Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board
|
|
|
- Kevin McDonald
- 10 years ago
- Views:
Transcription
1 Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board Abstract Introduction Management of stage III non small-cell lung cancer (NSCLC) is complex and requires careful work-up, staging, and decision making. Stage III NSCLC comprises a heterogeneous population of patients, so accurate staging is important. Multiple treatment approaches are available, and appropriate selection must be individualized based on patient and tumor characteristics. Multidisciplinary evaluation is generally necessary in deciding between surgical and nonsurgical approaches and between chemotherapy or chemoradiation. In this webcast, a multidisciplinary virtual thoracic oncology tumor board reviews the case of a 55-year-old former smoker with stage III NSCLC. They review relevant data for treatment planning and debate the appropriate work-up and management of this case. Key messages from their discussions are summarized here. Diagnosis and Work-Up of Locally Advanced NSCLC Invasive procedures are, unfortunately, necessary to accurately diagnose nodal involvement. Positron emission tomography (PET) scan and other imaging tools are not sufficiently accurate to diagnose mediastinal lymph node positivity, so a positive PET scan merits further work-up before definitive treatment planning. Lymph node staging generally requires either mediastinoscopy or endobronchial ultrasound with transbronchial needle aspiration of the lymph nodes (EBUS-TBNA). Endoscopic esophageal ultrasound with needle aspiration is a less well-studied approach, but when combined with EBUS-TBNA, allows for evaluation of some additional groups of nodes that would otherwise not be accessible by EBUS-TBNA alone. Mediastinoscopy is the gold standard for lymph node staging, but EBUS-TBNA has shown good sensitivity and specificity in recent studies. It is also important to think ahead, because if restaging following induction therapy is likely to be needed, it is best to avoid performing two mediastinoscopies. In such cases, EBUS-TBNA would be preferred as the initial staging modality. Lymph node staging distinguishes stage IIIA from stage IIIB NSCLC, which is important in determining candidacy for surgery. Surgical Versus Nonsurgical Approaches Patients with stage IIIB NSCLC are generally not considered candidates for surgery and would therefore be treated with definitive chemoradiation. There is considerably more debate about resection for patients with stage IIIA NSCLC. Stage IIIA is potentially curable disease with 5-year survival rates of 20% to 30% or greater.
2 The only data available to drive decision making regarding whether to perform surgery for stage IIIA NSCLC are from the Intergroup 0139/RTOG 9309 study presented by Albain et al at the 2005 annual meeting of the American Society of Clinical Oncology. In this study, 396 patients with T1-3N2M0 NSCLC were randomized to receive chemoradiation followed by either surgery or continued radiation. Chemoradiation consisted of cisplatin, etoposide, and radiation therapy with 45 Gy. The nonsurgical group continued radiation to 61 Gy. Following surgery or continued radiation therapy, all patients received consolidative chemotherapy with two cycles of cisplatin/etoposide. The surgical arm had significantly better progression-free survival (PFS), which at 5 years was 22.4% versus 11.1% with chemoradiation alone (P =.017). However, no statistically significant difference in overall survival (OS) was observed. At 5 years, OS was 27.2% with surgery versus 20.3% without surgery (P <.1). Perioperative mortality may explain the lack of survival advantage for the surgical group in INT 0139/RTOG One quarter of the surgical patients died in the perioperative period, with the highest mortality rate in patients who underwent right pneumonectomy. A post hoc subgroup analysis did find a significant OS advantage for those who underwent lobectomy compared with matched patients in the chemoradiation group (36% versus 18% 5-year OS, respectively; P =.002). Based on this analysis, surgery would be the preferred management for patients who are candidates for lobectomy, especially those with single-station N2 disease. Appropriate candidates should be referred to high-volume centers with multidisciplinary tumor boards and surgeons experienced in lobectomy. Arguments in favor of a nonsurgical approach (ie, chemoradiation) are that: (1) no OS benefit was seen in the INT 0139/RTOG 9309 study in the overall study population; (2) no prospective randomized data show a survival advantage for surgery over concurrent chemoradiation; and (3) phase II studies of chemoradiation with current radiation techniques yield similar outcomes to studies combining chemoradiation and surgery. It should also be noted that many patients are not surgical candidates because lung cancer often occurs in