ACL Non-Operative Protocol
|
|
|
- Alicia Campbell
- 10 years ago
- Views:
Transcription
1 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the knee s stability is the Anterior Cruciate Ligament (ACL). The ACL attaches from the front part of the tibia to the back part of the femur. The purpose of this ligament is to keep the tibia from sliding forward and rotating on the femur. For this reason, the ACL is most susceptible to injury when twisting or rotational forces are placed on the knee. Although this can happen with contact, approximately 70% of ACL tears occur during non-contact events when athletes are cutting, decelerating or landing from a jump. After the ACL is torn, the knee is less stable and it becomes difficult to maintain a high level of activity without the knee buckling or giving way. It is particularly difficult to perform the repetitive cutting and pivoting that is required in many sports. Treatment Options Regardless of how the ACL is torn, your physician will work with you to determine a personalized course of treatment. People participating in sports or work related activities that require a lot of pivoting, cutting, or jumping may decide to have surgery. Depending on your lifestyle, however; conservative treatment may be the best option. In the case of an isolated ACL tear with no other ligamentous or cartilage involvement, the associated pain and dysfunction can be successfully treated with physical therapy. The initial course of treatment in physical therapy includes rest, anti-inflammatory measures and activity modification. After the swelling resolves and normal range of motion and strength is achieved, a decision between you and your physician can be made to determine further treatment options. If a non-surgical approach is chosen, it is imperative to maintain the strength, balance, and range of motion you gained in physical therapy to avoid further injury. At this juncture, many people elect to use a sports brace and limit their participation in activities that require a lot of pivoting, cutting or jumping. If conservative measures are unsuccessful and recurrent buckling persists, you and your physician may elect to have the ACL reconstructed. Recovery/Time off Work Page 1
2 Recovering from a torn ACL is not an easy process. It can be a long and difficult recovery that requires a tremendous commitment to rehabilitation. You must be an active participant during this process, performing daily exercises to ensure the return of your range of motion and strength. Recovery for a non-operative ACL tear is variable and largely dependent on your goals. People with desk jobs may take up to one week off from work due to pain. Manual laborers can be out of work for up to 6-8 weeks. Athletes will not be able to return to their sport immediately and will have to avoid cutting, pivoting, and jumping. Some people can cope with their injury and return to sports but typically require at least 8-10 weeks of physical therapy. Ultimately, return to sport and work is dependent on how you progress in therapy and whether you continue to have episodes of knee buckling. Recovery is different for every individual. Your personal time table for return to activities and work will be addressed by your physician and physical therapist throughout your course of treatment. At Home Immediately after the injury, resting and icing your knee can help control swelling and reduce some of your pain. Ice should be applied 3-5 times a day for minutes at a time. Always maintain one layer between the ice and your skin. A pillow case or paper towel serves as a good barrier to protect your skin. Your surgeon may prescribe pain medicine for you after your injury. Please call the doctor s office if you have any questions regarding medication. As a result of the injury, your knee is unstable and your thigh muscles can become extremely weak. It may be difficult to support the weight of your body when walking for the first few days. Crutches and/or a brace may be provided by your doctor to protect the knee from continued episodes of giving way and allow your knee to recover. Once the strength in your leg begins to return and you can demonstrate normal walking mechanics, your physical therapist will instruct you to wean away from the crutches. This typically takes less than 1-2 weeks. Surgery Sometimes, conservative treatment is unsuccessful and recurrent buckling persists. In this case, you and your physician may decide to have the ACL reconstructed. ACL reconstruction surgery is not a primary repair procedure. This means that the ligament ends cannot simply be sewn back together. The new ACL must come from another source and grafted into place in the knee. There are a few different graft options used for the ACL graft and each patient should consult with his or her surgeon to determine the best choice. During the procedure, a tunnel is drilled through the tibia and the new ACL graft is passed through it and anchored into place. Regardless of what type of graft is used, having an ACL reconstruction requires a significant commitment to physical therapy. Recovery is variable and rehabilitation can take anywhere from 6 months to a year. Page 2
