EIN (Endometrial Intraepithelial Neoplasia) and Ambiguous Premalignant Endometrial Lesions
|
|
|
- Lee Wiggins
- 9 years ago
- Views:
Transcription
1 EIN (Endometrial Intraepithelial Neoplasia) and Ambiguous Premalignant Endometrial Lesions ASCP Course 1341 Saturday, October 31, 2009 Chicago, IL Course Director:George L. Mutter, MD Associate Professor of Pathology, Harvard Medical School Div. of Women's and Perinatal Pathology, Department of Pathology Brigham and Women's Hospital, 75 Francis Street, Boston, MA (617) Phone (617) FAX website: Page 1
2 Index: Page Course Description 3 Schedule 4 Introduction 4 The Benign Endometrial Hyperplasia Sequence 6 Endometrial Intraepithelial Neoplasia 12 Pitfalls of EIN Diagnosis: A Practical Approach 20 Endometrial Metaplasias and Ambiguous Lesions 23 References 32 Case Presentations 35 Page 2
3 Course Description: This 3-hour course will review diagnosis of neoplastic and metaplastic lesions of the endometrium, with special emphasis on revised criteria for recognition of precancers. A rationale for functional segregation into precancerous (EIN, Endometrial Intraepithelial Neoplasia) and non-precancerous categories will be presented, based upon data from genetic, morphometric, and clinical outcome studies. A mini symposium format will integrate didactic presentation with discussion of representative patient examples in topical sessions. Clinical material will be organized to illustrate the broad variety of presentations of specific categories of disease, and be accompanied by discussions of their resulting clinical management. This course is relevant to any pathologist engaged in the interpretation of endometrial biopsies (trainees and established pathologists). Major objectives and Topics Covered: This course is designed to review criteria for diagnosis of neoplastic and metaplastic lesions of the endometrium, with special emphasis on revised criteria for recognition of precancers. A rationale for functional segregation into precancerous (EIN, Endometrial Intraepithelial Neoplasia) and non-precancerous categories will be presented, based upon new data from genetic, morphometric, and clinical outcome studies. Special attention will be paid to resolution of heterogenous categories of endometria formerly classified as "hyperplastic" and metaplastic. Accurate diagnosis requires judicious handling of mimics and of potentially confounding factors (sampling errors, artifacts, and superimposed hormonal effects), which will be covered in detail. The genetic basis and morphologic presentation of independent tumorigenetic pathways for endometrioid vs. papillary serous carcinomas will be presented. At the end of the course participants should be able to: -Discuss and apply EIN criteria for diagnosis of endometrial precancers -Develop a diagnostic strategy for endometrial lesions with non-endometrioid differentiation ( metaplasias ) -Integrate pathophysiologic concepts into diagnostic and therapeutic practice -Recognize sampling and interpretive limitations in diagnosis of endometrial disease Page 3
4 Schedule Saturday, Oct 31, pm 1:00pm Introduction Title: The Benign Endometrial Hyperplasia Sequence of Estrogen Effects Title: Diagnosis of endometrial Precancers: EIN :45 pm Coffee break Title: Pitfalls of EIN Diagnosis Title: Endometrial Metaplasias and Ambiguous Lesions Title: Review and Discussion of Cases Questions and Concluding Remarks Page 4
5 INTRODUCTION The diagnostic strategies outlined here are based upon an integrated picture of endometrial carcinogenesis from diffuse hormonal changes (benign hyperplasia sequence) to the earliest recognizable premalignant cells (Endometrial Intraepithelial Neoplasia, EIN) 1. In the past, both generalized hormonal responses and localized premalignant lesions were lumped under the term endometrial hyperplasia, with various modifiers such as adenomatous, mild, moderate, and severe, and atypical that had no uniform meaning. The WHO 1994 classification system subdivided hyperplasias by architectural complexity and cytologic atypia 2. Although this practice has been widespread, and has had a benefit of unifying terminology, it fails to optimally stratify patients according to those pathologic mechanisms and cancer risks necessary for appropriate therapeutic triaging. Diagnoses are poorly reproducible 3. Recent molecular studies have provided evidence that the use of the term hyperplasia is conceptually correct for some but not all of these lesions. For these reason, we have chosen to present a practically oriented disease classification in which the hormonal effects of unopposed estrogens (benign hyperplasia) and emergent neoplastic precancerous lesions (endometrial intraepithelial neoplasia (EIN)) are separately diagnosed using non-overlapping terminology and discrete criteria 4. Table I: Endometrial Diagnostic Schema and ICD9 Codes Functional Nomenclature Topography Category Benign Endometrial Hyperplasia EIN, Endometrial Intraepithelial Neoplasia Endometrial adenocarcinoma, endometrioid type, well differentiated Diffuse Focal progressing to diffuse Focal progressing to diffuse Prolonged Estrogen Effect Precancerous Malignant Treatment Hormonal therapy, Symptomatic Hormonal or surgical Surgical stage-based ICD9 Code Page 5
6 Part I: The Disordered Proliferative And Benign Endometrial Hyperplasia Sequence Benign endometrial hyperplasias 5 do not have a singular histopathologic appearance, but rather demonstrate sequential changes occurring in a combination and severity that reflects the quantity and duration of unopposed estrogen exposure 6. Characteristic histologic features include irregular remodeling of glands, variably accompanied by vascular thrombi, stromal breakdown and randomly scattered cytologic changes. Some estrogen induced changes persist, with modification, even after the estrogen level declines or is quenched by addition of progestins. This aggregate group of benign endometrial hyperplasias can thus be envisioned as a temporal sequence of estrogen-induced changes in which the appearance at any single time point is codetermined by the trajectory of prior morphologic changes and the current hormonal environment. Prolonged estrogen exposure unmitigated by opposing progestins confers a modest 2-10 fold increased endometrial cancer risk 7-9. Those benign endometrial hyperplasias that develop histologically discontinuous EIN lesions are associated with dramatically increased cancer risk. The challenge to the pathologist is to divide the diverse histologic presentations of benign endometrial hyperplasia into functionally defined subgroups, while maintaining a sharp diagnostic boundary with premalignant EIN lesions. Pathophysiology Benign endometrial hyperplasia is encountered most frequently around the time of the menopause, when the normal cycle of sequentially regulated estrogen and progesterone is perturbed in tempo and amount. It can also occur, however, in young women and teenagers, in whom anovulatory cycles are also the norm. The primary pathology in all these cases is a systemic excess of estrogens, albeit one in which the endometrium is secondarily altered and a frequent source of symptomatic bleeding. The pathognomonic feature of persistent estrogen stimulation is architectural changes of individual glands distributed randomly throughout the entire hormonally responsive region of the endometrium (superficial functionalis). Prolonged proliferation as a result of unopposed estrogens first gives rise to disordered proliferative endometrium, and over time an increasingly irregular distribution of individually variable endometrial glands which are known as benign hyperplasia. Disordered proliferative endometrium and the earliest phases of benign hyperplasia of the endometrium thus share a common pathogenesis, and present a continuous spectrum of overlapping histopathologic features (Table II) rather than sharply different appearances. Precise discrimination is somewhat arbitrary. In a woman of childbearing age, there is characteristically prolonged or excessive bleeding at intervals that are initially longer than normal. Microinfarcts and estrogen withdrawal are responsible for symptomatic bleeding 10;11. Both mechanisms may be effective at different times in patients with benign hyperplasia. Patchy stromal breakdown secondary to estrogen-induced microthrombi can produce intermittent spotting. A relative reduction in the prolonged estrogen stimulation causes apoptosis of the endometrial glands and stroma of the hypertrophied functionalis 11, and resultant heavy shedding. Occasionally, decline in estrogen levels is sufficiently gradual that generalized apoptosis and shedding fail to take place. Superimposition of progesterone upon a benign endometrial hyperplasia occurs in women with delayed ovulation, sporadic corpus luteum development in the perimenopausal years, or therapeutic administration of progestins following an extended follicular phase. Down-regulation of estrogen receptors by progestins leads to a dominant progestational effect, regardless of the presence or absence of continued estrogen production. In this environment menstrual shedding is Page 6
7 delayed, as progestins have the capacity to directly support the endometrium. Progesterone related stromal and secretory glandular changes develop within the setting of irregular glands previously developed under the influence of estrogens. Thus, the histologic appearance at diagnosis may be heavily modified by intermittent or accompanying progestins although the causal event in benign hyperplasia is unopposed estrogen. Table II: Histological Features of Benign endometrial hyperplasia (not all are present in every case) Feature mitotic activity scattered cysts tubal metaplasia variable gland density bulky specimen fibrin thrombi microinfarcts with epithelial change low or absent mitoses secretory change stromal predecidualization global breakdown Comment similar to normal Disordered Proliferativ e Benign Hyperplasia active phase proliferation + + within functionalis, exhausted phase Benign Hyperplasia with superimposed progestin effect random placement randomly involves scattered tubular or cystic glands. +/- cilia regularly irregular secondary to gland proliferation and remodeling reflects prolonged proliferative activity often separate or Shedding following Benign Hyperplasia displaced randomly placed, multifocal, with intervening intact reflects decline in estrogen variable extent depending on exposure + + may be patchy or lacking, depending on progestin exposure architectural clues obscured, cytology degenerative Page 7
8 Figure 1: Progressive Effects of Unopposed Estrogens. Early effects of unopposed estrogen are scattered cysts in an otherwise normal appearing proliferative endometrium, known as disordered proliferative endometrium. Continued exposure causes a progressive spectrum of histopathologic change (left to right) including increasing irregularity of gland density and shape, scattered alterations of cytologic appearance known as benign hyperplasia. Established benign hyperplasias demonstrate a high degree of remodeling between glands and stroma of the expanded, hyperplastic, endometrial compartment, in which the ratio of glands to stroma exceeds 1.0 in most or all of the endometrial compartment. Fibrin thrombi, stromal breakdown and associated reactive epithelial changes commonly develop, and must be carefully distinguished from neoplastic processes. Diagnostic Features Abundant curettings with characteristically diffuse and widespread morphologic features typify endometria altered by unopposed estrogens. The histologic changes of disordered proliferative and benign endometrial hyperplasia are conceptually and morphologically well represented as a unified disease spectrum, separate and discontinuous from EIN. The histologic hallmark of the benign hyperplasias is a generalized but non-uniform proliferation of architecturally variably shaped glands that equal or exceed the quantity of the stroma. Disordered proliferative endometrium. Disordered proliferative endometrium is an exaggeration of the normal proliferative phase without significant increase in the overall ratio of glands to stroma. The changes involve the entire endometrial compartment, and are evident at low magnification as sacculated dilations (microcysts) randomly scattered amongst tubular glands lined by mitotically active epithelial cells. The stroma is usually dense, cellular and abundant, and mitoses may also be encountered. Some background tubular glands are slightly irregular and minimal budding and branching is commonly seen. Ciliated cell change (tubal metaplasia) of endometrial glandular cells is common, reflecting estrogen's pivotal role in the process. The estrogen primed cell often has substantial cytoplasm. Characteristically, glands affected by tubal differentiation are randomly interspersed amongst proliferative glands, and they also may demonstrate tubular, branching, or cystic architecture. Page 8
9 Benign endometrial hyperplasia. Benign endometrial hyperplasia develops from disordered proliferative endometrium under the continued influence of unopposed estrogens. The entire endometrial compartment contains variable gland densities caused by remodeling of stroma and glands to the extent that in some areas the gland to stroma ratio exceeds 1:1. It is the increased gland density that distinguishes benign hyperplasia from disordered proliferative endometrium. Individual glands may be tubular, cystic, or branching, and these forms are commingled throughout. On a large scale the endometrium appears uniformly affected, however, at medium magnification local admixtures of individually variable glands present quite differing appearances among separate microscopic fields. This combination of low magnification uniformity, made up of variable medium magnification fields, can be described as regularly irregular. A critical feature of benign hyperplasia is that the cytology does not change between architecturally crowded and uncrowded areas. This reflects the systemic hormonal etiology of the process that similarly exposes the entire endometrium, and allows its distinction from EIN. Cytologic characteristics may change over time with the evolving hormonal state of the patient, and superimposition of local factors such as breakdown and repair. During the established phase of active estrogen exposure glands are proliferative and interposed tubal metaplasia is common. Unopposed estrogen states are the most common setting in which fibrin thrombi are seen in the intact endometrial functionalis 10. Fibrin thrombi are rarely seen in normal late secretory endometrium, and there is little evidence that vascular thrombosis is a primary mechanism of normal menstrual shedding. Sometime after initiation of cystic gland dilatation the endothelial lining of ectatic superficial endometrial vessels becomes damaged and occlusive luminal fibrin thrombi form. Thrombi are often intimately associated with discrete areas of surrounding stromal breakdown, which has been interpreted either as a cause or effect of the vascular lesion. Whatever the sequence and mechanism of events, the two are linked in disordered proliferative endometrium and benign hyperplasias, and are responsible for patchy non-synchronous endometrial breakdown and resultant symptoms of spotting and intermenstrual bleeding. Collapse of intervening brokendown stroma may lead to close apposition of endometrial glands, degenerative epithelial changes, and dislodgement of vascular thrombi from their tissue context. Estrogen production from persistent follicles or by peripheral conversion following the menopause is inconstant. When the estrogen level declines slowly, massive breakdown does not occur and the glands lose mitotic activity. These endometria retain the architectural features of a bulky endometrium with altered gland architecture, but the glands demonstrate a mitotically inactive and non-stratified appearance and may be karyorrhectic. With waning estrogen levels, endometrial bulk declines towards an atrophic pattern, sometimes with cysts. Differential diagnosis of Benign Endometrial Hyperplasia A commonly encountered pattern that may be mistaken for benign endometrial hyperplasia is composed of prominent cystically dilated glands with flimsy walls composed of scant fibrous stroma. The terms cystic atrophy or cystic atrophic endometrium describe these lesions, which show cuboidal or flattened and inactive cells lining the distended glands. Furthermore, the glands in cystic atrophy lack budding and infoldings. Endometrial polyps may have many of the features of endometrial hyperplasia, but they are localized lesions with a distinctive stroma. Polyps arise as monoclonal overgrowths of genetically altered endometrial stromal cells with secondary induction of polyclonal benign glands through as yet undefined stromal-epithelial interactive mechanisms 12;13. Thick walled blood vessels and fibrous stroma commonly seen in polyps are lacking in benign endometrial hyperplasia. Because polyps are focal lesions, specimens obtained by undirected biopsy or curettage typically contain Page 9
