Clinical Practice Guidelines for the Prevention, Diagnosis and Management of Lung Cancer
|
|
|
- Roland Webster
- 10 years ago
- Views:
Transcription
1
2 Clinical Practice Guidelines for the Prevention, Diagnosis and Management of Lung Cancer APPROVED BY THE NHMRC ON 18 MARCH 2004
3 The Cancer Council Australia 2004 ISBN Print: Online: This work is copyright. Apart from any use as permitted under the Copyright Act 1968, no part may be reproduced by any process without prior written permission from The Cancer Council Australia. Requests and enquiries concerning reproduction and rights should be addressed to the Copyright Officer, The Cancer Council Australia, GPO Box 4708, Sydney NSW 2001, Australia. Website: [email protected] These guidelines were approved by the National Health and Medical Research Council at its 152nd Session on 18 March 2004, under section 14A of the National Health and Medical Research Council Act Approval for the guidelines by NHMRC is granted for a period not exceeding five years, at which date the approval expires. The NHMRC expects that all guidelines will be reviewed no less than once every five years. Readers should check with The Cancer Council Australia for any reviews or updates of these guidelines. Disclaimer This document is a general guide to appropriate practice, to be followed subject to the clinician s judgement and the patient s preference in each individual case. The guidelines are designed to provide information to assist decision-making and are based on the best evidence available at the time of compilation (September 2002). Conflict of interest The development of these clinical practice guidelines has been by a non-remunerated working party of the Australian Cancer Network with further support from The Cancer Council Australia, the Clinical Oncological Society of Australia and a grant in support from the Department of Health and Ageing to the National Cancer Control Initiative for editing and review services. Some members of the working party have received sponsorship to attend scientific meetings; been supported in the conducting of clinical trials; or been involved in an advisory capacity by pharmaceutical houses. These guidelines can be downloaded from the National Health and Medical Research Council website: Copies of the document can be ordered through the Australian Cancer Network on (02) or [email protected].
4 CONTENTS Foreword Executive Summary Summary of recommendations and guidelines vii xii xiii SECTION I: SETTING THE SCENE 1. Epidemiology Lung cancer in Australia Pathogenesis and classification Aetiology Survival 12 SECTION II: PREVENTION & DIAGNOSIS 2. Prevention and screening Smoking cessation Nutrition Chemoprevention Case finding Screening Initial assessment and prognostic factors Appropriate referral for suspected lung cancer Diagnosis of lung cancer Staging lung cancer Prognostic factors Follow-up 60 SECTION III: PATIENT SUPPORT & DEFINITIVE TREATMENT 4. Supporting the patient during diagnosis and treatment Information provision Prevalence of anxiety, depression and distress Quality of life Counselling, support and psychological treatments 74 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer iii
5 5. Non-small cell lung cancer Management of non-small cell lung cancer by stage Surgery Radiotherapy Chemotherapy and adjuvant or neo-adjuvant treatment of locoregional non-small cell lung cancer Chemotherapy in advanced/metastatic non-small cell lung cancer Small cell lung cancer Management of small cell lung cancer by stage Chemotherapy and small cell lung cancer Radiotherapy 125 SECTION IV: SYMPTOM CONTROL 7. Palliative care Palliative care for the person with lung cancer Special problems in supportive care and care of advanced lung cancer Palliative radiation Thoracic symptoms Superior vena cava obstruction (SVCO) Spinal cord compression Bone metastases Brain metastases Alternative and complementary therapies General Effectiveness, safety and cost Discussing alternative therapies 182 SECTION V: ECONOMIC CONSIDERATIONS 10. Cost effectiveness Economic burden of lung cancer in Australia Role of economic evidence in the development of guidelines 190 iv Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
6 APPENDICES Appendix 1 TNM Staging 213 Appendix 2 Modified staging for small cell lung cancer 222 Appendix 3 Performance status criteria of the Eastern Cooperative Oncology Group (ECOG) 224 Appendix 4 Systemic therapy for non-small cell lung cancer an afterword 225 Appendix 5 Asbestos and other environmental carcinogens 229 Appendix 6 National Tobacco Strategy Action Plan 252 Appendix 7 Levels of evidence for diagnostic tests 254 Appendix 8 A model for pathology reporting of lung cancer 255 Appendix 9 Membership of the Australian Cancer Network Management of Lung Cancer Guideline Working Party 258 Appendix 10 Submissions received following public consultation 260 Appendix 11 Guideline development process 266 Appendix 12 Contacts for help services 273 LIST OF ABBREVIATIONS 275 GLOSSARY 277 INDEX 282 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer v
7 TABLES Table 1 1 Incidence and mortality rates from lung cancer per 100,000 population, 1996, standardised to the world standard population 5 Table 2 1 Pooled estimates of relative risks of lung cancer in former smokers and current smokers compared to never smokers 7 Table 3 1 Effect of environmental tobacco smoke on non-smokers 8 Table 4 1 Age and smoking adjusted odds ratios (95% CI) for risk of lung cancer following previous lung disease in case-control studies 11 Table 5 1 Five-year survival from lung cancer international comparisons 12 Table 1 5 Management of non-small cell lung cancer stage by stage 83 Table 2 5 Survival for patients with Stage 1 and 2 non-small cell lung cancer 85 Table 3 5 Trials of surgery with or without preoperative chemotherapy in stage IIIA NSCLC 96 Table 4 5 Randomised trials of new agents versus supportive care 99 Table 5 5 Randomised trials of new agents plus cisplatin versus cisplatin 101 Table 6 5 Randomised trials of new agents 103 Table 1 6 Management of small cell lung cancer stage by stage 119 Table 1 7 Pain unrelated to the cancer or pain related to treatment 147 Table 1 10 Burden of disease attributable to lung cancer in Australia, Table 2 10 Summary of NRT cost effectiveness literature 194 Table 3 10 Summary of mass media and other anti-smoking campaigns cost-effectiveness literature 195 Table 4 10 Summary of screening cost effectiveness literature 198 Table 5 10 Results of studies investigating costs and outcomes of alternative chemotherapy regimens 202 Table 1 Non-asbestos occupational carcinogens for lung cancer Appendix FIGURES Figure 1 1 Figure 2 1 Trends in age-standardised incidence and mortality rates for cancer of the lung, Australia 3 Average annual incidence and mortality rates from lung cancer, Australia vi Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
8 FOREWORD In 1993, the National Health and Medical Research Council (NHMRC) established a working party to develop clinical practice guidelines for the management of early breast cancer. According to Professor Richard Smallwood, the then chair of the NHMRC, the objective of the guidelines is not only to assist practitioners to make decisions about appropriate health care for specific clinical circumstances, but also to assist consumers by providing them with comprehensive information about choices available in their treatment. The development of the guidelines was based on two key principles: it had to be a multidisciplinary process and the guidelines were to be based on the best available evidence. The early breast cancer guidelines were published in 1995 in two editions; one for the professional carers of women with breast cancer, and one for consumers. After endorsement by the NHMRC they were published in conjunction with the National Breast Cancer Centre. Following the success and wide acceptance of the early breast cancer guidelines, the newly established Australian Cancer Network proceeded with the development of guidelines for other common cancers. To assist in this process, the NHMRC has published A guide to the development, implementation and evaluation of clinical practice guidelines 1. To date clinical guidelines for melanoma, familial and colorectal cancer have been published and are widely used. At the time of writing, guidelines for the management of non-melanoma skin, prostate and epithelial ovarian cancer were under development, and it seemed logical that lung cancer, which is responsible for 22.8% of male and 14.8% of female cancer deaths in Australia 2, more than any other, should also be included in the program. That there was a need for management guidelines was evident from two recent Australian surveys of lung cancer management. The first of these, based on Victorian data from 1993, and published in 2000, revealed that 16% of patients with small cell lung cancer, and 21% with non-small cell lung cancer received no treatment at all 3. In the second survey of Australian respiratory physicians and oncologists conducted in 1996, a wide variety of treatment recommendations were made for a single hypothetical case scenario 4. For a patient with a T2N2M0 adenocarcinoma of the left main bronchus with a positive subcarinal node, there were similar levels of support for no fewer than six different treatment strategies. Such a variety of approaches to the same problem might be due to an absence of good evidence supporting any one approach, or it might be that busy practitioners do not have the time to carefully evaluate and weigh the existing evidence. It might be asked What difference are guidelines likely to make in a disease with an almost uniformly poor prognosis? Some sobering comparative international survival data suggest that differences in philosophy and management may be important. Recently reported five-year survival for lung cancer in the UK was only 6%, compared with 11% for New South Wales and 14% for US whites 5. While some of these differences Clinical practice guidelines for the prevention, diagnosis and management of lung cancer vii
9 may be due to the distribution of prognostic factors in the various patient populations, it is unlikely that there are major differences in the natural history of the disease from country to country, and it therefore seems probable that the management policies and practices were also contributory. Survival is not the only measure of success in patients with lung cancer. Symptom palliation and quality of life may be more important considerations for the majority of patients who have incurable disease. It is noteworthy that in the Victorian survey, good symptom control was achieved in only 55% of those patients treated with palliative intent 2. A Working Party to develop guidelines for the management of lung cancer was assembled with the assistance of Emeritus Professor Tom Reeve from the Australian Cancer Network, and met for the first time in Melbourne in April The members of the working party were selected because of their area of expertise, as well as ensuring wide geographic representation to reflect the national nature of the project. All medical members, who were drawn from the clinical interest groups involved in the prevention, diagnosis and treatment of lung cancer, had the endorsement of the college with which they are affiliated. In addition to the medical members, the working party also had nursing and consumer representatives. Using the NHMRC document 1 as their guide, the members formed smaller multidisciplinary groups to examine the best available evidence in order to make recommendations under the following headings: prevention and screening initial and pretreatment assessment supportive care non-small cell lung cancer (locoregional) non-small cell lung cancer (metastatic/ recurrent) small cell lung cancer. The Working Party decided that the management of pleural mesothelioma would not be part of its brief. The evidence would be researched and assigned to a level according the following scale: I II III.1 III.2 Evidence obtained from a systematic review of all relevant randomised controlled trials. Evidence obtained from at least one properly designed randomised controlled trial. Evidence obtained from well designed pseudo-randomised controlled trials (alternate allocation or some other method). Evidence obtained from comparative studies with concurrent controls and allocation not randomised [cohort studies], case-control studies, or interrupted time series with a control group. viii Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
10 III.3 IV Evidence obtained from comparative studies with historical control, two or more single arm studies or interrupted time series without a parallel control group. Evidence from case series, either post-test or pre-test and post-test. For diagnostic tests, for which randomised trials may not be appropriate, the scale of evidence used is that recommended by the Oxford Centre for Evidence Based Medicine 6. This scale has been included as Appendix 7. For some clinical scenarios, high-level evidence supporting one intervention over another may not be available; where this is the case, the guidelines say so, and make recommendations about the further research that is required. In considering the evidence, the Working Party has taken account of an intervention s effectiveness, rather than its cost. A preliminary set of guidelines, based on evidence obtained from searches of electronic databases and with the assistance of the Cochrane Collaboration, was presented to a workshop held in Brisbane in association with the Annual Scientific Meeting of the Thoracic Society of Australia and New Zealand in March The guidelines were then further refined after the Working Party s meeting in June 2001, and have undergone a significant editing process since that time. The process has been specifically designed so as not to exclude contributions from individuals or groups who have additional evidence that may have escaped the notice of the working party members. The draft guidelines were advertised for public review and 23 submissions were received. An executive committee under the chair of Professor Robert Burton reviewed the submissions and appropriate incorporation or modifications made in the guidelines where necessary. Each question raised has been considered. The submissions were collated in exemplary fashion by Dr Karen Pedersen of the National Cancer Control Initiative (NCCI). The intention is to make the best evidence widely available to inform the decisions of health care professionals and consumers; the guidelines are not prescriptive. We have tried to keep the document succinct so that it is easy to use in everyday practice. It is not intended to be a comprehensive textbook of lung cancer. For those who wish to examine the evidence in more detail, references have been provided alongside every guideline. During the review process, it was pointed out that some of the guidelines were based on studies which were unblinded to both the researcher and the reviewer, yet the evidence was classified as level I. The reality is that for many treatments in oncology, their method of administration and associated toxicities make double blind studies impractical. Further, the use of hard endpoints such as survival in many of the studies diminishes the risk of observer bias in interpreting the outcome. A number of the reviewers felt that it was not enough to state in the guideline boxes that there were differences between treatments, but asked if it was possible to include some standard measure of the magnitude of any differences, for example increase Clinical practice guidelines for the prevention, diagnosis and management of lung cancer ix
11 in median survival in months. However, the differences in outcome can be expressed in so many ways median, one-year, five-year survival; hazard ratios and per cent reduction in risk of death; palliation, toxicity and quality of life outcomes and so on that a standard method of quantifying differences was not thought appropriate. The chapters dealing with the treatment of lung cancer are subdivided into sections according to therapeutic modality, rather than disease stage. We recognise that in the modern era of multidisciplinary care, this method of presenting the evidence may limit its practical application. We have therefore included tables at the beginning of Chapters 5 and 6 in which the recommended management of lung cancer is set out by stage to reflect the clinical situations which confront the practicing clinician. Publication of the guidelines does not complete the process. Unless there is evidence of the implementation of the guidelines in practice, then the whole exercise will have achieved nothing. A meeting is to be held prior to the Annual Scientific Meeting of the Thoracic Society of Australia and New Zealand in April 2003 under the auspices of NCCI. This meeting should provide a powerful springboard for the dissemination and implementation. Once the guidelines have been disseminated, they will need to be piloted in hospitals and clinics to test their applicability and relevance. Next, they will need to be evaluated, in particular whether their implementation has had any effect on health outcomes. Finally, they will need to be revised within five years to ensure they reflect contemporary knowledge. The Working Party noted that the following topics should be considered as research priorities: 1. Screening of high-risk populations using new imaging technologies. 2. The role of surgery in locally advanced non-small cell lung cancer. 3. Strategies to reduce the incidence of brain metastases in non-small cell lung cancer. 4. Role of multidisciplinary care in lung cancer. 5. Role of clinical lung cancer nurse specialist. 6. Barriers to patient access to optimal care. 7. Improved palliation of dyspnoea. 8. Developing appropriate follow-up criteria and strategies. The Working Party hopes that health practitioners and consumers find the Guidelines for the prevention, diagnosis and management of lung cancer a useful resource in the management of this difficult disease. We welcome feedback on any aspect of this publication. Associate Professor David Ball Chair, ACN Management of Lung Cancer Guidelines Working Party x Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
12 References 1. National Health and Medical Research Council. A guide to the development, implementation and evaluation of clinical practice guidelines. Canberra, AGPS, Australian Institute of Health and Welfare. Australia s Health Canberra, AIHW, Richardson GE, Thursfield VJ, Giles GG. Reported management of lung cancer in Victoria in 1993: comparison with best practice. Med J Aust 2000; 172: Van Houtte P, Ball D, Danhier S, Scalliet P. Treatment indications and clinical target volume. In Progress and perspectives in the treatment of lung cancer Springer- Verlag, Berlin 1999; Supramaniam R, Smith D, Coates M, Armstrong B. Survival from cancer in New South Wales in 1980 to New South Wales Cancer Council, Oxford Centre for Evidence-Based Medicine. Levels of evidence and grades of recommendation At Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xi
13 EXECUTIVE SUMMARY Lung cancer causes a major burden to the health of Australians in terms of morbidity and mortality. The Guidelines for the prevention, diagnosis and management of lung cancer provide an evidence-based document produced by a multi-disciplinary working party to facilitate sound decision-making. The Guidelines are guidelines; they are not rules and are not prescriptive in any sense. Tobacco smoke and inhalation of environmental tobacco smoke, medical radiation in some specific subgroups and a history of previous lung disease are factors associated with an increased risk of lung cancer. Effective interventions through the medical profession, nursing and individual or group counselling can be helpful in assisting people not to start or to quit smoking. Personalised information is more effective than general information. Assessment of people with suspected pulmonary neoplasm is multi-factorial and should not rely on chest X-ray alone. Evaluation should aim to provide a defined diagnostic outcome and an appropriate therapeutic path. No defined pattern for screening for lung cancer has yet been established. Newer approaches eg. with or without spiral CT are being explored. Surgical resection of non-small cell lung cancer gives the best results of any form of treatment. Radiation and chemotherapy of patients with non-small cell lung cancer need to be carefully aligned to stage of disease and risks of surgery. Small cell lung cancer is rarely a surgical disease. Radiotherapy and chemotherapy both play significant roles in patient management and their application needs to be evaluated in relation to the patient s clinical status. Palliative care and psycho-oncology services provide significant assistance to clinicians, patients and their families. It is important that such assistance be sought in the management of patients with lung cancer. Palliative care may include a wide range of clinical services including surgery, radiotherapy, chemotherapy, physiotherapy, etc. The Guidelines have a valuable Appendix directing attention to asbestos and other environmental carcinogens. (Appendix 5) xii Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
14 SUMMARY OF RECOMMENDATIONS AND GUIDELINES Guideline Level of Evidence Refs Page SECTION II: PREVENTION AND DIAGNOSIS Chapter 2 Prevention and screening 19 Strategies to Help People Stop Smoking Effective interventions include advice from doctors, structured interventions from nurses, and individual/ group counselling. I 8,9, 10,11 25 Generic self-help materials are no better than brief advice, but more effective than doing nothing. Personalised materials are more effective than standard materials. All currently available forms of nicotine replacement therapy are effective. Bupropion and nortriptyline increase effectiveness as evidenced by quit rates. Personalised smoking cessation advice for inpatients together with at least one month of follow-up increases quit rates. I I I I I Strategies that do not help people stop smoking Acupuncture, hypnotherapy, aversion therapy, immunotherapy and exercise have not been shown to effectively increase quit rates. I 21,22 23,24 26 Chemoprevention Strategies in Lung Cancer Data do not support the use of currently reported chemoprevention strategies in lung cancer. II 86,87,88, 89,90,91, 92,93,94 31 Dietary Supplementation with Beta Carotene Diet supplemented with pharmacological doses of beta-carotene increases the risk of lung cancer in heavy smokers. II 82,83, 84,85 31 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xiii
15 Guideline Level of Evidence Refs Page Population Screening for Lung Cancer No forms of population screening for lung cancer, including regular chest radiography, with or without sputum cytology even in high-risk groups, have been shown to improve outcomes and screening is not recommended. I II 108,111, 113, , Helical CT Screening In view of the limited information available on outcome, helical CT screening for lung cancer is not recommended except in the context of a well-designed clinical trial. III 3 114,122, 124, Chapter 3 Initial assessment and prognostic factors 47 Clinical Management All individuals with suspected lung cancer should be referred to a specialist with expertise in the management of lung disease for an opinion. Sputum Cytology Sputum cytology is recommended to help establish a positive diagnosis of lung cancer in individuals with a central pulmonary mass. Bronchoscopy and FNA Fibreoptic bronchoscopy is a procedure that has a high diagnostic yield (accuracy) in lung cancer. In the diagnostic approach to suspected endobronchial lung tumours, bronchoscopy is usually the appropriate initial investigation for endobronchial evaluation and pathological confirmation. Fine needle aspiration is an appropriate initial investigative option for the pathological diagnosis of peripheral lung lesions in the absence of contraindications. IV 1 49 III (O) 16,17 51 III (O) 26,30 52 IV (O) IV (O) 19,20 52 xiv Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
16 Guideline Level of Evidence Refs Page PET Scanning in Diagnosis Pet scanning is accurate in differentiating benign from malignant pulmonary lesions. It is highly predictive for diagnosis of lung masses when a tissue diagnosis is not readily available. Staging Non-small Cell Lung Cancer Patients with mediastinal nodes larger than 1cm in transverse diameter on CT who otherwise have resectable lung disease should undergo further staging evaluation. PET Scanning in Staging Non-small Cell Lung Cancer PET has been found to be more accurate than CT in mediastinal nodal staging for non-small cell lung cancer. A negative PET is highly specific, but positive PET nodes are not always malignant and histological confirmation may be required before advancing to definitive management. M Staging of Non-small Cell Lung Cancer If clinical assessment for metastases is abnormal, then further investigations are indicated, as metastases will be confirmed in 50% of such cases. Routine bone scanning in non-small cell lung cancer is of little clinical value if there are no abnormal clinical or biochemical features. The role of routine brain imaging in non-small cell lung cancer asymptomatic patients is unclear, but the detection rate is low. PET is more accurate in overall M staging than conventional staging methods. I (O) 31,32,33 53 I (O) 51,54 54 I (O) 51,58,59 55 I (O) III (O) 64,70 56 III (O) 74,75 56 II (O) 76,77,78 57 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xv
17 Guideline Level of Evidence Refs Page Staging Small Cell Lung Cancer Once a metastatic site is identified, further anatomical staging at asymptomatic sites does not alter standard treatment or prediction of outcome but it does increase costs. Prognosis NSCLC TNM stage, performance status and weight loss are independent prognostic factors in patients with non-small cell lung cancer, and should be documented at diagnosis in all patients. Prognosis SCLC In patients with small cell lung cancer, stage (limited versus extensive) and performance status are essential prognostic factors, and should be documented at diagnosis in every case. Follow-up There is insufficient evidence to recommend any particular schedule of follow-up of patients after treatment for lung cancer. After the period of risk for treatment-related complications has elapsed, six monthly clinical assessments with a chest x-ray is reasonable. There is no evidence that higher levels of imaging (CT or PET), tumour markers or bronchoscopy in asymptomatic patients have any influence on outcome and their routine use in follow-up is not recommended. II IV IV IV SECTION III: PATIENT SUPPORT AND DEFINITIVE TREATMENT Chapter 4 Supporting the Patient During Diagnosis and Treatment Informing the Patient Patients should be provided with adequate information, as this is associated with enhanced patient psychological wellbeing. 69 III xvi Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
18 Guideline Level of Evidence Refs Page Clinicians should follow the NHMRC recommended guidelines on the breaking of bad news, providing information about treatments and the discussion of prognosis. Psychosocial Care in Lung Cancer It is critical to recognise distress, anxiety and depressive disorders in patients with lung cancer as treatment with combined pharmacotherapy (antidepressants) and psychotherapy is efficacious. IV 1 72 I 2,26,27 73 Quality of Life in Lung Cancer The potential impact of treatment on quality of life in patients with lung cancer should be included in discussions of treatment alternatives. II 18,30,31, 32,33,34 74 Psychosocial and Supportive Services in Quality of Life in Cancer Psychological interventions and early referral to psycho-oncology and palliative care services improves quality of life in patients with cancer. I II 2,26,27 38,39 75 Chapter 5 Non-Small Cell Lung Cancer (NSCLC) 81 Surgical Resection Surgical resection is recommended for early stage non-small cell lung cancer, as this gives the best results of any form of treatment. Lobectomy Lobectomy is preferred to limited resection in patients with operable T1 N0 NSCLC. Regional Lymph Node Assessment Regional lymph node assessment should be performed with all lung resections for NSCLC. Radical mediastinal lymph node dissection whilst more accurately staging the patient provides no significant survival advantage over appropriate mediastinal lymph node sampling. II 4 85 II II 19,20,22 87 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xvii
19 Guideline Level of Evidence Refs Page Radiotherapy In patients with inoperable NSCLC and who have no evidence of distant metastases, radiotherapy is recommended to locoregional disease because it may be associated with a survival advantage compared with placebo. Radiotherapy Dose In patients with locoregional inoperable NSCLC and with good performance status, higher doses of radiotherapy are associated with better response and possibly survival. Doses in the vicinity of 60Gy in six weeks are recommended because they are safe and give the highest response rates. Radiotherapy and Chemotherapy The combination of cisplatin-based chemotherapy and radical radiotherapy in patients with good performance status is associated with a small but significant survival advantage compared with radiotherapy alone in NSCLC. Timing of Radiotherapy and Cisplatin Therapy Concomitant cisplatin and radiotherapy are associated with a better survival than if the two treatments are given sequentially. When to Avoid Radiotherapy Postoperative radiotherapy in patients with completely resected Stage I or II NSCLC is not recommended because of its detrimental effect on survival. Adjuvant Therapy The administration of adjuvant platinum-based chemotherapy is not recommended following surgery because it has not been definitively shown to significantly improve survival. II II 28,31 89 I 35,36 90 II 42,43 91 I I xviii Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
20 Guideline Level of Evidence Refs Page Neo-adjuvant Therapy For Stage IIIA patients managed surgically, platinum-based combination chemotherapy should be given prior to surgery as it improves survival. Neo-adjuvant chemotherapy may be beneficial in earlier stage disease, but the evidence is currently insufficient to support routine use (see Table 3 5). II 51,52, 59,60 95 Chemotherapy Chemotherapy is appropriate treatment for patients with advanced NSCLC who have good performance status (ECOG 2) and are otherwise medically fit as it has been shown to improve survival. Chemotherapy can result in beneficial effects on symptoms and quality of life in patients with advanced NSCLC. Combination Chemotherapy Combination chemotherapy is preferable to single agent therapy in patients with advanced NSCLC. For patients where combination chemotherapy is contraindicated, single agent therapy with one of the new agents (either a taxane, gemcitabine or vinorelbine) is appropriate. I II 69, I II 83, Choice of Chemotherapy Agents At the present time, no one chemotherapy regimen can be recommended over another. Based on currently available trial results, various combinations of a platinum drug plus a new agent are reasonable options for performance status 0 or 1 patients. II 85,86, 87, The use of combinations of three or more drugs, and the use of non-platinum combinations require further investigation before incorporation into standard practice. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xix
21 Guideline Level of Evidence Refs Page Carboplatin can be used instead of cisplatin in combination chemotherapy. II 92,93, Chemotherapy Doses and Cycles There is no indication to use greater than standard doses or dose intensity of chemotherapy in advanced NSCLC. II 85,102, 103, Continuing multi-agent platinum-based chemotherapy beyond three to four cycles does not provide additional survival benefit. Patients receiving chemotherapy for advanced NSCLC should be evaluated for effectiveness of treatment after two to three cycles. Treatment should be discontinued if no benefit is seen. Second Line Chemotherapy In selected good performance status patients, second-line chemotherapy with docetaxel may be considered. II 105, IV II 108, Chapter 6 Small Cell Lung Cancer 117 Platinum as Optimal Chemotherapy Platinum containing regimens produce superior survival to that seen with other regimens. For patients with limited disease, when used in conjunction with thoracic irradiation, there is no evidence that any combination is superior to the doublet of cisplatin and etoposide. I 6,7 123 I 12, Cycles of Chemotherapy Four to six cycles of chemotherapy should be given. II 2, 21, 22, First and Second Line Chemotherapy Where a platinum agent and etoposide have been given first line, then appropriate second-line regimens include the combination of cyclophosphamide, adriamycin and vincristine, or single agent topotecan. These regimens are of similar efficacy. II xx Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
22 Guideline Level of Evidence Refs Page If first line chemotherapy has produced a response which has gone beyond eight months duration, it is reasonable to trial the first line drug again. Chemotherapy and Radiotherapy In patients with limited stage small cell lung cancer, the addition of thoracic radiotherapy to standard combination chemotherapy improves overall survival and should be incorporated into a comprehensive treatment plan. III I 35,36, Thoracic radiotherapy should be offered early in relation to the course of chemotherapy rather than late. Evidence supports the administration of chemotherapy concurrent with radiotherapy over sequential chemotherapy-radiotherapy administration. II 2,38,39, 40,41, 42, Accelerated radiotherapy is associated with a survival advantage compared with standard fractionation. Prophylactic Cranial Irradiation For patients who have achieved a complete response after induction therapy, prophylactic cranial irradiation is associated with a reduction in rate of brain metastases and prolongation of survival. II I SECTION IV: SYMPTOM CONTROL Chapter 7 Palliative Care 135 Specialist Palliative Care Services Specialist palliative care services should be used to improve outcomes in the care of patients with cancer (lung cancer included). I Management of Dyspnoea Counselling, breathing retraining, relaxation, and teaching coping and adaptive strategies can improve dyspnoea and functional capacity in lung cancer patients. II IV Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xxi
23 Guideline Level of Evidence Refs Page Other non-pharmacological measures to be considered for dyspnoea include acupuncture as a complementary procedure. IV 34, A therapeutic trial of morphine and/or benzodiazepines is recommended for dyspnoea in patients with advanced cancer. II IV Nebulized morphine can improve dyspnoea in some terminally ill lung cancer patients. A supervised therapeutic trial may be worthwhile. III 3 IV 53 57, Nebulized lignocaine has not proven to be better than nebulized saline in relief of breathlessness. Cough Suppression Oral opioids are recommended for suppression of non-productive cough in lung cancer. Inhaled sodium cromoglycate could be tried in cough from non-small cell lung cancer that is resistant to standard therapy. Nebulised lignocaine can be useful as a cough suppressant - special precautions need to be taken (see text). Pain Management Unrelieved or poorly controlled pain leads to increased anxiety about the future and general anxiety that interferes with daily living. Management of moderate to severe cancer pain should include the appropriate introduction and dose titration of opioids. Neuropathic Pain Management Extrapolation from therapeutic approaches to neuropathic pain in other diseases indicates that antidepressants and anti-convulsants offer effective palliation. IV II 66, II IV IV IV 73, I xxii Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
24 Guideline Level of Evidence Refs Page Bowel Care The best laxative for terminally ill patients using opioids is yet to be determined. Senna and lactulose have shown equal efficacy. Management of Pleural Effusion Pleural effusion is best managed by talc insufflation following thoracoscopic exploration and complete drainage of fluid. Management of Pericardial Effusion Pericardiocentesis can be safely performed under echocardiographic control. The outcome is effective. III IV IV Chapter 8 Palliative Radiation 161 Radiotherapy in Palliation of Cancer Radiotherapy is an effective modality for the management of certain symptoms caused by uncontrolled intrathoracic disease, and short courses of radiotherapy are as effective as more fractionated regimens. There appears to be improved survival in patients with a good performance status receiving higher doses of palliative radiotherapy, compared to single or two fraction courses. External beam radiotherapy appears to provide better palliation compared to endobronchial brachytherapy, but brachytherapy might be of benefit in patients with endobronchial obstructing lesions. Superior Vena Cava Obstruction in Cancer A histological diagnosis is desirable before treatment of superior vena cava obstruction. Chemotherapy on its own is effective in superior vena cava obstruction due to small cell lung cancer. II 1,2,3 164 II 4,5,8 164 II 7,8 164 IV II 10, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xxiii
25 Guideline Level of Evidence Refs Page Management of Metastatic Spinal Cord Compression Dexamethasone should be started on suspicion of spinal cord compression and whilst awaiting assessment. II III If spinal cord compression is suspected, whether on symptomatic or clinical grounds the investigation of choice is MRI scan. Surgery followed by radiotherapy is the treatment of choice for spinal cord compression. When surgery is not considered appropriate, radiotherapy should be started immediately. Radiotherapy is considered as effective as surgery in achieving symptomatic relief. Radiotherapy in Management of Skeletal Metastases Palliative radiotherapy remains the most effective single modality for the treatment of local metastatic bone pain. III 3 13, II III 3 12,18, IV In the treatment of skeletal metastases trials have shown that 8Gy single fraction is as efficacious for pain relief as other schedules. II 22,24,25, 26,27, In patients who have widespread bony lesions consideration can be given to single fraction hemi-body radiation palliation. Bisphosphonates in Management of Bone Metastases Bisphosphonates improve pain in people with symptomatic bone metastases from lung cancer. III I 33,34, Irradiation and Radiotherapy for Skeletal Metastases Radiotherapy is effective palliation for brain metastases from lung cancer. II 39,46, 47, Resection of solitary cerebral metastases followed by radiotherapy potentially results in increased local control and a longer disease-free survival than radiotherapy alone. III 2 III 3 40, xxiv Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
26 Guideline Level of Evidence Refs Page Stereotactic radiosurgery may be a suitable alternative to resection. III 3 43, Doses of whole brain radiotherapy ranging from 10Gy in a single fraction to 40Gy in 20 fractions have similar effectiveness in symptom palliation and times to disease progression. Shorter courses, for example 20Gy in five fractions, are recommended because of patient convenience. II 39,48, 49, Re-irradiation for progressive brain metastases may be considered in selected patients without progressive disease at other sites. Chapter 9 Alternative and complementary therapies Educational and Psychosocial Care in Cancer Educational and psychosocial care has been found to benefit adults with cancer in relation to anxiety, depression, mood, nausea, vomiting, pain and knowledge. Aromatherapy and Anxiety in Radiotherapy Aromatherapy has not been shown to reduce anxiety in patients with cancer undergoing radiotherapy. IV I II Clinical practice guidelines for the prevention, diagnosis and management of lung cancer xxv
27 SECTION I SETTING THE SCENE 1. EPIDEMIOLOGY 1.1 Lung cancer in Australia 1.2 Pathogenesis and classification 1.3 Aetiology Tobacco smoke Trends in smoking Environmental tobacco smoke Cannabis use and lung cancer Medical radiation Indoor radon Cooking fuels Previous lung disease Genetic susceptibility Asbestos and other environmental carcinogens 1.4 Survival Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 1
28 1.1 LUNG CANCER IN AUSTRALIA Lung cancer is a serious health problem in Australia. It was the fifth most common cancer reported to Australian cancer registries in 1998, but the leading cause of death from cancer, responsible for 20.1% of cancer deaths 1,2. In the year 2000, lung cancer accounted for 22.8% of male and 14.8% of female cancer deaths and 5.3% of all deaths in Australia 3. There were new cases of lung cancer in Australia during 1998 and deaths. About one in 28 Australians are likely to develop lung cancer during their lifetime and for those who died during 1998, there were an estimated life-years lost as a result of premature death before reaching 75 years of age 1. Over the period , the incidence of lung cancer in males fell to 58 cases per population whereas the incidence in females rose to 23 cases per population. The mortality rate in males declined to 53 cases per in 1998 but remained relatively stable in females at 19 cases per population as shown in Figure Prior to the mid-1980s the rates had been increasing in males for more than 50 years 4,5. Figure 1 1 Trends in age-standardised incidence and mortality rates for cancer of the lung, Australia 1 New cases and deaths per 100,000 population Incidence males Mortality males Incidence females Mortality females Incidence males Mortality males Incidence females Mortality females 80Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 3
29 The incidence and mortality rates increase with advancing age in both males and females. In 1998, the incidence rate peaked in the year age group and the mortality rate peaked in the year age group in both males and females in Australia 1. An important element of the current epidemiology of lung cancer in Australia 80 is its migration to an older cohort. The fraction of new lung cancers that were seen above age years increased from 39% in 1985 to more than 49% Incidence in males This increase was from 60 40% to 50% in men and 37% to 48% in women. This becomes relevant as age and comorbidity affects the feasibility of some treatment options Lung cancer incidence and mortality vary between the states and territories (Figure 2 1). 40 Both incidence and mortality age-standardised rates are markedly lower in males in the Australian 30 Capital Territory (ACT) and higher in the Northern Incidence Territory. females The rates in females 20 are also notably higher in the Northern Territory. However, it should be noted that the numbers of cases in the Northern Territory and ACT are Mortality far lower femalesthan in the 10 states, due to the relatively smaller populations in the territories 1. 0 Mortality males The Australian 1984 lung cancer 1986 incidence 1988 and 1990mortality 1992 rates 1994 are lower 1996 than rates 1998 in North America and Europe (Table 1 1). The Australian rates given in Table 1 1 are different to those above, because they have been standardised to the world standard population rather than the Australian population for purposes of comparison. Figure 2 1 Average annual incidence and mortality rates from lung cancer, Australia Age-standardised incidence/mortality rate per population Incidence males Mortality males Incidence females Mortality females NSW VIC QLD WA SA TAS ACT NT 4 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
30 Table 1 1 Incidence and mortality rates from lung cancer per population, 1996, standardised to the world standard population 7,8,9 Incidence rate Mortality rate Males Females Males Females Australia United States United Kingdom European Union PATHOGENESIS AND CLASSIFICATION Lung cancer appears to arise in the bronchi in response to repetitive carcinogenic stimuli, inflammation and irritation. Disruption of cell development occurs in the mucosal lining and progresses to elevate or erode the basal membrane. The tumour then spreads throughout the lung and will eventually metastasise to the lymph nodes and other parts of the body 10. There are four main histologic classifications of lung cancer. These are squamous cell carcinomas, adenocarcinomas, small cell carcinomas and large cell carcinoma. Because the behaviour and management of squamous cell carcinoma, adenocarcinoma and large cell carcinomas are very similar, they are often grouped together as non-small cell lung cancer (NSCLC) in contrast to small cell lung cancer (SCLC), which has a distinct natural history and management. Squamous cell carcinoma is most commonly found in men and shows the strongest relationship with smoking. This tumour arises in the larger and more central bronchi and tends to spread locally. It metastasises later than other types, but grows rapidly at its site of origin. Adenocarcinoma was previously known as the most common type of lung cancer in women and non-smokers, however, the incidence of adenocarcinoma has increased in the last two decades and it is now the most common histological subtype in both males and females. The reason for the increasing incidence of adenocarcinoma is not well understood, but may be related to changing patterns of smoking. Adenocarcinomas tend to be peripherally located, smaller and vary histologically from well-differentiated tumours to solid masses with occasional mucin-producing glands and cells. Small cell carcinomas are highly malignant and have a distinctive cell type. They may be round and oval (oat cells) or have spindle-shaped or polygonal cells, and are probably derived from neuroendocrine cells of the epithelial lining of the bronchi. They have a Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 5
31 strong relationship to cigarette smoking and are the most aggressive of all lung tumours, metastasising widely and virtually incurable by surgical means. Large cell carcinomas are likely to be undifferentiated squamous cell and adenocarcinoma. They usually consist of large polygonal cells with vesicular nuclei 10, AETIOLOGY TOBACCO SMOKE Smoking is the largest single cause of lung cancer, responsible for 90% of lung cancers in males and 65% of lung cancers in females in Australia, and continues to rise 12. Certain industrial exposures and atmospheric pollutants, including environmental tobacco smoke, also increase an individual s risk of lung cancer (refer to Appendix 5, p 229). The first case-control studies supporting a link between smoking and lung cancer incidence were published in the 1950s. Since that time, further evidence has accumulated to show the relationship of lung cancer incidence to the timing, duration, intensity and other characteristics of smoking. Three of the largest cohort studies on current male smokers were those by Hammond, Doll et al and McLaughlin et al 13,14,15. These all found increased lung cancer death rates with increasing amounts smoked, such that those smoking 10 or more cigarettes per day had a relative risk of lung cancer of approximately 10. Similar results were found in females 16,17. Doll and Peto found that not only did the excess risk of lung cancer rise in proportion to the square of the number of cigarettes smoked per day, but to the fourth or fifth power of the duration of smoking 18. This effect has been replicated in other studies 19,20. Cigar and pipe smoking are also associated with increased risk of lung cancer, although the extent of the risk varies between studies. A relative risk of seven was found in the British Physicians Study compared with Swedish cohort studies, which found similar risks to those in cigarette smokers 14,21. The relative risk of lung cancer declines with increased time since quitting, eventually approaching that of non-smokers 13,14,15. The results of a 1995 meta-analysis 22 of nine cohort studies and seven case-control studies on the effects of the relationship between cigarette smoking and lung cancer are shown in Table 2 1. This meta-analysis excluded studies published prior to 1980 and studies for which the majority of cases were diagnosed before 1975 in order to be representative of present day risk, as smoking habits and composition of cigarettes have changed substantially over time. Studies were also excluded if they did not separate the effects of former smoking from current smoking or never smoking, or there was no adjustment for age or control groups having smoking-related diseases. 6 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