3 Rehabilitation **The following is an outlined progression for rehab. Time tables are approximate and advancement from phase to phase as well as specific exercises performed should be based on each individual patient s case and sound clinical judgment by the rehab professional. ** Phase 1 (Acute Phase) Goals Control pain and swelling Restore pain free ROM Improve flexibility Normalize gait mechanics Establish good quadriceps activation Precautions WBAT with crutches until demonstrates normal gait mechanics Alert physician if patient reports episodes of knee buckling Recommended Exercises Range of Motion Patella mobilization (Medial/Lateral, Superior/Inferior) 2 Sets of 20 Repetitions Belt stretch (calf/hamstring) Hold 30 Seconds 3-5 Repetitions Heel slides 2 Sets of 20 Repetitions Prone quad stretch Hold 30 Seconds 3-5 Repetitions Cycle (minimal resistance) Minutes Daily Strength Quad sets 2-3 Sets of 20 Repetitions Add sets 2-3 Sets of 20 Repetitions SLR *(no Lag)* 2-3 Sets of Repetitions Hip Abd/Add/Ext/ER (against gravity) 2-3 Sets of Repetitions Body weight squats (partial range) 2-3 Sets of Repetitions Standing TKE with Theraband/cable column 2-3 Sets of Standing or prone hamstring curls 2-3 Sets of Repetitions Heel raises 2-3 Sets of Repetitions Guidelines Swelling and ROM deficits must be resolved before progressing to next phase. Use exercise bike daily if possible for minutes. Perform ROM exercises 3-5 times a day. Perform strengthening exercises 1 time a day. Page 3
4 Phase 2 (Sub-Acute/ Phase) Goals Avoid patella femoral pain Maintain ROM and flexibility Restore muscle strength Improve neuromuscular control Precautions D/C crutches if have not already Alert physician if patient reports episodes of knee buckling Recommended Exercises Range of Motion Continue ROM and initiate LE flexibility exercises Cycle/elliptical Minutes Continue Open Chain hip and knee strength from phase 1 progress with ankle weights Hamstring strengthening (progress from standing curl, leg curl machine, to curl on pball, single leg dead lift) 2-3 Sets of Repetitions Leg press (progress from double-limb to single limb) 2-3 Sets of Repetitions Step-up progressions (forward and lateral) 2-3 Sets of Repetitions Squat progression (limit to 90 degrees) 2-3 Sets of Repetitions Plank, side plank, single-limb bridge 2 Sets of 30 seconds each (15 seconds each leg with bridge) Static Single-limb balance 3 Sets of seconds (progress eyes open to eyes closed, foam, BOSU, *sport specific if applicable) Guidelines Perform all ROM and flexibility exercises once a day. If possible, cycle daily. Perform strengthening exercises 3-5 times a week (frequency and volume programmed by PT). Phase 3 (Limited Return to Activity Phase) Goals Avoid patella femoral pain Maintain ROM and flexibility Progress with single leg strengthening to maximize strength Progress dynamic proprioception exercises to maximize neuromuscular control Initiate plyometrics and light jogging Gradually begin return to sport activities pending physician s clearance Page 4
5 Precautions Must avoid patella femoral stress Caution pivoting and lateral movements Alert physician if patient reports episodes of knee buckling Recommended Exercises Range of Motion and Flexibility Continue ROM and flexibility exercises as needed Cardio Cycle/elliptical/treadmill with progressive resistance Continue progressing Phase 2 strengthening exercises Step-up progressions (increase height of step) 2-3 Sets of Repetitions Single-limb dead lift 2-3 Sets of Repetitions Static lunge progressions (forward/backward/lateral) 2 Sets of 50 feet Single-limb balance with perturbations 3 Sets of seconds (progress eyes open to eyes closed, foam, BOSU, *sport specific if applicable) Plyometrcs *emphasize eccentric control, avoiding increased trunk flexion, dynamic genu valgum, and femoral internal rotation, must have appropriate strength to progress to plyometric program* (see page 7 for more detailed progression) Simple double-limb jumps Complex double-limb jumps Guidelines Perform stretching program daily. Cardio