Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas
|
|
|
- Norah Henry
- 10 years ago
- Views:
Transcription
1 Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director, CURE DDRC
2 D e n n is M. J e nse n, M D C Professor, Department of Medicine S m t w c fi t w p o A David Geffen School of Medicine at University of California, Los Angeles Director, Hemostasis Program Co-Director, Gastroenterology Procedures Unit Associate Director, CURE: Digestive Diseases Research Center Los Angeles, California
3 The Utility of Endoscopic Doppler in the Management of Acute Peptic Ulcer Hemorrhage: Treatment of an Ulcer Rebleed Presented By: Dennis M. Jensen, MD, Professor of Medicine, David Geffen School of Medicine at UCLA, Associate Director, CURE DDRC C ase H is to ry Seven days prior to this presentation, an 80 year old Caucasian male had a 1.5 cm chronic ulcer with severe upper gastrointestinal (UGI) bleeding and a non-bleeding visible vessel (NBVV) which was treated with epinephrine injection and multipolar probe coagulation (MPEC). He had a past medical history of chronic atrial fibrillation, congestive heart failure, coronary artery disease, hypertension and chronic renal insufficiency, all controlled medically. He was treated after the initial endoscopy (EGD) with high dose proton pump inhibitor (PPI) infusion for 72 hours and then with twice daily oral PPI. Helicobacter pylori serology and antigen were negative. Aspirin 81 mg/day was restarted 3 days after the UGI bleed. 1 Just before discharge and 7 days after the prior EGD and hemostasis, the patient rebled. This was manifested by melena, hematochezia, hypotension, and an acute hemoglobin fall from 9 grams to 6.5 grams. He was volume resuscitated, transfused 3 units of red blood cells (RBCs), and transferred back to the ICU. A repeat EGD two hours after metoclopramide was performed with a large channel (3.8 mm) therapeutic endoscope that had a separate channel for target jet irrigation. 1a FIGURE 1. A non-bleeding visible vessel (NBVV) was seen in the gastric ulcer (GU) base, near the edge at the 12 o clock position, after blood and clots were washed off. This indicated a high risk stigma of recent hemorrhage (SRH) for rebleeding. Because of the rebleed after prior combination therapy and the size and depth of the ulcer, locating the direction of the underlying artery and obliterating it were necessary to prevent rebleeding in this high risk patient. 2 2a FIGURE 2. The endoscopic Doppler probe was utilized to interrogate the base of the ulcer and the area adjacent to and on the NBVV. This demonstrated a loud arterial signal at a shallow depth ( 1.5 mm) setting, and located the direction of the artery in the ulcer base prior to repeat hemostasis. 3 3a FIGURE 3. A 10 French (F) multipolar electro-coagulation (MPEC) probe was utilized to coaptively coagulate the NBVV and the artery underneath it. Standard CURE Hemostasis group settings (12 watts, firm pressure, and 10 second treatment pulses) were utilized until the visible vessel was flattened and well coagulated. These are the usual visual endpoints for successful thermal coagulation of chronic appearing peptic ulcers. The VTI Endoscopic Doppler System
4 4 4a FIGURE 4. The NBVV was white and appeared well coagulated. However, the question in such a high risk patient was whether the underlying arterial blood flow had been occluded and the artery had been coaptively sealed. 5 5a FIGURE 5. Doppler examination was repeated and a persistent, loud arterial signal was detected at the shallow ( 1.5 mm) and mid ( 4 mm) depth settings. Further treatment now had to be considered - more MPEC or hemoclips? 6 6a FIGURE 6. Hemoclipping of the NBVV and underlying patent artery were chosen for definitive hemostasis. Unlike thermal coagulation which can increase the ulcer size and depth, hemoclipping causes little tissue damage. Also some current hemoclips reach 2-3 mm into the submucosa and can seal the underlying artery. One hemoclip (HC) was placed on the side of the NBVV in the direction where the artery was located by the Doppler probe. 7 7a FIGURE 7. Another hemoclip (HC) was placed on the opposite side of the NBVV to seal the underlying artery. The location of the artery as detected by the Doppler probe at baseline guided the hemostasis and the placement of the hemoclips. 8 8a FIGURE 8. Post hemoclipping, the Doppler probe was used to document that the arterial flow in the ulcer underneath the NBVV had been obliterated. No Doppler signal was heard at the shallow or mid depth settings; the ulcer was now Doppler negative.
5 Clinical Follow-up The patient was treated for 72 hours with high dose PPI infusion and after that with twice daily oral PPI. A full liquid diet was started after the patient awoke from conscious sedation. He had no further UGI bleeding and was continued on 81 mg/day of aspirin. Warfarin was restarted 7 days after the EGD. He had healing of the gastric ulcer documented by repeat EGD, 8 weeks after hospital discharge. Clinical Significance When the endoscopist visualizes a NBVV in the base of an ulcer in a patient with an acute peptic ulcer bleed, there is uncertainty about the location of the underlying vessel, its proximity to the visible vessel, and its course in the ulcer base. Until the development and availability of endoscopic Doppler technology, the only ways to detect location, course, and patency of the underlying artery were either via surgery or angiography. With endoscopic Doppler, refined risk stratification, targeted endoscopic hemostasis, and potential improvements in patient outcomes in non-variceal upper gastrointestinal hemorrhage are now feasible. In this patient, the positive (post-mpec treatment) Doppler signal indicated the applied endoscopic therapy had failed to abolish the arterial blood supply to the ulcer and hence, the patient was at increased risk of recurrent bleeding from the ulcer. Without the use of the endoscopic Doppler probe, it would not have been possible for the endoscopist to determine, by visual inspection alone, whether or not endoscopic therapy had been successful at