10 commingled normal endometrium with a completely different histologic pattern. This is not the case with benign endometrial hyperplasia where the entire functionalis is affected. Despite these differences, there are individual cases in which the distinction between an endometrial polyp and lesions in the benign hyperplasia sequence can be difficult, and endometrial polyp remains one of the most common causes of an incorrect diagnosis of hyperplasia. Figure 2: Sequential Modulation of Benign Endometrial Hyperplasia. Accurate recognition of the class of changes referable to unopposed estrogen, here encompassed within the benign endometrial hyperplasia categories, is facilitated by recognition of their dynamic character and secondary modification within a sequential framework. Cessation or progesterone inhibition of prolonged estrogenic stimulation may occur at any time, at which point benign hyperplasias lose their mitotic activity and the endometrium is no longer proliferative. Architectural changes of the estrogen-driven interval are retained, so that a diagnosis of benign hyperplasia can provide indirect evidence of the prior hormonal state of unopposed estrogens. Benign endometrial hyperplasia with superimposed progestin effect. Superimposition of endogenous or exogenous progestins upon benign endometrial hyperplasia shuts down mitotic activity, and may initiate secretory change with or without subsequent stromal pre-decidualization. The most common endogenous progesterone source is delayed ovulation in a perimenopausal woman, where the corpus luteum is formed on an abnormal schedule, or otherwise is unable to elaborate normal quantities of progesterone. Similar effects can be seen in women having benign hyperplasia treated by low dose or intermittent progestins, such as are seen in many oral contraceptive formulations. High dose progestins, in contrast, usually induce pronounced stromal decidualization. The architecturally abnormal glands may persist within this background, but tend to become atrophic with time. Page 10
11 Withdrawal shedding following benign hyperplasia Cessation of estrogenic stimulation, such as occurs systemically upon shutdown or exhaustion of the persistently active ovarian follicle, leads to rapid endometrial-wide stromal breakdown and heavy menses. This occurs through a direct apoptotic effect upon endometrial stromal and epithelial cells, rather than thrombosis-initiated infarction responsible for breakdown during the estrogen rich period. Evidence of secretory and predecidual change may or may not be present, depending on whether delayed ovulation occurred, and the extent of tissue preservation. Architectural features of cysts and irregular gland distribution are increasingly obscured by stromal collapse, eventually yielding a nondescript collection of individual glands with extensive reactive changes. For these reasons, it can be difficult to confirm in the late stages of shedding whether the preceding cycle was normal or abnormal, or whether a benign hyperplasia was present or not. Fibrin thrombi, which are durable sequelae of many benign hyperplasias, remain identifiable despite extensive stromal breakdown. Page 11
12 Part II: Endometrial Intraepithelial Neoplasia EIN and Ambiguous Endometrial Lesions: ASCP1341, 2009 Biology of EIN: Endometrial Intraepithelial Neoplasia Endometria Intraepithelial Neoplasia (EIN) is a clonal proliferation of architecturally and cytologically altered premalignant endometrial glands which are prone to malignant transformation to endometrioid (Type I) endometrial adenocarcinoma 1. EIN lesions are non-invasive genetically altered neoplasms which arise focally, and may convert to malignant phenotype upon acquisition of additional genetic damage. Diagnostic criteria for EIN have been developed by histopathologic correlation with clinical outcomes, molecular changes, and objective computerized histomorphometry. EIN should not be confused with unrelated serous intraepithelial carcinoma (serous EIC), which is an early phase of (Type II) papillary serous adenocarcinomas of the endometrium. Management of EIN lesions follows guidelines long established for atypical endometrial hyperplasia. A high concurrent cancer rate (26%), and concern that sampling errors may miss an occult tumor, have led to a prevailing view that immediate hysterectomy is justified by its combined diagnostic and therapeutic benefits. Young patients wishing to preserve fertility, and women who are poor surgical risks, are candidates for hormonal (progestin) therapy. Systemic progestins can successfully ablate up to 90% of endometrial precancers in young women 14, although it is not possible in advance to predict that fraction which will respond. A decision to treat hormonally must thus be made between the clinician and patient in full light of the risks, and with the precondition that regular followup surveillance can be performed. Figure 3: Clonal Origin of EIN. The first genetic changes (such as PTEN inactivation) which Malignant Initiation Transformation Normal Histology (Polyclonal? Latent Clone ) EIN (Monoclonal Premalignant Neoplasm) Adenocarcinoma (Monoclonal Malignant Neoplasm) initiate endometrial carcinogenesis are unaccompanied by any phenotypic alterations at the light microscopic level. This latent, phase of cytologically and architecturally normal but genetically altered cells may persist for years in a normally menstruating woman. Low cancer risk, combined with lack of a rational therapeutic response, are reasons that systematic screening and treatment of these latent phase lesions is unwarranted at present. As additional genetic damage accumulates, higher risk morphologically altered mutant clones declare themselves by demonstrating those architectural and cytologic alterations that distinguish EIN. Malignant transformation of EIN lesions, which occurs at least 46-times more frequently than non-ein tissues, warrants careful diagnosis and treatment. Endocrine modifiers of endometrial cancer risk act upon the latent and EIN phases of this sequence by tipping the balance of clonal expansion vs. involution. Page 12
13 A combined molecular and histopathologic model for EIN: Latent, premalignant, and malignant phases of EIN-mediated endometrial carcinogenesis are diagrammed in Figure 3. In almost half of apparently normal women, histologically unremarkable proliferative endometria contain a small fraction of (PTEN tumor suppressor gene) mutant endometrial glands. This phase may be construed as latent because not only do the mutated glands look completely normal under the microscope, but they progress to EIN and cancer at very low efficiency. This latent phase may persist for years, with continued presence of scattered and interspersed mutant glands after many menstrual cycles 15. Mutant glands are probably represented in the reserve population of cells that regenerate a new functionalis each month. Endocrine factors act upon these latent precancers to modulate involution, or progression to EIN. Transition to EIN requires accumulation of additional genetic damage in at least one latent precancer cell, which then clonally expands from its point of origin (indicated by expanding arrows) to form a contiguous grouping of a tightly packed and cytologically altered glands recognizable as EIN. The monoclonal precancer (EIN) develops internal heterogeneity through mutation, and advantageous events selected by local conditions result in hierarchical subclones (left to right) of varying success. EIN lesions have only marginal increases in growth potential, and retain susceptibility to further growth modulation by hormonal factors. Some involute. Others, through additional mutation and selection, reach a stage where hormonal support is no longer required for survival. Malignant transformation to cancer is defined by accumulation of sufficient genetic damage to permit invasion of adjacent stromal tissues. What Is EIN? Endometrial Intraepithelial Neoplasia, EIN 16;17, is the histopathologic presentation of premalignant endometrial disease which confers an elevated risk for endometrial cancer. The singular category of EIN is not stratified or divided into subgroups, and must be distinguished from earlier phases of latent premalignant disease, and endometrial carcinoma. This term was proposed by The Endometrial Collaborative Group 16 to accommodate changing concepts of premalignant endometrial disease and take advantage of revised diagnostic strategies. EIN needs to be treated, and the type of therapy decided between the patient and treating physician. Things that may influence the choice of surgical vs. hormonal therapy include but are not limited to: diagnostic confidence that a co-existing carcinoma has been excluded, desire for maintained fertility, ability to perform followup surveillance, and patient-specific hormonal and surgical risks. Clinicopathologic Foundations Of EIN Rigorous experimental validation of clinically and biologically defined endometrial precancers, and development of correlative diagnostic criteria is a multidisciplinary process. Key predictions expected of precancers which have now been fulfilled for EIN, and practical aspects of their clinical implementation are listed in Table III: Page 13
14 Table III: Precancer postulates fulfilled for EIN Postulate Precancers differ from normal tissues Precancers share some, but not all features with carcinoma Precancers can be diagnosed Precancers increase risk for carcinoma Epidemiologic and genetic mechanisms are linked Introducing precancer genotype into an animal produces premalignant lesions and heightened cancer risk Evidence Monoclonal Divergent genotype 21. Including PTEN 22-24, K-ras 25-27, and MLH1 changes 28. Both are monoclonal 18-20;29. Precancer-cancer lineage hierarchy 21. Computerized morphometry reference standard for EIN 29 High concurrent cancer rate in EIN 4;4;30 High future cancer rate in EIN The PTEN gene, mutated in EIN, is subject to hormonal modulation 24;35 100% of PTEN mutant heterozygote mice get endometrial hyperplasia and 21% evolve to carcinoma. 36 WHO Hyperplasia-EIN Concordances Concordances with EIN diagnostic system and were obtained by review of cases initially diagnosed using other endometrial hyperplasia classification schemes 31 Complex. Figure 4: Correlation of WHO and EIN Diagnoses. Gray portions of Bar Graphs show approximate percentages of each WHO hyperplasia class that will be diagnosed as EIN. Remaining WHO hyperplasias not diagnostic of EIN (white) will be allocated to unopposed estrogen (anovulatory), polyp, and other categories. Pie chart shows relative contributions of each hyperplasia type to the EIN diagnostic category in a series of 97 cases with 28 EIN examples 31. Atypical Hyperplasia 78% Non-Atypical Hyperplasia 44% 29% 7% Simple Non-Atypical Hyperplasia 4% 64% Endometrial Intraepithelial Neoplasia Page 14
15 Clinical Cancer Outcomes Following EIN Diagnosis The risk of developing endometrial cancer, as predicted by an EIN diagnosis are the basis for therapy 30;32;33. A recent Gynecologic Oncology Group trial of immediate hysterectomy in women diagnosed with EIN on endometrial biopsy or curettage shows 38% (of 148 patients with EIN) had concurrent adenocarcinoma at hysterectomy 37. Of the carcinomas seen at hysterectomy, 67% (37/55) had no myoinvasion, 25% %(14/55) had myoinvasion within the inner half of the myometrial thickness, and 7% (4/55) had deep myoinvasion to the outer half of the myometrial thickness. These GOG study results are based upon subjective EIN diagnosis. Other studies show the cancer predictive value of subjective (Figure 5) 31 and objective histomorphometric (Figure 6) 4 EIN diagnosis amongst mixed groups of patients with and without EIN. Subjective EIN diagnosis outperforms cancer prediction when compared to WHO hyperplasia criteria (Fig. 5). Excluding concurrent cancers that are diagnosed within the first year of EIN, patients with EIN lesions have an overall 45-fold long term increased cancer risk than those without EIN. (Figure 6). Figure 5: Cancer outcomes (black), by followup interval (vertical axis) of 97 endometrial biopsies diagnosed by WHO hyperplasia (left) or EIN (right) schema 31. Endometrial hyperplasias (left panel) were rediagnosed subjectively (without morphometry) as EIN or benign, non-ein (right panel). All 8 cancer outcomes (black symbols) followed an initial diagnosis of EIN. EIN has a better negative predictive value than atypical hyperplasia, as 2/8 cancer occurrences were seen in the nonatypical hyperplasia groups. Followup Interval, Days Outcome No Cancer Cancer Hyperperplasia Schema Simple no atypia Complex no atypia Complex atypical Benign, Non-EIN EIN Schema EIN Figure 6: Long term cancer progression in women with EIN 4. Cancer outcomes that occur more than one year after EIN diagnosis are bona-fide progression events from a premalignant to malignant phase of disease. Progression to cancer more than one year following EIN diagnosis is 45 times more likely compared to women without EIN. Note the tempo of cancer appearance indicates that it can take years for an EIN to evolve into adenocarcinoma Women with endometrial hyperplasia restratified into EIN vs. non-ein categories. 2/359 non-ein and 22/118 EIN cases developed adenocarcinoma. Cancer Free Survival 1.0 Benign (DS>1) EIN (DS<1) HR=45 \\ Followup Time, Months Page 15
