Serial Testing of Refugees for Latent Tuberculosis Using the QuantiFERON-Gold In-Tube: Effects of an Antecedent Tuberculin Skin Test
|
|
|
- Sybil Arnold
- 8 years ago
- Views:
Transcription
1 Am. J. Trop. Med. Hyg., 80(4), 2009, pp Copyright 2009 by The American Society of Tropical Medicine and Hygiene Serial Testing of Refugees for Latent Tuberculosis Using the QuantiFERON-Gold In-Tube: Effects of an Antecedent Tuberculin Skin Test Cristina A. Baker, * William Thomas, William M. Stauffer, Phillip K. Peterson, and Dean T. Tsukayama Infectious Diseases and International Medicine Division, University of Minnesota, Minneapolis, Minnesota; Division of Biostatistics, School of Public Health, University of Minnesota, Minneapolis, Minnesota; Infectious Diseases Division, Hennepin County Medical Center, Minneapolis, Minnesota Abstract. Screening for latent tuberculosis infection (LTBI) in refugee populations immigrating to low-incidence countries remains a challenge. We assessed the characteristics of the QuantiFERON-Gold In-Tube (QFT-GIT) compared with the tuberculin skin test (TST) in 198 refugees of all ages from tuberculosis-endemic countries. Diagnostic agreement between the first QFT-GIT and simultaneous TST was 78% (κ = 0.56) and between serial QFT-GITs was 89% (κ = 0.76). In serial QFT-GIT testing, 70% of subjects had an increased QFT-GIT value, perhaps the result of an antecedent TST in the setting of previous TB exposure. This boosting seemed to become less prevalent with time from TST and occurred less frequently in those with negative first QFT-GIT readings. Despite small changes in the quantitative results caused by nonspecific variation and boosting, the diagnostic result of the QFT-GIT was reliable. The QFT-GIT shows the potential to replace the TST for LTBI screening in refugees from tuberculosis-endemic areas. INTRODUCTION Over the last decade, the number of immigrants and refugees entering the United States from countries with a high prevalence of Mycobacterium tuberculosis (MTB) has continued to increase, leading to concerns about the potential public health impact. Currently, the rate of active tuberculosis among foreign-born persons is 9.7 times greater than among US-born persons. 1 The majority of these cases are believed to represent reactivation of infection acquired before immigration, highlighting the inadequacies of our current prevention and control strategies. The tuberculin skin test (TST), long the diagnostic method for diagnosing latent tuberculosis infection (LTBI), is hindered by suboptimal sensitivity and specificity. A number of factors may adversely affect the performance characteristics of the skin test among refugees, including previous vaccination with bacillus Calmette-Guérin (BCG) or the presence of non-tuberculous mycobacterial infection. Newer interferongamma (IFN-γ) release assays (IGRAs) have the potential to address many of the shortcomings of the TST in refugee populations such as eliminating false positives caused by BCG vaccination, distinguishing between tuberculous and nontuberculous mycobacterial infection (NTB), and providing test results after a single patient visit. 2 4 A recent meta-analysis found insufficient data to adequately characterize the performance of IGRAs in high-risk populations, such as refugees, and limited data regarding the tests reproducibility. 5 Previous studies have shown that IGRAs perform well in healthy individuals from tuberculosis-endemic areas. 6 8 One study looked at the performance of an IGRA for LTBI screening of asylum seekers in Norway. 9 However, to our knowledge, no studies have examined the reproducibility of these tests in refugees. An issue unique to refugees resettling to the United States that has potential to alter the IGRA assay s performance and utility in this population is the fact that TST testing is frequently repeated during relocation. During resettlement, refugees are * Address correspondence to Cristina A. Baker, Infectious Diseases and International Medicine Division, University of Minnesota, 420 Delaware St. SE, Minneapolis, MN bake0088@umn.edu 628 often repeatedly skin tested for LTBI because previous screening test results are lost or unavailable because of the transient medical care provided to this population during this time. It is unclear whether TST testing performed weeks earlier results in boosting of an IGRA result in this population. It is well known that serial tuberculin skin testing can result in a boosting of the skin test result, with the greatest effect seen when the interval between tests is 1 5 weeks. 10,11 However, it is unclear what role timing of TST placement plays in the boosting of an IGRA result. One study found no evidence of boosting caused by TST testing performed 3 days before IGRA testing. 12 Conversely, two recent studies reported potential evidence for boosting of the QuantiFERON Gold (the earlier version of the test) in subjects between 2 4 and 6 weeks after TST testing. 13,14 Domestic medical screening of refugees, which is encouraged by the Office of Refugee Resettlement for all newly arriving refugees, provides logistic challenges for the organizations assisting with resettlement. One practical challenge for clinics providing this care is coordinating tuberculin skin testing, which requires two clinic visits. A single-step test for TB that requires only one visit and performs at least as well as the TST would be desirable for many organizations and clinics serving this population. In this study, we assessed the performance of the QuantiFERON-TB Gold In-Tube (QFT-GIT) in a refugee population relocating to the United States. The goals of this study were 2-fold: to evaluate the utility of the QFT-GIT as a screening tool for LTBI in a refugee population from tuberculosis-endemic countries and to assess the reproducibility of the test in the setting of an antecedent TST. MATERIALS AND METHODS Study participants. Refugees who presented for their domestic refugee medical screening examination at the Hennepin Public Health Clinic (Minneapolis, MN) were recruited for the study between July 2006 and March Only individuals who had been in the United States for < 6 months were eligible for inclusion. Exclusion criteria included suspected or confirmed active tuberculosis, HIV infection, malignancy, liver or kidney disease, and treatment with immunosuppressive drugs. Informed consent was obtained according to
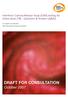
2 QUANTIFERON-GOLD IN-TUBE FOR LTBI TESTING IN REFUGEES 629 Figure 1. Study flow diagram of refugee screening and testing for latent tuberculosis infection with the QFT-GIT and the TST. protocols approved by the institution s Human Subject s Research Committee according to the Department of Health and Human Service s guidelines. Study design. Refugees were prospectively enrolled in the study. Each participant was evaluated at four time points ( Figure 1 ). At Visit 1, each participant had a TST placed and blood drawn for a QFT-GIT. At Visit 2 (48 72 hours later), TST tests were read, and subjects underwent a complete refugee screening exam. Approximately 6 weeks after the first visit, subjects returned for Visit 3, in which a repeat QFT-GIT was performed and a second TST was placed if the first TST had been negative (< 10 mm). At Visit 4 (48 72 hours later), the second TSTs were interpreted. The QFT-GIT test was performed by a trained technician according to the manufacturer s guidelines. In brief, 1 ml of whole blood was collected in each of the specialized blood collection tubes coated with saline (negative control), early secretory antigen target (ESAT-6), culture filtrate protein (CFP-10), and tuberculosis (TB-7.7) peptides (TB antigen tube), and phytohemagglutinin (PHA) (positive control). The tubes were incubated at 37 C within 16 hours of collection for hours. After incubation, the plasma was removed and frozen for future analysis. IFN-γ production was measured by ELISA. The amount of IFN-γ detected in the negative control tube (nil) was subtracted from the TB antigen and PHA-stimulated tubes. Results were interpreted as defined by the manufacturer s instructions. Samples from the TB antigen tube yielding 0.35 IU/mL IFN-γ were considered positive. Samples with < 0.35 or 0.35 IU/mL IFN-γ and < 25% of nil value were reported as negative. The test was deemed indeterminate in the event of a low IFN-γ response (< 0.5 IU/mL) to the PHA (positive control), suggesting anergy or a technical problem with the test (nil > 8.0 IU/mL). Statistical software was provided by the manufacturer. Values > 10 IU/mL are reported by the software as > 10 IU/mL. TSTs were performed using 0.l-mL test doses of tuberculin-purified protein derivative (bio-equivalent 5 TU of PPD-S; Aventis Pasteur, Toronto, Ontario, Canada ) injected intradermally into the volar aspect of the forearm. The transverse diameter of the induration was measured hours later by a trained healthcare provider. A TST was considered positive if 10 mm of skin induration was observed. TST conversion was defined as a skin test that went from negative (< 10 mm) to positive ( 10 mm) on repeat testing. Individuals performing TST measurements were blinded to the QFT-GIT results. Data analysis. χ 2 tests or Fisher exact tests were used to compare categorical characteristics, and t tests were used to compare continuous characteristics. Association between dichotomized TST and QFT-GIT results was assessed by positive and negative agreement 15 and κ. 16 Proportion of positive agreement is defined as twice the number of individuals with positive results on both tests, divided by the sum of those positive on one of the tests plus those positive on the other test; negative agreement is defined in a parallel way. Test