Your pacemaker system information
|
|
|
- David Roberts
- 10 years ago
- Views:
Transcription
1 Pacemaker Therapy
2
3 Your pacemaker system information Have your doctor or nurse complete these forms before you go home from the hospital. Pacemaker Model Number: Pacemaker Serial Number: Implant Date: Lead Model/Serial Numbers:
4 Your medical contact information Electrophysiologist Name/Phone Number: Cardiologist Name/Phone Number: Hospital Name/Address/Phone Number: Medications (list):
5 By Mail: Boston Scientific 4100 Hamline Avenue North St. Paul, Minnesota By Phone: Patients and families: Medical professionals: CARDIAC ( ) Worldwide: On the Internet: Medical Records: PATDATA ( ) 7 a.m. 7 p.m. (Central Time), Monday Friday [email protected]
6
7 Table of contents Introduction When is this device used?, 2 When is this device not used?, 3 How reliable is this device?, 3 Glossary Your heart s natural pacemaker Bradycardia, 17 Your pacemaker system The device, 21
8 Types of pacemakers, 23 The leads, 25 Implanting your pacemaker system Implant risks, 30 After your implant Medications, 37 Activities and exercise, 38 Your pacemaker system information, 38 Your identification card, 39 Living with your pacemaker system Special considerations, 42 What you should know about your pacemaker s battery, 47
9 Replacing your system, 48 Important safety information Operating household appliances and tools, 53 Theft detection and security systems, 62 Airport security, 64 Cellular phones, 65 Dental and medical procedures, 67 Summary Visit us on the Internet Notes and questions Index
10
11 Introduction Your doctor has recommended a pacemaker system to treat your slow heart rhythm. As a person with a slow heart rhythm, you may experience symptoms that can affect your quality of life. A pacemaker is designed to monitor and treat heart rhythm problems, greatly reducing the risks associated with them. This handbook will tell you how a pacemaker system treats heart rhythms that are too slow. It will discuss activities you can begin and those you should avoid after your surgery. It will talk about some of the changes that may occur in your life. It will also answer many 1
12 questions patients typically have. If you have questions about what you read in this handbook, ask your doctor or nurse. They are your best resource for information. The glossary is located at the front of the handbook. It defines many of the words you will see in the upcoming pages, as well as those you may hear from your doctors and nurses. When is this device used? Your doctor has decided that you should receive a pacemaker system to treat and monitor your slow heart rhythm. If you have any questions about when this device is used, ask your doctor. 2
13 When is this device not used? Patients who have additional medical conditions that may not allow the pacemaker to function appropriately should not receive a device. If you have any questions about when this device is not used, ask your doctor. How reliable is this device? It is Boston Scientific s intent to provide implantable devices of high quality and reliability. However, these devices may exhibit malfunctions that may result in lost or compromised ability to deliver therapy. Refer to Boston Scientific s CRM Product Performance Report on for more information about device performance, including 3
14 the types and rates of malfunctions that these devices have experienced historically. While historical data may not be predictive of future device performance, such data can provide important context for understanding the overall reliability of these types of products. Talk with your doctor about this product performance data, and the risks and benefits associated with the implantation of this system. 4
15 Glossary Adaptive rate The ability of a device to increase or decrease its pacing rate in response to bodily needs, activity, or exercise. Asynchrony A condition in which the heart fails to maintain a normal timing sequence between atrial and ventricular contractions. Atrioventricular (AV) node A cluster of cells located in the wall between the right and left atrium, just above the ventricles. This 5
16 part of the heart s electrical pathway helps carry signals from the atria to the ventricles. Atrioventricular (AV) synchrony The normal timing sequence for an atrial contraction followed, after a fraction of a second, by a ventricular contraction. Atrium (plural: atria) One of the two upper chambers of the heart specifically, the right atrium and left atrium. The atria collect blood as it comes into the heart and pump blood into the lower chambers (ventricles). Bradycardia An abnormally slow heartbeat, typically fewer than 60 beats per minute. 6
17 Catheter A thin, flexible tube or wire inserted into the body for a variety of purposes. Catheters are inserted into the heart during an electrophysiology (EP) test to monitor your heart s electrical activity. Hollow catheters are also used to carry a lead through a blood vessel. See also electrophysiology (EP) test or study. Device See pulse generator. ECG/EKG (electrocardiogram) A graphic representation of your heart s electrical signals. The graph shows how electrical signals travel through your heart. Your doctor can tell what kind of rhythm you have by looking at the pattern of your heartbeat. 7
18 Electromagnetic field Invisible lines of force that are the result of electrical fields (produced by voltage) and magnetic fields (produced by current flow). Electromagnetic fields decrease in strength the farther they are from their source. Electromagnetic interference (EMI) Interference that occurs when an electromagnetic field interacts with an implanted device. See also electromagnetic field. Electrophysiology (EP) test or study A test in which catheters (thin, flexible tubes or wires) are inserted into your heart to identify and measure the type of electrical signals in your heart. The test 8
19 results can help your doctor identify the origins of your abnormal heart rhythms, determine how well medications work, and decide what treatment is best for your condition. Heart attack See myocardial infarction (MI). Heart block A condition in which the electrical signals of your heart s natural pacemaker (SA node) are delayed or do not reach the ventricles. 9
20 Heart rhythm A series of heartbeats. You may hear your doctor refer to your rhythm as being normal or irregular. A normal heart rate typically ranges from 60 to 100 beats per minute at rest. Lead (pronounced leed ) An insulated wire that is implanted in the heart and connected to the device. The lead senses your heartbeat and delivers pacing pulses from the device to the heart. The leads are usually passed into your heart through a vein. Myocardial infarction (MI) Also called a heart attack. A myocardial infarction occurs when an artery that supplies blood to the heart becomes blocked. As a result, blood does not 10
21 reach some parts of the heart, and some of the heart tissue dies. Symptoms of a myocardial infarction may include shortness of breath, nausea, fatigue, and/or pain in the chest, arm, or neck. Pacemaker system A pulse generator (also called a device) and leads. A pacemaker system is implanted to monitor your heart rhythm and treat dangerously slow rhythms. Pectoral The area above the breast and below the collarbone. This is a common area for a device implant. Programmer Microcomputer-based equipment that is used to communicate with the device. The programmer is 11
22 used during testing and follow-up exams to gather and display information from the device. The doctor or technician also uses the programmer to adjust the device so that it senses and treats your slow heart rate. Pulse generator Also called a device. The pulse generator is the part of the pacemaker system that contains the electronics and battery; it is implanted under the skin in the pectoral (or, in some cases, abdominal) area. See also pectoral. Sinoatrial (SA) node The heart s natural pacemaker. The SA node is a small group of specialized cells in the upper right chamber of the heart (right atrium) that normally generates an 12
