Non-Small Cell Lung Cancer
|
|
|
- Dwain Thompson
- 8 years ago
- Views:
Transcription
1 NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Non-Small Cell Lung Cancer Version NCCN.org NCCN Guidelines for Patients available at Continue
2 CLINICAL ASSESSMENT PRETREATMENT EVALUATION g INITIAL TREATMENT Stage IA (peripheral T1ab, N0) Stage IB (peripheral T2a, N0) Stage I (central T1ab T2a, N0) Stage II (T1ab 2ab, N1; T2b, N0) Stage IIB (T3, N0) e PFTs (if not previously done) Bronchoscopy (intraoperative preferred) Pathologic mediastinal lymph node evaluation h (category 2B) PET/CT scan i (if not previously done) PFTs (if not previously done) Bronchoscopy Pathologic mediastinal lymph node evaluation h PET/CT scan i (if not previously done) Brain MRI (Stage II, Negative mediastinal nodes Positive mediastinal nodes Negative mediastinal nodes Positive mediastinal nodes Operable Medically inoperable Operable Medically inoperable Surgical exploration and resection j + mediastinal lymph node dissection or systematic lymph node sampling ablative radiotherapy k (SABR) l See Stage IIIA (NSCL-7) or Stage IIIB (NSCL-11) Surgical exploration and resection j,m + mediastinal lymph node dissection or systematic lymph node sampling N0 N1 RT including SABR j,k k,p See Adjuvant Treatment (NSCL-3) See Adjuvant Treatment (NSCL-3) Consider adjuvant chemotherapy n (category 2B) for highrisk stages IB-II o See Stage IIIA (NSCL-7) or Stage IIIB (NSCL-11) e T3, N0 related to size or satellite nodules. g Testing is not listed in order of priority and is dependent upon clinical circumstances, institutional processes, and judicious use of resources. h Methods for evaluation include mediastinoscopy, mediastinotomy, EBUS, EUS, and CT-guided biopsy. i Positive PET/CT scan findings for distant disease need pathologic or other radiologic confirmation. If PET/CT scan is positive in the mediastinum, lymph node status needs pathologic confirmation. j See Principles of Surgical Therapy (NSCL-B). k See Principles of Radiation Therapy (NSCL-C). l Interventional radiology ablation is an option for selected patients. m After surgical evaluation, patients likely to receive adjuvant chemotherapy may be treated with induction chemotherapy as an alternative. n See Chemotherapy Regimens for Neoadjuvant and Adjuvant Therapy (NSCL-D). o Examples of high-risk factors may include poorly differentiated tumors (including lung neuroendocrine tumors [excluding well-differentiated neuroendocrine tumors]), vascular invasion, wedge resection, tumors >4 cm, visceral pleural involvement, and incomplete lymph node sampling (Nx). These factors independently may not be an indication and may be considered when determining treatment with adjuvant chemotherapy. p See Chemotherapy Regimens Used with Radiation Therapy (NSCL-E). NSCL-2
3 CLINICAL PRESENTATION INITIAL TREATMENT Low risk of becoming symptomatic x Observation Surveillance (NSCL-14) Multiple lung cancers Asymptomatic Multiple lesions Solitary lesion (metachronous disease) High risk of becoming symptomatic x local therapy possible Parenchymal sparing resection (preferred) j,y or Radiation k or Ablation Symptomatic local therapy not possible Consider palliative chemotherapy ± local palliative therapy See Systemic Therapy for Metastatic Disease (NSCL-16) j See Principles of Surgical Therapy (NSCL-B). k See Principles of Radiation Therapy (NSCL-C). x Lesions at low risk of becoming symptomatic can be observed (eg, small subsolid nodules with slow growth). However, if the lesion(s) becomes symptomatic or becomes high risk for producing symptoms (eg, subsolid nodules with accelerating growth or increasing solid component or increasing FDG uptake, even while small), treatment should be considered. y Lung-sparing resection is preferred, but tumor distribution and institutional expertise should guide individual treatment planning. NSCL-10
4 CLINICAL ASSESSMENT Stage IV, M1b: limited sites aa PRETREATMENT EVALUATION Pathologic mediastinal lymph node evaluation h Bronchoscopy Brain MRI PET/CT scan i (if not previously done) Brain bb Adrenal Pathologic diagnosis by needle or resection INITIAL TREATMENT Surgical resection, j followed by whole brain RT k (WBRT) (category 1) or stereotactic radiosurgery k (SRS) or SRS + WBRT k (category 1 for one metastasis) or SRS k alone Local therapy for adrenal lesion cc (if lung lesion curable, based on T and N stage) (category 2B) dd or See Systemic Therapy for Metastatic Disease (NSCL-16) T1-2, N0-1; T3, N0 T1-2, N2; T3, N1-2; Any T, N3; T4, Any N Surgical resection of lung lesion j or SABR of lung lesion or Chemotherapy ee Chemotherapy ee Surgical resection of lung lesion j or SABR of lung lesion See Systemic Therapy for Metastatic Disease (NSCL-16) h Methods for evaluation include mediastinoscopy, mediastinotomy, EBUS, EUS, and CT-guided biopsy. i Positive PET/CT scan findings for distant disease need pathologic or other radiologic confirmation. If PET/CT scan is positive in the mediastinum, lymph node status needs pathologic confirmation. j See Principles of Surgical Therapy (NSCL-B). k See Principles of Radiation Therapy (NSCL-C). aa Aggressive local therapy may be appropriate for selected patients with limited-site oligometastatic disease. bb See NCCN Guidelines for Central Nervous System Cancers. cc May include adrenalectomy or RT (including SABR). dd Patients with N2 disease have a poor prognosis and systemic therapy should be considered. ee See Systemic Therapy for Advanced or Metastatic Disease (NSCL-F). NSCL-13
5 THERAPY FOR RECURRENCE AND METASTASIS Locoregional recurrence Endobronchial obstruction Resectable recurrence Mediastinal lymph node recurrence Superior vena cava (SVC) obstruction No prior RT Prior RT Laser/stent/other surgery j External-beam RT or brachytherapy k Photodynamic therapy Reresection (preferred) j External-beam RT or SABR k,l Concurrent chemoradiation k,p Systemic therapy ee Concurrent chemoradiation k,p (if not previously given) External-beam RT k SVC stent No evidence of disseminated disease Evidence of disseminated disease Observation or Systemic therapy ee (category 2B) See Systemic Therapy for Metastatic Disease (NSCL-16) Severe hemoptysis External-beam RT or brachytherapy k Laser or photodynamic therapy or embolization Surgery Localized symptoms Palliative external-beam RT k Distant metastases Diffuse brain metastases Bone metastasis Palliative external-beam RT k,bb Palliative external-beam RT k + orthopedic stabilization, if risk of fracture Consider bisphosphonate therapy or denosumab See Systemic Therapy for Metastatic Disease (NSCL-16) Solitary metastasis See pathway for Stage IV, M1b, solitary site (NSCL-13) Disseminated metastases See Systemic Therapy for Metastatic Disease (NSCL-16) j See Principles of Surgical Therapy (NSCL-B). k See Principles of Radiation Therapy (NSCL-C). l Interventional radiology ablation is an option for selected patients. p See Chemotherapy Regimens Used with Radiation Therapy (NSCL-E). bb See NCCN Guidelines for Central Nervous System Cancers. ee See Systemic Therapy for Advanced or Metastatic Disease (NSCL-F). NSCL-15
