Bradycardia CHAPTER 12 CODE SCENARIO
|
|
|
- Shana Cannon
- 9 years ago
- Views:
Transcription
1 Senecal-12.qxd 14/04/ :44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably in a monitored bed when the monitor alarm suddenly signaled an abnormal heart rate. The nurse finds the man unresponsive with a heart rate of 42 bpm. The code team arrives and finds the man unconscious in bed. The team leader assesses for a pulse and feels a faint carotid pulse at about 40 bpm corresponding to the QRS complexes on the monitor (Figure 12-1). FIGURE What is the cardiac rhythm? a. Pulseless electrical activity b. Type I second-degree (Wenckebach) c. Type II second-degree d. Third-degree The rhythm strip demonstrates P-waves that are dissociated from the QRS complexes (denoted by arrows in figure), which is indicative of third-degree, or complete,. Pathologic bradycardias (e.g., those that result in hypoperfusion) can be classified into one of several types. First-degree is defined as a prolonged PR interval and does not result in hypoperfusion. Type I second-degree, commonly known as Wenckebach, is defined as progressive PR prolongation until a QRS complex is entirely dropped. Similar to first-degree block, Wenckebach does not compromise cardiac output. Both type II second-degree and third-degree are malignant arrhythmias frequently associated with hemodynamic compromise. Type II second-degree is characterized by fixed PR intervals with intermittently dropped QRS complexes. This rhythm is a precursor to third-degree, in which there is complete dissociation of P-waves from the QRS complexes, as seen in this patient. 2. What is the first appropriate action for this patient? a. Initiate cardiopulmonary resuscitation (CPR) with bag-valve-mask (BVM) ventilation and cardiac compressions b. Establish large-bore IV access c. Intubate the patient d. Administer atropine 1 mg IV push In resuscitating this patient, several things should be occurring simultaneously. Ideally, a code cart containing standard code medications, a defibrillator, and airway equipment is immediately available. Realistically, it may take several minutes for the code cart to be wheeled into the patient s room. The patient should be placed on high-flow oxygen via a nonrebreather mask until a BVM can be obtained. Someone should be responsible for connecting the defibrillator and, in this case, preparing for 69
2 Senecal-12.qxd 14/04/ :44 AM Page PART II CARDIAC CODES transcutaneous pacing. Because this patient has been admitted to the hospital, IV access is probably already established. Largebore access is not a high priority immediately. CPR is not necessary in a patient who has a palpable pulse, albeit bradycardiac and weak. Intubation may be indicated, but it will take several minutes, and the most immediate priority in this patient is reversing the bradycardia that is likely the etiology of the patient s mental status decline. Atropine 1 mg IV push should be given as soon as possible. Ideally one person should be managing the airway and preparing for intubation, another person should be preparing the defibrillator for transcutaneous pacing, and a third should be preparing the code medications. In this case both atropine and epinephrine should be readily available. The patient is administered 1 mg of atropine IV and his pulse increases to 52 bpm. The patient becomes more alert and his blood pressure is 82/42, but his heart rate dips back down to the low 40s again. 3. What is the next appropriate step? a. Administer epinephrine 1 mg IV push b. Initiate transcutaneous pacing c. Start dopamine drip at 10 lg/kg/min d. Defibrillate at 50 J biphasic The effect of atropine in the setting of bradycardia is to block parasympathetic receptors, and thus augment sympathetic drive. Atropine acts primarily at the sinus node and atrioventricular (AV) node. However, in third-degree, the ventricular rate is determined by the escape pacemaker of the AV node or ventricular escape beats. Therefore, atropine is often ineffective in third-degree. Epinephrine has the effect of increasing sympathetic drive, thus promoting escape pacemakers in the AV node and ventricle. Epinephrine also directly increases cardiac contractility and cardiac output. The best way to reverse this patient s hypoperfusion is to reestablish a pacemaker that fires at greater than 60 bpm. If this is not accomplished by atropine alone, then the next best step is to start transcutaneous pacing. Epinephrine may transiently