Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction
|
|
|
- Shanon Hodges
- 9 years ago
- Views:
Transcription
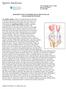
1 UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular joint. Joints are named for the two bones that articulate with each other. Most people think of the tibiofemoral joint when thinking of the knee. This is the joint that is primarily responsible for flexing (bending) and extending (straightening) of the knee. A small amount of rotation occurs at this joint as well. Ligaments are bundles of connective tissue that attach from bone to bone. There are four main ligaments that stabilize the knee. The collateral ligaments (medial and lateral) are on the inside and outside of the knee and provide side to side stability for the knee. The cruciate ligaments (anterior and posterior) are two large ligaments that cross in the middle of the knee and provide rotational stability and stability front to back. The posterior cruciate ligament is a large, broad ligament that attaches from the back of the tibia and travels forward as it moves up to attach to the femur (Figures 1 and 2). Its primary function is to resist posterior translation of the tibia on the femur, especially in flexion. It is also a secondary stabilizer for rotation and varus stability. Injuries of the posterior cruciate ligament (PCL) occur less frequently than those of the anterior cruciate ligament (ACL). The PCL is taught (tight) when the knee is in flexion, thus most PCL injuries occur in flexion. The most common cause of PCL tears (Figure 3) are sports injuries (37%) and trauma (56%). 1 In sports, the most common mechanism is falling on a flexed knee. In auto accidents, the most common mechanism is hitting the upper shin against the dashboard with the knee flexed during an accident (dashboard injury). Immediately after the injury it is common to have swelling in the knee, general knee pain and a loss of motion. 1 It is often difficult to predict the long term outcome of a PCL injury. 1 Some patients show significant symptoms and subsequent articular deterioration after a PCL injury, while others are essentially asymptomatic, maintaining normal function. 2 Evidence from randomized controlled trials to determine a single treatment of PCL injuries is lacking. Observational studies suggest that isolated PCL injuries may be treated conservatively, with good prognosis. Shelbourne treated 22 isolated grade 1 and grade 2 PCL injuries with extension bracing for six weeks. 3 In Shelbourne s study 19 of the 22 patients went on to show healing by MRI, and demonstrated stability. 3 Bracing is primarily effective when it can be started within one week of the injury. Surgical reconstruction is indicated in patients with PCL injuries that are Figure 1 Posterior (back) view of the knee with the PCL shaded in red combined with other ligament injuries in the knee (combination injuries or multi-ligamentous injuries), isolated grade 3 injuries or PCL injuries with chronic instability. Patients with chronic instability rarely suffer complete giving way episodes. More often it is a general sense of instability with pain in the front of their knee, especially with running or stair climbing. 1 Posterior laxity can be assessed with a posterior drawer test, the dial test or a KT1000 test, although laxity is not directly correlated to instability. Surgical reconstruction is done by replacing the torn PCL with a graft. This graft can be a single strand/ The health care team for the UW Badgers and proud sponsor of UW Athletics
2 bundle of tissue or two strands (double bundle). Grafts can be taken from areas of your own body (autograft), such as the patellar tendon, or from cadavers (allograft). To date there have not been significant differences in outcome studies comparing the various graft choices. 1 The grafts are placed and anchored in tunnels drilled in the femur and tibia. The rehabilitation process begins the first week after surgery. During the first four weeks the weight bearing and range of motion is limited to protect the healing of the graft. Hamstring exercises are also avoided because the hamstring pulls the tibia posteriorly (backward), which would cause stress to the healing graft. In phase 2 patients will begin to work more aggressively on strength and range of motion, usually discontinuing all use of the brace by six weeks. Prior to returning to sports, patients must regain strength, movement control, proprioception and force control. This often involves several months of progressive rehabilitation exercises. The rehabilitation guidelines below are presented in a criterion based progression. Specific time frames, restrictions and precautions are given to protect healing tissues and the surgical repair/reconstruction. General time frames are also given for reference to the average, but individual patients will progress at different rates depending on their age, associated injuries, pre-injury health status, rehab compliance and injury severity. Figure 2 Saggital PD MRI demonstrating a normal PCL Figure 3 Saggital T1 MRI demonstrating a torn PCL 2
