A Three-Way Comparison of Tuberculin Skin Testing, QuantiFERON-TB Gold and T-SPOT.TB in Children
|
|
|
- Elizabeth Ball
- 8 years ago
- Views:
Transcription
1 A Three-Way Comparison of Tuberculin Skin Testing, QuantiFERON-TB Gold and T-SPOT.TB in Children Tom G. Connell 1,2,3., Nicole Ritz 1,2,3., Georgia A. Paxton 4, Jim P. Buttery 1,2,3, Nigel Curtis 1,2,3 *, Sarath C. Ranganathan 1,2,5 1 Department of Paediatrics, University of Melbourne, Royal Children s Hospital Melbourne, Parkville, Victoria, Australia, 2 Murdoch Children s Research Institute, Royal Children s Hospital Melbourne, Parkville, Victoria, Australia, 3 Infectious Diseases Unit, Department of General Medicine, Royal Children s Hospital Melbourne, Parkville, Victoria, Australia, 4 Immigrant Health Service, Department of General Medicine, Royal Children s Hospital Melbourne, Parkville, Victoria, Australia, 5 Department of Thoracic Medicine Royal Children s Hospital Melbourne, Parkville, Victoria, Australia Abstract Background: There are limited data comparing the performance of the two commercially available interferon gamma (IFNc) release assays (IGRAs) for the diagnosis of tuberculosis (TB) in children. We compared QuantiFERON-TB gold In Tube (QFT- IT), T-SPOT.TB and the tuberculin skin test (TST) in children at risk for latent TB infection or TB disease. Methods and Findings: The results of both IGRAs were compared with diagnosis assigned by TST-based criteria and assessed in relation to TB contact history. Results from the TST and at least one assay were available for 96 of 100 children. Agreement between QFT-IT and T-SPOT.TB was high (93% agreement, k = 0.83). QFT-IT and T-SPOT.TB tests were positive in 8 (89%) and 9 (100%) children with suspected active TB disease. There was moderate agreement between TST and either QFT-IT (75%, k = 0.50) or T-SPOT.TB (75%, k = 0.51). Among 38 children with TST-defined latent TB infection, QFT-IT gold and T-SPOT.TB assays were positive in 47% and 39% respectively. Three TST-negative children were positive by at least one IGRA. Children with a TB contact were more likely than children without a TB contact to have a positive IGRA (QFT-IT LR 3.9; T-SPOT.TB LR 3.9) and a positive TST (LR 1.4). Multivariate linear regression analysis showed that the magnitude of both TST induration and IGRA IFN-c responses was significantly influenced by TB contact history, but only the TST was influenced by age. Conclusions: Although a high level of agreement between the IGRAs was observed, they are commonly discordant with the TST. The correct interpretation of a negative assay in a child with a positive skin test in clinical practice remains challenging and highlights the need for longitudinal studies to determine the negative predictive value of IGRAs. Citation: Connell TG, Ritz N, Paxton GA, Buttery JB, Curtis N, et al. (2008) A Three-Way Comparison of Tuberculin Skin Testing, QuantiFERON-TB Gold and T- SPOT.TB in Children. PLoS ONE 3(7): e2624. doi: /journal.pone Editor: Keertan Dheda, University College London, United Kingdom Received April 4, 2008; Accepted June 6, 2008; Published July 9, 2008 Copyright: ß 2008 Connell et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Funding: This project was supported by a grant from the John Burge Trust Victoria. Tom G Connell is supported by fellowship awards from the European Society of Paediatric Infectious Diseases and the Nossal. Institute of Global Health. Nicole Ritz is supported by fellowship awards from the Swiss National Science Foundation and the European Society of Paediatric Infectious Diseases. Funding bodies had no role in data analysis or in the preparation of the manuscript. Competing Interests: The authors have declared that no competing interests exist. * nigel.curtis@rch.org.au. These authors contributed equally to this work. Introduction The detection and treatment of latent tuberculosis (TB) infection is a key strategy in the control of TB [1,2]. Improved methods for detecting both latent TB infection and TB disease in children are needed. Interferon gamma release assays (IGRAs) incorporating Mycobacterium tuberculosis (MTB)-specific antigens have emerged as potential replacements for the century old tuberculin skin test (TST) [3]. IGRAs have been shown to have high sensitivity and specificity in adults [4] but there are few studies that have assessed their performance for the diagnosis of latent TB infection or TB disease specifically in children [5]. A recent meta-analysis highlighted an urgent need for more evidence for the use of IGRAs for the diagnosis of latent TB infection in children [6]. The aim of this study was to compare the performance of two commercial IGRAs with TST in the diagnosis of children at risk for latent TB infection or with suspected active TB disease at a tertiary paediatric hospital. Methods Patients and inclusion criteria The study was approved by the Human Research and Ethics Committee of the Royal Children s Hospital Melbourne. Patients were recruited prospectively from the hospital s TB, refugee health and infectious diseases clinics. Children at risk of latent TB infection or with suspected active TB disease were eligible for inclusion. At risk was defined as a recent TB contact and/or recent immigration from a country with a high prevalence of TB. Written informed consent was obtained from parents or participants in their preferred language. Demographic and clinical details were obtained from each patient by a detailed questionnaire, including: country and date of birth; TB exposure history; Bacille Calmette-Guérin (BCG) vaccination history; presence of BCG scar and symptoms suggestive of TB. All patients had a full clinical evaluation, a TST and blood tests including IGRA, full blood count and CD4 lymphocyte count. HIV tests were not done as part of this study. PLoS ONE 1 July 2008 Volume 3 Issue 7 e2624
2 Tuberculin skin test A Mantoux test was performed by intradermal injection of 10 international units tuberculin (Purified Protein Derivative (PPD) 100 IU/mL, CSL, Melbourne, Australia), the standard dose of tuberculin PPD used in Australia at the time of the study, by trained personnel and read after 48 to 72 hours. An assessment of the level of risk for TB infection was taken into consideration when defining the result of the TST, as recommended by recently modified local guidelines (Victorian Department of Human Services). A positive TST was defined as $10 mm in patients with moderate risk factors (origin from high prevalence country; age 1 to 5 years); and $5 mm in patients with high risk factors (household TB contact; age less than 1 year). If BCG was given within five years prior to the TST, the TST was considered positive if induration was $15 mm in moderate risk patients and $10 mm in high risk patients. In children with suspected active TB disease, TST induration $5 mm was considered positive. Victorian guidelines for TST interpretation are similar to those of the American Thoracic Society (ATS), except that the potential influence of prior BCG is taken into consideration. Chest radiography was undertaken in those with a positive TST or when clinically indicated, and reported by radiologists who were blinded to the results of the IGRAs for each patient. Children deemed to have latent TB infection were offered isoniazid preventive treatment. Interferon gamma release assays A whole blood assay, QuantiFERON-TB gold In-Tube (QFT- IT), Cellestis Ltd, Australia and an enzyme-linked immunospot assay (ELISPOT), T-SPOT.TB, Oxford Immunotec, Oxford, UK were carried out according to the manufacturers guidelines and defined as positive, negative or indeterminate based on manufacturers recommended criteria. The laboratory scientists undertaking the IGRAs were blinded to the clinical status of the patients. The QFT-IT (3 rd generation) assay incorporates an additional MTB-specific antigen TB 7.7 in addition to ESAT-6 and CFP-10. This assay was undertaken at the Victorian Infectious Disease Reference Laboratory Melbourne (VIDRL). The T-SPOT.TB test was undertaken in the Microbiology Research Laboratory at the Royal Children s Hospital Melbourne. Spots were counted with a magnifying glass and expressed as spots per million peripheral blood mononuclear cells (PBMC). Two further independent observers, also blinded to clinical status allocation, confirmed spot counts and assigned results. Definitions Latent TB infection was defined as an asymptomatic child with a positive TST and chest radiograph not suggestive of TB. Active TB disease was defined as a child with a positive TST with symptoms suggestive of TB and/or an abnormal chest radiograph consistent with TB, or a child with MTB cultured from clinical specimens. Symptoms considered suggestive of TB included the following: cough for more than two weeks, persistent fever, night sweats and weight loss. Uninfected was defined as a well child with a negative TST or a child with symptoms potentially suggestive of TB but in whom results of all investigations for TB were negative or a child with an alternative diagnosis and complete recovery in the absence of specific TB treatment. Statistics Data were analysed using Prism Graphpad (Version 5). Nonparametric unpaired data (TST indurations) were analysed by the Mann-Whitney U test. The mean age of children was compared using an unpaired t test or one-way anova. A Fisher s exact or chi-square test was used to compare proportions when the results of IGRAs were analysed as dichomatous outcomes, and an unpaired t test was used when IGRA antigen responses were analysed as continuous measures. Agreement between TST and IGRAs was assessed by the kappa statistic [7]. A multivariate linear regression model was used to determine the influence of age, BCG scar, origin from country with high TB prevalence and TB contact on the results of TST and IGRAs. Correlations were assessed using the Spearman s correlation coefficient. Results Clinical and demographic details are shown in Table 1. Of 101 children enrolled in the study, four (4%) failed to return for a TST Table 1. Demographic, clinical and laboratory details of study participants. Latent TB TB disease Uninfected (n = 38) (n = 9) (n = 49) Demographic Mean age in years (range) 10.2 ( ) 8.2 ( ) 8.4 ( ) Male 17 (45%) 5 (55%) 28 (57%) Born in high TB prevalence area 30 (79%) 8 (89%) 43 (88%) TB contact Household 16 (42%) 8 (89%) 10 (20%) Non-household 6 (16%) 1 (11%) 1 (2%) No known contact 16 (42%) 0 38 (78%) Clinical TB symptoms 1 (3%) * 6 (67%) 3 (6%) BCG Scar present 23 (61%) 1 (11%) 21 (43%) History but no scar 2 (5%) 1 (11%) 2 (4%) No evidence of prior BCG 13 (34%) 7 (78%) 20 (41%) Presence/absence of scar 6 (12%) not recorded Tuberculin skin test { 0 4 mm (82%) 5 9 mm 3 (8%) 1 (11%) 8 (16%) mm 12 (32%) 0 1 (2%) $15 mm 23 (60%) 7 (78%) 0 Induration median (range) 15 (8 37) 21 (6 24) 0 (0 10) Chest radiograph Normal 35 (92%) 1 (11%) { 19 (39%) Abnormal 2 (5%) 1 8 (89%) 1 (2%) Not done/unavailable 1 (3%) ** 0 29 (59%) Laboratory CD4 median (IQR) {{ 40% (38 52%) 43% (30 56%) 40% (35 52%) * Final diagnosis Klebsiella pneumoniae pneumonia; cough.2 weeks; sputum samples AFB negative. { One child with TB disease did not have a TST. { Extrapulmonary TB. 1 One child with evidence of prior TB; one child with right upper lobe opacification (K. pneumoniae on culture). Right upper lobe opacification (culture negative). ** Well, asymptomatic child; failed to attend for follow up CXR. {{ CD4 count available for 82 children. doi: /journal.pone t001 PLoS ONE 2 July 2008 Volume 3 Issue 7 e2624
