The increasing use of implanted cardiac pacemakers (ICP) and cardioverter/defibrillators
|
|
|
- Elijah Barrett
- 10 years ago
- Views:
Transcription
1 Safety of Electronic Apex Locators and Pulp Testers in Patients With Implanted Cardiac Pacemakers or Cardioverter/Defibrillators Brian L. Wilson, DMD,* Craig Broberg, MD, J. Craig Baumgartner, DDS, PhD,* Chris Harris, DMD,* and Jack Kron, MD Abstract The purpose of this study was to determine if electronic apex locators (EAL) or electric pulp testers (EPT) interfere with the function of implanted cardiac pacemakers (ICP) or cardioverter/defibrillators (ICD). Twenty-seven patients with ICPs or ICDs had continuous electrocardiogram monitoring and device interrogation to detect interferences during the use of two types of EALs and one EPT. No interferences were detected by any ICP or ICD. In six patients, with intermittent pacing, a significant increase in pacing was observed during EAL/EPT stimulation (p 0.05). Examination of RR intervals (a measure of intrinsic heart rate) demonstrated significantly longer RR intervals (slower intrinsic heart rate) during EAL/EPT stimulation (p 0.05). Evaluation of the electrocardiograms for each patient failed to show any abnormalities in pacing during testing. These findings led us to conclude that the increased pacing frequency observed was related to a slower intrinsic heart rate and not electrical interference with the cardiac devices. In conclusion, the two EALs and one EPT used in this study did not interfere with the functioning of any of the cardiac devices tested. (J Endod 2006;32: ) Key Words Electronic apex locators, electronic pulp testers, implanted cardiac pacemakers, implanted cardioverter/ defibrillators From the *Department of Endodontology, and Division of Cardiology, Oregon Health & Science University, Portland, Oregon. Address requests for reprint to Dr. Brian L. Wilson, Department of Endodontology, School of Dentistry, Oregon Health & Science University, 611 SW Campus Drive, Portland, OR address: [email protected] /$0 - see front matter Copyright 2006 by the American Association of Endodontists. doi: /j.joen The increasing use of implanted cardiac pacemakers (ICP) and cardioverter/defibrillators (ICD) raises concern regarding electrical interference that might cause device dysfunction or patient harm. In dentistry, the electric pulp tester (EPT) and electronic apex locator (EAL), which are approved by the Food and Drug Administration, are routinely used in providing endodontic treatment. Both of these devices apply an electric current directly to the patient s oral tissues. The American Association of Endodontics estimates that nearly 16 million root canal procedures are performed every year (1). It is likely that patients with ICP/ICDs needing endodontic care will be encountered frequently. The dental profession has become increasingly aware of the possibility of electrical interference in patients with ICP/ICDs. Currently, EALs and EPTs are not recommended for use in patients with ICPs (2, 3). No current recommendations from the manufactures (2, 3) exist for their use in patients with ICDs. However, because of the variety and sophistication of systems available and lack of current research, there is confusion over which dental equipment should be a cause for concern. The ICP and ICD are battery powered and implanted subcutaneously in either the pectoral or abdominal location. The devices are connected to the heart by electrodes and lead wires through which the cardiac rhythm is monitored and treatment, when indicated, is delivered by sending electrical charges to the heart. The life span of these devices is primarily determined by their battery, which lasts from 3 to 10 yr depending on the specific device and functions. Pacemakers correct bradycardia or an abnormal heart rate by stimulating (pacing) the heart. The first ICP was implanted in 1958 (4). Pacemakers at this time were nonprogrammable, asynchronous (fixed rate) devices that stimulate (pace) the heart, usually the ventricle (single chamber), continuously at a predetermined (fixed) rate. Since then, ICPs have evolved into multiprogrammable, synchronous (demand) devices that stimulate the heart, ventricle and or atrial (dual chamber), only when needed. Defibrillators function to correct cardiac arrhythmias. The first ICD was implanted in 1980, and ICD use was approved by the Food and Drug Administration in 1985 (5). Many of the ICDs today have incorporated pacing functions that allow them to treat patients with both bradycardias and tachycardias (6). Tachycardia, depending on the severity, can be treated by antitachycardia pacing, cardioversion pulses, or defibrillating shocks for more seriuous arrhythmias such as ventricular fibrillation (7). The function of ICDs and most ICPs is to sense the intrinsic cardiac electrical activity and deliver appropriate electrical therapy to the heart when indicated. Electromagnetic interference may interfere with the function of these cardiac devices in several ways. Interpretation of an extraneous electrical signal as a cardiac signal in origin may temporarily inhibit pacing of an ICP (8). With ICDs, the electrical signal may be sensed and result in antitiachycardia pacing or the delivery of an inappropriate defibrillating shock (9). The electrical signal may by interpreted as noise and temporarily cause reversion of an ICP to an asynchronous pacing mode, or the signal may inappropriately reprogram the cardiac device (8). Conducted electrical energy, such as that produced from electrocautery, may travel down the lead wires to the heart and induce ventricular or atrial fibrillation (8). EALs are used to determine working length within a tooth for endodontic treatment by measuring the electrical impedance between two electrodes using multiple signal frequencies (10). The accuracy of EALs in determining working length has led to a JOE Volume 32, Number 9, September 2006 Safety of Apex Locators and Pulp Testers 847
2 decrease in the number of radiographs required during root canal treatment (10). EPTs are used to determine vitality of pulpal tissue within teeth. During testing, the strength of the stimulus is increased from 15 to 350 volts, for the device used in this study (2). The value of EPTs lies in their ability to determine pulp vitality since other noninvasive vitality testing (thermal testing) becomes less reliable as people age (11). The available literature evaluating interference between EAL/EPTs and ICP/ICDs is limited, and conclusions are difficult to draw. There is only one study evaluating the effects of EALs on pacemakers. In 2002, an in vitro study reported that four out of five EALs tested with a single pacemaker showed normal pacing and only one produced an irregular pace recording on an oscilloscope (12). In 1974, an in vivo study using dogs showed that an EPT caused mode switching in a pacemaker to fix rate pacing (13). That study is commonly cited as a rationale for not using EPTs in patients with ICPs. However, in 1974 ICPs were relatively immature in the evolution of pacemaker sophistication. Further, the type of interference that was reported would not be problematic to patients, since functional pacing continued. Three more recent in vitro studies reported no effects of EPTs on pacemakers (14 16). Only two studies evaluate the effect of EPT use on ICPs in humans. In 1975, an in vivo study reported no effect in a selected subset of 14 patients using various ICPs (by Medtronic, Cordis, and General Electric) evaluated by electrocardiography (17). None of the ICPs tested are implanted in patients today. In 1991, a group in Germany studied EPT use in 26 patients with ICPs. The report found no interference from EPT use on pacemaker rate or electrocardiogram morphology (18). EALs were not tested, and patients with ICDs were not included. A 1996 case reported on a patient with a fixed-rate pacemaker