3 PHASE I (Surgery to 4 weeks after surgery) Range of Motion s Progression Criteria Physician appointments: 1-2 weeks and 4-6 weeks after surgery Rehabilitation appointments begin 1-3 days after surgery, meet 2 times per week Protection of the post-surgical knee Restore normal knee extension Eliminate effusion Restore leg control Weight bearing as tolerated using pain and gait as guides Must wear the brace for all weight bearing activities Progress from locked to unlocked when patient has good quadriceps control Use axillary crutches for normal gait No open chain hamstring strengthening or isolated hamstring exercises. No hamstring stretching. No bike Follow range of motion guidelines Weeks 0-4: range of motion = full extension to 90 flexion Extension: Knee extension on a bolster, avoid prone hangs secondary to hamstring guarding Flexion: use gravity or assistance to minimize hamstring activity, such as supine wall slides or seated knee flexion Quadriceps sets Open chain knee extension against gravity Straight leg raises Leg lifts in standing with brace on for balance and hip strength avoid hip extension 2 to hamstring restrictions Upper body circuit training or upper body ergometer Patient may progress to Phase II if they have met the above stated goals and have Painfree gait using brace without crutches, No effusion Knee flexion to 90 3
4 PHASE II (begin after meeting Phase I criteria, usually at 5 weeks after surgery) Rage of Motion s Progression Criteria Physician appointment: 8-12 weeks after surgery Rehabilitation appointments are 1-2 times per week Single leg stand control Normalize gait Good control and no pain with functional movements, including step up/down, squat, partial lunge (keeping the knee in less than 60 of knee flexion) Discontinue brace over weeks 4-6 as the patient gains leg control and balance No open chain hamstring strengthening or isolated hamstring exercises. No hamstring stretching. No bike Follow range of motion guidelines no forced hyperflexion Weeks 5-6: range of motion = full extension to 120 flexion Gradually attain full flexion, avoiding forced flexion Extension: Knee extension on a bolster, avoid prone hangs secondary to hamstring guarding Flexion: use gravity or assistance to minimize hamstring activity, such as supine wall slides or seated knee flexion Quadriccps strengthening closed chain exercises short of 70 of knee flexion Non-impact balance and proprioceptive drills Gait drills Hip and core strengthening Stretching for patient specific muscle imbalances Upper body circuit training or upper body ergometer Patient may progress to Phase III if they have met the above stated goals and have Normal gait on all surfaces Ability to carry out functional movements without unloading affected leg and without pain, while demonstrating good control Single-leg balance greater than 15 seconds Full range of motion. 4
5 PHASE III (begin after meeting Phase II criteria, usually about weeks) Progression Criteria Physician appointment: 3 and 4 months after surgery Rehabilitation appointments are 1-2 times per week Good control and no pain with functional movements, including step up/down, squat and lunge Good control and no pain with light agility and low-impact multi-plane drills No open chain hamstring strengthening or isolated hamstring exercises. Quadriceps strengthening closed chain (progressing to multi-plane) and open chain exercises Non-impact balance and proprioceptive drills Impact control exercises beginning 2 feet to 2 feet, progressing from 1 foot to other and then 1 foot to same foot Movement control exercise beginning with low velocity, single-plane activities and progressing to higher velocity, multi-plane activities Hip and core strengthening Stretching for patient specific muscle imbalances Upper body circuit training or upper body ergometer Patient may progress to Phase IV if they have met the above stated goals and have Normal gait on all surfaces Ability to carry out multi-plane functional movements with out unloading affected leg or pain, while demonstrating good control Ability to land from a sagittal, frontal and transverse plane leap with good control and balance 5
6 PHASE IV (begin after meeting Phase III criteria, usually about 24 weeks) Return To Sport/Work Criteria Physician appointment: 6, 9 and 12 months after surgery Rehabilitation appointments are 1time per every 2-4 weeks Good dynamic neuromuscular control and no pain with sport and workspecific movements, including impact Post-activity soreness should resolve within 24 hours Avoid post-activity swelling Sport/work specific balance and proprioceptive drills Progress impact control exercises to reactive strengthening and plyometrics. Incorporate running program as appropriate Continue quadriceps strengthening Hip and core strengthening Stretching for patient specific muscle imbalances Replicate sport or work specific energy demands Dynamic neuromuscular control with multi-plane activities, without instability, pain or swelling These rehabilitation guidelines were developed collaboratively by Marc Sherry, PT, LAT, CSCS ([email protected]) and the UW Sports Medicine physician group. Updated 10/2013 References 1. Petrigliano FA, McAllister DR. Isolated posterior cruciate ligament injuries of the knee. Sports Med Arthrosc. Dec 2006;14(4): Peccin MS, Almeida GJ, Amaro J, Cohen M, Soares BG, Atallah AN. Interventions for treating posterior cruciate ligament injuries of the knee in adults. Cochrane Database Syst Rev. 2005(2):CD Shelbourne KD, Jennings RW, Vahey TN. Magnetic resonance imaging of posterior cruciate ligament injuries: assessment of healing. Am J Knee Surg. Fall 1999;12(4): Chhabra A, Kline AJ, Harner CD. Singlebundle versus double-bundle posterior cruciate ligament reconstruction: scientific rationale and surgical technique. Instr Course Lect. 2006;55: Christel P. Basic principles for surgical reconstruction of the PCL in chronic posterior knee instability. Knee Surg Sports Traumatol Arthrosc. Sep 2003;11(5): Margheritini F, Rihn J, Musahl V, Mariani PP, Harner C. Posterior cruciate ligament injuries in the athlete: an anatomical, biomechanical and clinical review. Sports Med. 2002;32(6): At UW Health, patients may have advanced diagnostic and /or treatment options, or may receive educational materials that vary from this information. Please be aware that this information is not intended to replace the care or advice given by your physician or health care provider. It is neither intended nor implied to be a substitute for professional advice. Call your health provider immediately if you think you may have a medical emergency. Always seek the advice of your physician or other qualified health provider prior to starting any new treatment or with any question you may have regarding a medical condition. Copyright 2013 UW Health Sports Medicine Center 6 SM