6 PRINCIPLES OF RADIATION THERAPY (1 of 9) General Principles (see Table 1. Commonly Used Abbreviations in Radiation Therapy) cancer RT as a prominent part of their practice. evaluation or discussion should be provided for all patients with NSCLC. The critical goals of modern RT are to maximize tumor control and to minimize treatment toxicity. A minimum technologic standard is CTplanned 3D-CRT. 1 More advanced technologies are appropriate when needed to deliver curative RT safely. These technologies include (but are not limited to) 4D-CT and/or PET/CT simulation, IMRT/VMAT, IGRT, motion management, and proton therapy ( Reimbursement/Model-Policies.aspx). Nonrandomized comparisons of using advanced technologies versus older techniques demonstrate reduced toxicity and improved survival. 2-4 credentialing of both treatment planning and delivery such as required for participation in RTOG clinical trials employing advanced technologies. Useful references include the ACR-ASTRO Practice Guidelines for Radiation Oncology ( SABR (also known as SBRT) is recommended for patients who are medically inoperable or who refuse to have surgery after thoracic surgery evaluation. SABR has achieved primary tumor control rates and overall survival, comparable to lobectomy and higher than 3D-CRT in nonrandomized and population-based comparisons in medically inoperable or older patients D-CRT regimens are alternatives In patients treated with surgery, postoperative radiotherapy (PORT) is not recommended unless there are positive margins or upstaging to N2 (see below). The standard of care for patients with inoperable stage II and stage III is concurrent chemort ( pdf) RT interruptions and dose reductions for manageable acute toxicities should be avoided by employing supportive care. Sequential chemort or RT alone is appropriate for frail patients unable to tolerate concurrent therapy. 18,19 ( pdf) NSCL-C 1 OF 9
7 PRINCIPLES OF RADIATION THERAPY (2 of 9) (continued) 20,21 RT has a role before or after surgery. Preoperative concurrent chemort is an option for patients with resectable stage IIIA (minimal N2 and treatable with lobectomy) 22 and is recommended for resectable superior sulcus tumors Preoperative chemotherapy and postoperative RT is an alternative for patients with resectable stage IIIA. 25,26 The determination of resectability in trimodality therapy should be made prior to initiation of all treatment. chemotherapy in non-randomized analyses. 27,28 Although the optimal sequence is not established, PORT is generally administered after and is recommended for positive resection margins. PORT is not recommended for patients with pathologic stage N0-1 disease, because it has been associated with increased mortality, at least when using older RT techniques. 32 RT is recommended for local palliation or prevention of symptoms (such as pain, bleeding, or obstruction). achieves prolonged survival in a small proportion of well-selected patients with good performance status who have also received radical delivered safely to the involved sites. 33,34 See the NCCN Guidelines for Central Nervous System Cancers regarding RT for brain metastases. Target Volumes, Prescription Doses, and Normal Tissue Dose Constraints (See Tables 2 5 on NSCL-C 6 of 9 and NSCL-C 7 of 9) (primary and nodal) on imaging and pathologic assessment, CTV includes regions of presumed microscopic extent or dissemination, and PTV comprises the ITV (which includes margin for target motion) plus a setup margin for positioning and mechanical variability. PTV margin can be decreased by immobilization, motion management, and IGRT techniques. Consistent delineation of normal structures is critical for evaluating plans for safety. The RTOG consensus lung-contouring atlas is a useful resource. Commonly used prescription doses and normal tissue dose constraints are summarized in Tables 2 through 5. These are based on published experience, ongoing trials, historical data, modeling, and empirical judgment. 35,36 Useful references include the recent reviews of normal organ dose responses from the QUANTEC project NSCL-C 2 OF 9
8 PRINCIPLES OF RADIATION THERAPY (3 of 9) The high-dose intensity and conformity of SABR require minimizing the PTV. regimens. 42 regimens are appropriate as well. 42,43 adapted SABR regimens appear to be effective and safe, 43,44 while 54 to 60 Gy in 3 fractions is unsafe and should be avoided. 45 The dose for 5-fraction regimens is being studied prospectively in RTOG SABR is most commonly used for tumors up to 5 cm in size, though selected larger isolated tumors can be treated safely if normal tissue constraints are respected. 46 Prescription doses incompletely describe the actual delivered doses, which also strongly depend on how the dose is prescribed (to the isocenter vs. an isodose volume covering a proportion of the PTV), the degree of dose heterogeneity, whether tissue density heterogeneity corrections are used, and the type of dose calculation algorithm. 47,48 All of these must be considered when interpreting or emulating regimens from prior studies. IFI omitting ENI allows tumor dose escalation and is associated with a low risk of isolated nodal relapse, particularly in PET/CT staged patients One randomized trial found improved survival for IFI versus ENI, possibly because it enabled dose escalation. 54 IFI is 55 Dose escalation in RT alone, 56 sequential chemort, 57 or concurrent chemort 58 is associated with better survival in non-randomized comparisons. While doses of up to 74 Gy with concurrent chemotherapy can be delivered safely when normal tissue dose constraints are respected, preliminary results from RTOG 0617, comparing 60 versus 74 Gy with concurrent chemotherapy, found that 74 Gy does not improve overall survival, and therefore is not currently a standard dose. 63 A meta-analysis demonstrated improved survival with accelerated fractionation RT regimens, 64 safely be administered and achieve promising nodal clearance and survival rates, but require experience in thoracic surgical techniques to minimize the risk of surgical complications after high-dose RT. In PORT, the CTV includes the bronchial stump and high-risk draining lymph node stations. 69 Standard doses after complete resection are 50 to 54 Gy in 1.8 to 2 Gy fractions, but a boost may be administered to high-risk regions including areas of nodal extracapsular extension or microscopic positive margins. 29,30 Lung dose constraints should be more conservative as tolerance appears to be reduced after surgery. The ongoing European LungART trial provides useful guidelines for PORT technique. 70 NSCL-C 3 OF 9