32 Table 2 1 Pooled estimates of relative risks of lung cancer in former smokers and current smokers compared to never smokers 22 Sex Former smokers Current smokers (cigarettes per day) Any Male Female TRENDS IN SMOKING Future trends in lung cancer incidence can be predicted from past trends in smoking because lung cancer due to smoking usually takes 20 years or more to develop. The smoking prevalence of adult Australians has declined from around 72% of males in 1945 to 26% in The percentage of females smoking rose from 26% in 1945 to 33% in 1976, and subsequently dropped to 21% in ,24. While there were significant declines in the prevalence of smoking among adults and secondary school students in the latter part of the twentieth century, the rate of decline has slowed since the 1990s. From these trends we would predict that the incidence of lung cancer in males will continue to fall and that the incidence of lung cancer in females will reach a peak before There is a marked variation in smoking prevalence among population subgroups. The National Aboriginal and Torres Strait Islander Survey of 1994 found that among Indigenous Australians, 54% of males and 46% of females aged over 13 years reported that they smoked 25. The National Mental Health Survey found that 41.8% of Australians with a diagnosable mental health condition were current smokers 26. Furthermore, smoking prevalence has been shown to decrease with increased education and occupation status 27. ENVIRONMENTAL TOBACCO SMOKE Analysis of 39 published epidemiological studies of the risk of lung cancer in non-smokers who did and did not live with a smoker found an excess risk of lung cancer of 24% in female non-smokers who lived with a smoker 28. The meta-analysis included five cohort and 34 case-control studies and covered cases of lung cancer. The dose-response relationship showed that the risk of lung cancer in the non-smoker increased by 23% for every 10 cigarettes smoked per day by the smoker and by 11% for every 10 years of exposure (Table 3 1). Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 7
33 Table 3 1 Effect of environmental tobacco smoke on non-smokers 28 Excess risk Relative risk (95%CI) Risk of lung cancer in female non-smokers 24% 1.24 living with a smoker ( ) Risk of lung cancer for every 10 cigarettes smoked 23% 1.23 per day by cohabitant ( ) Risk of lung cancer for every 10 years 11% 1.11 of exposure resulting from living with a smoker ( ) The risk of lung cancer in non-smokers was also estimated by extrapolating from the risk in smokers, using urine or saliva concentrations of cotinine and nicotine 28. Cotinine and nicotine are tobacco specific and their concentrations in non-smokers exposed to environmental tobacco smoke are about 1% of those in smokers. Non-smokers exposed to environmental tobacco smoke therefore experience 1% of the excess risk of lung cancer seen in smokers. The relative risk of lung cancer in smokers compared to nonsmokers was approximated to be 20 13,14,15, thus giving an excess risk of 19. Therefore, the excess risk of lung cancer in non-smokers exposed to environmental tobacco smoke compared with smokers was 0.19, that is 1% of 19. CANNABIS USE AND LUNG CANCER Cannabis is smoked in the same way as tobacco in many countries including Australia. Cannabis (marijuana) smoke contains many of the same carcinogens as tobacco smoke, with some differences in the levels of certain chemicals. It appears to be mutagenic in microbial assays and carcinogenic in some animal tests 29. Cannabis use has been linked to the finding of molecular and morphological changes in bronchial epithelium, some of which can be found in at-risk or pre-neoplastic lesions of the airway 30. There are data linking cannabis use to aerodigestive cancers in the form of case reports. Otherwise, a large cohort study of nearly people failed to show an overall excess of cancer comparing cannabis users and non-users at study entry (RR 0.9, 95% CI ) 31. However, the potential limitations of the study included the relatively young age at follow-up compared to the usual age range of lung cancer sufferers, a small number of heavy or long term users, and technical ascertainment issues. In contrast, a smaller case-control study reported that marijuana use was associated with an increased risk of head and neck cancer after adjusting for potential confounders including cigarette smoking 32. Further studies are thus needed to more definitively assess the carcinogenic risk of cannabis smoke. Meanwhile, it is worth informing regular cannabis smokers, particularly those who also smoke tobacco, that they may have a higher risk of lung cancers based on current knowledge of the properties of cannabis and tobacco smoke. 8 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
34 MEDICAL RADIATION The risk of lung cancer may be elevated as a result of medical exposure to radiation. A study of the effect of medical radiation on lifetime non-smokers found no elevated risk in males who had received radiotherapy, but an increased risk of 4.4 in females. This risk became non-significant when adjusted for history of reproductive cancer 33, although recent evidence suggests greater risks for medical radiation in smokers who have had breast cancer 34. INDOOR RADON SEE APPENDIX 5 COOKING FUELS SEE APPENDIX 5 PREVIOUS LUNG DISEASE The risk of lung cancer in people who have pre-existing lung disease has been studied using case-control studies. Lung diseases studied include asthma, chronic bronchitis, emphysema, pneumonia, pleurisy and tuberculosis. The results of some of these studies are outlined in Table 4 1. They provide evidence for increased risk of lung cancer following bronchitis and emphysema and possibly asthma and tuberculosis. However, most of the studies have been carried out in females and may not be generalisable to males. Nevertheless, early studies provided some evidence for increased risk of lung cancer mortality following asthma in males but not females 35,36. Despite adjustment for smoking, differing odds ratios have been observed between smokers and non-smokers. The effect of diet, environmental tobacco smoke, time between diagnosis of lung disease and lung cancer, and the lung cancer cell type also need to be more fully examined. For example, in the study of Mayne et al 37, the results were no longer supportive when further adjustment for dietary variables was added to the model. Furthermore, in the study of Wu et al 38, none of the odds ratios were significant when the model was adjusted for all previous lung disease, age, area, ethnicity and education. GENETIC SUSCEPTIBILITY Some genotypes are thought to be associated with an increased risk of lung cancer 11. It is hoped that further developments in molecular biology and epidemiology will greatly extend our knowledge in this respect. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 9
35 ASBESTOS AND OTHER ENVIRONMENTAL CARCINOGENS Several reviews published between 1991 and 2000 have supported the cumulative exposure model for lung cancer risk as a consequence of asbestos exposure 39,40,41,42,43, 44,45,46, with no clearly delineated threshold 40 and with no requirement for asbestosis or diffuse pleural fibrosis as a prerequisite for attribution of lung cancer to asbestos 47. Criteria for compensation of asbestos-related lung cancer and approaches to apportionment of the relative contributions of asbestos and cigarette smoke to lung cancer induction are discussed elsewhere 39,46,47,48,49,50,51,52,53. A detailed review of Asbestos and other environmental carcinogens can be found in Appendix Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
36 Table 4-1 Age and smoking adjusted odds ratios (95% CI) for risk of lung cancer following previous lung disease in case-control studies Reference Odds ratio Disease adjustment Asthma Bronchitis Emphysema Pneumonia Pleurisy Tuberculosis Brownson et al, Age, smoking ( ) ( ) ( ) ( ) ( ) ( ) Mayne et al, Age, smoking ( ) ( ) ( ) Alavanja et al, Age, smoking ( ) ( ) ( ) ( ) ( ) ( ) Wu et al, Age, area, ethnicity, education ( ) ( ) ( ) ( ) ( ) ( ) Samet et al, Age, sex, ethnicity, smoking ( ) ( ) ( ) Wu et al, Age, smoking ( ) ( ) ( ) ( ) ( ) ( ) Wu-Williams Age, education, et al, smoking, study area ( ) ( ) Hinds et al, Age, smoking, ethnic group ( ) No adjustment for smoking as study on non-smokers only, defined as persons who had smoked fewer than 100 cigarettes and had not used any other form of tobacco for more than six months Study involved adenocarcinoma only Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 11
37 1.4 SURVIVAL Relative survival following a diagnosis of lung cancer, in the Australian states for which data were available, varied in the ranges of % in males and % in females at five years during the 1980s and 1990s 60,61,62. Recent Australian data for the period show a five-year relative survival for males of 11% and for females of 14% 63. These are compared with international figures in Table 5 1. When comparing survival and mortality data it should be noted that the denominator for survival is the population of patients with disease, whereas the denominator for the mortality rate from lung cancer is the whole population. Thus, the mortality rate may be low if there are a small number of cases with the disease, whereas poor survival results from patients with the disease dying relatively quickly. Table 5 1 Five-year survival from lung cancer international comparisons 9,59,60,61,62,64,65 Years after diagnosis Males Time Age 1 yr 2 yr 3 yr 4 yr 5 yr period group Australia All New South Wales South Australia All Queensland Western Australia Europe United States (SEER) 1991 All Females Time Age 1 yr 2 yr 3 yr 4 yr 5 yr period group Australia All New South Wales South Australia All Queensland Western Australia Europe United States (SEER) 1991 All Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
38 Survival decreases with increasing age and extent of the disease. Data from New South Wales show five-year relative survival from localised lung cancer to be 23.2% compared with 1.0% of cases where the disease had spread to distant organs 61. Survival from SCLC is lower than that from NSCLC and it also varies by histological subtype, being higher from adenocarcinoma and squamous cell carcinoma than large cell (undifferentiated) carcinoma 66. Data from the South Australian hospital-based cancer registries showed five-year survival in to be 5% from SCLC, 20% from adenocarcinoma, 18% from squamous cell carcinoma and 8% from large cell carcinoma 64. Trends in survival from lung cancer since the 1980s have remained fairly poor, despite the improvement in survival from SCLC, which has occurred largely as a result of the introduction of chemotherapy in the 1970s 66. References 1. Cancer in Australia Vol Canberra, Australian Institute of Health and Welfare, Australasian Association of Cancer Registries. 2. Causes of Death Australia Canberra, Australian Bureau of Statistics. 3. Australia s Health Cat no. AUS Canberra, Australian Institute of Health & Welfare. 4. Giles G., Hill D, Silver B. The Lung Cancer Epidemic in Australia, Australian Journal of Public Health 1991; 15: Holman C, Hatton W, Armstrong B, English D. Cancer mortality trends in Australia Perth, Health Department of Western Australia. 6. Morgan LC, Grayson D, Peters HE, Clarke CW, Peters MJ. Lung Cancer in New South Wales: Current Trends and the Influence of Age and Sex. Med J Aust 2000; 19;172(12): Ferlay J, Bray F, Sankila R, Parkin D. EUCAN: Cancer incidence, mortality and prevalence in the European Union 1996, version IARC. IARC CancerBase No. 4 ed. 8. Cancer in Australia Incidence and mortality data for 1996 and selected data for 1997 and Canberra, Australian Institute of Health and Welfare/ Australasian Association of Cancer. 9. Ries L, Kosary C, Hankey B, Miller B, Clegg L, Edwards B. SEER Cancer Statistics Review Bethesda, MD, National Cancer Institute. 10. Kobzik L. The Lung. Cotran R, Kumar V, Collins T (eds) Robbins Pathologic Basis of Disease (6th edn). Philadelphia: WB Saunders Company, Blot W, Fraumeni J. Cancers of the lung and pleura. Schottenfeld D, Fraumeni J (eds) Cancer Epidemiology and Prevention (2nd edn). Oxford: Oxford University Press, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 13
39 12. Ridolfo B, Stevenson C. The quantification of drug-caused morbidity and mortality in Australia, AIHW Cat No. PHE Canberra, Australian Institute of Health and Welfare. Drug Statistic Series no Hammond EC. Smoking in Relation to the Death Rates of One Million Men and Women. Natl Cancer Inst Monogr 1966; 19: Doll R, Peto R, Wheatley K, Gray R, Sutherland I. Mortality in Relation to Smoking: 40 Years Observations on Male British Doctors. BMJ 1994; 309(6959): McLaughlin JK, Hrubec Z, Blot WJ, Fraumeni JFJ. Smoking and Cancer Mortality Among U.S. Veterans: a 26-Year Follow-Up. Int J Cancer 1995; 60(2): Doll R, Gray R, Hafner B, Peto R. Mortality in Relation to Smoking: 22 Years Observations on Female British Doctors. Br Med J 1980; 280(6219): Garfinkel L, Stellman SD. Smoking and Lung Cancer in Women: Findings in a Prospective Study. Cancer Res 1988; 48(23): Doll R, Peto R. Cigarette Smoking and Bronchial Carcinoma: Dose and Time Relationships Among Regular Smokers and Lifelong Non-Smokers. J Epidemiol Community Health 1978; 32(4): Gao YT, Blot WJ, Zheng W, Fraumeni JF, Hsu CW. Lung Cancer and Smoking in Shanghai. Int J Epidemiol 1988; 17(2): Lubin JH, Blot WJ, Berrino F, Flamant R, Gillis CR, Kunze M, Schmahl D, Visco G. Patterns of Lung Cancer Risk According to Type of Cigarette Smoked. Int J Cancer 1984; 33(5): Carstensen JM, Pershagen G, Eklund G. Mortality in Relation to Cigarette and Pipe Smoking: 16 Years Observation of 25,000 Swedish Men. J Epidemiol Community Health 1987; 41(2): English D, Holman C, Milne E, et al. The quantification of drug caused morbidity and mortality in Australia Canberra, Commonwealth Department of Human Services and Health. 23. Tobacco in Australia, Facts and Issues (2nd edn). Carlton South, VIC: Victorian smoking and health program (QUIT Victoria), National Drug Strategy Household Survey: First results. AIHW Cat No. PHE Canberra, Australian Institute of Health and Welfare. Drug Statistics Series no National Aboriginal and Torres Strait Islander Survey 1994: Health of indigenious Australians Canberra, Australian Bureau of Statistics. 26. Mental health and well-being: profile of adults Western Australia Canberra, Australian Bureau of Statistics. 27. Hill DJ, White VM, Scollo MM. Smoking Behaviours of Australian Adults in 1995: Trends and Concerns. Med J Aust 1998; 168(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
40 28. Hackshaw AK, Law MR, Wald NJ. The Accumulated Evidence on Lung Cancer and Environmental Tobacco Smoke. BMJ 1997; 315(7114): Hall W, MacPhee D. Cannabis Use and Cancer. Addiction 2002; 97(3): Tashkin DP, Baldwin GC, Sarafian T, Dubinett S, Roth MD. Respiratory and Immunologic Consequences of Marijuana Smoking. J Clin Pharmacol 2002; 42(11 Suppl): 71S 81S. 31. Sidney S, Beck JE, Tekawa IS, Quesenberry CP, Friedman GD. Marijuana Use and Mortality. Am J Public Health 1997; 87(4): Zhang ZF, Morgenstern H, Spitz MR, Tashkin DP, Yu GP, Marshall JR, Hsu TC, Schantz SP. Marijuana Use and Increased Risk of Squamous Cell Carcinoma of the Head and Neck. Cancer Epidemiol Biomarkers Prev 1999; 8(12): Kabat GC. Recent Developments in the Epidemiology of Lung Cancer. Semin Surg Oncol 1993; 9(2): Neugut AI, Murray T, Santos J, Amols H, Hayes MK, Flannery JT, Robinson E. Increased Risk of Lung Cancer After Breast Cancer Radiation Therapy in Cigarette Smokers. Cancer 1994; 73(6): Robinette CD, Fraumeni JFJ. Asthma and Subsequent Mortality in World War II Veterans. J Chronic Dis 1978; 31(9 10): Reynolds P, Kaplan GA. Asthma and Cancer. Am J Epidemiol 1987; 125(3): Mayne ST, Buenconsejo J, Janerich DT. Previous Lung Disease and Risk of Lung Cancer Among Men and Women Nonsmokers. Am J Epidemiol 1999; 149(1): Wu AH, Fontham ET, Reynolds P, Greenberg RS, Buffler P, Liff J, Boyd P, Henderson BE, Correa P. Previous Lung Disease and Risk of Lung Cancer Among Lifetime Nonsmoking Women in the United States. Am J Epidemiol 1995; 141(11): Henderson DW, de Klerk NH, Hammar S, et al. Asbestos and lung cancer: is it attributable to asbestosis, or to asbestos fiber burden? Corrin B (ed) Pathology of Lung Tumors. New York: Churchill Livingstone, 1997: Hodgson JT, Darnton A. The Quantitative Risks of Mesothelioma and Lung Cancer in Relation to Asbestos Exposure. Ann Occup Hyg 2000; 44(8): Asbestos Research (HEI-AR). Asbestos in public commercial buildings: a literature review and synthesis of current knowledge Cambridge, Massachusetts, Health Effects Institute. 42. Henderson DW, Roggli VL, Shilkin KB, et al. Is asbestosis an obligate precursor for asbestos-induced lung cancer? Peters GA, Peters BJ (eds). Sourcebook on Asbestos Diseases, vol 11. Charlottesville: Michie Company, 1995; Egilman D, Reinert A. Lung Cancer and Asbestos Exposure: Asbestosis Is Not Necessary. Am J Ind Med 1996; 30(4): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 15
41 44. Case BW, Dufresne A. Asbestos, Asbestosis, and Lung Cancer: Observations in Quebec Chrysotile Workers. Environ Health Perspect 1997; 105 Suppl 5: Billings CG, Howard P. Asbestos Exposure, Lung Cancer and Asbestosis. Monaldi Arch Chest Dis 2000; 55(2): Henderson DW, Leigh J. Asbestos and lung cancer: a selective up-date to the Helsiniki Criteria for individual attribution. 36, Helsinki, Finnish Institute for Occupational Health. People and Work Research Reports, vol Consensus report: asbestos, asbestosis and cancer: the Helsinki criteria for diagnosis and attribution. 23, Helsinki, Scand J Work Environ Health. 48. Chase GR, Kotin P, Crump K, Mitchell RS. Evaluation for Compensation of Asbestos- Exposed Individuals. II. Apportionment of Risk for Lung Cancer and Mesothelioma. J Occup Med 1985; 27(3): Report on Occupational Diseases Fibre Years 1/ Sankt Augustin, Schriftenreihe des Hauptverbandes der gewerblichen Berufsgenossenschaften. 50. Leigh J, Berry GdKNH, Henderson DW. Asbestos-related lung cancer: apportionment of causation and damages to asbestos and tobacco smoke. Peters GA, Peters BJ (eds) Sourcebook on Asbestos Diseases, vol 13. Charlottesville: Michie Company, 1996: Baur X, Czuppon AB. Regulation and compensation of asbestos diseases in Germany. Peters GA, Peters BJ (eds) Sourcebook on Asbestos Diseases (1997 edn). Vol. 15. Charlottesville: Lexis, 2002: Hindry M. Asbestos-related disease compensation in France. Peters GA, Peters BJ (eds) Sourcebook on Asbestos Diseases (1997 edn). Vol. 16. Charlottesville: Lexis, 1997: Thimpont J, De Vuyst P. Occupational asbestos-related diseases in Belgium (epidemiological data and compensation criteria). Peters GA, Peters BJ (eds) Sourcebook on Asbestos Diseases, vol 17. Charlottesville: Lexis, 1998: Brownson RC, Alavanja MC. Previous Lung Disease and Lung Cancer Risk Among Women (United States). Cancer Causes Control 2000; 11(9): Alavanja MC, Brownson RC, Boice JDJ, Hock E. Preexisting Lung Disease and Lung Cancer Among Nonsmoking Women. Am J Epidemiol 1992; 136(6): Samet JM, Skipper BJ, Humble CG, Pathak DR. Lung cancer risk and vitamin A consumption in New Mexico. 131(2), American Review of Respiratory Disease Wu AH, Yu MC, Thomas DC, Pike MC, Henderson BE. Personal and Family History of Lung Disease As Risk Factors for Adenocarcinoma of the Lung. Cancer Res 1988; 48(24 Pt 1): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
42 58. Wu-Williams AH, Dai XD, Blot W, Xu ZY, Sun XW, Xiao HP, Stone BJ, Yu SF, Feng YP, Ershow AG. Lung Cancer Among Women in North-East China. Br J Cancer 1990; 62(6): Ward-Hinds M, Cohen H, Kolonel L. Tuberculosis and lung cancer risk in nonsmoking women. 125, American Review of Respiratory Disease. 60. Baade P, Coory M, Ring I. Cancer survival in Queensland 1982 to Brisbane, Health Information Centre, Queensland Health. 61. Supramaniam R, Smith D, Coates M, Armstrong B. Survival from cancer in New South Wales in 1980 to Sydney, New South Wales Cancer Council. 62. Threlfall T, Brameld K. Cancer survival in Western Australia residents, Perth, Health Department of Western Australia. 63. Cancer survival in Australia Vol Canberra, Australian Institute of Health and Welfare; Australasian Association of Cancer Registries. 64. SARC: Epidemiology of cancer in South Australia Adelaide, South Australian Cancer Registry. 65. Berrino F, Capocaccia R, Esteve J, et al. Survival of cancer patients in Europe: the Eurocare-2 study Lyon, IARC. 66. Janssen-Heijnen ML, Coebergh JW. Trends in Incidence and Prognosis of the Histological Subtypes of Lung Cancer in North America, Australia, New Zealand and Europe. Lung Cancer 2001; 31(2 3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 17
43 SECTION II PREVENTION AND DIAGNOSIS 2. PREVENTION AND SCREENING 2.1 Smoking cessation Interventions from doctors and nurses Behavioural and psychological interventions Self help Pharmacological interventions Nicotine replacement therapy Antidepressants and anxiolytics Other pharmacological therapies Other therapies Hospital admissions Conclusions 2.2 Nutrition 2.3 Chemoprevention Chemoprevention for lung cancer Chemoprevention for multiple cancers Reversal of premalignancy Prevention of second primary lung cancers Conclusion 2.4 Case finding 2.5 Screening Introduction Chest radiography Sputum cytology Low-dose helical computed tomography Biomarkers and fluorescence bronchoscopy Other methods for early lung cancer detection Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 19
44
45 2.1 SMOKING CESSATION Smoking is the largest single preventable cause of death and disease including lung cancer. Consequently, tobacco control measures, including taxation and price policy, advertising restrictions, public information, health promotion and smoking cessation support, are pivotal in reducing the burden of disease from smoking. The Ministerial Council on Drug Strategy endorsed an action plan under the National Drug Strategic Framework, the National Tobacco Strategy (NTS) 1999 to , in June This is reproduced in Appendix 6. Guidelines for smoking cessation have recently been published in Britain consisting of guidelines for clinicians, health administrators and managers in a complete version 1 in conjunction with a cost-effectiveness guidance 2 as well as a shortened version 3. These were based on systematic reviews by the Cochrane Tobacco Addiction Review Group and the US Agency for Health Care Policy and Research (AHCPR 4. Similarly, the US Public Health Service Report Treating tobacco use and dependence: a clinical practice guideline 5 has been published recently and summarised in a consensus statement 6. These were produced by a panel charged with identifying effective, experimentally validated tobacco dependence treatments and practices and highlight differences from the original AHCPR 1996 Smoking cessation clinical practice guideline. Overall the essential features of smoking cessation advice can be summarised as the five A s: Ask (about smoking at every opportunity) Advise (all smokers to stop) advice re cannabis see Chapter 1, section 1.3 Assess (willingness to quit) Assist (the smoker to stop) Arrange (follow-up). Further guideline details including effective counselling and behavioural techniques, pharmacotherapy, enhancing motivation to quit, brief strategies for preventing relapse, and intensive smoking cessation intervention components, are published in the aforementioned references. In addition, there are specific guidelines in relation to hospital patients, pregnant smokers, young people, low income smokers, sex, weight gain, training for health professionals, telephone help line workers and health administrators. The Royal Australian and New Zealand College of Obstetricians and Gynaecologists has published a statement regarding women and smoking, including information on smoking and pregnancy (see under College Statements). In addition, about 20 systematic reviews on smoking cessation are available in the Cochrane Library analysing randomised controlled trials of smoking cessation with at least six months follow-up. The Cochrane Library has recently reviewed the findings on the effectiveness of available interventions 7, which are briefly summarised below. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 21
46 INTERVENTIONS FROM DOCTORS AND NURSES Data on smoking cessation advice from a medical practitioner has been collected from 34 trials, including over smokers. In some trials, subjects were at risk of specified diseases (smoking related chest disease, diabetes, ischaemic heart disease), but most were from unselected (convenience sampling) populations. The most common setting for delivery of advice was primary care, but others included hospital wards and outpatient clinics, and industrial clinics 8. Pooled data from 16 trials of brief advice versus no advice (or usual care) revealed a small but significant increase in the odds of quitting (OR 1.69, CI ). Direct comparison of intensive versus minimal advice showed a small advantage of intensive advice (OR 1.44, CI ). The only study of the effect of smoking advice on mortality found no statistically significant differences in death rates at 20 years follow-up. The reviewers concluded that simple advice has a small effect on cessation rates. Nurses are also effective. A Cochrane review of 16 studies comparing nursing delivered smoking cessation interventions to a control or usual care, found intervention to significantly increase the odds of quitting (OR 1.50, CI ). There was, however, heterogeneity between the study results, but pooling using a random effects model did not alter the estimate of effect. The authors concluded that the results indicate that smoking cessation advice and counselling given by nurses to their patients is supported by evidence that these interventions can be effective 9. BEHAVIOURAL AND PSYCHOLOGICAL INTERVENTIONS Both individual counselling and group therapy increase the chances of quitting 10,11. Fifteen studies in an updated Cochrane review on individual behavioural counselling for smoking cessation compared individual counselling to a minimal intervention. Four studies compared different types or intensities of counselling. It was concluded that individual counselling was more effective than control. The odds ratio (the ratio of part to the remainder: it is used to express the chance that a particular outcome will occur) (OR) for successful smoking cessation was 1.62 (CI ). The authors failed to detect a greater effect of intensive counselling compared to brief counselling (OR 0.98, CI ) 11. Group therapy offers individuals the opportunity to learn behavioural techniques for smoking cessation and to provide each other with mutual support. The Cochrane review suggested that there was reasonable evidence that groups are better than self help and other less intensive interventions, however, they may be no better than advice from a health care provider 10. There is not enough evidence on their effectiveness compared to intensive individual counselling. From the point of view of the consumer, who is motivated to make a quit attempt, it is probably worth joining a group if one is available, as it will increase the likelihood of quitting. Group therapy may also be valuable as part of a comprehensive intervention that includes nicotine replacement therapy (NRT), which is frequently used as a component of smoking cessation strategies and includes 22 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
47 nicotine gum, transdermal patch, nicotine nasal spray, nicotine inhaler and nicotine sublingual tablets/lozenges, designed to replace the nicotine that can be obtained from tobacco smoking. Twenty-four mainly small trials studied aversion therapy consisting of pairing the pleasurable stimulus of smoking to an unpleasant stimulus. A Cochrane review concluded that the existing studies do not provide sufficient evidence to determine either the efficacy of rapid smoking, where subjects are encouraged to smoke at an increased rate (see Glossary), or whether there is a dose-response to aversive stimulation. Milder versions of aversive smoking seem to lack efficacy 12. Two studies of silver acetate, which causes an unpleasant taste when combined with cigarettes, showed no evidence of benefit, although confidence intervals were wide (OR 1.05, CI ) 13. Any effect of this agent is therefore likely to be smaller than NRT. SELF HELP Self-help materials include written leaflets, manuals, audiotapes, videos, and computer programs that may be given as an adjunct to brief advice or without any personal contact. A Cochrane review studied 51 randomised trials of smoking cessation with follow-up of a minimum of six months, where at least one arm tested a self-help intervention (structured programming for smokers trying to quit without intensive contact with a therapist) 14. Thirty-two trials compared self-help materials to no intervention or tested materials used in addition to advice. In 11 trials in which self help was compared to no intervention there was a pooled effect that just reached statistical significance (OR 1.24, CI ). Four further trials failed to find evidence of benefit for either adding self-help materials to face-to-face advice, or to NRT. There was evidence from 14 trials using materials tailored for the characteristics of individual smokers that such personalised materials were more effective than standard manuals (10 trials, OR 1.36, CI ) or no materials (three trials, OR 1.80, CI ). A small number of trials failed to detect benefit from using additional materials or targeted materials. Thus, standard self-help materials may increase quit rates compared to no intervention, but the effect is likely to be small. Telephone services can provide information and support for smokers. Counselling may be provided proactively or offered reactively to smokers who call smoking cessation help-lines. A recent Cochrane review of randomised or quasi-randomised controlled trials in which proactive or reactive telephone counselling to assist smoking cessation was offered to smokers or recent quitters, found that proactive telephone counselling can be effective compared to an intervention without personal contact 15, although the size of effect is uncertain. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 23
48 PHARMACOLOGICAL INTERVENTIONS NICOTINE REPLACEMENT THERAPY Nicotine replacement is available as chewing gum, transdermal patch, nasal spray, inhaler, sublingual tablet and lozenge. A Cochrane review identified 108 trials: 94 with a non-nrt control group. The odds ratio for abstinence with NRT compared to control was 1.73 (CI ) 16. The odds ratios for the different forms of NRT were 1.66 for gum, 1.76 for patches, 2.27 for nasal spray, 2.08 for inhaled nicotine and 1.73 for nicotine sublingual tablet. These odds were largely independent of the duration of therapy, the intensity of additional support provided or the setting in which the NRT was offered. In highly dependent smokers there was a significant benefit of 4mg gum compared with 2mg gum (OR 2.67, CI ). There was weak evidence that combinations of forms of NRT are more effective. Higher doses of nicotine patch may produce small increases in quit rates. Only one study directly compared NRT to another pharmacotherapy, in which bupropion was significantly more effective than nicotine patch or placebo. The conclusion was that all of the commercially available forms of NRT (nicotine gum, transdermal patch, nicotine nasal spray, nicotine inhaler and nicotine sublingual tablets) are effective as part of a strategy to promote smoking cessation. They increase quit rates approximately 1.5 to two-fold regardless of setting. The effectiveness of NRT appears to be largely independent of the intensity of additional support provided to the smoker. Provision of more intense levels of support, although beneficial in facilitating the likelihood of quitting, is not essential to the success of NRT. ANTIDEPRESSANTS AND ANXIOLYTICS Although anxiolytics have not yet been shown to be effective, there is evidence that some antidepressants can help quitting. A Cochrane review 17 considered randomised trials comparing antidepressant drugs to placebo or an alternative therapeutic control for smoking cessation. There was one trial each of moclobemide, sertraline and venlafaxine, two of fluoxetine and nortriptyline, and five trials of bupropion, one of which tested long-term use to prevent relapse. Nortriptyline and bupropion both increased cessation. In one trial the combination of bupropion and nicotine patch produced slightly higher quit rates than patch alone. Consequently, some antidepressants (nortriptyline and bupropion) can aid smoking cessation. For bupropion, pooled results of four trials with 12-month abstinence rates and three with six-month rates gave an estimated odds ratio of 2.54 (CI ). It is not clear whether these effects are specific for bupropion, or would occur with any antidepressant. 24 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
49 OTHER PHARMACOLOGICAL THERAPIES The antihypertensive clonidine shares some pharmacological effects with bupropion and tricyclic antidepressants. A Cochrane review of six trials showed evidence of efficacy (OR 1.89, CI ), but there were potential sources of bias, and its usefulness is limited by the side effects of sedation and postural hypotension 18. The nicotine antagonist mecamylamine has been investigated as a cessation aid in combination with nicotine replacement. Two small studies show that mecamylamine, started before cessation and continued afterwards, may help smoking cessation, and that a combination of mecamylamine and nicotine replacement, started before cessation, may increase cessation rates achieved with nicotine replacement alone 20. However, the reviewers concluded that the results require confirmation in larger studies before the treatment can be recommended clinically. Lobeline is a partial nicotine agonist derived from the leaves of an Indian tobacco plant and has been used in proprietary smoking remedies. A Cochrane review found no trials with six months of follow-up 21. Guidelines Strategies to Help People Stop Smoking Effective interventions include advice from doctors, structured interventions from nurses, and individual/ group counselling. Level of Evidence I Refs 8,9, 10,11 Generic self-help materials are no better than brief advice, but more effective than doing nothing. Personalised materials are more effective than standard materials. All currently available forms of nicotine replacement therapy are effective. Bupropion and nortriptyline increase effectiveness as evidenced by quit rates. Personalised smoking cessation advice for inpatients together with at least one month of follow-up increases quit rates. I 14 I 14 I 16 I 17 I 24 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 25
50 OTHER THERAPIES A Cochrane review of 22 studies concluded that acupuncture was not superior to sham acupuncture in smoking cessation at any time point 22. The odds ratio for early outcomes was 1.22 (CI ); the odds ratio after six months was 1.50 (CI ) and after 12 months was 1.08 (CI ). Similarly, when acupuncture was compared with other anti-smoking interventions, there were no differences in outcome at any time point. Acupuncture appeared to be superior to no intervention in the early results, but this difference was not sustained. The results with different acupuncture techniques do not show any one particular method (i.e. auricular acupuncture or non-auricular acupuncture) to be superior to control intervention. Another Cochrane review considered nine studies of hypnotherapy compared with 14 different control interventions 23. There was significant heterogeneity between the results of the individual studies, with conflicting results for the effectiveness of hypnotherapy compared to no treatment or to advice. There was no evidence for an effect of hypnotherapy compared to rapid smoking or psychological treatment. The reviewers concluded we have not shown that hypnotherapy has a greater effect on six month quit rates than other interventions or no treatment. Existing evidence does not show a clear benefit for exercise in smoking cessation 24. The meta-analysis studied eight trials, six of which had fewer than 25 people in each treatment arm. Only one of the eight trials offered evidence for exercise aiding smoking cessation, all but one of the other trials were too small to exclude reliably an effect of intervention. Trials are needed with larger sample sizes, equal contact control conditions, tailored and lifestyle exercise programs and measures of exercise adherence. Guideline Strategies that do not help people stop smoking Acupuncture, hypnotherapy, aversion therapy, immunotherapy and exercise have not been shown to effectively increase quit rates. Level of Evidence I Refs 21,22, 23,24 HOSPITAL ADMISSIONS An admission to hospital provides an opportunity to help people stop smoking. A Cochrane review found that intensive intervention (inpatient contact plus follow-up for at least one month) was associated with a significantly higher quit rate compared to control (OR 1.82, CI ). There was no strong evidence that clinical diagnosis affected the likelihood of quitting Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
51 CONCLUSIONS Many factors including societal attitudes, legislation and public health measures influence tobacco use. Many smokers can give up without clinical intervention. Nonetheless, it is clear that effective strategies are available and should be offered to all smokers who express a desire to quit. Effective interventions include advice from doctors, structured interventions from nurses and individual/group counselling, and include: Motivational interviewing 5 Concise, brief non-judgemental advice Arrange follow-up 6 Enlist support 5 Pharmacotherapy 16 Refer to QUIT line Flagging smoking status on case notes of all attending patients 5 Targeted to stage of change 11 Use the five A s NUTRITION Accurate measurement of the relationship between lung cancer and diet presents a number of difficulties. These include methodological problems in measurement of nutrient intake, which ideally should be measured at different points in time prior to the development of cancer. The history of smoking and exposure to environmental tobacco smoke is also required, but is often lacking in sufficient detail. As a result, studies have not always produced consistent results. Ziegler et al undertook a comprehensive review of the literature on nutrition and lung cancer, which was completed in The following section outlines their conclusions. Recent studies have generally shown that lung cancer risk is reduced at high levels of vegetable and/or fruit consumption, or at high levels of intake of carotenoids or vitamin C, which are markers of vegetable and fruit intake The specific mechanisms of this relationship have not yet been elucidated, although a large number of compounds found in edible plants have been shown to inhibit experimental mutagenesis and carcinogenesis in animals 50,51. Some micronutrients, such as the provitamin A carotenoids, vitamin C, vitamin E and selenium may inhibit carcinogenesis by functioning as antioxidants 52,53. However, while observational and biochemical studies indicated a protective effect for beta-carotene (a provitamin A carotenoid) 28,29,30,54,55,56,57,58 and led to the intervention trials described in section 2.3, evidence for a protective effect of vitamin C, vitamin E and selenium has been less conclusive 27,28,30,31,32,34,35,36,37,41,43,45,47,56,59,60,61,62,63,64,65,66. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 27
52 Study populations are generally divided into quintiles or quartiles according to their vegetable and/or fruit intake and the risk of lung cancer is compared across these groups. The smoking-adjusted relative risk (RR) of lung cancer in the highest quartile compared to the lowest quartile tends to be in the order of ,68,69,70. In some studies, the relationship between fruit and vegetable consumption and lung cancer has varied according to sex, race, smoking history and histologic subtype 26,32,38,43, 71,72. While these observations may be genuine, it is possible that they are attributable to small numbers in specific subgroups, methods of analysis or chance. Dietary fat has been identified as a tumour promoter in experimental animals and this has led to studies of its relationship with lung cancer 73. Some studies have provided support for this hypothesis but there have been a number of inconsistencies, particularly regarding the size of the association. The relevant component(s) of dietary fat (cholesterol, total and saturated fat) have also not been identified 25. Since 1995, further studies on the relationship between nutrition and lung cancer have been completed, but have not altered the conclusions reached above 72,74,75,76,77. With regard to carotenoids, recent research by Michaud et al found that alpha-carotene and lycopene were significantly associated with a lower risk of lung cancer, rather than beta-carotene, lutein and beta-cryptoxanthin 78. Further studies will be required to confirm this conclusion. Therefore, while evidence still points to the conclusion that increased vegetable and fruit intake decreases risk of lung cancer, the specific mechanism(s) by which this occurs and the specific nutrients involved have yet to be determined. 2.3 CHEMOPREVENTION Chemoprevention can be defined as the use of specific natural or synthetic agents to prevent, suppress or reverse carcinogenesis before the development of invasive malignancy. A fundamental tenet upon which its use is based, is the field cancerisation hypothesis in upper aerodigestive tract malignancy, which predicts that diffuse epithelial injury occurs as the result of inhaled carcinogens. Clinical evidence for field carcinogenesis comes from observing premalignant lesions and multiple primary tumours 79 and is reinforced by molecular studies 80, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
53 CHEMOPREVENTION FOR LUNG CANCER Two large randomised primary chemoprevention trials in lung cancer have studied individuals at increased risk for the development of lung cancer as the result of smoking or asbestos exposure. The Alpha-Tocopherol Beta Carotene (ATBC) trial randomised Finnish male smokers, aged years, in a 2 x 2 factorial design of alpha-tocopherol (50mg/day) and beta-carotene (20mg/day) to (1) beta-carotene alone, (2) alpha-tocopherol alone, (3) beta-carotene plus alpha-tocopherol, or (4) placebo. After dietary supplementation for five to eight years, those given beta-carotene (alone or with alpha-tocopherol) had a higher incidence of lung cancer (RR 1.18, CI ) and higher total mortality (RR 1.08, CI ). This effect appeared to be associated with heavier smoking and alcohol intake 82,83. Supplementation with alpha-tocopherol produced no overall effect on lung cancer (RR 0.99, CI ). The US Beta-Carotene and Retinol Efficacy Trial (CARET) randomised smokers, former smokers, and asbestos-exposed workers to beta-carotene (30mg/day) plus retinyl palmitate (25 000IU/day) or placebo. The trial was terminated early as it also found a harmful effect of beta-carotene over that of placebo: increased lung cancer (primary endpoint) incidence (RR 1.28, CI ) and total mortality (RR 1.17; CI ). The possibility of excess lung cancer incidence being associated with higher alcohol intake was considered 84,85. The two studies thus suggest that pharmacological doses of beta-carotene may increase lung cancer risk in relatively heavy smokers, that is, individuals at high risk for developing lung cancer. Lung cancer risks were not increased in subsets of moderate-intensity smokers (less than one pack per day) in the ATBC study, or in former smokers in the CARET study. Importantly however, those with higher pre-intervention serum or intake levels of beta-carotene had a lower lung cancer risk, supporting the premise that dietary vegetables and fruit may prevent the development of lung cancer. CHEMOPREVENTION FOR MULTIPLE CANCERS The randomised, double-blind, placebo-controlled Physicians Health Study of male physicians aged years studied the effects of beta-carotene and aspirin in cancer and cardiovascular disease. In this trial, 12 years of supplementation with beta-carotene (50mg on alternate days) had no effect on overall risk of cancer or of lung cancer among current (11% of study population) or former (39% of study population) smokers 86. In the Women s Health Study, female health professionals aged 45-years and over were randomised to aspirin, vitamin E and beta-carotene in a double blind, placebo-controlled design. The beta-carotene (50mg on alternate days) component was terminated early, but there was no evidence of benefit or harm on cancer risk including lung cancer after a limited treatment duration (median 2.1 years) at a median follow-up of 4.1 years 87. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 29
54 REVERSAL OF PREMALIGNANCY Morphological changes in the bronchial epithelium, for example metaplasia and dysplasia, have been used as endpoints in some chemoprevention studies. An early uncontrolled trial found that six months of etretinate (25mg/day) was effective in reversing squamous metaplasia in biopsy specimens from heavy smokers 88. However, a randomised chemoprevention trial found that isotretinoin (1mg/kg/day) was no better than placebo at reversing squamous metaplasia in bronchoscopic biopsies 89. Similarly, a randomised trial of etretinate (25 mg/day) was no different from placebo in reducing sputum atypia after six months treatment in 138 smoking subjects 90. A placebo-controlled randomised lung cancer chemoprevention trial of beta-carotene (50mg/day) plus retinol (25 000IU every other day) in approximately 750 US male asbestos workers also found no difference in the primary endpoint of prevalence of sputum atypia after a median intervention period of 58 months 91. These studies suggest that retinoids have minimal or no effect on metaplasia, a process which may vary spontaneously and with smoking cessation. Some have proposed that retinoids may be active in later stages of preneoplastic lung carcinogenesis but this remains to be tested. PREVENTION OF SECOND PRIMARY LUNG CANCERS The lifetime risk of second primary tumours (SPTs) following early stage lung cancer may be as high as 20 30%. These observations have provided the impetus to study chemoprevention for second primary lung cancer. Initial favourable results came from a small randomised study of high-dose retinyl palmitate ( IU/day), given in an adjuvant phase III trial following resection of Stage I NSCLC 92. Although there was no statistically significant improvement in disease-free survival for the retinyl palmitate group, there was an improvement in terms of time-to-new-primary cancers in the field of prevention (lung, head and neck, bladder). On the other hand, the European multicentre (EUROSCAN) study of participants, consisting of a 2 x 2 factorial design to study the efficacy of retinyl palmitate ( IU daily for one year followed by IU for the second year) and 600mg daily of the antioxidant N-acetyl-cysteine (following head and neck or lung cancer), found no benefit in terms of survival, event-free survival or SPTs for these patients, most of whom were former or current smokers 93. The recent randomised, double-blind, placebo-controlled trial of low-dose isotretinoin (30 mg/day) in preventing second primary tumours following Stage I NSCLC concluded that isotretinoin treatment did not improve the overall rates of SPTs, recurrences, or mortality 94. Secondary multivariate and subset analyses suggested that isotretinoin was harmful in current smokers and beneficial in never smokers. 30 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
