Peptic Upper Gastrointestinal Bleeding: Diagnosis and Treatment. A Monocentric Experience on a 5 Years Period
|
|
|
- Anne Kennedy
- 8 years ago
- Views:
Transcription
1 ORIGINAL ARTICLES Peptic Upper Gastrointestinal Bleeding: Diagnosis and Treatment. A Monocentric Experience on a 5 Years Period I. SPOREA 1, DANIELA LAZĂR 1, ALINA POPESCU 1, ROXANA ŞIRLI 1, A. GOLDIŞ 1, M. STRĂIN 1, ADRIANA TUDORA 1, MIRELA DĂNILĂ 1, V. DĂNILĂ 1, CORINA VERNIC 2 1 Department of Gastroenterology and Hepatology, 2 Department of Medical Biostatistics, University of Medicine and Pharmacy Timişoara, Romania Aim. We evaluated all the cases of upper gastrointestinal hemorrhages admitted in the Department of Endoscopy of our Clinic during a 5 years period. Material and method. 810 patients were included in our study, 64.3% males and 36.7% females, mean age 58.7±15.2 years (17 96 years). The main cause of the upper digestive hemorrhage was peptic ulcer (82.6%), equally divided in gastric and duodenal. All the ulcers were assessed according to the Forrest classification. Results. Endoscopic haemostasis was performed in 40% of all cases, only epinephrine injection (1/10,000) in 44.4% of cases; combined therapy (injection + clip or thermocoagulation) in 40.3% of the cases and clip or thermocoagulation alone in 15.3% of the cases. A marked reduction of haemostasis using epinephrine injection alone (as monotherapy) was observed during the period of study. Postendoscopic treatment rebleeding occurred in 19.8% of cases; 3.6% of the patients have had a fatal outcome and surgical treatment was needed in 2.7% of cases. Conclusion. In an experienced Department of Endoscopy, the majority of upper gastrointestinal hemorrhages can be endoscopically treated with good results. In the last years, endoscopical haemostatic bitherapy (adrenaline injection+clipping or bipolar coagulation) replaced injection of adrenaline like monotherapy for ulcer hemostasis. Key words: upper gastrointestinal hemorrhage, etiology, endoscopic haemostasis. Despite the progresses made in the last decade in the technique of endoscopic haemostasis, the non-variceal upper digestive bleeding (UDB) still remains a very important cause of death. The fatality rate in these cases is 5 10%, linked either to the severity of bleeding, or to the co-morbidities, more frequent in elder patients [1 3]. The role of emergency endoscopy is well defined in UDB: it must be performed in a hemodynamic stable patient, aimed at finding the source of bleeding and performing endoscopic haemostasis [4]. The main causes of non-variceal UDB are duodenal and gastric ulcers, but there are other conditions that may generate important blood loss (e.g. Dieulafoy lesion). The ever growing consumption of non-steroidal anti-inflammatory drugs (NSAID s) and aspirin, especially popular among the elderly, is the main cause of ulcers [5]. Also, Helicobacter pylori (Hp) related ulcers can sometimes lead to UDB in areas in which the prevalence of this infection is still rather high. Lately, therapeutic strategies began to be standardized for bleeding ulcers. Since Calvet s meta-analysis has been published in 2004 [6], the combined treatment, epinephrine injection (EI) + clip placement or thermal coagulation, is the standard of care regarding endoscopic treatment in bleeding ulcers (Forrest I or II), opposed to EI alone. The choice of the endoscopic technique that should be associated to EI, thermal coagulation or clip placement, is still subject of debate [7]. The aim of our study was to assess the main causes of non-variceal UDB cases addressed to the Department of Endoscopy from the Gastroenterology Clinic in Timişoara, as well as the haemostasis techniques that were used for haemorrhagic ulcers and their results, during a 5 years period. Most of the UDB cases from the South-Western part of Romania are addressed to the Department of Gastroenterology from the County Emergency Hospital Timişoara, where a total of 36,360 emergency case presentations were recorded in 2003; 40,794 in 2004; 49,800 in 2005; 51,650 in 2006 and 51,164 in ROM. J. INTERN. MED., 2009, 47, 4,
2 348 I. Sporea et al. 2 MATERIAL AND METHOD We retrospectively analyzed all the non-variceal UDB cases hospitalized in the Department of Gastroenterology of the County Emergency Hospital Timişoara, between January 1 st 2003 and December 31 st 2007, in order to analyze the frequency of bleeding from ulcers, the therapy employed for haemostasis for bleeding ulcers and the posttherapeutic results. On our batch we have assessed the following parameters: age, gender, type of lesion, number of ulcers, type of endoscopic haemostasis, signs of shock (systolic blood pressure-sbp, pulse rate-pr), hemoglobin value, number of administered blood units, use of NSAIDs or anticoagulation treatment, endoscopic second look, rate and moment of rebleeding, endoscopic treatment in case of rebleeding, number of hospitalization days, need of surgery and rate of deaths. All the ulcer lesions were classified using Forrest classification [8] and Rockall score was used [9]. RESULTS A number of 810 successive patients with non-variceal UDB were included in our study. Most of the patients were male 513 (64.3%) and 297 (36.7%) were female, with a mean age of 58.7±15.2 years (ranging from 17 to 96 years old). The main cause of UDB was ulcer, found in 82.6% of the cases (669 patients). In 17.4% cases (141 patients) other types of lesions were the cause of bleeding. THE GROUP OF PATIENTS WITH BLEEDING PEPTIC ULCERS From the 810 patients with UDB, in 669 (82.6%) cases gastric or duodenal ulcers were the cause of hemorrhage. From the 669 ulcers, 45% (301 patients) were gastric ones, 44.1% (295 patients) were duodenal and in 9.7% of the cases (65 patients) both gastric and duodenal ulcers were present. In a smaller number of cases 1.2% (8 patients) the ulcer occurred on an operated stomach. Out of the total of 669 patients with ulcer, 432 (64.6%) were male and 237 (35.4%) were female. In patients with UDB caused by ulcers, the mean age was 59.0±15.2 years (ranging from 17 to 96 years). In 47.5% (317 patients) of the cases, bleeding occurred in patients older than 60 years, a category of patients in which co-morbidities are often present. According to the age group, the bleeding ulcers occurred in: 20 years 7 cases (1%); years 30 cases (4.5%); years 42 cases (6.3%); years 101 cases (15%); years 172 cases (25.7%); years 147 cases (22%); years 128 cases (19.2%); years 40 cases (6.0%); > 90 years 2 cases (0.3%). (Fig. 1) Fig. 1. Distribution on age groups of patients with bleeding ulcer.