9 PRINCIPLES OF RADIATION THERAPY (4 of 9) The dose and fractionation of palliative RT should be individualized based on goals of care, symptoms, performance status, and logistical considerations. Shorter courses of RT provide similar pain relief as longer courses, but with a higher potential need for retreatment, and are preferred for patients with poor performance status and/or shorter life expectancy. For palliation of thoracic symptoms, higher dose/ with good performance status. 75 When higher doses (>30 Gy) are warranted, 3D-CRT should be used to reduce normal tissue irradiation. Radiation Therapy Simulation, Planning, and Delivery Simulation should be performed using CT scans obtained in the RT treatment position with appropriate immobilization devices. IV contrast with or without oral contrast is recommended for better target/organ delineation whenever possible in patients with central tumors or nodal disease. Because IV contrast can affect tissue heterogeneity correction calculations, density masking or use of a pre-contrast scan may be needed when intense enhancement is present. 76 contraindicated. A randomized trial of PET/CT versus CT-only RT planning demonstrated improved preemption of futile radical RT, decreased recurrences, and a trend toward improved overall survival with PET/CT RT planning. 77 Given the potential for rapid progression of NSCLC, 78,79 PET/CT should be obtained preferably within 4 weeks before treatment. It is ideal to obtain PET/CT in the treatment position. inhale/exhale or slow scan CT, or, ideally, 4D-CT. Photon beam energy should be individualized based on the anatomic location of the tumors and beam paths. In general, photon energies between 4 to 10 MV are recommended for beams passing through low-density lung tissue before entering the tumor. When there is no air gap before the beam enters the tumor (such as for some large mediastinal tumors or tumors attached to chest wall), higher energies may Tissue heterogeneity correction and accurate dose calculation algorithms that account for buildup and lateral electron scatter effects in heterogeneous density tissues are recommended. Heterogeneity correction with simple pencil beam algorithms is not recommended. 48 Respiratory motion should be managed when motion is excessive. This includes (but is not limited to) forced shallow breathing with abdominal compression, accelerator beam gating with the respiratory cycle, dynamic tumor tracking, active breathing control (ABC), or coaching/biofeedback techniques. If motion is minimal or the ITV is small, motion-encompassing targeting is appropriate. A useful resource for implementation of respiratory motion management is the report of AAPM Task Group IGRT including (but not limited to) orthogonal pair planar imaging and volumetric imaging (such as CBCT or CT on rails) is recommended when using SABR and 3D-CRT/IMRT with steep dose gradients around the target, when OARs are in close proximity to high-dose regions, and when using complex motion management techniques. NSCL-C 4 OF 9
10 PRINCIPLES OF RADIATION THERAPY (5 of 9) Table 1. Commonly Used Abbreviations in Radiation Therapy RT 2D-RT 3D-CRT Radiation Therapy or Radiotherapy 2-Dimensional RT 3-Dimensional Conformal RT 4D-CT 4-Dimensional Computed Tomography AAPM American Association of Physicists in Medicine ABC ACR Active Breathing Control American College of Radiology ASTRO American Society for Radiation Oncology BED CBCT CTV* ENI GTV* Biologically Effective Dose Cone-Beam CT Clinical Target Volume Elective Nodal Irradiation Gross Tumor Volume ICRU International Commission on Radiation Units and Measurements IFI IGRT IMRT ITV* OAR OBI PORT PTV* Involved Field Irradiation Image-Guided RT Intensity-Modulated RT Internal Target Volume Organ at Risk On-Board Imaging Postoperative RT Planning Target Volume QUANTEC Quantitative Analysis of Normal Tissue Effects in the Clinic RTOG Radiation Therapy Oncology Group SABR Stereotactic Ablative RT, also known as Stereotactic Body RT (SBRT) VMAT Volumetric Modulated Arc Therapy NSCL-C 5 OF 9
11 PRINCIPLES OF RADIATION THERAPY (6 of 9) Table 2. Commonly Used Doses for SABR Total Dose # Fractions Example Indications Table 3. Maximum Dose Constraints for SABR* OAR/Regimen 1 Fraction 3 Fractions 4 Fractions 5 Fractions Gy 1 Peripheral, small (<2 cm) tumors, esp. >1 cm from chest wall Gy 3 Peripheral tumors and >1 cm from chest wall Gy 4 Central or peripheral tumors <4 5 cm, especially <1 cm from chest wall Gy 5 Central or peripheral tumors, especially <1 cm from chest wall Gy 8 10 Central tumors Spinal Cord 14 Gy 18 Gy (6 Gy/fx) Esophagus 15.4 Gy 27 Gy (9 Gy/fx) Brachial Plexus Heart/ Pericardium 17.5 Gy 24 Gy (8 Gy/fx) 22 Gy 30 Gy (10 Gy/fx) 26 Gy (6.5 Gy/fx) 30 Gy (7.5 Gy/fx) 27.2 Gy (6.8 Gy/fx) 34 Gy (8.5 Gy/fx) Great Vessels 37 Gy NS 49 Gy (12.25 Gy/fx) Trachea & Proximal Bronchi 20.2 Gy 30 Gy (10 Gy/fx) 34.8 Gy (8.7 Gy/fx) 30 Gy (6 Gy/fx) 105% of PTV prescription^ 32 Gy (6.4 Gy/fx) 105% of PTV prescription^ 105% of PTV prescription^ 105% of PTV prescription^ Rib 30 Gy 30 Gy (10 Gy/fx) Skin 26 Gy 24 Gy (8 Gy/fx) 40 Gy (10 Gy/fx) 36 Gy (9 Gy/fx) 32.5 Gy (6.5 Gy/fx) 32 Gy (6.4 Gy/fx) Stomach 12.4 Gy NS 27.2 Gy (6.8 Gy/fx) NS *Based on constraints used in recent RTOG SABR trials (RTOG 0618, 0813, & 0915). NSCL-C 6 OF 9
