Technique Guide. 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis.
|
|
|
- June Hood
- 9 years ago
- Views:
Transcription
1 Technique Guide 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis.
2
3 Table of Contents Introduction 3.5 mm and 4.5 mm Curved Locking Compression 2 Plates (LCP) AO Principles 5 Indications 6 Fixation Principles 7 Minimally Invasive Reduction and 12 Plate Insertion Instruments Surgical Technique Toothed Reduction Handles (Bicortical) 13 for Enhanced Rotational Stability Plate Contouring (optional) 16 Plate Insertion 17 Reduction and Temporary Plate Placement 20 Screw Insertion 21 Screw Placement Verification 26 Implant Removal 28 Product Information Implants 29 Instruments 31 Set Lists 35 IMPORTANT: This device has not been evaluated for safety and compatibility in the MR environment. This device has not been tested for heating or migration in the MR environment. Image intensifier control Synthes
4 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) The Synthes Locking Compression Plates (LCP) are part of a plate and screw system that merges locking screw technology with conventional plating techniques. The Locking Compression Plate System has many similarities to existing plate fixation methods, but with a few important enhancements. Locking screws provide the ability to create a fixedangle construct while utilizing familiar AO plating techniques. A fixed-angle construct provides advantages in osteopenic bone or multifragment fractures where traditional screw purchase is compromised. Locking screws do not rely on plate-to-bone compression to maintain stability, but function similarly to multiple small angled blade plates. Plate features The Locking Compression Plates (LCP) Uniform hole spacing Load (compression) and neutral screw positions 2 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
5 Combi holes The Combi holes allow placement of standard cortex and cancellous bone screws on one side or threaded conical locking screws on the opposite side of each hole. Dynamic compression unit (DCU) hole section for standard screws Threaded hole section for locking screws Locking screw in threaded side of plate hole Holes in these plates are oriented so that the compression of the hole is always directed toward the middle of the plate. Cortex screw in compression side of plate hole Synthes 3
6 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Locking screws, self-tapping, with StarDrive recess The locking screws mate with the threaded plate holes to form a fixed-angle construct. Locking screw design The screw design has been modified, as compared to standard cortex screws, to enhance fixation and facilitate the surgical procedure. StarDrive recess The StarDrive recess provides improved torque transmission to the screw while retaining the screw on the screwdriver without the use of a holding sleeve. Large core diameter The large core diameter improves bending and shear strength, and distributes the load over a larger area in the bone. Self-tapping flutes Conical screwhead The conical head facilitates alignment of the locking screw in the threaded plate hole to provide a secure screw-plate construct. Thread profile The shallow thread profile of the locking screws results from the larger core diameter. This is possible because locking screws do not rely solely on the screw threads to create compression between the plate and the bone to maintain stability. 4 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
7 AO Principles In 1958, the AO formulated four basic principles, which have become the guidelines for internal fixation. 1 These principles, as applied to the 3.5 mm and 4.5 mm Curved Locking Compression Plates, are: Anatomic reduction The plates combine reduction and protection of soft tissues. Stable fixation Locking screws create a fixed-angle construct, providing angular stability. Preservation of blood supply Tapered end allows submuscular plate insertion. Submuscular plate insertion may preserve tissue viability. Limited-contact plate design reduces plate-to-bone contact. Reduced plate-to-bone contact may minimize vascular trauma and insult to bone. Early, active mobilization Plate features combined with AO technique create an environment for bone healing, expediting a return to optimal function. 1. M.E. Müller, M. Allgöwer, R. Schneider, and H. Willenegger: Manual of Internal Fixation, 3rd Edition. Berlin: Springer-Verlag Synthes 5
8 Indications The Synthes 3.5 mm Curved LCP Plates are intended for fixation of fractures, osteotomies and nonunions of the clavicle, scapula, olecranon, humerus, radius, pelvis, distal tibia and fibula, particularly in osteopenic bone for adult patients. The Synthes 4.5 mm Curved LCP Plates are intended for fixation of various long bones, such as the humerus, femur, and tibia. They are also for use in fixation of periprosthetic fractures, osteopenic bone, and nonunions or malunions in adult patients. The 3.5 mm and 4.5 mm Curved LCP Plates are also intended for fracture fixation of diaphyseal and metaphyseal areas of long bones in pediatric patients. 6 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
9 Fixation Principles The following points distinguish treatment using locking compression plate technology: Allows fracture treatment using compression plating with conventional cortex or cancellous bone screws Allows fracture treatment using locked plating with bicortical or unicortical locking screws Permits the combination of conventional and locking screw techniques Note: These LCP plates are suitable for a large number of fracture types. For that reason, this technique guide does not deal with any specific fracture type. Please refer also to the AO Principles of Fracture Management, 2 and the AO Manual of Fracture Management Internal Fixators. 3 a Unicortical screw fixation Unicortical locking screws provide stability and load transfer only at the near cortex due to the threaded connection between the plate and the screw. Screw stability and load transfer are accomplished at two points along the screw: the screwhead and near cortex. Because the screw is locked to the plate, fixation does not rely solely on the pullout strength of the screw or on maintaining friction between the plate and the bone. Bicortical screw fixation has long been the traditional method of compressing a plate to the bone where friction between the plate and the bone maintains stability. Screw stability and load transfer are accomplished at two points along the screw: the near and far cortices. a. Unicortical screws utilize the locked screw and the near cortex to achieve stability. b. Bicortical screws require two (2) cortices to achieve stability. b 2. Thomas P. Rüedi, et al, ed., AO Principles of Fracture Management, New York: Thieme, M. Wagner and R. Frigg, AO Manual of Fracture Management Internal Fixators, New York: Thieme, Synthes 7
10 Fixation Principles The following examples show the biomechanical features of conventional plating techniques, locked or bridge plating techniques, and a combination of both. Conventional plating F3 F2 Absolute stability The tensile force (F1) originating from tightening the screws presses the plate onto the bone (F2). The developing friction (F3) between the plate and the bone leads to stable plate fixation. To ensure absolute stability, the friction resistance must be higher than the axial forces (F4) arising during rehabilitation. F4 F1 F2 F4 Lag screw Interfragment compression is accomplished by using a lag screw. This is particularly important in intra-articular fractures which require a precise reduction of the joint surfaces. Lag screws can be angled in the plate hole, allowing placement of the screw perpendicular to the fracture line. Primary loss of reduction In conventional plating, even though the bone fragments are correctly reduced prior to plate application, fracture dislocation will result if the plate does not fit the bone. In addition, if the lag screw is not seated perpendicular to the fracture line (e.g., spiral fracture of the distal tibia), shear forces will be introduced. These forces may cause loss of reduction. 8 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
