American Journal of Gastroenterology ISSN
|
|
|
- Ann Paul
- 10 years ago
- Views:
Transcription
1 American Journal of Gastroenterology ISSN C 2006 by Am. Coll. of Gastroenterology doi: /j x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients with High-Risk Peptic Ulcer Bleeding After Successful Endoscopic Epinephrine Injection: A Prospective Randomized Comparative Trial Hwai-Jeng Lin, M.D., F.A.C.G., 1,2 Wen-Ching Lo, M.D., 3 Yang-Chih Cheng, M.D., 1,2 and Chin-Lin Perng, M.D., F.A.C.G. 4 1 Division of Gastroenterology, Department of Medicine, VGH-TAIPEI; 2 School of Medicine, National Yang-Ming University; 3 Zhongxiao Municipal Hospital, Taipei; and 4 I-Lan Hospital, Department of Health, Taiwan BACKGROUND: METHODS: Epinephrine injection is the most common endoscopic therapy for peptic ulcer bleeding. Controversy exists concerning the optimal dose of proton pump inhibitors (PPI) for patients with bleeding peptic ulcers after successful endoscopic therapy. The objective of this study was to determine the optimal dose of PPI after successful endoscopic epinephrine injection in patients with bleeding peptic ulcers. A total of 200 peptic ulcer patients with active bleeding or nonbleeding visible vessels (NBVV) who had obtained initial hemostasis with endoscopic injection of epinephrine were randomized to receive omeprazole 40 mg infusion every 6 h, omeprazole 40 mg infusion every 12 h or cimetidine (CIM) 400 mg infusion every 12 h. Outcomes were checked at 14 days after enrollment. RESULTS: Rebleeding episodes were fewer in the group with omeprazole 40 mg infusion every 6 h (6/67, 9%) as compared with that of the CIM infusion group (22/67, 32.8%, p < 0.01). The volume of blood transfusion was less in the group with omeprazole 40 mg every 6 h than in those groups with omepraole 40 mg infusion every 12 h (p = 0.001) and CIM 400 mg infusion every 12 h (p < 0.001). The hospital stay, number of patients requiring urgent operation, and death rate were not statistically different among the three groups. CONCLUSION: A combination of endoscopic epinephrine injection and a large dose of omeprazole infusion is superior to combined endoscopic epinephrine injection with CIM infusion for preventing recurrent bleeding from peptic ulcers with active bleeding or NBVV. (Am J Gastroenterol 2006;101: ) INTRODUCTION A bleeding peptic ulcer remains a serious medical problem with significant morbidity and mortality. Endoscopic therapy significantly reduces further bleeding, surgery, and mortality in patients with bleeding peptic ulcers and is now recommended as the first hemostatic modality for these patients (1, 2). Epinephrine injection alone or in combination with another technique has become the most popular endoscopic therapy for peptic ulcer bleeding because of its safety, low cost, and ease of application (3). Whether epinephrine injection in combination with a second hematostatic therapy is better than epinephrine injection alone remains controversial (4 6). Although a high initial hemostatic rate can be obtained with endoscopic injection of epinephrine, rebleeding occurs in 10 36% of these patients (3, 7, 8). In previous studies, patients received H-2 receptor-antagonists (H2RAs) intravenously after successful endoscopic hemostasis. In this way, intragastric ph could not be maintained higher than 4.0 for a long period in such patients (9 12). Therefore, their rebleeding rates were higher than expected. Pharmacologically, omeprazole can quickly achieve an optimal intragastric ph condition for support of the physiological cascade of hemostasis (13). The optimal dose has been determined as continuous infusion of 8 mg/h or 160 mg/day of omeprazole (13 15). If we used a proton pump inhibitor (PPI) instead of H2RAs following endoscopic therapy, would it be possible to prevent further bleeding in high-risk patients? So far, there have been several points of controversy concerning high-dose PPI, e.g., cost-effectiveness, ideal dosage, and whether such a regimen should be reserved for highrisk patients (6). Large dose of IV PPI has been found to 500
2 Omeprazole in Patients with Ulcer Bleeding 501 be effective in reducing rebleeding after successful endoscopic therapy (16 19). In contrast, there have been other reports of regular IV doses, regular or higher oral doses of PPI that could reduce the rebleeding rate as well (20 23). So far, the evidence of the efficacy of IV PPI after endosocpic epinephrine injection is still scarce. Therefore, it would be interesting to investigate the role and optimal dose of PPI in high-risk bleeding ulcer patients after successful endoscopic injection with epinephrine. The objective of this study is to assess the optimal dose of IV omeprazole versus cimetidine (CIM) in patients with bleeding peptic ulcers after initial hemostasis has been achieved with endoscopic injection of epinephrine. METHODS Patients were accepted for endoscopic therapy if a peptic ulcer with active bleeding or a nonbleeding visible vessel (NBVV) was observed within 12 h of hospital admission. The possibility of endoscopic therapy was discussed with patients and/or their relatives and a written informed consent was obtained before the trial. After initial hemostasis was achieved with endoscopic injection of diluted epinephrine, the patients were enrolled in this study. The study was approved by the Clinical Research Committee of the Veterans General Hospital, Taipei, Taiwan. Patients were excluded from the study if they were pregnant, did not obtain initial hemostasis with endoscopic injection of epinephrine, did not give written informed consent, had bleeding tendency (platelet count < /L, serum prothrombin <30% of normal, or were taking anticoagulants), uremia, or bleeding gastric cancer. For enrolled patients, an Olympus GIF-XQ240 end-view endoscope and an NM-8L injector were used to perform endoscopic injection. Epinephrine 1:10,000, ml aliquots was injected around the bleeder or NBVV. In general, approximately 8 20 ml of diluted epinephrine was injected for each bleeder. Patients enrolled in the study were randomly allocated into three groups using sealed envelopes containing a therapeutic option (CIM, omeprazole 40 mg q12 h and omeprazole 40 mg q6 h) derived from a randomized table. In the CIM group, we gave 400 mg continuous infusion every 12 h for 3 days. Thereafter, 400 mg of CIM was given orally twice daily for 2 months. In the omeprazole 40 mg q12 h (OME40q12h) group, we gave 40 mg omeprazole (AstraZeneca, Molndal, Sweden) continuous infusion every 12 h for 3 days. Thereafter, 20 mg omeprazole was given orally once daily for 2 months. In the omeprazole 40 mg q6 h (OME40q6h) group, we gave 40 mg continuous infusion every 6 h for 3 days. Thereafter, 20 mg omeprazole was given orally once daily for 2 months. Endoscopy was undertaken 72 h after enrollment. If no blood clot or hemorrhage was observed at