MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES. Source: ACLS Provider Manual. American Heart Association. 2001, Updated 2003.
|
|
|
- Sheila Richard
- 7 years ago
- Views:
Transcription
1 MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, Updated
2 ET Administration Atropine o First drug for symptomatic sinus bradycardia o May be beneficial in presence of AV block at the nodal level or ventricular asystole; will not be effective when infranodal block is suspected o Second drug (after epinephrine or vasopressin) for asystole or bradycardic pulseless electrical activity o Parasympathetic agent o Enhances both sinus node automaticity and AV conduction by direct vagolytic action o Use with caution in presence of myocardial ischemia and hypoxia; increases myocardial oxygen demand o Avoid in hypothermic bradycardia o Not effective for infranodal AV block and new third-degree block with wide QRS complexes Asystole or pulseless electrical activity o 1mg IVP o Repeat every 3-5 minutes as needed to a maximum dose of mg/kg Bradycardia o 0.5-1mg IV every 3-5 minutes as needed; not to exceed total dose of 0.04mg/kg o Use shorter dosing interval (3 minutes) and higher doses (0.04mg/kg) in severe clinical conditions Tracheal administration o 2-3mg diluted in 10ml NS 2
3 Epinephrine o Cardiac arrest: VF, pulseless, VT, asystole, PEA o Symptomatic bradycardia after atropine, dopamine, and transcutaneous pacing o Severe hypotension o Anaphylaxis or severe allergic reactions in combination with large fluid volumes, corticosteroids, antihistamines o Natural catecholamine with α- and β-adrenergic agonist activity which results in (a) increased blood flow to heart and brain, (b)increased SVR, SBP, DBP, and (c) increased myocardial oxygen requirements. Its primary benefit is α- vasoconstriction o Myocardial ischemia, angina, and increased myocardial oxygen demand may result from raising blood pressure and increasing heart rate o High doses may contribute to postresuscitation myocardial dysfunction o Higher doses may be required to treat poison/drug-induced shock Cardiac arrest o IV dose: 1mg (10ml of 1:10,000 solution) every 3-5 minutes during resuscitation with each dose followed by 20ml IV flush o Higher dose: Up to 0.2mg/kg may be use if 1mg dose fails o Continuous infusion: Add 30mg epinephrine (30ml of 1:1000 solution) to 250ml NS or D 5 W to run at 100ml/hr and titrate to response o Tracheal Route: 2-2.5mg diluted in 10ml NS Profound bradycardia or hypotension 2-10 mcg/min infusion; add 1mg of 1:1000 to 500ml NS and infuse at 1-5ml/min 3
4 Lidocaine o Cardiac arrest from VF/VT o Stable VT, wide-complex tachycardias of uncertain type, wide complex PSVT o Affects fast sodium channels, shortens refractory periods, and suppresses spontaneous depolarization o Local anesthetic which increases the fibrillation threshold. o Causes suppression of ventricular ectopy post MI. o Not recommended for prophylactic use in AMI o Reduce maintenance dose but not loading dose in presence of impaired liver function or left ventricular dysfunction o If signs of toxicity develop, discontinue infusion immediately Cardiac arrest from VF/VT o Initial dose of 1-1.5mg/kg IV o For refractory VF may give additional mg/kg IVP; can repeat in 5-10 minutes for a maximum total dose of 3mg/kg o A single dose of 1.5mg/kg IV in cardiac arrest is acceptable o Tracheal administration: 2-4mg/kg Perfusing arrhythmia: stable VT, wide complex tachycardia of uncertain type, significant ectopy o 1-1.5mg/kg IVP o Repeat mg/kg every 5-10 minutes for a maximum total dose of 3mg/kg Maintenance infusion o Use premixed bag of 2grams/250ml D 5 W o 1-4mg/minute (30-50 mcg/kg/minute). 4
5 Naloxone o Respiratory and neurologic depression due to opiate intoxication unresponsive to oxygen and hyperventilation o Competes with and replaces narcotic agonists at the narcotic receptor sites o May cause opiate withdrawal o May need to repeat dose(s) as effects may not outlast effects of narcotics; monitor for recurrent respiratory depression o Rare anaphylactic reactions have been reported o 0.4-2mg every 2 minutes o Higher doses used for complete narcotic reversal o Can administer up to 10mg over < 10 minutes o In suspected opiate-addicted patients, titrate until ventilations adequate with 0.2mg every 2 minutes X3 doses, then 1.4mg IVP o Endotracheal dose: mg 5