requiring root-canal treatment. Under consultation with the patient s cardiologist, an EAL was used. The patient experienced no adverse effects immediately or with follow-up (19). To our knowledge, no other human in vivo data is available on interactions of EALs with ICPs, and no data is available on the effects of any electrical dental device with ICDs. Currently, manufacturers of EPTs and EALs warn against using these devices in patients with ICPs (2, 3). Such warnings are based on speculation of potential risk of electromagnetic interference (EMI) rather than on scientific evidence. The purpose of the current study was to evaluate possible interactions of EPL/EAT use on ICP/ICDs in adult patients. Methods Patient Recruitment The study protocol was approved by the Oregon Health & Science University Institutional Review Board before enrolling patients. All patients aged 18 to 90 of any race or gender with working ICPs or ICDs were eligible for enrollment. The first five patients were recruited before their scheduled operation for their ICP/ICD generator change in the electrophysiology laboratory, where ready cardiovascular support and physical access to the device were available. The remaining patients were recruited after their regularly scheduled follow-up visit in the cardiology clinic. Patients who would not give written, informed consent were not enrolled. Patients who were pacemaker dependent (an intrinsic heart rate less than 40 beats/min) were excluded from this study. All willing patients signed informed consent before participation. Each of the first five patients was placed under conscious sedation and local anesthesia per usual protocols. After the existing cardiac device and lead ends had been exposed, but still in the tissue pocket, the telemetry wand was placed over the device in a sterile plastic sleeve for testing. The remainder of the implant operation proceeded under the TABLE 1. Specifications of Dental Equipment Tested EAL1 EAL2 EPT Device name Root ZX Endo Analyzer Endo Analyzer Voltage 80 mv AC 2 V AC V AC Amperes 10 ua 10 ua 1.5 ma (maximum) Frequency KHz KHz 10 KHz Power supply 7.5 V DC 9.0 V DC 9.0 V DC EAL1, electronic apex locator #1; EAL2, electronic apex locator #2; EPT, electronic pulp tester. direction of the supervising electrophysiologist. After these first five patients, all results were reviewed for any occurrence of adverse events by a cardiologist (CSB). As no adverse events were noted in the first five patients, additional patients were enrolled during their regularly scheduled follow-up visit in the cardiology clinic. The following data were obtained from each patient: age, gender, type of implanted cardiac device, manufacturer, date of implant, indication for original implant, and number and position of leads. Each device was interrogated to obtain mode, bradycardia pacing parameters, sensing parameters, rhythm detection, and therapy parameters. When necessary, pacing rate was decreased to document the underlying rhythm then returned to its previous rate. In patients with ICDs, tachyarrhythmia therapies (i.e. defibrillating shocks) were disabled. In some devices (Ventritex), disabling tachyarrhythmia therapies also disabled tachyarrhythmia sensing, leaving only bradycardia pacing capabilities. Otherwise, there were no changes in any setting made to any device. All patients were told they could stop any time by raising their hand. Patients were awake during testing with the telemetry wand in place. Stimulation Protocol The dental devices tested were: (a) Root ZX (Morita Corp, Irvine, CA) and (b) Endo Analyzer Model 8005 (Sybron Endo, Orange, CA). The Root ZX is an electronic apex locator. The Endo Analyzer has dual functions as an electonic apex locator and electric pulp tester. Device specifications are shown in Table 1. With the telemetry wand in place, the surface and intracardiac electrocardiogram were continuously printed during testing, which consisted of seven phases each lasting 30 s. During the test, the rhythm was continuously observed by a cardiologist (CSB). Phase 1 (Rest 1) was recorded at rest, to serve as a baseline of normal device function. Phase 2 (EAL1) was recorded during stimulation with the Root ZX, followed by phase 3 without stimulation (rest 2). Phase 4 (EAL2) was during stimulation with the Endo Analyzer in the electronic apex locator mode, followed by phase 5 without stimulation (rest 3). Phase 6 (EPT) was during stimulation with the Endo Analyzer in the electric pulp tester mode, followed by phase 7 without stimulation (rest 4). Following all recordings, each device was interrogated to check for program changes, mode switching or tachyarrhythmia sensing, and all tachyarrhythmia therapies were enabled. The EALs and EPT were employed to simulate normal clinical use by a practicing dentist (BLW). The contrary electrode was placed in contact with the patient s buccal mucosa using a metal clip placed in the corner of the mouth. The primary electrode (probe) was held in contact with each patient s gingival tissue. We did not have the patient hold the contrary electrode with their hand as is sometimes done in clinical practice. Function of EAL/EPTs was monitored to ensure good contact, but data from the devices were not recorded or analyzed. Predetermined criteria for cessation of EAL/EPT use were: ventricular pause 2 s, detection of ventricular tachyarrhythmia by the defibrillator, sudden unexplained observable mode switch from the pacemaker, syncope, patient discomfort, or preference. 848 Wilson et al. JOE Volume 32, Number 9, September 2006
3 Data Analysis All printed electrocardiograms were reviewed after the completion of the protocol. Each phase was reviewed, and the following data recorded: number of intrinsic heart beats, number of premature beats, number of paced beats, and RR interval (time duration between two consecutive R waves for each beat on the electrocardiogram). For all patients who were 100% ventricular paced (three total) the mean RR interval in milliseconds (pacing frequency) for each phase of testing were assessed. For all intermittently paced patients (six total) the percent of pacing (paced beats / total beats) for each phase of testing were assessed. For all patients who were not 100% paced (24 total), which includes intermittently paced patients (six total) and patients who had no pacing activity during testing (18 total), the mean RR interval in milliseconds for all naturally occurring heart beats, a measure of the intrinsic heart rate, for each phase of testing were assessed. The differences between phases for the pacing frequency, percent of pacing, and intrinsic heart rate were assessed with paired t tests. The following grouping of data was used for this analysis: (a) stimulation phases in total (EAL1, EAL2, and EPT) versus the rest phases in total (rest 1-4), and (b) each stimulation phase individually versus the rest phases in total. Differences between the rest phases were assessed with ANOVA. The data were examined for any evidence of abnormal sensing, abnormal detection of tachyarrhythmia, abnormal device mode switching or program changes. Of the 27 patients tested, only seven had devices that recorded RR intervals on the electrocardiograms. For the other 20 devices, the RR interval for each heart beat was manually recorded by measuring the distance between each R wave on the printed electrocardiogram using a digital micrometer (Mitutoyo, Tokyo, Japan), accurate to within 0.02 mm. The RR intervals for the seven patients with the recorded RR intervals on the electrocardiogram were also measured manually. These measurements were done in a blinded fashion by covering the RR interval data recorded on the electrocardiogram by the cardiac device until all the manual measurements were complete. The manually recorded RR interval data was compared with the RR interval data recorded by the cardiac devices for these seven patients