23 electrical signal. This signal runs through the heart and causes the heart to beat. Ventricle One of the two lower chambers of the heart. The right ventricle pumps blood to the lungs, and the left ventricle pumps oxygen-carrying blood from the lungs to the rest of the body. 13
24 14
25 Your heart s natural pacemaker Your heart works as both a mechanical pump and an electrical organ. It is able to beat because it produces electrical signals. These signals travel through the electrical pathways of your heart (Figure 1), causing the muscle contraction that pumps blood throughout your body. Normally these signals come from a small area in your heart called the sinoatrial ( SA) node. This area is located in the upper right chamber, or right atrium. When the SA node signals reach the two upper chambers of the heart (the atria), they contract at 15
26 SA node Atria AV node Electrical current Ventricles Figure 1. The heart and its electrical pathways. 16
27 the same time. The atrial contraction fills the two lower chambers (the ventricles) with blood (Figure 2). As the electrical signal travels through the ventricles, it causes them to contract, which pumps blood out to your body. The contraction of the heart muscle (ventricles) is what you feel as a heartbeat. After a brief rest, the cycle begins again. Bradycardia Sometimes the heart beats too slowly. This can be caused by the SA node not working properly or by a condition called heart block (Figure 3). Heart block exists when there is a problem with the electrical pathway between the atria and the ventricles. The 17
28 Blood flow to atria Blood flow through ventricles Figure 2. The heart and its blood flow. 18
29 Heart block SA node Figure 3. An example of heart block. 19
30 natural pacemaker signals sent out by the SA node could be delayed or may not reach the ventricles. During bradycardia, the chambers of the heart do not contract often enough to supply the proper amount of blood to your body. If you have bradycardia, you may feel tired or dizzy, or you may faint. 20
31 Your pacemaker system Your pacemaker system is designed to monitor and treat your heart rhythm. The system consists of a pulse generator (also called a device), which is typically implanted in your chest, and one or more leads, which are implanted in your heart and connected to the device. The device The device contains a small computer. It runs on a battery that is safely sealed within its case. The device continuously monitors your heart rhythm and 21
32 delivers electrical energy (as programmed by your physician) to pace your heart during a slow rhythm. As the device monitors your heart rhythm, it can also store information about your heart. Your doctor can review this information using a special computer called a programmer. The programmer communicates with the device from outside your body through a wand that is placed over your skin. With the programmer, your doctor can better evaluate the programmed therapy for your heart rhythm and adjust the settings if necessary. 22
33 Types of pacemakers There are two different types of pacemakers: singlechamber and dual-chamber. Both of these pacemakers continuously monitor your heart rate and send out pacing signals when necessary. It is important to discuss with your doctor which kind of pacemaker is right for you. Single-chamber pacemakers A single-chamber pacemaker has one lead to monitor signals from and deliver pacing pulses to one chamber of your heart (either the right atrium or right ventricle). This type of pacemaker is often selected for a person whose SA node sends out signals too slowly. 23
34 Dual-chamber pacemakers A dual-chamber pacemaker has two leads. One lead is placed in the right atrium, and the other lead is placed in the right ventricle. Because there are leads in two chambers, the pacemaker can monitor signals from and deliver pacing impulses to either or both of these heart chambers. A dual-chamber pacemaker may be selected for many different reasons. For some people, the SA node s signals are too slow and the electrical pathway to the ventricles is partly or completely blocked. A dualchamber pacemaker can help treat both problems. For other people, the timing of the atrial and ventricular 24
35 contractions is uncoordinated (asynchronous). A dual-chamber pacemaker can restore a normal timing sequence (also called AV synchrony). The leads A lead is an insulated wire implanted in your heart and connected to the device. A lead carries the heart signal to the device. It then carries energy from the device back to the heart to coordinate your heart rhythm. 25
36 Implanting your pacemaker system A pacemaker system is implanted during a surgical procedure. To keep you as comfortable as possible, you will be sedated for this surgery. During the procedure, your doctor will insert the lead into a vein, usually through a small incision near your collarbone. The doctor will then pass the lead through the vein into your heart (in either the right atrium or the right ventricle), where the tip of the lead will rest directly against your heart s inner wall (Figure 4). If your doctor decides your heart condition requires a dual-chamber system, an additional lead will be 26
37 Implanted pacemaker Lead in right ventricle Figure 4. An implanted single-chamber pacemaker system. 27
38 implanted. One lead will be positioned in the atrial chamber of your heart and the other will be positioned in the ventricular chamber (Figure 5). After the leads are positioned, they will be tested to make sure they clearly sense your heart signal and can adequately pace your heart. After this testing, the device will be connected to the leads and placed in position (usually below the collarbone, just beneath the skin). Your doctor will then test your pacemaker system to make sure it can appropriately monitor and treat your heart rhythm. 28
39 Implanted pacemaker Lead in right atrium Lead in right ventricle Figure 5. An implanted dual-chamber pacemaker system. 29
40 After your doctor has finished testing your system, the incision will be closed. You may experience some discomfort from the incision as you recover from the surgery. You should be able to return to normal activities soon after the procedure. Implant risks As with any surgical procedure, it is important to understand that, while complications do not happen very often, there are risks associated with the implantation of a device or lead. You should talk with your doctor about these risks, including those listed below. 30
41 Some of the risks encountered during the implant procedure include, but are not limited to, the following: Bleeding Formation of a blood clot Damage to adjacent structures (tendons, muscles, nerves) Puncture of a lung or vein Damage to the heart (perforation or tissue damage) Dangerous arrhythmias Heart attack Stroke Death 31
42 Some of the risks encountered after the system is implanted may include, but are not limited to, the following: You may develop an infection. You may experience erosion of the skin near your device. The device may move from the original implant site. The lead(s) may move out of place in the heart. The electrodes on the lead or the pacing pulses may cause an irritation or damaging effect on 32
43 the surrounding tissues, including heart tissue and nerves. You may have difficulty coping with having an implanted device. The device might be prevented from pacing due to electromagnetic interference (see Important safety information on page 52). You may receive pacing therapy when it is not needed (unnecessary therapy). The device might not be able to detect or appropriately treat your heart rhythms. 33
44 The device may exhibit malfunctions that may result in lost or compromised ability to deliver therapy. See How reliable is this device? on page 3. Be sure to talk with your doctor so that you thoroughly understand all of the risks and benefits associated with the implantation of this system. 34