obliterating the feeding blood vessel underneath the ulcer. Q & A with Dr. Jensen How did you know where to treat? The baseline Doppler probe indicated a patent artery (e.g. loud arterial signal) just underneath the NBVV at both the shallow ( 1.5 mm) and mid depth settings ( 4 mm). The Doppler probe also mapped out the direction of the artery for 3-5 mm on either side of the NBVV. This is where the artery is closest to the surface of the ulcer base and is the best location to treat with either MPEC or hemoclipping. The goal of the treatment is to completely occlude the vessel. Why did you choose MPEC treatment first? Because this was a firm, fibrotic ulcer, MPEC treatment was safe to use and is usually effective, if CURE Hemostasis guidelines are applied as detailed above. If MPEC treatment did not seal the underlying artery as documented by Doppler, the plan was then to apply hemoclips. Utilizing the hemoclips first and then trying to apply coaptive coagulation with MPEC treatment afterward, in the same location as the hemoclips usually is ineffective. Why did you cross clamp the NBVV instead of just placing 1 hemoclip on top of the NBVV? Knowing which direction the artery lies (with Doppler probe interrogation) usually allows the endoscopist to seal the underlying artery with 2 hemoclips. By placing a single hemoclip on top of the NBVV, which anatomically is the side hole in the underlying artery and is an organizing clot, often does not seal both sides of the patent underlying artery and may precipitate bleeding by the hemoclipping. Placing hemoclips on either side of the NBVV usually seals the underlying artery if these are deployed 2-3 mm below the ulcer base and the hemoclips are large and strong enough to grasp to that depth. With multiple hemoclips, is there any use of trying to close this type of ulcer or smaller bleeding ulcers with stigmata instead of treating them just adjacent to the SRH in the ulcer base? Doppler probe studies and prior anatomic studies of acute peptic ulcer hemorrhage reveal that the arteries dive deeper as the distance increases within a few mm away from the visible vessel in the ulcer base. Closing ulcers without sealing the artery would bury the underlying patent artery. This would increase the likelihood of rebleeding compared to focal treatment on and adjacent to the SRH in the ulcer base. How often is there residual arterial blood flow detected after standard (visually guided) MPEC treatment of NBVVs? In a recent CURE study (see Table 1), 26% of ulcers with NBVVs similar to this one had residual arterial blood flow detected by Doppler examination after standard (visually guided) MPEC treatment. So we now recommend Doppler monitoring to document completion of hemostasis in such cases with SRH. TABLE 1. For PUBs with Stigmata & Baseline (+) Doppler Residual Blood Flow after Injection or MPEC: Implications for Further Endoscopic Therapy SRH (+)Doppler Before Rx (+)Doppler After Rx % (+) After Rx Spurting Bleed % NBVV % 25.8% Adherent Clot % Flat Spot % Oozing Bleeding 7 0 0% Total % Jensen DM. GIE 2010: 71: AB113: 347m (updated 1/8/14) Scan to view the video that accompanies this case» The VTI Endoscopic Doppler System
6 Notes C A ( a r h b
7 Endoscopic Doppler for the Management of a Gastroesophageal Junction Ulcer with a Flat Spot versus a Non-bleeding Visible Vessel Presented By: Dennis M. Jensen, MD, Professor of Medicine, David Geffen School of Medicine at UCLA, Associate Director, CURE DDRC C ase H is to ry A 67 year old Caucasian man presented to the emergency room (ER) with a two day history of hematemesis, melena, dyspepsia, and syncope. He was hypotensive in the ER and thus was volume resuscitated and given 2 units red blood cells (RBCs). His initial hemoglobin was 7.8 and after the RBCs increased to Other baseline lab results included platelet count of 325,000, INR of 1 1a 2 2a 1.1, BUN of 80, and creatinine of 1.2. He gave a history of having upper gastrointestinal (UGI) bleeding from an ulcer about 3 years ago in another hospital. He also had gastroesophageal reflux disease (GERD) symptoms but was not on a proton pump inhibitor (PPI), aspirin, or NSAIDs. An urgent upper endoscopy (EGD) was performed. FIGURE 1. At the gastroesophageal junction (GEJ) there was a chronic appearing ulcer with a stigma of recent hemorrhage (SRH). It was difficult to determine even after target jet irrigation whether this was a flat spot or a non-bleeding visible vessel (NBVV). Besides a hiatal hernia, no other GI lesions were found on EGD. By current GI treatment guidelines for ulcer hemostasis, flat spots as a SRH are not recommended for endoscopic treatment, whereas NBVV are. Therefore, distinguishing these two or determining whether there was underlying arterial blood flow was very important and clinically relevant. FIGURE 2. An endoscopic Doppler probe was used to interrogate the SRH. There was underlying arterial blood flow detected at the shallow setting ( 1.5 mm) and the course of the artery was also mapped for 3-4 mm on either side of the SRH. 3 3a FIGURE 3. A large 10 French (F) size multipolar electrocautery (MPEC) probe at a low power setting and long coagulation pulses (12 watts and 8-10 second pulses) was used to treat the SRH and to coaptively coagulate the underlying artery. The lesion was tangential and the side of the probe was pressed firmly on the SRH during coagulation. The VTI Endoscopic Doppler System
8 4 4a FIGURE 4. The post-mpec appearance of the ulcer was of a flattened NBVV, well coagulated. No bleeding was induced during treatment. 5 5a FIGURE 5. The Doppler probe was used to recheck for arterial blood flow underneath the SRH. No arterial signal could be elicited. The ulcer was now Doppler negative. C li n ical Fo llow- up The patient was ultimately diagnosed and treated as having a GERD associated ulcer with severe UGI bleeding and a NBVV. He initially received 72 hours of IV PPI infusion (80 mg bolus and 8 mg/hr), followed by twice daily oral PPI. No rebleeding occurred in 60 days of follow-up and he was maintained on the oral PPI twice daily chronically thereafter.