exercise is recommended 3-5 times a week for minutes. Perform strengthening/proprioception exercises 3 times a week. Perform plyometric/jumping exercises 2 times a week. Monitor increased swelling with plyometrics. Decrease intensity if swelling persists. Strict attention must be paid to form and to minimize patella femoral pain with exercises. Phase 4 (Return to Activity/Sport Phase) Goals Maintain adequate ROM, flexibility and strength Continue progressive/dynamic strengthening, proprioceptive, plyometric and agility training Achieve adequate strength to return to sport (pending physician s clearance) Precautions Limited and controlled lateral movements Gradual return to sport pending physician s clearance Work with physician and physical therapist to develop specific return to sport progression Page 5
6 Recommended Exercises Stretching Continue daily lower extremity stretching Cardio Continue cardio program and progress intensity and duration Continue strengthening program from phase 3 (increase load and decrease repetition) Progress from static to dynamic lunges Continue advanced proprioceptive training (increase difficulty of drills) Plyometrics *emphasize eccentric control, avoiding increased trunk flexion, dynamic genu valgum and femoral internal rotation *(see page 7 for more detailed progression) Single-limb jumps Combination double-limb jumps Combination single-limb jumps Sport Specific Drills Initiate sports specific drills Begin speed/agility program (see page 8) Guidelines Perform stretching program daily. Cardio program is recommended 3-5 times a week for minutes Perform strengthening/proprioception exercises 3 times a week. Perform plyometric/jumping/agility exercises 2 times a week. Perform return to sport activities as directed by physician and physical therapist. Alert physician if patient reports episodes of knee buckling. Page 6
7 Phase 3 Simple Double-limb Jumping/Plyometric Progression *Limit foot contacts per workout Wall jumps Double-limb hops (anterior/posterior and medial/lateral over line) Box jump (6-8 inches max) Complex Double-limb Double-limb jump (for distance) Double-limb jump (for height) Double-limb jump (with 90⁰ or 180⁰ turn) Double-limb lateral jump/lateral box jump (side to side) Depth jump (6-8 inches max) *Focus on sticking each landing with good form in frontal and sagittal planes. Stress a soft landing with good eccentric control.* Phase 4 *Limit foot contacts per workout Single Limb Heiden/speed skater hop Single-limb hop (distance, height, lateral, 90⁰/180⁰ turn) Single-limb bounding Single-limb box jumps (6-8 inches max) Single-limb depth jumps (6-8 inches max) *Focus on sticking each landing with good form in frontal and sagittal planes. Stress a soft landing with good eccentric control.* Combination Jumps (Double-limb) Repetitive double-limb jumps (distance, height, lateral, turns) Jump for distance into jump for height Depth jump to jump for distance/height Depth jump to jump with 90⁰ turn Combination Jumps (Single-limb) Repetitive single-limb jumps (distance, height, lateral, 90⁰/180⁰ turn) Jump for distance into jump for height Depth jump to jump for distance/height Depth jump to jump with 90⁰ turn *String jumps together. Focus on quickly moving from jump to jump.* Page 7
8 Speed/Agility Progression *Work with physical therapist to establish proper warm-up and cool down before and after each workout agility session.* End of Phase 3/Phase 4 Forward/Backward Sprinting Workout 1: Sprint yards at ½ speed 10 reps. Workout 2: Sprint yards at ½ speed 5 reps. Sprint yards at ¾ speed 10 reps Workout 3: Sprint 100 yards at ½ speed 2 reps. Sprint 100 yards at ¾ speed 5 reps. Sprint yards at full speed 5 reps. Backpedal 50 yards at ½ speed 5 reps. Workout 4: Sprint 100 yards at ½ speed 1 rep. Sprint 100 yards at ¾ speed 2 reps. Sprint 50 yards at full speed 5 reps and 100 yards at full speed 5 reps. Backpedal 50 yards at ¾ speed 5 reps. Phase 4 Basic Change of Direction *Begin each workout with sprinting and backpedaling 50 yards (2 reps at ½ speed, 5 reps at full speed) Workout 5: T drill 3 reps at ½ speed, forward/backpedal shuttle 5/10/20 yard 3 reps at ½ speed Workout 6: T drill 3 reps full speed, forward/backpedal shuttle 5/10/20 yards 3 reps full speed, box drill with shuffling 3 reps at ½ speed Workout 7: Box drill with shuffling 3 reps at full speed, 10 yard shuttle run (quick direction change) 3 reps at full speed, Z drill 6 reps at ¾ speed Workout 8: Box drill with cuts 3 reps at full speed, 10 yard shuttle run (quick direction change) 3 reps at full speed, Z drill 6 reps at full speed Advanced Drills *Begin each workout with sprinting and backpedaling 50 yards (2 reps at ½ speed, 5 reps at full speed) Work with physical therapist to develop sport specific drills. Perform drills from previous weeks with use of ball, stick, etc. Perform drills seen in typical sports practice with supervision. Page 8