55 CONCLUSION Chemoprevention strategies to date have been disappointing for the primary prevention of lung cancer. There is an increased risk of lung cancer from pharmacological doses of beta-carotene in heavy smokers. For the prevention of second lung cancers, despite an initial promising study, a larger study failed to show any benefit for retinyl palmitate and/or N-acetyl cysteine. There are several currently ongoing studies of newer chemopreventative strategies which may provide additional information in the future 95,96,97. Guideline Chemoprevention Strategies in Lung Cancer Data do not support the use of currently reported chemoprevention strategies in lung cancer. Level of Evidence II Refs 86,87,88, 89,90,91,92, 93,94 Guideline Dietary Supplementation with Beta Carotene Diet supplemented with pharmacological doses of beta-carotene increases the risk of lung cancer in heavy smokers. Level of Evidence II Refs 82,83, 84, CASE FINDING Some experts distinguish between mass screening and case finding 98. Case finding has been defined as the examination or testing of a particular person who seeks clinical evaluation out of concern about a disease or defect or because of symptoms 99. Some clinicians recommend case finding on an individual basis particularly for very highrisk individuals such as smokers with additional risk factors (airway obstruction or a history of asbestos exposure) 99. At present there is insufficient evidence to support this approach. However, if and when the issue of screening arises in the context of a consultation, it would be reasonable for medical practitioners to exercise their clinical judgement and make decisions about the role of screening on a case by case basis. Any patient offered screening in this context should be fully informed about the potential risks and benefits. Patients should be given information about the risk of false negative and false positive results and the risk of being diagnosed with pseudodisease 100. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 31
56 2.5 SCREENING INTRODUCTION Currently, most lung cancers present at a stage when they are no longer potentially curable with surgical resection. Data from the Surveillance, Epidemiology, and End Results (SEER) program of the National Cancer Institute (USA) show that of invasive lung cancers, 15%, 24%, 48% and 13% are staged as having localised, regional, distant and unstaged disease respectively 101. Lung cancer screening offers the potential for tumours to be diagnosed at an earlier stage and this might lead to higher cure rates. Although primary prevention should continue to be the major focus of public health campaigns, in the near future the majority of lung cancer cases will be occurring among former smokers and there is a need to consider secondary prevention measures. Screening of high-risk individuals has previously been investigated in several randomised controlled trials 102,103,104,105,106,107,108. These studies were all conducted in the 1960s and 1970s and the findings have been summarised in a recent systematic review 109. The main conclusion that can be drawn from this review is that none of the lung cancer screening studies conducted to date have shown that screening alters the natural history of lung cancer. Because of limitations with previous studies further studies are being planned. Furthermore new screening tools such as helical (or spiral) computed tomography (CT) and biomarkers offer promise for the future. CHEST RADIOGRAPHY The major limitation of previous studies is that none of them included an unscreened control group. In the Mayo Lung Project, participants (male smokers) in the intervention group were offered four-monthly chest x-rays and sputum cytology examinations, while participants in the control group were advised to have an annual chest x-ray and sputum examination at the start of the study 110. In a Czech study, participants (male smokers) in the intervention group were offered six-monthly chest x-rays and sputum cytology examinations for the first three years and annual chest x-rays for the last three years of the study. The control group were offered a chest x-ray and sputum cytology examination at baseline and after three years followed by annual chest x-rays for the last three years of the study 107. The results from extended follow-up of these studies have recently been reported 111,112. Both studies showed that more frequent screening was not associated with a reduction in lung cancer mortality. In fact, screening with chest x-rays more frequently than annually was associated with a slight increase in lung cancer mortality compared with annual or less frequent screening 109. A multi-screening study currently being conducted in the USA has been designed to examine the efficacy of annual chest x-ray screening when compared with usual care. The PLCO (prostate, lung, colon and ovarian) cancer screening study is currently enrolling male and female subjects aged years Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
57 Participants randomised to the intervention group will be offered an annual chest x-ray for three years. The control group will not be offered active screening. Participants in the intervention group will also be offered screening tests for colon, ovarian (females) and prostate (males) cancer. The primary outcome is disease specific mortality. The results are not expected until SPUTUM CYTOLOGY Two of the randomised controlled studies conducted in the 1970s were designed to assess whether sputum cytology at four monthly intervals would reduce lung cancer mortality when added to annual chest x-ray screening 105,108,114. Each study had an almost identical study design. Both enrolled smokers over the age of 45 years. The intervention groups were offered annual chest x-rays and four-monthly sputum cytology examinations. The control groups were offered an annual chest x-ray only. In both studies, the addition of sputum cytology to annual chest radiography was not associated with a reduction in lung cancer mortality, however, the sample size in these studies was relatively small and the studies had insufficient statistical power to detect more marginal reductions in lung cancer mortality 109. Guideline Population Screening for Lung Cancer Level of Evidence Refs No forms of population screening for lung cancer, including regular chest radiography, with or without sputum cytology even in high-risk groups, have been shown to improve outcomes and screening is not recommended. I II 108,111, 113, ,107, 110 LOW-DOSE HELICAL COMPUTED TOMOGRAPHY Recent uncontrolled studies have shown that low-dose helical CT is a more sensitive screening tool than plain chest radiography 116,117. Although the findings of these studies are very promising, CT screening needs to be investigated in randomised controlled studies in order to determine whether early diagnosis and treatment will lead to a reduction in lung cancer mortality. Survival alone is not a reliable outcome measure in screening studies. Biases such as length-time, lead-time and overdiagnosis bias can produce an apparent improvement in survival even in the absence of a reduction in disease specific mortality 115. A pilot randomised controlled trial comparing annual chest radiography with annual low-dose helical CT is currently being conducted in the USA and other studies are being planned 115. In comparison to chest radiography, helical CT provides axial images of the lungs and mediastinum, with superior contrast resolution unhindered by superimposition of anatomical structures 118. As a result, CT has the potential to detect more lung cancers Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 33
58 when they are smaller and at an earlier stage. This is particularly relevant given the increasing proportion of adenocarcinomas, which are usually peripherally located in comparison to squamous cell carcinomas, which tend to be centrally located and less amenable to CT detection. The effective radiation dose for a low-dose helical CT screening examination is 0.65 millisieverts (msv) in men and 1.1mSv in women. This compares with 5.8mSv for a conventional high-definition CT diagnostic examination 119,120 and 0.015mSv for chest radiography. Because dose reduction in CT does not significantly decrease sensitivity for detection of small pulmonary nodules, low-dose helical CT has the potential to improve the early detection and prognosis of lung cancer. Clinical studies show that low-dose helical CT is a more sensitive screening tool for the detection of lung nodules and lung cancer than plain chest radiography 115,121,122. Uncontrolled studies of low-dose helical CT have reported encouraging findings; these include studies in Japan, Finland, Germany and the USA, many linked to the US initiated Early Lung Cancer Action Program (ELCAP) 116,123,124 (see also edu). These studies have assessed numbers and size of detected nodules, numbers of cancers detected and their size, stage, and surgical resectability. The results show that low-dose helical CT can detect lung cancers at a smaller size (less than 2cm in diameter) and earlier stage (58 100% Stage I) than chest radiography or current clinical practice (the mean diameter of the cancers detected in ELCAP was 8mm) 123. The potential benefit of this is shown by data from other studies indicating a significant survival benefit for Stage I lung cancers treated by lung resection, with up to about 70% five-year survival, in comparison to about 12% overall five-year survival for the usual care outcomes 125. Implementation of CT screening is critically dependent upon the availability of highquality investigational procedures including fine needle aspiration (FNA) biopsies 125. In evaluating the potential benefits of any such project, any improvement in lung cancer outcomes must be balanced against the morbidity and mortality imposed by investigation of small lung nodules, a significant proportion of which will be shown not to represent lung cancers, but benign inflammatory or other non-neoplastic lesions. Nonetheless, it has been suggested that screening projects using helical CT show sufficient promise to be worth implementation on an experimental basis, concentrating upon high-risk groups 125. There are indications that the cost per life year gained may be acceptable, but these depend on the assumptions made about benefits 126. It has been suggested that patients with a smoking history of more than 20 cigarettes per day and greater than 25 fibres/ml-years of asbestos exposure, who are aged older than 50 years and who have greater than 10 years following commencement of the asbestos exposure and cigarette smoking are particularly suitable for evaluation of screening by helical CT 125. The combination of low-dose helical CT and high-definition CT appears to provide good characterisation of lung cancers, with generally low rates of unnecessary surgical procedures. At this early stage of follow-up there is little available data on survival, and no data from controlled studies. Uncontrolled studies may not be able to determine if detection of small cancers will improve mortality rates, as distinct from post diagnosis survival rates, and the experience with conventional screening urges caution. 34 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
59 The studies (see National Cancer Control Initiative report, Lung cancer screening by helical computed tomography, available at NCCI website show high false positive rates for low-dose helical CT screening, although most positives can be resolved by further investigations without biopsy. No studies have yet examined how false positive results impact on the screenees quality of life. False negative rates for nodules also may be reasonably high; where both baseline and rescreening studies have been done between 36% and 66% of nodules detected on subsequent screening examinations were not seen on baseline scans. Technological advances and improved protocols may improve these figures, but wider use of the technique raises the issue of its performance by radiologists with less experience. The future availability of multi-slice/multi-detector helical CT scanners, and computer-assisted diagnosis and volumetrics, may significantly decrease the radiation exposure in a screening program. These advances may decrease the time for diagnosis of non-calcified nodules and decrease false negative rates, although these benefits may occur at the cost of higher false positive rates. The uncontrolled studies of low-dose helical CT screening are controversial. Their proponents claim that the results in terms of tumour size, stage, operability, and patient survival will demonstrate the benefits of the technique 127. Critics argue that because of the potential biases of lead-time, prevalence-duration bias, and overdiagnosis, which have all been demonstrated in the earlier trials of conventional radiology, uncontrolled studies may never provide firm evidence of benefit and may be misleading 119,128. One unanticipated benefit of ELCAP was a significant rate of smoking cessation (about 23%) 125. If this rate translates into long-term cessation, it would constitute an additional significant benefit and a major justification for implementation of an appropriate screening program based on helical CT. Guideline Helical CT Screening Level of Evidence Refs In view of the limited information available on outcome, helical CT screening for lung cancer is not recommended except in the context of a welldesigned clinical trial. III 3 114,122, 124,126 There are several randomised trials that are ongoing or being established in the US and in Europe. These are also reviewed in the NCCI report 129. BIOMARKERS AND FLUORESCENCE BRONCHOSCOPY Methods for detecting altered gene expression in sputum or bronchoalveolar lavage samples have been developed and several of these allow the determination of a molecular diagnosis of cancer years before clinical presentation 130. For some of these tests the test performance characteristics are currently being investigated in prospective studies 130. Other methods being investigated for the early detection of lung cancer Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 35
60 include immunologic based screening of sputum and fluorescence bronchoscopy 131. To date none of these methods have been used as a single screening technique in large randomised controlled population-based studies. Biomarkers are likely to be less accurate for the detection of small peripheral tumours but they might be a valuable complementary test to low-dose helical CT 132. OTHER METHODS FOR EARLY LUNG CANCER DETECTION Recent research on potential approaches to earlier diagnosis of lung cancer includes studies of genetic markers, developments in sputum cytology, immunostaining, oncogene mutations detected by polymerase chain reaction assays, developments in conventional and fluorescent bronchoscopy including laser induced fluorescence endoscopy and optical coherence tomography, virtual bronchoscopy, and analysis of volatile organic compounds in breath samples. All of these are primarily research issues at present. They are briefly reviewed in the NCCI report. References 1. Raw M, McNeill A, West R. Smoking Cessation Guidelines for Health Professionals. A Guide to Effective Smoking Cessation Interventions for the Health Care System. Health Education Authority. Thorax 1998; 53 Suppl 5 Pt 1: S Parrott S, Godfrey C, Raw M, West R, McNeill A. Guidance for Commissioners on the Cost Effectiveness of Smoking Cessation Interventions. Health Educational Authority. Thorax 1998; 53 Suppl 5 Pt 2: S Raw M, McNeill A, West R. Smoking Cessation: Evidence Based Recommendations for the Healthcare System. BMJ 1999; 318(7177): Website: US Agency for Health Care Policy and Research. US Agency for Health Care Policy and Research (AHCPR). 5. Fiore MC, et al. Treating Tobaco Use and Dependence: A Clinical Practice Guideline Rockville MD, US Dept of Health and Human Services, Public Health Services. 6. A Clinical Practice Guideline for Treating Tobacco Use and Dependence: A US Public Health Service Report. The Tobacco Use and Dependence Clinical Practice Guideline Panel, Staff, and Consortium Representatives. JAMA 2000; 283(24): Lancaster T, Stead L, Silagy C, Sowden A. Effectiveness of Interventions to Help People Stop Smoking: Findings From the Cochrane Library. BMJ 2000; 321(7257): Silagy C, Stead LF. Physician Advice for Smoking Cessation (Cochrane Review). Cochrane Database Syst Rev 2000; 2: CD Rice VH, Stead LF. Nursing Interventions for Smoking Cessation (Cochrane Review). Cochrane Database Syst Rev 2000; 3: CD Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
61 10. Stead LF, Lancaster T. Group Behaviour Therapy Programmes for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Lancaster T, Stead LF. Individual Behavioural Counselling for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Hajek P, Stead LF. Aversive Smoking for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Lancaster T, Stead LF. Silver Acetate for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Lancaster T, Stead LF. Self-Help Interventions for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Lichtenstein E, Glasgow RE, Lando HA, Ossip-Klein DJ, Boles SM. Telephone Counseling for Smoking Cessation: Rationales and Meta-Analytic Review of Evidence. Health Educ Res 1996; 11(2): Silagy C, Mant D, Fowler G, Lancaster T. Nicotine Replacement Therapy for Smoking Cessation. Cochrane Database Syst Rev 2000;(3): CD Hughes JR, Stead LF, Lancaster T. Anxiolytics and Antidepressants for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Gourlay SG, Stead LF, Benowitz NL. Clonidine for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Rigotti NA, Munafo MR, Murphy MF, Stead LF. Interventions for Smoking Cessation in Hospitalised Patients (Cochrane Review). Cochrane Database Syst Rev 2001; 2: CD Lancaster T, Stead LF. Mecamylamine (a Nicotine Antagonist) for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Stead LF, Hughes JR. Lobeline for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD White AR, Rampes H, Ernst E. Acupuncture for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Abbot NC, Stead LF, White AR, Barnes J, Ernst E. Hypnotherapy for Smoking Cessation. Cochrane Database Syst Rev 2000;(2): CD Ussher MH, West R, Taylor AH, McEwen A. Exercise Interventions for Smoking Cessation. Cochrane Database Syst Rev 2000;(3): CD Ziegler RG, Mayne ST, Swanson CA. Nutrition and Lung Cancer. Cancer Causes Control 1996; 7(1): Samet JM, Skipper BJ, Humble CG, Pathak DR. Lung cancer risk and vitamin A consumption in New Mexico. 131(2), American Review of Respiratory Disease Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 37
62 27. Kvale G, Bjelke E, Gart JJ. Dietary Habits and Lung Cancer Risk. Int J Cancer 1983; 31(4): Shekelle RB, Lepper M, Liu S, Maliza C, Raynor WJJ, Rossof AH, Paul O, Shryock AM, Stamler J. Dietary Vitamin A and Risk of Cancer in the Western Electric Study. Lancet 1981; 2(8257): Ziegler RG, Mason TJ, Stemhagen A, Hoover R, Schoenberg JB, Gridley G, Virgo PW, Fraumeni JFJ. Carotenoid Intake, Vegetables, and the Risk of Lung Cancer Among White Men in New Jersey. Am J Epidemiol 1986; 123(6): Hinds MW, Kolonel LN, Hankin JH, Lee J. Dietary Vitamin A, Carotene, Vitamin C and Risk of Lung Cancer in Hawaii. Am J Epidemiol 1984; 119(2): Kromhout D. Essential Micronutrients in Relation to Carcinogenesis. Am J Clin Nutr 1987; 45(5 Suppl): Shibata A, Paganini-Hill A, Ross RK, Henderson BE. Intake of Vegetables, Fruits, Beta-Carotene, Vitamin C and Vitamin Supplements and Cancer Incidence Among the Elderly: a Prospective Study. Br J Cancer 1992; 66(4): Fraser GE, Beeson WL, Phillips RL. Diet and Lung Cancer in California Seventh- Day Adventists. Am J Epidemiol 1991; 133(7): Knekt P, Jarvinen R, Seppanen R, Rissanen A, Aromaa A, Heinonen OP, Albanes D, Heinonen M, Pukkala E, Teppo L. Dietary Antioxidants and the Risk of Lung Cancer. Am J Epidemiol 1991; 134(5): Chow WH, Schuman LM, McLaughlin JK, Bjelke E, Gridley G, Wacholder S, Chien HT, Blot WJ. A Cohort Study of Tobacco Use, Diet, Occupation, and Lung Cancer Mortality. Cancer Causes Control 1992; 3(3): Steinmetz KA, Potter JD, Folsom AR. Vegetables, Fruit, and Lung Cancer in the Iowa Women s Health Study. Cancer Res 1993; 53(3): Byers T, Vena J, Mettlin C, Swanson M, Graham S. Dietary Vitamin A and Lung Cancer Risk: an Analysis by Histologic Subtypes. Am J Epidemiol 1984; 120(5): Byers TE, Graham S, Haughey BP, Marshall JR, Swanson MK. Diet and Lung Cancer Risk: Findings From the Western New York Diet Study. Am J Epidemiol 1987; 125(3): Gao YT, Blot WJ, Zheng W, Ershow AG, Hsu CW, Levin LI, Zhang R, Fraumeni JFJ. Lung Cancer Among Chinese Women. Int J Cancer 1987; 40(5): Pastorino U, Pisani P, Berrino F, Andreoli C, Barbieri A, Costa A, Mazzoleni C, Gramegna G, Marubini E. Vitamin A and Female Lung Cancer: a Case-Control Study on Plasma and Diet. Nutr Cancer 1987; 10(4): Fontham ET, Pickle LW, Haenszel W, Correa P, Lin YP, Falk RT. Dietary Vitamins A and C and Lung Cancer Risk in Louisiana. Cancer 1988; 62(10): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
63 42. Koo LC. Dietary Habits and Lung Cancer Risk Among Chinese Females in Hong Kong Who Never Smoked. Nutr Cancer 1988; 11(3): Le Marchand L, Yoshizawa CN, Kolonel LN, Hankin JH, Goodman MT. Vegetable Consumption and Lung Cancer Risk: a Population-Based Case-Control Study in Hawaii. J Natl Cancer Inst 1989; 81(15): Dartigues JF, Dabis F, Gros N, Moise A, Bois G, Salamon R, Dilhuydy JM, Courty G. Dietary Vitamin A, Beta Carotene and Risk of Epidermoid Lung Cancer in South-Western France. Eur J Epidemiol 1990; 6(3): Jain M, Burch JD, Howe GR, Risch HA, Miller AB. Dietary Factors and Risk of Lung Cancer: Results From a Case-Control Study, Toronto, Int J Cancer 1990; 45(2): Kalandidi A, Katsouyanni K, Voropoulou N, Bastas G, Saracci R, Trichopoulos D. Passive Smoking and Diet in the Etiology of Lung Cancer Among Non-Smokers. Cancer Causes Control 1990; 1(1): Candelora EC, Stockwell HG, Armstrong AW, Pinkham PA. Dietary Intake and Risk of Lung Cancer in Women Who Never Smoked. Nutr Cancer 1992; 17(3): Swanson CA, Mao BL, Li JY, Lubin JH, Yao SX, Wang JZ, Cai SK, Hou Y, Luo QS, Blot WJ. Dietary Determinants of Lung-Cancer Risk: Results From a Case-Control Study in Yunnan Province, China. Int J Cancer 1992; 50(6): Mayne ST, Janerich DT, Greenwald P, Chorost S, Tucci C, Zaman MB, Melamed MR, Kiely M, McKneally MF. Dietary Beta Carotene and Lung Cancer Risk in U.S. Nonsmokers. J Natl Cancer Inst 1994; 86(1): Dragsted LO, Strube M, Larsen JC. Cancer-Protective Factors in Fruits and Vegetables: Biochemical and Biological Background. Pharmacol Toxicol 1993; 72 Suppl 1: Steinmetz KA, Potter JD. Vegetables, Fruit, and Cancer. II. Mechanisms. Cancer Causes Control 1991; 2(6): Byers T, Perry G. Dietary Carotenes, Vitamin C, and Vitamin E As Protective Antioxidants in Human Cancers. Annu Rev Nutr 1992; 12: Comstock GW, Bush TL, Helzlsouer K. Serum Retinol, Beta-Carotene, Vitamin E, and Selenium As Related to Subsequent Cancer of Specific Sites. Am J Epidemiol 1992; 135(2): Kolonel LN, Hinds MW, Nomura AM, Hankin JH, Lee J. Relationship of Dietary Vitamin A and Ascorbic Acid Intake to the Risk for Cancers of the Lung, Bladder, and Prostate in Hawaii. Natl Cancer Inst Monogr 1985; 69: Willett WC, Polk BF, Underwood BA, Stampfer MJ, Pressel S, Rosner B, Taylor JO, Schneider K, Hames CG. Relation of Serum Vitamins A and E and Carotenoids to the Risk of Cancer. N Engl J Med 1984; 310(7): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 39
64 56. Stahelin HB, Rosel F, Buess E, Brubacher G. Cancer, Vitamins, and Plasma Lipids: Prospective Basel Study. J Natl Cancer Inst 1984; 73(6): Nomura AM, Stemmermann GN, Heilbrun LK, Salkeld RM, Vuilleumier JP. Serum Vitamin Levels and the Risk of Cancer of Specific Sites in Men of Japanese Ancestry in Hawaii. Cancer Res 1985; 45(5): Menkes MS, Comstock GW, Vuilleumier JP, Helsing KJ, Rider AA, Brookmeyer R. Serum Beta-Carotene, Vitamins A and E, Selenium, and the Risk of Lung Cancer. N Engl J Med 1986; 315(20): Nomura A, Heilbrun LK, Morris JS, Stemmermann GN. Serum Selenium and the Risk of Cancer, by Specific Sites: Case-Control Analysis of Prospective Data. Natl Cancer Inst 1987; 79(1): Virtamo J, Valkeila E, Alfthan G, Punsar S, Huttunen JK, Karvonen MJ. Serum Selenium and Risk of Cancer. A Prospective Follow-Up of Nine Years. Cancer 1987; 60(2): Knekt P, Aromaa A, Maatela J, Aaran RK, Nikkari T, Hakama M, Hakulinen T, Peto R, Saxen E, Teppo L. Serum Vitamin E and Risk of Cancer Among Finnish Men During a 10-Year Follow-Up. Am J Epidemiol 1988; 127(1): Knekt P, Aromaa A, Maatela J, Alfthan G, Aaran RK, Hakama M, Hakulinen T, Peto R, Teppo L. Serum Selenium and Subsequent Risk of Cancer Among Finnish Men and Women. J Natl Cancer Inst 1990; 82(10): Criqui MH, Bangdiwala S, Goodman DS, Blaner WS, Morris JS, Kritchevsky S, Lippel K, Mebane I, Tyroler HA. Selenium, Retinol, Retinol-Binding Protein, and Uric Acid. Associations With Cancer Mortality in a Population-Based Prospective Case-Control Study. Ann Epidemiol 1991; 1(5): van den Brandt PA, Goldbohm RA, Van t Veer P, Bode P, Dorant E, Hermus RJ, Sturmans F. A Prospective Cohort Study on Selenium Status and the Risk of Lung Cancer. Cancer Res 1993; 53(20): Kabuto M, Imai H, Yonezawa C, Neriishi K, Akiba S, Kato H, Suzuki T, Land CE, Blot WJ. Prediagnostic Serum Selenium and Zinc Levels and Subsequent Risk of Lung and Stomach Cancer in Japan. Cancer Epidemiol Biomarkers Prev 1994; 3(6): Garland M, Morris JS, Stampfer MJ, Colditz GA, Spate VL, Baskett CK, Rosner B, Speizer FE, Willett WC, Hunter DJ. Prospective Study of Toenail Selenium Levels and Cancer Among Women. J Natl Cancer Inst 1995; 87(7): Ziegler RG. Vegetables, Fruits, and Carotenoids and the Risk of Cancer. Am J Clin Nutr 1991; 53(1 Suppl): 251S 9S. 68. Byers T. Diet as a factor in the etiology and prevention of lung cancer. Samet J (ed) Epidemiology of lung cancer. New York: Marcel Dekker, 1994: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
65 69. Block G, Patterson B, Subar A. Fruit, Vegetables, and Cancer Prevention: a Review of the Epidemiological Evidence. Nutr Cancer 1992; 18(1): Steinmetz KA, Potter JD. Vegetables, Fruit, and Cancer. I. Epidemiology. Cancer Causes Control 1991; 2(5): Dorgan JF, Ziegler RG, Schoenberg JB, Hartge P, McAdams MJ, Falk RT, Wilcox HB, Shaw GL. Race and Sex Differences in Associations of Vegetables, Fruits, and Carotenoids With Lung Cancer Risk in New Jersey (United States). Cancer Causes Control 1993; 4(3): Feskanich D, Ziegler RG, Michaud DS, Giovannucci EL, Speizer FE, Willett WC, Colditz GA. Prospective Study of Fruit and Vegetable Consumption and Risk of Lung Cancer Among Men and Women. J Natl Cancer Inst 2000; 92(22): Tannenbaum A. The Genesis and Growth of Tumours. III. Effect of a High Fat Diet. Cancer Res 1942; 2: Voorrips LE, Goldbohm RA, Verhoeven DT, van Poppel GA, Sturmans F, Hermus RJ, van den Brandt PA. Vegetable and Fruit Consumption and Lung Cancer Risk in the Netherlands Cohort Study on Diet and Cancer. Cancer Causes Control 2000; 11(2): Brownson RC, Alavanja MC, Caporaso N, Simoes EJ, Chang JC. Epidemiology and Prevention of Lung Cancer in Nonsmokers. Epidemiol Rev 1998; 20(2): Cooper DA, Eldridge AL, Peters JC. Dietary Carotenoids and Lung Cancer: a Review of Recent Research. Nutr Rev 1999; 57(5 Pt 1): Albanes D. Beta-Carotene and Lung Cancer: a Case Study. Am J Clin Nutr 1999; 69(6): 1345S 50S. 78. Michaud DS, Feskanich D, Rimm EB, Colditz GA, Speizer FE, Willett WC, Giovannucci E. Intake of Specific Carotenoids and Risk of Lung Cancer in 2 Prospective US Cohorts. Am J Clin Nutr 2000; 72(4): Tucker MA, Murray N, Shaw EG, Ettinger DS, Mabry M, Huber MH, Feld R, Shepherd FA, Johnson DH, Grant SC, Aisner J, Johnson BE. Second Primary Cancers Related to Smoking and Treatment of Small-Cell Lung Cancer. Lung Cancer Working Cadre. J Natl Cancer Inst 1997; 89(23): Mao L, Lee JS, Kurie JM, Fan YH, Lippman SM, Lee JJ, Ro JY, Broxson A, Yu R, Morice RC, Kemp BL, Khuri FR, Walsh GL, Hittelman WN, Hong WK. Clonal Genetic Alterations in the Lungs of Current and Former Smokers. J Natl Cancer Inst 1997; 89(12): Wistuba II, Lam S, Behrens C, Virmani AK, Fong KM, LeRiche J, Samet JM, Srivastava S, Minna JD, Gazdar AF. Molecular Damage in the Bronchial Epithelium of Current and Former Smokers. J Natl Cancer Inst 1997; 89(18): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 41
66 82. The Effect of Vitamin E and Beta Carotene on the Incidence of Lung Cancer and Other Cancers in Male Smokers. The Alpha-Tocopherol, Beta Carotene Cancer Prevention Study Group. N Engl J Med 1994; 330(15): Albanes D, Heinonen OP, Taylor PR, Virtamo J, Edwards BK, Rautalahti M, Hartman AM, Palmgren J, Freedman LS, Haapakoski J, Barrett MJ, Pietinen P, Malila N, Tala E, Liippo K, Salomaa ER, Tangrea JA, Teppo L, Askin FB, Taskinen E, Erozan Y, Greenwald P, Huttunen JK. Alpha-Tocopherol and Beta-Carotene Supplements and Lung Cancer Incidence in the Alpha-Tocopherol, Beta- Carotene Cancer Prevention Study: Effects of Base-Line Characteristics and Study Compliance. J Natl Cancer Inst 1996; 88(21): Omenn GS, Goodman GE, Thornquist MD, Balmes J, Cullen MR, Glass A, Keogh JP, Meyskens FLJ, Valanis B, Williams JHJ, Barnhart S, Cherniack MG, Brodkin CA, Hammar S. Risk Factors for Lung Cancer and for Intervention Effects in CARET, the Beta-Carotene and Retinol Efficacy Trial. J Natl Cancer Inst 1996; 88(21): Omenn GS, Goodman GE, Thornquist MD, Balmes J, Cullen MR, Glass A, Keogh JP, Meyskens FL, Valanis B, Williams JH, Barnhart S, Hammar S. Effects of a Combination of Beta Carotene and Vitamin A on Lung Cancer and Cardiovascular Disease. N Engl J Med 1996; 334(18): Hennekens CH, Buring JE, Manson JE, Stampfer M, Rosner B, Cook NR, Belanger C, LaMotte F, Gaziano JM, Ridker PM, Willett W, Peto R. Lack of Effect of Long-Term Supplementation With Beta Carotene on the Incidence of Malignant Neoplasms and Cardiovascular Disease. N Engl J Med 1996; 334(18): Lee IM, Cook NR, Manson JE, Buring JE, Hennekens CH. Beta-Carotene Supplementation and Incidence of Cancer and Cardiovascular Disease: the Women s Health Study. J Natl Cancer Inst 1999; 91(24): Gouveia J, Mathe G, Hercend T, Gros F, Lemaigre G, Santelli G, Homasson JP, Gaillard JP, Angebault M, Bonniot JP, Lededente A, Marsac J, Parrot R, Pretet S. Degree of Bronchial Metaplasia in Heavy Smokers and Its Regression After Treatment With a Retinoid. Lancet 1982; 1(8274): Lee JS, Lippman SM, Benner SE, Lee JJ, Ro JY, Lukeman JM, Morice RC, Peters EJ, Pang AC, Fritsche HAJ. Randomized Placebo-Controlled Trial of Isotretinoin in Chemoprevention of Bronchial Squamous Metaplasia. J Clin Oncol 1994; 12(5): Arnold AM, Browman GP, Levine MN, D Souza T, Johnstone B, Skingley P, Turner-Smith L, Cayco R, Booker L, Newhouse M. The Effect of the Synthetic Retinoid Etretinate on Sputum Cytology: Results From a Randomised Trial. Br J Cancer 1992; 65(5): McLarty JW, Holiday DB, Girard WM, Yanagihara RH, Kummet TD, Greenberg SD. Beta-Carotene, Vitamin A, and Lung Cancer Chemoprevention: Results of an Intermediate Endpoint Study. Am J Clin Nutr 1995; 62(6 Suppl): 1431S 8S. 42 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
67 92. Pastorino U, Infante M, Maioli M, Chiesa G, Buyse M, Firket P, Rosmentz N, Clerici M, Soresi E, Valente M. Adjuvant Treatment of Stage I Lung Cancer With High-Dose Vitamin A. J Clin Oncol 1993; 11(7): van Zandwijk N, Dalesio O, Pastorino U, de Vries N, van Tinteren H. EUROSCAN, a Randomized Trial of Vitamin A and N-Acetylcysteine in Patients With Head and Neck Cancer or Lung Cancer. For the EUropean Organization for Research and Treatment of Cancer Head and Neck and Lung Cancer Cooperative Groups. J Natl Cancer Inst 2000; 92(12): Lippman SM, Lee JJ, Karp DD, Vokes EE, Benner SE, Goodman GE, Khuri FR, Marks R, Winn RJ, Fry W, Graziano SL, Gandara DR, Okawara G, Woodhouse CL, Williams B, Perez C, Kim HW, Lotan R, Roth JA, Hong WK. Randomized Phase III Intergroup Trial of Isotretinoin to Prevent Second Primary Tumors in Stage I Non- Small-Cell Lung Cancer. J Natl Cancer Inst 2001; 93(8): Hercberg S, Preziosi P, Briancon S, Galan P, Triol I, Malvy D, Roussel AM, Favier A. A Primary Prevention Trial Using Nutritional Doses of Antioxidant Vitamins and Minerals in Cardiovascular Diseases and Cancers in a General Population: the SU.VI.MAX Study-Design, Methods, and Participant Characteristics. SUpplementation En VItamines Et Mineraux AntioXydants. Control Clin Trials 1998; 19(4): Hercberg S, Galan P, Preziosi P, Roussel AM, Arnaud J, Richard MJ, Malvy D, Paul-Dauphin A, Briancon S, Favier A. Background and Rationale Behind the SU.VI.MAX Study, a Prevention Trial Using Nutritional Doses of a Combination of Antioxidant Vitamins and Minerals to Reduce Cardiovascular Diseases and Cancers. SUpplementation En VItamines Et Mineraux AntioXydants Study. Int J Vitam Nutr Res 1998; 68(1): Christen WG, Gaziano JM, Hennekens CH. Design of Physicians Health Study II--a Randomized Trial of Beta-Carotene, Vitamins E and C, and Multivitamins, in Prevention of Cancer, Cardiovascular Disease, and Eye Disease, and Review of Results of Completed Trials. Ann Epidemiol 2000; 10(2): Wolpaw DR. Early Detection in Lung Cancer. Case Finding and Screening. Med Clin North Am 1996; 80(1): Midthun D, Jett JR. Early Detection of Lung Cancer: Todays Approach. The Journal of Respiratory Diseases 1998; 19(1): Black WC. Overdiagnosis: An Underrecognized Cause of Confusion and Harm in Cancer Screening. J Natl Cancer Inst 2000; 92(16): SEER Cancer Statistics Review Bethesda, MD, USA, National Cancer Institute Burns DM. Primary Prevention, Smoking, and Smoking Cessation: Implications for Future Trends in Lung Cancer Prevention. Cancer 2000; 89(11 Suppl): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 43
68 103. Brett GZ. Earlier Diagnosis and Survival in Lung Cancer. Br Med J 1969; 4(678): Flehinger BJ, Kimmel M, Polyak T, Melamed MR. Screening for Lung Cancer. The Mayo Lung Project Revisited. Cancer 1993; 72(5): Flehinger BJ, Melamed MR, Zaman MB, Heelan RT, Perchick WB, Martini N. Early Lung Cancer Detection: Results of the Initial (Prevalence) Radiologic and Cytologic Screening in the Memorial Sloan-Kettering Study. Am Rev Respir Dis 1984; 130(4): Friedman GD, Collen MF, Fireman BH. Multiphasic Health Checkup Evaluation: a 16-Year Follow-Up. J Chronic Dis 1986; 39(6): Kubik A, Parkin DM, Khlat M, Erban J, Polak J, Adamec M. Lack of Benefit From Semi-Annual Screening for Cancer of the Lung: Follow-Up Report of a Randomized Controlled Trial on a Population of High-Risk Males in Czechoslovakia. Int J Cancer 1990; 45(1): Melamed MR, Flehinger BJ, Zaman MB, Heelan RT, Perchick WA, Martini N. Screening for Early Lung Cancer. Results of the Memorial Sloan-Kettering Study in New York. Chest 1984; 86(1): Manser, Rl, Irving LB, Stone C, Byrnes G, Abramson M, Campbell D. Screening for Lung Cancer (Cochrane Review). Cochrane Database Syst Rev 2002; 3: CD Fontana RS, Sanderson DR, Woolner LB, Taylor WF, Miller WE, Muhm JR, Bernatz PE, Payne WS, Pairolero PC, Bergstralh EJ. Screening for Lung Cancer. A Critique of the Mayo Lung Project. Cancer 1991; 67(4 Suppl): Marcus PM, Bergstralh EJ, Fagerstrom RM, Williams DE, Fontana R, Taylor WF, Prorok PC. Lung Cancer Mortality in the Mayo Lung Project: Impact of Extended Follow-Up. J Natl Cancer Inst 2000; 92(16): Kubik AK, Parkin DM, Zatloukal P. Czech Study on Lung Cancer Screening: Post-Trial Follow-Up of Lung Cancer Deaths Up to Year 15 Since Enrollment. Cancer 2000; 89(11 Suppl): Kramer BS, Gohagan J, Prorok PC, Smart C. A National Cancer Institute Sponsored Screening Trial for Prostatic, Lung, Colorectal, and Ovarian Cancers. Cancer 1993; 71(2 Suppl): Flehinger BJ, Melamed MR. Current Status of Screening for Lung Cancer. Chest Surg Clin N Am 1994; 4(1): Patz EFJ, Goodman PC, Bepler G. Screening for Lung Cancer. N Engl J Med 2000; 343(22): Henschke CI, McCauley DI, Yankelevitz DF, Naidich DP, McGuinness G, Miettinen OS, Libby DM, Pasmantier MW, Koizumi J, Altorki NK, Smith JP. Early Lung Cancer Action Project: Overall Design and Findings From Baseline Screening. Lancet 1999; 354(9173): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
69 117. Kaneko M, Eguchi K, Ohmatsu H, Kakinuma R, Naruke T, Suemasu K, Moriyama N. Peripheral Lung Cancer: Screening and Detection With Low-Dose Spiral CT Versus Radiography. Radiology 1996; 201(3): Zoetelief J, Geleijns J. Patient Doses in Spiral CT. Br J Radiol 1998; 71(846): Aberle DR, Gamsu G, Henschke CI, Naidich DP, Swensen SJ. A Consensus Statement of the Society of Thoracic Radiology: Screening for Lung Cancer With Helical Computed Tomography. J Thorac Imaging 2001; 16(1): Diederich S, Wormanns D, Semik M, Thomas M, Lenzen H, Roos N, Heindel W. Screening for Early Lung Cancer With Low-Dose Spiral CT: Prevalence in 817 Asymptomatic Smokers. Radiology 2002; 222(3): Patz EF, Jr., Black WC, Goodman PC. CT Screening for Lung Cancer: Not Ready for Routine Practice. Radiology 2001; 221(3): Ellis JR, Gleeson FV. Lung Cancer Screening. Br J Radiol 2001; 74(882): Henschke CI. Early lung cancer action project: findings on baseline and annual repeat screening CT. 36, Helsinki, Finnish Institute of Occupational Health. In: New advances in radiology and screening of asbestos-related diseases. People and Work Research Reports Henschke CI, Yankelevitz DF. Screening for Lung Cancer. J Thorac Imaging 2000; 15(1): Multiple. Summary - international expert meeting on new advances in radiology and screening of asbestos-related diseases. 36, Helsinki, Finnish Institute of Occupational Health. In: People and Work Research Reports Marshall D, Simpson KN, Earle CC, Chu CW. Economic Decision Analysis Model of Screening for Lung Cancer. Eur J Cancer 2001; 37(14): Miettinen OS. Screening for Lung Cancer: Can It Be Cost-Effective? CMAJ 2000; 162(10): Woloshin S, Schwartz LM, Welch HG. Tobacco Money: Up in Smoke? Lancet 2002; 359(9323): National Cancer Control Initiative website Tockman MS. Advances in Sputum Analysis for Screening and Early Detection of Lung Cancer. Cancer Control 2000; 7(1): Lam S, Shibuya H. Early Diagnosis of Lung Cancer. Clin Chest Med 1999; 20(1): Mulshine JL, Henschke CI. Prospects for Lung-Cancer Screening. Lancet 2000; 355(9204): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 45
70 3. INITIAL ASSESSMENT AND PROGNOSTIC FACTORS 3.1 Appropriate referral for suspected lung cancer 3.2 Diagnosis of lung cancer Chest x-ray and computed tomography scan Sputum cytology Fine needle aspiration and fibreoptic bronchoscopy Fluoro-deoxy glucose (FDG) PET Scan 3.3 Staging lung cancer Non-small cell lung cancer TNM staging T staging N staging M staging Small cell lung cancer Staging system Staging procedures for SCLC 3.4 Prognostic factors Non-small cell lung cancer Small cell lung cancer 3.5 Follow-up Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 47
71 3.1 APPROPRIATE REFERRAL FOR SUSPECTED LUNG CANCER Lung cancer has many presentations and occurs in individuals of varying ages and with a wide spectrum of comorbidities. When lung cancer is first suspected, the contribution of the tumour to reduced well-being and performance status of the patient may not be obvious, nor is the potential for a response to treatment always recognised. There is good Australian data that a significant number of patients with lung cancer do not receive a specialist opinion and are not considered for treatment 1. All people with suspected lung pathology should be referred to a specialist with expertise in the management of lung disease. Furthermore, patients with lung cancer should have access to a unit offering multidisciplinary care. Multidisciplinary care has been most useful in managing breast cancer, but remains unproven in managing lung cancer 2,3. Guideline - Lung Cancer - Clinical Management Level of Evidence Refs All individuals with suspected lung cancer should be referred to a specialist with expertise in the management of lung disease for an opinion. IV 1 This includes patients who may appear physically or mentally unfit for further investigation or treatment. The specialist opinion will either endorse this approach, or will identify tumour-related effects on the patient s physical and mental state that may respond to specific tumour treatment or palliative care. 3.2 DIAGNOSIS OF LUNG CANCER In most cases of suspected lung cancer it will be appropriate to confirm the diagnosis and establish the pathological subtype. Usually this is achieved with relatively non-invasive tests. Unless the diagnosis is confirmed histologically, there remains a possibility that the patient has some other condition which can be effectively treated. CHEST X-RAY AND COMPUTED TOMOGRAPHY SCAN The possibility of lung cancer is often raised by the presence of a solitary pulmonary nodule (SPN; lesion < 4cm) or lung mass (lesion > 4cm) on a chest x-ray. The challenge with SPNs is to diagnose all the lung cancers and to minimise invasive procedures in patients with benign lesions. Much research has been conducted in this area using chest x-ray, CT scanning and newer imaging and biological techniques. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 49
72 Early lung cancer can present as an asymptomatic SPN detected on a chest x-ray or CT scan taken for other reasons. However, the majority of SPNs are benign. A summary of five large series of resected non-calcified SPNs showed that 54% were granulomas, 28% primary lung cancers, 7% hamartomas and 4% metastases 4. Of 71 intrapulmonary coin lesions seen at The Prince Charles Hospital during , 48 were primary pulmonary malignancies and six were metastases. There were two cases each of tuberculosis, cryptococcosis, hamartoma and granuloma. Overall, 76% of the lesions were malignant and only 3% were tuberculous. These findings contrast with those from the same institution published 20 years ago, when malignancy comprised only 38% and tuberculosis 27% of lesions. Malignancy now seems to be the major cause of coin lesions in Australia. In this survey, 82% of SPNs that occurred in patients of over 50 years of age were malignant 5. The majority of individuals with lung cancer have symptoms at diagnosis 6. Lung masses with associated clinical features are likely to be malignant and the next step is to obtain a tissue diagnosis in the least invasive manner (discussed below). At present there is no specific protocol for investigating SPNs that can be recommended as a guideline. However, the following observations are relevant: KEY POINTS: These key points and a number of recommendations in this chapter have had evidence classified according to the Oxford Levels of Evidence for Diagnostic Tests, (see Appendix 7) and have been clearly identified -(O). Lack of growth is better than any morphological feature on imaging. Therefore, comparison with previous x-rays is very useful. A lesion that has remained stable for two years may be benign 7. Calcification is the single best morphological indicator of a benign lesion 8 (II-O). CT detects calcification more accurately than chest x-ray 9 (II-O). CT is the most sensitive imaging modality for identification of pulmonary nodules and is specific for the benign SPN with several diagnostic imaging findings. Specific patterns of calcification identified in a SPN by CT are highly specific for a benign diagnosis. However, the overall specificity of CT is poor because most lesions have indeterminate features and require invasive procedures for diagnosis 10 (III-O). An algorithm using low-dose helical CT followed by other investigations has recently been shown to be accurate in distinguishing benign from malignant SPNs 11. This is currently under further evaluation (II-O). Positron emission tomography (PET) has been shown in multiple studies to distinguish between malignant and benign SPNs with a sensitivity of 83 92% and specificity of about 90% 12,13. The overall cost-effectiveness of PET in relation to management of lung cancer has yet to be determined (refer to Chapter 10 and MSAC Assessment Report March Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
73 When the considerations above are combined with appropriate use of relatively non-invasive diagnostic procedures (see below), the need for surgical biopsy or excision of an undiagnosed SPN is low. SPUTUM CYTOLOGY Although cough is present in 50% of lung cancer patients at the time of diagnosis 14, sputum cytology is frequently negative because of lack of sputum, the peripheral position of the lesion or because of false negatives. The sensitivity of sputum cytology increases with the number of specimens obtained: from about 50% with a single specimen up to almost 90% with three or more specimens 15. It is highest with centrally placed squamous cell carcinomas and lowest with both peripheral tumours and centrally placed small cell carcinomas, because most of the tumour is below the mucosa. The use of induced ultrasonic nebulised sputum 16 and optimal processing 17 also increases the sensitivity of sputum cytology for the detection of lung cancer. The specificity of positive sputum cytology is high (97.9%) 18 and it is a non-invasive, readily available and inexpensive test. Guidelines - Lung Cancer - Sputum Cytology Level of Evidence Refs Sputum cytology is recommended to help establish a positive diagnosis of lung cancer in individuals with a central pulmonary mass. III-(O) 16,17 FINE NEEDLE ASPIRATION AND FIBREOPTIC BRONCHOSCOPY Percutaneous fine needle aspiration of a peripheral lung lesion under radiographic guidance is a relatively non-invasive diagnostic procedure with a sensitivity for detecting lung cancer of over 85% 19,20. For SPNs the negative predictive value of FNA has been reported as ranging from 52 84% 21,22. Sampling error is a problem and many experts would not rely on the result of a negative FNA alone to manage a SPN. The main risk is pneumothorax in individuals with bullous lung disease. This becomes clinically important if the pneumothorax is large or if the patient has a limited respiratory reserve. The diagnostic yield of transbronchial biopsies for peripheral nodules and lung masses is 30 50%, and less for lesions smaller than 2cm 23,24,25. The addition of bronchoalveolar lavage, brushings and bronchoscopic aspiration can increase the yield to about 75%. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 51
74 Lung cancer often develops in the central airways (especially the squamous and small cell types), usually as an endobronchial lesion. Bronchoscopy with washings, brushings and biopsies of an endobronchial lesion have a diagnostic yield (diagnostic accuracy) of close to 100% 26. Less commonly, a centrally located cancer has peribronchial and submucosal involvement causing extrinsic bronchial compression. Shure reported that bronchial biopsies have a lower yield in this setting (55%) whereas that of bronchoscopic needle aspiration was 71% and reached 91% with biopsies, needle aspiration, washings and brushings 27,28. Furthermore, bronchoscopy also gives staging information about central lesions. Mediastinal and peribronchial masses can be sampled using a Wang needle with a diagnostic accuracy of 25 40% 29,30. Fine needle aspiration can also be used to establish the diagnosis of lung cancer in patients presenting with accessible metastatic lesions. Endobronchial ultrasound is a new technique that is being evaluated in lung cancer and may increase the diagnostic utility of the Wang needle biopsy technique. Guidelines Lung Cancer Bronchoscopy and FNA Level of Evidence Refs Fibreoptic bronchoscopy is a procedure that has a high diagnostic yield (accuracy) in lung cancer. III (O) 26,30 In the diagnostic approach to suspected endobronchial lung tumours, bronchoscopy is usually the appropriate initial investigation for endobronchial evaluation and pathological confirmation. IV (O) 28 Fine needle aspiration is an appropriate initial investigation option for the pathological diagnosis of peripheral lung lesions in the absence of contraindications. IV (O) 19,20 FLUORO-DEOXY GLUCOSE (FDG) PET SCAN This non-invasive imaging technique has been found to be very accurate in differentiating benign from malignant pulmonary lesions where the lesion is of at least 1cm in size 13,31,32. A recent meta-analysis has suggested a sensitivity of 97% and a specificity of 78% 33. It was suggested that PET may be more accurate than FNA biopsy, with an accuracy of 94% compared to 86% respectively. It may also prove to be cost-effective 34, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