using paired t-test. The results revealed no significant difference between the manually recorded RR interval and the RR interval recorded by the cardiac devices (p 0.425, mean difference 1.17 ms, SD ms). All data analysis involving RR interval data was performed with both the manually measured and device recorded RR intervals for these seven patients, with no significant differences seen in the results. The following results presented were obtained using the device recorded RR interval data for the seven patients for which it was available and the manually recorded RR interval data for the 20 patients in which the device recorded data was not available. Results Patients Approximately half of the patients declined to participate, either because of unwillingness, pacemaker dependence, or inability to give informed consent. Twenty-seven patients were included in the study, five in the electrophysiology laboratory, and 22 in the cardiology clinic. The details of the patient population with average settings for tachycardia therapies and bradycardia pacing are listed in Table 2. All patients were able to complete the testing protocol and no patient complained of significant discomfort during or after testing. Summary of the cardiac devices tested are found in Table 3. Twenty-three (85%) of the implanted devices were ICDs and four (15%) were ICPs. Five devices had been implanted in the left abdomen, while all others had been implanted in the left pectoral region. The leads of the cardiac devices TABLE 2. Patient and Device Characteristics Mean S.D. Age Gender (f/m) 9/18 Years since implant Sensitivity of v lead (mv) Lower rate bpm Detection thresholds VT (ms) VF (ms) Device indication (no.) VT 15 (55%) VF 8 (30%) Sick sinus syndrome 2 (7%) Atrioventricular block 1 (4%) Tachy/brady syndrome 1 (4%) VT, ventricular tachycardia; VF, ventricular fibrillation. tested represented a range of types and manufacturers, and included four true bipolar leads, eight types of integrated bipolar leads, and one epicardial patch. Only two patients were in DDD pacing mode, while all other patients were in VVI pacing mode. These letters describe the pacing mode as set forth by the NBG (North American Society of Pacing and Electrophysiology/British Pacing and Electrophysiology Group Generic Pacemaker Code). DDD is the NBG code for dual-chamber pacing, which is pacing and sensing in both the atrium and ventricle with dual responses (inhibited or triggered pacing) to sensing of an intrinsic heart beat. VVI is the NBG code for ventricle pacing in which pacing and sensing occur only in the ventricle and pacing is inhibited if an intrinsic heart beat is sensed. Four of the 27 patients had active rate-modulation programming that use special sensors or programming to monitor body changes (motion of limbs, respiratory rate or changes in the intrinsic heart rate) to help adjust the heart rate to meet the changing demands of the body. Rate-modulation programming is denoted by the letter R in the fourth position of the NBG code (i.e. DDDR, VVIR). Results of Testing No adverse events were detected in any patient. Specifically, there were no periods of abnormal detection by any pacemaker, no ICD detected any tachyarrhythmia, and no artifacts were observed on any of the intracardiac electrocardiograms. No patient experienced palpitations or any cardiovascular symptom. Eight of the 27 patients were in normal sinus rhythm during the entire study. Nine patients experienced premature beats. In eight of these patients, ectopic beats were encountered with equal frequency throughout the study both with and without EAL/EPT use (including patient #1, who had periods of frequent ectopy including trigeminy and interrupted pacing, but no discernable difference with or without EAL/ EPT use). In patient #16, six PVCs were encountered with EAL/EPT use and eight without, however, all six PVCs during dental device testing occurred during EAL2, with none experienced during testing with EAL1 or EPT. The PVC s were seen on both surface and intracardiac electrograms, and were not thought to represent electrical artifact. Nine of the 27 patients were actively paced during the study. Of these nine patients, three were 100% ventricular paced. This includes patient #5 who was 100% ventricular paced during all test phases except in phase 5 (rest 3) and phase 6 (EPT) in which pacing occurred 88% and 89%, respectively. Patient #5, during these phases, had episodes of intrinsic heartbeats occurring before the programmed interval for delivery of a paced beat. Two of the three patients who were not 100% ventricular paced did not have ratemodulation programming, which includes patient #5. For these pa- JOE Volume 32, Number 9, September 2006 Safety of Apex Locators and Pulp Testers 849
4 TABLE 3. Summary of Devices Tested and Outcome ICDs Pt# Device Mode rest EAL1 rest EAL2 rest EPT rest Guidant 7 Ventak Prizm 2 VR 1860 VVI nsr nsr nsr nsr nsr nsr nsr 9 Ventak Prizm 2 VR 1860 VVI nsr nsr nsr nsr nsr nsr nsr 12 Ventak Prizm VR 1850 VVI nsr nsr nsr 1 pc 2 pc nsr nsr 20 Ventak Mini 2920 VVI nsr nsr nsr nsr nsr nsr nsr 21 Ventak Prizm VR 1850 VVIR 29% 30% 9% 29% 12% 38% 9% 22 Ventak Prizm 2 VR 1860 VVI sb sb sb sb sb sb sb 25 Ventak Mini IV 2920 VVI 0% 27% 0% 26% 0% 31% 0% Medtronic 1 Jewel 7220 VVI* 10% 28% 16% 3% 15% 6% 15% 2 Gem III R 7231cx VVI* nsr nsr nsr nsr nsr 1 pc nsr 3 Gem II DR 7273 DDD 100% 100% 100% 100% 100% 100% 100% 4 Gem DR 7271 VVI nsr 1 pc nsr nsr nsr nsr 1 pc 6 Micro Jewel 7221 VVI* nsr nsr nsr nsr nsr nsr nsr 8 Micro Jewel II 7223 cx VVI afib afib afib afib afib afib afib 10 Gem III VR 7231 VVI 3 pc 3 pc 2 pc 3 pc 4 pc 2 pc 3 pc 13 Gem II VR 7229 VVI nsr nsr nsr nsr nsr nsr nsr 16 Micro Jewel 7223 VVI 2 pc nsr 1 pc 6 pc 1 pc nsr 4 pc 19 Micro Jewel 7221 VVI* nsr nsr nsr nsr nsr nsr nsr 24 Gem 7227 VVI 1 pc nsr 1 pc 1 pc 2 pc 1 pc 2 pc 27 Gem II VR 7229 VVI 1 pc nsr nsr nsr nsr nsr nsr Ventritex 5 V-186 HV3 Profile MD VVI 100% 100% 100% 100% 88% 89% 100% 11 V-185 D Contour II VVI* nsr 1 pc nsr nsr nsr nsr nsr 23 V-185 AC Contour II VVI nsr nsr nsr nsr nsr nsr nsr 26 V-186 HV3 Profile MD VVI sa sa sa sa sa sa sa Pacemakers Medtronic 14 Kappa KDR 901 VVI 47% 74% 47% 52% 61% 71% 73% 15 Elite 7076 DDDR 4% 10% 7% 14% 10% 31% 10% 17 Kappa KSR 401/403 VVIR 100% 100% 100% 100% 100% 100% 100% 18 Sigma SSR 303 VVIR 46% 71% 39% 44% 44% 42% 35% Devices tested grouped by type and manufacturer. Because Ventritex tachyarrhythmia therapics could not be turned off without also turning off sensing, these essentially were bradypacing only devices at the time of testing. Devices implanted into left upper abdomen are denoted by (*), all other devices were implanted in left pectoral region. nsr, normal sinus rhythm; pc, premature ventricular contraction; sb, sinus bradycardia; afib, atrial fibrillation; sa, sinus arrhythmia. Numbers indicate percent ventricular paced, with underlying sinus rhythm, except Pt 15 who was 100% atrially paced. tients there was no change in the pacing interval (RR interval of paced beats) between any of the rest phases or stimulation phases with the dental devices. The RR interval for each paced beat remained constant throughout testing with these two patients with no delayed or premature pacing. The third 100% ventricular paced patient, patient #17, had rate-modulation programming turned on. During stimulation with the dental devices (EAL1, EAL2, and EPT), the pacing frequency (paced heart rate) decreased slightly to a rate of 61, 59, and 59 ppm (paced beats per minute), respectively, as evidenced by the increasing RR interval between paced beats. Over the subsequent 30-s rest phases, after the stimulation was stopped, the pacing frequency increased to about 63 ppm by the end of the rest phases. The device was a Medtronic Kappa KSR 401 pacemaker that had been placed 6 wk earlier for tachy/brady syndrome. Pacing mode was VVIR. The rate-modulation programming included 