Dual-time point PET/CT with F-18 FDG for the differentiation of malignant and benign bone lesions
|
|
|
- Austin Simpson
- 7 years ago
- Views:
Transcription
1 Skeletal Radiol (2009) 38: DOI /s SCIENTIFIC ARTICLE Dual-time point PET/CT with F-18 FDG for the differentiation of malignant and benign bone lesions Rong Tian & Minggang Su & Ye Tian & Fanglan Li & Lin Li & Anren Kuang & Jiancheng Zeng Received: 5 November 2008 / Revised: 16 December 2008 / Accepted: 26 December 2008 / Published online: 10 February 2009 # ISS 2009 Abstract Purpose The purpose of the present study was to evaluate whether 2-fluoro[fluorine-18]-2-deoxy-D-glucose (F-18 FDG) positron emission tomography (PET) could differentiate malignant and benign bone lesions and whether obtaining delayed F-18 FDG PET images could improve the accuracy of the technique. Methods In a prospective study, 67 patients with bone lesions detected by computed tomography (CT) or magnetic resonance imaging were included. Whole body PET/CT imaging was performed at 1 h (early) after the F-18 FDG injection and delayed imaging at 2 h post injection was R. Tian : M. Su : Y. Tian : F. Li : L. Li : A. Kuang Department of Nuclear Medicine, West China Hospital of Sichuan University, Chengdu, China R. Tian zeyiqin@yahoo.com M. Su suminggang@sina.com Y. Tian crazydiamond2000@163.com F. Li lifanglan@gmail.com L. Li lli@mail.sc.cninfo.net A. Kuang kuanganren@263.net J. Zeng (*) Department of Orthopaedics, West China Hospital of Sichuan University, Chengdu, China zeyiqin@126.com performed only in the abnormal region. Semiquantitative analysis was performed using maximum standardized uptake value (SUV max ), obtained from early and delayed images (SUV maxe and SUV maxd, respectively). The retention index (RI) was calculated according to the equation: RI=(SUV maxd SUV maxe ) 100/SUV maxe. Histopathology of surgical specimens and follow-up data were used as reference criteria. The SUV maxe and RI were compared between benign and malignant lesions. Results The final diagnoses revealed 53 malignant bone lesions in 37 patients and 45 benign lesions in 30 patients. There were statistically significant differences in the SUV maxe between the malignant and benign lesions (P= 0.03). The mean SUV maxe was 6.8±4.7 for malignant lesions and 4.5±3.3 for benign lesions. However, a considerable overlap in the SUV maxe was observed between some benign and malignant tumors. With a cutoff value of 2.5 for the SUV maxe, the sensitivity, specificity, and accuracy were 96.0%, 44.0%, and 72.4%, respectively. The positive predictive value (PPV) and negative predictive value (NPV) were 67.1% and 90.9%, respectively. There were significant differences in the RI between the malignant and benign lesions (P=0.004). But there was overlap between the two groups. The mean RI was 7±11 for the benign lesions and 18±11 for the malignant lesions. When an RI of 10 was used as the cutoff point, the sensitivity, specificity, and accuracy were 90.6%, 76.0%, and %, respectively. The PPV and NPV were 81.4% and 87.1%, respectively. Conclusions The results of this study indicate that dualtime point F-18 FDG PET may provide more help in the differentiation of malignant tumors from benign ones. Keywords F-18 FDG PET. Bone lesion. SUV max. Dual-time point DO00643; No of Pages
2 452 Skeletal Radiol (2009) 38: Introduction The differentiation of benign and malignant intraosseous lesions can often be accomplished by means of radiographs, computed tomography (CT), and magnetic resonance imaging (MRI). All of these methods of morphologic imaging are very important. Radiographs including CT and X-ray provide important information about the appearance, intraosseous extent, and internal characteristics of bone tumors. MRI is highly sensitive for the detection of bone marrow abnormalities, cortical destruction, or soft tissue tumors adjacent to or infiltrating neighboring bone [1]. However, the morphologic appearance of many lesions is non-specific. With some entities, the diagnosis can be difficult with radiographic imaging or MRI. Positron emission tomography (PET) with 2-fluoro [fluorine-18]-2-deoxy-d-glucose (F-18 FDG) has been used to differentiate malignant tumors from benign lesions [2, 3]. In the musculoskeletal system, some reports suggested a good correlation between glucose consumption measured by F-18 FDG and the aggressiveness of musculoskeletal tumors [4 7]. Dehdashti et al. [8] performed F-18 FDG PET studies in a series of 20 intraosseous lesions and emphasized that 14 of 15 malignant tumors and four of five benign lesions were correctly diagnosed, using a cutoff value of 2.0 for the SUV max. However, 13 of the 15 malignant tumors were metastatic carcinomas. Aoki et al. reported a statistically significant difference in the SUV max between benign and malignant bone tumors in 52 bone lesions. However, they observed a significant overlap of the SUV max among some of the benign and malignant bone tumors, and a high accumulation of F-18 FDG was reported in some benign bone tumors [9]. Other reports [10, 11] raised questions about a clear correlation between the F-18 FDG accumulation and the malignant potential of bone tumors. The value of F-18 FDG in the musculoskeletal system is questioned. F-18 FDG PET usually is performed 1 h after F-18 FDG administration. Some studies have shown that delayed PET (2 3 h post injection) might help in differentiating malignant lesions from benign ones [12 17]. But to our knowledge, there are only a few reports of the quantitative analysis of delayed PET imaging in differentiating malignant bone lesions from benign ones. Sahlmann et al. [18] investigated glucose metabolism in 17 patients with chronic bacterial osteomyelitis and four patients with malignant bone lesions by using a dual time point F-18 FDG PET (30 and 90 min after injection). They concluded that dual time point F-18 FDG PET may be of value in the differentiation between chronic bacterial osteomyelitis and malignant bone lesions. However, the patient number in the study was small and only one kind of benign bone lesion was investigated. The purpose of the present study was to evaluate whether the early time point of F-18 FDG PET imaging (1 h post injection) can differentiate malignant from benign bone lesions and to determine whether delayed F-18 FDG PET imaging can improve the accuracy of the technique. Materials and methods Patients In a current prospective study initiated in March 2007, 67 patients (46 males, 21 females; age range, 9 76 years; median age, 46±18 years) with suspected bone tumors or tumor-like lesions based upon their X-ray, CT, or MRI studies were examined by F-18 FDG PET. In those patients, 5 had X-ray images, 48 had diagnostic CT, 7 had MRI, and 7 had both CT and MRI before the PET/CT study. Each research subject gave his or her written informed consent before participating in the study. F-18 FDG PET image acquisition and reconstruction The study protocol was approved by our institutional ethics committee and informed consent was obtained in all cases. Patients were fasted for at least 4 6 h before intravenous administration of MBq of F-18 FDG (4 MBq/kg of body weight). A serum glucose concentration was obtained before the injection and the blood glucose levels were less than 200 mg/dl in all patients. The patients were at rest in a quiet room after the injection and the PET/CT scans were performed at 1 h (early) and 2 h (delayed) post injection with a PET/CT unit (Gemini GXL; Philips Medical Systems, The Netherlands). The CT image acquisition was performed by spiral CT at 0.75 s per rotation with 40 mas and 120 kvp, a section thickness of 4 mm, and a 4-mm interval. No intravenous contrast agent was administered. The PET emission images (early images) were acquired from the proximal thigh to the mid cranium, typically requiring six to seven bed positions with a 2-min acquisition in each position. Delayed PET emission images of the abnormal areas were acquired at 2 h after the administration of F-18 FDG, using two or three bed positions with a 2-min acquisition in each position. All PET images were reconstructed using an LOR algorithm, with CT-based attenuation correction applied. Integrated images were obtained by Syntegra software. PET image interpretation and calculation of related parameters Early and delayed PET images were reviewed on a computer monitor in the transaxial, coronal, and sagittal planes along with maximum-intensity-projection images. Two experienced nuclear medicine physicians independent-