16 How Is EIN Diagnosed? 5 (also see EIN is diagnosed by a pathologist using routine (hematoxylin and eosin stained) sections prepared from a representative endometrial sample 38;39. It is extremely important to note that diagnostic accuracy may be severely compromised by exogenous progestin-containing hormonal therapies. For this reason, primary diagnosis or followup surveillance of a suspected EIN lesion should be based whenever possible on a sample obtained while the patient is not on therapeutic hormones. For those patients on progestins, diagnostic tissue can be obtained 2-4 weeks after stopping exogenous hormones, after completion of a withdrawal bleed. Although computerized morphometry has been a useful tool in identifying features characteristic of EIN, such equipment is not required for routine diagnosis. Rather, pathologist interpretation of stated criteria at a standard microscope is adequate. It should be noted that EIN is a precursor of endometrioid endometrial adenocarcinomas and is unrelated to the "Endometrial Intraepithelial Carcinoma" proposed 40 to be the earliest stages of papillary serous type endometrial adenocarcinomas. A framework for EIN Diagnosis is shown in Table I at the beginning of this sylabus. Notable is the clear separation of endometrial changes caused by unopposed estrogens, and carcinoma, from EIN. 1.Topography of EIN The distribution of a lesion is useful in distinguishing between the diffuse, field-wide effects, of an abnormal hormonal environment (anovulation, or persistent estrogen effect), surface changes secondary to stromal breakdown, and more focal EIN. Clonal origin from a single cell requires EIN lesions to begin as local processes within the endometrial compartment. Early EIN lesions are easily diagnosed by their contrast in architecture and cytology with the background from which they have emerged. Over time, EIN lesions may completely overrun the background endometrium, thereby removing the convenient lesion-to-background contrast in morphology which assist in EIN diagnosis. For this reason, or because of fragmentation, many EIN lesions must be diagnosed without the benefit of comparison with companion benign tissues. Exclusion of artifact and careful evaluation of the architectural and cytologic features of EIN usually permits accurate diagnosis in these instances. 2.EIN Diagnostic Criteria All of the diagnostic criteria of Table IV, listed as A-E below, must be met in order to make an EIN diagnosis. The entire slide should first be scrutinized under low magnification for localizing lesions, and if found, these areas examined under higher power to assess possible changes in cytology within the architecturally distinct focus. Widespread EIN lesions that have replaced the entire endometrial compartment tend to have a sufficiently atypical cytology that background normal endometrium is no longer required as a reference point for accurate diagnosis. Size, architecture, and cytology features are easy EIN diagnostic criteria. Much more difficult are exclusion of benign mimics and adenocarcinoma from the differential diagnosis. There are no simple rules for benign mimic exclusion. The broad universe of competing entities can only be recognized on sight by one who has the easy familiarity that comes with experience. Consistent demarcation of the EIN-adenocarcinoma threshold remains important clinically because it provides a basis for the clinician to evaluate the risks of electing hormonal rather than surgical therapy in Page 16
17 younger patients who wish to retain fertility. Special diagnostic challenges, such as recognition of EIN within polyps, interpretation of subdiagnostically small or fragmented lesions, and interpretation of lesions with non-endometrioid differentiation have specific caveats presented below that should be carefully studied. Table IV: EIN Diagnostic Criteria. Modified after 17. EIN Criterion Architecture Cytology Size >1 mm Exclude mimics Exclude Cancer Area of Glands greater than Stroma Comments Cytology differs between architecturally crowded focus and background, or clearly abnormal. Maximum linear dimension exceeds 1mm. Benign conditions with overlapping criteria: Basalis, secretory, polyps, repair, etc.. Carcinoma if mazelike glands, solid areas, polygonal mosaic-like glands, myoinvasion, or significant cribriforming a.architecture: Gland area exceeds stromal area: A cardinal architectural feature of endometrial precancers is glandular crowding, with a threshold quantitative cutoff for EIN lesions of less than half of the tissue area occupied by stroma (Volume Percentage Stroma). Areas with large dominant cysts should always be avoided in making this assessment. Although EIN is an epithelial disease, visual assessment of the glands themselves is complicated by frequent artifactual displacement from associated stroma, pale staining of most epithelia, and visual "shimmering" between gland epithelia and lumens. These may all be avoided by focusing on the stromal compartment which has the significant advantages of a more uniform composition throughout the specimen, and superior staining qualities. By focusing on the stroma itself only intact fragments in which stroma has not been avulsed from glands will be evaluated. Careful review of graphic and histologic examples of varying stromal densities will assist in training your eye to classify patient material as above or below the diagnostic threshold. EIN lesions tend to cluster with a median volume percentage stroma of about 40% and non-ein (benign) lesions cluster at a median of approximately 75%. These differences are sufficiently great that visual assessment by a trained eye can be informative. b.cytology of architecturally crowded area is different than background, or clearly abnormal: There is no absolute standard for cytologic features of EIN lesions, but the cytology of EIN is usually clearly demarcated as divergent from that of co-existing benign endometrial tissues in the same patient. The manner of cytologic change in EIN varies considerably from patient to patient, and can include but not be limited to, increased variation in nuclear size and contour, clumped or granular chromatin texture, change in nucleoli, change in nuclear/cytoplasmic ratio, and altered cytoplasmic differentiation. Stereotypical static descriptions of cytologic atypia, such as nuclear rounding and appearance of nucleoli are met in many but not all EIN lesions. In this sense, a fixed Page 17
18 presentation of cytologic atypia is not a prerequisite for EIN. Attempts to define an absolute standard are confounded by the extreme morphologic plasticity of endometrial glandular cells under changing hormonal, repair, and differentiation conditions. Cytologic changes in some EIN lesions are manifest as a change in differentiation state to a tubal, mucinous, micropapillary, or eosinophilic phenotype. These must be distinguished from the scattered random pattern of hormonally, or surface located repair-induced metaplasias. Further details of how to interpret non-endometrioid EIN lesions are presented in the Pitfalls section below. In those cases with no normal glands for internal reference, it is necessary to assess the freestanding cytology of relevant fragments in the context of their architectural features. Some EIN lesions occupy the entire tissue sample, and should not be underdiagnosed for lack of a convenient benign gland in the area. c.size >1mm in maximum dimension: Accurate EIN diagnosis requires a contiguous field of glands sufficiently large to enable reliable assessment of architecture. A minimum lesion size of 1 mm maximum dimension was required in the previous clinical outcome studies 4;30;32;34 for an EIN lesion to achieve elevated cancer risk. That area of an EIN lesion which meets architectural (gland area) and cytologic (changed) criteria for diagnosis must measure a minimum of 1mm in maximum dimension, a scale which usually encompasses more than 5-10 glands. Most biopsy formats produce tissue fragments in excess of 1.5-2mm. The size requirement must be met in a single tissue fragment, not added amongst multiple fragments. There is no formal evidence that once beyond the minimum 1mm, EIN lesions should be stratified by size, but if a lesion is discretely focal, it may be of interest to the clinician to know what fraction of the available curettings contain lesion. Individual or small clusters of cytologically altered glands have an undefined natural history and are best diagnosed descriptively (See Pitfalls section below). d.exclusion of Benign Mimics Patients with one of the conditions listed below may still have an EIN, but this diagnosis should be made with careful consideration into how the coexisting factor(s) may modify the criteria for EIN diagnosis. If a specimen is refractory to confident diagnosis, a comment as to the nature of the problem may be useful in directing management. 1. Reactive changes caused by infection, physical disruption, recent pregnancy, or recent instrumentation. These can cause piling up of the epithelium, and loss of nuclear polarity.. 2. Artifactual gland displacement. Beware diagnosing an EIN lesion if the cytology is identical between areas with crowded compared to uncrowded glands! Many of these are artifactual disruptions where the stroma is sheared and glands pushed in apposition. 3. Persistent Estrogen Effect: Randomly scattered cysts of protracted estrogen exposure and occasional branching glands are commonly encountered in anovulatory or estrogen-exposed endometria. Gland density is uniformly irregular throughout the endometrial compartment, with occasional clusters of glands having a cytology identical to the uncrowded areas. These can be diagnosed as Benign Endometrial Hyperplasia if glands are significantly crowded, or in some mild cases as "disordered proliferative" endometrium. With increasing duration, microthrombi form and scattered stromal breakdown may be associated with epithelial piling along the collapsed stromal surfaces. 4. Mid to late secretory endometrium displays loss of nuclear polarity, nuclear enlargement, and variation in nuclear size which if measured objectively by computerized morphometry overlaps substantially with EIN lesions. Stromal responsiveness to progesterone is not homogenous at all endometrial depths. Lack of stromal pre-decidualization in the deeper Page 18
19 functionalis and superficial basalis makes glands appear crowded, and these same glands may display a worrisome cytology and complicated saw-toothed luminal profiles 5. Endometrial polyps contain irregularly spaced glands in which scattered glands may differ from native endometrium due to their tendency to have reduced hormonal responsiveness. Benign polyps may also have low volume percentage stroma caused by cysts (senile polyps) or random aggregations of glands. Approximately 10% of EIN lesions, however, will present within an endometrial polyp and these must be diagnosed as described below in the Pitfalls section. 6. Endometrial breakdown is one of the most common settings for overdiagnosis of a benign endometrium as a precancer or cancer. Breakdown may follow an ovulatory or anovulatory cycle and persist into the transitional period between late menses and early proliferative endometrium. Altered cytology is due to piling up of epithelial cells unsupported by stroma, and associated nuclear changes such as loss of polarity which may be accentuated under certain fixation conditions which exaggerate chromatin texture (Bouin's fixative). e.exclusion of Carcinoma Cancer may coexist with EIN in an individual patient, but should be always be separately diagnosed because current management of carcinoma differs from that for EIN. Keep in mind that absence of carcinoma in a tissue biopsy does not exclude the possibility of that the patient has a cancer which was unsampled during the biopsy procedure. An opinion should always be rendered based upon available material, and clearly stated. EIN is composed of individual glands lined by an epithelium one cell layer thick. The epithelium may be pseudostratified, but should not be cribriform or composed of solid areas of epithelial cells. Presence of any of the following features involving neoplastic glands is inconsistent with EIN, and a diagnosis of carcinoma should be entertained. 1. Meandering or mazelike lumens 2. Solid epithelium 3. Cribriform architecture. 4. Mosaic gland pattern of distorted polygonal glands with threadlike intervening stroma Myoinvasion. Unfortunately, myometrium is rarely available for evaluation in a biopsy or curettage specimen. Page 19
20 Pitfalls of EIN Diagnosis: A Practical Approach George L. Mutter, MD Introduction: Uncommon presentations of common diseases, and suboptimal specimens are two of the many sources of diagnostic difficulty in endometrial pathology. Combined with a "normal" reference point which changes dynamically throughout the month, and during the life cycle, the very definition of "abnormal" depends on the clinical setting. This section will serve as an introduction to some of the more common problems, with suggestions for coping strategies that will not compromise management of the patient 5. Table I: Pitfalls in EIN Diagnosis. Problem Fragmented or Distorted Incompatible History Interpretation Ambiguous Non-Endometrioid Differentiation Progestin Effect Uncertain Source Response Get levels and rebiopsy soon if still worried Call clinician or comment Consult peers. Descriptive Dx and state differential Dx. Use differentiation specific criteria Withdraw hormones and rebiopsy 2-4 weeks after cessation of withdrawal bleed Fractional D&C If confounding factors preclude a definitive classification of the specimen at hand, make a descriptive diagnosis and clearly communicate the character of the unresolved differential and specific reason for diagnostic uncertainty. Pathologists vary in their attitudes towards making clinical recommendations for followup within the pathology report. We do this routinely, especially if the sampling instrument or strategy needs to be changed in the next diagnostic procedure, or the clinician must discontinue progestins to improve diagnostic accuracy. Whatever the venue for communication, the pathologist is often well equipped to contribute a constructive plan for resolution of the diagnostic problem. For example, the patient who is biopsied while on exogenous progestins may be easier to evaluate after withdrawal of hormones. Confusing histologies such as those obscured by extensive altered cellular differentiation ("metaplasias") should be described clearly. Other specimens may be compromised by sampling errors, or superimposed regenerative epithelial changes. All should be clarified by additional studies, deeper levels or immediate resampling to detect the presence of diagnostic areas elsewhere, or followup with rebiopsy. If the patient is symptomatic, some clinicians will elect to treat with a trial of high Page 20
21 dose progestins followed by a post-withdrawal biopsy. Recommendations for interpretation of some commonly encountered diagnostic problems are listed in Table I. Subdiagnostic EIN-like lesion: Lesions suspicious for but subdiagnostic for EIN deserve clear description and if clinically appropriate, resampling. Obvious localizing lesions characterized by a changed cytology sometimes do not meet either the minimal 1 mm size or 50% volume percentage stroma EIN requirements. This is a heterogenous group composed of examples of poorly sampled EIN lesions, very early precursors of EIN that have not yet reached the diagnostic threshold, and subtle benign mimics. The fragment context of small or loosely packed localizing lesions should be evaluated after obtaining deeper levels. If the affected fragments in deeper levels remain <1mm in size, with densely packed lesional glands extending from edge to edge, there is a high likelihood that tissue disruption of a larger lesion is the problem. These may be diagnosed as Fragments of crowded glands with altered cytology consistent with, but not diagnostic of, EIN with a recommendation to resample within 3 months. If the fragment is large, but the focus of clustered cytologically altered glands remains <1mm, or has insufficient gland density for EIN, then sampling error is unlikely. This is a small category of cases, comprising roughly one fifth or one quarter of the frequency of easily diagnosed EIN lesions. These rare lesions are probably pre-ein precursors with a lower cancer risk than bona fide EIN. They should be diagnosed descriptively ( microscopic cluster of cytologically altered glands, See Note ) with a recommendation for followup biopsy in 6 months. Every effort should be made to avoid overdiagnosis of small groups of contrasting glands as EIN. Patients with unopposed estrogens may randomly have a few tubal glands in proximity, polyps can contain irregular distributions of glands, and the patient with endometritis or repair can have local effects which polarize the endometrium. Examination of the background context is most helpful in these circumstances. EIN within an Endometrial Polyp 41 : In general, all criteria for EIN diagnosis apply to EIN arising within a polyp, but the reference point for interpretation of EIN cytology and architecture are the background polyp itself, not the normal endometrial functionalis. EIN within polyps are best recognized as geographic regions of contiguous glands with an architecture and cytology readily distinguished from that of the background polyp. Avoid overreaction to bland dominant cysts lined by atrophic epithelium, as these are a common component of benign senile polyps or mixed endocervical-endometrial polyps. The benign polyp will have a regularly irregular distribution of glands. Cytologic variation will not appear in geographic clusters of glands, but rather interspersed or splayed on the periphery with loose boundaries. Random apposition of glands in proximity can be recognized by a cytology identical to that of more dispersed glands elsewhere in the polyp. On those occasions when EIN is diagnosed within a polyp, the polyp setting should be clearly mentioned in the report. If completely excised, a polypectomy may be curative. If incompletely excised, the physical bulk of a polyp can prevent adequate followup sampling by flexible devices (Pipelle). Non-Endometrioid EIN vs. Metaplasia 41 : EIN lesions with non-endometrioid cytology must be distinguished from benign metaplasias. A shift in cytodifferentiation may be the cytologic change which characterizes some EIN examples, which also meet other size, architecture, and exclusion criteria. In most instances Page 21