3 3 Peptic upper gastrointestinal bleeding 349 According to the Forrest classification, the hemorrhagic ulcers were (Fig.2): type I: 127/669 cases (19%) I a: 32/669 cases (4.8%); I b: 95/669 cases (14.2%); type II: 275/669 cases (41.1%) II a: 125/669 cases (18.7%); II b: 99/669 cases (14.8%); II c: 51/669 cases (7.6%); type III: 267/669 cases (39.9%). The mean Rockall score for these patients was 5.04±2.38 (ranging from 1 to 16 points). Regarding the drug-related etiology of ulcer, aspirin intake was blamed in 180 of the cases (26.9%), NSAID s in 35 of the cases (5.2%), 34 patients (5%) followed a chronic anticoagulant treatment, and 4 (0.6%) patients were treated with prednisone. In patients with ulcerous UDB, 2.7% of the cases (18/669 patients) had to be referred to surgery because the hemorrhage could not be managed by endoscopic therapy. Unfortunately 3.6% of the cases with ulcerous UDB died (24 of the 669 patients). THE ENDOSCOPIC THERAPY After the initial endoscopic assessment of the UDB, in patients with Forrest type Ia, Ib, IIa, and IIb endoscopic lesions, endoscopic haemostasis was performed. Either monotherapy, or combined treatment were performed. Fig. 2. Ulcers repartition according to the Forrest classification. In 268 patients (40.0% of cases) with bleeding ulcer, endoscopic therapy was performed, either monotherapy (EI) in 160 of the cases, or combined in 108 of the cases. Second look endoscopy was performed in 409 cases (61.1%), most frequently in the first 24 hours after the first endoscopy. Posttherapeutic rebleeding occurred in 53/268 cases (19.8%), mostly in the first 24 hours (21 cases), in 31 cases in the first 8 days after admission, only in one case it occurred 17 days after the first bleeding. Concerning the hemodynamic status of the patients, signs of hypovolemic shock were also searched for. SBP < 100 mmhg was observed in 99 patients (14.8%), and PR>100 bpm in 138 patients (20.6%). The mean level of Hb was of 10.60±30.8 g% (with a minimum of 3 g%), and the average number of blood units that were administered to these patients was of 2.35±1.43/patient (ranging from 1 to 9 units/patient). Blood was administered in 285 patients (42.6%). In the group of patients with ulcerous UDB, a mean number of 5.94±3.63 hospitalization days were needed (ranging from 1 to 40 days). Mono-therapy (n=160 patients) The following techniques were used as monotherapy during the first therapeutic endoscopy (Fig. 3): Epinephrine injection (EI) 1/10,000 in 119/160 of the cases (74.4%); Thermal coagulation (TC) 29/160 of the cases (18.1%); Clip placement (CP) 10/160 of the cases (6.2%); Banding ligation (B) 1/160 of the cases; Argon plasma coagulation (APC) 1/160 of the cases. In the majority of cases (74.4%), epinephrine injection 1/10,000 was used as mono-therapy. The mean volume of injected epinephrine solution was 8.52±4.43 ml/patient, ranging from 1 to 30 ml. Combined therapy (n=108 patients) The following therapeutic combinations were used (Fig. 4): EI + TC 73 cases (67.6%); EI + CP 22 cases (20.4%); Triple therapy: EI + TC + CP 9 cases (8.3%); TC + CP 3 cases (2.8%); EI + TC + APC 1 case (0.9%). Therefore, as a combined therapy, in approximately 2/3 of the cases association between EI and the TC was used.
4 350 I. Sporea et al. 4 Fig. 3. Techniques used as mono-therapy in UDB. Fig. 4. Combined techniques used for haemostasis in UDB. If further therapeutic endoscopy was needed (62 cases), the haemostatic technique most frequently used was EI (16 cases 25.7%), followed by the EI + TC combination (14 cases 22.6%) and TC alone (14 cases 22.6%), and CP combined or not with EI (6 cases 9.7% mono-therapy and 6 cases 9.7% of combined therapy. Sometimes, all three techniques were used (6 cases 9.7%). Concerning the use of adrenaline injection (119 cases = 44.7%) vs. definitive therapy (147 cases= 55.3%) we obtained the following results: Epinephrine injection (1/10,000) in 119 cases; Definitive therapy (combined therapy or directly TC or CP) in 147 cases from which: EI + TC: 73 cases (49.6%) EI + CP: 22 cases (14.9%) CP: 10 cases (6.8%) TC: 29 cases (19.7%) EI + TC + CP: 9 cases (6.2%) TC + CP: 3 cases (2.1%) EI + TC + APC: 1 case (0.7%) Regarding the type of endoscopic treatment, we noticed a statistically significant decrease in the number of epinephrine injections between 2003 and % vs. 21.5% (p< ES) (Table I, Fig. 5). Table I Types of endoscopic treatment during the analyzed period Year Epinephrine injection alone Number of patients (%) Combined treatment (two or more techniques) + Definitive treatment (89.2%) 6 (10.8%) (51.1%) 22 (48.9%) (42.6%) 35 (57.4%) (14.6%) 35 (85.4%) (22.2%) 49 (77.8%) Fig. 5. The trend of the endoscopic treatment during time.
5 5 Peptic upper gastrointestinal bleeding 351 DISCUSSION The Endoscopy Department of the Gastroenterology Clinic in Timişoara receives a great number of the UDBs from Timiş County, but also from the neighboring areas. The emergency endoscopy service is manned by 5 up to 12 senior and junior endoscopists (fellows of gastroenterology in the last two years), depending on the analyzed period. The endoscopies were performed during working hours, or on call, out of working hours. The patients have been haemodynamically stabilized before the endoscopy. Also, after the endoscopic haemostatic procedures, all patients received high doses of i.v. PPI s: omeprazole, esomeprazole or pantoprazole, 80 mg bolus followed by 8 mg/hour infusion for 72 hours, and then an oral PPI, 40 mg once daily for the remaining hospitalization days. This standard procedure of PPI administration after therapeutic endoscopy, in continuous infusion after a previous bolus dose, is used by most groups (10, 11). It was demonstrated that high doses of PPI following haemostasis significantly reduce the rebleeding rate (OR 0.49, 95%CI ) and the need for surgical intervention, as compared to placebo or H2 RA [11]. Also, in patients with highrisk endoscopic lesions (i.e. spurting and oozing bleeding, or non-bleeding visible vessel), postendoscopic high dose PPI infusion reduces the mortality in treated patients (OR 0.53, 95% CI ) [11][12]. It was also demonstrated [13] that PPI administration in bolus, followed by continuous infusion in the pre-endoscopic period (especially endoscopy was delayed for up to 12 hours), reduces the number of active bleedings and the number of endoscopic haemostatic procedures. In our group of 810 patients with nonvariceal UDB, the main causes of hemorrhage were, as expected, gastric and duodenal ulcers, in more than 80% of the cases. Other studies have also demonstrated ulcers to be the most frequent cause of bleeding [14], with an incidence almost equal for gastric and duodenal ulcers (29% vs. 30%), similar to our data (45% vs. 44.1%). The mean age in our patients with nonvariceal UDB was 58.7 years (ranging from 17 to 96 years), lower than in Imperiale s study (63.4 years) (15), Romagnuolo s study (66 years) (16) or than in Parente s study (67.3 years) [10]. We compared our data to other studies regarding the mean number of blood units (in our group 2.3 units/patient, ranging from 1 to 9); the mean number of hospitalization days (in our group 5.7 days); the rate of transfers to surgery (in our group 2.7% of the cases); and the mortality 3.6% in our group. In Parente s study [10], in a group of 272 patients, the mean number of blood units administered was of 1.8 and 3 units/patient (senior vs. junior endoscopists, respectively), and the transfer to the surgical department was 4% vs. 10% (senior vs. junior endoscopists), yielding an average of 5.5%. The mortality in this study was 13.2%. In Schemmer s study [14], in a group of 121 patients, the mortality rate was 14%; in Romagnuolo s study (16) in a group of 1860 patients, mortality was 5.3%. In Lau s study [13], performed on 638 patients, the mortality rate was 2.5%, the mean number of transfused blood units was 1.5, and 1.6% of the cases needed surgery. In Imperiale s study [15] performed on 391 patients, death occurred in 3.1% of the cases. As one can observe, the mortality rate and the necessity for surgery varies very much from one study to another. The mortality rate varies between 2.5% [13] and % [10][14]. This wide variation is influenced by multiple factors: the mean age of the analyzed group; the incidence of severe co-morbidities [15][17]18]; the ulcer site (high risk in bulbar ulcers of the posterior wall) [14]; the experience of the endoscopists team, [10], etc. The mortality rate in our group 3.6% of the cases in a large group of patients is a relatively low one. We think that it was positively influenced by the rather low mean age of the group. Considering the ageing population in which UDB occurs more and more often, (a fact that we obviously acknowledged in the last decade), we expect that the mortality rate will probably increase. The number of cases sent to surgery, approximately 4.7% of the cases diagnosed with non-variceal UDB, also fits within the limits of the published data. The second issue that we wish to analyze in this paper is the endoscopic haemostasis. Out of the 669 cases of UDB on ulcers, in 268 patients (approximately 40%), an endoscopic therapy was needed. The remaining ulcers did not need any endoscopic therapy, since they were type II c or III lesions according to the Forrest classification. Regarding the choice of the haemostasis technique, the decision regarding injecting epinephrine 1/10,000 alone, or using a combination of EI with a second technique (bipolar coagulation or clip
6 352 I. Sporea et al. 6 placing), each endoscopy unit has its own strategy. Calvet s meta-analysis [6] demonstrated the superiority of the combined therapy versus simple EI, so the haemostasis strategy changed in most centers (including our own). The current standard of care regarding haemostasis always includes the CP or TC. A recent meta-analysis published by Malmo in 2007, including 2472 patients [19], compared EI to EI + a second endoscopic technique. It demonstrated that combined endoscopic therapy reduces the risk of recurrent bleeding (OD=0.59 [ ], p=0.0001) and the risk of emergency surgery (OR=0.6 6[ ], p=0.03) and showed a trend toward a reduction of the death risk (OR=0.68 [ ], p=0.06), but failed to demonstrate that any combination of treatments is better than either mechanical therapy alone (CP) or thermal therapy (TC) alone. Since our study is a retrospective one, initiated on January 1 st 2003, it includes cases of EI used as monotherapy (119 cases). Regarding the rebleeding rate, from the 268 ulcers that were treated in our department, rebleeding occurred in 19.8% of the cases. These results are similar to the published ones: 18.0% in Romagnuolo s study [16]; 21% in Wolf s study, who also demonstrated that mild to moderate anticoagulation does not increase the risk of re-bleeding following endoscopic therapy [20]; 4.6% in Imperiale s study [15]; 14% 37% in Parente s study, depending on the endoscopist s experience [10]; and 2.8% 20.3% in Liou s study, depending on the volume of injected epinephrine solution [21]. These large studies demonstrated a wide rebleeding rate range, from 2.8% to 37%, influenced by many factors, out of which the experience of the endoscopist and volume of injected epinephrine seem to have statistical significance. Regarding the combined therapy, in our study the endoscopists preferred the association of EI with TC (in 67.6% of the cases), rather than EI + CP (in 20.4% of the cases), in the rest of the cases various combinations of haemostasis techniques being used. These differences are probably due to personal preferences, but we must emphasize that there are some localizations where CP is more difficult to perform (posterior wall of the duodenal bulb, posterior wall of the gastric body and lesser curve of the stomach) [7]. Regarding the superiority of the TC over CP or vice-versa, Sung s analysis [7], performed on 1,156 patients, showed no improvement in definitive haemostasis with CP as compared with TC (81.5% vs 81.2%; RR 1.00, 95% CI ). There were also no differences between CP and TC regarding rebleeding, the need for surgery and mortality. The same study revealed that the rate of definitive haemostasis was higher with CP (86.5%) than with EI (75.4%), RR 1.14, (95% CI ), as well as in CP+EI (88.5%) as compared with EI alone (78.1%), RR 1.13, (95% CI ). The conclusion of this study was that successful application of CP is superior to EI alone, but comparable to TC in obtaining definitive haemostasis. Based on the most recent scientific studies, the endoscopist can decide to perform CP, or TC, depending on his/her preferences and experience and on the localization of the endoscopic lesions. Most often, he/she will inject epinephrine 1/10,000, especially in the case of active bleeding lesions (type Ia or I b according to the Forrest classification). In conclusion, the analysis of the 810 cases of non-variceal UDB, hospitalized in an experienced endoscopy center, has shown that more than 80% of these hemorrhages were caused by gastric or duodenal ulcers (with approximately equal incidence). Ulcerous UDB had in our department a mortality rate of 3.6%, and the rate of haemostatic surgical interventions was 2.7%. Regarding hemorrhagic ulcers, endoscopic haemostasis was needed in 40% of the cases. In endoscopically treated ulcers, rebleeding occurred in 19.8% of the cases. During the time of this study, we observed a decreasing number of epinephrine injections in favor of definitive treatment (bipolar coagulation or clipping). In an experienced endoscopic center, the endoscopic treatment of ulcerous UDB was successful in the overwhelming majority of cases, the mortality rate and the transfer rate to surgery can be maintained at relatively low levels. Scop. Am evaluat toate cazurile de hemoragie digestivă superioară investigate în cadrul Departamentului de Endoscopie al clinicii noastre pe o perioadă de 5 ani.