6 IVPB Administration Amiodarone o A wide variety of atrial and ventricular tachyarrhythmias o For rate control of rapid atrial arrhythmias in patients with impaired LV function when digoxin ineffective o Class III antiarrhythmic agent which inhibits adrenergic stimulation and prolongs the action potential and refractory period in myocardial tissue o Decreases AV conduction and sinus node function o May produce vasodilation and hypotension o May have negative inotropic effects o May prolong QT interval Cardiac arrest o 300mg IVP diluted in 20-30ml D 5 W o Consider additional 150mg IVP in 3-5 minutes o Maximum cumulative dose 2.2gm/24 hours IV Wide-complex tachycardia (stable) o Rapid infusion: 150mg IV over first 10 minutes (15mg/min); may repeat rapid infusion (150mg IV) every 10 minutes as needed o Slow infusion: 360mg IV over 6 hours (1mg/min) o Maintenance infusion: 540mg IV over 18 hours (0.5mg/min) o Preparation: 150mg amiodarone in 150ml D 5 W; expires 2 hours from time of preparation o Maximum cumulative dose 2.2gm/24 hours IV 6
7 Dopamine o Second drug for symptomatic bradycardia (after atropine) o Hypotension (SBP mmhg) with signs and symptoms of shock o Norepinephrine precursor that stimulates dopamine, β-, and α-adrenergic receptors (dose dependent) o Use in patients with hypovolemia only after volume replacement o Caution in cardiogenic shock with accompanying congestive heart failure o May cause tachyarrhythmias, excessive vasoconstriction o Taper slowly o Do not mix with sodium bicarbonate o Use as a premixed bag of 400mg/250ml D5W or put 400mg in 250ml NS; titrate to patient response Low dose o 1-5 mcg/kg/min continuous infusion Moderate dose (cardiac doses) o 5-10 mcg/kg/min continuous infusion High dose (vasopressor doses) o mcg/kg/min 7
8 Epinephrine o Cardiac arrest: VF, pulseless, VT, asystole, PEA o Symptomatic bradycardia after atropine, dopamine, and transcutaneous pacing o Severe hypotension o Anaphylaxis or severe allergic reactions in combination with large fluid volumes, corticosteroids, antihistamines o Natural catecholamine with α- and β-adrenergic agonist activity which results in (a) increased blood flow to heart and brain, (b)increased SVR, SBP, DBP, and (c) increased myocardial oxygen requirements o Primary benefit is α-vasoconstriction o Myocardial ischemia, angina, and increased myocardial oxygen demand may result from raising blood pressure and increasing heart rate o High doses may contribute to postresuscitation myocardial dysfunction o Higher doses may be required to treat poison/drug-induced shock Cardiac arrest o IV dose: 1mg (10ml of 1:10,000 solution) every 3-5 minutes during resuscitation with each dose followed by 20ml IV flush o Higher dose: Up to 0.2mg/kg may be use if 1mg dose fails o Continuous infusion: Add 30mg epinephrine (30ml of 1:1000 solution) to 250ml NS or D 5 W to run at 100ml/hr and titrate to response o Tracheal Route: 2-2.5mg diluted in 10ml NS Profound bradycardia or hypotension o 2-10 mcg/min infusion; add 1mg of 1:1000 to 500ml NS and infuse at 1-5ml/min 8
9 Isoproterenol o Use with caution as temporizing measure if external pacer is not available for treatment of symptomatic bradycardia o Refractory torsades de pointes unresponsive to magnesium sulfate o Temporary control of bradycardia in heart transplant patients when denervated heart unresponsive to atropine o Poisoning from beta-adrenergic blockers o Synthetic sympathomimetic amine with pure β-adrenergic activity plus inotropic and chrontropic activity which can (a) increase HR/CO, contractility and (b) decrease MAP secondary to vasodilation o Do not use for treatment of cardiac arrest o Can increase myocardial oxygen requirements which may increase myocardial ischemia o Do not give with epinephrine (can cause VF/VT) o Do not administer to patents with poison/drug induced shock except for beta-adrenergic blocker poisoning o Mix 1mg in 250ml NS, LR, or D 5 W o Infuse at 2-10 mcg/min o Titrate to adequate heart rate o In torsades de pointes, titrate to increase heart rate until VT is suppressed 9
10 Lidocaine o Cardiac arrest from VF/VT o Stable VT, wide-complex tachycardias of uncertain type, wide complex PSVT o Affects fast sodium channels, shortens refractory periods, and suppresses spontaneous depolarization o Local anesthetic which increases the fibrillation threshold o Causes suppression of ventricular ectopy post MI o Not recommended for prophylactic use in AMI o Reduce maintenance dose but not loading dose in presence of impaired liver function or left ventricular dysfunction o If signs of toxicity develop, discontinue infusion immediately Cardiac arrest from VF/VT o Initial dose of 1-1.5mg/kg IV o For refractory VF may give additional mg/kg IVP; can repeat in 5-10 minutes for a maximum total dose of 3mg/kg o A single dose of 1.5mg/kg IV in cardiac arrest is acceptable o Tracheal administration: 2-4mg/kg Perfusing arrhythmia: stable VT, wide complex tachycardia of uncertain type, significant ectopy o 1-1.5mg/kg IVP o Repeat mg/kg every 5-10 minutes for a maximum total dose of 3mg/kg Maintenance infusion o Use premixed bag of 2grams/250ml D 5 W o 1-4mg/minute (30-50 mcg/kg/minute) 10
