ACLS PROTOCOLS. Chest Pain / Acute Coronary Syndrome
|
|
|
- Linda Montgomery
- 10 years ago
- Views:
Transcription
1 ACLS PROTOCOLS CHEST PAIN / ACLS Chest Pain / Acute Coronary Syndrome ARRHYTHMIAS / ACLS Sinus Bradycardia Narrow - Complex Tachycardia Wide - Complex Tachycardia CARDIAC ARREST / ACLS Cardiac Arrest Asystole / Pulseless Electrical Activity (PEA) Ventricular Fibrillation (V-FIB) / Pulseless Ventricular Tachycardia (V-Tach) Post - Resuscitation Cardiac Care Induced Hypothermia Left Ventricular Assist Device (LVAD)
2 UNIVERSAL PATIENT CARE PROTOCOL CHEST PAIN / ACLS CHEST PAIN / ACUTE CORONARY SYNDROME Patient has Chest Pain that is possibly cardiac in nature / Hx OXYGEN to maintain SpO2 >94 >95% = 4 L NC, <95% = 15 L NRB Obtain 12 lead and transmit B EMT B A Advanced A M MED CONTROL M If arrhythmia exists go to appropriate Arrhythmia Protocol Evaluate 12 Lead EKG (If Positive for ST Elevation Activate Cath Lab) (If Left Bundle Branch Block with symptoms Activate Cath Lab) IV/IO PROTOCOL ASPIRIN 324 mg/ 325 mg PO NITROGLYCERIN 0.4 mg SL/Spray (If BP > 100 Systolic with IV - may give total of 3 1 q 5 min) (EMT, Pt Assisted with Med Control) If ST segment changes are found in Leads ll, lll and AVF (inferior wall) conduct a right side 12 lead EKG. Move V4 to right side of chest on the midclavicular line <same location as on the left> and run 12 lead again. Label 12 lead as "right side" look to V4 in the right side 12 lead for ST segment changes and notify ER. Do not delay transport while obtaining RV4 12 Lead (If there is ST Elevation in RV4 DO NOT give Nitroglycerin, Beta Blocker, or Morphine) DO NOT give Nitroglycerin if patient has taken a Phosphodiesterase Inhibitors (ED enhancement drugs within hours) MORPHINE SULFATE 2 4 mg Slow IV/IO/IM/IN q5 min (Max = 10 mg if no relief with a total of 3 NTG) Give Zofran 4mg IV/IO/IM for nausea Zofran Oral Disolving Tabs 8 mg Oral Confirmed STEMI on 12 Lead Brilinta 180 mg PO **If Brilinta is not available - Plavix 600 mg PO** Heparin 60units/kg max dose of 4000units IV Reassess and Monitor CONTACT MEDICAL CONTROL TRANSPORT Consider Transport to a Facility With PCI Capabilities if Patient is Showing Signs of a ST Elevation MI 2
3 CHEST PAIN / ACLS CHEST PAIN / ACUTE CORONARY SYNDROME HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Age Medications Past medical history (MI, Angina, Diabetes) Allergies Recent physical exertion Onset Palliation / Provocation Quality (crampy, constant, sharp, dull, etc.) Region / Radiation / Referred Severity (0-10) Time (duration / repetition) CP (pain, pressure, aching, vice like tightness) Location (substernal, epigastric, arm, jaw, neck, shoulder) Radiation of pain Pale, diaphoresis Shortness of breath Nausea, vomiting, dizziness Trauma vs. Medical Angina vs. Myocardial infarction Pericarditis Pulmonary embolism Asthma / COPD Pneumothorax Aortic dissection or aneurysm GE reflux or hiatal hernia Esophageal spasm Chest wall injury or pain Pleural pain KEY POINTS All cardiac chest pain patients must have an IV, O2 and monitor. Exam: Mental Status, Skin, Neck, Lung, Heart, Abdomen, Back, Extremities, Neuro. If patient has taken nitroglycerin without relief, consider potency of the medication. If positive ECG changes, establish a second IV while en route to the hospital. Monitor for hypotension after administration of nitroglycerin and morphine. Nitroglycerin and Morphine may be repeated per dosing guidelines in Appendix 1:Medications. Diabetics, women and geriatric patients often have atypical pain, or generalized complaints. Refer to the Sinus Bradycardia Protocol if indicated (HR < 60 bpm) or Wide & Narrow Complex Tachycardia Protocol (HR > 150 bpm) and hypotension. If the patient becomes hypotensive from Nitroglycerin administration, place the patient in the Trendelenburg position and administer a 250 ml Normal Saline bolus. Be prepared to administer Naloxone (Narcan) if the patient experiences respiratory depression or hypotension due to Morphine administration. If pulmonary edema is present, refer to the PULMONARY EDEMA/CHF PROTOCOL. Be suspicious of a Silent MI in the elderly, diabetics, and women. Consider other causes of chest pain such as aortic aneurysm, pericarditis, and pulmonary embolism. Aspirin can be administered to a patient on Coumadin unless the patient s physician has advised them otherwise. If the patient took a dose of Aspirin that was less than 325 mg in the last 24 hours, then additional Aspirin can be administered to achieve a therapeutic dose of 325 mg. DO NOT administer Nitroglycerin to a patient who took an erectile dysfunction medication (Viagra, Cialis, Levitra, etc) within the last hours due to potential for severe hypotension. Nitroglycerin can be administered to a patient by EMS if the patient has already taken 3 of their own prior to your arrival. Document it if the patient had any changes in their symptoms or a headache after taking their own Nitroglycerin. Check and document the expiration date of the patient s prescribed Nitroglycerin. Nitroglycerin can be administered to a hypertensive patient complaining of chest discomfort without Medical Direction permission. Nitroglycerin can be administered without an IV as long as the patient takes Nitroglycerin at home and has a BP greater than120 mmhg. All patients complaining chest discomfort must be administered at least 4 lpm of oxygen by nasal cannula. Administer oxygen by non-rebreather or assist the patient s ventilations as indicated. 3
4 ARRHYTHMIAS / ACLS SINUS BRADYCARDIA UNIVERSAL PATIENT CARE PROTOCOL B EMT B A Advanced A M MED CONTROL M Apply Cardiac Monitor / Obtain 12 lead EKG and transmit IV/IO PROTOCOL Evaluate 12 Lead EKG (Look for ST Elevation) Hypotension, AMS, Chest Pain, Shock Blood Pressure < 90 Systolic No Monitor and Reassess Yes ATROPINE IV/IO 0.5 mg (max 3mg) Repeat every 3-5 minutes Use with Coution if type II 2 nd or 3 rd degree heart block EXTERNAL TRANSCUTANEOUS PACING Start at 10 over the intrinsic rate and adjust for BP > 90 Consider DOPAMINE 2-10 mcg/kg/min Iv/IO Titrate to HR > 60 & BP > 90 systolic Dopamine Simple calculation for approx 5 mcg/kg/min (must be 1600 mcg/ml concentration) *Take the Patients weight in lbs and remove the last digit (175lbs = 17) * Subtract 2 from that figure (17-2=15) *This gives you the number of drops per min using a 60gtts set. (titrate to desired effect) Example: 175lbs patient. 175 remove the 5 is = 15 drops per min (approx 5 mcg/kg/min) CONTACT MEDICAL CONTROL TRANSPORT 4
5 ARRHYTHMIAS / ACLS SINUS BRADYCARDIA HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Past medical history Medications Beta-Blockers Calcium channel blockers Clonidine Digitalis Pacemaker HR < 60/min Chest pain Respiratory distress Hypotension or Shock Altered mental status Syncope Acute myocardial infarction Hypoxia Hypothermia Sinus bradycardia Head injury (elevated ICP) or Stroke Spinal cord lesion Sick sinus syndrome AV blocks (1, 2, or 3 ) KEY POINTS Exam: Mental Status, Neck, Skin, Lungs, Heart, Abdomen, Extremities, Neuro. Pharmacological treatment of bradycardia is based upon the presence or absence of hypotension. If hypotension exists, treat. If blood pressure is adequate, monitor only. Use Atropine with caution, if the patient s rhythm is a Type II second-degree heart block or a third degree heart block. Transcutaneous pacing is the treatment of choice for Type II second-degree heart blocks and third degree heart blocks. If the patient is critical and an IV is not established, initiate pacing with Medical Direction permission. If the patient converts to another rhythm, refer to the appropriate protocol and treat accordingly. 5