the ulcer base, the patient was discharged and followed up in the outpatient department. Patients vital signs were checked every hour for the first 12 h, every 2 h for the second 12 h, and every 4 h for the following 24 h until they stabilized, then four times daily. The hemoglobin level and hematocrit were checked at least once daily, and a blood transfusion was given if the hemoglobin level decreased to lower than 90 g/l or if the patient s vital signs deteriorated. The attending physicians or surgeons were made aware of the exact endoscopic findings and treatment given in each case. Active bleeding was defined as a continuous blood flow spurting or oozing from the ulcer base. An NBVV at endoscopy was defined as a discrete protuberance at the ulcer base that was resistant to washing and was often associated with the freshest clot in the ulcer base. Shock was defined as systolic blood pressure lower than 100 mmhg and a pulse rate of more than 100/min accompanied by cold sweats, pallor, and oliguria. Initial hemostasis was defined as no visible hemorrhage lasting for 5 min after endoscopic therapy. Ultimate hemostasis was defined as no rebleeding during the 14 days following endoscopic therapy. Rebleeding was suspected upon unstable vital signs, continuous tarry, bloody stools, or a drop in the hemoglobin level of more than 20 g/l within 24 h was observed during hospitalization. For these patients, an emergency endoscopy was performed immediately. Rebleeding was determined if a fresh blood clot or bleeding in the ulcer base was found after endoscopic therapy. All patients with rebleeding were treated with heater probe thermocoagulation (HPT) unless they refused. For the HPT, we used an Olympus GIF-XQ240 endoscope or an Olympus GIF-2T10 endoscope, an Olympus heater probe unit (Olympus Optical, Tokyo, Japan) and a 2.4 or 3.2 mm probe. During therapy, the distal tip of the heater probe was applied directly to the bleeding site. Initially, four to five pulses of 30 J/pulse were given. Afterwards, we withdrew the probe slowly. If rebleeding occurred, we repeated the above procedure until the bleeding stopped. Thereafter, we gave several pulses of J/pulse in the area surrounding the bleeding site. The bleeding site was observed for 5 min. It was then challenged with maximal water irrigation for 10 s. If any further bleeding occurred, we started the initial procedure again as above. An emergency operation was performed if bleeding could not be controlled with HPT or if rebleeding occurred after two attempts with HPT therapy. At entry to the study, the following data were recorded: age, sex, the location of the ulcer (esophagus, stomach, and duodenum), ulcer size, the appearance of the gastric contents (clear, coffee ground, and blood), endoscopic findings (spurting, oozing, and NBVV), number of shock, hemoglobin, number of patients with nonsteroidal anti-inflammatory drugs ingestion, number of positive rapid urease test, and comorbid illness. The primary end points were recurrent bleeding before discharge and within 14 days. At day 14, volume of blood transfused, number of surgeries performed, and the mortality rates of the three groups were compared as well. Patients who had positive urease tests received a 1-wk course of omeprazole (20 mg twice daily), clarithromycin (500 mg twice daily), and amoxicillin (1 g twice daily) after discharge.
3 502 Lin et al. The sample size estimation was based on an expected rebleeding rate of 30% in the CIM group (8). The trial was designed to detect a 25% difference in favor of the omeprazole group with a type I error of 0.05 and type II error of 0.2. At least 43 patients were required for each group. One way analysis of variance was used to compare age, volume of blood transfusion, volume of injected epinephrine, ulcer size, hemoglobin, and length of hospital stay. The χ 2 test, with or without Yates s correction, and Fisher s exact test were used when appropriate to compare the location of bleeders, endoscopic findings, gastric contents, number of patients with Helicobacter pylori infection, number of patients with NSAID ingestion, number in shock, number with comorbid illness, hemostasis, emergency operation, and mortality among three groups. A p value of less than 0.05 was considered significant. RESULTS Between January 2003 and January 2005, 1,721 patients whose main symptoms were hematemesis, tarry stool, or both, visited the emergency room. A total of 1,520 patients received an emergency endoscopic examination within 12 h of arrival at the emergency department. A total of 1,380 patients had peptic ulcers. Patients with active bleeding or NBVV were found in 214 patients (Fig. 1). Fourteen patients were excluded from the study for the following reasons: lack of informed consent (n = 2), bleeding tendency (n = 3), lack of cooperation (n = 2), gastric malignancy (n = 3), and in- ability to obtain initial hemostasis with endoscopic injection of epinephrine (n = 4). In total, there were 200 patients enrolled in this study (66 patients in the OME40q12h group, 67 patients in the OME40q6h group, and 67 patients in the CIM group). The three groups were well matched for the factors affecting outcome (Table 1). Table 2 shows the clinical outcome of the studied patients. We injected a similar dose of epinephrine among three groups. Rebleeding occurred in 14 (21.2%) patients in the OME40q12h group (7 patients within 24 h, four on the 2nd day, and three on the 3rd day), 6 (9%) patients in the OME40q6h group (5 patients within 24 h, 1 on the 2nd day), and 22 (32.8%) patients in the CIM group (18 patients within 24 h, 2 on the 2nd day, one on the 3rd day, and 1 on the 7th day). The rebleeding rate of the OME40q6h group was lower than that of the CIM group (p = , risk ratio = 0.27, 95% CI: ). During routine follow-up endoscopic examination on the 3rd day, ulcers with clean bases were found in 42 patients (OMEq12h), 50 patients (OMEq6h), and 40 patients (CIM); ulcers with pigmented spots were found in 10 patients (OMEq12h), 11 patients (OMEq6h), and 6 patients (CIM), respectively. Rebleeding occurred in 14 patients (21.2%) in the OME40q12h group. Of these patients, 11 patients received heater probe therapy and recovered uneventfully; 1 patient received embolization and recovered uneventfully; 1 patient received injection of epinephrine plus pure ethanol (he died of sepsis and continuous bleeding thereafter); 1 patient refused Patients with active bleeding or NBVV (n=214) Exclusion (n=14) Lack of consent (n=2) Bleeding tendency (n=3) Lack of cooperation (n=2) Gastric malignany (n-3) Inability to obtain initial hemostasis (n=4) Patients randomized and treated (n=200) OME40q12h (n=66) OME40q6h (n=67) Cimetidine (n=67) Rebleeding (n=14) Hemostasis (n=52) Rebleeding (n=6) Hemostasis (n=61) Rebleeding (n=22) Hemostasis (n=45) Figure 1. Test profile. Patients with active bleeding or NBVV.