9% activity of daily living rate, which adjusted the paced heart rate in accordance with changes in the respiratory rate. The optimization for the rate-modulation was on, and activity contribution set at minimum. The change in the pacing frequency throughout testing did not exceed the 9% activity of daily living rate. Changes in the paced heart rate during testing may be explained by changes in the patients respiratory rate during testing. Breath holding by the patient during the stimulation phases, when the probe was contacted to the oral cavity, would result in a detectable decrease in the respiratory rate over the 30 s period and result in slower pacing as measured by an increasing RR interval. A return to a normal breathing pattern by the patient, after the removal of the dental device probe from their mouth, would result in an increase in the pacing frequency to the normal resting rate as determined by their respiratory rate at rest. Six patients were paced intermittently during the testing protocol. The percent of pacing during the combined stimulation phases with the dental devices (EAL1, EAL2, and EPT) shows a significant increase in pacing compared to the combined nonstimulation rest phases; 34.8% versus 22.4%, respectively (p 0.026). No significant difference in the percent of pacing between the four separate rest phases 1 through 4 was detected (p 0.988). Evaluation of each stimulation phase independently shows a significant increase in the percent of pacing during EAL1 (43.4%, p 0.026), EPT (38.4%, p 0.023) and a nonsignificant trend of an increase in pacing during EAL2 use (30.9%, p 0.148) compared to the percent of pacing of the combined rest phases (22.4%) (Fig. 1). The intrinsic (natural) heart rate for all patients who were not continuously (100%) paced was evaluated by comparing the mean RR interval for each phase of testing. The mean RR intervals of the stimulation phases (EAL1, EAL2, and EPT), assessed combined or individually, were significantly longer than the mean RR interval of the combined rest phases (p values 0.001); (Fig. 2). The average increase in the mean RR interval during the stimulation phases was 32 ms, which is a decrease in the heart rate of about 2 bpm. No significant difference in the mean RR interval between the four separate rest phases 1 through 4 was detected (p 0.946). Fig. 3 is an example of patient #23 showing the change in the heart rate, as measured by the RR interval, over the entire testing protocol. Examination of the RR intervals on the electrocardiograms of all patients in regards to the interval between each paced beat and the preceding heart beat revealed the following. First, for all patients without rate-modulation programming, each paced beat occurred at the time interval determined by the programming of the cardiac device. There was no detection of any delayed or premature pacing during the testing protocol. Second, for all patients with rate-modulation programming, each paced beat occurred within the specific range as determined by the cardiac device programming. 850 Wilson et al. JOE Volume 32, Number 9, September 2006
5 Figure 1. The mean percent of pacing of each phase of testing for the six patients (#1, 14, 15, 18, 21, and 25) with intermittent pacing. Significant differences (**) for EAL1 (p 0.026, SE ), EPT (p 0.023, SE ) and a nonsignificant trend for EAL2 (p 0.148, SE ) (paired t-test) were seen when comparing each stimulation phase with the combined rest phases 1 through 4 (rest). No significant differences detected between the individual rest phases 1-4, p (ANOVA). Percent of pacing calculated by (# paced beats/# total heart beats). Error bars represent standard error. Figure 2. The data represents the mean RR interval (ms) of all heart beats for each phase of testing for patients not 100% ventricular paced (includes intermittently paced and nonpaced patients, 24 total). The mean RR interval of the stimulation phases (EAL1, EAL2, EPT), assessed combined or individually were significantly longer than the mean RR interval of the combined rest phases 1 through 4, ** (p 0.001, SE to 7.944) (paired t-test). The increased mean RR interval during each of the stimulation phases represents a slowing of the heart rate. No significant difference detected between the individual rest phases 1 through 4, p (ANOVA). Error bars represent the standard error. Figure 3. The RR interval (ms) of all heart beats for each phase of testing for patient #23. No paced beats were detected or delivered during the testing protocol. The RR intervals during the stimulation phases (EAL1, EAL2, and EPT) tended to increase, representing a slowing of the heart rate. During the rest phases (rest 1-4) the RR intervals tended to decrease, representing a faster heart rate. Discussion The patient population in this study represents patients coming to a university electrophysiology service and not necessarily those in a typical endodontic practice. The majority of the devices tested were ICDs. This reflects the fact that ICDs require more frequent generator replacement, that they receive more regular follow up in clinic, and that we excluded patients who were pacemaker dependent. Many of the devices we tested were newly implanted. Although one device was 14 yr old, it is difficult to be certain that other older devices would behave similarly. There are two advantages to studying ICDs. First, ICDs have an increased sensitivity, since they are designed for early detection of ventricular tachyarrhythmias. Second, the most likely cause of concern is the detection of electromagnetic interference as false ventricular tachycardia or fibrillation by the ICD resulting in an inappropriate shock therapy to be delivered (9). A significant increase in pacing, measured as the percent of paced beats, was detected during stimulation of the oral tissues with the dental devices in patients who were intermittently paced. Before a conclusion may be drawn from this observation it is prudent to first determine if the increase in pacing seen during stimulation with the dental devices is a result of interference with the cardiac device or a normal response to a change in the patients physiology (i.e. intrinsic heart rate). The underlying intrinsic heart rate during each phase of testing was determined for all patients not continuously paced, which included 18 patients who were not paced and 6 patients who were only intermittently paced during the testing protocol. The RR interval between each heartbeat was measured and then averaged for each phase of testing. The RR interval is the time in milliseconds between two consecutive heartbeats, a measure of heart rate. This data revealed an interesting finding in that a significant increase in the RR interval, a decreasing heart rate, was seen during each stimulation phase. The RR interval then decreased, an increase in the heart rate, during the following rest phases of nonstimulation. During the stimulation phases (EAL1, EAL2, and EPT) there was an overall significant decrease in the heart rate by an average of 2 to 3 beats/minute. Two possible hypotheses are proposed for the slowing of the heart rate during the stimulation phases with the dental devices. First, the electrical current from the apex locators and pulp tester being delivered to the oral cavity may have stimulated the vagal nerve increasing the parasympathetic stimulation to the heart resulting in a slightly slower heart rate. A second possibility is that during the stimulation test phases, were a probe was placed in contact with oral tissues, patients responded by holding their breath. A slight decrease in a patients respiratory rate may have a physiologic response of slowing the intrinsic heart rate. The RR interval for every paced beat was evaluated for all patients who were paced during the testing protocol, excluding patients with rate modulation programming. This data was compared with the programming of the cardiac devices, and this failed to show any delay or premature delivery of any paced beat. All paced beats occurred when expected as determined by the programming of the cardiac devices. JOE Volume 32, Number 9, September 2006 Safety of Apex Locators and Pulp Testers 851