9 Time Phase 1 Acute Phase Weight Bearing and Gait *WBAT with crutches and progress to FWB and d/c crutches when patient can demonstrate normal gait mechanics Focus Range of Motion Recommended Exercises Precautions *Control pain and swelling *Restore pain free ROM *Restore normal gait mechanics *Establish good quadriceps activation *Emphasize knee extension equal to contralateral limb *Goal is to achieve full flexion ROM Patella mobilization, calf/hamstring stretches, heel slides, prone quad stretching, bicycle Quad/Add sets, SLR (no lag), hip Abd/Add/Ext/ER, partial range squats, standing TKE, standing or prone hamstring curl, heel raises *Minimize joint effusion and edema *Alert physician if patient reports episodes of knee buckling Phase 2 Sub-Acute Phase Phase 3 Limited Return to Activity/Sport *FWB *Straight ahead jogging per physician approval *Maintain ROM and flexibility *Progress strengthening *Improve neuromuscular control *Maintain ROM and flexibility *Maximize strength, initiate single leg exercises *Maximize neuromuscular control *Initiate plyometrics and light jogging *Initiate return to sport/work activities with physician approval *Maintain full ROM and optimize LE flexibility *Maintain full ROM and optimize LE flexibility ROM Continue Phase 1 exercises and initiate LE flexibility exercises, bicycle/elliptical with increased resistance Continue Phase 1 strengthening, leg press, leg curl machine, step-ups, squats, plank series, single-limb balance Single-limb balance exercises ROM/Stretching Continue ROM and flexibility exercises as needed Cardio Bicycle/elliptical/treadmill with progressive resistance Progress Phase 2 strengthening, step-up progressions, single-limb dead lifts, static lunges Single-limb balance with perturbations Plyometrics Double-limb simple and complex plyometrics *Minimize joint effusion and edema *Alert physician if patient reports episodes of knee buckling *Avoid patella femoral joint stress *Alert physician if patient reports episodes of knee buckling *Avoid patella femoral joint stress especially with plyometrics *Monitor increased knee effusion with plyometrics *Caution pivoting or lateral movements *Not cleared to return sports Page 9
10 Phase 4 Return to Activity/Sport *Sport specific program per physician clearance * Maintain ROM, flexibility, and strength *Continue dynamic strengthening and proprioceptive exercises *Continue plyometrics and initiate agility training *Progress sport specific drills *Continue daily LE stretching ROM/Stretching Continue daily stretching Cardio Bicycle/elliptical/treadmill with progressive resistance Progress Phase 3 strengthening, increase load and decrease repetitions Progress Phase 3 proprioceptive training increasing difficulty of drills Plyometrics Begin single-limb plyometrics, advance double-limb and single-limb combination jumps Sport Specific Drills Begin speed and agility program *Alert physician if patient reports episodes of knee buckling *Avoid patella femoral joint stress especially with plyometrics *Monitor increased knee effusion with plyometrics *Caution pivoting or lateral movements *Cleared for return to sport per physician *Reviewed by Michael Geary, MD Page 10
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Hip Bursitis/Tendinitis
 Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt
 Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Rehabilitation of Sports Hernia
 Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Post Surgery Rehabilitation Program for Knee Arthroscopy
 Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Inland Orthopaedic Surgery & Sports Medicine
 Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
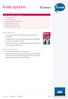 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes
 Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Strength Training for the Knee
 Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
Medial Collateral Ligament (MCL) Rehabilitation Protocol
 Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Post Surgery Rehabilitation Program
 Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
PREVENTING ACL INJURIES IN SOCCER. By Brian Goodstein, MS, ATC, CSCS
 PREVENTING ACL INJURIES IN SOCCER By Brian Goodstein, MS, ATC, CSCS ACL injuries can be devastating to a soccer player s competitive season. For this reason, reputable medical institutions like the Cincinnati