6 ARRHYTHMIAS / ACLS NARROW COMPLEX TACHYCARDIA If <150 bpm Consider Sinus Tachycardia Look for and treat reversible causes H s & T s UNIVERSAL PATIENT CARE PROTOCOL Cardiac Monitor IV/IO PROTOCOL >150 bpm Stable B EMT B A Advanced A M MED CONTROL M Unstable Vagal Maneuvers Attempt Stable Procedures or you may go directly to Cardioversion ADENOSINE 6 mg IV/IO followed by 20mL N/S flush Consider Sedation with Cardioversion Ativan 1-2 mg IV/IO/IN or Versed 2 mg IV/IO/IN if Ativan is unavailable No Response ADENOSINE 12 mg IV/IO followed by 20 ml N/S flush CARDIOVERSION Synchronized Biphasic: 100J 200J 300J 360J Or manufacturer s recommendations No response No Response Repeat CARDIOVERSION Synchronized Monitor and Reassess Metoprolol 5 mg IV/IO if HR> 60 and B/P > 110 systolic May Repeat in 3 minutes if B/P>110 + HR>60 If rhythm changes, Go to Appropriate Protocol CONTACT MEDICAL CONTROL TRANSPORT 6
7 ARRHYTHMIAS / ACLS NARROW COMPLEX TACHYCARDIA HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Medications (Aminophylline, diet pills, thyroid supplements, decongestants, Digoxin) Diet (caffeine, chocolate) Drugs (nicotine, cocaine) Past medical history History of palpitations / heart racing Syncope / near syncope HR > 150/Min QRS < 0.12 Sec Dizziness, CP, SOB Potential presenting rhythm Sinus tachycardia PSVT Atrial fibrillation / flutter Multifocal atrial tachycardia Heart disease (WPW, Valvular) Sick sinus syndrome Myocardial infarction Electrolyte imbalance Exertion, Pain, Emotional stress Fever Hypoxia Hypovolemia or anemia Drug effect / Overdose Hyperthyroidism Pulmonary embolus KEY POINTS Exam: Mental Status, Skin, Neck, Lung, Heart, Abdomen, Back, Extremities, Neuro Adenosine may not be effective in identifiable atrial flutter/fibrillation, but is not harmful. Monitor for respiratory depression and hypotension associated with Versed. Continuous pulse oximetry is required for all patients. Document all rhythm changes with monitor strips and obtain monitor strips with each therapeutic intervention. If the patient converts to another rhythm, refer to the appropriate protocol and treat accordingly. Examples of vagal maneuvers include bearing down, coughing, or blowing into a syringe. DO NOT perform a carotid massage. If possible, the IV should be initiated in either the left or right AC. When administering Adenosine follow the bolus with 20 ml rapid bolus of normal saline. Record EKG strips during Adenosine administration. Perform a 12-Lead EKG prior to and after Adenosine conversion or cardioversion of SVT. If the patient converts into ventricular fibrillation or pulseless ventricular tachycardia immediately DEFIBRILLATE the patient and refer to the appropriate protocol and treat accordingly. Give a copy of the EKGs and code summaries to the receiving facility upon arrival. 7
8 ARRHYTHMIAS / ACLS WIDE COMPLEX TACHYCARDIA V-Fib Pulseless V-Tach Protocol UNIVERSAL PATIENT CARE PROTOCOL No Palpate Pulse Yes B EMT B A Advanced A M MED CONTROL M Apply Cardiac Monitor IV/IO PROTOCOL Stable Polymorphic Unstable Versed 2 mg IV/IO Regular / Monomorphic Consider Adenosine 6mg IV/IO May Consider additional Adenosine 12mg IV/IO Prepare for immediate Cardioversion If V-Tach or uncertain rhythm AMIODARONE 150 mg IV/IO (Over 10 minutes) Consider Sedation with Cardioversion Ativan 1-2 mg IV/IO/IN or Versed 2 mg IV/IO/IN if Ativan is unavailable Monitor and obtain 12-lead EKG Transmit to ED Paramedics Reassess for underlying rhythm Consider Synchronized Cardioversion with sedation If (Polymorphic VT) torsades de pointes Consider Magnesium grams IV/IO Over 5 min Synchronized CARDIOVERSION Biphasic: 100J 200J 300J 360J Or manufacturer s recommendations (If Polymorphic 200J) AMIODARONE 150 mg IV/IO (Over 10 minutes) For Polymorphic Consider Magnesium Sulfate If V-Tach or uncertain rhythm AMIODARONE 150 mg IV/IO (Over 10 minutes) CONTACT MEDICAL CONTROL TRANSPORT 8
9 ARRHYTHMIAS / ACLS WIDE COMPLEX TACHYCARDIA HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Past medical history Medications, diet, drugs Syncope / near-syncope Palpitations Pacemaker Allergies Ventricular tachycardia on ECG (Runs or sustained) Conscious Rapid pulse Chest pain Shortness of breath Dizziness Rate usually bpm for sustained V-Tach Artifact / device failure Cardiac Endocrine / Metabolic Drugs Pulmonary KEY POINTS Exam: Mental Status, Skin, Neck, Lung, Heart, Abdomen, Back, Extremities, Neuro. For witnessed / monitored ventricular tachycardia, try having patient cough or deliver a precordial thump. Polymorphic V-Tach (Torsades de Pointes) may benefit from the administration of magnesium sulfate and may require non-sync cardioversion. If the patient converts to another rhythm, refer to the appropriate protocol and treat accordingly. If the patient relapses back into wide complex tachycardia / ventricular tachycardia, initiate synchronized cardioversion with the joules setting that previously cardioverted the patient. Record EKG strips during Amiodarone administration. Perform a Code Summary and attach it to the patient run report. Be sure to treat the patient and not the monitor. 9
10 CARDIAC ARREST / ACLS CARDIAC ARREST Withhold Resuscitation Follow Local County Coroner Procedures Yes UNIVERSAL PATIENT CARE PROTOCOL Criteria for Death Criteria for DNR Start CPR B EMT B A Advanced A M MED CONTROL M Yes Review DNR Comfort Care Guidelines CONTACT MEDICAL CONTROL Attach Cardiac Monitor Defibrillator/ AED Go to Appropriate Protocol Follow AED Prompts (if applicable) If V-Fib is witnessed by EMS Immediately Dfibrillate CPR x 5 cycles / 2 minutes Airway Protocol Consider: Termination of Resuscitation Efforts Protocol Follow AED Prompts (if applicable) Maintain CPR / Airway IV/IO PROTOCOL CONTACT MEDICAL CONTROL TRANSPORT AT ANY TIME Return of Spontaneous Circulation GO TO POST RESUSCITATION CARDIAC CARE PROTOCOL 10
11 CARDIAC ARREST / ACLS CARDIAC ARREST HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Events leading to arrest Estimated down time Past medical history Medications Existence of terminal illness DNR or Living Will Unresponsive Apneic Pulseless Signs of lividity, rigor mortis Medical vs Trauma V-fib vs Pulseless V-tach Asystole Pulseless electrical activity (PEA) KEY POINTS Exam: Mental Status, Neck, Skin, Lungs, Heart, Abdomen, Extremities, Neuro. Success is based on proper planning and execution. Procedures require space and patient access. Make room to work. If witnessed arrest consider a precordial thump. Reassess airway frequently and with every patient move. Maternal Arrest - Treat mother per appropriate protocol with immediate notification to Medical Control and rapid transport. If the patient converts to another rhythm, refer to the appropriate protocol and treat accordingly. Attempt to obtain patient history from family members or bystanders. Estimated down time Medical history Complaints prior to arrest Bystander CPR prior to EMS arrival AED use prior to EMS arrival Administer Dextrose only if the patient has a Glucose Level < 70 mg/dl. Dextrose should be administered as soon a hypoglycemia is determined. DO NOT administer Narcan until the patient has been resuscitated and is known or suspected to have used narcotics. Reassess the patient if the interventions do not produce any changes. If indicated, refer to the Termination of Resuscitative Efforts Protocol. 11