6 Patient #17, a patient who was continuously paced during the testing protocol, exhibited noticeable changes in the pacing frequency during both the stimulation and rest phases. These changes can be fully explained by potential physiologic differences. For patient #17, the pacemaker had rate-modulation programming turned on. For this particular device, the rate-modulation is based on respiratory rate, which the device samples at a rate of 16 Hz. Thus, during a 30-s period, if the patient held their breath or slowed their respiratory rate, the device would in fact respond quickly enough to slow the paced rate within that period, as we observed. Although the respiratory rates for patients with rate-modulation programming were not determined, it is reasonable to assume that placement of the EAL or EPT in their oral cavity during testing may result in a patient holding their breath or slowing their respiratory rate that would explain the changes in pacing frequency observed. The six patients in this study with intermittent pacing had a resting heart rate close to the programmed lower rate limit of their cardiac devices. When the resting heart rate falls below the lower rate limit of the cardiac device a paced beat is delivered. A slight decrease in the intrinsic heart rate, as has been shown during EAL/EPT stimulation, would result in the intrinsic heart rate being slower than the lower rate limit set by their cardiac device a greater proportion of the time. This would result in an increased amount of pacing to maintain the heart rate at the lower limit set by the cardiac device. There was no detection of any adverse symptom or effect from EPT/EAL use in any of the 27 patients. In no instance could we demonstrate that electrical stimulation with any of the dental devices was directly detected by any of the cardiac devices evaluated. Furthermore, we did not detect any interference with ICP/ICDs, including mode change, triggering, or device malfunction. These findings lead us to conclude that the increased pacing seen during stimulation with the dental devices, in a subset of patients, was a result of the proper and expected functioning of the cardiac devices in response to a slowing of the patients natural underlying (intrinsic) heart rate and not to dysfunction of or interference with the cardiac devices. Our study was limited to a relatively small patient sample size, and definitely not adequate to claim that no device in any patient would result in complications. However, we deliberately chose to enroll patients with any type of device or lead configuration, and purposely did not change any of the programmed settings. Our findings add confidence to allow more widespread study of interactions between these devices and challenge the manufacturers claim that they not be used with ICP/ICDs. Future studies may wish to enhance the potential of detecting interferences by using the hand electrode or lowering the detection threshold of the devices. No evidence of any interference was encountered when the EAL/ EPTs were used as described in patients with working, implanted cardiac devices. Based on the findings in this study we conclude that EAL/ EPTs are safe for use in patients with ICP/ICDs. References 1. Am Association of Endodontists 2004; Web page: 2. Analytic. Endo Analyzer Model 8005; Operation manual. 3. Morita J, Root ZX Operation manual; Imich W, Parsonnet V, Myers GH. In: Giuliani ER, Gersh BJ, McGoon MD, Hayes DL, Schaff HV, eds. Mayo clinic practice of cardiology, 3rd ed. St. Louis: Mosby; 1996: Mirowski M, Reid PR, Mower MM, et al. Termination of malignant ventricular arrhythmias with an implanted automatic defibrillator in human beings. N Engl J Med 1980;303: Elliott L, Gilkerson J. Advances in dual chamber implantable cardioverter/defibrillators. J Interven Cardiol 1998;11: Greene HL. The implantable cardioverter-defibrillator. Clin Cardiol 2000;23: Madigan JD, Choudhri AF, Chen J, Spotnitz HM, Oz MC, Edwards N. Surgical management of the patient with an implanted cardiac device. implications of electromagnetic interference. Ann Surg 1999;230: Pinski SL, Trohman RG. Permanent pacing via implantable defibrillators. Pace 2000;23: Kobayashi C. Electronic canal length measurement. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1995;79: Peters DD, Baumgartner JC, Lorton L. Adult pulpal diagnosis. I. Evaluation of the positive and negative responses to cold and electrical pulp tests. J Endod 1994;20: Garofalo RR. The effect of electronic apex locators on cardiac pacemaker function. J Endod 2002;28: Woolley LH, Woodworth J, Dobbs JL. A preliminary evaluation of the effects of electrical pulp testers on dogs with artificial pacemakers. J Am Dental Association 1974;91: Luker J. The pacemaker patient in the dental surgery. J Dentistry 1982;10: Miller CS, Leonelli FM, Latham E. Selective interference with pacemaker activity by electrical dental devices. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998;85: Adams D. The cardiac pacemaker and ultrasonic scalers. Br Dental J 1982;152: Simon AB. The individual with a pacemaker in the dental environment. J Am Dental Assoc 1975;91: Zappa U. [Effect of electrically powered dental devices on cardiac parameter function in humans]. Parodontology 1991;2: Beach CW, Bramwell JD, Hutter JW. Use of an electronic apex locator on a cardiac pacemaker patient. J Endod 1996;22: Wilson et al. JOE Volume 32, Number 9, September 2006
Basics of Pacing. Ruth Hickling, RN-BSN Tasha Conley, RN-BSN
 Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI
 Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
CCAD Training Manual. Cardiac Rhythm Management (CRM)
 CCAD Training Manual Cardiac Rhythm Management (CRM) Version 1.0 A D Cunningham 19/3/2008 Introduction This manual is intended to assist users of the Notes Client version of the CCAD Cardiac Rhythm Management
CCAD Training Manual Cardiac Rhythm Management (CRM) Version 1.0 A D Cunningham 19/3/2008 Introduction This manual is intended to assist users of the Notes Client version of the CCAD Cardiac Rhythm Management
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ
 «Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
The science of medicine. The compassion to heal.
 A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Pacers use a 5-letter code: first 3 letters most important
 PACEMAKERS 2 Pacemakers: Nomenclature Pacers use a 5-letter code: first 3 letters most important t First Letter: Chamber Paced A= Atrium V= Ventricle D= Dual (A+V) 2nd Letter: Chamber Sensed A= Atrium
PACEMAKERS 2 Pacemakers: Nomenclature Pacers use a 5-letter code: first 3 letters most important t First Letter: Chamber Paced A= Atrium V= Ventricle D= Dual (A+V) 2nd Letter: Chamber Sensed A= Atrium
What Are Arrhythmias?
 What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
Introduction. Planned surgical procedures
 Guidelines for the perioperative management of patients with implantable pacemakers or implantable cardioverter defibrillators, where the use of surgical diathermy/electrocautery is anticipated. Introduction
Guidelines for the perioperative management of patients with implantable pacemakers or implantable cardioverter defibrillators, where the use of surgical diathermy/electrocautery is anticipated. Introduction
Pacemaker Counter and Histogram Operation and Interpretation. Percentage of total count. Figure 2. Detailed ALTRUA Paced and Sensed Event Counters
 A Closer Look SUMMARY This article provides information regarding the operation and interpretation of Event Counters and Histograms available in ALTRUA, INSIGNIA, PULSAR MAX II, and DISCOVERY II pacemakers.