11 Norepinephrine o Severe cardiogenic shock and hemodynamically significant hypotension (SBP <70 mmhg) with low total peripheral resistance o Agent of last resort for management of ischemic heart disease and shock o Causes α- and β-adrenergic stimulation to increase contractility, HR, and vasoconstriction which improves coronary blood flow o Increases myocardial oxygen requirements because it raises blood pressure and heart rate o Use with caution in patients with acute ischemia as may induce arrhythmias; monitor cardiac output o Extravasation causes tissue necrosis o If extravasation occurs, administer phentolamine 5-10mg in 10-15ml saline solution and infiltrate into area o Dilute 4mg in 250ml D 5 W or D 5 NS; avoid dilution in NS alone o mcg/minute titrated up to a maximum dose of 30 mcg/min to improve blood pressure o Do not administer in same IV line as alkaline solutions o Poison/drug induced hypotension may require higher doses to achieve adequate perfusion 11
12 Procainamide o PSVT uncontrolled by adenosine and vagal maneuvers as long as blood pressure stable o Stable wide-complex tachycardia of unknown origin o AF with rapid rate in Wolff-Parkinson-White syndrome o Decreases myocardial excitability and conduction velocity o May depress myocardial contractility by increasing the electrical stimulation threshold of ventricle, HIS-Purkinje system, and through direct cardiac effects o Reduce maximum total dose to 12mg/kg and maintenance infusion to 1-2mg/min if cardiac or renal dysfunction o Proarrhythmic especially if AMI, hypokalemia, or hypomagnesemia o If impaired LV function, may induce hypotension o Use with caution with other drugs that prolong QT interval such as amiodarone or sotalol Recurrent VF/VT o 20mg/min IV infusion; maximum total dose 17mg/kg o Up to 50mg/min may be administered to total dose of 17mg/kg in urgent situations Other indications o 20mg/min IV infusion until one of the following occur: arrhythmia suppression, hypotension, QRS widens by >50%, or total dose of 17mg/kg is given Maintenance Infusion o Make infusion as 1 gram in 250ml D5W for concentration of 4mg/ml o 1-4mg/min 12
13 IVP Administration Adenosine o Drug of first choice for most forms of narrow-complex PSVT o Effective in terminating arrhythmias due to reentry involving the AV node or sinus node o Does not convert AF, AFl, or VT o Slows AV conduction and can interrupt AV nodal reentry pathways o Side effects including flushing, CP or tightness, brief periods of asystole or bradycardia, or ventricular ectopy usually transient. o Transient periods of sinus bradycardia and ventricular ectopy are common after termination of SVT o Avoid in patients receiving dipyridamole o Less effective in patients taking theophylline o Contraindicated in poison/drug-induced tachycardia o Initial bolus of 6mg IVP over 1-3 seconds, followed immediately with 20ml NS flush, then elevate the extremity o If needed, repeat with dose of 12mg after 1-2 minutes o If needed, a third dose of 12mg may be given after 1-2 minutes. 13
14 Amiodarone o A wide variety of atrial and ventricular tachyarrhythmias o For rate control of rapid atrial arrhythmias in patients with impaired LV function when digoxin ineffective o Class III antiarrhythmic agent which inhibits adrenergic stimulation and prolongs the action potential and refractory period in myocardial tissue o Decreases AV conduction and sinus node function o May produce vasodilation and hypotension o May have negative inotropic effects o May prolong QT interval Cardiac arrest o 300mg IVP diluted in 20-30ml D 5 W o Consider additional 150mg IVP in 3-5 minutes o Maximum cumulative dose 2.2gm/24 hours IV Wide-complex tachycardia (stable) o Rapid infusion: 150mg IV over first 10 minutes (15mg/min); may repeat rapid infusion (150mg IV) every 10 minutes as needed o Slow infusion: 360mg IV over 6 hours (1mg/min) o Maintenance infusion: 540mg IV over 18 hours (0.5mg/min) o Preparation: 150mg amiodarone in 150ml D 5 W; expires 2 hours from time of preparation o Maximum cumulative dose 2.2gm/24 hours IV 14