22 they are localizing lesions with a classic EIN geography composed of mucinous, tubal, or eosinophilic glands. A special case are those glandular lesions containing round intraluminal expansile squamous morules. These morules may be quite abundant, creating distortion of the volumetric relationships between gland and stromal compartments. Since it is the glandular, not morular component of these lesions which have premalignant behavior, the bulk contributed by morules should be mentally excluded when assessing the size of the glandular vs. stromal compartments 42. If possible, search for morule poor areas with glands that meet EIN criteria. The differential diagnosis between EIN and carcinoma may have special considerations in non endometrioid lesions. Solid morules surrounded by a peripheral garland of lumen-containing glands resemble a cribriform pattern that may easily be overinterpreted as adenocarcinomas. True cribriforming involves glandular epithelium only, and should not be diagnosed when the cells separating individual lumens are squamous. Criteria for diagnosis of a mucinous and squamous adenocarcinomas are different than those for endometrioid adenocarcinomas. The distinction between EIN and carcinoma in these cases must be made using differentiation-state appropriate criteria. Confounding progestin exposure: Progestins, whether endogenous or pharmacologic, alter endometrial gland cytology and variably expand the stromal compartment to modify gland-stromal relationships. EIN lesions exposed to progestins tend to display nuclear shrinkage and homogenization of coarse chromatin, with pseudodecidual change responsible for separation of glands making them appear less crowded. In contrast, nuclei of glands in normal secretory endometrium greatly enlarge, and the proportion of glands to stroma varies by height within the functionalis. The paradoxical result is that in the presence of progestins EIN lesions become more bland, and normal endometrium more worrisome. In its most extreme form, pregnant patients with Arias Stella phenomenon have dramatic epithelial atypia caused by polyploidy, and these areas typically demonstrate minimal stromal decidualization, resulting in very crowded gland architecture. Many EIN lesions rebiopsied in the midst of a course of therapeutic progestins will no longer be diagnostic. For this reason, the pathologist should avoid providing assurance of therapeutic efficacy from a biopsy secured while still on progestins. When diagnostic features are present, EIN lesions can and should be diagnosed through a progestin effect. This may be somewhat deceptive to the clinician, however, as much of the therapeutic benefit of progestin therapy is conferred by the massive wave of apoptosis and endometrial shedding which follows withdrawal of progestins 43. The patient still on hormones has not yet reached the culmination of therapy, so the significance of persistent EIN lesions in that setting is unclear. This combination of interpretive difficulties for the pathologist, and premature endpoint for the patient, makes biopsy while still on progestins an inappropriate followup for a known EIN lesion. A recommendation for rebiopsy 2-54 weeks after withdrawal of hormones is in the best interest of the patient. Page 22
23 Endometrial Metaplasias and Ambiguous Lesions George L. Mutter, MD Introduction: Endometrial metaplasias are defined as epithelial differentiations that differ from the conventional endometrioid epithelium. In this segment the term metaplasia is synonymous with (altered) differentiation. The latter interpretation is preferable when referring to endometrial intraepithelial neoplasia or cancer to avoid confusing metaplasia in these settings with a benign process or implying that the distinction between metaplasia and neoplasia can always be made. However, for simplicity, the term metaplasia will be used here. Heterotopic differentiation, or "metaplasia", is an altered differentiated cellular phenotype seen as a predominant or minor pattern of some Type I, or endometrioid, endometrial carcinomas and their precursor lesions. In a sense, metaplastic changes are the pathologist s disease. They are not recognized clinical disorders and the clinician does not routinely record rule out metaplasia on the pathology requisition. Rather, metaplastic changes are a spectrum of processes that may be benign, premalignant (EIN), or malignant (carcinoma) 1. When the pathologist encounters altered differentiation during the examination of endometrial biopsies or curettings, he or she must decide which of these contexts is the setting for altered differentiation, and use diagnostic terminology which clearly advises the clinical caregiver to pursue the most appropriate course of action. Metaplasias? Process Benign Premalignant Malignant Diagnosis Background process, with metaplasia EIN, with differentiation Adenocarcinoma, with differentiation A central problem is that a change in differentiation state alone is a nonspecific reflection of the state of endometrial tissue. Metaplasia in the endometrium may occur in benign conditions, arise in association with premalignant lesions (EIN) or be a part of endometrial carcinomas 41;44. Because of the wide range of entities associated with metaplasia, these changes can be viewed as a parallel universe composed of altered differentiation that interdigitates with, and mirrors the biology of, the endometrial surface and glandular epithelium. Endometrial "metaplasias" are best thought of simply as an altered differentiation state, in which the context, molecular biology, and subsequent natural history must be examined to determine whether an individual example is benign, premalignant, or malignant. We prefer to avoid use of "metaplasia" as a diagnostic entity, but rather diagnose the functional class of disease first, with a secondary description of differentiation state. Page 23
24 Geometry of Benign, Premalignant, and Malignant lesions Benign Premalignant Malignant Repair Anovulatory EIN Carcinoma Surface Repair Estrogen Mutation, Clonal Aggressive Regularly Irregular Figure: Topography of Metaplasia. Large scale topography has been greatly underestimated as a useful feature in resolving the reactive, premalignant, or malignant characteristics of of metaplastic lesions. It is the geographic aggregation of similarly altered endometrial glands, a reflection of clonal growth, which is seen in EIN and adenocarcinoma but not in hormonally induced changes. Careful examination of tissue integrity, including stromal breakdown and presence or absence of inflammation, will assist in identification of localizing reactive processes that may include a metaplastic component. EIN lesions with complete, or more often partial, mucinous, squamous morular, tubal, eosinophilic, or micropapillary differentiation must be distinguished from their benign counterparts using standard EIN criteria. Altered differentiation state is only one of the many ways in which lesion cytology can be offset from the background in EIN. The change in cytology may involve the cytoplasm primarily, with a variable degree of nuclear change. To some extent, the specific type of altered differentiation dictates additional elements that must be incorporated into the diagnosis. For example, the morular component of EIN with squamous morules should be ignored in calculating the ratio of glands to stroma. Morules are functionally inert, and it is the abundance of glandular elements relative to stroma that determines cancer risk. Morules surrounded by glands present a cribriform-like appearance that should not be confused with adenocarcinoma. Guidelines for separation of EIN from carcinoma may be modified in non-endometrioid lesions. Each of the following categories illustrates a range of epithelial changes that depict a spectrum from benign to malignant. The portrayed range of epithelial histologies does not necessarily imply that each is part of a biologic progression or continuum. The morphologic distinction between syncitial, mucinous, ciliated (tubal), eosinophilic and even squamous metaplasia may not always be clear-cut, inasmuch as many of these patterns may be present in the same specimen or locus. Moreover, certain metaplasias are unclassifiable, consisting only of cells with pale or eosinophilic cytoplasm and no specific form of differentiation. Page 24
25 Squamous Differentiation 45 Squamous Differentiation Benign Premalignant Surface Repair, ( syncitial metaplasia ) Endometritis w/squamous Differentiation (Ichthyosis) Isolated Squamous morules (+/- local gland changes) EIN, with squamous morular differentiation Malignant Endometrial Adenocarcinoma, Endometrioid Type, (Type I) with squamous (morular) differentiation Squamous metaplasia is most commonly seen as a squamous morule within an individual gland. Squamous morules can be observed in endometria ranging from proliferative to carcinoma, and be part of distinctive entities such as atypical polypoid adenomyomas. The most important parameter determining the management of a lesion containing squamous morules is the degree of associated glandular complexity and atypia. Squamous morules may be associated with architecturally and cytologically normal glands, or an EIN. Squamous morules, unlike endometrial galnds, are devoid of estrogen and progesterone receptors and thus refractory to hormonally mediated progression to carcinoma. It is the glanduar, not squamous components or EIN, that are prone to progress to carcinoma. Management is based upon the glandular pattern. Isolated squamous morules may persist following involution of the glandular component. If morules are found in isolation, an undersampled coexisting EIN lesion must be excluded by repeat evaluation. Cribriform gland architecture is one specific feature which if present, can be used to distinguish between an EIN and adenocarcinoma. Squamous morules, commonly surrounded by a garland of glands mimicking a cribriform arrangement, should not be misinterpreted as carcinoma. Page 25
26 Morule Natural History Emergent Glandular Clone Intraluminal Morule Subclone EIN with Morules Isolated Morules Morules Shed Gland Involution by Progestins Figure: Squamous Morules: Model of endometrial morule evolution. Neoplastic premalignant glands (blue) emerge from a background of normal polyclonal glands (black). Mutational changes within the premalignant lesion induce squamous trans-differentiation of a subset of cell from the neoplastic clone to create intraluminal squamous morules (red). Modulating influences of progestins (cancer protecting) and estrogens (cancer promoting) act specifically upon glandular elements. Morules lack sex hormone receptors and significant mitotic activity. Estrogens promote progression of the glandular element of a precancer to a glandular (adeno) carcinoma. Progestins lead to selective involution of premalignant glands, with shedding or persistence of hormonerefractory morules. Modified after 44. Page 26
27 Mucinous differentiation 46 Mucinous Differentiation Benign Polyp, mixed endometrial/endocervical type Surface degeneration with mucinous change Premalignant EIN, with tubal differentiation Malignant Endometrial Adenocarcinoma, Endometrioid Type, (Type I) with mucinous differentiation Mucinous change in the endometrium also runs a spectrum from architecturally simple strips of benign endocervical type cells to obvious frank mucinous carcinoma. The problem in distinguishing benign from potentially malignant mucinous change in the endometrium centers upon its relatively bland cytomorphology, and frequent uncertainy regarding its site of origin (cervix vs. endometrium). Fractional curettage may assist in the latter. The degree of concern over mucinous endometrial change parallels the degree of architectural complexity. Mixed endometrial-endocervical polyps are common, as is extracelluar mucin droplets in degenerative epithelium. Excluding these benign processes, development of bona fide cytoplasmic mucinous differentiation within the endometrium is often associated with a neoplastic process. EIN lesions with mucinous differentiation usually have a mixed differentiation state, of which mucinous is only one component. These should be diagnosed using EIN criteria. Adenocarcinomas with mucinious differentiation fall into two general architectural categoris, both of which are biologic subsets of the Type I (or "endometrioid") class of carcinomas. First are those frank mucinous carcinomas in which the presence of both complex architecture and cytologic atypia makes the diagnosis relatively straightforward. The second category consists of a complex, exophytic, mucinous proliferation characterized by delicate philiform excresences supported by a thready fibrous core, often acoompanied by small glands with rigid, punched out appearing lumens such as seen in microglandular hyperplasia of the endocervix. The cytology may be very bland, and these are recognized as carcinomas either through the microglandular component, or simple abundance of complex contiguious fronds of mucinious epithelium. Cytologic atypia and mytoses, when present, are minimal. Page 27
28 Tubal differentiation Tubal Differentiation Benign Anovulatory, with tubal differentiation Premalignant EIN, with tubal differentiation Malignant Endometrial Adenocarcinoma, Endometrioid Type, (Type I) with tubal differentiation Tubal metaplasia is not conspicuous in cycling endometrium but is very frequent in anovulatory endometria or endometria responding to hormonal replacement therapy. Because it is induced by systemically circulating estrogens, individual metaplastic glands are randomly distributed theoughout the endometrial compartment in a "regularly irregular" manner. Like squamous metaplasia, tubal metaplasia can present with a spectrum of cytologic changes. Classically, tubal metaplasia contains prominent cilia and cells with round nuclei and cytoplasmic clearing mimicking cells seen in the normal fallopian tube. At times the clear cells occur in groups and on tangential section may have a honeycomb appearance. When this lesion presents as prominent cilia within architecturally normal gland tracts, the diagnosis of tubal metaplasia is made without further qualification. However, like squamous metaplasia and other metaplasias to be discussed, tubal metaplasia can in some cases present as "tubal differentiation", in which the cilia are not conspicuous and the morphologic pattern is that of a pseudostratified epithelium with sporadically placed clear cells. In some instances this epithelia may contain loss of cell polarity and variable cytologic atypia. We subclassify such cases based upon the glandular pattern. If the gland architecture is crowded in a discrete focus offset from the background endometrial glands a diagnosis of EIN should be considered. We have observed well-differentiated endometrial adenocarcinomas which retain some degree of tubal differentiation, including cillia. This may also be accompanied by mucinous or secretory differentiation. They are discriminated from EIN with tubal differentiation, but the presence of architectural features of carcinoma. Page 28
