Immunohistology of the Mediastinum
|
|
|
- Colleen Sutton
- 10 years ago
- Views:
Transcription
1 Immunohistology of the Mediastinum Mark R. Wick 1 CHPTER OUTLINE Introduction 301 iology of antigens/antibodies 301 lgorithmic immunohistochemistry of mediastinal disease 302 Immunohistologic findings in specific diseases of the mediastinum 304 Cystic thyoma versus cystic seminoma 304 Differential diagnosis of other thymoma variants 304 enign peripheral nerve sheath tumors and ganglioneuromas 305 Fibrogenic and myofibroblastic proliferations 305 Malignant smallcell mediastinal neoplasms 306 Mediastinal smallcell meuroendocrine carcinoma 306 asaloid squamous carcinoma of the mediastinum 307 Neuroblastoma of the mediastinum 307 Mediastinal primitive neuroectodermal tumor 307 Rhabdomyosarcoma of the mediastinum 307 Smallcell malignant lymphomas of the mediastinum 309 Other smallcell mediastinal neoplasms 310 Large polygonal cell neoplasms of the mediastinum 311 Primary thymic carcinomas 311 Parathyroid carcinoma of the mediastinum 314 Malignant mediastinal germ cell tumors 314 Mediastinal carcinoid tumor 314 Mediastinal paragangliomas 314 Mediastinal largecell nonhodgkin s lymphoma 316 Mixed small and large cell malignancies 318 Mixed largecell and smallcell nonhodgkin s lymphoma 318 Mixedcellularity Hodgkin s disease 318 Lymphoepitheliomalike carcinoma 318 Malignant spindle cell tumors 319 Sarcomatoid thymic carcinoma 319 Spindle cell carcinoid tumor of the thymus 321 Sarcomatoid mediastinal malignant mesothelioma 322 Sarcomatoid thymic yolk sac tumor 322 Mediastinal leiomyosarcoma 322 Prognostic markers in mediastinal tumors 322 INTRODUCTION The mediastinum is a relatively confined anatomic site, but it is capable of harboring a wide variety of pathologic processes, both nonneoplastic and neoplastic. These include proliferations of somatic epithelial, lymphoid, mesenchymal, and germ cell types. Surgical pathology of mediastinal disorders is made all the more challenging by the fact that small biopsies taken either by mediastinoscopy or closed needle biopsy have become routine as the primary method of diagnosis. 1 6 Therefore, one is often faced with the need to perform numerous immunostains on such material in order to obtain a meaningful diagnosis in the absence of much morphological detail. This chapter presents a synopsis of immunohistologic information as applied to that specific context. There will be no attempt to be encyclopedic in regard to the scope of pathologic entities that may arise in the mediastinum, or the panoply of immunoreactants that have been assessed in them. Rather, emphasis is placed on practical differential diagnosis and the role that immunohistology plays in that process. IOLOGY OF NTIGENS/NTIODIES There are very few cellular proliferations of the mediastinum neoplastic or otherwise that are unique to it, and therefore the spectrum of immunoreactants that is of interest in this topographic region overlaps significantly with that considered in other chapters. Hence, the biochemical attributes of intermediate filament subtypes, various membrane glycoproteins synthesized by epithelial and hematopoietic cells, and cytoplasmic differentiationrelated proteins will not be recounted. The reader is referred to primary discussions of carcinomas, hematolymphoid lesions, specific mesenchymal prolif 301
2 IMMUNOHISTOLOGY OF THE MEDISTINUM erations, etc., elsewhere in this text. However, a few remarks will be made here on reactants that appear to be restricted to mediastinal disorders, or are elaborated in a singular fashion in those diseases. Thymic Hormones: Several hormonal proteins are apparently synthesized by epithelial cells of the thymus, and these are thought to have distant effects on the development or function of the immunologic system. Such moieties include thymopoietic, thymic humoral factor, thymosin, facteur thymique serique, thymic factor X, thymic plasma recirculating factor, thymotoxin, thymulin, and thymin. 7 mong them, only thymosin has been evaluated immunohistochemically in human neoplasms, primarily in thymomas, with reactivity being observed in >80%. 8 Nevertheless, there have been no systematic studies of the differential diagnostic utility (or lack thereof) of thymic hormones, and their practical role in the surgical pathology laboratory is consequently unknown. Keratin Subclasses: s in many other organs, keratin subsets have been analyzed in the normal thymus and in tumors deriving from it. 9,10 In particular, keratins 7, 13, and 18 appear to be expressed in this spectrum of tissues. Keratin 13 is restricted to epithelial cells of the thymic medulla, but is shared by thymomas of all types. 9 Indeed, keratins 7 and 18 likewise appear to be preferentially seen in neoplastic proliferations of this gland. 9,10 LGORITHMIC IMMUNOHISTOCHEMISTRY OF MEDISTINL DISESE Perhaps in reaction to the overwhelming number of antibodies that one may now apply to diagnostic questions in surgical pathology, shotgun approaches to immunohistology have become worryingly common. Concerns over medicolegal liabilities also may prompt one to empty the reservoir of reagents in the evaluation of difficult cases. Nonetheless, published experience with wellcharacterized procedures and antibodies has made this temptation unnecessary. Indeed, a sufficient body of data on reagent specificity and sensitivity is now available that one may codify it by means of integration into algorithms. djunctive algorithmic diagnosis has several benefits. It provides reproducible strategies for the resolution of recurring problems in histopathology, gives one a prescribed sequence in which the results of predefined antibodymediated stains may be interpreted, and compensates for the reality that no single reagent is likely to provide a definitive answer in any given case. The last of these three points is an important one, because it has been fashionable (but largely noncontextual and fatuous, in the author s opinion) to embrace the practice of antibody bashing with regard to the specificity of individual reagents. There are several caveats that must be heeded before immunohistochemical algorithms can be safely and effectively applied. They include the following points: 1. The user (pathologist) must control the processing of all tissues in his or her own laboratory under stringent conditions. If specimen fixation times or conditions vary wildly, so will antibody reactivity patterns. 2. The user (not the manufacturer or distributor) must determine the optimal dilutions of all antibody reagents personally. Simple acceptance of commercial recommendations is unwise; published scientific papers on such reagents are more helpful in giving one practical information on this point. 3. The user must accrue data on the spectra of reactivity for all antibodies, over a broad group of pathologic conditions or neoplasms, as processed and studied in his or her own laboratory. Failing the feasibility of this approach, the pathologist must adopt exactly the same method of fixation, processing, and staining that is used in published investigations that provide the desired information. 4. lgorithms must be based on formal statistical analyses of specificity, sensitivity, and ayesian predictive values, as applied to predefined differential diagnostic problems. This approach allows for the determination of relative values for each determinant in wellcharacterized settings. 5. The sequence of interpretation of a group of immunostains should be governed by their relative statistical values, moving from most specific to least specific or from highest positive predictive value to lowest. 6. Discrete morphological categories must be determined for application of the foregoing principles. For example, the author generically classifies all morphologically indeterminate and undifferentiated neoplasms of the mediastinum into one of three major groups small cell, large polygonal cell, and spindle cell/pleomorphic tumors constitute those clusters. 7. Immunohistochemical data must be applied only in the context of thorough morphological analysis and wellformulated differential diagnosis. It is and will always be true that immunostains are merely diagnostic adjuncts and do not take the place of skill in the interpretation of slides stained with hematoxylin and eosin. poor histodiagnostician will probably be a worse immunohistochemist! Hence, one must always see to it that clinical information, histologic differential diagnosis, and immunohistologic interpretations fit together in a sensible fashion. 8. lgorithms should be flexible. s new reagents are introduced and suitably characterized, they may be integrated into preexisting schemes to replace or supplement older antibodies. 302
3 IMMUNOHISTOLOGY OF THE MEDISTINUM 10 Table 10.1 ntibodies used in the algorithmic immunohistochemical analysis of mediastinal diseases ntigen ntibody Source Dilution (clone) Cytokeratins E1 oehringer 1:100 Mannheim E1/E3 oehringer 1:150 Mannheim CM5.2 ecton 1:150 Dickinson MK6 Triton 1:40 iosciences CK20 ITKs2O.8 DKO 1:40 Vimentin V9 iogenex 1:2000 Desmin 033 iogenex 1:2000 Epithelial membrane E29 DKO 1:400 antigen Carcinoembryonic NG oehringer 1:4000 antigen Mannheim Epithelial antigen EREP4 DKO 1:200 Calretinin Polyclonal Zymed 1:750 Neuronspecific Polyclonal iogenex 1:450 enolase Chromogranin LK2H1O oehringer 1:4000 Mannheim Synaptophysin SY38 oehringer 1:40 Mannheim CD57 Leu7 ecton 1:20 Dickinson S100 protein Polyclonal DKO 1:300 ntimelanoma HM45 iogenex 1:60 Tyrosinase T311 Novocastra 1:20 MRT1 103 iogenex 1:25 Musclespecific actin HHF35 iogenex 1:400 lphaisoform actin I4 iogenex 1:2 Myogenin F5D DKO 1:10 MyoD1 ntimyod1 DKO 1:10 Placental alkaline Polyclonal DKO 1:800 phosphatase NG, Not given by manufacturer. ntigen ntibody Source Dilution (clone) lpha fetoprotein C3 iogenex 1:40 CD31 JC/70 DKO 1:40 CD34 Myl 0 DKO 1:800 CD45 PD7/ DKO 1:80 CD3 Polyclonal DKO 1:40 CD5 CD5/54/4 Vector 1:4 4C7 Vector 1:100 CD43 MT1 iogenex 1:50 DFT1 DKO 1:50 CD45RO UCHL1 DKO 1:120 CD20 L26 DKO 1:200 Membranebound M2 iogenex 1:80 cell antigen CD74 LN2 iogenex 1:8 CD15 LeuM1 ecton 1:150 Dickinson CD30 erh2 DKO 1:40 ntihodgkin s L.36 DKO 1:200 disease ntilarge cell NH9 DKO 1:200 lymphoma Lysozyme Polyclonal DKO 1:400 Cathepsin Polyclonal ICN iomed 1:800 Myeloid/Histiocyte MC387 DKO 1:800 ntigen CD68 KP1 DKO 1:800 Myeloperoxidase Polyclonal DKO 1:250 Ki67 MI1 MC 1:200 PCN PC10 Novocastra 1:400 p53 DO1 Oncogene Sci 1:160 D07 DKO 1:240 Working examples of practical algorithms used in the author s laboratory are presented throughout the following chapter. The statistical data used to construct them were gathered over a period of several years using specimens that were fixed routinely in 10% neutralbuffered formalin; primary antibody incubations at 4 C for hours; the Elite avidinbiotinperoxidase complex method of immunodetection (Vector Laboratories, urlingame, C); and the antibody reagents listed in Table