12 PRINCIPLES OF RADIATION THERAPY - References (8 of 9) 1 Chen AB, Neville BA, Sher DJ, et al. Survival outcomes after radiation therapy for stage III non-small-cell lung cancer after adoption of computed tomography-based simulation. J Clin Oncol 2011;29: Unresectable, Locally Advanced Non-Small-Cell Lung Cancer Receiving Concomitant Chemoradiotherapy. Int J Radiat Oncol Biol Phys 2010;76: for nonsmall cell lung cancer. Cancer 2011;117: Chang JY, Komaki R, Lu C, et al. Phase 2 study of high-dose proton therapy with concurrent chemotherapy for unresectable stage III nonsmall cell lung cancer. Cancer 2011;117: Timmerman R, Paulus R, Galvin J, et al. Stereotactic Body Radiation Therapy for Inoperable Early Stage Lung Cancer. JAMA 2010;303: Baumann P, Nyman J, Hoyer M, et al. Outcome in a prospective phase II trial of medically inoperable stage I nonsmall-cell lung cancer patients treated with stereotactic body radiotherapy. J Clin Oncol 2009;27: Onishi H, Shirato H, Nagata Y, et al. Stereotactic body radiotherapy (SBRT) for operable stage I non-small-cell lung cancer: can SBRT be comparable to surgery? Int J Radiat Oncol Biol Phys 2011;81: Grutters JPC, Kessels AGH, Pijls-Johannesma M, et al. Comparison of the effectiveness of radiotherapy with photons, protons and carbon-ions for non-small cell lung cancer: a meta-analysis. Radiother Oncol 2010;95: Palma D, Visser O, Lagerwaard FJ, et al. Impact of introducing stereotactic lung radiotherapy for elderly patients with stage I non-small-cell lung cancer: a population-based time-trend analysis. J Clin Oncol 2010;28: Shirvani SM, Jiang J, Chang JY, et al. Comparative effectiveness of 5 treatment strategies for early-stage nonsmall cell lung cancer in the elderly. Int J Radiat Oncol Biol Phys 2012;84: Grills IS, Mangona VS, Welsh R, et al. Outcomes After Stereotactic Lung Radiotherapy or Wedge Resection for Stage I Non-Small-Cell Lung Cancer. J Clin Oncol 2010;28: Crabtree TD, Denlinger CE, Meyers BF, et al. Stereotactic body radiation therapy versus surgical resection for stage I non-small cell lung cancer. J Thorac Cardiovasc Surg 2010;140: Bogart JA, Hodgson L, Seagren SL, et al. Phase I study of accelerated conformal radiotherapy for stage I nonsmall-cell lung cancer in patients with pulmonary dysfunction: CALGB J Clin Oncol 2010;28: Zhao L, West BT, Hayman JA, et al. High radiation dose may reduce the negative effect of large gross tumor volume in patients with medically inoperable early-stage non-small cell lung cancer. Int J Radiat Oncol Biol Phys 2007;68: Aupérin A, Le Péchoux C, Rolland E, et al. Meta-analysis of concomitant versus sequential radiochemotherapy in locally advanced non-small-cell lung cancer. J Clin Oncol 2010;28: O'Rourke N, Roqué I Figuls M, Farré Bernadó N, Macbeth F. Concurrent chemoradiotherapy in non-small cell lung cancer. Cochrane Database Syst Rev 2010:CD Curran WJ Jr, Paulus R, Langer CJ, et al. Sequential vs. concurrent chemoradiation for stage III non-small cell lung cancer: randomized phase III trial RTOG J Natl Cancer Inst 2011;103: Sause W, Kolesar P, Taylor S IV, et al. Final results of phase III trial in regionally advanced unresectable nonsmall cell lung cancer: Radiation Therapy Oncology Group, Eastern Cooperative Oncology Group, and Southwest Oncology Group. Chest 2000;117: Dillman RO, Herndon J, Seagren SL, et al. Improved survival in stage III non-small-cell lung cancer: seven-year follow-up of cancer and leukemia group B (CALGB) 8433 trial. J Natl Cancer Inst 1996;88: Baumann M, Herrmann T, Koch R, et al. Final results of the randomized phase III CHARTWEL-trial (ARO 97-1) comparing hyperfractionated-accelerated versus conventionally fractionated radiotherapy in non-small cell lung cancer (NSCLC). Radiother Oncol 2011;100: Mauguen A, Le Péchoux C, Saunders MI, et al. Hyperfractionated or accelerated radiotherapy in lung cancer: an individual patient data meta-analysis. J Clin Oncol 2012;30: Albain KS, Swann RS, Rusch VW, et al. Radiotherapy plus chemotherapy with or without surgical resection for stage III non-small-cell lung cancer: a phase III randomised controlled trial. Lancet 2009;374: Kunitoh H, Kato H, Tsuboi M, et al. Phase II trial of preoperative chemoradiotherapy followed by surgical resection in patients with superior sulcus non-small-cell lung cancers: report of Japan Clinical Oncology Group trial J Clin Oncol 2008;26: Rusch VW, Giroux DJ, Kraut MJ, et al. Induction chemoradiation and surgical resection for superior sulcus non-smallcell lung carcinomas: long-term results of Southwest Oncology Group Trial 9416 (Intergroup Trial 0160). J Clin Oncol 2007;25: Thomas M, Rube C, Hoffknecht P, et al. Effect of preoperative chemoradiation in addition to preoperative chemotherapy: a randomized trial in stage III non-small-cell lung cancer. Lancet Oncol 2008;9: Higgins K, Chino JP, Marks LB, et al. Preoperative chemotherapy versus preoperative chemoradiotherapy for stage III (N2) non-small-cell lung cancer. Int J Radiat Biol Phys 2009;75: Douillard J-Y, Rosell R, De Lena M, et al. Impact of postoperative radiation therapy on survival in patients with complete resection and stage I, II, or IIIA non-small-cell lung cancer treated with adjuvant chemotherapy: the adjuvant Navelbine International Trialist Association (ANITA) Randomized Trial. Int J Radiat Oncol Biol Phys 2008;72: Lally BE, Zelterman D, Colasanto JM, et al. Postoperative radiotherapy for stage II or III non-small-cell lung cancer using the surveillance, epidemiology, and end results database. J Clin Oncol 2006;24: Feigenberg SJ, Hanlon AL, Langer C, et al. A phase II study of concurrent carboplatin and paclitaxel and thoracic radiotherapy for completely resected stage II and IIIA non-small cell lung cancer. J Thorac Oncol 2007;2: Bradley JD, Paulus R, Graham MV, et al. Phase II trial of postoperative adjuvant paclitaxel/carboplatin and thoracic radiotherapy in resected stage II and IIIA non-small-cell lung cancer: promising long-term results of the Radiation Therapy Oncology Group--RTOG J Clin Oncol 2005;23: Keller SM, Adak S, Wagner H, et al. A randomized trial of postoperative adjuvant therapy in patients with completely resected stage II or IIIA non-small-cell lung cancer. Eastern Cooperative Oncology Group. N Engl J Med 2000; 343: Burdett S, Stewart L, Group PM-a. Postoperative radiotherapy in non-small-cell lung cancer: update of an individual patient data meta-analysis. Lung Cancer 2005;47: one organ. Am J Clin Oncol 2010;33: sites of metastatic disease. Clin Cancer Res 2008;14: Kong FM, Pan C, Eisbruch A, Ten Haken RK. Physical models and simpler dosimetric descriptors of radiation late toxicity. Semin Radiat Oncol 2007;17: Timmerman RD. An overview of hypofractionation and introduction to this issue of seminars in radiation oncology. Semin Radiat Oncol 2008;18: Marks LB, Yorke ED, Jackson A, et al. Use of normal tissue complication probability models in the clinic. Int J Radiat Oncol Biol Phys 2010;76:S Marks LB, Bentzen SM, Deasy JO, et al. Radiation dose-volume effects in the lung. Int J Radiat Oncol Biol Phys 2010; 76:S Werner-Wasik M, Yorke E, Deasy J, et al. Radiation dose-volume effects in the esophagus. Int J Radiat Oncol Biol Phys 2010;76:S Gagliardi G, Constine LS, Moiseenko V, et al. Radiation dose-volume effects in the heart. Int J Radiat Oncol Biol Phys 2010;76:S Kirkpatrick JP, van der Kogel AJ, Schultheiss TE. Radiation dose-volume effects in the spinal cord. Int J Radiat Oncol Biol Phys 2010;76:S Onishi H, Shirato H, Nagata Y, et al. Hypofractionated stereotactic radiotherapy (HypoFXSRT) for stage I non-small cell lung cancer: updated results of 257 patients in a Japanese multi-institutional study. J Thorac Oncol 2007; 2:S Lagerwaard FJ, Haasbeek CJA, Smit EF, et al. Outcomes of risk-adapted fractionated stereotactic radiotherapy for stage I non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 2008;70: NSCL-C 8 OF 9
