the Cardiovascular System
|
|
|
- Marshall Lloyd
- 9 years ago
- Views:
Transcription
1 5 Chapter Anatomy Jones and & Physiology Bartlett Learning, LLC of the Cardiovascular System OUTLINE Introduction The Heart Structures of the Heart Conduction System Functions of the Heart The Blood Vessels and Circulation Blood Vessels Blood Pressure Blood Circulation Summary Critical Thinking Websites Review Questions OBJECTIVES pathway between the atrial and ventricular syncytia. Jones & After Bartlett reading Learning, this chapter, LLC readers should be able to: Jones AV bundle: & Bartlett The bundle Learning, of His; a large LLC structure that receives 1. Describe the organization of the cardiovascular NOT FOR SALE system OR DISTRIBUTION and the heart. NOT FOR the cardiac SALE impulse OR from DISTRIBUTION the distal AV node. It enters the upper part of the interventricular septum. 2. Identify the layers of the heart wall. Blood volume: The sum of formed elements and plasma 3. Describe the general features of the heart. volumes in the vascular system; most adults have about 5 L 4. Answer the question of why the left ventricle is of blood. more muscular than the right ventricle. 5. Describe the components Jones and & Bartlett functions of Learning, the LLC Capillaries: The smallest-diameter blood Jones vessels, & Bartlett which Learning, LL conducting system NOT of FOR the heart. SALE OR DISTRIBUTION connect the smallest arterioles NOT to the FOR smallest SALE venules. OR DISTRIBUT Cardiac conduction system: The initiation and distribution 6. Explain the events of the cardiac cycle. of impulses through the myocardium that coordinates the 7. Define cardiac output and stroke volume. cardiac cycle. 8. Distinguish among the types of blood vessels, their Cardiac cycle: A heartbeat; it consists of a complete series structures, and their functions. of systolic and diastolic events. 9. Jones Identify the & major Bartlett arteries Learning, and veins of LLC the Cardiac output: The volume discharged from the ventricle NOT pulmonary FOR SALE circuit as OR well DISTRIBUTION as the areas they serve. 10. Describe the hepatic portal system. KEY TERMS Aorta: The largest in the body, the aorta originates from the left ventricle of the heart and extends down to the abdomen, where it branches off. Aortic arch: The second section of the aorta; it branches into the brachiocephalic trunk, left common carotid, and left subclavian. Aortic valve: Located at the base of the aorta, the aortic valve has three cusps and opens to allow blood to leave the left ventricle during contraction. Arteries: Elastic vessels able to carry blood away from the heart under high pressure. Arterioles: Subdivisions of arteries; they are thinner and have muscles that are innervated by the sympathetic nervous system. Atria: The upper chambers of the heart; they receive blood returning to the heart. Atrioventricular node (AV node): A mass of specialized tissue located in the inferior interatrial septum beneath the endocardium; it provides the only normal conduction per minute, calculated by multiplying stroke volume by heart rate, in beats per minute. Cardiac veins: Those veins that branch out and drain blood from the myocardial capillaries to join the coronary sinus. Carotid sinuses: Enlargements near the base of the carotid Jones and Bartlett Publishers. arteries that contain baroreceptors and help to control blood pressure.
2 36 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System KEY TERMS continued Cerebral arterial circle: The circle of Willis; it connects the vertebral and internal carotid systems. Chordae tendineae: Strong fibers originating from the papillary muscles that attach to the cusps of the tricuspid valve. Coronary arteries: The first two aortic branches, which supply blood to the heart tissues. Coronary sinus: An enlarged vein joining the cardiac veins; it empties into the right atrium. Diastole: The relaxation of a heart structure. Diastolic Jones pressure: & Bartlett The lowest Learning, pressure that remains LLC in the arteries before the next ventricular contraction. Electrocardiogram (EKG): The recording of electrical changes in the myocardium during the cardiac cycle. The EKG machine works by placing nodes on the skin that connect via wires and respond to weak electrical changes of the heart. The abbreviation EKG is more commonly used than ECG. Endocardium: The inner layer of the heart wall. Epicardium: The outer layer of the heart wall. Functional syncytium: A mass of merging cells that functions as a unit. Hepatic portal system: The veins that drain the abdominal viscera, originating in the stomach, intestines, pancreas, and spleen, to carry blood through a hepatic portal vein to the liver. Inferior vena cava: Along with the superior vena cava, one of the two largest veins in the body; it is formed by the joining of the common iliac veins. Mitral Jones valve: The & bicuspid Bartlett valve; Learning, it lies between LLC the left atrium and NOT left ventricle, FOR SALE preventing OR blood DISTRIBUTION from flowing back into the left atrium from the ventricle. Myocardium: The thick middle layer of the heart wall that is mostly made of cardiac tissue. Pacemaker: The term used to refer to the sinoatrial node (SA node). Papillary muscles: Those muscles that contract as the heart s ventricles contract, pulling on the chordae tendineae to prevent the cusps from swinging back into the atrium. Pericardium: A membranous structure that encloses the heart and proximal ends of the large blood vessels and that consists of double layers. Peripheral resistance: A force produced by friction between blood and blood vessel walls. Pulmonary circuit: The venules and veins, which send deoxygenated blood to the lungs to receive oxygen and unload carbon dioxide. Introduction The human heart pumps blood through the arteries, which connect to smaller arterioles and then even smaller capillaries. It is here that nutrients, electrolytes, dissolved gases, and waste products are exchanged between the blood and surrounding tissues. The capillaries are thin-walled vessels interconnected with the smallest arteries and smallest veins. Pulmonary valve: Lying at the base of the pulmonary trunk, this valve has three cusps and allows blood to leave the right ventricle while preventing backflow into the ventricular chamber. Purkinje fibers: Consisting of branches of the AV bundle that spread and enlarge, these fibers are located near the papillary muscles; they continue to the heart s apex and cause the ventricular walls to contract in a twisting motion. Septum: A solid, wall-like structure that separates the left atria and ventricle from the right atria and ventricle. Sinoatrial node (SA node): A small mass of specialized tissue just beneath the epicardium in the right atrium that initiates impulses Jones through & the Bartlett myocardium Learning, to stimulate LLC contraction of cardiac muscle fibers. Stroke volume: The volume of blood discharged from the ventricle with each contraction; it is usually about 70 ml. Superior vena cava: Along with the inferior vena cava, one of the two largest veins in the body; the superior vena cava is formed by the joining of the brachiocephalic veins. Systemic circuit: The arteries and arterioles, which send oxygenated blood and nutrients to the body cells while removing wastes. Systole: The contraction of a heart structure. Systolic pressure: The maximum pressuring during ventricular contraction. Thyrocervical arteries: Those that branch off to the thyroid and parathyroid glands, larynx, trachea, esophagus, pharynx, and muscles of the neck, shoulder, and back. Tricuspid valve: Lying between the right atrium and ventricle, this valve allows blood to move from the right atrium into the right ventricle while preventing backflow. Vasoconstriction: The contraction of blood vessels, which reduces their diameter. Vasodilation: The relaxation of blood vessels, which increases their diameter. Veins: Blood vessels that carry blood back to the atria; they are less elastic than arteries. Ventricles: The lower chambers of the heart; they receive blood from the atria, which they pump out into the arteries. Venules: Microscopic vessels that link capillaries to veins. Vertebral arteries: One of the main divisions of the subclavian and common carotid arteries; the vertebral arteries run upward through the cervical vertebrae into the skull and supply blood to the vertebrae, their ligaments, and their muscles. Viscosity: Thickness or stickiness; the resistance of fluid to flow. In a biologic fluid, viscosity is caused by the attraction of cells to one another. Approximately 7,000 L of blood is pumped by the heart every day. In an average person s life, the heart will contract about 2.5 billion times. Blood flow throughout the body begins its return to the heart when the capillaries return blood to the venules and then to the larger veins. The cardiovascular system, therefore, consists of a closed circuit: the heart, arteries, arterioles, capillaries, venules, and veins (see Figure 5 1). The venules Jones and Bartlett Publishers.
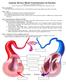
3 The Heart 37 Jugular vein Carotid Superior vena cava Inferior vena cava Renal Renal vein Aorta Common iliac Subclavian Subclavian vein Common NOT FOR SALE iliac vein OR DISTRIBUTION Aorta Pulmonary Hepatic vein Mesenteric arteries Femoral Femoral vein Great saphenous vein Pulmonary arteries Vena cavae Venules Right ventricle Oxygen-poor, CO 2 -rich blood Pulmonary circuit Systemic circuit Capillary beds of lungs where gas exchange occurs Left ventricle Pulmonary veins Aorta and branches Arterioles Capillary beds of all body tissues where gas exchange occurs Oxygen-rich, CO 2 -poor blood Pulmonary circulation Mesenteric veins Systemic circulation (b) NOT FOR (a) SALE OR DISTRIBUTION Figure 5 1 The circulatory system. (a) The circulatory system consists of a series of vessels that transport blood to and from the heart, the pump. (b) The circulatory system has two major circuits: the pulmonary circuit, which transports blood to and from the lungs, and the systemic circuit, which transports blood to and from the body (excluding the lungs). and veins are part of the pulmonary circuit because they send deoxygenated blood to the lungs to receive oxygen and unload carbon dioxide. The arteries and arterioles are part of the systemic circuit because they send oxygenated blood and nutrients to the body cells while removing wastes. All body tissues require circulation to survive. The Heart The human heart is a muscular organ containing four chambers that is situated just to the left of the midline of the thoracic cavity. It is approximately the size of a man s closed fist. The upper two chambers (atria) are divided by a wall- Jones and Bartlett Publishers.