increase heart rate and blood pressure, but bradycardia will likely recur within several minutes as the drug wears off. Epinephrine imparts a massive sympathetic surge and workload on a heart that likely has baseline impairment. If the patient remains hypotensive, dopamine can be started to increase inotropy. Transcutaneous pacing is initiated and set at a rate of 60 bpm, and a dopamine drip is started at 10 µg/kg/min (Figure 12-2). The patient becomes more alert and a repeat blood pressure is 108/68. The patient is transferred to the ICU where a right subclavian central venous line is placed and transvenous pacing is initiated. FIGURE 12-2 Transcutaneously paced rhythm. Answers: 1-d; 2-d; 3-b DEFINITION Bradycardia is defined as a heart rate of less than 60 bpm. This may be perfectly normal in young, healthy adults or in patients who are taking AV nodal blocking agents. Bradycardia is considered pathologic if it results in decreased cardiac output to the point where it causes symptoms (Box 12-1). Pathologic bradycardia occurs most commonly in elderly people with underlying cardiac conduction abnormalities. It occurs less commonly in cases of toxic ingestion (e.g., overdose of AV nodal blockers, digoxin, organophosphates, and others). It is important to remember that the heart rate is determined by the pulse and not what is
3 Senecal-12.qxd 14/04/ :44 AM Page 71 CHAPTER 12 BRADYCARDIA 71 BOX 12-1 Common symptoms and signs associated with symptomatic bradycardia Lightheadedness Fatigue/weakness Syncope Nausea Diaphoresis Shortness of breath Weak pulses Hypotension TABLE 12-1 Characteristics of s Type of Characteristics First-degree Second-degree type I (Wenckebach) Second-degree type II Third-degree PR prolongation > 200 msec (five small boxes) Progressive PR prolongation until a QRS complex is dropped Fixed PR interval with intermittently dropped QRS complex AV dissociation (P-waves are completely dissociated from QRS complexes) displayed on the monitor. For example, a patient may be in bigeminy (e.g., alternating sinus beat with an ectopic ventricular beat) with a displayed heart rate of 80. But if the ectopic ventricular contractions are not strong enough to effect forward blood flow, then the actual pulse rate is 40 and the patient is bradycardic. ETIOLOGY Symptomatic bradycardia is the result of one of two possible physiologic disturbances. The first is the depression of the dominant pacemaker, or the sinus node. The second is the result of a conduction system delay, most typically at the AV node. Either form of bradycardia may result in the firing of secondary pacemakers in the heart, resulting in escape beats. These secondary pacemakers include the AV node (junctional escape beats) and ventricle (ventricular escape beats). Sinus Node Dysfunction (Sick Sinus Syndrome) Sinus node dysfunction has several manifestations, including, sinus pauses, bradycardia, and tachycardiabradycardia syndrome. A sinus pause is a period greater than 5 seconds during which there is no atrial depolarization, which appears as a period of asystole on the monitor. This may result in symptoms such as lightheadedness, blurred vision, nausea, or syncope. Tachycardia-bradycardia syndrome is manifested by periods of tachycardia, often rapid atrial fibrillation, followed by periods of profound bradycardia. Sinus node dysfunction is most commonly the result of acute or chronic cardiac ischemia, dilated cardiomyopathy, or medications. AV Block AV block occurs when conduction through the atria, AV node, and proximal His-Purkinje system is impaired. Table 12-1 summarizes the increasing degrees of AV block based on ECG criteria. First-degree AV block is characterized by PR interval prolongation (more than 200 msec or 5 small boxes) and is generally a benign finding. Figure 12-3 depicts a rhythm strip with first-degree. Second-degree is divided into type I (Wenckebach) and type II. Type I second-degree AV block (Wenckebach) is caused by a conduction disturbance within the AV node. It is characterized by the progressive lengthening of the PR interval until the impulse is not conducted, resulting in a dropped QRS complex (Figure 12-4). A resetting of the original PR interval follows each dropped beat. Similar to first-degree AV block, type I second-degree AV block is infrequently clinically significant, except that it may eventually progress to type II second-degree or to third-degree. FIGURE 12-3 First-degree : PR interval is greater than 200 msec.