3 Skeletal Radiol (2009) 38: ly evaluated the F-18 FDG uptake semiquantitatively. The evaluating physicians were unaware of the clinical histories or the results of CT or MRI. The PET images were compared with the corresponding CT or MR images for accurate anatomic identification of the tumor. Any difference of opinion was resolved by consensus. For semiquantitative analysis, a circular region of interest (ROI) was placed over the identified bone lesion using the transverse PET image. For lesions visualized on PET, the ROIs were placed over the entire F-18 FDG-avid lesion, including the largest amount of radioactivity. When little or no lesion-related radioactivity was visually discernible, the ROI was placed at the position of the lesion on the CT or MR images. The standardized uptake value (SUV) was calculated using the following formula: SUV=tissue concentration (MBq/g)/[injected dose (MBq)/ body weight (g)]. The maximal SUV (SUV max ) in the lesion ROI was calculated for each ROI. Furthermore, we evaluated the change in the uptake in the lesions as the retention index (RI), computed as follows: RI=(SUV maxd SUV maxe ) 100/SUV maxe. Final diagnosis The final diagnosis was made by histological examination or by following up for at least 1 year with CT, MRI, or PET/CT imaging. When a tissue-based diagnosis was not available, lesion was considered malignant if an increase in size or change of character (lytic to sclerotic) was confirmed with follow-up imaging, including CT, magnetic resonance (MR), or PET/CT, with or without exacerbation of clinical symptoms; whereas, lesion was considered benign if the size and character of the lesion remained unchanged without treatment over at least 1 year [19]. Statistical analysis Differences in semiquantitative parameters were analyzed by the Student s t test. All semiquantitative data were expressed as mean±sd. For all analyses, P values of less than 0.05 were considered statistically significant. Receiver-operating-characteristic (ROC) curves for the SUV maxe and the RI were derived and evaluated by comparing the areas under the curves. The sensitivity, specificity, PPV, and NPV for the SUV maxe and RI were determined. Significance was assumed if the probability of a first-degree error was less than 0.05 (x 2 >3.841). Results The final diagnoses were confirmed by histologic examination in 60 patients (91 lesions) and by clinical and imaging followup ranging between 14 and 18 months (mean 15.5 months) in 7 patients (7 lesions). Of these 98 lesions, 53 (39 primary and 14 metastatic, all based on histological verification) were malignant in 37 patients and 45 were benign (38 based on histological verification) in 30 patients. The malignant lesions were comprised of 6 osteosarcomas, 4 Ewing s sarcomas, 3 chondrosarcomas, 13 myelomas, 11 primary bone non- Hodgkin s lymphomas, 2 neuroblastomas, and 14 bone metastases. Among the metastatic bone lesions were eight lung adenocarcinomas, two esophageal carcinomas, two renal carcinomas, one hepatic cell cancer, and one thyroid cancer. The benign lesions were comprised of six giant cell tumors, seven tuberculosis, three osteomyelitis, ten fibrous dysplasia, five osteoblastomas, four bone hemangiomas, three fractures, three eosinophilic granulomas, two osteitis, and two enchondromas. The histological subtypes are shown in Table 1. There were statistically significant differences in the SUV maxe between the malignant and benign lesions (P= 0.03). The SUV maxe in the malignant group was higher than that in the benign group. The mean SUV maxe was 6.8±4.7 (range, ) for malignant lesions and 4.5±3.3 (range, ) for benign lesions. However, a considerable overlap in the SUV maxe was observed between some benign and malignant tumors (Fig. 1). In the malignant group, most of lesions showed a high uptake of F-18 FDG. A particularly high uptake of F-18 FDG was seen in all 11 malignant lymphomas, 12 of 14 metastatic lesions, 7 of 13 myelomas, and all 6 osteosarcomas, whereas glucose consumption was lower in the other neoplasms, such as was seen in 6 of 13 myelomas, 2 metastatic lesions from hepatic cell cancer and thyroid cancer, and in 2 chondrosarcomas. The benign Table 1 The histological subtypes of benign and malignant lesions Malignant 53 Metastasis tumors 14 Primary tumors 39 Non-Hodgkin s lymphoma 11 Myeloma 13 Osteosarcoma 6 Ewing s sarcomas 4 Chondrosarcoma 3 Neuroblastoma 2 Benign 45 Giant cell tumor 6 Tuberculosis 7 Osteomyelitis 3 Fibrous dysplasia 10 Osteoblastoma 5 Bone hemangioma 4 Fracture 3 Eosinophilic granulomas 3 Osteitis 2 Lesions (n)
4 454 Skeletal Radiol (2009) 38: Fig. 1 Box and whisker plot of SUV maxe for benign and malignant bone lesions. The top of the boxes represent the mean and error bars represent the range of SUV maxe. Although there is a statistically significant difference between the SUV maxe of the benign and malignant bone lesions (p<0.05), there are significant overlaps between the malignant and the benign lesions (p<0.05) lesions that showed a high accumulation of F-18 FDG included all of the giant cell tumors (Fig. 2), tuberculosis, Langerhans cell histiocytosis, osteomyelitis, osteoblastoma (Fig. 3), and some of the fibrous dysplasia, whereas the glucose consumption was substantially lower in the other benign lesions. The characteristics of the benign lesions showing an increasing FDG uptake over time are shown in Table 2. With a cutoff value of 2.5 for the SUV maxe, 51 of the 53 malignant lesions and 20 of the 45 benign lesions were characterized correctly, and the sensitivity, specificity, and accuracy of the F-18 FDG PET for the differentiation of benign from malignant intraosseous lesions were 96.0%, 44.0%, and 72.4%, respectively. The positive and negative predictive values were 67.1% and 90.9%, respectively. There were significant differences in the RI between the malignant and benign lesions (P=0.004). The RIs in the malignant group were higher than those in the benign group. But there was still overlap between the two groups (Fig. 4). The mean RI was 7±11 (range, 7 to 23) for the benign lesions and 18±11 (range, 7 to 46) for the malignant lesions (Fig. 5). When an RI of 10 was used as the cutoff point,48 of the 53 malignant lesions and 34 of the 45 benign lesions were characterized correctly, and the sensitivity, specificity, and accuracy of the F-18 FDG PET for differentiation of benign from malignant intraosseous lesions were 90.6% and 76.0%, and % respectively. The positive and negative predictive values were 81.4% and 87.1%, respectively. Three of 16 myeloma lesions and two of 14 metastatic lesions (from thyroid cancer and hepatic cell carcinoma) showed decreased uptakes of F-18 FDG in the delayed image. In the benign group, a particularly high RI was observed in TB and chronic osteomyelitis. The diagnostic value of F-18 FDG PET using semiquantitative analysis for the differentiation of benign and malignant bone lesions is shown in Table 3. ROC analyses were performed to compare the roles of the SUV maxe and RI in the differentiation of malignant from benign lesions. The areas under curves (AUCs) for the SUV maxe and RI were (95%CI ) and (95%CI ), respectively. The AUCs for RI were statistically higher than those for the SUV maxe (P=0.03). Discussion The usefulness of F-18 FDG has been reported in the distinction of benign from malignant bone tumors [6, 7, 20]. However, other reports [10] raised the question of a clear correlation between F-18 FDG accumulation and the malignant potential of bone tumors. A high accumulation of F-18 FDG has been reported in some benign bone diseases [9]. The current study showed that although the SUV maxe in the malignant bone lesions was statistically higher than that in the benign lesions in total, a considerable overlap of SUV maxe was observed between the two groups. This indicated that early F-18 FDG PET imaging (1 h post injection) might not give more information for the differen- Fig. 2 Biopsy-proved giant cell tumor. a CT imaging showed bone destruction and soft tissue invasion in the proximal tibia (arrow). b Integrated image showed high uptake of F-18 FDG in the bone destruction area (SUV maxe =13.92; arrow)