4 Omeprazole in Patients with Ulcer Bleeding 503 Table 1. Clinical Variables of Patients at Entry to the Study OME40q6h OME40q12h CIM (n = 67) (n = 66) (n = 67) Age (mean, yr) Sex (M/F) 58/9 57/9 61/6 Location of bleeders Stomach Duodenum Esophagus Endoscopic findings Spurting Oozing NBVV Clot Gastric contents Blood Coffee grounds Clear Number in shock Number with medical illness Mean ulcer size (cm) Number of positive urease test Number with NSAID ingestion Mean hemoglobin (g/l) Mean body weight (kg) No statistical difference among three groups. further management and died thereafter. Rebleeding occurred in 6 patients in the OME40q6h group. They received heater probe therapy and recovered uneventfully. Rebleeding occurred in 22 patients in the CIM group. Of these patients, 14 patients received heater probe therapy and recovered uneventfully; 2 patients received injection of epinephrine plus pure ethanol and recovered uneventfully; 3 patients refused further endosocpic therapy due to underlying malignancy and died thereafter; 3 patients received operation and recovered smoothly. The volume of blood transfusion was lower in the OME40q6h group than in those of the OME40q12h group (p = 0.001) and the CIM group (p < 0.001). There were fewer surgical interventions and number of deaths in the OME40q6h group and OME40q12h group as compared with those in the CIM group, but the difference was not statistically significant. The duration of hospital stay was not statistically different among the three groups. No patient had perforation, aspiration pneumonia, or fever within 1 wk following endoscopic therapy in any group. DISCUSSION The use of PPI after obtaining successful endoscopic therapy has been supported in many studies. In a consensus meeting for clinical guidelines, an IV bolus followed by continuous infusion of PPI was recommended in bleeding peptic ulcer patients who had undergone successful endoscopic therapy (16). In a recent meta-analysis, Andriulli et al. found that combination of endotherapy with PPI was beneficial for patients with bleeding peptic ulcers (20). In a meta-analysis of 11 randomized comparative trials, Gisbert et al. found that PPI was more effective than H2RAs in preventing recurrent bleeding and reducing the need for surgery (24). However, there may be several limitations in these studies. For example, the dose and route of PPI administration along with the modality of endoscopic therapy were different among various studies. In this study, we tried to evaluate the role of omeprazole with a unified dose and route following endoscopic injection of epinephrine in bleeding ulcer patients. Patients with major bleeding and endoscopic evidence of an ulcer with active bleeding or a NBVV are at high risk for persistent or recurrent bleeding and should receive endoscopic therapy (2). Our prospective randomized trial was designed to ascertain whether IV large dose of omeprazole therapy after initial endoscopic hemostasis might further reduce the rebleeding rate in such patients. Endoscopic injection with diluted epinephrine is easy to apply and is widely used throughout the world. This is the main reason that we decided to choose epinephrine injection as the therapeutic modality in this study. Unfortunately, the rebleeding rate following epinephrine injection was not negligible. In our previous observation, the rebleeding rates following epinephrine injection were 16 36% (8, 25). In one large meta-analysis series, the rebleeding rate was 18.8% (108/575) (6). After obtaining initial hemostasis, rebleeding is the most important prognostic factor. If the rebleeding rate can be lowered with IV PPI, endoscopic injection with epinephrine will be the most ideal modality for endoscopic therapy. In our previous observations, rebleeding episodes occurred within Table 2. Results of Patients Receiving Endoscopic Treatment OME40q6h (n = 67) OME40q12h (n = 66) CIM (n = 67) p Value Volume of injected epinephrine (ml) 9.64 ( ) 9.83 ( ) 9.30 ( ) 0.67 Volume of blood transfusion after therapy (ml) 710 ( ) 1,241 (487 1,995) 1,317 (947 1,660) <0.01 Number achieving initial hemostasis Number of rebleeding <0.01 Number receiving heater probe Number of surgeries Hospital stay (days) 5.89 ( ) 7.64 ( ) 7.92 ( ) 0.21 Number of deaths For volume of injected epinephrine, blood transfusion, and hospital stay, data are expressed as mean (95% CI). p = between OME40q6h group and OME 40q12h group; p < between OME 40q6h group and CIM group. p < 0.01 between OME40q6h and CIM groups.