4 38 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System like structure called the interatrial septum. The lower two chambers (ventricles) are divided by a similar structure called the interventricular septum. Between each atrium and ventricle, valves allow blood to flow in one direction, preventing backflow. Blood flow through the heart is shown in Figure 5 2. Blood that is low in oxygen flows into the right atrium from the veins known as the superior vena cava and inferior vena cava. The superior vena cava carries blood from the head, neck, chest, and arms. The inferior vena cava carries blood from the remainder of the trunk and the legs. Blood in the right atrium then flows through the right atrioventricular (tricuspid) valve into the right ventricle. From here it begins the pulmonary Jones circuit, & with Bartlett deoxygenated Learning, blood flowing LLC into the right NOT and left FOR pulmonary SALE arteries OR DISTRIBUTION and their smaller branches. The blood becomes oxygenated while moving through the lungs capillary beds. Also in this part of the system, carbon dioxide is released. Structures of the Heart The heart lies inside the thoracic cavity, resting on the diaphragm. It is hollow and cone-shaped, varying in size. The heart is within the mediastinum in between the lungs. Its posterior border is near the vertebral column, and its anterior border is near the sternum. Right pulmonary vein Superior vena cava (from head) Right pulmonary Right atrium Inferior vena cava (from body) Right ventricle Endocardium Myocardium Figure 5 2 Blood flow through the heart. Deoxygenated (carbon-dioxide-enriched) blood (blue arrows) flows into the right atrium from the systemic circulation and is pumped into the right ventricle. The blood is then pumped from the right ventricle into the pulmonary, which delivers it to the lungs. In the lungs, the blood releases its carbon dioxide and absorbs oxygen. Reoxygenated blood (red arrows) is returned to the left atrium, then flows into the left ventricle, which pumps it to the rest of the body through the systemic circuit. An average adult has a heart that is about 14 cm long by 9 cm wide. The base of the heart is actually the upper portion, where it is attached to several large blood vessels. This portion lies beneath the second rib. The distal end of the heart extends downward, to the left, ending in a blunt point called the apex, which is even with the fifth intercostal space. The three layers comprising the wall of the heart are the outer pericardium, middle myocardium, and inner endocardium (see Figure 5 2). The pericardium consists of connective tissue and some deep adipose tissue, and it protects the heart by reducing friction. The thick myocardium is mostly made of cardiac muscle tissue that is organized in planes and richly supplied by blood capillaries, lymph capillaries, and nerve fibers. Jones It pumps & blood Bartlett out of Learning, the chambers of LLC the heart. The endocardium is made up of epithelium and connective tissue with many elastic and collagenous fibers. It also contains blood vessels and specialized cardiac muscle fibers known as Purkinje fibers. The inside of the heart is divided into four hollow chambers, with two on the left and two on the right. The upper chambers are called atria and receive blood returning to the heart. They have auricles, which are small projections that extend anteriorly. The lower chambers are called ventricles and receive blood from the atria, which they pump out into the arteries (see Figure 5 2). The left atria and ventricle are separated from the right atria and ventricle by a solid walllike structure (septum). This keeps blood from one side of the heart from mixing with blood from the other side Aorta (except in a developing fetus). The atrioventricular valve (AV valve), Left pulmonary which consists of the mitral valve on Jones the & left Bartlett and the Learning, tricuspid valve LLC on the right, ensures one-way blood flow between the atria and ventricles. Left pulmonary The right atrium receives blood vein from two large veins called the superior vena cava and the inferior vena cava as well as a smaller vein (the coronary sinus), which drains blood into Left atrium the right atrium from the heart s myocardium. The tricuspid valve has projections (cusps) and lies between the right atrium and ventricle. This valve allows blood to move from the right atrium into the right ventricle while Interventricular preventing backflow. The cusps of the septum tricuspid valve are attached to strong fibers called chordae tendineae, which originate from small papillary Left ventricle muscles that project inward from the Pericardium ventricle walls. These muscles contract as the ventricle contracts. When the tricuspid valve closes, they pull on the chordae tendineae to prevent the cusps from swinging back into the atrium. Jones and Bartlett Publishers. The right ventricle s muscular wall is thinner than that of the left ventricle, as it only pumps blood to the
5 The Heart 39 lungs with a low resistance to blood flow. The Right left ventricle is thicker because it must force pulmonary Aorta blood to all body parts, with a much higher arteries resistance to blood flow. As the right ventricle Left pulmonary contracts, its blood increases in pressure to Superior arteries vena cava passively close the tricuspid valve. Therefore, this blood can only exit through the pulmonary Right trunk, which divides into Jones the left and & right Bartlett pulmonary arteries that supply the lungs. At the veins veins Learning, pulmonary LLC Left pulmonary trunk s base, there is a pulmonary valve with Right atrium three cusps that allow blood to leave the right Left atrium ventricle while preventing backflow into the Right atrioventriculaventricular Left atrio- ventricular chamber (see Figure 5 3). Four Jones pulmonary & Bartlett veins (two Learning, from each of LLC(tricuspid) Jones & Bartlett Learning, (tricuspid) LLC the lungs) supply the left atrium with blood. valve valve Blood passes from the left atrium into the left ventricle through the mitral valve (bicuspid Inferior vena valve), preventing blood from flowing back cava (from body) into the left atrium from the ventricle. Like Semilunar valves the tricuspid valve, the papillary muscles and Chordae Jones tendineae & Bartlett Learning, LLC chordae tendineae prevent the mitral valve s cusps from swinging back into the left atrium Left ventricle Right ventricle when the ventricle contracts. The mitral valve (a) Septum closes passively, directing blood through the large known as the aorta. At the base of the aorta is the aortic valve, with three cusps. This valve opens to allow blood to leave the left NOT ventricle FOR during SALE con-otraction. When the ventricle relaxes, the valve DISTRIBUTION closes to prevent blood from backing up into the ventricle. The mitral and tricuspid valves are known as atrioventricular valves because they lie Jones between & the Bartlett atria and Learning, ventricles. The LLC pulmonary NOT FOR and aortic SALE valves OR have DISTRIBUTION half-moon shapes and are therefore referred to as semilunar valves. Table 5 1 summarizes the various heart valves. The right atrium receives low-oxygen blood through the vena cava and coronary sinus. As (b) the right atrium contracts, the blood passes Figure 5 3 NOT Heart FOR valves. SALE (a) A cross-section OR DISTRIBUTION of the heart showing the four through the tricuspid valve into the right ventricle (see Figure 5 3). As the right ventricle chordae tendineae. chambers and the location of the major vessels and valves. (b) Photograph of contracts, the tricuspid valve closes. Blood moves through the pulmonary valve into the The left atrium contracts, moving blood through the pulmonary trunk and pulmonary arteries. It then enters the mitral valve into the left ventricle. When the left ventricle capillaries of the alveoli of the lungs, where gas exchanges contracts, the mitral valve closes. Blood moves through the occur. This freshly oxygenated NOT FOR blood then SALE returns OR to DISTRIBUTION the heart aortic valve into the aorta and its branches. The first two aortic branches are called the right and left coronary through the pulmonary veins, into the left atrium. arteries. Table 5 1 The Heart Valves Heart Valve Location Action Tricuspid valve Between right atrium and right ventricle During ventricular contraction, it prevents blood from moving from right ventricle into right atrium. Pulmonary valve At entrance to pulmonary trunk During ventricular relaxation, it prevents blood from moving from pulmonary trunk into right ventricle. Mitral (bicuspid) valve Between left atrium and left ventricle During ventricular contraction, it prevents blood from moving from left ventricle into left atrium. Aortic valve At entrance to aorta During ventricular relaxation, it prevents blood from moving from aorta into left ventricle. Jones and Bartlett Publishers.
6 40 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System They supply blood to the heart tissues, with openings lying almost simultaneously. The impulse passes along junctional just beyond the aortic valve. fibers of the conduction system to a mass of specialized tissue FOR called SALE the atrioventricular OR DISTRIBUTION node (AV node), located in NOT FOR SALE The body OR tissues DISTRIBUTION require continual beating of the heart NOT because they need freshly oxygenated blood to survive. Coronary branches supply many capillaries in the myocar- The AV node provides the only normal conduction pathway the inferior interatrial septum, beneath the endocardium. dium. These arteries have smaller branches with connections between the atrial and ventricular syncytia. Impulses are called anastomoses between vessels providing alternate blood slightly delayed due to the small diameter of the junctional pathways (collateral circulation). Jones These & Bartlett pathways may Learning, supply LLC fibers. The atria, therefore, have more Jones time & to Bartlett contract and Learning, LL oxygen and nutrients to NOT the myocardium FOR SALE when OR blockage DISTRIBUTION of a empty all of their blood into the NOT ventricles FOR before SALE ventricular OR DISTRIBUT coronary occurs. Branches of the cardiac veins drain contraction occurs. blood from the myocardial capillaries, joining an enlarged vein, When the cardiac impulse reaches the distal AV node, the coronary sinus, which empties into the right atrium. it passes into a large AV bundle (bundle of His), entering the upper part of the interventricular septum. Nearly halfway down the septum, Jones these & Bartlett branches spread Learning, into enlarged LLC Conduction Jones System & Bartlett Learning, LLC Strands NOT and FOR clumps SALE of specialized OR DISTRIBUTION cardiac muscle contain Purkinje fibers, NOT extending FOR SALE into the papillary OR DISTRIBUTION muscles. They only a few myofibrils and are located throughout the heart. continue to the heart s apex, curving around the ventricles These areas initiate and distribute impulses through the myocardium, comprising the cardiac conduction system that numerous small branches that become continuous with car- and passing over their lateral walls. The Purkinje fibers have coordinates the cardiac cycle (see Figure 5 4). The sinoatrial Bartlett node (SA Learning, node) is a small LLC mass of specialized tissue just Jones lation causes & Bartlett the ventricular Learning, walls to LLC contract in a twisting diac muscle fibers and irregular whorls. Purkinje fiber stimu- Jones & beneath the epicardium, in the right atrium. It is located near motion, to force blood into the aorta and pulmonary trunk. the opening of the superior vena cava, with fibers continuous An electrocardiogram (EKG) is used to record electrical changes in the myocardium during the cardiac cycle. with those of the atrial syncytium. The SA node s cells can reach threshold on their own, initiating impulses through the myocardium, stimulating congram, the abbreviation EKG is more commonly used. Because Although ECG is the correct abbreviation for electrocardiotraction of cardiac muscle fibers. Its rhythmic activity occurs phlebotomists do not generally perform this procedure, it is 70 to 80 times per minute in a normal adult. Since it generates the heart s rhythmic NOT contractions, FOR SALE it is often OR referred DISTRIBUTION to ions that influence heart action NOT are potassium FOR SALE and calcium. OR DISTRIBUT not discussed in depth in this chapter. The most important as the pacemaker. Excess extracellular potassium ions (hyperkalemia) decrease The path of a cardiac impulse travels from the SA node contraction rates and forces, while deficient extracellular into the atrial syncytium, and the atria begin to contract potassium ions (hypokalemia) may cause a potentially life- SINOATRIAL (SA) NODE (pacemaker) Atrioventricular bundle Purkinje fibers R ATRIOVENTRICULAR (AV) NODE Interventricular septum P T Conduction myofibers (Purkinje fibers) Right and left branches of AV bundle Figure 5 4 The cardiac conduction system. Also shown is a tracing of an EKG. The P wave corresponds to atrial depolarization, the QRS coplex to ventricular depolarization, and the T wave to ventricular repolarization. Q S Jones and Bartlett Publishers.