5 Skeletal Radiol (2009) 38: Fig. 3 Biopsy-proved osteoblastoma. a CT imaging showed bone expansion and cortical destruction (arrow). b Integrated image showed high uptake of F-18 FDG in destruction area (SUV maxe =5.33; arrow) tiation of benign from malignant intraosseous lesions. This result corresponds with the findings from Kole et al. [10, 11]. Kole et al. investigated the glucose metabolism in 19 malignant and 7 benign bone tumors with F-18 FDG PET. They found that there was a large overlap between the rate of glucose consumption (MRglc) of benign and malignant lesions and thus concluded that it was not possible to differentiate between benign and malignant bone tumors with F-18 FDG PET. However, other reports showed a clear distinction in the uptake of F-18 FDG between benign and malignant intraosseous lesions. Dehdashti et al. [8] studied 20 patients with intraosseous lesions and reported that the SUV was helpful in the diagnosis of benign and malignant intraosseous lesions. However, they investigated only 3 primary bone tumors and 12 metastatic lesions, so their patient group was not representative of patients with primary bone tumors. Shin et al. [20] analyzed the characteristics and amount of F-18 FDG uptake in 91 patients with soft tissue and bone tumors, and investigated the ability of F-18 FDG PET/CT to differentiate malignant from benign tumors. They found that F-18 FDG PET/CT reliably differentiated malignant soft tissue and bone tumors from benign ones using a cutoff level of 3.4 for SUV max, although there were many false-positive and false-negative lesions. However, this was a retrospective study. Schulte et al. reported 202 histologically verified bone lesions and found a sensitivity of 93% and a specificity of 66.7% using a cutoff level of 3.0 for the tumorto-background ratio. They concluded that F-18 FDG PET provides a promising tool for estimating the biologic activity of skeletal lesions. But, they also found that aggressive benign lesions could not be distinguished from sarcomas, and their data showed that the sensitivity and specificity depended on the variety of histologic subtypes included in a study and on the cutoff level defined by the investigators. The different histologic subtypes of lesions included in various studies and the different number of cases in these reports may be the cause of the varying opinions on the value of early F-18 FDG PET. The known false-positive lesions include giant cell tumor, osteoid osteoma, histiocytosis-x, chondroblastoma, enchondroma, and non-ossifying fibroma in benign tumors. The false-negative malignant tumors were chondrosarcomas [9, 21, 22]. In the current study, benign lesions such as giant cell tumors, tuberculosis, Langerhans cell histiocytosis, osteomyelitis, osteoblastoma, fibrous dysplasia, and fracture showed a particularly high uptake of F-18 FDG. Some of these benign lesions, Table 2 SUV maxe for benign lesion Histological Lesions (n) SUV maxe (mean±sd) Giant cell tumor 6 8.9±3.4 ( ) Tuberculosis 7 7.8±3.4 ( ) Osteomyelitis 3 8.4±3.3 ( ) Fibrous dysplasia ±0.7 ( ) Osteoblastoma 5 5.0±0.4 ( ) Bone hemangioma 4 1.8±0.3 ( ) Fracture 3 2.8±0.7 ( ) Eosinophilic granuloma ±3 ( ) enchondroma 2 2.0±0.3 ( ) Osteitis 2 1.8±0.4 ( ) Fig. 4 Box and whisker plot of RI for benign and malignant lesions. The top of the boxes represent the mean and error bars represent the range of RI. Although there are overlaps between the malignant and benign lesions, there is a statistically significant difference between the RI of the benign and malignant bone lesions (p<0.05)
6 456 Skeletal Radiol (2009) 38: Fig. 5 Biopsy-proved chondrosarcoma in a 39-year-old woman with paralysis in both lower limbs. a Early fused image shows increased uptake of F-18 FDG at her vertebra (SUV maxe = 5.81; arrow). b The delayed fused image shows more uptake at her vertebra (SUV maxd =7.28, RI=25; arrow) than does the early image. c CT imaging showed bone destruction in both the right aspect of the vertebral body and the posterior elements, and faint calcification was seen in the soft-tissue mass such as giant cell tumors, Langerhans cell histiocytosis, and osteoblastoma can be categorized as histiocytic or giantcell-containing lesions and are known to show locally aggressive features in conventional radiological imaging, such as ill-defined margins, interrupted periosteal reactions, and extensive surrounding edema [21]. Histiocytes and giant cells in tissues are in the monocyte macrophage lineage [23]. Macrophages play a central role in the host response to injury and infection, and their energy is predominantly supplied by means of intracellular glucose metabolism. Although it is still controversial whether histiocytic cells and giant cells in primary bone tumors are reactive or neoplastic, these cells might partially contribute to the high uptake of F-18 FDG in the benign bone lesions [9]. Increased F-18 FDG uptake might similarly reflect the local aggressiveness of these benign bone lesions, but the results revealed no additional information helpful in their differentiation from malignant tumors. The high uptake of F-18 FDG in fibrous dysplasia lesions may be attributed to fibroblasts, which are the predominant proliferating cells of fibrous dysplasia lesions and are known to show a relatively high accumulation of F-18 FDG [24]. Our study indicated that the SUV maxe in some fibrous dysplasia lesions were less than 2.5. The difference in the SUV maxe among fibrous dysplasia lesions may be due to a difference in the amount of actively proliferating fibroblasts [21]. Active granulomatous processes, such as tuberculosis and eosinophilic granuloma, have been reported to accumulate F-18 FDG. Granulomatous lesions are characterized by cellular infiltrates, granuloma formation, and macrophage proliferation. Activated inflammatory cells have markedly increased glycolysis and the hexose monophosphate shunt is stimulated by phagocytosis, with increases of times baseline values common in these stimulated cells [25 27]. In our study, one of three fracture lesions showed a high uptake of F-18 FDG (SUV maxe =3.6). This was proven to be an acute benign fracture. The reason why acute benign fractures have a high uptake of F-18 FDG may be related to the inflammatory infiltrate associated with the acute healing process. Our results are similar to other reports. Bredella et al. [28] reported the usefulness of F-18 FDG PET for the differen- Table 3 Diagnostic value of F-18 FDG PET using semiquantitative analysis for the differentiation of benign and malignant bone lesions Parameter Sensitivity (%) Specificity (%) Accuracy (%) NPV (%) PPV (%) Early image RI SUVmaxEy cutoff=2.5; RI cutoff=10 NPV Negative predictive value, PPV positive predictive value
7 Skeletal Radiol (2009) 38: tiation of benign and malignant fracture. Their study showed that the range of SUV maxe for benign fracture was 0.7 to 4.9. This study also indicated that dual-time point F-18 FDG PET may provide more help in differentiating malignant bone tumors from benign ones. The results in this study demonstrated that there was a difference in the RI between benign and malignant lesions and the areas under curves (AUCs) for RI were statistically higher than those for the SUV maxe. This suggests that dual-time point imaging may provide more information than early imaging in the differentiation of benign and malignant bone lesions. To our knowledge, there are only a few reports of the quantitative analysis of delayed PET imaging in differentiating malignant bone lesions from benign ones. Sahlmann et al. [18] investigated glucose metabolism in 17 patients with chronic bacterial osteomyelitis and 4 patients with malignant bone lesions by using a dual-time point F-18 FDG PET. They concluded that dual-time point F-18 FDG PET may be of value in the differentiation between chronic bacterial osteomyelitis and malignant bone lesions. However, the patient number in the study was small and they only investigated one kind of benign bone lesion. Our findings are consistent with other results of the role of dual-time point F-18 FDG PET for the differentiation of malignant lesions from benign ones. Xiu et al. analyzed the retention index (RI) of 46 patients with pulmonary nodules with borderline levels of increased F-18 FDG activity on the initial PET scan. They found that the dual-time point imaging yielded the most accurate result when an RI threshold of 10% was used [17]. Mavi et al. investigated 152 patients with newly diagnosed breast cancer who underwent dual-time point imaging for reoperative staging. They found that the sensitivity and accuracy was improved in dual-time point imaging [16]. In head and neck cancer patients, a 12% change of the SUV max between two PET scans was noted in malignant cancer, whereas benign inflammatory lesions and physiologic F-18 FDG uptake lesions showed a stable pattern over time, or a slight decline [29]. There are also other reports which claimed that dual-time point F-18 FDG PET might have the capability to differentiate malignant lesions from benign ones [15, 30]. Although numerous studies demonstrated