4 IMMUNOHISTOLOGY OF THE MEDISTINUM IMMUNOHISTOLOGIC FINDINGS IN SPECIFIC DISESES OF THE MEDISTINUM Cystic thymoma versus cystic seminoma In many respects, cystic thymomas are morphologically quite similar to thymic cysts However, more pertinently, they may also be confused with intrathymic seminomas which manifest prominent cystic changes. 14,15 These lesions are usually separated from one another adequately by conventional microscopy, inasmuch as cystic seminoma typically displays a much greater degree of nuclear atypia than thymoma. However, in small biopsies this feature may not be clear. The periodic acid Schiff stain is helpful in delineating the glycogen content that typifies seminomas, and may be used to screen for the neoplastic cell aggregates in this particular setting. Similarly, immunostains for placental alkaline phosphatase (PLP) and with a broadly reactive mixture of monoclonal antibodies to keratin are helpful in this setting. Seminomas are uniformly PLP positive (with a distinct cellmembranous pattern of reactivity), but <15% will label for keratin On the other hand, thymoma is universally keratin positive and always lacks PLP. 17,18 Differential diagnosis of other thymoma variants The favored nosological scheme for thymomas divides them into several discrete categories based on microscopic morphology: lymphocyte predominant (>66% lymphocytes), epithelial predominant (>66% epithelial cells), mixed lymphoepithelial (34 66% epithelial cells), and spindle cell (a subtype of epithelialpredominant thymoma featuring a nearly exclusive composition by fusiform tumor cells). 17,19 22 However, it must be stated forthrightly that thymoma must be defined as a cytologically bland epithelial neoplasm in order for this system to have clinical usefulness. That utility is not one of prognostication, but rather a cue to the consideration of dissimilar differential diagnostic categories which attend each of the four major histologic categories outlined above. Salient diagnostic problems that are specific to these tumor subgroups are presented below. The distinction between thymoma and primary thymic carcinoma (which may, occasionally, arise in transition from thymoma) will be considered later in this discussion. Lymphocytepredominant thymoma versus lymphoid hyperplasia In patients with myasthenia gravis, one is asked to distinguish between true thymic hyperplasia 23 and thymoma in surgical specimens. In general, thymoma does not manifest the presence of internal lymphoid follicles, although the latter do occur rarely. In that circumstance, immunostaining for keratin reveals a finely arborizing network of interconnecting epithelial cell processes between the lymphocytes in thymoma (Fig. 10.1), which is not seen in lymphoid hyperplasia. 18,19,24 Lymphocytepredominant thymoma versus lymphoma The imitation of lymphoblastic lymphoma (LL) by selected lymphocyterich thymomas is enhanced by the peculiar features of infiltrating lymphocytes in some of the latter tumors; these may show convoluted nuclear contours, increased nucleocytoplasmic ratios, and brisk mitotic activity, 19 as typically seen in LL. Moreover, the immunophenotypes of the lymphocytes in thymomas and those of LL cells are remarkably comparable. oth populations are typically labeled for CD1a, CD2, CD3, CD5, CD43, CD99 (MIC2), and bcl2, as well as terminal deoxynucleotidyl transferase. 26,27,30 36 Con Fig Keratin in lymphocytepredominant thymoma (). Note the delicately interlocking pattern of reactivity (). 304
5 IMMUNOHISTOLOGY OF THE MEDISTINUM 10 Fig CD34 positivity () in true hemangiopericytoma () of the mediastinum. sequently, immunohistochemical distinctions between these neoplasms must be made with extreme caution. The most helpful immunostain in this differential diagnosis and one that the author, through regrettable mistakes, has made routine is an assessment of keratin reactivity. The elaborately interconnecting epithelial cells of lymphocytepredominant thymoma (LPT), which are not seen in LL, are distinctive. This pattern is essential to differential diagnosis, because LL and other lymphomas of thymus may demonstrate entrapped nonneoplastic thymic epithelial cells that are visible (but widely separated and noninterconnecting) on keratin immunostains. 5,37 Predominantly epithelial spindlecell thymoma versus fibrous histiocytoma and hemangiopericytoma Predominantly epithelial thymomas (PET) that are constituted by spindle cells may be difficult to separate diagnostically from fibrous histiocytomas (FH) or hemangiopericytomas (HPCs) by conventional histologic study. 19 Immunohistochemistry is a more discerning method toward that end, particularly when only small biopsy specimens are available for analysis. Pseudomesenchymal thymomas are universally positive for keratin and lack vimentin, 18 whereas FH and HPC show the opposite of that pattern. 38 In addition, HPC commonly demonstrates reactivity for CD34 (Fig. 10.2), 39 whereas the latter determinant is not expected in thymomas. KEY DIGNOSTIC POINTS: Thymus The elaborate keratinpositive meshwork of thymic epithelial cells is present in thymoma, but not in areas of thymic hyperplasia or lymphoma. Spindle cells of hemangiopericytoma, not thymoma, are CD34. enign peripheral nerve sheath tumors and ganglioneuromas The overwhelming majority of neoplasms encountered in the posterior mediastinum are neurogenic in nature s such, they often show morphologic similarities to one another thereby presenting diagnostic difficulties. Specifically, Schwanncell neoplasms (peripheral nerve sheath tumors; PNST) are usually subdivided into neurofibromas and neurilemmomas (schwannomas), because of their differing associations with von Recklinghausen s disease and risk of malignant transformation They also must be separated from ganglioneuromas. 41,46 ll of these proliferations are reactive for vimentin and S100 protein in a uniform manner. In fact, S100 negativity should cast serious doubt on any of the three diagnoses under discussion. Fine et al. 47 have observed that calretinin is present in most schwannomas but only a small number of neurofibromas, making that marker potentially useful in detailed diagnosis. Synaptophysin, a synaptic vesiclerelated protein that is typical of neuronal and neuroendocrine lesions, 48 is a helpful determinant for the labeling of ganglion cells (which may be focal or widely scattered) in ganglioneuromas. Fibrogenic and myofibroblastic proliferations Four cytologically bland spindlecell proliferations of the mediastinum may be mistaken for one another histologically; namely, solitary fibrous tumor (SFT), desmoidtype fibromatosis, sclerosing mediastinitis, and inflammatory myofibroblastic tumor (inflammatory pseudotumor). The immunophenotype of SFT features reactivity for vimentin and CD34, with a lack of keratin, epithelial membrane antigen, S100 protein, desmin, and actin. 305
6 IMMUNOHISTOLOGY OF THE MEDISTINUM Fig Musclespecific actin (M) () is present in the proliferating cells of this mediastinal desmoidtype fibromatosis (). Fig () This dense fibroinflammatory mass in the mediastinum has the appearance of a tumefactive fibroinflammatory lesion (fibrosing mediastinitis). However, biopsy of an adjacent lymph node () demonstrated classic ReedSternberg cells (labeled for CD30), establishing a diagnosis of the total obliterative nodular sclerosing subtype of Hodgkin s disease. In contrast, fibromatoses and inflammatory pseudotumors show a mixture of cells labeling for vimentin and musclespecific or alphaisoform actin, with or without desmin (Fig. 10.3) The distinction between the latter two lesions must therefore be made on the basis of morphologic features alone. Sclerosing mediastinitis (SM) is comprised by spindle cells that are only reactive for vimentin. However, an important caution must be remembered in reference to lesions thought to be SM. That is, selected malignant lymphomas (especially obliterative total sclerosis Hodgkin s disease 14,59 ), metastatic carcinomas, or desmoplastic mesotheliomas may engender a densely fibrotic response in the mediastinal soft tissue or lymph node groups. The actual tumor cells in such cases are consequently sparse, and may be surprisingly bland cytologically. ccordingly, they may be overlooked, leading to diagnostic mistakes (Fig 10.4) Thus, stains for keratin, CD15, CD20, CD30, and CD45 should be routine in the assessment of putative cases of SM. Malignant smallcell mediastinal neoplasms Tables 10.2, 10.3; Figures Mediastinal smallcell neuroendocrine carcinoma (grade III neuroendocrine carcinoma, smallcell type) Nearly all smallcell neuroendocrine carcinomas (SCNCs) involving the mediastinum are metastatic, 63 usually from tumors of the lungs or esophagus. Immunophenotypically, SCNC commonly demonstrates perinuclear punctate labeling for keratin (Fig. 10.9), 18 which is a specific marker of neuroendocrine lineage in a smallcell neoplasm. Less frequently, it will show reactivity for one of several neuroendocrine markers such as chromogranin, synaptophysin, CD57, or specific neuropeptides There are currently no reliable discriminants to distinguish between primary (thymic) and secondary mediastinal SCNCs; thyroid transcription factor1 (TTF1) is seen in 85 95% of pulmonary 306