15 Atropine o First drug for symptomatic sinus bradycardia o May be beneficial in presence of AV block at the nodal level or ventricular asystole; will not be effective when infranodal block is suspected o Second drug (after epinephrine or vasopressin) for asystole or bradycardic pulseless electrical activity o Parasympathetic agent o Enhances both sinus node automaticity and AV conduction by direct vagolytic action o Use with caution in presence of myocardial ischemia and hypoxia; increases myocardial oxygen demand o Avoid in hypothermic bradycardia o Not effective for infranodal AV block and new third-degree block with wide QRS complexes Asystole or pulseless electrical activity o 1mg IVP o Repeat every 3-5 minutes as needed to a maximum dose of mg/kg Bradycardia o 0.5-1mg IV every 3-5 minutes as needed; not to exceed total dose of 0.04mg/kg o Use shorter dosing interval (3 minutes) and higher doses (0.04mg/kg) in severe clinical conditions Tracheal administration o 2-3mg diluted in 10ml NS 15
16 Calcium Chloride o Know or suspected hyperkalemia o Hypocalcemia o Antidote for toxic effects (hypotension and arrhythmias) from calcium channel blocker overdose of beta-adrenergic blocker overdose o Prophylactically before IV calcium channel blockers to prevent hypotension o Moderates nerve and muscle performance via action potential excitation threshold regulation o Do not use routinely in cardiac arrest o Do not mix with sodium bicarbonate. Hyperkalemia and calcium channel blocker overdose o 8-16mg/kg (usually 5-10ml) slow IVP o May be repeated as needed Prophylaxis before IV calcium channel blockers o 2-4mg/kg (usually 2ml) slow IVP 16
17 Dextrose o Reverse severe hypoglycemia; symptomatically may manifest as nausea, hunger, headache, irritability, lethargy, ataxia, mental confusion o Helps reverse the effect of too much insulin or insufficient food intake while on antidiabetic medications. o None in an acute emergency. o 10-50ml of Dextrose 50%. 17
18 Epinephrine o Cardiac arrest: VF, pulseless, VT, asystole, PEA o Symptomatic bradycardia after atropine, dopamine, and transcutaneous pacing o Severe hypotension o Anaphylaxis or severe allergic reactions in combination with large fluid volumes, corticosteroids, antihistamines o Natural catecholamine with α- and β-adrenergic agonist activity which results in (a) increased blood flow to heart and brain, (b)increased SVR, SBP, DBP, and (c) increased myocardial oxygen requirements. Its primary benefit is α- vasoconstriction o Myocardial ischemia, angina, and increased myocardial oxygen demand may result from raising blood pressure and increasing heart rate o High doses may contribute to postresuscitation myocardial dysfunction o Higher doses may be required to treat poison/drug-induced shock Cardiac arrest o IV dose: 1mg (10ml of 1:10,000 solution) every 3-5 minutes during resuscitation with each dose followed by 20ml IV flush o Higher dose: Up to 0.2mg/kg may be use if 1mg dose fails o Continuous infusion: Add 30mg epinephrine (30ml of 1:10,000 solution) to 250ml NS or D5W to run at 100ml/hr and titrate to response o Tracheal Route: 2-2.5mg diluted in 10ml NS Profound bradycardia or hypotension o 2-10 mcg/min infusion; add 1mg of 1:1000 to 400ml NS and infuse at 1-5ml/min 18
19 Lidocaine o Cardiac arrest from VF/VT o Stable VT, wide-complex tachycardias of uncertain type, wide complex PSVT o Affects fast sodium channels, shortens refractory periods, and suppresses spontaneous depolarization o A local anesthetic which increases the fibrillation threshold. o Causes suppression of ventricular ectopy post MI o Not recommended for prophylactic use in AMI o Reduce maintenance dose but not loading dose in presence of impaired liver function or left ventricular dysfunction o If signs of toxicity develop, discontinue infusion immediately Cardiac arrest from VF/VT o Initial dose of 1-1.5mg/kg IV o For refractory VF may give additional mg/kg IVP; can repeat in 5-10 minutes for a maximum total dose of 3mg/kg o A single dose of 1.5mg/kg IV in cardiac arrest is acceptable o Tracheal administration: 2-4mg/kg Perfusing arrhythmia: stable VT, wide complex tachycardia of uncertain type, significant ectopy o 1-1.5mg/kg IVP o Repeat mg/kg every 5-10 minutes for a maximum total dose of 3mg/kg Maintenance infusion o Use premixed bag of 2grams/250ml D 5 W o 1-4mg/minute (30-50 mcg/kg/minute) 19