the value of dual-time point F-18 FDG PET in the differentiation of malignant lesions from benign ones, there are other reports which claimed that dual-time point F-18 FDG PET might have a limited capability to differentiate malignant lesions from benign ones. Hamada et al. [31] found that there was no significant difference in the RI between malignant and benign soft-tissue lesions and indicated that the delayed F-18 FDG PET scan might not help to differentiate malignant soft-tissue tumors from benign ones. However, there was bias in their case selection. Although the results in our study demonstrated that there was a difference in the RI between benign and malignant lesions, there was overlap between the two groups. Three of 16 myeloma lesions and 2 of 14 metastatic lesions showed decreased uptakes of F-18 FDG in the delayed image. In the benign group, a particularly high RI was observed in TB and chronic osteomyelitis. The reasons for the overlap are not clear. Our study has limitations. In particular, the number of histologic subtypes of lesions in this study is not sufficient to analyze according to subgroups. In a future study, the inclusion of a large number of lesions in each subtype is recommended. Besides, in this study, CT was used only as attenuation correction, although its additional value in the differential diagnosis of benign vs. malignant primary bone lesions with F-18 FDG PET/CT has been reported recently [32]. Conclusions Dual-time point F-18 FDG PET is practical in the daily work routine. This study indicated that dual-time point F-18 FDG PET may provide more help in differentiating malignant tumors from benign ones. According to the results of this study, dual-time point F-18 FDG PET was recommended for the evaluation of unclear bone lesions. The inclusion of a larger number of cases, including those with different histologic subtypes, is recommended for future studies. Acknowledgments We thank BioMed Proofreading for assistance in editing the manuscript. We also thank Luyi Zhou, Ph.D., for biostatistical assistance. References 1. Erlemann R. MRI is highly sensitive for the detection of bone marrow abnormalities, cortical destruction or soft tissue tumors adjacent or infiltrating neighboring bones. Eur J Radiol 2006; 58(1): Hillner BE, Siegel BA, Shields AF, et al. Relationship between cancer type and impact of PET and PET/CT on intended management: findings of the National Oncologic PET Registry. J Nucl Med 2008; 49(12): Kim SK, Allen-Auerbach M, Goldin J, et al. Accuracy of PET/CT in characterization of solitary pulmonary lesions. J Nucl Med 2007; 48(2): Dimitrakopoulou-Strauss ASL, Heichel T, Wu H, Burger C, Bernd L, Ewerbeck V. The role of quantitative 18 F-FDG PET studies for the differentiation of malignant and benign bone lesions. J Nucl Med 2002; 43(4): Kern KA, Brunetti A, Norton JA, et al. Metabolic imaging of human extremity musculoskeletal tumors by PET. J Nucl Med 1988; 29(2): Adler LP, Blair HF, Makley JT, et al. Noninvasive grading of musculoskeletal tumors using PET. J Nucl Med 1991; 32(8): Griffeth LK, Dehdashti F, McGuire AH, et al. PET evaluation of soft-tissue masses with fluorine-18 fluoro-2-deoxy-d- glucose. Radiology 1992; 182(1):
8 458 Skeletal Radiol (2009) 38: Dehdashti FSB, Griffeth LK, Fusselman MJ, Trask DD, McGuire AH. Benign versus malignant intraosseous lesions: discrimination by means of PET with 2-[F-18]fluoro-2-deoxy-D-glucose. Radiology 1996; 200(1): Aoki J, Watanabe H, Shinozaki T, et al. FDG PET of primary benign and malignant bone tumors: standardized uptake value in 52 lesions. Radiology 2001; 219(3): Kole AC, Nieweg OE, Hoekstra HJ, van Horn JR, Koops HS, Vaalburg W. Fluorine-18-fluorodeoxyglucose assessment of glucose metabolism in bone tumors. J Nucl Med 1998; 39(5): Schulte M, Brecht-Krauss D, Heymer B, et al. Grading of tumors and tumorlike lesions of bone: evaluation by FDG PET. J Nucl Med 2000; 41(10): Zhuang H, Pourdehnad M, Lambright ES, et al. Dual time point 18 F-FDG PET imaging for differentiating malignant from inflammatory processes. J Nucl Med 2001; 42(9): Lan XL, Zhang YX, Wu ZJ, Jia Q, Wei H, Gao ZR. The value of dual time point 18 F-FDG PET imaging for the differentiation between malignant and benign lesions. Clinical radiology 2008; 63(7): Matthies A, Hickeson M, Cuchiara A, Alavi A. Dual time point 18 F-FDG PET for the evaluation of pulmonary nodules. J Nucl Med 2002; 43(7): Ma S-Y, See L-C, Lai C-H, et al. Delayed 18 F-FDG PET for detection of paraaortic lymph node metastases in cervical cancer patients. J Nucl Med 2003; 44(11): Mavi A, Urhan M, Yu JQ, et al. Dual time point 18 F-FDG PET imaging detects breast cancer with high sensitivity and correlates well with histologic subtypes. J Nucl Med 2006; 47(9): Xiu Y, Bhutani C, Dhurairaj T, et al. Dual-time point FDG PET imaging in the evaluation of pulmonary nodules with minimally increased metabolic activity. Clin Nucl Med 2007; 32(2): Sahlmann CO, Siefker U, Lehmann K, Meller J. Dual time point 2-[18F]fluoro-2 -deoxyglucose positron emission tomography in chronic bacterial osteomyelitis. Nucl Med Commun 2004; 25(8): Daisuke U, Shinya S, Masanori I, et al. Added value of SPECT/ CT fusion in assessing suspected bone metastasis: comparison with scintigraphy alone and nonfused scintigraphy and CT. Radiology 2005; 238(11): Shin DS, Shon OJ, Han DS, Choi JH, Chun KA, Cho IH. The clinical efficacy of 18 F-FDG-PET/CT in benign and malignant musculoskeletal tumors. Ann Nucl Med 2008; 22(7): Aoki J, Endo K, Watanabe H, Shinozaki T, Yanagawa T, Ahmed AR, et al. FDG-PET for evaluating musculoskeletal tumors. J Orthop Sci 2003; 8(3): Feldman F, Heertum RV, Manus C. 18 FDG PET scanning of benign and malignant musculoskeletal lesions. Skeletal Radiol 2003; 32: Meszaros K, Lang CH, Bagby GJ, Spitzer JJ. Contribution of different organs to increased glucose consumption after endotoxin administration. J Biol Chem 1987; 262(23): Strobel K, Bode B, Lardinois D, Exner U. PET-positive fibrous dysplasia a potentially misleading incidental finding in a patient with intimal sarcoma of the pulmonary artery. Skeletal Radiology 2007; 36: Conill C, Setoain X, Colomo L, et al. Diagnostic efficacy of bone scintigraphy, magnetic resonance imaging, and positron emission tomography in bone metastases of myxoid liposarcoma. J Magn Reson Imaging 2008; 27(3): Goo JM, Im J-G, Do K-H, et al. Pulmonary tuberculoma evaluated by means of FDG PET: findings in 10 cases. Radiology 2000; 216(1): Knight SB, Delbeke D, Stewart JR, Sandler MP. Evaluation of pulmonary lesions with FDG-PET: comparison of findings in patients with and without a history of prior malignancy. Chest 1996; 109(4): Bredella MA, Essary B, Torriani M, Ouellette HA, Palmer WE. Use of FDG-PET in differentiating benign from malignant compression fractures. Skeletal Radiol 2008; 37(5): Hustinx R, Smith RJ, Benard F, Rosenthal DI, Machtay M, Farber LA, et al. Dual time point fluorine-18 fluorodeoxyglucose positron emission tomography: a potential method to differentiate malignancy from inflammation and normal tissue in the head and neck. Eur J Nucl Med 1999; 26(10): Yoshihiro N, Yuka Y, Naruhide K, Shinya I, Yasuhiro S, Ohkawa M. Dual-time-point FDG-PET for evaluation of lymph node metastasis in patients with non-small-cell lung cancer. Ann Nucl Med 2008; 22: Hamada K, Tomita Y, Ueda T, et al. Evaluation of delayed 18 F-FDG PET in differential diagnosis for malignant soft-tissue tumors. Ann Nucl Med 2006; 20(10): Strobel K, Exner UE, Stumpe KD, Hany TF, Bode B, Mende K, et al. The additional value of CT images interpretation in the differential diagnosis of benign vs. malignant primary bone lesions with 18 F-FDG- PET/CT. Eur J Nucl Med Mol Imaging 2008; 35(11):
False positive PET in lymphoma
 False positive PET in lymphoma Thomas Krause Introduction and conclusion 2 3 Introduction 4 FDG-PET in staging of lymphoma 34 studies with 2227 Patients CT FDG-PET Sensitivity 63 % 89 % (58%-100%) (63%-100%)
False positive PET in lymphoma Thomas Krause Introduction and conclusion 2 3 Introduction 4 FDG-PET in staging of lymphoma 34 studies with 2227 Patients CT FDG-PET Sensitivity 63 % 89 % (58%-100%) (63%-100%)
CHARACTERSTIC RADIOGRAPHIC APPEARANCE
 OSTEOLYTIC LESIONS APPROACH AGE Metastatic Neuroblastoma in infant and young child. Metastases and multiple myeloma in middle aged and elderly. Ewing s sarcoma and simple bone cyst in children and teens.
OSTEOLYTIC LESIONS APPROACH AGE Metastatic Neuroblastoma in infant and young child. Metastases and multiple myeloma in middle aged and elderly. Ewing s sarcoma and simple bone cyst in children and teens.