7 IMMUNOHISTOLOGY OF THE MEDISTINUM 10 Table 10.2 Immunoreactants used in the differential diagnosis of small cell indeterminate and undifferentiated neoplasms of the mediastinum Keratin (monoclonal mixture) Keratin (monoclonal mixture) Epithelial membrane antigen Vimentin Desmin Musclespecific actin MyoD1 Myogenin Neuronspecific enolase Synaptophysin Chromogranin CD15 CD45 CD99 (MIC2 protein) erep4 S100 protein HM45 MRT1 Tyrosinase neuroendocrine tumors of that type, 70,71 but there are no meaningful data on the expression of that marker in primary thymic endocrine tumors. asaloid squamous cell carcinoma of the mediastinum asaloid squamous cell carcinoma (SCC) also may be either a primary thymic tumor, 68,72,73 or a mediastinal metastasis from a primary neoplasm of the oropharynx, hypopharynx, larynx, esophagus, lungs, or anorectal region. 73 Keratin is universally present in SCC with a diffuse cytoplasmic pattern of labeling, and reactivity for epithelial membrane antigen, keratin 5/6, and p63 may also be observed. 19,71,73,74 Neuroendocrine determinants are, in the author s experience, consistently absent. Neuroblastoma of the mediastinum Characteristically, neuroblastoma (NL) is a disease of young children, 42,75 and it is usually located in such patients in the posterior mediastinum. 76,77 Nonetheless, rare examples of this tumor or its congeners have also been reported in the anterior mediastinum in adults. 78,79 The immunoprofile of NL includes variable reactivity for vimentin and neurofilament protein; a substantial proportion of cases will lack both of these proteins. 80 Neural features are reflected by positivity for CD56, CD57, and synaptophysin (Fig ). 41,81 NLs are universally devoid of markers of myogenous differentiation (desmin, actin, MyoD1, myogenin), a hematolymphoid lineage (CD45) and epithelial character (keratin, epithelial membrane antigen). 52,78 N84 is a monoclonal antibody that was raised specifically against NL; although it is not specific for that neoplasm, this marker is seen in the great majority of neuroblastic tumors. 82 Mediastinal primitive neuroectodermal tumor The primitive neuroectodermal tumor (PNET) may rarely occur in the mediastinum, either in the anterior or posterior compartments. 83 The immunophenotype of PNET is similar to that of neuroblastoma, but the former of those lesions shows more uniform reactivity for vimentin and only occasionally is labeled for neurofilament protein. 38 Moreover, the CD99 (p30/32 [MIC2]) and M2 antigens and beta2microglobulin are consistently seen in PNET but not NL (Fig ) Synaptophysin, CD56, and CD57 are detectable in many cases of PNET as well, and examples of this tumor with divergent differentiation will also demonstrate focal reactivity for keratin, desmin, and actin. 38,88 Such lesions also have been termed desmoplastic small cell tumor of the peritoneum, rhabdomyosarcomalike small cell tumors of soft tissue, and ectomesenchymomas, among other designations. In some instances, it may be difficult to distinguish between a solid alveolar rhabdomyosarcoma (see below) that is MIC2 positive and a PNET with divergent rhabdomyoblastic differentiation, especially if synaptophysin is absent. In such cases, one may have to rely on cytogenetic evaluations, seeking the characteristic t(2;13) or t(1;13) chromosomal translocations of alveolar rhabdomyosarcoma or the t(11;22) translocation of PNET. nother possible avenue of discrimination is represented by immunostaining for FLI1, a nuclear transcription factor that is expressed in most PNETs. It has not been observed in histologically similar striated muscle sarcomas. 89 Rhabdomyosarcoma of the mediastinum Rhabdomyosarcoma (RMS) of the mediastinum is almost exclusively observed in children and adolescents, 41,90,91 and may demonstrate embryonal or alveolar architectural features (see Ch. 15). Nearly all rhabdomyosarcomas express desmin (Fig ) and musclespecific actin, together with vimentin. Myoglobin is observed only in large maturing rhabdomyoblasts, and is therefore 307
8 IMMUNOHISTOLOGY OF THE MEDISTINUM Table 10.3 Percentages of immunoreactivity for selected markers in malignant small cell tumors of the mediastinum with indeterminate or undifferentiated histologic features Tumor KER EM VIM DES MS MYOD1 MYOGN S100 HM45 TYR MRT1 NSE SYN CG EREP4 CD45 CD15 CD99 ES/PNET RMS LL/TL* /78 85/52 10 SCMM PNL MSCSCC MSCDC SCNC SCUS * Unless otherwise indicated, the given percentage of reactivity applies to both tumor entities. KER, keratin (mixture of monoclonal antibodies); EM, epithelial membrane antigen;vim, vimentin; DES, desmin; MS, musclespecific actin; MYOGN, myogenin; S100, S100 protein; TYR, tyrosinase; NSE, neuronspecific (gamma dimer) enolase; SYN, synaptophysin; CG, chromogranin ; PNET, primitive neuroectodermal tumor; ES, Ewing s sarcoma; RMS, rhabdomyosarcoma; LL, lymphoblastic lymphoma; TL, tumefactive acute myelogenous leukemia; SCMM, small cell malignant melanoma; PNL, peripheral neuroblastoma; MSCSCC, metastatic small cell squamous cell carcinoma; MSCDC, metastatic small cell adenocarcinoma; SCNC, small cell neuroendocrine carcinoma; SCUS, small cell undifferentiated sarcoma. Data from Frisman D. Immunoquery. vailable at and the author s experience. Divergent PNET Small cell neuroendocrine carcinoma Metastatic small cell adenocarcinoma DES/MS/MyoD1/MyG NSE/SYN/CG CD15/erEP4 Malignant lymphoma or leukemia Malignant melanoma Metastatic small cell squamous carcinoma CK CD45 S100/HM45/ EM MRT1/TYR VIM Rhabdomyosarcoma PNET/ Ewing s tumor DES/MS/MyoD1/MyG NSE/SYN/CG Technically inadequate specimen Undifferentiated sarcoma NSE/SYN/CG/MIC2 Peripheral neuroblastoma (may be positive for neurofilament protein) Fig lgorithm for immunohistologic evaluation of malignant smallcell tumors of the mediastinum. 308
9 IMMUNOHISTOLOGY OF THE MEDISTINUM KER EM SYN CG NSE MIC2 PNET SCNC PNET RMS SCNC Fig Markers of interest in the differential diagnosis of primitive neuroectodermal tumor versus smallcell neuroendocrine carcinoma of the mediastinum. 100 Fig Relative rates of positivity for CD99 (MIC2) in primitive neuroectodermal tumor versus rhabdomyosarcoma versus smallcell neuroendocrine carcinoma of the mediastinum PNET RMS DES MS MyoD1 MYOGN Fig Markers of interest in the differential diagnosis of primitive neuroectodermal tumor versus rhabdomyosarcoma of the mediastinum. not a particularly useful marker of RMS in its purely smallcell form. Synaptophysin is lacking in RMS, but some cases do demonstrate labeling for CD56, CD57, or MIC2. 38,52,85,86,92 The specificity of desmin and actin for the diagnosis of RMS could be challenged, because these determinants may also be seen in smoothmuscle neoplasms. Despite that truism, this argument seems superfluous to the author because a smallcell variant of leiomyosarcoma does not exist. In any event, nuclear proteins which are apparently restricted to striated muscle namely, MyoD1 and myogenin 92,93 can be applied effectively to the differential diagnosis in question. Fig Characteristic perinuclear dots of immunoreactivity for keratin (K) are evident in this smallcell neuroendocrine carcinoma of the mediastinum. Smallcell malignant lymphomas of the mediastinum Several smallcell nonhodgkin s lymphomas (SCNHLs) may be observed in the mediastinum as primary lesions. These include lymphoblastic lymphoma (LL) (see above), small noncleaved cell (urkitt s/nonurkitt s) lymphoma (SNCL), 97,98 and lymphomas of the mucosaassociated lymphoid tissue (MLTomas). 99,100 Immunohistochemical analysis is helpful in separating between these tumor types diagnostically. They usually express the CD45 (leukocyte common) antigen, although uncommon examples of LL lack that marker. LL also is commonly labeled with CD43 reagents (L60, Leu22, MT1); CD99 antibodies such as H71, O13, or 12E7; anticd10 (common acute lymphoblastic 309
10 IMMUNOHISTOLOGY OF THE MEDISTINUM Fig Diffuse reactivity for synaptophysin (SYN) () in mediastinal neuroblastoma (). Fig Labeling for CD99 (MIC2) () in primitive neuroectodermal tumor of the mediastinum (). but keratin, CD56, CD57, synaptophysin, desmin, actin, MyoD1, and myogenin are not detectable in any of these three SCNHLs. Roughly 50% are positive for vimentin. 104 Fig Immunoreactivity for desmin in rhabdomyosarcoma of the mediastinum. leukemia antigen); and antibodies to bcl2 protein and TdT (Fig ). 27 SNCL expresses CD20, with or without bcl2 protein. 27 In MLTomas, reactivity for CD20 and CD79a is evident, but CD10, CD43, CD99, bcl2, and TdT are absent CD5 is variably present, Other smallcell mediastinal neoplasms In addition to those smallcell tumors presented in the foregoing sections, others of a metastatic nature also may involve the mediastinum. These include smallcell osteosarcoma and Ewing s sarcoma of bone, as well as smallcell malignant melanoma. Except for the last of these possibilities, the primary lesion in such cases is typically obvious and there is no question of whether the intrathoracic neoplasm might have arisen there. Nonetheless, melanomas are certainly capable of producing distant metastasis in the absence of an obvious primary source. Furthermore, they may assume the guise of a smallcell neoplasm, closely resembling SCNC. 105 Immunohistochemical characteristics of smallcell melanomas include uniform labeling for S100 protein, tyrosinase, MRT1, and the HM45 antigen, 105,106 none of which is expected in other smallcell neoplasms of the mediastinum. 310
11 IMMUNOHISTOLOGY OF THE MEDISTINUM 10 Table 10.4 Immunoreactants used in the differential diagnosis of large cell indeterminate and undifferentiated neoplasms of the mediastinum Keratin (monoclonal mixture) Vimentin Synaptophysin Chromogranin CD15 CD30 CD45 Placentalike alkaline phosphatase Fig Nuclear labeling for terminal deoxynucleotidyl transferase in lymphoblastic lymphoma of the thymus. Large polygonalcell neoplasms of the mediastinum Tables 10.4, 10.5; Figures ) Primary thymic carcinomas lthough primary thymic carcinoma (PTC) is an exciting diagnosis because of its rarity, it should be remembered that most neoplasms thought to represent that entity will ultimately prove to represent metastases. Immunohistochemical analysis of PTCs reveals uniform labeling for keratin and p63, 107 and many cases also Carcinoembryonic antigen erep4 Calretinin S100 protein HM45 Tyrosinase MRT1 Malignant melanoma S100/HM45/MRT1/TYR CD15/CD30 PLP Germ cell tumor SYG/CG CD45 Malignant lymphoma (including Hodgkin s disease) or leukemia Paraganglioma Nonneuroendocrine carcinoma VIM Keratin erep4/ce Sarcoma SYG/CG Neuroendocrine carcinoma Technically inferior specimen Mesothelioma Calretinin Nonneuroendocrine carcinoma Fig lgorithm for immunohistologic evaluation of malignant large polygonalcell tumors of the mediastinum. 311
12 IMMUNOHISTOLOGY OF THE MEDISTINUM Table 10.5 Percentages of immunoreactivity for selected markers in malignant large polygonal cell tumors of the mediastinum with indeterminate or undifferentiated histologic features Tumor KER CE VIM CLRET PLP S100 HM45 TYR MRT1 SYN CG EREP4 CD45 CD15 CD30 PTDC MDC PNEC MNEC LCL/TL* 0 0/ /85 3/85 23/3 LCL SYNHD MELN SEMIN EMC YST EPSRCS a V V 0 V V PSCC MSCC LELCT MESOTH PRGNG * Unless otherwise indicated, the given percentage of reactivity applies to both tumor entities. a Epithelioid synovial sarcoma is reactive for keratin in 100% of cases and erep4 in 90% of cases. Epithelioid malignant peripheral nerve sheath tumor is reactive for S100 protein in 80% of cases. V, variable, usually postitive. KER, keratin (mixture of monoclonal antibodies); CE, carcinoembryonic antigen;vim, vimentin; CLRET, calretinin; PLP, placental alkaline phosphatase; S100, S100 protein; TYR, tyrosinase; SYN, synaptophysin; CG, chromogranin ; PTDC, primary thymic adenocarcinoma; MDC, metastatic adenocarcinoma; PNEC, primary neuroendocrine carcinoma; MNEC, metastatic neuroendocrine carcinoma; LCL, large cell lymphoma; TL, tumefactive acute myelogenous leukemia; LCL, anaplastic large cell lymphoma; SYNHD, syncytial Hodgkin s disease; MELN, malignant melanoma; SEMIN, seminoma; EMC, embryonal carcinoma;yst, yolk sac tumor; EPSRCS, sarcomas with epithelioid features; PSCC, primary thymic squamous cell carcinoma; MSCC, metastatic squamous cell carcinoma; LELCT, lymphoepitheliomalike carcinoma of the thymus; MESOTH, mesothelioma; PRGNG, malignant paraganglioma. Data from Frisman D. Immunoquery. vailable at and the author s experience. express epithelial membrane antigen (EM). Carcinoembryonic antigen, secretory component, G8, MOC31, calretinin, HME1, erep4, and the TG72 antigen are variably seen as well, especially in tumors that show partial or uniform glandular differentiation. 103 However, vimentin, thrombomodulin, WT1 protein, and TTF1 are characteristically undetectable in polygonalcell PTC variants. 18,104,107,108 potential pitfall in interpretation is represented by the socalled hepatoid variant of PTC, which comprises sheets of large oncocytoid cells like those of metastatic hepatocellular carcinoma (MHCC). 109 Indeed, hepatoid thymic carcinoma and MHCC share potential reactivity for HepPR1, which is usually regarded as a hepatocytic marker. 110 Several reports have been made on the expression of CD5 by the epithelial cells of thymic carcinoma but not those of conventional thymoma (Fig ) ,111 This statement must be qualified in part, because atypical epithelialpredominant thymomas that is, those in which there is evidence of cytologic atypia that is insufficient for an outright diagnosis of malignancy 17,21,40 also show CD5 positivity in 40% of cases. 106 Saad et al. 108 also found that the majority of primary poorly differen 312