9 Q & A with Dr. Jensen How would you have treated this SRH if you did not have a Doppler probe? It would have been difficult to decide on medical treatment alone (for a spot) versus endoscopic and medical treatment (for a NBVV). That is because the SRH could have been either a flat spot or a NBVV (that was almost flat). Whether there was underlying arterial flow (which is much more common in ulcers with NBVV than flat spots) was the clinically relevant question regarding endoscopic treatment. The Doppler probe clarified the potential risk of rebleeding as high (because of underlying blood flow) and also guided endoscopic hemostasis (by mapping the course of the underlying artery). In your experience with UGI bleeding ulcers (PUBs), how common are NBVVs versus flat spots and how often is arterial blood flow found underneath these SRH with the Doppler probe? In an ongoing prospective study with the Doppler probe of 147 patients with PUBs, the prevalence of flat spots was 25.7% (37/144) and the rate of Doppler positive arterial blood flow underneath flat spots was 40.5% (15/37). In contrast, NBVVs were found in 35.4% (51/144) of all PUB s and 90.2% (46/51) had arterial flow under the NBVVs detected by the Doppler probe (see Table 1). TABLE 1. Baseline Doppler Results: Implications for Risk Stratification of Ulcers SRH N (+)Doppler Before Rx % (+) Before Rx Spurting Bleed % NBVV % 86.4% Adherent Clot % Oozing Alone % Flat Spot Alone % Jensen DM. GIE 2010: 71: AB113: 347m (updated 1/8/14) Weren t you concerned about the risk of transmural injury or perforation on coagulation with a thermal probe for such a GEJ ulcer and why didn t you use hemoclipping instead? The ulcer appeared to be chronic, firm, and fibrotic. MPEC treatment of such ulcers utilizing the CURE Hemostasis Group treatment parameters employed is easy, safe, and effective for such chronic ulcers at the GEJ in my experience. Also, placement of hemoclips in such a tangential position of a GEJ ulcer would have been difficult. Either a side viewing or oblique viewing endoscope would have been needed to effectively deploy hemoclips onto the SRH and underlying artery in this tangentially located GEJ ulcer. Although I would have changed endoscopes and used hemoclips if the artery remained patent after initial MPEC treatment, such retreatment was unnecessary in this patient because the repeat Doppler examination was negative for residual arterial blood flow. With NBVV in chronic ulcers such as this one, how often is residual blood flow found using the Doppler probe under and around the NBVV after standard visually guided endoscopic hemostasis with MPEC treatment? Forty-five patients with NBVVs and positive baseline arterial flow were studied by Doppler examination before and after standard MPEC treatment. Among those who were restudied with Doppler after MPEC hemostasis, 26.7% (12/45) still had residual arterial blood flow just underneath or on either side of the coagulated NBVV (see Table 2). These patients are at high risk of rebleeding. TABLE 2. For PUBs with Stigmata & Baseline (+) Doppler Residual Blood Flow after Injection or MPEC: Implications for Further Endoscopic Therapy SRH (+)Doppler Before Rx (+)Doppler After Rx % (+) After Rx Spurting Bleed % NBVV % 25.8% Adherent Clot % Flat Spot % Oozing Bleeding 7 0 0% Total % Jensen DM. GIE 2010: 71: AB113: 347m (updated 1/8/14) What are the treatment implications of those Doppler findings and what do you do if there is residual arterial flow - epinephrine injection, APC, further MPEC treatment, or hemoclipping? Epinephrine only transiently reduces or eliminates the arterial blood flow under SRH. Furthermore, APC provides superficial coagulation and does not effectively coaptively coagulate underlying arteries in PUBs. So the choice is either more MPEC - which can be effective and safe in chronic, fibrotic ulcers, or the deployment of hemoclips on either side of the SRH to clip the underlying artery. I use either or both of the latter two approaches depending on the ulcer appearance, location, and concern about perforation with further MPEC treatment. Applying hemoclips next to the SRH in the ulcer base may require using an oblique or side viewing endoscope and is often more difficult than MPEC treatment in a tangentially located ulcer. The VTI Endoscopic Doppler System
10 Notes C A s m o o t a c
11 The Endoscopic Doppler in Surveillance Colonoscopy: Guide to Prophylactic Clipping of Subsurface Blood Flow in Post-Polypectomy Induced Ulcers in High Risk Patients Presented By: Dennis M. Jensen, MD, Professor of Medicine, David Geffen School of Medicine at UCLA, Associate Director, CURE DDRC C ase H is to ry An 80 year old Caucasian female was referred for open access surveillance colonoscopy. She had a history of two tubular adenomas without dysplasia 5 years ago. She also had a past history of diverticulitis, mild coronary artery disease (CAD), moderate obesity, gastroesophageal reflux disease (GERD), and osteoarthritis (OA). She stopped taking 81 mg/day of aspirin (for CAD) and ibuprofen 200 mg TID (for OA) two days ago. An elective colonoscopy was performed. 1 1a FIGURE 1. A sessile polyp was seen behind a fold in the right colon on the surveillance colonoscopy. It was smooth and somewhat multi-lobulated, approximately mm in length, 8-10 mm wide, and 6-7 mm high. 2 2a FIGURE 2. A saline, methylene blue mixture was used in multiple injections of 2-6 cc to raise the polyp up, prior to snare polypectomy. This usually lifts benign polyps off the submucosa and facilitates en bloc polyp resection with snare cautery. Then, a rotatable snare was used to perform the polypectomy. Good coagulation without bleeding was achieved. 3 3a FIGURE 3. However, snare polypectomy left a post-polypectomy induced ulcer (PPIU). In the base of the PPIU, there appeared to be a non-bleeding visible vessel (NBVV). The question was whether this was at high risk to cause delayed PPIU bleeding and whether prophylactic treatment was warranted in this patient who needed to resume aspirin for CAD and nonsteroidal anti-inflammatory medications (NSAIDs) for OA (her major chronic co-morbidities). The VTI Endoscopic Doppler System
12 4 4a FIGURE 4. Therefore, a Doppler probe was used to interrogate the base of the PPIU and the visualized NBVV. At the mid depth setting ( 4 mm), arterial blood flow was detected focally below the NBVV and on either side of it for 2-3 mm. This provided a guide for prophylactic hemoclipping of the underlying artery at the NBVV. 5 5a FIGURE 5. Two hemoclips (HC), one on either side of the NBVV in the base of the PPIU as localized by the Doppler probe, were placed with the goal of obliterating arterial blood flow underneath the NBVV. This was focal treatment. This contrasts with a recent recommendation by experts to close PPIUs with multiple hemoclips in patients at a high risk for delayed hemorrhage from the PPIU. Instead, Doppler guided focal treatment of the stigma of recent hemorrhage (SRH) and invisible artery in the PPIU using 2 hemoclips was employed in this case. 6 6a FIGURE 6. After hemoclipping, the Doppler probe was utilized to interrogate the PPIU beneath and around the hemoclips. There was no arterial blood flow detected in the PPIU behind the 2 hemoclips. 7 7a FIGURE 7. Absence of underlying arterial blood flow was confirmed by interrogation with the Doppler probe at different positions in the PPIU, including between the hemoclips, as shown here.