75 PET has been useful in the diagnosis of lung masses where a tissue diagnosis is not possible. Its high negative predictive value for malignancy suggests that PET-negative lesions can be safely observed 31,32.False negative studies are rare, but have been reported in bronchioloalveolar carcinoma and certain low-grade adenocarcinoma. False positive results are not uncommon and have been reported in granulomatous disease such as sarcoidosis, tuberculosis and histoplasmosis 36. This is an important consideration when PET is used to select individuals for curative surgery (see below). Guideline Lung Cancer PET Scanning in Diagnosis PET scanning is accurate in differentiating benign from malignant pulmonary lesions. It is highly predictive for diagnosis of lung masses when a tissue diagnosis is not readily available. Level of Evidence Refs I (O) 31,32, STAGING LUNG CANCER Accurate histological diagnosis should precede staging procedures. The pathological findings are best reported in a synoptic manner, as seen in Appendix 7. NON-SMALL CELL LUNG CANCER The aim of staging NSCLC is to accurately identify the group of patients who will have a survival benefit from surgical resection or radical chemoradiation (Stage I to IIIA). Inherent in this approach is the assumption that the individual is medically fit for, and agrees to, the treatment. It should also be understood that clinical stage (ctnm) is less accurate than pathological stage (ptnm), and will therefore be associated with different outcomes. Staging NSCLC at the time of diagnosis according to the TNM system (revised 2002), guides management and predicts outcome. Information about staging is also of epidemiological importance, being used for health resource planning and research. Determination of T stage requires measurement of tumour size and determination of the presence or absence of atelectasis, pleural effusion, ipsilateral lung nodule(s), or involvement of central airways, mediastinal structures, the pleura, the chest wall, the diaphragm or a vertebral body. Determination of N stage involves identification of bronchial, hilar, mediastinal and extra-pulmonary lymphadenopathy. In a few situations, simple radiology may be sufficient to define the T and N stages for practical purposes, for example, an obvious pleural effusion, direct chest wall invasion with bone erosion or gross hilar and mediastinal lymph node enlargement. However, in the large majority of cases, a chest x-ray does not define the T or N status accurately enough to guide management. In particular, a significant number of T1N0 and T2N0 lesions on chest x-ray staging are up-staged when reassessed with other staging techniques. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 53
76 TNM STAGING T staging CT has been the conventional imaging modality in delineating the size and local extent of the primary cancer 37,38. In the assessment of chest wall invasion, the overall accuracy of CT has been reported to be 39 86% 39,40,41. Magnetic resonance imaging (MRI) has a similar reported accuracy but has been found to be more superior in the assessment of local invasion including brachial plexus involvement in superior sulcus tumour and in cases where the CT findings are equivocal. This is a result of MRI s superior soft tissue contrast resolution and multi-planar capabilities 41,42,43,44. CT and MRI have similar reported accuracies in the assessment of mediastinal involvement, in the range of 50 90%, although MRI has been shown to be slightly better due to superior soft tissue contrast between tumour and fat and blood vessels 45,46,47. FDG PET is not generally the modality of choice in the assessment of local extent and invasion due to its inferior resolution compared to CT/MRI. FDG PET has, however, been found to be useful in differentiating tumour from adjacent consolidated or collapsed lung, which may improve staging accuracy and treatment planning 48. N staging CT is the most widely used modality in the evaluation of hilar and mediastinal nodal disease using the size criteria in which a short axis more than 1cm is considered pathological 49. This is a non-specific criterion. Optimal scanning techniques including adequate contrast enhancement and thin sections of the hilar regions have significant impact on its diagnostic accuracy. As a consequence the sensitivity and specificity of CT N staging are approximately 60 65% and 60 70% respectively 41,50,51,52. Similar diagnostic accuracy has been reported with MRI 45. Because CT assessment incorrectly over-stages or under-stages T and N status in up to 40% of cases 53 some form of surgical sampling is required to confirm the CT results 54. The value of mediastinoscopy as a staging procedure is widely accepted 55, however it is often limited by the accessibility of lymph nodes and is prone to sampling errors. Thus, in two studies a third of the negative mediastinoscopies were found to have disease at thoracotomy 56,57. Anterior mediastinotomy allows access to some nodes that cannot be sampled by mediastinoscopy. Guideline Staging Non-small Cell Lung Cancer Level of Evidence Refs Patients with mediastinal nodes larger than 1cm in transverse diameter on CT who otherwise have resectable lung disease should undergo further staging evaluation. I (O) 51,54 54 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
77 PET staging of N status has an accuracy of around 90% (81 99% reported), sensitivity of % and specificity of 90 99% 58,59,60. A mean sensitivity of 79% and specificity of 91% for PET, and 60% and 77% respectively for CT, were reported in a meta-analysis 51. FDG PET has also been shown to separate N2 and N3 disease reliably,54,52,61. The high negative predictive value of PET in mediastinal staging allows patients with a negative scan to proceed to thoracotomy without invasive mediastinal staging 62. False positive results have been reported in granulomatous disease and other inflammatory conditions, and surgical sampling of nodes may be required before denying curative treatment. Overall, FDG PET has been found to modify staging and change the management plan in 30 40% of patients 61,56,54. Guideline PET Scanning in Staging Non-small Cell Lung Cancer Level of Evidence Refs PET has been found to be more accurate than CT in mediastinal nodal staging for non-small cell lung cancer. A negative PET is highly specific, but positive PET nodes are not always malignant and histological confirmation may be required before advancing to definitive management. I (O) 51,58,59 M staging Metastatic NSCLC causes problems for staging because it is common, involves many different sites without any predictable patterns and is often asymptomatic. The common metastatic sites are liver, adrenals, brain and bone, however, many other regions can be involved. About 25% of patients are found to have metastases at presentation 63 and many of these do not have extensive local disease 64,65. There is a correlation between T and N stage and the presence of metastases with squamous cell carcinoma but not with large cell or adenocarcinoma 65. If the clinical assessment for metastases is positive at presentation, 50% of patients will have metastases. However, many patients found to have metastases on routine screening are asymptomatic 65. Also postmortem studies of patients who died in the peri-operative period following curative surgery 66, and PET studies of individuals staged by conventional methods as M0, have shown occult metastases in about 20% 67,68. In spite of the risk of occult metastases, there is no good evidence to recommend routine imaging of extrathoracic sites in all cases of NSCLC in the absence of suspicious clinical or laboratory findings 40,41,69,70. In Australian practice, imaging of the upper abdomen is routinely included in CT scanning of the thorax performed for T and N assessment. Isolated liver metastases are uncommon 63 and the impact of CT of the liver on M staging is low. Adrenal lesions are frequently seen, but two thirds are adenomas 71. Chemical shift MRI imaging is reliable Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 55
78 in differentiating adenomas from adrenal metastases when CT findings are equivocal 72. Other alternatives include CT densitometry using non-enhanced CT attenuation of the lesions, washout of CT contrast enhancement 73 and PET scans. However, biopsy confirmation is generally required before altering management. Bone metastases are found at presentation in 9 15% of patients. Most of these are apparent clinically or cause an elevated serum calcium or alkaline phosphatase. A plain radiograph, radionuclide bonescan or MRI are useful modalities to investigate suspected bony metastases. Because the incidence of occult bony metastases is less than 4% 64,70, routine bone scans are not recommended. Isolated cerebral metastases are rare and asymptomatic disease is reported in only % of patients, usually with large cell carcinoma or adenocarcinoma 74,75. The value of routine brain imaging in asymptomatic NSCLC (all types) is not established, although it is often done for large cell carcinoma and adenocarcinomas. Both CT and MRI are used to detect cerebral metastases, though MRI is the more sensitive modality 64. PET is more accurate in the detection of metastatic disease in adrenal glands and the skeleton compared to CT and radionuclide bone scan 76,77,78. Occult extrathoracic metastases were detected in up to 24% of patients by whole body FDG PET 67,68,79. Overall, staging by PET has been shown to be more accurate than conventional imaging and this can impact on clinical management in up to two thirds of patients and may be cost-effective in clinical practice 61,68,80,81. PET staging has been found to be a powerful predictor of survival and translates to more superior prognostic stratification compared to conventional staging methods 56,68,82. In summary, M staging of NSCLC is difficult because there are no clearly proven pathways using conventional tests, and PET, which is clearly superior for detecting (non-cerebral) metastases, is not universally available. The following guidelines are recommended: Guidelines M Staging of Non-small Cell Lung Cancer Level of Evidence Refs If clinical assessment for metastases is abnormal, then further investigations are indicated, as metastases will be confirmed in 50% of such cases. Routine bone scanning in non-small cell lung cancer is of little clinical value if there are no abnormal clinical or biochemical features. The role of routine brain imaging in non-small cell lung cancer asymptomatic patients is unclear, but the detection rate is low. I (O) 65 III (O) 64,70 III (O) 74,75 56 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
79 Guidelines M Staging of Non-small Cell Lung Cancer (continued) Level of Evidence Refs PET is more accurate in overall M staging than conventional staging methods. II (O) 76,77,78 SMALL CELL LUNG CANCER (SCLC) Small cell lung cancer (SCLC) comprises 15 25% of all lung cancers. It is distinguished from NSCLC by a rapid tumour doubling time and high growth fraction. Small cell lung cancer forms in the central airways in 80 90% of cases. At presentation up to 70% have already metastasised; most commonly to bone, liver, brain, bone marrow, retroperitoneal lymph nodes, soft tissue and adrenals. STAGING SYSTEM Accurate staging is important in SCLC because it guides treatment and helps to predict outcomes. However, the TNM staging system is not as useful for SCLC as with NSCLC because at presentation more than 90% of SCLC have either locally invasive mediastinal disease or metastases. Surgical management is rarely an option and therefore accurate intrathoracic staging is usually not required. In the few patients who do present with very localised SCLC and undergo surgical resection, the TNM staging system is prognostically important 83,84. The staging system used for the majority of SCLC divides them into limited disease and extensive disease at presentation (see Appendix 2). Limited disease essentially consists of tumour involving a single hemithorax and its regional lymph nodes, however, there are several controversial issues (see Appendix 2). Whilst all patients with SCLC are treated with combination chemotherapy, limited disease stage defines a group who have a better prognosis and who benefit from the routine addition of thoracic radiotherapy. STAGING PROCEDURES FOR SCLC Until recently full anatomical staging using several imaging modalities and bone marrow biopsy has been standard practice in Australia and the USA. In contrast, European groups have used clinical and blood markers along with limited imaging techniques to group patients into limited disease or extensive disease stages and to predict prognosis. There is now good evidence that the latter approach is at least as good at determining treatment groups and predicting outcome and it is substantially cheaper, less invasive and simpler. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 57
80 This more limited and targeted approach has now been advocated for routine use by a number of North American expert panels 10,85,86. It essentially consists of information from the clinical examination, a number of blood markers and a step-wise imaging approach to establish extensive disease or limited disease stage. Once a site of extensive disease is established further imaging is not required 87. Guideline Staging Small Cell Lung Cancer Level of Evidence Refs Once a metastatic site is identified, further anatomical staging at asymptomatic sites does not alter standard treatment or prediction of outcome but it does increase costs. II PROGNOSTIC FACTORS The literature related to prognostic factors in both NSCLC and SCLC is extensive, and a thorough review is beyond the scope of this document. The reader is referred to the UICC publication on prognostic factors 88 and a consensus statement 89 for a more comprehensive treatment of the subject and relevant bibliography. NON-SMALL CELL LUNG CANCER A consensus group of the International Association for the Study of Lung Cancer, after reviewing the literature, agreed that TNM stage; performance status; and weight loss are independent prognostic factors in patients with NSCLC. The group also listed a number of possible factors, these included sex; serum LDH and albumin; haemoglobin, white cell count and platelets; and age. Histology was thought to be a possible factor in patients with early stage squamous cell carcinoma, inasmuch as the recurrence rate for patients with T1N0 disease has been reported to be lower than that of patients with adenocarcinoma when both are treated by surgical resection 90. Although certain biologic and molecular markers show considerable promise as prognostic factors, it is not yet clear that any of these provides consistent additional information over and above what is available from stage, performance status and weight loss 91,92. The UICC s publication on prognostic factors divides them into three categories: disease related, patient related and environment related 93. It further recognises that there may be differences in the prognostic significance of some factors depending on disease extent and type of treatment Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
81 For NSCLC, essential prognostic factors are: tumour related stage hypercalcaemia superior vena caval obstruction patient related performance status weight loss environment related resection margin (for patients managed surgically) chemoradiotherapy for selected Stage III chemotherapy for selected Stage IV. Two studies have suggested that experience with administering treatment may also be an important environmental prognostic factor. The survival of patients was superior both for surgery 94 and chemoradiotherapy 95 in institutions with greater experience. Guideline Non-small Cell Lung Cancer Prognosis Level of Evidence Refs TNM stage, performance status and weight loss are independent prognostic factors in patients with non-small cell lung cancer, and should be documented at diagnosis in all patients. IV 88 SMALL CELL LUNG CANCER As with NSCLC, stage is an essential prognostic factor in SCLC, but is usually simplified as either limited or extensive. The definitions of these staging terms are not always consistent between institutions, as the distinction limited disease defined as that which can be encompassed within an acceptable radiotherapy field is dependent on subjective assessment by a radiation oncologist. There is a case to be made for a more objective staging system, perhaps a return to TNM, to better refine prognostic categories and guide treatment. Additional disease related factors include serum LDH and the presence of brain metastases 88. Performance status is an essential host related factor, with age, sex and weight loss as additional factors 88,96. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 59
82 Guideline Small Cell Lung Cancer Prognosis Level of Evidence Refs In patients with small cell lung cancer, stage (limited versus extensive) and performance status are essential prognostic factors, and should be documented at diagnosis in every case. IV FOLLOW-UP Follow-up of cancer patients, especially those who have been treated with curative intent, is a traditional practice often performed regardless of the efficacy of available salvage therapies. Assessment of response to treatment can provide prognostic information 97 and is important to the patient who may wish to plan for the future. Benefits attributed to ongoing follow-up of patients who have been treated for lung cancer include: recognition and treatment of toxicities; identification and treatment of second primary lung cancers or metastatic disease; and periodic reassurance for the patient if recurrent disease is not found. Accurate follow-up information is useful for clinical audit and research. However, there are costs involved, particularly if imaging or procedures such as bronchoscopy form part of the process (refer to p 200). A systematic review of follow-up of lung cancer patients who had been treated with curative intent could find no evidence of a patient benefit from the use of advanced imaging (CT or PET) or serum levels of tumour markers 98. Further, the authors found no evidence that any particular strategy led to a survival advantage. They recommended that patients be followed for three to six-monthly after curative therapy in order to detect and manage complications, and thereafter at six monthly intervals for two years and then annually. A reasonable assessment at each visit would consist of a history, physical examination and chest x-ray. Quality of life and patient satisfaction were assessed in a UK trial in which patients who had completed their initial anticancer treatment were randomised to follow-up by clinical nurse specialists in lung cancer or to routine two to three-monthly routine medical outpatient appointments 99. Patients randomised to nurse led follow-up rated their dyspnoea significantly less severe at three months compared with those receiving conventional medical follow up; they were less likely to have chest radiographs, and more likely to have radiotherapy. Patient satisfaction was consistently better on the nurse led follow-up arm. There was no difference in survival between the two arms. The role of the specialist lung cancer nurse in follow-up of lung cancer patients would seem to be worthy of research in the Australian setting. 60 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
83 Guideline Follow-up Level of Evidence Refs There is insufficient evidence to recommend any particular schedule of follow-up of patients after treatment for lung cancer. After the period of risk for treatment-related complications has elapsed, six monthly clinical assessments with a chest x-ray is reasonable. There is no evidence that higher levels of imaging (CT or PET), tumour markers or bronchoscopy in asymptomatic patients have any influence on outcome and their routine use in follow-up is not recommended. IV 98 References 1. Richardson GE, Thursfield VJ, Giles GG. Reported Management of Lung Cancer in Victoria in 1993: Comparison With Best Practice. Anti-Cancer Council of Victoria Lung Cancer Study Group. Med J Aust 2000; 172(7): Selby P, Gillis C, Haward R. Benefits From Specialised Cancer Care. Lancet 1996; 348(9023): Optimising Cancer Care in Australia Clinical Oncological Society of Australia, The Cancer Council Australia and National Cancer Control Initiative. 4. Siegelman SS, Zerhouni EA, Leo FP, Khouri NF, Stitik FP. CT of the Solitary Pulmonary Nodule. Am J Roentgenol 1980; 135(1): Francis DB, Zimmerman PV. Intrapulmonary Coin Lesions: the Changing Patterns. Med J Aust 1986; 144(3): Chute CG, Greenberg ER, Baron J, Korson R, Baker J, Yates J. Presenting Conditions of 1539 Population-Based Lung Cancer Patients by Cell Type and Stage in New Hampshire and Vermont. Cancer 1985; 56(8): Yankelevitz DF, Henschke CI. Does 2-Year Stability Imply That Pulmonary Nodules Are Benign? Am J Roentgenol 1997; 168(2): Gurney JW, Lyddon DM, McKay JA. Determining the Likelihood of Malignancy in Solitary Pulmonary Nodules With Bayesian Analysis. Part II. Application. Radiology 1993; 186(2): Zerhouni EA, Stitik FP, Siegelman SS, Naidich DP, Sagel SS, Proto AV, Muhm JR, Walsh JW, Martinez CR, Heelan RT,. CT of the Pulmonary Nodule: a Cooperative Study. Radiology 1986; 160(2): Patz EFJ. Imaging Bronchogenic Carcinoma. Chest 2000; 117(4 Suppl 1): 90S 5S. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 61
84 11. Henschke CI, McCauley DI, Yankelevitz DF, Naidich DP, McGuinness G, Miettinen OS, Libby DM, Pasmantier MW, Koizumi J, Altorki NK, Smith JP. Early Lung Cancer Action Project: Overall Design and Findings From Baseline Screening. Lancet 1999; 354(9173): Kubota K, Matsuzawa T, Fujiwara T, Ito M, Hatazawa J, Ishiwata K, Iwata R, Ido T. Differential Diagnosis of Lung Tumor With Positron Emission Tomography: a Prospective Study. J Nucl Med 1990; 31(12): Lowe VJ, Fletcher JW, Gobar L, Lawson M, Kirchner P, Valk P, Karis J, Hubner K, Delbeke D, Heiberg EV, Patz EF, Coleman RE. Prospective Investigation of Positron Emission Tomography in Lung Nodules. J Clin Oncol 1998; 16(3): Patel AM, Peters SG. Clinical Manifestations of Lung Cancer. Mayo Clin Proc 1993; 68(3): Risse EK, Vooijs GP, van t Hof MA. Relationship Between the Cellular Composition of Sputum and the Cytologic Diagnosis of Lung Cancer. Acta Cytol 1987; 31(2): Khajotia RR, Mohn A, Pokieser L, Schalleschak J, Vetter N. Induced Sputum and Cytological Diagnosis of Lung Cancer. Lancet 1991; 19;338(8773): Rizzo T, Schumann GB, Riding JM. Comparison of the Pick-and-Smear and Saccomanno Methods for Sputum Cytologic Analysis. Acta Cytol 1990; 34(6): Tockman MS, Mulshine JL. Sputum Screening by Quantitative Microscopy: a New Dawn for Detection of Lung Cancer? Mayo Clin Proc 1997; 72(8): Bonfiglio TA. Fine Needle Aspiration Biopsy of the Lung. Pathol Annu 1981; 16 Pt 1: Barbazza R, Toniolo L, Pinarello A, Scapinello A, Falconieri G, Di Bonito L. Accuracy of Bronchial Aspiration Cytology in Typing Operable (Stage I II) Pulmonary Carcinomas. Diagn Cytopathol 1992; 8(1): Mitruka S, Landreneau RJ, Mack MJ, Fetterman LS, Gammie J, Bartley S, Sutherland SR, Bowers CM, Keenan RJ, Ferson PF,. Diagnosing the Indeterminate Pulmonary Nodule: Percutaneous Biopsy Versus Thoracoscopy. Surgery 1995; 118(4): Rio F, Lobato S, Pino J, et al. Value of CT-Guided Fine Needle Aspiration in Solitary Pulmonary Nodules With Negative Fibreoptic Bronchoscope. Acta Radiol 1994; 35: Cortese DA, McDougall JC. Biopsy and Brushing of Peripheral Lung Cancer With Fluoroscopic Guidance. Chest 1979; 75(2): Ellis JH, Jr. Transbronchial Lung Biopsy Via the Fiberoptic Bronchoscope. Experience With 107 Consecutive Cases and Comparison With Bronchial Brushing. Chest 1975; 68(4): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
85 25. Hanson RR, Zavala DC, Rhodes ML, Keim LW, Smith JD. Transbronchial Biopsy Via Flexible Fiberoptic Bronchoscope; Results in 164 Patients. Am Rev Respir Dis 1976; 114(1): Shure D, Astarita RW. Bronchogenic Carcinoma Presenting As an Endobronchial Mass. Chest 1983; 83(6): Shure D, Fedullo PF. Transbronchial Needle Aspiration in the Diagnosis of Submucosal and Peribronchial Bronchogenic Carcinoma. Chest 1985; 88(1): Mazzone P, Jain P, Arroliga AC, Matthay RA. Bronchoscopy and Needle Biopsy Techniques for Diagnosis and Staging of Lung Cancer. Clin Chest Med 2002; 23(1): , ix. 29. Wang KP, Marsh BR, Summer WR, Terry PB, Erozan YS, Baker RR. Transbronchial Needle Aspiration for Diagnosis of Lung Cancer. Chest 1981; 80(1): Shiner RJ, Rosenman J, Katz I, Reichart N, Hershko E, Yellin A. Bronchoscopic Evaluation of Peripheral Lung Tumours. Thorax 1988; 43(11): Prauer HW, Weber WA, Romer W, Treumann T, Ziegler SI, Schwaiger M. Controlled Prospective Study of Positron Emission Tomography Using the Glucose Analogue [18f]Fluorodeoxyglucose in the Evaluation of Pulmonary Nodules. Br J Surg 1998; 85(11): Gupta NC, Maloof J, Gunel E. Probability of Malignancy in Solitary Pulmonary Nodules Using Fluorine-18-FDG and PET. J Nucl Med 1996; 37(6): Gould MK, Maclean CC, Kuschner WG, Rydzak CE, Owens DK. Accuracy of Positron Emission Tomography for Diagnosis of Pulmonary Nodules and Mass Lesions: a Meta-Analysis. JAMA 2001; 285(7): Pitman AG, Hicks RJ, Kalff V, Binns DS, Ware RE, McKenzie AF, Ball DL, MacManus MP. Positron Emission Tomography in Pulmonary Masses Where Tissue Diagnosis Is Unhelpful or Not Possible. Med J Aust 2001; 175(6): Dewan NA, Reeb SD, Gupta NC, Gobar LS, Scott WJ. PET-FDG Imaging and Transthoracic Needle Lung Aspiration Biopsy in Evaluation of Pulmonary Lesions. A Comparative Risk-Benefit Analysis. Chest 1995; 108(2): Bomanji JB, Costa DC, Ell PJ. Clinical Role of Positron Emission Tomography in Oncology. Lancet Oncol 2001; 2(3): Templeton PA, Caskey CI, Zerhouni EA. Current Uses of CT and MR Imaging in the Staging of Lung Cancer. Radiol Clin North Am 1990; 28(3): Epstein DM, Stephenson LW, Gefter WB, van der Voorde F, Aronchik JM, Miller WT. Value of CT in the Preoperative Assessment of Lung Cancer: a Survey of Thoracic Surgeons. Radiology 1986; 161(2): Quint LE, Francis IR, Wahl RL, Gross BH, Glazer GM. Preoperative Staging of Non-Small-Cell Carcinoma of the Lung: Imaging Methods. Am J Roentgenol 1995; 164(6): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 63
86 40. Klein JS, Webb WR. The Radiologic Staging of Lung Cancer. J Thorac Imaging 1991; 7(1): Webb WR, Gatsonis C, Zerhouni EA, Heelan RT, Glazer GM, Francis IR, McNeil BJ. CT and MR Imaging in Staging Non-Small Cell Bronchogenic Carcinoma: Report of the Radiologic Diagnostic Oncology Group. Radiology 1991; 178(3): Webb WR, Sostman HD. MR Imaging of Thoracic Disease: Clinical Uses. Radiology 1992; 182(3): Rapoport S, Blair DN, McCarthy SM, Desser TS, Hammers LW, Sostman HD. Brachial Plexus: Correlation of MR Imaging With CT and Pathologic Findings. Radiology 1988; 167(1): Padovani B, Mouroux J, Seksik L, Chanalet S, Sedat J, Rotomondo C, Richelme H, Serres JJ. Chest Wall Invasion by Bronchogenic Carcinoma: Evaluation With MR Imaging. Radiology 1993; 187(1): Martini N, Heelan R, Westcott J, Bains MS, McCormack P, Caravelli J, Watson R, Zaman M. Comparative Merits of Conventional, Computed Tomographic, and Magnetic Resonance Imaging in Assessing Mediastinal Involvement in Surgically Confirmed Lung Carcinoma. J Thorac Cardiovasc Surg 1985; 90(5): McLoud TC. CT of Bronchogenic Carcinoma: Indeterminate Mediastinal Invasion. Radiology 1989; 173(1): Webb WR, Jensen BG, Sollitto R, de Geer G, McCowin M, Gamsu G, Moore E. Bronchogenic Carcinoma: Staging With MR Compared With Staging With CT and Surgery. Radiology 1985; 156(1): Hicks RJ, Kalff V, MacManus MP, Ware RE, Hogg A, McKenzie AF, Matthews JP, Ball DL. (18)F-FDG PET Provides High-Impact and Powerful Prognostic Stratification in Staging Newly Diagnosed Non-Small Cell Lung Cancer. J Nucl Med 2001; 42(11): Glazer GM, Gross BH, Quint LE, Francis IR, Bookstein FL, Orringer MB. Normal Mediastinal Lymph Nodes: Number and Size According to American Thoracic Society Mapping. Am J Roentgenol 1985; 144(2): McLoud TC, Bourgouin PM, Greenberg RW, Kosiuk JP, Templeton PA, Shepard JA, Moore EH, Wain JC, Mathisen DJ, Grillo HC. Bronchogenic Carcinoma: Analysis of Staging in the Mediastinum With CT by Correlative Lymph Node Mapping and Sampling. Radiology 1992; 182(2): Dwamena BA, Sonnad SS, Angobaldo JO, Wahl RL. Metastases From Non-Small Cell Lung Cancer: Mediastinal Staging in the 1990s-Meta-Analytic Comparison of PET and CT. Radiology 1999; 213(2): Scott WJ, Gobar LS, Terry JD, Dewan NA, Sunderland JJ. Mediastinal Lymph Node Staging of Non-Small-Cell Lung Cancer: a Prospective Comparison of Computed Tomography and Positron Emission Tomography. J Thorac Cardiovasc Surg 1996; 111(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
87 53. Lewis JW, Jr., Pearlberg JL, Beute GH, Alpern M, Kvale PA, Gross BH, Magilligan DJ, Jr. Can Computed Tomography of the Chest Stage Lung Cancer? Yes and No. Ann Thorac Surg 1990; 49(4): Valk PE, Pounds TR, Hopkins DM, Haseman MK, Hofer GA, Greiss HB, Myers RW, Lutrin CL. Staging Non-Small Cell Lung Cancer by Whole-Body Positron Emission Tomographic Imaging. Ann Thorac Surg 1995; 60(6): Goldstraw P. The Practice of Cardiothoracic Surgeons in the Perioperative Staging of Non-Small Cell Lung Cancer. Thorax 1992; 47(1): Coleman RE. PET in Lung Cancer. J Nucl Med 1999; 40(5): Marom EM, McAdams HP, Erasmus JJ, Goodman PC, Culhane DK, Coleman RE, Herndon JE, Patz EFJ. Staging Non-Small Cell Lung Cancer With Whole-Body PET. Radiology 1999; 212(3): Steinert HC, Hauser M, Allemann F, Engel H, Berthold T, von Schulthess GK, Weder W. Non-Small Cell Lung Cancer: Nodal Staging With FDG PET Versus CT With Correlative Lymph Node Mapping and Sampling. Radiology 1997; 202(2): Wahl RL, Quint LE, Greenough RL, Meyer CR, White RI, Orringer MB. Staging of Mediastinal Non-Small Cell Lung Cancer With FDG PET, CT, and Fusion Images: Preliminary Prospective Evaluation. Radiology 1994; 191(2): Pieterman RM, van Putten JW, Meuzelaar JJ, Mooyaart EL, Vaalburg W, Koeter GH, Fidler V, Pruim J, Groen HJ. Preoperative Staging of Non-Small-Cell Lung Cancer With Positron-Emission Tomography. N Engl J Med 2000; 343(4): Kalff V, Hicks RJ, MacManus MP, Binns DS, McKenzie AF, Ware RE, Hogg A, Ball DL. Clinical Impact of (18)F Fluorodeoxyglucose Positron Emission Tomography in Patients With Non-Small-Cell Lung Cancer: a Prospective Study. J Clin Oncol 2001; 19(1): Berlangieri SU, Scott AM, Knight SR, Fitt GJ, Hennessy OF, Tochon-Danguy HJ, Clarke CP, McKay WJ. F 18 Fluorodeoxyglucose Positron Emission Tomography in the Non-Invasive Staging of Non-Small Cell Lung Cancer. Eur J Cardiothorac Surg 1999; 16 Suppl 1: S25 S Quint LE, Tummala S, Brisson LJ, Francis IR, Krupnick AS, Kazerooni EA, Iannettoni MD, Whyte RI, Orringer MB. Distribution of Distant Metastases From Newly Diagnosed Non-Small Cell Lung Cancer. Ann Thorac Surg 1996; 62(1): Salvatierra A, Baamonde C, Llamas JM, Cruz F, Lopez-Pujol J. Extrathoracic Staging of Bronchogenic Carcinoma. Chest 1990; 97(5): Sider L, Horejs D. Frequency of Extrathoracic Metastases From Bronchogenic Carcinoma in Patients With Normal-Sized Hilar and Mediastinal Lymph Nodes on CT. Am J Roentgenol 1988; 151(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 65
88 66. Matthews MJ, Kanhouwa S, Pickren J, Robinette D. Frequency of Residual and Metastatic Tumor in Patients Undergoing Curative Surgical Resection for Lung Cancer. Cancer Chemother Rep ; 4(2): MacManus MP, Hicks RJ, Matthews JP, Hogg A, McKenzie AF, Wirth A, Ware RE, Ball DL. High Rate of Detection of Unsuspected Distant Metastases by pet in Apparent Stage III Non-Small-Cell Lung Cancer: Implications for Radical Radiation Therapy. Int J Radiat Oncol Biol Phys 2001; 50(2): Saunders CA, Dussek JE, O Doherty MJ, Maisey MN. Evaluation of Fluorine-18- Fluorodeoxyglucose Whole Body Positron Emission Tomography Imaging in the Staging of Lung Cancer. Ann Thorac Surg 1999; 67(3): Little AG, Stitik FP. Clinical Staging of Patients With Non-Small Cell Lung Cancer. Chest 1990; 97(6): Stitik FP. Staging of Lung Cancer. Radiol Clin North Am 1990; 28(3): Oliver TWJ, Bernardino ME, Miller JI, Mansour K, Greene D, Davis WA. Isolated Adrenal Masses in Nonsmall-Cell Bronchogenic Carcinoma. Radiology 1984; 153(1): Mayo-Smith WW, Boland GW, Noto RB, Lee MJ. State-of-the-Art Adrenal Imaging. Radiographics 2001; 21(4): Korobkin M. CT Characterization of Adrenal Masses: the Time Has Come. Radiology 2000; 217(3): Mintz BJ, Tuhrim S, Alexander S, Yang WC, Shanzer S. Intracranial Metastases in the Initial Staging of Bronchogenic Carcinoma. Chest 1984; 86(6): Silvestri GA, Littenberg B, Colice GL. The Clinical Evaluation for Detecting Metastatic Lung Cancer. A Meta-Analysis. Am J Respir Crit Care Med 1995; 152(1): Erasmus JJ, Patz EFJ, McAdams HP, Murray JG, Herndon J, Coleman RE, Goodman PC. Evaluation of Adrenal Masses in Patients With Bronchogenic Carcinoma Using 18F-Fluorodeoxyglucose Positron Emission Tomography. Am J Roentgenol 1997; 168(5): Boland GW, Goldberg MA, Lee MJ, Mayo-Smith WW, Dixon J, McNicholas MM, Mueller PR. Indeterminate Adrenal Mass in Patients With Cancer: Evaluation at PET With 2-[F-18]-Fluoro-2-Deoxy-D-Glucose. Radiology 1995; 194(1): Bury T, Dowlati A, Paulus P, Corhay JL, Hustinx R, Ghaye B, Radermecker M, Rigo P. Whole-Body 18FDG Positron Emission Tomography in the Staging of Non-Small Cell Lung Cancer. Eur Respir J 1997; 10(11): Weder W, Schmid RA, Bruchhaus H, Hillinger S, von Schulthess GK, Steinert HC. Detection of Extrathoracic Metastases by Positron Emission Tomography in Lung Cancer. Ann Thorac Surg 1998; 66(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
89 80. Gambhir SS, Hoh CK, Phelps ME, Madar I, Maddahi J. Decision Tree Sensitivity Analysis for Cost-Effectiveness of FDG-PET in the Staging and Management of Non-Small-Cell Lung Carcinoma. J Nucl Med 1996; 37(9): Dietlein M, Weber K, Gandjour A, Moka D, Theissen P, Lauterbach KW, Schicha H. Cost-Effectiveness of FDG-PET for the Management of Potentially Operable Non- Small Cell Lung Cancer: Priority for a PET-Based Strategy After Nodal-Negative CT Results. Eur J Nucl Med 2000; 27(11): MacManus MP, Hicks RJ, Ball DL, Kalff V, Matthews JP, Salminen E, Khaw P, Wirth A, Rischin D, McKenzie A. F 18 Fluorodeoxyglucose Positron Emission Tomography Staging in Radical Radiotherapy Candidates With Nonsmall Cell Lung Carcinoma: Powerful Correlation With Survival and High Impact on Treatment. Cancer 2001; 92(4): Shepherd FA, Ginsberg R, et al. Staging and Prognostic Factors in Small-Cell Lung Cancer. Lung Cancer 1989; 5(119). 84. Karrer K, Shields TW, Denck H, Hrabar B, Vogt-Moykopf I, Salzer GM. The Importance of Surgical and Multimodality Treatment for Small Cell Bronchial Carcinoma. J Thorac Cardiovasc Surg 1989; 97(2): Darling GE. Staging of the Patient With Small Cell Lung Cancer. Chest Surg Clin N Am 1997; 7(1): Feld R, Sagwan U LBM. Staging and prognostic factors for small cell lung cancer. Pass HI, Mitchell JB, Johnson D.H., Turrisi AT, Minna J.D. (eds) Lung Cancer - Principles and Practice (2nd edn).lippincott Williams and Wilkins, Richardson GE, Venzon DJ, Edison M, Brown M, Frame JN, Ihde DC, Johnson BE. Application of an Algorithm for Staging Small-Cell Lung Cancer Can Save One Third of the Initial Evaluation Costs. Arch Intern Med 1993; 153(3): Brundage M, Mackillop W. Lung Cancer. Gospodarowicz MK, Henson DE, Hutter RVP, O Sullivan B, Sobin LH, Wittekind C (eds) Prognostic Factors in Cancer (2nd edn). New York: Wiley-Liss, 2001: Feld R, Abratt R, Graziano S, Jassem J, Lacquet L, Ninane V, Paesmans M, Rocmans P, Schiepers C, Stahel R, Stephens R. Pretreatment Minimal Staging and Prognostic Factors for Non-Small Cell Lung Cancer. Lung Cancer 1997; 17 Suppl 1:S Postoperative T1 N0 Non-Small Cell Lung Cancer. Squamous Versus Non-Squamous Recurrences. The Lung Cancer Study Group. J Thorac Cardiovasc Surg 1987; 94(3): Strauss GM, Kwiatkowski DJ, Harpole DH, Lynch TJ, Skarin AT, Sugarbaker DJ. Molecular and Pathologic Markers in Stage I Non-Small-Cell Carcinoma of the Lung. J Clin Oncol 1995; 13(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 67
90 92. Graziano SL. Non-Small Cell Lung Cancer: Clinical Value of New Biological Predictors. Lung Cancer 1997; 17 Suppl 1:S Gospodarowicz MK, O Sullivan B. Prognostic factors: principles and application. Gospodarowicz MK, Henson DE, Hutter RVP, O Sullivan B, Sobin LH, Wittekind C (eds) Prognostic Factors in Cancer (2nd edn). New York: Wiley-Liss, 2001: Bach PB, Cramer LD, Schrag D, Downey RJ, Gelfand SE, Begg CB. The Influence of Hospital Volume on Survival After Resection for Lung Cancer. N Engl J Med 2001; 19;345(3): Lee JS, Scott CB, Komaki R, Ettinger DS, Sause WT. Impact of Institutional Experience on Survival Outcome of Patients Undergoing Combined Chemoradiation Therapy for Inoperable Non-Small-Cell Lung Cancer. Int J Radiat Oncol Biol Phys 2002; 52(2): Feld R, Sagman U, Le Blanc M. Staging and prognostic factors for small cell lung cancer. Pass HI, Mitchell JB, Johnson D.H., Turrisi AT, Minna J.D. (eds) Lung Cancer: principles and practice (2nd edn). Philadelphia: Lippincott Williams and Wilkins, 2000: Mac Manus MP, Hicks RJ, Matthews JP, McKenzie A, Rischin D, Salminen EK, Ball DL. Positron Emission Tomography Is Superior to Computed Tomography Scanning for Response-Assessment After Radical Radiotherapy or Chemoradiotherapy in Patients With Non-Small-Cell Lung Cancer. J Clin Oncol 2003; 21(7): Colice GL, Rubins J, Unger M. Follow-Up and Surveillance of the Lung Cancer Patient Following Curative-Intent Therapy. Chest 2003; 123(1 Suppl): 272S 83S. 99. Moore S, Corner J, Haviland J, Wells M, Salmon E, Normand C, Brada M, O Brien M, Smith I. Nurse Led Follow Up and Conventional Medical Follow Up in Management of Patients With Lung Cancer: Randomised Trial. BMJ 2002; 325(7373): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
91 SECTION III PATIENT SUPPORT AND DEFINITIVE TREATMENT 4. SUPPORTING THE PATIENT DURING DIAGNOSIS AND TREATMENT 4.1 Information provision 4.2 Prevalence of anxiety, depression and distress 4.3 Quality of life 4.4 Counselling, support and psychological treatments Social support Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 69
92
93 4.1 INFORMATION PROVISION The diagnosis and treatment of lung cancer is a major stressful life event for every individual afflicted and requires an adaptive adjustment to sustain quality of life. Attention to information provision and communication with the patient, to their psychological adaptation and their social needs are fundamental dimensions of care that will enhance their quality of life while striving to prolong survival. Consumer satisfaction surveys of patients with cancer repeatedly identify information provision as a major source of unmet needs 1. A meta-analysis of educational interventions in cancer has shown that the provision of adequate information is related to increased psychological wellbeing 2. Effective communication skills ensure that this information is clearly explained and understood 3,4. Studies have shown that only part of the initial consultation is remembered 5. Therefore clinicians need to recognise that the integration of information is a gradual process that requires both time and the opportunity to ask questions at subsequent visits. It is not necessary to make treatment decisions at the initial consultation unless the patient clearly chooses to do so. For non-english patients, professional interpreter services should be used and use of family members as interpreters avoided. When breaking bad news, two points are particularly important: firstly, care should be taken to deliver the information in language that the patient understands and secondly, appropriate support, including the attendance of significant others, if desired by the patient, should be provided. Tape recording of such sessions should be routinely offered 6. The NHMRC recommends the following approach for breaking bad news, adapted from The Cancer Council New South Wales 1 : give bad news in a quiet, private place allow enough uninterrupted time in the initial meeting assess the individual s understanding provide information simply and honestly encourage individuals to express their feelings respond to individual s feelings with empathy give a broad time-frame for the prognosis avoid the notion that nothing can be done arrange a time to review the situation discuss treatment options offer assistance to tell others provide information about support services provide written information offer a tape recording of the session. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 71
94 In our society, most patients wish to be fully informed of all available information, and usually want a close relative or friend present during this interview 7. In general, cancer patients should be invited to guide the clinician about the level of detail they wish to receive and their desire for active involvement in decision making 8. Discussion of the actions that can be taken and what the diagnosis means, are at least, if not more, important than the disclosure of the initial diagnosis 9. The clinician s choice of words is critical, as being deliberately vague or using euphemisms can significantly impair communication 10. Clinicians should review both the patient s understanding of what they have been told and their reaction to this news, as a means of increasing integration of this information and providing emotional support. Patients are entitled to make their own decisions about treatments or procedures, but need adequate information on which to base these decisions. One study of patients with lung cancer found that 29% perceived a discrepancy between their desired role in decision making and their actual role 11. Nearly two thirds sought an active, collaborative decision making style 11. Clinicians should provide information in a form and manner that helps the patient to understand the treatment options available, and which is tailored to the patient s circumstances, personality, level of education and understanding, expectations, fears, beliefs, values and cultural background 12. In regard to prognosis, a study of patients with metastatic incurable cancer revealed that the information most sought by patients included longest survival time with treatment, five-year survival rates, and average survival. Words and numbers were preferred to graphs 13. There can be difficulty in comparing results between studies as the outcome may be reported in different ways. For instance survival outcomes can be reported as a percentage of survival at a particular time point, for example, one-year or five-year survival rates, median survival, survival curves, or hazard ratios. Each of these provides different information, and discussion of prognosis may require all of these factors to be discussed in an easily comprehensible fashion that is applicable to the individual. Guidelines Informing the Patient Level of Evidence Refs Patients should be provided with adequate information, as this is associated with enhanced patient psychological wellbeing. Clinicians should follow the NHMRC recommended guidelines on the breaking of bad news, providing information about treatments and the discussion of prognosis. III 3 2 IV 1 72 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
95 4.2 PREVALENCE OF ANXIETY, DEPRESSION AND DISTRESS Studies screening patients with lung cancer for evidence of psychological distress have reported rates between 15% 14 and 25% 15. As the disease becomes more advanced, these rates climb as high as 69% 16. Studies specifically seeking to identify anxiety disorders have recorded rates between 13% and 50% 17,18,19, while those delineating depressive disorders have identified rates between 9% and 36% 17,18,20,21,22. In an important study conducted by the British Medical Research Council Lung Cancer Working Party, depression was identified in 33% of patients (n=322) before treatment and persisted in more than 50% of patients following treatment. Small cell lung cancer patients had a three-fold higher prevalence of depression than NSCLC patients 22. In an Australian study of patients with advanced cancer in the palliative care setting, up to half of the patients, one third of their spouses and one quarter of their offspring showed evidence of substantial psychological distress warranting specific support 23. The distress reverberates through the family in this setting, such that both patient- and family- centred models of care need to be utilised. Predictors of anxiety and depressive disorders in patients with lung cancer include poor performance status 22,24, poorly treated pain 16, female gender 22,25 (especially with early stage disease), living alone, lacking confidants and having a hopeless/helpless coping attitude 25. Pretreatment physical symptom burden, fatigue and physician-rated performance status were also independent predictors of depression, but histological subtype was not 22. Meta-analyses to evaluate the efficacy of treatment of anxiety and depressive disorders in patients with cancer have demonstrated the importance of recognition and treatment of these medical problems 2,26,27. Trials of antidepressants in cancer populations show the same level of efficacy as that seen in the treatment of depression in non-cancer populations 28,29. Guideline Psychosocial Care in Lung Cancer Level of Evidence Refs It is critical to recognise distress, anxiety and depressive disorders in patients with lung cancer as treatment with combined pharmacotherapy (antidepressants) and psychotherapy is efficacious. I 2,26,27 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 73
96 4.3 QUALITY OF LIFE Examination of symptoms at presentation and during treatment for lung cancer show the pattern to be virtually the same for patients with SCLC and NSCLC 30. Prominent symptoms that affect quality of life include disease-related chest symptoms (shortness of breath, cough and pain); constitutional symptoms (fatigue, anorexia); and psychological concerns (insomnia, decreased libido, worry) 18,30. In addition, prophylactic cranial irradiation is associated with a transient increase in sickness and vomiting 31. Studies have varied in their conclusion as to the effect of chemotherapy on quality of life. One study in SCLC showed a diminishing of quality of life with continuing chemotherapy for regimens such as cyclophosphamide/vincristine/etoposide (level II evidence), and this burden of treatment needs to be balanced against tumour response 31. However, several studies comparing chemotherapy with best supportive care in advanced NSCLC have shown maintenance or improvement in measures of quality of life 32,33,34. The routine use of computerised quality of life screening using typical scales such as the European Organization for Research and Treatment of Cancer (EORTC) QLQ C30 has not been shown to improve outcome in patient wellbeing or satisfaction with care in patients with lung cancer 35. This contrasts with screening for depression or distress, which does generate a significant clinical improvement 36. Guideline Quality of Life in Lung Cancer Level of Evidence Refs The potential impact of treatment on quality of life in patients with lung cancer should be included in discussions of treatment alternatives. II 18,30,31, 32,33, COUNSELLING, SUPPORT AND PSYCHOLOGICAL TREATMENTS A range of psychological therapies is available to assist in enhancing coping and relieving distress in patients with lung cancer. These interventions can be delivered individually or via group or family approaches, and follow well described models of psychotherapy including the supportive-expressive, cognitive-behavioural, interpersonal, existential and psychodynamic schools of psychotherapy. They enhance emotional adjustment (sense of control, self esteem, living with uncertainty, fear of death, complicated grief and depression); improve functional status (activities of daily living, social and role functioning, vocational activities); improve knowledge of lung cancer and its treatment; improve treatment- and disease-related symptoms (for example, nausea, vomiting, pain etc); and increase overall quality of life. Meta-analyses have confirmed the benefits of these psychological treatments in various cancers 2,26, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