13 IMMUNOHISTOLOGY OF THE MEDISTINUM CLRET CE erep 4 0 KER SYN CG Carcinoma Mesothelioma NEC PRGNG Fig Markers of interest in the differential diagnosis of carcinoma versus mesothelioma erep4 CE S100 SYN CG DC NEC Fig Markers of interest in the differential diagnosis between poorly differentiated adenocarcinoma and neuroendocrine carcinoma of the mediastinum. tiated lung carcinomas (the principal differential diagnostic alternative for PTC) also were CD5 reactive. Some variability exists in the literature concerning mutant p53 protein as another potential discriminant between thymoma and thymic carcinoma In general, however, it can be stated that immunostains done with the DO1 and DO3 antibodies against mutant p53 are much more likely to yield positive results in PTC than in conventional thymoma. Hence, this determinant could serve as an adjunct in making the diagnostic distinction between those two entities. Similar claims have been made for Mcl1 protein 115 and the Fas antigen, 116 but data on those reactants in thymic neoplasms are scarce. Other primary malignant tumors of the thymic region, such as germ cell tumors and lymphomas, are Fig Relative reactivity patterns for neuroendocrine carcinoma and malignant paraganglioma of the mediastinum KER S100 CD45 PLP Carcinoma Melanoma LCL Seminoma Fig Markers of interest in the differential diagnosis of carcinoma versus metastatic melanoma versus largecell non Hodgkin s lymphoma versus seminoma of the mediastinum. typically CD5 negative. 105,106,111 Future studies will be necessary to determine whether such observations withstand the test of time. On the other hand, it has been found that MIC2positive lymphocytes are lacking in both PTCs and metastatic carcinomas in the thymic region in the majority of cases, indicating that CD99 has no role in making the distinction between those neoplasms. 25 nother facet of PTCs that should be mentioned is their capacity for occult neuroendocrine differentiation. Even though there may be no overt morphological evidence of neuroendocrine features in such lesions, immunoreactivity may be observed for synaptophysin, 313
14 IMMUNOHISTOLOGY OF THE MEDISTINUM chromogranin, CD56, or CD57 (Fig ). 117 The biological significance of those findings is currently uncertain, but they are not sufficiently compelling to change the diagnostic classification of these tumors to that of outright neuroendocrine carcinoma. KEY DIGNOSTIC POINTS: Primary Thymic Carcinoma Keratin and P63. CD5 typically positive. TTF1 and WT1 are both negative. Parathyroid carcinoma of the mediastinum Parathyroid carcinoma (PC) may be seen intrathymically or in the soft tissue of the anterosuperior mediastinum. Its resemblance to thymic neuroendocrine carcinoma is considerable in some cases, and paraganglioma also enters into differential diagnosis The diagnosis of malignant parathyroid lesions is typically straightforward clinically, because of the striking levels of hypercalcemia with which they are associated. Nevertheless, nonsecretory PCs may require immunohistologic evaluation for definitive diagnosis. This can be accomplished through documenting the intracellular presence of parathyroid hormone, which is restricted to parathyroid lesions among the contextual diagnostic possibilities (Fig ). 121 Otherwise, the immunophenotypes of PC and other neuroendocrine carcinomas are largely superimposable. 120 Malignant mediastinal germ cell tumors Pure or mixed mediastinal germ cell tumors with seminomatous, embryonal carcinomatous, endodermal sinus tumor, and choriocarcinomatous elements all have the potential to arise in the mediastinum or involve it metastatically. 15,16, Immunohistology is often indispensable in the characterization of such neoplasms, especially in limited tissue samples. The typical phenotype of seminoma is that of a keratin and EMnegative tumor with uniform, cellmembranebased reactivity for CD117 and PLP (Fig ). 16,127,128 pproximately 10 15% of such lesions, however, will indeed demonstrate limited labeling for keratin proteins. 16 Embryonal carcinomas and yolk sac carcinomas differ from the latter description in their acquisition of intense, diffuse keratin positivity and potential labeling for alpha fetoprotein (FP). 16,125,129 In addition, embryonal carcinoma paradoxically manifests the presence of CD30 (Fig ), 130 which is typically conceptualized as a hematopoietic determinant. Choriocarcinoma is also globally keratin reactive, but that neoplasm is further typified by the immunohistologic presence of EM and betahuman chorionic gonadotropin. 16,131 Fig Diffuse immunoreactivity for CD5 in primary thymic carcinoma. KEY DIGNOSTIC POINTS: Mediastinal Germ Cell Tumors Seminoma is CD117, PLP, keratin (rarely focally ). Embryonal carcinoma keratin, CD30; yolk sac tumor keratin, FP, choriocarcinoma keratin, EM. Mediastinal carcinoid tumor (neuroendocrine carcinoma, grades I and II) Immunohistochemically, neuroendocrine carcinomas of the thymus show reproducible positivity for keratin, neuronspecific (gammadimeric) enolase, synaptophysin, CD56, CD57, and chromogranin. 18, Furthermore, even those lesions that have not produced a clinical endocrinopathy can show, at an intracellular level, the presence of specific neuropeptides Mediastinal paragangliomas Intrathoracic paragangliomas (PGs) may arise in either the anterior mediastinal compartment, in association with the aorticopulmonary root, or a paravertebral location. 135,139,140 The neural nature of paragangliomas is reflected by their lack of labeling for keratin and EM. They instead express neurofilament protein, with or without vimentin, in likeness to NL. 135 Stains for S100 protein can be used to label sustentacular cells that surround cellular nests in PGs (Fig ), 141 and the tumor cells themselves often contain one of the enkephalin peptides. 142 Labeling for chromogranin is universal in these neoplasms. 314
15 IMMUNOHISTOLOGY OF THE MEDISTINUM 10 Fig Occult labeling for synaptophysin (S) () in a primary thymic carcinoma that did not have neuroendocrine characteristics by conventional morphologic study (). Fig Immunoreactivity for parathyroid hormone (PTH) () in primary mediastinal parathyroid carcinoma (). Fig Membranebased immunolabeling for placental alkaline phosphatase (plap) () in primary mediastinal seminoma (). 315
16 IMMUNOHISTOLOGY OF THE MEDISTINUM Mediastinal largecell nonhodgkin s lymphoma Table 10.6; Figure fter Hodgkin s disease, largecell nonhodgkin s lymphoma (LCNHL) is the next most common primary malignancy of the mediastinum. 104 Immunohistology reveals crisp cellmembranous reactivity for CD45 in virtually all LCNHLs. 37,104, However, rare examples of Ki1 (CD30) (largecell anaplastic) lymphoma have been reported at this site, 147 some of which have been CD45 negative. Therefore, it is prudent to evaluate the possible presence of CD30 in the assessment of possible LCNHLs; in the context of simultaneous keratin negativity, that marker is specific for a diagnosis of lymphoma. 104 The belief that most mediastinal LCNHLs show cell differentiation is supported by reactivity for CD20, PX5, and CD79a in most instances (Fig ), 145,146,148,149 including those with anaplastic features. 147 Only exceptional LCNHLs with Tcell or true histiocytic differentiation have been reported in the mediastinum. 104 Fig Diffuse positivity for CD30 in thymic embryonal carcinoma. Syncytial mediastinal Hodgkin s disease Hodgkin s lymphoma (HL) is the most common cytologically malignant mediastinal neoplasm. 104 lthough it is felt to arise in the thymus or perithymic lymph nodes in the thorax, this lesion also may involve other contiguous structures by direct extension Most examples of HL are recognizable without the need for immunohistology, but one of its variants, syncytial HL, in which mononuclear ReedSternberg cells are arranged in sheets, may closely simulate the appearance of a carcinoma or LCNHL. 153 The typical immunophe Fig Labeling of sustentacular cells for S100 protein () and chromogranin () in mediastinal paraganglioma (C). S 100 protein tends to be lost when tumors of this type acquire overtly malignant biological properties. C 316
