Eastern Suburbs Sports Medicine Centre
|
|
|
- Sheryl Barrett
- 10 years ago
- Views:
Transcription
1 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation program is our current regime and is based upon current clinical information regarding open and closed chain exercise, early mobilisation, progressive controlled loading of the knee joint and years of experience in returning people back to their previous level of sport or recreation. The time frame stated in this program should be flexible and act only as a guide. Progression should be based on an individual basis. Factors that may influence expectations of progression include the patient s age, their attitude to exercise and associated pathology including meniscal, chondral and other ligamentous damage. Copyright 2002
2 STAGE ONE - ACUTE POST OP Time Frame 0-2 weeks Goals 1. Wound healing (sutures removed approximately day 10). 2. Reduce post operative pain and swelling. 3. Regain full extension. 4. Full weight bearing. 5. Wean off crutches and normalise gait. 6. Promote muscle control. Treatment Guidelines 1. Pain and swelling reduction with ice, intermittent pressure pump, soft tissue massage and exercise. 2. Patella mobilisation. 3. Active range of motion of the knee joint, calf and gentle hamstring stretching, co-contraction (non weight bearing progressing to standing) to aid in re-gaining range of movement, muscle control and full weight bearing. Aim for full extension within two weeks. Full flexion will take longer and will generally steadily improve without the effort of focal heavy stretching. 2
3 Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright Gait retraining encouraging extension at heel strike. Full weight bearing is encouraged. nb. As hamstring strains and pain are common in the first six weeks, care needs to be taken with the intensity of hamstring activation on cocontraction exercises. Over emphasis of hamstring contraction may lead to hamstring strain at this stage. Light hamstring loading continues into the next stage with progression of general rehabilitation. Resisted hamstring loading should be avoided until approximately week six. STAGE TWO - QUADRICEPS CONTROL Time frame weeks approx. Goals 1. Full active range of movement 2. Normal gait with reasonable weight bearing tolerance 3. Minimal pain and effusion 4. Develop muscular control for a controlled pain free single leg lunge 5. Avoid hamstring strain 6. Develop early proprioceptive awareness Treatment Guidelines 1. Use active, passive and hands on techniques to promote full range of movement. 3
4 Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright Progress closed chain exercise (quarter squats and single leg lunge) as pain allows. The emphasis is on pain free loading, VMO and gluteal activation. 3. Introduce gym based exercise equipment including leg press and stationary cycle. 4. Once the wound has healed water based exercise can begin. This can include wading, bicycle action in the water, simple range of motion and gentle swimming (no breastroke). 5. Begin proprioception exercises including single standing leg balance on the ground and on the mini-tramp. This can be progressed by introducing body movement whilst standing on one leg. 6. Develop a calf routine including bilateral progressing to single calf raise and stretching. 7. Refrain from isolated loading of the hamstrings (due to ease of tear). Hamstrings will be progressively loaded through closed chain and also gym based activity. STAGE THREE - HAMSTRING/QUADRICEPS STRENGTHENING Time Frame weeks Goals 1. To begin specific hamstring loading. 2. Increase total leg strength. 4
5 Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright Promote good quadriceps control in lunge and hopping activity in preparation for running. Treatment Guidelines 1. Focal hamstring loading begins and is progressed steadily throughout the next stages of rehabilitation. a. Active prone knee flexion which can be quickly progressed to include a light weight and then gradually progressed by increasing the weight. b. Bilateral bridging off a chair. This can be progressed by moving onto a single leg bridge and then single leg bridge with weight held across the abdomen. c. Single straight leg dead lift initially active and then can be made more difficult by adding dumb bell weights. A key point with hamstring loading is that it is never pushed into pain and volumes and intensities are carefully progressed. Any minor setback of subtle strain or tightness post exercise should be managed with a downgrading of hamstring based exercises. 2. Gym based activity including leg press, light squats and stationery bike can be progressively increased in intensity as pain and control allow. It is important to detect and avoid effusion post exercise. Any effusion that is exacerbated with exercise should signal a reduction of training intensity. Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright
6 3. Once single leg lunge control is good comparable to the other side hopping can be introduced. Hops can be made more difficulty by including variation such as forwards/back, side to side off a step and in a quadrant. 4. Running may begin towards the latter part of this stage. Certain criteria must be met prior to the onset of running. These include: a. No anterior knee pain. b. A pain free lunge and hop that is comparable in control to the other side. c. The knee also must have no effusion. Jogging should begin with a walk/jog. Ideally, this is done on a treadmill to monitor landing action and also to carefully monitor effusion post exercise. Again, any increase in effusion following jogging should be met in a reduction in training intensity. Walk/jogging should be attempted for 2-3 times per week for 1-2 weeks before progressing onto jogging alone. 5. Proprioception exercises are made more difficult with more aggressive manoeuvres in standing leg balance and also by progressing hopping based activity. 6. Expand calf routine to include eccentric loading. Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright
7 STAGE FOUR - SPORTS SPECIFIC Time Frame months Goals 1. Increase total leg strength. 2. Develop running endurance speed, change of direction. 3. Advanced proprioception. 4. Preparing for a return to sport and recreational lifestyle. Treatment Guidelines 1. These activities should build in intensity and volume over this time frame. Controlled sport specific activities should be included in the progression of running and gym loads through this time frame. Increasing effusion post running that isn t easily managed with ice should result in a reduction of running loads. 2. Advanced proprioception to include controlled hopping and turning and balance correction. 3. Continue to increase intensity with training loads of gym based exercise programme. 4. Monitor potential problems associated with increasing loads. 5. No open chain resisted leg extension unless authorised by your surgeon. Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright
8 STAGE FIVE - RETURN TO SPORT Time Frame - 6 months plus Goals 1. A safe return to sport and normal recreational lifestyle. Treatment Guidelines 1. Full training for 1 month prior to active return to competitive sport. 2. Preparation for body contact sports. Begin with low intensity one on one contests and progress by increasing intensity and complexity in preparation for drills that one might be expected to do at training. 3. To develop running endurance as to be able to handle a normal training session. 4. Full range, no effusion, good quadriceps control for lunge, hopping and hop and turn type activity. Circumference measures of thigh and calf to within 1cm of the other side. 002 Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright 2 8
9 POTENTIAL PROBLEMS 1. Infection. The patient may complain in the acute post op period of significantly increased pain (constant throbbing in nature), fever and be generally unwell. The knee may present with increased swelling and demonstrate heat. The surgeon should be contacted immediately. 2. Deep venous thrombosis. Increased swelling, tenderness to palpation and pain particularly in the calf may be signs of a DVT. Again, this should be assessed immediately by the surgeon. 3. Functional instability. Poor quadriceps control and too early removal of crutch usage may result in the patient feeling that their knee gives way or feels unstable. This is not related to a structural instability but rather a lack of quadriceps control due to pain and swelling associated with the surgery. 4. Hamstring strain and pain. As hamstring tendons (semi-tendinosisn and gracilis) are utilised as a graft donor site, hamstring soreness is typical in the acute post op period. Over zealous rehabilitation and daily activity can lead to hamstring strain which can delay progression and require modification of rehabilitation. 5. Poor range of motion. Current surgical techniques usually allow for relatively quick restoration to full range of movement. Fortunately, arthrofibrosis is quite rare. Delaying surgery for several weeks following initial injury can reduce the risk of arthrofibrosis. Regaining full extension and muscle control in end range of extension is a priority early in rehabilitation. This is essential in the restoration of a normal gait. Exercise, calf and hamstring stretching, gentle extension stretches, soft tissue techniques and patella mobilisation will promote full extension. Flexion will usually progress with rehabilitation and only require to be pushed in later stages if full flexion has not been restored. Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright
10 6. Recurring effusion. Persistent or recurring joint swelling may be a problem through the midlate stages of rehabilitation. Typically, it may happen in those patients who have had meniscal and/or chondral pathology or those who spend long periods in standing. It is also common with significant progressions in running and training intensity. Anti-inflammatory medication and ice following rehab can also be useful strategies to manage a persistent effusion. A cautious approach to rehab and running progression is also essential. 7. Anterior knee pain. This can be a problem at any stage through rehabilitation. Poor VMO, too rapid progression of closed chain exercise, over zealous daily activity, abnormal gait (flexed knee at heel strike), too early return or too sudden progression of running loads may overload the patellofemoral joint and/or patella tendon and cause irritation. 8. Poor landing mechanism. Patients with reduced quadriceps control on lunging and hopping activity (reduced knee flexion on landing) are not ready to resume running and doing so usually results in altered running action causing joint soreness and potentially patella tendonitis or patellofemoral pain. 9. Graft failure. Graft failure can occur. The risk of graft failure should not prevent a person from returning to their pre-injury level of sport or activity once full function of their knee is restored. Eastside Physiotherapy, 160 Belmore Road, Randwick NSW 2031 Ph (02) , Fax (02) Copyright
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI MR GREG CRIAG MR IAN COLLIER DECEMBER, 2004 INTRODUCTION Anterior cruciate ligament reconstruction
AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI MR GREG CRIAG MR IAN COLLIER DECEMBER, 2004 INTRODUCTION Anterior cruciate ligament reconstruction
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
Hip Arthroscopy Post-operative Rehabilitation Protocol
 Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Non-Operative Protocol
 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL Rehabilitation Protocol
 ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1
 Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt
 Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
Post Surgery Rehabilitation Program for Knee Arthroscopy
 Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Rehabilitation After ACL Reconstruction
 CENTRE PERTH ORTHOPAEDIC & SPORTS MEDICINE Rehabilitation After ACL Reconstruction Dr Keith Holt Philosophy of Rehabilitation Rehabilitation, as it applies to the recovery period from Orthopaedic Surgery,
CENTRE PERTH ORTHOPAEDIC & SPORTS MEDICINE Rehabilitation After ACL Reconstruction Dr Keith Holt Philosophy of Rehabilitation Rehabilitation, as it applies to the recovery period from Orthopaedic Surgery,
Rehabilitation Programme following Hip Arthroscopy
 Rehabilitation Programme following Hip Arthroscopy Updated May 2010 Hip Arthroscopy Patient information and rehabilitation programme: The Hip Joint The hip is a ball-and-socket joint and is the largest
Rehabilitation Programme following Hip Arthroscopy Updated May 2010 Hip Arthroscopy Patient information and rehabilitation programme: The Hip Joint The hip is a ball-and-socket joint and is the largest
Rehabilitation of Sports Hernia
 Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Strength Training for the Knee
 Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
ChondroCelect Rehabilitation Program
 ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Rehabilitation after ACL Reconstruction: From the OR to the Playing Field. Mark V. Paterno PT, PhD, MBA, SCS, ATC
 Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
Meniscus Repair Rehabilitation Dr. Walter R. Lowe
 Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Steps to Success: A Guide to Knee Rehabilitation
 Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
A Patient s Guide to ACL Reconstruction Surgery
 Mr. Vikas Vedi, BSc(Hons), MBBS, FRCS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon A Patient s Guide to ACL Reconstruction Surgery Bishops Wood Hospital Rickmansworth Road Northwood Middlesex HA6 2JW
Mr. Vikas Vedi, BSc(Hons), MBBS, FRCS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon A Patient s Guide to ACL Reconstruction Surgery Bishops Wood Hospital Rickmansworth Road Northwood Middlesex HA6 2JW
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
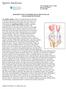 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes
 Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Dr. O Meara s. Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com
 Dr. O Meara s Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol Hamstring Stretching & Strengthening
Dr. O Meara s Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol Hamstring Stretching & Strengthening
GALLAND/KIRBY INTERVAL DISTANCE RUNNING REHABILITATION PROGRAM
 GALLAND/KIRBY INTERVAL DISTANCE RUNNING REHABILITATION PROGRAM PHASE I: WALKING PROGRAM Must be able to walk, pain free, aggressively (roughly 4.2 to 5.2 miles per hour), preferably on a treadmill, before
GALLAND/KIRBY INTERVAL DISTANCE RUNNING REHABILITATION PROGRAM PHASE I: WALKING PROGRAM Must be able to walk, pain free, aggressively (roughly 4.2 to 5.2 miles per hour), preferably on a treadmill, before
Hip Bursitis/Tendinitis
 Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities
 Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
ACL Reconstruction Protocol
 ACL Reconstruction Protocol The primary emphasis of this ACL rehab protocol is on functional weight bearing exercises with a focus on restoring the balance between the quadriceps and hamstrings muscles,
ACL Reconstruction Protocol The primary emphasis of this ACL rehab protocol is on functional weight bearing exercises with a focus on restoring the balance between the quadriceps and hamstrings muscles,
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees
 Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Post Surgery Rehabilitation Program
 Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
ACL Reconstruction Rehabilitation Protocol
 Peter J. Millett, MD, MSc The Steadman Clinic Vail, CO www.drmillett.com Table of Contents Preoperative Rehabilitation Phase...3 Understanding Surgery...7 Postoperative Days 1-7...8 Postoperative Days
Peter J. Millett, MD, MSc The Steadman Clinic Vail, CO www.drmillett.com Table of Contents Preoperative Rehabilitation Phase...3 Understanding Surgery...7 Postoperative Days 1-7...8 Postoperative Days
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
The Guide to Rehabilitation of Anterior Cruciate Ligament (ACL) Reconstruction
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road, Chester, CH4 7QP, Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road, Chester, CH4 7QP, Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Rehabilitation Guidelines for Autologous Chondrocyte Implantation. Ashley Conlin, PT, DPT, SCS, CSCS
 Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Recent Injuries. www.physiofirst.org.uk
 Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Ira K. Evans, M.D. Sports Medicine North Orthopedic Specialty Center One Orthopedics Drive Peabody, MA 01960. www.sportsmednorth.