13 Clinical Follow-up The patient had no bleeding during the procedure and none after resuming aspirin and NSAIDs the day after the colonoscopy. The polyp histology was a tubular adenoma without dysplasia. Q & A with Dr. Jensen In high risk patients undergoing routine polypectomy during elective screening or surveillance colonoscopy, how often do you find an artery in PPIUs by Doppler examination? For such patients who have benign appearing colon polyps, we are prospectively studying this issue using Doppler to interrogate non-bleeding PPIUs. To date, the rates of finding focal arteries in PPIUs depends upon the size of the PPIU. For PPIUs < 10 mm, the prevalence rate of arterial blood flow detection was < 5%; for PPIUs mm in size, the rate of Doppler detection of arterial flow was 25%; and for PPIUs > 15 mm, the rate was 56%. How has this information with Doppler interrogation of PPIUs been utilized to prophylactically treat high risk patients? We are utilizing the Doppler finding as a guide to prophylactic treatment with hemoclips to obliterate the arterial blood flow in PPIUs. To obliterate arterial blood flow in the PPIU, hemoclips are placed on either side of the SRH or on either end of the detected invisible vessel as mapped by Doppler after polypectomy. As rechecked by Doppler after the hemoclipping, this has been effective in every case as prophylactic treatment and no patient has had delayed PPIU hemorrhage even after starting anticoagulants or antiplatelet drugs. Why not just use multiple hemoclips to close the PPIU in high risk patients, as reported by other experts, rather than using Doppler, which has the potential of increasing costs of such prophylactic treatment? The answers to this question are very clinically relevant and have important direct cost implications for the future. First, it is not possible to close all PPIUs with current endoscopic hemoclips, particularly any measuring mm. Second, closing the PPIUs without sealing the artery in the base of the PPIU leaves the artery patent -- when the colonic hemoclips fall off, the underlying artery is exposed and potentially can result in delayed PPIU hemorrhage, particularly for patients on anticoagulants or antiplatelet drugs. Third, and relevant to direct costs, is that many hemoclips (5-8) are often necessary to attempt closure of large PPIUs, and all PPIUs after polypectomies in the same patient with multiple polyps removed. When this closure approach is used to close all PPIUs, patients who do not have arteries in the base of PPIUs are automatically treated prophylactically -- this is clinically unnecessary. According to our recent Doppler study of PPIUs, this would include > 95% of PPIUs 10 mm; 75% of PPIUs mm; and 44% of PPIUs 15 mm in size. Fourth, localization of underlying arteries in PPIUs is feasible and easy with Doppler. Endoscopic Doppler facilitates focal treatment of arteries in the PPIU. This eliminates unnecessary hemoclipping or other prophylactic treatments. In my opinion, further study of Doppler guided treatment of high risk patients with PPIUs is needed. Are there outcomes studies that document whether prophylactic hemoclipping improves patient outcomes after elective colonoscopy? These are no randomized controlled studies (RCS) either with or without Doppler to document changes in outcomes such as delayed bleeding rates. However, a recent, large, retrospective cohort study by Drs. H. Liaquat and D. Rex (Gastrointestinal Endoscopy 2013;77:401-7) in high risk patients reported a lower rate of delayed PPIU hemorrhage compared to historical controls without prophylactic endoscopic hemoclipping. There are obvious limitations to such a retrospective study. A prospective RCS utilizing Doppler as a guide to prophylactic treatment in high risk patients such as those on anticoagulants is warranted in my opinion. Meanwhile, focal treatment with hemoclips guided by Doppler should be considered in high risk patients to prevent delayed PPIU hemorrhage. The problem of clinically significant delayed PPIU bleeding is illustrated by the next case presentation ( Endoscopic Doppler in the Management of Lower Gastrointestinal Bleeding: Treatment of Delayed Post-Polypectomy Bleeding ). Scan to view the video that accompanies this case» The VTI Endoscopic Doppler System
14 Endoscopic Doppler in the Management of Lower Gastrointestinal Bleeding: Treatment of Delayed Post-Polypectomy Bleeding Presented By: Dennis M. Jensen, MD, Professor of Medicine, David Geffen School of Medicine at UCLA, Associate Director, CURE DDRC C ase H is to ry A 52 year old Hispanic man with end stage renal disease (ESRD) and dilated cardiomyopathy was an inpatient undergoing evaluation for heart and kidney transplantation. He had a past history of mitral regurgitation, dilated cardiomyopathy, pulmonary and systemic hypertension, and chronic renal failure (on hemodialysis). He had an elective screening colonoscopy 6 days prior to this presentation with cecal polypectomy of a one cm sessile polyp. He had been on 81 mg of aspirin/day and regional heparin with hemodialysis. 1 Six days after the initial colonoscopy, the patient developed inpatient severe hematochezia with hypotension, and severe anemia with a fall in hemoglobin from 9.5 to 7.0. He was transferred to the coronary care unit. A nasogastric (NG) tube was placed which was negative for bile or blood. He then received 8 liters of GoLYTELY colon preparation, 3 units red blood cells (RBCs), and hemodialysis prior to urgent colonoscopy within 15 hours of the start of bleeding. 1a FIGURE 1. The patient s colon was well prepped and there was no intraluminal blood or stool. In the base of the cecum was a small (< 10 mm diameter), shallow, post-polypectomy induced ulcer (PPIU) with a non-bleeding visible vessel (NBVV) in the base. No other lesions with stigmata of recent hemorrhage (SRH) were found on this urgent colonoscopy. 2 2a FIGURE 2. A colon length Doppler probe was used to interrogate the NBVV and base of the PPIU for underlying blood flow, and to map the direction of the vessel. Arterial flow was detected with the shallow ( 1.5 mm) and mid Doppler depth settings ( 4 mm). The artery was mapped as lying straight across the PPIU, detected for about 4-5 mm on either side of the NBVV.
15 3 3a FIGURE 3. Two hemoclips (HC s) were placed, 1 on either side of the NBVV along the course of the underlying artery as mapped by the baseline Doppler examination. Some bleeding was induced but was controlled by the hemoclipping. 4 4a FIGURE 4. The Doppler probe was used to document obliteration of underlying arterial blood flow after application of the two hemoclips. No arterial signal could be detected. cli n ical fo llow- up (after second colonoscopy and hemostasis) The patient continued on aspirin 81 mg/day and resumed evaluation for heart and kidney transplants. He had no rebleeding and was later discharged to await dual organ transplantations. Q & A w i t h D r. J e nse n On how many cases of delayed PPIU hemorrhage have you and your CURE Hemostasis Group performed urgent colonoscopy, and what were the SRH and Doppler findings in these patients? The CURE Hemostasis Research group and I have prospectively evaluated and performed urgent colonoscopy after purge on more than 50 patients with delayed PPIU hemorrhage and more than 90% had SRH, with the most common being NBVV, adherent clot, or flat spot. When the PPIUs were studied with the colonoscopic Doppler probe, 92% had patent arteries underlying the SRH. How are you utilizing Doppler as a guide for focal hemostasis of patients with delayed bleeding from PPIUs? Similar to this case, we localize the artery in the base of the PPIU and treat on either side of the SRH in the PPIU to obliterate underlying arterial blood flow. Hemoclips are almost always used instead of epinephrine (which does not cause permanent obliteration of patent arteries and blood flow) or thermal coagulation (which causes tissue damage, increases the size and depth of the PPIU, may cause transmural damage, and can increase the risk of perforation). Are there cases in which you do not treat PPIUs endoscopically when they have caused delayed bleeding? When Doppler examination does not detect underlying blood flow in clean PPIUs (without SRH) or PPIUs with flat spots, we do not treat these PPIUs endoscopically with hemoclips or other techniques. All those PPIUs with SRH and positive Doppler interrogation for arterial blood flow are currently treated with hemoclips. In patients hospitalized for severe delayed PPIU hemorrhage, why not just close the PPIUs with hemoclips and forgo the use of the Doppler probe? There are multiple reasons and these are the same as for primary prophylactic hemoclipping (refer to previous case for details). Hemoclipping for PPIU closure buries the underlying artery (without occluding it), over-treats patients without Doppler detected arteries underlying SRH (who will not benefit from such treatment), and is usually not possible with current transendoscopically deployed hemoclips (for large PPIUs > mm). I now recommend focal treatment as guided by Doppler, which is easier to perform, and specifically targets the underlying artery. S ca n to vie w t he video t hat accompa n ies t his case» The VTI Endoscopic Doppler System
