with the X-Stop implant is not indicated for stenosis at the L2/3 and L5-S1 levels and therefore, open decompressive laminectomy may still provide more predictable outcomes for patients with multi-level stenosis. Spine specialists must put clinical success into perspective. The X-Stop device can be placed under a local anesthetic, with a shorter length of stay, and allows for immediate postoperative mobilization and quicker return to function. Complications are relatively few when compared to laminectomy with or without fusion. If treatment with the X-Stop does not meet the patient s expectation, the implant can easily be removed and a laminectomy can still be performed. A return to the operating room, however, drives up health care costs when one considers a second hospitalization and utilization of additional resources such as visiting nurse services and extended care facilities. Therefore, clinicians must question whether the cost of this new technology (or lack of reimbursement) is justified when studies so far have failed to show a statistically significant difference in long term outcomes.
7 Perhaps the greatest value in this procedure is its ability to obviate the need for concomitant spinal fusion when spinal stenosis is associated with a spondylolisthesis. In elderly patients with significant medical co-morbidities including diabetes, autoimmune diseases, osteoporosis and history of tobacco use, adding a fusion to address the potential instability suggested by the existence of a spondylolisthesis adds significant morbidity to the decompression. IPD with the X-Stop device may also prove to be the more appropriate intervention for the high risk, symptomatic candidate with moderate stenosis whose multiple medical co-morbidities preclude them from being medically cleared to undergo a general anesthetic. Clearly, proper patient selection is essential for optimal clinical results. Historically, surgical intervention has been limited to a choice between decompressive lumbar laminectomy with or without fusion. This new technology provides another potential treatment option. 9 The authors recognize the limitations of this study in that no objective preoperative questionnaire was obtained, Furthermore; it was not a prospective, randomized multi-center controlled study. It would be beneficial to compare patients undergoing IPD with the X-Stop implant with those undergoing decompressive laminectomy so that definitive conclusions can be ascertained with respect to clinical improvement of symptoms. References: 1. Hsu, K. e. (2006). "Quality of life of lumbar spinal stenosis-treated patients in whom the X STOP interspinous device was implanted." J Neurosurg Spine 5(Dec): Siddiqui, M. e. (2006). "Influence of X Stop on Neural Foramina and Spinal Canal Area in Spinal Stenosis." Spine 31(25): Atlas, S. e. (2005). "Long-Term Outcomes of Surgical and Nonsurgical Management of Lumbar Spinal Stenosis: 8 to 10 Year Results from the Maine Lumbar Spine Study." Spine 30(8): Chiu, J. e. "Interspinous Process Decompression (IPD) System (XSTOP) for the treatment of Lumbar Spinal Stenosis." Orthopaedic Surgery: 11.
8 5. Anderson, P. e. (2006). "Treatment of neurogenic claudication by interspinous decompression: application of the X STOP device in patients with lumbar degenerative spondylolisthesis." J Neurosurg: Spine 4(June): Foker, S. e. (2006). "Patient-based outcomes for the operative treatment of degenerative lumbar spinal stenosis." Eur Spine J 15: Eichholz, K. e. (2006). "Is the XSTOP interspinous implant a safe and effective treatment for neurogenic intermittent claudication?" Neurology 2(Jan): Zucherman, J. e. (2004). "A prospective randomized multi-center trial for the treatment of lumbar spinal stenosis with the XSTOP interspinous implant: 1 year results." Eur Spine J 13(July): Zucherman, J. e. (2005). "A Multicenter, Prospective, Randomized Trial Evaluating the X STOP Interspinous Process Decompression System for the Treatment of Neurogenic Intermittent Claudication." Spine 30(12): Kondrashov, D. e. (2006). "Interspinous Process Decompression with the X-STOP Device for Lumbar Spinal Stenosis." J Spinal Discord Tech 19(July): 5.
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Issued and entered this _6th_ day of October 2010 by Ken Ross Commissioner ORDER I PROCEDURAL BACKGROUND
 STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Motion Preservation. Hansen Yuan, MD President, Spine Arthroplasty Society
 Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
Surgical Treatment for Lumbar Spinal Stenosis Dynamic Interspinous Distraction Interlaminar Stabilization Implant - Coflex
 International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011
 1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Surgical Technique. coflex Surgical Technique
 Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Lumbar Spinal Stenosis
 Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
OUTLINE. Anatomy Approach to LBP Discogenic LBP. Treatment. Herniated Nucleus Pulposus Annular Tear. Non-Surgical Surgical
 DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes.
 Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
IP'Lumbar Spinal Stenosis
 A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
10801 Sixth St, Suite 120 Rancho Cucamonga, CA 91730 Tel (909) 890-2000 Fax (909) 890-2003 Visit our web site at: www.iehp.org.
 Percutaneous Image-Guided Lumbar Decompression for Lumbar Spinal Stenosis (PILD), Including the Commercial Procedure Known as Minimally Invasive Lumbar Decompression (mild -Vertos Medical) Policy: Based
Percutaneous Image-Guided Lumbar Decompression for Lumbar Spinal Stenosis (PILD), Including the Commercial Procedure Known as Minimally Invasive Lumbar Decompression (mild -Vertos Medical) Policy: Based
Balloon Kyphoplasty. Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures.
 Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis
 Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Research Article Partial Facetectomy for Lumbar Foraminal Stenosis
 Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis
 Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
REVIEW DECISION. Review Reference #: R0103014 Board Decision under Review: March 3, 2009
 REVIEW DECISION Re: Review Reference #: R0103014 Board Decision under Review: March 3, 2009 Date: Review Officer: Lyall Zucko The worker requests a review of the decision of WorkSafeBC (the Board) dated
REVIEW DECISION Re: Review Reference #: R0103014 Board Decision under Review: March 3, 2009 Date: Review Officer: Lyall Zucko The worker requests a review of the decision of WorkSafeBC (the Board) dated
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Imaged-Guided Minimally Invasive Lumbar Page 1 of 9 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Image-Guided Minimally Invasive Lumbar Professional Institutional
Imaged-Guided Minimally Invasive Lumbar Page 1 of 9 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Image-Guided Minimally Invasive Lumbar Professional Institutional
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Image-Guided Minimally Invasive Lumbar Decompression for Spinal Stenosis
 Image-Guided Minimally Invasive Lumbar Decompression for Spinal Stenosis Policy Number: 7.01.126 Last Review: 6/2015 Origination: 5/2010 Next Review: 6/2016 Policy Blue Cross and Blue Shield of Kansas
Image-Guided Minimally Invasive Lumbar Decompression for Spinal Stenosis Policy Number: 7.01.126 Last Review: 6/2015 Origination: 5/2010 Next Review: 6/2016 Policy Blue Cross and Blue Shield of Kansas
Hitting a Nerve: The Triggers of Sciatica. Bruce Tranmer MD FRCS FACS
 Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Overview Anatomy of the spinal canal What is spinal stenosis? > 1
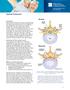 Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Patients with pain in the neck, arm, low back, or leg (sciatica) may benefit from ESI. Specifically, those with the following conditions:
 Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
PARADIGM SPINE. Brochure. coflex Interlaminar Stabilization
 PARADIGM SPINE Brochure Interlaminar Stabilization SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options. The continuum
PARADIGM SPINE Brochure Interlaminar Stabilization SPINAL STENOSIS WITH BACK PAIN THE RATIONALE FOR STABILIZATION For the treatment of spinal stenosis, surgeons have various treatment options. The continuum
Image-guided Spine Procedures for Relief of Severe Lower Back Pain:
 Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
mild Lumbar Decompression for the Treatment of Lumbar Spinal Stenosis
 The Neuroradiology Journal 24: 620-626, 2011 www.centauro.it mild Lumbar Decompression for the Treatment of Lumbar Spinal Stenosis D.F. SCHOMER 1, D. SOLSBERg 1, W. WONg 2, B.W. CHOPkO 3 1 Radiology Imaging
The Neuroradiology Journal 24: 620-626, 2011 www.centauro.it mild Lumbar Decompression for the Treatment of Lumbar Spinal Stenosis D.F. SCHOMER 1, D. SOLSBERg 1, W. WONg 2, B.W. CHOPkO 3 1 Radiology Imaging
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis
 Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Low Back Pain (LBP) Prevalence. Low Back Pain (LBP) Prevalence. Lumbar Fusion: Where is the Evidence?
