How To Understand The Immune System
|
|
|
- Kathlyn Bennett
- 5 years ago
- Views:
Transcription
1 Specific Defense: Adaptive Immunity CHAPTER SUMMARY Elements of Specific Immunity (pp ) The body augments the mechanisms of nonspecific defense with another line of defense that destroys invaders while "learning" in the process. This third line of defense retains a memory of specific pathogens so that when it encounters them a second time, it responds rapidly and effectively. This response is called adaptive immunity or specific immunity. Antigens Antigens are substances that trigger specific immune responses. The three-dimensional shape of a region of an antigen that is recognized by the immune system is the antigenic determinant (or epitope). Effective antigen molecules are large, complex, stable, degradable, and foreign to their host. The most effective antigens therefore are large foreign macromolecules such as proteins, glycoproteins, and phospholipids, but complex carbohydrates and lipids, as well as some bacterial DNA, can be antigenic. Although immunologists characterize antigens in various ways, one clinically important way is to group them according to their relationship to the body: Exogenous antigens include toxins and other secretions and components of microbial cell walls, membranes, flagella, and pili. Protozoa, fungi, bacteria, and viruses that reproduce inside a body's cells produce endogenous antigens. The immune system can only "see" and respond to these antigens if they are incorporated into the cell's cytoplasmic membrane. Autoantigens (or self antigens) are antigenic molecules found on an individual's normal (uninfected) cells. Immune cells that recognize autoantigens as foreign are normally eliminated during the development of the immune system. This phenomenon, called self-tolerance, prevents the body from mounting an immune response against itself. The Cells, Tissues, and Organs of the Lymphatic System The lymphatic system is composed of lymphatic vessels, which conduct the flow of lymph-a colorless, watery liquid similar in composition to blood plasma-from local tissues and returns it to the circulatory system. It also includes lymphoid tissues and organs that are directly involved in specific immunity, including lymph nodes, the thymus, the spleen, the tonsils, and mucosa-associated lymphoid tissue (MALT). Cells with a central role in specific immunity, called lymphocytes, migrate to and persist in various lymphoid organs, where they are available to encounter foreign invaders in the blood and lymph. The red bone marrow contains stem cells which give rise to lymphocytes, which are distinguished according to the glycoproteins on their cell surfaces with 145
2 146 Study Guide for Microbiology cluster ofdifferentiation numbers, such as CD4, CD95, etc. After their production in the bone marrow, lymphocytes must undergo a maturation process. B lymphocytes mature in the bone marrow, and T lymphocytes mature in lymphatic organs where they are influenced by chemical signals from the thymus. After maturation, they migrate to secondary lymphoid organs and tissues, including the lymph nodes in the neck, groin, and armpit, the spleen, and other accumulations of lymphoid tissue. B Lymphocytes (B Cells) and Immunoglobulins B lymphocytes, also called B cells, arise and mature in the bone marrow. Those that are actively fighting against exogenous antigens are called plasma cells, and secrete soluble, antigen-binding proteins called antibodies or immunoglobulins (Ig) into the blood or lymph. Historically, bodily fluids were called humors, and thus the activity of B cells is said to be part of a humoral immune response. A basic antibody molecule is formed of four polypeptide chains-two heavy chains and two light chains-linked with disulfide bonds in such a way that a basic antibody molecule looks like the letter Y with three regions: a stem and two arms connected by a flexible hinge region. The antibody stem is called the Fe region. Among all B cells, there are five basic types of heavy chains, and these give their names to five classes of antibodies: IgG, IgM, IgA, IgE, and IgD. The arms of each heavy and light chain vary in amino acid sequence, and thus each is called a variable region. The antigen-binding site is formed by the variable regions of a heavy and light chain of an antibody. Antigen-binding sites are complementary to antigenic determinants. Once antibodies are bound to antigens, they function in several ways. These include: Activation of complement (discussed in Chapter 15) Stimulation of inflammation (discussed in Chapter 15) Neutralization of toxins by binding to critical portions, or of bacteria or viruses by blocking attachment molecules on their surfaces Opsonization, or enhanced phagocytosis, whereby antibodies act as opsonins, molecules that stimulate phagocytosis Agglutination, the clumping of antibody molecules bound with two microbial cells each, which hinders the activity of pathogens and increases the chance that they will be phagocytized The class involved in any given humoral immune response depends on the type of invading antigen, the portal of entry involved, and the antibody function required: Immunoglobulin G (IgG) is the predominant antibody class found in the bloodstream and the primary defender against invading bacteria. Immunoglobulin A (IgA) is the antibody class most commonly associated with various body secretions, including tears and milk. IgA pairs with a secretory component to form secretory IgA. Immunoglobulin M (IgM) is the third most common antibody class and the predominant antibody produced first during a primary humoral immune response. Immunoglobulin E (IgE) is the signal antibody molecule that triggers the release of cell-damaging molecules onto parasites, particularly parasitic worms. Immunoglobulin D (IgD) is a membrane-bound antibody molecule found in some animals as a B cell receptor. The surface of each B cell is covered with about 500,000 identical copies of B cell receptor (BCR), an antibody that is not secreted but instead remains integral to the cytoplasmic membrane. BCRs are antibody-like proteins that are complementary