7 7 Peptic upper gastrointestinal bleeding 353 Material şi metodă. Am inclus în studiul nostru 810 pacienţi, 64.3% bărbaţi şi 36.7% femei, cu vârsta medie 58.7±15.2 ani (17 96 ani). Principala cauză de hemoragie digestivă superioară a fost ulcerul peptic (82.6%), cu distribuţie egală pentru ulcerele gastrice şi duodenale. Toate ulcerele au fost evaluate după clasificarea Forrest. Rezultate. La 40% din cazuri s-a efectuat hemostază endoscopică, în 44.4% din cazuri aceasta constând doar din injectare de adrenalină (1/10.000); terapie combinată (injectare + clipare sau termocoagulare) a fost folosită în 40.3% din cazuri, iar cliparea sau termocoagularea ca monoterapii au fost folosite în 15.3% din cazuri. Pe perioada studiului s-a observat o reducere importantă a proporţiei folosirii injectării de adrenalină ca monoterapie hemostatică. Resângerarea post-terapie endoscopică a apărut la 19.8% din cazuri; 3.6% din pacienţi au decedat iar 2.7% din cazuri au necesitat intervenţie chirurgicală. Concluzie. Într-un Departament de Endoscopie cu experienţă majoritatea hemoragiilor digestive superioare pot fi tratate endoscopic cu rezultate bune. În ultimii ani biterapia (injectarea de adrenalină + clipare sau coagulare bipolară) a înlocuit monoterapia prin injectare de adrenalină în terapia hemostatică a ulcerelor. Corresponding author: I. Sporea Snagov Str Timişoara isporea@umft.ro REFERENCES 1. LONGSTRETH G.F., Epidemiology of hospitalization for acute upper gastrointestinal hemorrhage: a population based study. Am. J. Gastroenterol., 1995; 90: TARGOWNIK L.W., NABALAMBA A., Trends in management and outcome of acute non-variceal upper gastrointestinal bleeding: Clin. Gastroenterol. and Hepatol., 2006; 4: AMERICAN SOCIETY OF GASTROINTESTINAL ENDOSCOPY. GUIDELINE, The role of endoscopy in acute nonvariceal upper GI hemorrhage. Gastrointest. Endosc., 2004; 60: COOK D.J., GAYATT G.H., SALENA B.J., LAINE L.A., Endoscopic therapy for acute non-variceal hemorrhage: a metaanalysis. Gastroenterology, 1992; 102: LANAS A., GARCIA-RODRIGUEZ L.A., ARROYO M.T. et al., Risk of upper gastrointestinal ulcer bleeding associated with selective cyclo-oxygenase-2 inhibitors, traditional non-aspirin non-steroidal anti-inflammatory drugs, aspirin and combinations. Gut, 2006; 55: CALVET X., VERGARA M., BRULLET E., GISBERT J.P., CAMPO R., Addition of a second endoscopic treatment following epinephrine injection improve outcome in high risk bleeding ulcers. Gastroenterology, 2004; 126: SUNG J.J.Y., TSOI K.T., LAI L.H., WU J.C., LAU J.Y., Endoscopic clipping versus injection and thermo-coagulation in the treatment of non-variceal upper gastrointestinal bleeding: a meta-analysis. Gut, 2007; 10: FORREST J.A., FINLAYSON N.D., SHEARMAN D.J., Endoscopy in gastrointestinal bleeding. Lancet, 1974; 2: ROCKALL T.A., LOGAN R.F., DEVLIN H.B., NORTHFIELD T.C., Risk assessment after acute upper gastrointestinal haemorrhage. Gut, 1996, 38 (3): PARENTE F., ANDERLONI A., BARGIGGIA S. et al., Outcome of non-variceal acute upper gastrointestinal bleeding in relation to the time of endoscopy and the experience of the endoscopist: A two-year survey. World J. Gastroenterol., 2005; 11, LEONTIADIS G.I., SREEDHARAN A., DORWARD S. et al., Systematic reviews of the clinical effectiveness and costeffectiveness of proton pump inhibitors in acute upper gastrointestinal bleeding. Health Technology Assessment, 2007; 51: LEONTIADIS G.I., SHARMA V.K., HOWDEN C.W., Proton pump inhibitor therapy for peptic ulcer bleeding: Cochrane Collaboration meta-analysis of randomized controlled trials. Mayo Clin. Proc., 2007; 82: LAU J.Y., LEUNG W.K., WU J.C.Y. et al., Omeprazole before endoscopy in patients with gastrointestinal bleeding. NEJM, 2007; 356: SCHEMMER P., DECKER F., DEI-ANANE G. et al., The vital threat of an upper gastrointestinal bleeding: Risk factors analysis of 121 consecutive patients. World J. Gastroenterol., 2006; 12:
8 354 I. Sporea et al IMPERIALE T.F., DOMINITZ J.A., PROVENZALE D.T. et al., Predicting poor outcome from acute upper gastrointestinal hemorrhage. Arch. Intern. Med., 2007; 167: ROMAGNUOLO J., BARKUN A.N., ENNS R., ARMSTRONG D., GREGOR J., Simple clinical predictors may obviate urgent endoscopy in selected patients with nonvariceal upper gastrointestinal tract bleeding. Arch. Intern. Med., 2007; 167: ENNS R.A., GAGNON Y.M., BARKUN A.N., ARMSTRONG D., GREGOR J.C., FEDORAK R.N., RUGBE INVESTIGATORS GROUP, Validation of the Rockall scoring system for outcomes from non-variceal upper gastrointestinal bleeding in a Canadian setting. World J. Gastroenterol., 2006; 12: THAM T.C., JAMES C., KELLY M., Predicting outcome of acute non-variceal upper gastrointestinal hemorrhage without endoscopy using the clinical Rockall Score. Postgrad. Med. J., 2006; 82: MARMO R., ROTONDANO G., PISCOPO R., BIANCO M., D ANGELLA R., CIPOLLETTA L., Dual therapy versus monotherapy in the endoscopic treatment of high-risk bleeding ulcers: A meta-analysis of controlled trials. Am. J. Gastroenterol., 2007; 102: WOLF A.T., WASAN S.K., SALZMAN J.R., Impact of anticoagulation on rebleeding following endoscopic therapy for nonvariceal upper gastrointestinal hemorrhage. Am. J. Gastroenterol., 2007; 102: LIOU T.C., LIN S.C., WANG H.Y., CHANG W.H., Optimal injection volume of epinephrine for endoscopic treatment of peptic ulcer bleeding. World J. Gastroenterol., 2006; 12: Received August 1, 2009
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial
 Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD
 Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
American Journal of Gastroenterology ISSN 0002-9270
 American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points
 372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Rob Enns University of British Columbia, Vancouver. Grigorios Leontiadis McMaster University, Hamilton
 Rob Enns University of British Columbia, Vancouver Grigorios Leontiadis McMaster University, Hamilton Accreditation This event has been approved as an accredited (Section1) group learning activity as defined
Rob Enns University of British Columbia, Vancouver Grigorios Leontiadis McMaster University, Hamilton Accreditation This event has been approved as an accredited (Section1) group learning activity as defined
SIGN. Management of acute upper and lower gastrointestinal bleeding. September 2008. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
Optimal injection volume of epinephrine for endoscopic treatment of peptic ulcer bleeding
 PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 May 21; 12(19): 3108-3113 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION
PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 May 21; 12(19): 3108-3113 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION
A. Ketorolac*** B. Naproxen C. Ibuprofen D. Celecoxib
 1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding
 Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Management by the intensivist of gastrointestinal bleeding in adults and children
 Osman et al. Annals of Intensive Care 2012, 2:46 REVIEW Open Access Management by the intensivist of gastrointestinal bleeding in adults and children David Osman 1*, Michel Djibré 2, Daniel Da Silva 3,