5 504 Lin et al. 3 days following endoscopic therapy in most instances (26 28). Therefore, we gave high-dose omeprazole in the first 3 days following endoscopic therapy. In this study, we found that patients receiving omeprazole 40 mg IV infusion every 6 h after successful initial hemostasis had a lower rebleeding rate (6/67 vs 22/67, p < 0.01) and a lower volume of blood transfusion (mean 710 ml vs 1,317 ml, p < 0.001) as compared with patients who received CIM 400 mg every 12 h intravenously. Hsu et al. recently conducted a similar study (29). They enrolled peptic ulcer patients with active bleeding or major signs of recent bleeding. They gave pantoprazole 40 mg IV bolus followed by 40 mg every 12 h for 3 days in one group, and ranitidine 50 mg intravenously every 8 h for 3 days in another group after endoscopic injection of distilled water. The rebleeding rate was lower in the pantoprazole group (2/52 vs 8/50, p = 0.04) when compared with that of the ranitidine group. How about the role of oral PPIs in these patients? Khuroo et al. demonstrated that the recurrent bleeding rate was reduced to 11.8% in patients with visible vessels who received oral omeprazole 40 mg twice daily for 5 days (30). Javid et al. gave oral omeprazole 40 mg every 12 h for 5 days as compared with placebo in patients with high-risk peptic ulcer bleeding after endoscopic injection of epinephrine plus 1% polidocanol (23). They found that oral omeprazole is effective in reducing hospital stay, rebleeding rate, and the need for blood transfusion. Kaviani et al. conducted a similar study which favored oral omeprazole in high-risk patients in reducing the rebleeding rate after endoscopic injection (22). In a meta-analysis, Andriulli et al. also found that oral PPI reduced the rebleeding rate and the need for surgery (20). Unfortunately, there was no data showing intragastric ph in these studies. In our study, we did not give oral PPI to the studied patients because intragastric ph exceeds 4.0 only after frequent high dosages (31, 32). Since rebleeding episodes occur within 24 h in the majority of patients (26), if we gave oral PPI to the patients, the rebleeding may have occurred before high intragastric ph was achieved. An intragastric ph higher than 6.0 is a prerequisite for preventing rebleeding in patients with bleeding peptic ulcers (33). Therefore, a drug that rapidly increases intragastric ph and lasts for 3 4 days is necessary to prevent rebleeding. Under such conditions, IV PPI is the drug of choice. How about the effects of PPI dosage on rebleeding? In a randomized, double-blind study, Udd et al. found that regulardose and high-dose omeprazole are both effective in preventing rebleeding after endoscopic therapy in bleeding peptic ulcer patients (21). However, intragastric ph cannot be elevated within a short period of time with the use of regular dose of PPI. In this way, rebleeding may occur. In addition, they included 38 patients with a low-risk rebleeding rate (Forrest IIc, ulcers with a black base). Such patients with low-risk endoscopic stigmata are not indicated for endoscopic hemostatic therapy (16). In addition, the endoscopic therapies are different among studied cases. Subsequently, there may be some bias in this study. In our study, higher dosage of PPI (160 mg/day) was more beneficial than lower dosage of PPI (80 mg/day) in decreasing the volume of blood transfusion. There was a lower rebleeding tendency for the OMEq6h group as compared with that of the OMEq12h group (6/67 vs 14/66, p = 0.083). It may have clinical significance showing that a bigger dose of PPI is favored in high-risk patients. There may be one limitation in this study. Endoscopic therapy with epinephrine injection may be suboptimal. In our previous study, we used HPT or multipolar electrocoagulation to treat the patients and obtained a lower rebleeding rate (18). Under this situation, a smaller sample size may be enough to show statistically significant difference. CONCLUSION Large dose of IV PPI reduces the rebleeding rate in high-risk patients with bleeding peptic ulcers who have obtained initial hemostasis with epinephrine injection. ACKNOWLEDGMENT We are indebted to Ms. Betty Tzu-en Lin and Alex Jen-hao Lin for assistance of this study. STUDY HIGHLIGHTS What is Current Knowledge Endoscopic injection of epinephrine is a standard hemostatic modality for bleeding peptic ulcer. The optimal dose of proton pump inhibitor to prescribe post hemostatic therapy is unclear. What is New Here A randomized controlled trial tested whether an infusion of emeprazole (40mg 6 or 12 hourly) or cimetidine (400mg 12 hourly) prevented rebleeding in high risk patients (active bleeding or non-bleeding visible vessels successfully treated with epinephrine injection endoscopically). Rebleeding occurred in 22/67 on cimetidine compared with 14/66 on omeprazole 40mg 12 hourly and 6/67 on omeprazole 40mg 6 hourly. After initial hemostasis, high dose intravenous proton pump inhibitor therapy is superior to intravenous H2 receptor antagonist therapy. Reprint requests and correspondence: Hwai-Jeng Lin, M.D., F.A.C.G., Division of Gastroenterology, Department of Medicine, VGH-TAIPEI, Shih-Pai Rd, Sec 2, Taipei 11217, Taiwan. Received July 15, 2005; accepted September 28, 2005.
6 Omeprazole in Patients with Ulcer Bleeding 505 REFERENCES 1. Cook DJ, Guyatt GH, Salena BJ, et al. Endoscopic therapy for acute nonvariceal upper gastrointestinal hemorrhage: A meta-analysis. Gastroenterology 1992;102: Consensus Development Panel. Consensus statement on the therapeutic endoscopy and bleeding ulcers. Gastrointest Endosc 1990;36:S Villanueva C, Balanzó J, Terras X, et al. Value of secondlook endoscopy after injection therapy for bleeding peptic ulcer: A prospective and randomized trial. Gastrointest Endosc 1994;40: British Society of Gastroenterology Endoscopy Committee. Non-variceal upper gastrointestinal hemorrhage: Guidelines. Gut 2002;51(suppl 4):iv Feu F, Brullet E, Calvet X, et al. Guidelines for the diagnosis and treatment of acute non-variceal upper gastrointestinal bleeding. J Gastroenterol Hepatol 2003;26: Calvet X, Vergara M, Brullet E, et al. Addition of a second endoscopic treatment following epinephrine injection improves outcome in high-risk bleeding ulcers. Gastroenterology 2004;126: Chung SCS, Leong HT, Chan ACW, et al. Epinephrine or epinephrine plus alcohol for injection of bleeding ulcers: A prospective randomized trial. Gastrointest Endosc 1996;43: Lin HJ, Perng CL, Lee SD. Is sclerosant injection mandatory after epinephrine injection for arrest of peptic ulcer haemorrhage? A prospective randomized comparative study. Gut 1993;34: Cederberg C, Thompson ABR, Kirdeikis P, et al. Effect of continuous intravenous infusion of omeprazole on 24-hour