11 Secondary loss of reduction Under axial load, postoperative, secondary loss of reduction may occur by toggling of the screws. Since cortex screws do not lock to the plate, the screws cannot oppose the acting force and may loosen, or be pushed axially through the plate holes. Blood supply to the bone The periosteum is compressed under the plate area, reducing or even interrupting blood supply to the bone. The result is delayed bone healing due to temporary osteoporosis underneath the plate. Synthes 9
12 Fixation Principles Bridge/locked plating using locking screws Screws lock to the plate, forming a fixed-angle construct Bone healing is achieved indirectly by callus formation when using locking screws exclusively Maintenance of primary reduction Once the locking screws engage the plate, no further tightening is possible. Therefore, the implant locks the bone segments in their relative positions regardless of degree of reduction. Precontouring the plate minimizes the gap between the plate and the bone, but an exact fit is not necessary for implant stability. This feature is especially advantageous in minimally or less invasive plating techniques because these techniques do not allow exact contouring of the plate to the bone surface. Stability under load By locking the screws to the plate, the axial force is transmitted over the length of the plate. The risk of a secondary loss of the intraoperative reduction is reduced. Blood supply to the bone Locking the screw into the plate does not generate additional compression between the plate and the bone. Therefore, the periosteum will be protected and the blood supply to the bone preserved. 10 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
13 Combined internal fixation The combination of conventional compression plating and locked plating techniques enhances plate osteosynthesis. The result is a combination, or Combi, hole that, depending on the indication, allows standard compression plating, locked/ bridge plating or a combination of both. Internal fixation using a combination of locking screws and standard screws Note: If a combination of cortex and locking screws is used, a cortex screw should be inserted first to pull the plate to the bone. If locking screws (1) have been used to fix a plate to a fragment, subsequent insertion of a standard screw (2) in the same fragment without loosening and retightening the locking screw is NOT RECOMMENDED. 1 1 Note: If a locking screw is used first, care should be taken to ensure that the plate is held securely to the bone to avoid spinning of the plate about the bone. Dynamic compression Once the metaphyseal fragment has been fixed with locking screws, the fracture can be dynamically compressed using standard screws in the DCU portion of the Combi hole. Locked and standard plating techniques First, use lag screws to anatomically reconstruct the joint surfaces The behavior of a locking screw is not the same as that of a lag screw. With the locked plating technique, the implant locks the bone segments in their relative positions regardless of how they are reduced A plate used as a locked/bridge plate does not produce any additional compression between the plate and the bone The unicortical insertion of a locking screw causes no loss of stability 2 Synthes 11
14 Minimally Invasive Reduction and Plate Insertion Instruments Minimally invasive surgery supports the principles of biological internal fixation by avoiding long incisions and extensive soft tissue stripping associated with conventional techniques. Devascularization of the fragments can be minimized by indirect reduction and an improved healing process can be expected. The Minimally Invasive Reduction Instruments are intended for obtaining intraoperative fixation using minimally invasive, indirect reduction techniques. The Minimally Invasive Plate Insertion Instruments are indicated for plate insertion through minimal incision(s) after temporary reduction has been achieved. The Minimally Invasive Reduction and Plate Insertion Instrument Set includes: Reduction handles to gain and maintain stable intraoperative fixation of a fracture Soft tissue retractors to subcutaneously prepare a plate pathway over long distances through a small incision A plate holder with clamping feet for easy, percutaneous manipulation of a plate along the bone Reduction handles Toothed reduction handles provide rotational stability during manipulation of bone fragments. Soft tissue retractors The offset blade allows easy preparation of a cavity for percutaneous plate insertion. The asymmetric tip allows a choice of insertion angle. The blade length can be adjusted using a combination wrench. The blade can be completely removed for easy cleaning of the cannulated handle. Plate holder The plate holder is for percutaneous insertion of most LCP and LC-DCP plates. A simple clamping mechanism provides guidance and easy handling of a plate under soft tissue. Nine interchangeable clamping feet are available for use with the plate holder. 12 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
15 Toothed Reduction Handles (Bicortical) for Enhanced Rotational Stability 1 Insert threaded rod Instruments for 3.0 mm threaded rods mm Protection Sleeve, slotted mm/3.0 mm Drill Sleeve mm Threaded Rod, self-drilling tip Instruments for 5.0 mm threaded rods mm Protection Sleeve, slotted mm/5.0 mm Drill Sleeve mm Threaded Rod, self-drilling tip Insert a self-drilling threaded rod through the drill sleeve assembly (drill sleeve and protection sleeve) and into the bone so that the self-drilling tip is embedded in the far cortex. Remove the drill sleeve. Synthes 13
16 Toothed Reduction Handles (Bicortical) for Enhanced Rotational Stability 2 Attach reduction handle Instruments for 3.0 mm threaded rods Reduction Handle, toothed, for 3.0 mm Threaded Rod mm Protection Sleeve, slotted Adjusting Nut, for 3.0 mm Threaded Rod mm Threaded Rod, self-drilling tip Instruments for 5.0 mm threaded rods Reduction Handle, toothed, for 5.0 mm Threaded Rod mm Protection Sleeve, slotted Adjusting Nut, for 5.0 mm Threaded Rod mm Threaded Rod, self-drilling tip Slide the toothed reduction handle over the threaded rod and through the slotted protection sleeve to the bone. Slide the adjusting nut over the threaded rod and tighten it onto the reduction handle. Note: Tightening the adjusting nut excessively may cause the threaded rod to strip out of the bone. Remove the protection sleeve by sliding back the release. A second toothed reduction handle can be attached using the same technique. 14 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
17 3 Reduce fracture Instruments for 3.0 mm threaded rods Medium Combination Clamp, MR Safe mm Carbon Fiber Rod Instruments for 5.0 mm threaded rods Large Combination Clamp, MR Conditional mm Carbon Fiber Rod If needed, apply combination clamps and a carbon fiber rod without tightening the construct. Reduce the fragments. 4 Temporary fixation Instrument mm/11 mm Wrench Using the 8 mm/11 mm wrench, firmly tighten the combination clamps to temporarily hold the reduction. After definitive treatment of the fracture, remove the reduction instruments. The large reduction instruments are shown in these illustrations. Use the same technique for the small reduction instruments. Note: Reduction instruments, including threaded rods, are not indicated for postoperative use. Synthes 15
18 Plate Contouring (optional) Use the AO preoperative planner template for the 3.5 mm and 4.5 mm curved LCP plates. Note: Templates are available in two sizes: actual size and 115% magnification in which the image is enlarged 15% to correspond to typical radiological magnification; however, variations in magnification levels are common. Required sets Small Fragment LCP Instrument and Implant Set or Large Fragment LCP Instrument and Implant Set or Periarticular LCP Plating System, with 5.0 mm Locking Screws Bending instruments */ Bending Irons * * Bending Pliers * Plate Bending Press Use the bending instruments to contour the locking compression plate to the anatomy. Note: The plate holes are designed to accept some degree of deformation. When bending the plate, place the bending irons on two adjacent holes. This ensures that the threaded holes will not be distorted. Significant distortion of the locking holes will reduce locking effectiveness. Please refer to the AO Principles of Fracture Management, 4 and the AO Manual of Fracture Management Internal Fixators Rüedi. 5. Wagner. * Also available 16 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
