ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
|
|
|
- Laureen Lindsey
- 7 years ago
- Views:
Transcription
1 Daniel P. Duggan, D.O. The Sports Clinic Calle de la Magdalena, Suite 229 Laguna Hills, CA Phone: (949) Fax: (949) ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION The anterior cruciate ligament (ACL) is one of four major ligaments that stabilize the knee joint. A ligament is a tough band of fibrous tissue, similar to a rope, which connects the bones together at a joint. The ACL prevents the lower bone (the tibia) from sliding forward too much and stabilizes the knee joint to allow cutting, twisting and jumping activity. The most common mechanism that tears the ACL is the combination of a sudden stopping motion of the leg while quickly twisting the knee. This can happen in sports such as basketball and soccer when a player lands on the leg when coming down from a rebound, or is running down the field and makes an abrupt stop to pivot. In skiing the ACL is commonly injured when a skier slides back while falling. These excess forces cause the ACL to pop. When the ACL tears the person feels the knee move out of joint and often hears or feels a pop. If he or she tries to stand on the leg it may feel unstable and give out. The knee usually swells a great deal initially (often within two hours), and it becomes painful and difficult to walk. It is also possible to injure other structures inside your knee when the ACL is torn. The meniscus is a crescent shaped shock absorber between the femur and tibia, and each knee has one on the inside (medial) and outside (lateral) of the knee joint. When the tibia suddenly moves forward the meniscus can also be torn. Similarly the articular cartilage (the smooth liner of the joint) can also be injured. If this articular cartilage is injured the joint no longer moves smoothly. Stiffness, pain, swelling and grinding can occur. Eventually arthritis can develop. Finally, it is also possible to injure the other ligaments of the knee, which can cause pain or instability with activity. Tears of the outer ligament (the lateral collateral ligament, or LCL) often do require surgical repair, while tears of the inner ligament (the medial collateral ligament, or MCL) often heal completely over six to eight weeks and usually do not require surgery.
2 If no other structure than the ACL is injured the knee usually regains its range of motion and is painless after six to eight weeks. The knee will typically feel completely normal, but may be a trick knee. If a knee does not have an ACL, it can give way or be unstable when the person pivots or changes direction. It is usually possible to run straight ahead without any problems, but when the athlete makes a quick turning motion the knee tends to give way and collapse. This abnormal motion can damage other structures in the knee. If a person does not engage in sports and is relatively inactive, the knee can feel quite normal even if the ACL is torn. Thus, many patients, especially over the age of 30 may not need to have the ACL reconstructed, especially if they do not participate in sports that require quick changes in direction. In younger athletic patients or those older patients that still participate in sports at a high level, however, the knee will tend to re-injure frequently and give way during activities in which the person quickly changes direction. Therefore in these groups it is best to reconstruct the torn ACL. In those in whom ACL reconstruction is not undertaken it may be necessary to modify activities and avoid high-risk sports such as basketball, football, and soccer. Wearing a knee brace may help prevent further injury but will not completely stabilize a knee that has a torn ACL. Exercises that restore the muscle strength, power, coordination, and endurance will also improve knee function and help stabilize the knee. However, a fully rehabilitated knee that has a torn ACL can still give way if a quick change in direction is unexpected. It is best to wait for the pain and swelling from the initial injury to subside and allow other associated injuries to heal prior to performing ACL surgery. If surgery is done too soon after injury, rehabilitation is difficult; the knee may get stiff and have permanent loss of motion. The athlete will usually get back to sports more quickly if the knee is allowed to recover from the initial injury and regain its full painless range of motion prior to any surgery (usually about six weeks). The best treatment for the initial period after an ACL injury is to protect the joint and apply ice and use crutches for several weeks. As the swelling and pain subside, and the patient can put weight on the leg the crutches can be discontinued. The emphasis is then on regaining knee motion. Exercises designed to build up knee strength should not be done at this point in order to avoid damaging the cartilage under the kneecap (patella). There may be some examples when immediate surgery is indicated following injury, such as in a knee dislocation when multiple ligaments are torn. Your doctor will discuss this with you should you fall into one of these categories.
