THE HEART Dr. Ali Ebneshahidi
|
|
|
- Joanna Kennedy
- 9 years ago
- Views:
Transcription
1 THE HEART Dr. Ali Ebneshahidi
2 Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned from body tissues) to the lungs for gas exchange, while the left heart pumps oxygenated blood (returned from the lungs) to tissues cells for sustaining cellular respiration. 2. Attached to the heart is blood vessels that transport blood in various circulation pathways - pulmonary blood vessels transport blood between the heart and the lungs, and systemic blood vessels transport blood between the heart and body tissues.
3
4 Heart chambers Hollow cavities within the heart for containing blood. Two smaller chambers called atrium are near the base, and two larger chambers called ventricle are close to the apex. Right atrium (RA) after receiving deoxygenated blood from body tissues through the superior and inferior vena cava, pumps the blood into the right ventricle (RV) via the right atria ventricular orifice. RV then pumps the blood to the lungs for gas exchange, through the pulmonary trunk and arteries. Left atrium (LA) after receiving oxygenated blood from the lungs through the pulmonary veins, pumps the blood into the left ventricle (LV) via the left atria ventricular orifice.
5 LV then pumps the blood to the body tissues for supplying oxygen to every body cell, through the aorta. RA and LA are separated by a central heart wall called interatrial septum, while RV and LV are separated by interventricular septum. LV has a thicker myocardium layer (for stronger contractions) and contains rough ridges called trabeculae carneae (for containing a larger blood volume in exercising conditions). Note: Coronary arteries (from the first branching of aorta) supply oxygenated blood to the cardiac muscle.
6
7 Heart Valves Two heart valves located between atria and ventricles are called atrioventricular valves (AV valves) which include the tricuspid valve between RA and RV, and bicuspid valve (or mitral valve) between LA and LV. Two heart valves located at the exiting arteries are called semilunar valves (SL valves) which include the plumonic semilunar valve at the base of pulmonary trunk, and the aortic semilunar valve at the base of aorta. Each AV valve consists of cusps (extensions of endocradium), chordae tendineae, and papillary muscles (the latter two are designed to prevent eversion of the cusps into the atria). AV valves prevent backflow into atria, while SL valves prevent backflow into ventricles.
8
9 Circulation Pathways: Pulmonary circuit allows deoxygenated blood to be transported into the lungs for gas exchange, so that oxygenated blood can once again flows into the left heart. Deoxygenated blood from body tissues superior & inferior vena cava RA tricuspid valve RV plumonic SL valve pulmonary arteries lungs (gas exchange occurs) oxygenated blood travels in pulmonary veins LA bicuspid valve LV.
10
11 Coronary circuit Coronary circuit allows oxygenated blood to be delivered to cardiac muscle cells in the heart wall, and its deoxygenated blood is drained back to the RA. Oxygenated blood in LV aortic SL valve aorta coronary arteries arterioles capillaries in myocardium (gas exchange occurs) deoxygenated blood travels into venules cardiac veins coronary sinus RA.
12 Coronary Circulation: Arterial Supply
13 Coronary Circulation: Venous Supply
14 Systemic Circuit Systemic circuit allows oxygenated blood from the left heart to be delivered to tissue cells through arteries and arterioles, and deoxygenated blood is transported back to the right heart through veins and venues. Oxygenated blood in LV aortic SL valve aorta arteries arterioles capillaries in tissues (gas exchange occurs) deoxygenated blood travels in venules veins superior & inferior vena cava RA.
15 Cardiac cycles are mainly controlled by nerve impulse, while hormones only can influence the heart rate. Two mechanisms to regulate cardiac cycles - intrinsic control (consists of pacemakers and a conduction system) and extrinsic control (consists of sympathetic and parasympathetic nerves, and hormones, that influence the pacemakers and affect the heart rate).
16 Impulse conducting system of the heart (Intrinsic control) Group of muscle cells specialized for conduction rather than contraction. Innervated by both the sympathetic and parasympathetic nervous system. Regulate cardiac rhythm, and adapts cardiac output to the physiologic needs of the body. Components: 1. Sinoatrial node (pace maker), cluster of excitable cells which sets cardiac rhythm. Located near the inlet of the superior vena cava. 2. Atrial syncytium, a mass of merging cells that act as a unit. Cardiac muscle fibers function like those of skeletal muscles, but the fibers connect in branching networks. Stimulation of any part of the network send impulses throughout the heart, which contracts as a unit.