patients with other pulmonary diseases, such as chronic obstructive pulmonary disorder. Pulmonary function testing should be performed, and predicted function postlobectomy should be calculated before deciding whether a patient is medically fit to undergo surgery. Preoperative Induction Therapy For patients who are considered surgical candidates, the next question is whether preoperative induction therapy should consist of chemotherapy alone or chemoradiation. No prospective randomized phase III study has been completed to address this issue. The rationale for using chemotherapy alone is that it has reduced toxicity compared with chemoradiation, and morbidity and mortality are particularly reduced in pneumonectomy patients. Furthermore, it is easier to perform mediastinoscopy for restaging and easier to perform surgery after chemotherapy than after chemoradiation. For these reasons, many cancer centers prefer to give induction chemotherapy alone and then postoperative chemoradiation. In a phase II RTOG study, docetaxel/cisplatin produced a pathologic
3 complete response in 19% of patients with stage IIIA pn2 NSCLC. The study was originally intended to have a concurrent chemoradiation arm using the same chemotherapy regimen, but was never completed due to inadequate accrual. The rationale for preoperative chemoradiation is that it is associated with an increased pathologic response and likelihood of nodal clearance or downstaging compared with chemotherapy alone. It may in fact be necessary for patients with bulky disease in order to facilitate resection. For those receiving chemoradiation, radiation doses of 45 to 74 Gy have been studied. Higher doses (74 Gy) are usually given with 3-D conformal approaches since they reduce the volume of normal tissue exposed to radiation and therefore are associated with less risk of toxicity. Outside of clinical trials, standard practice for those receiving chemoradiation is usually to treat with radiation to a total of about 66 Gy. Following induction therapy, it may be helpful to restage the patient before surgery, particularly if a pneumonectomy is planned. Restaging is less necessary before a lobectomy. The decision regarding whether to restage is influenced by not only the type of surgery to be performed but also by whether a mediastinoscopy was done previously. If restaging is performed, a mediastinoscopy is preferred if not previously performed because a needle biopsy has reduced sensitivity after induction therapy. However, if the patient had a prior mediastinoscopy, a repeat mediastinoscopy should be avoided because it has reduced sensitivity and specificity and increased safety risks. Whether or not mediastinal lymph nodes are restaged, assessment for distant disease with PET scan and brain MRI is warranted. Managing Residual Disease Currently, most patients are treated with a total of four cycles of chemotherapy, which includes the induction cycles. The INT 0139/RTOG 9309 protocol called for all patients to receive consolidative chemotherapy with two cycles of cisplatin/etoposide. Although not all patients were able to complete that regimen in the trial, it is still considered the standard of care, particularly since development of systemic metastases remains a concern. That said, it has not been definitively demonstrated that postoperative chemotherapy or chemoradiation adds additional benefit over induction therapy and surgery. The Hoosier Oncology Group conducted a study in patients with unresectable stage IIIA/B NSCLC. In this study, patients were treated with cisplatin/etoposide and concurrent chemoradiation, and those with no evidence of disease progression were then randomized to either three cycles of docetaxel or observation. Docetaxel added no survival benefit but considerable toxicity, including an increase in treatment-related death. It is not entirely clear that these data can be extrapolated to patients undergoing resection, but they at least point to the fact that this issue requires further study. Prevention of brain metastases is another concern in patients with stage III disease. Good results have been seen in small-cell lung cancer with prophylactic cranial irradiation
4 (PCI). A few small prospective randomized studies in NSCLC have shown a decrease in central nervous system (CNS) metastases with PCI. The recently completed RTOG 0214 study randomized patients with stage IIIA/B NSCLC to PCI or observation. Although targeted accrual was never met, and the study had to close early, it did show a significant decrease in the incidence of CNS metastases at 1 year in the PCI group (7.7%) compared with controls (18%; P =.004). On the other hand, there was no significant benefit seen in terms of disease-free survival (DFS) or OS at 1 year. Longer follow-up is needed to determine whether the difference in incidence of CNS metastases will ultimately translate into a significant DFS or OS benefit. Follow-up should