16 Notes C A s b h h o A s a c
17 Endoscopic Doppler in the Management of Colonic Diverticular Bleeds Presented By: Dennis M. Jensen, MD, Professor of Medicine, David Geffen School of Medicine at UCLA, Associate Director, CURE DDRC C ase H is to ry A 73 year old African American female with polymyositis (on steroids), diabetes mellitus, obesity, and arthritis was admitted by her rheumatologist with severe painless hematochezia. Her hemoglobin (Hgb) fell from 13.5 to 10.0 with IV fluids and she had normal coagulation tests. There was no hypotension, melena or abdominal pain. A nasogastric (NG) tube was placed and removed after bile was suctioned. A private gastroenterologist saw the patient, ordered a colon prep of 4 liters of GoLYTELY, and performed a colonoscopy that afternoon. The colonoscopy showed clots, blood and 1 fluid throughout the colon and rectum, extensive diverticulosis without stigmata of recent hemorrhage (SRH) and large internal hemorrhoids. No definitive diagnosis was possible. Within 8 hours, the hematochezia recurred and the hemoglobin dropped below 9.0. The GI hemostasis team was called to see the patient as a second opinion. The patient received 2 units of packed red blood cells (RBCs). She had an NG tube placed and received 7L of GoLYTELY until the rectal effluent was clear of all clots and blood. An urgent colonoscopy was then performed. 1a FIGURE 1. With the 7 liters of the Golytely prep, the colon was very well prepped. A large deep descending colon diverticulum was found that had a SRH - a non-bleeding visible vessel (NBVV), that was pulsatile, located in the diverticulum base. This represented the bleeding site and was classified as a definitive diverticular hemorrhage. There was also some fresh blood in and around the diverticulum. An artery was seen to cross the base of the diverticulum. 2 2a FIGURE 2. A colon length Doppler probe was used to interrogate the NBVV. This yielded a loud arterial signal on the NBVV and on either side of it for < 5 mm, at the shallow ( 1.5 mm) and mid ( 4 mm) Doppler depth settings. 3 3a FIGURE 3. An injection needle was used to place 1:20,000 epinephrine submuscosally in 1-2 cc aliquots in the base of the diverticulum TIC and around the NBVV. Blanching and vasoconstriction of the muscosa was evident. The VTI Endoscopic Doppler System
18 4 4a FIGURE 4. With the diverticulum rotated 90 degrees by the endoscopist so that the artery ran from the 12 to the 6 o clock direction, a total of three hemoclips were deployed in the base of the diverticulum. One hemoclip was placed on the NBVV and one on either side of it, along the artery. 5 5a FIGURE 5. The Doppler probe was used to check for residual blood flow along the artery in the base of the diverticulum after placement of the three hemoclips. No Doppler signal was detected, so no further endoscopic treatment was required. 6 6a FIGURE 6. Spot tattoos were placed near the diverticulum with the NBVV, to help relocate the diverticulum, if rebleeding occurred. C li n ical Fo llow- up After the procedure, the patient resumed her regular medications and was advanced from a full-liquid to normal diet within 24 hours. The patient had no abdominal discomfort or complications. She has been followed for four years and has not had further colonic bleeding.
19 Q & A with Dr. Jensen In patients with a diagnosis of diverticular hemorrhage, how often does your group find a diverticulum with SRH and make a diagnosis of definitive diverticular bleed? With urgent colonoscopy in hospitalized patients after purging with 6-8 liters of polyethylene glycol based prep, about one third of patients with true diverticular hemorrhage have a definitive diverticular hemorrhage diagnosed and about two thirds have presumptive diverticular bleeding. The latter is diagnosed when we find diverticula without SRH but presume the diverticula to be the source of bleeding because all other procedures are negative for SRH or other lesions (e.g. anoscopy, push enteroscopy, and capsule endoscopy). How often is the Doppler examination positive in patients with SRH (e.g. definitive diverticular hemorrhage) vs. no SRH (e.g. presumptive diverticular hemorrhage)? In ongoing studies prior to endoscopic treatment of SRH, interrogation with a Doppler probe gave an arterial signal in 92% of the definitive diverticular bleed group (22 of 24 patients). In the patients with presumptive diverticular bleeding, arterial blood flow was not detected in any patient (0% - 0 of 22 patients), despite the fact that vessels were seen either at the neck or in the base of the diverticula in the presumptive group. How has the Doppler probe helped you beyond what you can see via colonoscopy in patients with diverticular hemorrhage? The Doppler probe refines both risk stratification and treatment of definitive diverticular bleeds. In several cases when colonoscopists found a flat spot, erosion, or small clot either at the neck or base of the diverticulum and were uncertain about whether these were true SRH, the Doppler probe interrogation revealed arterial blood flow and a definitive diagnosis could be made. These lesions were then treated. The Doppler probe also allows the colonoscopist to map the direction of the artery and guide treatment along the artery on either side of the SRH. Finally, checking for residual blood flow after standard colonoscopic treatment confirms complete hemostasis. Those with residual blood flow warrant further, safe treatment to yield definitive hemostasis. What is complete hemostasis of definitive diverticular hemorrhage? I define complete hemostasis as control of active bleeding, flattening with MPEC treatment or hemoclipping of NBVV (if present), and absence of residual arterial blood flow underneath and nearby the SRH after colonoscopic treatments. I recommend hemoclipping of SRH and arteries in the base of diverticula. This treatment with hemoclips on the SRH and on either side of it is to obliterate underlying blood flow. Confirmation of no residual blood flow after treatment is performed using the Doppler probe. Alternatively, MPEC treatment is recommended with coaptive coagulation if the SRH is at the neck of the diverticulum, and is followed by checking for residual blood flow with Doppler after treatment. What do you do if there is residual arterial flow after visually guided hemostasis and what do you use to complete hemostasis? If colonoscopic treatment was in the base or neck of the diverticulum with hemoclips, I apply more hemoclips on the focal point where the Doppler signal was still positive after initial treatment. If MPEC treatment was used at the neck, I apply more MPEC coagulation with the side of the probe at low power (12 watts, 2 second pulses), moderate pressure preferably with a 10 French (F) sized probe. Alternatively, I hemoclip the point where the Doppler was positive for residual arterial blood flow. It is important to repeat the Doppler interrogation after treatment. I also tattoo the area nearby the diverticulum with the SRH in case the patient rebleeds and it is necessary to find the bleeding site. The VTI Endoscopic Doppler System
20 Vascular Technology 12 Murphy Drive Nashua, NH The VTI Endoscopic Doppler System* Ordering Information: International: The procedures and patient care expressed or depicted in these cases are those of the physician and do not necessarily reflect the opinions, policies or recommendations of Vascular Technology or any of its employees. For further information and detailed instructions on the use of Vascular Technology s Endoscopic Doppler System, please refer to the Instructions for Use included with Vascular Technology s product packages. Indications, Contraindications, Warnings and Instructions for Use can be found in the product labeling supplied with each device. Rx Only. GoLYTELY is a trademark of Braintree Laboratories, Inc. Spot is a trademark of GI Supply Vascular Technology *US Patent No. 8,206, Rev0
HemoClip: Guidelines & Atlas
 HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD
 Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding.
 Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding. Through innovation and continuous educational support, we offer a wide range
Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding. Through innovation and continuous educational support, we offer a wide range
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D.
 Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
Endoscopic Management of Acute Lower Gastrointestinal Bleeding
 American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2008.02075.x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management
UGI Tract Hemorrhage. GI Tract Emergencies. UGI Hemorrhage. David D. Markowitz, MD. UGI tract hemorrhage Comorbid disease
 UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
understanding GI bleeding
 understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
How to Effectively Code for Endoscopic Procedures in Gastroenterology
 How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication.
 Captivator II Single-Use Snares The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare
Captivator II Single-Use Snares The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare
LOWER GASTROINTESTINAL BLEEDING GED/05/08
 LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
Flexible sigmoidoscopy the procedure explained Please bring this booklet with you
 Flexible sigmoidoscopy the procedure explained Please bring this booklet with you Exceptional healthcare, personally delivered Introduction You have been advised by your GP or hospital doctor to have an
Flexible sigmoidoscopy the procedure explained Please bring this booklet with you Exceptional healthcare, personally delivered Introduction You have been advised by your GP or hospital doctor to have an
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
Patients who fail to bring a driver/someone to stay with them for the night will have their procedure cancelled immediately.
 Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Colonoscopy Data Collection Form
 Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Stopping Anti-platelet Agents: Will You Cause a Stroke?
 Stopping Anti-platelet Agents: Will You Cause a Stroke? Glenn M. Eisen MD,MPH The Oregon Clinic-West Hills GI Clinical Professor of Medicine, OHSU Thanks for staying. 1 Don t cause a stroke Objective(s)
Stopping Anti-platelet Agents: Will You Cause a Stroke? Glenn M. Eisen MD,MPH The Oregon Clinic-West Hills GI Clinical Professor of Medicine, OHSU Thanks for staying. 1 Don t cause a stroke Objective(s)
ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding
 PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
Captivator II. Single-Use Snares
 Captivator II Single-Use Snares Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare line
Captivator II Single-Use Snares Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare line
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
STROKE PREVENTION IN ATRIAL FIBRILLATION. TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: ABBREVIATIONS: BACKGROUND:
 STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
HOW I DO IT Approach to lower gastrointestinal bleeding
 HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
The degree of liver inflammation or damage (grade) Presence and extent of fatty liver or other metabolic liver diseases
 ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
A. Ketorolac*** B. Naproxen C. Ibuprofen D. Celecoxib
 1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
Atrial fibrillation: medicines to help reduce your risk of a stroke what are the options?
 Patient decision aid Atrial fibrillation: medicines to help reduce your risk of a stroke what are the options? http://guidance.nice.org.uk/cg180/patientdecisionaid/pdf/english Published: June 2014 About
Patient decision aid Atrial fibrillation: medicines to help reduce your risk of a stroke what are the options? http://guidance.nice.org.uk/cg180/patientdecisionaid/pdf/english Published: June 2014 About
Learning Luncheon 7: Endoscopic Mucosal Resection: When, Where and How?
 Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Post-DDW OAG Course - Therapeutic Endoscopy
 Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
Evolution of Barrett s esophagus
 Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Inpatient Anticoagulation Safety. To provide safe and effective anticoagulation therapy through a collaborative approach.
 Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Prescriber Guide. 20mg. 15mg. Simply Protecting More Patients. Simply Protecting More Patients
 Prescriber Guide 20mg Simply Protecting More Patients 15mg Simply Protecting More Patients 1 Dear Doctor, This prescriber guide was produced by Bayer Israel in cooperation with the Ministry of Health as
Prescriber Guide 20mg Simply Protecting More Patients 15mg Simply Protecting More Patients 1 Dear Doctor, This prescriber guide was produced by Bayer Israel in cooperation with the Ministry of Health as
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Patient information on endoscopic mucosal resection (EMR) (Endoscopic removal of polyps) Your questions answered
 Patient information on endoscopic mucosal resection (EMR) (Endoscopic removal of polyps) Your questions answered Page 1 of 7 Contents What is a colonic polyp Page 3 What is an endoscopic mucosal resection
Patient information on endoscopic mucosal resection (EMR) (Endoscopic removal of polyps) Your questions answered Page 1 of 7 Contents What is a colonic polyp Page 3 What is an endoscopic mucosal resection
Having an Endoscopic Mucosal Resection (EMR)
 Having an Endoscopic Mucosal Resection (EMR) Patient Information Author ID: N Prasad Leaflet Number: End 011 Name of Leaflet: Having an Endoscopic Mucosal Resection (EMR) Date Produced: March 2014 Review
Having an Endoscopic Mucosal Resection (EMR) Patient Information Author ID: N Prasad Leaflet Number: End 011 Name of Leaflet: Having an Endoscopic Mucosal Resection (EMR) Date Produced: March 2014 Review
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR)
 HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
DVT/PE Management with Rivaroxaban (Xarelto)
 DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
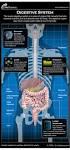 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial
 Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy. Case Series
 ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
Anticoagulants in Atrial Fibrillation
 Anticoagulants in Atrial Fibrillation Starting and Stopping Them Safely Carmine D Amico, D.O. Overview Learning objectives Introduction Basic concepts Treatment strategy & options Summary 1 Learning objectives
Anticoagulants in Atrial Fibrillation Starting and Stopping Them Safely Carmine D Amico, D.O. Overview Learning objectives Introduction Basic concepts Treatment strategy & options Summary 1 Learning objectives
ESD for colorectal lesions I am in favour. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
LOWER GI ENDOSCOPIES So why is CMS yanking our chain? General Concepts for all GI Endoscopy Procedures
 LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
What is Barrett s esophagus? How does Barrett s esophagus develop?