intragastric ph in fasting DU patients: Comparison to repeated bolus doses of omeprazole or ranitidine. Gastroenterology 1992;102(suppl):A Reynolds JR, Walt RP, Clark AG, et al. Intragastric ph monitoring in acute upper gastrointestinal bleeding and the effect of intravenous cimetidine and ranitidine. Aliment Pharmacol Ther 1987;1: Peterson WL, Barnett C, Feldman M, et al. Reduction of twenty-four-hour gastric acidity with combination drugs therapy in patients with duodenal ulcer. Gastroenterology 1979;77: Merki HS, Witzel L, Kaufman D, et al. Continuous intravenous infusion of famotidine maintain high intragastric ph in duodenal ulcer. Gut 1988;29: Brunner G, Luna P, Thiesemann C. Drugs for ph control in upper gastrointestinal bleeding. Aliment Pharmacol Ther 1995;9(suppl 1): Brnner GHG, Thiesemann C. The potential clinical role of intravenous omeprazole. Digestion 1992;51(suppl 1): Walt RP, Reynolds JR, Langman MJS, et al. Intravenous omeprazole rapidly raises intragastric ph. Gut 1985;26: Barkun A, Bardou M, Marshall JK, et al. Consensus recommendations for managing patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med 2003;139: Lau JY, Sung JJ, Lee KK, et al. Effect of intravenous omeprazole on recurrent bleeding after endoscopic treatment of bleeding peptic ulcers. N Engl J Med 2000;343: Lin HJ, Lo WC, Lee FY, et al. A prospective randomized comparative trial showing that omeprazole prevents rebleeding in patients with bleeding peptic ulcer after successful endoscopic therapy. Arch Int Med 1998;158: Leontiadis GI, Sharma VK, Howden CW. Systemic review and meta-analysis of proton pump inhibitor therapy in peptic ulcer bleeding. BMJ 2005;300: Andriulli A, Annese V, Caruso N, et al. Proton-pump inhibitors and outcome of endoscopic hemostasis in bleeding peptic ulcer: A series of meta-analysis. Am J Gastroenterol 2005;100: Udd M, Miettinen P, Palmu A, et al. Regular-dose versus high-dose omeprazole in peptic ulcer bleeding. Scand J Gastroenterol 2001;36: Kaviani MJ, Hashemi MR, Kazemifar AR, et al. Effect of oral omeprazole in reducing re-bleeding in bleeding peptic ulcers: A prospective, double-blind, randomized, clinical trial. Aliment Pharmacol Ther 2003;17: Javid G, Masoodi I, Zargar SA, et al. Omeprazole as adjuvant therapy to endoscopic combination injection sclerotherapy for treating bleeding peptic ulcer. Am J Med 2001;111: Gisbert JP, Gonzalez X, Calvet M, et al. Proton pump inhibitors versus H2-antagonists: A meta-analysis of the efficacy in treating bleeding peptic ulcer. Aliment Pharmacol Ther 2001;15: Lin HJ, Hsieh YH, Tseng GY, et al. A prospective, randomized trial of large- versus small-volume endoscopic injection of epinephrine for peptic ulcer bleeding. Gastrointest Endosc 2002;55: Lin HJ, Perng CL, Lee YL, et al. Clinical courses and predictors for rebleeding in patients with peptic ulcers and non-bleeding visible vessels: A prospective study. Gut 1994;35: Lin HJ, Perng CL, Wang K, et al. Long-term results of heater probe thermocoagulation for patients with massive peptic ulcer bleeding: A prospective observation. Am J Gastroenterol 1995;90: Lin HJ, Wang K, Perng CL, et al. Natural history of bleeding peptic ulcer with a tightly adherent blood clot: A prospective observation. Gastrointest Endosc 1996;43: Hsu PI, Lo GH, Lo CC, et al. Intravenous pantoprazole versus ranitidine for prevention of rebleeding after endoscopic hemostasis of bleeding peptic ulcers. World J Gastroenterol 2004;10: Khuroo MS, Yattoo GN, Javid G, et al. A comparison of omeprazole and placebo for bleeding peptic ulcer. N Engl J Med 1997;336: Cederberg C, Thomson A, Mahachai V, et al. Effect of intravenous and oral omeprazole on 24 hour intragastric acidity in duodenal ulcer patients. Gastroenterology 1992;103: Merki HS, Wilder-Smith CH. Do continuous infusions of omeprazole and ranitidine retain their effect with prolonged dosing? Gastroenterology 1994;106: Collins R, Langman M. Treatment with histamine H2 antagonists in acute upper gastrointestinal hemorrhage. Implications of randomized trials. N Engl J Med 1985;313:660 6.
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD
 Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Optimal injection volume of epinephrine for endoscopic treatment of peptic ulcer bleeding
 PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 May 21; 12(19): 3108-3113 World Journal of Gastroenterology ISSN 1007-9327 [email protected] 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION
PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 May 21; 12(19): 3108-3113 World Journal of Gastroenterology ISSN 1007-9327 [email protected] 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial
 Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
A. Ketorolac*** B. Naproxen C. Ibuprofen D. Celecoxib
 1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
SIGN. Management of acute upper and lower gastrointestinal bleeding. September 2008. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
Management and Prevention of Upper GI Bleeding
 Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
Management and Prevention of Upper GI Bleeding By Jiwon Kim, Pharm.D., BCPS, FCSHP Reviewed by Clarence Chant, Pharm.D., FCSHP, FCCP, BCPS; and Steven E. Pass, Pharm.D., FCCP, FCCM, BCPS Learning Objectives
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
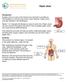 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding
 Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Gastrointestinal bleeding: the management of acute upper gastrointestinal bleeding NICE guideline Draft for consultation, December 2011 If you wish to comment on this version of the guideline, please be
Gruppo di lavoro: Malattie Tromboemboliche
 Gruppo di lavoro: Malattie Tromboemboliche 2381 Soluble Recombinant Thrombomodulin Ameliorates Hematological Malignancy-Induced Disseminated Intravascular Coagulation More Promptly Than Conventional Anticoagulant
Gruppo di lavoro: Malattie Tromboemboliche 2381 Soluble Recombinant Thrombomodulin Ameliorates Hematological Malignancy-Induced Disseminated Intravascular Coagulation More Promptly Than Conventional Anticoagulant
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
understanding GI bleeding
 understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
understanding GI bleeding a consumer education brochure American College of Gastroenterology 4900B South 31st Street, Arlington, VA 22206 703-820-7400 www.acg.gi.org American College of Gastroenterology
STROKE PREVENTION IN ATRIAL FIBRILLATION. TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: ABBREVIATIONS: BACKGROUND:
 STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE)
 Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders. By: Jalal Hejazi PhD, MSc.
 Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol)
 NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol) Date of First Issue 10/05/2010 Approved 16/06/2010 Current Issue Date 18/11/2015
NHS FORTH VALLEY Guidelines for use of high dose Intravenous Esomeprazole in Adults (Previously called the Hong Kong Protocol) Date of First Issue 10/05/2010 Approved 16/06/2010 Current Issue Date 18/11/2015
Dual Antiplatelet Therapy. Stephen Monroe, MD FACC Chattanooga Heart Institute
 Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Dual Antiplatelet Therapy Stephen Monroe, MD FACC Chattanooga Heart Institute Scope of Talk Identify the antiplatelet drugs and their mechanisms of action Review dual antiplatelet therapy in: The medical
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013
 Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013 Family physician with Rivergrove Medical Clinic Practice in the north end since 1985 Medical Director of the Wellness
Kevin Saunders MD CCFP Rivergrove Medical Clinic Wellness Institute @ SOGH April 17 2013 Family physician with Rivergrove Medical Clinic Practice in the north end since 1985 Medical Director of the Wellness
Novel Anticoagulation Agents DISCLOSURES. Objectives ATRIAL FIBRILLATION TRIALS. NOAC Comparison 6/12/2015
 Novel Anticoagulation Agents DISCLOSURES James W. Haynes, MD Department of Family Medicine Univ of TN Health Science Center (Chattanooga) Objectives Understand mechanism of action behind the NOAC agents
Novel Anticoagulation Agents DISCLOSURES James W. Haynes, MD Department of Family Medicine Univ of TN Health Science Center (Chattanooga) Objectives Understand mechanism of action behind the NOAC agents
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
New Anticoagulants: What to Use What to Avoid
 New Anticoagulants: What to Use What to Avoid Bruce Davidson, MD, MPH Clinical Professor of Medicine Pulmonary and Critical Care Medicine Division University of Washington School of Medicine Seattle USA
New Anticoagulants: What to Use What to Avoid Bruce Davidson, MD, MPH Clinical Professor of Medicine Pulmonary and Critical Care Medicine Division University of Washington School of Medicine Seattle USA
Articles Presented. Journal Presentation. Dr Albert Lo. Dr Albert Lo
 * This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
* This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
Venous Thromboembolism: Long Term Anticoagulation. Dan Johnson, Pharm.D.
 Venous Thromboembolism: Long Term Anticoagulation Dan Johnson, Pharm.D. Disclosures No financial relationships with products discussed Off-label use of drug therapy always discussed Objectives Review clinical
Venous Thromboembolism: Long Term Anticoagulation Dan Johnson, Pharm.D. Disclosures No financial relationships with products discussed Off-label use of drug therapy always discussed Objectives Review clinical
Digestive System (continued) Digestive System. Stomach. Peptic Ulcer Disease
 Digestive System Digestive System (continued) Responsible for breaking down food, absorbing nutrients, eliminating wastes Alimentary canal Also known as gastrointestinal tract Reaches from mouth to anus
Digestive System Digestive System (continued) Responsible for breaking down food, absorbing nutrients, eliminating wastes Alimentary canal Also known as gastrointestinal tract Reaches from mouth to anus
DVT/PE Management with Rivaroxaban (Xarelto)
 DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
New Oral Anticoagulants
 New Oral Anticoagulants Tracy Minichiello, MD Associate Professor of Medicine Chief, San FranciscoVA Anticoagulation and Thrombosis Service Ansell, J. Hematology Copyright 2010 American Society of Hematology.
New Oral Anticoagulants Tracy Minichiello, MD Associate Professor of Medicine Chief, San FranciscoVA Anticoagulation and Thrombosis Service Ansell, J. Hematology Copyright 2010 American Society of Hematology.
PACKAGE LEAFLET: INFORMATION FOR THE USER Omeprazol XXX 40 mg powder for solution for infusion omeprazole
 PACKAGE LEAFLET: INFORMATION FOR THE USER Omeprazol XXX 40 mg powder for solution for infusion omeprazole Read all of this leaflet carefully before you start using this medicine. - Keep this leaflet. You
PACKAGE LEAFLET: INFORMATION FOR THE USER Omeprazol XXX 40 mg powder for solution for infusion omeprazole Read all of this leaflet carefully before you start using this medicine. - Keep this leaflet. You
Management of the new antiplatelets and anticoagulants
 Management of the new antiplatelets and anticoagulants Session No.: 1 Name: C. Boustiere, T Ponchon Guidelines : Anti-thrombotic agents and digestive endoscopy 2006 : French guideline (SFED) 2007 : Japanese
Management of the new antiplatelets and anticoagulants Session No.: 1 Name: C. Boustiere, T Ponchon Guidelines : Anti-thrombotic agents and digestive endoscopy 2006 : French guideline (SFED) 2007 : Japanese
Inpatient Anticoagulation Safety. To provide safe and effective anticoagulation therapy through a collaborative approach.
 Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
What can I eat? Peptic ulcers. What are peptic ulcers? What tests are needed? Will the ulcer come back? What causes a peptic ulcer?
 In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
NSAIDs and Peptic Ulcers
 NSAIDs and Peptic Ulcers National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is a peptic ulcer? A peptic ulcer is a sore
NSAIDs and Peptic Ulcers National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is a peptic ulcer? A peptic ulcer is a sore
ABOUT XARELTO CLINICAL STUDIES
 ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
TEST QUESTIONS GASTROINTESTINAL BLEEDING
 TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
Treatments for Barrett s Oesophagus
 Treatments for Barrett s Oesophagus Introduction This leaflet describes the various ways in which Barrett s Oesophagus is treated. It has been produced in association with Heartburn Cancer UK (HCUK), a
Treatments for Barrett s Oesophagus Introduction This leaflet describes the various ways in which Barrett s Oesophagus is treated. It has been produced in association with Heartburn Cancer UK (HCUK), a
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting
 Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
Disclosure. New Agents for Treatment of DVT. Prevalence of DVT VTE. Normal Hemostasis 7/17/2015. Mark Oliver, MD, RVT, RPVI,FSVU
 New Agents for Treatment of DVT Disclosure PI Adopt and Amplify trials Mark Oliver, MD, RVT, RPVI,FSVU BMS and Pfizer Speaker VTE Venous Thromboembolism Recognized DVT s New : 170,000 Recurrent : 90,000
New Agents for Treatment of DVT Disclosure PI Adopt and Amplify trials Mark Oliver, MD, RVT, RPVI,FSVU BMS and Pfizer Speaker VTE Venous Thromboembolism Recognized DVT s New : 170,000 Recurrent : 90,000
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department!
 Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
New Anticoagulants: When and Why Should I Use Them? Disclosures
 Winship Cancer Institute of Emory University New Anticoagulants: When and Why Should I Use Them? Christine L. Kempton, MD, MSc Associate Professor of Pediatrics and Hematology and Medical Oncology Hemophilia
Winship Cancer Institute of Emory University New Anticoagulants: When and Why Should I Use Them? Christine L. Kempton, MD, MSc Associate Professor of Pediatrics and Hematology and Medical Oncology Hemophilia
Guideline Statement for the Treatment of Disseminated Intravascular Coagulation
 Guideline Statement for the Treatment of Disseminated Intravascular Coagulation Introduction Though a rare occurrence in the perioperative setting, disseminated intravascular coagulation (DIC) is a syndrome
Guideline Statement for the Treatment of Disseminated Intravascular Coagulation Introduction Though a rare occurrence in the perioperative setting, disseminated intravascular coagulation (DIC) is a syndrome
DUAL ANTIPLATELET THERAPY. Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania
 DUAL ANTIPLATELET THERAPY Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania DUAL ANTIPLATELET THERAPY (DAPT) Dual antiplatelet regimen
DUAL ANTIPLATELET THERAPY Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania DUAL ANTIPLATELET THERAPY (DAPT) Dual antiplatelet regimen
New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis
 New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis Holster IL, Valkhoff VE, Kuipers EJ, Tjwa ET Departments of Gastroenterology and Hepatology,
New Oral Anticoagulants Increase Risk for Gastrointestinal Bleeding - A Systematic Review and Meta-Analysis Holster IL, Valkhoff VE, Kuipers EJ, Tjwa ET Departments of Gastroenterology and Hepatology,
A study to Evaluate PPI s effect on vitamin D levels. Rani Hanna M.D., M.S. PGY-3 Joseph Grisanti, MD
 A study to Evaluate PPI s effect on vitamin D levels Rani Hanna M.D., M.S. PGY-3 Joseph Grisanti, MD The sunshine vitamin Existed over 500 million years. Prehormone, not only a vitamin. Two major sources:
A study to Evaluate PPI s effect on vitamin D levels Rani Hanna M.D., M.S. PGY-3 Joseph Grisanti, MD The sunshine vitamin Existed over 500 million years. Prehormone, not only a vitamin. Two major sources:
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Inhibit terminal acid secretion from parietal cells by blocking H + /K + - ATPase pump
 Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
CDEC FINAL RECOMMENDATION
 CDEC FINAL RECOMMENDATION RIVAROXABAN (Xarelto Bayer Inc.) New Indication: Pulmonary Embolism Note: The Canadian Drug Expert Committee (CDEC) previously reviewed rivaroxaban for the treatment of deep vein
CDEC FINAL RECOMMENDATION RIVAROXABAN (Xarelto Bayer Inc.) New Indication: Pulmonary Embolism Note: The Canadian Drug Expert Committee (CDEC) previously reviewed rivaroxaban for the treatment of deep vein
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl
 NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
NnEeWw DdEeVvEeLlOoPpMmEeNnTtSs IiıNn OoRrAaLl AaNnTtIiıCcOoAaGgUuLlAaTtIiıOoNn AaNnDd RrEeVvEeRrSsAaLl Mikele Wissing, RN June 2014 Introduction until recently, was the unrivaled medication for treatment
Medication Management Improvement System Protocol #4 Potentially Inappropriate Use of NSAIDs
 Medication Management Improvement System Protocol #4 Potentially Inappropriate Use of NSAIDs Problem: Use of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) in clients with any one of the following risk
Medication Management Improvement System Protocol #4 Potentially Inappropriate Use of NSAIDs Problem: Use of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) in clients with any one of the following risk
POAC CLINICAL GUIDELINE
 POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
CLINICAL PRACTICE GUIDELINES
 CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
CLINICAL PRACTICE GUIDELINES April 2003 MOH/P/PAK/ (GU) MANAGEMENT OF NON-VARICEAL UPPER GASTROINTESTINAL BLEEDING MINISTRY OF HEALTH MALAYSIAN SOCIETY ACADEMY OF MEDICINE, MALAYSIA OF MALAYS IA GASTROENTEROLOGY
American College of Gastroenterology Guideline on the Management of Helicobacter pylori Infection
 American Journal of Gastroenterology ISSN 0002-9270 C 2007 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2007.01393.x Published by Blackwell Publishing American College of Gastroenterology
American Journal of Gastroenterology ISSN 0002-9270 C 2007 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2007.01393.x Published by Blackwell Publishing American College of Gastroenterology
The Role of the Newer Anticoagulants
 The Role of the Newer Anticoagulants WARFARIN = Coumadin DAGIBATRAN = Pradaxa RIVAROXABAN = Xarelto APIXABAN = Eliquis INDICATION DABIGATRAN (Pradaxa) RIVAROXABAN (Xarelto) APIXABAN (Eliquis) Stroke prevention
The Role of the Newer Anticoagulants WARFARIN = Coumadin DAGIBATRAN = Pradaxa RIVAROXABAN = Xarelto APIXABAN = Eliquis INDICATION DABIGATRAN (Pradaxa) RIVAROXABAN (Xarelto) APIXABAN (Eliquis) Stroke prevention
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas
 Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Duration of Dual Antiplatelet Therapy After Coronary Stenting
 Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
HemoClip: Guidelines & Atlas
 HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
Association between Proton Pump Inhibitors and Clostridium difficile
 Association between Proton Pump Inhibitors and Clostridium difficile Lauren Petrik and Nicholas Hellebusch, Pharm.D. Candidates 2013, Tatum Mead, Pharm.D. UMKC School of Pharmacy Clostridium difficile,
Association between Proton Pump Inhibitors and Clostridium difficile Lauren Petrik and Nicholas Hellebusch, Pharm.D. Candidates 2013, Tatum Mead, Pharm.D. UMKC School of Pharmacy Clostridium difficile,
Paul G. Lee. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume III, 1998-1999. A. Objective
 A comparison of six months of anticoagulation with extended anticoagulation for a first episode of venous thromboembolism in patients with thrombophilia Paul G. Lee A. Objective a. To evaluate the risk
A comparison of six months of anticoagulation with extended anticoagulation for a first episode of venous thromboembolism in patients with thrombophilia Paul G. Lee A. Objective a. To evaluate the risk
The author has no disclosures
 Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 [email protected] This presentation will discuss unlabeled and investigational use of products The author
Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 [email protected] This presentation will discuss unlabeled and investigational use of products The author
New anticoagulants: Monitoring or not Monitoring? Not Monitoring
 The 2 nd World Congress on CONTROVERSIES IN HEMATOLOGY (COHEM) Barcelona, Spain September 6 8, 2012 New anticoagulants: Monitoring or not Monitoring? Not Monitoring Anna Falanga, MD Immunohematology and
The 2 nd World Congress on CONTROVERSIES IN HEMATOLOGY (COHEM) Barcelona, Spain September 6 8, 2012 New anticoagulants: Monitoring or not Monitoring? Not Monitoring Anna Falanga, MD Immunohematology and
Thrombosis and Hemostasis
 Thrombosis and Hemostasis Wendy Lim, MD, MSc, FRCPC Associate Professor, Department of Medicine McMaster University, Hamilton, ON Overview To review the important developments in venous thromboembolism
Thrombosis and Hemostasis Wendy Lim, MD, MSc, FRCPC Associate Professor, Department of Medicine McMaster University, Hamilton, ON Overview To review the important developments in venous thromboembolism
UW MEDICINE PATIENT EDUCATION. Xofigo Therapy. For metastatic prostate cancer. What is Xofigo? How does it work?