29 Eosinophilic (Oxyphilic) Differentiation Eosinophilic Differentiation a subset of Tubal/Papillary Benign Anovulatory, with eosinophilic differentiation Endometritis, with eosinophilic differentiation Premalignant EIN, with eosinophilic differentiation Malignant Endometrial Adenocarcinoma, Endometrioid Type, (Type I) with eosinophilic differentiation Eosinophilic metaplasia is an uncommon form of differentiation characterized by an oxyphilic appearance to the individual cells. Eosinophilic metaplasia bears some resemblance to tubal metaplasia but is devoid of cilia. Because its distinguish feature is eosinophilic cytoplasm, eosinophilic metaplasia is basically a descriptive entity. The epithelium is typically arranged in a single layer of cuboidal cells with uniform round nuclei. Similar to tubal and mucinous metaplasias, classification of eosinophilic metaplasia is linked to degree of architectural complexity and large scale topography (diffuse vs. localizing). Eosinophilic changes are occasionally seen in polyps, EIN and in endometrial carcinoma. Page 29
30 Papillary Differentiation: Papillary Differentiation Benign Anovulatory, with degenerative changes Menstrual with secondary surface changes Premalignant EIN, with micropapillary differentiation Malignant Endometrial Adenocarcinoma, Endometrioid Type, (Type I), with papillary differentiation vs. Endometrial Adenocarcinoma, Papillary Serous Type, (Type II). Some endometrial metaplasias might best be classified as papillary, a group that typically overlaps with eosinophilic and tubal metaplasias. Such alterations include surface reparative changes (papillary syncytial metaplasia), and proliferations containing mucinous, eosinophilic or tubal metaplasia. We generally approach papillary syncytial proliferations as a generic group of changes in which certain features suggest benign processes and other features warrant closer follow-up. Papillary syncytial metaplasia is a bland accentuation of reparative surface changes, is often associated with stromal breakdown, and is benign. When papillary proliferations are associated with an architecture suggesting EIN or carcinoma, those entities must be excluded. Page 30
31 Secretory Metaplasia Secretory Differentiation Benign Secretory Endometrium Hypersecretory endometrium (incl. A-S) Premalignant EIN, with secretory differentiation Malignant Endometrial Adenocarcinoma, Endometrioid Type, (Type I) with secretory differentiation Hormonally induced hypersecretory changes of a non-neoplastic and benign character may present with very crowded architecturally complex glands, with or without large pleomorphic nuclei. The prototypical example of this is the Arias Stella phenomenon. Secretory changes may be seen in EIN and adenocarcinoma. These can occur either as a hormonally induced secretory change within neoplastic cells, or represent an intrinsically altered differentiation state acquired upon neoplastic transformation. these may be resolved by careful examination of the background normal endometrium to determine if effects of circulating progestins are evident. Cytology of secretory EIN and adenocarcinoma may be quite bland, with small nuclei displaced to varying degress by cytoplasmic vacuoles. Page 31
32 References 1. Mutter GL, Zaino RJ, Baak JPA, Bentley RC, Robboy SJ. The Benign Endometrial Hyperplasia Sequence and Endometrial Intraepithelial Neoplasia. Int J Gynecol Pathol 2007; 26: Scully RE, Bonfiglio TA, Kurman RJ, Silverberg SG, Wilkinson EJ. Uterine corpus. Histological Typing of Female Genital Tract Tumors. New York: Springer-Verlag, 1994: Zaino RJ. Endometrial hyperplasia: is it time for a quantum leap to a new classification? Int J Gynecol Pathol 2000; 19(4): Baak JP, Mutter GL, Robboy S et al. The molecular genetics and morphometry-based endometrial intraepithelial neoplasia classification system predicts disease progression in endometrial hyperplasia more accurately than the 1994 World Health Organization classification system. Cancer 2005; 103(11): Mutter GL, Zaino RJ, Baak JPA, Bentley RC, Robboy SJ. Benign endometrial hyperplasia and EIN. In: Robboy SJ, Mutter GL, Prat J, Bentley R, Russell P, Anderson MC, editors. Robboy's Pathology of the Female Reproductive Tract. New York, New York: Elsevier, 2008: Writing Group for the PEPI Trial. Effects of hormone replacement therapy on endometrial histology in postmenopausal women. The Postmenopausal Estrogen/Progestin Interventions (PEPI) Trial. JAMA 1996; 275: Parazzini F, La Vecchia C, Bocciolone L, Franceschi S. The epidemiology of endometrial cancer. Gynecol Oncol 1991; 41: Shapiro S, Kelly JP, Rosenberg L et al. Risk of localized and widespread endometrial cancer in relation to recent and discontinued use of conjugated estrogens. N Engl J Med 1985; 313(16): Zeleniuch-Jacquotte A, Akhmedkhanov A, Kato I et al. Postmenopausal endogenous oestrogens and risk of endometrial cancer: results of a prospective study. Br J Cancer 2001; 84(7): Ferenczy A. Pathophysiology of endometrial bleeding. Maturitas 2003; 45(1): Song J, Rutherford T, Naftolin F, Brown S, Mori G. Hormonal regulation of apoptosis and the Fas and Fas ligand system in human endometrial cells. Mol Hum Reprod 2002; 8(5): Fletcher J, Pinkus J, Lage J, Morton C, Pinkus G. Clonal 6p21 rearrangement is restricted to the mesenchymal component of an endometrial polyp. Genes Chrom Cancer 1992; 5: Dal Cin P, Vanni R, Marras S et al. Four cytogenetic subgroups can be identified in endometrial polyps. Cancer Res 1995; 55: Randall TC, Kurman RJ. Progestin treatment of atypical hyperplasia and well-differentiated carcinoma of the endometrium in women under age 40. Obstet Gynecol Surv 1997; 90(3): Mutter GL, Ince TA, Baak JPA, Kust G, Zhou X, Eng C. Molecular identification of latent precancers in histologically normal endometrium. Cancer Res 2001; 61: Mutter GL, The Endometrial Collaborative Group. Endometrial intraepithelial neoplasia (EIN): Will it bring order to chaos? Gynecol Oncol 2000; 76: Silverberg SG, Mutter GL, Kurman RJ, Kubik-Huch RA, Nogales F, Tavassoli FA. Tumors of the uterine corpus: epithelial tumors and related lesions. In: Tavassoli FA, Stratton MR, editors. WHO Classification of Tumors: Pathology and Genetics of Tumors of the Breast and Female Genital Organs. Lyon, France: IARC Press, 2003: Esteller M, Garcia A, Martinez-Palones JM, Xercavins J, Reventos J. Detection of clonality Page 32
33 and genetic alterations in endometrial pipelle biopsy and its surgical specimen counterpart. Lab Invest 1997; 76: Mutter GL, Chaponot M, Fletcher J. A PCR assay for non-random X chromosome inactivation identifies monoclonal endometrial cancers and precancers. Am J Pathol 1995; 146: Jovanovic AS, Boynton KA, Mutter GL. Uteri of women with endometrial carcinoma contain a histopathologic spectrum of monoclonal putative precancers, some with microsatellite instability. Cancer Res 1996; 56: Mutter GL, Boynton KA, Faquin WC, Ruiz RE, Jovanovic AS. Allelotype mapping of unstable microsatellites establishes direct lineage continuity between endometrial precancers and cancer. Cancer Res 1996; 56: Levine RL, Cargile CB, Blazes MS, Van Rees B, Kurman RJ, Ellenson LH. PTEN mutations and microsatellite instability in complex atypical hyperplasia, a precursor lesion to uterine endometrioid carcinoma. Cancer Res 1998; 58: Maxwell G, Risinger J, Gumbs C et al. Mutation of the PTEN tumor supressor gene in endometrial hyperplasias. Cancer Res 1998; 58: Mutter GL, Lin MC, Fitzgerald JT et al. Altered PTEN expression as a diagnostic marker for the earliest endometrial precancers. J Natl Cancer Inst 2000; 92: Duggan BD, Felix JC, Muderspach LI, Tsao J-L, Shibata DK. Early mutational activation of the c-ki-ras oncogene in endometrial carcinoma. Cancer Res 1994; 54: Sasaki H, Nishii H, Takahashi H et al. Mutation of the Ki-ras protooncogene in human endometrial hyperplasia and carcinoma. Cancer Res 1993; 53: Mutter GL, Wada H, Faquin W, Enomoto T. K-ras mutations appear in the premalignant phase of both microsatellite stable and unstable endometrial carcinogenesis. Mol Pathol 1999; 52: Esteller M, Catasus L, Matias-Guiu X et al. hmlh1 Promoter Hypermethylation Is an Early Event in Human Endometrial Tumorigenesis. Am J Pathol 1999; 155(5): Mutter GL, Baak JPA, Crum CP, Richart RM, Ferenczy A, Faquin WC. Endometrial precancer diagnosis by histopathology, clonal analysis, and computerized morphometry. J Pathol 2000; 190: Dunton C, Baak J, Palazzo J, van Diest P, McHugh M, Widra E. Use of computerized morphometric analyses of endometrial hyperplasias in the prediction of coexistent cancer. Am J Obstet Gynecol 1996; 174: Hecht JL, Ince TA, Baak JP, Baker HE, Ogden MW, Mutter GL. Prediction of endometrial carcinoma by subjective endometrial intraepithelial neoplasia diagnosis. Mod Pathol 2005; 18: Baak JPA, Nauta J, Wisse-Brekelmans E, Bezemer P. Architectural and nuclear morphometrical features together are more important prognosticators in endometrial hyperplasias than nuclear morphometrical features alone. J Pathol 1988; 154: Orbo A, Baak JP, Kleivan I et al. Computerised morphometrical analysis in endometrial hyperplasia for the prediction of cancer development. A long-term retrospective study from northern Norway. J Clin Pathol 2000; 53(9): Baak JP, Orbo A, van Diest PJ et al. Prospective multicenter evaluation of the morphometric D-score for prediction of the outcome of endometrial hyperplasias. Am J Surg Pathol 2001; 25(7): Mutter GL, Lin MC, Fitzgerald JT, Kum JB, Ziebold U, Eng C. Changes in endometrial PTEN expression throughout the human menstrual cycle. J Clin Endocrinol Metab 2000; 85: Stambolic V, Tsao MS, Macpherson D, Suzuki A, Chapman WB, Mak TW. High incidence of Page 33
34 breast and endometrial neoplasia resembling human Cowden syndrome in pten+/- mice. Cancer Res 2000; 60(13): Mutter GL, Kauderer J, Baak JPA, Alberts DA. Biopsy histomorphometry predicts uterine myoinvasion by endometrial carcinoma: A Gynecologic Oncology Group Study. Hum Pathol 2008; 39: Mutter GL. Endometrial Intraepithelial Neoplasia: A new standard for precancer diagnosis. Cont Ob Gyn 2001; 46: Mutter GL. Histopathology of genetically defined endometrial precancers. Int J Gynecol Pathol 2000; 19: Ambros RA, Sherman ME, Zahn CM, Bitterman P, Kurman RJ. Endometrial intraepithelial carcinoma: A distinctive lesion specifically associated with tumors displaying serous differentiation. Hum Pathol 1995; 26: Carlson JW, Mutter GL. Endometrial Intraepithelial Neoplasia Is Associated With Polyps And Frequently Has Metaplastic Change. Histopathology 2008; 53: Lin MC, Lomo L, Baak JPA et al. Squamous Morules Are Functionally Inert Elements of Premalignant Endometrial Neoplasia. Mod Path 2008; e-pub ahead of Press. 43. Wang S, Pudney J, Song J, Schwartz PE, Zheng W. Mechanisms involved in the evolution of progestin resistence in human endometrial hyperplasia - Precursor of endometrial cancer. Gynecol Oncol 2003; 88: Mutter GL, Nucci MR, Robboy SJ. Endometritis, metaplasias, and miscellaneous changes. In: Robboy SJ, Mutter GL, Prat J, Bentley RC, Russell P, Anderson MC, editors. Robboy's Pathology of the Female Reproductive Tract. New York, New York: Elsevier, 2009: Lin MC, Lomo L, Baak JPA et al. Squamous Morules Are Functionally Inert Elements of Premalignant Endometrial Neoplasia. Mod Path 2009; 22: Nucci M, Crum CP, Prasad C, Mutter GL. Mucinous endometrial epithelial proliferations: a morphologic spectrum of changes with diverse clinical significance. Mod Path 2000; 12: Page 34
35 Case Presentations Introduction: The last session of the course, is structured as a case-oriented presentation of 12 cases. The physically small size of many of the lesion makes it impossible to distribute copies of original glass histological sections to course participants. Images will be provided online at in the downloads section. We hope the electronic images will enable you to view higher quality images than can be reproduced in the usual syllabus. Case-oriented presentation includes classic examples of readily recognizable entities, and controversial cases that when presented within our Division they elicited conflicting opinions and heated discussions. Their very contentiousness makes them excellent examples of the problems we face routinely in endometrial pathology, and provide a solid ground to explore the practical options available to the practicing pathologist. In some cases, additional clinical data (outcome) or elaborative special studies will be presented. Other Resources: Interested participants are referred to the website which has online diagnostic tutorials, image archives, and geneticmorphologic concordance data. Page 35
36 Case 1 History: 46 year old woman with irregular cycles and bleeding. Microscopic: The endometrium is proliferative with architectural changes of unopposed estrogens. We prefer to call this lesion lacking a precancerous potential as benign endometrial hyperplasia or disordered proliferative, understanding that some pathologists might also prefer the term simple nonatypical hyperplasia. The tissue fragments are abundant and large. The gland diameter varies from tubular to cystic in a regularly irregular pattern. Gland area exceeds that of stroma focally, but the cytology in those areas is no different than the background. Tubal metaplasia is present, but metaplastic glands are randomly interspersed with non-metaplastic glands, rather than defining a compact geographic zone replaced by metaplastic glands. Vascular thrombi, which are always abnormal in the endometrium, are associated with breakdown, further altering gland relationships. Diagnosis: Benign endometrial hyperplasia, active type (Disordered proliferative endometrium, unopposed estrogen effect) Case 2 History: 51 year old woman with with bleeding. Endometrial curettage. Microscopic: Two patterns are present. One is areas of proliferative endometrium as typified by round, widely spaced proliferative glands. The other pattern, EIN, is present in geographic regions of variably sized and shaped glands arranged in a crowded fashion. The area of glands greatly exceeds that of stroma. Followup: A hysterectomy performed 3 months later showed the additional presence of an endometrial cancer. Case 3 History: 51 year old postmenopausal woman. EMC. Microscopic: Irregular gland density and scattered cysts are prominent under low magnification. Gland cytology is fairly uniform throughout, without mitoses. Crowded areas do not have a different cytology. The diffeential diagnosis includes endometrial polyp, but the stroma is not fibrous and blood vessels are not thickened. This patient is probably not postmenopausal, but rather experiencing abnormal and irregular menstrual cycles. Likely she had an anovulatory cycle which caused cyst formation, then very slow decline of estrogens which was not sufficiently rapid to produce shedding. The result is the architecture of an extrogen altered endometrium, lacking mitoses and fibrin thrombi. An estrogen induced fieldwide lesion with no circulating estrogen at the time of biopsy. Page 36
37 Diagnosis: Benign endometrial hyperplasia (exhausted type) Case 4 History: 49 year old woman with complex endometrial hyperplasia without atypia diagnosed elsewhere on this endometrial sampling. Microscopic: There is a clearly localizing lesion against a regular proliferative background. The focus of crowded glands is readily recognizable as an EIN because the gland area exceeds that of the stroms, and these glands have a cytology differing from the background. Diagnosis: EIN arising from a proliferative background. Followup: Patient got adenocarcinoma 2 years later. Case 5 History: 47 year old woman with a diagnosis of simple endometrial hyperplasia without atypia made on this biopsy elsewhere. Microscopic: This EIN lesion occupies almost the entire endometrium. It is evident because of rare overrun glands with a differing cytology, and tight packing of the neoplastic glands. Diagnosis: Endometrial Intraepithelial Neoplasia Followup: Patient had adenocarcinoma in hysterectomy 8 months later Case 6 History: 47 year old woman with irregular bleeding and a 9mm endometrial stripe on ultrasound. Microscopic: Discrete focus of crowded, cytologically altered glands which are subdiagnostic of EIN because size (1mm) and glandular crowding (VPS<50%) EIN criteria are not met. Page 37