include history, physical examination, and neurologic examination. It also typically includes chest computed tomography (CT) scan every 3 to 6 months, although there is no specific evidence to confirm that regular CT scanning affects longterm outcomes. Patients should be evaluated for new primary as well as recurrent tumors. Managing Isolated Brain Metastases Isolated brain metastases can be treated with whole-brain radiation therapy (WBRT), stereotactic radiosurgery (SRS), a combination of WBRT and SRS, or craniotomy and resection. SRS is most appropriate for patients with disease that is limited in size and involves no more than three lesions because it is associated with good locoregional control and the least amount of morbidity. The addition of SRS to WBRT may also improve outcomes in patients with low-volume CNS disease. RTOG 9508 showed increased mean survival time in patients treated with WBRT and SRS compared with WBRT alone (6.5 versus 4.9 months; P =.0393). An ongoing RTOG study will help determine whether the addition of targeted biologic therapy (erlotinib) or chemotherapy (temozolomide) adds benefit to WBRT + SRS. Patients with brain metastases may also need treatment for symptom relief, for example, with steroids, particularly if vasogenic edema is present. Managing Systemic Relapse There is some debate as to whether systemic relapse following neoadjuvant chemoradiation therapy should be managed with traditional first-line or second-line options for metastatic NSCLC, given the prior exposure to chemotherapy. First-line therapy would consist of retreatment with a platinum doublet chemotherapy regimen, usually favoring carboplatin over cisplatin in the United States, often coupled with pemetrexed. One-year survival with these regimens is now 30% to 40%. Long duration between neoadjuvant therapy and the appearance of metastases would favor treating the metastases with first-line platinum-based therapy. Based on ECOG 4599 by Sandler et al, it would also be appropriate to consider adding bevacizumab for patients who do not have brain metastases or requirements for ongoing anticoagulation. Second-line options would be either docetaxel, pemetrexed, or erlotinib. It would also be appropriate to enroll patients with systemic relapse after neoadjuvant therapy in clinical
5 trials of targeted agents, such as vandetanib, gefinitib, erlotinib, cetuximab, and newer agents targeting Akt, mtor, and Ras pathways. Molecular markers are now being used as a way of identifying patients most likely to respond to certain therapies. For example, ERCC1 mutations may predict platinum resistance, and RRM1 is a molecular determinant of gemcitabine efficacy. The MADe IT Study by Simon et al used both of these markers to guide choice of either docetaxel/vinorelbine, gemcitabine/docetaxel, carboplatin/docetaxel, or carboplatin/gemcitabine and reported a 1-year survival rate of 59%. In addition, epidermal growth factor receptor mutations are known to be predictive of response to tyrosine kinase inhibitors, such as erlotinib. Positive findings with molecular markers point to the need to preserve tissue when samples are obtained, including early in the work-up, such as during an EBUS-TBNA. Conclusion There are many controversies regarding optimal management of patients with stage III NSCLC. Numerous options for work-up and treatment are available, and data to guide decision making are somewhat limited. A multidisciplinary review of options is generally needed to determine the best management plan for individual patients. Suggested Readings Albain KS, Swann RS, Rusch VR, et al. Phase III study of concurrent chemotherapy and radiotherapy (CT/RT) vs CT/RT followed by surgical resection for stage IIIA(pN2) nonsmall cell lung cancer (NSCLC): outcomes update of North American intergroup 0139 (RTOG 9309). Abstract Presented at: 42nd annual meeting of the American Society of Clinical Oncology; May 13-17, 2005; Orlando, Fla. Allen AM, Mentzer SJ, Yeap BY, et al. Pneumonectomy after chemoradiation. The Dana-Farber Cancer Institute/Brigham and Women s Hospital Experience. Cancer. 2008;112: Andrews DW, Scott CB, Sperduto PW, et al. Whole brain radiation therapy with or without stereotactic radiosurgery boost for patients with one to three brain metastases: phase III results of the RTOG 9508 randomised trial. Lancet. 2004;363: Betticher DC, Schmitz S-F H, Totsch M, et al. Mediastinal lymph node clearance after docetaxel-cisplatin neoadjuvant chemotherapy is prognostic of survival in patients with stage IIIA pn2 non small-cell lung cancer: a multicenter phase II trial. J Clin Oncol. 2003;21: Bradley JD, Graham M, Suzanne S, et al. Phase I Results of RTOG L-0117; a phase I/II dose intensification study using 3DCRT and concurrent chemotherapy for patients with inoperable NSCLC. Abstract Presented at: 42nd annual meeting of the American Society of Clinical Oncology; May 13-17, 2005; Orlando, Fla.