17 Impulse conduction
18 3. Action potential spreads through atrial musculature. 4. Junctional fibers impulses travel from cell to cell by gap junctions. 5. Atrioventricular node group of excitable fibers located to the right of the upper portion of the interventricular septum, picks up the wave of depolarization of atria and relays it to: 6. Bundle of His nerve like group of excitable tissue which spreads action potential down the IV septum and soon divides into a left or right branch which run down the septum and on the apex split into: 7. Purkinje fibers which carry the action potential concentrically to the ventricular musculature, running subendocardially. 8. Ventricular syncytium.
19
20 Functions of the cardiac conduction system 1. Causes both atria to contract simultaneously and generate enough hydrostatic pressure to open both AV valves so that blood flows to ventricles. 2. Causes the ventricles to contract a few milliseconds later, overcome the resistance of the semilunar valves and generate enough hydrostatic pressure to circulate the blood through the pulmonary and systemic pathways. 3. Adapts the heart to beat under different functional demands. Sympathetic nervous system increases rate and output, parasympathetic decreases.
21 Extrinsic Control In extrinsic control, pressure receptors along the aorta and common carotid arteries detect changes in blood pressure and send nerve impulses to the cardiac centers in medulla oblongata, which in turn activates either sympathetic nerves (to increase heart rate and contractility) or parasympathetic nerves (to decrease heart rate and contractility). These nerves innervate the SA node, changing the basic rhythm in cardiac action. Hormones such as epinephrine and norepinephrine can also have the same stimulatory effect on the SA node. Note: Emotion, stress, body temperature, ions (potassium, calcium), certain drugs, and alcohol can indirectly affect the intrinsic and extrinsic mechanisms.
22 Extrinsic Control
23 Cardiac Excitability & Contractility 1. The duration of the cardiac action potential is very long, lasting throughout contraction. Action potentials in cardiac muscle is 100 times longer than in skeletal muscles. 2. There are prolonged refractory periods. 3. Cardiac muscle contractions are always brief twitches. In skeletal muscles, contractions resulting from rapid repetitive stimulation can summate to provide sustained contraction. This can not happen in cardiac muscle because the long refractory period cancels any stimulus that occurs before the heart has a chance to relax. - Relaxtion between beats is essential for the heart to fill with blood, to be pumped at the next beat. Summation of contractions (tetanus) does not occur due to long refractory periods. Note Ca ++ entry prolongs the period of depolarization.
24 4. Cardiac muscles are interconnected by gap junctions the heart beat is All or None, and spreads. 5. Cardiac muscles excites itself. Normally skeletal muscles will contract only if it receives a nerve impulse. Nerves that carry impulses to the heart influence the rate and strength of contraction, but they do not initiate the primitive heartbeat. 6. Excitation for the heart beat arises from within the cardiac muscle itself; spontaneous depolarization of the SA node cell which spread to other cells. Syncytium refers to cells that contract as a unit. - SA and AV node cells are pacemaker cells; they have intrinsic automaticity characterized by spontaneous depolarization which perhaps may be due to a decreased membrane permeability to K +.
25 Electrocardiogram ( EKG or ECG ) A graphic record of the electrical activity of the heart. P wave: small up ward wave representing atria depolarization Atrial systole occurs by the end of P wave so, the P wave is atrial excitation. P Q interval: Represents the conduction through the atrial musculature, and AV delay (due to passage of action potential through the A V junction).
26 Q wave: Action potential spreads through the muscle of the septum between the ventricles, mostly from left to right and produces the small, variable, and usually negative wave, the Q wave. R wave: Action potential spreads through the big mass of ventricular muscle at the apex producing a large positive deflection, called the R wave.
27 S wave: Action potential continues to spread through the last part of the bases of the ventricles, producing the usually inverted S wave (front to back Action potential). QRS complex: indicates ventricular depolarization and coincides with atrial repolarization. S T segment: indicate the time between ventricular depolarization and beginning of repolarization.
28 Note: S T segment is elevated in acute myocardial infarctions. During S-T interval, all of ventricle stays "excited". Q T interval: Showes events in ventricular activity from beginning of depolarization until end of repolarization. T wave: Indicates the ventricular repolarization (recovery of the ventricles to the resting state).