12 CARDIAC ARREST / ACLS ASYSTOLE / PULSELESS ELECTRICAL ACTIVITY (PEA) Withhold Resuscitation Follow Local County Coroner Procedures Yes UNIVERSAL PATIENT CARE PROTOCOL Criteria for Death Criteria for DNR Start CPR B EMT B A Advanced A M MED CONTROL M Yes Review DNR Comfort Care Guidelines CONTACT MEDICAL CONTROL Airway Protocol IV/ IO PROTOCOL Apply Cardiac Monitor (AED) ASYSTOLE/PULSELESS ELECTRICAL ACTIVITY (PEA) Resume CPR for 5 cycles End Stage Renal Pt. Consider: Calcium Chloride 1 gram (10cc) slow IVP & Sodium Bicarbonate 50mEq or 1mEq/kg IVP DO NOT MIX IN SAME IV LINE EPINEPHRINE 1 mg IV / IO 1:10,000 Solution Repeat every 3-5 minutes Or VASOPRESSIN 40 U IV / IO Give ONE Dose AT ANY TIME Consider: Termination of Resuscitation Efforts CONTACT MEDICAL CONTROL TRANSPORT Return of Spontaneous Circulation GO TO POST RESUSCITATION CARDIAC CARE PROTOCOL 12
13 CARDIAC ARREST / ACLS ASYSTOLE / PULSELESS ELECTRICAL ACTIVITY (PEA) HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Past medical history Medications Tricyclics Digitalis Beta blockers Calcium channel blockers Events leading to arrest End stage renal disease Estimated down time Suspected hypothermia Suspected overdose DNR or Living Will Pulseless Apneic No electrical activity on ECG Cyanosis Medical or Trauma Hypoxia Potassium (hypo / hyper) Acidosis Hypothermia Device (lead) error Death Hypovolemia Cardiac tamponade Drug overdose (Tricyclics, Digitalis, Beta blockers, Calcium channel blockers) Massive Myocardial infarction Tension pneumothorax Pulmonary embolus Hypovolemia Hypoxia Hydrogen ion (acidosis) Hypo-hyperkalemia Hypoglycemia Hypothermia CONSIDER TREATABLE CAUSES Tamponade, cardiac Tension Pneumothorax Thrombosis (coronary or pulmonary ACS or PE) Trauma Toxins KEY POINTS Exam: Mental Status, Neck, Skin, Lungs, Heart, Abdomen, Extremities, Neuro. Always confirm asystole in more than one lead. Consider each possible cause listed in the differential: Survival is based on identifying and correcting the cause! Discussion with Medical Control can be a valuable tool in developing a differential diagnosis and identifying possible treatment options. Early identification and treatment of reversible causes of PEA increases the chance of a successful outcome. If the patient converts to another rhythm, refer to the appropriate protocol and treat accordingly. Consider volume infusion for all patients in PEA. Be alert for fluid overload. Vasopressin is not repeated. If given, Epinephrine may be used 5 minutes after Vasopressin if still in arrest, 1mg of Epinephrine 1:10,000 would then be administered every 3-5 minutes. Treat as ventricular fibrillation if you cannot differentiate between asystole and fine ventricular fibrillation. Medical Direction must be contacted prior to administering antidotes for all poisonings/overdoses except for narcotic overdoses. Dextrose 50% should only be administered to a patient with a confirmed blood glucose level less that 70 mg/dl. 13
14 CARDIAC ARREST / ACLS VENTRICULAR FIBRILLATION (V FIB) PULSELESS VENTRICULAR TACHYCARDIA (V TACH) Withhold Resuscitation UNIVERSAL PATIENT CARE PROTOCOL B EMT B A Advanced A Follow Local County Coroner Procedures Yes Criteria for Death Criteria for DNR M MED CONTROL M Review DNR Comfort Care Guidelines Start CPR X 5 cycles / 2 minutes If V-Fib is Witnessed by EMS immediately 200J CONTACT MEDICAL CONTROL Apply Cardiac Monitor Defibrillator / AED Defibrillate Biphasic: 200J or Monophasic 360J Resume effective CPR / 2 minutes, then check rhythm AIRWAY PROTOCOL IV/IO PROTOCOL IO PROTOCOL Continue effective CPR / 2 minutes, then check rhythm EPINEPHRINE 1 mg IV / IO 1:10,000 Solution Repeat every 3-5 minutes OR VASOPRESSIN 40 u. IV / IO Max 1 Dose Defibrillate Biphasic: 300J or Monophasic 360J Return of Spontaneous Circulation GO TO POST RESUSCITATION INDUCED HYPOTHERMIA CARDIAC CARE PROTOCOL Continue effective CPR / 2 minutes, then check rhythm Give Antiarrhythmic during CPR AMIODARONE 300 mg IV/IO May 150 mg IV in 3-5 minutes Defibrillate Biphasic: 360J or Monophasic 360J Continue effective CPR / 2 minutes, then check rhythm TRANSPORT CONTACT MEDICAL CONTROL Consider: Termination of Resuscitation Efforts 14
15 CARDIAC ARREST / ACLS VENTRICULAR FIBRILLATION (V FIB) PULSELESS VENTRICULAR TACHYCARDIA (V TACH) HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Estimated down time Past medical history Medications Events leading to arrest Renal failure / dialysis DNR or living will Unresponsive Apneic Pulseless Ventricular fibrillation or ventricular tachycardia on EKG/monitor Asystole Artifact / device failure Cardiac Endocrine / Metabolic Drugs Pulmonary KEY POINTS Exam: Mental Status, Neck, Skin, Lungs, Heart, Abdomen, Extremities, Neuro. Effective CPR should be as continuous as possible with a minimum of 5 cycles or 2 minutes. Reassess and document endotracheal tube placement and ET CO2 frequently: after every move, and at transfer. Polymorphic V-Tach (Torsades de Pointes) may benefit from administration of magnesium sulfate. If the patient converts to another rhythm, or has a return of circulation, refer to the appropriate protocol and treat accordingly. If the patient converts back to ventricular fibrillation or pulseless ventricular tachycardia after being converted to ANY other rhythm, defibrillate at the previous setting used. Defibrillation following effective CPR is the definitive therapy for ventricular fibrillation and pulseless ventricular tachycardia. Vasopressin is not repeated and may be administered in place of the first or second dose of epinephrine only. If given, Epinephrine may be used 5 minutes after Vasopressin if still in arrest, 1mg of Epinephrine 1:10,000 would then be administered every 3-5 minutes. 15
16 CARDIAC ARREST / ACLS POST RESUSCITATION CARDIAC CARE B EMT B A Advanced A M MED CONTROL M UNIVERSAL PATIENT CARE PROTOCOL Begin Induced Hypothermia Protocol Continue Ventilatory Support with 100% OXYGEN IV/IO PROTOCOL Apply Cardiac Monitor Obtain 12 Lead Vital Signs Hypotension Ventricular Ectopy Bradycardia NS bolus 20 ml/kg IV/IO DOPAMINE 5 20 mcg/kg/min IV/IO Titrate to effect AMIODARONE 150 mg IV/IO in 100 ml bag over 10 minutes Treat per Bradycardia Protocol if Hypotensive Dopamine Simple calculation for approx 5 mcg/kg/min (must be 1600 mcg/ml concentration) *Take the Patients weight in lbs and remove the last digit (175lbs = 17) * Subtract 2 from that figure (17-2=15) *This gives you the number of drops per min using a 60gtts set. (titrate to desired effect) Example: 175lbs patient. 175 remove the 5 is = 15 drops per min (approx 5 mcg/kg/min) If arrest reoccurs, revert to appropriate protocol and/or initial successful treatment CONTACT MEDICAL CONTROL TRANSPORT 16