PREVENTING ACL INJURIES IN SOCCER By Brian Goodstein, MS, ATC, CSCS ACL injuries can be devastating to a soccer player s competitive season. For this reason, reputable medical institutions like the Cincinnati
Meniscus Repair Rehabilitation Dr. Walter R. Lowe
 Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Prevention & Management of ACL Injury. Ian Horsley PhD, MCSP Lee Herrington PhD, MCSP
 Prevention & Management of ACL Injury Ian Horsley PhD, MCSP Lee Herrington PhD, MCSP ACL injury ACL injury 30/100,000, 40% sports injuries (NHS) Limited statistics in UK related to sport Rugby Union 2002-2004
Prevention & Management of ACL Injury Ian Horsley PhD, MCSP Lee Herrington PhD, MCSP ACL injury ACL injury 30/100,000, 40% sports injuries (NHS) Limited statistics in UK related to sport Rugby Union 2002-2004
Rehabilitation after ACL Reconstruction: From the OR to the Playing Field. Mark V. Paterno PT, PhD, MBA, SCS, ATC
 Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
PHASE I ANKLE REHABILITATION EXERCISES
 PHASE I ANKLE REHABILITATION EXERCISES SWELLING CONTROL S REST: Keep your standing and walking activities to a minimum while swelling is a problem. ICE: Use an ice pack in a moist towel for 10-15 minutes
PHASE I ANKLE REHABILITATION EXERCISES SWELLING CONTROL S REST: Keep your standing and walking activities to a minimum while swelling is a problem. ICE: Use an ice pack in a moist towel for 10-15 minutes
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities
 Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
HIPABDUCTOR REPAIR PROTOCOL (Gluteus Medius/Minimus Repair)
 R. JOHN ELLIS, JR., M.D. LAWRENCE A. SCHAPER, M.D. MARK G. SMITH, M.D. G. JEFFREY POPHAM, M.D. AKBAR NAWAB, M.D. MICHAEL SALAMON, M.D. MATTHEW PRICE, M.D. DANIEL RUEFF, M.D. ELLIS & BADENHAUSEN ORTHOPAEDICS,
R. JOHN ELLIS, JR., M.D. LAWRENCE A. SCHAPER, M.D. MARK G. SMITH, M.D. G. JEFFREY POPHAM, M.D. AKBAR NAWAB, M.D. MICHAEL SALAMON, M.D. MATTHEW PRICE, M.D. DANIEL RUEFF, M.D. ELLIS & BADENHAUSEN ORTHOPAEDICS,
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees
 Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Physical Therapy Corner: Knee Injuries and the Female Athlete
 Physical Therapy Corner: Knee Injuries and the Female Athlete Knee injuries, especially tears of the anterior cruciate ligament, are becoming more common in female athletes. Interest in women s athletics
Physical Therapy Corner: Knee Injuries and the Female Athlete Knee injuries, especially tears of the anterior cruciate ligament, are becoming more common in female athletes. Interest in women s athletics
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
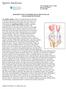 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
Kelly Corso MS, ATC, CES, FMSC, CSST
 ACL Injury Prevention Program Kelly Corso MS, ATC, CES, FMSC, CSST What is the ACL??? The ACL or anterior cruciate ligament, attaches the front top portion of the shin bone (tibia) to the back bottom portion
ACL Injury Prevention Program Kelly Corso MS, ATC, CES, FMSC, CSST What is the ACL??? The ACL or anterior cruciate ligament, attaches the front top portion of the shin bone (tibia) to the back bottom portion
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Cincinnati Sportsmedicine and Orthopaedic Center
 Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
Hip Arthroscopy Labral Repair Rehabilitation Protocol
 Hip Arthroscopy Labral Repair Rehabilitation Protocol PHASE 1: INITIAL Diminish pain and inflammation Protect integrity of repaired tissue Prevent muscular inhibition Restore ROM within the restrictions
Hip Arthroscopy Labral Repair Rehabilitation Protocol PHASE 1: INITIAL Diminish pain and inflammation Protect integrity of repaired tissue Prevent muscular inhibition Restore ROM within the restrictions
Rehabilitation after ACL Reconstruction
 Rehabilitation after ACL Reconstruction John Nyland, DPT, EdD Artur Proniewicz, MD Paul Mazzone, BS Athletic Training Program Kosair Charities College of Health and Natural Sciences Spalding University,
Rehabilitation after ACL Reconstruction John Nyland, DPT, EdD Artur Proniewicz, MD Paul Mazzone, BS Athletic Training Program Kosair Charities College of Health and Natural Sciences Spalding University,
Rehabilitation After ACL Reconstruction
 CENTRE PERTH ORTHOPAEDIC & SPORTS MEDICINE Rehabilitation After ACL Reconstruction Dr Keith Holt Philosophy of Rehabilitation Rehabilitation, as it applies to the recovery period from Orthopaedic Surgery,