45 After your implant As you recover from your implant surgery, you will find that your device may allow you to return to an active lifestyle. It is important that you become actively involved in your recovery by following your doctor s instructions, including: Report any redness, swelling, or drainage from your incisions. Avoid lifting heavy objects until instructed by your doctor. 35
46 Walk, exercise, and bathe according to your doctor s instructions. Do not wear tight clothing that could irritate the skin over your device. Contact your doctor if you develop a fever that does not go away in two or three days. Ask your doctor any questions you may have about your pacemaker system, heart rhythm, or medication. Avoid rubbing your device or the surrounding chest area. If directed by your doctor, limit arm movements that could affect your lead system. 36
47 Avoid rough contact that could result in blows to your implant site. Tell your other doctors, dentists, and emergency personnel that you have an implanted device and show them your Medical Device Identification Card. Contact your doctor if you notice anything unusual or unexpected, such as new symptoms or symptoms like the ones you experienced before you received your device. Medications Your pacemaker system is designed to help treat your heart condition. However, you may need to 37
48 continue taking certain medications as well. It is important that you follow your doctor s instructions regarding any medications. Activities and exercise Your doctor will help you decide what level of activity is best for you. He or she can help answer your questions about lifestyle changes, travel, exercise, work, hobbies, and resuming sexual intimacy. Your pacemaker system information Have your doctor or nurse complete the Your pacemaker system information form at the front of this handbook before you go home from the hospital. 38
49 Your identification card Whether you are going away for the weekend or running a quick errand, carry your Medical Device Identification Card with you. In an emergency, the card will alert medical and security personnel that you have an implanted device. You will be given a temporary Medical Device Identification Card when you receive your device. Boston Scientific will mail you a permanent Medical Device Identification Card about six to eight weeks after your implant. 39
50 Your Medical Device Identification Card contains your name, your doctor s name and phone number, and the model numbers of your device and leads. If you move or select a new doctor, please call Boston Scientific Medical Records at to update your records. When you notify us of a change, we will send you a new identification card reflecting the change. 40
51 Living with your pacemaker system It is important to follow your doctor s instructions and keep your scheduled follow-up appointments. You should also do the following: Ask your doctor if you have any questions about or notice anything unusual with your device. Take the medications prescribed for you as instructed by your doctor. Carry your identification card and medication list with you at all times. 41
52 Tell your family doctor, dentist, and emergency personnel that you have a pacemaker. Special considerations Your doctor might ask you to avoid activities where the risk of unconsciousness could endanger you or others. These activities might include driving, swimming or boating alone, or climbing a ladder. Driving Driving laws and symptoms caused by your heart rhythm are often the deciding factors in whether 42
53 you will be allowed to drive. Your doctor will advise you about what is best for your safety and the safety of others. When to call your doctor Your doctor will provide guidelines for when you should contact him or her. In general, phone your doctor if you: Have a heart rate that drops below the minimum rate set for your pacemaker. Have symptoms of an abnormal heart rhythm and have been instructed to call. Notice any swelling, redness, or drainage from your incisions. 43
54 Develop a fever that does not go away in two or three days. Have questions about your device, heart rhythm, or medications. Plan to travel or move away. Work with your doctor to develop a follow-up plan while you are away. Notice anything unusual or unexpected, such as new symptoms or symptoms like the ones you had before you received your device. Remember that your pacemaker is designed to monitor and treat your slow heart rate. It can be a great source of reassurance for you and your friends and family. 44
55 Follow-up visits Your doctor will schedule regular follow-up visits. It is important that you attend these visits, even if you are feeling well. Your pacemaker has many programmable features; follow-up visits will help your doctor program your pacemaker to best meet your individual needs. During your visit, the doctor or nurse will use a programmer to check your device. The programmer is a special external computer that can communicate with your device in two ways: 1. By using radio frequency (RF) telemetry communication, if you have an RF-enabled device. 45
56 2. By using wanded telemetry communication. In this case, the doctor or nurse will place a wand over your skin near your device. A typical follow-up visit takes about 20 minutes. During your visit, your doctor or nurse will use the programmer to interrogate, or check, your device. They will review your device s memory to evaluate its performance since your last visit. If necessary, they will adjust your device s programmed settings. They will also check the battery to see how much energy is left. 46
57 What you should know about your pacemaker s battery A battery, safely sealed inside your device, provides the energy needed to monitor your heart rhythm and pace your heart. Just like any other type of battery, the battery in your device will be used up over time. Since the battery is permanently sealed within your device, it cannot be replaced when its energy is depleted. Instead, your entire device will need to be replaced (see Replacing your system on page 48). How long your pacemaker s battery lasts depends upon the settings your doctor programs and how much therapy you receive. 47
58 How will you know if your pacemaker s battery is running down? Device batteries have very predictable behavior over time. Your device will regularly check its own battery. At every follow-up visit, the doctor or nurse will also check to see how much energy is remaining in the battery. When the battery s energy level decreases to a certain point, your device will need to be replaced. Replacing your system Eventually, the energy in your device s battery will decrease to a point where your device will need to be replaced (see What you should know about your pacemaker s battery on page 47). Your doctor will 48
59 monitor your device s battery levels and determine when to replace your device. To replace your device, your doctor will surgically open the pocket of skin where your device is located. He or she will disconnect your old device from your leads and then check to make sure your leads work properly with your new device. In rare instances, your leads may not work properly with your new device, and your doctor may need to replace the leads. Your doctor will determine if your leads should be replaced. Should a lead need to be replaced, your doctor will insert a new lead into a vein, similar to how the 49
60 original lead was implanted. See Implanting your pacemaker system on page 26. Your doctor will then connect the leads to your new device. Finally, he or she will test your new system to make sure it is working properly. After the testing is complete, the pocket of skin will be closed. You may experience some discomfort from the incision as you recover from the surgery. You should be able to return to normal activities soon after the procedure. 50
61 Risks Risks encountered during a device and/or lead replacement procedure are similar to the risks of the initial implant, such as infection, tissue damage, and bleeding. See Implant risks on page 30. Be sure to talk with your doctor about the potential risks when making decisions about replacing your system. 51