3 Chapter 16 Specific Defense: Adaptive Immunity 147 to antigens. A BCR has the same shaped binding sites as do the antibodies that can be synthesized by that cell. T Lymphocytes (T Cells) An adult's red bone marrow produces lymphocytes that leave the bone marrow to mature under the influence of the thymus. These T lymphocytes, or T cells, generate about half a million copies of T cell receptor (TCR) in the cytoplasmic membrane. Because T cells act directly against antigens, their activity is considered to be part of a cell-mediated immune response. Immunologists recognize two types of T cells: Cytotoxic T cells are distinguished by the presence of the CD8 cell-surface glycoprotein. They directly kill infected cells, as well as abnormal body cells such as cancer cells. Helper T cells have CD4 glycoprotein. They help to regulate the activity of B cells and cytotoxic T cells during an immune response. There are two subpopulations: THI cells activate cytotoxic T cells to secrete perforins and granzymes that destroy infected or abnormal cells, and TH2 cells function in conjunction with B cells. Immune System Cytokines Cytokines are soluble regulatory proteins that act as intercellular signals when released by certain body cells including kidney cells, skin cells, and immune cells. Cytokines of the immune system include: Interleukins (ILs) which signal among leukocytes Interferons (IFNs) which, as discussed in Chapter 15, are antiviral proteins that also act as cytokines Growth factors, which stimulate stem cells to divide Tumor necrosis factor (TNF), which is secreted by macrophages and T cells to kill tumor cells and to regulate immune responses Chemokines, which signal leukocytes to rush to a site of inflammation or infection and activate other leukocytes The Body's Preparations for a Specific Immune Response (pp ) The body prepares for specific immune responses by killng lymphocytes with receptors complementary to autoantigens, making major histocompatibility complex proteins, and processing antigens so that they can be recognized by lymphocytes. Lymphocyte Editing by Clonal Deletion Cells with receptors that respond to autoantigens are selectively killed via apoptosis in a process known as clonal deletion (because daughter cells--clones-are deleted). Surviving lymphocytes and their descendents respond only to foreign antigens. When self-tolerance is impaired, the result is an autoimmune disease. The Roles of the Major Histocompatibility Complex The major histocompatibility complex is a cluster of genes located on each copy of chromosome 6 (in humans), which codes for major histocompatibility antigens. These antigens, which are present in the cell membranes of leukocytes, hold and
4 148 Study Guide for Microbiology position antigenic determinants for presentation to T cells. Class I MHC molecules are found on the cytoplasmic membranes of all nucleated cells. Class II MHC proteins are found only on B lymphocytes and special cells called antigen presenting cells (APCs). These include monocytes, macrophages, and their close relatives, such as dendritic cells. Antigens are captured, ingested, and degraded into antigenic determinants by APCs. They are then bound to MHC molecules, and inserted to present the antigenic determinant on the outer surface of the APCs cytoplasmic membrane. Antigen Processing Since large antigens with repeating antigenic determinants can be processed by B cells without the help of T cells, they are called T-independent antigens. Most antigens are smaller and B cells targeted against them cannot function without assistance from helper T cells. These antigens are therefore called T-dependent antigens. The Humoral Immune Response (pp ) B Cell Activation and Clonal Selection Humoral immunity can be viewed as consisting of the following series of cellular interactions, which are mediated by membrane-bound proteins as well as cytokines: 1. Antigen presentation (discussed earlier) 2. Differentiation of THinto TH2 cells 3. Clonal selection, in which only the B cell with BCRs complementary to the antigenic determinant will be recognized 4. Activation of B cell by the TH2 cell such that it proliferates rapidly Memory B Cells and the Establishment of Immunologic Memory A small percentage of the cells produced by B cell proliferation do not secrete antibodies but survive as memory B cells, long-lived cells with BCRs complementary to the specific antigen that triggered their production. In a primary immune response, relatively small amounts of antibodies are produced slowly and are of limited effectiveness. When an antigen is encountered a second time, the activation of memory cells in the secondary immune response ensures that the immune response is rapid and strong. Enhanced immune responses to subsequent exposures are called memory responses. The Cell-Mediated Immune Response (pp ) The body uses cell-mediated immune responses to fight intracellular pathogens such as viruses that have invaded body cells, as well as abnormal body cells such as cancer cells. Cytotoxic T cells recognize abnormal molecules expressed on the surface of an infected, cancerous, or foreign cell. Cytotoxic T cells function only in the presence of cytokines from THI cells. The Perforin-Granzyme Cytotoxic Pathway In the perforin-granzyme pathway, cytotoxic T cells destroy their targeted cells by secreting perforins and granzymes, toxic protein molecules. Perforins perforate cell membranes and granzymes activate apoptotic enzymes in the target cell, thereby forcing the cell to commit suicide.
5 Chapter 16 Specific Defense: Adaptive Immunity 149 The CD95 Cytotoxic Pathway In the CD95 cytotoxic pathway, when cytotoxic T cells contact their target cells, the binding of their CD95 protein with CD95 on the target cell activates enzymes that trigger apoptosis. Memory T Cells Some activated T cells become memory T cells, and can persist for months or even years in lymphoid tissues. Contact with an antigenic determinant matching its TCR prompts the memory T cell to immediately produce cytotoxic T cells. As with humoral immunity, a memory response is more rapid and more effective than a primary response. T Cell Regulation The body carefully regulates cell-mediated immunity so that T cells do not respond to autoantigens. To prevent autoimmunity, T cells require additional signals from an APC. If they do not receive these signals, they will not respond. Types of Acquired Immunity (pp ) Immunologists categorize specific immunity as either naturally or artificially acquired, and as either active or passive. Naturally Acquired Active Immunity Naturally acquired active immunity occurs when the body responds to exposure to antigens by mounting specific immune responses. Naturally Acquired Passive Immunity Naturally acquired passive immunity occurs when a fetus, newborn, or child receives antibodies across the placenta or within breastmilk. Artificially Acquired Active Immunity Artificially acquired active immunity occurs when the body receives antigens by injection, as with vaccinations, and mounts a specific immune response. Artificially Acquired Passive Immunity Artificially acquired passive immunity occurs when the body receives, via injection, preformed antibodies in antitoxins or antisera, which can destroy fast-acting and potentially fatal pathogens such as rabies virus. KEY THEMES Once past the first and second lines of defense, pathogens are faced with the last, and best, line of defense we have-the immune system. The complex association of cells, tissues, and chemicals that make up the immune system are responsible for specifically "seeing" antigens and disposing of them. As you study this chapter, focus on the following: Active immunity is necessary for full protection against disease-causing microorganisms: Nonspecific defenses protect us against the majority of