4 Senecal-12.qxd 14/04/ :44 AM Page PART II CARDIAC CODES FIGURE 12-4 Second-degree type I (Wenckebach); note that the PR interval progressively lengthens until a QRS complex is not conducted at all. Additionally, type I second-degree AV block may be seen in patients with inferior myocardial ischemia. Type II second-degree AV block and third-degree AV block are more malignant arrhythmias that are associated with a conduction disturbance below the level of the AV node. In type II second-degree AV block, QRS complexes are intermittently dropped with intervening complexes that have normal PR intervals (Figure 12-5). Type II second-degree often precedes third-degree. Third-degree heart block is characterized by the complete absence of atrial impulse conduction through the AV node. Although P-waves (which represent atrial depolarization) occur at a regular rate on the ECG, none of the atrial impulses are conducted to the ventricles. Therefore, for the ventricle to depolarize, it must be triggered by a ventricular pacemaker, which typically triggers at a rate of 30 to 40 bpm. This results in complete dissociation of P-waves and QRS complexes, with the rate of P-waves being significantly faster than the rate of QRS complexes (Figure 12-6). TREATMENT Asymptomatic Patients Can Wait The treatment of bradycardia depends on the stability of the patient. Signs and symptoms of inadequate tissue perfusion, including mental status changes, hypotension, chest pain, and difficulty breathing, indicate instability. Prompt treatment is warranted in these patients (Box 12-2). In stable patients, the treatment depends on the etiology of the bradycardia. For stable sick sinus syndrome, the patient can be closely monitored for further decompensation. These patients usually require permanent pacemaker placement by a cardiologist in the cath lab. Patients with first-degree or type I second-degree AV block require no treatment unless they develop symptoms. Conversely, given the unstable nature of type II second-degree and thirddegree AV block, transvenous pacing is often required emergently until a permanent pacemaker can be implanted. Think Cardiac Ischemia Acute myocardial infarction (MI) is a common cause of bradycardia; therefore, obtaining a 12-lead ECG early is important. Occlusion of the right coronary artery, causing ST-segment elevation in the inferior leads, often results in second- and third-degree. Inferior MI is also frequently associated with increased parasympathetic tone. Symptoms of inferior MI tend to be vagal in nature, and include nausea, diaphoresis, abdominal discomfort, and bradycardia. Inferior MI may also be associated with right ventricular FIGURE 12-5 Second-degree type II ; note that the second and sixth P-waves are not followed by a QRS complex. FIGURE 12-6 Third-degree ; arrows indicate P-waves that are dissociated from the QRS complexes.
5 Senecal-12.qxd 14/04/ :44 AM Page 73 CHAPTER 12 BRADYCARDIA 73 BOX 12-2 Critical steps in treating bradycardia BOX 12-4 Dopamine 1. Identify symptomatic bradycardia 2. Establish ABCs, IV, O 2, monitor 3. Apply transcutaneous pacing pads and defibrillator leads 4. Identify specific s 5. Identify associated cardiac ischemia 6. Reach for atropine as first-line drug 7. Establish transcutaneous pacing if atropine is ineffective 8. Start vasopressors if patient continues to be hypotensive 9. Know when transvenous pacing is indicated If the maximum dose of atropine (0.04 mg/kg or about 2 3 mg) has been administered without effect, a dopamine infusion should be started at 5 lg/kg/min. The dose can be titrated up to 20 lg/kg/min as needed to restore heart rate and blood pressure. Dopamine is a catecholamine that stimulates beta-adrenergic receptors, causing an increase in cardiac contractility and chronicity. Dopamine at higher doses also stimulates alpha-adrenergic receptors, resulting in peripheral vasoconstriction and increased blood pressure. infarction. Symptomatic bradycardia in these patients often responds to a fluid bolus, which increases right ventricular filling and thus increases cardiac output. Acute anterior ST-segment elevation MI, or occlusion of the left coronary or left anterior descending artery, can cause third-degree due to ischemia of the AV node. These patients require immediate cardiac catheterization. If cardiac catheterization is not available, systemic thrombolysis and transcutaneous pacing should be initiated. Unstable Patients Require Intervention The first line of therapy is atropine mg IV given in 3- to 5-minute intervals up to a total dose of 0.04 mg/kg. While atropine is being administered, the external pacing pads should be placed on the patient and transcutaneous pacing initiated. If the patient remains hypotensive after these measures, then