7 The Blood Vessels and Circulation 41 threatening abnormal heart rhythm (arrhythmia). Excess flow backward at this point due to a valve malfunction, a extracellular calcium ions (hypercalcemia) can cause the heart heart murmur will result. To summarize, the right side of the NOT FOR SALE to contract OR for DISTRIBUTION an abnormally long time, while low extracellular calcium ions (hypocalcemia) depress heart action. pumps oxygen-rich blood toward the body tissues. NOT heart FOR pumps SALE oxygen-poor OR DISTRIBUTION blood to the lungs, and the left side The contraction of the heart is called systole, and its relaxation is called diastole. The systolic blood pressure is the first Functions of the Heart number in a blood pressure reading, measuring the strength The heart chambers are coordinated Jones & so Bartlett that their Learning, actions are LLC of contraction. The diastolic blood Jones pressure & is Bartlett the second Learning, LL effective. The atria contract NOT (atrial FOR systole) SALE as OR the ventricles DISTRIBUTION number in a blood pressure reading, NOT measuring FOR SALE the strength OR DISTRIBUT relax (ventricular diastole). Likewise, ventricles contract of relaxation. The right ventricle does not need to pump blood (ventricular systole) as atria relax (atrial diastole). Then a with as much force as the left ventricle. This is so because brief period of relaxation of both atria and ventricles occurs. the right ventricle supplies blood to the nearby lungs and the This complete series of events makes up a heartbeat, also pulmonary vessels are wide and relatively short. This means called Jones a cardiac & cycle. Bartlett Learning, LLC that the walls of Jones the right & ventricle Bartlett are thinner Learning, and less LLC muscular than those NOT of the FOR left ventricle, SALE which OR DISTRIBUTION must pump blood One NOT cardiac FOR cycle SALE causes OR pressure DISTRIBUTION in the heart chambers to rise and fall and valves to open and close. Early during diastole, pressure in the ventricles is low, causing the AV valves to the entire body. to open and the ventricles to fill with blood. Nearly 70% of returning blood enters the ventricles before contraction. As the atria contract, the remaining 30% is pushed into the ventricles. As the ventricles contract, ventricular pressure rises. When ventricular pressure exceeds atrial pressure, the AV valves close and papillary muscles contract, preventing the cusps of the AV valves from bulging into the atria excessively. During ventricular contraction, the AV valves are closed, and atrial pressure is low. Blood flows into the atria while the ventricles are contracting, so that the atria are prepared for Blood Vessels the next cardiac cycle. As ventricular pressure exceeds pulmonary trunk and aorta pressure, the pulmonary and aortic valves open. Blood is ejected from the ventricles into these arteries, and ventricular pressure drops. When ventricular pressure is lower than in the aorta and pulmonary trunk, the semilunar valves close. When NOT ventricular FOR SALE pressure OR is lower DISTRIBUTION than atrial pressure, the AV valves open, and the ventricles begin to refill. A heartbeat makes a characteristic double thumping sound when heard through a stethoscope. This is due to the vibrations of the heart tissues related to the valves closing. The first thumping sound occurs during ventricular contraction when the AV valves close. The second sound occurs during ventricular relaxation when the pulmonary and aortic valves close. Cardiac muscle fibers are similar in function to skeletal muscle fibers, but are connected in branched networks. If any part of the network is stimulated, impulses are sent through- out the heart, and it contracts as a single unit. A functional syncytium is a mass of merging cells that functions as a unit. There are two of these structures in the heart: one in the atrial walls and another in the ventricular walls. A small area of the right atrial floor is the only part of the heart s muscle fibers that is not separated by the heart s fibrous skeleton. Here, cardiac conduction system fibers connect the atrial syncytium NOT and the FOR ventricular SALE syncytium. OR DISTRIBUTION Newly oxygenated blood flows into the left and right pulmonary veins, returning to the left atrium (see Figure 5 3). Blood then flows through the left atrioventricular (bicuspid or mitral) valve into the left ventricle, passing through the aortic semilunar valve into the systemic circuit (via the ascending aorta). The systemic circuit moves blood to the body tissues, supplying their required oxygen. Should blood The Blood Vessels and Circulation The blood vessels of the human body carry blood to every type of tissue and organ. Vessels decrease in size as they move away from the heart (arteries and arterioles), ending in the capillaries, and then increase in size as they move toward the heart (venules and veins). The largest in the body is the aorta, with the largest veins being the venae cavae, each being approximately 1 in wide. There are five general classes of blood vessels in the cardiovascular system: arteries, arterioles, capillaries, venules, and veins (see Figure 5 5). Arteries are elastic vessels that are very strong, able to carry blood away from the heart under high pressure. They Jones subdivide & Bartlett into thinner Learning, tubes that LLC give rise to branched, NOT finer FOR arterioles. SALE An OR s DISTRIBUTION wall consists of three distinct layers, as shown in Figure 5 6. The innermost tunica interna is made up of a layer of simple squamous epithelium known as endothelium. It rests on a connective tissue membrane with many elastic, collagenous fibers. The endothelium helps prevent blood clotting and may also help in regulating blood flow. It releases nitric oxide to relax the smooth muscle of the vessel. Vein walls are similar but not identical to walls. The middle tunica media makes up most of an arterial wall, including smooth muscle fibers and a thick elastic connective tissue layer. The outer tunica externa (tunica adventitia) is thinner, mostly made up of connective tissue with irregular fibers it is attached to the surrounding tissues. Smooth and arteriole muscles are innervated by the sympathetic nervous system. Vasomotor fibers receive impulses to contract and reduce blood vessel diameter (vasoconstriction). When inhibited, the muscle fibers relax and the vessel s diameter increases (vasodilation). Jones & Bartlett Changes in Learning, and arteriole LLC diameters greatly NOT affect FOR blood SALE flow OR and pressure. DISTRIBUTION Larger arterioles also have three layers in their walls, which get thinner as arterioles lead to capillaries. Very small arteriole walls only have an endothelial lining and some smooth muscle fibers, with a small amount of surrounding connective tissue. The smallest-diameter blood vessels are capillaries, which connect the smallest arterioles to the smallest venules. The Jones and Bartlett Publishers.
8 42 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System From heart To heart Elastic arteries Capillaries Muscular arteries and arterioles Venules and medium veins Large veins Figure 5 5 The structure and diameter of blood vessel walls walls of capillaries are also composed of endothelium and form the semipermeable layer through which substances in blood are exchanged with substances in tissue fluids surrounding cells of the body. Capillary walls have thin slits where endothelial cells overlap. These slits have various sizes, affecting permeability. Capillaries of muscles have smaller openings than those of the glands, kidneys, and small intestine. Tissues with higher metabolic rates (such as muscles) have many more capillaries than those with slower metabolic rates (such as cartilage). Some capillaries pass directly from arterioles to venules while others have highly branched networks (see Figure 5 7). Precapillary sphincters control blood distribution through capillaries. Based on the demands of cells, these sphincters constrict or relax so that blood can follow specific pathways to meet Jones tissue cellular & Bartlett requirements. Learning, LLC NOT Gases, metabolic FOR SALE by-products, OR DISTRIBUTION and nutrients are exchanged between capillaries and the tissue fluid surrounding body Endothelium cells. Capillary walls allow the diffusion of blood with high levels of oxygen and nutrients. They also allow high levels of carbon dioxide and other wastes to move from the tissues into the capillaries. Plasma proteins usually cannot move through the capillary walls due to their large size, so they remain in the blood. Blood pressure generated when capillary walls contract provides force for filtration via hydrostatic pressure. 81 West Street Main Street 132 Clark Street Jones & Morales Bartlett Avenue Learning, LLC Bruno Street Jones & Bartlett Learning, LL East Street 65 Tunica intima Metarteriole NOT FOR SALE Tunica OR DISTRIBUTION media NOT FOR SALE Venule OR DISTRIBUT Tunica adventitia Arteriole Capillaries Figure 5 6 General structure of the blood vessel. The shown here consists of three major layers, the tunica intima, tunica media, and tunica adventitia. Precapillary sphincters Figure 5 7 Similar to the way roadways are designed, larger arterioles and venules are interconnected with smaller capillaries. Jones and Bartlett Publishers.