retest reliability for IFN-γ responses from the first and second QFT- GIT was measured using an intraclass correlation coefficient. A nonparametric regression smoother, lowess, was used to estimate mean change over time in Figure 4. Data analyses were performed with SPSS (version 14.0; SPSS, Chicago, IL), SAS (SAS version 9.1; SAS Institute, Cary, NC), and R (R Development Core Team; ). Graphics were produced in R. RESULTS A total of 198 refugees arriving in the United States between April 2006 and January 2007 were enrolled in the study, with an average time between arrival and enrollment of 62 days (range, days). Three refugees did not return for the second visit. A total of 159 refugees (80%) attended their third visit for repeat QFT-GIT testing. The most common reason for failure to return for Visit 3 was loss to follow-up. Five (3%) subjects refused repeat testing. Of the 87 subjects eligible for a repeat TST (first TST < 10 mm), 41 (47%) returned to have the test interpreted. The 45 patients who did not complete repeat TST testing did not differ in characteristics (age, sex, country of origin) from those who returned for retesting (data not shown). The low TST retesting rate was caused by a combination of patient fatigue and inadequate clinic resources to ensure a fourth patient visit. The average time between testing at Visits 2 and 3 was 7.5 weeks (range, 2 52 weeks). The majority of subjects were young, female, and Somali. The likelihood of testing positive for LTBI with both tests differed across categories of age and sex ( Table 1 ). Comparison of simultaneous TST and QFT-GIT. Of the 195 subjects who completed both tests, 55.4% were TST positive and 53.8% were QFT-GIT positive. No initial QFT-GIT tests were indeterminate. Diagnostic agreement between the two tests was 78% ( Table 2 ). Of refugees who were initially TST negative and QFT-GIT positive (N = 20), 12 (60%) had a QFT-GIT that narrowly exceeded the diagnostic cut-point for positivity of 0.35 IU/mL (range, IU/mL). To evaluate the effect of the value of the QFT-GIT cutpoint on diagnostic agreement with the TST, we calculated
3 630 BAKER AND OTHERS Table 1 Demographic characteristics for 195 refugees with TST and at least one QFT-GIT and comparison of subgroups with jointly positive and negative test results among 195 refugees enrolled in the study Characteristics Frequency (%) ( N = 195) TST+/QFT GIT+ (%) ( N = 85) TST /QFT GIT (%) ( N = 67) P * Age (median) 19 (range 1 81) Adult 140 (72) 72 (85) 40 (60) Child (< 18 years of age) 55 (28) 13 (15) 27 (40) Sex Male 67 (34) 44 (52) 20 (30) Female 128 (66) 41 (48) 47 (70) Country of origin Somalia 149 (76) 65 (76) 54 (81) Ethiopia 26 (13) 11 (13) 9 (13) Liberia 6 (3) 5 (6) 2 (3) Eritrea 1 (0.5) 1 (1) 0 Ghana 1 (0.5) 0 0 Zimbabwe 1 (0.5) 0 0 Ukraine 5 (2.5) 1 (1) 0 Russian Federation 2 (1) 1 (1) 0 China 4 (2) 1 (1) 2 (3) * P value was calculated using χ 2 for age and sex and Fisher exact test for country of origin. κ and positive and negative agreement with TST for cutpoints ranging from 0 to 2.0 IU/mL ( Figure 2 ). All measures of agreement were found to increase as the cut-point rose from 0.35 IU/mL, reaching their maximum at a cut-point of IU/mL. Serial QFT-GIT testing. Serial testing was completed in 159 subjects. One repeat test was indeterminate. Observed diagnostic agreement between the initial and repeat QFT- GIT was 89% (κ = 0.76; 95% CI: ) and the intraclass correlation of QFT-GIT values was (95% CI: ). Changes from the first to second QFT-GIT are shown in Figure 3. Did the initial TST increase or boost the second QFT-GIT, and if so, was this effect related to time from TST? Of 159 subjects with repeated QFT-GIT measurements, 122 subjects had a first QFT-GIT IFN-γ value < 10.0, so that an increase was possible, and had a recorded interval from TST. These intervals ranged from 2 to 52 weeks, but only eight intervals were > 16 weeks; because these are too sparsely scattered to provide much information, we restricted attention to the 114 subjects with intervals of 16 weeks or less. Figure 4 shows the change from the first QFT-GIT plotted against time from TST for these 114 subjects with a nonparametric-regression estimate of mean change as a function of time. As is visually evident in Figure 3, subjects with a positive first QFT-GIT reading tended to experience larger increases. Our null hypothesis was that changes in serial QFT-GIT IFN-γ values are random with median zero, that is, that the chance of an increase is 50%. Boosting would be shown by a significantly higher proportion of increases than decreases. To test this, we divided the 114 subjects into two groups as to whether their interval after the TST was < 5 or > 5 weeks; there is a gap in the data at Week 5 ( Figure 4 ). In the 38 subjects retested 2 5 weeks after TST, the second QFT-GIT increased 87%, with a mean increase of 2.8 ± 0.5 (SE) IU/ ml, whereas for 76 subjects retested 5 16 weeks after TST, 69% increased with mean change 0.8 ± 0.2 IU/mL. Both proportions of increases were larger than the null value of 50% (P < 0.002), and the first was also significantly greater than the second (P = 0.033). In addition, both mean changes were significantly greater than zero. In this group of refugees, there was strong evidence for boosting in the second QFT- GIT, with the rate and size of increase diminishing with time from TST. Table 2 Agreement between initial QFT-GIT and TST TST negative TST positive* QFT-GIT negative 67 (34) 23 (12) QFT-GIT positive 20 (10) 85 (44) * TST positive: 10 mm of induration. Percent of total (number of refugees = 195). QFT-GIT positive: 0.35 IU/mL IFN -γ. Overall agreement 78% ( )/195 Proportion of tests with positive (95% CI: ) agreement Proportion of tests with negative (95% CI: ) agreement κ 0.56 (95% CI: ) Figure 2. Three measures of agreement (κ, positive agreement, negative agreement) between TST and initial QFT-GIT, computed as the minimum value for a positive reading on the QFT-GIT, which varies from 0 to 2.0. The recommended value is 0.35, indicated by a vertical line.
4 QUANTIFERON-GOLD IN-TUBE FOR LTBI TESTING IN REFUGEES 631 Figure 4. Change from first to second QFT-GIT for 114 subjects against the time from TST. O = subjects with a positive QFT-GIT reading; = subjects with a negative QFT-GIT reading. The curve is a nonparametric regression estimate of the mean change as a function of time. One large decrease ( 8.1) is not shown but was included in computation. There were no cases of discordance observed among refugees with initial QFT-GIT IFN-g values > 1.0. DISCUSSION Figure 3. Change from first to second QFT-GIT for 159 subjects. Dots above the dashed line at 0.35 had a positive reading on the QFT- GIT. A second QFT-GIT measurement of 6.1 is not shown. Ignoring time from TST, 86% of subjects with a positive first QFT-GIT reading increased on the second QFT-GIT, whereas 68% of those with negative first QFT-GIT readings increased (P = for the difference). Both of these proportions were significantly greater than the null value of 50% (P < 0.004). Rates of increases were similar for those positive and negative on TST, 82% and 68%, respectively, but the difference did not reach significance (P = 0.059). However, because there was strong evidence for a time effect on boosting, averaging these rates over time may introduce bias. Among the 117 participants with initial QFT-GIT IFN-γ values 1.0 IU/mL, 18 had qualitatively discordant results (12 converted, 6 reverted). Discordance in serial testing was not related to sex or TST status or to time from TST. Refugees are a high-risk group for which an accurate diagnosis of LTBI is of paramount importance. Using the TST as a screening test in this population is fraught with diagnostic challenges such as false positives with BCG immunization 17 or NTM infection. In addition, skin testing requiring two clinic visits is a logistic challenge for refugees and public health clinics. Within our programmatic setting, only 47% of eligible patients completed repeat TST testing for the purpose of this study. This finding suggests that similar rates of return for follow-up testing during contact studies may be expected in comparable patient populations. In addition to the practical issues outlined above, our study supports previous findings that the QFT-GIT may have slightly better agreement with the TST than other generations of the test used in similar high-risk situations. In the study of Calvalho and others 18 of immigrants in Italy, agreement between the TST and QuantiFERON-TB Gold was 71%, (κ = 0.37). However, in the report of Winjie and others 9 of asylum seekers in Norway, agreement between the two tests was better at 79% (κ = 0.51). Similarly, we found positive and negative agreement of nearly 80% (κ = 0.56). Furthermore, we observed fewer indeterminate (N = 1) results than in other studies. 2 Screening with the QFT-GIT is not free of challenges. One concern is how to interpret a minimally positive QFT-GIT ( IU/mL) in the setting of a negative TST. Without a true gold standard or longitudinal studies following subjects with negative TSTs and positive QFT-GITs to determine the likelihood of developing active TB, it is difficult to know whether the QFT-GIT is in fact more sensitive and how to proceed clinically in terms of offering treatment of LTBI. Another potential issue with the QFT-GIT is reproducibility. As in serial skin testing, we observed nonspecific variation in serial QFT-GIT testing. Such nonspecific variation leading to discordance in serial testing has been observed in other studies. 19 We found that this nonspecific variation resulted in a small proportion of cases (11%) in which the diagnosis of LTBI based on QFT-GIT results could be called into question.