3 Table 2. Results of QuantiFERON-TB gold in-tube and T-SPOT.TB assays in each diagnostic category. QuantiFERON-TB gold In-Tube T-SPOT.TB Positive Negative Indeterminate Positive Negative Indeterminate All patients (n = 100) Latent TB (n = 38) 18 (47%) 20 (53%) (0) 15 (39%) 19 (50%) 4 (10%) * TB disease (n = 9) 8 (89%) 1 (11%) 0 9 (100%) 0 0 Uninfected (n = 49) 2 (4%) 44 (90%) 3 (6%) { 1 (2%) 38 (78%) 10 (20%) { No TST result (n = 4) 1 (25%) 3 (75%) (100%) 0 Patients with TB contact (n = 44) Latent TB (n = 22) 13 (59%) 9 (41%) 0 10 (46%) 10 (46%) 2 (9%) 1 TB disease (n = 9) 8 (89%) 1 (11%) 0 9 (100%) 0 0 Uninfected (n = 11) 1 (9%) 8 (73%) 2 (18%) 1 (9%) 5 (45%) 5 (45%) ** No TST result (n = 2) 1 (50%) 1 (50%) (100%) 0 * 3 inadequate PBMC; 1 cross contamination. { 1 high nil control; 2 inadequate mitogen control. { 3 high nil control; 4 inadequate PBMC; 2 technical; 1 cross contamination. 1 1 inadequate PBMC; 1 cross contamination. 1 inadequate mitogen control; 1 high nil control. ** 3 inadequate PBMC; 1 technical; 1 high nil control. doi: /journal.pone t002 reading and could not be categorised according to the study criteria. Mycobacterium gordanae was cultured from the sputum of one child, who was subsequently excluded from further analysis. Of the remaining 96 children, 82 (85%) originated from a high TB prevalence country. On the basis of pre-defined criteria for categorising patients to diagnostic groups, 38 (40%) children had latent TB infection, 9 (9%) TB disease and 49 (51%) were uninfected. The mean age of the children in the three groups was not significantly different (p = 0.19). No child had a clinical presentation consistent with HIV infection and all children had a CD4% within the normal range for age. The agreement between observers for the T-SPOT.TB assay results was high (interobserver reliability 96%). In four tests there was a discrepancy in assigning a result (one observer positive, two observers negative in each instance) with all four finally deemed negative by consensus. Although there were more indeterminate results with the T-SPOT.TB assay than with the QFT-IT assay overall (14/96 vs. 3/96, p = 0.009), the majority of indeterminate results for the T-SPOT.TB assay were attributable to potential laboratory error (Tables 2 and 3). Specifically, of the 14 indeterminate T-SPOT.TB assays, inadequate PBMC separation accounted for seven and cross-contamination occurred in two assays. Excluding these nine assays, the difference in the proportion of true indeterminate results between the two assays was not statistically significant (3/96 vs. 5/87, p = 0.48). The proportion of indeterminate results for both IGRA was higher in children younger than three years of age compared to those older than three years of age. Specifically, of 16 children younger than three years of age, two (12.5%) had an indeterminate QFT-IT assay result (one inadequate mitogen control, one high nil control) compared to one (1.1%) indeterminate result (inadequate mitogen control) in the 84 children older than three years of age (p = 0.06). Similarly, of the 16 children younger than three years of age, five (31.3%) had an indeterminate T.SPOT.TB assay result (four inadequate PBMC, one technical) compared to nine (10.7%) indeterminate results (three high nil control, two inadequate PBMC, two technical, two cross contamination) in the 84 children older than three years of age (p = 0.05). When the assays both yielded interpretable (ie non-indeterminate) results, the overall agreement between QFT-IT and T-SPOT.TB was high (93% agreement, k = 0.83, 95% CI ). However, the results between the two IGRAs were discordant in six children (Table 3). Results were QFT-IT positive / T-SPOT.TB negative in four children (two with household TB contact and positive TST of Table 3. Comparison of the results of QuantiFERON-TB gold in-tube and T-SPOT.TB assays. QuantiFERON-TB gold In-Tube Positive Negative Indeterminate T-SPOT.TB All patients (n = 100)* Positive 22 (22%) 2 (2%) 1 (1%) Negative 4 (4%)* 56 (55%)* 1 (1%) Indeterminate 3 (3%) 10 (10%) 1 (1%) Patients with latent TB infection (n = 38) Positive 14 (37%) 1 (3%) 0 Negative 2 (5%) 17 (45%) 0 Indeterminate 2 (5%) 2 (5%) 0 * Includes children where TST result was unavailable. k (95% CI) for agreement between T-SPOT.TB and QuantiFERON-TB gold In-Tube in all patients was 0.83 ( ) and in patients with latent TB infection was 0.82 ( ). doi: /journal.pone t003 PLoS ONE 3 July 2008 Volume 3 Issue 7 e2624
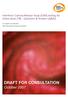
4 Figure 1. Venn diagram depicting agreement between tuberculin skin test, QuantiFERON-TB gold In Tube and T-SPOT.TB results for all children (n = 100). doi: /journal.pone g mm and 12 mm respectively, categorised as latent TB infection; one uninfected; one with a household TB contact in whom a TST result was unavailable). Results were QFT-IT negative / T- SPOT.TB positive in two children (one with household TB contact and a positive TST of 25 mm, categorised as latent TB infection; one with TB disease and a positive TST (22 mm)). There was only moderate agreement between TST and QFT- IT (75%, k = 0.50, 95% CI ) and between TST and T- SPOT.TB (75%, k = 0.51, 95% CI ) overall (Figure 1). The QFT-IT assay was positive in 18 (47%) and the T-SPOT.TB assay was positive in 15 (39%) of the 38 children with TST-defined latent TB infection (Table 2). Combining results from both IGRAs detected only one additional patient with TST-defined latent TB infection compared to QFT-IT alone, increasing the detection rate to 19/38 (50%). The results of both IGRAs were negative in 17 (45%) of the 38 children with TST-defined latent TB infection. Seven of these children had a TST induration $15 mm and eight had a TB contact (Table 4). Three (6.1%) of the 49 children with a negative TST categorised as uninfected by study criteria were positive by at least one IGRA. These comprised a 9-year old (QFT-IT positive / T-SPOT.TB indeterminate (high nil control)) with no prior BCG immunisation, who was a household TB contact; a BCG-immunised 15-year old (QFT-IT positive / T-SPOT.TB negative) from a high TB prevalence country with no known TB contact; and a 2-year old (QFT-IT indeterminate / T-SPOT.TB positive) with no prior BCG immunisation, who was a household TB contact. Of the children with TB disease, results of the QFT-IT and T-SPOT.TB tests were positive in 8 (89%) and 9 (100%) children respectively. The responses to the MTB-specific antigens for both IGRAs are shown in Figure 2. In the T-SPOT.TB assay, the mean (SEM) IFN-c response to ESAT-6 and CFP-10 was higher in children with TB disease compared to those with latent TB infection (ESAT (125.7) vs (51.1) spot forming cells per million PBMC (SFC/ 10 6 ), p = 0.07; CFP (146.2) vs (35.6) SFC/10 6, p = 0.007). Similarly the IFN-c response to ESAT-6 and CFP-10 was higher in children with latent TB infection compared to uninfected children (ESAT (51.1) vs (10.4) SFCs/10 6, p = 0.001; CFP (35.6) vs (5.6) SFCs/10 6,p=0.0004).Inthe QFT-IT assay mean (SEM) IFN-c responses to ESAT-6, CFP-10 and TB 7.7 were also significantly higher in children with TB disease compared to those with latent TB infection (12.44 (1.9) vs (1.06) IU/ml, p = 0.002). Similarly, children with latent TB infection had significantly higher mean IFN-c responses than uninfected children (4.65 (1.06) vs (0.03) IU/ml, p,0.0001). The influence of age, BCG scar, origin from country with high TB prevalence and TB contact on the results of TST and IGRAs was assessed. There was no significant difference in the median TST induration between BCG-immunised and BCG-non-immunised children overall or within the subgroup of children with latent TB infection (all children with TST.0 mm (n = 55): 13 mm vs. 17 mm; p = 0.25; children with latent TB infection (n = 38): 15 mm vs. 17 mm; p = 0.47). Among the 87 children with latent TB infection or who were uninfected, the mean age of those with a positive or negative QFT-IT (10.3 vs 9.2 years, p = 0.4) or T-SPOT.TB (10.3 vs 9.5 years, p = 0.54) assay was similar. Children with a TB contact were more likely than those without a TB contact to have a positive TST, a positive QFT-IT and a positive T-SPOT.TB (Table 5). In a multivariate linear regression analysis, age (p = 0.03) and TB contact (p,0.0001), but not BCG scar (p = 0.86) or origin from a country with high TB prevalence (p = 0.30), were significantly correlated with the magnitude of TST induration. In contrast, the only factor that significantly influenced the magnitude of the IFN-c response in the IGRAs was TB contact (QFT-IT and T.SPOT.TB, p,0.0001). The proportion of children with a TB contact who had a positive TST (at both a 5 mm and a 10 mm cut-off) was higher than the proportion with a Table 4. Details of the results from children with latent TB infection and negative QuantiFERON-TB gold in tube or T.SPOT.TB results. IGRA result TST induration (mm) $5 to9 $10 to 14 $15 QFT-IT T-SPOT.TB No. of children (No. non BCG immunised) All patients with latent TB infection (n = 22) Negative (1 positive) 3 (2) 7 (2) 10 (3) (2 positive) Negative 3 (2) 9 (2) 7 (3) Both negative 3 (2) 7 (2) 7 (3) Either negative 3 (2) 9 (2) 10 (3) Patients with latent TB infection and TB contact (n = 11) Both negative 3 (2) 2 (2) 3 (1) Either negative 3 (2) 4 (2) 4 (1) doi: /journal.pone t004 PLoS ONE 4 July 2008 Volume 3 Issue 7 e2624