9 The Blood Vessels and Circulation 43 Blood pressure is strongest when blood leaves the heart Blood Pressure and weaker as the distance from the heart increases because of Blood pressure is defined as the force that blood exerts against NOT FOR SALE friction (peripheral OR DISTRIBUTION resistance) between the blood and the vessel walls. Therefore, blood pressure is highest in the arteries, pressure in arteries supplied by the aortic branches, even the inner walls of blood vessels. It most commonly refers to less so in the arterioles, and lowest in the capillaries. Filtration though it actually occurs throughout the vascular system. occurs mostly at the arteriolar ends of capillaries because the Arterial blood pressure rises and falls according to cardiac pressure is higher than at the venular ends. Plasma proteins cycle phases. The maximum pressure during ventricular trapped in capillaries create Jones an osmotic & Bartlett pressure Learning, that pulls LLC contraction is called the systolic pressure. water into the capillaries NOT (colloid FOR osmotic SALE pressure). OR DISTRIBUTION The lowest pressure that remains NOT FOR in the arteries SALE before OR DISTRIBUT Capillary blood pressure favors filtration while plasma the next ventricular contraction is called the diastolic pressure. Arterial blood pressure is measured with a device called colloid osmotic pressure favors reabsorption. At the venular ends of capillaries, blood pressure has decreased due to a sphygmomanometer (blood pressure cuff). Its results are resistance so that reabsorption can occur. reported as a fraction of the systolic pressure over the diastolic pressure, Jones such as 120/80. & Bartlett The upper Learning, (first) number LLC More Jones fluid usually & Bartlett leaves capillaries Learning, than returns LLCto them. Lymphatic NOT FOR capillaries SALE have closed OR DISTRIBUTION ends and collect excess fluid indicates the NOT arterial FOR systolic SALE pressure OR in millimeters DISTRIBUTION of mercury (mm Hg), and the lower (second) number indicates the to return it via lymphatic vessels to the venous circulation. Unusual events may cause excess fluid to enter spaces between arterial diastolic pressure, also in millimeters of mercury. A tissue cells, often in response to chemicals such as histamine. If millimeter of mercury is a unit of pressure that is equal to enough fluid leaks out, lymphatic vessels can be overwhelmed, of normal atmospheric pressure. This means that a Jones & and Bartlett affected Learning, tissues swell and LLC become painful. Jones blood pressure & Bartlett of 120/80 Learning, displaces 120 LLC mm Hg on a sphygmomanometer, FOR SALE showing OR the DISTRIBUTION systolic pressure, and also displaces Venules are microscopic vessels that link capillaries to NOT veins, which carry blood back to the atria. Vein walls are 80 mm Hg on the same device, showing diastolic pressure. similar to arteries but have poorly developed middle layers. Figure 5 8 shows changes in blood pressure as the distance Because they have thinner walls that are less elastic than from the left ventricle increases. arteries, their lumens have a greater diameter. The walls are distended as blood surges into them Many veins have flaplike valves projecting inward from from the ventricles, but they recoil Jones almost immediately. & Bartlett This Learning, LL their linings. These valves often have two structures that close expansion and recoiling can be felt as a pulse in an near if blood begins to back NOT up in FOR the vein. SALE They aid OR in returning DISTRIBUTION the surface of the skin. Most commonly, the radial is blood to the heart, opening if blood flow is toward the heart, used to take a person s pulse, although the carotid, brachial, but closing if it reverses. Unlike the arteries, veins do not and femoral arteries are also checked. Arterial blood pressure depends on heart rate, stroke volume, blood volume, have sufficient pressure from the contractions of the heart to keep blood moving through them. To keep blood flowing, peripheral resistance, and blood viscosity. the veins Jones rely on & the Bartlett movement Learning, of nearby skeletal LLCmuscles, Heart action determines the amount of blood entering as well NOT as the FOR opening SALE and closing OR DISTRIBUTION of the valves within them. the arterial system NOT with FOR each SALE ventricular OR contraction. DISTRIBUTION Stroke Therefore, a major structural difference between veins and volume is defined as the volume of blood discharged from arteries is that arteries do not have valves. the ventricle with each contraction. An average adult male s Veins also act as reservoirs for blood in certain conditions, stroke volume is about 70 ml. The cardiac output is defined such as during arterial hemorrhage. Resulting venous constrictions Bartlett help Learning, to maintain blood LLCpressure by returning more Jones calculated & Bartlett by multiplying Learning, the stroke volume LLC by the heart rate, as the volume discharged from the ventricle per minute. It is Jones & NOT FOR SALE blood to OR the heart, DISTRIBUTION ensuring an almost normal blood flow NOT in FOR beats per SALE minute. OR So DISTRIBUTION if the stroke volume is 70 ml and the even when up to one-quarter of the blood volume is lost. See heart rate is 75 beats per minute (bpm), the cardiac output Table 5 2 for a summary of blood vessel characteristics. is 5,250 ml/min. Blood pressure varies with cardiac output Table 5 2 Characteristics of Blood Vessels Type of Vessel Vessel Wall Actions Artery Arteriole Three-layer thick wall (endothelial lining, middle smooth muscle and elastic connective tissue layer, and outer connective tissue layer) Three-layer thinner wall (smaller arterioles have an endothelial lining, some smooth muscle tissue, and a small amount of connective tissue) Carries relatively high-pressure blood from the heart to the arterioles Helps control blood flow from arteries to capillaries by vasoconstriction or vasodilation Capillary One layer of squamous epithelium Has a membrane allowing nutrients, gases, and wastes to be exchanged between blood and tissue fluid Venule Thinner wall than arterioles, with less smooth muscle and elastic connective tissue Jones & Bartlett Vein Learning, Thinner wall LLC than arteries but similar layers; poorly developed middle layer; some have flaplike valves Connects capillaries to veins Jones and Bartlett Publishers. Carries relatively low-pressure blood from venules to the heart; valves prevent blood backflow; veins serve as blood reservoirs
10 44 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System and increases or decreases based upon similar changes in stroke volume or heart rate. NOT FOR SALE Blood OR volume DISTRIBUTION is defined as the sum of formed elements and plasma volumes in the vascular system. Blood volume varies with age, body size, and gender. Most adults have approximately 5 L of blood, which makes up 8% of the body weight in kilograms. Blood pressure and volume are usually directly proportional. Any Jones changes & in Bartlett volume can Learning, initially LLC alter pressure. When NOT measures FOR are taken SALE to restore OR DISTRIBUTION normal blood volume, normal blood pressure can be reestablished. Fluid balance fluctuations may also affect blood volume. The resistance of arteries to blood flow is defined as Direction of peripheral resistance. The degree of peripheral resistance blood flow is determined Jones by & the Bartlett blood vessel Learning, diameter LLC and the force Jones & Bartlett Total Learning, cross-sectional LLC of contraction exerted by vascular smooth muscle. Therefore, peripheral resistance is a factor that accounts for blood area of vessels pressure. Blood pressure Viscosity is defined as the resistance of a fluid to flow. In a biologic fluid, viscosity is caused by the attraction of molecules Bartlett or cells Learning, to one another. LLCThe higher the viscosity, the Jones & greater the resistance to flowing. Blood viscosity is increased by blood cells and plasma proteins. The greater the resistance, Velocity of blood the greater the force needed to move the blood. Blood pressure rises as blood viscosity increases, and vice versa. Blood pressure (BP) is calculated by multiplying cardiac output (CO) by peripheral resistance (PR). Normal arterial pressure is maintained by regulating these two factors. Ideally, the volume of blood NOT discharged FOR SALE from the OR heart DISTRIBUTION should be equal to the volume entering the atria and ventricles. Fiber length and force of contraction are interrelated because of the stretching of the cardiac muscle cell just before contraction. Arteries Capillaries Veins This is known as the Frank-Starling law of the heart, and it is important Jones during & Bartlett exercise when Learning, greater amounts LLC of blood Jones Arterioles& Bartlett Venules Learning, LLC return NOT to the FOR heart SALE from the OR veins. DISTRIBUTION Figure 5 8 NOT Blood pressure FOR in SALE the circulatory OR system. DISTRIBUTION Blood Peripheral resistance also controls blood pressure. pressure declines in the circulatory system as the vessels branch. Changes in the diameters of arterioles regulate peripheral Arterial pressure pulses because of the heartbeat, but pulsation is lost by the time the blood reaches the capillary networks, creating an resistance. The vasomotor center of the medulla oblongata even flow through body tissues. Blood pressure continues to decline controls peripheral resistance. When arterial blood pressure in the venous side of the circulatory system. Jones & increases Bartlett suddenly, Learning, baroreceptors LLC in the aorta and carotid NOT FOR SALE arteries OR alert DISTRIBUTION the vasomotor center, which vasodilates the vessels to decrease peripheral resistance. Carbon dioxide, arteries, which enter the right and left lungs, respectively. oxygen, and hydrogen ions also influence peripheral resistance by affecting precapillary sphincters and smooth arteworks associated with the walls of the alveoli, where gas is Repeated divisions connect to arterioles and capillary netriole wall muscles. exchanged between blood and air. The pulmonary capillaries Blood flow through the venous system depends only lead to venules and then veins. Four pulmonary veins, two slightly on heart action, but more so on skeletal muscle contraction, movements of from each lung, return blood to the left atrium, completing NOT breathing, FOR and SALE the vasoconstriction OR DISTRIBUTION the vascular loop of the pulmonary NOT circuit. FOR SALE OR DISTRIBUT of veins (venoconstriction). As skeletal muscles press on veins The systemic circuit involves the movement of freshly with valves, some blood moves from one valve section to oxygenated blood from the left atrium to left ventricle, then another, helping to push blood forward through the venous into the aorta and its branches, leading to all body tissues. system to the heart. During inspiration, thoracic cavity pressure is reduced while abdominal cavity pressure is increased. that returns Eventually it makes its way to the companion vein system blood Jones to the & right Bartlett atrium. Learning, LLC Blood NOT is then FOR squeezed SALE out of OR abdominal DISTRIBUTION veins and forced into thoracic veins. When venous pressure is low, the walls of the The Arteries veins contract to help force blood out toward the heart. The largest-diameter in the body is the aorta, extending upward from the left ventricle to arch over the heart to Blood Circulation the left, descending anterior and to the left of the vertebral Jones & Blood Bartlett enters Learning, the pulmonary LLC circuit from the right ventricle Jones column. & The Bartlett first portion Learning, of the aorta LLC is called the ascending NOT FOR SALE through OR the pulmonary DISTRIBUTION trunk, which extends upward posteriorly from the heart. It divides into right and left pulmonary left and right coronary arteries originate in the aortic NOT aorta. FOR It SALE begins at OR the aortic DISTRIBUTION valve of the left ventricle. The sinus. Jones and Bartlett Publishers.