17 CARDIAC ARREST/ ACLS POST RESUSCITATION CARDIAC CARE HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Respiratory arrest Cardiac arrest Return of pulse Continue to address specific differentials associated with the original Arrythmia KEY POINTS Exam: Mental Status, Neck, Skin, Lungs, Heart, Abdomen, Extremities, Neuro. Most patients immediately post resuscitation will require ventilator assistance. The condition of post-resuscitation patients fluctuates rapidly and continuously, and they require close monitoring. Appropriate post-resuscitation management can best be planned in consultation with Medical Control. This is the period of time between restoration of spontaneous circulation and the transfer of care at the emergency department. The focus is aimed at optimizing oxygenation and perfusion. Adequate oxygenation is the key to a good outcome. 17
18 CARDIAC ARREST / ACLS INDUCED HYPOTHERMIA Return of Spontaneous Circulation Patient is still unresponsive / Comatose B EMT B A Advanced A M MED CONTROL M Airway Protocol NO Advanced Airway in place (ET or King Airway) With ET CO 2 >20 mmhg? Expose patient apply ice packs to axilla and groin Apply Cooling Collar if available Cold Saline Bolus 20 ml/kg to max 2 liters Dopamine mcg/kg/min Target BP 90 Discontinue Cooling Measures <33 C Reassess >33C Temperature Continue to monitor temperature and go to post resuscitation protocol Post Resuscitation Protocol Dopamine Simple calculation for approx 5 mcg/kg/min (must be 1600 mcg/ml concentration) *Take the Patients weight in lbs and remove the last digit (175lbs = 17) * Subtract 2 from that figure (17-2=15) *This gives you the number of drops per min using a 60gtts set. (titrate to desired effect) Example: 175lbs patient. 175 remove the 5 is = 15 drops per min (approx 5 mcg/kg/min) 18
19 CARDIAC ARREST/ ACLS INDUCED HYPOTHERMIA HISTORY SIGNS AND SYMPTOMS DIFFERENTIAL DIAGNOSIS Non-traumatic cardiac arrest (drowning and hanging are permissible in this protocol Return of pulse Continue to address specific differentials associated with the original Arrythmia KEY POINTS Criteria for Induced Hypothermia ROSC not related to blunt/penetrating trauma or hemorrhage Age 12 or older with adult body habitus Advanced airway in place (ET or King Airway) with no purposeful response to pain If no advanced airway can be obtained, cooling may only be initiated on order from online medical control Take care to protect patient modesty. Undergarments may remain in place during cooling. Do not delay transport to cool Frequently monitor airway, especially after each patient move Patients may develop metabolic alkalosis with cooling. Do not hyperventilate 19
20 CARDIAC ARREST/ ACLS Left Ventricular Assist Device (LVAD) Ventricular assist device patients (VAD) are special care situations. Unless these patients are in cardiac arrest they need to be transported to their VAD implantation center. Local or regional hospitals are not equipped to handle these patients. B EMT B A Advanced A M MED CONTROL M UNIVERSAL PATIENT CARE PROTOCOL Determine if VAD is functioning Auscultate chest and upper abdominal quadrants Continuous Humming sound = pump is working Many pumps are non-pulsatile; patient may not have palpable pulses, measurable BP, or Pulse Oximetery. Use other indicators of perfusion such as skin signs, mental status, and Capnography. Contact Appropriate VAD team Cleveland Clinic Pager University Hospital Pager The Patient should have a companion (Family member, friend, caretaker, etc) who is knowledgeable in the function of the VAD. Utilize this resource regarding specifics of each type of VAD system. Keep the companion with the patient Keep all equipment with the patient Not Functioning / Alarming Find Accompanying Instructions for Device 1. Page / call VAD team 2. Check that all Wires / Leads Connected to Controller / Power 3. Check Power Sources 4. Change Power Sources (Only change 1 battery at a time) 5. Attempt Re-start or Start in Backup Mode 6. Switch to Back-Up Controller (If Instructed by VAD Coordinator) IF unable to Maintain Pump Operation Follow VAD team instructions Treat for Cardiogenic Shock Rapid Transport Patient Unstable Treat Per Standard ACLS Protocols Pacing OK Defibrillation OK ACLS drugs OK Chest Compressions only as ABSOLUTE last resort Functioning Do not ever shut off Patient Stable Treat Per Standard Medical Protocols TRANSPORT to appropriate facility (Air Transport OK for VAD Patients) CONTACT receiving facility CONSULT Medical Direction where indicated 20
21 MEDICATIONS ADENOSINE (Adenocard) ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS ADULT DOSAGE PEDIATRIC DOSAGE KEY POINTS Slows conduction time and can interrupt re-entrant pathways through the AV node Slows the sinus rate Supra Ventricular Tachycardia (SVT) Consider in Regular Wide Complex Tachycardia Paroxysmal Supra Ventricular Tachycardia (PSVT) Wolf Parkinson White (WPW) Second or third degree AV block, sick sinus syndrome Ventricular tachycardia Hypersensitivity to Adenosine It is helpful to inform the patient of likely side effects prior to medication administration Facial flushing Shortness of breath Chest pain Palpitations Brief period of sinus arrest /Transient Dysrhythmias Headache Lightheadedness Hypotension Nausea Initial Dose 6 mg rapid IVP (over 1-3 sec) immediately followed with a 20 ml saline flush Repeat Dose If no response is observed after 1 min., administer 12 mg rapid IVP (over 1-3 sec) immediately followed with a 20 ml saline flush. Max dose 30 mg Initial Dose 0.1 mg/kg rapid IVP followed with a 10 ml saline flush Repeat Dose If no response is observed after 1-2 min., administer 0.2 mg/kg rapid IVP followed with a 10 ml saline flush. Max dose 0.5 mg/kg up to 6mg Adenosine has a short half life, and should be administered rapidly followed by a rapid IV/IO flush Reassess after each medication administration, refer to the appropriate protocol and treat accordingly. Perform a 12 Lead EKG prior to the administration of Adenosine and after the rhythm converts Record rhythm during and post administration
22 MEDICATIONS AMIODARONE (Cordarone) ACTIONS INDICATIONS CONTRAINDICATIONS Prolongs the refractory period and action potential duration Ventricular Fibrillation (refractory to shock treatment) Pulseless Ventricular Tachycardia (refractory to shock treatment) Polymorphic VT and wide complex tachycardia Hypersensitivity (including iodine) Cardiogenic shock Second and Third degree AV block Severe sinus bradycardia Severe sinus node dysfunction SIDE EFFECTS ADULT DOSAGE Tremors, Paresthesia, Ataxia Headache, Fatigue Abdominal pain, Nausea/Vomiting, Hepatic failure Arrhythmia, Bradycardia, Sinus arrest, Heart block (Prolonged QT), Heart failure Acute Respiratory Distress Syndrome, Severe pulmonary edema Blue-Gray skin Ventricular Fibrillation and Pulseless Ventricular Tachycardia 300 mg IV/IO bolus Repeat Dose: 150 mg IV/IO in 3-5 minutes, Max 2.2 g IV/24hrs PEDIATRIC DOSAGE KEY POINTS Wide Complex Tachycardia 150 mg IV/IO over 10 minutes (15 mg/min) Repeat Dose: 150 mg IV/IO every 10 minutes prn, Max 2.2 g IV/24hrs Ventricular Fibrillation and Pulseless Ventricular Tachycardia 5 mg/kg IV/IO bolus Ventricular Arrhythmias Loading dose 5 mg/kg IV/IO over mins Avoid excessive movement and shaking of the medication