Osman et al. Annals of Intensive Care 2012, 2:46 REVIEW Open Access Management by the intensivist of gastrointestinal bleeding in adults and children David Osman 1*, Michel Djibré 2, Daniel Da Silva 3,
British Society of Gastroenterology. St. Elsewhere's NHS Foundation Trust. National Comparative Audit of Blood Transfusion
 British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood December 2007 St. Elsewhere's NHS Foundation Trust National Comparative Audit of Blood
British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood December 2007 St. Elsewhere's NHS Foundation Trust National Comparative Audit of Blood
Peptic ulcers are a common cause of nonvariceal upper
 original article ractices in peptic ulcer bleeding controversies among university- versus nonuniversity-affiliated gastroenterologists Justin Cheung MD FRCC 1, Grant Sawisky MD 2, Robert Enns MD FRCC 3,
original article ractices in peptic ulcer bleeding controversies among university- versus nonuniversity-affiliated gastroenterologists Justin Cheung MD FRCC 1, Grant Sawisky MD 2, Robert Enns MD FRCC 3,
Management of Acute Bleeding from a Peptic Ulcer
 The new england journal of medicine review article Current Concepts Management of Acute Bleeding from a Peptic Ulcer Ian M. Gralnek, M.D., M.S.H.S., Alan N. Barkun, M.D., C.M., M.Sc., and Marc Bardou,
The new england journal of medicine review article Current Concepts Management of Acute Bleeding from a Peptic Ulcer Ian M. Gralnek, M.D., M.S.H.S., Alan N. Barkun, M.D., C.M., M.Sc., and Marc Bardou,
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Management and Prevention of Upper GI Bleeding
 Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
None. Dual Antiplatelet Therapy Plus Systemic Anticoagulation: Bleeding Risk and Management. 76 year old male LINGO 1/5/2015
 Financial Disclosure Information Dual Antiplatelet Therapy Plus Systemic Anticoagulation: Bleeding Risk and Management Robert D. McBane, M.D. Division of Cardiology Mayo Clinic Rochester Dual Antiplatelet
Financial Disclosure Information Dual Antiplatelet Therapy Plus Systemic Anticoagulation: Bleeding Risk and Management Robert D. McBane, M.D. Division of Cardiology Mayo Clinic Rochester Dual Antiplatelet
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Dual Antiplatelet Therapy. Stephen Monroe, MD FACC Chattanooga Heart Institute
 Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Diagnosis and treatment of patients with gastrointestinal bleeding
 Current Anaesthesia & Critical Care (2004) 15, 123 132 ARTICLE IN PRESS www.elsevier.com/locate/cacc MEDICAL Diagnosis and treatment of patients with gastrointestinal bleeding C. Meaden, A.J. Makin* UK
Current Anaesthesia & Critical Care (2004) 15, 123 132 ARTICLE IN PRESS www.elsevier.com/locate/cacc MEDICAL Diagnosis and treatment of patients with gastrointestinal bleeding C. Meaden, A.J. Makin* UK
NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol)
 NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol) Date of First Issue 10/05/2010 Approved 16/06/2010 Current Issue Date 18/11/2015
NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol) Date of First Issue 10/05/2010 Approved 16/06/2010 Current Issue Date 18/11/2015
ORIGINAL ARTICLE: Clinical Endoscopy
 ORIGINAL ARTICLE: Clinical Endoscopy Immediate unprepared hydroflush colonoscopy for severe lower GI bleeding: a feasibility study Aparna Repaka, MD, Matthew R. Atkinson, MD, Ashley L. Faulx, MD, Gerard
ORIGINAL ARTICLE: Clinical Endoscopy Immediate unprepared hydroflush colonoscopy for severe lower GI bleeding: a feasibility study Aparna Repaka, MD, Matthew R. Atkinson, MD, Ashley L. Faulx, MD, Gerard
Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage
 Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage Brian P. Bosworth A. Outcomes in Lower Gastrointestinal Bleeding Acute
Determination of Clinical Decision Rules and Risk Stratification of Patients Admitted with Acute Lower Gastrointestinal Hemorrhage Brian P. Bosworth A. Outcomes in Lower Gastrointestinal Bleeding Acute
Management of bleeding gastroduodenal ulcers
 CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Management of bleeding gastroduodenal ulcers Stig Borbjerg Laursen, Henrik Stig Jørgensen & Ove B. Schaffalitzky de Muckadell The guideline has been approved
CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Management of bleeding gastroduodenal ulcers Stig Borbjerg Laursen, Henrik Stig Jørgensen & Ove B. Schaffalitzky de Muckadell The guideline has been approved
CLINICAL PRACTICE GUIDELINES
 CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
Rebleeding and survival after acute lower gastrointestinal bleeding
 The American Journal of Surgery 188 (2004) 485 490 Scientific paper Rebleeding and survival after acute lower gastrointestinal bleeding Thomas Anthony, M.D.*, Pradeep Penta, B.S., Robert D. Todd, B.S.,
The American Journal of Surgery 188 (2004) 485 490 Scientific paper Rebleeding and survival after acute lower gastrointestinal bleeding Thomas Anthony, M.D.*, Pradeep Penta, B.S., Robert D. Todd, B.S.,
(ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding?
 (ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding? Dennis M. Jensen 1, Robert Stuart 2, Henrik Ahlbom 3, Stefan Eklund 3, Alan Barkun
(ASGE 617b) Is There a Subgroup of Patients With Forrest Ib (Oozing) Peptic Ulcer Bleeding at Increased Risk of Rebleeding? Dennis M. Jensen 1, Robert Stuart 2, Henrik Ahlbom 3, Stefan Eklund 3, Alan Barkun
Gastrointestinal (GI) bleeding
 Gastrointestinal (GI) bleeding Somchai Leelakusolvong, M.D. Div of Gastroenterology, Dept of Medicine, Siriraj Endoscopy Center e-mail address: srsll@mahidol.ac.th 07-07-2010 RCPT อ ตรด ตถ GI Bleeding
Gastrointestinal (GI) bleeding Somchai Leelakusolvong, M.D. Div of Gastroenterology, Dept of Medicine, Siriraj Endoscopy Center e-mail address: srsll@mahidol.ac.th 07-07-2010 RCPT อ ตรด ตถ GI Bleeding
Articles Presented. Journal Presentation. Dr Albert Lo. Dr Albert Lo
 * This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
* This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a
 AMP particles - absorbable polysaccharide hemostat in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a prospective, randomized
AMP particles - absorbable polysaccharide hemostat in comparison with metallic hemoclip for hemostasis and preventing post-procedure bleeding after endoscopic mucosal resection(emr): a prospective, randomized
STROKE PREVENTION IN ATRIAL FIBRILLATION. TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: ABBREVIATIONS: BACKGROUND:
 STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
FOR THE PREVENTION OF ATRIAL FIBRILLATION RELATED STROKE
 www.bpac.org.nz keyword: warfarinaspirin FOR THE PREVENTION OF ATRIAL FIBRILLATION RELATED STROKE Key Concepts In atrial fibrillation (AF) warfarin is more effective than aspirin for stroke prevention.
www.bpac.org.nz keyword: warfarinaspirin FOR THE PREVENTION OF ATRIAL FIBRILLATION RELATED STROKE Key Concepts In atrial fibrillation (AF) warfarin is more effective than aspirin for stroke prevention.