20 Magnesium Sulfate o Cardiac arrest only if torsades de pointes or suspected hypomagnesemia o Refractory VF after lidocaine o Torsades de pointes with a pulse o Life-threatening ventricular arrhythmias due to digitalis toxicity o Not recommended for prophylactic administration in hospitalized patients with AMI. o Magnesium deficiency causes arrthymias o Magnesium facilitates repolarization by enhancing the intracellular potassium influx and dilating coronary arteries o Rapid administration may cause a fall in blood pressure o Use with caution if renal failure is present Cardiac arrest for hypomagnesemia or torsades de pointes o 1-2 grams (2-4ml of a 50% solution) diluted in 10ml of D 5 W IVP Torsades de pointes when not in cardiac arrest o Loading dose of 1-2 grams mixed in ml of D 5 W over 5-60 minutes IV o Follow with gm/hour IV titrating to control the torsades Acute myocardial infarction o Loading dose of 1-2 grams mixed in ml D 5 W over 5-60 minutes IV o Follow with gm/hr IV for up to 24 hours 20
21 Naloxone o Respiratory and neurologic depression due to opiate intoxication unresponsive to oxygen and hyperventilation o Competes with and replaces narcotic agonists at the narcotic receptor sites o May cause opiate withdrawal o May need to repeat dose(s) as effects may not outlast effects of narcotics; monitor for recurrent respiratory depression o Rare anaphylactic reactions have been reported o 0.4-2mg every 2 minutes o Higher doses used for complete narcotic reversal o Can administer up to 10mg over < 10 minutes o In suspected opiate-addicted patients, titrate until ventilations adequate with 0.2mg every 2 minutes X3 doses, then 1.4mg IVP o Endotracheal dose: mg 21
22 Sodium Bicarbonate o Known preexisting hyperkalemia o If known preexisting bicarbonate-responsive acidosis such as diabetic ketoacidosis o To alkalinize urine in case of aspirin, tricyclic antidepressant, cocaine, or diphenhydrmine overdose o If prolonged resuscitation with effective ventilation or upon return of spontaneous circulation after long arrest interval o Enhances a sodium shift intracellularly, buffers acidosis, decreases toxicity of tricyclic antidepressants, increases the clearance of acidic drugs o Adequate ventilation and CPR, not bicarbonate, are the major buffer agents in cardiac arrest o Not recommended for routine use in cardiac arrest patients o 1mEq/kg IV bolus o Repeat half this dose every 10 minutes o Use arterial blood gas analysis to guide bicarbonate therapy; an acute change in PaCO 2 of 1 mmhg is associated with an increase of decrease in ph of U 22
23 Vasopressin o Alternative pressor to epinephrine in the treatment of adult shock-refractory VF o May be useful for hemodynamic support in septic shock o Natural antidiuretic hormone which is a potent vasoconstrictor resulting in (a) increased BP and SVR and (b) decreased CO, HR, myocardial oxygen consumption and contractility o Increased peripheral vascular resistance may provoke cardiac ischemia and angina o Not recommended for responsive patients with coronary artery disease 40 units IVP X1. 23
24 Verapamil o Alternative drug, after adenosine, used to terminate PSVT with narrow QRS complex and adequate blood pressure and preserved LV function o May control ventricular response in patients with AF, AFl, or multifocal atrial tachycardia. o Blocks the flow of calcium and sodium and slows conduction o Terminates reentrant arrhythmias o Controls the ventricular response in AF/Afl; causes coronary vasodilation. o Give only to patients with narrow-complex PSVT or arrhythmias known to be of supraventricular origin o Avoid in patients with WPW and AF, SSS, or second- or third-degree AV block without pacemaker o May decrase myocardial contractility and mya exacerbate CHF in patients with LV dysfunction o Use with extreme caution in patients receiving oral betablockers o 2.5-5mg IVP over 2 minutes o Second dose: 5-10mg, if needed, in minutes for maximum dose of 20mg o Alternative: 5mg IVP every 15 minutes to total dose of 30mg o Administer over 3 minutes in older patients 24
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS
 Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Stimulates HR, BP, CO, and vasoconstriction. Stimulates renal, venous, mesenteric arterial. basic chart below) (alpha receptors) vasoconstriction
 Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Alabama Medications. Christopher J. Colvin January 2010
 Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
table of contents drug reference
 table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010!
 ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
Arrest. What s a Nurse to do?
 Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia
 Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
DIPHENHYDRAMINE (Benadryl)
 DIPHENHYDRAMINE (Benadryl) Classification: Antihistamine (H1 blocker) Antihistamine; appear to compete with histamine for cell receptor sites on effector cells. Therapeutic Relieves effects of histamine
DIPHENHYDRAMINE (Benadryl) Classification: Antihistamine (H1 blocker) Antihistamine; appear to compete with histamine for cell receptor sites on effector cells. Therapeutic Relieves effects of histamine
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com
 Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
IU Health ACLS Study Guide
 IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
PALS Interim Study Guide
 PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
Septic Shock: Pharmacologic Agents for Hemodynamic Support. Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident
 Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Dysrhythmia Assessment and Management Scenarios
 Dysrhythmia Assessment and Management Scenarios Authors: John Guerriero, EMT-P, Gene Iannuzzi, RN, CCRN, EMT-P, Arther Romano, EMT-P, Kevin Brown, MD, EMT-P 1 An Important Word About the Therapies Discussed
Dysrhythmia Assessment and Management Scenarios Authors: John Guerriero, EMT-P, Gene Iannuzzi, RN, CCRN, EMT-P, Arther Romano, EMT-P, Kevin Brown, MD, EMT-P 1 An Important Word About the Therapies Discussed
Vasopressors. Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco
 Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
PREPARATIONS: Adrenaline 1mg in 1ml (1:1000) Adrenaline 100micrograms in 1ml (1:10,000)
 ADRENALINE Acute hypotension Via a CENTRAL venous line Initially 100-300 nanograms/kg/minute 0.1-0.3 microgram/kg/minute adjusted according to response up to a maximum of 1.5 micrograms/kg/minute. Increase
ADRENALINE Acute hypotension Via a CENTRAL venous line Initially 100-300 nanograms/kg/minute 0.1-0.3 microgram/kg/minute adjusted according to response up to a maximum of 1.5 micrograms/kg/minute. Increase
ANZCOR Guideline 12.4 Medications and Fluids in Paediatric Advanced Life Support
 ANZCOR Guideline 12. Medications and Fluids in Paediatric Advanced Life Support Who does this guideline apply to? This guideline applies to infants and children. Summary Who is the audience for this guideline?
ANZCOR Guideline 12. Medications and Fluids in Paediatric Advanced Life Support Who does this guideline apply to? This guideline applies to infants and children. Summary Who is the audience for this guideline?
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
ACLS Drugs, Cardioversion, Defibrillation and Pacing
 A p p e n d i x 4 ACLS Drugs, Cardioversion, Defibrillation and Pacing Drug/Therapy / Adult Dosage ACE Inhibitors (Angiotensin- Converting Enzyme Inhibitors) Enalapril Captopril Lisinopril Ramipril ACE
A p p e n d i x 4 ACLS Drugs, Cardioversion, Defibrillation and Pacing Drug/Therapy / Adult Dosage ACE Inhibitors (Angiotensin- Converting Enzyme Inhibitors) Enalapril Captopril Lisinopril Ramipril ACE
Adrenergic agonists. R. A. Nimmi Dilsha Department of pharmacy Faculty of Health Sciences The Open University of Sri Lanka
 Adrenergic agonists R. A. Nimmi Dilsha Department of pharmacy Faculty of Health Sciences The Open University of Sri Lanka Outline Recall Introduction to adrenergic agonists Classification of adrenergic
Adrenergic agonists R. A. Nimmi Dilsha Department of pharmacy Faculty of Health Sciences The Open University of Sri Lanka Outline Recall Introduction to adrenergic agonists Classification of adrenergic
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) Pharmacist Objectives. Pharmacists in the ER. Background
 The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
Emergency Medical Programs. Common Drugs - Indications & Administration
 - Indications & Administration Table of Contents ACTIVATED CHARCOAL 3 ADENOSINE (Adenocard) 4 ALBUTEROL (Proventil, Ventolin) 5 AMIODARONE (Cordarone) 6 ASPIRIN 7 ATROPINE (Atropine, Component of Mark
- Indications & Administration Table of Contents ACTIVATED CHARCOAL 3 ADENOSINE (Adenocard) 4 ALBUTEROL (Proventil, Ventolin) 5 AMIODARONE (Cordarone) 6 ASPIRIN 7 ATROPINE (Atropine, Component of Mark
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Levophed Norepinephrine Bitartrate Injection, USP
 Levophed Norepinephrine Bitartrate Injection, USP R x only DESCRIPTION Norepinephrine (sometimes referred to as l-arterenol/levarterenol or l-norepinephrine) is a sympathomimetic amine which differs from