38 These lesions are infrequently encountered, with only one of these subdiagnostic cases seen for every 4-5 bona fide EINs. There are two possible interpretations that the pathologist should consider. First is that this section is tangential to the lesion epicenter, and deeper levels may become diagnostic. Second is the possibility that this is a pre-ein ( latent EIN, or LEIN ) lesion, only a fraction of which will proceed to become diagnostic EIN over time. Further research is needed to elaborate the likelihood and natural history of the latter possibility. Microscopic examination discloses a background of small, inactive, tubular glands locally punctuated by a grouped cluster of glands with enlarged nuclei and tall epithelia. The perimeter is poorly formed, as affected glands radiate outward in a splaying fashion. The lesion epicenter has a gland area greater than stroma, but measures less than 1 mm in maximum dimension. Diagnosis: Inactive endometrium. Crowded focus of cytologically altered glands. See note. Note: This discrete lesion is subdiagnostic for EIN, and has an uncertain natural history. Followup evaluation (biopsy in 6 months) is recommended. Followup: Biopsy 2 months later showed an endometrial polyp and proliferative endometrium with breakdown. Case 7 History: 48 year old with menorrhagia and endometrial hyperplasia on prior biopsy. Microscopic: Squamous morules abound in this specimen, being distributed in almost all fragments at a high density. Expansile round squamous morules are in many areas associated with a peripheral garland of endometrial glands. Theses epithelial complexes, with their punched out centripetal lumens have a distinctive cribriform appearance. Not all areas contain morules, however, and quite crowded areas of glands with few or no morules are seen. The lesional extent is so great that the entire compartment is replaced, and no normal structures are available for comparison. When evaluating tissues, it is best to ignore the morules and concentrate on glands. Morules lack estrogen and progesterone receptors, are mitotically quiescent, and part of same clone as glands. They are terminally differentiated elements. Often the morule resides within the gland itself and the diagnosis of EIN or carcinoma rests with the microscopic pattern of the glands. If glands are found where there is any significant cribriform pattern, the diagnosis is carcinoma. Sometimes the morules are extensive, coalesce and bridge glands, giving rise to the appearance of: garlanding of glands about solid morule. There are differences of opinions, even among the authors of this workshop, as to whether this should be considered as a state of premalignancy or malignancy itself. Diagnosis: EIN with extensive squamous morular differentiation. Followup: After 6 months of Megace therapy, the glands, but not the morular cytology changed. After continued Megace therapy, all morules disappeared. Page 38
39 Case 8 History: Woman with irregular bleeding and an intrauterine filling defect on ultrasound. Microscopic: Microscopic examination shows large, closely packed glands with jagged saw-tooth luminal infoldings covering expanses with little visible stroma. The glandular epithelium has abundant pink cytoplasm and large round to oval nuclei with prominent nucleoli. Bordering these areas are glands separated by more abundant stroma and fewer redundant infoldings. Diagnosis Secretory endometrium, 26 Day. Case 09: History: 59 year old with bleeding since polypectomy 3 months ago. D&C. Microscopic: This lesion is composed of papillary fronds of mucinous epithelial cells unsupported by intervening fibrous stroma. Nuclei are round and large, but without significant mitotic activity or nucleoli. Polys have percolated through the lesional fragments. There is no necrosis. Although the nuclear alignment suggests single-cell layers, on closer inspection individual fronds are comprised of redundant or piled up epithelial layers several cells deep. There is no epithelial-stromal interface in the illustrated fragment to illustrate relationships with the remaining endometrium and myometrium. Diagnosis: Endometrial adenocarcinoma, well differentiated, with mucinious differentiation. Followup: Endometrial curettings six months later showed foci of well differentiated endometrial adenocarcinoma with tubal and mucinous differentiation. This was arising in a background of (EIN) atypical endometrial hyperplasia. Case 10 History: 62 year old woman with an endometrial polyp Microscopic: Low power examination discloses a polyp with large, thin walled cystic glands. Nearby are regions of closely packed glands with round nuclei that contrast with the bland atrophic cyst lining. The epithelium in these areas is abundant, forming redundant intraglandular folds and clefts. A few nests disclose a cribriform pattern (the differing views as to the amount of cribriform pattern that must be present before considering a specimen as carcinoma will be discussed). The diagnosis of EIN uses identical criteria regardless of setting, but the background for comparison in this case is a polyp, which is a disease of the stroma itself (monoclonal benign stromal neoplasm). The irregular architecture and varying of the polyp cytology can be confusing. Look for a discrete localizing lesion, and in the diagnosis make it clear it is within a polyp. This Page 39
40 might have clinical significance (may require sharp curette for complete removal). About 10% of EIN lesions are within polyps. Diagnosis: EIN arising within endometrial polyp Case 11 History: Menorrhagia in 54 year old. Endometrial biopsy. Microscopic: This lesion has very atypical glands with a papillary epithelium demonstrating some tubal features. These reside in a dense stroma in which occasional plasma cells indicate an inflammatory component. The possible polyp background, combined with endometritis, make it difficult to evaluate the significance of the rather low gland density, and altered cytology. I would go ahead and diagnose an EIN lesion because the VPS is focally low, and inflammatory cells are not seen within the glandular epithelium itself. Diagnosis: EIN with micropapillary differentiation arising in endometrial polyp. Case 12 History: 52 year old with perimenopausal bleeding. Irregular menses for 4 months. Large endocervical polyp on exam. Pipelle biopsy. Microscopic: This secretory endometrium is punctuated by zonal clusters of tubular proliferative glands. There are no plasma cells that might indicate an endometritis, nor are there stigmata of a polyp in the affected fragments. The secretory glands would be unremarkable if uniformly present rather than admixed. In contrast, the proliferative glands are a bit crowded together, have occasional cystically dilated lumens, and some branching. Diagnosis: Mixed secretory and proliferative endometrium with focal gland crowding. Recommend re-biopsy in 3-6 months. Page 40
The Benign Endometrial Hyperplasia Sequence
 Page 1 Slide 1 Introduction A mini lecture from www.endometrium endometrium.org The Benign Endometrial Hyperplasia Sequence This is Dr. George Mutter, I am a gynecologic pathologist at Harvard Medical
Page 1 Slide 1 Introduction A mini lecture from www.endometrium endometrium.org The Benign Endometrial Hyperplasia Sequence This is Dr. George Mutter, I am a gynecologic pathologist at Harvard Medical
Polyps. Hyperplasias. CAP 2011: Course AP104. The High Risk Benign Endometrium. Mutter and Nucci 1
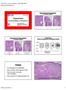 Course AP104 Endometrial Hyperplasia A morphologic Definition Hyperplasias Hormonal Effect or Precancer? George L. Mutter, MD Harvard Medical School and Brigham and Women s Hospital Boston, MA Endometrial
Course AP104 Endometrial Hyperplasia A morphologic Definition Hyperplasias Hormonal Effect or Precancer? George L. Mutter, MD Harvard Medical School and Brigham and Women s Hospital Boston, MA Endometrial
Recognizing the High Risk Benign Endometrial Biopsy. Faculty. Course AP104. George L. Mutter, MD, FCAP 1 Marisa R.
 Course AP104 Recognizing the High Risk Benign Endometrial Biopsy Faculty George L. Mutter, MD, FCAP 1 Marisa R. Nucci, MD, FCAP 2 1 Assoc. Prof. of Pathology, Harvard Medical School Division of Women s
Course AP104 Recognizing the High Risk Benign Endometrial Biopsy Faculty George L. Mutter, MD, FCAP 1 Marisa R. Nucci, MD, FCAP 2 1 Assoc. Prof. of Pathology, Harvard Medical School Division of Women s
EIN. (Endometrial Intraepithelial Neoplasia): Improved Criteria for diagnosing endometrial precancer. Stanley J. Robboy, MD, FCAP,
 EIN (Endometrial Intraepithelial Neoplasia): Improved Criteria for diagnosing endometrial precancer Stanley J. Robboy, MD, FCAP, FFPath FRCPI (Hon), FRCPath (UK, Hon) Professor of Pathology, Duke University
EIN (Endometrial Intraepithelial Neoplasia): Improved Criteria for diagnosing endometrial precancer Stanley J. Robboy, MD, FCAP, FFPath FRCPI (Hon), FRCPath (UK, Hon) Professor of Pathology, Duke University
Abnormal Uterine Bleeding FAQ Sheet
 Abnormal Uterine Bleeding FAQ Sheet What is abnormal uterine bleeding? Under normal circumstances, a woman's uterus sheds a limited amount of blood during each menstrual period. Bleeding that occurs between
Abnormal Uterine Bleeding FAQ Sheet What is abnormal uterine bleeding? Under normal circumstances, a woman's uterus sheds a limited amount of blood during each menstrual period. Bleeding that occurs between
Explanation of your PAP smear
 Explanation of your PAP smear Approximately 5-10% of PAP smears in the United States are judged to be abnormal. Too often, the woman who receives this news worries that she already has, or will develop,
Explanation of your PAP smear Approximately 5-10% of PAP smears in the United States are judged to be abnormal. Too often, the woman who receives this news worries that she already has, or will develop,
ATLAS OF HEAD AND NECK PATHOLOGY THYROID PAPILLARY CARCINOMA
 Papillary carcinoma is the most common of thyroid malignancies and occurs in all age groups but particularly in women under 45 years of age. There is a high rate of cervical metastatic disease and yet
Papillary carcinoma is the most common of thyroid malignancies and occurs in all age groups but particularly in women under 45 years of age. There is a high rate of cervical metastatic disease and yet
The menstrual cycle Hypophysis
 Normal endometrium Tumors of the uterine corpus by MB The endometrium comprises the zona functionalis zf (superficial two thirds) ) and the zona basalis zb (deep one third) The zf responds to hormonal
Normal endometrium Tumors of the uterine corpus by MB The endometrium comprises the zona functionalis zf (superficial two thirds) ) and the zona basalis zb (deep one third) The zf responds to hormonal
Basic Professional Training Program for Associate Medical Technologist
 Basic Professional Training Program for Associate Medical Technologist Basic Cytology Part 2 (Preparartion and normal morphology) Normal Morphology in Liquid based Gynecologic Cytology Speaker: Mr. Fung
Basic Professional Training Program for Associate Medical Technologist Basic Cytology Part 2 (Preparartion and normal morphology) Normal Morphology in Liquid based Gynecologic Cytology Speaker: Mr. Fung
Adenocarcinoma of the endometrium is the most
 Current Commentary Management of Endometrial Precancers Cornelia L. Trimble, MD, Michael Method, MD, MPH, Mario Leitao, MD, Karen Lu, MD, Olga Ioffe, MD, Moss Hampton, MD, Robert Higgins, MD, Richard Zaino,
Current Commentary Management of Endometrial Precancers Cornelia L. Trimble, MD, Michael Method, MD, MPH, Mario Leitao, MD, Karen Lu, MD, Olga Ioffe, MD, Moss Hampton, MD, Robert Higgins, MD, Richard Zaino,
Diagnostic Challenge. Department of Pathology,
 Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Nicole Kounalakis, MD
 Breast Disease: Diagnosis and Management Nicole Kounalakis, MD Assistant Professor of Surgery Goal of Breast Evaluation The goal of breast evaluation is to classify findings as: normal physiologic variations
Breast Disease: Diagnosis and Management Nicole Kounalakis, MD Assistant Professor of Surgery Goal of Breast Evaluation The goal of breast evaluation is to classify findings as: normal physiologic variations
Abnormal Uterine Bleeding
 Abnormal Uterine Bleeding WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Abnormal uterine bleeding is one of the most common reasons women see their doctors. It can occur at any age and has
Abnormal Uterine Bleeding WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Abnormal uterine bleeding is one of the most common reasons women see their doctors. It can occur at any age and has
Gynecology Abnormal Pelvic Anatomy and Physiology: Cervix. Cervix. Nabothian cysts. cervical polyps. leiomyomas. Cervical stenosis
 Gynecology Abnormal Pelvic Anatomy and Physiology: (Effective February 2007) pediatric, reproductive, and perimenopausal/postmenopausal (24-28 %) Cervix Nabothian cysts result from chronic cervicitis most
Gynecology Abnormal Pelvic Anatomy and Physiology: (Effective February 2007) pediatric, reproductive, and perimenopausal/postmenopausal (24-28 %) Cervix Nabothian cysts result from chronic cervicitis most
Why I don t recommend endometrial ablation
 Why I don t recommend endometrial ablation Endometrial ablation is a major operative procedure that: o Is ineffective because, according to all research, 40% will ultimately still need a hysterectomy,
Why I don t recommend endometrial ablation Endometrial ablation is a major operative procedure that: o Is ineffective because, according to all research, 40% will ultimately still need a hysterectomy,
Why would you need a hysterectomy?
 Why would you need a hysterectomy? Removal of the uterus is performed to prevent, alleviate, or treat pain, pressure, bleeding, or cancer. Each reason is described in detail in the following pages. Benign
Why would you need a hysterectomy? Removal of the uterus is performed to prevent, alleviate, or treat pain, pressure, bleeding, or cancer. Each reason is described in detail in the following pages. Benign
Something Old, Something New.
 Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Update on Abnormal Uterine Bleeding. Susan M. Sheridan, M.D., F.A.C.O.G Casper Obstetrical and Gynecological Associates Casper, WY
 Update on Abnormal Uterine Bleeding Susan M. Sheridan, M.D., F.A.C.O.G Casper Obstetrical and Gynecological Associates Casper, WY Defining Abnormal Uterine Bleeding (AUB) Normal menstrual cycle Frequency
Update on Abnormal Uterine Bleeding Susan M. Sheridan, M.D., F.A.C.O.G Casper Obstetrical and Gynecological Associates Casper, WY Defining Abnormal Uterine Bleeding (AUB) Normal menstrual cycle Frequency
The Menstrual Cycle. Model 1: Ovarian Cycle follicular cells
 The Menstrual Cycle REVIEW questions to complete before starting this POGIL activity 1. Gonads produce both gametes and sex steroid hormones. For the female, name the: A. gonads ovaries B. gametes oocyte/ovum/egg
The Menstrual Cycle REVIEW questions to complete before starting this POGIL activity 1. Gonads produce both gametes and sex steroid hormones. For the female, name the: A. gonads ovaries B. gametes oocyte/ovum/egg
Understanding CA 125 Levels A GUIDE FOR OVARIAN CANCER PATIENTS. foundationforwomenscancer.org
 Understanding CA 125 Levels A GUIDE FOR OVARIAN CANCER PATIENTS foundationforwomenscancer.org Contents Introduction...1 CA 125................................... 1 The CA 125 Test...2 The Use of the CA
Understanding CA 125 Levels A GUIDE FOR OVARIAN CANCER PATIENTS foundationforwomenscancer.org Contents Introduction...1 CA 125................................... 1 The CA 125 Test...2 The Use of the CA
LESSON 3.5 WORKBOOK. How do cancer cells evolve? Workbook Lesson 3.5
 LESSON 3.5 WORKBOOK How do cancer cells evolve? In this unit we have learned how normal cells can be transformed so that they stop behaving as part of a tissue community and become unresponsive to regulation.