LOWER GASTROINTESTINAL BLEEDING GED/05/08
 LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
9/5/14. Objectives. Atrial Fibrillation (AF)
 Novel Anticoagulation for Prevention of Stroke in Patients with Atrial Fibrillation Objectives 1. Review current evidence on use of warfarin in individuals with atrial fibrillation 2. Compare the three
Novel Anticoagulation for Prevention of Stroke in Patients with Atrial Fibrillation Objectives 1. Review current evidence on use of warfarin in individuals with atrial fibrillation 2. Compare the three
DUAL ANTIPLATELET THERAPY. Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania
 DUAL ANTIPLATELET THERAPY Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania DUAL ANTIPLATELET THERAPY (DAPT) Dual antiplatelet regimen
DUAL ANTIPLATELET THERAPY Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania DUAL ANTIPLATELET THERAPY (DAPT) Dual antiplatelet regimen
New Treatments for Stroke Prevention in Atrial Fibrillation. John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013
 New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl
 NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
understanding GI bleeding
 understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Tranexamic Acid. Tranexamic Acid. Overview. Blood Conservation Strategies. Blood Conservation Strategies. Blood Conservation Strategies
 Overview Where We Use It And Why Andreas Antoniou, M.D., M.Sc. Department of Anesthesia and Perioperative Medicine University of Western Ontario November 14 th, 2009 Hemostasis Fibrinolysis Aprotinin and
Overview Where We Use It And Why Andreas Antoniou, M.D., M.Sc. Department of Anesthesia and Perioperative Medicine University of Western Ontario November 14 th, 2009 Hemostasis Fibrinolysis Aprotinin and
Treating delayed endoscopic sphincterotomy-induced bleeding: Epinephrine injection with or without thermotherapy
 Online Submissions: wjg.wjgnet.com World J Gastroenterol 2009 October 14; 15(38): 4823-4828 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.15.4823 2009 The WJG Press and
Online Submissions: wjg.wjgnet.com World J Gastroenterol 2009 October 14; 15(38): 4823-4828 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.15.4823 2009 The WJG Press and
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department!
 Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
UGI Tract Hemorrhage. GI Tract Emergencies. UGI Hemorrhage. David D. Markowitz, MD. UGI tract hemorrhage Comorbid disease
 UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
Gruppo di lavoro: Malattie Tromboemboliche
 Gruppo di lavoro: Malattie Tromboemboliche 2381 Soluble Recombinant Thrombomodulin Ameliorates Hematological Malignancy-Induced Disseminated Intravascular Coagulation More Promptly Than Conventional Anticoagulant
Gruppo di lavoro: Malattie Tromboemboliche 2381 Soluble Recombinant Thrombomodulin Ameliorates Hematological Malignancy-Induced Disseminated Intravascular Coagulation More Promptly Than Conventional Anticoagulant
NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS
 NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS Date of First Issue 01/12/ 2012 Approved 15/11/2012 Current Issue Date 29/10/2014 Review Date 29/10/2016
NHS FORTH VALLEY RIVAROXABAN AS TREATMENT FOR DEEP VEIN THROMBOSIS AND PULMONARY EMBOLISM IN ADULTS Date of First Issue 01/12/ 2012 Approved 15/11/2012 Current Issue Date 29/10/2014 Review Date 29/10/2016
DISCLOSURES RISK ASSESSMENT. Stroke and Heart Disease -Is there a Link Beyond Risk Factors? Daniel Lackland, MD
 STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
Traveller s Thrombosis. Dr. Peter Verhamme Vascular Medicine and Haemostasis UZ Leuven
 Traveller s Thrombosis Dr. Peter Verhamme Vascular Medicine and Haemostasis UZ Leuven Case 1: To thromboprophylaxe or not Women, aged 49, BMI 29, Combined Oral Contraceptives. Family history of provoked
Traveller s Thrombosis Dr. Peter Verhamme Vascular Medicine and Haemostasis UZ Leuven Case 1: To thromboprophylaxe or not Women, aged 49, BMI 29, Combined Oral Contraceptives. Family history of provoked
4/9/2015. Risk Stratify Our Patients. Stroke Risk in AF: CHADS2 Scoring system JAMA 2001; 285: 2864-71
 Anticoagulation in the 21 st Century Adam Karpman, D.O. Saint Francis Medical Center/Oklahoma State University Medical Center Disclosures: None Atrial Fibrillation Most common arrhythmia in clinical practice.
Anticoagulation in the 21 st Century Adam Karpman, D.O. Saint Francis Medical Center/Oklahoma State University Medical Center Disclosures: None Atrial Fibrillation Most common arrhythmia in clinical practice.
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
High Risk Emergency Medicine
 High Risk Emergency Medicine Minor Head Injuries in Patients on Oral Anticoagulants David Thompson, MD, MPH Assistant Professor Department of Emergency Medicine No relevant financial relationships to disclose
High Risk Emergency Medicine Minor Head Injuries in Patients on Oral Anticoagulants David Thompson, MD, MPH Assistant Professor Department of Emergency Medicine No relevant financial relationships to disclose
Getting smart about dyspnea and life saving drug therapy in ACS patients. Kobi George Kaplan Medical Center Rehovot
 Getting smart about dyspnea and life saving drug therapy in ACS patients Kobi George Kaplan Medical Center Rehovot 78 year old female Case description Presented with resting chest pain and dyspnea Co morbidities:
Getting smart about dyspnea and life saving drug therapy in ACS patients Kobi George Kaplan Medical Center Rehovot 78 year old female Case description Presented with resting chest pain and dyspnea Co morbidities:
Management of the new antiplatelets and anticoagulants
 Management of the new antiplatelets and anticoagulants Session No.: 1 Name: C. Boustiere, T Ponchon Guidelines : Anti-thrombotic agents and digestive endoscopy 2006 : French guideline (SFED) 2007 : Japanese
Management of the new antiplatelets and anticoagulants Session No.: 1 Name: C. Boustiere, T Ponchon Guidelines : Anti-thrombotic agents and digestive endoscopy 2006 : French guideline (SFED) 2007 : Japanese
Cost-Saving Approach to Patients on Long-Term Anticoagulation Who Need Endoscopy: A Decision Analysis
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 8, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0002-9270(03)00445-3 Cost-Saving Approach
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 8, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0002-9270(03)00445-3 Cost-Saving Approach
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
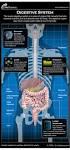 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding
 PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
Research funding was provided by TAP Pharmaceutical Products, Inc.