6 Curran WJ, Scott CB, Langer CJ, et al. Long-term benefit is observed in a phase III comparison of sequential vs concurrent chemoradiation for patients with unresected stage III nsclc: RTOG Abstract Presented at: 39th annual meeting of the American Society of Clinical Oncology; May 29-June 3, 2003; Chicago, Ill. Fournel P, Robinet G, Thomas P, et al. Randomized phase III trial of sequential chemoradiotherapy compared with concurrent chemoradiotherapy in locally advanced non small-cell lung cancer: groupe Lyon-Saint-Etienne d Oncologie Thoracique Groupe Francais de Pneumo-Cancérologie NPC Study. J Clin Oncol. 2005;23: Furuse K, Fukuoka M, Kawahara M, et al. Phase III study of concurrent versus sequential thoracic radiotherapy in combination with mitomycin, vindesine, and cisplatin in unresectable stage III non-small-cell lung cancer. J Clin Oncol. 1999;17: Gore EM, Bae K, Wong S, et al. A phase III comparison of prophylactic cranial irradiation versus observation in patients with locally advanced non-small cell lung cancer: initial analysis of Radiation Therapy Oncology Group Abstract Presented at: 45th annual meeting of the American Society of Clinical Oncology; May 29-June 2, 2009; Orlando, Fla. Hanna N, Neubauer M, Yiannoutsos C, et al. Phase III study of cisplatin, etoposide, and concurrent chest radiation with or without consolidation docetaxel in patients with inoperable stage III non small-cell lung cancer: The Huber RM, Schmidt M, Flentje M, et al. Induction chemotherapy and following simultaneous radio/chemotherapy versus induction chemotherapy and radiotherapy alone in inoperable NSCLC (Stage IIIA/IIIB). Abstract Presented at: 39th annual meeting of the American Society of Clinical Oncology; May 29-June 3, 2003; Chicago, Ill. Mina L, Neubauer MA, Ansari R, et al. Phase III trial of cisplatin (P) plus etoposide (E) plus concurrent chest radiation (XRT) with or without consolidation docetaxel (D) in patients (pts) with inoperable stage III non-small cell lung cancer (NSCLC): HOG LUN 01-24/USO-023 updated results. Abstract Presented at: 44th annual meeting of the American Society of Clinical Oncology; May 30-June 3, 2008; Chicago, Ill. Mountain CF, Dresler CM. Regional lymph node classification for lung cancer staging. Chest. 1997;111: Sandler A, Gray R, Perry MC, et al. Paclitaxel carboplatin alone or with bevacizumab for non small-cell lung cancer. N Engl J Med. 2006;355: Shepherd FA, Pereira JR, Ciuleanu T, et al. Erlotinib in previously treated non small-cell lung cancer. N Engl J Med. 2005;353: Simon GR, Williams CC, Chiappori AA, et al. Molecular analysis-directed individualized therapy (MADeIT) in advanced non-small cell lung cancer (NSCLC). Abstract 7502.