3 ACL Reconstruction Surgery Surgical reconstruction of a torn ACL involves replacing the torn ACL with a tendon (called a graft) from another part of the knee or a cadaver donor, and putting it into a position to take the place of the torn ACL. Examples of commonly employed grafts include the middle third of the patellar tendon (the tendon connecting the knee cap to the tibial bone), hamstring tendons, and Achilles tendons. In the case of patellar tendon and hamstring grafts, they may be obtained either from your own tissue or a cadaver donor (called allograft). In the case of Achilles tendon, the grafts are always obtained from a cadaver donor. For most of these procedures the operation is done arthroscopically instead of making big incisions. Associated injuries such as torn menisci, loose bodies, etc. are addressed at the same time. If patellar tendon graft is used, a small incision is made on the inner side of the leg just below the knee cap to take the graft (this results in a small area of numbness on the front of the knee). If a hamstring tendon graft is used a small incision is made on the inside of the leg below the knee joint. Guides are used to place the graft in the proper position of your knee. The graft is then pulled into bony tunnels and secured in place with screws. Postoperatively, an accelerated rehabilitation program allows the quickest return of function. A knee brace and crutches are used for the first 2-6 weeks after surgery, depending on the choice of graft. The amount of weight you are allowed to put on your leg will depend on the choice of graft as well. Numerous studies have been done to try to prove superiority of one graft choice over another, and as it currently stands no choice offers clear benefits over all the others in all situations. Your surgeon will discuss with you the pros and cons of the various graft options.
4 The risks of ACL reconstruction include but are not limited to: Permanent numbness in the front of the knee 100% Other nerve injuries 0.5% Patellofemoral pain (knee cap) 5% Stiffness or reduced motion of the knee 10% Re-injury 5-10% Superficial infection 1% Deep infection 0.5% Blood clots 2-3% Delay in regaining motion 5% How soon will I? Return to work Sedentary General office Light physical Medium Heavy Return to sports Normal walking/stairs Light individual sports Running/jumping Contact/high performance 1-2 weeks 2-3 weeks 6-8 weeks 3 months 4 months 1-2 months 3-4 months 6 months 9 months Postoperative Instructions You will wake up in the operating room with a brace and ice pack in place. You will also have white compression stockings on both legs. These are to help prevent blood clots and should be worn for the first two weeks following surgery. Depending on your surgery, you may have a continuous passive motion (CPM) machine, which is designed to help your knee move and regain your full motion. You should plan on using this at least 10 hours per day. The machine should be set to -5 0 of extension and of flexion. It is set to pause for five seconds in extension. After 4-5 days try to have the CPM machine to 90 0 of flexion The most important aspect is to have your knee out straight You can adjust the speed. Many patients find it easier to sleep with the machine in slower speeds, and have faster speeds when up during the day.
5 You will be sent home with a prescription for pain medication. In addition to the pain medication you should take one adult strength aspirin every day for 14 days, in order to help prevent blood clots. The pain medication can make you constipated. If this is the case, take an over the counter stool softener such as Colace while taking the pain medication. You will be sent home from the recovery room after a few hours. You will need someone else to drive you home. Activities and advice for in the hospital and while at home: 1. Please call with any concerns: (949) Apply ice to the knee, as it will be quite helpful. After two days, you can change the dressing to a smaller one to allow the cold to better get to the knee. Be sure to leave the little pieces of tape (steri-strips) in place. 3. After two days it is okay to shower and get the wound wet, but do not soak the wound as you would in a bath tub or hot tub. 4. After knee surgery there is a variable amount of pain and swelling. This will dissipate after several days. Continue to take the pain medicine you were prescribed as needed. Remember it is called pain control, not pain elimination. If you notice calf pain or excessive swelling in the lower leg, call your doctor. 5. It is important to look out of signs of infection following joint replacement surgery. These can include: fever (temperature > , chills, nausea, vomiting, diarrhea, redness around your incision, or yellow or green drainage from your incision. Should any of these be present please contact Dr. Duggan s office immediately. 6. You should start your physical therapy approximately 3 weeks after your surgery. 7. You will have an office visit scheduled approximately days after your surgery.