23 MEDICATIONS ASPIRIN B EMT B A Advanced A ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS SUPPLIED ADULT DOSAGE PEDIATRIC DOSE Blocks platelet aggregation Chest pain suggestive of a MI 12-Lead EKG indicating a possible MI Hypersensitivity Active ulcer disease Impaired renal function Upset stomach GI bleeding Mucosal lesions Bronchial spasm in some asthma patients 325 mg tablet or 81 mg chewable tablet 325 mg tablet or 324 mg (81 mg x 4 tablets) PO Not Recommended for Pediatric Use
24 MEDICATIONS ATIVAN (LORAZEPAM) A Advanced A ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS ADULT DOSAGE PEDIATRIC DOSE Sedative Anticonvulsant Amnestic (induces amnesia) Status epilepticus Sedation prior to transcutaneous pacing and synchronized cardioversion in the conscious patient Known hypersensitivity Altered mental status of unknown origin Head injury Respiratory insufficiency May cause respiratory depression, respiratory effort must be continuously monitored with Capnography Should be used with caution with hypotensive patients and patients with altered mental status Lorazepam (Ativan) potentiates alcohol or other CNS depression Respiratory depression Hypotension Lightheadedness Confusion Slurred speech Amnesia 1 2 mg IV / IO / IM / IN Not Recommended for Pediatric Use
25 MEDICATIONS ATROPINE SULFATE ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS SUPPLIED ADULT DOSAGE PEDIATRIC DOSAGE Increases sinus node firing Increases conduction through the AV node by blocking vagal activity Increases cardiac output Decreases ectopic beats or fibrillation of the ventricles Symptomatic sinus bradycardia Organophosphate poisoning/nerve agent exposure Known hypersensitivity Atrial flutter/fibrillation where there is a rapid ventricular response Glaucoma narrow angle 2 nd and 3 rd degree AV Block with wide QRS complex Use with extreme caution in myocardial infarction May increase myocardial oxygen demand May trigger tachy-dysrhythmias Patient needs to be warned about side effects Doses smaller than 0.5 mg or administered too slowly may slow rather than speed up the heart rate Excessive doses in adults may precipitate ventricular tachycardia or fibrillation Dry mouth, thirst, urinary retention Blurred vision, pupillary dilation, headache Flushed skin Tachycardia Prefilled syringes containing 1 mg in 10 ml Auto-Injector containing 2 mg (nerve agent exposure only) Bradycardia 0.5 mg IV/IO (1.0 mg ETT) every 5 minutes Max dose 0.04 mg/kg or 3 mg Organophosphate Poisoning 2 5mg IVP, IM, or IO every 5 min Bradycardia 0.02 mg/kg IV/IO, repeated X 1, 5 minutes (minimum dose 0.1 mg), Max single dose 0.5 mg CHILD / 1.0 mg ADOLESCENT, Max total dose 1.0 mg CHILD / 2.0 mg ADOLESCENT Organophosphate Poisoning 0.2 mg/kg IV/IO, repeat every 3-5 minutes / Max dose 0.5mg Child Max dose 1.0mg Adolescent.
26 MEDICATIONS BiCarbonate (Sodium BiCarbonate) ACTIONS INDICATIONS CONTRAINDICATIONS SIDE EFFECTS ADULT DOSAGE PEDS DOSAGE Buffers metabolic acidosis Enhances the urinary excretion of tricyclics Metabolic Acidosis from cardiac arrest Tricyclic Overdose Hyperkalemia Post Crushing Entrapment Heart Failure Seizures Tissue necrosis if infiltration Can precipitate with Calcium 50mEq IVP for tricyclic overdose 50mEq or 1mEq/kg IVP for cardiac arrest asystole or PEA 50 meq IVP for cardiac arrest with prolonged down time(10 minutes) 50mEq to 100mEq Post Crushing Entrapment 1mEq/kg IV/IO Diluted in 1:1 NS or as advised By Med Command
27 MEDICATIONS BRILINTA (ticagrelor) ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS ADULT DOSAGE PEDIATRIC DOSAGE A P2Y12 platelet inhibitor indicated to reduce the rate of thrombotic cardiovascular events in patients with acute coronary syndrome, Acute Coronary Syndrome / STEMI 12-Lead EKG indicating a ST elevation MI History of intracranial hemorrhage Active pathological bleeding Severe hepatic impairment Increased risk of bleeding Dyspnea Bleeding Dyspnea 180mg PO (2 90mg Tablets) NOT RECOMMENDED FOR PEDIATRIC USE
28 MEDICATIONS CALCIUM CHLORIDE ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS ADULT DOSAGE PEDIATRIC DOSAGE KEY POINTS Reverses overdose with magnesium sulfate or calcium channel blockers (such as verapamil) Antidote magnesium sulfate and calcium channel blocker toxicity Hyperkalemia Beta Blocker overdose Known dialysis patient in cardiac arrest Hypersensitivity to calcium chloride Do not infuse with sodium bicarbonate will combine to form an insoluble precipitate Can cause ventricular fibrillation when pushed too fast or given to a patient who has been taking digitalis 1 gram (10cc) slow IVP NOT RECOMMENDED FOR PEDIATRIC USE Previously, calcium was used in resuscitation because it was believed to stimulate the heart to beat in asystole and to strengthen cardiac contractions in electromechanical dissociation careful recent studies have failed to show any benefit from using calcium in cardiac arrest, and indeed the effects of calcium may be harmful in that situation
29 MEDICATIONS DOPAMINE (Intropine) ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS ADULT DOSAGE Alpha and beta adrenergic receptor stimulator Dopaminergic receptor stimulator Dilates renal and mesenteric blood vessels Vasoconstriction Arterial resistance Increases cardiac output Increases preload Cardiogenic shock Distributive Shock Cyanide poisoning (contact Medical Control) Known hypersensitivity /Allergy Hypovolemic hypotension VF or VT Do not mix with bicarbonate, dopamine may be inactivated by alkaline solutions Extravasation may cause tissue necrosis Ectopic beats, palpitations Tachycardia, angina Nausea/vomiting VF or VT Dyspnea Headache 2-20mcg/kg/min IV drip. Start 5 micrograms/kg/minute IV/IO infusion, titrate to effect Simple calculation for approx 5 mcg/kg/min (must be 1600 mcg/ml concentration) *Take the Patients weight in lbs and remove the last digit (175lbs = 17) * Subtract 2 from that figure (17-2=15) *This gives you the number of drops per min using a 60gtts set. (titrate to desired effect) Example: 175lbs patient. 175 remove the 5 is =15 drops per min (approx 5 mcg/kg/min)
30 MEDICATIONS HEPARIN ACTIONS INDICATIONS CONTRAINDICATIONS SIDE EFFECTS ADULT DOSAGE Anticoagulant Acute Coronary Syndrome LVAD malfunction Hypersensitivity to Heparin Active bleeding Trauma Severe hypertension Aortic dissection Pregnancy Major surgery within the last 14 days Symptoms of CVA Bleeding 60 units/kg IV Maximum dose (4000 units) KEY POINTS