62 Important safety information Your device has built-in features that protect it from interference produced by most electrical equipment. Most of the things you handle or work around on a daily basis are not going to affect your device. However, your device is sensitive to strong electromagnetic interference ( EMI) and can be affected by certain sources of electric or magnetic fields. If your employment requires you to be close to large industrial generators or sources of radar you may need special consideration before returning to work. If your work takes place in such an environment, please talk 52
63 with your physician. He or she may ask you to contact Boston Scientific Patient Services. Operating household appliances and tools Use the following guidelines for safe interaction with many common tools, appliances, and activities. Items that are safe under normal use: Air purifiers Blenders CD/DVD Players Clothes washing machines and dryers 53
64 Electric blankets Electric can openers Electric invisible fences Electric toothbrushes Fax/copy machines Hair dryers Heating pads Hot tubs/whirlpool baths NOTE: Consult with your doctor before using a hot tub. Your medical condition may not permit this activity; however, it will not harm your device. 54
65 Laser tag games Microwave ovens Ovens (electric, convection, or gas) Pagers Patient alert devices Personal computers Personal digital assistants (PDAs) NOTE: PDAs that also function as cell phones should be kept at least 6 inches away from your device. See Cellular phones on page 65. Portable space heaters 55
66 Radios (AM and FM) Remote controls (TV, garage door, stereo, camera/video equipment) Stoves (electric or gas) Tanning beds Televisions TV or radio towers (safe outside of restricted areas) Vacuum cleaners VCRs Video games 56
67 Warnings and precautions If you use any of the following items, it is important that you keep them the recommended distance away from your device to avoid interaction. Items that should not be placed directly over your device, but are otherwise safe to use: Cordless (household) telephones Electric razors Hand-held massagers 57
68 Portable MP3 and multimedia players (such as ipods ) that do not also function as a cellular phone (see Cellular phones on page 65) NOTE: While portable MP3 players themselves should not interfere with your device, the headphones or earbuds should be stored at least 6 inches (15 cm) away from your device, and you should avoid draping the headphones around your neck. ipod is a registered trademark of Apple Inc. 58
69 Items that should remain at least 6 inches (15 cm) away from your device: Cellular phones, including PDAs and portable MP3 players with integrated cellular phones NOTE: For more information on cellular phones, see Cellular phones on page 65. Devices transmitting Bluetooth or Wi-Fi signals (cellular phones, wireless Internet routers, etc.) Headphones and earbuds NOTE: It is safe to use headphones and earbuds, but you should refrain from draping them around your neck and from storing them in a breast or other shirt pocket that places them within 6 inches (15 cm) of your device. Bluetooth is a registered trademark of Bluetooth SIG, Inc. 59
70 Magnetic wands used in the game of Bingo Items that should remain at least 12 inches (30 cm) away from your device: Battery-powered cordless power tools Chain saws Corded drills and power tools Lawn mowers Leaf blowers Remote controls with antennas Shop tools (drills, table saws, etc.) Slot machines 60
71 Snowblowers Stereo speakers Items that should remain at least 24 inches (60 cm) away from your device: Arc welders CB and police radio antennas Running motors and alternators, especially those found in vehicles NOTE: Avoid leaning over running motors and alternators of a running vehicle. Alternators create large magnetic fields that can affect your device. However, the distance required to drive or ride in a vehicle is safe. 61
72 Items that should not be used: Body-fat measuring scales Jackhammers Magnetic mattresses and chairs Stun guns If you have questions about the EMI safety of a particular appliance, tool, or activity, please call Boston Scientific Patient Services at Theft detection and security systems Electronic antitheft systems and security gates or tag readers that include radio frequency identification 62
73 (RFID) equipment (often found in store and library doorways, and in point-of-entry access control systems) should not cause you any worry if you follow these guidelines: Walk through theft detection and security systems at a normal pace. Do not lean against or linger near these systems. If you are near an electronic antitheft, security, or entry control system and suspect interaction (experience symptoms) with your device from one of these systems, promptly move away from equipment nearby and inform your doctor. 63
74 Your Boston Scientific implantable device is unlikely to set off the alarm from an electronic antitheft or security system. Airport security Your device contains metal parts that may set off airport security metal detector alarms. The security archway will not harm your device. Tell security personnel that you have an implanted device and show them your Medical Device Identification Card. Airport security wands could temporarily affect your device. If possible, ask to be hand-searched instead of 64
75 being searched with a handheld wand. If a wand must be used, inform the security personnel that you have an implanted device. Tell the security personnel not to hold the wand over your device and to perform the search quickly. If you have questions about airport security, call your doctor or Boston Scientific Patient Services at Cellular phones Keep your cellular phone at least 6 inches (15 cm) away from your device. Your cellular phone is a source of EMI and could affect your device s operation. This interaction is temporary, and moving the phone away 65
76 from your device will return it to proper function. To reduce the chance of interaction, follow these precautions: Maintain a distance of at least 6 inches (15 cm) between the cellular phone and your device. If the phone transmits more than 3 watts, increase the distance to 12 inches (30 cm). Hold the cellular phone to your ear on the opposite side of your body from your device. Do not carry a cellular phone in a breast pocket or on a belt if that places the phone within 6 inches (15 cm) of your device. 66
77 These precautions apply only to cellular phones, not to household cordless phones. However, you should avoid placing your household cordless phone receiver directly over your device. Dental and medical procedures Some medical procedures could damage or otherwise affect your device. Be sure to always tell your dentist and physicians that you have an implanted device so that they can take the necessary precautions. Be especially careful with the following procedures: Magnetic resonance imaging (MRI): This is a diagnostic test that uses a strong electromagnetic 67
78 field. MRI scans can severely damage your device and should not be performed. Hospitals keep MRI equipment in rooms marked with signs that indicate magnets are inside. Do not go inside these rooms. Diathermy: This uses an electrical field to apply heat to tissues in the body and could damage your device or injure you. Diathermy should not be performed. Electrocautery: This is used during surgical procedures to stop vessels from bleeding. If electrocautery must be used, talk with your heart doctor and the doctor performing the medical procedure. 68
79 Electrolysis and Thermolysis: These are dermatology or hair removal procedures that pass electrical current into the skin. Talk with your heart doctor before having any electrolysis or thermolysis treatment. External defibrillation: This is a procedure, typically used in medical emergencies, that uses external equipment to deliver an electrical shock to your heart to restore a rapid and irregular heart rate to a normal rhythm. External defibrillation can affect your device, but can still be performed if necessary. If you receive external defibrillation, be sure to contact your physician as soon as possible 69