A Closer Look SUMMARY This article provides information regarding the operation and interpretation of Event Counters and Histograms available in ALTRUA, INSIGNIA, PULSAR MAX II, and DISCOVERY II pacemakers.
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Implantable Cardioverter Defibrillator Therapy
 Implantable Cardioverter Defibrillator Therapy A Message to Patients Boston Scientific Corporation acquired Guidant Corporation in April 2006. During our transition period, you may see both the Boston
Implantable Cardioverter Defibrillator Therapy A Message to Patients Boston Scientific Corporation acquired Guidant Corporation in April 2006. During our transition period, you may see both the Boston
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Implantable pacemakers and implantable cardioverter
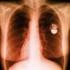 BRIEF REPORT EAS SYSTEMS AND INTERACTIONS WITH IMPLANTABLE CARDIAC DEVICES Electronic Article Surveillance Systems and Interactions With Implantable Cardiac Devices: Risk of Adverse Interactions in Public
BRIEF REPORT EAS SYSTEMS AND INTERACTIONS WITH IMPLANTABLE CARDIAC DEVICES Electronic Article Surveillance Systems and Interactions With Implantable Cardiac Devices: Risk of Adverse Interactions in Public
What Can I Do about Atrial Fibrillation (AF)?
 Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
Reimbursement Information For Electrophysiology and Arrhythmia Service Procedures 1
 GE Healthcare Information For Electrophysiology and Arrhythmia Procedures 1 2011 Update www.gehealthcare.com/reimbursement This overview addresses coding, coverage, and payment for electrophysiology procedures
GE Healthcare Information For Electrophysiology and Arrhythmia Procedures 1 2011 Update www.gehealthcare.com/reimbursement This overview addresses coding, coverage, and payment for electrophysiology procedures
New CPT Codes for Cardiac Device Monitoring SIDE-BY-SIDE COMPARISON 2008-2009
 New CPT Codes for Cardiac Device Monitoring SIDE-BY-SIDE COMPARISON 2008-2009 Effective January 1, 2009 NEW CPT 1 CODES FOR CARDIAC DEVICE MONITORING Twenty-three new CPT codes for Cardiac Device Monitoring
New CPT Codes for Cardiac Device Monitoring SIDE-BY-SIDE COMPARISON 2008-2009 Effective January 1, 2009 NEW CPT 1 CODES FOR CARDIAC DEVICE MONITORING Twenty-three new CPT codes for Cardiac Device Monitoring
Management of Pacing Wires After Cardiac Surgery
 Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Electrophysiology Heart Study - EPS -
 Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Catheter Ablation. A Guided Approach for Treating Atrial Arrhythmias
 Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
UCSF Anesthesia Resident Pearls: Cardiac Implantable Electronic Devices: Pacemakers and ICDs Table of Contents
 UCSF Anesthesia Resident Pearls: Cardiac Implantable Electronic Devices: Pacemakers and ICDs Table of Contents Page 1 Intro Indications for Pacers and ICDs Page 2 Differentiating between Pacers and ICDs
UCSF Anesthesia Resident Pearls: Cardiac Implantable Electronic Devices: Pacemakers and ICDs Table of Contents Page 1 Intro Indications for Pacers and ICDs Page 2 Differentiating between Pacers and ICDs
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Basic principles of pacing
 CHAPTER 1 Basic principles of pacing Malcolm Kirk The aim of this chapter is to give sufficient background and information about cardiac pacemakers to allow interpretation of electrocardiograms (ECGs)
CHAPTER 1 Basic principles of pacing Malcolm Kirk The aim of this chapter is to give sufficient background and information about cardiac pacemakers to allow interpretation of electrocardiograms (ECGs)
Dual Chamber Temporary Pacemaker
 5388 Dual Chamber Temporary Pacemaker Technical Manual Caution: Federal Law (USA) restricts this device to sale by c or on the order of a physician. 0123 MODEL 5388 0 Technical Manual 0 Dual Chamber Temporary
5388 Dual Chamber Temporary Pacemaker Technical Manual Caution: Federal Law (USA) restricts this device to sale by c or on the order of a physician. 0123 MODEL 5388 0 Technical Manual 0 Dual Chamber Temporary
Michael Hartman, CRNA, DNP, MSN, BSN, BA
 Michael Hartman, CRNA, DNP, MSN, BSN, BA Intrinsic Conduction Automaticity-cardiac cells ability to spontaneously depolarize and initiate impulse Depolarization-cardiac cells go to a+ intracellular and
Michael Hartman, CRNA, DNP, MSN, BSN, BA Intrinsic Conduction Automaticity-cardiac cells ability to spontaneously depolarize and initiate impulse Depolarization-cardiac cells go to a+ intracellular and
What to Know About. Atrial Fibrillation
 Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Electrocardiographic Issues in Williams Syndrome
 Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
Electrocardiographic Issues in Williams Syndrome R. Thomas Collins II, MD Assistant Professor, Pediatrics and Internal Medicine University of Arkansas for Medical Sciences Arkansas Children s Hospital
PACEMAKERS AND ANTITACHYCARDIA DEVICES WILLIAM BATSFORD, M.D.
 CHAPTER 26 PACEMAKERS AND ANTITACHYCARDIA DEVICES WILLIAM BATSFORD, M.D. INTRODUCTION The heart s natural pacemaker is an electrical timing device that controls the rate of the heart s muscular contractions,
CHAPTER 26 PACEMAKERS AND ANTITACHYCARDIA DEVICES WILLIAM BATSFORD, M.D. INTRODUCTION The heart s natural pacemaker is an electrical timing device that controls the rate of the heart s muscular contractions,
IMAGEREADY MR CONDITIONAL DEFIBRILLATION SYSTEM
 MRI TECHNICAL GUIDE IMAGEREADY MR CONDITIONAL DEFIBRILLATION SYSTEM REF D000, D002, D010, D012, D020, D022, D044, D046, D050, D052, D140, D142, D150, D152, D174, D176, G058, G148, G158, G179, 0265, 0266,
MRI TECHNICAL GUIDE IMAGEREADY MR CONDITIONAL DEFIBRILLATION SYSTEM REF D000, D002, D010, D012, D020, D022, D044, D046, D050, D052, D140, D142, D150, D152, D174, D176, G058, G148, G158, G179, 0265, 0266,
SW012. Installation software for the Right Ventricular Lead Integrity Alert feature. Reference Manual
 Installation software for the Right Ventricular Lead Integrity Alert feature Reference Manual Caution: Federal law (USA) restricts this device to sale by or on the order of a physician. The following list
Installation software for the Right Ventricular Lead Integrity Alert feature Reference Manual Caution: Federal law (USA) restricts this device to sale by or on the order of a physician. The following list
Understanding the Electrocardiogram. David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem
 Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona
 Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
VCA Veterinary Specialty Center of Seattle
 An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
INSERTABLE CARDIAC MONITORING SYSTEM. UNLOCK the ANSWER. Your heart and long-term monitoring
 INSERTABLE CARDIAC MONITORING SYSTEM UNLOCK the ANSWER Your heart and long-term monitoring UNLOCK the ANSWER Irregular heartbeats can be related to a variety of conditions, including unexplained fainting,
INSERTABLE CARDIAC MONITORING SYSTEM UNLOCK the ANSWER Your heart and long-term monitoring UNLOCK the ANSWER Irregular heartbeats can be related to a variety of conditions, including unexplained fainting,
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
Treatments to Restore Normal Rhythm
 Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
MRI Case Study MRI Cervical Spine
 MRI Case Study MRI Cervical Spine Jewish Hospital Louisville, KY The Revo MRI SureScan pacing system is MR Conditional designed to allow patients to undergo MRI under the specified conditions for use.