7 Presented at: 43rd annual meeting of the American Society of Clinical Oncology; June 1-5, 2007; Chicago, Ill Socinski MA, Blackstock AW, Bogart JA, et al. Randomized phase II trial of induction chemotherapy followed by concurrent chemotherapy and dose-escalated thoracic conformal radiotherapy (74 Gy) in stage III non small-cell lung cancer: CALGB J Clin Oncol. 2008;26: Sonnet JR, Suntharalingam M, Edelman MJ, et al. Pulmonary resection after curative intent radiotherapy (>59 Gy) and concurrent chemotherapy in non-small-cell lung cancer. Ann Thorac Surg. 2004;78: Toloza EM, Harpole L, McCrory DC. Noninvasive staging of non-small cell lung cancer. Chest. 2003;123:137S-146S.
Management of stage III A-B of NSCLC. Hamed ALHusaini Medical Oncologist
 Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Adjuvant Therapy Non Small Cell Lung Cancer. Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015
 Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Maintenance therapy in in Metastatic NSCLC. Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai
 Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group
 REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
Radiotherapy in locally advanced & metastatic NSC lung cancer
 Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
SAKK Lung Cancer Group. Current activities and future projects
 SAKK Lung Cancer Group Current activities and future projects SAKK Lung Cancer Group Open group of physicians interested in lung cancer Mostly Medical Oncologists, but also Thoracic Surgeons Radiation
SAKK Lung Cancer Group Current activities and future projects SAKK Lung Cancer Group Open group of physicians interested in lung cancer Mostly Medical Oncologists, but also Thoracic Surgeons Radiation
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
National Horizon Scanning Centre. Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer. December 2007
 Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
POLICY A. INDICATIONS
 Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
Treatment of Stage III Non-small Cell Lung Cancer
 CHEST Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER, 3RD ED: ACCP GUIDELINES Treatment of Stage III Non-small Cell Lung Cancer Diagnosis and Management of Lung Cancer, 3rd ed: American College of
CHEST Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER, 3RD ED: ACCP GUIDELINES Treatment of Stage III Non-small Cell Lung Cancer Diagnosis and Management of Lung Cancer, 3rd ed: American College of
Moving forward, where are we with Clinical Trials?
 Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline
 Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline An ASCO Endorsement of Treatment of Small Cell Lung Cancer:
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline An ASCO Endorsement of Treatment of Small Cell Lung Cancer:
Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study
 Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
TRATTAMENTO COMBINATO RADIO- CHEMIOTERAPICO NEL III STADIO NSCLC
 TRATTAMENTO COMBINATO RADIO- CHEMIOTERAPICO NEL III STADIO NSCLC Dr.ssa Sara Ramella Radioterapia Oncologica Campus Bio-Medico Trimodality therapy offers a promising chance of long-term survival Evidenze
TRATTAMENTO COMBINATO RADIO- CHEMIOTERAPICO NEL III STADIO NSCLC Dr.ssa Sara Ramella Radioterapia Oncologica Campus Bio-Medico Trimodality therapy offers a promising chance of long-term survival Evidenze
Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART
 Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART Goals Discuss treatment options for stage 4 lung cancer: New and old Discuss new developments in personalized
Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART Goals Discuss treatment options for stage 4 lung cancer: New and old Discuss new developments in personalized
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Controversies in Management of. Inoperable NSCLC. Inoperable NSCLC. Introduction:
 Inoperable NSCLC Controversies in Management of Inoperable NSCLC Introduction: It is difficult to overemphasize the magnitude of lung cancer as Public Health Problem in our society. - In US, Lung cancer