5 632 BAKER AND OTHERS This seemed to occur only in refugees with initial QFT-GIT IFN-γ values < 1.0 IU/mL, suggesting that a QFT-GIT result with a value > 1.0 IU/mL may be more likely to indicate a true positive. Within our population of refugees, diagnostic agreement between simultaneous TST and QFT-GIT was found to increase as the cut-point for QFT-GIT test positivity was raised, reaching a maximum at a cut-point of IU/mL. This suggests that, in a population with presumed high rates of LTBI, a higher cut-point might result in fewer instances in which refugees without LTBI are misclassified as having LTBI (false positive). On the other hand, raising the cut-point for the sake of better agreement may increase the likelihood of a false negative. From a public health and patient perspective, this may not be wise, because the potential for a missed diagnosis of LTBI would likely present a greater hazard to the patient and the public. Given that there is no gold standard for LTBI testing, longitudinal studies looking at the likelihood of developing active TB after a positive QFT-GIT will ideally provide more information on the appropriate cut-point for the test. We observed that, during serial testing, a significant proportion (2/3) of refugees had a higher second QFT-GIT test value. Those with a positive first QFT-GIT reading tended to experience larger increases. We speculate that this difference may be the result of boosting of a true-positive QFT-GIT from an antecedent skin test. Although the presence of a possible boosting phenomenon was qualitatively present in some cases, it did not frequently affect the diagnostic results of the QFT- GIT. In the 70% of refugees that had a larger second QFT- GIT value, only 7% had tests that qualitatively converted from negative to positive. Previous studies examining whether TST testing results in boosting of QFT-GIT results were inconclusive and suggested that the presence of boosting may be related to the time interval between testing with the two modalities. 12,13 We found that there was strong evidence for boosting of the second QFT- GIT but that the rate and size of increase diminished with time from TST. Therefore, it seems that skin testing performed > 6 weeks before screening with the QFT-GIT would be less likely to result in boosting of the QFT-GIT result. There were some important limitations to our study. We did not collect individual data on BCG vaccination because confirmation of immunization was unavailable. However, we felt confident that the literature supported the QFT-GIT s high specificity with respect to BCG, 5 and the majority of subjects in our study were Somali, a group with one of the highest annual TB case rates (889/100,000) among the foreign-borne in the United States. 20 As well, all patients received a TST, which limited our ability to definitively conclude whether the increased IFN-γ values seen with the second QFT-GIT were caused by boosting or other host factors. In conclusion, the QFT-GIT holds promise to replace the TST for LTBI screening in refugee populations resettling to low-incidence countries. Boosting of a QFT-GIT result because of an antecedent TST in the context of prior tuberculosis exposure may occur in refugees who are screened with both modalities during the resettlement process or during contact studies. Such boosting should be considered to be caused by prior infection with TB because the QFT-GIT s specificity eliminates the possibility of boosting caused by BCG. Although observed, boosting rarely seems to alter the clinical applicability of the test. Furthermore, the rate and size of boosting seems to diminish over time from TST, with little boosting seen after 6 weeks. In a refugee screening setting, it is reasonable to consider a QFT-GIT positive if its value is > 0.35 IU/mL, given the high prevalence of LTBI in refugees from TB-endemic countries and the potentially greater personal and public health risk of a missed diagnosis. Ideally, longitudinal studies looking at the likelihood of developing active TB given a minimally positive QFT-GIT will help to clarify the issue of the appropriate cut-point for the test. Finally, additional research is needed to better understand the reasons for the test s variability in this and other populations. Studies looking at the interaction between host factors and test reproducibility would be of interest. Received June 5, Accepted for publication November 20, Acknowledgments: The authors thank Kathy Kennedy from the Hennepin County Medical Center Microbiology Laboratory for technological expertise. Financial support: This work was funded, in part, by a research grant from the International Society of Travel Medicine. The QuantiFERON-TB Gold In-Tube tests were provided at no cost by Cellestis. Disclaimer: The authors state that they have no conflicts of interest. Authors addresses: Cristina A. Baker, William M. Stauffer, Phillip K. Peterson, and Dean T. Tsukayama, Infectious Diseases and International Medicine Division, University of Minnesota, 420 Delaware St. SE, Minneapolis, MN 55455, s: bake0088@umn.edu, stauf005@umn.edu, peter137@umn.edu, and tsuka001@umn.edu. William Thomas, Division of Biostatistics, School of Public Health University of Minnesota, 420 Delaware St. SE, Minneapolis, MN 55455, thoma003@umn.edu. REFERENCES 1. Centers for Disease Control, Trends in tuberculosis United States, Morbid Mortal Wkly Rev MMWR 57: Ferrara G, Losi M, D Amico R, Roversi P, Piro R, Meacci M, Meccugni B, Dori IM, Andreani A, Bergamini BM, Mussini C, Rumpianesi F, Fabbri LM, Richeldi L, Use in routine clinical practice of two commercial blood tests for diagnosis of infection with Mycobacterium tuberculosis : a prospective study. Lancet 367: Shah SS, McGowan JP, Klein RS, Converse PJ, Blum S, Gourevitch MN, Agreement between Mantoux skin testing and QuantiFERON-TB assay using dual mycobacterial antigens in current and former injection drug users. Med Sci Monit 12: MT11 MT Taggart EW, Hill HR, Ruegner RG, Litwin CM, Evaluation of an in vitro assay for interferon gamma production in response to the Mycobacterium tuberculosis -synthesized peptide antigens ESAT-6 and CFP-10 and the PPD skin test. Am J Clin Pathol 125: Menzies D, Pai M, Comstock G, Meta-analysis: new tests for the diagnosis of latent tuberculosis infection: areas of uncertainty and recommendations for research. Ann Intern Med 146: Dewan PK, Grinsdale J, Liska S, Wong E, Fallstad R, Kawamura LM, Feasibility, acceptability, and cost of tuberculosis testing by whole-blood interferon-gamma assay. BMC Infect Dis 6: Mahomed H, Hughes EJ, Hawkridge T, Minnies D, Simon E, Little F, Hanekom WA, Geiter L, Hussey GD, Comparison of mantoux skin test with three generations of a whole blood IFNgamma assay for tuberculosis infection. Int J Tuberc Lung Dis 10: Pai M, Gokhale K, Joshi R, Dogra S, Kalantri S, Mendiratta DK, Narang P, Daley CL, Granich RM, Mazurek GH, Reingold AL,
6 QUANTIFERON-GOLD IN-TUBE FOR LTBI TESTING IN REFUGEES 633 Riley LW, Colford JM Jr, Mycobacterium tuberculosis infection in health care workers in rural India: comparison of a whole-blood interferon gamma assay with tuberculin skin testing. JAMA 293: Winje BA, Oftung F, Korsvold GE, Mannsaker T, Jeppesen AS, Harstad I, Heier BT, Heldal E, Screening for tuberculosis infection among newly arrived asylum seekers: comparison of QuantiFERONTB Gold with tuberculin skin test. BMC Infect Dis 8: Menzies D, Interpretation of repeated tuberculin tests. Boosting, conversion, and reversion. Am J Respir Crit Care Med 159: Cauthen GM, Snider DE Jr, Onorato IM, Boosting of tuberculin sensitivity among Southeast Asian refugees. Am J Respir Crit Care Med 149: Leyten EM, Prins C, Bossink AW, Thijsen S, Ottenhoff TH, van Dissel JT, Arend SM, Effect of tuberculin skin testing on a Mycobacterium tuberculosis -specific IFN-{gamma} assay. Eur Respir J 29: Naseer A, Naqvi S, Kampmann B, Evidence for boosting Mycobacterium tuberculosis -specific IFN-gamma responses at 6 weeks following tuberculin skin testing. Eur Respir J 29: Choi JC, Shin JW, Kim JY, Park IW, Choi BW, Lee MK, The effect of previous tuberculin skin test on the follow-up examination of whole-blood interferon-gamma assay in the screening for latent tuberculosis infection. Chest 133: Graham P, Bull B, Approximate standard errors and confidence intervals for indices of positive and negative agreement. J Clin Epidemiol 51: Cohen J, A coefficient of agreement for nominal scales. Educ Psychol Meas 20: Farhat M, Greenaway C, Pai M, Menzies D, False-positive tuberculin skin tests: what is the absolute effect of BCG and nontuberculous mycobacteria? Int J Tuberc Lung Dis 10: Carvalho AC, Pezzoli MC, El-Hamad I, Arce P, Bigoni S, Scarcella C, Indelicato AM, Scolari C, Carosi G, Matteelli A, QuantiFERON-TB Gold test in the identification of latent tuberculosis infection in immigrants. J Infect 55: Pai M, Joshi R, Dogra S, Mendiratta DK, Narang P, Kalantri S, Reingold AL, Colford JM Jr, Riley LW, Menzies D, Serial testing of health care workers for tuberculosis using interferongamma assay. Am J Respir Crit Care Med 174: Cain KP, Benoit SR, Winston CA, Mac Kenzie WR, Tuberculosis among foreign-born persons in the United States. JAMA 300:
Lisa Y. Armitige, MD, PhD has the following disclosures to make:
 Interferon Gamma Release Assays (IGRAs) Lisa Y. Armitige, MD, PhD May 13, 2015 TB for Pulmonologist Phoenix, AZ March 13, 2015 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following
Interferon Gamma Release Assays (IGRAs) Lisa Y. Armitige, MD, PhD May 13, 2015 TB for Pulmonologist Phoenix, AZ March 13, 2015 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following
T tuberculin Skin Test (TST) and QFT-GIT in Military Personnel
 2 COMPARISON OF MANTOUX AND QUANTIFERON-TB GOLD TEST FOR DIAGNOSIS OF LATENT TUBERCULOSIS INFECTION IN ARMY PERSONNEL Willeke P.J. Franken 1, Joost F. Timmermans 2, Corine Prins 1, Evert-Jan H.J. Slootman
2 COMPARISON OF MANTOUX AND QUANTIFERON-TB GOLD TEST FOR DIAGNOSIS OF LATENT TUBERCULOSIS INFECTION IN ARMY PERSONNEL Willeke P.J. Franken 1, Joost F. Timmermans 2, Corine Prins 1, Evert-Jan H.J. Slootman
CDC TB Testing Guidelines and Recent Literature Update
 Pocket Guide QuantiFERON -TB Gold CDC TB Testing Guidelines and Recent Literature Update Using IGRAs for TB screening in your patients June 2010 A full copy of the US Centers for Disease Control and Prevention
Pocket Guide QuantiFERON -TB Gold CDC TB Testing Guidelines and Recent Literature Update Using IGRAs for TB screening in your patients June 2010 A full copy of the US Centers for Disease Control and Prevention
What is an IGRA? What is an IGRA? Are they available here? How do I use them? Learning Objectives
 What is an IGRA? Are they available here? How do I use them? Debbie Staley, RN, MPH TB Nurse Consultant VDH Division of Disease Prevention TB Control Program Learning Objectives Participants will be able
What is an IGRA? Are they available here? How do I use them? Debbie Staley, RN, MPH TB Nurse Consultant VDH Division of Disease Prevention TB Control Program Learning Objectives Participants will be able
Guidelines for TB Blood Testing. Minnesota Department of Health TB Prevention and Control Program June 2011
 Guidelines for TB Blood Testing Minnesota Department of Health TB Prevention and Control Program June 2011 Outline Interferon-Gamma Release Assays aka TB blood tests 1. What are they? 2. What are the current
Guidelines for TB Blood Testing Minnesota Department of Health TB Prevention and Control Program June 2011 Outline Interferon-Gamma Release Assays aka TB blood tests 1. What are they? 2. What are the current
Role of Quantiferon-TB Gold Assays in Detecting Latent Tuberculous Infection among Contacts of Active Tuberculous Patients *
 Med. J. Cairo Univ., Vol. 79, No. 1, June 169-175, 2011 www.medicaljournalofcairouniversity.com Role of Quantiferon-TB Gold Assays in Detecting Latent Tuberculous Infection among Contacts of Active Tuberculous
Med. J. Cairo Univ., Vol. 79, No. 1, June 169-175, 2011 www.medicaljournalofcairouniversity.com Role of Quantiferon-TB Gold Assays in Detecting Latent Tuberculous Infection among Contacts of Active Tuberculous
Journal of Infectious Diseases Advance Access published January 26, 2015
 Journal of Infectious Diseases Advance Access published January 26, 2015 1 Effect of immune status on serial QuantiFERON-TB Gold In-Tube LTBI screening in persons with HIV in a low TB incidence country
Journal of Infectious Diseases Advance Access published January 26, 2015 1 Effect of immune status on serial QuantiFERON-TB Gold In-Tube LTBI screening in persons with HIV in a low TB incidence country
Interferon-gamma-release assays: Better than tuberculin skin testing?
 REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will use and interpret the new blood tests for tuberculosis correctly CYNDEE MIRANDA, MD Department of Infectious Disease, Medicine Institute, Cleveland
REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will use and interpret the new blood tests for tuberculosis correctly CYNDEE MIRANDA, MD Department of Infectious Disease, Medicine Institute, Cleveland
DRAFT FOR CONSULTATION
 Interferon Gamma Release Assay (IGRA) testing for tuberculosis (TB) - Questions & Answers (Q&As) For Health Care Workers HPA Tuberculosis Programme Board DRAFT FOR CONSULTATION October 2007 Interferon
Interferon Gamma Release Assay (IGRA) testing for tuberculosis (TB) - Questions & Answers (Q&As) For Health Care Workers HPA Tuberculosis Programme Board DRAFT FOR CONSULTATION October 2007 Interferon
Interferon-gamma Release Assays: the Good, the Bad, and the Ugly
 Interferon-gamma Release Assays: the Good, the Bad, and the Ugly Susan E. Dorman, MD Center for TB Research Johns Hopkins University School of Medicine Maryland Center for Tuberculosis Control and Prevention
Interferon-gamma Release Assays: the Good, the Bad, and the Ugly Susan E. Dorman, MD Center for TB Research Johns Hopkins University School of Medicine Maryland Center for Tuberculosis Control and Prevention
Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB)
 Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB) Draft Interim HPA Guidance HPA Tuberculosis Programme Board Health Protection
Health Protection Agency position statement on the use of Interferon Gamma Release Assay (IGRA) tests for Tuberculosis (TB) Draft Interim HPA Guidance HPA Tuberculosis Programme Board Health Protection
Tuberculosis Contact Investigation in a Renal Dialysis Center: Blood Vs. Skin test
 Tuberculosis Contact Investigation in a Renal Dialysis Center: Blood Vs. Skin test Kevin L. Winthrop M.D., M.P.H. Assistant Professor of Medicine Divisions of Infectious Diseases and Public Health and
Tuberculosis Contact Investigation in a Renal Dialysis Center: Blood Vs. Skin test Kevin L. Winthrop M.D., M.P.H. Assistant Professor of Medicine Divisions of Infectious Diseases and Public Health and
Frequently Asked Questions
 Frequently Asked Questions QuantiFERON -TB Gold Health Professionals www.quantiferon.com 2 FAQ - Health Professionals Table of contents About TB 6 What is latent TB? And how is it different from active
Frequently Asked Questions QuantiFERON -TB Gold Health Professionals www.quantiferon.com 2 FAQ - Health Professionals Table of contents About TB 6 What is latent TB? And how is it different from active
QuantiFERON -TB Gold In-Tube test (QFT-GIT) for the screening of latent tuberculosis in recent immigrants to Italy
 NEW MICROBIOLOGICA, 32, 369-376, 2009 QuantiFERON -TB Gold In-Tube test (QFT-GIT) for the screening of latent tuberculosis in recent immigrants to Italy Annalisa Saracino 1, Gaetano Scotto 1, Chiara Fornabaio
NEW MICROBIOLOGICA, 32, 369-376, 2009 QuantiFERON -TB Gold In-Tube test (QFT-GIT) for the screening of latent tuberculosis in recent immigrants to Italy Annalisa Saracino 1, Gaetano Scotto 1, Chiara Fornabaio
Nevada State Health Division Technical Bulletin
 Nevada State Health Division Technical Bulletin Topic: Using QuantiFERON and Tuberculin Skin Test to Screen for TB Section/Program/Contact: Bureau of Community Health / Tuberculosis Program / Susanne Paulson,
Nevada State Health Division Technical Bulletin Topic: Using QuantiFERON and Tuberculin Skin Test to Screen for TB Section/Program/Contact: Bureau of Community Health / Tuberculosis Program / Susanne Paulson,
Chapter 3 Testing for Tuberculosis Infection and Disease
 Chapter 3 Testing for Tuberculosis Infection and Disease Table of Contents Chapter Objectives.... 45 Introduction.... 47 Identifying High-Risk Groups for M. tuberculosis Testing... 47 Testing Methods for
Chapter 3 Testing for Tuberculosis Infection and Disease Table of Contents Chapter Objectives.... 45 Introduction.... 47 Identifying High-Risk Groups for M. tuberculosis Testing... 47 Testing Methods for
Perils and Pitfalls in Clinical Trials of Diagnostic Tests for Tuberculosis. Richard O Brien, MD Foundation for Innovative New Diagnostics Geneva
 Perils and Pitfalls in Clinical Trials of Diagnostic Tests for Tuberculosis Richard O Brien, MD Foundation for Innovative New Diagnostics Geneva 1 Outline of Presentation Statement of the problem Common
Perils and Pitfalls in Clinical Trials of Diagnostic Tests for Tuberculosis Richard O Brien, MD Foundation for Innovative New Diagnostics Geneva 1 Outline of Presentation Statement of the problem Common
No influence of haemodialysis on interferon production in the QuantiFERON-TB Gold-In-Tube test
 ORIGINAL ARTICLE JN EPHROL 24( 2011; 05) : 625-630 DOI:10.5301/JN.2011.6325 No influence of haemodialysis on interferon production in the QuantiFERON-TB Gold-In-Tube test Martine Hoogewerf 1, Greet J.
ORIGINAL ARTICLE JN EPHROL 24( 2011; 05) : 625-630 DOI:10.5301/JN.2011.6325 No influence of haemodialysis on interferon production in the QuantiFERON-TB Gold-In-Tube test Martine Hoogewerf 1, Greet J.
Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention
 Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention Screening Infants and Children for Tuberculosis in Massachusetts Executive Summary In Massachusetts,
Massachusetts Department of Public Health Division of Global Populations and Infectious Disease Prevention Screening Infants and Children for Tuberculosis in Massachusetts Executive Summary In Massachusetts,
Serial Testing for TB Infection with IGRAs: Understanding the Sources of Variability
 Serial Testing for TB Infection with IGRAs: Understanding the Sources of Variability Niaz Banaei MD Assistant Professor of Pathology and Medicine Director, Fellowship in Global Health Diagnostics Director,
Serial Testing for TB Infection with IGRAs: Understanding the Sources of Variability Niaz Banaei MD Assistant Professor of Pathology and Medicine Director, Fellowship in Global Health Diagnostics Director,
Assessing patients for infection with Mycobacterium tuberculosis
 ORIGINAL STUDIES The Likelihood of an Indeterminate Test Result from a Whole-Blood Interferon- Release Assay for the Diagnosis of Mycobacterium tuberculosis Infection in Children Correlates With Age and
ORIGINAL STUDIES The Likelihood of an Indeterminate Test Result from a Whole-Blood Interferon- Release Assay for the Diagnosis of Mycobacterium tuberculosis Infection in Children Correlates With Age and
An Evaluation of QuantiFERON-TB Gold In-Tube and Immunological Tests for TB Diagnosis in Iraqi Patients
 An Evaluation of QuantiFERON-TB Gold In-Tube and Immunological Tests for TB Diagnosis in Iraqi Patients Mohemid M. Al-Jebouri 1 and Nuha M. Wahid 2 1 Department of Microbiology, College of Medicine, University
An Evaluation of QuantiFERON-TB Gold In-Tube and Immunological Tests for TB Diagnosis in Iraqi Patients Mohemid M. Al-Jebouri 1 and Nuha M. Wahid 2 1 Department of Microbiology, College of Medicine, University
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California
 Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection
 San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection Rationale When to Screen for TB Choosing the Right TB Test Patient Registration Pre-Test
San Francisco Guidelines on the Use of QuantiFERON-TB Gold (In Tube Method) for the Diagnosis of Latent TB Infection Rationale When to Screen for TB Choosing the Right TB Test Patient Registration Pre-Test
Updated Guidelines for Using Interferon Gamma Release Assays to Detect Mycobacterium tuberculosis Infection United States, 2010
 Morbidity and Mortality Weekly Report www.cdc.gov/mmwr Recommendations and Reports June 25, 2010 / Vol. 59 / No. RR-5 Updated Guidelines for Using Interferon Gamma Release Assays to Detect Mycobacterium
Morbidity and Mortality Weekly Report www.cdc.gov/mmwr Recommendations and Reports June 25, 2010 / Vol. 59 / No. RR-5 Updated Guidelines for Using Interferon Gamma Release Assays to Detect Mycobacterium
Pediatric Latent TB Diagnosis and Treatment
 Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
SPECIAL FEATURES: HEALTH POLICY
 Public Health Nursing 0737-1209/ 2013 Wiley Periodicals, Inc. doi: 10.1111/phn.12083 SPECIAL FEATURES: HEALTH POLICY Cost-effectiveness of Using Quantiferon Gold (QFT-G) versus Tuberculin Skin Test (TST)
Public Health Nursing 0737-1209/ 2013 Wiley Periodicals, Inc. doi: 10.1111/phn.12083 SPECIAL FEATURES: HEALTH POLICY Cost-effectiveness of Using Quantiferon Gold (QFT-G) versus Tuberculin Skin Test (TST)
University of Nebraska Medical Center, Department of Health Services Research and Administration, Omaha, NE
 Research Mycobacterium Tuberculosis Infection, Immigration Status, and Diagnostic Discordance: A Comparison of Tuberculin Skin Test and QuantiFERON -TB Gold In-Tube Test Among Immigrants to the U.S. Fernando
Research Mycobacterium Tuberculosis Infection, Immigration Status, and Diagnostic Discordance: A Comparison of Tuberculin Skin Test and QuantiFERON -TB Gold In-Tube Test Among Immigrants to the U.S. Fernando
Interferon Gamma Release Assays (IGRAs) in the Diagnosis of Tuberculosis
 Interferon Gamma Release Assays (IGRAs) in the Diagnosis of Tuberculosis Richard B. Clark, PhD, D(ABMM) Quest Diagnostics Nichols Institute Chantilly, VA Dale Schwab, PhD, D(ABMM) Quest Diagnostics Nichols
Interferon Gamma Release Assays (IGRAs) in the Diagnosis of Tuberculosis Richard B. Clark, PhD, D(ABMM) Quest Diagnostics Nichols Institute Chantilly, VA Dale Schwab, PhD, D(ABMM) Quest Diagnostics Nichols
Recent Advances in The Treatment of Mycobacterium Tuberculosis
 Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY. Stephanie N. Lin MD 2/12/2016
 TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
The QuantiFERON-TB Gold test in the diagnosis and. treatment of latent tuberculosis in patients from a
 The QuantiFERON-TB Gold test in the diagnosis and treatment of latent tuberculosis in patients from a Norwegian outpatient clinic Anne Margarita Dyrhol-Riise 1, Gerd Gran 2, Tore Wenzel Larsen 3, Bjørn
The QuantiFERON-TB Gold test in the diagnosis and treatment of latent tuberculosis in patients from a Norwegian outpatient clinic Anne Margarita Dyrhol-Riise 1, Gerd Gran 2, Tore Wenzel Larsen 3, Bjørn
(In-Tube Method) The Whole Blood IFN-gamma Test Measuring Responses to ESAT-6, CFP-10 & TB7.7 Peptide Antigens PACKAGE INSERT
 (In-Tube Method) The Whole Blood IFN-gamma Test Measuring Responses to ESAT-6, CFP-10 & TB7.7 Peptide Antigens PACKAGE INSERT For In Vitro Diagnostic Use BlanK Page INDEX 1. INTENDED USE 2 2. SUMMARY AND
(In-Tube Method) The Whole Blood IFN-gamma Test Measuring Responses to ESAT-6, CFP-10 & TB7.7 Peptide Antigens PACKAGE INSERT For In Vitro Diagnostic Use BlanK Page INDEX 1. INTENDED USE 2 2. SUMMARY AND
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015
 Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
A Three-Way Comparison of Tuberculin Skin Testing, QuantiFERON-TB Gold and T-SPOT.TB in Children
 A Three-Way Comparison of Tuberculin Skin Testing, QuantiFERON-TB Gold and T-SPOT.TB in Children Tom G. Connell 1,2,3., Nicole Ritz 1,2,3., Georgia A. Paxton 4, Jim P. Buttery 1,2,3, Nigel Curtis 1,2,3
A Three-Way Comparison of Tuberculin Skin Testing, QuantiFERON-TB Gold and T-SPOT.TB in Children Tom G. Connell 1,2,3., Nicole Ritz 1,2,3., Georgia A. Paxton 4, Jim P. Buttery 1,2,3, Nigel Curtis 1,2,3
What You Need to Know About Collecting QuantiFERON (QFT) TB Gold In-Tube Samples
 What You Need to Know About Collecting QuantiFERON (QFT) TB Gold In-Tube Samples I. What is QuantiFERON (QFT) TB Gold In-Tube? II. III. QFT is an interferon-gamma release assay (IGRA). QFT is a blood test.
What You Need to Know About Collecting QuantiFERON (QFT) TB Gold In-Tube Samples I. What is QuantiFERON (QFT) TB Gold In-Tube? II. III. QFT is an interferon-gamma release assay (IGRA). QFT is a blood test.