19 Plate Insertion 1 Insert soft tissue retractors Instruments mm/11 mm Wrench Soft Tissue Retractor, small, extendible Optional instrument Small Soft Tissue Retractor Blade, long To adjust the length of the soft tissue retractors, loosen the clamping sleeve with the 8 mm/11 mm wrench. Use the 8 mm wrench for the small retractor. Slide the blade within the handle to an appropriate length and tighten the clamping sleeve. Warning: Do not over tighten the clamping sleeve as this could lead to breakage. Do not extend the blade beyond the line marked MAX. Insert the soft tissue retractor through an incision to prepare a cavity for percutaneous plate insertion. Synthes 17
20 Plate Insertion 2 Assemble plate holder 3 Instruments for 3.5 mm narrow plates Large Hexagonal Key, for large screws Clamping Foot, for , for 3.5 mm LCP and 3.5 mm LC-DCP Plate Holder, for Minimally Invasive Plating Osteosynthesis Instruments for 3.5 mm broad and 4.5 mm narrow plates Clamping Foot, for , for 4.5 mm/5.0 mm Narrow LCP and 4.5 mm Narrow LC-DCP Connecting Screw, for Plate Holder 4 2 Push the connecting screw through the plate holder until it clicks into place (1). Insert a clamping foot into the plate holder (2). Engage the connecting screw into the clamping foot, but do not fully tighten (3). Slide the selected plate into the clamping foot (4). Firmly tighten the connecting screw with the large hexagonal key. 18 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
21 3 Insert plate 4 Remove plate holder Instrument Large Hexagonal Key, for large screws Use the large hexagonal key to remove the connecting screw from the plate holder. Remove the plate holder from the clamping foot. Slide the clamping foot from the plate. Synthes 19
22 Reduction and Temporary Plate Placement 1 Reduce and position plate Instruments for 3.5 mm plates Push-Pull Reduction Device Threaded Plate Holder or Threaded Plate Holder, long Instruments for 4.5 mm plates Push-Pull Reduction Device Threaded Plate Holder The plate may be temporarily held in place with standard plate holding forceps, a push-pull reduction device or a K-wire. Note: The middle of the plate should be positioned over the fracture site if compression of the fracture fragments is desired. The push-pull reduction device is designed to temporarily hold the plate to the bone through a plate hole. The device is self-drilling and connects with the Synthes quick coupling for power insertion. Insert into the near cortex only. After power insertion, turn the collet clockwise until it pulls the plate securely to the bone. Note: Take care to avoid inserting this device in a hole that will be needed immediately for plate fixation. However, the device may be removed and a screw inserted through the same plate hole. A threaded plate holder can also be used as an aid to position the plate on the bone. The plate holder may also function as an insertion handle for use with minimally invasive plating techniques. 20 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
23 Screw Insertion 1 Insert screws Determine whether standard cortex screws, cancellous bone screws or locking screws will be used for fixation. A combination of all may be used. Note: If a combination of cortex, cancellous and locking screws is used, a standard screw should be used first to pull the plate to the bone. Warning: If a locking screw is used first, care should be taken to ensure that the plate is held securely to the bone to avoid spinning of the plate about the bone. Insertion of a cortex or cancellous bone screw Instruments for 3.5 mm cortex or cancellous bone screws mm Drill Bit Small Hexagonal Screwdriver Depth Gauge, for small screws mm Universal Drill Guide Instruments for 4.5 mm cortex or cancellous bone screws mm Drill Bit Large Hexagonal Screwdriver Depth Gauge, for large screws mm Universal Drill Guide Predrill both cortices using the universal drill guide for an eccentric (compression) or neutral (buttress) insertion of cortex screws. Note: The LC-DCP drill guide and the DCP drill guide are NOT suitable for use with LCP plates. Synthes 21
24 Screw Insertion 1 Insert screws continued Neutral insertion of a standard screw When pressing the universal drill guide into the DCU portion of the LCP plate, it will center itself and allow neutral predrilling. Dynamic compression, eccentric insertion of a cortex screw To drill a hole for dynamic compression, place the universal drill guide eccentrically at the edge of the DCU portion of the LCP plate hole, without applying pressure. Tightening of the cortex screws will result in dynamic compression corresponding to that of the LC-DCP plate. Measure for screw length using the depth gauge and insert the appropriate length cortex or cancellous bone screw. 22 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
25 Insertion of locking screws Instruments for 3.5 mm locking screws mm Drill Bit mm Threaded Drill Guide StarDrive Screwdriver, T15 or StarDrive Screwdriver Shaft, T Depth Gauge, for small screws * Torque Limiting Attachment, 1.5 Nm or * Torque Limiting Attachment, 1.5 Nm, quick coupling Instruments for 5.0 mm locking screws mm Drill Bit mm Threaded Drill Guide StarDrive Screwdriver, T25 or StarDrive Screwdriver Shaft, T Depth Gauge, for large screws * Torque Limiting Attachment, 4 Nm or * Torque Limiting Attachment, 4 Nm, for AO Reaming Coupler Reminder: The locking screw is not a lag screw. Use standard screws when a precise anatomical reduction (e.g., joint surfaces) or interfragmentary compression is required. Before inserting the first locking screw, perform anatomical reduction and fix the fracture with lag screws, if necessary. After the insertion of locking screws, an anatomical reduction will no longer be possible without loosening the locking screw. Screw the threaded drill guide into an LCP plate hole until fully seated. * Also available Synthes 23
26 Screw Insertion 1 Insert screws continued Insertion of locking screws continued Note: Since the direction of a locking screw is determined by plate design, final screw position may be verified with a K-wire prior to insertion. This becomes especially important when the plate has been contoured or applied in metaphyseal regions around joint surfaces (refer to Screw Placement Verification on page 26). Warning: Do not try to bend the plate using the threaded drill guide because damage may occur to the plate hole threads. Use the drill bit to drill the desired depth. Remove the threaded drill guide. Use the depth gauge to determine screw length. 24 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
27 Insert the locking screw under power using a torque limiting attachment and StarDrive screwdriver shaft. Note: Recheck each locking screw before closing to verify that the screws are securely locked to the plate. Screwheads must be flush with the plate in the locked position before they can be considered fully seated. Warning: Always use a torque limiting attachment (TLA) when using power to insert locking screws. Alternative method of locking screw insertion Use the StarDrive screwdriver to manually insert the appropriate length locking screw. Carefully tighten the locking screw, as excessive force is not necessary to produce effective screw-to-plate locking. Synthes 25
28 Screw Placement Verification 2 Verify screw placement Instruments for 3.5 mm locking screws mm Kirschner Wire with Thread mm Wire Sleeve Direct Measuring Device Instruments for 5.0 mm locking screws mm Non-Threaded Guide Wire Direct Measuring Device mm Wire Sleeve Since the direction of a locking screw is determined by plate design, final screw position may be verified with a K-wire before insertion. This becomes especially important when the plate has been contoured or applied in metaphyseal regions around joint surfaces. With the threaded drill guide in place, insert the wire sleeve into the threaded drill guide. Insert a threaded Kirschner wire through the wire sleeve and drill to the desired depth. Verify K-wire placement under image intensification to determine if final screw placement is acceptable. Important: The K-wire position represents the final position of the locking screw. 26 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