6 150 Study Guide for Microbiology invaders, but if they are breached, the immune system has to be able to respond decisively to the challenge. B cells are involved in tagging: One of the primary roles of B cells and antibodies is to tag foreign cells and infected cells for destruction. This is one method of controlling immune damage. T cells are involved in killing: Once labeled for destruction, T cells clear the body of free pathogens as well as microbially infected cells. QUESTIONS FOR FURTHER REVIEW Answers to these questions can be found in the answer section at the back of this study guide. Refer to the answers only after you have attempted to solve the questions on your own. Multiple Choice 1. Acquired immunity is most beneficial because it provides: a. Immediate responses to all foreign invaders b. Specific responses geared to specific invaders c. Passive barrier protection against all invaders d. None of the above 2. Which of the molecules listed below would make the best antigens? a. Molecules with stable, defined shapes b. Large molecules rather than small molecules c. Visible molecules rather than hidden molecules d. All of the above 3. The main function of B cells is to: a. Circulate in the blood and phagocytize microbes b. Secrete protective antigens c. Secrete protective antibodies d. Lyse infected cells 4. Which of the following activities of antibodies would prevent the attachment of a virus to a host cell? a. Agglutination b. Neutralization c. Opsonization d. All of the above would prevent attachment 5. A microbially infected cell would most likely be killed by a: a. CD8 expressing T cell c. Cytotoxic T cell b. Helper T cell d. Both a and c 6. B cells work in conjunction with which T lymphocyte? a. Cytotoxic T cell b. Type 1 helper T cell c. Type 2 helper T cell d. B cells do not work with T cells of any type 7. Which of the following is not an immune system cytokine? a. Growth factor c. Interleukin b. Interferon d. Antibody
7 Chapter 16 Specific Defense: Adaptive Immunity Which of the following cells would possess MHC I antigens? a. B cell c. Skin cell b. T cell d. All of the above 9. The best example of a T-independent antigen would be a: a. Viral capsid protein b. Bacterial plasma membrane protein c. Bacterial capsule polysaccharide d. Fungal DNA fragment 10. Antigen presenting cells present antigens to: a. Type 1 helper T cells c. Memory cells b. B cells d. All of the above 11. Which of the following statements is true about both the Perforin-Granzyme cytotoxic pathway and the CD95 cytotoxic pathway? a. Both stimulate apoptosis in the target cell b. Both involve specific interaction of type 1 helper T cells with infected cells c. Both involve specific interactions with cytotoxic T cells and specific receptors on the infected host cells d. None of the above are true 12. Secondary immune responses involve: a. Memory B cells b. Memory T cells c. Immediate responses without the need for activation of immune cells d. All of the above Fill in the Blanks 1. Adaptive immunity is over the course of one's lifetime. This is in contrast to nonspecific defenses which are the same since birth. 2. are molecules that trigger specific immune responses. These molecules can further be broken down into which are the specific, three-dimensional regions recognized by the immune system. 3. The two major types of lymphocytes are and 4. Plasma cells are (Bff) cells that secrete _ These plasma cells are part of the (humoral/cellmediated) immune response.
8 152 Study Guide for Microbiology 5. For each statement presented, indicate which antibody (or antibodies) best fits the description. Answer IgG, IgM, IgA, IgE, or IgD. You may use each answer more than once and some statements may fit more than one antibody. a. The most common antibody in the blood: _ b. Involved in response to parasitic worms: _ c. Activates complement: _ d. Pentameric antibodies in serum: _ e. Found in body secretions: _ f. Function remains unknown; this antibody is not present in all animals: 6. The term used to describe the process of cell suicide is _ During clonal deletion, the process named prevents lymphocytes that recoglllze from becoming part of the circulating immune cells. 7. MHC I molecules are found on cells while MHC II molecules are found on and cells (in each case, name the cell type). The only cells that do not express either MHC I or MHC II antigens are 8. For an infected cell to be killed, APCs stimulate _ cells into becoming cells. These cells then activate cells which bind the infected cell to kill it through one of two pathways: or _ 9. Acquired immune responses can be either an or process. Antibodies that cross the placenta from mother to child is an example of immunity.
9 Chapter 16 Specific Defense: Adaptive Immunity Immune memory can only be achieved through _ (active/passive) immune responses. Short-Answer Questions for Thought and Review 1. Describe the difference between the three major types of antigens. Which type of antigen will lead to the best immune response? 2. Sketch the structure of an antibody and indicate which part designates antibody class, where antigenic determinants are bound, which parts are constant, and which parts vary. 3. Explain the absolute necessity for the process of clonal deletion. 4. Explain why clonal selection is necessary in a humoral immune response. 5. Compare and contrast a primary immune response and a secondary immune response to the same antigen. Critical Thinking 1. Based on the structure of the lymphatic system, its tissues, vessels, and cells, explain why the immune system does not actively patrol the brain or spinal cord. 2. For someone born with a genetic disease where B cells are not produced, what types of immune responses would be missing? 3. Follow the fate of an exogenous pathogenic bacterium through the immune system. Assume it is phagocytized by a macrophage but that the bacterium cannot infect the macrophage.
10 154 Study Guide for Microbiology Concept Building Questions 1. Explain why bacterial DNA is a good antigen but would not be useful in actually producing protective immunity against bacterial infection. Answer in terms of what you know about the immune system and the structure of various microbes. What other types of structures would also be antigenic but not protective? 2. Some microbes are classified partly by serotype-that is, by the antigens they display and the antibodies they elicit. Even though antigens are derived from fairly constant proteins, glycoproteins and polysaccharides on the microbial surface, why are specific antigens a better or more useful classification parameter than the whole structural element itself?
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Name (print) Name (signature) Period. (Total 30 points)
 AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
Microbiology AN INTRODUCTION EIGHTH EDITION
 TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
2) Macrophages function to engulf and present antigen to other immune cells.
 Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Chapter 43: The Immune System
 Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
The Immune System: A Tutorial
 The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
10. T and B cells are types of a. endocrine cells. c. lymphocytes. b. platelets. d. complement cells.
 Virus and Immune System Review Directions: Write your answers on a separate piece of paper. 1. Why does a cut in the skin threaten the body s nonspecific defenses against disease? a. If a cut bleeds, disease-fighting
Virus and Immune System Review Directions: Write your answers on a separate piece of paper. 1. Why does a cut in the skin threaten the body s nonspecific defenses against disease? a. If a cut bleeds, disease-fighting
The Immune System. 2 Types of Defense Mechanisms. Lines of Defense. Line of Defense. Lines of Defense
 The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
Immunity. Humans have three types of immunity innate, adaptive, and passive: Innate Immunity
 Immunity Humans have three types of immunity innate, adaptive, and passive: Innate Immunity Everyone is born with innate (or natural) immunity, a type of general protection. Many of the germs that affect
Immunity Humans have three types of immunity innate, adaptive, and passive: Innate Immunity Everyone is born with innate (or natural) immunity, a type of general protection. Many of the germs that affect
The Body s Defenses CHAPTER 24
 CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
Lymph capillaries, Lymphatic collecting vessels, Valves, Lymph Duct, Lymph node, Vein
 WLHS/A&P/Oppelt Name Lymphatic System Practice 1. Figure 12-1 provides an overview of the lymphatic vessels. First color code the following structures. Color code in Figure 12-1 Heart Veins Lymphatic vessels/lymph
WLHS/A&P/Oppelt Name Lymphatic System Practice 1. Figure 12-1 provides an overview of the lymphatic vessels. First color code the following structures. Color code in Figure 12-1 Heart Veins Lymphatic vessels/lymph
ANIMALS FORM & FUNCTION BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES. Animals Form & Function Activity #4 page 1
 AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
Chapter 14: The Lymphatic System and Immunity
 Chapter 14: The Lymphatic System and Immunity Major function of the Lymphatic System o Network of vessels that collect and carry excess fluid from interstitial spaces back to blood circulation o Organs
Chapter 14: The Lymphatic System and Immunity Major function of the Lymphatic System o Network of vessels that collect and carry excess fluid from interstitial spaces back to blood circulation o Organs
Chapter 3. Immunity and how vaccines work
 Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES JASON CYSTER SECTION 13
 SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
SECTION 13 HUMORAL IMMUNE RE- SPONSES: ACTIVATION OF B CELLS AND ANTIBODIES CONTACT INFORMATION Jason Cyster, PhD (Email) READING Basic Immunology: Functions and Disorders of the Immune System. Abbas,
One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types:
 Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
Basics of Immunology
 Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
LESSON 3: ANTIBODIES/BCR/B-CELL RESPONSES
 Introduction to immunology. LESSON 3: ANTIBODIES/BCR/B-CELL RESPONSES Today we will get to know: The antibodies How antibodies are produced, their classes and their maturation processes Antigen recognition
Introduction to immunology. LESSON 3: ANTIBODIES/BCR/B-CELL RESPONSES Today we will get to know: The antibodies How antibodies are produced, their classes and their maturation processes Antigen recognition
B cell activation and Humoral Immunity
 B cell activation and Humoral Immunity Humoral immunity is mediated by secreted antibodies and its physiological function is defense against extracellular microbes (including viruses) and microbial exotoxins.
B cell activation and Humoral Immunity Humoral immunity is mediated by secreted antibodies and its physiological function is defense against extracellular microbes (including viruses) and microbial exotoxins.
1) Siderophores are bacterial proteins that compete with animal A) Antibodies. B) Red blood cells. C) Transferrin. D) White blood cells. E) Receptors.
 Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Hapten - a small molecule that is antigenic but not (by itself) immunogenic.
 Chapter 3. Antigens Terminology: Antigen: Substances that can be recognized by the surface antibody (B cells) or by the TCR (T cells) when associated with MHC molecules Immunogenicity VS Antigenicity:
Chapter 3. Antigens Terminology: Antigen: Substances that can be recognized by the surface antibody (B cells) or by the TCR (T cells) when associated with MHC molecules Immunogenicity VS Antigenicity:
CHAPTER 35 HUMAN IMMUNE SYSTEM STANDARDS:SC.912.L.14.52 & SC.912.L.14.6
 CHAPTER 35 HUMAN IMMUNE SYSTEM STANDARDS:SC.912.L.14.52 & SC.912.L.14.6 SECTION 1 - Infectious Disease 1.Identify the causes of infectious disease. 2.Explain how infectious diseases are spread. Causes
CHAPTER 35 HUMAN IMMUNE SYSTEM STANDARDS:SC.912.L.14.52 & SC.912.L.14.6 SECTION 1 - Infectious Disease 1.Identify the causes of infectious disease. 2.Explain how infectious diseases are spread. Causes
The Immune System and Disease
 Chapter 40 The Immune System and Disease Section 40 1 Infectious Disease (pages 1029 1033) This section describes the causes of disease and explains how infectious diseases are transmitted Introduction
Chapter 40 The Immune System and Disease Section 40 1 Infectious Disease (pages 1029 1033) This section describes the causes of disease and explains how infectious diseases are transmitted Introduction
Chapter 16: Innate Immunity
 Chapter 16: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity The Body s Defenses The body has 2 types of defense
Chapter 16: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity The Body s Defenses The body has 2 types of defense
Unit 9: The Lymphatic and Immune Systems NURSING PHYSIOLOGY (NRSG237)
 Unit 9: The Lymphatic and Immune Systems Dr. Moattar Raza Rizvi NURSING PHYSIOLOGY (NRSG237) Functions: Transports Excess Interstitial Fluid Back to Bloodstream Lymphatic vessels collect lymph from loose
Unit 9: The Lymphatic and Immune Systems Dr. Moattar Raza Rizvi NURSING PHYSIOLOGY (NRSG237) Functions: Transports Excess Interstitial Fluid Back to Bloodstream Lymphatic vessels collect lymph from loose
Supplemental Material CBE Life Sciences Education. Su et al.
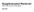 Supplemental Material CBE Life Sciences Education Su et al. APPENDIX Human Body's Immune System Test This test consists of 31 questions, with only 1 answer to be selected for each question. Please select
Supplemental Material CBE Life Sciences Education Su et al. APPENDIX Human Body's Immune System Test This test consists of 31 questions, with only 1 answer to be selected for each question. Please select
Immune System Memory Game
 Immune System Memory Game Recommended Age: 12 years old Time: 45 minutes Everyday our bodies come in contact with millions of tiny organisms and particles that could potentially make us sick. Despite this,
Immune System Memory Game Recommended Age: 12 years old Time: 45 minutes Everyday our bodies come in contact with millions of tiny organisms and particles that could potentially make us sick. Despite this,
Activation and effector functions of HMI
 Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Figure 14.2 Overview of Innate and Adaptive Immunity
 I M M U N I T Y Innate (inborn) Immunity does not distinguish one pathogen from another Figure 14.2 Overview of Innate and Adaptive Immunity Our first line of defense includes physical and chemical barriers
I M M U N I T Y Innate (inborn) Immunity does not distinguish one pathogen from another Figure 14.2 Overview of Innate and Adaptive Immunity Our first line of defense includes physical and chemical barriers
Recognition of T cell epitopes (Abbas Chapter 6)
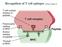 Recognition of T cell epitopes (Abbas Chapter 6) Functions of different APCs (Abbas Chapter 6)!!! Directon Routes of antigen entry (Abbas Chapter 6) Flow of Information Barrier APCs LNs Sequence of Events
Recognition of T cell epitopes (Abbas Chapter 6) Functions of different APCs (Abbas Chapter 6)!!! Directon Routes of antigen entry (Abbas Chapter 6) Flow of Information Barrier APCs LNs Sequence of Events
Unit Four. Human Anatomy & Physiology
 Human Anatomy & Physiology 16 Lymphatic System URLs http://www.howstuffworks.com/immune-system.htm http://www.thebody.com/step/immune.html http://www.emc.maricopa.edu/faculty/farabee/biobk/ BioBookIMMUN.html
Human Anatomy & Physiology 16 Lymphatic System URLs http://www.howstuffworks.com/immune-system.htm http://www.thebody.com/step/immune.html http://www.emc.maricopa.edu/faculty/farabee/biobk/ BioBookIMMUN.html
B Cell Generation, Activation & Differentiation. B cell maturation
 B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
B Cell Generation, Activation & Differentiation Naïve B cells- have not encountered Ag. Have IgM and IgD on cell surface : have same binding VDJ regions but different constant region leaves bone marrow
CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS
 CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS See APPENDIX (1) THE PRECIPITIN CURVE; (2) LABELING OF ANTIBODIES The defining characteristic of HUMORAL immune responses (which distinguishes them from CELL-MEDIATED
CHAPTER 2 ANTIGEN/ANTIBODY INTERACTIONS See APPENDIX (1) THE PRECIPITIN CURVE; (2) LABELING OF ANTIBODIES The defining characteristic of HUMORAL immune responses (which distinguishes them from CELL-MEDIATED
Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 14 The Lymphoid System and Immunity. Multiple-Choice Questions
 Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 14 The Lymphoid System and Immunity Multiple-Choice Questions 1) The lymphoid system is composed of A) lymphatic vessels. B) lymph nodes.
Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 14 The Lymphoid System and Immunity Multiple-Choice Questions 1) The lymphoid system is composed of A) lymphatic vessels. B) lymph nodes.
Core Topic 2. The immune system and how vaccines work
 Core Topic 2 The immune system and how vaccines work Learning outcome To be able to describe in outline the immune system and how vaccines work in individuals and populations Learning objectives Explain
Core Topic 2 The immune system and how vaccines work Learning outcome To be able to describe in outline the immune system and how vaccines work in individuals and populations Learning objectives Explain
Functions of Blood. Collects O 2 from lungs, nutrients from digestive tract, and waste products from tissues Helps maintain homeostasis
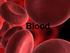 Blood Objectives Describe the functions of blood Describe blood plasma Explain the functions of red blood cells, white blood cells, and platelets Summarize the process of blood clotting What is Blood?
Blood Objectives Describe the functions of blood Describe blood plasma Explain the functions of red blood cells, white blood cells, and platelets Summarize the process of blood clotting What is Blood?
White Blood Cells (WBCs) or Leukocytes
 Lec.5 Z.H.Al-Zubaydi Medical Physiology White Blood Cells (WBCs) or Leukocytes Although leukocytes are far less numerous than red blood cells, they are important to body defense against disease. On average,
Lec.5 Z.H.Al-Zubaydi Medical Physiology White Blood Cells (WBCs) or Leukocytes Although leukocytes are far less numerous than red blood cells, they are important to body defense against disease. On average,
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer
 Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Immunity and how vaccines work
 1 Introduction Immunity is the ability of the human body to protect itself from infectious disease. The defence mechanisms of the body are complex and include innate (non-specific, non-adaptive) mechanisms
1 Introduction Immunity is the ability of the human body to protect itself from infectious disease. The defence mechanisms of the body are complex and include innate (non-specific, non-adaptive) mechanisms
The Lymphatic System. Dr. Naim Kittana, PhD
 The Lymphatic System Dr. Naim Kittana, PhD 1 Disclosure The material and the illustrations are adopted from the textbook Human Anatomy and Physiology / Ninth edition/ Eliane N. Marieb 2013 Dr. Naim Kittana,
The Lymphatic System Dr. Naim Kittana, PhD 1 Disclosure The material and the illustrations are adopted from the textbook Human Anatomy and Physiology / Ninth edition/ Eliane N. Marieb 2013 Dr. Naim Kittana,
BLOOD-Chp. Chp.. 6 What are the functions of blood? What is the composition of blood? 3 major types of plasma proteins
 6.1 Blood: An overview BLOOD-Chp Chp.. 6 What are the functions of blood? Transportation: oxygen, nutrients, wastes, carbon dioxide and hormones Defense: against invasion by pathogens Regulatory functions:
6.1 Blood: An overview BLOOD-Chp Chp.. 6 What are the functions of blood? Transportation: oxygen, nutrients, wastes, carbon dioxide and hormones Defense: against invasion by pathogens Regulatory functions:
Overview of the Cattle Immune System 1
 Oregon State University BEEF043 Beef Cattle Library Beef Cattle Sciences Overview of the Cattle Immune System 1 Reinaldo F. Cooke 2 Introduction On average, the U.S. cattle industry loses more than $1
Oregon State University BEEF043 Beef Cattle Library Beef Cattle Sciences Overview of the Cattle Immune System 1 Reinaldo F. Cooke 2 Introduction On average, the U.S. cattle industry loses more than $1
Autoimmunity and immunemediated. FOCiS. Lecture outline
 1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
Welcome to Mini Med School at the Child & Family Research Institute
 Glossary Welcome to Mini Med School at the Child & Family Research Institute On behalf of the Faculty and Staff at the Child & Family Research Institute (CFRI), we would like to welcome you to CFRI s
Glossary Welcome to Mini Med School at the Child & Family Research Institute On behalf of the Faculty and Staff at the Child & Family Research Institute (CFRI), we would like to welcome you to CFRI s
37 2 Blood and the Lymphatic System Slide 1 of 34
 1 of 34 Blood is a connective tissue that contains both dissolved substances and specialized cells. 2 of 34 The functions of blood include: collecting oxygen from the lungs, nutrients from the digestive
1 of 34 Blood is a connective tissue that contains both dissolved substances and specialized cells. 2 of 34 The functions of blood include: collecting oxygen from the lungs, nutrients from the digestive
Some terms: An antigen is a molecule or pathogen capable of eliciting an immune response
 Overview of the immune system We continue our discussion of protein structure by considering the structure of antibodies. All organisms are continually subject to attack by microorganisms and viruses.
Overview of the immune system We continue our discussion of protein structure by considering the structure of antibodies. All organisms are continually subject to attack by microorganisms and viruses.
T Cell Maturation,Activation and Differentiation
 T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
The Immune System. How your immune system works. Organs of the Immune System
 UW MEDICINE PATIENT EDUCATION The Immune System How your immune system works The immune system is a network of special cells, tissues, and organs that defend the body against attacks from foreign invaders,
UW MEDICINE PATIENT EDUCATION The Immune System How your immune system works The immune system is a network of special cells, tissues, and organs that defend the body against attacks from foreign invaders,
Final Review. Aptamers. Making Aptamers: SELEX 6/3/2011. sirna and mirna. Central Dogma. RNAi: A translation regulation mechanism.