11 The Blood Vessels and Circulation 45 This origination occurs at the base of the ascending aorta, slightly superior to the aortic valve. The aortic arch curves across the superior surface of the heart. It connects the ascending aorta with the descending aorta (see Figure 5 9). Three arteries originate along the aortic arch. They deliver blood to the head, neck, shoulders, and upper limbs. These arteries are as follows: 1. The brachiocephalic trunk 2. The left common carotid 3. The left subclavian The brachiocephalic trunk ascends only for a short distance before it branches to form the right subclavian and right common carotid arteries. The descending aorta is continuous with the Jones aortic arch. & Bartlett The diaphragm Learning, divides the LLC descending aorta NOT into a FOR superior SALE thoracic OR aorta DISTRIBUTION and an inferior abdominal aorta. The branches of the thoracic aorta include the bronchial, pericardial, esophageal, mediastinal, and intercostal arteries. The abdominal aorta, beginning immediately inferior to the diaphragm, is a continuation of the thoracic aorta (see Figure 5 9). It delivers blood to the abdominopelvic organs and structures. The abdominopelvic branches of the aorta include the following: celiac, phrenic, superior mesenteric, suprarenal, renal, gonadal, inferior mesenteric, lumbar, middle sacral, and common lilac arteries. Table 5 3 summarizes the major branches of the aorta. The subclavian and common carotid arteries supply blood to the neck, head, and brain. The main divisions of these arteries are the vertebral and thyrocervical arteries. The vertebral arteries run upward through the cervical vertebrae into the skull and supply blood to the vertebrae and to their ligaments and muscles. They unite in the cranial cavity to form Jones the basilar & Bartlett, Learning, which branches LLC to the pons, midbrain, NOT FOR and cerebellum. SALE OR It ultimately DISTRIBUTION divides into the two posterior cerebral arteries. The posterior cerebral arteries help form the cerebral arterial circle (also known as the circle of Willis), connecting the vertebral and internal carotid systems (see Figure 5 10). These united systems provide alternate blood pathways to circumvent blockages and reach brain tissues and to equalize blood pressure in the brain s blood supply. The thyrocervical arteries give off branches to the thyroid and parathyroid glands, larynx, trachea, esophagus, pharynx, and muscles of the neck, shoulder, and back. The left and right common carotid arteries separate into the internal and external carotid arteries. Table 5 4 discusses these arteries. Near the base of the carotid arteries are enlargements (carotid sinuses) that contain baroreceptors and help to control blood pressure. Jones & Bartlett Learning, LLC The subclavian, which is a branch of the brachiocephalic, continues into the arm, passing between the clavicle and first rib to become the axillary. It becomes the brachial and gives rise to a deep brachial. The ulnar leads down to the lower arm, on the ulnar side of the forearm to the wrist. Some of its branches supply the elbow joint, while others supply the muscles of the forearm. The radial provides blood to the wrist and hand, traveling along the radial side of the forearm to the wrist. It also supplies the lateral muscles of the forearm. Near the wrist, it approaches the surface, providing a point where the radial pulse may easily be taken. The internal thoracic branches into two anterior intercostal arteries supplying the intercostal muscles and mammary glands. The posterior intercostal arteries supply other intercostal muscles as well as the vertebrae, spinal cord, and deeper back muscles. The internal thoracic and external iliac provide blood to the anterior abdominal wall while the Jones phrenic & Bartlett and lumbar Learning, supply LLC blood to posterior and lateral abdominal wall structures. The major vessels of the arterial system include the common iliac Table 5 3 Major Branches of the Aorta Branch Area of Aorta Main Regions or Organs Supplied Right and left coronary arteries Ascending aorta Heart Brachiocephalic Arch of the aorta Left common carotid Left subclavian Descending aorta: Jones & Bartlett Learning, Thoracic aorta LLC Bronchial Pericardial Esophageal Mediastinal Posterior intercostal Descending aorta: Celiac Phrenic Superior mesenteric Suprarenal Renal Gonadal Inferior mesenteric Lumbar Middle sacral Common iliac Abdominal aorta Right upper limb and right side of head Left side of head Left upper limb Bronchi Pericardium Esophagus Mediastinum Thoracic wall Upper digestive tract organs Diaphragm Small and large intestines Adrenal gland Kidney Ovaries or testes Lower large intestine Abdominal wall (posterior) Sacrum and coccyx Lower abdominal wall, pelvic organs, lower limbs Jones and Bartlett Publishers.
12 46 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System Internal carotid External carotid Vertebral Brachiocephalic trunk Axillary Ascending aorta Brachial Abdominal aorta Superior mesenteric Inferior mesenteric Common iliac External iliac Deep palmar Common carotid arteries Subclavian Arch of the aorta Descending aorta Thoracic aorta Branches of celiac trunk Renal Gonadal Radial Ulnar Superficial palmar Digital arteries Femoral Popliteal Anterior tibial Posterior tibial Peroneal Arcuate Figure 5 9 Overview of the arteries Jones and Bartlett Publishers.
13 The Blood Vessels and Circulation 47 Posterior cerebral Circle of Willis Superficial temporal Basilar Vertebral Internal carotid External carotid Common carotid Middle cerebral Superior thyroid Anterior cerebral Jones & Bartlett Learning, Ophthalmic LLC Common iliac Internal iliac Maxillary Facial Lingual External iliac Internal pudental Obturator Deep femoral Lateral femoral circumflex Medial femoral circumflex Femoral Jones & Bartlett Learning, LLC Thyrocervical Jones & Subclavian Bartlett Learning, LLC Brachiocephalic trunk Popliteal Arch of the aorta Anterior tibial (a) Ascending aorta Descending aorta Common carotid Vertebral Thyrocervical Posterior tibial Peroneal Costocervical Suprascapula Thoracoacromial Axillary Posterior humeral circumflex Anterior humeral circumflex Brachial Deep brachial Dorsalis pedis Arcuate (c) Medial plantar Metatarsal arteries Radial Ulnar (b) Deep palmar Jones & Bartlett Learning, Superficial palmar LLC NOT FOR SALE OR Digital DISTRIBUTION arteries Figure 5 10 Detailed views of the arteries in the body Jones and Bartlett Publishers.
14 48 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System Table 5 4 Major Branches of the Carotid Arteries Branch Carotid Artery Main Regions or Organs Supplied Superior thyroid Lingual Facial Occipital Posterior auricular Maxillary Superficial temporal Ophthalmic Anterior choroid Anterior cerebral External Internal Larynx and thyroid gland Salivary glands and tongue Chin, lips, nose, palate, and pharynx Meninges, neck muscles, and posterior scalp Ear and lateral scalp Cheeks, eyelids, jaw, and teeth Parotid salivary gland and surface of face and scalp Eyes and eye muscles Brain and choroid plexus Frontal and parietal lobes of brain arteries, internal iliac, femoral, popliteal, Veins that drain blood from the lower limbs are also subdivided, like those of the upper limbs, into deep and superficial anterior tibial, and posterior tibial. groups. The deep anterior tibial vein and posterior tibial vein The Veins merge to from the popliteal vein (which is located deep in The vessels of the venous system are more difficult to follow the leg, behind the knee), continuing upward as the femoral than those of the arterial system. They connect in irregular Jones vein and & then Bartlett the external Learning, iliac vein. LLC networks, with many unnamed vessels joining to form larger The saphenous veins of the lower leg communicate with veins. Larger veins typically parallel the locations of arteries one another as well as the deeper veins of the leg and thigh, and have similar names. The veins from all parts of the body allowing blood to return to the heart from the lower extremities by several routes. In the pelvis, vessels carry blood away besides the lungs and heart converge into the superior vena cava and inferior vena cava, leading to the right atrium. from the reproductive, urinary, and digestive organs via the The external jugular veins descend on either side of the internal iliac veins. These unite with the external iliac veins neck and empty into the right subclavian vein and left subclavian vein (see Figure to form the common iliac veins and eventually the inferior NOT 5 11). FOR The SALE internal OR jugular DISTRIBUTION veins vena cava. The great saphenous vein runs the entire length descend through the neck to join the subclavian veins, forming brachiocephalic veins on each side, above the clavicles. vein in the body. of the leg (see Figure 5 12c) and is considered the longest They then merge to form the superior vena cava. Deep and superficial veins drain the upper limbs and shoulders. Jones The & superficial Bartlett veins Learning, connect via LLC complex networks NOT just FOR under the SALE skin and OR communicate DISTRIBUTION with the deeper The cardiovascular system consists of the heart and blood Summary vessels (see Figure 5 12). The basilic vein ascends to join the vessels. It provides oxygen and nutrients to tissues while brachial vein, merging to form the axillary vein. The cephalic removing wastes. The heart is located within the mediastinum, resting on the diaphragm. The wall of the heart has vein ascends upward to empty into the axillary vein, and later it becomes the subclavian vein. three layers: the epicardium, myocardium, and endocardium. The brachiocephalic and azygos veins drain the abdominal and thoracic walls. The azygos vein ascends through the Jones The heart & Bartlett is divided into Learning, two atria and LLC two ventricles. Blood NOT low FOR in oxygen SALE and OR high in DISTRIBUTION carbon dioxide enters the right side mediastinum to join the superior vena cava. Its tributaries of the heart and is pumped into the pulmonary circulation. include the posterior intercostal veins, superior hemiazygos veins, and inferior hemiazygos veins. The right and left dioxide, it returns to the left side of the heart. The left ven- After oxygenation in the lungs and some removal of carbon ascending lumbar veins have vessels from the lumbar and tricle pumps blood out of the heart to the rest of the body. sacral regions. The cardiac cycle consists of the atria contracting while Most veins carry blood directly to the heart s atria, except the ventricles relax, and vice versa. Electrical activity of the for veins that drain the abdominal viscera (see Figure 5 13). cardiac cycle can be recorded via an electrocardiogram. The They originate in the stomach, intestines, pancreas, and cardiac cycle consists of the P wave, QRS complex, and T spleen to carry blood through a hepatic portal vein to the wave. Blood vessels form a closed circuit of tubes that carry liver. This pathway is called the hepatic portal system. It blood from the heart to the body cells and back again. This includes the right and left gastric veins, superior mesenteric circuit consists of arteries, arterioles, capillaries, venules, and vein, and splenic vein. veins. Blood pressure is the force that blood exerts against NOT The liver FOR helps SALE to regulate OR DISTRIBUTION blood concentrations of the insides of blood vessels. It is measured as systolic pressure over diastolic pressure, meaning the pressure produced absorbed amino acids and lipids. It modifies them into usable cells, oxidizes them, or changes them into forms that can be during ventricular contraction over the pressure produced stored. Hepatic portal venous blood usually contains bacteria from intestinal capillaries. Large Kupffer cells in the liver The pulmonary circuit consists of vessels that carry blood when the ventricles relax. phagocytize microorganisms before they can leave the liver. Jones from the & Bartlett right ventricle Learning, to the lungs LLC and back to the left This blood then travels through merged vessels into hepatic NOT atrium. FOR The SALE systemic OR DISTRIBUTION circuit consists of vessels that lead veins, emptying into the inferior vena cava. from the left ventricle to the body cells and back to the heart, Jones and Bartlett Publishers.
