ACLS PRE-TEST ANNOTATED ANSWER KEY
|
|
|
- Allan White
- 9 years ago
- Views:
Transcription
1 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011
2 Question 1: Question 2: There is no pulse with this rhythm. Question 3:
3 Question 4: Question 5: Question 6:
4 Question 7: Question 8:
5 Question 9: Question 10: Question 11:
6 Question 12: Question 13: Question 14:
7 Question 15: Question 16:
8 Question 17: Question 18: Question 19:
9 Question 20: Question 21: Which of the following statements about the use of magnesium in cardiac arrest is most accurate? Magnesium is indicated for shock-refractory monomorphic VT. Magnesium is indicated for VF/pulseless VT associated with torsades de pointes. Magnesium is contraindicated for VT associated with a normal QT interval. Magnesium is indicated for VF refractory to shock and amiodarone or lidocaine. Question 22: A patient with ST-segment elevation MI has ongoing chest discomfort. Fibrinolytic therapy has been ordered. Heparin 4000 units IV bolus was administered, and a heparin infusion of 1000 units per hour is being administered. Aspirin was not taken by the patient because he had a history of gastritis treated 5 years ago. Your next action is to: Give aspirin 160 to 325 mg chewed immediately. Give 75 mg enteric-coated aspirin orally. Give 325 mg enteric-coated aspirin rectally. Substitute clopidogrel 300 mg loading dose. Question 23: A patient has sinus bradycardia with a heart rate of 36/min. Atropine has been administered to a total of 3 mg. A transcutaneous pacemaker has failed to capture. The patient is confused, and her blood pressure is 110/60 mm Hg. Which of the following is now indicated? Give additional 1 mg atropine. Start dopamine 10 to 20 mcg/kg per minute. Give normal saline bolus 250 ml to 500 ml. Start epinephrine 2 to 10 mcg/min.
10 Question 24: A 62-year-old man suddenly experienced difficulty speaking and left-side weakness. He was brought to the emergency department. He meets initial criteria for fibrinolytic therapy, and a CT scan of the brain is ordered. What are the guidelines for antiplatelet and fibrinolytic therapy> Do not give aspirin for at least 24 hours if rtpa is administered. Give aspirin 160 mg and clopidogrel 75 mg orally. Administer heparin if CT scan is negative for hemorrhage. Administer aspirin 160 to 325 mg chewed immediately. Question 25: A patient with possible ST-segment elevation MI has ongoing chest discomfort. Which of the following would be a contraindication to the administration of nitrates? Heart rate 90/min. Left ventricular infarct with bilateral rales. Blood pressure greater than 180 mm Hg. Use of a phosphodiesterase inhibitor within 12 hours Question 26: A patient is in cardiac arrest. Ventricular fibrillation has been refractory to a second shock. Of the following, which drug and dose should be administered first by the IV/IO route? Epinephrine 1 mg Vasopressin 20 units Sodium bicarbonate 50 meq Atropine 1 mg Question 27: A 35-year-old woman has palpitations, light-headedness, and a stable tachycardia. The monitor shows a regular narrow-complex QRS at a rate of 180/min. Vagal maneuvers have not been effective in terminating the rhythm. An IV has been established. What drug should be administered IV? Lidocaine 1mg/kg Adenosine 6 mg Epinephrine 2 to 10 mcg/kg per minute Atropine 0.5 mg Question 28: A patient with sinus bradycardia and heart rate of 42/min has diaphoresis and a blood pressure of 80/60 mm Hg. What is the initial dose of atropine? 0.1mg 3 mg 1 mg 0.5 mg Question 29: A patient is in refractory ventricular fibrillation and has received multiple appropriate defibrillation shocks, epinephrine 1 mg IV twice, and an initial dose of 300 mg amiodarone IV. The patient is intubated. A second dose of amiodarone is now called for. The recommended second dose of amiodarone is: An endotracheal dose of 2 to 4 mg/kg. 300 mg IV push. 1 mg/kg IV push. An infusion of 1 to 2 mg/min. 150 mg IV push.