6 Phase I: immediate post-op phase (0-2 weeks after surgery) Goals: 1. Protect the reconstruction 2. Ensure wound healing 3. Attain and maintain full knee extension 4. Gain knee flexion (bending) to 90 degrees 5. Decrease knee and leg swelling 6. Promote quadriceps muscle strength 7. Avoid blood pooling in the leg veins Activities: 1. Continuous passive motion (CPM). This should be used at least 10 hours per day. You may use it anywhere that is comfortable. Use it at night while sleeping. It is very important that you straighten your knee completely. After 5 to 7 days of using the machine, if you have achieved greater than 100 degrees of flexion you can stop using the CPM machine. 2. Brace/crutches/weight bearing: your knee brace is set to allow you to bend and straighten your knee. Use it when walking or out of bed, but it may be removed for range of motion exercises. In cases where a meniscus repair surgery was done as part of your surgery you will need to keep the brace locked in extension (fully straight) when walking for 6 weeks after surgery. a. If you had a patellar tendon autograft (your own tendon), you can put as much weight on your leg as you feel like. You should use the crutches in the beginning, but can stop using them when you feel as though your knee can support you. You will still need to wear your brace for the first six weeks after surgery. There may be some circumstances where restricted weight bearing will be necessary. Your doctor and therapist will discuss this with you if this is the case. b. If you had a hamstring autograft or allograft, you will be allowed to put 50% weight on your leg with crutches and a brace for the first six weeks after surgery. c. If you had a patellar tendon allograft (cadaver tendon) you will be allowed to put 50% weight on your leg with crutches and a brace for the first six weeks after surgery. 3. Your nurse or therapist will demonstrate the proper form for walking with crutches:
7 a. Put the crutches forward about one step s length b. Put the injured leg forward in line with the crutch tips c. Touch the foot of the injured leg to the floor and put as much weight down as is comfortable (brace on and locked) d. While bearing weight on the injured leg, take a step through with the uninjured leg. 4. Elastic stockings: wear an elastic stocking below the knee until your first postoperative visit. Do at least 10 ankle pump exercises each hour to help prevent blood clots. Take one adult aspirin daily for the first two weeks 5. It is okay to remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri-strips) across the incision. You can wrap an elastic bandage (ACE wrap) around the knee at other times to control swelling. You may shower and get your incision wet (unless there is any drainage from your incisions). Do not soak the incision in a bathtub or hot tub until the stitches have been removed. Exercises Program: 7 days per week, 3-4 times per day. Quadriceps setting 1-2 sets reps Heel prop 5 minutes Heels slides with towel assist 5-15 minutes Sitting heel slides 1-2 sets reps Straight leg raises 1-2 sets reps Patellar mobilization 1 set reps Hip abduction 3 sets 10 reps Ankle pumps 10 per hour Prone hang 5 minutes Quadriceps Setting Lie or sit with knee fully straight. Tighten and hold the front thigh muscle making the knee flat and straight (this should make your knee flatten against the bed or floor). Hold 5 seconds for each contraction. Heel Prop Lie on your back with a rolled up towel under your heel, or sit in a chair with the heel on a stool. Let the knee relax into extension (straight). If
8 the knee will not straighten fully, you can place a small weight (2-5 lbs) on the thigh just above the kneecap. Try to hold for 5 minutes. Try to practice quadriceps setting in this position. Patellar Mobilization With the knee fully extended, grasp the edges of your kneecap between your thumb and index finger. Move the kneecap side to side and up and down. Heel slides with towel assist While sitting or lying on your back, actively slide your heel backward to bend the knee. Hold this bent position for five seconds then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise. You can assist by using a towel to pull your heel back. Sitting Heel Slides While sitting in a chair or over the edge of the bed, support the operated leg with the uninvolved leg. Lower the operated leg, with the unoperated leg controlling, allowing the knee to bend. Do not go past 60 0 of bend at the knee. Hold for 5 seconds and slowly relieve the stretch by lifting the foot upward with the uninvolved leg to the straight position. Straight leg lift Tighten the quadriceps as much as you can. Lift your heel 4-6 inches from the floor. Tighten the quadriceps harder. Lower your leg back to the floor while continuing to tighten the quadriceps. If your knee bends when you attempt to lift do not do this exercise.