MRI Case Study MRI Cervical Spine Jewish Hospital Louisville, KY The Revo MRI SureScan pacing system is MR Conditional designed to allow patients to undergo MRI under the specified conditions for use.
Feature Vector Selection for Automatic Classification of ECG Arrhythmias
 Feature Vector Selection for Automatic Classification of ECG Arrhythmias Ch.Venkanna 1, B. Raja Ganapathi 2 Assistant Professor, Dept. of ECE, G.V.P. College of Engineering (A), Madhurawada, A.P., India
Feature Vector Selection for Automatic Classification of ECG Arrhythmias Ch.Venkanna 1, B. Raja Ganapathi 2 Assistant Professor, Dept. of ECE, G.V.P. College of Engineering (A), Madhurawada, A.P., India
Activity 4.2.3: EKG. Introduction. Equipment. Procedure
 Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Electromagnetic Interference of Pacemakers
 13 Electromagnetic Interference of Pacemakers Umashankar Lakshmanadoss MD 1, Priya Chinnachamy MD 2 and James P Daubert MD 3 1 Johns Hopkins Medical Institutions, Baltimore, MD, USA; 2 All India Institute
13 Electromagnetic Interference of Pacemakers Umashankar Lakshmanadoss MD 1, Priya Chinnachamy MD 2 and James P Daubert MD 3 1 Johns Hopkins Medical Institutions, Baltimore, MD, USA; 2 All India Institute
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation
 The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation 2 P a g e Table of Contents Introduction How the Heart Works 3 How the Heart s Electrical System Works 3 Commonly Used Heart
The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation 2 P a g e Table of Contents Introduction How the Heart Works 3 How the Heart s Electrical System Works 3 Commonly Used Heart
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Worldwide Experience with S-ICD: Early results from the EFFORTLESS Registry
 Worldwide Experience with S-ICD: Early results from the EFFORTLESS Registry Results published in European Heart Journal (March 2014) Pier D. Lambiase, Craig Barr, Dominic A.M.J. Theuns, Reinoud Knops,
Worldwide Experience with S-ICD: Early results from the EFFORTLESS Registry Results published in European Heart Journal (March 2014) Pier D. Lambiase, Craig Barr, Dominic A.M.J. Theuns, Reinoud Knops,
Establishing a Remote Monitoring Program. Martha Ferrara, FNP
 Establishing a Remote Monitoring Program Martha Ferrara, FNP Establishing a Remote Monitoring Program What is Remote Monitoring? Martha Ferrara, FNP, CCDS November 2012 CIED Timeline: Cardiovascular Implantable
Establishing a Remote Monitoring Program Martha Ferrara, FNP Establishing a Remote Monitoring Program What is Remote Monitoring? Martha Ferrara, FNP, CCDS November 2012 CIED Timeline: Cardiovascular Implantable
IMPLANTABLE CARDIOVERTER DEFIBRILLATORS (ICDs)
 Work with Your Doctor An ICD is not a cure for heart rhythm problems. You ll likely still need medications and other forms of treatment. But you can feel confident that your ICD will protect you from a
Work with Your Doctor An ICD is not a cure for heart rhythm problems. You ll likely still need medications and other forms of treatment. But you can feel confident that your ICD will protect you from a
Root ZX II Endodontic Predictability Apex Locator with Low Speed Handpiece. Thinking ahead. Focused on life.
 Root ZX II Endodontic Predictability Apex Locator with Low Speed Handpiece Thinking ahead. Focused on life. Root ZX II Key Features Endodontic Predictability As the world s best selling apex locator, Root
Root ZX II Endodontic Predictability Apex Locator with Low Speed Handpiece Thinking ahead. Focused on life. Root ZX II Key Features Endodontic Predictability As the world s best selling apex locator, Root
Your pacemaker system information
 Pacemaker Therapy Your pacemaker system information Have your doctor or nurse complete these forms before you go home from the hospital. Pacemaker Model Number: Pacemaker Serial Number: Implant Date:
Pacemaker Therapy Your pacemaker system information Have your doctor or nurse complete these forms before you go home from the hospital. Pacemaker Model Number: Pacemaker Serial Number: Implant Date:
Living with Your Pacemaker
 Brief Statement Additional Device Information An implantable pacemaker system relieves symptoms of heart rhythm disturbances. They do this by restoring normal heart rates. A normal heart rate provides
Brief Statement Additional Device Information An implantable pacemaker system relieves symptoms of heart rhythm disturbances. They do this by restoring normal heart rates. A normal heart rate provides
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Radiofrequency Ablation for Atrial Fibrillation. A Guide for Adults
 Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
PACEMAKER PATIENT INFORMATION
 PACEMAKER PATIENT INFORMATION Information Leaflet Your Health. Our Priority. Page 2 of 11 Contents What is a pacemaker? Why do I need a pacemaker? The heart and normal electrical conduction Complete or
PACEMAKER PATIENT INFORMATION Information Leaflet Your Health. Our Priority. Page 2 of 11 Contents What is a pacemaker? Why do I need a pacemaker? The heart and normal electrical conduction Complete or
Electrophysiology study (EPS)
 Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
A Patient Guide to Atrial Fibrillation and Catheter Ablation
 A Patient Guide to Atrial Fibrillation and Catheter Ablation Al-Sabah Arrhythmia Institute 1111 Amsterdam Avenue New York, NY 10025 Phone: 212-523-2400 Fax: 212-523-2571 www.stlukescardiology.org Printed
A Patient Guide to Atrial Fibrillation and Catheter Ablation Al-Sabah Arrhythmia Institute 1111 Amsterdam Avenue New York, NY 10025 Phone: 212-523-2400 Fax: 212-523-2571 www.stlukescardiology.org Printed
Cardiac Rhythm Management Devices (Part II)
 REVIEW ARTICLE Anesthesiology 2001; 95:1492 1506 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Cardiac Rhythm Management Devices (Part II) Perioperative Management
REVIEW ARTICLE Anesthesiology 2001; 95:1492 1506 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Cardiac Rhythm Management Devices (Part II) Perioperative Management
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It?