15 Summary 49 External jugular vein Vertebral vein Internal jugular vein Superior vena cava Axillary vein Subclavian vein Brachiocephalic veins Hepatic portal vein Superior mesenteric vein Inferior vena cava Common iliac vein Internal iliac vein Cephalic vein Brachial vein Basilic vein Splenic vein Renal vein Inferior mesenteric vein Radial vein Ulnar vein External iliac vein Digital veins Femoral vein Great saphenous vein Popliteal vein Posterior tibial vein Anterior tibial vein Small saphenous vein Dorsal venous arch Dorsal digital veins Figure 5 11 Overview of the veins in the body. For clarity, the right kidney is not shown. Jones and Bartlett Publishers.
16 50 CHAPTER 5 Anatomy and Physiology of the Cardiovascular System Superior sagittal sinus Jones & Bartlett Inferior Learning, vena cava LLC Common iliac vein Straight sinus Occipital vein Transverse sinus Posterior auricular vein Facial vein Jones & Bartlett Learning, Ophthalmic LLCvein Superficial temporal vein Internal iliac vein External iliac vein Femoral circumflex vein Deep femoral vein External jugular vein Vertebral vein Internal jugular vein Superior and middle thyroid veins Femoral vein Great saphenous vein Subclavian vein Superior vena cava Right brachiocephalic vein Left brachiocephalic vein Popliteal vein (a) Brachiocephalic vein Subclavian vein Small saphenous vein Posterior tibial vein Anterior tibial vein Axillary vein Brachial vein Cephalic vein Basilic vein Jones & Bartlett Median cubital Learning, vein LLC Intercostal veins Superior vena cava Hemiazygos vein NOT Dorsal FOR venous SALE arch OR DISTRIBUTION Metatarsal veins (c) Median antebrachial vein Jones Basilic & vein Bartlett Learning, LLC Ulnar vein Deep palmar venous arch Superficial palmar venous arch Digital veins (b) Figure 5 12 Detailed views of the arteries Jones and Bartlett Publishers.
17 Summary 51 including the aorta and its branches. The aorta is the largest 6. The function of an atrium is to in the body, with respect to diameter. A. pump blood to the lungs NOT FOR B. SALE pump blood OR into DISTRIBUTION the systemic circuit CRITICAL THINKING C. pump blood to the heart muscle D. collect blood Two phlebotomists were studying together to take the 7. The left and right pulmonary arteries carry blood to National Certification Exam. One of them was questioning the other about the anatomy Jones and & physiology Bartlett of Learning, the heart LLC A. brain the and circulatory system. The questions that follow were what B. liver he asked. C. lungs 1. How many veins return blood to the right atrium? D. kidneys Name these veins. 8. The pacemaker cells of the heart are located in the 2. Where in the heart are the Purkinje fibers located? A. SA node 3. Where is the lowest blood pressure found in the blood B. AV node Jones & Bartlett Learning, LLC vessels? C. left NOT ventricle FOR SALE OR DISTRIBUTION D. left atrium WEBSITES 9. Which of the following blood vessels returns blood to the left atrium? A. inferior vena cava Jones & Bartlett jhtml?identifier=4473 Learning, LLC Jones B. & Bartlett superior vena Learning, cava LLC C. pulmonary vein NOT FOR SALE OR DISTRIBUTION D. pulmonary trunk _Structure.php 10. Each of the following factors will increase cardiac outhttp:// put, EXCEPT _circulation.html A. increased parasympathetic stimulation B. increased sympathetic stimulation C. increased venous return D. increased heart rate The difference between the systolic and diastolic pres-.htm sures is referred to as A. a pulse REVIEW QUESTIONS B. circulatory pressure C. blood Jones pressure& Bartlett Learning, LLC Multiple NOT Choice FOR SALE OR DISTRIBUTION D. mean NOT arterial FOR pressure SALE OR DISTRIBUTION 12. Blood from the brain returns to the heart via a vein 1. Blood leaving the left ventricle enters the called the A. pulmonary trunk A. external jugular B. pulmonary B. internal jugular C. inferior vena cava Jones C. & Bartlett vertebral vein Learning, LLC D. aorta NOT FOR SALE D. azygos vein 2. The OR right DISTRIBUTION ventricle pumps blood to the 13. Branches off of the aortic arch include the A. systemic circuit A. brachio and right axillary arteries B. lungs B. right and left subclavian arteries C. left atrium C. right and left common carotid arteries D. right atrium D. left subclavian and left common carotid arteries 3. The visceral pericardium Jones is the & Bartlett same as thelearning, LLC 14. Nutrients from the digestive tract enter the A. epicardiuma. hepatic vein B. endocardium B. hepatic portal vein C. myocardium C. inferior vena cava D. parietal pericardium D. azygos vein 4. The mitral valve is located between the 15. The longest vein in the human body is the Jones A. right atrium & Bartlett and right Learning, ventricle LLC A. inferior vena cava NOT B. left FOR atrium SALE and left OR ventricle DISTRIBUTION B. superior NOT vena FOR cava SALE OR DISTRIBUTION C. left ventricle and aorta C. saphenous vein D. right ventricle and pulmonary trunk D. femoral vein 5. The heart wall is composed of how many layers? A. two Jones & Bartlett B. three Learning, LLC C. four D. five Jones and Bartlett Publishers.
18 Jones and Bartlett Publishers.
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Blood Vessels and Circulation
 13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
Functions of Blood System. Blood Cells
 Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Chapter 20: The Cardiovascular System: The Heart
 Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back
 Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Chapter 19 Ci C r i cula l t a i t o i n
 Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Cardiovascular Physiology
 Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014
 Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014 Philip J. Bergmann Lab Objectives 1. To learn how blood flows through a dual circuit circulation with lungs. 2. To
Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014 Philip J. Bergmann Lab Objectives 1. To learn how blood flows through a dual circuit circulation with lungs. 2. To
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School
 Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Circulatory System and Blood
 Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
THE HEART Dr. Ali Ebneshahidi
 THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
Cardiology. Anatomy and Physiology of the Heart.
 Cardiology Self Learning Package Module 1: Anatomy and Physiology of the Heart. Module 1: Anatomy and Physiology of the Heart Page 1 CONTENT Introduction Page 3 How to use the ECG Self Learning package.page
Cardiology Self Learning Package Module 1: Anatomy and Physiology of the Heart. Module 1: Anatomy and Physiology of the Heart Page 1 CONTENT Introduction Page 3 How to use the ECG Self Learning package.page
Circulatory System Review
 Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Page 1. Introduction The blood vessels of the body form a closed delivery system that begins and ends at the heart.
 Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
Blood vessels. transport blood throughout the body
 Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes.
 Circulatory system. Basic function: To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes. Not all organisms have a circulatory system -
Circulatory system. Basic function: To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes. Not all organisms have a circulatory system -
The Circulatory System. Chapter 17 Lesson 1
 The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
12.1: The Function of Circulation page 478
 12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
THE HEART AND CIRCULATION HENRY S. CABIN, M.D.
 CHAPTER 1 THE HEART AND CIRCULATION HENRY S. CABIN, M.D. INTRODUCTION The cardiovascular system is an elaborate network that performs two major tasks: It delivers oxygen and nutrients to body organs and
CHAPTER 1 THE HEART AND CIRCULATION HENRY S. CABIN, M.D. INTRODUCTION The cardiovascular system is an elaborate network that performs two major tasks: It delivers oxygen and nutrients to body organs and
Note: The left and right sides of the heart must pump exactly the same volume of blood when averaged over a period of time
 page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
Human Anatomy & Physiology II with Dr. Hubley
 Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
Human Anatomy and Physiology II Laboratory
 Human Anatomy and Physiology II Laboratory The Circulation (Two Weeks) 1 This lab involves two weeks work studying the vasculature of the human body. Both weeks involve the exercise in the lab manual entitled
Human Anatomy and Physiology II Laboratory The Circulation (Two Weeks) 1 This lab involves two weeks work studying the vasculature of the human body. Both weeks involve the exercise in the lab manual entitled
THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM
 CHAPTER 6: THE CIRCULATORY SYSTEM THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM Most of the cells in the human body are not in direct contact with the external environment, so rely on the circulatory
CHAPTER 6: THE CIRCULATORY SYSTEM THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM Most of the cells in the human body are not in direct contact with the external environment, so rely on the circulatory
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Chapter 16: Circulation
 Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
CHAPTER 15: THE CARDIOVASCULAR SYSTEM. 2. Describe the location, size, and orientation of the human heart.