ALTERNATIVES TO THE TUBERCULIN SKIN TEST: INTERFERON-γ ASSAYS IN THE DIAGNOSIS OF MYCOBACTERIUM TUBERCULOSIS INFECTION
 Indian Journal of Medical Microbiology, (2005) 23 (3):151-158 Review Article ALTERNATIVES TO THE TUBERCULIN SKIN TEST: INTERFERON-γ ASSAYS IN THE DIAGNOSIS OF MYCOBACTERIUM TUBERCULOSIS INFECTION M Pai
Indian Journal of Medical Microbiology, (2005) 23 (3):151-158 Review Article ALTERNATIVES TO THE TUBERCULIN SKIN TEST: INTERFERON-γ ASSAYS IN THE DIAGNOSIS OF MYCOBACTERIUM TUBERCULOSIS INFECTION M Pai
Diagnosis of Tuberculosis Infection
 Diagnosis of Tuberculosis Infection CONTENTS Introduction... 7.2 Purpose... 7.2 Policy... 7.2 High-Risk Groups... 7.3 Diagnosis of Tuberculosis Infection... 7.4 Interferon gamma release assays... 7.4 Mantoux
Diagnosis of Tuberculosis Infection CONTENTS Introduction... 7.2 Purpose... 7.2 Policy... 7.2 High-Risk Groups... 7.3 Diagnosis of Tuberculosis Infection... 7.4 Interferon gamma release assays... 7.4 Mantoux
Paediatrica Indonesiana. Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation
 Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Childhood Tuberculosis Some Basic Issues. Jeffrey R. Starke, M.D. Baylor College of Medicine
 Childhood Tuberculosis Some Basic Issues Jeffrey R. Starke, M.D. Baylor College of Medicine TUBERCULOSIS IS A SOCIAL DISEASE WITH MEDICAL IMPLICATIONS THE GREAT PARADOX OF TUBERCULOSIS A CAUTIONARY TALE
Childhood Tuberculosis Some Basic Issues Jeffrey R. Starke, M.D. Baylor College of Medicine TUBERCULOSIS IS A SOCIAL DISEASE WITH MEDICAL IMPLICATIONS THE GREAT PARADOX OF TUBERCULOSIS A CAUTIONARY TALE
T()LED() Name ofpolicy: Mandatory Tuberculosis (TB) Screening of Students from World Health Organization Designated High TB Prevalence Countries
 Name ofpolicy: Mandatory Tuberculosis (TB) Screening of Students from World Health Organization Designated High TB Prevalence Countries Policy Number: 3364-81-04-030 T()LED() Revision date: I 0/22/13 Approving
Name ofpolicy: Mandatory Tuberculosis (TB) Screening of Students from World Health Organization Designated High TB Prevalence Countries Policy Number: 3364-81-04-030 T()LED() Revision date: I 0/22/13 Approving
Tuberculosis. Subject. Goal/Objective. Instructions. Rationale. Operations Directorate, Health Branch Immigration Medical Examination Instructions
 Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Pregnancy and Tuberculosis. Information for clinicians
 Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
The Cost Effectiveness of Interferon Gamma Release Assays Versus Tuberculin Skin Tests in Health Care
 ORIGINAL INVESTIGATION Cost-effectiveness of Interferon Gamma Release Assays vs Tuberculin Skin Tests in Health Care Workers Marie A. de Perio, MD; Joel Tsevat, MD, MPH; Gary A. Roselle, MD; Stephen M.
ORIGINAL INVESTIGATION Cost-effectiveness of Interferon Gamma Release Assays vs Tuberculin Skin Tests in Health Care Workers Marie A. de Perio, MD; Joel Tsevat, MD, MPH; Gary A. Roselle, MD; Stephen M.
Refugees with diabetes mellitus have higher prevalence of latent tuberculosis infection
 Refugees with diabetes mellitus have higher prevalence of latent tuberculosis infection Matthew Magee Division of Epidemiology and Biostatistics School of Public Health, Georgia State University Saturday,
Refugees with diabetes mellitus have higher prevalence of latent tuberculosis infection Matthew Magee Division of Epidemiology and Biostatistics School of Public Health, Georgia State University Saturday,
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG
 TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
Department of Internal Medicine, Division of Cardiovascular Diseases. Department of Internal Medicine. Department of Internal Medicine
 Use of the QuantiFERON -TB Gold Assay in Pregnant Patients Bassem M.Chehab, M.D. 1, K. James Kallail, Ph.D. 2, Riad O. El Fakih, M.D. 3, Rosalee E. Zackula, M.A. 4, Garold O. Minns, M.D. 2 1 University
Use of the QuantiFERON -TB Gold Assay in Pregnant Patients Bassem M.Chehab, M.D. 1, K. James Kallail, Ph.D. 2, Riad O. El Fakih, M.D. 3, Rosalee E. Zackula, M.A. 4, Garold O. Minns, M.D. 2 1 University
CTCA POSITION ON TB EXAMINATION OF SCHOOL EMPLOYEES AND VOLUNTEERS
 CTCA POSITION ON TB EXAMINATION OF SCHOOL EMPLOYEES AND VOLUNTEERS Introduction Although progress has been made, tuberculosis (TB) continues to be a significant public health problem; appropriate TB examination
CTCA POSITION ON TB EXAMINATION OF SCHOOL EMPLOYEES AND VOLUNTEERS Introduction Although progress has been made, tuberculosis (TB) continues to be a significant public health problem; appropriate TB examination
Managing Contacts. Challenges... 202. General Principles... 204. Summary of Options... 205. Variables to Consider... 205. Treatment Options...
 10 Managing Contacts Challenges............ 202 General Principles...... 204 Summary of Options.... 205 Variables to Consider... 205 Treatment Options...... 206 Treatment of Children... 209 Window Prophylaxis....
10 Managing Contacts Challenges............ 202 General Principles...... 204 Summary of Options.... 205 Variables to Consider... 205 Treatment Options...... 206 Treatment of Children... 209 Window Prophylaxis....
For reprint orders, please contact reprints@future-drugs.com. Diagnosis of latent. Expert Rev. Anti Infect. Ther. 3(6), 981 993 (2005)
 Review For reprint orders, please contact reprints@future-drugs.com Diagnosis of latent Mycobacterium tuberculosis infection: is the demise of the Mantoux test imminent? James S Rothel and Peter Andersen
Review For reprint orders, please contact reprints@future-drugs.com Diagnosis of latent Mycobacterium tuberculosis infection: is the demise of the Mantoux test imminent? James S Rothel and Peter Andersen
Frequently Asked Questions
 Frequently Asked Questions QuantiFERON-TB Gold Health Professionals www.quantiferon.com Table of contents About TB 4 What is latent TB? And how is it different to active TB disease? 4 What is the meaning
Frequently Asked Questions QuantiFERON-TB Gold Health Professionals www.quantiferon.com Table of contents About TB 4 What is latent TB? And how is it different to active TB disease? 4 What is the meaning
Role of QuantiFERON-TB Test in Detection of Children Infected with Mycobacterium tuberculosis
 ORIGINAL ARTICLE Tanaffos (2010) 9(3), 22-27 2010 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Role of QuantiFERON-TB Test in Detection of Children Infected with Mycobacterium
ORIGINAL ARTICLE Tanaffos (2010) 9(3), 22-27 2010 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Role of QuantiFERON-TB Test in Detection of Children Infected with Mycobacterium
Interferon-gamma release assays during follow-up of tuberculin skin test-positive contacts
 INT J TUBERC LUNG DIS 12(11):1286 1294 2008 The Union Interferon-gamma release assays during follow-up of tuberculin skin test-positive contacts W. P. J. Franken,* S. M. Arend,* S. F. T. Thijsen, J. J.
INT J TUBERC LUNG DIS 12(11):1286 1294 2008 The Union Interferon-gamma release assays during follow-up of tuberculin skin test-positive contacts W. P. J. Franken,* S. M. Arend,* S. F. T. Thijsen, J. J.
How To Test For Latent Tuberculosis
 IGRAs: What do they tell and what don t they tell us? 2 nd European Advanced Clinical Tuberculosis Course Monday 22 nd September 2014 Amsterdam, Netherlands Ibrahim Abubakar Professor of Infectious Disease
IGRAs: What do they tell and what don t they tell us? 2 nd European Advanced Clinical Tuberculosis Course Monday 22 nd September 2014 Amsterdam, Netherlands Ibrahim Abubakar Professor of Infectious Disease
Tuberculin Skin Testing
 Document Number PD2009_005 Publication date 30-Jan-2009 Tuberculin Skin Testing Functional Sub group Clinical/ Patient Services - Infectious diseases Clinical/ Patient Services - Medical Treatment Population
Document Number PD2009_005 Publication date 30-Jan-2009 Tuberculin Skin Testing Functional Sub group Clinical/ Patient Services - Infectious diseases Clinical/ Patient Services - Medical Treatment Population
Research Article Tuberculin Skin Tests versus Interferon-Gamma Release Assays in Tuberculosis Screening among Immigrant Visa Applicants
 Tuberculosis Research and Treatment, Article ID 217969, 11 pages http://dx.doi.org/10.1155/2014/217969 Research Article Tuberculin Skin Tests versus Interferon-Gamma Release Assays in Tuberculosis Screening
Tuberculosis Research and Treatment, Article ID 217969, 11 pages http://dx.doi.org/10.1155/2014/217969 Research Article Tuberculin Skin Tests versus Interferon-Gamma Release Assays in Tuberculosis Screening
American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine
 American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine West Virginia University gjuckett@hsc.wvu.edu Objectives
American College Health Association (ACHA) TB Screening and Targeted Testing Recommendations Gregory Juckett, MD, MPH Professor of Family Medicine West Virginia University gjuckett@hsc.wvu.edu Objectives
QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company
 QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company P1078 TB APPRISE TB Ante vs. Postpartum Prevention with INH in HIV Seropositive mothers and their Exposed
QuantiFERON TB Gold In Tube Method (QGIT Test) Manufacturer: Cellestis Inc. (USA) a QIAGEN Company P1078 TB APPRISE TB Ante vs. Postpartum Prevention with INH in HIV Seropositive mothers and their Exposed
Santa Clara County Tuberculosis Screening Requirement for School Entrance Effective June 1, 2014. Frequently Asked Questions
 Frequently Asked Questions A child has history of BCG vaccination, should they have TST or IGRA? According to the American Academy of Pediatrics Red Book (2012), Interferon Gamma Release Assay (IGRA) is
Frequently Asked Questions A child has history of BCG vaccination, should they have TST or IGRA? According to the American Academy of Pediatrics Red Book (2012), Interferon Gamma Release Assay (IGRA) is
Int j med invest.2(3):166-175 October
 Original article The comparison of tuberculin skin test and quantiferon-tb gold test for the determination of latent tuberculosis infection ın healthcare workers in a pulmonary diseases hospital Derya
Original article The comparison of tuberculin skin test and quantiferon-tb gold test for the determination of latent tuberculosis infection ın healthcare workers in a pulmonary diseases hospital Derya
Guidelines for Tuberculosis Control in New Zealand 2010 Chapter 8: Diagnosis and Treatment of Latent Tuberculosis Infection
 Guidelines for Tuberculosis Control in New Zealand 2010 Chapter 8: Diagnosis and Treatment of Latent Tuberculosis Infection Ministry of Health. 2010. Guidelines for Tuberculosis Control in New Zealand
Guidelines for Tuberculosis Control in New Zealand 2010 Chapter 8: Diagnosis and Treatment of Latent Tuberculosis Infection Ministry of Health. 2010. Guidelines for Tuberculosis Control in New Zealand
Pathologie Biologie 57 (2009) e49 e53. Original article
 Pathologie Biologie 57 (2009) e49 e53 Original article IFNg and antibody responses among French nurses during a tuberculosis contact tracing investigation Réponse IFNg et anticorps parmi les personnels
Pathologie Biologie 57 (2009) e49 e53 Original article IFNg and antibody responses among French nurses during a tuberculosis contact tracing investigation Réponse IFNg et anticorps parmi les personnels
Risk for Tuberculosis in Swiss Hospitals. Content. Introduction. Dr. med. Alexander Turk Zürcher Höhenklinik Wald alexander.turk@zhw.