 DOES THE DOSING FREQUENCY OF PROTON PUMP INHIBITORS (PPIs) AFFECT SUBSEQUENT RESOURCE UTILIZATION AND COSTS AMONG PATIENTS DIAGNOSED WITH GASTROESOPHAGEAL REFLUX DISEASE (GERD)? Boulanger L 1, Mody R 2,
DOES THE DOSING FREQUENCY OF PROTON PUMP INHIBITORS (PPIs) AFFECT SUBSEQUENT RESOURCE UTILIZATION AND COSTS AMONG PATIENTS DIAGNOSED WITH GASTROESOPHAGEAL REFLUX DISEASE (GERD)? Boulanger L 1, Mody R 2,
Rubén Casado Arroyo, 1,2 Mónica Polo-Tomas, 2 Maria P Roncalés, 2 James Scheiman, 3 Ángel Lanas 2,3,4 ORIGINAL ARTICLE. Antiplatelet therapy
 ORIGINAL ARTICLE Lower GI bleeding is more common than upper among patients on dual antiplatelet therapy: long-term follow-up of a cohort of patients commonly using PPI co-therapy Rubén Casado Arroyo,
ORIGINAL ARTICLE Lower GI bleeding is more common than upper among patients on dual antiplatelet therapy: long-term follow-up of a cohort of patients commonly using PPI co-therapy Rubén Casado Arroyo,
Endoscopic Submucosal Dissection (E.S.D.) vs. Endoscopic Mucosal Resection (E.M.R.) in Colombia. Advocating E.M.R.
 Controversies in Gastroenterology Endoscopic Submucosal Dissection (E.S.D.) vs. Endoscopic Mucosal Resection (E.M.R.) in Colombia. Advocating E.M.R. Raúl Cañadas Garrido, MD. 1 1 Internist-Gastroenterologist.
Controversies in Gastroenterology Endoscopic Submucosal Dissection (E.S.D.) vs. Endoscopic Mucosal Resection (E.M.R.) in Colombia. Advocating E.M.R. Raúl Cañadas Garrido, MD. 1 1 Internist-Gastroenterologist.
Long term anticoagulant therapy in patients with atrial fibrillation at high risk of stroke: a new scenario after RE-LY trial
 Long term anticoagulant therapy in patients with atrial fibrillation at high risk of stroke: a new scenario after RE-LY trial Camillo Autore Università di Roma Sapienza II Facoltà di Medicina e Chirurgia
Long term anticoagulant therapy in patients with atrial fibrillation at high risk of stroke: a new scenario after RE-LY trial Camillo Autore Università di Roma Sapienza II Facoltà di Medicina e Chirurgia
ABOUT XARELTO CLINICAL STUDIES
 ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
What can I eat? Peptic ulcers. What are peptic ulcers? What tests are needed? Will the ulcer come back? What causes a peptic ulcer?
 In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
Postpolypectomy haemorrhage following removal of large polyps using mechanical haemostasis or epinephrine: a meta-analysis
 Original Article Postpolypectomy haemorrhage following removal of large polyps using mechanical haemostasis or epinephrine: a meta-analysis United European Gastroenterology Journal 0(0) 1 8! Author(s)
Original Article Postpolypectomy haemorrhage following removal of large polyps using mechanical haemostasis or epinephrine: a meta-analysis United European Gastroenterology Journal 0(0) 1 8! Author(s)
Surgical Management of GI Bleeding. VA Case Presentation. 0-24 hours 9/18/2012
 Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
New Anticoagulants: What to Use What to Avoid
 New Anticoagulants: What to Use What to Avoid Bruce Davidson, MD, MPH Clinical Professor of Medicine Pulmonary and Critical Care Medicine Division University of Washington School of Medicine Seattle USA
New Anticoagulants: What to Use What to Avoid Bruce Davidson, MD, MPH Clinical Professor of Medicine Pulmonary and Critical Care Medicine Division University of Washington School of Medicine Seattle USA
Aktuelle Literatur aus der Notfallmedizin
 05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
05.02.2014 Aktuelle Literatur aus der Notfallmedizin prä- und innerklinisch Aktuelle Publikationen aus 2012 / 2013 PubMed hits zu emergency medicine 12,599 Abstract OBJECTIVES: Current American Heart
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Appendix G - Identification and Selection of Studies
 FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
Gloucestershire Hospitals
 TRUST GUIDELINE In the case of hard copies of this policy the content can only be assured to be accurate on the date of issue marked on the document. The Policy framework requires that the policy is fully
TRUST GUIDELINE In the case of hard copies of this policy the content can only be assured to be accurate on the date of issue marked on the document. The Policy framework requires that the policy is fully
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas
 Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Rivaroxaban for acute coronary syndromes
 Northern Treatment Advisory Group Rivaroxaban for acute coronary syndromes Lead author: Nancy Kane Regional Drug & Therapeutics Centre (Newcastle) May 2014 2014 Summary Current long-term management following
Northern Treatment Advisory Group Rivaroxaban for acute coronary syndromes Lead author: Nancy Kane Regional Drug & Therapeutics Centre (Newcastle) May 2014 2014 Summary Current long-term management following
Program Approved by AoA, NCOA. Website: www.homemeds.org
 MEDICATION MANAGEMENT IMPROVEMENT SYSTEM: HomeMeds SM The HomeMeds SM system is a collaborative approach to identifying, assessing, and resolving medication problems in community-dwelling older adults.
MEDICATION MANAGEMENT IMPROVEMENT SYSTEM: HomeMeds SM The HomeMeds SM system is a collaborative approach to identifying, assessing, and resolving medication problems in community-dwelling older adults.