5 Figure 2. Results of T-SPOT.TB (panels A and B) and QuantiFERON-TB gold In Tube assays (panel C) according to tuberculin skin test-based diagnosis. The dotted line depicts the test cut-off value for a positive test. doi: /journal.pone g002 positive IGRA indicating a higher sensitivity for the TST in this setting (Table 5). In contrast, the IGRAs appeared to be more specific (with respect to TB contact) than the TST. Discussion This is the largest study to date to compare the two currently available commercial IGRAs with TST for the diagnosis of latent TB infection specifically in children. The level of agreement between QFT-IT and T-SPOT.TB in our study (k = 0.83) was higher than that observed in the studies by Arend et al (k = 0.59) [8] and Leyten et al [9] (k = 0.71). The infrequent occurrence of discordant results between the IGRAs suggests that either assay can be used depending on resources and availability. However, there was significant discordance between the results of TST and both IGRAs. This is important because IGRAs are increasingly considered potential replacements for TST for the detection of latent TB infection [10,11]. Specifically, of 38 children with TSTdefined latent TB infection, less than half had a positive QFT-IT or T-SPOT.TB. A critical question, with important implications for the future use and interpretation of IGRAs, is whether this is the result of false positive TST or false negative IGRA results [12]. Several studies have questioned the sensitivity of IGRAs [8,13,14,15,16,17,18,19,20]. We previously found poor agreement between QFT-TB Gold (an earlier 2 nd generation QuantiFERON assay) and TST (k = 0.3) for the diagnosis of latent TB infection [14]. In our previous study, a high proportion of children with a household TB contact positive by TST were negative by QFT-TB Gold and the assay was negative in almost half of the children with a TST.15 mm. Compared with our previous study, we found better agreement between TST and both QFT-IT and T-SPOT.TB although it is not clear whether this is clinically significant. For the QFT-IT assay, better agreement may be explained by the incorporation of an additional MTB-specific antigen (TB 7.7) conferring increased sensitivity [18]. However, the sensitivity of IGRAsforthedetectionoflatentTBinfectioninchildrenremains questionable with our finding that in children with TST indurations $15 mm who had latent TB infection, only 13/23 (57%) QFT-IT Table 5. The influence of TB contact on TST, QFT-IT and T-SPOT.TB results for the 87 children with latent TB infection (n = 38) or who were uninfected (n = 49). TB contact Proportion positive with TB contact Proportion negative without TB contact LR (95% CI) Yes No TST (cut off $5 mm) Pos /33 (67%) 29/54 (54%) 1.4 ( ) Neg TST (cut off $10 mm) Pos /33 (58%) 37/54 (68%) 1.8 ( ) Neg TST (cut off $15 mm Pos /33 (39%) 44/54 (81%) 2.1 ( ) Neg QFT-IT Pos /31 (45%) 47/53 (89%) 3.9 ( ) Neg T-SPOT.TB Pos /26 (42%) 42/47 (89%) 3.9 ( ) Neg doi: /journal.pone t005 PLoS ONE 5 July 2008 Volume 3 Issue 7 e2624
6 Figure 3. Relationship between results of QuantiFERON-TB gold In Tube and T-SPOT.TB assays and TST induration diameter in the 46 children with a positive tuberculin skin test (38 with TST-defined latent TB infection and 8 with TB disease). The broken line indicates a TST induration of 15 mm. QFT = QuantiFERON-TB gold In Tube, T-Sp = T-SPOT.TB assays, Indet = Indeterminate, TST = tuberculin skin test. doi: /journal.pone g003 assays and 12/19 (63%) T-SPOT.TB assays were positive (Figure 3). Furthermore, in the 22 children with TST-defined latent TB infection with either a negative QFT-IT or a negative T-SPOT.TB result, almost a third had a TB contact and almost half had a TST $15 mm and, importantly, discordant results occurred even in the absence of BCG vaccination. Of note, there were three children (including one without prior BCG vaccination) with a TB contact and TST $15 mm in whom the results of both IGRAs were negative. Our results are consistent with a recent large TB contact investigation in non-bcg vaccinated adults in which the QFT-IT and T-SPOT.TB assays were positive in only 42% and 51% respectively of those with a TST induration $15 mm [8]. Similarly, in another recent study, less than half of immigrants with a TST induration $15 mm were positive by QFT-TB Gold and the overall agreement between TST and QFT-TB Gold was poor (k = 0.37) [21]. Another study in adults showed poor agreement between QFT-IT, an ELISPOT assay and a 6 day lymphocyte-stimulation assay [9]. Of 27 TST positive adults (mean induration 16 mm), 9 (33%) and 11 (46%) individuals tested positive by QFT-IT and ELISPOT respectively. One explanation for these results as well as the findings in our study is that discordant results are due to superior sensitivity of TST for the detection of latent TB infection revealing false negative IGRA. However, the finding of three children in our study (two with a household TB contact) with a negative TST and at least one positive IGRA appears to be inconsistent with this explanation. The alternate explanation for discordant TST and IGRA results is that IGRA have superior specificity and reveal false positive TST results [22,23,24]. The lack of a gold standard for latent TB infection is a recognised inherent limitation of all studies that investigate the use of IGRAs for the detection of latent TB infection. Therefore estimating the sensitivity of any new test for latent TB infection is problematic. In the absence of a recognised gold standard, analysis of results with respect to TB contact history is one way to infer potential superiority of one test over another for the detection of latent TB infection. Although it is recognised that not all individuals exposed to a smear positive TB contact will subsequently become infected, this has become an accepted gold standard on which to base comparative evaluations. Our finding that IGRAs have higher specificity than TST at any cut off with respect to TB contact history is consistent with the possibility that IGRAs have superior specificity for the detection of children with true latent TB infection. There are at least four further potential explanations for discordance between TST and IGRAs results. Firstly, in contrast to the TST which remains positive for a protracted period after past or cleared MTB infection [8,25] recent evidence suggests that QFT- IT and T-SPOT.TB assays detect more recent or ongoing infection [26,27]. This may be because the IGRAs predominantly detect effector MTB-specific T cells in an overnight stimulation assay whereas TST induration is measured at hours allowing for the expansion of memory T cell populations [8,13]. Interestingly a 6- day lymphocyte-stimulation test correlated better with TST than overnight IGRA in one study [9]. Secondly, IGRAs may revert to negative following clearance of TB infection [28]. Thirdly, prior sensitisation by non-tuberculosis mycobacteria, which is common in high TB prevalence countries, could lead to false positive TST results in some patients. In a recent study, 24% of children with nontuberculosis mycobacteria had TST indurations.15 mm [29] and TST indurations.20 mm have been reported in this setting [30]. Lastly, the dose of the tuberculin PPD used in skin test reagents worldwide is not standardised. Though unlikely, the standard use of 10 IU of tuberculin PPD in Australia at the time of the study potentially resulted in more false positive TST results. The correct interpretation of a negative IGRA in a patient with a positive TST in routine clinical practice is challenging, particularly if the patient has a documented TB contact. In the absence of definitive evidence to confirm that discordant results are attributable to false positive TST results, our current practice is to offer isoniazid preventive treatment irrespective of IGRA result. However, a recent Japanese high school TB contact investigation provides preliminary evidence for withholding preventive treatment in individuals with TST positive / IGRA negative results [31]. Of 349 students in this study, 95 had a positive TST (defined as erythema $30 mm in those with prior BCG and contact with smear positive index case) of whom only four had a positive QFT- TB Gold assay result. Preventive treatment was offered to these four only, significantly reducing the number of students in whom chemoprophylaxis was prescribed. Importantly, no student has subsequently developed TB disease during a three and a half year follow up. However, this study had a relatively short follow up and does not address the issue of discordant results in young children in whom the risk of progression to TB disease may be higher. Also, until recently, it was not uncommon for individuals in Japan to have multiple BCG immunisations, potentially increasing the magnitude of TST responses. In addition, the measurement of erythema in defining a positive TST is unique to Japan and questions the applicability of these findings in countries where the measurement of induration is standard, despite limited evidence that there is good correlation between erythema and induration [32]. Therefore, before this approach can be considered safe, further, larger studies with longer follow-up are needed to PLoS ONE 6 July 2008 Volume 3 Issue 7 e2624
7 investigate the natural history of children with TST positive / IGRA negative results and their risk of developing TB disease. Despite this, the UK National Institute for Clinical Excellence guidelines for the management of latent TB infection already recommend withholding preventive treatment in children over two years of age with a positive TST in whom the result of an IGRA is negative [33]. The higher rate of indeterminate results in the T-SPOT.TB assay compared with QFT-IT was attributable to a number of factors. The T-SPOT.TB is operationally more complex than the QFT-IT and 9 of the 14 indeterminate T-SPOT.TB results were attributable to potential laboratory error. The laboratory scientist undertaking the T-SPOT.TB assay underwent specific training prior to the study but given the relative complexity of the assay and the number of processing steps, the chance of a laboratory error occurring seems to be higher for the T-SPOT.TB assay. The indeterminate results potentially attributable to laboratory error were included in our analysis as they reflect real world practice. However, indeterminate results have been reported less frequently in the T-SPOT.TB assay than the QFT-IT assay in other studies [34]. The proportion of indeterminate QFT-IT assays was significantly less than the 17% reported in our previous study (p,0.001), the majority of which were due to a high nil control response [14,35]. In the present study only one assay had a high nil control response as defined by the manufacturer s latest guidelines for test interpretation that allow a significantly higher background (nil control) response of up to 8 IU/ml. In our current study, 14% of children had a background IFN-c response $1 IU/ ml and 6% had a background $2 IU/mL. Several other studies References 1. (2000) Targeted tuberculin testing and treatment of latent tuberculosis infection. Am J Respir Crit Care Med 161: S Smieja MJ, Marchetti CA, Cook DJ, Smaill FM (2000) Isoniazid for preventing tuberculosis in non-hiv infected persons. Cochrane Database Syst Rev: CD Pai M, Kalantri S, Dheda K (2006) New tools and emerging technologies for the diagnosis of tuberculosis: Part I. Latent tuberculosis. Expert Rev Mol Diagn 6: Richeldi L (2006) An update on the diagnosis of tuberculosis infection. Am J Respir Crit Care Med 174: Pai M, Dheda K, Cunningham J, Scano F, O Brien R (2007) T-cell assays for the diagnosis of latent tuberculosis infection: moving the research agenda forward. Lancet Infect Dis 7: Menzies D, Pai M, Comstock G (2007) Meta-analysis: new tests for the diagnosis of latent tuberculosis infection: areas of uncertainty and recommendations for research. Ann Intern Med 146: Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33: Arend SM, Thijsen SF, Leyten EM, Bouwman JJ, Franken WP, et al. (2007) Comparison of two interferon-gamma assays and tuberculin skin test for tracing tuberculosis contacts. Am J Respir Crit Care Med 175: Leyten EM, Arend SM, Prins C, Cobelens FG, Ottenhoff TH, et al. (2007) Discrepancy between Mycobacterium tuberculosis-specific interferon-{gamma} release assays using short versus prolonged in vitro incubation. Clin Vaccine Immunol. 