History. Female age 64. Tumour right kidney on scan. Partial nephrectomy. Tumour 18mm diameter.
|
|
|
- Nathan Powers
- 9 years ago
- Views:
Transcription
1 FRCPath Part 2 Histopathology Examination Histology short cases Commentary. Case 1. History. Female age 64. Tumour right kidney on scan. Partial nephrectomy. Tumour 18mm diameter. Diagnosis: Angiomyolipoma of kidney. Average mark 3.12/5 This case was included as a good example of a relatively uncommon lesion, but nevertheless a lesion that candidates sitting the FRCPath Part 2 exam should be expected to diagnose with confidence. Pass marks were awarded to candidates who gave a diagnosis or renal angiomyolipoma and gave a competent basic description. Diagnoses of epithelioid angiomyolipoma were also accepted. Additional marks were awarded to candidates who gave a more complete answer and added value to their answers as follows. Extensive sampling should be undertaken in order to exclude other soft tissue and sarcomatoid tumours. Immunohistochemical staining might include smooth muscle markers and melanocytic markers (actin, desmin, HMB45, melan A). Additional commentary could have included useful clinical information such as confirming that this is a benign tumour cured by local excision (although vessel space invasion and regional lymph node invasion may occasionally be seen). Angiomyolipoma is part of the PECOMA group of tumours and has associations with the tuberose sclerosis complex. Angiomyolipomas are usually solitary but multiple tumours are seen in up to 20% of individuals and multiple lesions are more common in tuberose sclerosis. Candidates who made a diagnosis of benign vascular hamartoma or benign mesenchymal tumour were awarded a borderline fail. Any malignant diagnoses were awarded a clear fail mark. The majority of the candidates answered this question well, and most added some value with useful commentaries. Most candidates provided the correct diagnosis and mentioned appropriate immunohistochemical markers and the association with tuberose sclerosis. Few mentioned the need for extensive sampling or mentioned that these tumours are part of the PECOMA family of tumours.
2 Case 2. Female 39. Excision of tumour rectus sheath, anterior abdominal wall. Poorly defined tumour measuring 55mm in greatest dimension. Diagnosis: fibromatosis, desmoid type. Average mark 2.82/5 This case was selected as a good example of a locally aggressive lesion which candidates should have been able to recognise and diagnose with confidence. To pass this question candidates had to make a confident diagnosis of fibromatosis or give a differential diagnosis which favoured fibromatosis, as well as providing a competent description of the lesion. Additional marks were given for the following: Appropriate immunohistochemistry: positivity for smooth muscle actin and also B-catenin in 75% of cases. Negative staining for desmin and H-caldesmon. Clinical history, noting the age and gender of the patient, both of which are typical (ie: women of child bearing age). Also worth noting that desmoid tumours may arise in pregnancy and be oestrogen responsive. Borderline fails were awarded to candidates who provided lists of benign/ locally aggressive differential diagnoses including but not clearly favouring fibromatosis. Clear fails were awarded to candidates diagnosing sarcoma or other forms of malignancy with metastatic potential. Diagnoses of non-aggressive benign tumours or scar tissue were also awarded fails, as failing to observe the locally aggressive nature of the condition would result in inappropriate surgical management. This question was generally answered well by candidates but a significant proportion of answers lacked confidence, giving a differential diagnosis of spindle cell tumours without favouring fibromatosis as the diagnosis. Many candidates did not consider clinicopathological correlations. A few candidates favoured sarcoma as a diagnosis. Case 3. Male, 49. Dysphagia. Inflamed oesophagus with pseudomembranes. Also has tonsillitis. Oesophageal biopsies. Diagnosis: herpetic oseophagitis. Average mark: 3.18/5
3 This case was selected as a good example of the effects of viral infection, and although uncommonly encountered in oesophageal biopsies this is a process which any pathologist in general reporting practice might be expected to diagnose with confidence. Pass marks were awarded to candidates who gave a competent diagnosis of ulcerative oesophagitis of viral origin. Additional marks were given to: Candidates who correctly appreciated the nuclear features of herpetic oesophagitis and offered a confident diagnosis of herpetic oesophagitis rather than viral oesophagitis NOS Candidates who sought clinical correlation, recognising that the condition is more common in immunocompromised individuals. Candidates who suggested immunohistochemistry, viral culture or serology to confirm herpes simplex virus infection Borderline fails were awarded to candidates diagnosing ulcerative oesophagitis without mention of viral origin. An outright fail would have been awarded to any candidate who had made a malignant diagnosis. This question was well answered by the majority of candidates. A few candidates made a diagnosis of viral oesophagitis without suggesting herpes simplex virus. Case 4. Female 37. Multiple suspicious lung lesions, PET scan positive. Wedge excision of lesion left lung lower lobe. Diagnosis: features suggestive of Wegener s granulomatosis. Mean score 2.77/5 This was a moderately difficult case, testing the ability of candidates to safely assess a granulomatous process in the lung and think laterally to exclude infectious aetiology as well as considering systemic disease. Candidates should have realised the need to consider the likely diagnosis but also exclude other important possibilities, given the radically different treatments and the clinical consequences of failing to exclude infectious aetiology. Pass marks were awarded to candidates providing an adequate description of the lesion including necrosis, palisaded histiocytes, granulomas and obliterative vasculitis and who offered a differential diagnosis of necrotising granulomatous processes to include Wegener s granulomatosis, as well as possibly fungal infections, mycobacterial infections and rheumatoid nodule. Additional marks were given to candidates:-
4 Who suggested appropriate special stains to consider fungal and mycobacterial infections. Elastin stains to confirm vasculitis also gained additional marks. Clinical and radiological correlation (ANCA tests) Borderline fails were given to candidates who offered a single confident diagnosis of any specific form of necrotising granulomatous condition without offering a differential diagnosis or suggesting special stains or seeking clinical correlation. In the opinion of the examiners the histology suggests a variety of conditions and definite diagnosis of a single condition was not possible without additional investigation and seeking clinical correlation. Clear fails were given to candidates who offered malignant diagnoses. Many candidates answered this question well, correctly recognising the necrotising granulomatous inflammation with vasculitis and offering appropriate differential diagnosis and additional investigations. A small minority made inappropriate malignant diagnoses. A small number only considered infectious aetiology. Case 5. Female, 81. Ulcerated area, skin, left nipple. Biopsy left nipple. Adenoma of nipple. Average mark 2.69/5 This case was selected as a good example of a benign lesion which may mimic malignancy. The history and anatomical location should have been helpful. A pass mark was awarded to candidates favouring a diagnosis of nipple adenoma (or any appropriate alternative name for this condition), and providing a good description of a lesion with bland cytology and including a definite myoepithelial layer. Candidates able to offer a confident diagnosis of nipple adenoma and noting the likely incomplete nature of the excision and advising MDT discussion were awarded additional marks. Candidates who offered differential diagnoses which included but did not favour nipple adenoma were given borderline fail marks, as were candidates who diagnosed intraduct papilloma NOS or atypical ductal hyperplasia. Candidates who offered malignant diagnoses, or differential diagnoses favouring malignancy, were awarded clear fails. A confident diagnosis of a malignant lesion affecting the nipple would be likely to result in mastectomy. This question was generally well answered by candidates. The terminology used was variable. A minority of candidates offered clear malignant diagnosis.