 CHAPTER 15: THE CARDIOVASCULAR SYSTEM OBJECTIVES: 1. List the organs that compose the cardiovascular system and discuss the general functions of this system. 2. Describe the location, size, and orientation
CHAPTER 15: THE CARDIOVASCULAR SYSTEM OBJECTIVES: 1. List the organs that compose the cardiovascular system and discuss the general functions of this system. 2. Describe the location, size, and orientation
CHAPTER 9 BODY ORGANIZATION
 CHAPTER 9 BODY ORGANIZATION Objectives Identify the meaning of 10 or more terms relating to the organization of the body Describe the properties of life Describe the function for the structures of the
CHAPTER 9 BODY ORGANIZATION Objectives Identify the meaning of 10 or more terms relating to the organization of the body Describe the properties of life Describe the function for the structures of the
3. Tunica adventitia is the outermost layer; it is composed of loosely woven connective tissue infiltrated by nerves, blood vessels and lymphatics
 Blood vessels and blood pressure I. Introduction - distribution of CO at rest II. General structure of blood vessel walls - walls are composed of three distinct layers: 1. Tunica intima is the innermost
Blood vessels and blood pressure I. Introduction - distribution of CO at rest II. General structure of blood vessel walls - walls are composed of three distinct layers: 1. Tunica intima is the innermost
2161-1 - Page 1. Name: 1) Choose the disease that is most closely related to the given phrase. Questions 10 and 11 refer to the following:
 Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Human Body Vocabulary Words Week 1
 Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
Vocabulary Words Week 1 1. arteries Any of the blood vessels that carry blood away from the heart to all parts of the body 2. heart The muscular organ inside the chest that pumps blood through the body
Cardiovascular System
 Topics to Review Diffusion Skeletal muscle fiber (cell) anatomy Membrane potential and action potentials Action potential propagation Excitation-contraction coupling in skeletal muscle skeletal muscle
Topics to Review Diffusion Skeletal muscle fiber (cell) anatomy Membrane potential and action potentials Action potential propagation Excitation-contraction coupling in skeletal muscle skeletal muscle
LECTURE 3: CARDIOVASCULAR SYSTEM - BLOOD VESSELS
 LECTURE 3: CARDIOVASCULAR SYSTEM - BLOOD VESSELS INTRODUCTION To fully grasp the circulatory system and the processes that may progress to heart disease, it is vital that one comprehend the functioning
LECTURE 3: CARDIOVASCULAR SYSTEM - BLOOD VESSELS INTRODUCTION To fully grasp the circulatory system and the processes that may progress to heart disease, it is vital that one comprehend the functioning
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY Human beings are arguably the most complex organisms on this planet. Imagine billions of microscopic parts, each with its own identity,
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY Human beings are arguably the most complex organisms on this planet. Imagine billions of microscopic parts, each with its own identity,
Chapter 2 - Anatomy & Physiology of the Respiratory System
 Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
By Casey Schmidt and Wendy Ford
 By Casey Schmidt and Wendy Ford Body systems Digestive System Circulatory System Respiratory System Excretory System Immune System Reproductive System Nervous System Muscular System Skeletal System Endocrine
By Casey Schmidt and Wendy Ford Body systems Digestive System Circulatory System Respiratory System Excretory System Immune System Reproductive System Nervous System Muscular System Skeletal System Endocrine
Chapter 15. Sympathetic Nervous System
 Chapter 15 Sympathetic Nervous System Somatic versus Autonomic Pathways Somatic efferent innervation ACh Myelinated fiber Somatic effectors (skeletal muscles) Autonomic efferent innervation ACh ACh or
Chapter 15 Sympathetic Nervous System Somatic versus Autonomic Pathways Somatic efferent innervation ACh Myelinated fiber Somatic effectors (skeletal muscles) Autonomic efferent innervation ACh ACh or
Human Anatomy and Physiology The Respiratory System
 Human Anatomy and Physiology The Respiratory System Basic functions of the respiratory system: as a Gas exchange supply oxygen to aerobic tissues in the body and remove carbon dioxide waste product. in-
Human Anatomy and Physiology The Respiratory System Basic functions of the respiratory system: as a Gas exchange supply oxygen to aerobic tissues in the body and remove carbon dioxide waste product. in-
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Medical Terminology, Anatompy & Physiology
 1. Which of the following BEST describes the anatomical position? a. Supine with arms crossed over the chest and knees slightly bent b. Standing, facing forward, with arms raised above the head c. Standing,
1. Which of the following BEST describes the anatomical position? a. Supine with arms crossed over the chest and knees slightly bent b. Standing, facing forward, with arms raised above the head c. Standing,
The Body s Transport System
 Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
Lecture Outline. Cardiovascular Physiology. Cardiovascular System Function. Functional Anatomy of the Heart
 Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
BIOL 1108 Vertebrate Anatomy Lab
 BIOL 1108 Vertebrate Anatomy Lab This lab explores major organs associated with the circulatory, excretory, and nervous systems of mammals. Circulatory System Vertebrates are among the organisms that have
BIOL 1108 Vertebrate Anatomy Lab This lab explores major organs associated with the circulatory, excretory, and nervous systems of mammals. Circulatory System Vertebrates are among the organisms that have
Human Anatomy & Physiology General
 Human Anatomy & Physiology General Biology is the study of life but, what exactly is life? how are living things different from nonliving things eg. a human from a rock eg. a a human from a robot eg. a
Human Anatomy & Physiology General Biology is the study of life but, what exactly is life? how are living things different from nonliving things eg. a human from a rock eg. a a human from a robot eg. a
The digestive system eliminated waste from the digestive tract. But we also need a way to eliminate waste from the rest of the body.
 Outline Urinary System Urinary System and Excretion Bio105 Lecture 20 Chapter 16 I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system 1
Outline Urinary System Urinary System and Excretion Bio105 Lecture 20 Chapter 16 I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system 1
Our Human Body On-site student activities Years 5 6
 Our Human Body On-site student activities Years 5 6 Our Human Body On-site student activities: Years 5-6 Student activity (and record) sheets have been developed with alternative themes for students to
Our Human Body On-site student activities Years 5 6 Our Human Body On-site student activities: Years 5-6 Student activity (and record) sheets have been developed with alternative themes for students to
Overview of the Cardiovascular System
 Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
BIO 137: CHAPTER 1 OBJECTIVES
 BIO 137: CHAPTER 1 OBJECTIVES 1. Define the terms anatomy and physiology, and explain their relationship using an example of a human structure with its corresponding function. A. ANATOMY = the study of
BIO 137: CHAPTER 1 OBJECTIVES 1. Define the terms anatomy and physiology, and explain their relationship using an example of a human structure with its corresponding function. A. ANATOMY = the study of
33.1 The Circulatory System
 33.1 The Circulatory System Lesson Objectives Identify the functions of the human circulatory system. Describe the structure of the heart and explain how it pumps blood through the body. Name three types
33.1 The Circulatory System Lesson Objectives Identify the functions of the human circulatory system. Describe the structure of the heart and explain how it pumps blood through the body. Name three types
ACLS Chapter 3 Rhythm Review Instructor Lesson Plan to Accompany ACLS Study Guide 3e
 ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
Biology 224 Human Anatomy and Physiology II Week 8; Lecture 1; Monday Dr. Stuart S. Sumida. Excretory Physiology
 Biology 224 Human Anatomy and Physiology II Week 8; Lecture 1; Monday Dr. Stuart S. Sumida Excretory Physiology The following ELEVEN slides are review. They will not be covered in lecture, but will be
Biology 224 Human Anatomy and Physiology II Week 8; Lecture 1; Monday Dr. Stuart S. Sumida Excretory Physiology The following ELEVEN slides are review. They will not be covered in lecture, but will be
1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood?
 1 1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood? 2 The plan shows the blood system of a mammal. What does the part labelled X represent? A heart
1 1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood? 2 The plan shows the blood system of a mammal. What does the part labelled X represent? A heart
CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT
 CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT BLOOD CIRCULATION AND TRANSPORT HUMAN BEING PLANTS Function of heart Wilting Structure of heart Blood vessels: characteristics and functions Transpiration: function
CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT BLOOD CIRCULATION AND TRANSPORT HUMAN BEING PLANTS Function of heart Wilting Structure of heart Blood vessels: characteristics and functions Transpiration: function
2.2.1 Pressure and flow rate along a pipe: a few fundamental concepts
 1.1 INTRODUCTION Single-cell organisms live in direct contact with the environment from where they derive nutrients and into where they dispose of their waste. For living systems containing multiple cells,
1.1 INTRODUCTION Single-cell organisms live in direct contact with the environment from where they derive nutrients and into where they dispose of their waste. For living systems containing multiple cells,
A. function: supplies body with oxygen and removes carbon dioxide. a. O2 diffuses from air into pulmonary capillary blood
 A. function: supplies body with oxygen and removes carbon dioxide 1. ventilation = movement of air into and out of lungs 2. diffusion: B. organization a. O2 diffuses from air into pulmonary capillary blood
A. function: supplies body with oxygen and removes carbon dioxide 1. ventilation = movement of air into and out of lungs 2. diffusion: B. organization a. O2 diffuses from air into pulmonary capillary blood
Level 2 Certificate in Fitness Instructing Unit 1: Anatomy and Physiology
 Level 2 Certificate in Fitness Instructing Unit 1: Anatomy and Physiology These questions have been compiled based on the information available for the above qualification and unit. This mock should be
Level 2 Certificate in Fitness Instructing Unit 1: Anatomy and Physiology These questions have been compiled based on the information available for the above qualification and unit. This mock should be
Chapter 20: Tissues & Organ Systems
 Chapter 20: Tissues & Organ Systems The Importance of Homeostasis The maintenance of a relatively constant internal environment, i.e., homeostasis, is essential for life. Cellular conditions that need
Chapter 20: Tissues & Organ Systems The Importance of Homeostasis The maintenance of a relatively constant internal environment, i.e., homeostasis, is essential for life. Cellular conditions that need
Cardiovascular System:! Pulmonary circuit:!! right ventricle!!! lungs!!!! left atrium! Systemic circuit:!! left ventricle!