LESSON 3.5 WORKBOOK How do cancer cells evolve? In this unit we have learned how normal cells can be transformed so that they stop behaving as part of a tissue community and become unresponsive to regulation.
Changes in Breast Cancer Reports After Second Opinion. Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain
 Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Introduction. Materials and Methods
 POSTPARTUM OVULATION By Konald A. Prem, M.D. Professor, Department of Obstetrics and Gynecology University of Minnesota Medical School Paper presented at the 1971 La Leche League Convention in Chicago
POSTPARTUM OVULATION By Konald A. Prem, M.D. Professor, Department of Obstetrics and Gynecology University of Minnesota Medical School Paper presented at the 1971 La Leche League Convention in Chicago
R-16: Chronic nonspecific cervisit
 R-16: Chronic nonspecific cervisit Ectoservikal squamous epithelium Endoservical columnar epithelium Dilated cystic endoservical glands lymphoplasmocytes R18:Squamous cell carcinoma insitu Neoplastic epithelium
R-16: Chronic nonspecific cervisit Ectoservikal squamous epithelium Endoservical columnar epithelium Dilated cystic endoservical glands lymphoplasmocytes R18:Squamous cell carcinoma insitu Neoplastic epithelium
Frequently Asked Questions About Ovarian Cancer
 Media Contact: Gerri Gomez Howard Cell: 303-748-3933 [email protected] Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Media Contact: Gerri Gomez Howard Cell: 303-748-3933 [email protected] Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Intraobserver and Interobserver Reproducibility of WHO and Gleason Histologic Grading Systems in Prostatic Adenocarcinomas
 International Urology and Nephrology 28 (1), pp. 73-77 (1996) Intraobserver and Interobserver Reproducibility of WHO and Gleason Histologic Grading Systems in Prostatic Adenocarcinomas $. O. OZDAMAR,*
International Urology and Nephrology 28 (1), pp. 73-77 (1996) Intraobserver and Interobserver Reproducibility of WHO and Gleason Histologic Grading Systems in Prostatic Adenocarcinomas $. O. OZDAMAR,*
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE
 Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
INFLAMMATION AND REACTIVE CHANGES IN CERVICAL EPITHELIUM
 INFLAMMATION AND REACTIVE CHANGES IN CERVICAL EPITHELIUM Inflammation is a response of a tissue to injury, often caused by invading microorganisms. The suffix which indicates inflammation is "-itis" (the
INFLAMMATION AND REACTIVE CHANGES IN CERVICAL EPITHELIUM Inflammation is a response of a tissue to injury, often caused by invading microorganisms. The suffix which indicates inflammation is "-itis" (the
From this site: http://www.energeticnutrition.com /vitalzym/fibroid_tumors.html Uterine Fibroid Tumors
 From this site: http://www.energeticnutrition.com /vitalzym/fibroid_tumors.html Uterine Fibroid Tumors Uterine Fibroid Tumors A woman s fibroisis condition usually associated with estrogen dominance. Uterine
From this site: http://www.energeticnutrition.com /vitalzym/fibroid_tumors.html Uterine Fibroid Tumors Uterine Fibroid Tumors A woman s fibroisis condition usually associated with estrogen dominance. Uterine
Cystic Neoplasms of the Pancreas: A multidisciplinary approach to the prevention and early detection of invasive pancreatic cancer.
 This lecture is drawn from the continuing medical education program Finding Hope: Prevention, Early Detection and Treatment of Pancreatic Cancer, Nov, 2011. Robert P. Jury, MD Cystic Neoplasms of the Pancreas:
This lecture is drawn from the continuing medical education program Finding Hope: Prevention, Early Detection and Treatment of Pancreatic Cancer, Nov, 2011. Robert P. Jury, MD Cystic Neoplasms of the Pancreas:
OVARIAN CYSTS. Types of Ovarian Cysts There are many types of ovarian cysts and these can be categorized into functional and nonfunctional
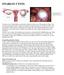 OVARIAN CYSTS Follicular Cyst Ovarian cysts are fluid-filled sacs that form within or on the ovary. The majority of these cysts are functional meaning they usually form during a normal menstrual cycle.
OVARIAN CYSTS Follicular Cyst Ovarian cysts are fluid-filled sacs that form within or on the ovary. The majority of these cysts are functional meaning they usually form during a normal menstrual cycle.
Cervical Cancer The Importance of Cervical Screening and Vaccination
 Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
PRIMARY SEROUS CARCINOMA OF PERITONEUM: A CASE REPORT
 PRIMARY SEROUS CARCINOMA OF PERITONEUM: A CASE REPORT Dott. Francesco Pontieri (*) U.O. di Anatomia Patologica P.O. di Rossano (CS) Dott. Gian Franco Zannoni Anatomia Patologica Facoltà di Medicina e Chirurgia
PRIMARY SEROUS CARCINOMA OF PERITONEUM: A CASE REPORT Dott. Francesco Pontieri (*) U.O. di Anatomia Patologica P.O. di Rossano (CS) Dott. Gian Franco Zannoni Anatomia Patologica Facoltà di Medicina e Chirurgia
Classificazioni citologiche: verso uno schema internazionale unificato?
 Cytology and molecular biology for thyroid nodules diagnos6c categories to clinical ac6ons From Classificazioni citologiche: verso uno schema internazionale unificato? A. Crescenzi Diagnostic categories
Cytology and molecular biology for thyroid nodules diagnos6c categories to clinical ac6ons From Classificazioni citologiche: verso uno schema internazionale unificato? A. Crescenzi Diagnostic categories
Outline. Workup for metastatic breast cancer. Metastatic breast cancer
 Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium
 Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Understanding Endometriosis - Information Pack
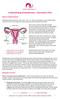 What is endometriosis? Endometriosis (pronounced en- doh mee tree oh sis) is the name given to the condition where cells like the ones in the lining of the womb (uterus) are found elsewhere in the body.
What is endometriosis? Endometriosis (pronounced en- doh mee tree oh sis) is the name given to the condition where cells like the ones in the lining of the womb (uterus) are found elsewhere in the body.
What is Cancer? Cancer is a genetic disease: Cancer typically involves a change in gene expression/function:
 Cancer is a genetic disease: Inherited cancer Sporadic cancer What is Cancer? Cancer typically involves a change in gene expression/function: Qualitative change Quantitative change Any cancer causing genetic
Cancer is a genetic disease: Inherited cancer Sporadic cancer What is Cancer? Cancer typically involves a change in gene expression/function: Qualitative change Quantitative change Any cancer causing genetic
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is a disorder that affects as many as 5 10% of women. PCOS has three key features: 1) high levels of hormones called androgens; 2) irregular menstrual
Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is a disorder that affects as many as 5 10% of women. PCOS has three key features: 1) high levels of hormones called androgens; 2) irregular menstrual
Common Cancers & Hereditary Syndromes
 Common Cancers & Hereditary Syndromes Elizabeth Hoodfar, MS, LCGC Regional Cancer Genetics Coordinator Kaiser Permanente Northern California Detect clinical characteristics of hereditary cancer syndromes.
Common Cancers & Hereditary Syndromes Elizabeth Hoodfar, MS, LCGC Regional Cancer Genetics Coordinator Kaiser Permanente Northern California Detect clinical characteristics of hereditary cancer syndromes.
Ovarian Cyst. Homoeopathy Clinic. Introduction. Types of Ovarian Cysts. Contents. Case Reports. 21 August 2002
 Case Reports 21 August 2002 Ovarian Cyst Homoeopathy Clinic Check Yourself If you have any of the following symptoms call your doctor. Sense of fullness or pressure or a dull ache in the abdomen Pain during
Case Reports 21 August 2002 Ovarian Cyst Homoeopathy Clinic Check Yourself If you have any of the following symptoms call your doctor. Sense of fullness or pressure or a dull ache in the abdomen Pain during
The society for lower genital tract disorders since 1964.
 The society for lower genital tract disorders since 1964. Updated Consensus Guidelines for Managing Abnormal Cervical Cancer Screening Tests and Cancer Precursors American Society for and Cervical Pathology
The society for lower genital tract disorders since 1964. Updated Consensus Guidelines for Managing Abnormal Cervical Cancer Screening Tests and Cancer Precursors American Society for and Cervical Pathology
Cytology of Lymph Nodes
 Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
Understanding your pathology report
 Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Fertility Preservation in Women with Cancer. Objectives. Patient #1 10/24/2011. The audience will understand: How cancer therapy affects fertility.
 Fertility Preservation in Women with Cancer Leslie R. DeMars Dartmouth-Hitchcock Medical Center Objectives The audience will understand: How cancer therapy affects fertility. Who should be considered for
Fertility Preservation in Women with Cancer Leslie R. DeMars Dartmouth-Hitchcock Medical Center Objectives The audience will understand: How cancer therapy affects fertility. Who should be considered for
Treating heavy menstrual bleeding caused by fibroids or polyps
 Treating heavy menstrual bleeding caused by fibroids or polyps With today s medical advances the outlook for successful treatment of fibroids and polyps has never been better. You don t have to live with
Treating heavy menstrual bleeding caused by fibroids or polyps With today s medical advances the outlook for successful treatment of fibroids and polyps has never been better. You don t have to live with
Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system.
 Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Ovarian Cysts Introduction Ovarian cysts are a very common female condition. An ovarian cyst is a fluid-filled sac on an ovary in the female reproductive system. Most women have ovarian cysts sometime
Understanding Your Risk of Ovarian Cancer
 Understanding Your Risk of Ovarian Cancer A WOMAN S GUIDE This brochure is made possible through partnership support from Project Hope for Ovarian Cancer Research and Education. Project HOPE FOR OVARIAN
Understanding Your Risk of Ovarian Cancer A WOMAN S GUIDE This brochure is made possible through partnership support from Project Hope for Ovarian Cancer Research and Education. Project HOPE FOR OVARIAN
BREAST CANCER RISK ASSESSMENT AND PRIMARY PREVENTION FOR HIGH RISK PATIENTS, RACHEL CATHERINE JANKOWITZ, MD 1
 FOR HIGH RISK PATIENTS, RACHEL CATHERINE JANKOWITZ, MD 1 Hello, my name is Rachel Jankowitz, I m an assistant professor of medicine in the Division of Hematology Oncology at the University of Pittsburgh
FOR HIGH RISK PATIENTS, RACHEL CATHERINE JANKOWITZ, MD 1 Hello, my name is Rachel Jankowitz, I m an assistant professor of medicine in the Division of Hematology Oncology at the University of Pittsburgh
Cancer of the Cervix
 Cancer of the Cervix WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 A woman's cervix (the opening of the uterus) is lined with cells. Cancer of the cervix occurs when those cells change,
Cancer of the Cervix WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 A woman's cervix (the opening of the uterus) is lined with cells. Cancer of the cervix occurs when those cells change,
Carcinosarcoma of the Ovary
 Carcinosarcoma of the Ovary A Rare Finding Presented By: Kathryn Kiely Anisa I. Kanbour School of Cytotechnology of the University of Pittsburgh Medical Center Pittsburgh, PA Patient History 55 year old
Carcinosarcoma of the Ovary A Rare Finding Presented By: Kathryn Kiely Anisa I. Kanbour School of Cytotechnology of the University of Pittsburgh Medical Center Pittsburgh, PA Patient History 55 year old
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS
 WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS This is a patient information booklet providing specific practical information about gall bladder polyps in brief. Its aim is to provide the patient
WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS This is a patient information booklet providing specific practical information about gall bladder polyps in brief. Its aim is to provide the patient
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Abnormal Uterine Bleeding. Howard Herrell, MD FACOG
 Abnormal Uterine Bleeding Howard Herrell, MD FACOG Disclosures I, Howard Herrell, DO NOT have a financial interest/arrangement or affiliation with one or more organizations that could be perceived as a
Abnormal Uterine Bleeding Howard Herrell, MD FACOG Disclosures I, Howard Herrell, DO NOT have a financial interest/arrangement or affiliation with one or more organizations that could be perceived as a
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency Pre-authorisation Evaluation of Medicines for Human Use London, 13 October 2005 Doc. Ref. EMEA/CHMP/021/97 Rev. 1 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE
European Medicines Agency Pre-authorisation Evaluation of Medicines for Human Use London, 13 October 2005 Doc. Ref. EMEA/CHMP/021/97 Rev. 1 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500. Endometriosis
 Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
Endometriosis WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 The lining of the uterus is called the endometrium. Sometimes, endometrial tissue grows elsewhere in the body. When this happens
Reproductive System & Development: Practice Questions #1
 Reproductive System & Development: Practice Questions #1 1. Which two glands in the diagram produce gametes? A. glands A and B B. glands B and E C. glands C and F D. glands E and F 2. Base your answer
Reproductive System & Development: Practice Questions #1 1. Which two glands in the diagram produce gametes? A. glands A and B B. glands B and E C. glands C and F D. glands E and F 2. Base your answer
Competency 1 Describe the role of epidemiology in public health
 The Northwest Center for Public Health Practice (NWCPHP) has developed competency-based epidemiology training materials for public health professionals in practice. Epidemiology is broadly accepted as
The Northwest Center for Public Health Practice (NWCPHP) has developed competency-based epidemiology training materials for public health professionals in practice. Epidemiology is broadly accepted as
Common Breast Complaints:
 : Palpable mass Abnormal mammogram with normal physical exam Vague thickening or nodularity Nipple Discharge Breast pain Breast infection or inflammation The physician s goal is to determine whether the
: Palpable mass Abnormal mammogram with normal physical exam Vague thickening or nodularity Nipple Discharge Breast pain Breast infection or inflammation The physician s goal is to determine whether the
Information Model Requirements of Post-Coordinated SNOMED CT Expressions for Structured Pathology Reports
 Information Model Requirements of Post-Coordinated SNOMED CT Expressions for Structured Pathology Reports W. Scott Campbell, Ph.D., MBA James R. Campbell, MD Acknowledgements Steven H. Hinrichs, MD Chairman
Information Model Requirements of Post-Coordinated SNOMED CT Expressions for Structured Pathology Reports W. Scott Campbell, Ph.D., MBA James R. Campbell, MD Acknowledgements Steven H. Hinrichs, MD Chairman
Practical Effusion Cytology
 Practical Effusion Cytology A Community Pathologist s Approach to Immunocytochemistry in Body Fluid Cytology Emily E. Volk, MD William Beaumont Hospital Troy, MI College of American Pathologists 2004.