5 Case 6 Female, 58. Hysterectomy for clinically enlarged uterus. Confluent nodular mass in myometrium, 140mm diameter. Diagnosis: endometrial stromal sarcoma. Average mark: 2.77/5 This case was selected as a good example of a malignant lesion that candidates presenting for the FRCPath part 2 exam might be expected to diagnose with confidence. Pass marks were given to candidates giving a competent description and favouring a diagnosis of endometrial stromal sarcoma. Candidates were not penalised for describing the lesion as low grade, although at the time of the exam low grade and high grade sub classification was not in recommended use. Additional marks were awarded to Candidates able to make a confident diagnosis of endometrial stromal sarcoma. Candidates choosing to use CD10 immunohistochemistry to confirm their diagnosis Candidates who indicated an understanding of the natural history of endometrial stromal sarcoma, noting the tumour s tendency to late abdominal recurrence but overall good prognosis despite recurrence, and the tumour s sensitivity to radiotherapy and endocrine therapy. Borderline fails were awarded to candidates offering broad differential diagnoses including but not favouring endometrial stromal sarcoma. Clear fails were awarded to candidates suggesting malignant diagnoses other than stromal sarcoma, or making definite benign diagnoses. This case was well answered by candidates, with most using appropriate terminology and many suggesting appropriate further investigations. Few candidates offered much in the way of clinicopathological correlation or prognostic information. A small minority of candidates did not include endometrial stromal sarcoma in their differential diagnosis. Case 7 Male, age 77. Right axillary lymphadenopathy. Lymph node biopsy. Diagnosis: B cell mature follicular lymphoma. Average mark: 2.74/5
6 This case was selected as a good example of a common form of lymphoma which a pathologist in general histological practice will encounter commonly, and would be expected to distinguish from benign conditions and refer appropriately. Candidates were awarded pass marks for a competent description of the histological features and a confident diagnosis of low grade non-hodgkin s lymphoma of follicular type or a differential diagnosis that clearly favoured follicular lymphoma. Additional marks were given to Candidates indicating appropriate immunohistochemical and cytogenetic/molecular investigations to confirm the diagnosis (e.g. - B cell markers [CD19, CD20, CD22, CD79a], CD10, BCL6, BCL2, proliferation markers, negativity for T cell markers, BCL2 gene rearrangements, t (14:18)(q32:21). Understanding of morphological grading systems bases on the number of centroblasts per high power field Understanding of prognostic factors (grade, proliferation fraction) Indicating the need for specialist referral and MDT discussion, in line with improving outlines guidance. Borderline fails were awarded to candidates offering lists of differential diagnoses which did not commit to or favour follicular lymphoma, or diagnosing lymphoma not otherwise specified, without suggesting further categorisation. Borderline fails were also awarded to candidates making confident diagnoses of other forms of lymphoma. Clear fails were given to candidates diagnosing or favouring benign reactive or granulomatous conditions, Castleman s disease or non-lymphomatous malignancy or metastatic disease. Most candidates answered this question well and suggested appropriate ancillary investigations and MDT referral. Many candidates attempted to grade the lesion, and candidates were not penalised for misgrading the lesion (this lymphoma had originally been reported as a grade 2 follicular lymphoma). A few candidates offered inappropriate diagnoses of reactive follicular hyperplasia, Hodgkin s Disease of other low grade non-hodgkin s lymphoma. Case 8 Male, 62. Exophytic growth, left scalp. Excised. Diagnosis: metastatic renal cell carcinoma. Average mark: 2.66/5 This case was set to test candidates ability to deal with cutaneous malignancy, and test the ability of candidates to consider appropriate differential diagnoses rather than jump to conclusions based on
7 H&E sections alone. This is a common diagnostic dilemma faced by all consultant histopathologists in routine practice. It is important in such cases to think laterally and to consider both cutaneous and metastatic malignancy, and suggest appropriate immunohistochemistry to resolve the differential diagnosis, using histological clues to guide further testing. Pass marks were awarded to candidates who gave a good description of a nested malignant lesion, making a confident diagnosis of malignancy and offering a sensible differential diagnosis but offering little in the way of added value or focussed additional investigations. Additional marks were given to candidates who offered a sensible reasoned differential diagnosis that might include metastatic renal cell carcinoma, non-small cell carcinoma of lung and malignant melanoma, and a directed economic panel of immunohistochemical markers to confirm the diagnosis. Candidates were also given credit for seeking additional clinical history or searching the laboratory computer system for previous primary tumour diagnoses. Borderline fails were awarded to candidates who made confident diagnoses of specific forms of malignancy without offering a differential diagnosis or suggesting a useful panel of immunohistochemical markers. Clear fails were awarded to candidates making a confident benign diagnosis. This question was answered variably by candidates. Many candidates offered appropriate differential diagnoses and ancillary investigations. A significant minority of candidates were more specific than the histology allowed, and offered confident diagnoses of primary or metastatic melanoma, squamous cell carcinoma, atypical fibroxanthoma, spindle cell tumours and adnexal skin tumours. Some candidates were confident that they had seen an in situ melanomatous component. Occasional candidates derived benign diagnoses, including histiocytic lesions. Case 9. Female, 80. Vomiting and gastric stasis. Abnormal gastric mucosa at endoscopy. Gastroscopic biopsies. Diffuse type gastric adenocarcinoma. Average mark 2.88/5 This case was chosen as a straightforward example of diffuse type gastric adenocarcinoma, and was designed to test the ability of candidates to provide a confident diagnosis of malignancy in mucosal biopsies. Pass marks were awarded to candidates giving a good description of the biopsies and noting the presence of a neoplastic infiltrate including signet ring cells and occasional acinar forms. Candidates were expected to give a confident diagnosis of malignancy of likely epithelial origin. Candidates who included lymphoma in their differential diagnosis were not marked down, provided that they
8 indicated an intention to perform appropriate immunohistochemical investigations to prove or exclude this diagnosis. Additional marks were given to candidates making a confident diagnosis of diffuse type gastric adenocarcinoma and suggesting appropriate economic use of immunohistochemistry and/or mucin stains to confirm the diagnosis. Candidates who equivocated as to a malignant diagnosis or who preferred a diagnosis of metastatic malignancy were given borderline fails. Candidates who gave benign diagnoses (including gastric xanthelasma) or arrived at confident diagnoses of lymphoma without use of immunohistochemistry were given clear fails. Most candidates approached this case sensibly and logically, giving good descriptions and appropriate confident diagnoses or differential diagnoses with focussed and appropriate immunohistochemistry. Some candidates favoured metastatic disease. A few candidates noted surface epithelial dysplasia and intestinal metaplasia, neither of which was present in the biopsies. A very few candidates made inappropriate benign diagnoses including gastric atrophy, xanthelasma and lymphocytic gastritis. Case 10 Male, 55. Skin biopsy lesion below left ear. Diagnosis: monomorphic basal cell adenoma of salivary gland origin. Average mark 2.16/5 This case was designed to test the ability of candidates to think laterally, consider the clinical history and examine the whole section for clues. The case derived from primary care and a General Practitioner with an interest in minor surgery took the biopsy and submitted it to a District General Pathology laboratory where it was reported by a general pathologist. This is a scenario which any pathologist in general pathology practice in a District General Hospital might be expected to encounter on occasion. All sections included normal parotid gland (the presence of salivary gland in all slides was carefully checked when the slide sets were assembled). Just under one third of candidates correctly associated the anatomical information (just below left ear) and the presence of normal salivary gland tissue and then interpreted this as a benign salivary gland neoplasm. A few of these candidates gave excellent answers, correctly diagnosing basal cell adenoma. Others gave diagnoses of benign salivary neoplasms, but favoured other types of salivary neoplasia.