97 Relaxation-based therapies provide benefits by reducing anxiety, treatment-related phobias such as needle phobia, conditioned nausea and vomiting, and insomnias 2. Existential distress, which finds expression in fear of the reality or process of dying, essential aloneness, meaninglessness and unrealistic fears about the processes of treatment, can be ameliorated with supportive-expressive or cognitive-behavioural therapies. Furthermore, compliance with medical therapies can be improved. Early referral for specialist support from a clinical psychologist or consultation-liaison psychiatrist is worthwhile when symptoms of distress or high risk for psychiatric morbidity become evident. Randomised controlled trials of early versus late referral to palliative care services show strong evidence of the benefits of early referral in reducing time spent in hospital, enhancing symptom control, increasing family satisfaction and permitting death to occur in the desired location 37,38,39. Early referral to community-based domiciliary palliative care services, where available, may have several benefits and enhance quality of life 40. Guideline Psychosocial and Supportive Services in Quality of Life in Cancer Psychological interventions and early referral to psycho-oncology and palliative care services improves quality of life in patients with cancer. Level of Evidence I II Refs 2,26,27 38,39 SOCIAL SUPPORT A number of people involved in the patient s care may be involved in providing support in either a formal or informal manner. These can include family, friends, doctors, nurses, and other health care professionals, and together form the treatment team. Co-ordination and continuity of care ensure high quality treatment for patients with lung cancer. The choice of the person to co-ordinate this care should be made by the patient in conjunction with their general practitioner and specialists. This co-ordinator need not necessarily be a health professional. Assistance with transport, care of children or other family members, home support, respite care and volunteer assistance are some of the many means of social support. State and Territory Cancer Councils provide support through a telephone help line (the national telephone contact number for all such services is ). Professional guidance or the support of volunteers is available through such services, together with information about local community self-help groups and related services. Regional Cancer Councils offer a range of educational pamphlets to assist patients and their families. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 75
98 In summary, the social support needs for patients with lung cancer and their families include: access to cancer support services and community self-help groups information about community social support resources assistance with transport, child care, home help guidance about financial and disability support. References 1. Girgis A, Sanson-Fisher R. How to break bad news: Interactional skills training manual for general practitioners, junior medial officers, nurses and surgeons Sydney, New South Wales Cancer Council. 2. Devine EC, Westlake SK. The Effects of Psychoeducational Care Provided to Adults With Cancer: Meta-Analysis of 116 Studies. Oncol Nurs Forum 1995; 22(9): Fallowfield LJ, Hall A, Maguire GP, Baum M. Psychological Outcomes of Different Treatment Policies in Women With Early Breast Cancer Outside a Clinical Trial. BMJ 1990; 301(6752): Roberts CS, Cox CE, Reintgen DS, Baile WF, Gibertini M. Influence of Physician Communication on Newly Diagnosed Breast Patients Psychologic Adjustment and Decision-Making. Cancer 1994; 74(1 Suppl): Dunn SM, Butow PN, Tattersall MH, Jones QJ, Sheldon JS, Taylor JJ, Sumich MD. General Information Tapes Inhibit Recall of the Cancer Consultation. J Clin Oncol 1993; 11(11): Scott TJ, Entwhistle VA, Sowden AJ, Watt I. Recordings or summaries of consultations for people with cancer. In the Cochrane Library, Issue Butow PN, Kazemi JN, Beeney LJ, Griffin AM, Dunn SM, Tattersall MH. When the Diagnosis Is Cancer: Patient Communication Experiences and Preferences. Cancer 1996; 77(12): Degner LF, Kristjanson LJ, Bowman D, Sloan JA, Carriere KC, O Neil J, Bilodeau B, Watson P, Mueller B. Information Needs and Decisional Preferences in Women With Breast Cancer. JAMA 1997; 277(18): Lind SE, DelVecchio GM, Seidel S, Csordas T, Good BJ. Telling the Diagnosis of Cancer. J Clin Oncol 1989; 7(5): Dunn SM, Patterson PU, Butow PN, Smartt HH, McCarthy WH, Tattersall MH. Cancer by Another Name: a Randomized Trial of the Effects of Euphemism and Uncertainty in Communicating With Cancer Patients. J Clin Oncol 1993; 11(5): Davidson JR, Brundage MD, Feldman-Stewart D. Lung Cancer Treatment Decisions: Patients Desires for Participation and Information. Psychooncology 1999; 8(6): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
99 12. NHMRC General guidelines for medical practitioners on providing information to patients Canberra, AGPS. 13. Hagerty RG, Butow P, Tattersall MHN, Ellis PE, Pendlebury S, Lobb EA. Discussing prognosis and treatment goals with patient with metastatic cancer: evidencebased strategies. Proceedings of the 29th Annual Scientific Meeting of the Clinical Oncological Society of Australia Ginsburg ML, Quirt C, Ginsburg AD, MacKillop WJ. Psychiatric Illness and Psychosocial Concerns of Patients With Newly Diagnosed Lung Cancer. CMAJ 1995; 152(5): Bergman B, Sullivan M, Sorenson S. Quality of Life During Chemotherapy for Small Cell Lung Cancer. I. An Evaluation With Generic Health Measures. Acta Oncol 1991; 30(8): Kaasa S, Malt U, Hagen S, Wist E, Moum T, Kvikstad A. Psychological Distress in Cancer Patients With Advanced Disease. Radiother Oncol 1993; 27(3): Aass N, Fossa SD, Dahl AA, Moe TJ. Prevalence of Anxiety and Depression in Cancer Patients Seen at the Norwegian Radium Hospital. Eur J Cancer 1997; 33(10): Bailey AJ, Parmar MK, Stephens RJ. Patient-Reported Short-Term and Long-Term Physical and Psychologic Symptoms: Results of the Continuous Hyperfractionated Accelerated Radiotherapy (CHART) Randomized Trial in Non-Small-Cell Lung Cancer. CHART Steering Committee. J Clin Oncol 1998; 16(9): Hyodo I, Eguchi K, Takigawa N, Segawa Y, Hosokawa Y, Kamejima K, Inoue R. Psychological Impact of Informed Consent in Hospitalized Cancer Patients. A Sequential Study of Anxiety and Depression Using the Hospital Anxiety and Depression Scale. Support Care Cancer 1999; 7(6): Hughes JE. Depressive Illness and Lung Cancer. II. Follow-Up of Inoperable Patients. Eur J Surg Oncol 1985; 11(1): Hopwood P, Thatcher N. Preliminary Experience With Quality of Life Evaluation in Patients With Lung Cancer. Oncology (Huntingt) 1990; 4(5): Hopwood P, Stephens RJ. Depression in Patients With Lung Cancer: Prevalence and Risk Factors Derived From Quality-of-Life Data. J Clin Oncol 2000; 18(4): Kissane D, Burns W, et al. Psychological Morbidity in the Families of Patients With Cancer. Psychooncology 1994; 3: Cella DF, Orofiamma B, Holland JC, Silberfarb PM, Tross S, Feldstein M, Perry M, Maurer LH, Comis R, Orav EJ. The Relationship of Psychological Distress, Extent of Disease, and Performance Status in Patients With Lung Cancer. Cancer 1987; 60(7): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 77
100 25. Akechi T, Kugaya A, Okamura H, Nishiwaki Y, Yamawaki S, Uchitomi Y. Predictive Factors for Psychological Distress in Ambulatory Lung Cancer Patients. Support Care Cancer 1998; 6(3): Meyer TJ, Mark MM. Effects of Psychosocial Interventions With Adult Cancer Patients: a Meta-Analysis of Randomized Experiments. Health Psychol 1995; 14(2): Sheard T, Maguire P. The Effect of Psychological Interventions on Anxiety and Depression in Oncology: Results of Two Meta-Analyses. Psychooncology 2001; 5(3S): Bruera E, Neumann CM. The Uses of Psychotropics in Symptom Management in Advanced Cancer. Psychooncology 1998; 7(4): Breitbart W. Psychotropic Adjuvant Analgesics for Pain in Cancer and AIDS. Psychooncology 1998; 7(4): Hopwood P, Stephens RJ. Symptoms at Presentation for Treatment in Patients With Lung Cancer: Implications for the Evaluation of Palliative Treatment. The Medical Research Council (MRC) Lung Cancer Working Party. Br J Cancer 1995; 71(3): Geddes DM, Dones L, Hill E, Law K, Harper PG, Spiro SG, Tobias JS, Souhami RL. Quality of Life During Chemotherapy for Small Cell Lung Cancer: Assessment and Use of a Daily Diary Card in a Randomized Trial. Eur J Cancer 1990; 26(4): Anderson H, Hopwood P, Stephens RJ, Thatcher N, Cottier B, Nicholson M, Milroy R, Maughan TS, Falk SJ, Bond MG, Burt PA, Connolly CK, McIllmurray MB, Carmichael J. Gemcitabine Plus Best Supportive Care (BSC) Vs BSC in Inoperable Non-Small Cell Lung Cancer-a Randomized Trial With Quality of Life As the Primary Outcome. UK NSCLC Gemcitabine Group. Non-Small Cell Lung Cancer. Br J Cancer 2000; 83(4): Roszkowski K, Pluzanska A, Krzakowski M, Smith AP, Saigi E, Aasebo U, Parisi A, Pham TN, Olivares R, Berille J. A Multicenter, Randomized, Phase III Study of Docetaxel Plus Best Supportive Care Versus Best Supportive Care in Chemotherapy- Naive Patients With Metastatic or Non-Resectable Localized Non-Small Cell Lung Cancer (NSCLC). Lung Cancer; 27(3): Effects of Vinorelbine on Quality of Life and Survival of Elderly Patients With Advanced Non-Small-Cell Lung Cancer. The Elderly Lung Cancer Vinorelbine Italian Study Group. 1999; 91(1): Taenzer P, Bultz BD, Carlson LE, Speca M, DeGagne T, Olson K, Doll R, Rosberger Z. Impact of Computerized Quality of Life Screening on Physician Behaviour and Patient Satisfaction in Lung Cancer Outpatients. Psychooncology 2000; 9(3): McLachlan S, Kissane DW. Use of touch-screen computerised screening of cancer outpatients in a needs assessment randomised trial. Journal of Clinical Oncology Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
101 37. McCusker J, Stoddard AM. Effects of an Expanding Home Care Program for the Terminally Ill. Med Care 1987; 25(5): Higginson IJ, Wade AM, McCarthy M. Effectiveness of Two Palliative Support Teams. J Public Health Med 1992; 14(1): Jones RV, Hansford J, Fiske J. Death From Cancer at Home: the Carers Perspective. BMJ 1993; 306(6872): Hinton J. Can Home Care Maintain an Acceptable Quality of Life for Patients With Terminal Cancer and Their Relatives? Palliat Med 1994; 8(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 79
102 5. NON-SMALL CELL LUNG CANCER 5.1 Management of non-small cell lung cancer by stage 5.2 Surgery Surgical resection for early stage disease (clinical Stages I and II) Extent of pulmonary resection Nodal assessment 5.3 Radiotherapy Radiotherapy in the treatment of locoregional non-small cell lung cancer Dose of radiotherapy Duration of radiotherapy Radiotherapy versus radiotherapy plus chemotherapy Chemotherapy versus radiotherapy with or without chemotherapy Timing of chemotherapy/radiotherapy regimens Frequency of chemotherapy Cisplatin or carboplatin Radiotherapy or surgery for Stage III disease Postoperative radiotherapy Complications of thoracic radiotherapy 5.4 Chemotherapy and adjuvant or neo-adjuvant treatment of locoregional non-small cell lung cancer Surgery and adjuvant chemotherapy Surgery and neo-adjuvant chemotherapy 5.5 Chemotherapy in advanced/metastatic non-small cell lung cancer General aspects The role of systemic chemotherapy in advanced non-small cell lung cancer Appropriate chemotherapy for treating advanced non-small cell lung cancer Single agent versus combination chemotherapy Optimal combination chemotherapy for advanced non-small cell lung cancer New versus old combinations with platinum Cisplatin versus carboplatin trials Trials comparing new drug plus platinum combinations Non-platinum new drug combinations Appropriate dose and duration of chemotherapy The role of second-line chemotherapy and other agents in advanced non-small cell lung cancer Biological agents Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 81
103 5.1 MANAGEMENT OF NON-SMALL CELL LUNG CANCER BY STAGE The optimal treatment for lung cancer is surgery. This approach implies that the tumour is at an early stage and that the patient is suitable for optimal regimen. When the disease is more advanced and technically unresectable, or the patient is not fit for surgery radiotherapy, chemotherapy or palliation are appropriate. Table 1 5 provides pathways for care. Table 1 5 Management of non-small cell lung cancer stage by stage Optimal regimen If patient is not suitable for optimal regimen, treat depending on symptoms and performance status Stages I & II Surgical resection Radical radiotherapy +/- chemotherapy (good performance status) Stage IIIA Stage IIIB Induction chemotherapy Surgical resection +/- Mediastinal radiotherapy or Radical combination chemoradiotherapy Radical combination chemoradiotherapy or Palliative management (poor performance status) or Observation if not symptomatic Palliative radiotherapy or chemotherapy or Observation if not symptomatic Stage IV Chemotherapy Palliative radiotherapy and Palliative radiotherapy for specific sites of disease (brain, bone pain). Some patients with solitary brain metastases may be suitable for surgical excision or Supportive care alone Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 83
104 5.2 SURGERY SURGICAL RESECTION FOR EARLY STAGE DISEASE (CLINICAL STAGES I & II) Surgical resection has been shown to result in the best five-year disease-free survival rates compared to any other form of treatment for NSCLC. Since the first successful pneumonectomy for NSCLC by Dr Evarts Graham in St Louis in , there have been refinements in patient selection, operative techniques and perioperative management which have translated into better survival with reduced postoperative morbidity and mortality. In looking at historical series of early stage lung cancer survival, it must be remembered that there has been a great variation in the degree of characterisation of metastases and node staging from the techniques used for the evaluation (including CT scanning, PET scanning, routine or selective mediastinoscopy, node sampling or node dissection at operation) as well as the difficulties of naming mediastinal and hilar node disease according to whichever node map was utilised. A recommendation for node classification was revised in and this is currently used in Australia for description of node locations both anatomically and pathologically. Lung cancer survival following surgical resection was reviewed by Rubins 3 comparing those patients treated between with those treated between This demonstrated that stage for stage the survival over the 47-year period had not altered but the operative mortality had reduced markedly. Surgery outperforms radiation therapy in the treatment of early stage NSCLC in those patients fit enough to tolerate the required resection. Morrison 4 reported a randomised study comparing radical radiation employing 45Gy in four weeks for early stage disease versus surgical resection. At four years there was a reported 7% survival in the radiation group compared to 23% in the surgical group. Gauden 5 reported the largest retrospective study of radiation for early stage lung cancer demonstrating a five year recurrence-free survival of 23% with the median survival being 19.5 months, significantly less than that reported in comparable surgical series for non-small cell lung cancer. The Japanese Lung Cancer Screening Research Group 6 studied 69 patients with Stage 1 lung cancer treated non-surgically with either chemotherapy or radiotherapy and found the five-year survival to be 14.3% in screen-detected asymptomatic patients and 3.7% for symptomatic patients. This study emphasised the poor prognosis for Stage I NSCLC patients treated without surgical resection. Many reviews have been published supporting surgery as the preferred form of treatment for early stage non-small cell lung cancer 7,8,9,10,11. The overall reported survival for patients with pathological Stage I and II disease is as follows: 84 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
105 Table 2 5 Pathological stage Survival for patients with stage 1 and 2 non-small cell lung cancer 12 Five-year survival (range) Stage I T1 N0 76.0% (68 83%) T2 N0 59.5% (54 65%) Stage II T1 N1 51.9% (40 63%) T2 N1 40.3% (39 45%) T3 N0 38.0% (25 55%) Guideline Non-small Cell Lung Cancer Surgical Resection Level of Evidence Refs Surgical resection is recommended for early stage non-small cell lung cancer, as this gives the best results of any form of treatment. II 4 EXTENT OF PULMONARY RESECTION The extent of pulmonary resection required to yield the optimal survival rates has been reviewed since the first successful pneumonectomy in Pneumonectomy was initially thought necessary for potential cure but survival data reported in the 1950s indicated that lobectomy was equally effective provided both macroscopic and microscopic clearance of tumour was achieved. Lobectomy was associated with lower operative and long-term mortality and morbidity compared with pneumonectomy. Lobectomy with mediastinal lymph node dissection is now the gold standard for surgical resection of NSCLC. Pneumonectomy is appropriately reserved for those patients with centrally placed primary tumours crossing the interlobar fissure, involving the main stem bronchi or main pulmonary arteries or in the presence of malignant hilar nodal disease in Stage II NSCLC. For patients with direct invasion of structures adjacent to the lung (T3: parietal pleura, chest wall, pericardium, diaphragm) en bloc resection of lung and involved extra pulmonary structures is associated with five-year survival in excess of 50% in those In whom complete microscopic resection is achieved and the nodal status is N0 13,14. As with malignancies elsewhere in the body, thoracic surgeons have assessed the role of lesser resections, namely pulmonary segmentectomy or wedge resections, for early stage NSCLC. In a retrospective review Warren and Faber 15 recorded 173 patients with Stage I NSCLC who had undergone either lobectomy or segmental resection. The fiveyear survival was similar, but there was a significant increase of locoregional recurrence in the segmental resection group (23%) compared to those undergoing lobectomy (5%). Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 85
106 The Lung Cancer Study Group 16 in a prospective, multi-institutional randomised trial compared lobectomy with minimal resection, most commonly segmentectomy. All patients were assessed as fit for lobectomy, and randomised in the operating theatre after frozen section confirmed T1 N0 staging with hilar and mediastinal lymph node sampling. Two hundred and forty seven patients were randomised. In those patients randomised to limited resection there was a significantly increased local recurrence rate, as well as an increased mortality rate related to their lung cancer. The study concluded that because of the higher death rate and a locoregional recurrence rate associated with limited resection (either segmentectomy or wedge resection), lobectomy still must be the surgical procedure of choice for patients with peripheral T1 N0 NSCLC 16. Ichinose 17 studied the correlation of tumour size with lymphatic invasion in resected peripheral Stage I NSCLC and found that as the tumour increased in size, the chance of lymphatic invasion increased from 25% in tumours less than 1cm in diameter to 57% in tumours greater than 3.1cm in diameter. This study emphasised the benefit of lobectomy over lesser resections in Stage I NSCLC. Furthermore, limited resections are not appropriate for patients with Stage I NSCLC who have adequate pulmonary function for lobectomy. The operative approach for lobectomy has traditionally been via a thoracotomy. Recently video-assisted thoracoscopic techniques (VATS) have been utilised successfully for pulmonary resections including regional lymph node assessment. Sugi 18 studied 100 consecutive patients with clinical Stage IA (T1 N0) NSCLC. Forty-eight patients underwent VATS lobectomy and 52 patients open lobectomy; lymph node dissection was performed in both groups. There were no differences in local recurrence rates (6%) or five-year survival (90% VATS, 85% open) between the two groups. Further studies are required to provide definitive evidence on the relative effectiveness and safety of lobectomy via VATS as compared with open thoracotomy. Guideline Non-small Cell Lung Cancer Lobectomy Level of Evidence Refs Lobectomy is preferred to limited resection in patients with operable T1 N0 NSCLC. II 16 NODAL ASSESSMENT Intra-operative and subsequent pathological regional node examination, as with most malignancies, is important in the management of NSCLC. There has been controversy regarding the extent of lymph dissection necessary for optimal results. Asamura 19 demonstrated that if extensive lymph node sampling is performed, 25% of patients are found to have unsuspected positive nodes (N1 10%, N2 15%). In patients with positive mediastinal nodes 25% had no hilar node involvement. In Asamura s series, Stage I patients had a five-year survival of 92% and a ten-year survival of 87%. 86 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
107 However, the study could not definitively relate the increased survival identified in these Stage I patients as being due to the lymph node resection, as opposed to simply more accurately identifying those patients that were truly Stage I disease. There has also been debate over whether mediastinal lymphadenectomy has a therapeutic advantage for resected lung cancer. Izbicki et al 20 randomised 182 patients with NSCLC to either standard mediastinal lymphadenectomy (removal of lymph nodes suspected of being involved in the hilar or mediastinal regions) or en bloc radical mediastinal lymphadenectomy (as described by Naruke et al 21 ), where all tissue containing mediastinal lymph nodes is removed and en bloc skeletonising of the mediastinum is performed. When matched to T and N status, no difference in survival, site or recurrence was shown. Not surprisingly, staging was more detailed in the radical lymph node dissection group. A prospective randomised study by Sugi 22 studied 115 patients with peripheral NSCLC less than 2cm in diameter. Patients were randomly assigned to lobectomy with lymph node sampling or lobectomy with radical systematic lymph node dissection. There was no difference in the detection of N1 or N2 positive nodes, no difference in either the local, distant or recurrence rates or in the five-year survival between the two groups (84% for node sampling group and 81% in the node dissection group). Guideline Non-small Cell Lung Cancer Regional Lymph Node Assessment Level of Evidence Refs Regional lymph node assessment should be performed with all lung resections for NSCLC. Radical mediastinal lymph node dissection whilst more accurately staging the patient provides no significant survival advantage over appropriate mediastinal lymph node sampling. II 19,20,22 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 87
108 5.3 RADIOTHERAPY RADIOTHERAPY IN THE TREATMENT OF LOCOREGIONAL NSCLC It has been known for many years that ionizing radiation is capable of killing lung cancer cells and reducing tumour size. In 1932, Pancoast described responses of tumours treated with radiotherapy, but acknowledged that the results for the most part, have been discouraging 23. In 1955, Bromley and Szur were able to confirm Pancoast s original observations through histopathologic examination of 66 lung cancers that were irradiated before resection. Although 17% of the cancers were of the oat cell variety, no tumour was found in 29 of 62 (46.7%) specimens examined 24. These findings led to uncertainty about the relative values of surgical resection and radiotherapy in the management of operable lung cancer, which was subsequently resolved by a randomised trial conducted at the Hammersmith Hospital. This study showed a statistically significant survival benefit for patients randomised to have radical surgery compared with patients randomised to have radiotherapy (45Gy of megavoltage irradiation), particularly for the subgroup with squamous cell carcinoma 4. The Hammersmith trial has had a profound influence on subsequent practice such that surgery came to be, and is still regarded as, the treatment of choice for fit patients with resectable lung cancer. Subsequent studies were designed to examine the value of radiotherapy in the management of patients with inoperable NSCLC, in particular, to determine whether the locoregional cytotoxic effects of radiotherapy translate into a survival advantage compared with placebo or a policy of observation 25,26,27. Three randomised trials designed to test this hypothesis have been published. One large North American study conducted by the Veterans Administration Lung Cancer Study Group (VALCSG), involving 800 patients, revealed a small but statistically significant advantage for patients with pathologically proven lung cancer confined to the chest who were randomised to radiotherapy compared with placebo 25. Patients with SCLC were included in this study, but subset analysis indicated that the survival advantage was essentially confined to patients with non-small cell histology/cytology. Two smaller European studies, which included radiotherapy and observation as two of the treatment arms, failed to reveal a survival advantage associated with the use of immediate radiotherapy 26,27. Not only were these studies smaller than the VALCSG study (249 and 117 patients respectively), and less likely to detect a difference between treatment policies, one study (unlike the VALCSG study), included patients without pathological confirmation of the diagnosis 25, and the other closed prematurely because of poor accrual Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
109 Guideline Non-small Cell Lung Cancer Radiotherapy Level of Evidence Refs In patients with inoperable NSCLC and who have no evidence of distant metastases, radiotherapy is recommended to locoregional disease because it may be associated with a survival advantage compared with placebo. II 25 DOSE OF RADIOTHERAPY The influence of radiotherapy dose on survival in patients with good performance status who have locoregional inoperable NSCLC has been investigated in four randomised trials 28,29,30,31. A dose of 60Gy given over six weeks was shown to be associated with an improved response rate, but not survival, compared with lower doses in a study of the Radiation Therapy Oncology Group (RTOG) 28. Importantly, the higher dose did not appear to be associated with increased toxicity. Similarly, no improvement in survival was observed when doses of 50Gy versus 42Gy 29 and 50Gy versus 40Gy 30 were compared. A British study showed a small but statistically significant survival benefit for 39Gy versus 17Gy 31. A comparison of hyperfractionated radiotherapy (69.6Gy given as 1.2Gy fractions, twice a day) revealed no advantage compared with 60Gy given by conventional fractionation, and that the hyperfractionated schedule was significantly inferior to combined modality treatment with chemotherapy and radiotherapy 32. Guideline Non-small Cell Lung Cancer Radiotherapy Dose Level of Evidence Refs In patients with locoregional inoperable NSCLC and with good performance status, higher doses of radiotherapy are associated with better response and possibly survival. Doses in the vicinity of 60Gy in six weeks are recommended because they are safe and give the highest response rates. II 28,31 DURATION OF RADIOTHERAPY It has recently been recognised that prolonging the time over which some epithelial cancers are treated with radiotherapy reduces the probability of local control, most likely by allowing accelerated repopulation of surviving clonogens. To minimise the chance of this occurring, treatment schedules that reduce overall treatment time (accelerated radiotherapy) have been designed and tested. The best known is the CHART (continuous hyperfractionated accelerated radiotherapy) regimen, in which Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 89
110 36 treatments are given in a 12 day period, with six hour intervals between treatments and without weekend interruption. The CHART schedule was shown to be superior to conventionally fractionated radiotherapy in a large multicentre trial, with a 22% reduction in relative risk of death across all patients and a 30% reduction in risk of death for patients with squamous cell carcinoma 33. This trial included patients with Stage I and II disease, for whom a similar reduction in risk was observed as for patients with more advanced disease. The better survival was due predominantly to improved local control, thus providing proof of the principle that radiotherapy can increase survival in selected patients with NSCLC. The combination of chemotherapy and radiotherapy is also associated with a survival advantage (see following section). Only one study has directly compared accelerated radiotherapy with combined chemotherapy and radiotherapy. This was a small study with less power than the CHART study to detect a survival advantage, and there was no clear benefit for any of the treatment arms 34. Thus, it remains unclear whether the survival advantage associated with CHART is of a greater magnitude than that achievable with combined chemotherapy and radiotherapy. As the main drawback associated with the CHART regimen is the timing of much of the treatment outside normal working hours, its use is unlikely to be widely adopted unless it can be shown to have significant advantages over combined chemotherapy and radiotherapy. RADIOTHERAPY VERSUS RADIOTHERAPY PLUS CHEMOTHERAPY Using survival as the endpoint, two meta-analyses have established the superiority of combined cisplatin-based chemotherapy and radical radiotherapy over radical radiotherapy alone 35,36. No survival advantage was observed if the chemotherapy did not contain cisplatin. The magnitude of the effect was similar for patients with Stage I or II disease as well as for those with Stage III disease. The benefit was most evident in patients with good performance status. A survival advantage was also observed in patients with poor performance status but this was not statistically significant. Guideline Non-small Cell Lung Cancer Radiotherapy and Chemotherapy Level of Evidence Refs The combination of cisplatin-based chemotherapy and radical radiotherapy in patients with good performance status is associated with a small but significant survival advantage compared with radiotherapy alone in NSCLC. I 35,36 The combination of cisplatin and radical radiotherapy was associated with a 13% reduction in risk of death, translating into an absolute survival benefit of 4% at two years and 2% at five years. 90 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
111 CHEMOTHERAPY VERSUS RADIOTHERAPY WITH OR WITHOUT CHEMOTHERAPY There are a number of studies in which radiotherapy and chemotherapy have been compared directly, but in none of these has a survival advantage been demonstrated for one treatment modality over the other 26,37,38,39. When the combination of radiotherapy and chemotherapy was compared with chemotherapy alone, in a small Japanese study of patients with Stage III disease who responded to initial cisplatin-based chemotherapy, there was a significant survival advantage for patients having the combined treatment 40. However, in a larger European study of similar design (patients without evidence of distant metastases who had responded to chemotherapy were randomised to further chemotherapy, or to radiotherapy), the addition of radiotherapy to chemotherapy did not significantly influence survival compared with chemotherapy alone, although it did result in significantly better local control 41. TIMING OF CHEMOTHERAPY/RADIOTHERAPY REGIMENS In a meta-analysis, all but one of eleven cisplatin trials had employed sequential chemotherapy followed by radiotherapy 35. Seven comparisons of concurrent cisplatin/ radiotherapy and six comparisons of sequential treatment were found to be associated with similar reductions in risk of death in a later meta-analysis 36. Two recent studies published since the meta-analyses comparing concomitant chemotherapy and radiotherapy with sequential chemotherapy followed by radiotherapy have revealed a survival advantage in favour of concurrent treatment 42,43. Guideline Non-small Cell Lung Cancer Timing of Radiotherapy and Cisplatin Therapy Level of Evidence Refs Concomitant cisplatin and radiotherapy are associated with a better survival than if the two treatments are given sequentially. II 42,43 FREQUENCY OF CHEMOTHERAPY The original European Organization for Research and Treatment of Cancer (EORTC) study, which demonstrated a survival advantage for the concomitant daily administration of cisplatin compared with radical radiotherapy alone, had a third arm in which patients were randomised to have weekly cisplatin 44. The survival in this arm was intermediate between the other two arms, but was not significantly different from either. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 91
112 CISPLATIN OR CARBOPLATIN Both cisplatin and carboplatin have been shown to potentiate radiation-induced cytotoxicity in human lung cancer cell lines in preclinical studies 45. The effects of carboplatin are similar to those of cisplatin, but of a slightly lower magnitude 26,45,46. Carboplatin, however, has less neurological, renal and gastrointestinal toxicity than cisplatin. The combination of radical radiotherapy and concomitant carboplatin has been tested against radiotherapy alone, but not against cisplatin and radical radiotherapy. Two studies have shown a survival advantage for the combination of carboplatin and hyperfractionated radiotherapy 47,48. Three other studies were inconclusive, showing no clear benefit for the addition of concomitant carboplatin to radiotherapy 34,49,50. RADIOTHERAPY OR SURGERY FOR STAGE III DISEASE Locally advanced disease characterised by mediastinal lymph node involvement (N2) is usually treated by radiotherapy. Recently there has been increasing interest in the use of surgery in patients with this disease stage, particularly with the demonstration of a survival advantage in two small randomised trials of chemotherapy followed by surgical resection (with and without postoperative radiotherapy) compared with locoregional treatment alone 51,52. However, in two small trials, the same strategy of preoperative chemotherapy and surgery was compared with radiotherapy 53 and with chemotherapy followed by radiotherapy 54, and there was no evidence of a survival advantage for either approach. POSTOPERATIVE RADIOTHERAPY The role of postoperative radiotherapy in patients who have had complete resection of NSCLC has recently been evaluated by meta-analysis 55. This revealed that in patients with Stage I or II disease, postoperative radiotherapy was detrimental to survival, compared with patients randomised to surgery alone. In patients with Stage III disease the effect of radiotherapy on survival was inconclusive. However, radiotherapy did appear to be associated with a reduction in local recurrence. It is possible that if smaller volumes of normal lung are irradiated using more modern radiotherapy techniques, the improvement in local control might result in a survival advantage. Postoperative radiotherapy using these techniques in patients with Stage III disease warrants further investigation. Guideline Non-small Cell Lung Cancer When to Avoid Radiotherapy Level of Evidence Refs Postoperative radiotherapy in patients with completely resected Stage I or II NSCLC is not recommended because of its detrimental effect on survival. I Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
113 COMPLICATIONS OF THORACIC RADIOTHERAPY Acute side effects of thoracic radiotherapy include anorexia, fatigue and oesophagitis. Oesophagitis is more severe and prolonged in patients treated with accelerated radiotherapy 34. Delayed side effects include pneumonitis and lung fibrosis. The risk of pneumonitis increases with dose and the volume of lung irradiated. The magnitude of these two risk factors can be expressed as a single quantity, either as the mean lung dose 56, or as the percentage of lung receiving a specified minimum dose derived from dose-volume histogram analysis 57, to predict the probability of a patient developing serious pneumonitis. Much more information correlating risk of pneumonitis with the mean lung dose or the V 20 (volume of lung receiving 20Gy or more) is required, however, in one single institution series, fatal pneumonitis was not observed if the V 20 was less than 32% 57. Spinal cord injury is a potential complication of thoracic radiotherapy, but rarely seen if the dose is under 50Gy using conventional 2Gy fractions. Schultheiss has estimated the risks to be 0.2% after 45Gy and 1 5% at five years after 60Gy with conventional fractionation CHEMOTHERAPY AND ADJUVANT OR NEO- ADJUVANT TREATMENT OF LOCOREGIONAL NON-SMALL CELL LUNG CANCER SURGERY AND ADJUVANT CHEMOTHERAPY The strongest evidence regarding the role of postsurgical adjuvant chemotherapy is derived from the meta-analysis of randomised trials comparing adjuvant chemotherapy to no adjuvant chemotherapy carried out by the Non-Small Cell Lung Cancer Collaborative Group. Patients who received adjuvant chemotherapy in five trials using non-platinum based regimens had worse survival. There was a 15% increase in the relative risk of death (p=0.005) with an absolute reduction in survival of 4% at two years and 5% at five years. These regimens are alkylating agent-based and are no longer used in clinical practice. In eight trials investigating platinum-based regimens, there was a 13% decrease in the relative risk of death with adjuvant chemotherapy (p=0.08). Absolute survival was improved by 3% at two years and 5% at five years. These differences were not statistically significant. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 93
114 The meta-analysis also addressed the question of the role of combined chemotherapy and radiotherapy given in the adjuvant setting. Four trials compared adjuvant chemoradiation versus adjuvant irradiation alone. For cisplatin-based combination chemotherapy there was a 6% decrease in the relative risk of death (p=0.46). Absolute survival was increased with chemotherapy by 2% at two years and 2% at five years. These differences were not statistically significant 35. Guideline Non-small Cell Lung Cancer Adjuvant Therapy Level of Evidence Refs The administration of adjuvant platinum-based chemotherapy is not recommended following surgery because it has not been definitively shown to significantly improve survival. I 35 SURGERY AND NEO-ADJUVANT CHEMOTHERAPY Under this section, studies were included where patients planned for surgical resection were randomised to receive chemotherapy or no chemotherapy prior to surgery (with or without radiotherapy). A list of these trials is given in Table 3 5. Evidence for the benefit of neo-adjuvant cisplatin-based chemotherapy comes from the two fully published trials 51,52, for which long-term follow-up has recently been published 59,60. Four other studies using cisplatin-based chemotherapy 61,62,63,64 and one using single agent docetaxel 65,66 were inconclusive. In the study from Roth et al, 60 patients with Stage IIIA NSCLC were randomised to surgery alone (32 patients), or surgery preceded by three cycles of cisplatin, etoposide and cyclophosphamide (28 patients) 52,59. Postoperative radiotherapy was given to patients with unresectable disease, or if the resection had been incomplete. The trial was stopped after a single unplanned interim analysis due to significantly improved median survival in the chemotherapy arm, 64 months versus 11 months (p<0.008). An update of this study, with median follow-up of 82 months, has recently been reported 59. Median survival was 21 months in the perioperative chemotherapy arm and 14 months in the surgery-alone arm (p=0.056 log rank test, p=0.048 Breslow-Gehan- Wilcoxon test). The overall three- and five-year survival was 43% and 36% respectively for the chemotherapy arm, and 19% and 15% for the surgery-alone arm. 94 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
115 In the second fully reported study, from Rosell et al, 60 patients with Stage IIIA NSCLC were randomised to surgery, or surgery preceded by three cycles of mitomycin C, ifosfamide and cisplatin 51,60. All patients received thoracic irradiation after surgery. Interim analyses were planned for 12, 18 and 24 months from the start of the study. Accrual was stopped after 24 months when a significant median survival difference in favour of the chemotherapy arm became apparent, 20 months versus 5 months, (p<0.001). A recent seven-year update of the results of this study showed that median survival was 22 months for the chemotherapy group and 10 months for the surgeryalone group (p=0.005 log rank test) 60. Three- and five-year survival rates were 20% and 17% respectively for the chemotherapy arm, compared with 5% and 0% for the surgery-alone arm. Further studies are required to establish the categories of Stage IIIA patients for whom the neo-adjuvant chemotherapy followed by surgery is appropriate, and to clarify its efficacy relative to non-surgical interventions. Guideline Lung Cancer Neo-adjuvant Therapy Level of Evidence Refs For Stage IIIA patients managed surgically, platinumbased combination chemotherapy should be given prior to surgery as it improves survival. Neo-adjuvant chemotherapy may be beneficial in earlier stage disease, but the evidence is currently insufficient to support routine use (see Table 3 5). II 51,52, 59,60 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 95
116 Table 3 5 Trials of surgery with or without preoperative chemotherapy in Stage IIIA non-small cell lung cancer Author Stage No (patients) Design Outcomes Pass 1992 (61)* Stage III (N2) 27 CT + S + CT vs S + RT Median survival CT/S 29 months vs S 16 months (p=0.095). Roth 1994 (52)* Stage IIIA 60 CT + S +/- CT Trial stopped at unplanned interim analysis. Roth 1998 (59)* vs S +/- RT Median survival superior in CT arm, 21 months (CEP) vs 14 months (p=0.05). 5-year survival superior in the CT arm, 36% v 15%. Rosell 1994 (51)* Stage IIIA 60 CT + S + RT Trial stopped at planned interim analysis. Rosell 1999 (60)* vs S + RT Median survival superior in CT arm, 22 months (MIC) vs 10 months. (p=0.005), 5-year survival superior in the CT arm, 17% vs 0%. Depierre 1999 (63)* Stage IB IIIA 373 CT + S +/- CT vs S Median survival superior in CT arm, 37 months Stage IIIA 167 (MIC) vs 26 months (p=0.09). On multivariate analysis, relative risk of death for CT arm 0.77 (p=0.05). Perioperative mortality non-significantly increased in CT arm. Mattson 2000 (66)* Stage IIIA 274 CT + RT vs RT or Median survival superior in CT arm, 15 months CT + S vs S (docetaxel) vs 13 months (ns). Elias 1997 (62)* Stage IIIA (N2) 47 CT + S + CT + RT Median survival CT/S 19 months RT/S 23 months (ns). vs RT+S+RT (PE) Ichinose 2000 (64)* Stage IIIA (N2) 62 CT + S vs S (PV) Median survival CT/S 18 months S 16 months (p = 0.6). * = reference CT chemotherapy; S surgery; RT radiotherapy; CEP cyclophosphamide, etoposide, cisplatin; MIC mitomycin, ifosfamide, cisplatin; PE cisplatin, etoposide; PV cisplatin vindesine; ns non-significant 96 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
117 5.5 CHEMOTHERAPY IN ADVANCED/METASTATIC NON-SMALL CELL LUNG CANCER GENERAL ASPECTS Patients with advanced/metastatic NSCLC consist of those patients whose disease is either: Stage IV (distant metastases) at the time of diagnosis of NSCLC Stage IV (distant metastases) developing after treatment for earlier stage NSCLC recurrent local intrathoracic disease after treatment for NSCLC unresectable Stage IIIB with disease beyond suitability for radical irradiation (for example, pleural effusion). There are a group of patients who present with earlier stage NSCLC, but who are not able to receive surgical or radical irradiation because of major comorbidity or other factors. While the management of such patients has elements in common with the management of advanced NSCLC, they are not usually included with advanced NSCLC patients in clinical trials, particularly trials of systemic therapies. The aim of treatment of advanced NSCLC is palliative. The palliative management of advanced NSCLC may involve treatment by oncologists, respiratory medicine physicians, palliative care physicians, and occasionally other medical specialists. The active participation of the patient s general practitioner is very important. The specific goals of treating advanced NSCLC are to: extend the patient s life relieve the patient s symptoms improve the patient s quality of life. When evaluating clinical trials, the important endpoints are therefore survival, changes in symptoms, and changes in quality of life. The response rate to a treatment, while often the primary endpoint of phase II trials, is not of comparable interest. The management of symptoms from metastatic NSCLC is covered elsewhere in these guidelines (refer to Chapters 7 and 8). Some sites of disease (for example, brain metastases with cerebral oedema, vertebral metastases with spinal cord compression) and syndromes (for example, malignant hypercalcaemia) are better palliated with non-chemotherapy treatments (for example, radiation therapy, bisphosphonates). Chemotherapy should not therefore be used as the primary treatment for these problems. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 97
118 THE ROLE OF SYSTEMIC CHEMOTHERAPY IN ADVANCED NON-SMALL CELL LUNG CANCER Three meta-analyses have been published examining the influence of chemotherapy on survival in advanced/metastatic NSCLC 35,67,68. The Non-Small Cell Lung Cancer Collaborative Group meta-analysis 35 was of 11 randomised controlled trials involving patients randomised to either chemotherapy or no chemotherapy. The other two meta-analyses were smaller (six and seven trials respectively) and all trials analysed by these groups were included in the Non-Small Cell Lung Cancer Collaborative Group meta-analysis. Therefore this analysis, which was based on individual patient data, is the most comprehensive. Chemotherapy provided a modest but highly statistically significant improvement in survival over supportive care alone 35. Statistical heterogeneity was apparent concerning the type of chemotherapy, such that a detrimental effect was observed for the two trials that used long-term administration of alkylating agent chemotherapy, no effect was seen in one trial that used vinca alkaloid/etoposide chemotherapy, and significant benefit was seen for the seven trials that used cisplatin-based chemotherapy. In the cisplatin chemotherapy trials (totalling 778 patients), the hazard ratio for death at one year was 0.73 (CI ), corresponding to an absolute improvement in one-year survival from 16% to 26% and an improvement in median survival from 4.0 months to 5.5 months. For all chemotherapy trials (1190 patients), the hazard ratio for death at one year was 0.84 (CI ). This meta-analysis examined the influence of disease extent on the beneficial effect of cisplatin-based chemotherapy, analysing the following: metastatic versus non-metastatic, histological subtype (squamous versus adenocarcinoma versus other), performance status ( good versus poor ), age, and sex. All subgroups were found to derive benefit from treatment 35. Data on relief of symptoms and changes in quality of life were not uniformly collected in the trials that were combined in these meta-analyses, and no analysis of these endpoints was performed. Since the publication of the Non-Small Cell Lung Cancer Collaborative Group metaanalysis, six other trials have been reported where patients were randomly allocated to treatment with chemotherapy or to not receive chemotherapy. Cullen et al 69 used a combination of cisplatin, ifosfamide and mitomycin C in a trial of 351 patients with metastatic NSCLC. There was a significant prolongation of median survival (6.7 months versus 4.8 months, p=0.03) with chemotherapy. Quality of life was assessed in a subset of patients only, and showed an improvement over the first six weeks with chemotherapy, whereas it progressively declined in the no-chemotherapy patients. A study from Thailand randomised 287 patients to either cisplatin; ifosfamide and epirubicin chemotherapy; cisplatin/mitomycin C/vinblastine chemotherapy or no chemotherapy. Survival was significantly prolonged in both chemotherapy arms, and quality of life (using modified, translated Western scales) was significantly improved with chemotherapy Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