Radiologic Evaluation of Bone Tumors. Alan Laorr, MD Chief, Musculoskeletal Radiology Suburban Radiologic Consultants Minneapolis, Minnesota
 Radiologic Evaluation of Bone Tumors Alan Laorr, MD Chief, Musculoskeletal Radiology Suburban Radiologic Consultants Minneapolis, Minnesota Dx of Bone Tumors I. Clinical Information II. Location III. Morphology
Radiologic Evaluation of Bone Tumors Alan Laorr, MD Chief, Musculoskeletal Radiology Suburban Radiologic Consultants Minneapolis, Minnesota Dx of Bone Tumors I. Clinical Information II. Location III. Morphology
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer
 In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
In Practice Whole Body MR for Visualizing Metastatic Prostate Cancer Prostate cancer is the second most common cancer in men worldwide, accounting for 15% of all new cancer cases. 1 Great strides have
PET/CT: Basic Principles, Applications in Oncology
 PET/CT: Basic Principles, Applications in Oncology Mabel Djang, HMS III Overview PET Basics and Limitations PET/CT - Advantages and Limitations Applications of PET/CT in oncology Summary 2 Principles of
PET/CT: Basic Principles, Applications in Oncology Mabel Djang, HMS III Overview PET Basics and Limitations PET/CT - Advantages and Limitations Applications of PET/CT in oncology Summary 2 Principles of
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice
 Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
Sodium Fluoride PET/CT Bone Imaging: Theory and Practice George Segall, M.D. Stanford University Why F-18 Fluoride? Faster Higher Resolution Anatomic Correlation Chemiadsorption Hydroxyapatite Ca10(PO4)6(OH)2
Use of FDG-PET in differentiating benign from malignant compression fractures
 Skeletal Radiol (2008) 37:405 413 DOI 10.1007/s00256-008-0452-5 SCIENTIFIC ARTICLE Use of FDG-PET in differentiating benign from malignant compression fractures Miriam A. Bredella & Brendan Essary & Martin
Skeletal Radiol (2008) 37:405 413 DOI 10.1007/s00256-008-0452-5 SCIENTIFIC ARTICLE Use of FDG-PET in differentiating benign from malignant compression fractures Miriam A. Bredella & Brendan Essary & Martin
Bone Windows for Distinguishing Malignant from Benign Primary Bone Tumors on FDG PET/CT
 Ivyspring International Publisher Research Paper 524 Journal of Cancer 2013; 4(7): 524-530. doi: 10.7150/jca.6259 Bone Windows for Distinguishing Malignant from Benign Primary Bone Tumors on FDG PET/CT
Ivyspring International Publisher Research Paper 524 Journal of Cancer 2013; 4(7): 524-530. doi: 10.7150/jca.6259 Bone Windows for Distinguishing Malignant from Benign Primary Bone Tumors on FDG PET/CT
PET. Can we afford PET-CT. Positron annihilation. PET-CT scanner. PET detection
 PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
PET-CT Can we afford PET-CT John Buscombe New technology Combines functional information-pet anatomical information-ct Machine able to perform both studies in single imaging episode PET imaging depends
A Diagnostic Chest XRay: Multiple Myeloma
 Daniela Marinho Tridente, VI FCMSCSP October 2013 A Diagnostic Chest XRay: Multiple Myeloma Daniela Marinho Tridente, VI FCMSCSP Our Learning Agenda Introduction of our patient His imaging data and findings
Daniela Marinho Tridente, VI FCMSCSP October 2013 A Diagnostic Chest XRay: Multiple Myeloma Daniela Marinho Tridente, VI FCMSCSP Our Learning Agenda Introduction of our patient His imaging data and findings
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
MANAGEMENT OF BENIGN BONE TUMORS
 MANAGEMENT OF BENIGN BONE TUMORS HISTORY AND EXAMINATION An adequate history and physical examination are the first and most important steps in evaluating a patient with a musculoskeletal tumor PRESENTING
MANAGEMENT OF BENIGN BONE TUMORS HISTORY AND EXAMINATION An adequate history and physical examination are the first and most important steps in evaluating a patient with a musculoskeletal tumor PRESENTING
Low-dose CT Imaging. Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital
 Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7
 Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7 Authors Ronald C. Walker 1,2, Tracy L. Brown 3, Laurie B. Jones-Jackson
Continuing Medical Education Article Imaging of Multiple Myeloma and Related Plasma Cell Dyscrasias JNM, July 2012, Volume 53, Number 7 Authors Ronald C. Walker 1,2, Tracy L. Brown 3, Laurie B. Jones-Jackson
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Patterns of nodal spread in thoracic malignancies
 Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
Patterns of nodal spread in thoracic malignancies Poster No.: C-0977 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: R. dos Santos, M. Duarte, J. Alpendre, J. Castaño, Z. Seabra, Â.
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1. Jonathan C. Daniel 2. Kenneth S.
 PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
Elements of PET/CT Reporting
 Elements of PET/CT Reporting 1. Clinical History a. Indication i. tumor type ii. abnormality to be evaluated iii. specific clinical question b. Relevent history i. biopsy results ii. chemotherapy iii.
Elements of PET/CT Reporting 1. Clinical History a. Indication i. tumor type ii. abnormality to be evaluated iii. specific clinical question b. Relevent history i. biopsy results ii. chemotherapy iii.
Oncology. Objectives. Cancer Nomenclature. Cancer is a disease of the cell Cancer develops when certain cells begin to grow out of control
 Oncology Objectives Describe the etiology and pathophysiological mechanisms of cancer Discuss medical and family history findings relevant to cancer Identify general signs and symptoms associated with
Oncology Objectives Describe the etiology and pathophysiological mechanisms of cancer Discuss medical and family history findings relevant to cancer Identify general signs and symptoms associated with
Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice
 Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice By Howard (Jack) West, MD May, 2009 Hello and welcome to the GRACE audio podcast on PET scanning. This one is with Dr. David
Interview with David Djang, MD On PET Scan in Oncology: Principles and Practice By Howard (Jack) West, MD May, 2009 Hello and welcome to the GRACE audio podcast on PET scanning. This one is with Dr. David
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
The Lewin Group undertook the following steps to identify the guidelines relevant to the 11 targeted procedures:
 Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Crosswalk for Positron Emission Tomography (PET) Imaging Codes G0230 G0030, G0032, G0034, G0036, G0038, G0040, G0042, G0044, G0046
 Positron Emission Tomography (PET) CPT to HCPCS Level Crosswalk Changes below from CMS Change Request 3741 Transmittals 518 & 31 published on April 1, 2005; mplementation of CPT codes are effective January
Positron Emission Tomography (PET) CPT to HCPCS Level Crosswalk Changes below from CMS Change Request 3741 Transmittals 518 & 31 published on April 1, 2005; mplementation of CPT codes are effective January
PET/CT in Breast Cancer
 PET/CT in Breast Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria Overview Introduction Locorregional
PET/CT in Breast Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria Overview Introduction Locorregional
PET/CT-MRI First clinical experience
 20 th April 2013, Barcelona, Sp PET/CT-MRI First clinical experience Philippe Appenzeller, MD Staff Radiologist and Nuclear Medicine Physician Department Medical Imaging, University Hospital Zurich PET/CT-MR
20 th April 2013, Barcelona, Sp PET/CT-MRI First clinical experience Philippe Appenzeller, MD Staff Radiologist and Nuclear Medicine Physician Department Medical Imaging, University Hospital Zurich PET/CT-MR
Case Report: Whole-body Oncologic Imaging with syngo TimCT
 Case Report: Whole-body Oncologic Imaging with syngo TimCT Eric Hatfield, M.D. 1 ; Agus Priatna, Ph.D. 2 ; John Kotyk, Ph.D. 1 ; Benjamin Tan, M.D. 1 ; Alto Stemmer 3 ; Stephan Kannengiesser, Ph.D. 3 ;
Case Report: Whole-body Oncologic Imaging with syngo TimCT Eric Hatfield, M.D. 1 ; Agus Priatna, Ph.D. 2 ; John Kotyk, Ph.D. 1 ; Benjamin Tan, M.D. 1 ; Alto Stemmer 3 ; Stephan Kannengiesser, Ph.D. 3 ;
2011 Radiology Diagnosis Coding Update Questions and Answers
 2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
CHAPTER 2. Neoplasms (C00-D49) March 2014. 2014 MVP Health Care, Inc.
 Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Incidence of Incidental Thyroid Nodules on Computed Tomography (CT) Scan of the Chest Performed for Reasons Other than Thyroid Disease
 International Journal of Clinical Medicine, 2011, 2, 264-268 doi:10.4236/ijcm.2011.23042 Published Online July 2011 (http://www.scirp.org/journal/ijcm) Incidence of Incidental Thyroid Nodules on Computed
International Journal of Clinical Medicine, 2011, 2, 264-268 doi:10.4236/ijcm.2011.23042 Published Online July 2011 (http://www.scirp.org/journal/ijcm) Incidence of Incidental Thyroid Nodules on Computed
Comparison of Threshold-Based Segmentation Methods on Pre- and Post- Therapy PET Scans
 M. Phillips, S.F. Barrington, D.L.G. Hill, P.K. Marsden 1 Comparison of Threshold-Based Segmentation Methods on Pre- and Post- Therapy PET Scans Michael Phillips 1 Michael.Phillips.1@city.ac.uk Sally F.
M. Phillips, S.F. Barrington, D.L.G. Hill, P.K. Marsden 1 Comparison of Threshold-Based Segmentation Methods on Pre- and Post- Therapy PET Scans Michael Phillips 1 Michael.Phillips.1@city.ac.uk Sally F.
.org. Metastatic Bone Disease. Description
 Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Radiologic Diagnosis of Spinal Metastases
 September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
September 2002 Radiologic Diagnosis of Spinal Metastases Natalie J. M. Dailey, Harvard Medical Student Year III Our Patient s Presenting Story 70 year old male Presents to the hospital for laparascopic
5 Localized Bone Lesions
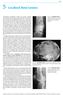 75 5 Localized Bone Lesions Conventional radiography remains the primary imaging modality for the evaluation of skeletal lesions. The combination of conventional radiography, which has a high specificity
75 5 Localized Bone Lesions Conventional radiography remains the primary imaging modality for the evaluation of skeletal lesions. The combination of conventional radiography, which has a high specificity
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Differential diagnosis of vertebral compression fracture using in-phase/opposed-phase and Short TI inversion recovery imaging
 Differential diagnosis of vertebral compression fracture using in-phase/opposed-phase and Short TI inversion recovery imaging Poster No.: C-0795 Congress: ECR 2013 Type: Scientific Exhibit Authors: A.
Differential diagnosis of vertebral compression fracture using in-phase/opposed-phase and Short TI inversion recovery imaging Poster No.: C-0795 Congress: ECR 2013 Type: Scientific Exhibit Authors: A.
SPECT and PET imaging in porcine inflammation and infection models. UCPH pig model network seminar
 SPECT and PET imaging in porcine inflammation and infection models UCPH pig model network seminar Friday November 21. 2014, 8.30 12.00, auditorium A2 70.02, Thorvaldsensvej 40, 1871 Frederiksberg C. See
SPECT and PET imaging in porcine inflammation and infection models UCPH pig model network seminar Friday November 21. 2014, 8.30 12.00, auditorium A2 70.02, Thorvaldsensvej 40, 1871 Frederiksberg C. See
Metastatic Prostate Cancer Causing Complete Obstruction of the IVC
 Department of Radiology Henry Ford Health System Detroit, Michigan Metastatic Prostate Cancer Causing Complete Obstruction of the IVC Jennifer Johnston MSIII, Wayne State Medical School Stage 4 Metastatic
Department of Radiology Henry Ford Health System Detroit, Michigan Metastatic Prostate Cancer Causing Complete Obstruction of the IVC Jennifer Johnston MSIII, Wayne State Medical School Stage 4 Metastatic
Comparison of radiation dose from X-ray, CT, and PET/ CT in paediatric patients with neuroblastoma using a dose monitoring program
 Comparison of radiation dose from X-ray, CT, and PET/ CT in paediatric patients with neuroblastoma using a dose monitoring program Poster No.: C-0591 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific
Comparison of radiation dose from X-ray, CT, and PET/ CT in paediatric patients with neuroblastoma using a dose monitoring program Poster No.: C-0591 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific
Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method
 Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method Christopher Martel, M.Sc., CHP Lisa Thornhill,, NRRPT, RT(NM) Boston University Medical Center Thyroid Carcinoma New cases and deaths in
Treating Thyroid Cancer using I-131 Maximum Tolerable Dose Method Christopher Martel, M.Sc., CHP Lisa Thornhill,, NRRPT, RT(NM) Boston University Medical Center Thyroid Carcinoma New cases and deaths in
Response Criteria for Malignant Lymphoma 2007. Cheson Criteria. Quick Reference Guide
 Response Criteria for Malignant Lymphoma 2007 Cheson Criteria Quick Reference Guide Table of Contents Summary of Assessments...3 Baseline Lesion Burden...4 What isameasurable Lesion?...5 Choosing Target
Response Criteria for Malignant Lymphoma 2007 Cheson Criteria Quick Reference Guide Table of Contents Summary of Assessments...3 Baseline Lesion Burden...4 What isameasurable Lesion?...5 Choosing Target
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy
 Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
CPT CODE PROCEDURE DESCRIPTION. CT Scans 70450 CT HEAD/BRAIN W/O CONTRAST 70460 CT HEAD/BRAIN W/ CONTRAST 70470 CT HEAD/BRAIN W/O & W/ CONTRAST
 CPT CODE PROCEDURE DESCRIPTION CT Scans 70450 CT HEAD/BRAIN W/O CONTRAST 70460 CT HEAD/BRAIN W/ CONTRAST 70470 CT HEAD/BRAIN W/O & W/ CONTRAST 70480 CT ORBIT W/O CONTRAST 70481 CT ORBIT W/ CONTRAST 70482
CPT CODE PROCEDURE DESCRIPTION CT Scans 70450 CT HEAD/BRAIN W/O CONTRAST 70460 CT HEAD/BRAIN W/ CONTRAST 70470 CT HEAD/BRAIN W/O & W/ CONTRAST 70480 CT ORBIT W/O CONTRAST 70481 CT ORBIT W/ CONTRAST 70482
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Diagnostic performance of MRI in differentiating metastatic from acute osteoporotic compression fractures of the spine
 Diagnostic performance of MRI in differentiating metastatic from acute osteoporotic compression fractures of the spine Poster No.: C-1399 Congress: ECR 2013 Type: Scientific Exhibit Authors: J. Martel,
Diagnostic performance of MRI in differentiating metastatic from acute osteoporotic compression fractures of the spine Poster No.: C-1399 Congress: ECR 2013 Type: Scientific Exhibit Authors: J. Martel,
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease)
 Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
Lytic Lesions of Bone: A Histopathological and Radiological Correlative Study
 Academic Medical Journal of India 83 Volume III - Issue 3 www.medicaljournal.in July - September 2015 ORIGINAL RESEARCH Lytic Lesions of Bone: A Histopathological and Radiological Correlative Study Lilarani
Academic Medical Journal of India 83 Volume III - Issue 3 www.medicaljournal.in July - September 2015 ORIGINAL RESEARCH Lytic Lesions of Bone: A Histopathological and Radiological Correlative Study Lilarani
PET/CT in Lymphoma. Ur Metser, M.D. Division Head, Molecular Imaging Joint Department of Medical Imaging, UHN- MSH- WCH University of Toronto
 PET/CT in Lymphoma Ur Metser, M.D. Division Head, Molecular Imaging Joint Department of Medical Imaging, UHN- MSH- WCH University of Toronto Outline 1. Introduction: PET/CT, how does it work? 2.Current
PET/CT in Lymphoma Ur Metser, M.D. Division Head, Molecular Imaging Joint Department of Medical Imaging, UHN- MSH- WCH University of Toronto Outline 1. Introduction: PET/CT, how does it work? 2.Current
New Hampshire Childhood Cancer
 Introduction: New Hampshire Childhood Cancer New Hampshire, Childhood Cancer, January 2009 Issue Brief Cancer in children is relatively uncommon, impacting fewer than twenty two of every 100,000 children
Introduction: New Hampshire Childhood Cancer New Hampshire, Childhood Cancer, January 2009 Issue Brief Cancer in children is relatively uncommon, impacting fewer than twenty two of every 100,000 children
Diagnostic Accuracy of Sonographic Criteria for Evaluation of Cervical Lymphadenopathy
 Diagnostic Accuracy of Sonographic Criteria for Evaluation of Cervical Lymphadenopathy Michael Ying, MPhil, Anil Ahuja, FRCR, Constantine Metreweli, FRCR Although ultrasonographic criteria for abnormal
Diagnostic Accuracy of Sonographic Criteria for Evaluation of Cervical Lymphadenopathy Michael Ying, MPhil, Anil Ahuja, FRCR, Constantine Metreweli, FRCR Although ultrasonographic criteria for abnormal
NEOPLASMS C00 D49. Presented by Jan Halloran CCS
 NEOPLASMS C00 D49 Presented by Jan Halloran CCS 1 INTRODUCTION A neoplasm is a new or abnormal growth. In the ICD-10-CM classification system, neoplastic disease is classified in categories C00 through
NEOPLASMS C00 D49 Presented by Jan Halloran CCS 1 INTRODUCTION A neoplasm is a new or abnormal growth. In the ICD-10-CM classification system, neoplastic disease is classified in categories C00 through
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Approach to Lower Extremity Osteomyelitis. A radiologic tour of a patient encounter
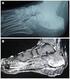 Approach to Lower Extremity Osteomyelitis A radiologic tour of a patient encounter David Guo,, HMS III Gillian Lieberman, MD BIDMC, October 2009 Our learning goals Review lower extremity anatomy Discuss
Approach to Lower Extremity Osteomyelitis A radiologic tour of a patient encounter David Guo,, HMS III Gillian Lieberman, MD BIDMC, October 2009 Our learning goals Review lower extremity anatomy Discuss
Disclosures for Elena Zamagni
 Prognostic relevance of 18F-FDG PET/CT in newly diagnosed multiple myeloma patients receiving upfront autologous stem-cell transplantation: a prospective study Zamagni E. 1, Nanni C. 2, Patriarca F. 3,
Prognostic relevance of 18F-FDG PET/CT in newly diagnosed multiple myeloma patients receiving upfront autologous stem-cell transplantation: a prospective study Zamagni E. 1, Nanni C. 2, Patriarca F. 3,
Spatial mismatch in CT-defined vs. NaF PET-defined lesions: implications for diagnostic bone biopsies
 Spatial mismatch in CT-defined vs. NaF PET-defined lesions: implications for diagnostic bone biopsies Stephanie Harmon, Song Chen, Peter Ferjancic, Timothy Perk, Michael Tuite, and Robert Jeraj University
Spatial mismatch in CT-defined vs. NaF PET-defined lesions: implications for diagnostic bone biopsies Stephanie Harmon, Song Chen, Peter Ferjancic, Timothy Perk, Michael Tuite, and Robert Jeraj University
Multi-slice Helical CT Scanning of the Chest
 Multi-slice Helical CT Scanning of the Chest Comparison of different low-dose acquisitions Lung cancer is the main cause of deaths due to cancer in human males and the incidence is constantly increasing.