9 The majority of candidates did not notice the salivary gland tissue hence offered diagnoses of benign skin adnexal tumours or vascular tumours. A minority offered malignant diagnoses, failing to note the bland nature of the neoplasm. This question was marked in a very lenient manner. Credit was given to candidates who correctly interpreted the lesion as benign. Borderline fails were awarded to candidates making diagnoses of benign non-salivary neoplasms and providing otherwise good descriptions. Clear fails were awarded to candidates making a definite diagnosis of malignancy. Case 11 Female, age 44 Itchy rash extensor surfaces. Incisional biopsy skin left arm. Diagnosis: dermatitis herpetiformis Average mark: 3.13/5 This case was selected as a good example of a blistering skin lesion with characteristic history and histological features which should have helped candidates make a diagnosis. Pass marks were awarded to candidates who gave a good description of the key histological features and identified the main abnormality as papillary dermal microabscesses. Dermatitis herpetiformis should have at least been been mentioned in the differential diagnosis. Additional marks were awarded to Candidates favouring a diagnosis of dermatitis herpetiformis. Candidates describing appropriate immunofluorescent studies Description of the likely immunofluorescent staining pattern (granular IgA deposition in dermal papillae) Appreciation of the typical histological features of DH and arriving at a confident diagnosis of DH Appreciation of the clinical history of an itchy rash affecting extensor surfaces and correlation with the histology Candidates acknowledging the clinical association with gluten hypersensitivity/ coeliac disease Borderline fails were given to candidates who described some of the cogent histological features but failed to observe the neutrophilic infiltrate in the papillary dermis. A clear fail would have been given to any candidate who failed to note that this was an inflammatory dermatosis or gave a malignant diagnosis.
10 This question was answered very well by the majority of candidates. All candidates recognised this as a dermatosis. Most candidates correctly diagnosed this as dermatitis herpetiformis and added value by suggesting immunofluorescent studies and seeking a clinical history of coeliac disease. A few candidates preferred a diagnosis of pemphigoid and some described vasculitis. Case 12. Male, age 57. Haematuria. At cystoscopy, nodule bladder wall. Bladder wall biopsies. Average mark 1.99/5. This case was designed to assess the candidates ability to recognise an uncommon but well recognised non-neoplastic condition, and assess the whole section for clues. Pass marks were given to candidates giving an adequate description and noting the presence of an amorphous eosinophilic deposit in the bladder wall. Candidates had to recognise the presence of characteristic amyloid material or give a list of differential diagnoses including and favouring amyloid. Additional marks were given to candidates:- Giving a more complete description, noting the vascular reaction superficial to the amyloid (and correlating this with haematuria) and suggesting Congo red stain or other tinctorial stains to confirm amyloid. Showing knowledge of the biology of amyloidosis and understanding that this is likely to be AL type amyloid, secondary amyloidosis being much less common in the bladder Understanding the need to refer to the National Amyloidosis Centre Candidates giving a reasonable description and a differential diagnosis including but not favouring amyloidosis were given a borderline fail. Candidates not mentioning amyloidosis at all or giving a malignant diagnosis were given clear fails. Many candidates found this case difficult. However, over one third of candidates correctly observed the amyloid material and suggested suitable additional investigations. Few candidates indicated any additional understanding of the nature of amyloidosis of the bladder. The majority of candidates chose inappropriate malignant diagnoses. This case demonstrates the need for candidates to appreciate the clinical history and look at all of the material on the slide. The clinical history indicated that this was a nodule in the bladder wall rather than a surface lesion. The biopsies were deep and substantial. Urologists rarely take deep biopsies for superficial lesions such as carcinoma in situ (a common answer provided by candidates). A small but significant number of candidates did correctly observe the characteristic amyloid
11 material. To pass this question candidates had to assess all of the material on the slide and think laterally to consider basic pathological processes. Case 13. Female, age 91. Lesion left breast. Excised. Diagnosis: grade 1 secretory carcinoma of breast. Average mark: 2.56/5 This case was included in order to assess the ability of candidates to recognise special types of breast cancer and assess and record minimum dataset items. There was considerable opportunity for candidates to add value in their answers. Pass marks were given to candidates correctly diagnosing invasive breast carcinoma but offering little else in the way of special type or dataset items. Additional marks were given to :- Candidates who provided most dataset items (grade, size, absence of vessel space invasion. Candidates who recognised that this was a special type but failed to recognise that this was a secretory carcinoma were given some additional marks. Candidates who suggested the possibility that this was carcinoma metastatic to the breast and suggested appropriate immunohistochemistry to consider this possibility. Confident comment on the absence of DCIS Candidatesuggesting appropriate ancillary tests (ER, PgR, HER2). Top marks would have been given to candidates recognising all of the above and giving a description of the features of a secretory carcinoma and a confident diagnosis of secretory carcinoma. Candidates who made a confident diagnosis of metastatic disease without mentioning the need for immunohistochemistry were given a borderline fail. Candidates failing to recognise a malignant lesion were given a clear fail. Overall the majority of candidates passed this question but few managed to gain additional marks by including data set items or recognising that this was a special type of breast cancer. Dataset items were often incomplete. A common error was to identify ductal carcinoma in situ: although no candidates failed because of this error it did limit their ability to gain additional marks.
12 Case 14 Female, 60. Vaginal discharge, pyometra. Endometrial curettage. Diagnosis: granulomatous endometritis. Average mark: 2.55/5 This case was set to assess the ability of candidates to assess granulomatous inflammation in a slightly unusual clinical setting and consider the clinical significance of this pattern of inflammation. In this particular instance culture had revealed that the patient had M.Bovis infection. Candidates were given a pass mark for describing the presence of granulomatous endometritis in inactive endometrium and indicating that tuberculosis has to be excluded. Candidates also had to confidently exclude the possibility of malignant disease. Additional marks were given to candidates:- Who demonstrated specific understanding of the naturel history of tuberculous endometritis Who suggested special stains for acid alcohol fast bacilli but understood that these might be negative hence indicated the need to exclude TB by culture or PCR techniques Candidates who appreciated the need for exhaustive investigations to exclude TB Borderline fail marks were given to candidates who described granulomatous endometritis but did not appreciate the need to exclude tuberculosis. Borderline fails were also awarded to candidates diagnosing any form of endometrial hyperplasia. Clear fails were awarded to candidates failing to note the presence of granulomatous inflammation and/or making a diagnosis of malignancy. The majority of candidates correctly recognised granulomatous inflammation and suggested appropriate investigations to consider tuberculosis. Only a few candidates managed to add significant value to their answers by appreciating the need for other investigations to exclude TB, given that ZN stain can often be negative in this situation. A small number of candidates over-interpreted the fragmented and inflamed endometrial epithelium as hyperplastic or even malignant.