29 Depolarization & Repolarization of the Heart
30 Cardiodynamics 1. A cardiac cycle (or a heartbeat) consists of 3 phases of events. Relaxation period when all 4 heart chambers are relaxed, all 4 heart valves are closed, and blood is coming into the 2 atria through the veins. Ventricular filling - when 70% of the blood in atria flow passively into ventricles due to gravity, followed by 30% of the blood being pumped by atrial systole (contraction of atria); during this phase, AV valves are open while SL valves are still closed. Ventricular systole - after all the blood in atria gets into ventricles, AV valves close, atria go into relaxation (atrial diastoles), and ventricles contract to pump the blood into exiting arteries (LV into aorta and RV into pulmonary trunk) which opens the SL valves.
31 SL valves will close after almost all ventricular blood is ejected (there is always 60 ml blood remained in each ventricle, a volume called endsystolic volume or ESV). Then the ventricles relax (ventricular diastole), and a new cardiac cycle will follow. 2. Each cardiac cycle takes about 0.8 second to complete. 3.Toward the end of ventricular filling, when pressure builds up in the ventricles AV valves begin to close. Now papillary muscles contract, pulling the chordae and cusps, to prevent eversion (overbulging) of the cusps into the atria. 4. In each cardiac cycle, the two atria contract and relax simultaneously - a phenomenon called atrial syncytum. The same is true for the ventricles, which is known as ventricular syncytum. Note: when cardiac muscles in heart chambers lose this syncytum ability, fibrillation occurs which can be fatally out of control.
32 Cardiac cycle
33 Cardiac output: volume of blood pumped by the heart each minute = stroke volume (volume of each beat) Heart rate C.H.R) [# beats / min]. Stroke volume: determined by the volume of blood in the heart at the beginning of systole (end diastolic volume) minus the amount of blood remaining in the ventricles when the valves close at the end of systole (end systolic volume). SV (ml / beat) = EDV (120 ml) ESV (50 ml) = 70 ml / beat Note: End diastolic volume is the amount of blood that collects in a ventricle during diastole. End systolic volume is the amount of blood remaining in the ventricle after it has contracted.
34 Left ventricular pressure-volume change
35 Degree of stretch of heart muscle: Frank starling law: stretching muscle fibers, increase their length and produces increased contractile force of the heart. The contractile force is the preload (degree of stretch of cardiac muscle cells just before they contract).
36
37 Auscultation The process of studying heart sounds using a stethoscope. Each cardiac cycle generates 4 heart sounds, usually only the first two sounds are audible. S1 (or lubb) sound is the loudest, caused by the closure of AV valves at the beginning of ventricular systole; it matches the R wave in ECG. S2 (or dupp ) sound is second loudest, caused by the closure of SL valves at beginning of ventricular diastole; it matches the T wave in ECG. S3 sound is noises generated by ventricular filling in the first 1/3 atrial blood flow into ventricles. S4 sound is noises generated by atrial systole in the remaining 30% of atrial blood being pumped into ventricles.
38 Heart Sounds
39 Sinus rhythm Normal cardiac action or heart rate for female is about beats/min, for male, about beats/ min., and for fetus, about beats/min. Arrhythmias are any abnormal hear beat. Bradycardia is slow heart rate (<60 beats/min) which is normal during sleep, but can be induced by low body temperature, parasympathetic stimulation, and certain drugs. It is indicated by a Short PQ interval and a flat T wave on the ECG. Tachycardia is fast heart rate (> 100 beats/min) which is normal during exercising or excitement, but can be induced by high body temperature, sympathetic stimulation, drugs, heart diseases, anemia, or shock. It is indicated by a lack of P,Q, S, or T wave, with only highfrequency of upward and downward deflections on the ECG.
40 Flutter is very high heart rate (>250 beats/min) which is usually pathological (e.g. bacterial infection or inflammation of myocardium). It is indicated by many small, unrecognized waves, then a big upward/downward wave on the ECG. Fibrillation is high but uncoordinated heart rate caused by regions of myocardium contracting and relaxing independently (lack of syncytum). Atrial fibrillation is not very serious if ventricles are functioning normally. Ventricular fibrillation is usually fatal (the most common cause of sudden death) where blood cannot be pumped properly into the lunges and body tissues. It is indicated by extremely irregular waves on the ECG, and usually Q and S waves are absent.