 The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
MRI SureScan Pacing System
 MRI SureScan Pacing System Step-by-step Instructions For A Successful MRI Scan Timothy S. E. Albert, MD Medical Director Advanced Diagnostic Imaging Center Monterey, CA Lisa L. Hungate, BS, RN clinical
MRI SureScan Pacing System Step-by-step Instructions For A Successful MRI Scan Timothy S. E. Albert, MD Medical Director Advanced Diagnostic Imaging Center Monterey, CA Lisa L. Hungate, BS, RN clinical
Evaluation copy. Analyzing the Heart with EKG. Computer
 Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Advantages of Right-Sided Implantation of Permanent Cardiac Pacemakers Performed by a Surgeon
 Advantages of Right-Sided Implantation of Permanent Cardiac Pacemakers Performed by a Surgeon 7 Davor Horvat General Hospital in Karlovac, Croatia 1. Introduction A pacemaker is a medical device which
Advantages of Right-Sided Implantation of Permanent Cardiac Pacemakers Performed by a Surgeon 7 Davor Horvat General Hospital in Karlovac, Croatia 1. Introduction A pacemaker is a medical device which
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
HEART RHYTHM DISORDERS CRAIG A. McPHERSON, M.D., AND LYNDA E. ROSENFELD, M.D.
 HEART RHYTHM DISORDERS CRAIG A. McPHERSON, M.D., AND LYNDA E. ROSENFELD, M.D. INTRODUCTION Heart rhythm disorders, called arrhythmias, pose one of the paradoxes of medicine. Almost anyone s heart will
HEART RHYTHM DISORDERS CRAIG A. McPHERSON, M.D., AND LYNDA E. ROSENFELD, M.D. INTRODUCTION Heart rhythm disorders, called arrhythmias, pose one of the paradoxes of medicine. Almost anyone s heart will
2013 Medicare Physician Coding and Reimbursement Changes
 2013 Medicare Physician Coding and Reimbursement Changes Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent of Medtronic s Economic Strategies
2013 Medicare Physician Coding and Reimbursement Changes Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent of Medtronic s Economic Strategies
HEART AND VASCULAR INSTITUTE. The Johns Hopkins Arrhythmia Service. A guide for patients and their families
 HEART AND VASCULAR INSTITUTE The Johns Hopkins Arrhythmia Service A guide for patients and their families TABLE OF CONTENTS Understanding Your Heart 3 What Are Arrhythmias? 6 Diagnosing Arrhythmias 14
HEART AND VASCULAR INSTITUTE The Johns Hopkins Arrhythmia Service A guide for patients and their families TABLE OF CONTENTS Understanding Your Heart 3 What Are Arrhythmias? 6 Diagnosing Arrhythmias 14
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
STANDARDS FOR IMPLANTATION AND FOLLOW-UP OF CARDIAC RHYTHM MANAGEMENT DEVICES IN ADULTS January 2013
 1. INTRODUCTION STANDARDS FOR IMPLANTATION AND FOLLOW-UP OF CARDIAC RHYTHM MANAGEMENT DEVICES IN ADULTS January 2013 This document replaces the previous Heart Rhythm UK documents Clinical Guidance by Consensus
1. INTRODUCTION STANDARDS FOR IMPLANTATION AND FOLLOW-UP OF CARDIAC RHYTHM MANAGEMENT DEVICES IN ADULTS January 2013 This document replaces the previous Heart Rhythm UK documents Clinical Guidance by Consensus
Guidelines for Perioperative Management of Pacemakers and Defibrillators
 Guidelines for Perioperative Management of Pacemakers and Defibrillators Developed By: Deborah Wolbrette, MD, Medical Director, Electrophysiology Lab, Dept of Cardiology Kane High, MD, Department of Anesthesiology
Guidelines for Perioperative Management of Pacemakers and Defibrillators Developed By: Deborah Wolbrette, MD, Medical Director, Electrophysiology Lab, Dept of Cardiology Kane High, MD, Department of Anesthesiology
School of Health Sciences
 School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
Chronic Vagus Nerve Stimulation: A New Treatment Modality for Congestive Heart Failure
 Chronic Vagus Nerve Stimulation: A New Treatment Modality for Congestive Heart Failure Gaetano M. De Ferrari, MD Dept. of Cardiology, Fondazione IRCCS Policlinico S. Matteo, Pavia, Italy for the CardioFit
Chronic Vagus Nerve Stimulation: A New Treatment Modality for Congestive Heart Failure Gaetano M. De Ferrari, MD Dept. of Cardiology, Fondazione IRCCS Policlinico S. Matteo, Pavia, Italy for the CardioFit
Atrioventricular (AV) node ablation
 Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Ngaire has Palpitations
 Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Rome, Italy December 4-7, 2012 Rome Cavalieri TIMETABLE
 Rome, Italy December 4-7, 2012 Rome Cavalieri Monday, December 3 ROOM Terrazza Monte Mario PATIENT MANAGEMENT CONCEPTS AND CONTROVERSIES IN ELECTROPHYSIOLOGY BIOTRONIK International Fellows Program (IFP)
Rome, Italy December 4-7, 2012 Rome Cavalieri Monday, December 3 ROOM Terrazza Monte Mario PATIENT MANAGEMENT CONCEPTS AND CONTROVERSIES IN ELECTROPHYSIOLOGY BIOTRONIK International Fellows Program (IFP)
Medtronic CareLink Network :: PACE article: Remote monitoring of ICDs: A prospective analysis
 Remote Monitoring of Implantable Cardioverter Defibrillators: A Prospective Analysis Reprinted with permission from Pacing and Clinical Electrophysiology (PACE) Schoenfeld MH, Compton SJ, Mead RH, et al.
Remote Monitoring of Implantable Cardioverter Defibrillators: A Prospective Analysis Reprinted with permission from Pacing and Clinical Electrophysiology (PACE) Schoenfeld MH, Compton SJ, Mead RH, et al.
Purpose: To outline the care of patients with permanent or temporary pacemakers.
 University of Kentucky / UK HealthCare Policy and Procedure Policy # NR08-03 Title/Description: Care of Patients with Pacemakers Purpose: To outline the care of patients with permanent or temporary pacemakers.
University of Kentucky / UK HealthCare Policy and Procedure Policy # NR08-03 Title/Description: Care of Patients with Pacemakers Purpose: To outline the care of patients with permanent or temporary pacemakers.
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
TOP 5. The term cardiac arrhythmia encompasses all cardiac. Arrhythmias in Dogs & Cats. Sinus Arrhythmia. TOP 5 Arrhythmias Seen in Dogs & Cats
 Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
Top 5 ardiology Peer reviewed TOP 5 rrhythmias in Dogs & ats shley Jones, DVM mara Estrada, DVM, DVIM (ardiology) University of Florida The term cardiac arrhythmia encompasses all cardiac rhythms other
Advances in the Treatment of Atrial Fibrillation At VCU Medical Center
 Contact Us For additional information or to schedule an appointment with one of our specialists, please call: Ken Ellenbogen, M.D. Cardiology/Electrophysiology 804-828-7565 or 804-628-0147 You can also
Contact Us For additional information or to schedule an appointment with one of our specialists, please call: Ken Ellenbogen, M.D. Cardiology/Electrophysiology 804-828-7565 or 804-628-0147 You can also
About the British Heart Foundation
 Heart rhythms About the British Heart Foundation The British Heart Foundation (BHF) is the nation s heart charity, saving lives through pioneering research, patient care and vital information. What you
Heart rhythms About the British Heart Foundation The British Heart Foundation (BHF) is the nation s heart charity, saving lives through pioneering research, patient care and vital information. What you
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