17 IMMUNOHISTOLOGY OF THE MEDISTINUM 10 Table 10.6 Immunoreactants used in the differential diagnosis of hematopoietic diseases of the mediastinum Keratin HM45 MRT1 Tyrosinase Placentalike alkaline phosphatase CD3 CD15 CD20 CD30 CD43 CD45 CD45RO CD68 CD74 M2 L.36 NH9 Cathepsin Lysozyme Myeloperoxidase notype of the ReedSternberg cells of HL is that of CD45 negativity, in contrast to its presence in almost all cases of LCNHL. 18,104 On the other hand, Reed cells in syncytial HL coexpress CD15 and CD30 (Fig ). CD15 is not seen in most LCNHLs, enabling a distinction to be made between these tumor types. 104 Nonetheless, it must be acknowledged that there is a potential overlap between Hodgkin s lymphoma and selected examples of CD30 LCNHL. This makes cytogenetic studies particularly for abnormalities at the 5q35 locus, which typify Ki1 largecell lymphomas 154,155 a wise inclusion in this context. In reference to its distinction from carcinomas in the mediastinum, syncytial HL uniformly lacks keratin, 18,104,153 unlike malignant epithelial neoplasms. Other mediastinal hematopoietic tumors Two other hematopoietic neoplasms that may present in the mediastinum are represented by granulocytic sarcoma (extramedullary myelogenous leukemia) 156,157 and extraosseous plasmacytoma. 158,159 Immunoreactivity for CD15, CD33, CD34, CD68, and myeloperoxidase is expected in granulocytic sarcoma but not LCNHL (Fig ) Extraosseous plasmacytoma of the mediastinum (EPM) can potentially imitate the microscopic appearance of neuroendocrine neoplasms, as well as that of largecell lymphomas. 158,159 EPM is reactive for lightchain immunoglobulins (Fig ), CD38, and CD138 (syndecan1), 163 but not for keratin, chromogranin, or synaptophysin. 164 special diagnostic trap attending this tumor is its potential to express an EMlike substance; 165 for the unwary, this result may appear to support a mistaken interpretation of neuroendocrine neoplasia. Malignant epithelioid mesothelioma of the mediastinum lthough malignant mesotheliomas are usually regarded as tumors of the peripheral pleurae or the peritoneum, they also can be seen in the mediastinum, where they likely take origin from the hilar reflections of the pleural surfaces. The immunophenotype of mesothelioma features intense keratin reactivity in all of its histologic variants, including the purely epithelioid form, and the same is true of calretinin. 166 Vimentin coexpression also may be seen in roughly 50% of mesothelioma cases, and there is also heterogeneous (and not entirely specific) labeling for such determinants as HME1 167 and thrombomodulin. 168 Specialized markers of carcinomatous differentiation, including CE, CD15, p63, TTF1, blood group (e.g.,,, H, and Lewis) antigens, and the C724 antigen (recognized by antibody 72.3), are absent in mesotheliomas Metastatic mediastinal carcinoma and melanoma s stated earlier in this discussion, most nonhematopoietic malignancies of the mediastinum should be presumed metastatic until proven otherwise. Immunohistologic analysis is only variably productive in establishing a site of origin for secondary carcinomas in this location. If determinants are found that are unassociated with PTCs, such as TTF1, thyroglobulin, prostatespecific antigen, S100 protein, PLP, C 199 (an enteric carcinoma marker), or C 125 (a serosal and müllerian tract marker), 172 it is likely that the lesion being studied is a metastasis. Conversely, the presence of coexpression of keratin 5/6, p63, and CD5 would, at least tentatively, appear to support a thymic origin for such a neoplasm. 111 Mediastinal implants of an amelanotic malignant melanoma rarely represent the initial manifestation of that tumor, 173 in the face of no detectable cutaneous or mucosal disease. In that scenario, the differential diagnosis would also include primary or metastatic somatic 317
18 IMMUNOHISTOLOGY OF THE MEDISTINUM Non hematopoietic neoplasm or Langerhans cell histiocytosis (positivity for cell S100 protein only Hodgkin s disease vs. largecell anaplastic nonhodgin s ML CK/S100/HM45/TYR/MRT1/PLP NH9 Large cell anaplastic nonhodgin s ML CD45 CD15/CD30/CD74/L.36 Technically inadequate specimen VIM CD3/CD45RO Probable sarcoma LYSO/MPX Tcell lymphoma CD20/CD74/M2/L.36 CD43 Granulocytic sarcoma cell lymphoma True histiocytic neoplasm CD68/C NonHodgkin s ML, not otherwise specified Fig lgorithm for immunohistologic evaluation of hematopoietic neoplasms of the mediastinum. carcinomas, malignant germ cell tumors, and lymphomas. Immunohistochemical studies show that metastatic largecell melanomas of the mediastinum are devoid of keratin, EM, PLP, CD15, CD30, and CD45. Instead, they react with antibodies to vimentin, S100 protein, tyrosinase, and the MRT1 and HM45 antigens. 106,172,174 Mixed smallcell and largecell malignancies Mixed largecell and smallcell nonhodgkin s lymphoma There is still some controversy on the definition of mixed large and smallcell nonhodgkin s lymphoma (MNHL), as it is distinguished from LCNHL. The author uses the rather arbitrary criterion that no more than 30% large cells should be seen in mixed nonhodgkin s lymphomas. The immunoprofile of MNHL separates it from other malignant mixedcell neoplasms of the mediastinum. It includes reactivity for CD45 in all lesional cells, as well as positivity for CD20 in cell tumors or CD3, CD43, or CD45R0 in Tcell neoplasms. 175 Keratin is universally absent, but some p63 isoforms are variably expressed by nonhodgkin lymphomas of various types. 176 Mixedcellularity Hodgkin s disease Mixedcellularity Hodgkin s disease is superficially similar histologically to MNHL; however, the former of those lesions fails to show labeling for CD45 in the large tumor cells (Reed cells). Moreover, they also lack CD3, CD20, CD43, and CD45R0, but express CD15, with or without CD30, with a distinctive Golgi zone and cellmembranous staining pattern. 104,153,177 EM may be observed in some cases of mixedcellularity Hodgkin s disease, but keratin is consistently absent. 177 Lymphoepitheliomalike carcinoma Lymphoepitheliomalike carcinoma (LELC) of the thymus features an admixture of large epithelioid cells and small lymphocytes, in likeness to the image of classical nasopharyngeal carcinoma. ll cases of LELC are immunoreactive for keratin (Fig ), p63, and EM. Conversely, the large tumor cells are devoid of PLP, CD3, CD15, CD20, CD30, CD43, CD45, and CD45R0. 18,69 318
19 IMMUNOHISTOLOGY OF THE MEDISTINUM 10 Fig Immunoreactivity for CD45 [L= Leukocyte common antigen] () and CD20 ( 20 ) () in primary largecell lymphoma of the thymic region (C). C Fig Typical cellmembranous and Golgizone labeling for CD15 in the ReedSternberg cells of mediastinal Hodgkin s disease (L = LeuM1). Malignant spindle cell mediastinal tumors Tables 10.7, 10.8; Figures Sarcomatoid thymic carcinoma Fig Diffuse cytoplasmic reactivity for myeloperoxidase in granulocytic sarcoma of the mediastinum. Comparatively few examples of sarcomatoid thymic carcinoma (STC) have been reported. 69, Microscopically, this lesion is characterized by fascicles of fusiform and pleomorphic tumor cells, with little internal organization. Some cases, however, contain limited foci in which cohesive epithelioid cell nests are admixed with spindlecell elements. 72 iphasic STCs with carcinoidal elements have also been documented. 181 Snover et al. 72 reported an example of STC with focally welldefined rhabdomyogenic differentiation, complete with cytoplasmic crossstriations. Some observers may choose to 319
20 IMMUNOHISTOLOGY OF THE MEDISTINUM Fig Monotypic labeling for lambda lightchain immunoglobulin () and negativity for kappa lightchain () in primary plasmacytoma (C) of the mediastinum. C Table 10.7 Immunoreactants used in the differential diagnosis of spindle cell indeterminate and undifferentiated neoplasms of the mediastinum Keratin (monoclonal mixture) Epithelial membrane antigen Calretinin Vimentin Desmin Musclespecific actin lpha fetoprotein Fig Delicately interlocking reactivity for keratin (K) in primary lymphoepitheliomalike carcinoma of the thymus. label such lesions as carcinosarcomas, 182 but it is the author s opinion that they are basically epithelial in nature; i.e., metaplastic or sarcomalike carcinomas. 183 Immunohistochemically, the fusiform and pleomorphic cells of STCs express vimentin. Labeling for keratin and EM is also seen, but it may be quite focal (Fig ). 19,183 This finding opens the door to the possibility that a small biopsy specimen could fail to demonstrate any epithelial markers because of sampling artifact. Synaptophysin Chromogranin Tumors showing divergent components, such as myogenic elements, may additionally exhibit immunoreactivity for desmin, actin, myoglobin, MyoD1, or myogenin. 69,72 Obviously, those potential results underscore the difficulty of establishing a firm diagnosis of STC with limited tissue samples. 320
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Immunohistochemistry of soft tissue tumors
 Immunohistochemistry of soft tissue tumors Immunohistochemistry Major advances : antigen retrieval techniques (HIER) sensitive detection systems numerous antibodies of good quality Standardization : automated
Immunohistochemistry of soft tissue tumors Immunohistochemistry Major advances : antigen retrieval techniques (HIER) sensitive detection systems numerous antibodies of good quality Standardization : automated
Index. F Factor VIII-related antigen, see VWF FactorXIIIa, for dermatofibroma, 272-275 5-HT, see Serotonin
 A Acantholytic squamous cell carcinoma vs epithelioid angiosarcoma, 56-57 Acinic cell carcinoma of pancreas, 76-77 vs ductal adenocarcinoma, 74-75 vs islet cell tumor, 78-81 Adenomatoid tumor vs hemangioma,
A Acantholytic squamous cell carcinoma vs epithelioid angiosarcoma, 56-57 Acinic cell carcinoma of pancreas, 76-77 vs ductal adenocarcinoma, 74-75 vs islet cell tumor, 78-81 Adenomatoid tumor vs hemangioma,
Seattle. Case Presentations. Case 1. 76 year old female with a history of breast cancer 12 years ago. Now presents with a pleural effusion.
 Seattle Montreal IAP September 2006 Case Presentations Allen M. Gown, M.D. Medical Director and Chief Pathologist PhenoPath Laboratories Clinical Professor of Pathology University of British Columbia Case
Seattle Montreal IAP September 2006 Case Presentations Allen M. Gown, M.D. Medical Director and Chief Pathologist PhenoPath Laboratories Clinical Professor of Pathology University of British Columbia Case
THE PATHOLOGY OF MEDIASTINAL MASSES. Anatomic Distribution of Mediastinal Masses
 Page 1 of 5 THE PATHOLOGY OF MEDIASTINAL MASSES Dr. S. Boag 549-6666 Ext. 4190, mailto:%[email protected] 1. INTRODUCTION A wide range of process, neoplastic and non-neoplastic, can produce
Page 1 of 5 THE PATHOLOGY OF MEDIASTINAL MASSES Dr. S. Boag 549-6666 Ext. 4190, mailto:%[email protected] 1. INTRODUCTION A wide range of process, neoplastic and non-neoplastic, can produce
Immunohistochemical differentiation of metastatic tumours
 Immunohistochemical differentiation of metastatic tumours Dr Abi Wheal ST1. TERA 3/2/14 Key points from a review article written by Daisuke Nonaka Intro Metastatic disease is the initial presentation in
Immunohistochemical differentiation of metastatic tumours Dr Abi Wheal ST1. TERA 3/2/14 Key points from a review article written by Daisuke Nonaka Intro Metastatic disease is the initial presentation in
Diagnosis of Mesothelioma Pitfalls and Practical Information
 Diagnosis of Mesothelioma Pitfalls and Practical Information Mary Beth Beasley, M.D. Mt Sinai Medical Ctr Dept of Pathology One Gustave L Levy Place New York, NY 10029 (212) 241-5307 [email protected]
Diagnosis of Mesothelioma Pitfalls and Practical Information Mary Beth Beasley, M.D. Mt Sinai Medical Ctr Dept of Pathology One Gustave L Levy Place New York, NY 10029 (212) 241-5307 [email protected]
HKCPath Anatomical Pathology Peer Review and Scores : PDF version for download
 AP2003R1 http://hkcpath.org. Correspondence: [email protected] 1of 10 07/08/2003 HKCPath Anatomical Pathology Peer Review and Scores : PDF version for download AP141 Bone Marrow: Metastatic Carcinoma from
AP2003R1 http://hkcpath.org. Correspondence: [email protected] 1of 10 07/08/2003 HKCPath Anatomical Pathology Peer Review and Scores : PDF version for download AP141 Bone Marrow: Metastatic Carcinoma from
Pathology of lung cancer
 Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
Disclosures. Learning Objectives. Effusion = Confusion. Diagnosis Of Serous Cavity Effusions - Beware The Mesothelial Cell!