9 Hip abduction Lie on your unoperated side. Keep your knees fully extended (straight). Raise the operated limb upward to a 45 0 angle. Hold for one second then lower slowly. Ankle Pumps Move the ankle up and down to help stimulate circulation in the leg. Prone Hang Lie face down across your bed so that the kneecap is just off the edge of the mattress. Let your leg drop down toward the floor so that your knee straightens fully. If the knee will not fully extend, then attach a weight around the ankle to help pull the leg down. Use an amount of weight as described in the heel prop exercise.
10 Phase II: early rehabilitation phase (weeks 2-6 after surgery) Goals: 1. Maintain full passive knee extension (at least 0-50 of hyperextension) 2. Gradually increase knee flexion 3. Diminish swelling and pain 4. Muscle control and activation 5. Restore proprioceptive and neuromuscular control 6. Normalize patellar mobility 7. Normal gait without crutches (if autograft) Activities: 1. Continue to use ice to decrease swelling. It should be used for 20 minutes at least three times per day. 2. Brace/crutches: In cases where patellar tendon autograft is used, you can discontinue using your crutches when you are comfortable doing so. Continue using your brace. In cases of hamstring grafts or allograft patellar tendons continue with partial (50%) weight bearing with the crutches and brace. In cases where a meniscus repair surgery was done as part of your surgery you will need to keep the brace locked in extension (fully straight) when walking for 6 weeks after surgery. 3. You may stop wearing the compression stockings and can stop taking the aspirin. 4. You will have a visit with Dr. Duggan at days after surgery. If your wound is dry, you will likely be able to get the wound wet in a bath or hot tub at this point. Irrespective of whether your right or left leg was operated on, it is unlikely you will be allowed to drive at this point. Exercises The following exercises will be demonstrated to you by your physical therapist. He or she will also give you a home exercise program. You should strive to do your home exercise program at least 3-4 times per day, every day. The success of your reconstruction depends on your rehab.
11 Exercises: Quadriceps setting Heel prop Prone hang Heel slides with towel assist Straight leg raises Standing hamstring curl Standing toe-raises Hip abduction 1/3 knee bends Wall slides Optional exercises: If you did not have a meniscus repair as part of your surgery you may do leg press and hamstring extension exercises on a machine under the supervision of your therapist. You need to have achieved the following, though, in order to do this: 1. Full passive knee extension 2. Full extension while quadriceps setting 3. Flexion of 125 degrees 4. Minimal swelling
12 Phase III: progressive strengthening and neuromuscular control phase (weeks 6-12 after surgery). Goals: 1. Restore full knee range of motion ( ) 2. Improve lower extremity strength 3. Enhance proprioception, balance and neuromuscular control 4. Improve muscular endurance 5. Restore limb confidence and function 6. Protect the reconstruction (avoid falling) Activities: 1. The brace can be discontinued after you see Dr. Duggan at your 6 week visit. Concentrate on walking with a heel to toe gait without a limp. In some cases, use of the brace will continue if your knee requires a longer period of protection. 2. Continue to use ice for 20 minutes after each workout 3. You are cleared to drive when bearing weight on your operative leg is comfortable and you have good control of the leg. If your left leg was operated on, you should be clear to drive at this point. Precautions When Exercising Avoid pain at the patellar tendon site Avoid pain and/or crepitus at the patella Build up resistance and repetitions gradually Perform exercises slowly avoiding quick direction change and impact loading Exercise frequency should be 2 to 3 times a week for strength building Be consistent and regular with the exercise schedule Exercises: Range of motion/strengthening: Quadriceps setting Heel prop Prone hang Heel slides with towel assist Straight leg raises Standing hamstring curl
13 Standing toe-raises- single leg Hip abduction Squat to chair Wall slides Single leg strengthening progression Stretching exercises: Hamstring stretch, 3-5 reps holding 15 to 30 seconds Quadriceps stretch, 3-5 reps holding 15 to 30 seconds Calf stretch, 3-5 reps holding 15 to 30 seconds Optional exercises: Seated Leg Press Roman Chair Hamstring Curl Calf Raise Machine HIP Abductor/Adductor Machine Hip Flexor Machine Cardiovascular conditioning can begin at this phase: Stationary bicycle Walking Rowing Elliptical trainer Water workout DO NOT perform any of the following exercises: Knee extension weight lifting machine Lunges Running Stairmaster Jumping Step exercises with impact Pivoting or cutting