13 Case 15 Female, 58. Lytic lesions in skull. Curettage of lytic lesion. Diagnosis: metastatic follicular carcinoma of thyroid gland. Average mark: 2.56/5 This case was designed to assess the candidates ability to think laterally and recognise metastatic disease in an unusual location. Pass marks were given to candidates who correctly diagnosed metastatic follicular carcinoma of thyroid, giving a competent description but with no added value. Additional marks were given to candidates giving a more complete description and suggesting appropriate immunohistochemistry to confirm (TTF1, thyroglobulin) although arguably immunohistochemical staining would not have been necessary given the characteristic histological features. Borderline fails were given to candidates describing thyroid carcinoma NOS, or finding features of papillary carcinoma. Borderline fails were also given to candidates giving differential diagnoses of metastatic adenocarcinoma, but including thyroid in the differential. Clear fails were given to candidates diagnosing benign lesions, failing to recognise characteristic thyroid morphology or diagnosing non-thyroid malignancy. This question was well answered by many candidates, but approximately one third of candidates had either clear or borderline fails, usually because they did not recognise thyroid carcinoma or favour the diagnosis in a differential. A few candidates found features of papillary carcinoma of thyroid. Occasional candidates diagnosed primary bone or soft tissue malignancy. Some candidates did not appreciate the history (female, lytic lesion) and diagnosed metastatic prostatic carcinoma. Case 16 Male, 25. Lesion segment VI of liver. Resected. Diagnosis: fibrolamellar hepatocellular carcinoma. Average mark: 2.48/5 This case aimed to identify candidates confident in diagnosing primary hepatic malignancy and able to identify an important and well recognised hepatocellular carcinoma variant.
14 Pass marks were awarded to candidates giving a good description of the lesion and offering a differential diagnosis including fibrolamellar hepatocellular carcinoma and perhaps wishing to seek further opinion, given that this is a relatively uncommon neoplasm. Additional marks were awarded for the following:- Confident diagnosis of fibrolamellar HCC Noting relatively normal surrounding liver tissue without evidence of cirrhosis or other chronic liver disease Awareness of different epidemiology of fibrolamellar HCC (younger patients, not associated with antecedent liver disease) Awareness of better prognosis than classical hepatocellular carcinoma Awareness of potential for resection of this tumour Indicating immunohistochemical staining pattern and potential differences between classical HCC and fibrolamellar HCC Borderline fails were awarded to candidates diagnosis classical HCC without considering fibrolamellar HCC. Clear fails were given to candidates who made benign diagnoses or diagnosed cholangiocarcinoma or metastatic malignancy. Candidates approached this question variably. More than half of the candidates achieved passes and some added considerable value to their answers by considering the epidemiology of the tumour and making helpful clinical correlations. Candidates who failed the question seemed to be unaware of the entity or the helpful clinical history (age of patient) and background normal liver. A proportion of candidates gave a differential diagnosis of conventional HCC and hepatic adenoma. Case 17 Male 64. Smoker. Lesion left lung upper lobe on chest x-ray. Segmental excision, left lung upper lobe. Diagnosis: typical carcinoid tumour. Average mark 2.34/5 This case was chosen as a good example of a relatively common neoplasm which might be seen as a biopsy in any hospital. Pass marks were awarded to candidates giving a good description of a circumscribed tumour with favourable histological features and favouring a diagnosis of typical carcinoid tumour/ well differentiated neuroendocrine carcinoma or low grade neuroendocrine tumour.
15 Additional marks were given to candidates who:- Suggested appropriate immunohistochemical stains to confirm the diagnosis Made a confident diagnosis of typical carcinoid tumour Attempted to stage the tumour Commented on favourable prognosis. Borderline fails were given to candidates who did not favour the diagnosis of typical carcinoid tumour in their differential diagnoses, or offered a confident diagnosis of atypical carcinoid tumour. Clear fails were given to candidates giving any other malignant diagnosis, any other benign diagnoses or favouring high grade lesions. Candidates approached this case variably. Just under half of the candidates passed the question, and those who did pass the question generally managed to add value to their answers by describing appropriate immunohistochemistry or offering useful clinical information. Many candidates appeared confused by the terminology of neuroendocrine tumours, and gave good descriptions of a typical carcinoid tumour and then a confident diagnosis of an atypical carcinoid tumour. A few candidates called this a benign carcinoid tumour. Occasional candidates thought that this was a metastatic tumour, and some misdiagnosed the lesion as a large cell carcinoma or a small cell carcinoma. Only a few candidates mentioned staging. Case 18 Female, 2 months. Swelling lower mandible, blue discolouration under submucosa. Curettage anterior mandible. Diagnosis: Langerhans cell histiocytosis. Average mark: 2.58/5 This case was set to identify candidates able to make a confident diagnosis of a relatively uncommon but characteristic histiocytic condition. Although this case arose in an infant, the condition can be seen in older age groups. To gain a pass mark a candidate had to give a competent description of a cellular lesion including histiocytes, Langerhans cells and eosinophils and lacking any atypia or mitotic activity. Candidates had to list Langerhans cell histiocytosis as part of their differential and suggest an immunohistochemical panel including S100 to confirm the diagnosis. Additional marks were given to candidates making a confident diagnosis of Langerhan s cell histiocytosis and confirming the need to use an immunohistochemical panel including S100 and
16 CD1a. Mention of Braf mutations and staging investigations to look for more widespread disease also gained additional marks. Borderline fails were given to candidates describing a histiocytic proliferation but not mentioning Langerhans cell histiocytosis. Clear fails were given to candidates offering a clear diagnosis of malignancy (including lymphoma) or diagnosing a granulomatous condition. Most candidates answered this question very well, and most added value to their answers, with appropriate immunohistochemical investigation and additional clinical information. A small subset of candidates failed to recognise the histiocytic nature of the lesion and diagnosed giant cell lesions of bone or small blue cell tumours. Case 19. Male, 67. Clinically naevus anterior abdominal wall, recent change in appearance. Excised. Diagnosis: superficial spreading melanoma. Average mark: 2.52/5 This case was chosen to assess the ability of candidates to interpret melanocytic lesions and make confident diagnosis of melanocytic malignancy. To gain a pass mark candidates had to identify an atypical compound melanocytic lesion and favour a differential diagnosis of melanoma or superficial spreading melanoma. Additional marks were given to candidates able to make a confident diagnosis of malignant melanoma and describe key features including lesional asymmetry, Pagetoid invasion, cytological atypia and incipient ulceration. Additional marks were also given to candidates offering correct and useful staging information in terms of Breslow depth and mitotic rate. Indicating the need for appropriate MDT discussion also gained marks. Correct interpretation of vertical growth phase was also helpful. Borderline fails were given to candidates who recognised a melanocytic lesion but were undecided as to benign or malignant interpretation. Clear fails were awarded to candidates not recognising this as a melanocytic lesion or calling the lesion a benign naevus or dysplastic naevus outright. Well over half of the candidates recognised this lesion as a melanoma and many added considerable value to their answers. Some candidates were indecisive and had difficulty in recognising and interpreting the dermal component, describing the growth phase incorrectly, thereby losing marks. A few candidates gave confident and clinically misleading benign diagnoses.