11 Question 30: A patient with a possible acute coronary syndrome has ongoing chest discomfort unresponsive to 3 sublingual nitroglycerin tablets. There are no contraindications, and 4 mg of morphine sulfate was administered. Shortly afterward, blood pressure falls to 88/60 mm Hg, and the patient has increased chest discomfort. You should: Give normal saline 250 ml to 500 ml fluid bolus. Give an additional 2 mg of morphine sulfate. Give sublingual nitroglycerin 0.4 mg. Start dopamine at 2 mcg/kg per minute and titrate to a systolic blood pressure reading of 100 mm Hg. Question 31: A patient has a rapid irregular wide-complex tachycardia. The ventricular rate is 138/min. He is asymptomatic, with a blood pressure of 110/70 mm Hg. He has a history of angina. Which of the following actions is recommended? Giving adenosine 6 mg IV bolus. Seeking expert consultation. Giving lidocaine 1 to 1.5 mg IV bolus. Immediate synchronized cardioversion. Question 32: You arrive on the scene with the code team. High-quality CPR is in progress. An AED has previously advised no shock indicated. A rhythm check now finds asystole. After resuming high-quality compressions, your next action is to: Gain IV or IO access. Place an esophageal-tracheal tube or laryngeal mask airway. Attempt endotracheal intubation with minimal interruptions in CPR. Call for a pulse check. Question 33: A patient is in pulseless ventricular tachycardia. Two shocks and 1 dose of epinephrine have been given. Which is the next drug/dose to anticipate to administer? Amiodarone 300 mg Amiodarone 150 mg Vasopressin 40 units Epinephrine 3 mg Lidocaine 0.5 mg/kg Question 34: Your patient has been intubated. IV/IO access is not available. Which combination of drugs can be administered by the endotracheal route? Vasopressin, amiodarone, lidocaine Amiodarone, lidocaine, epinephrine Epinephrine, vasopressin, amiodarone Lidocaine, epinephrine, vasopressin Question 35: A patient is in cardiac arrest. Ventricular fibrillation has been refractory to an initial shock. What is the recommended route for drug administration during CPR? Femoral vein IV or IO Central line Endotracheal
12 External jugular vein Question 36: A patient is in refractory ventricular fibrillation. High-quality CPR is in progress, and shocks have been given. One does of epinephrine was given after the second shock. An antiarrhythmic drug was given immediately after the third shock. What drug should the team leader request to be prepared for administration next? Escalating dose of epinephrine 3 mg. Second dose of epinephrine 1 mg Repeat the antiarrhythmic drug Sodium bicarbonate 50 meq Question 37: A 57-year-old woman has palpitations, chest discomfort, and tachycardia. The monitor shows a regular wide-complex ORS at a rate of 180/min. She becomes diaphoretic, and her blood pressure is 80/60 mm Hg. The next action is to: Give amiodarone 300 mg IV push. Perform immediate electrical cardioversion. Establish IV access. Obtain a 12-lead ECG. Question 38: Bradycardia requires treatment when: The blood pressure is less than 100 mm Hg systolic with or without symptoms. The heart rate is less than 60/min with or without symptoms. The patient s 12-lead ECG show an MI. Chest pain or shortness of breath is present. Question 39: Which of the following statements is most accurate regarding the administration of vasopressin during cardiac arrest? Vasopressin can be administered twice during cardiac arrest. Vasopressin is indicated for VF and pulseless VT before delivery of the first shock. The correct dose of vasopressin is 40 units administered by IV or IO. Vasopressin is recommended instead of epinephrine for the treatment of asystole. Question 40: A patient is in cardiac arrest. High-quality chest compressions are being given. The patient is intubated and an IV has been started. The rhythm is asystole. Which is the first drug/dose to administer? Epinephrine 1 mg or vasopressin 40 units IV or IO. Atropine 1 mg IV or IO. Atropine 0.5 mg IV or IO. Epinephrine 3 mg via endotracheal route. Dopamine 2 to 20 mcg/kg per minute IV or IO. Question 41: A 45-year-old woman with a history of palpitations develops light-headedness and palpitations. She has received adenosine 6 mg IV for the rhythm shown above without conversion of the rhythm. She is now extremely apprehensive. Blood pressure is 108/70 mm Hg. What is the next appropriate intervention?