10. Lalvani A (2007) Diagnosing tuberculosis infection in the 21st century: new tools to tackle an old enemy. Chest 131: Mazurek GH, Jereb J, Lobue P, Iademarco MF, Metchock B, et al. (2005) Guidelines for using the QuantiFERON-TB Gold test for detecting Mycobacterium tuberculosis infection, United States. MMWR Recomm Rep 54: Pai M, Menzies D (2007) The new IGRA and the old TST: making good use of disagreement. Am J Respir Crit Care Med 175: Cehovin A, Cliff JM, Hill PC, Brookes RH, Dockrell HM (2007) Extended culture enhances sensitivity of a gamma interferon assay for latent Mycobacterium tuberculosis infection. Clin Vaccine Immunol 14: Connell TG, Curtis N, Ranganathan SC, Buttery JP (2006) Performance of a whole blood interferon gamma assay for detecting latent infection with Mycobacterium tuberculosis in children. Thorax 61: Dewan PK, Grinsdale J, Kawamura LM (2007) Low sensitivity of a whole-blood interferon-gamma release assay for detection of active tuberculosis. Clin Infect Dis 44: have reported assays with high nil control responses [19,36]. We have previously highlighted our concern about the validity of reporting assays with background levels $2 IU/mL [35]. For the T-SPOT.TB assay, four had background nil control responses $40 SFCs/10 6. The cause of high nil control responses in IGRA warrants further investigation. In conclusion we have shown high agreement between QFT-IT and T-SPOT.TB in children. Discordant results between TST and IGRAs are common (most often TST positive, IGRA negative) and highlight the need for further longitudinal studies to determine the negative predictive value of IGRAs and the validity of current recommendations for the investigation and treatment of latent TB infection in children. Acknowledgments We thank Bindu Bali, Andrea Smith, Kate Thompson, and Barry Linnane for their assistance in patient recruitment to this study. We thank Rosemary Carzino for undertaking the T-SPOT.TB assays. We thank David Leslie and Norbert Ryan for helpful discussions. We are grateful to Marc Terbruegge for helpful comments on the manuscript. We also thank all the families for participating in this study. Author Contributions Conceived and designed the experiments: SR TGC NC NR JPB. Performed the experiments: NR. Analyzed the data: SR TGC NC NR GAP. Contributed reagents/materials/analysis tools: SR NC. Wrote the paper: SR TGC NC NR GAP JPB. Performed experiments with laboratory scientist: NR. Wrote the first draft of the manuscript: TC. Enrolled patients: TC NR GP JB SR. 16. Ferrara G, Losi M, Meacci M, Meccugni B, Piro R, et al. (2005) Routine Hospital Use of a New Commercial Whole Blood Interferon-{gamma} Assay for the Diagnosis of Tuberculosis Infection. Am J Respir Crit Care Med 172: Hill PC, Brookes RH, Adetifa IMO, Fox A, Jackson-Sillah D, et al. (2006) Comparison of Enzyme-Linked Immunospot Assay and Tuberculin Skin Test in Healthy Children Exposed to Myocbacterium tuberculosis. Pediatrics 117: Mahomed H, Hughes EJ, Hawkridge T, Minnies D, Simon E, et al. (2006) Comparison of mantoux skin test with three generations of a whole blood IFNgamma assay for tuberculosis infection. Int J Tuberc Lung Dis 10: Mazurek GH, Weis SE, Moonan PK, Daley CL, Bernardo J, et al. (2007) Prospective comparison of the tuberculin skin test and 2 whole-blood interferongamma release assays in persons with suspected tuberculosis. Clin Infect Dis 45: Mazurek GH, Zajdowicz MJ, Hankinson AL, Costigan DJ, Toney SR, et al. (2007) Detection of Mycobacterium tuberculosis infection in United States Navy recruits using the tuberculin skin test or whole-blood interferon-gamma release assays. Clin Infect Dis 45: Carvalho AC, Pezzoli MC, El-Hamad I, Arce P, Bigoni S, et al. (2007) QuantiFERON-TB Gold test in the identification of latent tuberculosis infection in immigrants. J Infect 55: Ewer K, Deeks J, Alvarez L, Bryant G, Waller S, et al. (2003) Comparison of T- cell-based assay with tuberculin skin test for diagnosis of Mycobacterium tuberculosis infection in a school tuberculosis outbreak. Lancet 361: Harada N, Nakajima Y, Higuchi K, Sekiya Y, Rothel J, et al. (2006) Screening for Tuberculosis Infection Using Whole-Blood Interferon- gamma and Mantoux Testing Among Japanese Healthcare Workers. Infect Control Hosp Epidemiol 27: Lalvani A, Pathan AA, Durkan H, Wilkinson KA, Whelan A, et al. (2001) Enhanced contact tracing and spatial tracking of Mycobacterium tuberculosis infection by enumeration of antigen-specific T cells. Lancet 357: Menzies D (1999) Interpretation of repeated tuberculin tests. Boosting, conversion, and reversion. Am J Respir Crit Care Med 159: Mori T, Harada N, Higuchi K, Sekiya Y, Uchimura K, et al. (2007) Waning of the specific interferon-gamma response after years of tuberculosis infection. Int J Tuberc Lung Dis 11: Suzuki K, Onozaki I, Shimura N, Harada N, Mori T (2004) QuantiFERON- TB-2nd Generation in the elderly persons. Kekkaku 79: Hill PC, Brookes RH, Fox A, Jackson-Sillah D, Jeffries DJ, et al. (2007) Longitudinal assessment of an ELISPOT test for Mycobacterium tuberculosis infection. PLoS Med 4: e192. PLoS ONE 7 July 2008 Volume 3 Issue 7 e2624
8 29. Detjen AK, Keil T, Roll S, Hauer B, Mauch H, et al. (2007) Interferon-gamma release assays improve the diagnosis of tuberculosis and nontuberculous mycobacterial disease in children in a country with a low incidence of tuberculosis. Clin Infect Dis 45: Haimi-Cohen Y, Zeharia A, Mimouni M, Soukhman M, Amir J (2001) Skin indurations in response to tuberculin testing in patients with nontuberculous mycobacterial lymphadenitis. Clin Infect Dis 33: Higuchi K, Harada N, Mori T, Sekiya Y (2007) Use of QuantiFERON-TB Gold to investigate tuberculosis contacts in a high school. Respirology 12: Kimura M, Comstock GW, Mori T (2005) Comparison of erythema and induration as results of tuberculin tests. Int J Tuberc Lung Dis 9: Taylor RE, Cant AJ, Clark JE (2007) Potential impact of NICE tuberculosis guidelines in paediatric TB screening. Arch Dis Child. 34. Ferrara G, Losi M, D Amico R, Roversi P, Piro R, et al. (2006) Use in routine clinical practice of two commercial blood tests for diagnosis of infection with Mycobacterium tuberculosis: a prospective study. Lancet 367: Curtis N, Connell T, Buttery JP, Ranganathan S (2006) Whole blood IFNgamma assay for detecting TB in children. author reply. Thorax 61: Nakaoka H, Lawson L, Bertel Squire S, Coulter B, Ravn P, et al. (2006) Risk for Tuberculosis among children. Emerg Infect Dis 12: PLoS ONE 8 July 2008 Volume 3 Issue 7 e2624
T tuberculin Skin Test (TST) and QFT-GIT in Military Personnel
 2 COMPARISON OF MANTOUX AND QUANTIFERON-TB GOLD TEST FOR DIAGNOSIS OF LATENT TUBERCULOSIS INFECTION IN ARMY PERSONNEL Willeke P.J. Franken 1, Joost F. Timmermans 2, Corine Prins 1, Evert-Jan H.J. Slootman
2 COMPARISON OF MANTOUX AND QUANTIFERON-TB GOLD TEST FOR DIAGNOSIS OF LATENT TUBERCULOSIS INFECTION IN ARMY PERSONNEL Willeke P.J. Franken 1, Joost F. Timmermans 2, Corine Prins 1, Evert-Jan H.J. Slootman
What is an IGRA? What is an IGRA? Are they available here? How do I use them? Learning Objectives
 What is an IGRA? Are they available here? How do I use them? Debbie Staley, RN, MPH TB Nurse Consultant VDH Division of Disease Prevention TB Control Program Learning Objectives Participants will be able
What is an IGRA? Are they available here? How do I use them? Debbie Staley, RN, MPH TB Nurse Consultant VDH Division of Disease Prevention TB Control Program Learning Objectives Participants will be able
Guidelines for TB Blood Testing. Minnesota Department of Health TB Prevention and Control Program June 2011
 Guidelines for TB Blood Testing Minnesota Department of Health TB Prevention and Control Program June 2011 Outline Interferon-Gamma Release Assays aka TB blood tests 1. What are they? 2. What are the current
Guidelines for TB Blood Testing Minnesota Department of Health TB Prevention and Control Program June 2011 Outline Interferon-Gamma Release Assays aka TB blood tests 1. What are they? 2. What are the current
Role of Quantiferon-TB Gold Assays in Detecting Latent Tuberculous Infection among Contacts of Active Tuberculous Patients *
 Med. J. Cairo Univ., Vol. 79, No. 1, June 169-175, 2011 www.medicaljournalofcairouniversity.com Role of Quantiferon-TB Gold Assays in Detecting Latent Tuberculous Infection among Contacts of Active Tuberculous
Med. J. Cairo Univ., Vol. 79, No. 1, June 169-175, 2011 www.medicaljournalofcairouniversity.com Role of Quantiferon-TB Gold Assays in Detecting Latent Tuberculous Infection among Contacts of Active Tuberculous
Lisa Y. Armitige, MD, PhD has the following disclosures to make:
 Interferon Gamma Release Assays (IGRAs) Lisa Y. Armitige, MD, PhD May 13, 2015 TB for Pulmonologist Phoenix, AZ March 13, 2015 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following
Interferon Gamma Release Assays (IGRAs) Lisa Y. Armitige, MD, PhD May 13, 2015 TB for Pulmonologist Phoenix, AZ March 13, 2015 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following
DRAFT FOR CONSULTATION
 Interferon Gamma Release Assay (IGRA) testing for tuberculosis (TB) - Questions & Answers (Q&As) For Health Care Workers HPA Tuberculosis Programme Board DRAFT FOR CONSULTATION October 2007 Interferon
Interferon Gamma Release Assay (IGRA) testing for tuberculosis (TB) - Questions & Answers (Q&As) For Health Care Workers HPA Tuberculosis Programme Board DRAFT FOR CONSULTATION October 2007 Interferon
Interferon-gamma-release assays: Better than tuberculin skin testing?
 REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will use and interpret the new blood tests for tuberculosis correctly CYNDEE MIRANDA, MD Department of Infectious Disease, Medicine Institute, Cleveland
REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will use and interpret the new blood tests for tuberculosis correctly CYNDEE MIRANDA, MD Department of Infectious Disease, Medicine Institute, Cleveland
CDC TB Testing Guidelines and Recent Literature Update
 Pocket Guide QuantiFERON -TB Gold CDC TB Testing Guidelines and Recent Literature Update Using IGRAs for TB screening in your patients June 2010 A full copy of the US Centers for Disease Control and Prevention
Pocket Guide QuantiFERON -TB Gold CDC TB Testing Guidelines and Recent Literature Update Using IGRAs for TB screening in your patients June 2010 A full copy of the US Centers for Disease Control and Prevention
Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB)
 Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB) Draft Interim HPA Guidance HPA Tuberculosis Programme Board Health Protection
Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB) Draft Interim HPA Guidance HPA Tuberculosis Programme Board Health Protection
Paediatrica Indonesiana. Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation
 Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Assessing patients for infection with Mycobacterium tuberculosis
 ORIGINAL STUDIES The Likelihood of an Indeterminate Test Result from a Whole-Blood Interferon- Release Assay for the Diagnosis of Mycobacterium tuberculosis Infection in Children Correlates With Age and
ORIGINAL STUDIES The Likelihood of an Indeterminate Test Result from a Whole-Blood Interferon- Release Assay for the Diagnosis of Mycobacterium tuberculosis Infection in Children Correlates With Age and
Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention
 Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention Screening Infants and Children for Tuberculosis in Massachusetts Executive Summary In Massachusetts,
Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention Screening Infants and Children for Tuberculosis in Massachusetts Executive Summary In Massachusetts,
Journal of Infectious Diseases Advance Access published January 26, 2015
 Journal of Infectious Diseases Advance Access published January 26, 2015 1 Effect of immune status on serial QuantiFERON-TB Gold In-Tube LTBI screening in persons with HIV in a low TB incidence country
Journal of Infectious Diseases Advance Access published January 26, 2015 1 Effect of immune status on serial QuantiFERON-TB Gold In-Tube LTBI screening in persons with HIV in a low TB incidence country
Serial Testing of Refugees for Latent Tuberculosis Using the QuantiFERON-Gold In-Tube: Effects of an Antecedent Tuberculin Skin Test
 Am. J. Trop. Med. Hyg., 80(4), 2009, pp. 628 633 Copyright 2009 by The American Society of Tropical Medicine and Hygiene Serial Testing of Refugees for Latent Tuberculosis Using the QuantiFERON-Gold In-Tube:
Am. J. Trop. Med. Hyg., 80(4), 2009, pp. 628 633 Copyright 2009 by The American Society of Tropical Medicine and Hygiene Serial Testing of Refugees for Latent Tuberculosis Using the QuantiFERON-Gold In-Tube:
Perils and Pitfalls in Clinical Trials of Diagnostic Tests for Tuberculosis. Richard O Brien, MD Foundation for Innovative New Diagnostics Geneva
 Perils and Pitfalls in Clinical Trials of Diagnostic Tests for Tuberculosis Richard O Brien, MD Foundation for Innovative New Diagnostics Geneva 1 Outline of Presentation Statement of the problem Common
Perils and Pitfalls in Clinical Trials of Diagnostic Tests for Tuberculosis Richard O Brien, MD Foundation for Innovative New Diagnostics Geneva 1 Outline of Presentation Statement of the problem Common
Interferon-gamma Release Assays: the Good, the Bad, and the Ugly
 Interferon-gamma Release Assays: the Good, the Bad, and the Ugly Susan E. Dorman, MD Center for TB Research Johns Hopkins University School of Medicine Maryland Center for Tuberculosis Control and Prevention
Interferon-gamma Release Assays: the Good, the Bad, and the Ugly Susan E. Dorman, MD Center for TB Research Johns Hopkins University School of Medicine Maryland Center for Tuberculosis Control and Prevention
Frequently Asked Questions
 Frequently Asked Questions QuantiFERON -TB Gold Health Professionals www.quantiferon.com 2 FAQ - Health Professionals Table of contents About TB 6 What is latent TB? And how is it different from active
Frequently Asked Questions QuantiFERON -TB Gold Health Professionals www.quantiferon.com 2 FAQ - Health Professionals Table of contents About TB 6 What is latent TB? And how is it different from active
Tuberculosis Contact Investigation in a Renal Dialysis Center: Blood Vs. Skin test
 Tuberculosis Contact Investigation in a Renal Dialysis Center: Blood Vs. Skin test Kevin L. Winthrop M.D., M.P.H. Assistant Professor of Medicine Divisions of Infectious Diseases and Public Health and
Tuberculosis Contact Investigation in a Renal Dialysis Center: Blood Vs. Skin test Kevin L. Winthrop M.D., M.P.H. Assistant Professor of Medicine Divisions of Infectious Diseases and Public Health and
Nevada State Health Division Technical Bulletin
 Nevada State Health Division Technical Bulletin Topic: Using QuantiFERON and Tuberculin Skin Test to Screen for TB Section/Program/Contact: Bureau of Community Health / Tuberculosis Program / Susanne Paulson,
Nevada State Health Division Technical Bulletin Topic: Using QuantiFERON and Tuberculin Skin Test to Screen for TB Section/Program/Contact: Bureau of Community Health / Tuberculosis Program / Susanne Paulson,
Pregnancy and Tuberculosis. Information for clinicians
 Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Serial Testing for TB Infection with IGRAs: Understanding the Sources of Variability
 Serial Testing for TB Infection with IGRAs: Understanding the Sources of Variability Niaz Banaei MD Assistant Professor of Pathology and Medicine Director, Fellowship in Global Health Diagnostics Director,
Serial Testing for TB Infection with IGRAs: Understanding the Sources of Variability Niaz Banaei MD Assistant Professor of Pathology and Medicine Director, Fellowship in Global Health Diagnostics Director,
Int j med invest.2(3):166-175 October
 Original article The comparison of tuberculin skin test and quantiferon-tb gold test for the determination of latent tuberculosis infection ın healthcare workers in a pulmonary diseases hospital Derya
Original article The comparison of tuberculin skin test and quantiferon-tb gold test for the determination of latent tuberculosis infection ın healthcare workers in a pulmonary diseases hospital Derya
Role of QuantiFERON-TB Test in Detection of Children Infected with Mycobacterium tuberculosis
 ORIGINAL ARTICLE Tanaffos (2010) 9(3), 22-27 2010 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Role of QuantiFERON-TB Test in Detection of Children Infected with Mycobacterium
ORIGINAL ARTICLE Tanaffos (2010) 9(3), 22-27 2010 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Role of QuantiFERON-TB Test in Detection of Children Infected with Mycobacterium
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY. Stephanie N. Lin MD 2/12/2016
 TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
For reprint orders, please contact reprints@future-drugs.com. Diagnosis of latent. Expert Rev. Anti Infect. Ther. 3(6), 981 993 (2005)
 Review For reprint orders, please contact reprints@future-drugs.com Diagnosis of latent Mycobacterium tuberculosis infection: is the demise of the Mantoux test imminent? James S Rothel and Peter Andersen
Review For reprint orders, please contact reprints@future-drugs.com Diagnosis of latent Mycobacterium tuberculosis infection: is the demise of the Mantoux test imminent? James S Rothel and Peter Andersen
Updated Guidelines for Using Interferon Gamma Release Assays to Detect Mycobacterium tuberculosis Infection United States, 2010
 Morbidity and Mortality Weekly Report www.cdc.gov/mmwr Recommendations and Reports June 25, 2010 / Vol. 59 / No. RR-5 Updated Guidelines for Using Interferon Gamma Release Assays to Detect Mycobacterium
Morbidity and Mortality Weekly Report www.cdc.gov/mmwr Recommendations and Reports June 25, 2010 / Vol. 59 / No. RR-5 Updated Guidelines for Using Interferon Gamma Release Assays to Detect Mycobacterium
Pediatric Latent TB Diagnosis and Treatment
 Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California
 Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
How To Test For Latent Tuberculosis
 IGRAs: What do they tell and what don t they tell us? 2 nd European Advanced Clinical Tuberculosis Course Monday 22 nd September 2014 Amsterdam, Netherlands Ibrahim Abubakar Professor of Infectious Disease
IGRAs: What do they tell and what don t they tell us? 2 nd European Advanced Clinical Tuberculosis Course Monday 22 nd September 2014 Amsterdam, Netherlands Ibrahim Abubakar Professor of Infectious Disease
Comparison of Quantiferon-TB Gold versus Tuberculin Skin Test for Tuberculosis Screening in Inflammatory Bowel Disease Patients
 Comparison of Quantiferon-TB Gold versus Tuberculin Skin Test for Tuberculosis Screening in Inflammatory Bowel Disease Patients Gianluca Andrisani, Alessandro Armuzzi, Alfredo Papa, Manuela Marzo, Carla
Comparison of Quantiferon-TB Gold versus Tuberculin Skin Test for Tuberculosis Screening in Inflammatory Bowel Disease Patients Gianluca Andrisani, Alessandro Armuzzi, Alfredo Papa, Manuela Marzo, Carla
No influence of haemodialysis on interferon production in the QuantiFERON-TB Gold-In-Tube test
 ORIGINAL ARTICLE JN EPHROL 24( 2011; 05) : 625-630 DOI:10.5301/JN.2011.6325 No influence of haemodialysis on interferon production in the QuantiFERON-TB Gold-In-Tube test Martine Hoogewerf 1, Greet J.
ORIGINAL ARTICLE JN EPHROL 24( 2011; 05) : 625-630 DOI:10.5301/JN.2011.6325 No influence of haemodialysis on interferon production in the QuantiFERON-TB Gold-In-Tube test Martine Hoogewerf 1, Greet J.