Multi-slice Helical CT Scanning of the Chest Comparison of different low-dose acquisitions Lung cancer is the main cause of deaths due to cancer in human males and the incidence is constantly increasing.
Primary Extradural Tumours and Metastasis of the Spine. Cody Bünger Spine Center/Sarcoma Center Aarhus University Hospital, Aarhus Sygehus Denmark
 Primary Extradural Tumours and Metastasis of the Spine Cody Bünger Spine Center/Sarcoma Center Aarhus University Hospital, Aarhus Sygehus Denmark Klassifikation af ekstradurale spinale tumorer Benigne
Primary Extradural Tumours and Metastasis of the Spine Cody Bünger Spine Center/Sarcoma Center Aarhus University Hospital, Aarhus Sygehus Denmark Klassifikation af ekstradurale spinale tumorer Benigne
.org. Osteochondroma. Solitary Osteochondroma
 Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
HERC Coverage Guidance Advanced Imaging for Staging of Prostate Cancer Disposition of Public Comments
 Table of Contents Commenters... 1 Public Comments... 2 References Provided by Commenters... 6 Commenters Identification Stakeholder A Medical Imaging & Technology Alliance (MITA), Arlington, VA [Submitted
Table of Contents Commenters... 1 Public Comments... 2 References Provided by Commenters... 6 Commenters Identification Stakeholder A Medical Imaging & Technology Alliance (MITA), Arlington, VA [Submitted
BEYOND 18 F-FDG: INTRODUCTION TO NEW RADIOPHARMACEUTICALS
 BEYOND F-FDG: INTRODUCTION TO NEW RADIOPHARMACEUTICALS Asti Mattia Nuclear Medicine Department Santa Maria Nuova Hospital, Reggio Emilia, Italy SUMMARY: F-Labelled Choline analogues. Comparison between
BEYOND F-FDG: INTRODUCTION TO NEW RADIOPHARMACEUTICALS Asti Mattia Nuclear Medicine Department Santa Maria Nuova Hospital, Reggio Emilia, Italy SUMMARY: F-Labelled Choline analogues. Comparison between
Innovative RT SBRT. The variables with REQ in superscript are required.
 The variables with REQ in superscript are required. The variables with a are single-select variables; only one answer can be selected. The variables with a are multi-select variables; multiple answers
The variables with REQ in superscript are required. The variables with a are single-select variables; only one answer can be selected. The variables with a are multi-select variables; multiple answers
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA
 KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
KIDNEY FUNCTION RELATION TO SIZE OF THE TUMOR IN RENAL CELL CANCINOMA O.E. Stakhvoskyi, E.O. Stakhovsky, Y.V. Vitruk, O.A. Voylenko, P.S. Vukalovich, V.A. Kotov, O.M. Gavriluk National Canсer Institute,
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT
 1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Information Pathway. Myeloma tests and investigations. Paraprotein measurement
 Information Pathway Myeloma UK Broughton House 31 Dunedin Street Edinburgh EH7 4JG Tel: + 44 (0) 131 557 3332 Fax: + 44 (0) 131 557 9785 Myeloma Infoline 0800 980 3332 www.myeloma.org.uk Charity No. SC
Information Pathway Myeloma UK Broughton House 31 Dunedin Street Edinburgh EH7 4JG Tel: + 44 (0) 131 557 3332 Fax: + 44 (0) 131 557 9785 Myeloma Infoline 0800 980 3332 www.myeloma.org.uk Charity No. SC
Thomas de los Reyes PGY 1 Department of Urologic Sciences University of British Columbia. Meet Mr. S
 Thomas de los Reyes PGY 1 Department of Urologic Sciences University of British Columbia Meet Mr. S 74 M admitted for back pain X-ray: sclerotic lesions along spine PSA 800 Nuclear Medicine Bone Scan 1
Thomas de los Reyes PGY 1 Department of Urologic Sciences University of British Columbia Meet Mr. S 74 M admitted for back pain X-ray: sclerotic lesions along spine PSA 800 Nuclear Medicine Bone Scan 1
Locoregional recurrence or persistence of papillary carcinoma: radioiodine treatment
 Locoregional recurrence or persistence of papillary carcinoma: radioiodine treatment Michele Klain, Marco Salvatore Department of Functional and Biomorphological Science University of Naples "Federico
Locoregional recurrence or persistence of papillary carcinoma: radioiodine treatment Michele Klain, Marco Salvatore Department of Functional and Biomorphological Science University of Naples "Federico
Introduction: Tumor Swelling / new growth / mass. Two types of growth disorders: Non-Neoplastic. Secondary / adaptation due to other cause.
 Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Variations in PET/CT Methodology for Oncologic Imaging at U.S. Academic Medical Centers: An Imaging Response Assessment Team Survey
 Variations in PET/CT Methodology for Oncologic Imaging at U.S. Academic Medical Centers: An Imaging Response Assessment Team Survey Michael M. Graham 1, Ramsey D. Badawi 2, and Richard L. Wahl 3 1 University
Variations in PET/CT Methodology for Oncologic Imaging at U.S. Academic Medical Centers: An Imaging Response Assessment Team Survey Michael M. Graham 1, Ramsey D. Badawi 2, and Richard L. Wahl 3 1 University
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
First floor, Main Hospital North Services provided 24/7 365 days per year
 First floor, Main Hospital North Services provided 24/7 365 days per year General Radiology (X-ray) Fluoroscopy Ultrasound (Sonography) Nuclear Medicine P.E.T. imaging Computed Tomography (CT scan) Magnetic
First floor, Main Hospital North Services provided 24/7 365 days per year General Radiology (X-ray) Fluoroscopy Ultrasound (Sonography) Nuclear Medicine P.E.T. imaging Computed Tomography (CT scan) Magnetic
Aggressive vs. nonaggressive bone lesions. Anthony Pease, DVM, MS, DACVR
 Aggressive vs. nonaggressive bone lesions Anthony Pease, DVM, MS, DACVR The evaluation of the musculoskeletal system is difficult due to the numerous soft tissues as well as the bone structures involved.