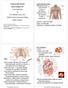 Cardiovascular System:! Heart (Chapter 20)! Lecture Materials! for! Amy Warenda Czura, Ph.D.! Suffolk County Community College! Primary Sources for figures and content:! Eastern Campus! Marieb, E. N. Human
Cardiovascular System:! Heart (Chapter 20)! Lecture Materials! for! Amy Warenda Czura, Ph.D.! Suffolk County Community College! Primary Sources for figures and content:! Eastern Campus! Marieb, E. N. Human
Name Class Date Laboratory Investigation 24A Chapter 24A: Human Skin
 Name Class Date Laboratory Investigation 24A Chapter 24A: Human Skin Human Anatomy & Physiology: Integumentary System You may refer to pages 386-394 in your textbook for a general discussion of the integumentary
Name Class Date Laboratory Investigation 24A Chapter 24A: Human Skin Human Anatomy & Physiology: Integumentary System You may refer to pages 386-394 in your textbook for a general discussion of the integumentary
Administrative. Patient name Date compare with previous Position markers R-L, upright, supine Technical quality
 CHEST X-RAY Administrative Patient name Date compare with previous Position markers R-L, upright, supine Technical quality AP or PA ( with x-ray beam entering from back of patient, taken at 6 feet) Good
CHEST X-RAY Administrative Patient name Date compare with previous Position markers R-L, upright, supine Technical quality AP or PA ( with x-ray beam entering from back of patient, taken at 6 feet) Good
ORGAN SYSTEMS OF THE BODY
 ORGAN SYSTEMS OF THE BODY DEFINITIONS AND CONCEPTS A. Organ a structure made up of two or more kinds of tissues organized in such a way that they can together perform a more complex function that can any
ORGAN SYSTEMS OF THE BODY DEFINITIONS AND CONCEPTS A. Organ a structure made up of two or more kinds of tissues organized in such a way that they can together perform a more complex function that can any
UNIT 1 BODY PLAN AND ORGANIZATION LECTURE
 UNIT 1 BODY PLAN AND ORGANIZATION LECTURE 1.03 CONTRAST THE SCIENCES OF ANATOMY AND PHYSIOLOGY A. Anatomy Anatomy is the scientific study of structures and the relationship of.. structures to each other.
UNIT 1 BODY PLAN AND ORGANIZATION LECTURE 1.03 CONTRAST THE SCIENCES OF ANATOMY AND PHYSIOLOGY A. Anatomy Anatomy is the scientific study of structures and the relationship of.. structures to each other.
Introduction to Animal Systems
 Human Body Systems Introduction to Animal Systems Recurring Themes in Biology 1. Correlation between structure and function( seen at many levels) 2. Life is organized at many levels from Smallest ----
Human Body Systems Introduction to Animal Systems Recurring Themes in Biology 1. Correlation between structure and function( seen at many levels) 2. Life is organized at many levels from Smallest ----
Divisions of the Skeletal System
 OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
Learning Objectives for Anatomy & Physiology
 Learning Objectives for Anatomy & Physiology Anatomy & Physiology by Visible Body contains 12 units. Below is a listing of each unit, the chapters within it, and the unit s associated learning objectives.
Learning Objectives for Anatomy & Physiology Anatomy & Physiology by Visible Body contains 12 units. Below is a listing of each unit, the chapters within it, and the unit s associated learning objectives.
Factors Affecting Blood Pressure. Vessel Elasticity Blood Volume Cardiac Output
 Factors that Affect Pressure Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction pressure is affected by several factors:
Factors that Affect Pressure Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction pressure is affected by several factors:
Investigating the Human Body On-site student activities: Years 7-8 Investigating the Human Body On-site student activities Years 7 8
 Investigating the Human Body On-site student activities Years 7 8 Student activity (and record) sheets have been developed with alternative themes for students to use as guides and focus material during
Investigating the Human Body On-site student activities Years 7 8 Student activity (and record) sheets have been developed with alternative themes for students to use as guides and focus material during
Chapter 15. Autonomic Nervous System (ANS) and Visceral Reflexes. general properties Anatomy. Autonomic effects on target organs
 Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
ANATOMY AND PHYSIOLOGY OF THE PULMONARY SYSTEM Section 1 Part B Reading Assignment: Des Jardins - Chapter 1, pp. THE LOWER AIRWAY I.
 ANATOMY AND PHYSIOLOGY OF THE PULMONARY SYSTEM Section 1 Part B Reading Assignment: Des Jardins - Chapter 1, pp. THE LOWER AIRWAY I. Cartilaginous Airways A. Trachea 1. extends from the cricoid cartilage
ANATOMY AND PHYSIOLOGY OF THE PULMONARY SYSTEM Section 1 Part B Reading Assignment: Des Jardins - Chapter 1, pp. THE LOWER AIRWAY I. Cartilaginous Airways A. Trachea 1. extends from the cricoid cartilage
Chetek-Weyerhaeuser High School
 Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Milwaukee School of Engineering [email protected]. Case Study: Factors that Affect Blood Pressure Instructor Version
 Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
REVIEW for BIOLOGY UNIT TEST
 REVIEW for BIOLOGY UNIT TEST NOTE: The Unit Test will cover everything we have learned in the Biology Unit, starting from cell structures, cell division, various organ systems, disorders, organ donation,
REVIEW for BIOLOGY UNIT TEST NOTE: The Unit Test will cover everything we have learned in the Biology Unit, starting from cell structures, cell division, various organ systems, disorders, organ donation,
THE HUMAN BODY SYSTEMS
 Name Period Date THE HUMAN BODY SYSTEMS System Function Diagram Major Organs Digestive 1. take in food (ingestion) 2. digest food into smaller molecules and absorb nutrients 3. remove undigestable food
Name Period Date THE HUMAN BODY SYSTEMS System Function Diagram Major Organs Digestive 1. take in food (ingestion) 2. digest food into smaller molecules and absorb nutrients 3. remove undigestable food
UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM
 BIOLOGY - 2201 UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM What happens to your body as you run? Breathing, heart rate, temperature, muscle pain, thirsty... Homeotasis Homeostasis is the process of maintaining
BIOLOGY - 2201 UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM What happens to your body as you run? Breathing, heart rate, temperature, muscle pain, thirsty... Homeotasis Homeostasis is the process of maintaining
Blood Pressure Regulation
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Phlebotomy Handbook Blood Collection Essentials Seventh Edition
 Phlebotomy Handbook Blood Collection Essentials Seventh Edition Diana Garza Kathleen Becan-McBride Chapter Four The Cardiovascular System Introduction Circulatory system is a transport system. Contributes
Phlebotomy Handbook Blood Collection Essentials Seventh Edition Diana Garza Kathleen Becan-McBride Chapter Four The Cardiovascular System Introduction Circulatory system is a transport system. Contributes
Every cell in the animal body must acquire the energy
 52 Circulation Concept Outline 52.1 The circulatory systems of animals may be open or closed. Open and Closed Circulatory Systems. All vertebrates have a closed circulation, while many invertebrate animals
52 Circulation Concept Outline 52.1 The circulatory systems of animals may be open or closed. Open and Closed Circulatory Systems. All vertebrates have a closed circulation, while many invertebrate animals
Heart Rate and Physical Fitness
 Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Provided by the American Venous Forum: veinforum.org
 CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
MOCK Level 3 Anatomy and Physiology for Exercise and Health
 MULTIPLE CHOICE QUESTION PAPER Paper number APEH 3.0 Please insert this reference number in the appropriate boxes on your candidate answer sheet Title Time allocation 50 minutes MOCK Level 3 Anatomy and
MULTIPLE CHOICE QUESTION PAPER Paper number APEH 3.0 Please insert this reference number in the appropriate boxes on your candidate answer sheet Title Time allocation 50 minutes MOCK Level 3 Anatomy and
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Sign up to receive ATOTW weekly email [email protected]
 INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
Questions on The Nervous System and Gas Exchange
 Name: Questions on The Nervous System and Gas Exchange Directions: The following questions are taken from previous IB Final Papers on Topics 6.4 (Gas Exchange) and 6.5 (Nerves, hormones and homeostasis).
Name: Questions on The Nervous System and Gas Exchange Directions: The following questions are taken from previous IB Final Papers on Topics 6.4 (Gas Exchange) and 6.5 (Nerves, hormones and homeostasis).
Normal & Abnormal Intracardiac. Lancashire & South Cumbria Cardiac Network
 Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
MEASURING AND RECORDING BLOOD PRESSURE
 MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
Nerve Tissue. Muscle Tissue. Connective Tissue
 Human Body Tissues Levels of Organization 1. Cells 2. = groups of similar cells that perform a 3. Organ = 4. = group of organs Four Major Tissues 1. 2. 3. 4. Epithelial Tissue Nerve Tissue Muscle Tissue
Human Body Tissues Levels of Organization 1. Cells 2. = groups of similar cells that perform a 3. Organ = 4. = group of organs Four Major Tissues 1. 2. 3. 4. Epithelial Tissue Nerve Tissue Muscle Tissue
Eating, pooping, and peeing THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM Ingested food is not technically in the body until it is absorbed so it needs to be: Mechanically and chemically reduced Transported by the blood to the cells Large portions are not
THE DIGESTIVE SYSTEM Ingested food is not technically in the body until it is absorbed so it needs to be: Mechanically and chemically reduced Transported by the blood to the cells Large portions are not
North Bergen School District Benchmarks
 Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
Reavis High School Anatomy and Physiology Curriculum Snapshot
 Reavis High School Anatomy and Physiology Curriculum Snapshot Unit 1: Introduction to the Human Body 10 days As part of this unit, students will define anatomy, physiology, and pathology. They will identify
Reavis High School Anatomy and Physiology Curriculum Snapshot Unit 1: Introduction to the Human Body 10 days As part of this unit, students will define anatomy, physiology, and pathology. They will identify
Urinary System Lab Guide
 Urinary System Lab Guide I. Prelab Questions Name 1. Describe the location of the kidneys. 2. Describe the following structures: a. renal cortex b. renal pyramid c. renal column d. minor calyx e. renal
Urinary System Lab Guide I. Prelab Questions Name 1. Describe the location of the kidneys. 2. Describe the following structures: a. renal cortex b. renal pyramid c. renal column d. minor calyx e. renal
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