 Central Dogma Final Review Section Week 10 DNA RNA Protein DNA DNA replication DNA RNA transcription RNA Protein translation **RNA DNA reverse transcription http://bass.bio.uci.edu/~hudel/bs99a/lecture20/lecture1_1.html
Central Dogma Final Review Section Week 10 DNA RNA Protein DNA DNA replication DNA RNA transcription RNA Protein translation **RNA DNA reverse transcription http://bass.bio.uci.edu/~hudel/bs99a/lecture20/lecture1_1.html
Antibody Structure, and the Generation of B-cell Diversity CHAPTER 4 04/05/15. Different Immunoglobulins
 Antibody Structure, and the Generation of B-cell Diversity B cells recognize their antigen without needing an antigen presenting cell CHAPTER 4 Structure of Immunoglobulin G Different Immunoglobulins Differences
Antibody Structure, and the Generation of B-cell Diversity B cells recognize their antigen without needing an antigen presenting cell CHAPTER 4 Structure of Immunoglobulin G Different Immunoglobulins Differences
Candy Antigens and Antibodies
 LAB ACTIVITY: Candy Antigens and Antibodies TEACHER S EDITION Curricular Links: Biology 20, Science 30 Class Time: 1 period Suggested Answers: Question 1: What is the main function of red blood cells?
LAB ACTIVITY: Candy Antigens and Antibodies TEACHER S EDITION Curricular Links: Biology 20, Science 30 Class Time: 1 period Suggested Answers: Question 1: What is the main function of red blood cells?
Immuno-Oncology Therapies to Treat Lung Cancer
 Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
2006 7.012 Problem Set 6 KEY
 2006 7.012 Problem Set 6 KEY ** Due before 5 PM on WEDNESDAY, November 22, 2006. ** Turn answers in to the box outside of 68-120. PLEASE WRITE YOUR ANSWERS ON THIS PRINTOUT. 1. You create an artificial
2006 7.012 Problem Set 6 KEY ** Due before 5 PM on WEDNESDAY, November 22, 2006. ** Turn answers in to the box outside of 68-120. PLEASE WRITE YOUR ANSWERS ON THIS PRINTOUT. 1. You create an artificial
The Human Immune System
 The Human Immune System What is the immune system? The body s defense against disease causing organisms, malfunctioning cells, and foreign particles The First Line of Defense Skin The dead, outer layer
The Human Immune System What is the immune system? The body s defense against disease causing organisms, malfunctioning cells, and foreign particles The First Line of Defense Skin The dead, outer layer
Name Date Class. This section explains what kinds of organisms cause infectious disease and how infectious diseases are spread.
 Fighting Disease Name Date Class Infectious Disease This section explains what kinds of organisms cause infectious disease and how infectious diseases are spread. Use Target Reading Skills Before you read,
Fighting Disease Name Date Class Infectious Disease This section explains what kinds of organisms cause infectious disease and how infectious diseases are spread. Use Target Reading Skills Before you read,
Immunity Unit Test Z
 Immunity Unit Test Z Name MB Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Which of the pathogens in Figure 31.1 cause disease by taking over healthy
Immunity Unit Test Z Name MB Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Which of the pathogens in Figure 31.1 cause disease by taking over healthy
Cardiovascular System. Blood Components
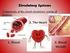 Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
Exercise 9: Blood. Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826.
 Exercise 9: Blood Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826. Blood Typing The membranes of human red blood cells (RBCs) contain a variety of cell surface proteins called
Exercise 9: Blood Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826. Blood Typing The membranes of human red blood cells (RBCs) contain a variety of cell surface proteins called
Why use passive immunity?
 Vaccines Active vs Passive Immunization Active is longer acting and makes memory and effector cells Passive is shorter acting, no memory and no effector cells Both can be obtained through natural processes:
Vaccines Active vs Passive Immunization Active is longer acting and makes memory and effector cells Passive is shorter acting, no memory and no effector cells Both can be obtained through natural processes:
SQA CfE Higher Human Biology Unit 4: Immunology and Public Health
 SCHOLAR Study Guide SQA CfE Higher Human Biology Unit 4: Immunology and Public Health Authored by: Eoin McIntyre Reviewed by: Sheena Haddow Previously authored by: Mike Cheung Eileen Humphrey Eoin McIntyre
SCHOLAR Study Guide SQA CfE Higher Human Biology Unit 4: Immunology and Public Health Authored by: Eoin McIntyre Reviewed by: Sheena Haddow Previously authored by: Mike Cheung Eileen Humphrey Eoin McIntyre
Overview. Transcriptional cascades. Amazing aspects of lineage plasticity. Conventional (B2) B cell development
 Overview B cell development Transcriptional cascades Amazing aspects of lineage plasticity Conventional (B2) B cell development What happens to an autoreactive B cell? B1 vs B2 cells Key anatomical sites
Overview B cell development Transcriptional cascades Amazing aspects of lineage plasticity Conventional (B2) B cell development What happens to an autoreactive B cell? B1 vs B2 cells Key anatomical sites
IMMUNE SYSTEM. The body s defense against:
 The body s defense against: IMMUNE SYSTEM disease causing organisms or infectious agents malfunctioning cells or abnormal body cells as cancer foreign cells or particles Basic Immunity Depends on the ability
The body s defense against: IMMUNE SYSTEM disease causing organisms or infectious agents malfunctioning cells or abnormal body cells as cancer foreign cells or particles Basic Immunity Depends on the ability
Immunology. B lymphocytes & Antibodies. 20.10.2014, Ruhr-Universität Bochum Marcus Peters, [email protected]
 Immunology B lymphocytes & Antibodies 20.10.2014, Ruhr-Universität Bochum Marcus Peters, [email protected] What is an antibody? An antibody is a glycoprotein, which specifically binds to a substance,
Immunology B lymphocytes & Antibodies 20.10.2014, Ruhr-Universität Bochum Marcus Peters, [email protected] What is an antibody? An antibody is a glycoprotein, which specifically binds to a substance,
MISSION DEBRIEFING: Teacher Guide
 Activity on the IMMUNE SYSTEM: The Body Fights Back In this activity, the students will use a hands-on approach to learn about the immune system and how it fights off pathogens that invade the body. They
Activity on the IMMUNE SYSTEM: The Body Fights Back In this activity, the students will use a hands-on approach to learn about the immune system and how it fights off pathogens that invade the body. They
ELISA BIO 110 Lab 1. Immunity and Disease
 ELISA BIO 110 Lab 1 Immunity and Disease Introduction The principal role of the mammalian immune response is to contain infectious disease agents. This response is mediated by several cellular and molecular
ELISA BIO 110 Lab 1 Immunity and Disease Introduction The principal role of the mammalian immune response is to contain infectious disease agents. This response is mediated by several cellular and molecular
Blood, Lymphatic and Immune Systems
 Component 3-Terminology in Healthcare and Public Health Settings Unit 4-Blood, Lymphatic and Immune Systems This material was developed by The University of Alabama at Birmingham, funded by the Department
Component 3-Terminology in Healthcare and Public Health Settings Unit 4-Blood, Lymphatic and Immune Systems This material was developed by The University of Alabama at Birmingham, funded by the Department
KEY CHAPTER 14: BLOOD OBJECTIVES. 1. Describe blood according to its tissue type and major functions.