80 following the emergency to verify that your device is functioning properly. Lithotripsy: This is a medical procedure that is used to break up stones in the urinary tract (e.g., kidney stones). Lithotripsy can damage your device if certain precautions are not taken. Talk with your heart doctor as well as the doctor performing the procedure about what can be done to protect your device. Therapeutic radiation treatment for cancer: This procedure can affect your device and will require special precautions. If you should need radiation treatment, talk with your heart doctor as well as the doctor performing the medical procedure. 70
81 Transcutaneous Electrical Nerve Stimulation (TENS) unit: This is a device prescribed by physicians or chiropractors for control of chronic pain. A TENS unit can affect your device and will require special precautions. If you must use a TENS unit, talk with your heart doctor. Most medical and dental procedures will not affect your device. Some examples include: Dental drills and cleaning equipment Diagnostic X-rays Diagnostic ultrasound procedures Mammograms 71
82 NOTE: Mammograms will not interfere with your device. However, your device could be damaged if it gets compressed in the mammogram machine. Make sure the doctor or technician knows that you have an implanted device. EKG machines CT scans If you need to undergo any surgical procedures, tell your dentist and/or doctor that you have a pacemaker system. They can contact the physician who monitors your device to find the best way to provide treatment. If you have questions about a specific appliance, tool, medical procedure, or piece of equipment, please 72
83 talk with your doctor or call Boston Scientific Patient Services at
84 Summary It is natural for you to feel anxious or nervous about receiving a pacemaker. Remember that your pacemaker system can be a great source of reassurance for you and your friends and family. Talking with other pacemaker patients is often helpful while adjusting to your new device. Ask your doctor, nurse, or Boston Scientific representative if there is a local pacemaker patient support group in your area. The information presented in this handbook is intended to help you understand more about your heart condition 74
85 and your device. If you have questions about what you have read, be sure to ask your doctor or nurse. They are your best resource for information about your particular needs or situation. 75
86 Visit us on the Internet Boston Scientific s patient-focused website, LifeBeat Online, offers a variety of information of interest to people with cardiac devices, including cardiac news, health tips, patient stories, frequently asked questions about living with your implanted device, and links to additional resources. You can also subscribe to have the free newsletter delivered to your address. 76
87 Notes and questions Use this space to write down questions or additional information about your device: 77
88 78
89 Index A Activities, 38, 42 Airport security, 64 Atria, 15 B Battery, 47 end of life, 47, 48 Bluetooth, 59 Bradycardia, 17 C Calling your doctor, 43 Catheter, 7 Cellular phones, 59, 65 Cordless phones, 57, 67 CT scans, 72 Boating, 42 79
90 D Dental equipment, 71 Dental procedures, 67 Dermatology procedures, 69 Device, 21 dual-chamber, 24 implanting, 26 reliability, 3 replacing, 48 single-chamber, 23 Diathermy, 68 Driving, 42 E EKG machines, 72 Electrocautery, 68 Electrolysis, 69 Electromagnetic interference (EMI), 52 Electronics precautions, 52 Electrophysiology, 8 Exercise, 38 External defibrillation, 69 F Follow-up visits, 45 80
91 G Glossary, 5 H Hair removal procedures, 69 Heart block, 17 Heart function, 15 Household appliances precautions, 53 I Identification card, 39 Implanting the system, 26 recovery, 35 risks, 30 ipods, 58 L Ladders, 42 Leads, 25 implanting, 26 replacing, 49 Lithotripsy, 70 Living with your device, 41 ID card, 39 M Mammograms, 71 81
92 Medical procedures, 67 Medications, 37 MP3 and multimedia players, 58 MRI, 67 P Pacemaker system, 21 device, 21 dual-chamber, 24 implanting, 26 leads, 25 reliability, 3 replacing, 48 risks, 30 single-chamber, 23 Precautions, 52 airport security, 64 cellular phones, 59, 65 dental procedures, 67 diathermy, 68 electrocautery, 68 electrolysis, 69 external defibrillation, 69 household appliances, 53 lithotripsy, 70 medical procedures, 67 MRI, 67 radiation treatment, 70 TENS unit, 71 82
93 theft detection and security systems, 62 thermolysis, 69 tools, 53 Programmer, 22, 45 Pulse generator, see Device R Radar, 52 Radiation treatment, 70 Radio frequency (RF) telemetry, 45 Recovery, 35 Reliability, 3 Replacing the system, 48 risks, 51 Risks, see Precautions electromagnetic interference, 52 implant procedure, 31 post-implant, 32 replacement procedure, 51 S Safety, see Precautions Security systems, 62 Sinoatrial (SA) node, 15 Swimming, 42 83
94 T Telemetry communication radio frequency (RF), 45 wanded, 46 TENS units, 71 Theft detection and security systems, 62 Thermolysis, 69 Tools precautions, 53 Traveling, 38, 44 airport security, 64 U Ultrasound, 71 V Ventricles, 17 W Wanded telemetry, 46 Warnings, see Precautions X X-rays, 71 84
95 85
96 86
97
98 Boston Scientific 4100 Hamline Avenue North St. Paul, MN USA Tel: Medical Professionals: CARDIAC ( ) Patients and Families: * * 2014 Boston Scientifi c Corporation or its affi liates. All rights reserved. Brady EN US
Implantable Cardioverter Defibrillator Therapy
 Implantable Cardioverter Defibrillator Therapy A Message to Patients Boston Scientific Corporation acquired Guidant Corporation in April 2006. During our transition period, you may see both the Boston
Implantable Cardioverter Defibrillator Therapy A Message to Patients Boston Scientific Corporation acquired Guidant Corporation in April 2006. During our transition period, you may see both the Boston
Living with Your Pacemaker
 Brief Statement Additional Device Information An implantable pacemaker system relieves symptoms of heart rhythm disturbances. They do this by restoring normal heart rates. A normal heart rate provides
Brief Statement Additional Device Information An implantable pacemaker system relieves symptoms of heart rhythm disturbances. They do this by restoring normal heart rates. A normal heart rate provides
Caring for Your Pacemaker
 Patient Education Caring for Your Pacemaker What you need to know Weekdays between 8 a.m. and 4:30 p.m., call an Electrophysiology (EP) Nurse at 206-598-4555. Weekends, holidays, or after hours, call the
Patient Education Caring for Your Pacemaker What you need to know Weekdays between 8 a.m. and 4:30 p.m., call an Electrophysiology (EP) Nurse at 206-598-4555. Weekends, holidays, or after hours, call the
Living With Your Pacemaker
 2012 Living With Your Pacemaker Living With Your Pacemaker The pamphlet will help you learn what your new pacemaker can do for you. The heart s natural pacemaker Your heart s natural pacemaker controls
2012 Living With Your Pacemaker Living With Your Pacemaker The pamphlet will help you learn what your new pacemaker can do for you. The heart s natural pacemaker Your heart s natural pacemaker controls
Pacemaker. My follow-up questions: Living With Your. sjm.com
 My follow-up questions: Global Headquarters Cardiac Rhythm One St. Jude Medical Drive Management Division St. Paul, Minnesota 55117 15900 Valley View Court USA Sylmar, California 91342 + 1 651 756 2000
My follow-up questions: Global Headquarters Cardiac Rhythm One St. Jude Medical Drive Management Division St. Paul, Minnesota 55117 15900 Valley View Court USA Sylmar, California 91342 + 1 651 756 2000
PACEMAKER PATIENT INFORMATION
 PACEMAKER PATIENT INFORMATION Information Leaflet Your Health. Our Priority. Page 2 of 11 Contents What is a pacemaker? Why do I need a pacemaker? The heart and normal electrical conduction Complete or
PACEMAKER PATIENT INFORMATION Information Leaflet Your Health. Our Priority. Page 2 of 11 Contents What is a pacemaker? Why do I need a pacemaker? The heart and normal electrical conduction Complete or
What Are Arrhythmias?