13 PRINCIPLES of RADIATIoN THERAPY - References (9 of 9) 44 Chang JY, Li QQ, Xu QY, et al. Stereotactic body radiation therapy for centrally located early stage or isolated 2014;88: : dimensional conformal thoracic radiation therapy with induction and concurrent carboplatin and paclitaxel in study using three-dimensional conformal radiation therapy and concurrent chemotherapy for patients with inoperable 80 NSCL-C 9 of 9
14 Thorascopic Lobectomy General Principles Principles of RT
15 Principles of RT SABR Principles of RT Target Volumes, Prescription Doses, and Normal Tissue Dose Constraints Principles of RT Principles of Radiation Therapy Principles of RT
16 Principles of Radiation Therapy Radiation Simulation, Planning, and Delivery Principles of RT Simulation, Planning, and Delivery Principles of RT Stereotactic Ablative Radiotherapy Principles of RT
17 Radiofrequency Ablation Whole Brain RT and Stereotactic Radiosurgery Stereotactic Ablative Radiotherapy
18
19
20
21
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
National Imaging Associates, Inc. Clinical guideline: NON SMALL CELL LUNG CANCER
 National Imaging Associates, Inc. Clinical guideline: NON SMALL CELL LUNG CANCER Original Date: March 2011 Page 1 of 10 Radiation Oncology Last Review Date: June 2012 Guideline Number: NIA_CG_122 Last
National Imaging Associates, Inc. Clinical guideline: NON SMALL CELL LUNG CANCER Original Date: March 2011 Page 1 of 10 Radiation Oncology Last Review Date: June 2012 Guideline Number: NIA_CG_122 Last
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
How To Improve Lung Cancer Survival With Radiation Therapy
 Clinical Controversies: Proton Therapy for Thoracic Tumors Dirk De Ruysscher, MD, PhD,* and Joe Y. Chang, MD, PhD Photon and proton therapy techniques have both improved dramatically over the past decade.
Clinical Controversies: Proton Therapy for Thoracic Tumors Dirk De Ruysscher, MD, PhD,* and Joe Y. Chang, MD, PhD Photon and proton therapy techniques have both improved dramatically over the past decade.
Radiotherapy in locally advanced & metastatic NSC lung cancer
 Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Implementation Date: April 2015 Clinical Operations
 National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Stage IIIB disease includes patients with T4 tumors,
 Guidelines on Treatment of Stage IIIB Non-small Cell Lung Cancer* James R. Jett, MD, FCCP; Walter J. Scott, MD, FCCP; M. Patricia Rivera MD, FCCP; and William T. Sause, MD, FACR Stage IIIB includes patients
Guidelines on Treatment of Stage IIIB Non-small Cell Lung Cancer* James R. Jett, MD, FCCP; Walter J. Scott, MD, FCCP; M. Patricia Rivera MD, FCCP; and William T. Sause, MD, FACR Stage IIIB includes patients
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Radiation Therapy for Non-Small Cell Lung Cancer. Principles of Radiation Therapy for Non-small Cell Lung Cancer
 Chapter 4 Radiation Therapy for Non-Small Cell Lung Cancer Join Y. Luh, MD, FACP and Charles R. Thomas, Jr., MD Introduction Radiation is a form of energy that has both beneficial and harmful effects on
Chapter 4 Radiation Therapy for Non-Small Cell Lung Cancer Join Y. Luh, MD, FACP and Charles R. Thomas, Jr., MD Introduction Radiation is a form of energy that has both beneficial and harmful effects on
Clinical Commissioning Policy: Stereotactic Ablative Body Radiotherapy for Non- Small-Cell Lung Cancer (Adult) April 2013 Reference: NHSCB/B01/P/a
 Clinical Commissioning Policy: Stereotactic Ablative Body Radiotherapy for Non- Small-Cell Lung Cancer (Adult) April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy: Stereotactic
Clinical Commissioning Policy: Stereotactic Ablative Body Radiotherapy for Non- Small-Cell Lung Cancer (Adult) April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy: Stereotactic
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Helical TomoTherapy for Lung Cancer Radiotherapy: Good Science Pays Clinical Dividends Peter Hoban, Ph.D., TomoTherapy Inc.
 CLINICAL FEATURE Helical TomoTherapy for Lung Cancer Radiotherapy: Good Science Pays Clinical Dividends Peter Hoban, Ph.D., TomoTherapy Inc. The Challenge Lung cancer kills more people each year in the
CLINICAL FEATURE Helical TomoTherapy for Lung Cancer Radiotherapy: Good Science Pays Clinical Dividends Peter Hoban, Ph.D., TomoTherapy Inc. The Challenge Lung cancer kills more people each year in the
Radiotherapy in Lung
 Radiotherapy in Lung CancerAnatomy Oblique fissure in both lungs. Horizontal fissure in Right lung. Trachea bifurcates at the level of T5. Lymph nodes are divided into stations. Intrapulmonary, bronchopulmonary
Radiotherapy in Lung CancerAnatomy Oblique fissure in both lungs. Horizontal fissure in Right lung. Trachea bifurcates at the level of T5. Lymph nodes are divided into stations. Intrapulmonary, bronchopulmonary
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Management of stage III A-B of NSCLC. Hamed ALHusaini Medical Oncologist
 Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Particle Therapy for Lung Cancer. Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org
 Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Jedi Wisdom for Lung Cancer Radiotherapy: May the Force Be With You
 Jedi Wisdom for Lung Cancer Radiotherapy: May the Force Be With You SHAUN LOEWEN MD PhD FRCPC Assistant Professor, University of Manitoba Radiation Oncologist, CancerCare Manitoba Disclosure Relationship
Jedi Wisdom for Lung Cancer Radiotherapy: May the Force Be With You SHAUN LOEWEN MD PhD FRCPC Assistant Professor, University of Manitoba Radiation Oncologist, CancerCare Manitoba Disclosure Relationship
Lung Cancer Treatment
 Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Guidelines for the treatment of breast cancer with radiotherapy
 London Cancer Guidelines for the treatment of breast cancer with radiotherapy March 2013 Review March 2014 Version 1.0 Contents 1. Introduction... 3 2. Indications and dosing schedules... 3 2.1. Ductal
London Cancer Guidelines for the treatment of breast cancer with radiotherapy March 2013 Review March 2014 Version 1.0 Contents 1. Introduction... 3 2. Indications and dosing schedules... 3 2.1. Ductal
Innovative RT SBRT. The variables with REQ in superscript are required.