119 The other four trials compared single agent chemotherapy using one of the newer cytotoxic agents introduced in the 1980s and 1990s (hereafter referred to new agents) 71,72,73,74. These trials are summarised in Table 4 5. Significant beneficial effects were found on survival and/or symptom control and quality of life in all studies. Patients with performance status of greater than 2 (see Appendix 3) or with other major co-existing medical problems were generally excluded from clinical trials. Many other clinical factors have been shown to be markers of poor prognosis in advanced NSCLC patients 75. However, there is no evidence that benefit experienced from chemotherapy is confined to particular patient subgroups. In particular, both a meta-analysis and a large randomised trial did not identify extent of metastatic disease, histological subtype, age, or sex as predictors of benefit 35,69. Only one trial has specifically enrolled only elderly (age 70 years) patients 74. This trial showed significant prolongation of survival with single-agent vinorelbine chemotherapy compared to supportive care. Table 4 5 Randomised trials of new agents versus supportive care Study agent Patients Survival Quality of life Ref Paclitaxel 157 Significantly improved No significant 71 with paclitaxel difference Gemcitabine 300 No significant Better QOL and 72 difference better symptom control with gemcitabine Docetaxel 207 Significantly improved Better QOL and 73 with docetaxel better symptom control with docetaxel Vinorelbine 191* Significantly improved Better QOL and 74 with vinorelbine better symptom control with vinorelbine * trial restricted to patients aged > 70 years. QOL quality of life Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 99
120 Guidelines Non-small Cell Lung Cancer Chemotherapy Level of Evidence Refs Chemotherapy is appropriate treatment for patients with advanced NSCLC who have good performance status (ECOG 2) and are otherwise medically fit as it has been shown to improve survival. Chemotherapy can result in beneficial effects on symptoms and quality of life in patients with advanced NSCLC. I 35 II 69,70 APPROPRIATE CHEMOTHERAPY FOR TREATING ADVANCED NON-SMALL CELL LUNG CANCER SINGLE AGENT VERSUS COMBINATION CHEMOTHERAPY The evidence for benefit from cisplatin-based chemotherapy on survival was derived from trials where cisplatin was combined with older drugs including vinca alkaloids (vindesine, vinblastine), etoposide, doxorubicin, cyclophosphamide and mitomycin C 35. Another meta-analysis (using only published trials, without individual patient data) has examined the effect on response rates, survival and toxicity of combination chemotherapy compared to single-agent chemotherapy 76. Combination chemotherapy produced a significantly higher response rate, significantly better six- and 12-month survival and higher levels of toxicity. However, benefit on survival was not apparent when only trials that had cisplatin or vinorelbine as the single-agent arm were considered, suggesting that the overall benefit was attributable to older trials where the single-agent arm was ineffective. Further studies are required to better define the role of single-agent therapy with the new agents compared to combination chemotherapy. This is particularly important for patients with performance status 2, who may not tolerate combination chemotherapy, as well as for better performance status patients. Several more recent trials have compared the combination of a new drug plus cisplatin with cisplatin alone. These are summarised in Table 5 5. All trials except one have shown significantly improved survival with the combination. 100 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
121 Table 5 5 Randomised trials of new agents plus cisplatin versus cisplatin New agent Patients Survival Quality of life Ref Paclitaxel 414 No significant No significant difference difference 77 Vinorelbine 432 Significant survival Not assessed 78 advantage with combination Gemcitabine 552 Significant survival No significant 79 advantage with difference combination Tirapazamine 446 Significant survival No significant 80 advantage with difference combination One phase III trial of 169 patients has compared single agent gemcitabine to the combination of cisplatin and vindesine. Survival and control of symptoms were equivalent, but quality of life improved in more patients in the gemcitabine arm 81,82. Two smaller trials have compared single agent gemcitabine to the combination of cisplatin and etoposide 83,84. With short follow-up, both trials reported no difference in response rate or survival. As expected, in all these trials, the cisplatin arms had more severe toxicity than single-agent therapy. None of these trials is large enough to be adequately powered to exclude inferior survival with gemcitabine compared to the combination therapy. Guidelines Non-small Cell Lung Cancer Combination Chemotherapy Level of Evidence Refs Combination chemotherapy is preferable to single agent therapy in patients with advanced NSCLC. For patients where combination chemotherapy is contraindicated, single agent therapy with one of the new agents (either a taxane, gemcitabine or vinorelbine) is appropriate. I 76 II 83,84 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 101
122 OPTIMAL COMBINATION CHEMOTHERAPY FOR ADVANCED NSCLC NEW VERSUS OLD COMBINATIONS WITH PLATINUM A series of trials have compared old platinum combinations (for example, cisplatin plus vinca alkaloid, cisplatin plus etoposide/teniposide) to new platinum combinations. The new combinations tested include cisplatin combined with paclitaxel 85,86, vinorelbine 87, gemcitabine 88,89, tirapazamine 90 and irinotecan 91. In some studies there was a modest survival benefit for the new regimen 85,87 and in others improved quality of life 86. In the remainder, survival and quality of life outcomes were similar in both arms. CISPLATIN VERSUS CARBOPLATIN TRIALS Combination chemotherapy regimens using either cisplatin or cisplatin replaced by carboplatin have been directly compared in three phase III trials 92,93,94. There was no consistent evidence of the superiority of one drug over the other. Emesis and renal toxicity were greater with cisplatin whereas haematological toxicity was greater with carboplatin. TRIALS COMPARING NEW DRUG PLUS PLATINUM COMBINATIONS Many trials have been performed in the last five years comparing various new regimens. The large majority of these have been published only in abstract form. The results of some of the largest trials are summarised in Table 6 5. The largest trial 95 was conducted by the Eastern Cooperative Oncology Group (ECOG) in the US. Over patients were randomised to the control arm of paclitaxel over 24 hours plus cisplatin 85 or one of three other regimens. Response rate and overall survival times were not significantly higher in any of the three experimental arms. A marginal but statistically significant benefit in time to progression was found in the cisplatin/gemcitabine arm, however, the chemotherapy in this arm was administered every four weeks, rather than every three weeks as in the control arm, making assessment of this endpoint difficult. Toxicity was variable, but less acute emesis and febrile neutropenia occurred in the carboplatin/paclitaxel arm. The inconvenience of the 24-hour paclitaxel infusion makes this regimen less suited to the palliative setting. While no significant disadvantage occurred with cisplatin/docetaxel, the activity of docetaxel in second-line therapy (see below) indicates alternative drugs may be preferable for first-line therapy. The above ECOG trial was originally intended to enrol patients with performance status 0,1 or 2 but a high rate of toxicity resulted in termination of accrual of performance status 2 patients. Most other trials in Table 6 5 have been restricted to performance status 0 or 1 patients. 102 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
123 Two trials have evaluated the addition of a third new agent to a new drug plus platinum combination 96,97. In one trial 96 the initial report has shown significant benefit to the triplet combination. Other trials examining various triplet combinations are being conducted. Table 6 5 Randomised trials of new agents Design Patients Outcome Ref cisplatin/paclitaxel vs 1207 Survival and response rates equivalent. 95 cisplatin/gemcitabine vs Longer time to progression with cisplatin/docetaxel vs cisplatin/gemcitabine. Less nausea carboplatin/paclitaxel and febrile neutropenia with carboplatin/paclitaxel. cisplatin/gemcitabine vs 371 Triplet arms had superior survival and 96 cisplatin/gemcitabine/paclitaxel vs longer time to worsening symptoms. cisplatin/gemcitabine/vinorelbine paclitaxel/carboplatin vs 329 Equivalent response rate, survival 98 paclitaxel/gemcitabine and toxicity. paclitaxel/carboplatin vs 444 Equivalent survival and QOL. Less 99 cisplatin/vinorelbine haematological toxicity and emesis with carboplatin/paclitaxel. docetaxel/cisplatin vs 414 Equivalent response rate and survival. 100 docetaxel/gemcitabine More diarrhoea with docetaxel/ cisplatin. Both arms received G-CSF support. gemcitabine/cisplatin vs 180 Cisplatin/vinorelbine closed at interim 97 vinorelbine/cisplatin vs analysis because of worse survival. cisplatin/vinorelbine/gemcitabine Accrual continues to other arms. gemcitabine/vinorelbine vs 120* Closed at interim analysis because 101 vinorelbine of survival benefit with combination. Longer time to symptom and QOL deterioration with combination. *Trial restricted to patients aged 70 years QOL = quality of life; G-CSF = granulocyte colony stimulating factors Other platinum-ased combinations such as carboplatin plus gemcitabine or carboplatin plus vinorelbine have been investigated in phase II trials and have shown some activity, but phase III data to support their use is lacking. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 103
124 NON-PLATINUM NEW DRUG COMBINATIONS Two phase III trials have compared the combination of two new drugs with a platinum plus one new drug combination 98,100 (Table 6 5). Neither trial showed any benefit of the non-platinum arm in terms of response rate or survival. Both trials failed to show a marked reduction in toxicity with the omission of platinum. One trial restricted to elderly patients compared the combination of gemcitabine and vinorelbine to vinorelbine alone 101. This trial was closed with accrual of only 120 patients because an interim analysis showed a significant benefit with the combination. The results obtained with the vinorelbine alone arm in this trial appear substantially worse than the previous trial performed by this group 74. Guidelines Non-small Cell Lung Cancer Choice of Chemotherapy Agents Level of Evidence Refs At the present time, no one chemotherapy regimen can be recommended over another. Based on currently available trial results, various combinations of a platinum drug plus a new agent are reasonable options for performance status 0 or 1 patients. The use of combinations of three or more drugs, and the use of non-platinum combinations require further investigation before incorporation into standard practice. Carboplatin can be used instead of cisplatin in combination chemotherapy. II 85,86,87,88 II 92,93,94 APPROPRIATE DOSE AND DURATION OF CHEMOTHERAPY The clinical trials evaluating various cytotoxics in NSCLC have used doses derived from phase I and II studies where routine use of colony-stimulating factor support, stem-cell support or use of cytoprotectants such as amifostine was not permitted. Only a small number of trials have specifically addressed cytotoxic doses in NSCLC patients. Two trials evaluating higher does of paclitaxel 85,102 have shown no survival benefit for the higher dose. Increased frequency 103 or dose of cisplatin 104 have not been shown to be more effective than four weekly administration or lower doses (50 mg/m 2 ) respectively. In most of the discussed clinical trials in advanced NSCLC, treatment was generally administered for up to six to nine cycles in the absence of disease progression or severe toxicity. The cumulative non-haematological toxicity seen with agents such as platinum, paclitaxel, docetaxel and vinorelbine makes prolonged administration unfeasible. In trials where symptom control has been assessed in detail, improvement with chemotherapy is apparent within two to three cycles, and correlates with response or non-progression on radiological assessments. 104 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
125 Two recent trials have addressed the duration of chemotherapy. One trial 105 compared the administration of three or six cycles of the older cisplatin/vinblastine/ mitomycin C combination, and reported that there were no differences in survival or symptom relief between the schedules. A second trial 106 used the more currently accepted combination of carboplatin and paclitaxel. Patients were randomised to receive four cycles or to continue to receive treatment until documented disease progression. No difference in survival was reported, and as expected the continuous arm had an increasing incidence of peripheral neuropathy. Neither of these trials directly randomised only responding patients to continue or cease treatment, although a retrospective analysis of the data from the first trial suggests that stopping therapy is not detrimental to these patients 106. As only a minority of advanced NSCLC patients will show significant reduction of tumour mass with chemotherapy, it is particularly necessary to take care to avoid continuation of ineffective therapy. Guidelines Non-Small Cell Lung Cancer Chemotherapy Doses and Cycles There is no indication to use greater than standard doses or dose intensity of chemotherapy in advanced NSCLC. Level of Evidence II Refs 85,102, 103,104 Continuing multi-agent platinum-based chemotherapy beyond three to four cycles does not provide additional survival benefit. Patients receiving chemotherapy for advanced NSCLC should be evaluated for effectiveness of treatment after two to three cycles. Treatment should be discontinued if no benefit is seen. II 105,106 IV 106 THE ROLE OF SECOND-LINE CHEMOTHERAPY AND OTHER AGENTS IN ADVANCED NON-SMALL CELL LUNG CANCER Most studies in which the use of second-line chemotherapy at the time of progression or relapse has been evaluated are phase II trials 107. These involve small numbers of patients and little information is provided on the performance status and the extent and nature of prior treatment of the patients. The rate of response to treatment is often the major endpoint assessed and the trial designs do not allow for any reliable assessment of patient benefit to be made. Two randomised phase III studies of docetaxel in patients previously treated with cisplatin-based chemotherapy are available. Both showed a survival advantage: one compared docetaxel with best supportive care 108 and the other compared docetaxel with vinorelbine or cyclophosphamide 109. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 105
126 BIOLOGICAL AGENTS The role of biological agents in NSCLC is an emerging area of research. Numerous compounds are in various phases of preclinical and clinical development. A promising group of small molecules are inhibitors of the epidermal growth-factor tyrosine kinase. Early phase studies suggest that symptom improvement can occur with the use of these compounds. However, further research is required before these compounds have an established place in lung cancer management. Guideline Non-small Cell Lung Cancer Second Line Chemotherapy Level of Evidence Refs In selected good performance status patients, secondline chemotherapy with docetaxel may be considered. II 108,109 References 1. Graham EA, Singh JJ. Successful Removal of the Entire Lung for Carcinoma of the Bronchus. JAMA 1933; 101: Mountain CF, Dresler CM. Regional Lymph Node Classification for Lung Cancer Staging. Chest 1997; 111(6): Rubins JB, Ewing SL, Leroy S, Humphrey EW, Morrison V. Temporal Trends in Survival After Surgical Resection of Localized Non-Small Cell Lung Cancer. Lung Cancer 2000; 28(1): Morrison R, Deeley TJ, Cleland WP. The Treatment of Carcinoma of the Bronchus: a Clinical Trial to Compare Surgery and Super Voltage Radiotherapy. Lancet 1963; 1(683): Gauden S, Ramsay J, Tripcony L. The Curative Treatment by Radiotherapy Alone of Stage I Non-Small Cell Carcinoma of the Lung. Chest 1995; 108(5): Sobue T, Suzuki T, Matsuda M, Kuroishi T, Ikeda S, Naruke T. Survival for Clinical Stage I Lung Cancer Not Surgically Treated. Comparison Between Screen-Detected and Symptom-Detected Cases. The Japanese Lung Cancer Screening Research Group. Cancer 1992; 69(3): Nesbitt J, Putnam J, Garrett L, et al. Survival in Early Stage Non-Small Cell Lung Cancer. Ann Thorac Surg 1995; 60: Martini N, Burt ME, Bains MS, McCormack PM, Rusch VW, Ginsberg RJ. Survival After Resection of Stage II Non-Small Cell Lung Cancer. Ann Thorac Surg 1992; 54(3): Moores DW, McKneally MF. Treatment of Stage I Lung Cancer (T1N0M0, T2N0M0). Surg Clin North Am 1987; 67(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
127 10. Holmes EC. Treatment of Stage II Lung Cancer (T1N1 and T2N1). Surg Clin North Am 1987; 67(5): Martini N, Beattie EJJ. Results of Surgical Treatment in Stage I Lung Cancer. J Thorac Cardiovasc Surg 1977; 74(4): Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest 1997; 111(6): McCaughan BC, Martini N, Bains MS, McCormack PM. Chest Wall Invasion in Carcinoma of the Lung. Therapeutic and Prognostic Implications. J Thorac Cardiovasc Surg 1985; 89(6): Piehler JM, Pairolero PC, Weiland LH, Offord KP, Payne WS, Bernatz PE. Bronchogenic Carcinoma With Chest Wall Invasion: Factors Affecting Survival Following En Bloc Resection. Ann Thorac Surg 1982; 34(6): Warren W, Faber P. Segmentectomy Versus Lobectomy in Patients With Stage 1 Pulmonary Carcinoma. J Thorac Cardiovasc Surg 1994; 107: Ginsberg RJ, Rubinstein LV. Randomized Trial of Lobectomy Versus Limited Resection for T1 N0 Non-Small Cell Lung Cancer. Lung Cancer Study Group. Ann Thorac Surg 1995; 60(3): Ichinose Y, Yano T, Yokoyama H, Inoue T, Asoh H, Katsuda Y. The Correlation Between Tumor Size and Lymphatic Vessel Invasion in Resected Peripheral Stage I Non-Small-Cell Lung Cancer. A Potential Risk of Limited Resection. J Thorac Cardiovasc Surg 1994; 108(4): Sugi K, Kaneda Y, Esato K. Video-Assisted Thoracoscopic Lobectomy Achieves a Satisfactory Long-Term Prognosis in Patients With Clinical Stage IA Lung Cancer. World J Surg 2000; 24(1): Asamura H, Nakayama H, Kondo H, Tsuchiya R, Shimosato Y, Naruke T. Lymph Node Involvement, Recurrence, and Prognosis in Resected Small, Peripheral, Non-Small-Cell Lung Carcinomas: Are These Carcinomas Candidates for Video- Assisted Lobectomy? J Thorac Cardiovasc Surg 1996; 111(6): Izbicki JR, Passlick B, Pantel K, Pichlmeier U, Hosch SB, Karg O, Thetter O. Effectiveness of Radical Systematic Mediastinal Lymphadenectomy in Patients With Resectable Non-Small Cell Lung Cancer: Results of a Prospective Randomized Trial. Ann Surg 1998; 227(1): Naruke T, Suemasu K, Ishikawa S. Lymph Node Mapping and Curability at Various Levels of Metastasis in Resected Lung Cancer. J Thorac Cardiovasc Surg 1978; 76(6): Sugi K, Nawata K, Fujita N, Ueda K, Tanaka T, Matsuoka T, Kaneda Y, Esato K. Systematic Lymph Node Dissection for Clinically Diagnosed Peripheral Non-Small- Cell Lung Cancer Less Than 2 Cm in Diameter. World J Surg 1998; 22(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 107
128 23. Pancoast HK, Pendergrass EP. Primary Bronchogenic Carcinoma of the Lungs. Am J Radiology 1932; 27: Bromley LL, Szur L. Combined Radiotherapy and Resection for Carcinoma of the Bronchus. Lancet 1955; 2(937): Wolf J, Patno ME, Roswit B, D Esopo N. Controlled Study of Survival of Patients With Clinically Inoperable Lung Cancer Treated With Radiation Therapy. Am J Med 1966; 40(3): Durrant KR, Berry RJ, Ellis F, Ridehalgh FR, Black JM, Hamilton WS. Comparison of Treatment Policies in Inoperable Bronchial Carcinoma. Lancet 1971; 1(7702): Gregor A, Macbeth FR, Paul J, Cram L, Hansen HH. Radical Radiotherapy and Chemotherapy in Localized Inoperable Non-Small-Cell Lung Cancer: a Randomized Trial. J Natl Cancer Inst 1993; 85(12): Perez CA, Stanley K, Rubin P, Kramer S, Brady L, Perez-Tamayo R, Brown GS, Concannon J, Rotman M, Seydel HG. A Prospective Randomized Study of Various Irradiation Doses and Fractionation Schedules in the Treatment of Inoperable Non-Oat-Cell Carcinoma of the Lung. Preliminary Report by the Radiation Therapy Oncology Group. Cancer 1980; 45(11): Petrovich Z, Stanley K, Cox JD, Paig C. Radiotherapy in the Management of Locally Advanced Lung Cancer of All Cell Types: Final Report of Randomized Trial. Cancer 1981; 48(6): Sealy R, Lagakos S, Barkley T, Ryall R, Tucker RD, Lee RE, Ehlers G. Radiotherapy of Regional Epidermoid Carcinoma of the Lung: a Study in Fractionation. Cancer 1982; 49(7): Macbeth FR, Bolger JJ, Hopwood P, Bleehen NM, Cartmell J, Girling DJ, Machin D, Stephens RJ, Bailey AJ. Randomized Trial of Palliative Two-Fraction Versus More Intensive 13-Fraction Radiotherapy for Patients With Inoperable Non-Small Cell Lung Cancer and Good Performance Status. Medical Research Council Lung Cancer Working Party. Clin Oncol (R Coll Radiol) 1996; 8(3): Sause WT, Scott C, Taylor S, Johnson D, Livingston R, Komaki R, Emami B, Curran WJ, Byhardt RW, Turrisi AT. Radiation Therapy Oncology Group (RTOG) and Eastern Cooperative Oncology Group (ECOG) 4588: Preliminary Results of a Phase III Trial in Regionally Advanced, Unresectable Non-Small-Cell Lung Cancer. J Natl Cancer Inst 1995; 87(3): Saunders M, Dische S, Barrett A, Harvey A, Gibson D, Parmar M. Continuous Hyperfractionated Accelerated Radiotherapy (CHART) Versus Conventional Radiotherapy in Non-Small-Cell Lung Cancer: a Randomised Multicentre Trial. CHART Steering Committee. Lancet 1997; 350(9072): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
129 34. Ball D, Bishop J, Smith J, O Brien P, Davis S, Ryan G, Olver I, Toner G, Walker Q, Joseph D. A Randomised Phase III Study of Accelerated or Standard Fraction Radiotherapy With or Without Concurrent Carboplatin in Inoperable Non-Small Cell Lung Cancer: Final Report of an Australian Multi-Centre Trial. Radiother Oncol 1999; 52(2): Chemotherapy in Non-Small Cell Lung Cancer: a Meta-Analysis Using Updated Data on Individual Patients From 52 Randomised Clinical Trials. Non-Small Cell Lung Cancer Collaborative Group. BMJ 1995; 311(7010): Pritchard RS, Anthony SP. Chemotherapy Plus Radiotherapy Compared With Radiotherapy Alone in the Treatment of Locally Advanced, Unresectable, Non- Small-Cell Lung Cancer. A Meta-Analysis. Ann Intern Med 1996; 125(9): Berry RJ, Laing AH, Newman CR, Peto J. The Role of Radiotherapy in Treatment of Inoperable Lung Cancer. Int J Radiat Oncol Biol Phys 1977; 2(5 6): Kaasa S, Thorud E, Host H, Lien HH, Lund E, Sjolie I. A Randomized Study Evaluating Radiotherapy Versus Chemotherapy in Patients With Inoperable Non-Small Cell Lung Cancer. Radiother Oncol 1988; 11(1): Johnson DH, Einhorn LH, Bartolucci A, Birch R, Omura G, Perez CA, Greco FA. Thoracic Radiotherapy Does Not Prolong Survival in Patients With Locally Advanced, Unresectable Non-Small Cell Lung Cancer. Ann Intern Med 1990; 113(1): Kubota K, Furuse K, Kawahara M, Kodama N, Yamamoto M, Ogawara M, Negoro S, Masuda N, Takada M, Matsui K. Role of Radiotherapy in Combined Modality Treatment of Locally Advanced Non-Small-Cell Lung Cancer. J Clin Oncol 1994; 12(8): Sculier JP, Paesmans M, Lafitte JJ, Baumohl J, Thiriaux J, van Cutsem O, Recloux P, Bureau G, Berchier MC, Zacharias C, Mommen P, Bosschaerts T, Berghmans T, van Houtte P, Ninane V, Klastersky J. A Randomised Phase III Trial Comparing Consolidation Treatment With Further Chemotherapy to Chest Irradiation in Patients With Initially Unresectable Locoregional Non-Small-Cell Lung Cancer Responding to Induction Chemotherapy. European Lung Cancer Working Party. Ann Oncol 1999; 10(3): Furuse K, Fukuoka M, Kawahara M, Nishikawa H, Takada Y, Kudoh S, Katagami N, Ariyoshi Y. Phase III Study of Concurrent Versus Sequential Thoracic Radiotherapy in Combination With Mitomycin, Vindesine, and Cisplatin in Unresectable Stage III Non-Small-Cell Lung Cancer. J Clin Oncol 1999; 17(9): Movsas B, Scott C, Curran W, et al. A quality-adjusted time without symptoms or toxicity (QTWiST) analysis of radiation therapy oncology Group [RTOG] Proceedings of American Society of Clinical Oncology Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 109
130 44. Schaake-Koning C, van den Bogaert W, Dalesio O, Festen J, Hoogenhout J, van Houtte P, Kirkpatrick A, Koolen M, Maat B, Nijs A. Effects of Concomitant Cisplatin and Radiotherapy on Inoperable Non-Small-Cell Lung Cancer. N Engl J Med 1992; 326(8): Groen HJ, Sleijfer S, Meijer C, Kampinga HH, Konings AW, De Vries EG, Mulder NH. Carboplatin- and Cisplatin-Induced Potentiation of Moderate-Dose Radiation Cytotoxicity in Human Lung Cancer Cell Lines. Br J Cancer 1995; 72(6): Schwachofer JH, Crooijmans RP, Hoogenhout J, Kal HB, Theeuwes AG. Effectiveness in Inhibition of Recovery of Cell Survival by Cisplatin and Carboplatin: Influence of Treatment Sequence. Int J Radiat Oncol Biol Phys 1991; 20(6): Jeremic B, Shibamoto Y, Acimovic L, Djuric L. Randomized Trial of Hyperfractionated Radiation Therapy With or Without Concurrent Chemotherapy for Stage III Non-Small-Cell Lung Cancer. J Clin Oncol 1995; 13(2): Jeremic B, Shibamoto Y, Acimovic L, Milisavljevic S. Hyperfractionated Radiation Therapy With or Without Concurrent Low-Dose Daily Carboplatin/Etoposide for Stage III Non-Small-Cell Lung Cancer: a Randomized Study. J Clin Oncol 1996; 14(4): Clamon G, Herndon J, Cooper R, Chang AY, Rosenman J, Green MR. Radiosensitization With Carboplatin for Patients With Unresectable Stage III Non-Small- Cell Lung Cancer: a Phase III Trial of the Cancer and Leukemia Group B and the Eastern Cooperative Oncology Group. J Clin Oncol 1999; 17(1): Groen HJ, Van der Leest AHW, Snoek JD, et al. Phase III Study of Continuous Carboplatin Over 6 Weeks With Radiation Versus Radiation Alone in Stage III Non- Small Cell Lung Cancer. Proceedings of American Society of Clinical Oncology 1999; 18(466a). 51. Rosell R, Gomez-Codina J, Camps C, Maestre J, Padille J, Canto A, Mate JL, Li S, Roig J, Olazabal A. A Randomized Trial Comparing Preoperative Chemotherapy Plus Surgery With Surgery Alone in Patients With Non-Small-Cell Lung Cancer. N Engl J Med 1994; 330(3): Roth JA, Fossella F, Komaki R, Ryan MB, Putnam JBJ, Lee JS, Dhingra H, De Caro L, Chasen M, McGavran M. A Randomized Trial Comparing Perioperative Chemotherapy and Surgery With Surgery Alone in Resectable Stage IIIA Non- Small-Cell Lung Cancer. J Natl Cancer Inst 1994; 86(9): Shepherd FA, Johnston MR, Payne D, Burkes R, Deslauriers J, Cormier Y, de Bedoya LD, Ottaway J, James K, Zee B. Randomized Study of Chemotherapy and Surgery Versus Radiotherapy for Stage IIIA Non-Small-Cell Lung Cancer: a National Cancer Institute of Canada Clinical Trials Group Study. Br J Cancer 1998; 78(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
131 54. Inculet R, Scott C, Dar A, et al. Phase III Study Comparing Chemotherapy and Radiation Therapy With Preoperative Chemotherapy and Surgical Resection in Patients With Non-Small Cell Lung Cancer With Spread to Mediastinal Nodes [N2]: a Radiation Therapy Oncology Group Study [RTOG 89 01]. Lung Cancer 1997; 18: Postoperative Radiotherapy in Non-Small-Cell Lung Cancer: Systematic Review and Meta-Analysis of Individual Patient Data From Nine Randomised Controlled Trials. PORT Meta-Analysis Trialists Group. Lancet 1998; 352(9124): Kwa SL, Lebesque JV, Theuws JC, Marks LB, Munley MT, Bentel G, Oetzel D, Spahn U, Graham MV, Drzymala RE, Purdy JA, Lichter AS, Martel MK, Ten Haken RK. Radiation Pneumonitis As a Function of Mean Lung Dose: an Analysis of Pooled Data of 540 Patients. Int J Radiat Oncol Biol Phys 1998; 42(1): Graham MV, Purdy JA, Emami B, Harms W, Bosch W, Lockett MA, Perez CA. Clinical Dose-Volume Histogram Analysis for Pneumonitis After 3D Treatment for Non-Small Cell Lung Cancer (NSCLC). Int J Radiat Oncol Biol Phys 1999; 45(2): Schultheiss TE, Kun LE, Ang KK, Stephens LC. Radiation Response of the Central Nervous System. Int J Radiat Oncol Biol Phys 1995; 31(5): Roth JA, Atkinson EN, Fossella F, Komaki R, Bernadette RM, Putnam JBJ, Lee JS, Dhingra H, De Caro L, Chasen M, Hong WK. Long-Term Follow-Up of Patients Enrolled in a Randomized Trial Comparing Perioperative Chemotherapy and Surgery With Surgery Alone in Resectable Stage IIIA Non-Small-Cell Lung Cancer. Lung Cancer 1998; 21(1): Rosell R, Gomez-Codina J, Camps C, Javier SJ, Maestre J, Padilla J, Canto A, Abad A, Roig J. Preresectional Chemotherapy in Stage IIIA Non-Small-Cell Lung Cancer: a 7-Year Assessment of a Randomized Controlled Trial. Lung Cancer 1999; 26(1): Pass HI, Pogrebniak HW, Steinberg SM, Mulshine J, Minna J. Randomized Trial of Neoadjuvant Therapy for Lung Cancer: Interim Analysis. Ann Thorac Surg 1992; 53(6): Elias AD, Herndon J, Kumar P, et al. A Phase III Comparison of Best Local- Regional Therapy With or Without Chemotherapy (CT) for Stage IIIA T1 3N2 Non-Small Cell Lung Cancer (NSCLC): Preliminary Results. Proceedings of American Society of Clinical Oncology 1997; 16: 448a. 63. Depierre A, Milleron B, Chevret D, et al. French Phase III Trial of Preoperative Chemotherapy (PCT) in Resectable Stage I (Except T1N0), II, IIIA Non-Small Cell Lung Caner (NSCLC). Lung Cancer 2000; 29 (Suppl 1): Ichinose Y, Tsuchiya R, Kato H. Randomized Trial of Chemotherapy Followed by Surgery Versus Surgery for Stage IIIA Non-Small Cell Lung Cancer. Lung Cancer 2000; 29(suppl 2): 173. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 111
132 65. Mattson K, ten Velde GP, Krofta K, et al. Early Results of an International Phase III Study Evaluating Taxotere As Neo-Adjuvant Therapy for Radically-Treatable Stage III NSCLC. Lung Cancer 2000; 29 (Suppl 1): Mattson K, ten Velde GP, Krofta K, et al. Taxotere As Neoadjuvant Therapy for Radically-Treatable Stage III NSCLC. Preliminary Results of an International Phase III Study. Proceedings of American Society of Clinical Oncology 2000; 19: 483a. 67. Grilli R, Oxman AD, Julian JA. Chemotherapy for Advanced Non-Small-Cell Lung Cancer: How Much Benefit Is Enough? J Clin Oncol 1993; 11(10): Souquet PJ, Chauvin F, Boissel JP, Cellerino R, Cormier Y, Ganz PA, Kaasa S, Pater JL, Quoix E, Rapp E. Polychemotherapy in Advanced Non Small Cell Lung Cancer: a Meta-Analysis. Lancet 1993; 342(8862): Cullen MH, Billingham LJ, Woodroffe CM, Chetiyawardana AD, Gower NH, Joshi R, Ferry DR, Rudd RM, Spiro SG, Cook JE, Trask C, Bessell E, Connolly CK, Tobias J, Souhami RL. Mitomycin, Ifosfamide, and Cisplatin in Unresectable Non-Small- Cell Lung Cancer: Effects on Survival and Quality of Life. J Clin Oncol 1999; 17(10): Thongprasert S, Sanguanmitra P, Juthapan W, Clinch J. Relationship Between Quality of Life and Clinical Outcomes in Advanced Non-Small Cell Lung Cancer: Best Supportive Care (BSC) Versus BSC Plus Chemotherapy. Lung Cancer 1999; 24(1): Ranson M, Davidson N, Nicolson M, Falk S, Carmichael J, Lopez P, Anderson H, Gustafson N, Jeynes A, Gallant G, Washington T, Thatcher N. Randomized Trial of Paclitaxel Plus Supportive Care Versus Supportive Care for Patients With Advanced Non-Small-Cell Lung Cancer. J Natl Cancer Inst 2000; 92(13): Anderson H, Hopwood P, Stephens RJ, Thatcher N, Cottier B, Nicholson M, Milroy R, Maughan TS, Falk SJ, Bond MG, Burt PA, Connolly CK, McIllmurray MB, Carmichael J. Gemcitabine Plus Best Supportive Care (BSC) Vs BSC in Inoperable Non-Small Cell Lung Cancer-a Randomized Trial With Quality of Life As the Primary Outcome. UK NSCLC Gemcitabine Group. Non-Small Cell Lung Cancer. Br J Cancer 2000; 83(4): Roszkowski K, Pluzanska A, Krzakowski M, Smith AP, Saigi E, Aasebo U, Parisi A, Pham TN, Olivares R, Berille J. A Multicenter, Randomized, Phase III Study of Docetaxel Plus Best Supportive Care Versus Best Supportive Care in Chemotherapy-Naive Patients With Metastatic or Non-Resectable Localized Non-Small Cell Lung Cancer (NSCLC). Lung Cancer 2000; 27(3): Effects of Vinorelbine on Quality of Life and Survival of Elderly Patients With Advanced Non-Small-Cell Lung Cancer. The Elderly Lung Cancer Vinorelbine Italian Study Group. 1999; 91(1): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
133 75. Paesmans M, Sculier JP, Libert P, Bureau G, Dabouis G, Thiriaux J, Michel J, van Cutsem O, Sergysels R, Mommen P. Prognostic Factors for Survival in Advanced Non-Small-Cell Lung Cancer: Univariate and Multivariate Analyses Including Recursive Partitioning and Amalgamation Algorithms in 1,052 Patients. The European Lung Cancer Working Party. J Clin Oncol 1995; 13(5): Lilenbaum RC, Langenberg P, Dickersin K. Single Agent Versus Combination Chemotherapy in Patients With Advanced Nonsmall Cell Lung Carcinoma: a Meta-Analysis of Response, Toxicity, and Survival. Cancer 1998; 82(1): Gatzemeier U, von Pawel J, Gottfried M, ten Velde GP, Mattson K, DeMarinis F, Harper P, Salvati F, Robinet G, Lucenti A, Bogaerts J, Gallant G. Phase III Comparative Study of High-Dose Cisplatin Versus a Combination of Paclitaxel and Cisplatin in Patients With Advanced Non-Small-Cell Lung Cancer. J Clin Oncol 2000; 18(19): Wozniak AJ, Crowley JJ, Balcerzak SP, Weiss GR, Spiridonidis CH, Baker LH, Albain KS, Kelly K, Taylor SA, Gandara DR, Livingston RB. Randomized Trial Comparing Cisplatin With Cisplatin Plus Vinorelbine in the Treatment of Advanced Non-Small-Cell Lung Cancer: a Southwest Oncology Group Study. J Clin Oncol 1998; 16(7): Sandler AB, Nemunaitis J, Denham C, von Pawel J, Cormier Y, Gatzemeier U, Mattson K, Manegold C, Palmer MC, Gregor A, Nguyen B, Niyikiza C, Einhorn LH. Phase III Trial of Gemcitabine Plus Cisplatin Versus Cisplatin Alone in Patients With Locally Advanced or Metastatic Non-Small-Cell Lung Cancer. J Clin Oncol 2000; 18(1): von Pawel J, von Roemeling R, Gatzemeier U, Boyer M, Elisson LO, Clark P, Talbot D, Rey A, Butler TW, Hirsh V, Olver I, Bergman B, Ayoub J, Richardson G, Dunlop D, Arcenas A, Vescio R, Viallet J, Treat J. Tirapazamine Plus Cisplatin Versus Cisplatin in Advanced Non-Small-Cell Lung Cancer: A Report of the International CATAPULT I Study Group. Cisplatin and Tirapazamine in Subjects With Advanced Previously Untreated Non-Small-Cell Lung Tumors. J Clin Oncol 2000; 18(6): Vansteenkiste J, Vandebroek J, Nackaerts K, et al. Symptom Control in Advanced Non-Small Cell Lung Cancer: A Multi-Centre Propsective Randomised Phase III Study of Single Agent Gemcitabine Versus Cisplatin-Vindesine. Proc Am Soc Clin Oncol 2000; 19(488a). 82. Vansteenkiste J, Vandebroek J, Nackaerts K, et al. Gemcitabine Monotherapy Versus Cisplatin-Based Chemotherapy in Symptomatic Advanced Non Small Cell Lung Cancer: a Prospective Randomised Comparison of Symptom Control. Lung Cancer 2000; 29 (S1): Perng RP, Chen YM, Ming-Liu J, Tsai CM, Lin WC, Yang KY, Whang-Peng J. Gemcitabine Versus the Combination of Cisplatin and Etoposide in Patients With Inoperable Non-Small-Cell Lung Cancer in a Phase II Randomized Study. J Clin Oncol 1997; 15(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 113
134 84. Manegold C, Bergman B, Chemaissani A, Dornoff W, Drings P, Kellokumpu- Lehtinen P, Liippo K, Mattson K, van Pawel J, Ricci S, Sederholm C, Stahel RA, Wagenius G, van Walree N, ten Bokkel-Huinink W. Single-Agent Gemcitabine Versus Cisplatin-Etoposide: Early Results of a Randomised Phase II Study in Locally Advanced or Metastatic Non-Small-Cell Lung Cancer. Ann Oncol 1997; 8(6): Bonomi P, Kim K, Fairclough D, Cella D, Kugler J, Rowinsky E, Jiroutek M, Johnson D. Comparison of Survival and Quality of Life in Advanced Non-Small- Cell Lung Cancer Patients Treated With Two Dose Levels of Paclitaxel Combined With Cisplatin Versus Etoposide With Cisplatin: Results of an Eastern Cooperative Oncology Group Trial. J Clin Oncol 2000; 18(3): Giaccone G, Splinter TA, Debruyne C, Kho GS, Lianes P, van Zandwijk N, Pennucci MC, Scagliotti G, van Meerbeeck J, van Hoesel Q, Curran D, Sahmoud T, Postmus PE. Randomized Study of Paclitaxel-Cisplatin Versus Cisplatin- Teniposide in Patients With Advanced Non-Small-Cell Lung Cancer. The European Organization for Research and Treatment of Cancer Lung Cancer Cooperative Group. J Clin Oncol 1998; 16(6): Le Chevalier T, Brisgand D, Douillard JY, Pujol JL, Alberola V, Monnier A, Riviere A, Lianes P, Chomy P, Cigolari S. Randomized Study of Vinorelbine and Cisplatin Versus Vindesine and Cisplatin Versus Vinorelbine Alone in Advanced Non-Small-Cell Lung Cancer: Results of a European Multicenter Trial Including 612 Patients. J Clin Oncol 1994; 12(2): Cardenal F, Lopez-Cabrerizo MP, Anton A, Alberola V, Massuti B, Carrato A, Barneto I, Lomas M, Garcia M, Lianes P, Montalar J, Vadell C, Gonzalez-Larriba JL, Nguyen B, Artal A, Rosell R. Randomized Phase III Study of Gemcitabine-Cisplatin Versus Etoposide-Cisplatin in the Treatment of Locally Advanced or Metastatic Non-Small-Cell Lung Cancer. J Clin Oncol 1999; 17(1): Crino L, Scagliotti GV, Ricci S, De Marinis F, Rinaldi M, Gridelli C, Ceribelli A, Bianco R, Marangolo M, Di Costanzo F, Sassi M, Barni S, Ravaioli A, Adamo V, Portalone L, Cruciani G, Masotti A, Ferrara G, Gozzelino F, Tonato M. Gemcitabine and Cisplatin Versus Mitomycin, Ifosfamide, and Cisplatin in Advanced Non- Small-Cell Lung Cancer: A Randomized Phase III Study of the Italian Lung Cancer Project. J Clin Oncol 1999; 17(11): Shepherd F, Koschel G, von Pawel J, et al. Comparison of Tirazone (Tirapazamine) and Cisplatin Versus Etoposide and Cisplatin in Advanced Non- Small Cell Lung Cancer (NSCLC): Final Results of the International Phase III CATAPULT II Trial. Lung Cancer 2000; 29(S1): Fukuoka M, Nagao K, Ohashi Y, et al. Impact of Irinotecan (CPT 11)and Cisplatin (CDDP) on Survival in Previously Untreated Metastatic Non-Small Cell Lung Cancer (NSCLC). Proc Am Soc Clin Oncol 2000; 19(495a). 114 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
135 92. Klastersky J, Sculier JP, Lacroix H, Dabouis G, Bureau G, Libert P, Richez M, Ravez P, Vandermoten G, Thiriaux J. A Randomized Study Comparing Cisplatin or Carboplatin With Etoposide in Patients With Advanced Non-Small-Cell Lung Cancer: European Organization for Research and Treatment of Cancer Protocol J Clin Oncol 1990; 8(9): Jelic S, Radosavjelic D, Elezar E, et al. Survival advantage for carboplatin 500 mg/ m2 substituting cisplatin 120mg/m2 in combination with vindesine and mitomycin C in patients with stage IIIB and IV squamous cell bronchogenic carcinoma: a randomised study in 221 patients. Lung Cancer 18 (S1)[14] Gatzemeier U, Rosell R, Betticher D, et al. Randomised Pan-European Trial Comparing Paclitaxel (TAX)/Carboplatin (CAR) Versus Paclitaxel/Cisplatin (CIS) in Advanced Non-Small Cell Lung Cancer (NSCLC). Proc European Conference on Clinical Oncology Schiller JH, Harrington D, Sandler A. A Randomised Phase III Trial of Four Chemotherapy Regimens in Advanced Non-Small Cell Lung Cancer. Proc Am Soc Clin Oncol 2000; 19(1a). 96. Comella G, Frasci G, Panza N, et al. Cisplatin-Gemcitabine Vs Cisplatin- Gemcitabine-Vinorelbine Vs Cisplatin-Gemcitabine-Paclitaxel in Advanced Non-Small Cell Lung Cancer. Final Analysis of a Southern Italian Cooperative Oncology Group (SICOG) Phase III Trial. Ann Oncol 2000; 31(S4): Comella P, Frasci G, Panza N, Manzione L, De Cataldis G, Cioffi R, Maiorino L, Micillo E, Lorusso V, Di Rienzo G, Filippelli G, Lamberti A, Natale M, Bilancia D, Nicolella G, Di Nota A, Comella G. Randomized Trial Comparing Cisplatin, Gemcitabine, and Vinorelbine With Either Cisplatin and Gemcitabine or Cisplatin and Vinorelbine in Advanced Non-Small-Cell Lung Cancer: Interim Analysis of a Phase III Trial of the Southern Italy Cooperative Oncology Group. J Clin Oncol 2000; 18(7): Kosmidis P, Bacoyiannis C, Mylonakis N, et al. A Randomised Phase III Trial of Paclitaxel Plus Carboplatin Versus Paclitaxel Plus Gemcitabine in Advanced Non-Small Cell Lung Cancer (NSCLC). Proc Am Soc Clin Oncol 2000; 19(488a). 99. Kelly K, Crowley JJ, Bunn PAJ, et al. A Randomised Phase III Trial of Paclitaxel Plus Carboplatin (PC) Versus Vinorelbine Plus Cisplatin (VC) in Untreated Advanced Non-Small Cell Lung Cancer (NSCLC): A Southwest Oncology Group (SWOG) Trial. Proc Am Soc Clin Oncol 1999; 18(461a) Georgoulias V, Papadakis E, Alexopoulos A, Tsiafaki X, Rapti A, Veslemes M, Palamidas P, Vlachonikolis I. Platinum-Based and Non-Platinum-Based Chemotherapy in Advanced Non-Small-Cell Lung Cancer: a Randomised Multicentre Trial. Lancet 2001; 357(9267): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 115
136 101. Frasci G, Lorusso V, Panza N, Comella P, Nicolella G, Bianco A, De Cataldis G, Iannelli A, Bilancia D, Belli M, Massidda B, Piantedosi F, Comella G, De Lena M. Gemcitabine Plus Vinorelbine Versus Vinorelbine Alone in Elderly Patients With Advanced Non-Small-Cell Lung Cancer. J Clin Oncol 2000; 18(13): Kosmidis P, Mylonakis N, Skarlos D, Samantas E, Dimopoulos M, Papadimitriou C, Kalophonos C, Pavlidis N, Nikolaidis C, Papaconstantinou C, Fountzilas G. Paclitaxel (175 Mg/M2) Plus Carboplatin (6 AUC) Versus Paclitaxel (225 Mg/M2) Plus Carboplatin (6 AUC) in Advanced Non-Small-Cell Lung Cancer (NSCLC): a Multicenter Randomized Trial. Hellenic Cooperative Oncology Group (HeCOG). Ann Oncol 2000; 11(7): Font A, Moyano AJ, Puerto JM, Tres A, Garcia-Giron C, Barneto I, Anton A, Sanchez JJ, Salvador A, Rosell R. Increasing Dose Intensity of Cisplatin-Etoposide in Advanced Nonsmall Cell Lung Carcinoma: a Phase III Randomized Trial of the Spanish Lung Cancer Group. Cancer 1999; 85(4): Sculier JP, Lafitte JJ, Paesmans M, Thiriaux J, Alexopoulos CG, Baumohl J, Schmerber J, Koumakis G, Florin MC, Zacharias C, Berghmans T, Mommen P, Ninane V, Klastersky J. Phase III Randomized Trial Comparing Moderate-Dose Cisplatin to Combined Cisplatin and Carboplatin in Addition to Mitomycin and Ifosfamide in Patients With Stage IV Non-Small-Cell Lung Cancer. Br J Cancer 2000; 83(9): Smith IE, O Brien ME, Talbot DC, Nicolson MC, Mansi JL, Hickish TF, Norton A, Ashley S. Duration of Chemotherapy in Advanced Non-Small-Cell Lung Cancer: a Randomized Trial of Three Versus Six Courses of Mitomycin, Vinblastine, and Cisplatin. J Clin Oncol 2001; 19(5): Sockinski MA, Kies M, Schell MJ, et al. Duration of Therapy in Stage IIIB/IV Non- Small Cell Lung Cancer (NSCLC): A Multi-Institutional Phase III Trial. Proc Am Soc Clin Oncol 2001; 20(309a) Huisman C, Smit EF, Giaccone G, Postmus PE. Second-Line Chemotherapy in Relapsing or Refractory Non-Small-Cell Lung Cancer: a Review. J Clin Oncol 2000; 18(21): Shepherd FA, Dancey J, Ramlau R, Mattson K, Gralla R, O Rourke M, Levitan N, Gressot L, Vincent M, Burkes R, Coughlin S, Kim Y, Berille J. Prospective Randomized Trial of Docetaxel Versus Best Supportive Care in Patients With Non- Small-Cell Lung Cancer Previously Treated With Platinum-Based Chemotherapy. J Clin Oncol 2000; 18(10): Fossella FV, DeVore R, Kerr RN, Crawford J, Natale RR, Dunphy F, Kalman L, Miller V, Lee JS, Moore M, Gandara D, Karp D, Vokes E, Kris M, Kim Y, Gamza F, Hammershaimb L. Randomized Phase III Trial of Docetaxel Versus Vinorelbine or Ifosfamide in Patients With Advanced Non-Small-Cell Lung Cancer Previously Treated With Platinum-Containing Chemotherapy Regimens. The TAX 320 Non- Small Cell Lung Cancer Study Group. J Clin Oncol 2000; 18(12): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
137 6. SMALL CELL LUNG CANCER 6.1 Management of small cell lung cancer by stage 6.2 Chemotherapy and small cell lung cancer OCA and PE Alternating regimens Carboplatin versus cisplatin Oral etoposide Other regimens Maintenance therapy The optimum chemotherapy regimen Appropriate duration of chemotherapy Appropriate number of cycles of chemotherapy Dose escalation of chemotherapy Second-line chemotherapy Optimum second-line chemotherapy regimen 6.3 Radiotherapy Chest radiotherapy in limited stage small cell lung cancer Prophylactic cranial irradiation Other indications for thoracic radiotherapy Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 117
138 6.1 MANAGEMENT OF SMALL CELL LUNG CANCER BY STAGE Table 1 6 Management of small cell lung cancer stage by stage Optimal management If patient is not suitable for optimal management Limited Disease Platinum based chemotherapy (4 6 cycles) Palliative chemotherapy combined with thoracic radiotherapy +/- radiotherapy concomitant with first or second cycle Prophylactic cranial irradiation for complete responders Extensive Disease Combination chemotherapy (4 6 cycles) Symptom control Prophylactic cranial irradiation for complete responders 6.2 CHEMOTHERAPY AND SMALL CELL LUNG CANCER The recognition during the 1970s that SCLC is a systemic disease, best treated with chemotherapy, led to the relegation of radiotherapy to a secondary role in its management. Chemotherapy is associated with high response rates, but most patients subsequently relapse, and the efficacy of available cytotoxic drugs appears to have plateaued. Furthermore, observations in patients treated with chemotherapy alone revealed that the primary site, where the disease was usually bulkiest, and the brain, which is a chemotherapy sanctuary site, were common sites of treatment failure. Multimodality strategies designed to address these problems has resulted in a re-emergence of radiotherapy, particularly in the management of limited disease. As a result, about a quarter of patients with limited disease can now be cured with a combination of chemotherapy and radiotherapy, but the majority of patients who present with extensive disease will nearly all succumb to it. OCA AND PE The two most widely used regimens have been vincristine, adriamycin and cyclophosphamide (known variously as OCA, VAC, or CAV) and, more recently, cisplatin with etoposide (PE). Median survival of months in limited stage and 7 12 months in extensive stage SCLC have been routinely reported with either of these regimens. An analysis of results through the 1970s and 1980s for the control arms of 21 randomised phase III trials in extensive disease showed a modest improvement in median survival from 7.0 months, for patients enrolled between 1972 and 1981, to 8.9 months for the cohort 1. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 119