41
42 Blood pressure (120/80 mmhg) Systolic pressure is the highest pressure attained in the aorta and peripheral arteries when blood is ejected by the ventricles into the aorta. Diastolic pressure is the lowest pressure attained during relaxation or diastolic phase of the heart. Mean arterial blood pressure is the highest in the aorta and large arteries (100 Hg). It sharply decreases in small arteries and even more in arterioles (30 mmhg). After passage through the capillaries and in the small veins the pressure is about 15 mmhg. It falls to about 5mmHg upon entering the right atrium.
43 Pressure gradient in the blood vessels
44 Blood pressure is sensed by baroreceptors in the carotid sinuses and arch of the aorta. They send impulses to the cardiovascular centers in the brain stem which then send signals back to the peripheral vasculature and heart. The effector mechanism that maintains constancy of BP is dual [BP is increased by either increased CO or increased PR (peripheral resistance)]. Change in the diameter of arterioles, controlled y the vasomotor center of the medulla oblongata, regulate peripheral resistance. Resistance to flow is increased by decreasing blood vessel radius.
45 Cardiac Output Increased blood volume entering heart Increased stretch of myocardial fibers Greater force of myocardial contraction Greater stroke volume Increased cardiac output
46 Mechanism regulating B.P. by inhibiting S-A node Cardiac output increases Blood pressure rises Baroreceptors in aortic arch and carotid sinuses are stimulated Sensory impulse to cardiac center Parasympathetic impulse to the heart S-A node inhibited Heart rate decreases Blood Pressure return to normal.
47 Mechanism regulating B.P. by dilating arterioles Rising blood pressure Stimulation of baro- receptors in aortic arch and carotid sinuses Sensory impulses to vasomotor center Vasomotor center inhibited Less frequent sympathetic impulse to arteriole wall Vasodilation of arterioles Decrease peripheral resistance Blood pressure returns towards normal.
48 Renal Control of B.P. Reduced blood flow to kidneys Kidneys releases renin Renin leads to the production of angiotensin II Angiotensin II causes vasoconstriction Blood pressure elevated Increase blood flow to the kidneys.
49 Risk factors for stroke 1. Alcohol consumption 2. Diabetes 3. Elevated serum cholesterol 4. Family history of cardiovascular disease 5. Hypertension 6. Smoking 7. Transient ischemic attacks
50 Drugs to treat hypertension Angiotensin converting enzyme inhibitors: Block formation of Angiotensin II, preventing vasoconstriction. Beta blockers: lower heart rate. Ca ++ channel blockers: Dilate blood vessels by keeping Ca ++ ions out of muscle cells in vessel walls. Diuretics: increase urine output, lowering blood volume.
51 Atheroscleroses Atherosclerosis of arteries can occlude blood flow to the heart and brain and is a causative factor in up to 50% of all deaths in U.S.A., Europe, and Japan. A. Atherosclerosis begins with injury to the endothelium, the movement of monocytes and lymphocytes into the tunica interna and the conversion of monocytes into macrophages that engulf lipids. Smooth muscle cells then proliferate and secrete extra cellular matrix. B. Atherosclerosis is promoted by such risk factors as smoking, hypertension, and high plasma cholesterol concentration. LDLs which carry cholesterol into the artery wall, are oxidized by the endothelium and are a major contributor to atherosclerosis.
52 Occlusion of blood flow in the coronary arteries by atherosclerosis may produce ischemia of the heart muscle and angina pectoris, which may lead to myocardial infarction. The EKG can be used to detect abnormal cardiac rates, abnormal conduction between the atria and ventricles, and other abnormal patterns of electrical conduction in the heart.