 Disclosures Diagnosis Of Serous Cavity Effusions - Beware The Mesothelial Cell! No Relevant Financial Relationships with Commercial Interests Syed Z. Ali, M.D. Syed Z. Ali, M.D. Associate Professor of
Disclosures Diagnosis Of Serous Cavity Effusions - Beware The Mesothelial Cell! No Relevant Financial Relationships with Commercial Interests Syed Z. Ali, M.D. Syed Z. Ali, M.D. Associate Professor of
MODERN IMMUNOHISTOCHEMISTRY
 MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
Tumour Markers. What are Tumour Markers? How Are Tumour Markers Used?
 Dr. Anthony C.H. YING What are? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer cells or
Dr. Anthony C.H. YING What are? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer cells or
Contents. 1. Introduction and Approach to Fine Needle Aspiration Cytology... 1. 2. Head, Neck, Orbit and Salivary Glands... 12
 Contents 1. Introduction and Approach to Fine Needle Aspiration Cytology... 1 Complications 1 Fine Needle Aspiration Technique 1 Evaluation of FNAC Smear 4 Cell Morphology 4 Nucleus 4 Cytoplasm 6 Background
Contents 1. Introduction and Approach to Fine Needle Aspiration Cytology... 1 Complications 1 Fine Needle Aspiration Technique 1 Evaluation of FNAC Smear 4 Cell Morphology 4 Nucleus 4 Cytoplasm 6 Background
How To Test For Cancer
 Diagnosis Of Serous Cavity Effusions - Beware The Mesothelial Cell! Effusion = Confusion Syed Z. Ali, M.D. Professor of Pathology and Radiology The Johns Hopkins Hospital Baltimore, Maryland Diagnostic
Diagnosis Of Serous Cavity Effusions - Beware The Mesothelial Cell! Effusion = Confusion Syed Z. Ali, M.D. Professor of Pathology and Radiology The Johns Hopkins Hospital Baltimore, Maryland Diagnostic
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
The develpemental origin of mesothelium
 Mesothelioma Tallinn 14.12.06 Henrik Wolff Finnish Institute of Occupational Health The develpemental origin of mesothelium Mesodermal cavities (pleura, peritoneum and pericardium ) are lined with mesenchymal
Mesothelioma Tallinn 14.12.06 Henrik Wolff Finnish Institute of Occupational Health The develpemental origin of mesothelium Mesodermal cavities (pleura, peritoneum and pericardium ) are lined with mesenchymal
Practical Effusion Cytology
 Practical Effusion Cytology A Community Pathologist s Approach to Immunocytochemistry in Body Fluid Cytology Emily E. Volk, MD William Beaumont Hospital Troy, MI College of American Pathologists 2004.
Practical Effusion Cytology A Community Pathologist s Approach to Immunocytochemistry in Body Fluid Cytology Emily E. Volk, MD William Beaumont Hospital Troy, MI College of American Pathologists 2004.
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY
 MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo, Finland 2nd Nordic Conference on Applied
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo, Finland 2nd Nordic Conference on Applied
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY
 MALIGNANT MESOTHELIOMA CLASSIFICATION MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo,
MALIGNANT MESOTHELIOMA CLASSIFICATION MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo,
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Lymphohistiocytoid Mesothelioma An Often Misdiagnosed Variant of Sarcomatoid Malignant Mesothelioma
 Anatomic Pathology / LYMPHOHISTIOCYTOID MESOTHELIOMA Lymphohistiocytoid Mesothelioma An Often Misdiagnosed Variant of Sarcomatoid Malignant Mesothelioma Hasan S. Khalidi, MD, 1 L. Jeffrey Medeiros, MD,
Anatomic Pathology / LYMPHOHISTIOCYTOID MESOTHELIOMA Lymphohistiocytoid Mesothelioma An Often Misdiagnosed Variant of Sarcomatoid Malignant Mesothelioma Hasan S. Khalidi, MD, 1 L. Jeffrey Medeiros, MD,
The evolving pathology of solitary fibrous tumours. Luciane Dreher Irion MREH / CMFT / NSOPS
 The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
Ovarian tumors Ancillary methods
 Ovarian tumors Ancillary methods Ovarian tumor course Oslo, 24-25/11/14 Prof. Ben Davidson, MD PhD Department of Pathology, Norwegian Radium Hospital, Oslo University Hospital, Oslo, Norway Division of
Ovarian tumors Ancillary methods Ovarian tumor course Oslo, 24-25/11/14 Prof. Ben Davidson, MD PhD Department of Pathology, Norwegian Radium Hospital, Oslo University Hospital, Oslo, Norway Division of
PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry. M. Praet
 PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry M. Praet Pathology of the Pleura Normal serosa: visceral and parietal layers Inflammation Neoplasia: Primary: mesothelioma
PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry M. Praet Pathology of the Pleura Normal serosa: visceral and parietal layers Inflammation Neoplasia: Primary: mesothelioma
The term undifferentiated tumor has been used in reference
 Undifferentiated Tumor True Identity by Immunohistochemistry Armita Bahrami, MD; Luan D. Truong, MD; Jae Y. Ro, MD, PhD Context. Undifferentiated tumor refers to a heterogeneous group of neoplasms with
Undifferentiated Tumor True Identity by Immunohistochemistry Armita Bahrami, MD; Luan D. Truong, MD; Jae Y. Ro, MD, PhD Context. Undifferentiated tumor refers to a heterogeneous group of neoplasms with
Outline. Workup for metastatic breast cancer. Metastatic breast cancer
 Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
Efficient Tumor Immunohistochemistry A Differential Diagnosis-Driven Approach
 Efficient Tumor Immunohistochemistry A Differential Diagnosis-Driven Approach Publishing Team Erik Tanck (production manager/designer) Joshua Weikersheimer (publisher) Copyright 2006 by the American Society
Efficient Tumor Immunohistochemistry A Differential Diagnosis-Driven Approach Publishing Team Erik Tanck (production manager/designer) Joshua Weikersheimer (publisher) Copyright 2006 by the American Society
A 70-year old Man with Pleural Effusion
 Mesothelioma Diagnosis: Pitfalls and Latest Updates S Klebe and DW Henderson Recommendations Indisputable malignant cells on cytomorphological criteria which demonstrate a mesothelial phenotype, which
Mesothelioma Diagnosis: Pitfalls and Latest Updates S Klebe and DW Henderson Recommendations Indisputable malignant cells on cytomorphological criteria which demonstrate a mesothelial phenotype, which
IMMUNOHISTOCHEMICAL APPROACHES TO THE DIAGNOSIS OF UNDIFFERENTIATED MALIGNANT TUMORS
 IMMUNOHISTOCHEMICAL APPROACHES TO THE DIAGNOSIS OF UNDIFFERENTIATED MALIGNANT TUMORS Mark R. Wick, M.D. From the Division of Surgical Pathology & Cytopathology, University of Virginia Health System, Charlottesville,
IMMUNOHISTOCHEMICAL APPROACHES TO THE DIAGNOSIS OF UNDIFFERENTIATED MALIGNANT TUMORS Mark R. Wick, M.D. From the Division of Surgical Pathology & Cytopathology, University of Virginia Health System, Charlottesville,
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD
 TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
Immunohistochemical approaches to the diagnosis of undifferentiated malignant tumors
 Available online at www.sciencedirect.com Annals of Diagnostic Pathology 12 (2008) 72 84 Review Article Immunohistochemical approaches to the diagnosis of undifferentiated malignant tumors Mark R. Wick,
Available online at www.sciencedirect.com Annals of Diagnostic Pathology 12 (2008) 72 84 Review Article Immunohistochemical approaches to the diagnosis of undifferentiated malignant tumors Mark R. Wick,
Case of the. Month October, 2012
 Case of the Month October, 2012 Case The patient is a 47-year-old male with a 3-week history of abdominal pain. A CT scan of the abdomen revealed a suggestion of wall thickening at the tip of the appendix
Case of the Month October, 2012 Case The patient is a 47-year-old male with a 3-week history of abdominal pain. A CT scan of the abdomen revealed a suggestion of wall thickening at the tip of the appendix
DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE
 DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE Ryan Granger University of Rhode Island Cytotechnology program May 2, 2015 ASCT Annual Meeting Nashville, Tennessee DESMOPLASTIC SMALL ROUND
DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE Ryan Granger University of Rhode Island Cytotechnology program May 2, 2015 ASCT Annual Meeting Nashville, Tennessee DESMOPLASTIC SMALL ROUND
Tumor Patterns. Common Morphologic Patterns in Soft Tissue Tumors. Update on Lipomatous Tumors. MFH-like. Highly cellular spindle cell pattern
 Common Morphologic Patterns in Soft Tissue Tumors John R. Goldblum, M.D. Chairman, Department of Anatomic Pathology The Cleveland Clinic Professor of Pathology Cleveland Clinic Lerner College of Medicine
Common Morphologic Patterns in Soft Tissue Tumors John R. Goldblum, M.D. Chairman, Department of Anatomic Pathology The Cleveland Clinic Professor of Pathology Cleveland Clinic Lerner College of Medicine
Changes in Breast Cancer Reports After Second Opinion. Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain
 Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Académie internationale de Pathologie - Division arabe XX ème congrès 24-26 novembre 2008 Alger. Immunohistochemistry in malignant mesotheliomas
 Académie internationale de Pathologie - Division arabe XX ème congrès 24-26 novembre 2008 Alger Immunohistochemistry in malignant mesotheliomas Françoise Thivolet-Béjui Groupement Hospitalier Est Lyon-Bron
Académie internationale de Pathologie - Division arabe XX ème congrès 24-26 novembre 2008 Alger Immunohistochemistry in malignant mesotheliomas Françoise Thivolet-Béjui Groupement Hospitalier Est Lyon-Bron
Immunohistochemistry on cytology specimens from pleural and peritoneal fluid
 Immunohistochemistry on cytology specimens from pleural and peritoneal fluid Dr Naveena Singh Consultant Pathologist Bart health NHS Trust London United Kingdom Disclosures and Acknowledgements I have
Immunohistochemistry on cytology specimens from pleural and peritoneal fluid Dr Naveena Singh Consultant Pathologist Bart health NHS Trust London United Kingdom Disclosures and Acknowledgements I have
FNA Cytology of Mediastinal Lesions. Presenters: Xiaoqi Lin, M.D., Ph.D. Ritu Nayar, M.D.