CENTRE PERTH ORTHOPAEDIC & SPORTS MEDICINE Rehabilitation After ACL Reconstruction Dr Keith Holt Philosophy of Rehabilitation Rehabilitation, as it applies to the recovery period from Orthopaedic Surgery,
ACL Rehab. Here are a few tips on how to progress through an ACL rehab protocol with minimal problems;
 ACL Rehab The ACL rehab protocol is broken down into 5 phases, and there s a list of goals and outcome measures that need to be satisfied at the end of each phase to move onto the next one. You move through
ACL Rehab The ACL rehab protocol is broken down into 5 phases, and there s a list of goals and outcome measures that need to be satisfied at the end of each phase to move onto the next one. You move through
Hip Arthroscopy Post-operative Rehabilitation Protocol
 Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
Rehabilitation Guidelines for Lateral Ankle Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
Concussion Management Protocol for G-Force Program
 Concussion Management Protocol for G-Force Program Baseline ImPACT testing Recommended but not mandatory - Can be done anytime but ideally recommended before season begins - Ideally this should be done
Concussion Management Protocol for G-Force Program Baseline ImPACT testing Recommended but not mandatory - Can be done anytime but ideally recommended before season begins - Ideally this should be done
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction
 Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
ACL Reduction Helping you Keep it Together
 ACL Reduction Helping you Keep it Together What is the training program used in the ACL reduction Program? The ACL Reduction Program will be using the PEP (Prevent injury, Enhance Performance) Program
ACL Reduction Helping you Keep it Together What is the training program used in the ACL reduction Program? The ACL Reduction Program will be using the PEP (Prevent injury, Enhance Performance) Program
ACL Rehabilitation Protocol
 ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
ChondroCelect Rehabilitation Program
 ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
Preventing Volleyball Injuries: Knees, Ankles, and Stress Fractures
 Preventing Volleyball Injuries: Knees, Ankles, and Stress Fractures William W. Briner, Jr., MD, FACSM,FAAFP, Head Team Physician, U.S. Volleyball National Teams and Flavia Pereira Fortunately the risk
Preventing Volleyball Injuries: Knees, Ankles, and Stress Fractures William W. Briner, Jr., MD, FACSM,FAAFP, Head Team Physician, U.S. Volleyball National Teams and Flavia Pereira Fortunately the risk
Rehabilitation After Knee Meniscus Repair
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
UK HealthCare Sports Medicine Patient Education December 09
 Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee.
 Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Rehabilitation. Modalities and Rehabilitation. Basics of Injury Rehabilitation. Injury Rehabilitation. Vocabulary. Vocabulary
 Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Sports Injury Treatment
 Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
GALLAND/KIRBY INTERVAL DISTANCE RUNNING REHABILITATION PROGRAM
 GALLAND/KIRBY INTERVAL DISTANCE RUNNING REHABILITATION PROGRAM PHASE I: WALKING PROGRAM Must be able to walk, pain free, aggressively (roughly 4.2 to 5.2 miles per hour), preferably on a treadmill, before
GALLAND/KIRBY INTERVAL DISTANCE RUNNING REHABILITATION PROGRAM PHASE I: WALKING PROGRAM Must be able to walk, pain free, aggressively (roughly 4.2 to 5.2 miles per hour), preferably on a treadmill, before
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1
 Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
ACL Injury Prevention Through Proprioceptive & Neuromuscular Training Arlington Soccer Club April 1, 2010
 ACL Injury Prevention Through Proprioceptive & Neuromuscular Training Arlington Soccer Club April 1, 2010 Matthew R. McManus, PT Co-Owner & Regional Clinical Director - Massachusetts ProEx Physical Therapy
ACL Injury Prevention Through Proprioceptive & Neuromuscular Training Arlington Soccer Club April 1, 2010 Matthew R. McManus, PT Co-Owner & Regional Clinical Director - Massachusetts ProEx Physical Therapy
Goals of Post-operative operative Rehab. Surgical Procedures. Phase 1 Maximum protection and Mobility (1-4 weeks)
 Hip Arthroscopy - Post-Operative Care and Rehabilitation Franz Valenzuela, DPT, OCS Surgery corrects mechanical problems Rehabilitation corrects functional deficits Surgical Procedures Requires little
Hip Arthroscopy - Post-Operative Care and Rehabilitation Franz Valenzuela, DPT, OCS Surgery corrects mechanical problems Rehabilitation corrects functional deficits Surgical Procedures Requires little