17 Case 20. Male 59. Nasal swelling, destructive lesion involving sphenoid sinus. Lesion biopsied. Diagnosis: olfactory neuroblastoma. Average mark 2.53/5 This case was chosen to assess candidates knowledge of ENT lesions and recognise characteristic histological patterns. To gain a pass mark candidates had to give a competent description of the lesion and at least give a differential diagnosis including and favouring olfactory neuroblastoma. Additional marks were given to Candidates able to make a confident diagnosis of olfactory neuroblastoma Candidates suggesting appropriate immunohistochemical confirmation (CD56, NSE, chromogranin positive, cytokeratin, LCA, TTF1, CD99 negative and S100 positive in sustentacular cells) Candidates indicating the need for clinical correlation: awareness that prognosis dependent upon stage and grade Candidates aware of treatment options (surgery and radiotherapy) Candidates aware of grading systems Borderline fails were given to candidates offering a definite diagnosis of other types of small blue cell neoplasms or favouring a differential diagnosis of other types of small blue cell neoplasm. Clear fails were given to candidates offering benign diagnoses or confident diagnoses of other forms of malignancy (lymphoma, melanoma). This case was well-answered by the majority of candidates and only about one quarter of candidates failed. Most candidates recognised the entity and gave a good plan for investigating and confirming the diagnosis and excluding alternative possibilities. A few candidates did not consider the possibility of olfactory neuroblastoma in their differential or gave very restricted differentials and poor plans for investigating the lesion. May 2014
Changes in Breast Cancer Reports After Second Opinion. Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain
 Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
FRCPath Part 2 Histopathology Short Cases, autumn 2014
 FRCPath Part 2 Histopathology Short Cases, autumn 2014 Commentary Case 1 Female age 52: palpable lesion, left breast Breast, fat necrosis. Average: 2.6/5 This case was chosen as a good example of fat necrosis
FRCPath Part 2 Histopathology Short Cases, autumn 2014 Commentary Case 1 Female age 52: palpable lesion, left breast Breast, fat necrosis. Average: 2.6/5 This case was chosen as a good example of fat necrosis
Immunohistochemical differentiation of metastatic tumours
 Immunohistochemical differentiation of metastatic tumours Dr Abi Wheal ST1. TERA 3/2/14 Key points from a review article written by Daisuke Nonaka Intro Metastatic disease is the initial presentation in
Immunohistochemical differentiation of metastatic tumours Dr Abi Wheal ST1. TERA 3/2/14 Key points from a review article written by Daisuke Nonaka Intro Metastatic disease is the initial presentation in
The Diagnosis of Cancer in the Pathology Laboratory
 The Diagnosis of Cancer in the Pathology Laboratory Dr Edward Sheffield Christmas Select 74 Meeting, Queen s Hotel Cheltenham, 3 rd December 2014 Agenda Overview of the pathology of cancer How specimens
The Diagnosis of Cancer in the Pathology Laboratory Dr Edward Sheffield Christmas Select 74 Meeting, Queen s Hotel Cheltenham, 3 rd December 2014 Agenda Overview of the pathology of cancer How specimens
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Tumour Markers. What are Tumour Markers? How Are Tumour Markers Used?
 Dr. Anthony C.H. YING What are? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer cells or
Dr. Anthony C.H. YING What are? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer cells or
Immunohistochemistry of soft tissue tumors
 Immunohistochemistry of soft tissue tumors Immunohistochemistry Major advances : antigen retrieval techniques (HIER) sensitive detection systems numerous antibodies of good quality Standardization : automated
Immunohistochemistry of soft tissue tumors Immunohistochemistry Major advances : antigen retrieval techniques (HIER) sensitive detection systems numerous antibodies of good quality Standardization : automated
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Breast Cancer: from bedside and grossing room to diagnoses and beyond. Adriana Corben, M.D.
 Breast Cancer: from bedside and grossing room to diagnoses and beyond Adriana Corben, M.D. About breast anatomy Breasts are special organs that develop in women during puberty when female hormones are
Breast Cancer: from bedside and grossing room to diagnoses and beyond Adriana Corben, M.D. About breast anatomy Breasts are special organs that develop in women during puberty when female hormones are
MODERN IMMUNOHISTOCHEMISTRY
 MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
Frozen Section Diagnosis
 Frozen Section Diagnosis Dr Catherine M Corbishley Honorary Consultant Histopathologist St George s Healthcare NHS Trust and lead examiner final FRCPath Practical 2008-2011 Frozen Section Diagnosis The
Frozen Section Diagnosis Dr Catherine M Corbishley Honorary Consultant Histopathologist St George s Healthcare NHS Trust and lead examiner final FRCPath Practical 2008-2011 Frozen Section Diagnosis The
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Outline. Workup for metastatic breast cancer. Metastatic breast cancer
 Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
Index. F Factor VIII-related antigen, see VWF FactorXIIIa, for dermatofibroma, 272-275 5-HT, see Serotonin
 A Acantholytic squamous cell carcinoma vs epithelioid angiosarcoma, 56-57 Acinic cell carcinoma of pancreas, 76-77 vs ductal adenocarcinoma, 74-75 vs islet cell tumor, 78-81 Adenomatoid tumor vs hemangioma,
A Acantholytic squamous cell carcinoma vs epithelioid angiosarcoma, 56-57 Acinic cell carcinoma of pancreas, 76-77 vs ductal adenocarcinoma, 74-75 vs islet cell tumor, 78-81 Adenomatoid tumor vs hemangioma,
The evolving pathology of solitary fibrous tumours. Luciane Dreher Irion MREH / CMFT / NSOPS
 The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD
 TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
CHAPTER 2. Neoplasms (C00-D49) March 2014. 2014 MVP Health Care, Inc.
 Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Pediatric Oncology for Otolaryngologists
 Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
Pathology of lung cancer
 Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
YOUR LUNG CANCER PATHOLOGY REPORT
 UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
HKCPath Anatomical Pathology Peer Review and Scores : PDF version for download
 AP2003R1 http://hkcpath.org. Correspondence: [email protected] 1of 10 07/08/2003 HKCPath Anatomical Pathology Peer Review and Scores : PDF version for download AP141 Bone Marrow: Metastatic Carcinoma from
AP2003R1 http://hkcpath.org. Correspondence: [email protected] 1of 10 07/08/2003 HKCPath Anatomical Pathology Peer Review and Scores : PDF version for download AP141 Bone Marrow: Metastatic Carcinoma from
Contents. 1. Introduction and Approach to Fine Needle Aspiration Cytology... 1. 2. Head, Neck, Orbit and Salivary Glands... 12
 Contents 1. Introduction and Approach to Fine Needle Aspiration Cytology... 1 Complications 1 Fine Needle Aspiration Technique 1 Evaluation of FNAC Smear 4 Cell Morphology 4 Nucleus 4 Cytoplasm 6 Background
Contents 1. Introduction and Approach to Fine Needle Aspiration Cytology... 1 Complications 1 Fine Needle Aspiration Technique 1 Evaluation of FNAC Smear 4 Cell Morphology 4 Nucleus 4 Cytoplasm 6 Background
Understanding your pathology report
 Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Ductal carcinoma in situ (DCIS)
 DIAGNOSIS: DCIS Ductal carcinoma in situ (DCIS) This factsheet gives information on an early form of breast cancer called ductal carcinoma in situ (DCIS). It explains what it is, how your breast is made
DIAGNOSIS: DCIS Ductal carcinoma in situ (DCIS) This factsheet gives information on an early form of breast cancer called ductal carcinoma in situ (DCIS). It explains what it is, how your breast is made
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY
 MALIGNANT MESOTHELIOMA CLASSIFICATION MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo,
MALIGNANT MESOTHELIOMA CLASSIFICATION MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo,
Explanation of your PAP smear
 Explanation of your PAP smear Approximately 5-10% of PAP smears in the United States are judged to be abnormal. Too often, the woman who receives this news worries that she already has, or will develop,
Explanation of your PAP smear Approximately 5-10% of PAP smears in the United States are judged to be abnormal. Too often, the woman who receives this news worries that she already has, or will develop,
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY
 MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo, Finland 2nd Nordic Conference on Applied
MALIGNANT MESOTHELIOMA UPDATE ON PATHOLOGY AND IMMUNOHISTOCHEMISTRY Sisko Anttila, MD, PhD Jorvi Hospital Laboratory of Pathology Helsinki University Hospital Espoo, Finland 2nd Nordic Conference on Applied
Breast Cancer. Sometimes cells keep dividing and growing without normal controls, causing an abnormal growth called a tumor.
 Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Something Old, Something New.
 Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Introduction: Tumor Swelling / new growth / mass. Two types of growth disorders: Non-Neoplastic. Secondary / adaptation due to other cause.
 Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Efficient Tumor Immunohistochemistry A Differential Diagnosis-Driven Approach
 Efficient Tumor Immunohistochemistry A Differential Diagnosis-Driven Approach Publishing Team Erik Tanck (production manager/designer) Joshua Weikersheimer (publisher) Copyright 2006 by the American Society
Efficient Tumor Immunohistochemistry A Differential Diagnosis-Driven Approach Publishing Team Erik Tanck (production manager/designer) Joshua Weikersheimer (publisher) Copyright 2006 by the American Society
Policy Wording. Together, all the way.
 Cancer cover Policy Wording Together, all the way. Cancer Cover Insurance Policy Wording 1. Introducing your Policy 2. What is Cancer Cover Insurance? 3. About your Policy 4. Some terms defined 5. What
Cancer cover Policy Wording Together, all the way. Cancer Cover Insurance Policy Wording 1. Introducing your Policy 2. What is Cancer Cover Insurance? 3. About your Policy 4. Some terms defined 5. What
Cancer of the Cervix
 Cancer of the Cervix WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 A woman's cervix (the opening of the uterus) is lined with cells. Cancer of the cervix occurs when those cells change,
Cancer of the Cervix WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 A woman's cervix (the opening of the uterus) is lined with cells. Cancer of the cervix occurs when those cells change,
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
NEOPLASMS C00 D49. Presented by Jan Halloran CCS
 NEOPLASMS C00 D49 Presented by Jan Halloran CCS 1 INTRODUCTION A neoplasm is a new or abnormal growth. In the ICD-10-CM classification system, neoplastic disease is classified in categories C00 through
NEOPLASMS C00 D49 Presented by Jan Halloran CCS 1 INTRODUCTION A neoplasm is a new or abnormal growth. In the ICD-10-CM classification system, neoplastic disease is classified in categories C00 through
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY
 CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too.
 Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
THYROID CANCER. I. Introduction
 THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THE PATHOLOGY OF MEDIASTINAL MASSES. Anatomic Distribution of Mediastinal Masses
 Page 1 of 5 THE PATHOLOGY OF MEDIASTINAL MASSES Dr. S. Boag 549-6666 Ext. 4190, mailto:%[email protected] 1. INTRODUCTION A wide range of process, neoplastic and non-neoplastic, can produce
Page 1 of 5 THE PATHOLOGY OF MEDIASTINAL MASSES Dr. S. Boag 549-6666 Ext. 4190, mailto:%[email protected] 1. INTRODUCTION A wide range of process, neoplastic and non-neoplastic, can produce
Ovarian tumors Ancillary methods
 Ovarian tumors Ancillary methods Ovarian tumor course Oslo, 24-25/11/14 Prof. Ben Davidson, MD PhD Department of Pathology, Norwegian Radium Hospital, Oslo University Hospital, Oslo, Norway Division of
Ovarian tumors Ancillary methods Ovarian tumor course Oslo, 24-25/11/14 Prof. Ben Davidson, MD PhD Department of Pathology, Norwegian Radium Hospital, Oslo University Hospital, Oslo, Norway Division of
The develpemental origin of mesothelium
 Mesothelioma Tallinn 14.12.06 Henrik Wolff Finnish Institute of Occupational Health The develpemental origin of mesothelium Mesodermal cavities (pleura, peritoneum and pericardium ) are lined with mesenchymal
Mesothelioma Tallinn 14.12.06 Henrik Wolff Finnish Institute of Occupational Health The develpemental origin of mesothelium Mesodermal cavities (pleura, peritoneum and pericardium ) are lined with mesenchymal
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Cervical lymphadenopathy
 Cervical lymphadenopathy Introduction There are various classifications of lymphadenopathy, but a simple and clinically useful system is to classify lymphadenopathy as "generalized" if lymph nodes are
Cervical lymphadenopathy Introduction There are various classifications of lymphadenopathy, but a simple and clinically useful system is to classify lymphadenopathy as "generalized" if lymph nodes are
This factsheet aims to outline the characteristics of some rare lung cancers, and highlight where each type of lung cancer may be different.