Inoperable NSCLC Controversies in Management of Inoperable NSCLC Introduction: It is difficult to overemphasize the magnitude of lung cancer as Public Health Problem in our society. - In US, Lung cancer
Cetuximab (Erbitux) MM.04.005 05/10/2005. HMO; PPO; QUEST Integration 01/01/2015 Section: Prescription Drugs Place(s) of Service: Office: Outpatient
 Cetuximab (Erbitux) Policy Number: Original Effective Date: MM.04.005 05/10/2005 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2015 Section: Prescription Drugs Place(s)
Cetuximab (Erbitux) Policy Number: Original Effective Date: MM.04.005 05/10/2005 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2015 Section: Prescription Drugs Place(s)
Non-small cell lung cancer, advanced or metastatic, switch-therapy after gemcitabine/carboplatin
 COMPENDIA TRANSPARENCY TRACKING FORM DRUG: Docetaxel INDICATION: Non-small cell lung cancer, advanced or metastatic, switch-therapy after gemcitabine/carboplatin COMPENDIA TRANSPARENCY REQUIREMENTS 1 Provide
COMPENDIA TRANSPARENCY TRACKING FORM DRUG: Docetaxel INDICATION: Non-small cell lung cancer, advanced or metastatic, switch-therapy after gemcitabine/carboplatin COMPENDIA TRANSPARENCY REQUIREMENTS 1 Provide
EVIDENCE TABLE. Study Objective. (Purpose of Study)
 . Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest 997; (6):70-77.. Greene FL, Page DL, Fleming ID, et al, eds, for the American Joint Committee on Cancer. AJCC Cancer
. Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest 997; (6):70-77.. Greene FL, Page DL, Fleming ID, et al, eds, for the American Joint Committee on Cancer. AJCC Cancer
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
 Department of Veterans Affairs Health Services Research & Development Service Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
Department of Veterans Affairs Health Services Research & Development Service Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
Stage I, II Non Small Cell Lung Cancer
 Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
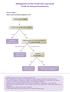 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Lung Cancer Treatment
 Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness
 Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness Investigators: Paul G. Shekelle, MD, PhD, Director Alicia R. Maher, MD Clinical
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness Investigators: Paul G. Shekelle, MD, PhD, Director Alicia R. Maher, MD Clinical
Concurrent Chemotherapy and Radiotherapy for Head and Neck Cancer
 Concurrent Chemotherapy and Radiotherapy for Head and Neck Cancer Ryan J. Burri; Nancy Y. Lee Published: 03/23/2009 Abstract and Introduction Abstract Head and neck cancer is best managed in a multidisciplinary
Concurrent Chemotherapy and Radiotherapy for Head and Neck Cancer Ryan J. Burri; Nancy Y. Lee Published: 03/23/2009 Abstract and Introduction Abstract Head and neck cancer is best managed in a multidisciplinary
Shifting the Paradigm for Maintenance Therapy for Non small-cell Lung Cancer
 J Hong Kong Col Radiol. 2010;13(Suppl):S16-21 ORIGINAL ARTICLE Shifting the Paradigm for Maintenance Therapy for Non small-cell Lung Cancer VHF Lee Department of Clinical Oncology, Queen Mary Hospital,
J Hong Kong Col Radiol. 2010;13(Suppl):S16-21 ORIGINAL ARTICLE Shifting the Paradigm for Maintenance Therapy for Non small-cell Lung Cancer VHF Lee Department of Clinical Oncology, Queen Mary Hospital,
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Future Directions in Clinical Research. Karen Kelly, MD Associate Director for Clinical Research UC Davis Cancer Center
 Future Directions in Clinical Research Karen Kelly, MD Associate Director for Clinical Research UC Davis Cancer Center Outline 1. Status of Cancer Treatment 2. Overview of Clinical Research at UCDCC 3.
Future Directions in Clinical Research Karen Kelly, MD Associate Director for Clinical Research UC Davis Cancer Center Outline 1. Status of Cancer Treatment 2. Overview of Clinical Research at UCDCC 3.