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Rehabilitation Guidelines for Lateral Ankle Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
How To Treat A Patella Dislocation
 Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
ACL Non-Operative Protocol
 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW Health Sports Rehabilitation Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW Health Sports Rehabilitation Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Platelet-Rich Plasma Rehabilitation Guidelines
 UW Health Sports Rehabilitation Platelet-Rich Plasma Rehabilitation Guidelines What is Tendinopathy? Tendons are strong bands of connective tissue comprised primarily of a substance called collagen. Mechanically,
UW Health Sports Rehabilitation Platelet-Rich Plasma Rehabilitation Guidelines What is Tendinopathy? Tendons are strong bands of connective tissue comprised primarily of a substance called collagen. Mechanically,
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair
 Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction
 1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
Physical Therapy Corner: Knee Injuries and the Female Athlete
 Physical Therapy Corner: Knee Injuries and the Female Athlete Knee injuries, especially tears of the anterior cruciate ligament, are becoming more common in female athletes. Interest in women s athletics
Physical Therapy Corner: Knee Injuries and the Female Athlete Knee injuries, especially tears of the anterior cruciate ligament, are becoming more common in female athletes. Interest in women s athletics
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt
 Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Rehabilitation after ACL Reconstruction: From the OR to the Playing Field. Mark V. Paterno PT, PhD, MBA, SCS, ATC
 Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEES A Physical Therapist s Perspective American Physical Therapy Association
 Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Evaluating Knee Pain
 Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Post Surgery Rehabilitation Program
 Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Strength Training for the Knee
 Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Medial Collateral Ligament (MCL) Rehabilitation Protocol
 Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Knee Kinematics and Kinetics
 Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Rehabilitation of Sports Hernia
 Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Rehabilitation Guidelines For SLAP Lesion Repair
 Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
Rehabilitation Guidelines For SLAP Lesion Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee. This is because the articular surface of
Rehabilitation Guidelines for Elbow Ulnar Collateral Ligament (UCL) Reconstruction
 Rehabilitation Guidelines for Elbow Ulnar Collateral Ligament (UCL) Reconstruction The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the
Rehabilitation Guidelines for Elbow Ulnar Collateral Ligament (UCL) Reconstruction The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the
Post Surgery Rehabilitation Program for Knee Arthroscopy
 Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine
 Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine Anterior Cruciate Ligament Injury Injury to the anterior cruciate ligament (ACL) is common, especially in athletic
Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine Anterior Cruciate Ligament Injury Injury to the anterior cruciate ligament (ACL) is common, especially in athletic
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
Rehabilitation Guidelines Following Proximal Hamstring Primary Repair
 Rehabilitation Guidelines Following Proximal Hamstring Primary Repair The hamstring muscle group consists of three muscles: the biceps femoris, semitendinosus and semimembranosus. All three of these muscles
Rehabilitation Guidelines Following Proximal Hamstring Primary Repair The hamstring muscle group consists of three muscles: the biceps femoris, semitendinosus and semimembranosus. All three of these muscles
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
Screening Examination of the Lower Extremities BUY THIS BOOK! Lower Extremity Screening Exam
 Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
AQUATIC/LAND BASED CLINICAL PROTOCOL FOR GRADE I/II MCL INJURY
 Frisbie Memorial Hospital Marsh Brook Rehabilitation Services Wentworth-Douglass Hospital AQUATIC/LAND BASED CLINICAL PROTOCOL FOR GRADE I/II MCL INJURY FREQUENCY: 2-3 times per week. DURATION: 4-6 weeks
Frisbie Memorial Hospital Marsh Brook Rehabilitation Services Wentworth-Douglass Hospital AQUATIC/LAND BASED CLINICAL PROTOCOL FOR GRADE I/II MCL INJURY FREQUENCY: 2-3 times per week. DURATION: 4-6 weeks
Preventing Knee Injuries in Women s Soccer
 Preventing Knee Injuries in Women s Soccer By Wayne Nelson, DC, CCRS The United States has recently seen a rapid increase in participation of young athletes with organized youth soccer leagues. As parents
Preventing Knee Injuries in Women s Soccer By Wayne Nelson, DC, CCRS The United States has recently seen a rapid increase in participation of young athletes with organized youth soccer leagues. As parents
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ACL Rehabilitation Protocol
 ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee.
 Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1
 Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Hip Bursitis/Tendinitis
 Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
What is Osteoarthritis? Who gets Osteoarthritis? What can I do when I am diagnosed with Osteoarthritis? What can my doctor do to help me?
 Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
Rehabilitation Guidelines for Shoulder Arthroscopy Front View Long head of bicep Acromion Figure 1 Shoulder anatomy Supraspinatus Image Copyright 2010 UW Health Sports Medicine Center. Short head of bicep
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING. Minni Titicula
 PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
Rehabilitation after ACL Reconstruction
 Rehabilitation after ACL Reconstruction John Nyland, DPT, EdD Artur Proniewicz, MD Paul Mazzone, BS Athletic Training Program Kosair Charities College of Health and Natural Sciences Spalding University,
Rehabilitation after ACL Reconstruction John Nyland, DPT, EdD Artur Proniewicz, MD Paul Mazzone, BS Athletic Training Program Kosair Charities College of Health and Natural Sciences Spalding University,
ORTHOPAEDIC KNEE CONDITIONS AND INJURIES
 11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
Rehabilitation. Modalities and Rehabilitation. Basics of Injury Rehabilitation. Injury Rehabilitation. Vocabulary. Vocabulary
 Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
PREVENTING ACL INJURIES IN SOCCER. By Brian Goodstein, MS, ATC, CSCS
 PREVENTING ACL INJURIES IN SOCCER By Brian Goodstein, MS, ATC, CSCS ACL injuries can be devastating to a soccer player s competitive season. For this reason, reputable medical institutions like the Cincinnati
PREVENTING ACL INJURIES IN SOCCER By Brian Goodstein, MS, ATC, CSCS ACL injuries can be devastating to a soccer player s competitive season. For this reason, reputable medical institutions like the Cincinnati
Rehabilitation After Knee Meniscus Repair
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs with Bicep Tenodesis (+/- subacromial decompression) The rehabilitation guidelines are presented in
Meniscus Repair Rehabilitation Dr. Walter R. Lowe
 Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair
 UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
UW Health SpoRTS Rehabilitation Rehabilitation Guidelines for Type I and Type II Rotator Cuff Repair and Isolated Subscapularis Repair The anatomic configuration of the shoulder joint (glenohumeral joint)
The Lateral Collateral Ligament Sprain. Ashley DeMarco. Pathology and Evaluation of Orthopedic Injuries I. Professor Rob Baerman
 1 The Lateral Collateral Ligament Sprain Ashley DeMarco Pathology and Evaluation of Orthopedic Injuries I Professor Rob Baerman 2 The Lateral Collateral Ligament Sprain Ashley DeMarco Throughout my research
1 The Lateral Collateral Ligament Sprain Ashley DeMarco Pathology and Evaluation of Orthopedic Injuries I Professor Rob Baerman 2 The Lateral Collateral Ligament Sprain Ashley DeMarco Throughout my research
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Inland Orthopaedic Surgery & Sports Medicine
 Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities
 Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes
 Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Rehabilitation Guidelines for Autologous Chondrocyte Implantation. Ashley Conlin, PT, DPT, SCS, CSCS
 Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