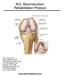 ACL Reconstruction Rehabilitation Protocol Ira K. Evans, M.D. Sports Medicine North Orthopedic Specialty Center One Orthopedics Drive Peabody, MA 01960 [email protected] Tel: (978) 818-6350 Fax: (978)
ACL Reconstruction Rehabilitation Protocol Ira K. Evans, M.D. Sports Medicine North Orthopedic Specialty Center One Orthopedics Drive Peabody, MA 01960 [email protected] Tel: (978) 818-6350 Fax: (978)
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
ORTHOPAEDIC KNEE CONDITIONS AND INJURIES
 11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
www.noc.nhs.uk ACL Reconstruction Information for Patients Delivering Excellence Hip and Knee service
 www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
FRONT PAGE HEADING. AFTER INJURY PRACTICAL GUIDELINES Janine Gray BSc (Physio), BSc (Med)(Hons) Exercise Science) MAIN HEADING.
 FRONT PAGE HEADING MAIN HEADING Sub Headings Body Copy Body Copy + Bold Body Copy + Bold + Italic Body Copy + Normal + Italic PHASES Style Body for tables OF REHABILITATION STYLE HEADING FOR TABLES AFTER
FRONT PAGE HEADING MAIN HEADING Sub Headings Body Copy Body Copy + Bold Body Copy + Bold + Italic Body Copy + Normal + Italic PHASES Style Body for tables OF REHABILITATION STYLE HEADING FOR TABLES AFTER
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY
 B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
Sports Injury Treatment
 Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Hip Arthroscopy Labral Repair Rehabilitation Protocol
 Hip Arthroscopy Labral Repair Rehabilitation Protocol PHASE 1: INITIAL Diminish pain and inflammation Protect integrity of repaired tissue Prevent muscular inhibition Restore ROM within the restrictions
Hip Arthroscopy Labral Repair Rehabilitation Protocol PHASE 1: INITIAL Diminish pain and inflammation Protect integrity of repaired tissue Prevent muscular inhibition Restore ROM within the restrictions
What is Osteoarthritis? Who gets Osteoarthritis? What can I do when I am diagnosed with Osteoarthritis? What can my doctor do to help me?
 Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Post-Operative Exercise Program
 785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
After Hip Arthroscopy
 After Hip Arthroscopy On your road to recovery... Rehabilitation is essential to help you return to an active life and reach your personal goals. This booklet provides goals, activities and milestones
After Hip Arthroscopy On your road to recovery... Rehabilitation is essential to help you return to an active life and reach your personal goals. This booklet provides goals, activities and milestones
Medial Collateral Ligament (MCL) Rehabilitation Protocol
 Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital
 By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
Rehabilitation After Knee Meniscus Repair
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Ankle Sprain. Information and Rehabilitation. Grade II. Grade I. Grade III
 514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
Today s session. Common Problems in Rehab. www.physiofitness.com.au/filex.htm LOWER BODY REHAB ESSENTIALS TIM KEELEY FILEX 2012
 Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist physiofitness.com.au facebook.com/physiofitness Today s session Essential list for the lower body Rehab starting point Focussing on activation,
Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist physiofitness.com.au facebook.com/physiofitness Today s session Essential list for the lower body Rehab starting point Focussing on activation,
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