14 Phase IV: advanced activity phase (weeks after surgery) Goals: 1. Normalize lower extremity strength 2. Enhance muscular power and endurance 3. Improve neuromuscular control 4. Perform selected sport-specific drills Criteria to progress to Phase IV: 1. AROM Quad strength 75% contralateral side 3. Knee extensor: flexor ratio 70-75% 4. No pain or effusion 5. Satisfactory clinical exam 6. Hop test 80% of contralateral leg Activities 1. Your activities will increase in this phase of rehab, however it is important to remember that you are not yet fully recovered from your surgery. Progressing too quickly or engaging in sports or other activity prior to being cleared to do so greatly increases the risk of failure of your surgery and compromise of your results. 2. At this time, light running on a soft level surface with a sports brace can begin if Dr. Duggan advises. You need to have full range of motion, good strength and no swelling to run safely. If you run, 3 times per week for 10 minutes is advisable for the first 2 weeks. If there is no pain or swelling, you can increase your running time by 1 minute per session for a maximum of 30 minutes. Walking and hiking on gentle trails can also be used for conditioning activity. 3. Avoid the following exercises as they place undue stress on your knee: a. Leg extension machine b. Stairmaster or stair climber machines c. Deep knee lunges or squats past 90 0 of knee flexion d. High impact exercises 4. Avoid pain at the patellar tendon site, as well as crepitus (crunching) at the patella 5. Build up resistance and repetitions gradually 6. Perform exercises slowly and avoid quick direction changes 7. Avoid impact loading
15 8. Exercise frequency should be at least 2-3 times per week for strength building 9. Be consistent and regular with exercise schedule Exercises May initiate straight ahead running program Light sports okay (golf pitch and putt) Continue strengthening drills o Leg press o Wall squats o Hip abduction and adduction o Hip flexion and extension o Keen extension o Hamstring curls o Seated and standing toe calf raises o Step down o Lateral step ups and lunges Weeks may initiate lateral agility drills and backward running. It is okay to start jump and plyometric training. Neuromuscular training: Lateral step overs (cones) Lateral lunges Tilt board drills Sports RAC repositioning on tilt board
16 Phase V: return to activity phase (weeks after surgery) Goals: 1. Gradual return to full-unrestricted sports 2. Achieve maximal strength and endurance 3. Normalize neuromuscular control 4. Progress skill training Criteria to enter Phase V: 1. Full ROM 2. Quadriceps bilateral comparison within 80% or greater 3. Hamstring bilateral comparison within 110% or greater 4. Quadriceps torque: body weight ratio 55% or greater 5. Hamstrings: quadriceps ratio 70% or greater 6. Prioprioceptive test 100% of contralateral leg 7. Functional test 85% or greater of contralateral leg Exercises: Continue strengthening exercises Continue neuromuscular control drills Continue plyometric drills Progress running and agility program Progress sport specific training o Running/cutting/agility drills o Gradual return to sport drills
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
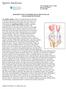 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Rehabilitation After Knee Meniscus Repair
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Strength Training for the Knee
 Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
UK HealthCare Sports Medicine Patient Education December 09
 Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
KNEE ARTHROSCOPY HANDBOOK
 KNEE ARTHROSCOPY HANDBOOK 1450 Ellis Street Suite 201 Bozeman, Montana 59715 (406) 587-0122 FAX (406) 587-5548 www.bridgerorthopedic.com Your Arthroscopy Handbook Contemplating surgery of any kind leads
KNEE ARTHROSCOPY HANDBOOK 1450 Ellis Street Suite 201 Bozeman, Montana 59715 (406) 587-0122 FAX (406) 587-5548 www.bridgerorthopedic.com Your Arthroscopy Handbook Contemplating surgery of any kind leads
ACL Non-Operative Protocol
 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
KNEES A Physical Therapist s Perspective American Physical Therapy Association
 Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Post Surgery Rehabilitation Program for Knee Arthroscopy
 Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
ACL Rehabilitation Protocol
 ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella)
 EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
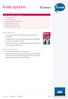 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
ACL Reconstruction Rehabilitation Protocol
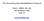 Peter J. Millett, MD, MSc The Steadman Clinic Vail, CO www.drmillett.com Table of Contents Preoperative Rehabilitation Phase...3 Understanding Surgery...7 Postoperative Days 1-7...8 Postoperative Days
Peter J. Millett, MD, MSc The Steadman Clinic Vail, CO www.drmillett.com Table of Contents Preoperative Rehabilitation Phase...3 Understanding Surgery...7 Postoperative Days 1-7...8 Postoperative Days
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Ira K. Evans, M.D. Sports Medicine North Orthopedic Specialty Center One Orthopedics Drive Peabody, MA 01960. www.sportsmednorth.