Levophed Norepinephrine Bitartrate Injection, USP R x only DESCRIPTION Norepinephrine (sometimes referred to as l-arterenol/levarterenol or l-norepinephrine) is a sympathomimetic amine which differs from
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins)
 Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Milwaukee School of Engineering Gerrits@msoe.edu. Case Study: Factors that Affect Blood Pressure Instructor Version
 Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Wilson County Emergency Management Agency Protocol Manual Protocols
 Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
OBJECTIVES. When the student has finished this module, he/she will be able to:
 Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
The management of cardiac arrest
 CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
Wide-Complex Tachycardias in the ED: Myths and Pitfalls
 Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Guideline for the management of arrhythmias
 Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
ACLS Rhythms for the ACLS Algorithms
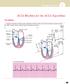 ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
Cardiovascular System & Its Diseases. Lecture #4 Heart Failure & Cardiac Arrhythmias
 Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Electrolyte Physiology. Something in the way she moves
 Electrolyte Physiology Something in the way she moves me Electrolyte Movement CONCENTRATION GRADIENT ELECTRICAL GRADIENT DRIVING FORCE NERNST NUMBER (E-ion) CONDUCTANCE (G-ion) PERMEABILITY CHANNELS: small
Electrolyte Physiology Something in the way she moves me Electrolyte Movement CONCENTRATION GRADIENT ELECTRICAL GRADIENT DRIVING FORCE NERNST NUMBER (E-ion) CONDUCTANCE (G-ion) PERMEABILITY CHANNELS: small
Paramedic Pediatric Medical Math Test
 Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Glucagon stimulates adenyl cyclase. Amrinone and milrinone inhibit phosphodiesteras e
 Beta-Adrenergic Blocker Poisoning John Gualtieri, PharmD Clinical Assistant Professor Dept. of Experimental and Clinical Pharmacology College of Pharmacy, Univ of Minnesota I. Objectives 1.) Described
Beta-Adrenergic Blocker Poisoning John Gualtieri, PharmD Clinical Assistant Professor Dept. of Experimental and Clinical Pharmacology College of Pharmacy, Univ of Minnesota I. Objectives 1.) Described
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
Team Leader. Ensures high-quality CPR at all times Assigns team member roles Ensures that team members perform well. Bradycardia Management
 ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
Pulseless Emergencies
 Pulseless Emergencies Nicole M. Acquisto, Pharm.D., BCPS Emergency Medicine Clinical Pharmacy Specialist University of Rochester Medical Center Nothing to disclose Disclosures Objectives Understand the
Pulseless Emergencies Nicole M. Acquisto, Pharm.D., BCPS Emergency Medicine Clinical Pharmacy Specialist University of Rochester Medical Center Nothing to disclose Disclosures Objectives Understand the
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
 ADRENALINE (EPINEPHRINE) ANAESTHESIA TUTORIAL OF THE WEEK 226 6 TH JUNE 2011 Prof. John Kinnear Southend University Hospital NHS Foundation Trust, UK Correspondence to John.Kinnear@southend.nhs.uk QUESTIONS
ADRENALINE (EPINEPHRINE) ANAESTHESIA TUTORIAL OF THE WEEK 226 6 TH JUNE 2011 Prof. John Kinnear Southend University Hospital NHS Foundation Trust, UK Correspondence to John.Kinnear@southend.nhs.uk QUESTIONS
GUIDELINE 11.5 MEDICATIONS IN ADULT CARDIAC ARREST
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.5 MEDICATIONS IN ADULT CARDIAC ARREST While the listed drugs have theoretical benefits in selected situations, no medication has been shown to improve long-term
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.5 MEDICATIONS IN ADULT CARDIAC ARREST While the listed drugs have theoretical benefits in selected situations, no medication has been shown to improve long-term
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
Paediatric Advanced Life Support
 Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Intravenous Infusions
 Intravenous Infusions 1 Intravenous Infusions This course will cover different types of common intravenous medication infusions including insulin, heparin, vasopressors, vasodilators, and anti-arrhythmics.
Intravenous Infusions 1 Intravenous Infusions This course will cover different types of common intravenous medication infusions including insulin, heparin, vasopressors, vasodilators, and anti-arrhythmics.