13 Repeat adenosine 3 mg IV. Perform immediate unsynchronized cardioversion. Sedate and perform synchronized cardioversion. Repeat adenosine 12 mg IV. Perform vagal maneuvers and repeat adenosine 6 mg IV. Question 42: A patient in the emergency department develops recurrent chest discomfort (8/10) suspicious for ischemia. His monitored rhythm becomes irregular as seen above. Oxygen is being administered by nasal cannula at 4 L/min, and an IV line is in place. Blood pressure is 160/96 mm Hg. There are no allergies or contraindications to any medication. You would first order: Sublingual nitroglycerin 0.4 mg. Morphine sulfate 2 to 4 mg IV. Lidocaine 1 mg/kg IV and infusion 2 mg/min. Amiodarone 150 mg IV. IV nitroglycerin initiated at 10 mcg/min and titrated to patient response. Question 43: Following initiation of CPR and 1 shock for VF, this rhythm is present on the next rhythm check. A second shock is given and chest compressions are resumed immediately. An IV is in place and no drugs have been given. Bag-mask ventilations are producing visible chest rise. What is your next order? Administer 3 sequential (stacked) shocks at 360 J (monophasic defibrillator). Prepare to give amiodarone 300 mg IV. Administer 3 sequential (stacked) shocks at 200 J (biphasic defibrillator). Perform endotracheal intubation; administer 100% oxygen. Prepare to give epinephrine 1 mg IV. Question 44: You arrive on the scene to find a 56-year-old diabetic woman with dizziness. She is pale and diaphoretic. Her blood pressure is 80/60 mm Hg. The cardiac monitor documents the rhythm below. She is receiving oxygen at 4 L/min by nasal cannula and an IV has been established. Your next order is:
14 Dopamine at 2 to 10 mcg/kg per minute. Sublingual nitroglycerin 0.4 mg. Morphine sulfate 4 mg IV. Atropine 0.5 mg IV. Atropine 1 mg IV. Question 45: A patient becomes unresponsive. You are uncertain if a faint pulse is present with the rhythm below. What is your next action? Order transcutaneous pacing. Begin CPR, starting with high-quality chest compressions. Start an IV and give epinephrine 1 mg IV. Consider causes of pulseless electrical activity. Start an IV and give atropine 1 mg. Question 46: This patient has been resuscitated from cardiac arrest. During the resuscitation, amiodarone 300 mg was administered. The patient developed severe chest discomfort with diaphoresis. He is now unresponsive. What is the next indicated action? Perform immediate synchronized cardioversion. Repeat amiodarone 150 mg IV. Give an immediate unsynchronized high-energy shock (defibrillation dose). Repeat amiodarone 300 mg IV. Give lidocaine 1 to 1.5 mg/kg IV. Question 47: You are monitoring the patient and note the rhythm below on the cardiac monitor. She has dizziness and her blood pressure is 80/40 mm Hg. She has an IV in place. What is your next action?