 What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
IMPLANTABLE CARDIOVERTER DEFIBRILLATORS (ICDs)
 Work with Your Doctor An ICD is not a cure for heart rhythm problems. You ll likely still need medications and other forms of treatment. But you can feel confident that your ICD will protect you from a
Work with Your Doctor An ICD is not a cure for heart rhythm problems. You ll likely still need medications and other forms of treatment. But you can feel confident that your ICD will protect you from a
The science of medicine. The compassion to heal.
 A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
Catheter Ablation. A Guided Approach for Treating Atrial Arrhythmias
 Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Electrophysiology study (EPS)
 Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
INSERTABLE CARDIAC MONITORING SYSTEM. UNLOCK the ANSWER. Your heart and long-term monitoring
 INSERTABLE CARDIAC MONITORING SYSTEM UNLOCK the ANSWER Your heart and long-term monitoring UNLOCK the ANSWER Irregular heartbeats can be related to a variety of conditions, including unexplained fainting,
INSERTABLE CARDIAC MONITORING SYSTEM UNLOCK the ANSWER Your heart and long-term monitoring UNLOCK the ANSWER Irregular heartbeats can be related to a variety of conditions, including unexplained fainting,
Atrioventricular (AV) node ablation
 Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Vagus Nerve Stimulation (VNS)
 Vagus Nerve Stimulation (VNS) Your doctor has suggested Vagus Nerve Stimulation (VNS) as an extra treatment to reduce the number of seizures you or your child has as well as how long they last. Either
Vagus Nerve Stimulation (VNS) Your doctor has suggested Vagus Nerve Stimulation (VNS) as an extra treatment to reduce the number of seizures you or your child has as well as how long they last. Either
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
What Can I Do about Atrial Fibrillation (AF)?
 Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
A Patient Guide to Atrial Fibrillation and Catheter Ablation
 A Patient Guide to Atrial Fibrillation and Catheter Ablation Al-Sabah Arrhythmia Institute 1111 Amsterdam Avenue New York, NY 10025 Phone: 212-523-2400 Fax: 212-523-2571 www.stlukescardiology.org Printed
A Patient Guide to Atrial Fibrillation and Catheter Ablation Al-Sabah Arrhythmia Institute 1111 Amsterdam Avenue New York, NY 10025 Phone: 212-523-2400 Fax: 212-523-2571 www.stlukescardiology.org Printed
Understanding. Pacemakers. Your Heart s Electrical System How a Pacemaker Can Help Your Heart Living with a Pacemaker
 Understanding Pacemakers Your Heart s Electrical System How a Pacemaker Can Help Your Heart Living with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at
Understanding Pacemakers Your Heart s Electrical System How a Pacemaker Can Help Your Heart Living with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at
Will I still need medicines for my arrhythmia? What kind of exercises can I do? Can I travel abroad? Is it possible to dislodge the ICD?