 The variables with REQ in superscript are required. The variables with a are single-select variables; only one answer can be selected. The variables with a are multi-select variables; multiple answers
The variables with REQ in superscript are required. The variables with a are single-select variables; only one answer can be selected. The variables with a are multi-select variables; multiple answers
Radiotherapy for Non-Small Cell Lung Cancer. Standard Treatment Options Radiotherapy Planning
 Radiotherapy for Non-Small Cell Lung Cancer I II Standard Treatment Options Radiotherapy Planning TNM Staging System Disease Staging - Management is based on disease stage - Stage I-II: early stage - Stage
Radiotherapy for Non-Small Cell Lung Cancer I II Standard Treatment Options Radiotherapy Planning TNM Staging System Disease Staging - Management is based on disease stage - Stage I-II: early stage - Stage
Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment.
 Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
Stomach (Gastric) Cancer. Prof. M K Mahajan ACDT & RC Bathinda
 Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
4.8 Lung cancer. 4.8.5 In the UK, three fractionation regimens are most commonly used:
 4.8 Lung cancer 4.8.1 In 2005, both NICE (National Institute for Health and Clinical Excellence) and SIGN (Scottish Intercollegiate Guidelines Network) published guidelines on the management of lung cancer.
4.8 Lung cancer 4.8.1 In 2005, both NICE (National Institute for Health and Clinical Excellence) and SIGN (Scottish Intercollegiate Guidelines Network) published guidelines on the management of lung cancer.
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引
 馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
Alternatives to Surgical Resection for Early Stage Lung Cancer
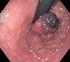 Alternatives to Surgical Resection for Early Stage Lung Cancer Neil A. Christie MD University of Pittsburgh Medical Center Department of Thoracic Surgery Allied Health Personnel Symposium AATS 2014 Conflicts
Alternatives to Surgical Resection for Early Stage Lung Cancer Neil A. Christie MD University of Pittsburgh Medical Center Department of Thoracic Surgery Allied Health Personnel Symposium AATS 2014 Conflicts
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate
 Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Esperienza di stereotassia polmonare al Campus Bio-Medico: tecnica e risultati Rolando M. D Angelillo
 Esperienza di stereotassia polmonare al Campus Bio-Medico: tecnica e risultati Rolando M. D Angelillo Università Campus Bio-Medico di Roma - Via Álvaro del Portillo, 21-00128 Roma Italia BED 10 > 100 Gy
Esperienza di stereotassia polmonare al Campus Bio-Medico: tecnica e risultati Rolando M. D Angelillo Università Campus Bio-Medico di Roma - Via Álvaro del Portillo, 21-00128 Roma Italia BED 10 > 100 Gy
Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of the Chest
 Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of the Chest File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_chest
Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of the Chest File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_chest
POLICY A. INDICATIONS
 Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
LUNG CANCER INTRODUCTION
 LUNG CANCER INTRODUCTION Lung cancer remains the leading cause of cancer death in the UK. Approximately 50% of those diagnosed present with stage IV disease. Significant advances in the management of lung
LUNG CANCER INTRODUCTION Lung cancer remains the leading cause of cancer death in the UK. Approximately 50% of those diagnosed present with stage IV disease. Significant advances in the management of lung
Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board
 Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board Abstract Introduction Management of stage III non small-cell lung cancer (NSCLC) is complex and requires careful work-up, staging,
Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board Abstract Introduction Management of stage III non small-cell lung cancer (NSCLC) is complex and requires careful work-up, staging,
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
Pulmonary function. Is patient potentially operable? Yes. tests 3. Yes. Pulmonary function. tests 3, if clinically indicated. Yes
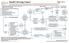 INITIAL EVALUATION Pathology consistent with small cell lung cancer History and physical Chest X-ray Laboratory studies to include: hematological and full chemistry panels CT chest and upper abdomen Pet
INITIAL EVALUATION Pathology consistent with small cell lung cancer History and physical Chest X-ray Laboratory studies to include: hematological and full chemistry panels CT chest and upper abdomen Pet
B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC
 Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015. 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV
 CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software.
 SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
Is an evidence-based approach realistic in non-small cell lung cancer (NSCLC)?
 Is an evidence-based approach realistic in non-small cell lung cancer (NSCLC)? Authors Key words P.A. Coucke, N. Barthelemy, L. Bosquee, J.P. van Meerbeeck NSCLC, sequential and concomitant chemo-radiotherapy,
Is an evidence-based approach realistic in non-small cell lung cancer (NSCLC)? Authors Key words P.A. Coucke, N. Barthelemy, L. Bosquee, J.P. van Meerbeeck NSCLC, sequential and concomitant chemo-radiotherapy,
Goals and Objectives: Breast Cancer Service Department of Radiation Oncology
 Goals and Objectives: Breast Cancer Service Department of Radiation Oncology The breast cancer service provides training in the diagnosis, management, treatment, and follow-up of breast malignancies, including
Goals and Objectives: Breast Cancer Service Department of Radiation Oncology The breast cancer service provides training in the diagnosis, management, treatment, and follow-up of breast malignancies, including
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer. A Single Institution Experience
 ORIGINAL ARTICLE Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer A Single Institution Experience Michael Hsie, MD,* Stefania Morbidini-Gaffney, MD,* Leslie J. Kohman, MD, Elisabeth
ORIGINAL ARTICLE Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer A Single Institution Experience Michael Hsie, MD,* Stefania Morbidini-Gaffney, MD,* Leslie J. Kohman, MD, Elisabeth
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
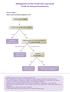 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
EVIDENCE TABLE. Study Objective. (Purpose of Study)
 . Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest 997; (6):70-77.. Greene FL, Page DL, Fleming ID, et al, eds, for the American Joint Committee on Cancer. AJCC Cancer
. Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest 997; (6):70-77.. Greene FL, Page DL, Fleming ID, et al, eds, for the American Joint Committee on Cancer. AJCC Cancer
Stage I, II Non Small Cell Lung Cancer
 Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Outcomes of Stereotactic Ablative Radiotherapy in Patients With Potentially Operable Stage I Non-Small Cell Lung Cancer
 CME International Journal of Radiation Oncology biology physics www.redjournal.org Clinical Investigation: Thoracic Cancer Outcomes of Stereotactic Ablative Radiotherapy in Patients With Potentially Operable
CME International Journal of Radiation Oncology biology physics www.redjournal.org Clinical Investigation: Thoracic Cancer Outcomes of Stereotactic Ablative Radiotherapy in Patients With Potentially Operable
Current Status and Perspectives of Radiation Therapy for Breast Cancer
 Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Non-Small Cell Lung Cancer
 NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Non-Small Cell Lung Cancer Version 3.2014 NCCN.org NCCN Guidelines for Patients available at www.nccn.org/patients Continue Version 3.2014,