 Risk for Tuberculosis in Swiss Hospitals 17. Tuberkulose Symposium Münchenwiler Risk for Tuberculosis in Swiss Hospitals Dr. med. Alexander Turk Zürcher Höhenklinik Wald alexander.turk@zhw.ch 1 Content
Risk for Tuberculosis in Swiss Hospitals 17. Tuberkulose Symposium Münchenwiler Risk for Tuberculosis in Swiss Hospitals Dr. med. Alexander Turk Zürcher Höhenklinik Wald alexander.turk@zhw.ch 1 Content
Targeted Testing for Tuberculosis Infection
 Targeted Testing for Tuberculosis Infection CONTENTS Introduction... 3.2 Purpose... 3.2 Policy... 3.2 When to Conduct Targeted Testing... 3.3 Approaches to increasing targeted testing and treatment for
Targeted Testing for Tuberculosis Infection CONTENTS Introduction... 3.2 Purpose... 3.2 Policy... 3.2 When to Conduct Targeted Testing... 3.3 Approaches to increasing targeted testing and treatment for
Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado
 Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado Developed by the Colorado Medical Directors Association and The Colorado Department of Public Health and Environment Introduction:
Tuberculosis Surveillance and Screening for Long Term Care Facilities in Colorado Developed by the Colorado Medical Directors Association and The Colorado Department of Public Health and Environment Introduction:
Basic research methods. Basic research methods. Question: BRM.2. Question: BRM.1
 BRM.1 The proportion of individuals with a particular disease who die from that condition is called... BRM.2 This study design examines factors that may contribute to a condition by comparing subjects
BRM.1 The proportion of individuals with a particular disease who die from that condition is called... BRM.2 This study design examines factors that may contribute to a condition by comparing subjects
Assisted Living - TB Risk Assessment
 Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
Comparison of Quantiferon-TB Gold versus Tuberculin Skin Test for Tuberculosis Screening in Inflammatory Bowel Disease Patients
 Comparison of Quantiferon-TB Gold versus Tuberculin Skin Test for Tuberculosis Screening in Inflammatory Bowel Disease Patients Gianluca Andrisani, Alessandro Armuzzi, Alfredo Papa, Manuela Marzo, Carla
Comparison of Quantiferon-TB Gold versus Tuberculin Skin Test for Tuberculosis Screening in Inflammatory Bowel Disease Patients Gianluca Andrisani, Alessandro Armuzzi, Alfredo Papa, Manuela Marzo, Carla
Tuberculosis And Diabetes. Dr. hanan abuelrus Prof.of internal medicine Assiut University
 Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Summary. Request for Advice
 Summary Health Council of the Netherlands. Vaccination of young children against tuberculosis. The Hague: Health Council of the Netherlands, 2011; publication no. 2011/04 Even though the global prevalence
Summary Health Council of the Netherlands. Vaccination of young children against tuberculosis. The Hague: Health Council of the Netherlands, 2011; publication no. 2011/04 Even though the global prevalence
Use of Interferon Gamma Release Assays as Confirmatory Test for Tuberculin Skin Test-Positive Patients in the Canadian Armed Forces
 Use of Interferon Gamma Release Assays as Confirmatory Test for Tuberculin Skin Test-Positive Patients in the Canadian Armed Forces Milan Patel Surgeon General Report Surgeon General Health Research Program
Use of Interferon Gamma Release Assays as Confirmatory Test for Tuberculin Skin Test-Positive Patients in the Canadian Armed Forces Milan Patel Surgeon General Report Surgeon General Health Research Program
Opportunistic Infections Related to Immune Suppressant and Biologic Drug Therapy in IBD
 Opportunistic Infections Related to Immune Suppressant and Biologic Drug Therapy in IBD Raymond Cross, M.D., M.S., AGAF Associate Professor of Medicine Director of the Inflammatory Bowel Disease Program
Opportunistic Infections Related to Immune Suppressant and Biologic Drug Therapy in IBD Raymond Cross, M.D., M.S., AGAF Associate Professor of Medicine Director of the Inflammatory Bowel Disease Program
Canadian Tuberculosis Standards
 Canadian Tuberculosis Standards 7 th Edition Chapter 4: Diagnosis of Latent Tuberculosis Infection Canadian Tuberculosis Standards, 7 th Edition is available on Internet at the following address: www.phac-aspc.gc.ca
Canadian Tuberculosis Standards 7 th Edition Chapter 4: Diagnosis of Latent Tuberculosis Infection Canadian Tuberculosis Standards, 7 th Edition is available on Internet at the following address: www.phac-aspc.gc.ca
Policy Directive: compliance is mandatory
 Policy Directive: compliance is mandatory Policy for Control of Tuberculosis in South Australian Health Services Policy developed by: Public Health and Clinical Coordination Approved at Portfolio Executive
Policy Directive: compliance is mandatory Policy for Control of Tuberculosis in South Australian Health Services Policy developed by: Public Health and Clinical Coordination Approved at Portfolio Executive
Role of QuantiFERON-TB Gold In-Tube test in detection of latent tuberculosis infection in health care contacts in Alexandria, Egypt
 Vol. 8(12), pp. 1310-1317, 19 March, 2014 DOI: 10.5897/AJMR2013.6502 ISSN 1996-0808 Copyright 2014 Author(s) retain the copyright of this article http://www.academicjournals.org/ajmr African Journal of
Vol. 8(12), pp. 1310-1317, 19 March, 2014 DOI: 10.5897/AJMR2013.6502 ISSN 1996-0808 Copyright 2014 Author(s) retain the copyright of this article http://www.academicjournals.org/ajmr African Journal of
Tuberculosis in children in Europe -the ptbnet
 Tuberculosis in children in Europe -the ptbnet Beate Kampmann FRCPCH PhD A/Professor in Paediatric Infection & Immunity Consultant Paediatrician Imperial College London, UK and Institute of Infectious
Tuberculosis in children in Europe -the ptbnet Beate Kampmann FRCPCH PhD A/Professor in Paediatric Infection & Immunity Consultant Paediatrician Imperial College London, UK and Institute of Infectious
Table. Positive Purified Protein Derivative Results (Pediatrics In Review Apr 2008)
 PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
DIVISION of SUBSTANCE ABUSE SERVICES. Tuberculosis Control Guidelines for Alcohol and Drug Abuse Treatment Programs
 DIVISION of SUBSTANCE ABUSE SERVICES Tuberculosis Control Guidelines for Alcohol and Drug Abuse Treatment Programs 1. Purpose: This policy provides guidance and instruction to identify and prevent tuberculosis
DIVISION of SUBSTANCE ABUSE SERVICES Tuberculosis Control Guidelines for Alcohol and Drug Abuse Treatment Programs 1. Purpose: This policy provides guidance and instruction to identify and prevent tuberculosis
Guidelines for Using the QuantiFERON -TB G Test for Detecting Mycobacterium tuberculosi Infection, United States
 Page 1 of 10 Recommendations and Reports December 16, 2005 / 54(RR15);49-55 Guidelines for Using the QuantiFERON -TB G Test for Detecting Mycobacterium tuberculosi Infection, United States Please note:
Page 1 of 10 Recommendations and Reports December 16, 2005 / 54(RR15);49-55 Guidelines for Using the QuantiFERON -TB G Test for Detecting Mycobacterium tuberculosi Infection, United States Please note:
Comparison of the QuantiFERON -TB Gold assay and tuberculin skin test to detect latent tuberculosis infection among target groups in Trinidad & Tobago
 Investigación original / Original research Comparison of the QuantiFERON -TB Gold assay and tuberculin skin test to detect latent tuberculosis infection among target groups in Trinidad & Tobago Shirematee
Investigación original / Original research Comparison of the QuantiFERON -TB Gold assay and tuberculin skin test to detect latent tuberculosis infection among target groups in Trinidad & Tobago Shirematee
Self-Study Modules on Tuberculosis
 Self-Study Modules on Tuberculosis Epidemiology of Tuberculosis U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for HIV/AIDS, Viral Hepatitis, STD,
Self-Study Modules on Tuberculosis Epidemiology of Tuberculosis U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for HIV/AIDS, Viral Hepatitis, STD,
ATTACHMENT 2. New Jersey Department of Health Tuberculosis Program FREQUENTLY ASKED QUESTIONS