139 Impressive results have been achieved with four cycles of PE in a recent study. Four hundred and nineteen patients with limited stage disease received identical chemotherapy but were randomised to differing schedules of thoracic radiotherapy. Two-year survival was 41% and five-year survival 16% for once daily therapy, while twice daily therapy was better, yielding 47% survival at two years and 26% at five years 2. A number of studies have compared outcomes with OCA and PE. Larger trials have included a study from the Southeastern Cancer Study Group, where 437 patients with extensive stage disease were randomised to 12 weeks of PE, or 18 weeks of either OCA or OCA/PE alternating. There was no difference in response or survival between the PE and OCA arms 3. In a South Western Oncology Group (USA) (SWOG) study, 400 limited stage patients were randomised to a platinum-containing arm of alternating PE and OCA, versus etoposide, vincristine, adriamycin and cyclophosphamide. Median survival was months and was not different between the arms 4. In a study from Fukuoka, 288 patients with limited or extensive stage disease were randomised to PE, OCA, or an alternating regimen. Patients also received radiotherapy. Response rates were 78% with PE and 55% with OCA. There was no difference in survival between these two regimens, but there was significantly more toxicity (haematological and neurological) in the OCA arm 5. Two meta-analyses have looked at randomised trials comparing platinum-containing and non-platinum regimens. The first, from Pujol, included 18 trials, with a total of patients. Response rate was higher for cisplatin-containing regimens, with an odds ratio of 1.35 (p< ). Survival favoured cisplatin-containing regimens, with sixmonth survival 68% versus 65% and 12-month survival 29% versus 24%. The odds ratio for survival was 0.87 at six months (p=0.03) and 0.80 at 12 months (p=0.002). Results were unaltered when considering only trials where both arms included etoposide 6. The second meta-analysis included 36 trials, and focused on the role of etoposide as well as cisplatin. Only fully published trials were included. Overall survival benefit was shown for regimens containing cisplatin (OR 0.61, p<0.001) or etoposide (OR 0.65, p<0.001.) Nine trials, involving patients, specifically compared a regimen containing both cisplatin and etoposide versus a regimen containing neither drug. The meta-analysis favoured the PE combination (OR 0.57, p<0.001) 7. Neither of the meta-analyses examined individual patient data, however, despite this limitation, there is clear benefit for regimens containing both cisplatin and etoposide. A further consideration for patients undergoing radiotherapy is the toxicity of the chemotherapy regimen in this context. OCA is associated with greater toxicity than PE when combined with radiotherapy. If radiotherapy is to be administered concurrently with chemotherapy then a combination of a platinum agent and etoposide is suggested. 120 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
140 ALTERNATING REGIMENS In an effort to improve results, alternating or sequential regimens, particularly of OCA and PE, have been used. Results have, for the most part, not shown an advantage for any particular approach. There were no significant differences in outcome in a trial of 437 patients with extensive disease randomised to 12 weeks of PE, 18 weeks of OCA or 18 weeks of alternating OCA/PE 3. In a phase III SWOG trial, 400 patients with limited stage disease were randomised to alternating PE/OCA or a combination of etoposide with OCA, with chest radiotherapy. There were no significant differences in response rate or survival 4. In a study from the National Cancer Institute of Canada, 300 patients with limited disease were randomised to three cycles of OCA followed sequentially by three cycles of PE, or alternation of the two regimens. There were no observed differences in patient outcome between the regimens 8. In a study of 129 patients, following initial therapy with four cycles of PE, responding patients were randomised to no further treatment or to consolidation with OCA. Survival was no different between the arms, but toxicity was increased in the consolidation group 9. However, some studies have shown improved results with alternating regimens. Two hundred and eighty nine patients with extensive disease were randomised to receive OCA or OCA alternating with PE. Alternating therapy was associated with improved response rate and overall survival 10. Alternating PE/OCA was also superior to OCA in the trial from Fukuoka, but not significantly superior to PE alone 5. Positive results in these two trials may be interpreted as superiority of a platinum-containing regimen. In summary, the evidence for alternating regimens is inconsistent. The superiority of alternating therapy has not been clearly demonstrated. CARBOPLATIN VERSUS CISPLATIN Carboplatin has been widely used in Australia to replace cisplatin in the PE regimen 11, although few trials have compared carboplatin and cisplatin regimens. In a study from Greece, patients were randomised to either cisplatin and etoposide, or carboplatin and etoposide. Patients could also receive radiotherapy. One hundred and forty three patients were included, 82 with limited disease. There was no difference in response rate or overall survival between the two arms. However, there was less toxicity (neutropenic sepsis, emesis, nausea and vomiting, neurotoxicity) in the carboplatin arm 12. Lassen has reported on 484 patients randomised to either cisplatin or carboplatin in combination with teniposide and vincristine. In addition, the regimen was alternated with one of three other regimens. There was no difference in response, survival or toxicity rates between the cisplatin and carboplatin arms 13. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 121
141 ORAL ETOPOSIDE Oral etoposide has been investigated as a potential effective, low-toxicity oral regimen for SCLC in randomised trials. Souhami and colleagues randomised 155 patients to six cycles of either oral etoposide (100mg bd x 5d) or alternating PE/OCA. The study was closed early due to toxicity. One-year survival was worse in the oral etoposide arm than the intravenous arm (9.8% versus 19.3% respectively, p<0.05), with median survival 4.8 months versus 5.9 months. With the exception of chemotherapy-induced emesis, symptom control and quality of life favoured the intravenous regimen 14. The UK Medical Research Council Lung Cancer Working Party trial was also stopped after interim analysis. Three hundred and thirty nine patients were randomised to oral etoposide (50mg bd for 10d), or either OCA or PE. Survival was inferior in the oral arm (OR 1.35, p=0.03), with median survival 130 days versus 183 days for the intravenous arm. Survival at six months was 35% and 49%, and at 12 months 11% and 13% for the oral and intravenous regimens respectively. The palliative benefits were similar for each of the arms 15. These data indicate that oral etoposide is inferior treatment to combination intravenous regimens in terms of survival, with no additional quality of life or symptom control benefit. OTHER REGIMENS The role of ifosfamide has been examined in a phase III study of 162 patients with extensive stage disease. Patients were randomised to receive PE or PE plus ifosfamide. Median survival was longer in the ifosfamide arm, 9.1 months versus 7.3 months, with 12 month survival of 36% versus 27% respectively 16. A smaller randomised trial of 92 patients including both limited and extensive disease showed no difference in response rates or survival when ifosfamide was added to cisplatin/etoposide 17. Trial JCOG 9511, investigating irinotecan (CPT-11), has been reported in abstract form only. One hundred and fifty four patients with extensive disease were randomised to receive either cisplatin/etoposide or cisplatin/irinotecan (PI). The trial was stopped at interim analysis. Response rate was 67% with PE and 89% with PI (0=0.013). Median survival was 287 days with PE and 390 days with PI (p=0.004) 18. A confirmatory study is currently being undertaken. MAINTENANCE THERAPY A number of trials have examined the role of maintenance therapy in SCLC, generally without improvements in overall survival. Patients with limited or extensive stage disease received ifosfamide, etoposide and an anthracycline (doxorubicin or epirubicin). Responding patients (n=84) were randomised to maintenance etoposide and vindesine for 12 courses, or no further therapy. Progression-free survival was increased but survival was not significantly different 19. The ECOG 7593 trial has been reported in abstract form only. Patients with extensive stage disease received initially four cycles of cisplatin and etoposide. Those stable or responding were then randomised (n=227) to four additional cycles of topotecan or no further therapy. Progression-free survival was improved but overall survival and 12 month survival was no different Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
142 THE OPTIMUM CHEMOTHERAPY REGIMEN Guidelines Small Cell Lung Cancer Platinum as Optimal Chemotherapy Level of Evidence Refs Platinum containing regimens produce superior survival to that seen with other regimens. For patients with limited disease, when used in conjunction with thoracic irradiation, there is no evidence that any combination is superior to the doublet of cisplatin and etoposide. I 6,7 I 12,13 APPROPRIATE DURATION OF CHEMOTHERAPY Studies have compared four to six cycles of chemotherapy versus longer treatment durations. In a study including both limited and extensive stage disease, 265 patients were randomised to six or 12 cycles of chemotherapy. Survival was not different between the arms 21. Six hundred and ten patients, again of mixed stage, were randomised to receive either four or eight cycles of cyclophosphamide, etoposide, and vincristine. Time to progression was increased in the longer arm, but survival was no different as long as patients in the short arm received further chemotherapy at relapse 22. Giaccone has reported on 434 patients of mixed stage, randomised to either five or 12 cycles of cyclophosphamide, adriamycin and etoposide. Again, time to progression was increased in the longer treatment arm, but survival was no different. There was increased toxicity in the longer chemotherapy group 23. A study from Turrisi et al, where patients received four cycles of PE, highlighted the outcomes that may be achieved with short duration chemotherapy. Two-year survival for 419 patients with limited stage disease was 41 47%, and five-year survival was 16 26% 2. APPROPRIATE NUMBER OF CYCLES OF CHEMOTHERAPY Guideline Small Cell Lung Cancer Cycles of Chemotherapy Level of Evidence Refs Four to six cycles of chemotherapy should be given. II 2,21,22,23 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 123
143 DOSE ESCALATION OF CHEMOTHERAPY In the 1970s, a clinical correlation was seen between chemotherapy dose and response, where patients received either cyclophosphamide 700mg/m 2 or 1 500mg/m 2, along with carmustine and methotrexate 24. Subsequent trials have generally failed to confirm these findings. A meta-analysis of 60 randomised trials from the 1970s and 1980s investigated the role of dose intensity for a range of regimens. The range of variation in dose intensity was narrow. In extensive disease, there was no significant correlation between dose-intensity and survival, and results for limited disease were not consistent across regimens 25. Ihde compared standard-dose and high dose PE in 90 patients with extensive stage SCLC. High-dose PE was delivered during the first two cycles only. A 46% increase in dose intensity did not improve outcome 26. The dose-intense four drug CODE regimen (cisplatin, vincristine, adriamycin, etoposide), given over nine weeks, was compared with an 18 week OCA/PE regimen in a trial where 220 patients with extensive disease were randomised. Dose intensity was doubled, while the total dose of drugs delivered was the same for both arms. There were excessive treatment-related deaths in the CODE arm, and there was no difference in survival 27. In a trial of similar design, CODE plus the cytokine G-CSF, was compared with alternating OCA/PE. Two hundred and twenty seven extensive stage disease patients were randomised and there was no difference in survival between the arms 28. Positive results have been reported in a number of studies. In a small study of 63 patients with extensive stage disease, patients were randomised to receive CODE or CODE plus G-CSF. Dose intensity was increased in the G-CSF arm, with a significant improvement in survival, from 32 weeks to 59 weeks 29. In a large study, 300 patients with good or intermediate prognosis were randomised to receive V-ICE (vincristine, ifosfamide, cisplatin, etoposide) either every three or four weeks. Patients were further randomised to receive either GM-CSF or no cytokine. GM-CSF did not alter the incidence of febrile neutropenia or the survival rate. Patients in the more intensive chemotherapy arm had improved survival (p=0.0014), with two-year survival increased from 18% to 33% 30. In a similar design trial, 403 good prognosis patients were randomised to receive six cycles of adriamycin, cyclophosphamide and etoposide (ACE) at either two or three week intervals. Patients in the two-week interval arm also received G-CSF. The received dose intensity was increased 34% in the two-week arm, and survival was improved from 39% to 47% at 12 months 31. Patients in the studies did not receive thoracic irradiation; similar results may have been obtained if radiation was included. Further studies are needed before a dose-intense approach may be considered to be standard therapy. 124 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
144 SECOND-LINE CHEMOTHERAPY A frequent approach has been to treat with OCA on relapse following PE as first-line therapy, and vice versa. Where a good response was obtained with a first-line regimen, and the response was durable, 79% of patients responded to re-treatment with the same regimen in a small phase II study. The best results were obtained where there was a first-line complete remission and response duration was over eight months 32. There have been no randomised studies comparing this approach to use of an alternative regimen. Topotecan has been compared to OCA as second-line therapy in a randomised trial, where patients relapsed at least 60 days after primary chemotherapy. There was no significant difference in response rate, time to progression or survival. Symptom control (dyspnoea, fatigue, anorexia, hoarseness, interference with daily living) was superior in the topotecan group 33. A number of the other newer chemotherapy drugs have been shown to be efficacious for second-line therapy in SCLC, including paclitaxel 34 and irinotecan. OPTIMUM SECOND-LINE CHEMOTHERAPY REGIMEN Guidelines Small Cell Lung Cancer First and Second Line Chemotherapy Level of Evidence Refs Where a platinum agent and etoposide have been given first line, then appropriate second-line regimens include the combination of cyclophosphamide, adriamycin and vincristine, or single agent topotecan. These regimens are of similar efficacy. II 33 If first line chemotherapy has produced a response which has gone beyond eight months duration, it is reasonable to trial the first line drug again. III RADIOTHERAPY CHEST RADIOTHERAPY IN LIMITED STAGE SMALL CELL LUNG CANCER There is strong evidence for the role of thoracic radiotherapy in patients having radical treatment for SCLC. This topic has been reviewed in a number of randomised controlled trials and meta-analyses 35,36,37. Two meta-analyses were published in 1992 and both showed a benefit for thoracic radiotherapy. In the first analysis, the odds ratio for Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 125
145 benefit of radiotherapy on two-year survival was 1.52 (p<0.001) equating to a 5.4% increase in two-year survival. The addition of radiotherapy also improved local control by 25.3%, the odds ratio being 3.02 (p<0.0001). There was an excess of treatment related deaths in the combined treatment group with an odds ratio of 2.54 (p<0.01), but this only equated to a 1.2% difference in risk of treatment-related death. The second metaanalysis showed the same overall survival increase (5.4 ± 1.4%), but at three, not two years. The relative risk of death in the combined modality treatment group was 0.86 (p=0.001), corresponding to a 14% reduction in the mortality rate. Most studies indicate additional benefit if the radiotherapy is given early rather than late 2,38,39,40,41,42,43 although in one randomised study (criticised for its methodology) there was no benefit for initial versus late chest irradiation 44. A second randomised study showed no clear benefit for concurrent over sequential treatment 45. The studies showing improved survival have generally used a total dose of at least 40Gy in 15Gy fractions over three weeks (or a biologically equivalent dose). Hyperfractionated thoracic radiotherapy has been shown in one large, fully published study to increase the long-term survival of patients with limited SCLC (five-year survival, 26% with hyperfractionated thoracic radiotherapy versus 16% with once daily radiotherapy). This was achieved with an increased rate of short-term Grade 3 esophagitis 2. Guidelines Small Cell Lung Cancer Chemotherapy and Radiotherapy Level of Evidence Refs In patients with limited stage small cell lung cancer, the addition of thoracic radiotherapy to standard combination chemotherapy improves overall survival and should be incorporated into a comprehensive treatment plan. I 35,36,37 Thoracic radiotherapy should be offered early in relation to the course of chemotherapy rather than late. Evidence supports the administration of chemotherapy concurrent with radiotherapy over sequential chemotherapy-radiotherapy administration. II 2, 38, 39, 40, 41, 42, 43 Accelerated radiotherapy is associated with a survival advantage compared with standard fractionation. II Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
146 PROPHYLACTIC CRANIAL IRRADIATION There is strong evidence to recommend prophylactic cranial irradiation (PCI) for patients who have achieved complete remission following chemotherapy or chemoradiotherapy. Data from randomised controlled trials demonstrate that PCI decreases the frequency of brain metastases and increases disease free survival in these patients 46,47,48,49,50,51. An individual patient data meta-analysis of seven randomised trials showed a relative risk of death in the treatment group as compared to the control group of 0.84 (p=0.01), an increased rate of disease free survival relative risk of recurrence of 0.75 (p<0.001) and a decreased cumulative incidence of brain metastasis (RR 0.46, p<0.001) 52. The cumulative incidence of brain metastasis at three years was 58.6% in the control group compared with 33.3% in the treatment group. There may be a dose-response relationship in SCLC and a dose of 30Gy in 3Gy fractions or 36Gy in 2Gy fractions is recommended. In the study reported by Gregor 47, PCI delivered as a dose of 24Gy in 2Gy fractions was no better than no PCI, while 36Gy in 18Gy fractions significantly reduced CNS relapse. Other studies have shown this benefit with doses varying from 24Gy in 8Gy fractions to 40Gy in 20Gy fractions 47,48,49,50,51. On the basis of non-randomised data, it is recommended that PCI be given as soon as possible after patients achieve complete remission. Suwinski et al noted a threshold in dose-response when PCI was delayed, consistent with rapid growth of untreated sub-clinical disease in SCLC 53. There is evidence from randomised controlled trials with data for up to 30 months of follow-up that PCI does not produce significant late neurotoxicity 46,47. There is evidence from one randomised controlled trial that PCI does not have a detrimental effect on quality of life in the first 12 months following the completion of therapy. There is insufficient evidence to comment on the long-term effects of PCI on quality of life 47. Guideline Small Cell Lung Cancer Prophylactic Cranial Irradiation Level of Evidence Refs For patients who have achieved a complete response after induction therapy, prophylactic cranial irradiation is associated with a reduction in rate of brain metastases and prolongation of survival. I 52 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 127
147 OTHER INDICATIONS FOR THORACIC RADIOTHERAPY There is no evidence of any value in giving consolidation thoracic radiotherapy to patients with metastatic disease beyond the chest at presentation. The treatment from presentation onwards is palliative. The role of radiotherapy as a palliative modality conforms to palliation criteria in any disease entity or site. Patients who are referred for consolidation thoracic radiotherapy after poor response to chemotherapy must have their histology reviewed as the first step in their management. If they are true SCLC, their prognosis is poor regardless of stage, with an expected median survival of two to three months only. Radiation therapy for these patients is palliative and is given when symptoms indicate. References 1. Chute JP, Chen T, Feigal E, Simon R, Johnson BE. Twenty Years of Phase III Trials for Patients With Extensive-Stage Small-Cell Lung Cancer: Perceptible Progress. J Clin Oncol 1999; 17(6): Turrisi AT, Kim K, Blum R, Sause WT, Livingston RB, Komaki R, Wagner H, Aisner S, Johnson DH. Twice-Daily Compared With Once-Daily Thoracic Radiotherapy in Limited Small-Cell Lung Cancer Treated Concurrently With Cisplatin and Etoposide. N Engl J Med 1999; 340(4): Roth BJ, Johnson DH, Einhorn LH, Schacter LP, Cherng NC, Cohen HJ, Crawford J, Randolph JA, Goodlow JL, Broun GO. Randomized Study of Cyclophosphamide, Doxorubicin, and Vincristine Versus Etoposide and Cisplatin Versus Alternation of These Two Regimens in Extensive Small-Cell Lung Cancer: a Phase III Trial of the Southeastern Cancer Study Group. J Clin Oncol 1992; 10(2): Goodman GE, Crowley JJ, Blasko JC, et al. Treatment of Limited Small-Cell Lung Cancer With Etoposide and Cisplatin Alternating With Vincristine, Doxorubicin and Cyclophosphamide Versus Concurrent Etoposide, Vincristine, Doxorubicin and Cyclophosphamide and Chest Radiotherapy; a Southwest Oncology Group Study. J Clin Oncol 1990; 8: Fukuoka M, Furuse K, Saijo N, Nishiwaki Y, Ikegami H, Tamura T, Shimoyama M, Suemasu K. Randomized Trial of Cyclophosphamide, Doxorubicin, and Vincristine Versus Cisplatin and Etoposide Versus Alternation of These Regimens in Small-Cell Lung Cancer. J Natl Cancer Inst 1991; 83(12): Pujol JL, Carestia L, Daures JP. Is There a Case for Cisplatin in the Treatment of Small-Cell Lung Cancer? A Meta-Analysis of Randomized Trials of a Cisplatin- Containing Regimen Versus a Regimen Without This Alkylating Agent. Br J Cancer 2000; 83(1): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
148 7. Mascaux C, Paesmans M, Berghmans T, Branle F, Lafitte JJ, Lemaitre F, Meert AP, Vermylen P, Sculier JP. A Systematic Review of the Role of Etoposide and Cisplatin in the Chemotherapy of Small Cell Lung Cancer With Methodology Assessment and Meta-Analysis. Lung Cancer 2000; 30(1): Feld R, Evans WK, Coy P, Hodson I, MacDonald AS, Osoba D, Payne D, Shelley W, Pater JL. Canadian Multicenter Randomized Trial Comparing Sequential and Alternating Administration of Two Non-Cross-Resistant Chemotherapy Combinations in Patients With Limited Small-Cell Carcinoma of the Lung. J Clin Oncol 1987; 5(9): Beith JM, Clarke SJ, Woods RL, Bell DR, Levi JA. Long-Term Follow-Up of a Randomised Trial of Combined Chemoradiotherapy Induction Treatment, With and Without Maintenance Chemotherapy in Patients With Small Cell Carcinoma of the Lung. Eur J Cancer 1996; 32A(3): Evans WK, Feld R, Murray N, Willan A, Coy P, Osoba D, Shepherd FA, Clark DA, Levitt M, MacDonald A. Superiority of Alternating Non-Cross-Resistant Chemotherapy in Extensive Small Cell Lung Cancer. A Multicenter, Randomized Clinical Trial by the National Cancer Institute of Canada. Ann Intern Med 1987; 107(4): Bishop JF, Raghavan D, Stuart-Harris R, Morstyn G, Aroney R, Kefford R, Yuen K, Lee J, Gianoutsos P, Olver IN. Carboplatin (CBDCA, JM-8) and VP in Previously Untreated Patients With Small-Cell Lung Cancer. J Clin Oncol 1987; 5(10): Skarlos DV, Samantas E, Kosmidis P, Fountzilas G, Angelidou M, Palamidas P, Mylonakis N, Provata A, Papadakis E, Klouvas G. Randomized Comparison of Etoposide-Cisplatin Vs. Etoposide-Carboplatin and Irradiation in Small-Cell Lung Cancer. A Hellenic Co-Operative Oncology Group Study. Ann Oncol 1994; 5(7): Lassen U, Kristjansen PE, Osterlind K, Bergman B, Sigsgaard TC, Hirsch FR, Hansen M, Dombernowsky P, Hansen HH. Superiority of Cisplatin or Carboplatin in Combination With Teniposide and Vincristine in the Induction Chemotherapy of Small-Cell Lung Cancer. A Randomized Trial With 5 Years Follow Up. Ann Oncol 1996; 7(4): Souhami RL, Spiro SG, Rudd RM, Ruiz dem, James LE, Gower NH, Lamont A, Harper PG. Five-Day Oral Etoposide Treatment for Advanced Small-Cell Lung Cancer: Randomized Comparison With Intravenous Chemotherapy. J Natl Cancer Inst 1997; 89(8): Girling DJ. Comparison of Oral Etoposide and Standard Intravenous Multidrug Chemotherapy for Small-Cell Lung Cancer: a Stopped Multicentre Randomised Trial. Medical Research Council Lung Cancer Working Party. Lancet 1996; 348(9027): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 129
149 16. Loehrer PJS, Ansari R, Gonin R, Monaco F, Fisher W, Sandler A, Einhorn LH. Cisplatin Plus Etoposide With and Without Ifosfamide in Extensive Small-Cell Lung Cancer: a Hoosier Oncology Group Study. J Clin Oncol 1995; 13(10): Miyamoto H, Nakabayashi T, Isobe H, Akita H, Kawakami Y, Arimoto T, Asakawa M, Suzuki A, Fujikane T, Shimizu T,. A Phase III Comparison of Etoposide/Cisplatin With or Without Added Ifosfamide in Small-Cell Lung Cancer. Oncology 1992; 49(6): Noda K, Nishiwaki Y, Kawahara M, et al. Randomized Phase III study of irinotecan and cisplatin versus etoposide and cisplatin in extensive-disease small-cell lung cancer: Japan Clinical Oncology Group study (JCOG9511). 19, 483a ASCO. 19. Sculier JP, Paesmans M, Bureau G, Giner V, Lecomte J, Michel J, Berchier MC, van Cutsem O, Kustner U, Kroll F, Sergysels R, Mommen P, Klastersky J. Randomized Trial Comparing Induction Chemotherapy Versus Induction Chemotherapy Followed by Maintenance Chemotherapy in Small-Cell Lung Cancer. European Lung Cancer Working Party. J Clin Oncol 1996; 14(8): Johnson D, Adak S, Cella D, et al. Topotecan vs observation following cisplatin plus etoposide in extensive stage small cell lung cancer (E7593): a phase III trial of the Eastern Cooperative Oncology Group (ECOG). 19, 482a ASCO. 21. Controlled Trial of Twelve Versus Six Courses of Chemotherapy in the Treatment of Small-Cell Lung Cancer. Report to the Medical Research Council by Its Lung Cancer Working Party. Br J Cancer 1989; 59(4): Spiro SG, Souhami RL, Geddes DM, Ash CM, Quinn H, Harper PG, Tobias JS, Partridge M, Eraut D. Duration of Chemotherapy in Small Cell Lung Cancer: a Cancer Research Campaign Trial. Br J Cancer 1989; 59(4): Giaccone G, Dalesio O, McVie GJ, Kirkpatrick A, Postmus PE, Burghouts JT, Bakker W, Koolen MG, Vendrik CP, Roozendaal KJ. Maintenance Chemotherapy in Small- Cell Lung Cancer: Long-Term Results of a Randomized Trial. European Organization for Research and Treatment of Cancer Lung Cancer Cooperative Group. J Clin Oncol 1993; 11(7): Cohen MH, Creaven PJ, Fossieck BEJ, Broder LE, Selawry OS, Johnston AV, Williams CL, Minna JD. Intensive Chemotherapy of Small Cell Bronchogenic Carcinoma. Cancer Treat Rep 1977; 61(3): Klasa RJ, Murray N, Coldman AJ. Dose-Intensity Meta-Analysis of Chemotherapy Regimens in Small-Cell Carcinoma of the Lung. J Clin Oncol 1991; 9(3): Ihde DC, Mulshine JL, Kramer BS, Steinberg SM, Linnoila RI, Gazdar AF, Edison M, Phelps RM, Lesar M, Phares JC. Prospective Randomized Comparison of High- Dose and Standard-Dose Etoposide and Cisplatin Chemotherapy in Patients With Extensive-Stage Small-Cell Lung Cancer. J Clin Oncol 1994; 12(10): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
150 27. Murray N, Livingston RB, Shepherd FA, James K, Zee B, Langleben A, Kraut M, Bearden J, Goodwin JW, Grafton C, Turrisi A, Walde D, Croft H, Osoba D, Ottaway J, Gandara D. Randomized Study of CODE Versus Alternating CAV/EP for Extensive- Stage Small-Cell Lung Cancer: an Intergroup Study of the National Cancer Institute of Canada Clinical Trials Group and the Southwest Oncology Group. J Clin Oncol 1999; 17(8): Furuse K, Fukuoka M, Nishiwaki Y, Kurita Y, Watanabe K, Noda K, Ariyoshi Y, Tamura T, Saijo N. Phase III Study of Intensive Weekly Chemotherapy With Recombinant Human Granulocyte Colony-Stimulating Factor Versus Standard Chemotherapy in Extensive-Disease Small-Cell Lung Cancer. The Japan Clinical Oncology Group. J Clin Oncol 1998; 16(6): Fukuoka M, Masuda N, Negoro S, Matsui K, Yana T, Kudoh S, Kusunoki Y, Takada M, Kawahara M, Ogawara M, Kodama N, Kubota K, Furuse K. CODE Chemotherapy With and Without Granulocyte Colony-Stimulating Factor in Small-Cell Lung Cancer. Br J Cancer 1997; 75(2): Steward WP, von Pawel J, Gatzemeier U, Woll P, Thatcher N, Koschel G, Clancy L, Verweij J, de Wit R, Pfeifer W, Fennelly J, von Eiff M, Frisch J. Effects of Granulocyte-Macrophage Colony-Stimulating Factor and Dose Intensification of V-ICE Chemotherapy in Small-Cell Lung Cancer: a Prospective Randomized Study of 300 Patients. J Clin Oncol 1998; 16(2): Thatcher N, Girling DJ, Hopwood P, Sambrook RJ, Qian W, Stephens RJ. Improving Survival Without Reducing Quality of Life in Small-Cell Lung Cancer Patients by Increasing the Dose-Intensity of Chemotherapy With Granulocyte Colony- Stimulating Factor Support: Results of a British Medical Research Council Multicenter Randomized Trial. Medical Research Council Lung Cancer Working Party. J Clin Oncol 2000; 18(2): Postmus PE, Berendsen HH, van Zandwijk N, Splinter TA, Burghouts JT, Bakker W. Retreatment With the Induction Regimen in Small Cell Lung Cancer Relapsing After an Initial Response to Short Term Chemotherapy. Eur J Cancer Clin Oncol 1987; 23(9): von Pawel J, Schiller JH, Shepherd FA, Fields SZ, Kleisbauer JP, Chrysson NG, Stewart DJ, Clark PI, Palmer MC, Depierre A, Carmichael J, Krebs JB, Ross G, Lane SR, Gralla R. Topotecan Versus Cyclophosphamide, Doxorubicin, and Vincristine for the Treatment of Recurrent Small-Cell Lung Cancer. J Clin Oncol 1999; 17(2): Groen HJ, Van der Leest AHW, Snoek JD, et al. Phase III Study of Continuous Carboplatin Over 6 Weeks With Radiation Versus Radiation Alone in Stage III Non-Small Cell Lung Cancer. Proceedings of American Society of Clinical Oncology 1999; 18(466a). 35. Warde P, Payne D. Does Thoracic Irradiation Improve Survival and Local Control in Limited-Stage Small-Cell Carcinoma of the Lung? A Meta-Analysis. J Clin Oncol 1992; 10(6): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 131
151 36. Pignon JP, Arriagada R, Ihde DC, Johnson DH, Perry MC, Souhami RL, Brodin O, Joss RA, Kies MS, Lebeau B. A Meta-Analysis of Thoracic Radiotherapy for Small-Cell Lung Cancer. N Engl J Med 1992; 327(23): Arriagada R, Pignon JP, Ihde DC, Johnson DH, Perry MC, Souhami RL, Brodin O, Joss RA, Kies MS, Lebeau B. Effect of Thoracic Radiotherapy on Mortality in Limited Small Cell Lung Cancer. A Meta-Analysis of 13 Randomized Trials Among 2,140 Patients. Anticancer Res 1994; 14(1B): Bunn PAJ, Lichter AS, Makuch RW, Cohen MH, Veach SR, Matthews MJ, Anderson AJ, Edison M, Glatstein E, Minna JD. Chemotherapy Alone or Chemotherapy With Chest Radiation Therapy in Limited Stage Small Cell Lung Cancer. A Prospective, Randomized Trial. Ann Intern Med 1987; 106(5): Kies MS, Mira JG, Crowley JJ, Chen TT, Pazdur R, Grozea PN, Rivkin SE, Coltman CAJ, Ward JH, Livingston RB. Multimodal Therapy for Limited Small-Cell Lung Cancer: a Randomized Study of Induction Combination Chemotherapy With or Without Thoracic Radiation in Complete Responders; and With Wide-Field Versus Reduced-Field Radiation in Partial Responders: a Southwest Oncology Group Study. J Clin Oncol 1987; 5(4): Johnson DH, Bass D, Einhorn LH, Crawford J, Perez CA, Bartolucci A, Omura GA, Greco FA. Combination Chemotherapy With or Without Thoracic Radiotherapy in Limited-Stage Small-Cell Lung Cancer: a Randomized Trial of the Southeastern Cancer Study Group. J Clin Oncol 1993; 11(7): Takada M, Fukuoka M, Kawahara M, Sugiura T, Yokoyama A, Yokota S, Nishiwaki Y, Watanabe K, Noda K, Tamura T, Fukuda H, Saijo N. Phase III Study of Concurrent Versus Sequential Thoracic Radiotherapy in Combination With Cisplatin and Etoposide for Limited-Stage Small-Cell Lung Cancer: Results of the Japan Clinical Oncology Group Study J Clin Oncol 2002; 20(14): Murray N, Coy P, Pater JL, Hodson I, Arnold A, Zee BC, Payne D, Kostashuk EC, Evans WK, Dixon P. Importance of Timing for Thoracic Irradiation in the Combined Modality Treatment of Limited-Stage Small-Cell Lung Cancer. The National Cancer Institute of Canada Clinical Trials Group. J Clin Oncol 1993; 11(2): Takada M, et al. Phase III Study of Concurrent Versus Sequential Thoracic Radiotherapy in Combination With Cisplatin and Etoposide for Lmited Stage Small-Cell Lung Cancer: Preliminary Results of the Japan Clinical Oncology Group (JCOG). Proc Am Soc Clin Oncol 1996; 15: 372a. 44. Work E, Nielsen OS, Bentzen SM, Fode K, Palshof T. Randomized Study of Initial Versus Late Chest Irradiation Combined With Chemotherapy in Limited-Stage Small- Cell Lung Cancer. Aarhus Lung Cancer Group. J Clin Oncol 1997; 15(9): Perry MC, Herndon JE, Eaton WL, Green MR. Thoracic Radiation Therapy Added to Chemotherapy for Small-Cell Lung Cancer: an Update of Cancer and Leukemia Group B Study J Clin Oncol 1998; 16(7): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
152 46. Arriagada R, Le Chevalier T, Borie F, Riviere A, Chomy P, Monnet I, Tardivon A, Viader F, Tarayre M, Benhamou S. Prophylactic Cranial Irradiation for Patients With Small-Cell Lung Cancer in Complete Remission. J Natl Cancer Inst 1995; 87(3): Gregor A, Cull A, Stephens RJ, Kirkpatrick JA, Yarnold JR, Girling DJ, Macbeth FR, Stout R, Machin D. Prophylactic Cranial Irradiation Is Indicated Following Complete Response to Induction Therapy in Small Cell Lung Cancer: Results of a Multicentre Randomised Trial. United Kingdom Coordinating Committee for Cancer Research (UKCCCR) and the European Organization for Research and Treatment of Cancer (EORTC). Eur J Cancer 1997; 33(11): Aroney RS, Aisner J, Wesley MN, Whitacre MY, Van Echo DA, Slawson RG, Wiernik PH. Value of Prophylactic Cranial Irradiation Given at Complete Remission in Small Cell Lung Carcinoma. Cancer Treat Rep 1983; 67(7 8): Ohonoshi T, Ueoka H, Kawahara S, Kiura K, Kamei H, Hiraki Y, Segawa Y, Hiraki S, Kimura I. Comparative Study of Prophylactic Cranial Irradiation in Patients With Small Cell Lung Cancer Achieving a Complete Response: a Long-Term Follow-Up Result. Lung Cancer 1993; 10(1 2): Wagner H, et al. A Randomized Phase III Study of Prophylactic Cranial Irradiation (PCI) Vs Observation (OBS) in Patients (PTS) With Small Cell Lung Cancer (SCLC) Achieving a Complete Response: Final Report of an Incomplete Trial by the Eastern Cooperative Oncology Group and Radiation Therapy Oncology Group. Proc Am Soc Clin Oncol 1996; 15: Laplanche A, Monnet I, Santos-Miranda JA, Bardet E, Le Pechoux C, Tarayre M, Arriagada R. Controlled Clinical Trial of Prophylactic Cranial Irradiation for Patients With Small-Cell Lung Cancer in Complete Remission. Lung Cancer 1998; 21(3): Auperin A, Arriagada R, Pignon JP, Le Pechoux C, Gregor A, Stephens RJ, Kristjansen PE, Johnson BE, Ueoka H, Wagner H, Aisner J. Prophylactic Cranial Irradiation for Patients With Small-Cell Lung Cancer in Complete Remission. Prophylactic Cranial Irradiation Overview Collaborative Group. N Engl J Med 1999; 341(7): Suwinski R, Lee SP, Withers HR. Dose-Response Relationship for Prophylactic Cranial Irradiation in Small Cell Lung Cancer. Int J Radiat Oncol Biol Phys 1998; 40(4): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 133
153 SECTION IV SYMPTOM CONTROL 7. PALLIATIVE CARE 7.1 Palliative care for the person with lung cancer General Specialist versus generalist palliative care Timing of referral Sites of palliative care Own residence Acute hospital Inpatient hospices Symptom management Dyspnoea Pharmacological treatment of dyspnoea Palliative home oxygen therapy Cough Haemoptysis Malignant airway obstruction Pain management Morphine for cancer pain Anti-inflammatories and co-analgesics in cancer pain Constipation Outcomes in palliative care 7.2 Special problems in supportive care and care of advanced lung cancer Pleural effusion Pericardial effusion Unilateral vocal cord paralysis Hypercalcaemia: severe hypercalcaemia is a medical emergency Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 135
154 7.1 PALLIATIVE CARE FOR THE PERSON WITH LUNG CANCER GENERAL Hospice and palliative care has been defined as a concept of care that provides co-ordinated medical, nursing and allied services for people who are terminally ill, delivered where possible in the environment of the person s choice, and which provides physical, psychological, emotional and spiritual support for patients and for patients families and friends. The provision of hospice and palliative care services includes grief and bereavement support for the family and other carers during the life of the patient and continuing after death 1. Palliative care utilises advanced planning rather than crisis intervention. It offers a multidisciplinary model of care that is focused on the whole person within their social and emotional context, rather than just the disease. However, a good knowledge of the natural history of the disease and relevant oncological practice is essential for palliative care 2. Only one fifth of patients with lung cancer survive a year after diagnosis and have a significant burden of symptoms, emphasising the importance of palliative care in the management of the patient with lung cancer 3,4. A palliative approach, involving attention to symptom control and the psychological, social and spiritual wellbeing of the patient and their family is relevant at all stages of the disease, and it has been argued that attention to these aspects combined with understanding of the patients feelings and concerns all contribute to improving quality of life of the person with lung cancer 4. Although focussing on quality of life, palliative care is also concerned with the quality of dying. Recent work by Christakis and co-workers 5 has identified by focus group work with health professionals, patients and carers some attributes of a good death. The most important positive components were: good pain and symptom management, clear decision-making, preparation for death, completion, contributing to others, and affirmation of the whole person. Patients and families tended to fear bad dying more than death itself. It was found that doctors had a biomedical emphasis with substantially different priorities to the other groups. Patients particularly valued continuing opportunities to make contributions of gifts, time and knowledge to those around them. Attributes of a bad death included the lack of opportunity to plan ahead and arrange personal affairs, so as to decrease the burden on family, and to say goodbye. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 137
155 SPECIALIST VERSUS GENERALIST PALLIATIVE CARE Palliative care services have evolved in different ways, but in metropolitan areas specialist consultant palliative care services are generally available to give advice on symptom control and other problems, both in hospital and in the community. Access to hospice or specialist palliative care beds is also generally available. An evolving role is that of a specialist respiratory nurse to provide support for newly diagnosed cancer patients and palliative care 6. However, in rural and remote areas, this access is more limited. Consultations may be by telephone or video-conferencing and access to specialist inpatient care may be limited by distance. The British Thoracic Society Lung Cancer Guidelines recommend that all hospital cancer units should consider holding sessions with a palliative medicine physician to ensure good liaison between the hospital and community 7. This would also ensure optimum symptom control and early attention to psychological, emotional and social issues. Most palliative care will be provided by the existing network of carers, co-ordinated by either the general practitioner or treating respiratory physician or oncologist, who in turn draws upon the expertise of other health professionals when particular issues arise. The National Strategy for Palliative Care encourages the use of existing networks and community services in conjunction with palliative care specialists to deliver palliative care 8. As the availability of specialist palliative care increases specialist palliative care teams should be utilised to achieve optimum outcomes for the patient with lung cancer, particularly when treating complex or difficult to resolve issues. The involvement of a specialist palliative care team in the care of patients with cancer in general increases patient and carer satisfaction, increases the amount of time spent at home by patients, reduces the time spent in hospital, reduces the overall cost of care and increases the likelihood of the patient dying where they wish 9. Guideline Specialist Palliative Care Services Level of Evidence Refs Specialist palliative care services should be used to improve outcomes in the care of patients with cancer (lung cancer included). I Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
156 TIMING OF REFERRAL Early referral to a palliative care service will usually be helpful and will be facilitated if the palliative care health professionals are already an integral part of the multidisciplinary treatment team at the cancer centre or treating hospital 10,11. Referral to a palliative care service should be based on need, not on life expectancy 12, but early referral to a palliative care team allows the establishment of access and contacts, and exploration of options for future care without the need for immediate decisions. Early referral will facilitate subsequent continuity of care between hospital, home and hospice, and thus mitigate against any sense of abandonment 13,14,15. General practitioners, who continue to be involved in the ongoing care of the patient, often initiate palliative care. The concept of parallel care, suggesting a close and continuing co-operation between oncological and palliative services throughout the course of the illness, is particularly important for patients with lung cancer. The involvement of palliative care professionals does not preclude the continuation or commencement of chemotherapy, courses of radiotherapy, or other surgical or procedural interventions aimed at reducing tumour burden or relieving symptoms 16. However, the concurrent use of validated quality of life measurements, in conjunction with clinical trials looking at survival end-points, is particularly recommended in improving outcomes for patients with lung cancer 4 (refer also to guideline in Chapter 4, p74). SITES OF PALLIATIVE CARE Palliative care emphasizes that care is delivered where possible in the environment of the patient s choice. Good communication between health professionals is essential to ensure smooth transition from one site to another. OWN RESIDENCE This refers to either the patient s own home, the home of another, a nursing home or hostel. Increasingly, staff in nursing homes and hostels are being called on to deliver palliative care where resources to care for a dying resident may be limited 17,18. The general practitioner will be the key medical practitioner in delivering palliative care at home, usually with the assistance of community nurses. The local palliative care service will usually be able to add the support of specialist palliative care nurses and a specialist palliative care physician as well as counsellors, pastoral care workers and volunteers. Links with other community services mean that assistance can be accessed for physiotherapy, nutritional support, occupational therapy and home help 8. It is essential that the patient and family have access to support 24 hours a day, seven days a week if unnecessary hospital admissions are to be avoided, and that they know who to call in the event of a crisis. Preference for home care may decrease during the course of the illness and hospital admission for terminal care be requested 19. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 139
157 Although reliable data is limited, home care programs, where there is adequate support for the carers, are generally assessed favourably 19,20,21,22. Carers and relatives of terminally ill patients report more support was needed during care at home, particularly for activities of daily living and domestic chores 23. Families undertaking home care experienced higher levels of stress and social disruption than those whose relatives were cared for in institutions 24. ACUTE HOSPITAL Even when no further curative treatment is anticipated, situations arise which will be best treated in an acute hospital. These include orthopaedic management of a fracture or potential fracture, radiotherapy for a painful bone metastasis, superior vena caval obstruction or spinal cord compression, thoracentesis, treatment of hypercalcaemia or pain, and symptom control. A family caring for a patient at home may need respite for many reasons, and an acute hospital may be the only site available. As the illness progresses and the patient s strength and time are limited, hospital outpatient visits for review may be burdensome and should be minimized by liaison between the hospital specialist, the local palliative care team and the general practitioner. Where patients wish to continue their direct links with a specialist physician or hospital team, an effective level of contact should be achieved with priority based on patient need, preference and convenience. Despite the availability of community based palliative care and hospices, many patients still die in acute care hospitals. Attention to symptom control, psychological and emotional support for the patient and family, and agreement on the goals of care can allow death to occur peacefully even in this setting. It is vital that news of death in hospital be communicated to the general practitioner and community team as soon as possible, and suitable follow-up arranged. INPATIENT HOSPICES Admission for short periods may be required for symptom assessment and review of medication if new problems arise. Admission for respite may be required for family and patient relief. Direct admission from the acute hospital may be required where the patient is so functionally compromised and symptomatically burdened that they have needs that are unable to be provided in the community. This may be particularly so for patients suffering from severe dyspnoea associated with lung cancer. If the patient s condition improves or stabilises at an acceptable level, then discharge to home may be considered on a temporary or even day/weekend leave basis. 140 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
158 At times, although patients undertake the majority of their care at home, their wish may be for hospice care in the terminal phase to reduce the burden on family carers. This change in preference for hospice rather than home care highlights the importance of having adequate hospice beds available 19. It is important to be clear who bears the primary responsibility for care in each setting. Continuity of care can be provided through clear communication between all health care providers and the patient and family, so that accurate and detailed information about all aspects of the patient s condition, treatment and wishes is known. SYMPTOM MANAGEMENT Good symptom control is fundamental to the practice of oncology and is essential for supporting patients with progressive and advanced disease. Patients with advanced lung cancer experience more symptoms than patients with a range of other cancers including breast, colon and malignant melanoma 25. Although gradual resolution of distress is observed in most patients, high levels of physical symptoms and emotional distress persist in those with lung cancer, with declining physical abilities adversely affecting emotional wellbeing 26. Physical symptoms most commonly reported are pain, dyspnoea, anorexia and fatigue, with cough, haemoptysis and insomnia also highlighted 25. In a study of patients with poor prognosis SCLC and advanced NSCLC presenting for treatment, a multiplicity of symptoms (average symptoms) were reported from a variety of domains. The commonest psychological symptoms were worry and anxious feelings, common constitutional symptoms were tiredness, lack of energy, lack of appetite and difficulty sleeping, while the most common chest symptoms were shortness of breath and cough. Overall the symptoms most frequently reported as severe were decreased sexual interest, lack of energy and shortness of breath 27. In a prospective study of 100 consecutive lung cancer patients, 86% reported pain (moderate to severe in 70%), 70% had dyspnoea, 68% had anorexia, 52% reported constipation and 52% were easily fatigued. The median number of symptoms reported was nine 28. Patients with advanced lung cancer have the highest prevalence of dyspnoea of all cancer patients 28,29. A study of 289 NSCLC patients reported cough (79%), dyspnoea (75%), malaise (47%) and anorexia (45%) as the most frequent symptoms on presentation 30. In this group of patients who were treated by surgery, radiotherapy or best supportive care, dyspnoea and cough were not as well palliated as pain and haemoptysis. The presence of high symptom distress in newly diagnosed lung cancer patients is a predictor of reduced survival 31,32. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 141