(In-Tube Method) The Whole Blood IFN-gamma Test Measuring Responses to ESAT-6, CFP-10 & TB7.7 Peptide Antigens PACKAGE INSERT
 (In-Tube Method) The Whole Blood IFN-gamma Test Measuring Responses to ESAT-6, CFP-10 & TB7.7 Peptide Antigens PACKAGE INSERT For In Vitro Diagnostic Use BlanK Page INDEX 1. INTENDED USE 2 2. SUMMARY AND
(In-Tube Method) The Whole Blood IFN-gamma Test Measuring Responses to ESAT-6, CFP-10 & TB7.7 Peptide Antigens PACKAGE INSERT For In Vitro Diagnostic Use BlanK Page INDEX 1. INTENDED USE 2 2. SUMMARY AND
Clinical description 2 Laboratory test for diagnosis 3. Incubation period 4 Mode of transmission 4 Period of communicability 4
 Tuberculosis Contents Epidemiology in New Zealand 2 Case definition 2 Clinical description 2 Laboratory test for diagnosis 3 Case classification 3 Spread of infection 4 Incubation period 4 Mode of transmission
Tuberculosis Contents Epidemiology in New Zealand 2 Case definition 2 Clinical description 2 Laboratory test for diagnosis 3 Case classification 3 Spread of infection 4 Incubation period 4 Mode of transmission
Santa Clara County Tuberculosis Screening Requirement for School Entrance Effective June 1, 2014. Frequently Asked Questions
 Frequently Asked Questions A child has history of BCG vaccination, should they have TST or IGRA? According to the American Academy of Pediatrics Red Book (2012), Interferon Gamma Release Assay (IGRA) is
Frequently Asked Questions A child has history of BCG vaccination, should they have TST or IGRA? According to the American Academy of Pediatrics Red Book (2012), Interferon Gamma Release Assay (IGRA) is
ALTERNATIVES TO THE TUBERCULIN SKIN TEST: INTERFERON-γ ASSAYS IN THE DIAGNOSIS OF MYCOBACTERIUM TUBERCULOSIS INFECTION
 Indian Journal of Medical Microbiology, (2005) 23 (3):151-158 Review Article ALTERNATIVES TO THE TUBERCULIN SKIN TEST: INTERFERON-γ ASSAYS IN THE DIAGNOSIS OF MYCOBACTERIUM TUBERCULOSIS INFECTION M Pai
Indian Journal of Medical Microbiology, (2005) 23 (3):151-158 Review Article ALTERNATIVES TO THE TUBERCULIN SKIN TEST: INTERFERON-γ ASSAYS IN THE DIAGNOSIS OF MYCOBACTERIUM TUBERCULOSIS INFECTION M Pai
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015
 Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Frequently Asked Questions
 Frequently Asked Questions QuantiFERON-TB Gold Health Professionals www.quantiferon.com Table of contents About TB 4 What is latent TB? And how is it different to active TB disease? 4 What is the meaning
Frequently Asked Questions QuantiFERON-TB Gold Health Professionals www.quantiferon.com Table of contents About TB 4 What is latent TB? And how is it different to active TB disease? 4 What is the meaning
Chapter 3 Testing for Tuberculosis Infection and Disease
 Chapter 3 Testing for Tuberculosis Infection and Disease Table of Contents Chapter Objectives.... 45 Introduction.... 47 Identifying High-Risk Groups for M. tuberculosis Testing... 47 Testing Methods for
Chapter 3 Testing for Tuberculosis Infection and Disease Table of Contents Chapter Objectives.... 45 Introduction.... 47 Identifying High-Risk Groups for M. tuberculosis Testing... 47 Testing Methods for
San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection
 San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection Rationale When to Screen for TB Choosing the Right TB Test Patient Registration Pre-Test
San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection Rationale When to Screen for TB Choosing the Right TB Test Patient Registration Pre-Test
Role of Interferon Gamma Release Assay in Active TB Diagnosis among HIV Infected Individuals
 Role of Interferon Gamma Release Assay in Active TB Diagnosis among HIV Infected Individuals Basirudeen Syed Ahamed Kabeer 1, Rajasekaran Sikhamani 5, Sowmya Swaminathan 2, Venkatesan Perumal 3, Paulkumaran
Role of Interferon Gamma Release Assay in Active TB Diagnosis among HIV Infected Individuals Basirudeen Syed Ahamed Kabeer 1, Rajasekaran Sikhamani 5, Sowmya Swaminathan 2, Venkatesan Perumal 3, Paulkumaran
Interferon Gamma Release Assays (IGRAs) in the Diagnosis of Tuberculosis
 Interferon Gamma Release Assays (IGRAs) in the Diagnosis of Tuberculosis Richard B. Clark, PhD, D(ABMM) Quest Diagnostics Nichols Institute Chantilly, VA Dale Schwab, PhD, D(ABMM) Quest Diagnostics Nichols
Interferon Gamma Release Assays (IGRAs) in the Diagnosis of Tuberculosis Richard B. Clark, PhD, D(ABMM) Quest Diagnostics Nichols Institute Chantilly, VA Dale Schwab, PhD, D(ABMM) Quest Diagnostics Nichols
The QuantiFERON-TB Gold test in the diagnosis and. treatment of latent tuberculosis in patients from a
 The QuantiFERON-TB Gold test in the diagnosis and treatment of latent tuberculosis in patients from a Norwegian outpatient clinic Anne Margarita Dyrhol-Riise 1, Gerd Gran 2, Tore Wenzel Larsen 3, Bjørn
The QuantiFERON-TB Gold test in the diagnosis and treatment of latent tuberculosis in patients from a Norwegian outpatient clinic Anne Margarita Dyrhol-Riise 1, Gerd Gran 2, Tore Wenzel Larsen 3, Bjørn
Appendix B: Provincial Case Definitions for Reportable Diseases
 Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Tuberculosis Revised August 2015 Tuberculosis 1.0 Provincial Reporting Confirmed and suspect cases
Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Tuberculosis Revised August 2015 Tuberculosis 1.0 Provincial Reporting Confirmed and suspect cases
LEARNING OUTCOMES. Identify children at risk of developing TB disease. Correctly manage and refer children suspected of TB. Manage child contacts
 TB in Children 1a TB IN CHILDREN 2 LEARNING OUTCOMES Identify children at risk of developing TB disease Correctly manage and refer children suspected of TB Manage child contacts 3 TB Infection and Disease
TB in Children 1a TB IN CHILDREN 2 LEARNING OUTCOMES Identify children at risk of developing TB disease Correctly manage and refer children suspected of TB Manage child contacts 3 TB Infection and Disease
An Evaluation of QuantiFERON-TB Gold In-Tube and Immunological Tests for TB Diagnosis in Iraqi Patients
 An Evaluation of QuantiFERON-TB Gold In-Tube and Immunological Tests for TB Diagnosis in Iraqi Patients Mohemid M. Al-Jebouri 1 and Nuha M. Wahid 2 1 Department of Microbiology, College of Medicine, University
An Evaluation of QuantiFERON-TB Gold In-Tube and Immunological Tests for TB Diagnosis in Iraqi Patients Mohemid M. Al-Jebouri 1 and Nuha M. Wahid 2 1 Department of Microbiology, College of Medicine, University
QuantiFERON -TB Gold In-Tube test (QFT-GIT) for the screening of latent tuberculosis in recent immigrants to Italy
 NEW MICROBIOLOGICA, 32, 369-376, 2009 QuantiFERON -TB Gold In-Tube test (QFT-GIT) for the screening of latent tuberculosis in recent immigrants to Italy Annalisa Saracino 1, Gaetano Scotto 1, Chiara Fornabaio
NEW MICROBIOLOGICA, 32, 369-376, 2009 QuantiFERON -TB Gold In-Tube test (QFT-GIT) for the screening of latent tuberculosis in recent immigrants to Italy Annalisa Saracino 1, Gaetano Scotto 1, Chiara Fornabaio
Tuberculosis. Subject. Goal/Objective. Instructions. Rationale. Operations Directorate, Health Branch Immigration Medical Examination Instructions
 Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Interim Guidance for Medical Schools on health checks for active and latent Tuberculosis in medical students returning from elective periods overseas
 Interim Guidance for Medical Schools on health checks for active and latent Tuberculosis in medical students returning from elective periods overseas This document has been developed by: Dr Mathina Darmalingam
Interim Guidance for Medical Schools on health checks for active and latent Tuberculosis in medical students returning from elective periods overseas This document has been developed by: Dr Mathina Darmalingam
Guidelines for Tuberculosis Screening of Healthcare Students in the greater Auckland region
 Guidelines for Tuberculosis Screening of Healthcare Students in the greater Auckland region Auckland Regional Public Health Service 2013 Document Controller: Updated December 2013 Medical Officer of Health,
Guidelines for Tuberculosis Screening of Healthcare Students in the greater Auckland region Auckland Regional Public Health Service 2013 Document Controller: Updated December 2013 Medical Officer of Health,
T()LED() Name ofpolicy: Mandatory Tuberculosis (TB) Screening of Students from World Health Organization Designated High TB Prevalence Countries
 Name ofpolicy: Mandatory Tuberculosis (TB) Screening of Students from World Health Organization Designated High TB Prevalence Countries Policy Number: 3364-81-04-030 T()LED() Revision date: I 0/22/13 Approving
Name ofpolicy: Mandatory Tuberculosis (TB) Screening of Students from World Health Organization Designated High TB Prevalence Countries Policy Number: 3364-81-04-030 T()LED() Revision date: I 0/22/13 Approving
Tuberculosis: FAQs. What is the difference between latent TB infection and TB disease?
 Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
Tuberculosis 89 (2009) S1, S41 S45. Contents lists available at ScienceDirect. Tuberculosis
 Tuberculosis 89 (2009) S1, S41 S45 Contents lists available at ScienceDirect Tuberculosis journal homepage: http://intl.elsevierhealth.com/journals/tube Latent tuberculosis infections in hard-to-reach
Tuberculosis 89 (2009) S1, S41 S45 Contents lists available at ScienceDirect Tuberculosis journal homepage: http://intl.elsevierhealth.com/journals/tube Latent tuberculosis infections in hard-to-reach
Department of Internal Medicine, Division of Cardiovascular Diseases. Department of Internal Medicine. Department of Internal Medicine
 Use of the QuantiFERON -TB Gold Assay in Pregnant Patients Bassem M.Chehab, M.D. 1, K. James Kallail, Ph.D. 2, Riad O. El Fakih, M.D. 3, Rosalee E. Zackula, M.A. 4, Garold O. Minns, M.D. 2 1 University
Use of the QuantiFERON -TB Gold Assay in Pregnant Patients Bassem M.Chehab, M.D. 1, K. James Kallail, Ph.D. 2, Riad O. El Fakih, M.D. 3, Rosalee E. Zackula, M.A. 4, Garold O. Minns, M.D. 2 1 University
The Cost Effectiveness of Interferon Gamma Release Assays Versus Tuberculin Skin Tests in Health Care
 ORIGINAL INVESTIGATION Cost-effectiveness of Interferon Gamma Release Assays vs Tuberculin Skin Tests in Health Care Workers Marie A. de Perio, MD; Joel Tsevat, MD, MPH; Gary A. Roselle, MD; Stephen M.