29 Measurement may be taken by sliding the tapered end of the direct measuring device over the K-wire down to the wire sleeve. Remove the direct measuring device, K-wire and wire sleeve, leaving the threaded drill guide in place. Use the drill bit to drill the near cortex. Remove the threaded drill guide. Insert the appropriate length locking screw. Synthes 27
30 Implant Removal 1 Unlock and remove screws To remove the plate, unlock all screws from the plate, then remove the screws completely from the bone. This prevents simultaneous rotation of the plate when removing the last locking screw. 2 Insert extraction chisel Instruments Extraction Chisel Shaft Extraction Chisel Tip mm/11 mm Wrench Soft Tissue Retractor, small, extendible Insert the extraction chisel shaft into the tip, by aligning the etched lines. Rotate 90 to lock the extraction chisel into place. Insert the extraction chisel into the handle of the soft tissue retractor, with the large flat surface of the tip facing up. Tighten the clamping sleeve with the 8 mm/11 mm wrench. Place the extraction chisel over the exposed end of the plate and slide it along the entire length of the plate. Important: The chisel tip is sharp. Use extreme caution when using the chisel in areas where it can come into contact with vascular and neurovascular structures. The chisel tip can be used with 3.5 mm narrow and broad and 4.5 mm narrow LCP plates. Remove the chisel and plate. 28 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
31 Screws Used with the 3.5 mm and 4.5 mm Curved Locking Compression Plates 3.5 mm Cortex Screws, self-tapping May be used in the DCU portion of the Combi holes Compress the plate to the bone or create axial compression 3.5 mm Locking Screws, self-tapping Create a locked, fixed-angle screw-plate construct Used in the locking portion of the Combi holes Threaded conical head 4.0 mm Cancellous Bone Screws May be used in the DCU portion of the Combi hole Compress the plate to the bone or create axial compression Fully or partially threaded shaft 4.0 mm Locking Screws, self-tapping** Create a locked, fixed-angle screw-plate construct Used in the locking portion of the Combi holes Threaded conical head 4.5 mm Cortex Screws, self-tapping** May be used in the DCU portion of the Combi holes Compress the plate to the bone or create axial compression 4.5 mm Cannulated Screws** May be used in the DCU portion of the Combi holes Compress the plate to the bone or create axial compression Self-drilling, self-tapping Fully or partially threaded shaft 5.0 mm Locking Screws, self-tapping** Create a locked, fixed-angle screw-plate construct Threaded conical head Note: All screws are available in implant-quality 316L stainless steel. For use with 3.5 mm LCP plates **For use with 4.5 mm LCP plates Synthes 29
32 Screws Used with the 3.5 mm and 4.5 mm Curved Locking Compression Plates continued 5.0 mm Periprosthetic Locking Screws, self tapping** Blunt tip allows unicortical fixation of fractures when an intramedullary implant is present 6.5 mm Cancellous Bone Screws** May be used in the DCU portion of the first and last Combi holes of the 4.5 mm narrow and broad LCP plates Compress the plate to the bone or create axial compression Fully or partially threaded shaft (16 mm, 24 mm and 32 mm thread lengths) Note: All screws are available in implant-quality 316L stainless steel. **For use with 4.5 mm LCP plates Curved LCP Plates Limited-contact plate design Tapered plate ends for submuscular plate insertion 3.5 mm Curved Narrow LCP Plates Available with 10 to 22 Combi holes 3.5 mm Curved Broad LCP Plates Available with 10 to 30 staggered Combi holes 4.5 mm Curved Narrow LCP Plates Available with 10 to 22 Combi holes 4.5 mm Curved Broad LCP Plates* Available with 12 to 26 staggered Combi holes Note: All plates are available in implant-quality 316L stainless steel. *Also available 30 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
33 Instruments Extraction Chisel Shaft Extraction Chisel Tip mm/11 mm Wrench Large Hexagonal Key Soft Tissue Retractor, small, extendible Reduction Handle, toothed, for 3.0 mm Threaded Rod Clamping Foot for the , for 3.5 mm LCP and 3.5 mm LC-DCP Synthes 31
34 Instruments mm Protection Sleeve, Slotted mm/3.0 mm Drill Sleeve Adjusting Nut, for 3.0 mm Threaded Rod mm Threaded Rod, self-drilling tip, 270 mm Small Soft Tissue Retractor Blade, long Reduction Handle, toothed, for 5.0 mm Threaded Rod 32 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
35 Plate Holder, for Minimally Invasive Plating Clamping Foot, for 4.5 mm/5.0 mm Narrow LCP and 4.5 mm Narrow LC-DCP Connecting Screw, for mm Protection Sleeve, slotted mm/5.0 mm Drill Sleeve Synthes 33
36 Instruments Adjusting Nut, for 5.0 mm Threaded Rod mm Threaded Rod, self-drilling tip, 380 mm */ Bending Irons * * Bending Pliers * Plate Bending Press Large Combination Clamp, MR Conditional *Also available 34 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
37 Medium Combination Clamp, MR Safe mm Carbon Fiber Rod, 350 mm mm Carbon Fiber Rod, 240 mm * Torque Limiting Attachment, 1.5 Nm * Torque Limiting Attachment, 4 Nm * Torque Limiting Attachment, 1.5 Nm, Quick coupling * Torque Limiting Attachment, 4 Nm, for AO reaming coupler *Also available Synthes 35
38 3.5 mm/4.5 mm Curved LCP Instrument Set ( ) Graphic Case mm/4.5 mm Curved LCP Instrument Graphic Case Instruments Extraction Chisel Shaft Extraction Chisel Tip mm/11 mm Wrench Large Hexagonal Key Soft Tissue Retractor, small, extendible Reduction Handle, toothed, for 3.0 mm Threaded Rod Clamping Foot for the , for 3.5 mm LCP and 3.5 mm LC-DCP mm Protection Sleeve, Slotted mm/3.0 mm Drill Sleeve Adjusting Nut, for 3.0 mm Threaded Rod mm Threaded Rod, self-drilling tip, 270 mm Small Soft Tissue Retractor Blade, long Reduction Handle, toothed, for 5.0 mm Threaded Rod Plate Holder, for Minimally Invasive Plating Clamping Foot, for 4.5 mm/5.0 mm Narrow LCP and 4.5 mm Narrow LC-DCP Connecting Screw, for mm Protection Sleeve, slotted mm/5.0 mm Drill Sleeve Adjusting Nut, for 5.0 mm Threaded Rod mm Threaded Rod, self-drilling tip, 380 mm Large Combination Clamp, MR Conditional Medium Combination Clamp, MR Safe mm Carbon Fiber Rod, 350 mm mm Carbon Fiber Rod, 240 mm Note: For additional information, please refer to package insert. 36 Synthes 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP) Technique Guide
39 3.5 mm/4.5 mm Curved Narrow LCP Implant Set ( ) Graphic Case mm/4.5 mm Curved LCP Implant Graphic Case Implants 3.5 mm Curved Narrow LCP Plates Holes Holes mm Curved Narrow LCP Plates Holes Holes mm Curved Broad LCP Plates Holes Holes Also available mm Curved Broad LCP Plates, holes S 4.5 mm Curved Broad LCP Plates, S holes / Bending Irons Bending Pliers Plate Bending Press Torque Limiting Attachment, 1.5 Nm Torque Limiting Attachment, 4.0 Nm Torque Limiting Attachment, 1.5 Nm Torque Limiting Attachment, 4.0 Nm Note: For additional information, please refer to package insert. Available nonsterile or sterile-packed. Add S to catalog number for sterile product. Synthes 37
40 Synthes (USA) 1302 Wrights Lane East West Chester, PA Telephone: (610) To order: (800) Fax: (610) Synthes (Canada) Ltd Meadowpine Boulevard Mississauga, Ontario L5N 6P9 Telephone: (905) To order: (800) Fax: (905) Synthes, Inc. or its affiliates. All rights reserved. Combi, DCP, LC-DCP, LCP and Synthes are trademarks of Synthes, Inc. or its affiliates. DS Studio Printed in U.S.A. 6/13 J9037-B
Technique Guide. Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
MINI FRAGMENT SYSTEM. Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW
 MINI FRAGMENT SYSTEM Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW TABLE OF CONTENTS INTRODUCTION Mini Fragment System 2 PRODUCT INFORMATION Plates 4 Screws 6
MINI FRAGMENT SYSTEM Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW TABLE OF CONTENTS INTRODUCTION Mini Fragment System 2 PRODUCT INFORMATION Plates 4 Screws 6
Technique Guide. 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System.