 15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Consent for Lumbar Spine Surgery and Fusion at
 STEPHEN MARANO, M.D. JAMES COOK PA-C Consent for Lumbar Spine Surgery and Fusion at Patient Name: Patient Diagnosis: Lumbar Spinal Stenosis (Narrowing of the canal where the spinal cord and nerves are
STEPHEN MARANO, M.D. JAMES COOK PA-C Consent for Lumbar Spine Surgery and Fusion at Patient Name: Patient Diagnosis: Lumbar Spinal Stenosis (Narrowing of the canal where the spinal cord and nerves are
Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization
 APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
SPINE AND NECK SURGERY: MAKING A DECISION THAT S RIGHT FOR YOU
 1. GET THE FACTS: Back and neck pain affects 8 out of 10 people at some point in their life. Acute back and neck pain comes on suddenly and usually lasts from a few days to a few weeks. Chronic back and
1. GET THE FACTS: Back and neck pain affects 8 out of 10 people at some point in their life. Acute back and neck pain comes on suddenly and usually lasts from a few days to a few weeks. Chronic back and
Dynamic stabilization of the lumbar spine Robert W. Molinari
 Dynamic stabilization of the lumbar spine Robert W. Molinari Purpose of review This is a review of the recent literature involving dynamic posterior stabilization in the lumbar spine. Recent findings As
Dynamic stabilization of the lumbar spine Robert W. Molinari Purpose of review This is a review of the recent literature involving dynamic posterior stabilization in the lumbar spine. Recent findings As
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
 Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Lateral Lumbar Interbody Fusion (LLIF or XLIF)
 Lateral Lumbar Interbody Fusion (LLIF or XLIF) NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Aleve, Ibuprofen, Motrin, Naprosyn, Mobic, etc) OR ASPIRIN PRODUCTS
Lateral Lumbar Interbody Fusion (LLIF or XLIF) NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Aleve, Ibuprofen, Motrin, Naprosyn, Mobic, etc) OR ASPIRIN PRODUCTS
Surgical Guideline for Lumbar Fusion (Arthrodesis)
 I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
Surgery for cervical disc prolapse or cervical osteophyte
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: [email protected]
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: [email protected]
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery
 Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated And Fenestrated Pedicle
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 5 Ver. III. (May. 2014), PP 77-81 Polymethylmethacrylate (PMMA) Augmentation Of A Cannulated
Diagnosis and Treatment of Lumbar Spinal Canal Stenosis
 Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Low Back Pains Diagnosis and Treatment of Lumbar Spinal Canal Stenosis JMAJ 46(10): 439 444, 2003 Katsuro TOMITA Department of Orthopedic Surgery, Kanazawa University Abstract: Lumbar spinal canal stenosis
Ben Okafor FRCS FRCS.orth Consultant Orthopaedic & Spine Surgeon Whipps Cross University Hospital
 Ben Okafor FRCS FRCS.orth Consultant Orthopaedic & Spine Surgeon Whipps Cross University Hospital Classification Pathology Clinical features Imaging Treatment Options Outcomes Definition: 1. Narrowing
Ben Okafor FRCS FRCS.orth Consultant Orthopaedic & Spine Surgeon Whipps Cross University Hospital Classification Pathology Clinical features Imaging Treatment Options Outcomes Definition: 1. Narrowing
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Consent for Anterior Cervical Discectomy With Fusion and a Metal Plate at
 STEPHEN MARANO, M.D. JAMES COOK PA-C Consent for Anterior Cervical Discectomy With Fusion and a Metal Plate at Patient Name: Patient Diagnosis: Cervical Degenerative Disc Disease (wear and tear on the
STEPHEN MARANO, M.D. JAMES COOK PA-C Consent for Anterior Cervical Discectomy With Fusion and a Metal Plate at Patient Name: Patient Diagnosis: Cervical Degenerative Disc Disease (wear and tear on the
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary?
 White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA
 LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
Medical Policy Manual. Topic: Interspinous and Interlaminar Stabilization/Distraction Devices (Spacers) Date of Origin: October 2006.
 Medical Policy Manual Topic: Interspinous and Interlaminar Stabilization/Distraction Devices (Spacers) Section: Surgery Date of Origin: October 2006 Last Reviewed Date: December 2015 Policy No: 155 Effective
Medical Policy Manual Topic: Interspinous and Interlaminar Stabilization/Distraction Devices (Spacers) Section: Surgery Date of Origin: October 2006 Last Reviewed Date: December 2015 Policy No: 155 Effective
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
LOW BACK PAIN. common of these conditions include: muscle strain ( pulled muscle ), weak core muscles
 LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN
 Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
Cox Technic Case Report #60 sent 5/13/08 1 UPPER LUMBAR DISC HERNIATION WITH CENTRAL AND FAR LATERAL STENOTIC CHANGES RESULTING IN ANTERIOR THIGH PAIN History, Examination & Imaging Review: A 53-year-old
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