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 20: The Cardiovascular System: The Heart
 Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Cardiovascular Physiology
 Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School
 Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back
 Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Functions of Blood System. Blood Cells
 Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
Human Anatomy & Physiology II with Dr. Hubley
 Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
Note: The left and right sides of the heart must pump exactly the same volume of blood when averaged over a period of time
 page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
Cardiovascular System
 Topics to Review Diffusion Skeletal muscle fiber (cell) anatomy Membrane potential and action potentials Action potential propagation Excitation-contraction coupling in skeletal muscle skeletal muscle
Topics to Review Diffusion Skeletal muscle fiber (cell) anatomy Membrane potential and action potentials Action potential propagation Excitation-contraction coupling in skeletal muscle skeletal muscle
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Lecture Outline. Cardiovascular Physiology. Cardiovascular System Function. Functional Anatomy of the Heart
 Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Blood Vessels and Circulation
 13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Circulatory System Review
 Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Milwaukee School of Engineering [email protected]. Case Study: Factors that Affect Blood Pressure Instructor Version
 Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Sign up to receive ATOTW weekly email [email protected]
 INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Chapter 19 Ci C r i cula l t a i t o i n
 Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Circulatory System and Blood
 Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
the Cardiovascular System
 5 Chapter Anatomy Jones and & Physiology Bartlett Learning, LLC of the Cardiovascular System OUTLINE Introduction The Heart Structures of the Heart Conduction System Functions of the Heart The Blood Vessels
5 Chapter Anatomy Jones and & Physiology Bartlett Learning, LLC of the Cardiovascular System OUTLINE Introduction The Heart Structures of the Heart Conduction System Functions of the Heart The Blood Vessels
Cardiovascular System:! Pulmonary circuit:!! right ventricle!!! lungs!!!! left atrium! Systemic circuit:!! left ventricle!
 Cardiovascular System:! Heart (Chapter 20)! Lecture Materials! for! Amy Warenda Czura, Ph.D.! Suffolk County Community College! Primary Sources for figures and content:! Eastern Campus! Marieb, E. N. Human
Cardiovascular System:! Heart (Chapter 20)! Lecture Materials! for! Amy Warenda Czura, Ph.D.! Suffolk County Community College! Primary Sources for figures and content:! Eastern Campus! Marieb, E. N. Human
PSIO 603/BME 511 1 Dr. Janis Burt February 19, 2007 MRB 422; 626-6833 [email protected]. MUSCLE EXCITABILITY - Ventricle
 SIO 63/BME 511 1 Dr. Janis Burt February 19, 27 MRB 422; 626-6833 MUSCLE EXCITABILITY - Ventricle READING: Boron & Boulpaep pages: 483-57 OBJECTIVES: 1. Draw a picture of the heart in vertical (frontal
SIO 63/BME 511 1 Dr. Janis Burt February 19, 27 MRB 422; 626-6833 MUSCLE EXCITABILITY - Ventricle READING: Boron & Boulpaep pages: 483-57 OBJECTIVES: 1. Draw a picture of the heart in vertical (frontal
Blood Pressure Regulation
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Cardiology. Anatomy and Physiology of the Heart.
 Cardiology Self Learning Package Module 1: Anatomy and Physiology of the Heart. Module 1: Anatomy and Physiology of the Heart Page 1 CONTENT Introduction Page 3 How to use the ECG Self Learning package.page
Cardiology Self Learning Package Module 1: Anatomy and Physiology of the Heart. Module 1: Anatomy and Physiology of the Heart Page 1 CONTENT Introduction Page 3 How to use the ECG Self Learning package.page
12.1: The Function of Circulation page 478
 12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes.
 Circulatory system. Basic function: To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes. Not all organisms have a circulatory system -
Circulatory system. Basic function: To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes. Not all organisms have a circulatory system -
Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014
 Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014 Philip J. Bergmann Lab Objectives 1. To learn how blood flows through a dual circuit circulation with lungs. 2. To
Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014 Philip J. Bergmann Lab Objectives 1. To learn how blood flows through a dual circuit circulation with lungs. 2. To
The Circulatory System. Chapter 17 Lesson 1
 The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Activity 4.2.3: EKG. Introduction. Equipment. Procedure
 Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Evaluation copy. Analyzing the Heart with EKG. Computer
 Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Overview of the Cardiovascular System
 Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
Key Medical Terms Associated with the Cardiovascular System
 1 Key Medical Terms Associated with the Cardiovascular System Aneurysm: A thin, weakened section of the wall of an artery or vein that bulges outward, forming a balloon-like sac. Common causes are atherosclerosis,
1 Key Medical Terms Associated with the Cardiovascular System Aneurysm: A thin, weakened section of the wall of an artery or vein that bulges outward, forming a balloon-like sac. Common causes are atherosclerosis,
CHAPTER 15: THE CARDIOVASCULAR SYSTEM. 2. Describe the location, size, and orientation of the human heart.