dopamine or epinephrine drips should be started. These patients should receive transvenous pacing as soon as possible, and the underlying cause of bradycardia should be sought out and treated expeditiously. See Boxes 12-3, 12-4, and 12-5 for more information on atropine, dopamine, and transcutaneous pacing. Unstable patients with bradycardia require immediate stabilization (see bradycardia algorithm on page 75). BOX 12-5 Transcutaneous pacing BOX 12-3 Atropine Atropine is a compound found in Atropa belladonna and other plants. As a tertiary amine, atropine is a tertiary amine and therefore lipid soluble and thus is widely distributed throughout the body. This results in a long duration of action. Atropine blocks muscarinic receptors, making it the prototypical anticholinergic agent. Its effect on the heart is mediated by competitive M 2 receptor blockade in the AV node resulting in uninhibited sympathetic tone that increases AV conduction and heart rate. Other anticholinergic effects of atropine include decreased salivation (especially in children), mydriasis (this effect lasts more than 72 hours), decreased gut motility, and decreased bladder tone (urinary retention). It is important to remember that pupils will be dilated and fixed after the administration of atropine; therefore, fixed pupils should not be misinterpreted as irreversible brain death. Another key point is that atropine acts at the AV node; therefore, atropine is not useful in bradycardias caused by type II second-degree and thirddegree AV block in which the conduction block is below the AV node. Transcutaneous pacing is a lifesaving intervention that is critical to treating symptomatic bradycardia. Most current defibrillators perform transcutaneous pacing, which provides electrical pacing impulses to the heart through the skin by cutaneous electrodes. The anode and cathode electrodes are contained in the large defibrillator pads that are also used for electrical defibrillation. Of note, the three defibrillator limb leads must also be attached to perform transcutaneous pacing. Once the leads are attached, the operator sets a pacing rate, typically 60 to 80 bpm. The electrical current is then titrated up until electrical capture is obtained. Starting with the dial at zero, the electrical current is gradually increased until contraction of external musculature occurs. This is often uncomfortable for an alert patient, and therefore sedation is required. As the current is increased, the operator monitors the cardiac rhythm. Capture is characterized by the presence of ventricular depolarizations following pacing impulses. Once capture occurs, the electrical current required to achieve capture is noted (typically 60 to 100 mamp) and maintained. The peripheral pulse rate should correspond with the set pacer rate if capture is occurring properly.
6 Senecal-12.qxd 14/04/ :44 AM Page PART II CARDIAC CODES KEY POINTS Treat only symptomatic bradycardia in the acute stage First-degree and type I second-degree AV block do not require treatment if asymptomatic Type II second-degree and third-degree AV block will require transvenous pacing Be wary of asymptomatic bradycardias that may deteriorate Type II second-degree AV block Third-degree AV block Remember the treatment sequence for symptomatic bradycardia Atropine Transcutaneous pacing Dopamine Epinephrine
7 Senecal-12.qxd 14/04/ :44 AM Page 75 CHAPTER 12 BRADYCARDIA 75 ALGORITHM: BRADYCARDIA Obtain 12-lead EKG to identify rhythm symptomatic Sinus bradycardia baseline? excess nodal blockade? Junctional rhythm patient on digoxin? (If yes, treat dig toxicity) Atropine 1 mg IV q 3 5 min x 3 Obtain 12-lead EKG symptoms persist Transcutaneous pacing Monitor Monitor hypotensive Dopamine 5 20 mcg/kg/min IV infusion OR Epinephrine 2 10 mcg/kg/min IV infusion OR 1st-degree 2nd-degree type I 2nd-degree type II 3rd-degree Isoproterenol 2 10 mcg/kg/min IV infusion Monitor Transvenous pacing
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
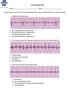 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Team Leader. Ensures high-quality CPR at all times Assigns team member roles Ensures that team members perform well. Bradycardia Management
 ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Interpreting AV (Heart) Blocks: Breaking Down the Mystery
 Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
TOP 5. The term cardiac arrhythmia encompasses all cardiac. Arrhythmias in Dogs & Cats. Sinus Arrhythmia. TOP 5 Arrhythmias Seen in Dogs & Cats
 Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
School of Health Sciences
 School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
IU Health ACLS Study Guide
 IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010.
 ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
VCA Veterinary Specialty Center of Seattle
 An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES. Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003.
 MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Understanding the Electrocardiogram. David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem
 Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Banner Staff Service ECG Study Guide
 Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
The science of medicine. The compassion to heal.
 A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS
 Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Advanced EKG Interpretation
 Advanced EKG Interpretation JUNCTIONAL RHYTHMS AND NURSING INTERVENTIONS Objectives Identify specific cardiac dysrhythmias Describe appropriate nursing interventions for specific dysrhythmias Junctional
Advanced EKG Interpretation JUNCTIONAL RHYTHMS AND NURSING INTERVENTIONS Objectives Identify specific cardiac dysrhythmias Describe appropriate nursing interventions for specific dysrhythmias Junctional
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
ACLS Chapter 3 Rhythm Review Instructor Lesson Plan to Accompany ACLS Study Guide 3e
 ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Arrest. What s a Nurse to do?
 Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Guideline for the management of arrhythmias
 Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
What Are Arrhythmias?
 What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
ACLS Rhythms for the ACLS Algorithms
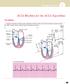 ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
RAPID INTERPRETATION OF. EKG s
 Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed
 Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
Introduction. Planned surgical procedures
 Guidelines for the perioperative management of patients with implantable pacemakers or implantable cardioverter defibrillators, where the use of surgical diathermy/electrocautery is anticipated. Introduction
Guidelines for the perioperative management of patients with implantable pacemakers or implantable cardioverter defibrillators, where the use of surgical diathermy/electrocautery is anticipated. Introduction
Key Medical Terms Associated with the Cardiovascular System
 1 Key Medical Terms Associated with the Cardiovascular System Aneurysm: A thin, weakened section of the wall of an artery or vein that bulges outward, forming a balloon-like sac. Common causes are atherosclerosis,
1 Key Medical Terms Associated with the Cardiovascular System Aneurysm: A thin, weakened section of the wall of an artery or vein that bulges outward, forming a balloon-like sac. Common causes are atherosclerosis,
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
Evaluation copy. Analyzing the Heart with EKG. Computer
 Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation
 The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation 2 P a g e Table of Contents Introduction How the Heart Works 3 How the Heart s Electrical System Works 3 Commonly Used Heart
The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation 2 P a g e Table of Contents Introduction How the Heart Works 3 How the Heart s Electrical System Works 3 Commonly Used Heart
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology
 Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology Chapter 4: Endocrine, Nutritional, and Metabolic Diseases (E00-E89) The diabetes mellitus codes are combination codes
Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology Chapter 4: Endocrine, Nutritional, and Metabolic Diseases (E00-E89) The diabetes mellitus codes are combination codes
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Department of Emergency and Disaster Medicine Medical University of LODZ
 Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
Catheter Ablation. A Guided Approach for Treating Atrial Arrhythmias
 Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
2015 Interim Resources for BLS
 2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
Acute Coronary Syndrome. What Every Healthcare Professional Needs To Know
 Acute Coronary Syndrome What Every Healthcare Professional Needs To Know Background of ACS Acute Coronary Syndrome (ACS) is an umbrella term used to cover a spectrum of clinical conditions that are caused
Acute Coronary Syndrome What Every Healthcare Professional Needs To Know Background of ACS Acute Coronary Syndrome (ACS) is an umbrella term used to cover a spectrum of clinical conditions that are caused
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ
 «Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia
 Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
Basics of Pacing. Ruth Hickling, RN-BSN Tasha Conley, RN-BSN
 Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
BIPOLAR LIMB LEADS UNIPOLAR LIMB LEADS PRECORDIAL (UNIPOLAR) LEADS VIEW OF EACH LEAD INDICATIVE ECG CHANGES
 BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Electrocardiography Review and the Normal EKG Response to Exercise
 Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
Electrophysiology Heart Study - EPS -
 Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
Septic Shock: Pharmacologic Agents for Hemodynamic Support. Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident
 Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