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Non-Small Cell Lung Cancer Version 3.2014 NCCN.org NCCN Guidelines for Patients available at www.nccn.org/patients Continue Version 3.2014,
Department of Radiation Oncology
 Department of Radiation Oncology Welcome to Radiation Oncology at Emory Clinic Every member of Emory Clinic Department of Radiation Oncology strives to provide the highest quality of care for you as our
Department of Radiation Oncology Welcome to Radiation Oncology at Emory Clinic Every member of Emory Clinic Department of Radiation Oncology strives to provide the highest quality of care for you as our
Outcomes of Patients With Stage III Nonsmall Cell Lung Cancer Treated With Chemotherapy and Radiation With and Without Surgery
 Outcomes of Patients With Stage III Nonsmall Cell Lung Cancer Treated With Chemotherapy and Radiation With and Without Surgery Hale B. Caglar, MD 1 ; Elizabeth H. Baldini, MD, MPH 1 ; Megan Othus, MS 2
Outcomes of Patients With Stage III Nonsmall Cell Lung Cancer Treated With Chemotherapy and Radiation With and Without Surgery Hale B. Caglar, MD 1 ; Elizabeth H. Baldini, MD, MPH 1 ; Megan Othus, MS 2
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group
 REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
Clinical Trials and Radiation Treatment. Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto
 Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
3.0 With final Comments for presentation at Sub Group Meeting 24. 24.11.10
 Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE LUNG CANCER Lung Site Group Lung Cancer Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE LUNG CANCER Lung Site Group Lung Cancer Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
American College of Radiology ACR Appropriateness Criteria
 American College of Radiology ACR Appropriateness Criteria Date of origin: 1996 Last review date: 2014 NONSURGICAL TREATMENT FOR LOCALLY ADVANCED NON SMALL-CELL LUNG CANCER: GOOD PERFORMANCE STATUS/DEFINITIVE
American College of Radiology ACR Appropriateness Criteria Date of origin: 1996 Last review date: 2014 NONSURGICAL TREATMENT FOR LOCALLY ADVANCED NON SMALL-CELL LUNG CANCER: GOOD PERFORMANCE STATUS/DEFINITIVE
Non-small Cell Lung Cancer: Locally Advanced
 Non-small Cell Lung Cancer: Locally Advanced Daniel W. Golden MD, PGY-5, Ryan Bair MD, PGY-3, and Matthew Koshy MD, Assistant Professor Pritzker School of Medicine, University of Chicago Chicago Clinical
Non-small Cell Lung Cancer: Locally Advanced Daniel W. Golden MD, PGY-5, Ryan Bair MD, PGY-3, and Matthew Koshy MD, Assistant Professor Pritzker School of Medicine, University of Chicago Chicago Clinical
Radiotherapy in Plasmacytoma and Myeloma. David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015
 Radiotherapy in Plasmacytoma and Myeloma David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015 Contents Indications for radiotherapy: Palliation in Multiple Myeloma Solitary Bone Plasmacytoma
Radiotherapy in Plasmacytoma and Myeloma David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015 Contents Indications for radiotherapy: Palliation in Multiple Myeloma Solitary Bone Plasmacytoma
Survey on the treatment of non-small cell lung cancer (NSCLC) in England and Wales
 Eur Respir J 1997; 10: 1552 1558 DOI: 10.1183/09031936.97.10071552 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Survey on the treatment
Eur Respir J 1997; 10: 1552 1558 DOI: 10.1183/09031936.97.10071552 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Survey on the treatment
Loco-regional Recurrence
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer AGO AGO e. e. V. V. Loco-regional Recurrence Loco-regional Recurrence Version 2002: Brunnert / Simon Versions 2003 2012: Audretsch
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer AGO AGO e. e. V. V. Loco-regional Recurrence Loco-regional Recurrence Version 2002: Brunnert / Simon Versions 2003 2012: Audretsch
Radioterapia panencefalica. Umberto Ricardi
 Radioterapia panencefalica Umberto Ricardi Background Systemic disease to the brain is unfortunately a quite common event Radiotherapy, especially with the great technical development during the past decades,
Radioterapia panencefalica Umberto Ricardi Background Systemic disease to the brain is unfortunately a quite common event Radiotherapy, especially with the great technical development during the past decades,
Acknowledgement. Prerequisites: Basic Concepts of IMRT. Overview. Therapy Continuing Education Course Clinical Implementation of IMRT for Lung Cancers
 Therapy Continuing Education Course Clinical Implementation of IMRT for Lung Cancers H. Helen Liu, PhD Department of Radiation Physics, U.T. MD Anderson Cancer Center, Houston, TX AAPM, Seattle, 2005 Acknowledgement
Therapy Continuing Education Course Clinical Implementation of IMRT for Lung Cancers H. Helen Liu, PhD Department of Radiation Physics, U.T. MD Anderson Cancer Center, Houston, TX AAPM, Seattle, 2005 Acknowledgement
BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER
 BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
5. Non small Cell Lung Cancer
 5. Non small Cell Lung Cancer Introduction The cancer registry in Sweden shows a continuous increase of lung cancer cases from 867 in 1958 when the registry started to 2 846 in 2000. The Swedish cancer
5. Non small Cell Lung Cancer Introduction The cancer registry in Sweden shows a continuous increase of lung cancer cases from 867 in 1958 when the registry started to 2 846 in 2000. The Swedish cancer
Corporate Medical Policy Brachytherapy Treatment of Breast Cancer
 Corporate Medical Policy Brachytherapy Treatment of Breast Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: brachytherapy_treatment_of_breast_cancer 7/1996 5/2015 5/2016 5/2015
Corporate Medical Policy Brachytherapy Treatment of Breast Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: brachytherapy_treatment_of_breast_cancer 7/1996 5/2015 5/2016 5/2015
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs. Case Study. Surgery. Lumpectomy and Radiation
 Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER
 AFA 08958 From Bench to Bedside From KK DT1 10/27/2015 12:04 PM 01 ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER Hak Choy, MD University of Texas Southwestern Medical Center Dallas, Texas, USA Orchestrating
AFA 08958 From Bench to Bedside From KK DT1 10/27/2015 12:04 PM 01 ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER Hak Choy, MD University of Texas Southwestern Medical Center Dallas, Texas, USA Orchestrating
Approccio multidisciplinare nei tumori del retto
 Approccio multidisciplinare nei tumori del retto F. Muñoz Radiation Oncology Department University of Torino, Italy RECENT CHANGES IN RECTAL CANCER DIAGNOSIS AND THERAPY Optimal staging by EUS and MRI
Approccio multidisciplinare nei tumori del retto F. Muñoz Radiation Oncology Department University of Torino, Italy RECENT CHANGES IN RECTAL CANCER DIAGNOSIS AND THERAPY Optimal staging by EUS and MRI
Intensity Modulated Radiation Therapy (IMRT) for Thyroid Cancer
 Thyroid Science 5(1):CLS1-8, 2010 www.thyroidscience.com Clinical and Laboratory Studies Intensity Modulated Radiation Therapy (IMRT) for Thyroid Cancer 1 2 5 Aruna Turaka, MD, Tianyu Li, MS, Jian Q. Yu,
Thyroid Science 5(1):CLS1-8, 2010 www.thyroidscience.com Clinical and Laboratory Studies Intensity Modulated Radiation Therapy (IMRT) for Thyroid Cancer 1 2 5 Aruna Turaka, MD, Tianyu Li, MS, Jian Q. Yu,
Radiation Protection in Radiotherapy
 Radiation Protection in Radiotherapy Albert Lisbona Medical Physics Department CLCC Nantes Atlantique 44805 Saint-Herblain France a-lisbona@nantes.fnclcc.fr Radiation therapy The lecture is oriented to
Radiation Protection in Radiotherapy Albert Lisbona Medical Physics Department CLCC Nantes Atlantique 44805 Saint-Herblain France a-lisbona@nantes.fnclcc.fr Radiation therapy The lecture is oriented to
Principles of Radiation Therapy A Bapsi Chakravarthy, MD Associate e P rofessor Professor Radiation Oncology
 Principles of Radiation Therapy A Bapsi Chakravarthy, MD Associate Professor Radiation Oncology Disclosure Information I have no financial relationships to disclose relevant to the conten of this presentation.