 KEY CHAPTER 14: BLOOD OBJECTIVES 1. Describe blood according to its tissue type and major functions. TISSUE TYPE? MAJOR FUNCTIONS connective Transport Maintenance of body temperature 2. Define the term
KEY CHAPTER 14: BLOOD OBJECTIVES 1. Describe blood according to its tissue type and major functions. TISSUE TYPE? MAJOR FUNCTIONS connective Transport Maintenance of body temperature 2. Define the term
Given these characteristics of life, which of the following objects is considered a living organism? W. X. Y. Z.
 Cell Structure and Organization 1. All living things must possess certain characteristics. They are all composed of one or more cells. They can grow, reproduce, and pass their genes on to their offspring.
Cell Structure and Organization 1. All living things must possess certain characteristics. They are all composed of one or more cells. They can grow, reproduce, and pass their genes on to their offspring.
The Structure and Function of the Lymphatic System
 The Structure and Function of the Lymphatic System The lymphatic system runs though the body and is made up of organs and lymphatic tissue, this includes organs like the spleen and thymus and also lymphatic
The Structure and Function of the Lymphatic System The lymphatic system runs though the body and is made up of organs and lymphatic tissue, this includes organs like the spleen and thymus and also lymphatic
Asthma (With a little SCID to start) Disclosures Outline Starting with the Immune System The Innate Immune System The Adaptive Immune System
 1 2 3 4 5 6 7 8 9 Asthma (With a little SCID to start) Lauren Smith, MD CHKD Pediatric Allergy/Immunology Disclosures None Will be discussing some medications that are not yet FDA approved Outline SCID
1 2 3 4 5 6 7 8 9 Asthma (With a little SCID to start) Lauren Smith, MD CHKD Pediatric Allergy/Immunology Disclosures None Will be discussing some medications that are not yet FDA approved Outline SCID
Understanding the Immune System
 Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases National Cancer Institute Understanding
Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases National Cancer Institute Understanding
MHC (MAJOR HISTOCOMPATIBILITY COMPLEX)
 MHC (MAJOR HISTOCOMPATIBILITY COMPLEX) MHC complex is group of genes on a single chromosome that codes the MHC antigens. Major as well as minor histocompatibility antigens (also called transplantation
MHC (MAJOR HISTOCOMPATIBILITY COMPLEX) MHC complex is group of genes on a single chromosome that codes the MHC antigens. Major as well as minor histocompatibility antigens (also called transplantation
Immunology Ambassador Guide (updated 2014)
 Immunology Ambassador Guide (updated 2014) Immunity and Disease We will talk today about the immune system and how it protects us from disease. Also, we ll learn some unique ways that our immune system
Immunology Ambassador Guide (updated 2014) Immunity and Disease We will talk today about the immune system and how it protects us from disease. Also, we ll learn some unique ways that our immune system
Cytotoxic T Lymphocytes (CTLs) and NK Cells. Effector T cells. After activation, naïve T cells differentiate into effector and memory T cells
 After activation, naïve T cells differentiate into effector and memory T cells Cytotoxic T Lymphocytes (CTLs) and NK Cells After activation, T cells remain in lymph nodes for 5-6 days Effector T cells
After activation, naïve T cells differentiate into effector and memory T cells Cytotoxic T Lymphocytes (CTLs) and NK Cells After activation, T cells remain in lymph nodes for 5-6 days Effector T cells
SYSTEM Teacher Pages THE IMMUNE. Your students will learn:
 Grade Level 3-5 Sergeant Cell s Immune System Defense Team Webquest Activity Summary Comparing immune cells with a police team, the webquest activity guides students to research the immune system online.
Grade Level 3-5 Sergeant Cell s Immune System Defense Team Webquest Activity Summary Comparing immune cells with a police team, the webquest activity guides students to research the immune system online.