 Technique Guide 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System. Table of Contents Introduction 4.5 mm LCP Proximal Femur Plates 2 AO Principles 4 Indications 5 Surgical
Technique Guide 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System. Table of Contents Introduction 4.5 mm LCP Proximal Femur Plates 2 AO Principles 4 Indications 5 Surgical
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Periarticular Proximal Tibial Locking Plate
 Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
PERIPROSTHETIC IMPLANTS
 PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
Technique Guide. 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system.
 Technique Guide 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm Variable
Technique Guide 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm Variable
Technique Guide. Screw Removal Set. Instruments for removing Synthes screws.
 Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
LCP Compact Foot/Compact Hand.
 LCP Compact Foot/Compact Hand. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Indications 2
LCP Compact Foot/Compact Hand. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Indications 2
Technique Guide. Orthopaedic Cable System. Cerclage solutions for general surgery.
 Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
Zimmer Periarticular Elbow Locking Plate System
 Zimmer Periarticular Elbow Locking Plate System Surgical Technique The Right Solutions for Fractures Around the Elbow Disclaimer This document is intended exclusively for physicians and is not intended
Zimmer Periarticular Elbow Locking Plate System Surgical Technique The Right Solutions for Fractures Around the Elbow Disclaimer This document is intended exclusively for physicians and is not intended
Technique Guide. 2.4 mm LCP Distal Radius System. A comprehensive plating system to address a variety of fracture patterns.
 Technique Guide 2.4 mm LCP Distal Radius System. A comprehensive plating system to address a variety of fracture patterns. Table of Contents Introduction 2.4 mm LCP Distal Radius System 2 AO Principles
Technique Guide 2.4 mm LCP Distal Radius System. A comprehensive plating system to address a variety of fracture patterns. Table of Contents Introduction 2.4 mm LCP Distal Radius System 2 AO Principles
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
LCP Olecranon Plate. The anatomical fixation system with angular stability for olecranon and proximal ulnar fractures.
 LCP Olecranon Plate. The anatomical fixation system with angular stability for olecranon and proximal ulnar fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments
LCP Olecranon Plate. The anatomical fixation system with angular stability for olecranon and proximal ulnar fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments
Technique Guide. DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation.
 Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Aesculap Veterinary Orthopaedics. Targon VET Interlocking Nail
 Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
Modular Sternal Cable System. Flexibility and strength in sternal closure and repair.
 Modular Sternal Cable System. Flexibility and strength in sternal closure and repair. Multiple closure options Stable fixation in all configurations Improved strength and flexibility compared to wire Modular
Modular Sternal Cable System. Flexibility and strength in sternal closure and repair. Multiple closure options Stable fixation in all configurations Improved strength and flexibility compared to wire Modular
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery.
 Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
NCB Periprosthetic Femur Plate System. Surgical Technique
 NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
NCB Proximal Humerus System. Surgical Technique
 NCB Proximal Humerus System Surgical Technique NCB Proximal Humerus System Surgical Technique 3 Surgical Technique NCB Proximal Humerus System Table of Contents Introduction 4 Cable Fixation Options 5
NCB Proximal Humerus System Surgical Technique NCB Proximal Humerus System Surgical Technique 3 Surgical Technique NCB Proximal Humerus System Table of Contents Introduction 4 Cable Fixation Options 5
TwinFix Cannulated Compression Screw
 TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
Technique Guide. Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
 Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Expert LFN. Lateral Femoral Nail.
 Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Technique Guide. Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting.
 Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
V-TEK IVP System 2.7 System 4.0
 V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
Cable System. For Orthopaedic Trauma Surgery.
 Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Titanium Wire with Barb and Needle. For canthal tendon procedures.
 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Surgical technique. End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue.
 Surgical technique End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue. Table of contents Indications and contraindications 3 Implants 4 Instruments 4 Preoperative planning
Surgical technique End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue. Table of contents Indications and contraindications 3 Implants 4 Instruments 4 Preoperative planning
LISS PLT. The less invasive stabilization system for proximal tibia fractures.
 LISS PLT. The less invasive stabilization system for proximal tibia fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the
LISS PLT. The less invasive stabilization system for proximal tibia fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the
Expert TN. Tibial Nail.
 Expert TN. Tibial Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Expert TN. Tibial Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
ACTIV ANKLE DISTAL AND DIAPHYSEAL FIBULA INNOVATION MEANS MOTION
 ACTIV ANKLE DISTAL AND DIAPHYSEAL FIBULA POLYAXIAL LOCKING FIXATION DUALTEC SYSTEM II Precontoured implants Polyaxiality of 20 2 surgical approaches : lateral and posterolateral ACTIV ANKLE The ACTIV ANKLE
ACTIV ANKLE DISTAL AND DIAPHYSEAL FIBULA POLYAXIAL LOCKING FIXATION DUALTEC SYSTEM II Precontoured implants Polyaxiality of 20 2 surgical approaches : lateral and posterolateral ACTIV ANKLE The ACTIV ANKLE
Battery Power Line. Battery-driven power tool system for orthopaedics and traumatology.
 Battery Power Line. Battery-driven power tool system for orthopaedics and traumatology. High performance Excellent torque for drilling and reaming Precise cutting with Synthes saw blades Battery Power
Battery Power Line. Battery-driven power tool system for orthopaedics and traumatology. High performance Excellent torque for drilling and reaming Precise cutting with Synthes saw blades Battery Power
Zimmer Natural Nail System. Cephalomedullary Nail Surgical Technique STANDARD
 Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
VariAx Distal Radius Locking Plate System. Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates
 VariAx Distal Radius Plate System Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates System Module The NEW VariAx Distal Radius Plating System represents the Next Generation of
VariAx Distal Radius Plate System Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates System Module The NEW VariAx Distal Radius Plating System represents the Next Generation of
OptiLock Periarticular Plating System For Proximal Tibial Fractures. Pre-Launch Surgical Technique
 OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
DARCO MRS. Locked Plating System for Reconstructive Rearfoot Surgery
 DARCO MRS Locked Plating System for Reconstructive Rearfoot Surgery DARCO MRS Locked plating system for reconstructive rearfoot surgery System Basics The DARCO MRS plating system for the rearfoot has been
DARCO MRS Locked Plating System for Reconstructive Rearfoot Surgery DARCO MRS Locked plating system for reconstructive rearfoot surgery System Basics The DARCO MRS plating system for the rearfoot has been
Expert ALFN. Adolescent Lateral Femoral Nail.