 There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
Lung Cancer. Ossama Tawfik, MD, PhD Professor, Vice Chairman Director of Anatomic &Surgical Pathology University of Kansas School of Medicine
 Lung Cancer Ossama Tawfik, MD, PhD Professor, Vice Chairman Director of Anatomic &Surgical Pathology University of Kansas School of Medicine Alexandria, Egypt July 1-1 3, 2008 OBJECTIVES Describe and
Lung Cancer Ossama Tawfik, MD, PhD Professor, Vice Chairman Director of Anatomic &Surgical Pathology University of Kansas School of Medicine Alexandria, Egypt July 1-1 3, 2008 OBJECTIVES Describe and
Directly Coded Summary Stage Is Back
 Directly Coded Summary Stage Is Back Donna M. Hansen, CTR Auditor & Training Coordinator California Cancer Registry June 30, 2015 1 Outline What is SEER Summary Stage 2000 (SS2000)? Summary Stage Housekeeping
Directly Coded Summary Stage Is Back Donna M. Hansen, CTR Auditor & Training Coordinator California Cancer Registry June 30, 2015 1 Outline What is SEER Summary Stage 2000 (SS2000)? Summary Stage Housekeeping
4/15/2013. bi/o carcin/ chem/o immun/o onc/o radi/o sarc/o. anabrachydysectoendoneo- -ectomy -genesis -oma -plasia -sarcoma
 Chapter Sixteen Oncology bi/o carcin/ chem/o immun/o onc/o radi/o sarc/o Combining Forms Prefixes and Suffixes Carcinogenesis anabrachydysectoendoneo- -ectomy -genesis -oma -plasia -sarcoma Causes of cancer
Chapter Sixteen Oncology bi/o carcin/ chem/o immun/o onc/o radi/o sarc/o Combining Forms Prefixes and Suffixes Carcinogenesis anabrachydysectoendoneo- -ectomy -genesis -oma -plasia -sarcoma Causes of cancer
95% of childhood kidney cancer cases are Wilms tumours. Childhood kidney cancer is extremely rare, with only 90 cases a year in
 James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Effusions: Mesothelioma and Metastatic Cancers
 Effusions: Mesothelioma and Metastatic Cancers Malignant Mesothelioma Incidence: 2,500 cases/year ~60-80% pts with pleural MM relationship with asbestos exposure Other risk factors: radiation, other carcinogens,
Effusions: Mesothelioma and Metastatic Cancers Malignant Mesothelioma Incidence: 2,500 cases/year ~60-80% pts with pleural MM relationship with asbestos exposure Other risk factors: radiation, other carcinogens,
Immunohistochemistry on cytology specimens from pleural and peritoneal fluid
 Immunohistochemistry on cytology specimens from pleural and peritoneal fluid Dr Naveena Singh Consultant Pathologist Bart health NHS Trust London United Kingdom Disclosures and Acknowledgements I have
Immunohistochemistry on cytology specimens from pleural and peritoneal fluid Dr Naveena Singh Consultant Pathologist Bart health NHS Trust London United Kingdom Disclosures and Acknowledgements I have
How to report Upper GI EMR/ESD specimens
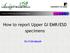 Section of Pathology and Tumour Biology How to report Upper GI EMR/ESD specimens Dr.H.Grabsch Warning. Most of the criteria, methodologies, evidence presented in this talk are based on studies in early
Section of Pathology and Tumour Biology How to report Upper GI EMR/ESD specimens Dr.H.Grabsch Warning. Most of the criteria, methodologies, evidence presented in this talk are based on studies in early
Adjuvant Therapy for Breast Cancer: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Adjuvant Therapy for Breast
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Adjuvant Therapy for Breast
Diagnostic Challenge. Department of Pathology,
 Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Case of the. Month October, 2012
 Case of the Month October, 2012 Case The patient is a 47-year-old male with a 3-week history of abdominal pain. A CT scan of the abdomen revealed a suggestion of wall thickening at the tip of the appendix
Case of the Month October, 2012 Case The patient is a 47-year-old male with a 3-week history of abdominal pain. A CT scan of the abdomen revealed a suggestion of wall thickening at the tip of the appendix
Diagnosis of Mesothelioma Pitfalls and Practical Information
 Diagnosis of Mesothelioma Pitfalls and Practical Information Mary Beth Beasley, M.D. Mt Sinai Medical Ctr Dept of Pathology One Gustave L Levy Place New York, NY 10029 (212) 241-5307 [email protected]
Diagnosis of Mesothelioma Pitfalls and Practical Information Mary Beth Beasley, M.D. Mt Sinai Medical Ctr Dept of Pathology One Gustave L Levy Place New York, NY 10029 (212) 241-5307 [email protected]
Cervical Cancer The Importance of Cervical Screening and Vaccination
 Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1557/14
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1557/14 BEFORE: M. Crystal: Vice-Chair HEARING: August 20, 2014 at Toronto Written DATE OF DECISION: December 4, 2014 NEUTRAL CITATION: 2014
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1557/14 BEFORE: M. Crystal: Vice-Chair HEARING: August 20, 2014 at Toronto Written DATE OF DECISION: December 4, 2014 NEUTRAL CITATION: 2014
Nicole Kounalakis, MD
 Breast Disease: Diagnosis and Management Nicole Kounalakis, MD Assistant Professor of Surgery Goal of Breast Evaluation The goal of breast evaluation is to classify findings as: normal physiologic variations
Breast Disease: Diagnosis and Management Nicole Kounalakis, MD Assistant Professor of Surgery Goal of Breast Evaluation The goal of breast evaluation is to classify findings as: normal physiologic variations
Practical Effusion Cytology
 Practical Effusion Cytology A Community Pathologist s Approach to Immunocytochemistry in Body Fluid Cytology Emily E. Volk, MD William Beaumont Hospital Troy, MI College of American Pathologists 2004.
Practical Effusion Cytology A Community Pathologist s Approach to Immunocytochemistry in Body Fluid Cytology Emily E. Volk, MD William Beaumont Hospital Troy, MI College of American Pathologists 2004.
Information Model Requirements of Post-Coordinated SNOMED CT Expressions for Structured Pathology Reports
 Information Model Requirements of Post-Coordinated SNOMED CT Expressions for Structured Pathology Reports W. Scott Campbell, Ph.D., MBA James R. Campbell, MD Acknowledgements Steven H. Hinrichs, MD Chairman
Information Model Requirements of Post-Coordinated SNOMED CT Expressions for Structured Pathology Reports W. Scott Campbell, Ph.D., MBA James R. Campbell, MD Acknowledgements Steven H. Hinrichs, MD Chairman
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium
 Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
How To Treat A Uterine Sarcoma
 EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition 2001 Uterus: Uterine Sarcomas Jeffrey L. Stern, MD Uterine sarcomas
EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition 2001 Uterus: Uterine Sarcomas Jeffrey L. Stern, MD Uterine sarcomas
A 70-year old Man with Pleural Effusion
 Mesothelioma Diagnosis: Pitfalls and Latest Updates S Klebe and DW Henderson Recommendations Indisputable malignant cells on cytomorphological criteria which demonstrate a mesothelial phenotype, which
Mesothelioma Diagnosis: Pitfalls and Latest Updates S Klebe and DW Henderson Recommendations Indisputable malignant cells on cytomorphological criteria which demonstrate a mesothelial phenotype, which
How CanCer becomes critical in the claims
 How CanCer becomes critical in the claims arena Cancer is a disease in which cells in your body grow in an uncontrolled way and form a lump called a tumour. In a healthy individual cells grow and reproduce
How CanCer becomes critical in the claims arena Cancer is a disease in which cells in your body grow in an uncontrolled way and form a lump called a tumour. In a healthy individual cells grow and reproduce
Today s Topics. Tumors of the Peritoneum in Women
 Today s Topics Tumors of the Peritoneum in Women Charles Zaloudek, M.D. Department of Pathology 505 Parnassus Ave., M563 University of California, San Francisco San Francisco, CA USA [email protected]
Today s Topics Tumors of the Peritoneum in Women Charles Zaloudek, M.D. Department of Pathology 505 Parnassus Ave., M563 University of California, San Francisco San Francisco, CA USA [email protected]
Seattle. Case Presentations. Case 1. 76 year old female with a history of breast cancer 12 years ago. Now presents with a pleural effusion.