15 Start transcutaneous pacing. Give atropine 1 mg IV. Give atropine 0.5 mg IV. Administer sedation and begin immediate transcutaneous pacing at 80/min. Start dopamine at 2 to 10 mcg/kg per minute and titrate to patient response. Question 48: You arrive on the scene to find CPR in progress. Nursing staff report that the patient was recovering from a pulmonary embolism and suddenly collapsed. There is no pulse or spontaneous respirations. High-quality CPR and effective bag-mask ventilation are being provided. An IV has been initiated. What would you do now? Give atropine 1 mg IV. Give atropine 0.5 mg IV Order immediate endotracheal intubation. Give epinephrine 1 mg IV. Initiate transcutaneous pacing. Question 49: A 35-year-old woman presents to the emergency department with a chief compliant of palpitations. She has no chest discomfort, shortness of breath, or light-headedness. Which of the following is indicated first? Perform vagal maneuvers. Give adenosine 12 mg IV slow push (over 1 to 2 minutes). Give metoprolol 5 mg IV and repeat if necessary. Give adenosine 3 mg IV bolus. Question 50: You are monitoring a patient. He suddenly has the persistent rhythm shown below. You ask about symptoms and he reports that he has mild palpitations, but otherwise he is clinically stable with unchanged vital signs. What is your next action?
16 Give an immediate synchronized shock. Give sedation and perform synchronized cardioversion. Administer magnesium sulfate 1 to 2 g IV diluted in 10 ml D5W given over 5 to 20 minutes. Give an immediate unsynchronized shock. Administer adenosine 6 mg; seek expert consultation. Question 51: The patient suddenly becomes unconscious and has a weak carotid pulse. Cardiac monitoring, supplementary oxygen, and an IV have been initiated. The code cart with all the drugs and transcutaneous pacer are immediately available. Next you would: Begin transcutaneous pacing. Initiate dopamine at 10 to 20 mcg/kg per minute and to patient response. Initiate dopamine at 2 to 10 mcg/kg per minute and titrate to patient response. Give atropine 0.5 mg IV. Initiate epinephrine at 2 to 10 mcg/kg per minute. Question 52: A patient s 12-lead ECG was transmitted by the paramedics and showed an acute MI. The above findings are seen on rhythm strip when a monitor is placed in emergency department. The patient had resolution of moderate (5.10) chest pain with 3 doses of sublingual nitroglycerin. Blood pressure is 104/70 mm Hg. Which intervention below is most important, reducing in-hospital and 30-day mortality? Reperfusion therapy. IV nitroglycerin for 24 hours. Temporary pacing. Atropine 0.5 mg IV, total dose 2 mg as needed. Atropine 1 mg IV, total dose 3 mg as needed. Question 53: This patient was admitted to the general medical ward with a history of alcoholism. A code is in progress and he has recurrent episodes of this rhythm. You review his chart. Notes about the 12-lead ECG say
17 that his baseline QT interval is high normal to slightly prolonged. He has received 2 doses of epinephrine 1 mg and 1 dose of amiodarone 300 mg IV so far. What would you order for his next medication? Lidocaine 1 to 1.5 mg IV and start infusion 2 mg/min. Repeat amiodarone 300 mg IV. Repeat amiodarone 150 mg IV. Give sodium bicarbonate 50 meq IV. Give magnesium sulfate 1 to 2 g IV diluted in 10 ml D5W given over 5 to 20 minutes Question 54: You are the code team leader and arrive to find a patient with above rhythm and CPR in progress. Team members report that the patient was well but reported chest pain and then collapsed. She has no pulse or respirations. Bag-mask ventilations are producing visible chest rise, high-quality CPR is in progress, and an IV has been established. What would be your next order? Administer atropine 1 mg. Perform endotracheal intubation. Start dopamine at 10 to 20 mcg/kg per minute. Administer epinephrine 1 mg. Administer amiodarone 300 mg. Question 55: A patient presents with the rhythm below and reports an irregular heartbeat. She has no other symptoms. Her medical history is significant for a myocardial infarction 7 years ago. Blood pressure is 110/70 mm Hg. What would you do at this time? Perform elective synchronized cardioversion with presedation. Continue monitoring and seek expert consultation. Administer nitroglycerin 0.4 sublingual or spray. Administer lidocaine 1mg/kg IV. Perform emergency synchronized cardioversion