New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis
 New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis Holster IL, Valkhoff VE, Kuipers EJ, Tjwa ET Departments of Gastroenterology and Hepatology,
New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis Holster IL, Valkhoff VE, Kuipers EJ, Tjwa ET Departments of Gastroenterology and Hepatology,
Thrombosis and Bleeding
 Many questions, few answers Thrombosis and Bleeding Pierre Noel MD Mayo Arizona Scope of the Problem Thrombosis PV 12-39% ET 11-25% MF 10% 60-70% of thrombosis are arterial Splanchnic and cerebral thrombosis
Many questions, few answers Thrombosis and Bleeding Pierre Noel MD Mayo Arizona Scope of the Problem Thrombosis PV 12-39% ET 11-25% MF 10% 60-70% of thrombosis are arterial Splanchnic and cerebral thrombosis
ΠΟΙΟ ΑΝΤΙΠΗΚΤΙΚΟ ΓΙΑ ΤΟΝ ΑΣΘΕΝΗ ΜΟΥ? ΚΛΙΝΙΚΑ ΠΑΡΑΔΕΙΓΜΑΤΑ. Σωκράτης Παστρωμάς Καρδιολόγος Νοσοκομείο Ερρίκος Ντυνάν
 ΠΟΙΟ ΑΝΤΙΠΗΚΤΙΚΟ ΓΙΑ ΤΟΝ ΑΣΘΕΝΗ ΜΟΥ? ΚΛΙΝΙΚΑ ΠΑΡΑΔΕΙΓΜΑΤΑ Σωκράτης Παστρωμάς Καρδιολόγος Νοσοκομείο Ερρίκος Ντυνάν The AF epidemic Mayo Clinic data (assuming a continued increase in the AF incidence) Mayo
ΠΟΙΟ ΑΝΤΙΠΗΚΤΙΚΟ ΓΙΑ ΤΟΝ ΑΣΘΕΝΗ ΜΟΥ? ΚΛΙΝΙΚΑ ΠΑΡΑΔΕΙΓΜΑΤΑ Σωκράτης Παστρωμάς Καρδιολόγος Νοσοκομείο Ερρίκος Ντυνάν The AF epidemic Mayo Clinic data (assuming a continued increase in the AF incidence) Mayo
Novel oral anticoagulant (NOAC) for stroke prevention in atrial fibrillation Special situations
 Novel oral anticoagulant (NOAC) for stroke prevention in atrial fibrillation Special situations Dardo E. Ferrara MD Cardiac Electrophysiology North Cascade Cardiology PeaceHealth Medical Group Which anticoagulant
Novel oral anticoagulant (NOAC) for stroke prevention in atrial fibrillation Special situations Dardo E. Ferrara MD Cardiac Electrophysiology North Cascade Cardiology PeaceHealth Medical Group Which anticoagulant
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting
 Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy
 Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy Judith Long, MD,RWJCS Perelman School of Medicine Philadelphia Veteran Affairs Medical Center Background Objective Overview Methods
Robert Okwemba, BSPHS, Pharm.D. 2015 Philadelphia College of Pharmacy Judith Long, MD,RWJCS Perelman School of Medicine Philadelphia Veteran Affairs Medical Center Background Objective Overview Methods
Breadth of indications matters One drug for multiple indications
 Breadth of indications matters One drug for multiple indications Sylvia Haas, MD, PhD Formerly of the Technical University of Munich Munich, Germany Disclosures: Sylvia Haas 1 Novel oral anticoagulants:
Breadth of indications matters One drug for multiple indications Sylvia Haas, MD, PhD Formerly of the Technical University of Munich Munich, Germany Disclosures: Sylvia Haas 1 Novel oral anticoagulants:
1/12/2016. What s in a name? What s in a name? NO.Anti-Coagulation. DOACs in clinical practice. Practical aspects of using
 What s in a name? Practical aspects of using DOACs (Direct Oral Anticoagulants) James L. Sebastian, MD, MACP Professor of Medicine (GIM) Medical College of Wisconsin February 5, 2016 DOAC NOAC NOAC ODI
What s in a name? Practical aspects of using DOACs (Direct Oral Anticoagulants) James L. Sebastian, MD, MACP Professor of Medicine (GIM) Medical College of Wisconsin February 5, 2016 DOAC NOAC NOAC ODI
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
New Oral Anticoagulants
 New Oral Anticoagulants Tracy Minichiello, MD Associate Professor of Medicine Chief, San FranciscoVA Anticoagulation and Thrombosis Service Ansell, J. Hematology Copyright 2010 American Society of Hematology.
New Oral Anticoagulants Tracy Minichiello, MD Associate Professor of Medicine Chief, San FranciscoVA Anticoagulation and Thrombosis Service Ansell, J. Hematology Copyright 2010 American Society of Hematology.
Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study
 Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
APSR RESPIRATORY UPDATES
 APSR RESPIRATORY UPDATES Volume 6, Issue 1 Newsletter Date: January 2014 APSR EDUCATION PUBLICATION Inside this issue: Venous thromboembolism Pulmonary embolism and deep vein thrombosis. 2 Outpatient versus
APSR RESPIRATORY UPDATES Volume 6, Issue 1 Newsletter Date: January 2014 APSR EDUCATION PUBLICATION Inside this issue: Venous thromboembolism Pulmonary embolism and deep vein thrombosis. 2 Outpatient versus
ESC Guidelines on the diagnosis and treatment of peripheral artery diseases Lower extremity artery disease. Erich Minar Medical University Vienna
 ESC Guidelines on the diagnosis and treatment of peripheral artery diseases Lower extremity artery disease Erich Minar Medical University Vienna for the Task Force on the Diagnosis and Treatment of Peripheral
ESC Guidelines on the diagnosis and treatment of peripheral artery diseases Lower extremity artery disease Erich Minar Medical University Vienna for the Task Force on the Diagnosis and Treatment of Peripheral
New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation. Joy Wahawisan, Pharm.D., BCPS April 25, 2012
 New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation Joy Wahawisan, Pharm.D., BCPS April 25, 2012 Stroke in Atrial Fibrillation % Stroke 1991;22:983. Age Range (years) CHADS 2 Risk
New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation Joy Wahawisan, Pharm.D., BCPS April 25, 2012 Stroke in Atrial Fibrillation % Stroke 1991;22:983. Age Range (years) CHADS 2 Risk
Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence
 Guidelines Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence Stroke/TIA Nearly 700,000 ischemic strokes and 240,000 TIAs every year in the United States Currently, the risk for
Guidelines Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence Stroke/TIA Nearly 700,000 ischemic strokes and 240,000 TIAs every year in the United States Currently, the risk for
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
HemoClip: Guidelines & Atlas
 HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
The author has no disclosures
 Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 Mary.bradbury@inova.org This presentation will discuss unlabeled and investigational use of products The author
Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 Mary.bradbury@inova.org This presentation will discuss unlabeled and investigational use of products The author
Learning Luncheon 7: Endoscopic Mucosal Resection: When, Where and How?
 Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
The 50-year Quest to Replace Warfarin: Novel Anticoagulants Define a New Era. CCRN State of the Heart 2012 June 2, 2012
 The 50-year Quest to Replace Warfarin: Novel Anticoagulants Define a New Era CCRN State of the Heart 2012 June 2, 2012 Disclosures I have I have been involved in trials of new anticoagulants and have received
The 50-year Quest to Replace Warfarin: Novel Anticoagulants Define a New Era CCRN State of the Heart 2012 June 2, 2012 Disclosures I have I have been involved in trials of new anticoagulants and have received
Evolution of Barrett s esophagus
 Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
New Oral AntiCoagulants (NOAC) in 2015
 New Oral AntiCoagulants (NOAC) in 2015 William R. Hiatt, MD Professor of Medicine and Cardiology University of Colorado School of Medicine President CPC Clinical Research Disclosures Received research
New Oral AntiCoagulants (NOAC) in 2015 William R. Hiatt, MD Professor of Medicine and Cardiology University of Colorado School of Medicine President CPC Clinical Research Disclosures Received research
Conserva)ve Treatment of PE/ DVT
 Conserva)ve Treatment of PE/ DVT Amir Kaki, MD FACC FSCAI Asst Prof of Medicine Wayne St SOM Medical Director Cardiac Catheteriza)on Lab Heart Hospital DMC Detroit, MI Incidence Acute pulmonary embolism
Conserva)ve Treatment of PE/ DVT Amir Kaki, MD FACC FSCAI Asst Prof of Medicine Wayne St SOM Medical Director Cardiac Catheteriza)on Lab Heart Hospital DMC Detroit, MI Incidence Acute pulmonary embolism