ORIGINAL INVESTIGATION Cost-effectiveness of Interferon Gamma Release Assays vs Tuberculin Skin Tests in Health Care Workers Marie A. de Perio, MD; Joel Tsevat, MD, MPH; Gary A. Roselle, MD; Stephen M.
Interferon-gamma release assays during follow-up of tuberculin skin test-positive contacts
 INT J TUBERC LUNG DIS 12(11):1286 1294 2008 The Union Interferon-gamma release assays during follow-up of tuberculin skin test-positive contacts W. P. J. Franken,* S. M. Arend,* S. F. T. Thijsen, J. J.
INT J TUBERC LUNG DIS 12(11):1286 1294 2008 The Union Interferon-gamma release assays during follow-up of tuberculin skin test-positive contacts W. P. J. Franken,* S. M. Arend,* S. F. T. Thijsen, J. J.
SPECIAL FEATURES: HEALTH POLICY
 Public Health Nursing 0737-1209/ 2013 Wiley Periodicals, Inc. doi: 10.1111/phn.12083 SPECIAL FEATURES: HEALTH POLICY Cost-effectiveness of Using Quantiferon Gold (QFT-G) versus Tuberculin Skin Test (TST)
Public Health Nursing 0737-1209/ 2013 Wiley Periodicals, Inc. doi: 10.1111/phn.12083 SPECIAL FEATURES: HEALTH POLICY Cost-effectiveness of Using Quantiferon Gold (QFT-G) versus Tuberculin Skin Test (TST)
Assisted Living - TB Risk Assessment
 Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
TB Diagnostics: looking back and looking forward
 TB Diagnostics: looking back and looking forward Raul V. Destura MD Institute of Molecular Biology and Biotechnology National Institutes of Health University of the Philippines, Manila Disturbing Statistics
TB Diagnostics: looking back and looking forward Raul V. Destura MD Institute of Molecular Biology and Biotechnology National Institutes of Health University of the Philippines, Manila Disturbing Statistics
Tuberculosis in children in Europe -the ptbnet
 Tuberculosis in children in Europe -the ptbnet Beate Kampmann FRCPCH PhD A/Professor in Paediatric Infection & Immunity Consultant Paediatrician Imperial College London, UK and Institute of Infectious
Tuberculosis in children in Europe -the ptbnet Beate Kampmann FRCPCH PhD A/Professor in Paediatric Infection & Immunity Consultant Paediatrician Imperial College London, UK and Institute of Infectious
Risk for Tuberculosis in Swiss Hospitals. Content. Introduction. Dr. med. Alexander Turk Zürcher Höhenklinik Wald alexander.turk@zhw.
 Risk for Tuberculosis in Swiss Hospitals 17. Tuberkulose Symposium Münchenwiler Risk for Tuberculosis in Swiss Hospitals Dr. med. Alexander Turk Zürcher Höhenklinik Wald alexander.turk@zhw.ch 1 Content
Risk for Tuberculosis in Swiss Hospitals 17. Tuberkulose Symposium Münchenwiler Risk for Tuberculosis in Swiss Hospitals Dr. med. Alexander Turk Zürcher Höhenklinik Wald alexander.turk@zhw.ch 1 Content
Guidelines for Tuberculosis Control in New Zealand 2010 Chapter 8: Diagnosis and Treatment of Latent Tuberculosis Infection
 Guidelines for Tuberculosis Control in New Zealand 2010 Chapter 8: Diagnosis and Treatment of Latent Tuberculosis Infection Ministry of Health. 2010. Guidelines for Tuberculosis Control in New Zealand
Guidelines for Tuberculosis Control in New Zealand 2010 Chapter 8: Diagnosis and Treatment of Latent Tuberculosis Infection Ministry of Health. 2010. Guidelines for Tuberculosis Control in New Zealand
Childhood Tuberculosis Some Basic Issues. Jeffrey R. Starke, M.D. Baylor College of Medicine
 Childhood Tuberculosis Some Basic Issues Jeffrey R. Starke, M.D. Baylor College of Medicine TUBERCULOSIS IS A SOCIAL DISEASE WITH MEDICAL IMPLICATIONS THE GREAT PARADOX OF TUBERCULOSIS A CAUTIONARY TALE
Childhood Tuberculosis Some Basic Issues Jeffrey R. Starke, M.D. Baylor College of Medicine TUBERCULOSIS IS A SOCIAL DISEASE WITH MEDICAL IMPLICATIONS THE GREAT PARADOX OF TUBERCULOSIS A CAUTIONARY TALE
American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine
 American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine West Virginia University gjuckett@hsc.wvu.edu Objectives
American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine West Virginia University gjuckett@hsc.wvu.edu Objectives
Table. Positive Purified Protein Derivative Results (Pediatrics In Review Apr 2008)
 PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
Hawaii Administrative Rules. Title 11. Department of Health. Chapter 164. Tuberculosis
 Hawaii Administrative Rules Title 11 Department of Health Chapter 164 Tuberculosis 11-164-1 Purpose 11-164-2 Definitions 11-164-3 Reports to the department 11-164-4 Content of report 11-164-5 Examination
Hawaii Administrative Rules Title 11 Department of Health Chapter 164 Tuberculosis 11-164-1 Purpose 11-164-2 Definitions 11-164-3 Reports to the department 11-164-4 Content of report 11-164-5 Examination
GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS IN SOUTH AFRICA
 GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS IN SOUTH AFRICA 2010 1 TB prophylaxis GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS Background
GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS IN SOUTH AFRICA 2010 1 TB prophylaxis GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS Background
Evaluation of a Whole-Blood Interferon-g Release Assay for the Detection of Mycobacterium tuberculosis Infection in 2 Study Populations
 MAJOR ARTICLE Evaluation of a Whole-Blood Interferon-g Release Assay for the Detection of Mycobacterium tuberculosis Infection in 2 Study Populations Bahrie Bellete, 1 Jacqueline Coberly, 2 Grace Link
MAJOR ARTICLE Evaluation of a Whole-Blood Interferon-g Release Assay for the Detection of Mycobacterium tuberculosis Infection in 2 Study Populations Bahrie Bellete, 1 Jacqueline Coberly, 2 Grace Link
April King-Todd 2014 National TB Conference Atlanta, Georgia June 10, 2014
 An Outbreak of TB Among the Homeless: The Aftermath in a High Incidence County April King-Todd, RN, MPH Los Angeles County Department of Public Health Tuberculosis Control Program National TB Nurses Coalition
An Outbreak of TB Among the Homeless: The Aftermath in a High Incidence County April King-Todd, RN, MPH Los Angeles County Department of Public Health Tuberculosis Control Program National TB Nurses Coalition
ATTACHMENT 2. New Jersey Department of Health Tuberculosis Program FREQUENTLY ASKED QUESTIONS
 ATTACHMENT 2 New Jersey Department of Health Tuberculosis Program FREQUENTLY ASKED QUESTIONS 1. QUESTION Is it required to submit the Annual Report of TB Testing in Schools Form (TB-57) to the New Jersey
ATTACHMENT 2 New Jersey Department of Health Tuberculosis Program FREQUENTLY ASKED QUESTIONS 1. QUESTION Is it required to submit the Annual Report of TB Testing in Schools Form (TB-57) to the New Jersey
Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado
 Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado Developed by the Colorado Medical Directors Association and The Colorado Department of Public Health and Environment Introduction:
Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado Developed by the Colorado Medical Directors Association and The Colorado Department of Public Health and Environment Introduction:
ASSESSMENT OF THE QUANTIFERON TB GOLD IN-TUBE TEST FOR THE DIAGNOSIS OF PULMONARY TUBERCULOSIS IN NAMIBIAN PATIENTS
 ASSESSMENT OF THE QUANTIFERON TB GOLD IN-TUBE TEST FOR THE DIAGNOSIS OF PULMONARY TUBERCULOSIS IN NAMIBIAN PATIENTS A THESIS SUBMITTED IN THE FULFILMENT OF THE REQUIREMENTS FOR THE DEGREE OF MASTER OF
ASSESSMENT OF THE QUANTIFERON TB GOLD IN-TUBE TEST FOR THE DIAGNOSIS OF PULMONARY TUBERCULOSIS IN NAMIBIAN PATIENTS A THESIS SUBMITTED IN THE FULFILMENT OF THE REQUIREMENTS FOR THE DEGREE OF MASTER OF
Research Article Tuberculin Skin Tests versus Interferon-Gamma Release Assays in Tuberculosis Screening among Immigrant Visa Applicants
 Tuberculosis Research and Treatment, Article ID 217969, 11 pages http://dx.doi.org/10.1155/2014/217969 Research Article Tuberculin Skin Tests versus Interferon-Gamma Release Assays in Tuberculosis Screening
Tuberculosis Research and Treatment, Article ID 217969, 11 pages http://dx.doi.org/10.1155/2014/217969 Research Article Tuberculin Skin Tests versus Interferon-Gamma Release Assays in Tuberculosis Screening
TB Intensive San Antonio, Texas November 11 14, 2014
 TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
Recent Advances in The Treatment of Mycobacterium Tuberculosis
 Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
KEYWORDS Childhood tuberculosis; Tuberculin, Interferon-g; Diagnosis, Paediatrics. San Francisco, CA 94110, USA
 Journal of Infection (2007) 54, 267e276 www.elsevierhealth.com/journals/jinf Comparison of a whole blood interferon-g assay with tuberculin skin testing for the detection of tuberculosis infection in hospitalized
Journal of Infection (2007) 54, 267e276 www.elsevierhealth.com/journals/jinf Comparison of a whole blood interferon-g assay with tuberculin skin testing for the detection of tuberculosis infection in hospitalized
Diagnosis of Tuberculosis Infection
 Diagnosis of Tuberculosis Infection CONTENTS Introduction... 7.2 Purpose... 7.2 Policy... 7.2 High-Risk Groups... 7.3 Diagnosis of Tuberculosis Infection... 7.4 Interferon gamma release assays... 7.4 Mantoux
Diagnosis of Tuberculosis Infection CONTENTS Introduction... 7.2 Purpose... 7.2 Policy... 7.2 High-Risk Groups... 7.3 Diagnosis of Tuberculosis Infection... 7.4 Interferon gamma release assays... 7.4 Mantoux
Tuberculosis Exposure Control Plan for Low Risk Dental Offices
 Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Regulations for Tuberculosis Control in Minnesota Health Care Settings
 Regulations for Tuberculosis Control in Minnesota Health Care Settings A guide for implementing tuberculosis (TB) infection control regulations in your facility Tuberculosis Prevention and Control Program
Regulations for Tuberculosis Control in Minnesota Health Care Settings A guide for implementing tuberculosis (TB) infection control regulations in your facility Tuberculosis Prevention and Control Program
TB Prevention, Diagnosis and Treatment. Accelerating advocacy on TB/HIV 15th July, Vienna
 TB Prevention, Diagnosis and Treatment Accelerating advocacy on TB/HIV 15th July, Vienna Diagnosis Microscopy of specially stained sputum is the main test for diagnosing TB (1 2 days) TB bacilli seen in
TB Prevention, Diagnosis and Treatment Accelerating advocacy on TB/HIV 15th July, Vienna Diagnosis Microscopy of specially stained sputum is the main test for diagnosing TB (1 2 days) TB bacilli seen in