 Expert ALFN. Adolescent Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Expert ALFN. Adolescent Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
TriLock 1.5 Implants for the Phalanges
 P R O D U C T IN F O RM AT I O N TriLock 1.5 Implants for the Phalanges APTUS Hand 2 TriLock 1.5 Implants for the Phalanges TriLock 1.5 The Smallest Locking System Small, slender, strong Low profile and
P R O D U C T IN F O RM AT I O N TriLock 1.5 Implants for the Phalanges APTUS Hand 2 TriLock 1.5 Implants for the Phalanges TriLock 1.5 The Smallest Locking System Small, slender, strong Low profile and
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
Elbow System 2.0, 2.8
 SurgicAL TecHNiqUE STEP by step Elbow System 2.0, 2.8 APTUS Elbow 2 Elbow System 2.0, 2.8 Elbow System 2.0, 2.8 3 Elbow System 2.0, 2.8 Contents 4-5 Features, Technique 6-13 Introduction and Indications
SurgicAL TecHNiqUE STEP by step Elbow System 2.0, 2.8 APTUS Elbow 2 Elbow System 2.0, 2.8 Elbow System 2.0, 2.8 3 Elbow System 2.0, 2.8 Contents 4-5 Features, Technique 6-13 Introduction and Indications
TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
 TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
ICUC One-Page Paper. Mixing a lag screw with a splinting protection plate Alberto Fernández Dell Oca, Pietro Regazzoni, Stephan Perren May 2016
 Mixing a lag screw with a splinting protection plate Alberto Fernández Dell Oca, Pietro Regazzoni, Stephan Perren May 2016 The 20th century has seen three essential improvements of surgical fracture fixation:
Mixing a lag screw with a splinting protection plate Alberto Fernández Dell Oca, Pietro Regazzoni, Stephan Perren May 2016 The 20th century has seen three essential improvements of surgical fracture fixation:
CLAW II. Polyaxial Compression Plating System SURGIC A L T ECHNIQUE
 CLAW II Polyaxial Compression Plating System SURGIC A L T ECHNIQUE Contents Chapter 1 2 3 3 3 Chapter 2 4 4 7 Chapter 3 8 8 8 8 8 8 8 9 11 11 11 Chapter 4 12 Introduction Intended Use Indications Contraindications
CLAW II Polyaxial Compression Plating System SURGIC A L T ECHNIQUE Contents Chapter 1 2 3 3 3 Chapter 2 4 4 7 Chapter 3 8 8 8 8 8 8 8 9 11 11 11 Chapter 4 12 Introduction Intended Use Indications Contraindications
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Scout Vessel Guard. A cover for vessels during anterior lumbar spine surgery.
 Scout Vessel Guard. A cover for vessels during anterior lumbar spine surgery. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Scout Vessel Guard 2
Scout Vessel Guard. A cover for vessels during anterior lumbar spine surgery. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Scout Vessel Guard 2
PATIENT SPECIFIC PLATES FOR MANDIBLE: CUSTOM MADE PLATES FOR TRAUMA AND RECONSTRUCTION
 PATIENT SPECIFIC PLATES FOR MANDIBLE: CUSTOM MADE PLATES FOR TRAUMA AND RECONSTRUCTION Derived from patient CT Data Customizable design features Strength with low profile This publication is not intended
PATIENT SPECIFIC PLATES FOR MANDIBLE: CUSTOM MADE PLATES FOR TRAUMA AND RECONSTRUCTION Derived from patient CT Data Customizable design features Strength with low profile This publication is not intended
Small Battery Drive. For orthopaedic trauma applications.
 Small Battery Drive. For orthopaedic trauma applications. Ergonomic, lightweight design Compatible with a wide variety of attachments Variable speed trigger with instant reverse and oscillation Small
Small Battery Drive. For orthopaedic trauma applications. Ergonomic, lightweight design Compatible with a wide variety of attachments Variable speed trigger with instant reverse and oscillation Small
TransFx External Fixation System Large and Intermediate Surgical Technique
 TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
SALVATION. Fusion Bolts and Beams SURGICAL TECHNIQUE
 SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
DHS/DCS System. Including LCP DHS and DHS Blade.
 DHS/DCS System. Including LCP DHS and DHS Blade. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of Contents
DHS/DCS System. Including LCP DHS and DHS Blade. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of Contents
Expert HAN. Expert Hindfoot Arthrodesis Nail.
 Expert HAN. Expert Hindfoot Arthrodesis Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Expert HAN. Expert Hindfoot Arthrodesis Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
How To Use A Phoenix Retrograde Femoral Nail
 Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
ZERO-P VA. Variable angle zero-profile anterior cervical interbody fusion (ACIF) device SURGICAL TECHNIQUE
 ZERO-P VA Variable angle zero-profile anterior cervical interbody fusion (ACIF) device SURGICAL TECHNIQUE Table of Contents Introduction Zero-P VA Instruments and Implants 2 AO Principles 4 Indications
ZERO-P VA Variable angle zero-profile anterior cervical interbody fusion (ACIF) device SURGICAL TECHNIQUE Table of Contents Introduction Zero-P VA Instruments and Implants 2 AO Principles 4 Indications
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Posterior Referencing. Surgical Technique
 Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Technique Guide. Norian SRS Fast Set Putty. Calcium phosphate bone void filler.
 Technique Guide Norian SRS Fast Set Putty. Calcium phosphate bone void filler. TableofContents Introduction Norian SRS Fast Set Putty 2 Indications and Contraindications 3 Basic Science 4 Surgical Technique
Technique Guide Norian SRS Fast Set Putty. Calcium phosphate bone void filler. TableofContents Introduction Norian SRS Fast Set Putty 2 Indications and Contraindications 3 Basic Science 4 Surgical Technique
Implant Extraction Guide Module One & Two
 Implant Extraction Set Implant Extraction Guide Module One & Two 1 Contents Page 1. Introduction 3 Introduction 3 Features and Benefits 3 Contraindications 3 2. Product Description 4 3. Technical Details
Implant Extraction Set Implant Extraction Guide Module One & Two 1 Contents Page 1. Introduction 3 Introduction 3 Features and Benefits 3 Contraindications 3 2. Product Description 4 3. Technical Details
MatrixNEURO CMF Matrix
 MatrixNEURO CMF Matrix This publication is not intended for distribution in the USA. MatrixNEURO Introduction The aim of surgical fracture treatment is to reconstruct the bony anatomy and restore its function.
MatrixNEURO CMF Matrix This publication is not intended for distribution in the USA. MatrixNEURO Introduction The aim of surgical fracture treatment is to reconstruct the bony anatomy and restore its function.