 CHAPTER 15: THE CARDIOVASCULAR SYSTEM OBJECTIVES: 1. List the organs that compose the cardiovascular system and discuss the general functions of this system. 2. Describe the location, size, and orientation
CHAPTER 15: THE CARDIOVASCULAR SYSTEM OBJECTIVES: 1. List the organs that compose the cardiovascular system and discuss the general functions of this system. 2. Describe the location, size, and orientation
Normal & Abnormal Intracardiac. Lancashire & South Cumbria Cardiac Network
 Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
Blood vessels. transport blood throughout the body
 Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
Electrophysiology Introduction, Basics. The Myocardial Cell. Chapter 1- Thaler
 Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
Heart Rate and Physical Fitness
 Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Introduction to CV Pathophysiology. Introduction to Cardiovascular Pathophysiology
 Introduction to CV Pathophysiology Munther K. Homoud, MD Tufts-New England Medical Center Spring 2008 Introduction to Cardiovascular Pathophysiology 1. Basic Anatomy 2. Excitation Contraction Coupling
Introduction to CV Pathophysiology Munther K. Homoud, MD Tufts-New England Medical Center Spring 2008 Introduction to Cardiovascular Pathophysiology 1. Basic Anatomy 2. Excitation Contraction Coupling
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Factors Affecting Blood Pressure. Vessel Elasticity Blood Volume Cardiac Output
 Factors that Affect Pressure Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction pressure is affected by several factors:
Factors that Affect Pressure Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction pressure is affected by several factors:
THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM
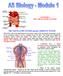 CHAPTER 6: THE CIRCULATORY SYSTEM THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM Most of the cells in the human body are not in direct contact with the external environment, so rely on the circulatory
CHAPTER 6: THE CIRCULATORY SYSTEM THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM Most of the cells in the human body are not in direct contact with the external environment, so rely on the circulatory
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
Normal Intracardiac Pressures. Lancashire & South Cumbria Cardiac Network
 Normal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform display
Normal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform display
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Starling s Law Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance
 Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance Just as the heart can initiate its own beat in the absence of any nervous or hormonal control, so also can the myocardium
Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance Just as the heart can initiate its own beat in the absence of any nervous or hormonal control, so also can the myocardium
THE HEART AND CIRCULATION HENRY S. CABIN, M.D.
 CHAPTER 1 THE HEART AND CIRCULATION HENRY S. CABIN, M.D. INTRODUCTION The cardiovascular system is an elaborate network that performs two major tasks: It delivers oxygen and nutrients to body organs and
CHAPTER 1 THE HEART AND CIRCULATION HENRY S. CABIN, M.D. INTRODUCTION The cardiovascular system is an elaborate network that performs two major tasks: It delivers oxygen and nutrients to body organs and
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Blood Pressure. Blood Pressure (mm Hg) pressure exerted by blood against arterial walls. Blood Pressure. Blood Pressure
 Blood Pressure Blood Pressure (mm Hg) pressure exerted by blood against arterial walls Systolic pressure exerted on arteries during systole Diastolic pressure in arteries during diastole 120/80 Borderline
Blood Pressure Blood Pressure (mm Hg) pressure exerted by blood against arterial walls Systolic pressure exerted on arteries during systole Diastolic pressure in arteries during diastole 120/80 Borderline
33.1 The Circulatory System
 33.1 The Circulatory System Lesson Objectives Identify the functions of the human circulatory system. Describe the structure of the heart and explain how it pumps blood through the body. Name three types
33.1 The Circulatory System Lesson Objectives Identify the functions of the human circulatory system. Describe the structure of the heart and explain how it pumps blood through the body. Name three types
3. Tunica adventitia is the outermost layer; it is composed of loosely woven connective tissue infiltrated by nerves, blood vessels and lymphatics
 Blood vessels and blood pressure I. Introduction - distribution of CO at rest II. General structure of blood vessel walls - walls are composed of three distinct layers: 1. Tunica intima is the innermost
Blood vessels and blood pressure I. Introduction - distribution of CO at rest II. General structure of blood vessel walls - walls are composed of three distinct layers: 1. Tunica intima is the innermost
Electrocardiography Review and the Normal EKG Response to Exercise
 Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Electrocardiogram and Heart Sounds
 Electrocardiogram and Heart Sounds An introduction to the recording and analysis of electrocardiograms, and the sounds of the heart. Written by Staff of ADInstruments Introduction The beating of the heart
Electrocardiogram and Heart Sounds An introduction to the recording and analysis of electrocardiograms, and the sounds of the heart. Written by Staff of ADInstruments Introduction The beating of the heart
Page 1. Introduction The blood vessels of the body form a closed delivery system that begins and ends at the heart.