3. Blood and blood products such as serum, plasma, and other blood components.
 Mississippi Downloaded 01/2011 101.11 Infectious Medical Waste. The term "infectious medical waste" includes solid or liquid wastes which may contain pathogens with sufficient virulence and quantity such
Mississippi Downloaded 01/2011 101.11 Infectious Medical Waste. The term "infectious medical waste" includes solid or liquid wastes which may contain pathogens with sufficient virulence and quantity such
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams
 MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams Document control Title Type Author/s Management of tuberculosis in prisons: Guidance for prison healthcare teams Operational
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams Document control Title Type Author/s Management of tuberculosis in prisons: Guidance for prison healthcare teams Operational
What You Need to Know About Collecting QuantiFERON (QFT) TB Gold In-Tube Samples
 What You Need to Know About Collecting QuantiFERON (QFT) TB Gold In-Tube Samples I. What is QuantiFERON (QFT) TB Gold In-Tube? II. III. QFT is an interferon-gamma release assay (IGRA). QFT is a blood test.
What You Need to Know About Collecting QuantiFERON (QFT) TB Gold In-Tube Samples I. What is QuantiFERON (QFT) TB Gold In-Tube? II. III. QFT is an interferon-gamma release assay (IGRA). QFT is a blood test.
Use of Nucleic Acid Amplification Tests in TB patients in California 2010-2012
 Use of Nucleic Acid Amplification Tests in TB patients in California 2010-2012 Lisa Pascopella, PhD, MPH Pennan Barry, MD, MPH Tuberculosis Control Branch, Division of Communicable Disease Control, Center
Use of Nucleic Acid Amplification Tests in TB patients in California 2010-2012 Lisa Pascopella, PhD, MPH Pennan Barry, MD, MPH Tuberculosis Control Branch, Division of Communicable Disease Control, Center
Role of QuantiFERON-TB Gold In-Tube test in detection of latent tuberculosis infection in health care contacts in Alexandria, Egypt
 Vol. 8(12), pp. 1310-1317, 19 March, 2014 DOI: 10.5897/AJMR2013.6502 ISSN 1996-0808 Copyright 2014 Author(s) retain the copyright of this article http://www.academicjournals.org/ajmr African Journal of
Vol. 8(12), pp. 1310-1317, 19 March, 2014 DOI: 10.5897/AJMR2013.6502 ISSN 1996-0808 Copyright 2014 Author(s) retain the copyright of this article http://www.academicjournals.org/ajmr African Journal of
Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective October 2014
 Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective October 2014 Students must remain in compliance throughout enrollment within the program. Students who are not in compliance
Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective October 2014 Students must remain in compliance throughout enrollment within the program. Students who are not in compliance
First-in-Man Open Clinical Trial of a Combined rdesat-6 and rcfp-10 Tuberculosis Specific Skin Test Reagent
 First-in-Man Open Clinical Trial of a Combined rdesat-6 and rcfp-10 Tuberculosis Specific Skin Test Reagent Winnie Bergstedt 1, Pernille N. Tingskov 2, Birgit Thierry-Carstensen 2, Søren T. Hoff 3, Henrik
First-in-Man Open Clinical Trial of a Combined rdesat-6 and rcfp-10 Tuberculosis Specific Skin Test Reagent Winnie Bergstedt 1, Pernille N. Tingskov 2, Birgit Thierry-Carstensen 2, Søren T. Hoff 3, Henrik
Pregnancy and Tuberculosis. Patient and Public information sheet
 Pregnancy and Tuberculosis Patient and Public information sheet Who is at risk of TB? Anyone can catch TB, but it is possible that pregnant women have a slightly higher risk of TB. Some people are more
Pregnancy and Tuberculosis Patient and Public information sheet Who is at risk of TB? Anyone can catch TB, but it is possible that pregnant women have a slightly higher risk of TB. Some people are more
CTCA POSITION ON TB EXAMINATION OF SCHOOL EMPLOYEES AND VOLUNTEERS
 CTCA POSITION ON TB EXAMINATION OF SCHOOL EMPLOYEES AND VOLUNTEERS Introduction Although progress has been made, tuberculosis (TB) continues to be a significant public health problem; appropriate TB examination
CTCA POSITION ON TB EXAMINATION OF SCHOOL EMPLOYEES AND VOLUNTEERS Introduction Although progress has been made, tuberculosis (TB) continues to be a significant public health problem; appropriate TB examination
Policy Directive: compliance is mandatory
 Policy Directive: compliance is mandatory Policy for Control of Tuberculosis in South Australian Health Services Policy developed by: Public Health and Clinical Coordination Approved at Portfolio Executive
Policy Directive: compliance is mandatory Policy for Control of Tuberculosis in South Australian Health Services Policy developed by: Public Health and Clinical Coordination Approved at Portfolio Executive
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG
 TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
Canadian Tuberculosis Standards
 Canadian Tuberculosis Standards 7 th Edition Chapter 4: Diagnosis of Latent Tuberculosis Infection Canadian Tuberculosis Standards, 7 th Edition is available on Internet at the following address: www.phac-aspc.gc.ca
Canadian Tuberculosis Standards 7 th Edition Chapter 4: Diagnosis of Latent Tuberculosis Infection Canadian Tuberculosis Standards, 7 th Edition is available on Internet at the following address: www.phac-aspc.gc.ca
Long-term Care - TB Risk Assessment
 Montana DPHHS Tuberculosis Program Long-term Care - TB Risk Assessment Long-term Care, Residential Treatment, ESRD (outpatient), Hospice (inpatient) Today s Date Facility Address Phone County Completed
Montana DPHHS Tuberculosis Program Long-term Care - TB Risk Assessment Long-term Care, Residential Treatment, ESRD (outpatient), Hospice (inpatient) Today s Date Facility Address Phone County Completed
University of Nebraska Medical Center, Department of Health Services Research and Administration, Omaha, NE
 Research Mycobacterium Tuberculosis Infection, Immigration Status, and Diagnostic Discordance: A Comparison of Tuberculin Skin Test and QuantiFERON -TB Gold In-Tube Test Among Immigrants to the U.S. Fernando
Research Mycobacterium Tuberculosis Infection, Immigration Status, and Diagnostic Discordance: A Comparison of Tuberculin Skin Test and QuantiFERON -TB Gold In-Tube Test Among Immigrants to the U.S. Fernando
E s t i m at i n g d i a g n o s t i c a c c u r a c y o f t e s t s f o r l at e n t
 R e s e a rc h a r ti cl e s E s t i m at i n g d i a g n o s t i c a c c u r a c y o f t e s t s f o r l at e n t t u b e r c u l o s i s i n f e c t i o n w i t h o u t a g o l d s ta n d a r d a m o
R e s e a rc h a r ti cl e s E s t i m at i n g d i a g n o s t i c a c c u r a c y o f t e s t s f o r l at e n t t u b e r c u l o s i s i n f e c t i o n w i t h o u t a g o l d s ta n d a r d a m o
Use of Interferon Gamma Release Assays as Confirmatory Test for Tuberculin Skin Test-Positive Patients in the Canadian Armed Forces
 Use of Interferon Gamma Release Assays as Confirmatory Test for Tuberculin Skin Test-Positive Patients in the Canadian Armed Forces Milan Patel Surgeon General Report Surgeon General Health Research Program
Use of Interferon Gamma Release Assays as Confirmatory Test for Tuberculin Skin Test-Positive Patients in the Canadian Armed Forces Milan Patel Surgeon General Report Surgeon General Health Research Program
PEOSH Model Tuberculosis Infection Control Program
 PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
Catalogue Number: 0594 0201 PACKAGE INSERT. For In Vitro Diagnostic Use
 Catalogue Number: 0594 0201 PACKAGE INSERT For In Vitro Diagnostic Use INDEX 1. INTENDED USE 2 2. SUMMARY AND EXPLANATION OF THE TEST 2 3. REAGENTS AND STORAGE 3 Components 3 Storage Instructions 4 Kit
Catalogue Number: 0594 0201 PACKAGE INSERT For In Vitro Diagnostic Use INDEX 1. INTENDED USE 2 2. SUMMARY AND EXPLANATION OF THE TEST 2 3. REAGENTS AND STORAGE 3 Components 3 Storage Instructions 4 Kit
QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company
 QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company P1078 TB APPRISE TB Ante vs. Postpartum Prevention with INH in HIV Seropositive mothers and their Exposed
QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company P1078 TB APPRISE TB Ante vs. Postpartum Prevention with INH in HIV Seropositive mothers and their Exposed
Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective February 2016
 Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective February 2016 Students must remain in compliance throughout enrollment within the program. Students who are not in compliance
Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective February 2016 Students must remain in compliance throughout enrollment within the program. Students who are not in compliance
DIVISION of SUBSTANCE ABUSE SERVICES. Tuberculosis Control Guidelines for Alcohol and Drug Abuse Treatment Programs
 DIVISION of SUBSTANCE ABUSE SERVICES Tuberculosis Control Guidelines for Alcohol and Drug Abuse Treatment Programs 1. Purpose: This policy provides guidance and instruction to identify and prevent tuberculosis
DIVISION of SUBSTANCE ABUSE SERVICES Tuberculosis Control Guidelines for Alcohol and Drug Abuse Treatment Programs 1. Purpose: This policy provides guidance and instruction to identify and prevent tuberculosis