Summary ID# 13095. Clinical Study Summary: Study H3E-EW-B012
 Page 1 Summary ID# 13095 Clinical Study Summary: Study H3E-EW-B012 First-line Treatment of Non-Small Cell Lung Cancer under Routine Conditions: Observational Study on Overall Survival Date summary electronically
Page 1 Summary ID# 13095 Clinical Study Summary: Study H3E-EW-B012 First-line Treatment of Non-Small Cell Lung Cancer under Routine Conditions: Observational Study on Overall Survival Date summary electronically
REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group
 REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group In the 2002 edition of the ASCO meeting, a total of 315 abstracts in the field of respiratory
REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group In the 2002 edition of the ASCO meeting, a total of 315 abstracts in the field of respiratory
Targeted Therapy What the Surgeon Needs to Know
 Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
4.8 Lung cancer. 4.8.5 In the UK, three fractionation regimens are most commonly used:
 4.8 Lung cancer 4.8.1 In 2005, both NICE (National Institute for Health and Clinical Excellence) and SIGN (Scottish Intercollegiate Guidelines Network) published guidelines on the management of lung cancer.
4.8 Lung cancer 4.8.1 In 2005, both NICE (National Institute for Health and Clinical Excellence) and SIGN (Scottish Intercollegiate Guidelines Network) published guidelines on the management of lung cancer.
B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC
 Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
National Clinical Trials Network Groups Update Fall 2014
 National Clinical Trials Network Groups Update Fall 2014 Walter J Curran, Jr, MD An NRG Oncology Group Chair Executive Director Winship Cancer Institute of Emory University Atlanta, GA NCTN Groups Update
National Clinical Trials Network Groups Update Fall 2014 Walter J Curran, Jr, MD An NRG Oncology Group Chair Executive Director Winship Cancer Institute of Emory University Atlanta, GA NCTN Groups Update
Lung Cancer & Mesothelioma 2011-2015
 Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
Pancreatic Cancer: FDA Approved Treatments and Clinical Trials
 Pancreatic Cancer: FDA Approved Treatments and Clinical Trials Vincent J Picozzi MD MMM Virginia Mason Medical Center Seattle WA 1 Pancreatic cancer is the hardest cancer of all to treat 2 Pancreatic cancer:
Pancreatic Cancer: FDA Approved Treatments and Clinical Trials Vincent J Picozzi MD MMM Virginia Mason Medical Center Seattle WA 1 Pancreatic cancer is the hardest cancer of all to treat 2 Pancreatic cancer:
Lung cancer case study
 Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Medication Policy Manual. Topic: Alimta, pemetrexed Date of Origin: May 12, 2010
 Medication Policy Manual Policy No: dru213 Topic: Alimta, pemetrexed Date of Origin: May 12, 2010 Committee Approval Date: February 17, 2015 Next Review Date: February 2016 Effective Date: March 1, 2015
Medication Policy Manual Policy No: dru213 Topic: Alimta, pemetrexed Date of Origin: May 12, 2010 Committee Approval Date: February 17, 2015 Next Review Date: February 2016 Effective Date: March 1, 2015
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology. Endorsement of the American College of Chest Physicians (ACCP) Guideline
 Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline Table of Contents Data Supplement 1: Summary of included
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline Table of Contents Data Supplement 1: Summary of included
New Trends & Current Research in the Treatment of Lung Cancer, Pt. II
 New Trends & Current esearch in the Treatment of Lung Cancer, Pt. II Howard (Jack) West, MD President & CEO, GACE Medical Director, Thoracic Oncology Program Swedish Cancer Institute Seattle, WA Cancer
New Trends & Current esearch in the Treatment of Lung Cancer, Pt. II Howard (Jack) West, MD President & CEO, GACE Medical Director, Thoracic Oncology Program Swedish Cancer Institute Seattle, WA Cancer
People Living with Cancer
 Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
ADJUVANT TREATMENT CLINICAL EVALUATION NEOADJUVANT TREATMENT
 te: Consider Clinical Trials as treatment options for eligible patients. Referral to a center with both pediatric oncology and orthopedic surgery is essential. CLINICAL EVALUATION This practice algorithm
te: Consider Clinical Trials as treatment options for eligible patients. Referral to a center with both pediatric oncology and orthopedic surgery is essential. CLINICAL EVALUATION This practice algorithm
Activity of pemetrexed in thoracic malignancies
 Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Lung Cancer Treatment: What should we expect from the specialists?