 ATTACHMENT 2 New Jersey Department of Health Tuberculosis Program FREQUENTLY ASKED QUESTIONS 1. QUESTION Is it required to submit the Annual Report of TB Testing in Schools Form (TB-57) to the New Jersey
ATTACHMENT 2 New Jersey Department of Health Tuberculosis Program FREQUENTLY ASKED QUESTIONS 1. QUESTION Is it required to submit the Annual Report of TB Testing in Schools Form (TB-57) to the New Jersey
Tube) in patients of Sarcoidosis from a population with high prevalence of tuberculosis infection
 Original article: laboratory research SARCOIDOSIS VASCULITIS AND DIFFUSE LUNG DISEASES 2011; 28; 95-101 Mattioli 1885 Interferon Gamma Release Assay (QuantiFERON-TB Gold in Tube) in patients of Sarcoidosis
Original article: laboratory research SARCOIDOSIS VASCULITIS AND DIFFUSE LUNG DISEASES 2011; 28; 95-101 Mattioli 1885 Interferon Gamma Release Assay (QuantiFERON-TB Gold in Tube) in patients of Sarcoidosis
April 22, 2015 Curry International Tuberculosis Center
 Tools for TB Elimination: Early Case Finding and Prevention Determining Your High-Risk Groups: Using the Universal Risk Assessment Tool Wednesday, d Sacramento, California Mike Carson, MS Program Manager
Tools for TB Elimination: Early Case Finding and Prevention Determining Your High-Risk Groups: Using the Universal Risk Assessment Tool Wednesday, d Sacramento, California Mike Carson, MS Program Manager
Tuberculosis infection in drug users: interferon-gamma release assay performance
 INT J TUBERC LUNG DIS 11(11):1183 1189 2007 The Union Tuberculosis infection in drug users: interferon-gamma release assay performance C. Z. Grimes,* L-Y. Hwang,* M. L. Williams,* C. M. Austin, E. A. Graviss
INT J TUBERC LUNG DIS 11(11):1183 1189 2007 The Union Tuberculosis infection in drug users: interferon-gamma release assay performance C. Z. Grimes,* L-Y. Hwang,* M. L. Williams,* C. M. Austin, E. A. Graviss
Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective October 2014
 Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective October 2014 Students must remain in compliance throughout enrollment within the program. Students who are not in compliance
Joint MSPAS/MPH Student Health and Immunization Clearance Requirements Effective October 2014 Students must remain in compliance throughout enrollment within the program. Students who are not in compliance
Tuberculosis 89 (2009) S1, S41 S45. Contents lists available at ScienceDirect. Tuberculosis
 Tuberculosis 89 (2009) S1, S41 S45 Contents lists available at ScienceDirect Tuberculosis journal homepage: http://intl.elsevierhealth.com/journals/tube Latent tuberculosis infections in hard-to-reach
Tuberculosis 89 (2009) S1, S41 S45 Contents lists available at ScienceDirect Tuberculosis journal homepage: http://intl.elsevierhealth.com/journals/tube Latent tuberculosis infections in hard-to-reach
Regulations for Tuberculosis Control in Minnesota Health Care Settings
 Regulations for Tuberculosis Control in Minnesota Health Care Settings A guide for implementing tuberculosis (TB) infection control regulations in your facility Tuberculosis Prevention and Control Program
Regulations for Tuberculosis Control in Minnesota Health Care Settings A guide for implementing tuberculosis (TB) infection control regulations in your facility Tuberculosis Prevention and Control Program
University of Bergen
 University of Bergen Comparison of Tuberculin Skin Test and QuantiFERON TB Gold In-tube Assay for the diagnosis of tuberculosis infection and disease in young children; study conducted as part of the development
University of Bergen Comparison of Tuberculin Skin Test and QuantiFERON TB Gold In-tube Assay for the diagnosis of tuberculosis infection and disease in young children; study conducted as part of the development
Alcohol abuse and smoking
 Alcohol abuse and smoking Important risk factors for TB? 18 th Swiss Symposium on tuberculosis Swiss Lung Association 26 Mach 2009 Knut Lönnroth Stop TB Department WHO, Geneva Full implementation of Global
Alcohol abuse and smoking Important risk factors for TB? 18 th Swiss Symposium on tuberculosis Swiss Lung Association 26 Mach 2009 Knut Lönnroth Stop TB Department WHO, Geneva Full implementation of Global
TUBERCULOSIS SCREENING GUIDELINES FOR CONNECTICUT SCHOOLS Connecticut Department of Public Health, Infectious Diseases Section June 2011
 TUBERCULOSIS SCREENING GUIDELINES FOR CONNECTICUT SCHOOLS Connecticut Department of Public Health, Infectious Diseases Section June 2011 These recommendations from the Connecticut Department of Public
TUBERCULOSIS SCREENING GUIDELINES FOR CONNECTICUT SCHOOLS Connecticut Department of Public Health, Infectious Diseases Section June 2011 These recommendations from the Connecticut Department of Public
Latent Tuberculosis Infection: A Guide for Primary Health Care Providers
 Latent Tuberculosis Infection: A Guide for Primary Health Care Providers A B Latent Tuberculosis Infection: A Guide for Primary Health Care Providers U.S. Department of Health and Human Services Centers
Latent Tuberculosis Infection: A Guide for Primary Health Care Providers A B Latent Tuberculosis Infection: A Guide for Primary Health Care Providers U.S. Department of Health and Human Services Centers
PEOSH Model Tuberculosis Infection Control Program
 PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
Chapter 1 Overview of Tuberculosis Epidemiology in the United States
 Chapter 1 Overview of Tuberculosis Epidemiology in the United States Table of Contents Chapter Objectives.... 1 Progress Toward TB Elimination in the United States.... 3 TB Disease Trends in the United
Chapter 1 Overview of Tuberculosis Epidemiology in the United States Table of Contents Chapter Objectives.... 1 Progress Toward TB Elimination in the United States.... 3 TB Disease Trends in the United
Originally published as:
 Originally published as: Reuss, A.M., Wiese-Posselt, M., Weißmann, B., Siedler, A., Zuschneid, I., An Der Heiden, M., Claus, H., Von Kries, R., Haas, W.H. Incidence rate of nontuberculous mycobacterial
Originally published as: Reuss, A.M., Wiese-Posselt, M., Weißmann, B., Siedler, A., Zuschneid, I., An Der Heiden, M., Claus, H., Von Kries, R., Haas, W.H. Incidence rate of nontuberculous mycobacterial
3. Blood and blood products such as serum, plasma, and other blood components.
 Mississippi Downloaded 01/2011 101.11 Infectious Medical Waste. The term "infectious medical waste" includes solid or liquid wastes which may contain pathogens with sufficient virulence and quantity such
Mississippi Downloaded 01/2011 101.11 Infectious Medical Waste. The term "infectious medical waste" includes solid or liquid wastes which may contain pathogens with sufficient virulence and quantity such
Maryland County Health Department Tuberculosis Infection Control Plan
 Maryland County Health Department Tuberculosis Infection Control Plan Introduction In 1998, the Division of TB Control developed a Tuberculosis (TB) Prevention Plan template for use by the local health
Maryland County Health Department Tuberculosis Infection Control Plan Introduction In 1998, the Division of TB Control developed a Tuberculosis (TB) Prevention Plan template for use by the local health
Guide to Biostatistics
 MedPage Tools Guide to Biostatistics Study Designs Here is a compilation of important epidemiologic and common biostatistical terms used in medical research. You can use it as a reference guide when reading
MedPage Tools Guide to Biostatistics Study Designs Here is a compilation of important epidemiologic and common biostatistical terms used in medical research. You can use it as a reference guide when reading
TB Intensive San Antonio, Texas November 11 14, 2014
 TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
Immunology Platform 2012
 Immunology Platform 2012 The scientific activity report of Immunology Platform of the Institut Pasteur du Cambodge for the period January 1st to December 31st, 2012. Scientific activity report Prepared
Immunology Platform 2012 The scientific activity report of Immunology Platform of the Institut Pasteur du Cambodge for the period January 1st to December 31st, 2012. Scientific activity report Prepared