18 Question 56: A patient was in refractory ventricular fibrillation. A third shock has just been administered. Your team looks to you for instructions. Your immediate next order is: Perform endotracheal intubation. Resume high-quality chest compressions. Check the carotid pulse. Give atropine 1 mg IV. Give amiodarone 300 mg IV. Question 57: You are evaluating a patient with chest discomfort lasting 15 minutes during transportation to the emergency department. He is receiving oxygen and 2 sublingual nitroglycerin tablets have relieved his chest discomfort. He reports no other symptoms but appears anxious. Blood pressure is 130/70 mm Hg. You observe the rhythm below on the monitor. What is your next action? Give atropine 0.5 mg IV. Initiate transcutaneous pacing (TCP). Start epinephrine 2 to 10 mcg/min and titrate to patient response. Continue monitoring the patient and seek expert consultation. Administer sublingual nitroglycerin 0.4 mg. Question 58: Following resuscitation with CPR and a single shock, you observe this rhythm while preparing the patient for transport. Your patient is stable and blood pressure is 120/80 mm Hg. She is apprehensive but has no symptoms other than palpitations. At this time you would: Give magnesium sulfate 1 to 2 g over 20 minutes. Seek expert consultation. Give lidocaine 1 to 1.5 mg IV and start infusion. Give amiodarone 300 mg IV and start infusion
19 Question 59: You are monitoring a patient with chest discomfort who suddenly becomes unresponsive. You observe the following rhythm on the cardiac monitor. A defibrillator is present. What is your first action? Intubate the patient and give epinephrine 2 to 4 mg via the endotracheal tube. Being CPR with chest compressions for 2 minutes or about 5 cycles of compressions and ventilations. Establish an IV and give epinephrine 1 mg. Establish and IV and give vasopressin 40 units. Give a single shock. Question 60: A patient has been resuscitated from cardiac arrest and is being prepared for transport. She is intubated and is receiving 100% oxygen. Blood pressure is 80/60 mm Hg. During the resuscitation, she received 2 doses of epinephrine 1 mg and 1 does of amiodarone 300 mg IV. You now observe this rhythm on the cardiac monitor. The rhythm abnormality is becoming more frequent and increasing in number. You should order: Amiodarone 150 mg IV bolus; start infusion. A repeat dose of epinephrine 1 mg IV. Lidocaine 1 to 1.5 mg IV; star infusion. 1 to 2 L of normal saline. Amiodarone 300 mg IV.
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Team Leader. Ensures high-quality CPR at all times Assigns team member roles Ensures that team members perform well. Bradycardia Management
 ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
IU Health ACLS Study Guide
 IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
American Heart Association. Pediatric Advanced Life Support. Written Precourse Self-Assessment. Questions and Answer Key for Students.
 E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
10. An infant with a history of vomiting and diarrhea arrives by ambulance. During your primary assessment the infant responds only to painful stimula
 1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
Practical ACLS Megacode Testing and Training Scenario Set for SimPad. Consolidated Instructor Manual. Frances Wickham Lee, DBA
 Practical ACLS Megacode Testing and Training Scenario Set for SimPad Consolidated Instructor Manual Frances Wickham Lee, DBA Scenario Authors: Frances Wickham Lee, DBA John Walker, BHS John Schaefer, MD
Practical ACLS Megacode Testing and Training Scenario Set for SimPad Consolidated Instructor Manual Frances Wickham Lee, DBA Scenario Authors: Frances Wickham Lee, DBA John Walker, BHS John Schaefer, MD
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE
 ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
table of contents drug reference
 table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Wilson County Emergency Management Agency Protocol Manual Protocols
 Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010!
 ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010.
 ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
ACLS123.com 818.766.1111 2012. ACLS Study Guide. Critical Care Training Center
 ACLS123.com 818.766.1111 2012 ACLS Study Guide Critical Care Training Center 12/1/2012 Course Overview This study guide is an outline of content that will be taught in the American Heart Association Accredited
ACLS123.com 818.766.1111 2012 ACLS Study Guide Critical Care Training Center 12/1/2012 Course Overview This study guide is an outline of content that will be taught in the American Heart Association Accredited
PALS Interim Study Guide
 PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC
 Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC Student Name: Test Bradycardia Management Recognizes symptomatic bradycardia Administers correct dose of atropine Prepares for second-line
Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC Student Name: Test Bradycardia Management Recognizes symptomatic bradycardia Administers correct dose of atropine Prepares for second-line
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES. Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003.
 MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
Alabama Medications. Christopher J. Colvin January 2010
 Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
THE REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE NEW YORK CITY PREHOSPITAL TREATMENT PROTOCOLS ADVANCED LIFE SUPPORT (PARAMEDIC) PROTOCOLS
 THE REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE NEW YORK CITY PREHOSPITAL TREATMENT PROTOCOLS ADVANCED LIFE SUPPORT (PARAMEDIC) PROTOCOLS July 2012 Version 07012012 The Regional Emergency Medical Services
THE REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE NEW YORK CITY PREHOSPITAL TREATMENT PROTOCOLS ADVANCED LIFE SUPPORT (PARAMEDIC) PROTOCOLS July 2012 Version 07012012 The Regional Emergency Medical Services
Department of Emergency and Disaster Medicine Medical University of LODZ
 Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. October 2006
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment Contents: Precourse Self-Assessment Memo Support Help for CD and FAQs Answer Sheet Self-Assessment
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment Contents: Precourse Self-Assessment Memo Support Help for CD and FAQs Answer Sheet Self-Assessment
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care
 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Presenter Name Disclosures
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Presenter Name Disclosures
WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets.
 ACLS STUDY GUIDE 2015 WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets. The AHA also requests the following in preparation
ACLS STUDY GUIDE 2015 WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets. The AHA also requests the following in preparation
AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW
 AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW Joseph Heidenreich, MD Texas A&M Health Science Center Scott & White Memorial Hospital Scott & White Memorial Hospital
AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW Joseph Heidenreich, MD Texas A&M Health Science Center Scott & White Memorial Hospital Scott & White Memorial Hospital
^'T:il,Tif,ll rt) Learn and Live..,
 ^'T:il,Tif,ll rt) Learn and Live.., American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment December 2006 Artrcrican Hr " nrr,r.iorl?rll ( karn and Live ECG Rhythm
^'T:il,Tif,ll rt) Learn and Live.., American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment December 2006 Artrcrican Hr " nrr,r.iorl?rll ( karn and Live ECG Rhythm
Resuscitation Patient Management Tool May 2015 CPA Event
 OPTIONAL: Local Event ID: Did pt. receive chest compressions and/or defibrillation during this event? criteria) (does NOT meet inclusion Date/Time the need for chest compressions ( or defibrillation when
OPTIONAL: Local Event ID: Did pt. receive chest compressions and/or defibrillation during this event? criteria) (does NOT meet inclusion Date/Time the need for chest compressions ( or defibrillation when
ANZCOR Guideline 12.4 Medications and Fluids in Paediatric Advanced Life Support
 ANZCOR Guideline 12. Medications and Fluids in Paediatric Advanced Life Support Who does this guideline apply to? This guideline applies to infants and children. Summary Who is the audience for this guideline?
ANZCOR Guideline 12. Medications and Fluids in Paediatric Advanced Life Support Who does this guideline apply to? This guideline applies to infants and children. Summary Who is the audience for this guideline?
DEBRIEFING GUIDE. The key components of an optimal code response: 1. Early recognition that the patient is deteriorating or has become unresponsive.
 DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
Medication Math OBJECTIVES INTRODUCTION. Jones & Bartlett Learning, LLC NOT FOR SALE OR DISTRIBUTION
 Medication Math C H A P T E R4 OBJECTIVES 1. Identify the basic units of measure for weight, length, and volume. 2. Accurately convert milliliters to cubic centimeters, kilograms to pounds, and milligrams
Medication Math C H A P T E R4 OBJECTIVES 1. Identify the basic units of measure for weight, length, and volume. 2. Accurately convert milliliters to cubic centimeters, kilograms to pounds, and milligrams
EMERGENCY MEDICAL SERVICES PRE-HOSPITAL TREATMENT PROTOCOLS
 EMERGENCY MEDICAL SERVICES PRE-HOSPITAL TREATMENT PROTOCOLS COMPLETE TEXT Eighth Edition Official Version # 8.03 Effective 3/1/2010 MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL
EMERGENCY MEDICAL SERVICES PRE-HOSPITAL TREATMENT PROTOCOLS COMPLETE TEXT Eighth Edition Official Version # 8.03 Effective 3/1/2010 MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) Pharmacist Objectives. Pharmacists in the ER. Background
 The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
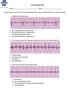 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Critical Care/ Emergency Department Medication Competency Exam
 Employee name: Score: / = % Critical Care/ Emergency Department Medication Competency Exam Please circle or write in (where applicable) the correct answer for each question below. There is only 1 correct
Employee name: Score: / = % Critical Care/ Emergency Department Medication Competency Exam Please circle or write in (where applicable) the correct answer for each question below. There is only 1 correct
BLS: basic cardiac life support. ACLS: advanced cardiac life support. PALS: paediatric advanced life support. VF: ventricular fibrillation
 RN-Initiated Emergency Cardiac Care: Decision Support Tool #2 Emergency Cardiac Care in Areas Using Cardiac Monitoring, Defibrillation and Emergency Cardiac Drugs Decision support tools are evidenced-based
RN-Initiated Emergency Cardiac Care: Decision Support Tool #2 Emergency Cardiac Care in Areas Using Cardiac Monitoring, Defibrillation and Emergency Cardiac Drugs Decision support tools are evidenced-based
The American Heart Association Guidelines Including Pediatric Resuscitation
 Lesson 3 The American Heart Association Guidelines Including Pediatric Resuscitation Sharon E. Mace, MD, FACEP, FAAP Objectives On completion of this lesson, you should be able to: 1. List the correct
Lesson 3 The American Heart Association Guidelines Including Pediatric Resuscitation Sharon E. Mace, MD, FACEP, FAAP Objectives On completion of this lesson, you should be able to: 1. List the correct
TENNESSEE EMERGENCY MEDICAL SERVICES PROTOCOL GUIDELINES. Index
 Introduction Definitions Index Cardiac Emergency (Adult & Pediatric) 101 Automatic External Defibrillator 102 New Onset Atrial Fibrillation and Flutter 103 Bradycardia 104 Acute Coronary Syndrome/STEMI
Introduction Definitions Index Cardiac Emergency (Adult & Pediatric) 101 Automatic External Defibrillator 102 New Onset Atrial Fibrillation and Flutter 103 Bradycardia 104 Acute Coronary Syndrome/STEMI
Allergy Emergency Treatment Protocol
 Allergy Emergency Treatment Protocol I. Initial evaluation of possible allergic reaction a. Cease administration of allergenic extracts b. Notify physician c. Record vital signs: blood pressure, pulse,
Allergy Emergency Treatment Protocol I. Initial evaluation of possible allergic reaction a. Cease administration of allergenic extracts b. Notify physician c. Record vital signs: blood pressure, pulse,
Paediatric Advanced Life Support
 Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials
 Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials 1 ADULT CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION TABLE OF CONTENTS PRIMARY AND SECONDARY ABCDs I. Primary ABCD s 03 II. Secondary
Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials 1 ADULT CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION TABLE OF CONTENTS PRIMARY AND SECONDARY ABCDs I. Primary ABCD s 03 II. Secondary
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Heart Attack: What You Need to Know
 A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference
 New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
The management of cardiac arrest
 CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
Drug List. Medication Adult Dosing Pediatric Dosing. V-fib / pulseless V-tach 300 mg IV push Repeat dose of 150 mg IV push for recurrent episodes
 Acetaminophen (Tylenol) 7-Pain Control-Adult 46-Pain Control-Pediatric 72-Fever 1000 mg po 15 mg/kg po Indicated for pain and fever control Avoid in patients with severe liver disease Adenosine (Adenocard)
Acetaminophen (Tylenol) 7-Pain Control-Adult 46-Pain Control-Pediatric 72-Fever 1000 mg po 15 mg/kg po Indicated for pain and fever control Avoid in patients with severe liver disease Adenosine (Adenocard)
Paramedic Pediatric Medical Math Test
 Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Authorized Procedure List
 Agency Name: Authorized Procedure List Agency Director Signature: Medical Director Signature: Airway Airway Assessment Oxygen Therapy--Nasal Cannula Oxygen Therapy--Non Rebreather Mask Oxygen Therapy-Partial
Agency Name: Authorized Procedure List Agency Director Signature: Medical Director Signature: Airway Airway Assessment Oxygen Therapy--Nasal Cannula Oxygen Therapy--Non Rebreather Mask Oxygen Therapy-Partial
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
OBJECTIVES. When the student has finished this module, he/she will be able to:
 Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
LIFEPAK 15 MONITOR/DEFIBRILLATOR
 LIFEPAK 15 MONITOR/DEFIBRILLATOR Setup Options This document describes how to enter Setup mode and change operating settings in the LIFEPAK 15 monitor/defibrillator. Defining Setup Options Setup mode
LIFEPAK 15 MONITOR/DEFIBRILLATOR Setup Options This document describes how to enter Setup mode and change operating settings in the LIFEPAK 15 monitor/defibrillator. Defining Setup Options Setup mode
Wide-Complex Tachycardias in the ED: Myths and Pitfalls
 Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
!!! BOLUS DOSE IV. Use 5-10 mcg IV boluses STD ADRENALINE INFUSION. Use IM adrenaline in advance of IV dosing!
 ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
School of Health Sciences
 School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
ACLS PROTOCOLS. Chest Pain / Acute Coronary Syndrome... 4-2
 ACLS PROTOCOLS CHEST PAIN / ACLS Chest Pain / Acute Coronary Syndrome... 4-2 ARRHYTHMIAS / ACLS Sinus Bradycardia... 4-4 Narrow - Complex Tachycardia... 4-6 Wide - Complex Tachycardia... 4-8 CARDIAC ARREST
ACLS PROTOCOLS CHEST PAIN / ACLS Chest Pain / Acute Coronary Syndrome... 4-2 ARRHYTHMIAS / ACLS Sinus Bradycardia... 4-4 Narrow - Complex Tachycardia... 4-6 Wide - Complex Tachycardia... 4-8 CARDIAC ARREST
Basic ECG rhythm interpretation skills (see our Six Second ECG Essentials or Mastery courses and our Six Second ECG Simulator online)
 SkillStat ACLS Precourse Package Thank you for choosing SkillStat Learning Inc. for your Advanced Life Support training needs. SkillStat Learning Inc. has delivered advanced practice programs to healthcare
SkillStat ACLS Precourse Package Thank you for choosing SkillStat Learning Inc. for your Advanced Life Support training needs. SkillStat Learning Inc. has delivered advanced practice programs to healthcare
Neonatal Reference Guide
 Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY
 Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
ADVANCED LIFE SUPPORT LEARNING PACKAGE
 SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
Basic Cardiac Rhythms Identification and Response
 Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
RESPONDING TO ANESTHETIC COMPLICATIONS
 RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
What Are Arrhythmias?
 What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials
 Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
Medical Tourism - The Role of Intervals inCardiovascular Cancer
 Acute Decompensated Heart Failure: Time Critical Interventions MO-51 / 1 Hour Faculty: Matthew Strehlow, MD, FACEP Monday, 10/26/2015 / 3:30 PM - 4:20 PM The treatment of congestive heart failure (CHF)
Acute Decompensated Heart Failure: Time Critical Interventions MO-51 / 1 Hour Faculty: Matthew Strehlow, MD, FACEP Monday, 10/26/2015 / 3:30 PM - 4:20 PM The treatment of congestive heart failure (CHF)
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