 Lung Cancer Treatment: What should we expect from the specialists? Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 2015 Summer CME Seminar Financial
Lung Cancer Treatment: What should we expect from the specialists? Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 2015 Summer CME Seminar Financial
Non small-cell lung cancer, mesothelioma, and thymoma
 CHAPTER 7 Non small-cell lung cancer, mesothelioma, and thymoma Robert J. McKenna, Jr., MD, Benjamin Movsas, MD, Dong M. Shin, MD, and Fadlo R. Khuri, MD NSC LUNG In the United States, lung cancer has
CHAPTER 7 Non small-cell lung cancer, mesothelioma, and thymoma Robert J. McKenna, Jr., MD, Benjamin Movsas, MD, Dong M. Shin, MD, and Fadlo R. Khuri, MD NSC LUNG In the United States, lung cancer has
Update on Small Cell Lung Cancer
 Welcome to Master Class for Oncologists Session 3: 2:45 PM - 3:30 PM Washington, DC March 28, 2009 Small Cell Lung Cancer: Best Practices & Recent Advances Speaker: Bruce E. Johnson, MD Professor of Medicine,
Welcome to Master Class for Oncologists Session 3: 2:45 PM - 3:30 PM Washington, DC March 28, 2009 Small Cell Lung Cancer: Best Practices & Recent Advances Speaker: Bruce E. Johnson, MD Professor of Medicine,
Lung Cancer: An Overview
 VOL. I Issue 2 2010 Lung Cancer: An Overview By Matthew F. Koscielski, M.D. Lung cancer is the most common cause of cancer mortality worldwide. In the United States there are about 220,000 new cases of
VOL. I Issue 2 2010 Lung Cancer: An Overview By Matthew F. Koscielski, M.D. Lung cancer is the most common cause of cancer mortality worldwide. In the United States there are about 220,000 new cases of
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Metastatic Breast Cancer 201. Carolyn B. Hendricks, MD October 29, 2011
 Metastatic Breast Cancer 201 Carolyn B. Hendricks, MD October 29, 2011 Overview Is rebiopsy necessary at the time of recurrence or progression of disease? How dose a very aggressive treatment upfront compare
Metastatic Breast Cancer 201 Carolyn B. Hendricks, MD October 29, 2011 Overview Is rebiopsy necessary at the time of recurrence or progression of disease? How dose a very aggressive treatment upfront compare
Small cell Lung cancer New Chemotherapy options. Nicolas Mach, MD,PD
 Small cell Lung cancer New Chemotherapy options Nicolas Mach, MD,PD > 40 negative Phase III trials List of unsucessful drugs Pemetrexed, imatinib, bevacizumab, bcl-2 antagonist, ASCT, CASE PRESENTATION
Small cell Lung cancer New Chemotherapy options Nicolas Mach, MD,PD > 40 negative Phase III trials List of unsucessful drugs Pemetrexed, imatinib, bevacizumab, bcl-2 antagonist, ASCT, CASE PRESENTATION
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Lung cancer is not just one disease. There are two main types of lung cancer:
 1. What is lung cancer? 2. How common is lung cancer? 3. What are the risk factors for lung cancer? 4. What are the signs and symptoms of lung cancer? 5. How is lung cancer diagnosed? 6. What are the available
1. What is lung cancer? 2. How common is lung cancer? 3. What are the risk factors for lung cancer? 4. What are the signs and symptoms of lung cancer? 5. How is lung cancer diagnosed? 6. What are the available