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
ADRENERGIC AND ANTI-ADRENERGIC DRUGS. Mr. D.Raju, M.pharm, Lecturer
 ADRENERGIC AND ANTI-ADRENERGIC DRUGS Mr. D.Raju, M.pharm, Lecturer SYMPATHETIC NERVOUS SYSTEM Fight or flight response results in: 1. Increased BP 2. Increased blood flow to brain, heart and skeletal muscles
ADRENERGIC AND ANTI-ADRENERGIC DRUGS Mr. D.Raju, M.pharm, Lecturer SYMPATHETIC NERVOUS SYSTEM Fight or flight response results in: 1. Increased BP 2. Increased blood flow to brain, heart and skeletal muscles
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
Critical Care/ Emergency Department Medication Competency Exam
 Employee name: Score: / = % Critical Care/ Emergency Department Medication Competency Exam Please circle or write in (where applicable) the correct answer for each question below. There is only 1 correct
Employee name: Score: / = % Critical Care/ Emergency Department Medication Competency Exam Please circle or write in (where applicable) the correct answer for each question below. There is only 1 correct
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
ADVANCED LIFE SUPPORT LEARNING PACKAGE
 SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
Interpretation of Laboratory Values
 Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Adrenergic, Adrenergic Blockers, Cholinergic and Cholinergic Blockers
 Adrenergic, Adrenergic Blockers, Cholinergic and Cholinergic Blockers Objective 1: Explain the difference between the sympathetic and parasympathetic nervous systems Autonomic Nervous System Sympathetic
Adrenergic, Adrenergic Blockers, Cholinergic and Cholinergic Blockers Objective 1: Explain the difference between the sympathetic and parasympathetic nervous systems Autonomic Nervous System Sympathetic
Chapter 2 Vasopressors and Inotropes
 Chapter 2 Vasopressors and Inotropes Scott W. Mueller and Robert MacLaren Introduction Medication errors and adverse drug events occur more frequently in the intensive care unit compared to general care
Chapter 2 Vasopressors and Inotropes Scott W. Mueller and Robert MacLaren Introduction Medication errors and adverse drug events occur more frequently in the intensive care unit compared to general care
ACLS PROTOCOLS. Chest Pain / Acute Coronary Syndrome... 4-2
 ACLS PROTOCOLS CHEST PAIN / ACLS Chest Pain / Acute Coronary Syndrome... 4-2 ARRHYTHMIAS / ACLS Sinus Bradycardia... 4-4 Narrow - Complex Tachycardia... 4-6 Wide - Complex Tachycardia... 4-8 CARDIAC ARREST
ACLS PROTOCOLS CHEST PAIN / ACLS Chest Pain / Acute Coronary Syndrome... 4-2 ARRHYTHMIAS / ACLS Sinus Bradycardia... 4-4 Narrow - Complex Tachycardia... 4-6 Wide - Complex Tachycardia... 4-8 CARDIAC ARREST
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
ACID- BASE and ELECTROLYTE BALANCE. MGHS School of EMT-Paramedic Program 2011
 ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
Essential facts for med-surg nurses
 Emergency cardiac drugs: Essential facts for med-surg nurses Emergencies on a med-surg unit can be daunting. By Ira Gene Reynolds, MSNEd, RN, PCCN-CMC IN THE HOSPITAL SETTING, emergencies typically occur
Emergency cardiac drugs: Essential facts for med-surg nurses Emergencies on a med-surg unit can be daunting. By Ira Gene Reynolds, MSNEd, RN, PCCN-CMC IN THE HOSPITAL SETTING, emergencies typically occur
!!! BOLUS DOSE IV. Use 5-10 mcg IV boluses STD ADRENALINE INFUSION. Use IM adrenaline in advance of IV dosing!
 ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
10. An infant with a history of vomiting and diarrhea arrives by ambulance. During your primary assessment the infant responds only to painful stimula
 1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials
 Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
Upstate University Health System Medication Exam - Version A
 Upstate University Health System Medication Exam - Version A Name: ID Number: Date: Unit: Directions: Please read each question below. Choose the best response for each of the Multiple Choice and Medication
Upstate University Health System Medication Exam - Version A Name: ID Number: Date: Unit: Directions: Please read each question below. Choose the best response for each of the Multiple Choice and Medication
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education November 2014 Hypothermia in Adults
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education November 2014 Hypothermia in Adults Death from exposure and accidental hypothermia occurs throughout the world
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education November 2014 Hypothermia in Adults Death from exposure and accidental hypothermia occurs throughout the world
Cardiopulmonary arrest (CPA) is defined as cessation of
 1 CE Credit Cardiopulmonary Resuscitation: Administering Fluids, Oxygen, and Drugs Amy N. Breton, CVT, VTS (ECC) Veterinary Emergency and Specialty Center of New England Waltham, Massachusetts This article
1 CE Credit Cardiopulmonary Resuscitation: Administering Fluids, Oxygen, and Drugs Amy N. Breton, CVT, VTS (ECC) Veterinary Emergency and Specialty Center of New England Waltham, Massachusetts This article
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