Chapter 18: Applications of Immunology
 Chapter 18: Applications of Immunology 1. Vaccinations 2. Monoclonal vs Polyclonal Ab 3. Diagnostic Immunology 1. Vaccinations What is Vaccination? A method of inducing artificial immunity by exposing
Chapter 18: Applications of Immunology 1. Vaccinations 2. Monoclonal vs Polyclonal Ab 3. Diagnostic Immunology 1. Vaccinations What is Vaccination? A method of inducing artificial immunity by exposing
Antibody Function & Structure
 Antibody Function & Structure Specifically bind to antigens in both the recognition phase (cellular receptors) and during the effector phase (synthesis and secretion) of humoral immunity Serology: the
Antibody Function & Structure Specifically bind to antigens in both the recognition phase (cellular receptors) and during the effector phase (synthesis and secretion) of humoral immunity Serology: the
Mechanical barriers are a crucial first line of defence. It would be impossible to provide an exhaustive list. Two examples are:
 Back to Index 1. The immune response to infection 1. Non-specific immunity The immune system has evolved to deal with infectious pathogens. There are several lines of host defence. When evaluating the
Back to Index 1. The immune response to infection 1. Non-specific immunity The immune system has evolved to deal with infectious pathogens. There are several lines of host defence. When evaluating the
Selective IgA deficiency (slgad) [email protected] 0800 987 8986 www.piduk.org
 Selective IgA deficiency (slgad) [email protected] 0800 987 8986 www.piduk.org About this booklet This booklet provides information on selective IgA deficiency (sigad). It has been produced by the PID UK
Selective IgA deficiency (slgad) [email protected] 0800 987 8986 www.piduk.org About this booklet This booklet provides information on selective IgA deficiency (sigad). It has been produced by the PID UK
Reproductive System & Development: Practice Questions #1
 Reproductive System & Development: Practice Questions #1 1. Which two glands in the diagram produce gametes? A. glands A and B B. glands B and E C. glands C and F D. glands E and F 2. Base your answer
Reproductive System & Development: Practice Questions #1 1. Which two glands in the diagram produce gametes? A. glands A and B B. glands B and E C. glands C and F D. glands E and F 2. Base your answer
Dendritic Cells: A Basic Review *last updated May 2003
 *last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
*last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
CHAPTER 9 IMMUNOGLOBULIN BIOSYNTHESIS
 CHAPTER 9 IMMUNOGLOBULIN BIOSYNTHESIS Although the process by which a functional gene for immunoglobulin HEAVY and LIGHT CHAINS is formed is highly unusual, the SYNTHESIS, POST- TRANSLATIONAL PROCESSING
CHAPTER 9 IMMUNOGLOBULIN BIOSYNTHESIS Although the process by which a functional gene for immunoglobulin HEAVY and LIGHT CHAINS is formed is highly unusual, the SYNTHESIS, POST- TRANSLATIONAL PROCESSING
Viral Attack! Your Clean-Up Crew to the Rescue! A Gallery Demonstration at Arizona Science Center
 Viral Attack! Your Clean-Up Crew to the Rescue! A Gallery Demonstration at Arizona Science Center Table of Contents Background Information Links Background Information What is the immune system? Our body
Viral Attack! Your Clean-Up Crew to the Rescue! A Gallery Demonstration at Arizona Science Center Table of Contents Background Information Links Background Information What is the immune system? Our body
Effector Mechanisms of Humoral Immunity
 Immunologie II für Naturwissenschaftler Effector Mechanisms of Humoral Immunity Beda M. Stadler Institute of Immunology Inselspital Bern, Switzerland http://www.immunology.unibe.ch/teaching/imm2/immuno2.htm
Immunologie II für Naturwissenschaftler Effector Mechanisms of Humoral Immunity Beda M. Stadler Institute of Immunology Inselspital Bern, Switzerland http://www.immunology.unibe.ch/teaching/imm2/immuno2.htm
The Circulatory System. Chapter 17 Lesson 1
 The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
Immune and Lymphatic Systems
 1. All of the following organs actively FIGHT pathogens EXCEPT: a. Cervical lymph nodes b. Tonsils c. Spleen d. Thymus e. Axillary lymph nodes 2. T lymphocytes gain immunocompetence within the: a. Bone
1. All of the following organs actively FIGHT pathogens EXCEPT: a. Cervical lymph nodes b. Tonsils c. Spleen d. Thymus e. Axillary lymph nodes 2. T lymphocytes gain immunocompetence within the: a. Bone
Types, production of antibodies and Antibody/antigen interaction
 Types, production of antibodies and Antibody/antigen interaction Antibodies Secreted by B lymphocytes Great diversity and specificity: >109 different antibodies; can distinguish between very similar molecules
Types, production of antibodies and Antibody/antigen interaction Antibodies Secreted by B lymphocytes Great diversity and specificity: >109 different antibodies; can distinguish between very similar molecules
VPM 152. INFLAMMATION: Chemical Mediators
 General Pathology VPM 152 INFLAMMATION: Chemical Mediators CHEMICAL MEDIATORS OF INFLAMMATION Definition: any messenger that acts on blood vessels, inflammatory cells or other cells to contribute to an
General Pathology VPM 152 INFLAMMATION: Chemical Mediators CHEMICAL MEDIATORS OF INFLAMMATION Definition: any messenger that acts on blood vessels, inflammatory cells or other cells to contribute to an
Understanding How Existing and Emerging MS Therapies Work
 Understanding How Existing and Emerging MS Therapies Work This is a promising and hopeful time in the field of multiple sclerosis (MS). Many new and different therapies are nearing the final stages of
Understanding How Existing and Emerging MS Therapies Work This is a promising and hopeful time in the field of multiple sclerosis (MS). Many new and different therapies are nearing the final stages of
1.1.2. thebiotutor. AS Biology OCR. Unit F211: Cells, Exchange & Transport. Module 1.2 Cell Membranes. Notes & Questions.
 thebiotutor AS Biology OCR Unit F211: Cells, Exchange & Transport Module 1.2 Cell Membranes Notes & Questions Andy Todd 1 Outline the roles of membranes within cells and at the surface of cells. The main
thebiotutor AS Biology OCR Unit F211: Cells, Exchange & Transport Module 1.2 Cell Membranes Notes & Questions Andy Todd 1 Outline the roles of membranes within cells and at the surface of cells. The main
Understanding the Immune System
 Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases Artwork by Jeanne Kelly Understanding
Understanding the Immune System How It Works U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES NATIONAL INSTITUTES OF HEALTH National Institute of Allergy and Infectious Diseases Artwork by Jeanne Kelly Understanding
TEMA 10. REACCIONES INMUNITARIAS MEDIADAS POR CÉLULAS.
 TEMA 10. REACCIONES INMUNITARIAS MEDIADAS POR CÉLULAS. The nomenclature of cytokines partly reflects their first-described function and also the order of their discovery. There is no single unified nomenclature,
TEMA 10. REACCIONES INMUNITARIAS MEDIADAS POR CÉLULAS. The nomenclature of cytokines partly reflects their first-described function and also the order of their discovery. There is no single unified nomenclature,
2161-1 - Page 1. Name: 1) Choose the disease that is most closely related to the given phrase. Questions 10 and 11 refer to the following:
 Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Blood: The Body s Vital Defense Force
 Blood: The body s vital defense force Ouch you ve cut your finger! A familiar red substance oozes out. As you reach for a bandage, take a moment to ponder the vital role this remarkable fluid performs.
Blood: The body s vital defense force Ouch you ve cut your finger! A familiar red substance oozes out. As you reach for a bandage, take a moment to ponder the vital role this remarkable fluid performs.
Biological cell membranes
 Unit 14: Cell biology. 14 2 Biological cell membranes The cell surface membrane surrounds the cell and acts as a barrier between the cell s contents and the environment. The cell membrane has multiple
Unit 14: Cell biology. 14 2 Biological cell membranes The cell surface membrane surrounds the cell and acts as a barrier between the cell s contents and the environment. The cell membrane has multiple
Chapter 19 Ci C r i cula l t a i t o i n
 Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