Lentur Cable System. Surgical Technique
 Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
INTRODUCTION Cerclage Cable Vs. Monofilament Wire
 B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
ACCORD Cable System. Surgical technique completed in conjunction with: Robert Barrack, MD St. Louis, Missouri. Paul Di Cesare, MD New York, New York
 Surgical Technique Innovations in Hip Surgery 2 ACCORD Cable System Surgical technique completed in conjunction with: Robert Barrack, MD St. Louis, Missouri Paul Di Cesare, MD New York, New York Fares
Surgical Technique Innovations in Hip Surgery 2 ACCORD Cable System Surgical technique completed in conjunction with: Robert Barrack, MD St. Louis, Missouri Paul Di Cesare, MD New York, New York Fares
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning. Orthodontics and Implantology
 ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
PFNA. With Augmentation Option.
 PFNA. With Augmentation Option. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning
PFNA. With Augmentation Option. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
FUSEFORCE. Hand Fixation System SURGIC A L T ECHNIQUE
 FUSEFORCE Hand Fixation System SURGIC A L T ECHNIQUE Contents Chapter 1 3 Chapter 2 4 Appendix A 7 Intended Use Surgical Technique Ordering Information Indication Sizing Reference Proper surgical procedures
FUSEFORCE Hand Fixation System SURGIC A L T ECHNIQUE Contents Chapter 1 3 Chapter 2 4 Appendix A 7 Intended Use Surgical Technique Ordering Information Indication Sizing Reference Proper surgical procedures
TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique. Table of Contents
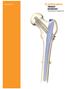 Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
SURGICAL TECHNIQUE STEP BY STEP MDO 2.0. MODUS Mandible
 SURGICAL TECHNIQUE STEP BY STEP MDO 2.0 MODUS Mandible LITERATURE 1) Bayram Mehmed et al. (2007) Mandibular Symphyseal Distraction Osteogenesis Using a Bone-Supported Distractor Angle Orthodontist, Vol.
SURGICAL TECHNIQUE STEP BY STEP MDO 2.0 MODUS Mandible LITERATURE 1) Bayram Mehmed et al. (2007) Mandibular Symphyseal Distraction Osteogenesis Using a Bone-Supported Distractor Angle Orthodontist, Vol.
Step-by-step instructions:
 Spark plug thread repair for Ford Triton cylinder heads Step-by-step instructions: Identification Installation Verification Specifically designed and tested for 4.6L, 5.4L, and 6.8L 2 and 4 valve heads,
Spark plug thread repair for Ford Triton cylinder heads Step-by-step instructions: Identification Installation Verification Specifically designed and tested for 4.6L, 5.4L, and 6.8L 2 and 4 valve heads,
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System
 *smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
*smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
DRAFT. Triathlon TS Knee System. Surgical Protocol. Version 1
 DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
C O N V E Y O R C O M P O N E N T S C H A I N S B E L T S B E A R I N G S
 C O N V E Y O R C O M P O N E N T S C H A I N S B E L T S B E A R I N G S January 2009 Issue 6 Valu Guide Brackets The Ultimate in Adjustability and Cost Savings Valu Guide brackets are part of a family
C O N V E Y O R C O M P O N E N T S C H A I N S B E L T S B E A R I N G S January 2009 Issue 6 Valu Guide Brackets The Ultimate in Adjustability and Cost Savings Valu Guide brackets are part of a family
Trillium 40 Axis Spring Tensioner Wire Replacement Instructions
 Trillium 40 Axis Spring Tensioner Wire Replacement Instructions 1 Overview The objective is to replace the broken axis spring tensioner wire. This requires the following tasks: 1. Remove the seismometer
Trillium 40 Axis Spring Tensioner Wire Replacement Instructions 1 Overview The objective is to replace the broken axis spring tensioner wire. This requires the following tasks: 1. Remove the seismometer
Introduction to JIGS AND FIXTURES
 Introduction to JIGS AND FIXTURES Introduction The successful running of any mass production depends upon the interchangeability to facilitate easy assembly and reduction of unit cost. Mass production
Introduction to JIGS AND FIXTURES Introduction The successful running of any mass production depends upon the interchangeability to facilitate easy assembly and reduction of unit cost. Mass production
Wiper Motor Marinco 2.5. Installation Instructions
 Wiper Motor Marinco 2.5 Installation Instructions Wiper Motor Marinco-2.5 The Marinco 2.5 Wiper Motor Offers the Following Features: Fully sealed base and housing which allows installation in outdoor wet
Wiper Motor Marinco 2.5 Installation Instructions Wiper Motor Marinco-2.5 The Marinco 2.5 Wiper Motor Offers the Following Features: Fully sealed base and housing which allows installation in outdoor wet
MatrixNEURO. The next generation cranial plating system.
 MatrixNEURO. The next generation cranial plating system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table
MatrixNEURO. The next generation cranial plating system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table
Fracture Fixation Devices Compression Hip Screws Cannulated/Bone Screws Bone Plates, Pins, Wires
 Fracture Fixation Devices Compression Hip Screws Cannulated/Bone Screws Bone Plates, Pins, Wires IMPORTANT MEDICAL INFORMATION EN SPECIAL NOTE Fracture fixation devices are used only as an aid to healing;
Fracture Fixation Devices Compression Hip Screws Cannulated/Bone Screws Bone Plates, Pins, Wires IMPORTANT MEDICAL INFORMATION EN SPECIAL NOTE Fracture fixation devices are used only as an aid to healing;
CETAC Z-Drive Assembly
 CETAC Z-Drive Assembly Replacement Guide Manual Part Number 610144 Rev 1, 2012 CETAC Technologies, Printed in USA Overview This guide describes the necessary steps to replace the Z-drive assembly on your
CETAC Z-Drive Assembly Replacement Guide Manual Part Number 610144 Rev 1, 2012 CETAC Technologies, Printed in USA Overview This guide describes the necessary steps to replace the Z-drive assembly on your
Assembly and Usage Instructions
 Assembly and Usage Instructions A Product 5885 West Van Horn Tavern Road Columbia, MO 65203 www.caldwellshooting.com Instruction #1001667 Limited Warranty Every Caldwell product is warrantied to be free
Assembly and Usage Instructions A Product 5885 West Van Horn Tavern Road Columbia, MO 65203 www.caldwellshooting.com Instruction #1001667 Limited Warranty Every Caldwell product is warrantied to be free
Versa-Fx II Femoral Fixation System Surgical Techniques
 Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Elo Touch Solutions Wall-mounting Kit for the 5501L IDS Touchmonitors
 Installation Manual Elo Touch Solutions Wall-mounting Kit for the 5501L IDS Touchmonitors SW602206 Rev B Table of Contents Chapter 1: Safety Warning... 3 Chapter 2: Kit Contents... 4 Included in Kit...
Installation Manual Elo Touch Solutions Wall-mounting Kit for the 5501L IDS Touchmonitors SW602206 Rev B Table of Contents Chapter 1: Safety Warning... 3 Chapter 2: Kit Contents... 4 Included in Kit...