 UW MEDICINE PATIENT EDUCATION Xofigo Therapy For metastatic prostate cancer This handout explains how the drug Xofigo is used to treat metastatic prostate cancer. What is Xofigo? Xofigo is a radioactive
UW MEDICINE PATIENT EDUCATION Xofigo Therapy For metastatic prostate cancer This handout explains how the drug Xofigo is used to treat metastatic prostate cancer. What is Xofigo? Xofigo is a radioactive
UGI Tract Hemorrhage. GI Tract Emergencies. UGI Hemorrhage. David D. Markowitz, MD. UGI tract hemorrhage Comorbid disease
 UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D.
 Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Enoxaparin for long term anticoagulation in patients unsuitable for oral anticoagulants
 Enoxaparin for long term anticoagulation in patients unsuitable for oral anticoagulants Traffic light classification- Amber 2 Information sheet for Primary Care Prescribers Relevant Licensed Indications
Enoxaparin for long term anticoagulation in patients unsuitable for oral anticoagulants Traffic light classification- Amber 2 Information sheet for Primary Care Prescribers Relevant Licensed Indications
Learning Luncheon 7: Endoscopic Mucosal Resection: When, Where and How?
 Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Optimal Management of Splenic/Portal Vein Thrombosis. David Mauchley University of Colorado
 Optimal Management of Splenic/Portal Vein Thrombosis David Mauchley University of Colorado Overview Portal Vein Thrombosis (PVT) Etiology Presentation/Clinical Aspects Diagnosis Management Cirrhotic vs.
Optimal Management of Splenic/Portal Vein Thrombosis David Mauchley University of Colorado Overview Portal Vein Thrombosis (PVT) Etiology Presentation/Clinical Aspects Diagnosis Management Cirrhotic vs.
Research funding was provided by TAP Pharmaceutical Products, Inc.
 DOES THE DOSING FREQUENCY OF PROTON PUMP INHIBITORS (PPIs) AFFECT SUBSEQUENT RESOURCE UTILIZATION AND COSTS AMONG PATIENTS DIAGNOSED WITH GASTROESOPHAGEAL REFLUX DISEASE (GERD)? Boulanger L 1, Mody R 2,
DOES THE DOSING FREQUENCY OF PROTON PUMP INHIBITORS (PPIs) AFFECT SUBSEQUENT RESOURCE UTILIZATION AND COSTS AMONG PATIENTS DIAGNOSED WITH GASTROESOPHAGEAL REFLUX DISEASE (GERD)? Boulanger L 1, Mody R 2,
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
HERTFORDSHIRE MEDICINES MANAGEMENT COMMITTEE (HMMC) RIVAROXABAN RECOMMENDED see specific recommendations for licensed indications below
 Name: generic (trade) Rivaroxaban (Xarelto ) HERTFORDSHIRE MEDICINES MANAGEMENT COMMITTEE (HMMC) RIVAROXABAN RECOMMENDED see specific recommendations for licensed indications below What it is Indications
Name: generic (trade) Rivaroxaban (Xarelto ) HERTFORDSHIRE MEDICINES MANAGEMENT COMMITTEE (HMMC) RIVAROXABAN RECOMMENDED see specific recommendations for licensed indications below What it is Indications
Thrombosis and Bleeding
 Many questions, few answers Thrombosis and Bleeding Pierre Noel MD Mayo Arizona Scope of the Problem Thrombosis PV 12-39% ET 11-25% MF 10% 60-70% of thrombosis are arterial Splanchnic and cerebral thrombosis
Many questions, few answers Thrombosis and Bleeding Pierre Noel MD Mayo Arizona Scope of the Problem Thrombosis PV 12-39% ET 11-25% MF 10% 60-70% of thrombosis are arterial Splanchnic and cerebral thrombosis
Analyzing Clinical Trial Findings of the Efficacy and Safety Profiles of Novel Anticoagulants for Stroke Prevention in Atrial Fibrillation
 Analyzing Clinical Trial Findings of the Efficacy and Safety Profiles of Novel Anticoagulants for Stroke Prevention in Atrial Fibrillation Drew Baldwin, MD Virginia Mason Seattle, Washington NCVH May 29,
Analyzing Clinical Trial Findings of the Efficacy and Safety Profiles of Novel Anticoagulants for Stroke Prevention in Atrial Fibrillation Drew Baldwin, MD Virginia Mason Seattle, Washington NCVH May 29,
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
Upper Endoscopy (EGD)
 Upper Endoscopy (EGD) Appointment Information: Patient Name: MRN: Physician Name: Location: _ For information on Directions, please visit: http://www.brighamandwomens.org/general/directions/directions.aspx
Upper Endoscopy (EGD) Appointment Information: Patient Name: MRN: Physician Name: Location: _ For information on Directions, please visit: http://www.brighamandwomens.org/general/directions/directions.aspx