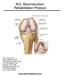 ACL Reconstruction Rehabilitation Protocol Ira K. Evans, M.D. Sports Medicine North Orthopedic Specialty Center One Orthopedics Drive Peabody, MA 01960 ike@sportsmednorth.com Tel: (978) 818-6350 Fax: (978)
ACL Reconstruction Rehabilitation Protocol Ira K. Evans, M.D. Sports Medicine North Orthopedic Specialty Center One Orthopedics Drive Peabody, MA 01960 ike@sportsmednorth.com Tel: (978) 818-6350 Fax: (978)
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
TOTAL KNEE REPLACEMENT
 PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1
 Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Post Surgery Rehabilitation Program
 Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
ROTATOR CUFF TEARS SMALL
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
ACL Reconstruction Rehabilitation
 ACL Reconstruction Rehabilitation The following exercises are commonly used for rehabilitation following ACL reconstruction surgery. However, each knee surgery is unique and each person s condition is
ACL Reconstruction Rehabilitation The following exercises are commonly used for rehabilitation following ACL reconstruction surgery. However, each knee surgery is unique and each person s condition is
PHASE I ANKLE REHABILITATION EXERCISES
 PHASE I ANKLE REHABILITATION EXERCISES SWELLING CONTROL S REST: Keep your standing and walking activities to a minimum while swelling is a problem. ICE: Use an ice pack in a moist towel for 10-15 minutes
PHASE I ANKLE REHABILITATION EXERCISES SWELLING CONTROL S REST: Keep your standing and walking activities to a minimum while swelling is a problem. ICE: Use an ice pack in a moist towel for 10-15 minutes
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Post-Operative Exercise Program
 785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
TOTAL HIP REPLACEMENT
 PENN ORTHOPAEDICS TOTAL HIP REPLACEMENT Home Exercise Program Maintain Your 3 HIP PRECAUTIONS! The purpose of your hip precautions is to allow for the best healing and the most successful outcomes from
PENN ORTHOPAEDICS TOTAL HIP REPLACEMENT Home Exercise Program Maintain Your 3 HIP PRECAUTIONS! The purpose of your hip precautions is to allow for the best healing and the most successful outcomes from
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt
 Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Anterior Cruciate Ligament Reconstruction Progression Rehabilitation Program By Jenna Hennebry, Erin Stiefel, and Lauren Schmidt Case Study: 18 year old female soccer player Isolated ACL rupture (planted
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Steps to Success: A Guide to Knee Rehabilitation
 Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Patella Realignment Tibial Tuberosity Transfer with Lateral Release
 Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
.org. Knee Arthroscopy. Description. Preparing for Surgery. Surgery
 Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Meniscus Tear: Exercises
 Meniscus Tear: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off the exercise if you
Meniscus Tear: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off the exercise if you
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Ankle Sprain. Information and Rehabilitation. Grade II. Grade I. Grade III
 514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Foot and Ankle Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Hip Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Medial Collateral Ligament Sprain: Exercises
 Medial Collateral Ligament Sprain: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off
Medial Collateral Ligament Sprain: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
Rehabilitation After Your Total Knee Replacement
 1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
www.noc.nhs.uk ACL Reconstruction Information for Patients Delivering Excellence Hip and Knee service
 www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Cincinnati Sportsmedicine and Orthopaedic Center
 Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
Cartilage Repair Center
 Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon
 Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon Knee Arthroscopy Physical Therapy Protocol This rehabilitation
Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon Knee Arthroscopy Physical Therapy Protocol This rehabilitation
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Inland Orthopaedic Surgery & Sports Medicine
 Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