 Seattle Montreal IAP September 2006 Case Presentations Allen M. Gown, M.D. Medical Director and Chief Pathologist PhenoPath Laboratories Clinical Professor of Pathology University of British Columbia Case
Seattle Montreal IAP September 2006 Case Presentations Allen M. Gown, M.D. Medical Director and Chief Pathologist PhenoPath Laboratories Clinical Professor of Pathology University of British Columbia Case
Leukemias and Lymphomas: A primer
 Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry. M. Praet
 PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry M. Praet Pathology of the Pleura Normal serosa: visceral and parietal layers Inflammation Neoplasia: Primary: mesothelioma
PATHOLOGY OF THE PLEURA: Mesothelioma and mimickers Necessity of Immunohistochemistry M. Praet Pathology of the Pleura Normal serosa: visceral and parietal layers Inflammation Neoplasia: Primary: mesothelioma
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
ATLAS OF HEAD AND NECK PATHOLOGY THYROID PAPILLARY CARCINOMA
 Papillary carcinoma is the most common of thyroid malignancies and occurs in all age groups but particularly in women under 45 years of age. There is a high rate of cervical metastatic disease and yet
Papillary carcinoma is the most common of thyroid malignancies and occurs in all age groups but particularly in women under 45 years of age. There is a high rate of cervical metastatic disease and yet
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
BREAST CANCER PATHOLOGY
 BREAST CANCER PATHOLOGY FACT SHEET Version 4, Aug 2013 This fact sheet was produced by Breast Cancer Network Australia with input from The Royal College of Pathologists of Australasia I m a nurse and know
BREAST CANCER PATHOLOGY FACT SHEET Version 4, Aug 2013 This fact sheet was produced by Breast Cancer Network Australia with input from The Royal College of Pathologists of Australasia I m a nurse and know
New Hampshire Childhood Cancer
 Introduction: New Hampshire Childhood Cancer New Hampshire, Childhood Cancer, January 2009 Issue Brief Cancer in children is relatively uncommon, impacting fewer than twenty two of every 100,000 children
Introduction: New Hampshire Childhood Cancer New Hampshire, Childhood Cancer, January 2009 Issue Brief Cancer in children is relatively uncommon, impacting fewer than twenty two of every 100,000 children
PROTOCOL OF THE RITA DATA QUALITY STUDY
 PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
General Rules SEER Summary Stage 2000. Objectives. What is Staging? 5/8/2014
 General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
Cytology of Lymph Nodes
 Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer
 Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer Version History Version Date Summary of Change/Process 0.1 09.01.11
Guideline for the Imaging of Patients Presenting with Breast Symptoms incorporating the guideline for the use of MRI in breast cancer Version History Version Date Summary of Change/Process 0.1 09.01.11
Chapter 2 Staging of Breast Cancer
 Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
GENERAL CODING. When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis.
 GENERAL CODING When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis. Exception: You must review and revise EOD coding for prostate
GENERAL CODING When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis. Exception: You must review and revise EOD coding for prostate
A23: Oncologic Disease- Tumor Markers
 A23: Oncologic Disease- Tumor Markers Diagnosis Tumor Markers and Genetic Markers Use for Specific Malignancy The following information is from multiple guideline sources as recommendations for use of
A23: Oncologic Disease- Tumor Markers Diagnosis Tumor Markers and Genetic Markers Use for Specific Malignancy The following information is from multiple guideline sources as recommendations for use of
PRIMARY SEROUS CARCINOMA OF PERITONEUM: A CASE REPORT
 PRIMARY SEROUS CARCINOMA OF PERITONEUM: A CASE REPORT Dott. Francesco Pontieri (*) U.O. di Anatomia Patologica P.O. di Rossano (CS) Dott. Gian Franco Zannoni Anatomia Patologica Facoltà di Medicina e Chirurgia
PRIMARY SEROUS CARCINOMA OF PERITONEUM: A CASE REPORT Dott. Francesco Pontieri (*) U.O. di Anatomia Patologica P.O. di Rossano (CS) Dott. Gian Franco Zannoni Anatomia Patologica Facoltà di Medicina e Chirurgia
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy
 Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
Metastatic Cervical Cancer s/p Radiation Therapy, Radical Hysterectomy and Attempted Modified Internal Hemipelvectomy Sarah Hutto,, MSIV Marc Underhill, M.D. January 27, 2009 Past History 45 yo female
 DIFFICULTIES IN THE PATHOLOGIC DIAGNOSIS OF LUNG CANCER Notice of Financial Disclosures (TV Colby MD) (Esp. in small biopsies) Personal Experience Thomas V. Colby, M.D. Mayo Clinic Arizona NONE This talk
DIFFICULTIES IN THE PATHOLOGIC DIAGNOSIS OF LUNG CANCER Notice of Financial Disclosures (TV Colby MD) (Esp. in small biopsies) Personal Experience Thomas V. Colby, M.D. Mayo Clinic Arizona NONE This talk
Metastasis. brain metastasis from bronchial carcinoma
 metastasis Metastasis brain metastasis from bronchial carcinoma How many genetic changes are needed for neoplastic transformation?... if you have some of these changes, but not all, you will never become
metastasis Metastasis brain metastasis from bronchial carcinoma How many genetic changes are needed for neoplastic transformation?... if you have some of these changes, but not all, you will never become
why? 75 percent The percentage of healthy individuals over age 40 who will become critically ill at some time in the future. 3
 Elite coverage can help protect your savings. USAble Life s 1 coverage helps protect your family from the financial impact that can occur as the result of a heart attack, stroke or even cancer by providing
Elite coverage can help protect your savings. USAble Life s 1 coverage helps protect your family from the financial impact that can occur as the result of a heart attack, stroke or even cancer by providing
Renal Tumors with Eosinophilic Cytoplasm: 2013 Classification. Jesse K. McKenney, MD Associate Head, Surgical Pathology
 Renal Tumors with Eosinophilic Cytoplasm: 2013 Classification Jesse K. McKenney, MD Associate Head, Surgical Pathology Renal Epithelial Neoplasia History 1981: WHO Classification of Renal Neoplasms 1.
Renal Tumors with Eosinophilic Cytoplasm: 2013 Classification Jesse K. McKenney, MD Associate Head, Surgical Pathology Renal Epithelial Neoplasia History 1981: WHO Classification of Renal Neoplasms 1.
Aggressive lymphomas. Michael Crump Princess Margaret Hospital
 Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
LifeProtect. Cancer Cover. For Intermediary Use Only
 LifeProtect Cancer Cover For Intermediary Use Only There are few families in Ireland that have been unaffected by cancer. In fact, 1 in 3 men and 1 in 4 women in Ireland* will suffer from cancer at some
LifeProtect Cancer Cover For Intermediary Use Only There are few families in Ireland that have been unaffected by cancer. In fact, 1 in 3 men and 1 in 4 women in Ireland* will suffer from cancer at some
This module consists of four units which will provide the user a basic knowledge of cancer as a disease.
 Module 5: What is Cancer? This module consists of four units which will provide the user a basic knowledge of cancer as a disease. After completing this module, cancer abstractors will be able to: Define
Module 5: What is Cancer? This module consists of four units which will provide the user a basic knowledge of cancer as a disease. After completing this module, cancer abstractors will be able to: Define
D. FREQUENTLY ASKED QUESTIONS
 ACR BI-RADS ATLAS D. FREQUENTLY ASKED QUESTIONS 1. Under MQSA, is it necessary to include a numeric assessment code (i.e., 0, 1, 2, 3, 4, 5, or 6) in addition to the assessment category in all mammography
ACR BI-RADS ATLAS D. FREQUENTLY ASKED QUESTIONS 1. Under MQSA, is it necessary to include a numeric assessment code (i.e., 0, 1, 2, 3, 4, 5, or 6) in addition to the assessment category in all mammography