 Living with an internal cardiac defibrillator (ICD) to regulate your heart The aim of this leaflet is to answer any questions you may have about living with an internal cardiac defibrillator (ICD). If
Living with an internal cardiac defibrillator (ICD) to regulate your heart The aim of this leaflet is to answer any questions you may have about living with an internal cardiac defibrillator (ICD). If
PATHWAY TO YOUR PACEMAKER. Patient Information Booklet (Disponible en français)
 PATHWAY TO YOUR PACEMAKER Patient Information Booklet (Disponible en français) PACEMAKER PATIENT PATHWAY WHAT IS A PACEMAKER? A pacemaker is a small device placed under the skin of your chest to help control
PATHWAY TO YOUR PACEMAKER Patient Information Booklet (Disponible en français) PACEMAKER PATIENT PATHWAY WHAT IS A PACEMAKER? A pacemaker is a small device placed under the skin of your chest to help control
VNS Therapy for Epilepsy
 VNS Therapy for Epilepsy This pamphlet provides general information for the public. It is not intended to cover all possible uses, directions, precautions, interactions or adverse effects involving any
VNS Therapy for Epilepsy This pamphlet provides general information for the public. It is not intended to cover all possible uses, directions, precautions, interactions or adverse effects involving any
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
NeuroPace. RNS System Patient Manual
 NeuroPace RNS System Patient Manual CAUTION: Federal law restricts this device to sale by or on the order of a physician. 01/2013 DN 1013555 Rev 2 1 2013 NeuroPace, Inc. 2 This Manual supports: RNS Neurostimulator
NeuroPace RNS System Patient Manual CAUTION: Federal law restricts this device to sale by or on the order of a physician. 01/2013 DN 1013555 Rev 2 1 2013 NeuroPace, Inc. 2 This Manual supports: RNS Neurostimulator
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Electrophysiology Heart Study - EPS -
 Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Patient Information Booklet. Endovascular Stent Grafts: A Treatment for Abdominal Aortic Aneurysms
 Patient Information Booklet Endovascular Stent Grafts: A Treatment for Abdominal Aortic Aneurysms TABLE OF CONTENTS Introduction 1 Glossary 2 Abdominal Aorta 4 Abdominal Aortic Aneurysm 5 Causes 6 Symptoms
Patient Information Booklet Endovascular Stent Grafts: A Treatment for Abdominal Aortic Aneurysms TABLE OF CONTENTS Introduction 1 Glossary 2 Abdominal Aorta 4 Abdominal Aortic Aneurysm 5 Causes 6 Symptoms
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
Heart Attack: What You Need to Know
 A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
Vagus Nerve Stimulator (VNS)
 Directorate of Children s Services Vagus Nerve Stimulator (VNS) Information booklet for parents/carers This is an information booklet for families and carers of young people who have, or are considering
Directorate of Children s Services Vagus Nerve Stimulator (VNS) Information booklet for parents/carers This is an information booklet for families and carers of young people who have, or are considering
What to Know About. Atrial Fibrillation
 Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Percutaneous Abscess Drainage
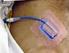 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Pacemakers. Information for people with pacemakers, and for their family and friends
 Pacemakers Information for people with pacemakers, and for their family and friends Produced by British Heart Foundation 14 Fitzhardinge Street London W1H 6DH Phone: 020 7935 0185 Website: www.bhf.org.uk
Pacemakers Information for people with pacemakers, and for their family and friends Produced by British Heart Foundation 14 Fitzhardinge Street London W1H 6DH Phone: 020 7935 0185 Website: www.bhf.org.uk
The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation
 The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation 2 P a g e Table of Contents Introduction How the Heart Works 3 How the Heart s Electrical System Works 3 Commonly Used Heart
The Patient s Guide to the Electrophysiologic Study (EPS) and Catheter Ablation 2 P a g e Table of Contents Introduction How the Heart Works 3 How the Heart s Electrical System Works 3 Commonly Used Heart
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
Living With Your CRT-D. A patient s guide to understanding Cardiac Resynchronization Therapy Defibrillators (CRT-Ds) Compliments of your doctor and
 Living With Your CRT-D A patient s guide to understanding Cardiac Resynchronization Therapy Defibrillators (CRT-Ds) Compliments of your doctor and 1 St. Jude Medical thanks James G. Porterfield, M.D.,
Living With Your CRT-D A patient s guide to understanding Cardiac Resynchronization Therapy Defibrillators (CRT-Ds) Compliments of your doctor and 1 St. Jude Medical thanks James G. Porterfield, M.D.,
Medical Procedures and EMI Precautions
 Medical Procedures and EMI Precautions for MR Conditional Cardiac Implantable Electronic Devices Manual for Health Care Professionals 0123 The following list includes trademarks or registered trademarks
Medical Procedures and EMI Precautions for MR Conditional Cardiac Implantable Electronic Devices Manual for Health Care Professionals 0123 The following list includes trademarks or registered trademarks
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Radiofrequency Ablation for Atrial Fibrillation. A Guide for Adults
 Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Living With Your ICD. A patient s guide to understanding Implantable Cardioverter Defibrillators (ICDs) Compliments of your doctor and
 Living With Your ICD A patient s guide to understanding Implantable Cardioverter Defibrillators (ICDs) Compliments of your doctor and St. Jude Medical thanks James G. Porterfield, M.D., and Linda M. Porterfield,
Living With Your ICD A patient s guide to understanding Implantable Cardioverter Defibrillators (ICDs) Compliments of your doctor and St. Jude Medical thanks James G. Porterfield, M.D., and Linda M. Porterfield,
Visited 9/14/2011. What is Atrial Fibrillation? What you need to know about Atrial Fibrillation. The Normal Heart Rhythm. 1 of 7 9/14/2011 10:50 AM
 1 of 7 9/14/2011 10:50 AM Current URL: What you need to know about Atrial Fibrillation What is atrial fibrillation? What causes atrial fibrillation? How is atrial fibrillation diagnosed? What are the dangers
1 of 7 9/14/2011 10:50 AM Current URL: What you need to know about Atrial Fibrillation What is atrial fibrillation? What causes atrial fibrillation? How is atrial fibrillation diagnosed? What are the dangers
PACEMAKERS AND ANTITACHYCARDIA DEVICES WILLIAM BATSFORD, M.D.
 CHAPTER 26 PACEMAKERS AND ANTITACHYCARDIA DEVICES WILLIAM BATSFORD, M.D. INTRODUCTION The heart s natural pacemaker is an electrical timing device that controls the rate of the heart s muscular contractions,
CHAPTER 26 PACEMAKERS AND ANTITACHYCARDIA DEVICES WILLIAM BATSFORD, M.D. INTRODUCTION The heart s natural pacemaker is an electrical timing device that controls the rate of the heart s muscular contractions,
Atrial Fibrillation (AF) Explained
 James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
Advances in the Treatment of Atrial Fibrillation At VCU Medical Center
 Contact Us For additional information or to schedule an appointment with one of our specialists, please call: Ken Ellenbogen, M.D. Cardiology/Electrophysiology 804-828-7565 or 804-628-0147 You can also
Contact Us For additional information or to schedule an appointment with one of our specialists, please call: Ken Ellenbogen, M.D. Cardiology/Electrophysiology 804-828-7565 or 804-628-0147 You can also
CARDIOLOGIST What does a cardiologist do? A cardiologist is a doctor who specializes in caring for your heart and blood vessel health.