31 MEDICATIONS KETOROLAC (Toradol) A Advanced A ACTIONS INDICATIONS CONTRAINDICATIONS SIDE EFFECTS ADULT DOSAGE PEDIATRIC DOSAGE NSAID analgesic Reduces pain Moderate pain Pain associated with kidney and gall stones >65 Years Old Hypersensitivity including aspirin or other NSAIDS Advanced renal impairment Suspected cerebrovascular bleeding Recent GI bleeding Nursing mothers Labor and delivery Asthma Edema Hypertension Rash Nausea Dizziness 30 mg IV, 60 mg IM (If <65 Year Old Only) 0.15 mg/kg IV or 0.3 mg/kg IM
32 MEDICATIONS MORPHINE SULFATE A Advanced A ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS ADULT DOSAGE PEDIATRIC DOSAGE Narcotic Analgesic Causes peripheral vasodilation Pulmonary edema MI pain unrelieved with nitro Pain management Pain secondary to burns Known hypersensitivity / Allergy Head injury or head trauma Hypotension Altered LOC Undiagnosed abdominal pain(consult Med Command) COPD Bradycardia Multiple trauma patients If the patient responds with respiratory depression or hypotension, administer Narcan to reverse the effects Routinely monitor the patient s respiratory effort and SpO2 Respiratory depression Altered LOC, constricted pupils Bradycardia Nausea/Vomiting Hypotension 2-4 mg slow IV/IO/IM/IN (If no relief, may repeat at 2 to 4 mg) For further doses over 10mg of Morphine, contact medical direction. Follow with Zofran Pain Management: mg/kg slow IV/IO/IM/IN KEY POINTS
33 MEDICATIONS NITROGLYCERIN A Advanced A ACTIONS INDICATIONS CONTRAINDICATIONS SIDE EFFECTS ADULT DOSAGE Decreases preload and afterlead Increases coronary blood flow Cardiac chest discomfort, angina STEMI Pulmonary edema Known hypersensitivity Hypotension (systolic BP <110, diastolic BP <60 Increased intracranial pressure Glaucoma CVA Erectile dysfunction drugs (contact med control) Headache Hypotension Dizziness, weakness Syncope Dilated pupils Cardiac Chest Discomfort 0.4 mg SL or spray May repeat every 5 minutes up to 3 doses if B/P systolic > 100mmHg PEDIATRIC DOSAGE KEY POINTS Not recommended in the prehospital setting
34 MEDICATIONS ONDANSETRON (Zofran) A Advanced A ACTIONS INDICATIONS CONTRAINDICATIONS SIDE EFFECTS ADULT DOSAGE PEDIATRIC DOSAGE KEY POINTS Antiemetic Nausea & vomiting Hypersensitivity Drowsiness, vertigo Blurred vision, headache Hypotension 4 mg slow IV/IO/IM - 8 mg Oral Dissolving Tabs Contact Medical Control
35 MEDICATIONS LOPRESSOR (Metoprolol) ACTIONS INDICATIONS CONTRAINDICATIONS SIDE EFFECTS Beta Blocker Decreases HR Decreases systolic BP Convert or slow ventricular response in SVT (adenosine preferred) Rate Control in SVT that will not convert Bronchial asthma CHF Second or third degree heart block Bradycardia Cardiogenic shock Cocaine use Bradycardia Heart block CHF Bronchospasm Hypotension ADULT DOSAGE PEDIATRIC DOSAGE 5 mg IV/IO over 1 minute. May repeat 5 mg after 3 minutes if inadequate response and B/P>110 and HR>60 Not recommended for Pediatric use
36 MEDICATIONS VERSED (Midazolam) A Advanced A ACTION INDICATIONS CONTRAINDICATIONS SIDE EFFECTS Sedative and hypnotic benzodiazepine Induces amnesia Conscious sedation Seizure Facilitate intubation Facilitate pacing / cardioversion Intolerance to benzodiazepines Narrow-angle glaucoma Shock Coma CNS amnesia, headache, dizziness, euphoria, comfusion, agitation, anxiety, delirium, drowsiness, muscle tremor, ataxia, dysphoria, slurred speech, and paresthesia. Cardiovascular hypotension, PVC s, tachycardia, vasocagel episode Eye blurred vision, diplopia, nystagmus, pinpoint pupils Respiratory coughing, bronchospasms, laryngospasm, apnea, hypoventilation, wheezing, airway, obstruction, tachypnea ADULT DOSAGE PEDIATRIC DOSAGE NOTE Skin swelling, burning, pain at the site of injection 2mg IV/IO max initial dose for sedation (may repeat as necessary) 2mg IV/IO or 5mg IM/IN max initial dose for seizures (may repeat as necessary) 5mg IM/IN for Violent Patients Versed may be administered IM or IN in actively seizing or violent patients whenever IV access is not achieved. Always be ready to assist ventilations Seizures 0.1mg/kg IV/IO to a max dose of 2mg 0.2mg/kg IN/IM to a max dose of 5mg For adult patients use only if Ativan is unavailable 44
37 MEDICATIONS MAGNESIUM SULFATE ACTIONS INDICATIONS CONTRAINDICATIONS SIDE EFFECTS Anticonvulsant Antiarrhythmic CNS depressant Seizures secondary to eclampsia Ventricular ectopy refractory to Amiodarone Torsades Adjunct to alleviate acute asthma attack Renal disease Heart blocks Respiratory depression CNS depression Hypotension Cardiac arrest ADULT DOSAGE Torsades grams SLOW IVP over 5 minutes (Max dose 4 grams) Eclampsia grams over 2-3 minutes PEDIATRIC DOSAGE KEY POINTS Asthma dose 45mg/kg IV to a total of 75mg/kg (approx 2 grams in adult Not recommended for pediatric use 27
38 MEDICATIONS VASOPRESSIN (Pitressin) ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS SUPPLIED ADULT DOSAGE Alpha agonist Causes vasoconstriction Increases smooth muscle activity Ventricular Fibrillation Pulseless Ventricular Tachycardia Known hypersensitivity Nephritis (inflammation of the kidney) Not recommended for responsive patients with CAD May provoke cardiac ischemia and angina Nausea/Vomiting Diarrhea Confusion Pain at IV site 20 Units / ml in a vial Cardiac Arrest / Ventricular Fibrillation / Pulseless Ventricular Tachycardia 40 Units IV/IO push (administered in place of the first or second dose of Epinephrine) PEDIATRIC DOSAGE Not recommended for pediatric use KEY POINTS The half-life of Vasopressin is approximately minutes 43
39 ACTIONS INDICATIONS CONTRAINDICATIONS PRECAUTIONS SIDE EFFECTS ADULT DOSAGE MEDICATIONS EPINEPHRINE (Adrenaline) Alpha and Beta adrenergic agonist Bronchodilation Increases heart rate and automaticity Increases cardiac contractility Increases myocardial electrical activity Increases systemic vascular resistance Increases blood pressure Cardiac arrest Allergic reaction/anaphylaxis Respiratory distress Acute Asthma Pediatric Bradycardia A Advanced A Hypersensitivity, Tachycardia, Hypertension, Hypothyroidism Angina / Chest pain, Coronary artery disease Pregnancy Blood pressure, pulse, and EKG must be routinely monitored Palpitations, ectopic beats, tachycardia Anxiety / Tremors Hypertension VF / VT Angina Asthma and Anaphylaxis Mild / Moderate Reaction (1-1,000) mg IM ONLY Consider 1:1000 2mg mixed with 1ml NS in nebulizer for Asthma Severe Anaphylaxis (1:10,000) 0.5 mg slow IV/IO over 5 minutes - EMT-P Only Cardiac Arrest 1:10,000 1 mg IV/IO every 3-5 minutes EMT-P Only PEDIATRIC DOSAGE Asthma and Anaphylaxis Mild Reaction Ages yrs (1:1,000) 0.03 mg/kg IM Under 10 yrs (1:1,000) 0.01mg/kg IM May use 1:1000 2mg mixed with 1ml NS in nebulizer aerosolized Severe Anaphylaxis Pending Arrest Ages yrs (1:10,000) 0.01mg/kg IV/IO over 5 minutes EMT-P Only Cardiac Arrest 1:10, mg/kg IV/IO push 0.1ml/kg EMT-P Only or 0.1 mg/kg 1:1000 ETT 0.1ml/kg EMT-P Only 18
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
Alabama Medications. Christopher J. Colvin January 2010
 Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
table of contents drug reference
 table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
IU Health ACLS Study Guide
 IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
Wilson County Emergency Management Agency Protocol Manual Protocols
 Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Arrest. What s a Nurse to do?
 Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Stimulates HR, BP, CO, and vasoconstriction. Stimulates renal, venous, mesenteric arterial. basic chart below) (alpha receptors) vasoconstriction
 Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Upstate University Health System Medication Exam - Version A
 Upstate University Health System Medication Exam - Version A Name: ID Number: Date: Unit: Directions: Please read each question below. Choose the best response for each of the Multiple Choice and Medication
Upstate University Health System Medication Exam - Version A Name: ID Number: Date: Unit: Directions: Please read each question below. Choose the best response for each of the Multiple Choice and Medication
New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010!
 ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
Drug List. Medication Adult Dosing Pediatric Dosing. V-fib / pulseless V-tach 300 mg IV push Repeat dose of 150 mg IV push for recurrent episodes
 Acetaminophen (Tylenol) 7-Pain Control-Adult 46-Pain Control-Pediatric 72-Fever 1000 mg po 15 mg/kg po Indicated for pain and fever control Avoid in patients with severe liver disease Adenosine (Adenocard)
Acetaminophen (Tylenol) 7-Pain Control-Adult 46-Pain Control-Pediatric 72-Fever 1000 mg po 15 mg/kg po Indicated for pain and fever control Avoid in patients with severe liver disease Adenosine (Adenocard)
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES. Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003.
 MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
SMO: Anaphylaxis and Allergic Reactions
 REGION I EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic SMO: Anaphylaxis and Allergic Reactions Overview: Allergic reactions can vary in severity from a mild reaction consisting of hives
REGION I EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic SMO: Anaphylaxis and Allergic Reactions Overview: Allergic reactions can vary in severity from a mild reaction consisting of hives
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
CBT/OTEP 243 Aspirin Administration for ACS
 Seattle-King County EMS Seattle-King County Emergency Medical Services Division Public Health - Seattle/King County 401 5th Avenue, Suite 1200 Seattle, WA 98104 (206) 296-4693 February 2009 CBT/OTEP 243
Seattle-King County EMS Seattle-King County Emergency Medical Services Division Public Health - Seattle/King County 401 5th Avenue, Suite 1200 Seattle, WA 98104 (206) 296-4693 February 2009 CBT/OTEP 243
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
!!! BOLUS DOSE IV. Use 5-10 mcg IV boluses STD ADRENALINE INFUSION. Use IM adrenaline in advance of IV dosing!
 ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
ADRENALINE IVI BOLUS IV Open a vial of 1:1000 ADRENALINE 1 mg /ml Add 1 ml to 9 ml N/Saline = 1mg adrenaline in 10 ml (or 100 mcg/ml) Add 1 ml 1:10,000 to 9 ml N/Saline = 100 mcg adrenaline in 10 ml (or
THE REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE NEW YORK CITY PREHOSPITAL TREATMENT PROTOCOLS ADVANCED LIFE SUPPORT (PARAMEDIC) PROTOCOLS
 THE REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE NEW YORK CITY PREHOSPITAL TREATMENT PROTOCOLS ADVANCED LIFE SUPPORT (PARAMEDIC) PROTOCOLS July 2012 Version 07012012 The Regional Emergency Medical Services
THE REGIONAL EMERGENCY MEDICAL ADVISORY COMMITTEE NEW YORK CITY PREHOSPITAL TREATMENT PROTOCOLS ADVANCED LIFE SUPPORT (PARAMEDIC) PROTOCOLS July 2012 Version 07012012 The Regional Emergency Medical Services
Team Leader. Ensures high-quality CPR at all times Assigns team member roles Ensures that team members perform well. Bradycardia Management
 ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
PRE-HOSPITAL CARE MEDICAL CONTROL PROTOCOLS AND PROCEDURES
 EMS Services PRE-HOSPITAL CARE MEDICAL CONTROL PROTOCOLS AND PROCEDURES TABLE OF CONTENTS 10. Appendix: pages Pharmacology Review / Medications 1-2 Adenosine (Adenocard) 3 Albuterol (Proventil / Ventolin)
EMS Services PRE-HOSPITAL CARE MEDICAL CONTROL PROTOCOLS AND PROCEDURES TABLE OF CONTENTS 10. Appendix: pages Pharmacology Review / Medications 1-2 Adenosine (Adenocard) 3 Albuterol (Proventil / Ventolin)
Pharmacology for the EMT
 Pharmacology for the EMT Presented by Wade Scoles RRT, NREMT Pharmacodynamics Everybody reacts to drugs differently Factors altering drug responses Age Body mass Sex Pathologic state Genetic factors Psychological
Pharmacology for the EMT Presented by Wade Scoles RRT, NREMT Pharmacodynamics Everybody reacts to drugs differently Factors altering drug responses Age Body mass Sex Pathologic state Genetic factors Psychological
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS
 Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
DIPHENHYDRAMINE (Benadryl)
 DIPHENHYDRAMINE (Benadryl) Classification: Antihistamine (H1 blocker) Antihistamine; appear to compete with histamine for cell receptor sites on effector cells. Therapeutic Relieves effects of histamine
DIPHENHYDRAMINE (Benadryl) Classification: Antihistamine (H1 blocker) Antihistamine; appear to compete with histamine for cell receptor sites on effector cells. Therapeutic Relieves effects of histamine
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
TENNESSEE EMERGENCY MEDICAL SERVICES PROTOCOL GUIDELINES. Index
 Introduction Definitions Index Cardiac Emergency (Adult & Pediatric) 101 Automatic External Defibrillator 102 New Onset Atrial Fibrillation and Flutter 103 Bradycardia 104 Acute Coronary Syndrome/STEMI
Introduction Definitions Index Cardiac Emergency (Adult & Pediatric) 101 Automatic External Defibrillator 102 New Onset Atrial Fibrillation and Flutter 103 Bradycardia 104 Acute Coronary Syndrome/STEMI
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins)
 Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
PALS Interim Study Guide
 PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com
 Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Drug List. Drug Adult Pediatric
 Acetaminophen (Tylenol) 8-Fever 10-Pain Control-Adult 11-Pain Control-Pediatric 47-Pediatric Seizure 1000 mg po 10 mg/kg po Indicated for pain and fever control Avoid in patients with severe liver disease
Acetaminophen (Tylenol) 8-Fever 10-Pain Control-Adult 11-Pain Control-Pediatric 47-Pediatric Seizure 1000 mg po 10 mg/kg po Indicated for pain and fever control Avoid in patients with severe liver disease
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier
 Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
Emergency Medical Programs. Common Drugs - Indications & Administration
 - Indications & Administration Table of Contents ACTIVATED CHARCOAL 3 ADENOSINE (Adenocard) 4 ALBUTEROL (Proventil, Ventolin) 5 AMIODARONE (Cordarone) 6 ASPIRIN 7 ATROPINE (Atropine, Component of Mark
- Indications & Administration Table of Contents ACTIVATED CHARCOAL 3 ADENOSINE (Adenocard) 4 ALBUTEROL (Proventil, Ventolin) 5 AMIODARONE (Cordarone) 6 ASPIRIN 7 ATROPINE (Atropine, Component of Mark
Paramedic Pediatric Medical Math Test
 Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Paramedic Pediatric Medical Math Test Name: Date: Problem 1 Your 4 year old pediatric patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE
 ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
PACKAGE LEAFLET: INFORMATION FOR THE USER. ADRENALINE (TARTRATE) STEROP 1 mg/1 ml Solution for injection. Adrenaline (Levorenine, Epinephrine)
 PACKAGE LEAFLET: INFORMATION FOR THE USER ADRENALINE (TARTRATE) STEROP 1 mg/1 ml Solution for injection Adrenaline (Levorenine, Epinephrine) Read all of this leaflet carefully before you start using this