 Barrett s Esophagus What is Barrett s esophagus? Barrett s esophagus is a pre-cancerous condition affecting the lining of the esophagus, the swallowing tube that carries foods and liquids from the mouth
Barrett s Esophagus What is Barrett s esophagus? Barrett s esophagus is a pre-cancerous condition affecting the lining of the esophagus, the swallowing tube that carries foods and liquids from the mouth
TEST QUESTIONS GASTROINTESTINAL BLEEDING
 TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding
 Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
STROKE PREVENTION IN ATRIAL FIBRILLATION
 STROKE PREVENTION IN ATRIAL FIBRILLATION OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention of ischemic stroke and arterial thromboembolism in patients
STROKE PREVENTION IN ATRIAL FIBRILLATION OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention of ischemic stroke and arterial thromboembolism in patients
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
COLORECTAL CANCER SCREENING
 COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
These parameters cannot, at the present time, be determined by non-invasive imaging techniques.
 Endoscopic Mucosal Resection for Upper Gastrointestinal Lesions Kenneth K. Wang, M.D. Chairman, WEO Publication and Guidelines Committee Professor of Medicine, Mayo Clinic Rochester, Minnesota Upper gastrointestinal
Endoscopic Mucosal Resection for Upper Gastrointestinal Lesions Kenneth K. Wang, M.D. Chairman, WEO Publication and Guidelines Committee Professor of Medicine, Mayo Clinic Rochester, Minnesota Upper gastrointestinal
A Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation
 Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation A Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation PATIENT EDUCATION GUIDE What is atrial fibrillation? Atrial fibrillation
Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation A Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation PATIENT EDUCATION GUIDE What is atrial fibrillation? Atrial fibrillation
Dorset Cardiac Centre
 P a g e 1 Dorset Cardiac Centre Patients with Atrial Fibrillation/Flutter undergoing DC Cardioversion or Ablation procedures- Guidelines for Novel Oral Anti-coagulants (NOACS) licensed for this use February
P a g e 1 Dorset Cardiac Centre Patients with Atrial Fibrillation/Flutter undergoing DC Cardioversion or Ablation procedures- Guidelines for Novel Oral Anti-coagulants (NOACS) licensed for this use February
New Treatments for Stroke Prevention in Atrial Fibrillation. John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013
 New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
Planning: Patient Goals and Expected Outcomes The patient will: Remain free of unusual bleeding Maintain effective tissue perfusion Implementation
 Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Presence and extent of fatty liver or other metabolic liver diseases
 UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
UC San Diego Health System Patient Information Sheet: Liver Biopsy What is a Liver Biopsy? A liver biopsy is a procedure where a qualified doctor (typically a hepatologist, radiologist or gastroenterologist)
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
9/28/15. Dabigatran. Rivaroxaban. Apixaban. Edoxaban. From the AC Forum Centers of Excellence website: Dabigatran, Rivaroxaban, & Apixaban
 Identify the FDA approved direct oral anticoagulants (DOACs) Linda Kelly, PharmD, PhC, CACP Presbyterian Healthcare Services Distinguish the differences in the dosing of DOACs for various indications Describe
Identify the FDA approved direct oral anticoagulants (DOACs) Linda Kelly, PharmD, PhC, CACP Presbyterian Healthcare Services Distinguish the differences in the dosing of DOACs for various indications Describe
Case Presentation: Diminutive polyps. Siwan Thomas-Gibson St. Marks Hospital London UK
 Case Presentation: Diminutive polyps Siwan Thomas-Gibson St. Marks Hospital London UK Case History 65 year old gentleman Bowel cancer screening FOBT positive No bowel symptoms No family history Smoker
Case Presentation: Diminutive polyps Siwan Thomas-Gibson St. Marks Hospital London UK Case History 65 year old gentleman Bowel cancer screening FOBT positive No bowel symptoms No family history Smoker
2016 Quick Reference Coding Chart
 43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
SAGES 2015 Flexible Endoscopy Course for Fellows
 Goals and Objectives: At the end of the course, the MIS fellow will be familiar with GI endoscopes, towers, and the instruments used for endoscopy and endoscopic surgery. The fellow will also be able to
Goals and Objectives: At the end of the course, the MIS fellow will be familiar with GI endoscopes, towers, and the instruments used for endoscopy and endoscopic surgery. The fellow will also be able to
Dabigatran (Pradaxa) Guidelines
 Dabigatran (Pradaxa) Guidelines Dabigatran is a new anticoagulant for reducing the risk of stroke in patients with atrial fibrillation. Dabigatran is a direct thrombin inhibitor, similar to warfarin, without
Dabigatran (Pradaxa) Guidelines Dabigatran is a new anticoagulant for reducing the risk of stroke in patients with atrial fibrillation. Dabigatran is a direct thrombin inhibitor, similar to warfarin, without
Surgical Management of GI Bleeding. VA Case Presentation. 0-24 hours 9/18/2012
 Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
Developing an endoscopic mucosal resection service in a district general hospital
 RESEARCH Developing an endoscopic mucosal resection service in a district general hospital Chris A Lamb, 1 Jamie A Barbour 2 1 Institute of Cellular Medicine, Newcastle University, The Medical School,
RESEARCH Developing an endoscopic mucosal resection service in a district general hospital Chris A Lamb, 1 Jamie A Barbour 2 1 Institute of Cellular Medicine, Newcastle University, The Medical School,
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Physician and other health professional services
 O n l i n e A p p e n d i x e s 4 Physician and other health professional services 4-A O n l i n e A p p e n d i x Access to physician and other health professional services 4 a1 Access to physician care
O n l i n e A p p e n d i x e s 4 Physician and other health professional services 4-A O n l i n e A p p e n d i x Access to physician and other health professional services 4 a1 Access to physician care
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES.
 PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
PHARMACOLOGICAL Stroke Prevention in Atrial Fibrillation STROKE RISK ASSESSMENT SCORES Vs. BLEEDING RISK ASSESSMENT SCORES. Hossam Bahy, MD (1992 2012), 19 tools have been identified 11 stroke scores 1
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
NHS FORTH VALLEY Rivaroxaban for Stroke Prevention in Atrial Fibrillation
 NHS FORTH VALLEY Rivaroxaban for Stroke Prevention in Atrial Fibrillation Date of First Issue 06/06/2012 Approved 06/06/2012 Current Issue Date 06/06/2012 Review Date 06/06/2014 Version 1.1 EQIA Yes /
NHS FORTH VALLEY Rivaroxaban for Stroke Prevention in Atrial Fibrillation Date of First Issue 06/06/2012 Approved 06/06/2012 Current Issue Date 06/06/2012 Review Date 06/06/2014 Version 1.1 EQIA Yes /
Stroke: Major Public Health Burden. Stroke: Major Public Health Burden. Stroke: Major Public Health Burden 5/21/2012
 Faculty Prevention Sharon Ewer, RN, BSN, CNRN Stroke Program Coordinator Baptist Health Montgomery, Alabama Satellite Conference and Live Webcast Monday, May 21, 2012 2:00 4:00 p.m. Central Time Produced
Faculty Prevention Sharon Ewer, RN, BSN, CNRN Stroke Program Coordinator Baptist Health Montgomery, Alabama Satellite Conference and Live Webcast Monday, May 21, 2012 2:00 4:00 p.m. Central Time Produced
Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013
 Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013 Family physician with Rivergrove Medical Clinic Practice in the north end since 1985 Medical Director of the Wellness
Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013 Family physician with Rivergrove Medical Clinic Practice in the north end since 1985 Medical Director of the Wellness
SIGN. Management of acute upper and lower gastrointestinal bleeding. September 2008. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
UW MEDICINE PATIENT EDUCATION. Xofigo Therapy. For metastatic prostate cancer. What is Xofigo? How does it work?
 UW MEDICINE PATIENT EDUCATION Xofigo Therapy For metastatic prostate cancer This handout explains how the drug Xofigo is used to treat metastatic prostate cancer. What is Xofigo? Xofigo is a radioactive
UW MEDICINE PATIENT EDUCATION Xofigo Therapy For metastatic prostate cancer This handout explains how the drug Xofigo is used to treat metastatic prostate cancer. What is Xofigo? Xofigo is a radioactive
New Oral Anticoagulants. How safe are they outside the trials?
 New Oral Anticoagulants How safe are they outside the trials? Objectives The need for anticoagulant therapy Indications for anticoagulation Traditional anticoagulant therapies Properties of new oral anticoagulants
New Oral Anticoagulants How safe are they outside the trials? Objectives The need for anticoagulant therapy Indications for anticoagulation Traditional anticoagulant therapies Properties of new oral anticoagulants
CHADS score of 5 or 6 Recent (within 3mo) stroke or TIA Rheumatic valvular heart disease CHADs score of 3 or 4
 LAMC Department of Pharmacy Services: ANTICOAGULATION: Surgical Intervention Table 1: Classification of Surgical interventions according to bleeding risk t required to discontinue anticoagulation Dental
LAMC Department of Pharmacy Services: ANTICOAGULATION: Surgical Intervention Table 1: Classification of Surgical interventions according to bleeding risk t required to discontinue anticoagulation Dental
CLINICAL GUIDELINE FOR MANAGEMENTS OF PATIENTS TAKING ANTICOAGULANTS IN ENDOSCOPY 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR MANAGEMENTS OF PATIENTS TAKING ANTICOAGULANTS IN ENDOSCOPY 1. Aim/Purpose of this Guideline 1.1. The purpose of this guideline is to assist decision making of whether anticoagulants
CLINICAL GUIDELINE FOR MANAGEMENTS OF PATIENTS TAKING ANTICOAGULANTS IN ENDOSCOPY 1. Aim/Purpose of this Guideline 1.1. The purpose of this guideline is to assist decision making of whether anticoagulants
Common Pathology Diagnoses: ICD-9 to ICD-10 Mapping
 PERFORMANCE THAT MATTERS NUMBER OF CODES 14,000 69,000 ICD-9 DIAGNOSIS CODES ICD-10 DIAGNOSIS CODES CODE STRUCTURE ICD-9-CM CODE FORMAT ICD-10-CM CODE FORMAT X X X X X X X X X X X X CATEGORY ETIOLOGY,
PERFORMANCE THAT MATTERS NUMBER OF CODES 14,000 69,000 ICD-9 DIAGNOSIS CODES ICD-10 DIAGNOSIS CODES CODE STRUCTURE ICD-9-CM CODE FORMAT ICD-10-CM CODE FORMAT X X X X X X X X X X X X CATEGORY ETIOLOGY,
MEDICAL ASSISTANCE HANDBOOK PRIOR AUTHORIZATION OF PHARMACEUTICAL SERVICES. A. Prescriptions That Require Prior Authorization
 MEDICAL ASSISTANCE HBOOK PRI AUTHIZATION OF PHARMACEUTICAL SERVICES I. Requirements for Prior Authorization of Anticoagulants A. Prescriptions That Require Prior Authorization Prescriptions for Anticoagulants
MEDICAL ASSISTANCE HBOOK PRI AUTHIZATION OF PHARMACEUTICAL SERVICES I. Requirements for Prior Authorization of Anticoagulants A. Prescriptions That Require Prior Authorization Prescriptions for Anticoagulants
Endo Conference: Large Polypectomy & EMR
 Endo Conference: Large Polypectomy & EMR Dr. Whang Feb 3, 2015 VOGELGRAM: genetic pathway of colorectal cancer & genes affected by point mutations Outline I. Baseline Colonoscopy II. Colon Polyps III.
Endo Conference: Large Polypectomy & EMR Dr. Whang Feb 3, 2015 VOGELGRAM: genetic pathway of colorectal cancer & genes affected by point mutations Outline I. Baseline Colonoscopy II. Colon Polyps III.
MEDICAL ASSISTANCE HANDBOOK PRIOR AUTHORIZATION OF PHARMACEUTICAL SERVICES. A. Prescriptions That Require Prior Authorization
 MEDICAL ASSISTANCE HBOOK I. Requirements for Prior Authorization of Anticoagulants A. Prescriptions That Require Prior Authorization Prescriptions for Anticoagulants which meet any of the following conditions
MEDICAL ASSISTANCE HBOOK I. Requirements for Prior Authorization of Anticoagulants A. Prescriptions That Require Prior Authorization Prescriptions for Anticoagulants which meet any of the following conditions
COMPARISON OF NEW ORAL ANTICOAGULANTS AND FREQUENTLY- ASKED QUESTIONS FROM PATIENTS. TARGET AUDIENCE: All Canadian health care professionals.
 COMPARISON OF NEW ORAL ANTICOAGULANTS AND FREQUENTLY- ASKED QUESTIONS FROM PATIENTS AND PHYSICIANS TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVES: To provide a comparison of the new
COMPARISON OF NEW ORAL ANTICOAGULANTS AND FREQUENTLY- ASKED QUESTIONS FROM PATIENTS AND PHYSICIANS TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVES: To provide a comparison of the new