Practical Effusion Cytology A Community Pathologist s Approach to Immunocytochemistry in Body Fluid Cytology Emily E. Volk, MD William Beaumont Hospital Troy, MI College of American Pathologists 2004.
Cytopathology Case Presentation #8
 Cytopathology Case Presentation #8 Emily E. Volk, MD William Beaumont Hospital, Troy, MI Jonathan H. Hughes, MD Laboratory Medicine Consultants, Las Vegas, Nevada Clinical History 44 year old woman presents
Cytopathology Case Presentation #8 Emily E. Volk, MD William Beaumont Hospital, Troy, MI Jonathan H. Hughes, MD Laboratory Medicine Consultants, Las Vegas, Nevada Clinical History 44 year old woman presents
All you need to know about Endometriosis. Nordica Fertility Centre, Lagos, Asaba, Abuja
 All you need to know about Endometriosis October, 2015 About The Author Nordica Lagos Fertility Centre is one of Nigeria's leading centres for world class Assisted Reproductive Services, with comfort centres
All you need to know about Endometriosis October, 2015 About The Author Nordica Lagos Fertility Centre is one of Nigeria's leading centres for world class Assisted Reproductive Services, with comfort centres
Benign Ovarian Masses
 Benign Ovarian Masses Anthony Hanbidge Learning Objectives Describe technique for assessment of ovarian masses Explain importance of transvaginal scan List the common benign masses Specify distinguishing
Benign Ovarian Masses Anthony Hanbidge Learning Objectives Describe technique for assessment of ovarian masses Explain importance of transvaginal scan List the common benign masses Specify distinguishing
SEMESTER VI 3 RD YEAR PATHOLOGY KIDNEY TUMORS
 SEMESTER VI 3 RD YEAR PATHOLOGY KIDNEY TUMORS LEARNING OBJECTIVES At the end of the lecture, students should be able to: Know the pathology of renal tumors. RENAL TUMORS RENAL PAPILLARY ADENOMA Common
SEMESTER VI 3 RD YEAR PATHOLOGY KIDNEY TUMORS LEARNING OBJECTIVES At the end of the lecture, students should be able to: Know the pathology of renal tumors. RENAL TUMORS RENAL PAPILLARY ADENOMA Common
Histopathology of Major Salivary Gland Neoplasms
 Histopathology of Major Salivary Gland Neoplasms Sam J. Cunningham, MD, PhD Faculty Advisor: Shawn D. Newlands, MD, PhD Faculty Advisor: David C. Teller, MD The University of Texas Medical Branch, Department
Histopathology of Major Salivary Gland Neoplasms Sam J. Cunningham, MD, PhD Faculty Advisor: Shawn D. Newlands, MD, PhD Faculty Advisor: David C. Teller, MD The University of Texas Medical Branch, Department
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
PSA Testing 101. Stanley H. Weiss, MD. Professor, UMDNJ-New Jersey Medical School. Director & PI, Essex County Cancer Coalition. weiss@umdnj.
 PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition [email protected] September 23, 2010 Screening: 3 tests for PCa A good screening
PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition [email protected] September 23, 2010 Screening: 3 tests for PCa A good screening
Adjuvant Therapy for Breast Cancer: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Adjuvant Therapy for Breast
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Adjuvant Therapy for Breast
Saturation Biopsy vs. 3D Spatial Biopsy vs. Free Hand Ultrasound biopsy for Targeted Prostate Cancer Therapies
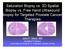 Saturation Biopsy vs. 3D Spatial Biopsy vs. Free Hand Ultrasound biopsy for Targeted Prostate Cancer Therapies John F. Ward, MD Assistant Professor University of Texas M. D. Anderson Cancer Center Ablation
Saturation Biopsy vs. 3D Spatial Biopsy vs. Free Hand Ultrasound biopsy for Targeted Prostate Cancer Therapies John F. Ward, MD Assistant Professor University of Texas M. D. Anderson Cancer Center Ablation
Today s Topics. Tumors of the Peritoneum in Women
 Today s Topics Tumors of the Peritoneum in Women Charles Zaloudek, M.D. Department of Pathology 505 Parnassus Ave., M563 University of California, San Francisco San Francisco, CA USA [email protected]
Today s Topics Tumors of the Peritoneum in Women Charles Zaloudek, M.D. Department of Pathology 505 Parnassus Ave., M563 University of California, San Francisco San Francisco, CA USA [email protected]
Abnormal Uterine Bleeding: Simple evaluation and management in premenopausal women
 Objectives Abnormal Uterine Bleeding: Simple evaluation and management in premenopausal women Provide a framework to evaluate abnormal uterine bleeding (AUB) Review medical and surgical management options
Objectives Abnormal Uterine Bleeding: Simple evaluation and management in premenopausal women Provide a framework to evaluate abnormal uterine bleeding (AUB) Review medical and surgical management options
Polycystic Ovarian Syndrome
 Polycystic Ovarian Syndrome What is Polycystic Ovarian Syndrome? Polycystic ovary syndrome (or PCOS) is a common condition affecting 3 to 5% of women of reproductive age. It is linked with hormonal imbalances,
Polycystic Ovarian Syndrome What is Polycystic Ovarian Syndrome? Polycystic ovary syndrome (or PCOS) is a common condition affecting 3 to 5% of women of reproductive age. It is linked with hormonal imbalances,
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD
 TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
MRI of the Uterus BENIGN. Jeffrey C. Weinreb, M.D. FACR [email protected] Yale University School of Medicine
 MRI of the Uterus BENIGN Jeffrey C. Weinreb, M.D. FACR [email protected] Yale University School of Medicine Normal Anatomy M Junctional JZ Zone EE Junctional Zone is the inner layer or the myometrium
MRI of the Uterus BENIGN Jeffrey C. Weinreb, M.D. FACR [email protected] Yale University School of Medicine Normal Anatomy M Junctional JZ Zone EE Junctional Zone is the inner layer or the myometrium
Guidelines for reporting histopathology of cervical carcinoma
 Guidelines for reporting histopathology of cervical carcinoma Naveena Singh, Consultant Pathologist Introduction Cancer management is multidisciplinary Histopathology report has a MAJOR impact on management
Guidelines for reporting histopathology of cervical carcinoma Naveena Singh, Consultant Pathologist Introduction Cancer management is multidisciplinary Histopathology report has a MAJOR impact on management
POSTMENOPAUSAL ASSESS AND WHAT TO DO
 POSTMENOPAUSAL OVARIAN CYSTS:HOW TO ASSESS AND WHAT TO DO Steven R. Goldstein, MD Professor of Obstetrics and Gynecology Director of Gynecologic Ultrasound Co-Director, Bone Densitometry New York University
POSTMENOPAUSAL OVARIAN CYSTS:HOW TO ASSESS AND WHAT TO DO Steven R. Goldstein, MD Professor of Obstetrics and Gynecology Director of Gynecologic Ultrasound Co-Director, Bone Densitometry New York University
CHAPTER 10 Uterine Synechiae
 CHAPTER 10 Uterine Synechiae Uterine synechiae are intrauterine adhesions. They may involve small focal areas of the endometrium (Figures 10.1a e), or they can be so extensive that they obliterate the
CHAPTER 10 Uterine Synechiae Uterine synechiae are intrauterine adhesions. They may involve small focal areas of the endometrium (Figures 10.1a e), or they can be so extensive that they obliterate the
Evaluation and Management of the Breast Mass. Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003
 Evaluation and Management of the Breast Mass Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003 Common Presentations of Breast Disease Breast Mass Abnormal
Evaluation and Management of the Breast Mass Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003 Common Presentations of Breast Disease Breast Mass Abnormal
Pap smears, cytology and CCHC lab work and follow up
 Pap smears, cytology and CCHC lab work and follow up What is a Pap Smear? A Pap smear (also known as the Pap test) is a medical procedure in which a sample of cells from a woman's cervix (the end of the
Pap smears, cytology and CCHC lab work and follow up What is a Pap Smear? A Pap smear (also known as the Pap test) is a medical procedure in which a sample of cells from a woman's cervix (the end of the
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
Ovarian Cancer: A Case Report
 Ovarian Cancer: A Case Report Abstract Ovarian cancer is a very common cancer among women. It is an extremely diverse disease requiring several treatment options. Occasionally ovarian cancer is diagnosed
Ovarian Cancer: A Case Report Abstract Ovarian cancer is a very common cancer among women. It is an extremely diverse disease requiring several treatment options. Occasionally ovarian cancer is diagnosed
HEALTH UPDATE. Polycystic Ovary Syndrome (PCOS)
 HEALTH UPDATE PO Box 800760 Charlottesville, VA 22908 Gynecology: (434) 924-2773 Polycystic Ovary Syndrome (PCOS) What is it? An endocrine (hormonal) disorder. Because there is such variability in how
HEALTH UPDATE PO Box 800760 Charlottesville, VA 22908 Gynecology: (434) 924-2773 Polycystic Ovary Syndrome (PCOS) What is it? An endocrine (hormonal) disorder. Because there is such variability in how
Breast Cancer Toolkit. Marion DePuit, MSN, Faith Community Nurse. Leslie Brown, BA, Community Advocate 9/2014. Understanding Breast Cancer
 GENERAL: Breast Cancer Toolkit Marion DePuit, MSN, Faith Community Nurse Leslie Brown, BA, Community Advocate 9/2014 Understanding Breast Cancer (Adapted from the American Cancer Society and Breast Cancer.org)
GENERAL: Breast Cancer Toolkit Marion DePuit, MSN, Faith Community Nurse Leslie Brown, BA, Community Advocate 9/2014 Understanding Breast Cancer (Adapted from the American Cancer Society and Breast Cancer.org)
worry When to Cervical Abnormalities CME Workshop What s the situation? What are the trends? By Dianne Miller, MD, FRCSC In this article:
 CME Workshop When to worry Cervical Abnormalities By Dianne Miller, MD, FRCSC What s the situation? Over 600,000 Papanicolaou s (Pap) smears were performed in British Columbia in 2000. Approximately 13,400
CME Workshop When to worry Cervical Abnormalities By Dianne Miller, MD, FRCSC What s the situation? Over 600,000 Papanicolaou s (Pap) smears were performed in British Columbia in 2000. Approximately 13,400
Applications of comprehensive clinical genomic analysis in solid tumors: obstacles and opportunities
 Applications of comprehensive clinical genomic analysis in solid tumors: obstacles and opportunities Vincent A. Miller, M.D. Foundation Medicine, Inc. AACR Annual Meeting 2012 Current Concepts session
Applications of comprehensive clinical genomic analysis in solid tumors: obstacles and opportunities Vincent A. Miller, M.D. Foundation Medicine, Inc. AACR Annual Meeting 2012 Current Concepts session
A Guide to Hysteroscopy. Patient Education
 A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
The Role of Genetic Testing in the Evaluation of Thyroid Nodules. Thyroid Cancer and FNA. Thyroid Cancer. Pure Follicular Cancers.
 Where does Molecular Analysis of FNA Specimens fit into the evaluation of thyroid nodules? The Role of Genetic Testing in the Evaluation of Thyroid Nodules Ultrasound TSH Risk factors Jill E. Langer, MD
Where does Molecular Analysis of FNA Specimens fit into the evaluation of thyroid nodules? The Role of Genetic Testing in the Evaluation of Thyroid Nodules Ultrasound TSH Risk factors Jill E. Langer, MD
HER2 Status: What is the Difference Between Breast and Gastric Cancer?
 Ask the Experts HER2 Status: What is the Difference Between Breast and Gastric Cancer? Bharat Jasani MBChB, PhD, FRCPath Marco Novelli MBChB, PhD, FRCPath Josef Rüschoff, MD Robert Y. Osamura, MD, FIAC
Ask the Experts HER2 Status: What is the Difference Between Breast and Gastric Cancer? Bharat Jasani MBChB, PhD, FRCPath Marco Novelli MBChB, PhD, FRCPath Josef Rüschoff, MD Robert Y. Osamura, MD, FIAC
Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy) for Paediatric Cancer Treatment
 Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy) for Paediatric Cancer Treatment Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy)
Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy) for Paediatric Cancer Treatment Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy)
Specialists In Reproductive Medicine & Surgery, P.A.
 Specialists In Reproductive Medicine & Surgery, P.A. Craig R. Sweet, M.D. www.dreamababy.com [email protected] Excellence, Experience & Ethics Endometriosis Awareness Week/Month Common Questions
Specialists In Reproductive Medicine & Surgery, P.A. Craig R. Sweet, M.D. www.dreamababy.com [email protected] Excellence, Experience & Ethics Endometriosis Awareness Week/Month Common Questions
From Menses to Menopause: How Hormones Can Affect Blood Glucose Levels. Christine Day, RN, MS, CNS-BC Lake Superior College
 From Menses to Menopause: How Hormones Can Affect Blood Glucose Levels Christine Day, RN, MS, CNS-BC Lake Superior College Overview Will review hormonal changes over the female lifespan Discuss the effects
From Menses to Menopause: How Hormones Can Affect Blood Glucose Levels Christine Day, RN, MS, CNS-BC Lake Superior College Overview Will review hormonal changes over the female lifespan Discuss the effects
Critical Appraisal of Article on Therapy
 Critical Appraisal of Article on Therapy What question did the study ask? Guide Are the results Valid 1. Was the assignment of patients to treatments randomized? And was the randomization list concealed?
Critical Appraisal of Article on Therapy What question did the study ask? Guide Are the results Valid 1. Was the assignment of patients to treatments randomized? And was the randomization list concealed?
Introduction: Tumor Swelling / new growth / mass. Two types of growth disorders: Non-Neoplastic. Secondary / adaptation due to other cause.
 Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