 Disclosure information The speakers have no relationship that represents a possible conflict of interest with respect to the content of this presentation. FNA Cytology of Mediastinal Lesions Presenters:
Disclosure information The speakers have no relationship that represents a possible conflict of interest with respect to the content of this presentation. FNA Cytology of Mediastinal Lesions Presenters:
Notice of Faculty Disclosure
 The Diagnosis of Malignant Mesothelioma Andrew Churg, MD Department of Pathology University of British Columbia Vancouver, BC, Canada [email protected] Notice of Faculty Disclosure In accordance with
The Diagnosis of Malignant Mesothelioma Andrew Churg, MD Department of Pathology University of British Columbia Vancouver, BC, Canada [email protected] Notice of Faculty Disclosure In accordance with
The Value of Thyroid Transcription Factor-1 in Cytologic Preparations as a Marker for Metastatic Adenocarcinoma of Lung Origin
 Anatomic Pathology / TTF-1 IN CYTOLOGY OF BODY FLUIDS The Value of Thyroid Transcription Factor-1 in Cytologic Preparations as a Marker for Metastatic Adenocarcinoma of Lung Origin Jonathan L. Hecht, MD,
Anatomic Pathology / TTF-1 IN CYTOLOGY OF BODY FLUIDS The Value of Thyroid Transcription Factor-1 in Cytologic Preparations as a Marker for Metastatic Adenocarcinoma of Lung Origin Jonathan L. Hecht, MD,
Something Old, Something New.
 Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Introduction: Tumor Swelling / new growth / mass. Two types of growth disorders: Non-Neoplastic. Secondary / adaptation due to other cause.
 Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Diagnostic Challenge. Department of Pathology,
 Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
20 Diagnostic Cytopathology, Vol 36, No 1 ' 2007 WILEY-LISS, INC.
 Utility of WT-1, p63, MOC31, Mesothelin, and Cytokeratin (K903 and CK5/6) Immunostains in Differentiating Adenocarcinoma, Squamous Cell Carcinoma, and Malignant Mesothelioma in Effusions Robert T. Pu,
Utility of WT-1, p63, MOC31, Mesothelin, and Cytokeratin (K903 and CK5/6) Immunostains in Differentiating Adenocarcinoma, Squamous Cell Carcinoma, and Malignant Mesothelioma in Effusions Robert T. Pu,
Lung Cancer. Ossama Tawfik, MD, PhD Professor, Vice Chairman Director of Anatomic &Surgical Pathology University of Kansas School of Medicine
 Lung Cancer Ossama Tawfik, MD, PhD Professor, Vice Chairman Director of Anatomic &Surgical Pathology University of Kansas School of Medicine Alexandria, Egypt July 1-1 3, 2008 OBJECTIVES Describe and
Lung Cancer Ossama Tawfik, MD, PhD Professor, Vice Chairman Director of Anatomic &Surgical Pathology University of Kansas School of Medicine Alexandria, Egypt July 1-1 3, 2008 OBJECTIVES Describe and
Thymic carcinoma: update of current diagnostic criteria and histologic types
 Seminars in Diagnostic Pathology 22, 198-212 Thymic carcinoma: update of current diagnostic criteria and histologic types Saul Suster, MD From the Department of Pathology, The Ohio State University and
Seminars in Diagnostic Pathology 22, 198-212 Thymic carcinoma: update of current diagnostic criteria and histologic types Saul Suster, MD From the Department of Pathology, The Ohio State University and
VM104 TUMORS OF THE PLEURA AND MEDIASTINUM
 VM104 TUMORS OF THE PLEURA AND MEDIASTINUM Saul Suster, MD Ohio State University Hospital Columbus, OH University of Texas MD Anderson Cancer Center Houston, Texas September 19, 2004 Page 2 of 26 THYMOMAS
VM104 TUMORS OF THE PLEURA AND MEDIASTINUM Saul Suster, MD Ohio State University Hospital Columbus, OH University of Texas MD Anderson Cancer Center Houston, Texas September 19, 2004 Page 2 of 26 THYMOMAS
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium
 Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Pathology Update THE ROLE OF IMMUNOHISTOCHEMISTRY IN THE DIFFERENTIAL DIAGNOSIS OF SOFT-TISSUE TUMORS
 Pathology Update THE ROLE OF IMMUNOHISTOCHEMISTRY IN THE DIFFERENTIAL DIAGNOSIS OF SOFT-TISSUE TUMORS Carlos A. Muro-Cacho, MD, PhD Pathology Service, H. Lee Moffitt Cancer Center & Research Institute
Pathology Update THE ROLE OF IMMUNOHISTOCHEMISTRY IN THE DIFFERENTIAL DIAGNOSIS OF SOFT-TISSUE TUMORS Carlos A. Muro-Cacho, MD, PhD Pathology Service, H. Lee Moffitt Cancer Center & Research Institute
Effusions: Mesothelioma and Metastatic Cancers
 Effusions: Mesothelioma and Metastatic Cancers Malignant Mesothelioma Incidence: 2,500 cases/year ~60-80% pts with pleural MM relationship with asbestos exposure Other risk factors: radiation, other carcinogens,
Effusions: Mesothelioma and Metastatic Cancers Malignant Mesothelioma Incidence: 2,500 cases/year ~60-80% pts with pleural MM relationship with asbestos exposure Other risk factors: radiation, other carcinogens,
Rare Thoracic Tumours
 Rare Thoracic Tumours 1. Epithelial Tumour of Trachea 1 1.1 General Results Table 1. Epithelial Tumours of Trachea: Incidence, Trends, Survival Flemish Region 2001-2010 Both Sexes Incidence Trend EAPC
Rare Thoracic Tumours 1. Epithelial Tumour of Trachea 1 1.1 General Results Table 1. Epithelial Tumours of Trachea: Incidence, Trends, Survival Flemish Region 2001-2010 Both Sexes Incidence Trend EAPC
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY
 CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
Pediatric Oncology for Otolaryngologists
 Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
PROTOCOL OF THE RITA DATA QUALITY STUDY
 PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
3-F. Pathology of Mesothelioma
 3-F. Pathology of Mesothelioma Kouki Inai Professor of Department of Pathology, Graduate School of Biomedical Science, Hiroshima University Introduction Mesothelioma is a peculiar type of malignancy, which
3-F. Pathology of Mesothelioma Kouki Inai Professor of Department of Pathology, Graduate School of Biomedical Science, Hiroshima University Introduction Mesothelioma is a peculiar type of malignancy, which
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1557/14
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1557/14 BEFORE: M. Crystal: Vice-Chair HEARING: August 20, 2014 at Toronto Written DATE OF DECISION: December 4, 2014 NEUTRAL CITATION: 2014
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1557/14 BEFORE: M. Crystal: Vice-Chair HEARING: August 20, 2014 at Toronto Written DATE OF DECISION: December 4, 2014 NEUTRAL CITATION: 2014
Cytology of Lymph Nodes
 Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
How To Test For Cancer With A Blood Test
 Histolab Products AB Eva Alströmer Jonas Falgén Helsingborg 7-8/10 2010 Table 1 Formalin Fixation Times and Estrogen Receptor Staining With 25 Minutes Antigen Retrieval Pretreatment Formalin Q-Score Difference
Histolab Products AB Eva Alströmer Jonas Falgén Helsingborg 7-8/10 2010 Table 1 Formalin Fixation Times and Estrogen Receptor Staining With 25 Minutes Antigen Retrieval Pretreatment Formalin Q-Score Difference
CatalogNo Product Name Size
 SIG-3250-1000 α-1-antichymotrypsin Polyclonal Antibody, Purified (SIGNET) SIG-3250-16 α-1-antichymotrypsin Polyclonal Antibody, Purified (SIGNET) L1 6mL SIG-3250-26 α-1-antichymotrypsin Polyclonal Antibody,
SIG-3250-1000 α-1-antichymotrypsin Polyclonal Antibody, Purified (SIGNET) SIG-3250-16 α-1-antichymotrypsin Polyclonal Antibody, Purified (SIGNET) L1 6mL SIG-3250-26 α-1-antichymotrypsin Polyclonal Antibody,
NEOPLASMS C00 D49. Presented by Jan Halloran CCS
 NEOPLASMS C00 D49 Presented by Jan Halloran CCS 1 INTRODUCTION A neoplasm is a new or abnormal growth. In the ICD-10-CM classification system, neoplastic disease is classified in categories C00 through
NEOPLASMS C00 D49 Presented by Jan Halloran CCS 1 INTRODUCTION A neoplasm is a new or abnormal growth. In the ICD-10-CM classification system, neoplastic disease is classified in categories C00 through
Bone Marrow Evaluation for Lymphoma. Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital
 Bone Marrow Evaluation for Lymphoma Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital Indications One of the most common indications for a bone marrow biopsy is to evaluate for malignant lymphoma.
Bone Marrow Evaluation for Lymphoma Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital Indications One of the most common indications for a bone marrow biopsy is to evaluate for malignant lymphoma.
Today s Topics. Tumors of the Peritoneum in Women
 Today s Topics Tumors of the Peritoneum in Women Charles Zaloudek, M.D. Department of Pathology 505 Parnassus Ave., M563 University of California, San Francisco San Francisco, CA USA [email protected]
Today s Topics Tumors of the Peritoneum in Women Charles Zaloudek, M.D. Department of Pathology 505 Parnassus Ave., M563 University of California, San Francisco San Francisco, CA USA [email protected]
BIOBANK LPCE-NICE CHEST
 BIOBANK LE-NIE HEST athologist : S. LASSALLE 01/03/2011 Time for frozen procedure : 10 mn LE / HU Unit atient : N LH 11-0004 N LB 11-0002 onsent : YES Age : 37 ID : TH ER Diagnosis and staging : Hodgkin
BIOBANK LE-NIE HEST athologist : S. LASSALLE 01/03/2011 Time for frozen procedure : 10 mn LE / HU Unit atient : N LH 11-0004 N LB 11-0002 onsent : YES Age : 37 ID : TH ER Diagnosis and staging : Hodgkin
Determination of the type and origin of metastatic
 Diagnosis of Metastatic Neoplasms An Immunohistochemical Approach Murli Krishna, MD N Context. It is important to determine the type and/or site of origin of metastatic tumors for optimal clinical management.
Diagnosis of Metastatic Neoplasms An Immunohistochemical Approach Murli Krishna, MD N Context. It is important to determine the type and/or site of origin of metastatic tumors for optimal clinical management.
CHAPTER 2. Neoplasms (C00-D49) March 2014. 2014 MVP Health Care, Inc.
 Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
PNL2 MELANOCYTIC MARKER IN IMMUNOHISTOCHEMICAL EVALUATION OF PRIMARY MUCOSAL MELANOMA OF THE HEAD AND NECK
 ORIGINAL ARTICLE PNL2 MELANOCYTIC MARKER IN IMMUNOHISTOCHEMICAL EVALUATION OF PRIMARY MUCOSAL MELANOMA OF THE HEAD AND NECK Luc G. Morris, MD, 1 Yong Hannah Wen, MD, PhD, 2 Daisuke Nonaka, MD, 2 Mark D.
ORIGINAL ARTICLE PNL2 MELANOCYTIC MARKER IN IMMUNOHISTOCHEMICAL EVALUATION OF PRIMARY MUCOSAL MELANOMA OF THE HEAD AND NECK Luc G. Morris, MD, 1 Yong Hannah Wen, MD, PhD, 2 Daisuke Nonaka, MD, 2 Mark D.
YOUR LUNG CANCER PATHOLOGY REPORT
 UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
Novocastra Liquid Mouse Monoclonal Antibody CD141 (Thrombomodulin)
 Novocastra Liquid Mouse Monoclonal Antibody CD141 (Thrombomodulin) Product Code: NCL-L-CD141 Leica Biosystems Newcastle Ltd Balliol Business Park West Benton Lane Newcastle Upon Tyne NE12 8EW United Kingdom
Novocastra Liquid Mouse Monoclonal Antibody CD141 (Thrombomodulin) Product Code: NCL-L-CD141 Leica Biosystems Newcastle Ltd Balliol Business Park West Benton Lane Newcastle Upon Tyne NE12 8EW United Kingdom
BIOBANK LPCE-NICE CHEST
 BIOBANK LE-NIE HEST athologist :. BUTORI 12/09/2013 LE / HU Unit atient : N LH13-3603 N LB 13-0691 ID : RO A onsent : YES Age : 54 Diagnosis and staging : chronic pleuresia 5x1000µL BIOBANK LE-NIE HEST
BIOBANK LE-NIE HEST athologist :. BUTORI 12/09/2013 LE / HU Unit atient : N LH13-3603 N LB 13-0691 ID : RO A onsent : YES Age : 54 Diagnosis and staging : chronic pleuresia 5x1000µL BIOBANK LE-NIE HEST
Interesting Case Review. Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA
 Interesting Case Review Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA History 63 y/o male with h/o CLL for 10 years Presents with worsening renal function and hypercalcemia
Interesting Case Review Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA History 63 y/o male with h/o CLL for 10 years Presents with worsening renal function and hypercalcemia
Renal Cell Carcinoma: Advances in Diagnosis B. Iványi, MD
 Renal Cell Carcinoma: Advances in Diagnosis B. Iványi, MD Department of Pathology University of Szeged, Hungary ISUP Vancouver Classification of Renal Neoplasia Am J Surg Pathol 37:14691489, 2013 13 histologic
Renal Cell Carcinoma: Advances in Diagnosis B. Iványi, MD Department of Pathology University of Szeged, Hungary ISUP Vancouver Classification of Renal Neoplasia Am J Surg Pathol 37:14691489, 2013 13 histologic
Oncology Best Practice Documentation
 Oncology Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Solid Tumors Lymphomas Leukemias Myelodysplastic Syndrome Pathology Findings
Oncology Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Solid Tumors Lymphomas Leukemias Myelodysplastic Syndrome Pathology Findings
Immunohistochemical classification of malignant lymphomas
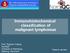 Immunohistochemical classification of malignant lymphomas Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark Thanks to Jan Klos Important issues Distinction from non-hematopoietic neoplasms
Immunohistochemical classification of malignant lymphomas Prof. Mogens Vyberg NordiQC Institute of Pathology Aalborg, Denmark Thanks to Jan Klos Important issues Distinction from non-hematopoietic neoplasms
III II II 111111111111111111111111111111111111111111 1 1111111111111 III. ge: /ears sex: Male Access
 UUID : 10F97F63 - EE6F-448D - 98E1-8AAA21F55753 TCGA - TS-A7PB-01A-PR Redacted III II II 111111111111111111111111111111111111111111 1 1111111111111 III Date Receive III 11111111111111111 11111111111 II
UUID : 10F97F63 - EE6F-448D - 98E1-8AAA21F55753 TCGA - TS-A7PB-01A-PR Redacted III II II 111111111111111111111111111111111111111111 1 1111111111111 III Date Receive III 11111111111111111 11111111111 II
The Use of Immunohistochemistry to Distinguish Reactive Mesothelial Cells From Malignant Mesothelioma in Cytologic Effusions
 The Use of Immunohistochemistry to Distinguish Reactive Mesothelial Cells From Malignant Mesothelioma in Cytologic Effusions Farnaz Hasteh, MD 1 ; Grace Y. Lin, MD, PhD 1 ; Noel Weidner, MD 1 ; and Claire
The Use of Immunohistochemistry to Distinguish Reactive Mesothelial Cells From Malignant Mesothelioma in Cytologic Effusions Farnaz Hasteh, MD 1 ; Grace Y. Lin, MD, PhD 1 ; Noel Weidner, MD 1 ; and Claire
A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on
 A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on examination. She also has fever, weight loss, and sweats. What
A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on examination. She also has fever, weight loss, and sweats. What
A Cytokeratin- and Calretinin-negative Staining Sarcomatoid Malignant Mesothelioma
 A Cytokeratin- and Calretinin-negative Staining Sarcomatoid Malignant Mesothelioma MICHAEL G. HURTUK and MICHELE CARBONE Cardinal Bernadin Cancer Center, Cancer Immunology Program, Department of Pathology,
A Cytokeratin- and Calretinin-negative Staining Sarcomatoid Malignant Mesothelioma MICHAEL G. HURTUK and MICHELE CARBONE Cardinal Bernadin Cancer Center, Cancer Immunology Program, Department of Pathology,
Renal Tumors with Eosinophilic Cytoplasm: 2013 Classification. Jesse K. McKenney, MD Associate Head, Surgical Pathology
 Renal Tumors with Eosinophilic Cytoplasm: 2013 Classification Jesse K. McKenney, MD Associate Head, Surgical Pathology Renal Epithelial Neoplasia History 1981: WHO Classification of Renal Neoplasms 1.
Renal Tumors with Eosinophilic Cytoplasm: 2013 Classification Jesse K. McKenney, MD Associate Head, Surgical Pathology Renal Epithelial Neoplasia History 1981: WHO Classification of Renal Neoplasms 1.
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
This module consists of four units which will provide the user a basic knowledge of cancer as a disease.
 Module 5: What is Cancer? This module consists of four units which will provide the user a basic knowledge of cancer as a disease. After completing this module, cancer abstractors will be able to: Define
Module 5: What is Cancer? This module consists of four units which will provide the user a basic knowledge of cancer as a disease. After completing this module, cancer abstractors will be able to: Define
Recommendations for the Reporting of Pleural Mesothelioma
 Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
New Hampshire Childhood Cancer
 Introduction: New Hampshire Childhood Cancer New Hampshire, Childhood Cancer, January 2009 Issue Brief Cancer in children is relatively uncommon, impacting fewer than twenty two of every 100,000 children
Introduction: New Hampshire Childhood Cancer New Hampshire, Childhood Cancer, January 2009 Issue Brief Cancer in children is relatively uncommon, impacting fewer than twenty two of every 100,000 children
Cytopathology Case Presentation #8
 Cytopathology Case Presentation #8 Emily E. Volk, MD William Beaumont Hospital, Troy, MI Jonathan H. Hughes, MD Laboratory Medicine Consultants, Las Vegas, Nevada Clinical History 44 year old woman presents
Cytopathology Case Presentation #8 Emily E. Volk, MD William Beaumont Hospital, Troy, MI Jonathan H. Hughes, MD Laboratory Medicine Consultants, Las Vegas, Nevada Clinical History 44 year old woman presents
NEU IM PROGRAMM. LOXO Antikörper für die Immunhistochemie (alphabetisch nach Bezeichnung sortiert) Art.Code Artikelbezeichnung Typ Einsatz Einheit
 A20002 Actin, Alpha-Smooth Muscle; Clone 1A4 monoklonal IHC 2 ml Ready-to-use A00002.0025 Actin, Alpha-Smooth Muscle; Clone 1A4 monoklonal IHC 25 ml Ready-to-use A00002 Actin, Alpha-Smooth Muscle; Clone
A20002 Actin, Alpha-Smooth Muscle; Clone 1A4 monoklonal IHC 2 ml Ready-to-use A00002.0025 Actin, Alpha-Smooth Muscle; Clone 1A4 monoklonal IHC 25 ml Ready-to-use A00002 Actin, Alpha-Smooth Muscle; Clone
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
General Rules SEER Summary Stage 2000. Objectives. What is Staging? 5/8/2014
 General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
Leukemias and Lymphomas: A primer
 Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
How To Diagnose And Treat A Tumour In An Effusion
 Effusions of the Serous Cavities Annika Dejmek Professor/Consultant in Cytopathology Clinical Pathology; Department of Laboratory Medicine, Malmö, Lund University 5th EFCS Tutorial Trondheim 2012 Pleura
Effusions of the Serous Cavities Annika Dejmek Professor/Consultant in Cytopathology Clinical Pathology; Department of Laboratory Medicine, Malmö, Lund University 5th EFCS Tutorial Trondheim 2012 Pleura
Lung Carcinomas New 2015 WHO Classification. Spasenija Savic Pathology
 Lung Carcinomas New 2015 WHO Classification Spasenija Savic Pathology ***EXPECTED SPRING 2015*** This authoritative, concise reference book provides an international standard for oncologists and pathologists
Lung Carcinomas New 2015 WHO Classification Spasenija Savic Pathology ***EXPECTED SPRING 2015*** This authoritative, concise reference book provides an international standard for oncologists and pathologists
Immunohistochemistry in diagnostic pathology of tumors. Approach, benefits, limits and pitfalls
 Aus dem Institut für Pathologie der Medizinischen Fakultät Charité Universitätsmedizin Berlin DISSERTATION Immunohistochemistry in diagnostic pathology of tumors. Approach, benefits, limits and pitfalls
Aus dem Institut für Pathologie der Medizinischen Fakultät Charité Universitätsmedizin Berlin DISSERTATION Immunohistochemistry in diagnostic pathology of tumors. Approach, benefits, limits and pitfalls
http://www.springer.com/3-540-22006-2
 http://www.springer.com/3-540-22006-2 1 Molecular Pathology Laboratory of the Future Christopher A. Moskaluk 1.1 The Past The integration of laboratory analysis with human medicine has traditionally been
http://www.springer.com/3-540-22006-2 1 Molecular Pathology Laboratory of the Future Christopher A. Moskaluk 1.1 The Past The integration of laboratory analysis with human medicine has traditionally been