Principles of Radiation Therapy A Bapsi Chakravarthy, MD Associate Professor Radiation Oncology Disclosure Information I have no financial relationships to disclose relevant to the conten of this presentation.
American College of Radiology ACR Appropriateness Criteria EARLY-STAGE NON SMALL-CELL LUNG CANCER
 Date of origin: 2013 American College of Radiology ACR Appropriateness Criteria EARLY-STAGE NON SMALL-CELL LUNG CANCER Expert Panel on Radiation Oncology Lung: Gregory M. M. Videtic, MD, CM 1 ; Kenneth
Date of origin: 2013 American College of Radiology ACR Appropriateness Criteria EARLY-STAGE NON SMALL-CELL LUNG CANCER Expert Panel on Radiation Oncology Lung: Gregory M. M. Videtic, MD, CM 1 ; Kenneth
RADIATION ONCOLOGY GUIDELINES
 MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
T reatment O utcomes of T hree-dimensional Conformal Radiotherapy for Stage III Non-Small Cell Lung Cancer
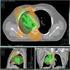 Cancer Res Treat. 2005;37(5):273-278 T reatment O utcomes of T hree-dimensional Conformal Radiotherapy for Stage III Non-Small Cell Lung Cancer Seung-Gu Yeo, M.D. 1, Moon-June Cho, M.D. 1,4, Sun-Young
Cancer Res Treat. 2005;37(5):273-278 T reatment O utcomes of T hree-dimensional Conformal Radiotherapy for Stage III Non-Small Cell Lung Cancer Seung-Gu Yeo, M.D. 1, Moon-June Cho, M.D. 1,4, Sun-Young
Corporate Medical Policy
 Corporate Medical Policy Intensity Modulated Radiation Therapy for Tumors of the Central File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_for_tumors
Corporate Medical Policy Intensity Modulated Radiation Therapy for Tumors of the Central File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_for_tumors
The expanding role of systemic treatment in non-small cell lung cancer neo-adjuvant therapy
 17 (Supplement 10): x108 x112, 2006 doi:10.1093/annonc/mdl247 The expanding role of systemic treatment in non-small cell lung cancer neo-adjuvant therapy E. Felip & E. Vilar Oncology Department, Vall d
17 (Supplement 10): x108 x112, 2006 doi:10.1093/annonc/mdl247 The expanding role of systemic treatment in non-small cell lung cancer neo-adjuvant therapy E. Felip & E. Vilar Oncology Department, Vall d
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
LUNG CANCER POPULATION STATUS & TREATMENT OPTIONS. By: Sweety Narang, RTT & Gurpreet Sandhu, RTT
 LUNG CANCER POPULATION STATUS & TREATMENT OPTIONS By: Sweety Narang, RTT & Gurpreet Sandhu, RTT OVERVIEW 1. Statistics on Lung Cancer Incidence & Mortality 2. Functions of the Lung 3. Etiology & Risk Factors
LUNG CANCER POPULATION STATUS & TREATMENT OPTIONS By: Sweety Narang, RTT & Gurpreet Sandhu, RTT OVERVIEW 1. Statistics on Lung Cancer Incidence & Mortality 2. Functions of the Lung 3. Etiology & Risk Factors
Tricia Cox on 7/18/2012 at Oncology Center. Sarah Randolf. Female
 SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
People Living with Cancer
 Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Concurrent Chemotherapy and Radiotherapy for Head and Neck Cancer
 Concurrent Chemotherapy and Radiotherapy for Head and Neck Cancer Ryan J. Burri; Nancy Y. Lee Published: 03/23/2009 Abstract and Introduction Abstract Head and neck cancer is best managed in a multidisciplinary
Concurrent Chemotherapy and Radiotherapy for Head and Neck Cancer Ryan J. Burri; Nancy Y. Lee Published: 03/23/2009 Abstract and Introduction Abstract Head and neck cancer is best managed in a multidisciplinary
Lung Cancer and Postoperative Radiotherapy
 . Fernando HC, Goldstraw P. The accuracy of clinical evaluative intrathoracic staging in lung cancer as assessed by postsurgical pathologic staging. Cancer 990; 65():50-506.. Keller SM, Adak S, Wagner
. Fernando HC, Goldstraw P. The accuracy of clinical evaluative intrathoracic staging in lung cancer as assessed by postsurgical pathologic staging. Cancer 990; 65():50-506.. Keller SM, Adak S, Wagner
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
ACR Appropriateness Criteria Nonsurgical Treatment for Non-Small-Cell Lung Cancer: Good Performance Status/Definitive Intent
 ACR Appropriateness Criteria Nonsurgical Treatment for Non-Small-Cell Lung Cancer: Good Performance Status/Definitive Intent Richard M. Gewanter, MD, Kenneth E. Rosenzweig, MD, Joe Yujiao Chang, MD, PhD,
ACR Appropriateness Criteria Nonsurgical Treatment for Non-Small-Cell Lung Cancer: Good Performance Status/Definitive Intent Richard M. Gewanter, MD, Kenneth E. Rosenzweig, MD, Joe Yujiao Chang, MD, PhD,