PACKAGE LEAFLET: INFORMATION FOR THE USER ADRENALINE (TARTRATE) STEROP 1 mg/1 ml Solution for injection Adrenaline (Levorenine, Epinephrine) Read all of this leaflet carefully before you start using this
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
PREPARATIONS: Adrenaline 1mg in 1ml (1:1000) Adrenaline 100micrograms in 1ml (1:10,000)
 ADRENALINE Acute hypotension Via a CENTRAL venous line Initially 100-300 nanograms/kg/minute 0.1-0.3 microgram/kg/minute adjusted according to response up to a maximum of 1.5 micrograms/kg/minute. Increase
ADRENALINE Acute hypotension Via a CENTRAL venous line Initially 100-300 nanograms/kg/minute 0.1-0.3 microgram/kg/minute adjusted according to response up to a maximum of 1.5 micrograms/kg/minute. Increase
Neonatal Reference Guide
 Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
And the. Two types of orders:
 1 PHARMACOLOGY And the EMT-B 2 MEDICAL DIRECTION Must have Dr. s orders to administer any drug to a Pt Local medical director can override any state set protocols Two types of orders: On-line : verbal
1 PHARMACOLOGY And the EMT-B 2 MEDICAL DIRECTION Must have Dr. s orders to administer any drug to a Pt Local medical director can override any state set protocols Two types of orders: On-line : verbal
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Adrenergic, Adrenergic Blockers, Cholinergic and Cholinergic Blockers
 Adrenergic, Adrenergic Blockers, Cholinergic and Cholinergic Blockers Objective 1: Explain the difference between the sympathetic and parasympathetic nervous systems Autonomic Nervous System Sympathetic
Adrenergic, Adrenergic Blockers, Cholinergic and Cholinergic Blockers Objective 1: Explain the difference between the sympathetic and parasympathetic nervous systems Autonomic Nervous System Sympathetic
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
CALIFORNIA EMERGENCY MEDICAL SERVICES (EMS) MECHANICAL CIRCULATORY SUPPORT (MCS) DEVICES BEST PRACTICES GUIDELINE
 CALIFORNIA EMERGENCY MEDICAL SERVICES (EMS) MECHANICAL CIRCULATORY SUPPORT (MCS) DEVICES BEST PRACTICES GUIDELINE Purpose: To provide information and direction regarding the care of patients who have a
CALIFORNIA EMERGENCY MEDICAL SERVICES (EMS) MECHANICAL CIRCULATORY SUPPORT (MCS) DEVICES BEST PRACTICES GUIDELINE Purpose: To provide information and direction regarding the care of patients who have a
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
Protocol in depth Asthma/COPD. [email protected]
 Protocol in depth Asthma/COPD [email protected] Asthma/COPD Narrowing of airways (an H4 histamine response causing inflammation and mucous production), leading to wheezing on inspiration and exhalation.
Protocol in depth Asthma/COPD [email protected] Asthma/COPD Narrowing of airways (an H4 histamine response causing inflammation and mucous production), leading to wheezing on inspiration and exhalation.
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics. Yen Tibayan, M.D. Division of Cardiovascular Medicine
 Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics Yen Tibayan, M.D. Division of Cardiovascular Medicine Case Presentation 69 y.o. woman calls 911 with the complaint of
Is it really so? : Varying Presentations for ACS among Elderly, Women and Diabetics Yen Tibayan, M.D. Division of Cardiovascular Medicine Case Presentation 69 y.o. woman calls 911 with the complaint of
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Acute Coronary Syndrome. What Every Healthcare Professional Needs To Know
 Acute Coronary Syndrome What Every Healthcare Professional Needs To Know Background of ACS Acute Coronary Syndrome (ACS) is an umbrella term used to cover a spectrum of clinical conditions that are caused
Acute Coronary Syndrome What Every Healthcare Professional Needs To Know Background of ACS Acute Coronary Syndrome (ACS) is an umbrella term used to cover a spectrum of clinical conditions that are caused
Heart Attack: What You Need to Know
 A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
The management of cardiac arrest
 CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
Nurse Practitioner. CLINICAL PROTOCOL Chest Pain
 Nurse INTRODUCTION: Patients presenting with chest pain require rapid evaluation. Myocardial ischaemia should be considered in all patients presenting with chest pain. Assessment of pain type and referral,
Nurse INTRODUCTION: Patients presenting with chest pain require rapid evaluation. Myocardial ischaemia should be considered in all patients presenting with chest pain. Assessment of pain type and referral,
ADENOSINE (Adenocard) Intermediate- CALL IN Paramedic. ALBUTEROL SULFATE Basic-CALL IN Intermediate-CALL IN Paramedic
 ADENOSINE (Adenocard) - CALL IN ALBUTEROL SULFATE Basic-CALL IN AMIODARONE (Cordarone) - CALL IN except in cardiac arrest- call while ASPIRIN Basic ATROPINE SULFATE - CALL IN except in cardiac arrest-
ADENOSINE (Adenocard) - CALL IN ALBUTEROL SULFATE Basic-CALL IN AMIODARONE (Cordarone) - CALL IN except in cardiac arrest- call while ASPIRIN Basic ATROPINE SULFATE - CALL IN except in cardiac arrest-
Summary of State Emergency Medical Control Committee (SEMCC) Approved Protocol Revisions September 1, 2015 NALOXONE
 October 22, 2015 Summary of State Emergency Medical Control Committee (SEMCC) Approved Protocol Revisions September 1, 2015 NALOXONE Summary: Expand Naloxone down to the Emergency Medical Technician (EMT)
October 22, 2015 Summary of State Emergency Medical Control Committee (SEMCC) Approved Protocol Revisions September 1, 2015 NALOXONE Summary: Expand Naloxone down to the Emergency Medical Technician (EMT)
EMS Course Requirements
 EMS Course Requirements The following outlines should be followed when creating your course syllabi. The minimum course hours must be met, but they can be exceeded depending on the needs of your class.
EMS Course Requirements The following outlines should be followed when creating your course syllabi. The minimum course hours must be met, but they can be exceeded depending on the needs of your class.
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference
 New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia
 Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
Pediatric Pharmacotherapy A Monthly Newsletter for Health Care Professionals Children s Medical Center at the University of Virginia Volume 2 Number 12 December 1996 Medications for Neonatal and Pediatric
Union EMS Local Formulary July 18, 2014
 July 18, 2014 Forward The intent of the Union EMS Local Formulary is to provide guidance during the implementation and use of the 2012 NCCEP Protocols, Policies and Procedures to the ALS and BLS Professionals
July 18, 2014 Forward The intent of the Union EMS Local Formulary is to provide guidance during the implementation and use of the 2012 NCCEP Protocols, Policies and Procedures to the ALS and BLS Professionals
PACKAGE LEAFLET: INFORMATION FOR THE USER. ADRENALINE (HCl) STEROP 0,8mg/1ml. Solution for injection. Adrenaline (Levorenine, Epinephrine)
 PACKAGE LEAFLET: INFORMATION FOR THE USER ADRENALINE (HCl) STEROP 0,4mg/1ml ADRENALINE (HCl) STEROP 0,8mg/1ml Solution for injection Adrenaline (Levorenine, Epinephrine) Read all of this leaflet carefully
PACKAGE LEAFLET: INFORMATION FOR THE USER ADRENALINE (HCl) STEROP 0,4mg/1ml ADRENALINE (HCl) STEROP 0,8mg/1ml Solution for injection Adrenaline (Levorenine, Epinephrine) Read all of this leaflet carefully
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
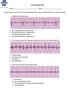 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS
 Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
RESPONDING TO ANESTHETIC COMPLICATIONS
 RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