LK Wallbox UNI Push. Assembly. Only intended for LK PE-X Universal Pipe X.
 LK Wallbox UNI Push Only intended for LK PE-X Universal Pipe X. LK Wallbox UNI Push 16 Single Article no. 188 06 38 LK Wallbox UNI Push 20 Single Article no. 188 06 39 LK Distance template LK Wallbox UNI
LK Wallbox UNI Push Only intended for LK PE-X Universal Pipe X. LK Wallbox UNI Push 16 Single Article no. 188 06 38 LK Wallbox UNI Push 20 Single Article no. 188 06 39 LK Distance template LK Wallbox UNI
FRONT BUMPER INSTALLATION INSTRUCTIONS 2007-2011 DODGE / MERCEDES SPRINTER
 Aluminess Products Inc 9402 Wheatlands Ct. #A Santee, CA 92071 619-449-9930 FRONT BUMPER INSTALLATION INSTRUCTIONS 2007-2011 DODGE / MERCEDES SPRINTER Please read before beginning Stainless steel hardware
Aluminess Products Inc 9402 Wheatlands Ct. #A Santee, CA 92071 619-449-9930 FRONT BUMPER INSTALLATION INSTRUCTIONS 2007-2011 DODGE / MERCEDES SPRINTER Please read before beginning Stainless steel hardware
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TomoFix Medial High Tibial Plate (MHT). For Medial High Tibial Osteotomies.
 TomoFix Medial High Tibial Plate (MHT). For Medial High Tibial Osteotomies. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO
TomoFix Medial High Tibial Plate (MHT). For Medial High Tibial Osteotomies. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO
Guidance for implant removal. Straumann Dental Implant System
 Guidance for implant removal Straumann Dental Implant System The ITI (International Team for Implantology) is academic partner of Institut Straumann AG in the areas of research and education. ContentS
Guidance for implant removal Straumann Dental Implant System The ITI (International Team for Implantology) is academic partner of Institut Straumann AG in the areas of research and education. ContentS
Cable Drum Installation
 20 Cable Drum Installation COUNTERBALANCE None Shake the TorqueMaster spring tube gently to extend the winding shafts out about 5" on each side. For single spring applications, there will be no left hand
20 Cable Drum Installation COUNTERBALANCE None Shake the TorqueMaster spring tube gently to extend the winding shafts out about 5" on each side. For single spring applications, there will be no left hand
Two most common lock nut groups: 1-Prevailing Torque Type Lock Nuts:
 Two most common lock nut groups: 1. PREVAILING TORQUE a design feature of the lock nut produces friction between threads of mated components thereby increasing the force needed to tighten as well as loosen
Two most common lock nut groups: 1. PREVAILING TORQUE a design feature of the lock nut produces friction between threads of mated components thereby increasing the force needed to tighten as well as loosen
Rebuild Instructions for 70001 and 70010 Transmission
 Rebuild Instructions for 70001 and 70010 Transmission Brinn, Incorporated 1615 Tech Drive Bay City, MI 48706 Telephone 989.686.8920 Fax 989.686.6520 www.brinninc.com Notice Read all instructions before
Rebuild Instructions for 70001 and 70010 Transmission Brinn, Incorporated 1615 Tech Drive Bay City, MI 48706 Telephone 989.686.8920 Fax 989.686.6520 www.brinninc.com Notice Read all instructions before
Foot Surgery Innovation in Forefoot Reconstruction BAROUK SCREW FRS SCREW TWISTOFF SCREW MEMORY STAPLE VARISATION STAPLE
 Foot Surgery Innovation in Forefoot Reconstruction BAROUK SCREW FRS SCREW TWISTOFF SCREW MEMORY STAPLE VARISATION STAPLE 3 Contents BAROUK Screw 2 FRS Screw 3 TWISTOFF Screw 4 MEMORY 12 and 20 Staples
Foot Surgery Innovation in Forefoot Reconstruction BAROUK SCREW FRS SCREW TWISTOFF SCREW MEMORY STAPLE VARISATION STAPLE 3 Contents BAROUK Screw 2 FRS Screw 3 TWISTOFF Screw 4 MEMORY 12 and 20 Staples
TABLE OF CONTENTS. Indications and Contraindications 3. Features and Benefits 4. Ease of connection 4 Stable fixation concept 5
 Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
TRIGEN TAN and FAN Intramedullary Nails
 Surgical Technique TRIGEN TAN and FAN Intramedullary Nails Surgical Technique Table of Contents Indications...2 TRIGEN TAN and FAN Case Examples...3 Design Features: TAN...4 Implant Specifications: TAN...5
Surgical Technique TRIGEN TAN and FAN Intramedullary Nails Surgical Technique Table of Contents Indications...2 TRIGEN TAN and FAN Case Examples...3 Design Features: TAN...4 Implant Specifications: TAN...5
STEADYfast Stabilizer Installation Notes Fifth Wheel and Travel Trailers 11/23/13
 STEADYfast Stabilizer Installation Notes Fifth Wheel and Travel Trailers 11/23/13 (See Supplemental Instructions for trailers with heavy duty round footplates and/or Power Leveling Systems) PHONE SUPPORT
STEADYfast Stabilizer Installation Notes Fifth Wheel and Travel Trailers 11/23/13 (See Supplemental Instructions for trailers with heavy duty round footplates and/or Power Leveling Systems) PHONE SUPPORT
Fixing Dental Implant Component Failure and Fracture: Retrieving the Fractured Implant Abutment Screw. Charles A. Mastrovich, DDS
 Fixing Dental Implant Component Failure and Fracture: Retrieving the Fractured Implant Abutment Screw Charles A. Mastrovich, DDS [email protected] www.mastrovichdental.com Evaluating component failure
Fixing Dental Implant Component Failure and Fracture: Retrieving the Fractured Implant Abutment Screw Charles A. Mastrovich, DDS [email protected] www.mastrovichdental.com Evaluating component failure
INSTRUCTION. Industrial Sewing Machines. No. 010012. First published : June 1997 Second edition : March 2001
 INSTRUCTION Industrial Sewing Machines First published : June 1997 Second edition : March 2001 No. 010012 INTRODUCTION Thank you for your purchasing Kansai Special's DLR Series. Read and study this instruction
INSTRUCTION Industrial Sewing Machines First published : June 1997 Second edition : March 2001 No. 010012 INTRODUCTION Thank you for your purchasing Kansai Special's DLR Series. Read and study this instruction
Depending on which elastic support you have you can secure the V2 power unit to the following seat bracket tubes: EXTERNAL DIAMETER 27.
 ASSEMBLY 1 - EPS V2 POWER UNIT (SOLUTION 5) 1.1 - POSITIONING INSIDE THE SEAT TUBE WITH ELASTIC SUPPORT IN THE SEAT BRACKET TUBE Depending on which elastic support you have you can secure the V2 power
ASSEMBLY 1 - EPS V2 POWER UNIT (SOLUTION 5) 1.1 - POSITIONING INSIDE THE SEAT TUBE WITH ELASTIC SUPPORT IN THE SEAT BRACKET TUBE Depending on which elastic support you have you can secure the V2 power