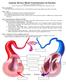 Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
Understanding the Electrocardiogram. David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem
 Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
The Body s Transport System
 Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
ACLS Chapter 3 Rhythm Review Instructor Lesson Plan to Accompany ACLS Study Guide 3e
 ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
Adult Cardiac Surgery ICD9 to ICD10 Crosswalks
 164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
2161-1 - Page 1. Name: 1) Choose the disease that is most closely related to the given phrase. Questions 10 and 11 refer to the following:
 Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Cardiovascular Biomechanics
 Cardiovascular Biomechanics Instructor Robin Shandas, Ph.D. Associate Professor of Pediatric Cardiology and Mechanical Engineering [email protected] (303) 837-2586 (MWF) / (303) 492-0553 (T,Th)
Cardiovascular Biomechanics Instructor Robin Shandas, Ph.D. Associate Professor of Pediatric Cardiology and Mechanical Engineering [email protected] (303) 837-2586 (MWF) / (303) 492-0553 (T,Th)
Common types of congenital heart defects
 Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Electrophysiology study (EPS)
 Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Dynamic Auscultation of Heart Sounds and Murmurs. Acknowledgement. Disclosures Real or Potential Conflicts of Interest
 Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
BIOL 1108 Vertebrate Anatomy Lab
 BIOL 1108 Vertebrate Anatomy Lab This lab explores major organs associated with the circulatory, excretory, and nervous systems of mammals. Circulatory System Vertebrates are among the organisms that have
BIOL 1108 Vertebrate Anatomy Lab This lab explores major organs associated with the circulatory, excretory, and nervous systems of mammals. Circulatory System Vertebrates are among the organisms that have
Catheter Ablation. A Guided Approach for Treating Atrial Arrhythmias
 Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
RACE I Rapid Assessment by Cardiac Echo. Intensive Care Training Program Radboud University Medical Centre NIjmegen
 RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
Chapter 15. Autonomic Nervous System (ANS) and Visceral Reflexes. general properties Anatomy. Autonomic effects on target organs
 Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Cardiovascular System & Its Diseases. Lecture #4 Heart Failure & Cardiac Arrhythmias
 Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University [email protected]
Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University [email protected]
Vtial sign #1: PULSE. Vital Signs: Assessment and Interpretation. Factors that influence pulse rate: Importance of Vital Signs
 Vital Signs: Assessment and Interpretation Elma I. LeDoux, MD, FACP, FACC Associate Professor of Medicine Vtial sign #1: PULSE Reflects heart rate (resting 60-90/min) Should be strong and regular Use 2
Vital Signs: Assessment and Interpretation Elma I. LeDoux, MD, FACP, FACC Associate Professor of Medicine Vtial sign #1: PULSE Reflects heart rate (resting 60-90/min) Should be strong and regular Use 2
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
What to Know About. Atrial Fibrillation
 Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Chapter 15 Anatomy and Physiology Lecture
 1 THE AUTONOMIC NERVOUS SYSTEM Chapter 15 Anatomy and Physiology Lecture 2 THE AUTONOMIC NERVOUS SYSTEM Autonomic Nervous System (ANS) regulates the activity of smooth muscles, cardiac muscles, and certain
1 THE AUTONOMIC NERVOUS SYSTEM Chapter 15 Anatomy and Physiology Lecture 2 THE AUTONOMIC NERVOUS SYSTEM Autonomic Nervous System (ANS) regulates the activity of smooth muscles, cardiac muscles, and certain
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
Chapter 16: Circulation
 Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Atrioventricular (AV) node ablation
 Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Every cell in the animal body must acquire the energy
 52 Circulation Concept Outline 52.1 The circulatory systems of animals may be open or closed. Open and Closed Circulatory Systems. All vertebrates have a closed circulation, while many invertebrate animals
52 Circulation Concept Outline 52.1 The circulatory systems of animals may be open or closed. Open and Closed Circulatory Systems. All vertebrates have a closed circulation, while many invertebrate animals
Systematic Approach to 12 Lead EKG Interpretation
 Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