 YOUR TREATMENT TEAM CARDIOLOGIST What does a cardiologist do? A cardiologist is a doctor who specializes in caring for your heart and blood vessel health. To become a cardiologist, a doctor completes additional
YOUR TREATMENT TEAM CARDIOLOGIST What does a cardiologist do? A cardiologist is a doctor who specializes in caring for your heart and blood vessel health. To become a cardiologist, a doctor completes additional
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Treatments to Restore Normal Rhythm
 Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Electroconvulsive Therapy - ECT
 Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
GENERAL HEART DISEASE KNOW THE FACTS
 GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
About the British Heart Foundation
 Pacemakers About the British Heart Foundation As the nation s heart charity, we have been funding cutting-edge research that has made a big difference to people s lives. But the landscape of heart disease
Pacemakers About the British Heart Foundation As the nation s heart charity, we have been funding cutting-edge research that has made a big difference to people s lives. But the landscape of heart disease
Activity 4.2.3: EKG. Introduction. Equipment. Procedure
 Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation and Ablation Therapy: A Patient s Guide
 Atrial Fibrillation and Ablation Therapy: A Patient s Guide ATRIAL FIBRILLATION CENTER AT UNIVERSITY OF ROCHESTER MEDICAL CENTER www.heart.urmc.edu 585-275-4775 INTRODUCTION Our goal at the Atrial Fibrillation
Atrial Fibrillation and Ablation Therapy: A Patient s Guide ATRIAL FIBRILLATION CENTER AT UNIVERSITY OF ROCHESTER MEDICAL CENTER www.heart.urmc.edu 585-275-4775 INTRODUCTION Our goal at the Atrial Fibrillation
Inferior Vena Cava Filter Placement and Removal
 Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION
 PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION This booklet was designed to help you and the important people in your life understand the treatment of high dose chemotherapy with stem cell support: a procedure
PERIPHERAL STEM CELL TRANSPLANT INTRODUCTION This booklet was designed to help you and the important people in your life understand the treatment of high dose chemotherapy with stem cell support: a procedure
Atrial Fibrillation Centre
 About this guide We have prepared this guide to help you to: learn about atrial fibrillation manage atrial fibrillation and reduce the risk of stroke find out about medicines and other treatment options
About this guide We have prepared this guide to help you to: learn about atrial fibrillation manage atrial fibrillation and reduce the risk of stroke find out about medicines and other treatment options
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona
 Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Living with. Atrial Fibrillation
 Living with Atrial Fibrillation U nderstanding Atrial Fibrillation An estimated 2.7 million Americans are living with atrial fibrillation (AF). That makes it the most common heart rhythm abnormality in
Living with Atrial Fibrillation U nderstanding Atrial Fibrillation An estimated 2.7 million Americans are living with atrial fibrillation (AF). That makes it the most common heart rhythm abnormality in
ICD/S-ICD patient information
 ICD/S-ICD patient information Promoting better understanding, diagnosis, treatment and quality of life for those affected by heart rhythm disorders (cardiac arrhythmias) www.heartrhythmcharity.org.uk Registered
ICD/S-ICD patient information Promoting better understanding, diagnosis, treatment and quality of life for those affected by heart rhythm disorders (cardiac arrhythmias) www.heartrhythmcharity.org.uk Registered
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Suffering from varicose veins? Patient Information. ELVeS Radial Minimally invasive laser therapy of venous insufficiency
 Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery
 Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Rate and Rhythm Control Stroke Prevention A Comprehensive Resource from the Heart Rhythm Society SM This information is not intended
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Rate and Rhythm Control Stroke Prevention A Comprehensive Resource from the Heart Rhythm Society SM This information is not intended
A Patient s Guide to the Calypso System for Breast Cancer Treatment
 A Patient s Guide to the Calypso System for Breast Cancer Treatment Contents Introduction How Radiation Works To Treat Cancer Radiation Treatment for Breast Cancer Special Concerns for Treating the Left
A Patient s Guide to the Calypso System for Breast Cancer Treatment Contents Introduction How Radiation Works To Treat Cancer Radiation Treatment for Breast Cancer Special Concerns for Treating the Left
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Patient Information. PORT-A-CATH Implantable Venous Access Systems
 Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation
 INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
Varicose Vein Treatment (Endovenous Ablation of Varicose Veins)
 Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
Transcatheter Aortic Valve Implantation (TAVI) A patient s guide
 Transcatheter Aortic Valve Implantation (TAVI) A patient s guide Valvular heart disease The heart is a muscle which pumps blood to your lungs and around the body. There are four valves within the heart.
Transcatheter Aortic Valve Implantation (TAVI) A patient s guide Valvular heart disease The heart is a muscle which pumps blood to your lungs and around the body. There are four valves within the heart.
Breast Cancer Radiation Therapy: What You Need to Know
 Breast Cancer Radiation Therapy: What You Need to Know The information in this pamphlet is for patients, family members and caregivers. What is radiation treatment? Radiation treatment uses high energy
Breast Cancer Radiation Therapy: What You Need to Know The information in this pamphlet is for patients, family members and caregivers. What is radiation treatment? Radiation treatment uses high energy
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Atrial Fibrillation. Information for you, and your family, whänau and friends. Published by the New Zealand Guidelines Group
 Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Indoor Environment Electromagnetic Radiation
 Indoor Environment Electromagnetic Radiation Purpose: To increase the students awareness of the sources of electric and magnetic fields and the potential for adverse health effects from prolonged exposure
Indoor Environment Electromagnetic Radiation Purpose: To increase the students awareness of the sources of electric and magnetic fields and the potential for adverse health effects from prolonged exposure
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
Ureteroscopy with Laser Lithotripsy
 Ureteroscopy with Laser Lithotripsy Introduction Kidney stones are fairly common. Although kidney stones can be very painful, they are treatable, and in many cases preventable. Your doctor may recommend
Ureteroscopy with Laser Lithotripsy Introduction Kidney stones are fairly common. Although kidney stones can be very painful, they are treatable, and in many cases preventable. Your doctor may recommend
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery
 CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
CARDIAC REHABILITATION PROGRAM
 CARDIAC REHABILITATION PROGRAM Preparation for the Cardiac Rehabilitation Program After your heart problem is stable, your physician or cardiologist will refer you to the Cardiac Rehabilitation program.
CARDIAC REHABILITATION PROGRAM Preparation for the Cardiac Rehabilitation Program After your heart problem is stable, your physician or cardiologist will refer you to the Cardiac Rehabilitation program.
Cardiac Catheter Lab Information for patients having a Coronary Angiogram
 Cardiac Catheter Lab Information for patients having a Coronary Angiogram Page 1 of 5 What is a Coronary Angiogram? This is a test that uses dye and special x-rays to show the inside of your coronary arteries.
Cardiac Catheter Lab Information for patients having a Coronary Angiogram Page 1 of 5 What is a Coronary Angiogram? This is a test that uses dye and special x-rays to show the inside of your coronary arteries.
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