Aggressive vs. nonaggressive bone lesions Anthony Pease, DVM, MS, DACVR The evaluation of the musculoskeletal system is difficult due to the numerous soft tissues as well as the bone structures involved.
AI CPT Codes. x x. 70336 MRI Magnetic resonance (eg, proton) imaging, temporomandibular joint(s)
 Code Category Description Auth Required Medicaid Medicare 0126T IMT Testing Common carotid intima-media thickness (IMT) study for evaluation of atherosclerotic burden or coronary heart disease risk factor
Code Category Description Auth Required Medicaid Medicare 0126T IMT Testing Common carotid intima-media thickness (IMT) study for evaluation of atherosclerotic burden or coronary heart disease risk factor
LUNG CANCER SCREENING: UNDERSTANDING LUNG NODULES. 1-800-298-2436 LungCancerAlliance.org
 LUNG CANCER SCREENING: UNDERSTANDING LUNG NODULES 1-800-298-2436 LungCancerAlliance.org 1 1 CONTENTS What is a Nodule?...3 Finding Nodules...4 If a Nodule Is Found...5 What Happens Next?...7 Questions
LUNG CANCER SCREENING: UNDERSTANDING LUNG NODULES 1-800-298-2436 LungCancerAlliance.org 1 1 CONTENTS What is a Nodule?...3 Finding Nodules...4 If a Nodule Is Found...5 What Happens Next?...7 Questions
Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine
 Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Douglas Van Nostrand, MD, FACP, FACNM Director, Nuclear Medicine
Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Salute to Dr. Saul Hertz Diagnostic and Therapeutic Uses of Radioiodine Douglas Van Nostrand, MD, FACP, FACNM Director, Nuclear Medicine
Post-PET Restaging Cancer Form National Oncologic PET Registry
 Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Post-PET Restaging Cancer Form National Oncologic PET Registry Facility ID #: Registry Case Number: Patient Name: Your patient had a PET scan on: mm/dd/yyyy. The PET scan was done for restaging of (cancer
Leukemias and Lymphomas: A primer
 Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
The Ontario Cancer Registry moves to the 21 st Century
 The Ontario Cancer Registry moves to the 21 st Century Rebuilding the OCR Public Health Ontario Grand Rounds Oct. 14, 2014 Diane Nishri, MSc Mary Jane King, MPH, CTR Outline 1. What is the Ontario Cancer
The Ontario Cancer Registry moves to the 21 st Century Rebuilding the OCR Public Health Ontario Grand Rounds Oct. 14, 2014 Diane Nishri, MSc Mary Jane King, MPH, CTR Outline 1. What is the Ontario Cancer
Intensity-Modulated Radiation Therapy (IMRT)
 Scan for mobile link. Intensity-Modulated Radiation Therapy (IMRT) Intensity-modulated radiotherapy (IMRT) uses linear accelerators to safely and painlessly deliver precise radiation doses to a tumor while
Scan for mobile link. Intensity-Modulated Radiation Therapy (IMRT) Intensity-modulated radiotherapy (IMRT) uses linear accelerators to safely and painlessly deliver precise radiation doses to a tumor while
An Update on Lung Cancer Diagnosis
 An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
The Di Bella Method (DBM) improves Survival, Objective Response and Performance Status in Breast Cancer
 BIT's 4th World Cancer Congress 2011 People s Republic of China Dalian The Di Bella Method (DBM) improves Survival, Objective Response and Performance Status in treated with DBM therapy Retrospective observational
BIT's 4th World Cancer Congress 2011 People s Republic of China Dalian The Di Bella Method (DBM) improves Survival, Objective Response and Performance Status in treated with DBM therapy Retrospective observational
Positron Emission Tomography - For Patients
 Positron Emission Tomography - For Patients A physician s written order is required for any PET-CT tests. How should I prepare for my PET-CT? PET-CT is more complicated than most other tests you may be
Positron Emission Tomography - For Patients A physician s written order is required for any PET-CT tests. How should I prepare for my PET-CT? PET-CT is more complicated than most other tests you may be
Case Number: RT2009-124(M) Potential Audiences: Intent Doctor, Oncology Special Nurse, Resident Doctor
 Renal Cell Carcinoma of the Left Kidney Post Radical Surgery with pt4 Classification with Multiple Lung and Single Brain Metastases: the Role and Treatment Consideration of Radiotherapy Case Number: RT2009-124(M)
Renal Cell Carcinoma of the Left Kidney Post Radical Surgery with pt4 Classification with Multiple Lung and Single Brain Metastases: the Role and Treatment Consideration of Radiotherapy Case Number: RT2009-124(M)
SPECT/CT Wrist. Wrist pain 3/27/2012
 Wrist pain Wrist joint - complicated anatomy complex biomechanics Imaging and management of wrist pain presents a significant challenge Significant economic burden SPECT/CT Wrist HK Mohan GSTT London Intra-capsular
Wrist pain Wrist joint - complicated anatomy complex biomechanics Imaging and management of wrist pain presents a significant challenge Significant economic burden SPECT/CT Wrist HK Mohan GSTT London Intra-capsular
PET Coding & Coverage: Including NOPR Sequel April 27, 2009. Presented by: Denise A. Merlino, MBA, CNMT, FSNMTS,CPC. Agenda
 Presented by: Barry Siegel, MD Mallinckrodt Institute of Radiology PET Coding & Coverage: Including NOPR Sequel April 27, 2009 Presented by: Denise A. Merlino, MBA, CNMT, FSNMTS,CPC President, Merlino
Presented by: Barry Siegel, MD Mallinckrodt Institute of Radiology PET Coding & Coverage: Including NOPR Sequel April 27, 2009 Presented by: Denise A. Merlino, MBA, CNMT, FSNMTS,CPC President, Merlino
UNDERSTANDING SERIES LUNG NODULES. 1-800-298-2436 LungCancerAlliance.org
 UNDERSTANDING SERIES LUNG NODULES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Nodule?...2 Finding Nodules...3 If a Nodule is Found... 4 What Happens Next?...6 Questions to Ask about Your Results...7
UNDERSTANDING SERIES LUNG NODULES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Nodule?...2 Finding Nodules...3 If a Nodule is Found... 4 What Happens Next?...6 Questions to Ask about Your Results...7
Multiple Myeloma with Pathologic Fracture: the Role and Treatment Consideration of RT
 Multiple Myeloma with Pathologic Fracture: the Role and Treatment Consideration of RT Case Number: RT2009-37(M) Potential Audiences: Intent Doctor, Oncology Special Nurse, Resident Doctor Purpose: to present
Multiple Myeloma with Pathologic Fracture: the Role and Treatment Consideration of RT Case Number: RT2009-37(M) Potential Audiences: Intent Doctor, Oncology Special Nurse, Resident Doctor Purpose: to present
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
Something Old, Something New.
 Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Molecular Imaging in Early Phase Oncology Trials
 Molecular Imaging in Early Phase Oncology Trials Lessons Learned Potential Role for SNM Network Susan Galbraith MB BChir PhD Vice-President Oncology Discovery Medicine & Clinical Biomarkers Bristol-Myers
Molecular Imaging in Early Phase Oncology Trials Lessons Learned Potential Role for SNM Network Susan Galbraith MB BChir PhD Vice-President Oncology Discovery Medicine & Clinical Biomarkers Bristol-Myers
PET (FDG) Scan for Solid Tumors PET (FDG) SCAN FOR SOLID TUMORS HS-112. Policy Number: HS-112. Original Effective Date: 6/18/2009
 Easy Choice Health Plan, Inc. Exactus Pharmacy Solutions, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Incorporated WellCare Health Insurance of Arizona, Inc., operating in Hawai i as Ohana
Easy Choice Health Plan, Inc. Exactus Pharmacy Solutions, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Incorporated WellCare Health Insurance of Arizona, Inc., operating in Hawai i as Ohana
MRI of Bone Marrow Radiologic-Pathologic Correlation
 MRI of Bone Marrow Radiologic-Pathologic Correlation Marilyn J. Siegel, M.D. Mallinckrodt Institute of Radiology Washington University School of Medicine St. Louis, MO and Visiting Scientist, AFIP, Washington,
MRI of Bone Marrow Radiologic-Pathologic Correlation Marilyn J. Siegel, M.D. Mallinckrodt Institute of Radiology Washington University School of Medicine St. Louis, MO and Visiting Scientist, AFIP, Washington,