159 The principles of symptom control, which are used as standard by clinicians include: assessment of the symptom, including understanding the meaning ascribed to it by the patient explanation of the likely cause investigations should only be undertaken if they will change the course of action to be followed institution of treatment based on the known or likely aetiology, available options for treatment, and the wishes of the patient monitoring of the response to treatment and modification as necessary. For guidelines on the management of symptoms not specifically addressed here, refer to Therapeutic guidelines: palliative care (first edition, September 2001). KEY POINT: Patients with lung cancer experience a high incidence of physical symptoms including fatigue, pain, dyspnoea, and cough requiring palliation during the course of their illness 25,27,28,29. DYSPNOEA Shortness of breath, or dyspnoea, is a term used to characterize a subjective experience of breathing discomfort that consists of qualitatively distinct sensations that vary in intensity. The experience derives from interactions among multiple physiological, social, and environmental factors, and may induce secondary physiological and behavioural responses 33. For patients it is impossible to separate the physical sensation from the emotional response 34. Patients report feelings of anxiety, fear and panic, frequently accompanied by a sense of impending death. Breathlessness is frequently intermittent, usually being triggered by exertion or occasionally, emotion. Shortness of breath imposes numerous restrictions on activity, functioning inside and outside the home, and social life 35. In one study of lung cancer patients, those with high dyspnoea scores had lower quality of life 36. The genesis and pathophysiology of dyspnoea is poorly understood, with multiple mechanisms possibly involved and patients using a range of descriptive terms. Intensity is possibly best measured using a visual analogue scale (VAS) while the Borg Category scale provides a range of descriptors and assesses the effect of exertion on the symptom 37. Objective measures of respiratory function using spirometry were not shown to be a reliable guide to subjective levels of dyspnoea reported by cancer patients using a visual analogue scale Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
160 In advanced lung cancer, dyspnoea is usually multifactorial. Reversible physical causes should be treated, such as: optimising management of pre-existing COPD with bronchodilators and steroids managing pleural effusion: thoracentesis, pleurodesis (pleuroperitoneal shunt) management of bronchial obstruction with laser, radiotherapy, stent 39 controlling cardiac failure using anticoagulation therapy for pulmonary embolism correcting anaemia treating infection controlling chest pain. The overriding principle of palliation remains is the treatment appropriate to the stage of the patient s illness and in accordance with their wishes and goals? Dyspnoea is usually associated with high levels of anxiety, and symptomatic treatments are aimed at reducing anxiety and the sensation of breathlessness. However, it may not be possible to relieve the symptom of dyspnoea completely 30,40,41. Non-pharmacological interventions for breathlessness in lung cancer have been reported to be successful, with improvement in distress from breathlessness, and functional capacity following three to six weeks of an integrative model of care involving breathing retraining, relaxation and teaching coping and adaptive strategies 34,42. Other nonpharmacological measures for reduction of dyspnoea include the use of a bedside fan, particularly directing cool air onto the cheeks 41,43,44. Acupuncture was effective in an open pilot study 45. Pharmacological treatment of dyspnoea Most studies of the role of opioids to reduce dyspnoea have been carried out in healthy subjects or in patients with COPD where there is little evidence to support their use 46,47. A few small, largely uncontrolled studies have looked at the role of morphine to relieve dyspnoea in patients with advanced cancer 48,49. In this very ill population of patients, high dropout rates occur. Side effects included increased sedation. Patients did report improvement in dyspnoea as rated on visual analogue scales 48,49. One randomised, placebo-controlled study of patients with dyspnoea and pain showed a reduction in dyspnoea with subcutaneous morphine 50. Morphine is recommended for symptomatic relief of dyspnoea on the basis of its action as a respiratory sedative and its possible role in resetting the sensitivity of the respiratory response to hypercapnea 51. Intermittent dosing is appropriate if dyspnoea is not continuous. The use of a concomitant antiemetic should be considered, and regular laxatives commenced. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 143
161 Nebulized morphine has been shown to be of benefit in some case series of cancer patients, particularly in relation to the quality of the dyspnoea reported, but randomised controlled trials are lacking and benefit is largely unproven 52,53,54,55,56. In one study which did demonstrate benefit, the effect appeared to be more pronounced in patients who were already using oral opioids, occurred within the first 24 hours, and patients needed to be able to tolerate the mask or mouthpiece used in the nebulized route 57. There is no consensus on the optimal drug, dose, or schedule for administration, but it has been suggested that the dose needs to be in the order of 20mg morphine sulphate (intravenous solution) 58. Bioavailability of nebulized morphine appears to be low 59, but it should not be assumed that it is safe to use oral and nebulized routes simultaneously. Nebulized morphine has resulted in bronchospasm, which has not been observed so far with nebulized fentanyl 51,60. Nebulized lignocaine at two dose levels has also been tried in a small series for breathlessness, but was no more effective than nebulized saline 61. Anxiolytics have also been used to relieve dyspnoea, and although results are not encouraging for long-term use, a trial of anxiolytic therapy on an individual basis is recommended 33. In unrelieved distress from severe dyspnoea, sedation using chlorpromazine, or a benzodiazepine such as diazepam or midazolam is recommended 51,62,65. Steroids may have a role in reducing dyspnoea by decreasing airway inflammation and oedema, particularly in lymphangitis carcinomatosis, and may also be useful temporarily in major airway obstruction 51. Palliative home oxygen therapy Home oxygen therapy is normally reserved for patients with demonstrated chronic hypoxaemia caused by chronic airflow obstruction. In these patients continuous oxygen therapy (for more than 15 hours/day) may improve quality of life and decrease mortality 63. For patients with dyspnoea associated with terminal lung cancer, the palliative effect of home oxygen may be over and above any effect on hypoxaemia. Supplemental oxygen has been shown to reduce dyspnoea in cancer patients who are hypoxic and symptomatic at rest 50. However, in another single-blinded cross over study of dyspnoeic cancer patients, half of whom had carcinoma of the lung and who had not previously used oxygen therapy, dyspnoea was relieved to the same extent by oxygen or medical air 64. The improvement in dyspnoea with oxygen could not be predicted by the level of hypoxia, and was potentiated by morphine and benzodiazepines but particularly benzodiazepines. 144 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
162 Guidelines Management of Dyspnoea Level of Evidence Refs Counselling, breathing retraining, relaxation, and teaching coping and adaptive strategies can improve dyspnoea and functional capacity in lung cancer patients. II IV Other non-pharmacological measures to be considered for dyspnoea include acupuncture as a complementary procedure. IV 34,45 A therapeutic trial of morphine and/or benzodiazepines is recommended for dyspnoea in patients with advanced cancer. Nebulized morphine can improve dyspnoea in some terminally ill lung cancer patients. A supervised therapeutic trial may be worthwhile. II IV III 3 IV ,58 Nebulized lignocaine has not proven to be better than nebulized saline in relief of breathlessness. IV 61 COUGH Cough has been reported as a symptom in 29 83% of palliative care patients 41,51. Persistent cough can be exhausting, can exacerbate chest wall pain, add to insomnia, and trigger vomiting at times. In patients with lung cancer, cough may be productive, with mucus, infected sputum, or blood expectorated, or non-productive, triggered by distortion of bronchial mucosa by endobronchial tumour. Other non-cancer causes of cough should be considered, such as cardiac failure, asthma or the use of angiotensin converting enzyme (ACE) inhibitors. Simple measures such as change in posture at night may help 55. Cough suppression by various linctuses often with codeine, pholcodeine, or dextramethorphan is usually first line. Their action may depend more on the sugar content, as only limited pharmacological activity has been detected at the dose of opioid included. Morphine has been demonstrated to suppress cough and other opioids including methadone have been recommended, but there is little evidence to choose one opioid from another for its anti-tussive effect 66,67. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 145
163 Nebulized lignocaine (5ml 1 2% up to four times daily) can be useful as a cough suppressant. The patient should fast immediately after use, but clear water is allowed and fasting only recommended for one hour in the palliative care setting 51,66,68. Nebulized bronchodilators should be available in case of bronchospasm 55. Inhaled sodium cromoglycate has been shown to reduce cough in NSCLC in one small randomised controlled trial 69. Expectorants and mucolytics appear to have little role. Nebulized saline can improve the effectiveness of coughing by loosening mucus. The use of antibiotics to treat a chest infection in a dying patient will need careful discussion with patient and family but may be indicated to improve comfort. If secretions are troublesome and the patient is unable to expectorate, measures to reduce secretions should be tried, for example hyoscine hydrobromide, atropine or glycopyrrolate 41,55. Guidelines Cough Suppression Level of Evidence Refs Oral opioids are recommended for suppression of non-productive cough in lung cancer. Inhaled sodium cromoglycate could be tried in cough from non-small cell lung cancer that is resistant to standard therapy. Nebulised lignocaine can be useful as a cough suppressant - special precautions need to be taken (see text). II 66,67 II 69 IV 51 HAEMOPTYSIS Haemoptysis can range from recurrent coughing of specks of blood, to massive, catastrophic haemorrhage (rare). It is important to exclude bleeding from other sites such as the nose or oropharynx. Radiotherapy or endobronchial laser may be used to control bleeding depending on the cause and prognosis. Oral fibrinolytic inhibitors, tranexamic acid and aminocaproic acid have been used in patients unable to undergo other treatments 70. Massive haemoptysis is widely feared, but occurs rarely. Even so, preparation is useful. If there has been a warning of prior smaller bleeds, it may be important to discuss further resuscitative steps, but the level of detail in this discussion is a matter for judgment. Opioids and a benzodiazepine such as midazolam or diazepam should be readily available, and can be injected intravenously (if available), the rate titrated to the patient s level of panic and consciousness 51, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
164 MALIGNANT AIRWAY OBSTRUCTION On occasions endobronchial lung malignancy may cause atelectasis, pneumonia or airway obstruction. Should the obstructive lesion be either inoperable or recurrent after previous resection the therapeutic options are limited. Chemotherapy is either ineffective or provides a brief response. Urgent radiotherapy can take several days to achieve an effect, so some mechanical or direct local approach may be necessary in the interval. The ability to manage acute airway obstruction can be life saving, airway relief should be expeditious and immediate, with low morbidity and mortality. It should not interfere with future definitive therapy. In patients with terminal malignancy, it should be economical in costs and should minimize hospitalisation 71. A number of techniques and appliances from coring out the tumour and application of cryotherapy to a range of stents, laser therapy and balloon dilatation are available. Reference to a succinct review of the subject is advised 71. PAIN MANAGEMENT Reported prevalence of pain in cancer patients in general ranges between 33 88% 72 increasing to 60 88% in advanced cancer. The majority of cancer pain should be controllable 72,73. Unrelieved or poorly controlled pain leads to increased anxiety about the future and general anxiety that interferes with daily living 74. Early recognition and accurate diagnosis is important. There may be more than one type of pain present and a detailed history for each pain is important. Recognition of the type of pain involved will lead to more accurate prescribing of analgesics and co-analgesics. Neuropathic pain can be recognised by words such as burning, pins and needles, or pain in the distribution of a nerve or dermatome, or the presence of allodynia (pain provoked by light touch). Table 1 7 Pain unrelated to the cancer or pain related to treatment Nociceptive pain syndromes: Somatic: Bone metastases Liver metastases-capsule distension Neuropathic pain syndromes associated with lung cancer: Mixed neuropathic and nociceptive pain syndromes: Visceral: Nodal metastases Mediastinal disease Pancoast syndrome (brachial plexus involvement from apical lung cancer) Post-thoracotomy neuropathic chest wall pain Neuropathic syndromes secondary to vertebral or para-vertebral metastases Tumour invasion of chest wall For example, mucositis from chemotherapy, dysphagia secondary to radiotherapy Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 147
165 Pain assessment includes: a detailed history of each pain, full examination, and psychosocial assessment a history of analgesics already used and the response to them investigations to confirm the diagnosis, depending on the stage of the disease and the treatment options contributions from the multidisciplinary team. Perception of pain in cancer will be influenced by the meaning of the pain for the patient. Worsening pain is often taken to mean disease progression, with the fear of escalating, uncontrolled pain and a painful death. Open discussion, allowing fears to be discussed, providing explanation of the symptom and reassurance of continued support is important. Analgesics are the mainstay of treatment of cancer pain but awareness of other modalities is important including psychological supportive therapies, relaxation, emotional support, massage and acupuncture. Anti-cancer therapies may be important for pain relief, for example, radiotherapy for bone pain or neuropathic pain (due to tumour compression of nerves). The treatment plan and follow-up program should be clearly communicated to all involved in caring; family, general practitioner and community services. Morphine for cancer pain Pain relief usually commences with regular mild analgesics for example, regular paracetamol, with appropriate co-analgesics (see below). Although the World Health Organization (WHO) method for control of cancer pain describes progression to a weak opioid, for example codeine with paracetamol 75, current palliative care practice does not recommend this step. The presence of paracetamol limits dose escalation leading to inadequate pain relief, and regular codeine can lead to severe constipation. Morphine is the drug of choice for moderate to severe cancer pain. Persistent pain calls for regular analgesia, with the aim of achieving pain relief at night and by day, and both at rest and on movement. Morphine has been safely used for cancer pain without development of tolerance or addiction, the most significant side effects being constipation, nausea and vomiting 76. However, many patients with lung cancer also have COPD, and the use of opioids has at times been limited by the fear of respiratory depression. Unlike normal experimental subjects and post-operative patients, opioidinduced respiratory depression did not occur in a group of cancer patients who were fully pain-controlled on a stable dose of oral morphine. A majority of this group had pre-existing COPD and/or carcinoma of the bronchus Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
166 The principles of pain relief using morphine (or any other opioid) include: Dose titration using a short acting formulation, for example, morphine mixture four hourly until stable 24 hour dose requirements are established. Introduction of a slow release formulation to provide continuous background analgesia. Provision of an immediate release formulation for breakthrough pain or for incident pain. Choice of the simplest available route for example oral, then subcutaneous or rectal. Anticipation of any side effects for example, prescribing an antiemetic for nausea (patients need to be warned of early side effects of possible nausea and some drowsiness initially), and introduction of regular laxatives to prevent constipation. If frequent breakthrough doses are required, the background dose should be increased in line with breakthrough requirements. In opioid prescribing there is no ceiling dose; the dose can be increased in response to unrelieved pain unless side effects supervene. Despite the emphasis on the oral route for drug delivery in palliative care, in the case of severe, uncontrolled pain, the intravenous route may be the most appropriate way to achieve rapid pain control. Many patients harbour concerns about addiction when using morphine, but their fears are unfounded 41,76. If pain is reduced by another modality, for example, radiotherapy to painful bone metastases or an apical lung cancer, then morphine can be reduced. This is usually done gradually, but if the dose reduction is not sufficient the side effects of nausea and drowsiness will reappear. If there are persistent side effects such as nausea, drowsiness or confusion, in the face of inadequate pain control, then the situation must be reassessed. If the pain is opioid responsive, it may be possible to change to another opioid and escalate the dose successfully, for example fentanyl, hydromorphone or methadone. Methadone is reemerging as having a useful role in poorly responsive pain, possibly due to N-methyl-Daspartate (NMDA) activity. Previous equianalgesic opioid dose tables should be ignored, as methadone dose equivalence varies with prior opioid dose. If the pain is poorly opioid-responsive, for example neuropathic pain, or bone pain, then co-analgesics should be introduced. Care should always be taken with opioid doses in the elderly and in the use of morphine in patients with renal failure. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 149
167 Guidelines Pain Management Level of Evidence Refs Unrelieved or poorly controlled pain leads to increased anxiety about the future and general anxiety that interferes with daily living. Management of moderate to severe cancer pain should include the appropriate introduction and dose titration of opioids. IV 74 IV 73,75 Anti-inflammatories and co-analgesics in cancer pain Non-steroidal anti-inflammatory drugs or the new cyclooxygenase (COX) II inhibitors appear to have an important role in cancer pain, particularly when there is bone pain or pain due to chest wall infiltration. The usual precautions and dose ceilings apply. A range of drugs has been used in neuropathic pain syndromes in other settings: tricyclic antidepressants membrane stabilising drugs including anti-convulsants local anaesthetics systemically or oral derivatives, for example, mexiletine, flecainide NMDA receptor antagonists, for example, ketamine steroids for nerve compression. Guideline Neuropathic Pain Management Level of Evidence Refs Extrapolation from therapeutic approaches to neuropathic pain in other diseases indicates that antidepressants and anti-convulsants offer effective palliation. I 78 Referral to a specialist pain clinic for consideration of a nerve block or spinal analgesia is recommended if pain is not well controlled. CONSTIPATION Constipation is a frequent and troublesome symptom in advanced cancer due to reduced mobility, reduced fibre and fluid intake and the use of opioids. In a lung cancer patient with dyspnoea, constipation can be a cause of severe distress. In one study of hospice inpatients, laxatives were required by 64% of those not using opioids and 87% of those using strong oral opioids 79. The use of fentanyl for analgesia is associated with less need 150 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
168 for laxatives than the use of morphine 80. The best laxative for terminally ill patients using opioids is yet to be determined, but in one study senna and lactulose showed equal efficacy, with senna being recommended on the basis of cost 81. Guideline Bowel Care Level of Evidence Refs The best laxative for terminally ill patients using opioids is yet to be determined. Senna and lactulose have shown equal efficacy. III 3 81 OUTCOMES IN PALLIATIVE CARE Studies already undertaken highlight the difficulty of capturing the complexity of the outcomes in palliative care for both the patients and their relatives 19,82. A number of outcome measures have been used in clinical audit in palliative care, but as yet there is no ideal tool 9. As symptoms worsen with increasing disease and approaching death, symptom assessment scales appear to reflect overall deterioration, rather than poor symptom control 83. Satisfaction with care has been suggested as a suitable outcome to assess quality of care 84. However, it has been argued that patient satisfaction ratings are uniformly high whatever model of care is examined and do not give useful information leading to change 20. One promising tool developed to measure family satisfaction with care in advanced cancer is the FAMCARE Scale 85. Cost-effectiveness of palliative care is rarely assessed. Increasing resources to better co-ordinate services for patients at home, to avoid the possibility of inefficient duplication of services to some patients and lack of services to others, resulted in a decrease in the overall cost of the services provided, particularly through avoiding inpatient admissions and utilisation of nurse home visits. There was no discernible difference to patient and family outcomes 86. A national study in the UK, where hospice and palliative care services are well established, demonstrated that there is still inadequate symptom control, particularly relating to pain and dyspnoea, as well as inadequate home services and difficulty in obtaining information 23. The need for education in palliative care and further resources was highlighted. (With acknowledgement to Clinical practice guidelines for the management of advanced breast cancer.) Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 151
169 7.2 SPECIAL PROBLEMS IN SUPPORTIVE CARE AND CARE OF ADVANCED LUNG CANCER PLEURAL EFFUSION The presence of an ipsilateral pleural effusion in association with a newly diagnosed NSCLC is a poor prognostic sign. Thoracocentesis should be performed with all the aspirated fluid sent for cytological evaluation including cell block preparation. If the cytology result is positive for malignant cells the prognosis is extremely poor and palliative management is appropriate including control of the malignant effusion if it recurs and causes symptoms. In the past this has often been done by intercostal tube drainage, with the tube left in place until the drainage falls to less than 100ml per day, and chemical pleurodesis by doxycycline or bleomycin. With the advent of thoracoscopic techniques the preferred approach now for recurrent symptomatic pleural effusion is thoracoscopic assessment under general anaesthetic, drainage of all the fluid and talc insufflation. This provides effective palliation provided the lung is capable of re-expansion. In a recent Australian review of this approach in 61 patients, 18 with lung cancer, the overall median survival was 220 days (115 days for lung cancer) and the 30 day mortality was zero. The ability to completely drain all fluid and obtain full lung expansion would appear to be a contributing factor 87. In patients with poor prognosis, or those in whom it is anticipated that chemotherapy will control the effusion, simple pleural aspiration may be sufficient to relieve symptoms. A retrospective audit of technique has been described which has identified a reduced rate of post-aspiration pneumothorax (p=0.0189) using an eight French gauge trocar and cannula, three way tap and sealed bag system 88. Guideline Management of Pleural Effusion Level of Evidence Refs Pleural effusion is best managed by talc insufflation following thoracoscopic exploration and complete drainage of fluid. IV 87 PERICARDIAL EFFUSION Symptomatic malignant pericardial effusions occur uncommonly in NSCLC and are a poor prognostic sign. Confirmation of the clinical diagnosis is by echocardiograph. If the effusion is of a significant size and causing right ventricular compression, it is best treated by pericardiocentesis under echocardiographic control by an experienced cardiologist. A pigtail catheter is inserted and left in place until there is minimal drainage and a sclerosing agent such as bleomycin can be instilled through the catheter prior to its removal Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
170 In NSCLC it is rarely indicated to proceed to a pericardial window for a malignant pericardial effusion secondary to the lung cancer. Guideline Management of Pericardial Effusion Level of Evidence Refs Pericardiocentesis can be safely performed under echocardiographic control. The outcome is effective. IV 89 UNILATERAL VOCAL CORD PARALYSIS Unilateral vocal cord paralysis is observed with both NSCLC and SCLC with significant mediastinal lymph node involvement on the left side. In this situation, treatment of the unilateral vocal cord paresis is palliation of significant symptoms, most commonly significant hoarseness, loss of volume, decreased phonation time and decreased vocal range as well as a significant incidence of aspiration 90,91. In NSCLC there is also an incidence of unilateral vocal cord paresis following radical surgery for centrally placed left sided lung cancers when the left recurrent laryngeal nerve may be damaged or deliberately divided in an attempt to provide curative surgical results 91. In these cases, depending on the stage of the disease, there may be prolonged survival with the symptoms related to the vocal paresis, as opposed to the former group, where the prognosis is poor and most patients do not survive 12 months. There are two principal procedures available; either injection laryngoplasty with teflon or thyroplasty, in which a window is created in the thyroid cartilage at the level of the vocal cords and a pre-fabricated dense hydroxyapatite implant is placed to bring the paralysed vocal cord to the midline. In the past, teflon injections were used more often but thyroplasty is becoming the procedure of choice because of a trend to superior voice and swallow outcomes. Following teflon laryngoplasty satisfactory phonation is achieved in over 85% of patients whilst the success rate with thyroplasty is slightly better, although the choice of procedure has not been subject to randomised study. Both procedures improve vocal and aspiration symptoms. HYPERCALCAEMIA: SEVERE HYPERCALCAEMIA IS A MEDICAL EMERGENCY (with acknowledgement to Clinical practice guidelines for the management of advanced breast cancer) Hypercalcaemia is a well recognised complication in lung cancer, occurring as a paraneoplastic phenomenon as well as in the presence of bone metastases. Among its many symptoms are thirst, polyuria, polydipsia, nausea and vomiting, constipation, muscle weakness, worsening of pain, confusion and obtundation. Mild cases may be difficult to recognise. In severe cases it can lead to death through renal failure, cardiac arrest or coma. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 153
171 Treatment of severe hypercalcaemia involves rehydration (with up to six litres per day of normal saline) plus a drug to stabilise calcium levels. Currently the best drugs belong to the bisphosphonate group, which includes pamidronate and sodium clodronate (see chapter 8, p169). Pamidronate is given intravenously over two to four hours in a dose of 30 90mg, depending on the level of serum calcium. It leads to lowering of serum calcium within 24 to 96 hours. It may be more effective than intravenous sodium clodronate in severe cases 92. References 1. Standards for Hospice and Palliative Care Provision Australian Association for Hospice and Palliative Care Inc. 2. Ashby MA, Kissane DW, Beadle GF, Rodger A. Psychosocial Support, Treatment of Metastatic Disease and Palliative Care. Med J Aust 1996; 164(1): Melville A, Eastwood A. A Wider Role in Managing Patients With Lung Cancer. Nurs Times 1998; 19 25;94(33): Montazeri A, Gillis CR, McEwen J. Quality of Life in Patients With Lung Cancer: a Review of Literature From 1970 to Chest 1998; 113(2): Steinhauser KE, Clipp EC, McNeilly M, Christakis NA, McIntyre LM, Tulsky JA. In Search of a Good Death: Observations of Patients, Families, and Providers. Ann Intern Med 2000; 132(10): Lowden B. The Care and Treatment of Lung Cancer. Nurs Times 1998; 94(9): Muers MF, Higgins BG, Johnston IDA, Rudolf M, Pearch SJ, Pickles H. British Thoracic Society Recommendations to Respiratory Physicians for Organising the Care of Patients With Lung Cancer. Thorax 1998; 53(Suppl 1): S1 S8. 8. National Palliative Care Strategy. A National Framework for Palliative Care Service Development Commonwealth Department of Health and Aged Care. 9. Hearn J, Higginson IJ. Outcome Measures in Palliative Care for Advanced Cancer Patients: a Review. J Public Health Med 1997; 19(2): von Gunten CF, Von Roenn JH, Johnson-Neely K, Martinez J, Weitzman S. Hospice and Palliative Care: Attitudes and Practices of the Physician Faculty of an Academic Hospital. Am J Hosp Palliat Care 1995; 12(4): Weissman DE, Griffie J. The Palliative Care Consultation Service of the Medical College of Wisconsin. J Pain Symptom Manage 1994; 9(7): Dudgeon DJ, Raubertas RF, Doerner K, O Connor T, Tobin M, Rosenthal SN. When Does Palliative Care Begin? A Needs Assessment of Cancer Patients With Recurrent Disease. J Palliat Care 1995; 11(1): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
172 13. McCusker J, Stoddard AM. Effects of an Expanding Home Care Program for the Terminally Ill. Med Care 1987; 25(5): Higginson IJ, Wade AM, McCarthy M. Effectiveness of Two Palliative Support Teams. J Public Health Med 1992; 14(1): Jones RV, Hansford J, Fiske J. Death From Cancer at Home: the Carers Perspective. BMJ 1993; 306(6872): NHMRC Clinical Practice Guidelines for the Management of Advanced Breast Cancer Canberra, NHMRC AGPS. 17. De Bellis A, Parker D. Providing Palliative Care in Australian Nursing Homes: Issues and Challenges. Geriaction 1998; 16(3): Parker D, De Bellis A. A Profile of Dying Residents in South Australian Nursing Homes. International Journal of Palliative Nursing 1999; 5(4): Hinton J. Can Home Care Maintain an Acceptable Quality of Life for Patients With Terminal Cancer and Their Relatives? Palliat Med 1994; 8(3): Hohl D. Patient Satisfaction in Home Care/Hospice. Nurs Manage 1994; 25(1): Di Mola G. Role and Evaluation of Palliative Home Care Services. Progress in Palliative Care 1995; 3(1): Dawson NJ. Need Satisfaction in Terminal Care Settings. Soc Sci Med 1991; 32(1): Addington-Hall J, McCarthy M. Dying From Cancer: Results of a National Population-Based Investigation. Palliat Med 1995; 9(4): Greer DS, Mor V. An Overview of National Hospice Study Findings. J Chronic Dis 1986; 39(1): Cooley ME. Symptoms in Adults With Lung Cancer. A Systematic Research Review. J Pain Symptom Manage 2000; 19(2): Ryan LS. Psychosocial Issues and Lung Cancer: a Behavioral Approach. Semin Oncol Nurs 1996; 12(4): Hopwood P, Stephens RJ. Symptoms at Presentation for Treatment in Patients With Lung Cancer: Implications for the Evaluation of Palliative Treatment. The Medical Research Council (MRC) Lung Cancer Working Party. Br J Cancer 1995; 71(3): Krech R, Davis J, Walsh D. Symptoms of Lung Cancer. Palliat Med 1992; 6: Vainio A, Auvinen A. Prevalence of Symptoms Among Patients With Advanced Cancer: an International Collaborative Study. Symptom Prevalence Group. J Pain Symptom Manage 1996; 12(1): Muers MF, Round CE. Palliation of Symptoms in Non-Small Cell Lung Cancer: a Study by the Yorkshire Regional Cancer Organisation Thoracic Group. Thorax 1993; 48(4): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 155
173 31. Kukull W, McCorkle R, Driever M. Journal of Psychosocial Oncology 1986; 4: Degner LF, Sloan JA. Symptom Distress in Newly Diagnosed Ambulatory Cancer Patients and As a Predictor of Survival in Lung Cancer. J Pain Symptom Manage 1995; 10(6): American Thoracic Society (1999). Dyspnea. Mechanisms, Assessment, and Management: a Consensus Statement. American Thoracic Society. Am J Respir Crit Care Med 1999; 159(1): Bailey C. Nursing As Therapy in the Management of Breathlessness in Lung Cancer. Eur J Cancer Care (Engl ) 1995; 4(4): O Driscoll M, Corner J, Bailey C. The Experience of Breathlessness in Lung Cancer. Eur J Cancer Care (Engl ) 1999; 8(1): Smith EL, Hann DM, Ahles TA, Furstenberg CT, Mitchell TA, Meyer L, Maurer LH, Rigas J, Hammond S. Dyspnea, Anxiety, Body Consciousness, and Quality of Life in Patients With Lung Cancer. J Pain Symptom Manage 2001; 21(4): Ripamonti C, Bruera E. Dyspnea: Pathophysiology and Assessment. J Pain Symptom Manage 1997; 13(4): Heyse-Moore L, Beynon T, Ross V. Does Spirometry Predict Dyspnoea in Advanced Cancer? Palliat Med 2000; 14(3): Witt C, Dinges S, Schmidt B, Ewert R, Budach V, Baumann G. Temporary Tracheobronchial Stenting in Malignant Stenoses. Eur J Cancer 1997; 33(2): Higginson I, McCarthy M. Measuring Symptoms in Terminal Cancer: Are Pain and Dyspnoea Controlled? J R Soc Med 1989; 82(5): Twycross RG. Symptom Control: the Problem Areas. Palliat Med 1993; 7 (Suppl): Corner J, Plant H, A Hern R, Bailey C. Non-Pharmacological Intervention for Breathlessness in Lung Cancer. Palliat Med 1996; 10(4): Kerr D. A Bedside Fan for Terminal Dyspnoea. The American Journal of Hospice Care 1989; Meek PM, Schwartz RM. Dyspnoea. Mechanisms, Assessment and Management: a Consensus Statement. American Journal Respiratory Crit Care Medicine 1999; 159: Filshie J, Penn K, Ashley S, Davis CL. Acupuncture for the Relief of Cancer-Related Breathlessness. Palliat Med 1996; 10(2): De Conno F, Spoldi E, Caraceni A, Ventafridda V. Does Pharmaclogical Treatment Affect the Sensation of Breathlessness in Terminal Cancer Patients? Palliat Med 1991; 5: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
174 47. Joffe D, Berend N. Assessment and Management of Dyspnoea. Respirology 1997; 2(1): Bruera E, Macmillan K, Pither J, MacDonald RN. Effects of Morphine on the Dyspnea of Terminal Cancer Patients. J Pain Symptom Manage 1990; 5(6): Boyd KJ, Kelly M. Oral Morphine As Symptomatic Treatment of Dyspnoea in Patients With Advanced Cancer. Palliat Med 1997; 11(4): Bruera E, de Stoutz N, Velasco-Leiva A, Schoeller T, Hanson J. Effects of Oxygen on Dyspnoea in Hypoxaemic Terminal-Cancer Patients. Lancet 1993; 342(8862): Ahmedzai S. Palliation of respiratory symptoms. Doyle D, Hanks G, McDonald N (eds). New York: Oxford University Press, Tooms A, McKenzie A, Grey H. Nebulised Morphine. Lancet 1993; 342(8879): Farncombe M, Chater S, Gillin A. The Use of Nebulized Opioids for Breathlessness: a Chart Review. Palliat Med 1994; 8(4): Peterson GM, Young RS, Dunne PF, Galloway JG, Parks TE. Pilot Study of Nebulised Morphine for Dyspnoea in Palliative Care Patients. Australian Journal of Hospital Pharmacy 1996; 26(5): Davis CL. ABC of Palliative Care. Breathlessness, Cough, and Other Respiratory Problems. BMJ 1997; 315(7113): Neudeck BL, Smith KM. Nebulized Morphine for the Treatment of Dyspnoea in Cancer Patients. Journal of Pharmacy Technology 1998; 14: Zeppetella G. Nebulized Morphine in the Palliation of Dyspnoea. Palliat Med 1997; 11(4): Ahmedzai S, Davis C. Nebulised Drugs in Palliative Care. Thorax 1997; 52 Suppl 2: S Chrubasik J, Wust H, Friedrich G, Geller E. Absorption and Bioavailability of Nebulized Morphine. Br J Anaesth 1988; 61(2): Worsley MH, MacLeod AD, Brodie MJ, Asbury AJ, Clark C. Inhaled Fentanyl As a Method of Analgesia. Anaesthesia 1990; 45(6): Wilcock A, Corcoran R, Tattersfield AE. Safety and Efficacy of Nebulized Lignocaine in Patients With Cancer and Breathlessness. Palliat Med 1994; 8(1): Walsh TD. Dyspnoea in Advanced Cancer. Lancet 1993; 342: Breslin AB, Colebatch HJ, Engel LA, Young IH. Adult Domiciliary Oxygen Therapy. The Thoracic Society of Australia and New Zealand. Med J Aust 1991; 154(7): Booth S, Kelly MJ, Cox NP, Adams L, Guz A. Does Oxygen Help Dyspnea in Patients With Cancer? Am J Respir Crit Care Med 1996; 153(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 157
175 65. Bruera E, Neumann CM. The Uses of Psychotropics in Symptom Management in Advanced Cancer. Psychooncology 1998; 7(4): Fuller RW, Jackson DM. Physiology and Treatment of Cough. Thorax 1990; 45(6): Luporini G, Barni S, Marchi E, Daffonchio L. Efficacy and Safety of Levodropropizine and Dihydrocodeine on Nonproductive Cough in Primary and Metastatic Lung Cancer. Eur Respir J 1998; 12(1): Dunlop RJ. Relief of Cough Associated With Bronchogenic Carcinoma. Current Therapeutics 1990; 31: Moroni M, Porta C, Gualtieri G, Nastasi G, Tinelli C. Inhaled Sodium Cromoglycate to Treat Cough in Advanced Lung Cancer Patients. Br J Cancer 1996; 74(2): Dean A, Tuffin P. Fibrinolytic Inhibitors for Cancer-Associated Bleeding Problems. J Pain Symptom Manage 1997; 13(1): Lung Cancer - Principles and Practice. Philadelphia: Lippincott Williams & Wilkins, Higginson IJ, Hearn J. A Multicenter Evaluation of Cancer Pain Control by Palliative Care Teams. J Pain Symptom Manage 1997; 14(1): Schug SA, Zech D, Dorr U. Cancer Pain Management According to WHO Analgesic Guidelines. J Pain Symptom Manage 1990; 5(1): Strang P. Existential Consequences of Unrelieved Cancer Pain. Palliat Med 1997; 11(4): Ventafridda V, Tamburini M, Caraceni A, De Conno F, Naldi F. A Validation Study of the WHO Method for Cancer Pain Relief. Cancer 1987; 59(4): Schug SA, Zech D, Grond S, Jung H, Meuser T, Stobbe B. A Long-Term Survey of Morphine in Cancer Pain Patients. J Pain Symptom Manage 1992; 7(5): Walsh TD. Opiates and Respiratory Function in Advanced Cancer. Recent Results Cancer Res 1984; 89: Collins SL, Moore RA, McQuay HJ, Wiffen P. Antidepressants and Anticonvulsants for Diabetic Neuropathy and Postherpetic Neuralgia: a Quantitative Systematic Review. J Pain Symptom Manage 2000; 20(6): Sykes NP. The Relationship Between Opioid Use and Laxative Use in Terminally Ill Cancer Patients. Palliat Med 1998; 12(5): Radbruch L, Sabatowski R, Loick G, Kulbe C, Kasper M, Grond S, Lehmann KA. Constipation and the Use of Laxatives: a Comparison Between Transdermal Fentanyl and Oral Morphine. Palliat Med 2000; 14(2): Agra Y, Sacristan A, Gonzalez M, Ferrari M, Portugues A, Calvo MJ. Efficacy of Senna Versus Lactulose in Terminal Cancer Patients Treated With Opioids. J Pain Symptom Manage 1998; 15(1): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
176 82. Rinck GC, van den Bos GA, Kleijnen J, de Haes HJ, Schade E, Veenhof CH. Methodologic Issues in Effectiveness Research on Palliative Cancer Care: a Systematic Review. J Clin Oncol 1997; 15(4): Rees E, Hardy J, Ling J, Broadley K, A Hern R. The Use of the Edmonton Symptom Assessment Scale (ESAS) Within a Palliative Care Unit in the UK. Palliat Med 1998; 12(2): Tierney AJ, Sladden S, Anderson J, King M, Lapsley I, Llewellyn S. Measuring the Costs and Quality of Palliative Care: a Discussion Paper. Palliat Med 1994; 8(4): Kristjanson LJ. Validity and Reliability Testing of the FAMCARE Scale: Measuring Family Satisfaction With Advanced Cancer Care. Soc Sci Med 1993; 36(5): Raftery JP, Addington-Hall JM, MacDonald LD, Anderson HR, Bland JM, Chamberlain J, Freeling P. A Randomized Controlled Trial of the Cost-Effectiveness of a District Co-Ordinating Service for Terminally Ill Cancer Patients. Palliat Med 1996; 10(2): Love D, White D, Kiroff G. Thoracoscopic Talc Pleurodesis for Malignant Pleural Effusion. ANZ J Surg 2003; 73(1 2): Thomas R, Maher J. Pneumothorax and Palliative Pleural Aspiration-an Audit of Technique. Palliat Med 1993; 7(2): Vaitkus PT, Herrmann HC, LeWinter MM. Treatment of Malignant Pericardial Effusion. JAMA 1994; 272(1): Kraus DH, Ali MK, Ginsberg RJ, Hughes CJ, Orlikoff RF, Rusch VW, Burt ME, McCormack PM, Bains MS. Vocal Cord Medialization for Unilateral Paralysis Associated With Intrathoracic Malignancies. J Thorac Cardiovasc Surg 1996; 111(2): Iseli TA, Brown CL, Sizeland AM, Berkowitz RG. Palliative Surgery for Neoplastic Unilateral Vocal Cord Paralysis. ANZ J Surg 2001; 71(11): Purohit OP, Radstone CR, Anthony C, Kanis JA, Coleman RE. A Randomised Double-Blind Comparison of Intravenous Pamidronate and Clodronate in the Hypercalcaemia of Malignancy. Br J Cancer 1995; 72(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 159
177 8. PALLIATIVE RADIATION 8.1 Thoracic symptoms 8.2 Superior vena cava obstruction 8.3 Spinal cord compression 8.4 Bone metastases Solitary lesions Pathological fractures Treatment of bone metastases Radiotherapy Chemotherapy Bisphosphonates Orthopaedic management Mechanisms of fracture and risk assessment General principles for prophylactic fixation 8.5 Brain metastases Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 161
178 8.1 THORACIC SYMPTOMS The Medical Research Council in the UK has published on a series of studies investigating the role of radiotherapy in the symptomatic management of locally advanced intrathoracic disease 1. Radiotherapy improved symptoms of haemoptysis, chest pain, dyspnoea and cough in 49 97% of patients studied. In the patient groups studied, there was no advantage with respect to palliation of symptoms in giving longer courses of radiotherapy, with poor prognosis patients gaining the same benefit from one fraction of radiotherapy compared to two, and in a slightly better prognosis group, two fractions of radiotherapy gave the same benefit as 10 fractions 1,2,3. A third study, in the series of studies in patients with good performance status, compared two fractions of treatment with a 13-fraction course. The two fraction group achieved more rapid palliation and had less dysphagia, but survival was longer in patients randomised to the higher dose 4. Similarly, a National Cancer Institute of Canada randomised study also showed improved survival in patients receiving 20Gy in five fractions when compared to patients receiving a single 10Gy fraction of treatment. This study again showed no difference in palliation of symptoms between the two trial arms 5. An Australian randomised study showed no benefit in adding 5-fluorouracil to a palliative course of radiotherapy, with an improved response rate in the combined treatment arm not being translated into better symptom control, but resulting in increased toxicity 6. A randomised study comparing endobronchial brachytherapy and external beam radiotherapy for palliation of symptoms from inoperable NSCLC showed external beam treatment provided better overall and more sustained palliation with fewer retreatments 7. A second randomised study which included patients with early stage disease, as well as more advanced cases (the rationale for treatment of these different groups is unclear) has shown that the addition of brachytherapy to external beam radiotherapy can provide short term improvement in dyspnoea scores, particularly in patients with obstructing tumours in the main bronchi causing atelectasis 8. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 163
179 Guidelines Radiotherapy in Palliation of Cancer Level of Evidence Refs Radiotherapy is an effective modality for the management of certain symptoms caused by uncontrolled intrathoracic disease, and short courses of radiotherapy are as effective as more fractionated regimens. There appears to be improved survival in patients with a good performance status receiving higher doses of palliative radiotherapy, compared to single or two fraction courses. External beam radiotherapy appears to provide better palliation compared to endobronchial brachytherapy, but brachytherapy might be of benefit in patients with endobronchial obstructing lesions. II 1,2,3 II 4,5,8 II 7,8 8.2 SUPERIOR VENA CAVA OBSTRUCTION Lung cancer accounts for approximately 80% of cases of superior vena cava obstruction (SVCO). Treatment without an effort to obtain a histological diagnosis cannot be justified (the complication rate of mediastinoscopy almost 100% successful in achieving a histological diagnosis is less than 5%) 9. The Cochrane Collaboration have conducted a systematic review of the subject and looked at 90 studies in which patients with either SCLC or NSCLC were accrued. The rates of relief of symptoms in SVCO in SCLC patients were 83% (216/260) and 76% (137/180) using chemotherapy and radiotherapy respectively, whilst synchronous chemo-radiotherapy provided relief of 87% patients (33/38). In NSCLC, radiotherapy relieved SVCO in 64% patients (105/165). Stent insertion relieved SVCO in 94% (135/143) of both SCLC and NSCLC patients 10. In a prospective randomised study looking at chemotherapy with or without radiotherapy in SCLC, 37 patients presented with SVCO. Nine of these relapsed or progressed during initial chemotherapy, but of the remaining 28 patients, 13 received chemotherapy alone and 15 chemotherapy and radiotherapy. This was, in effect, a subset analysis, and it did not show any benefit in adding radiotherapy after 12 weeks of cyclical chemotherapy Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
180 Guidelines Superior Vena Cava Obstruction in Cancer Level of Evidence Refs A histological diagnosis is desirable before treatment of superior vena cava obstruction. Chemotherapy on its own is effective in superior vena cava obstruction due to small cell lung cancer. IV 9 II 10, SPINAL CORD COMPRESSION Spinal cord compression is a medical emergency and urgent multidisciplinary management is advisable, with early diagnosis a powerful predictor of outcome 12. Patients who are known to have bony metastatic disease, and their carers, should be warned about the possibility and educated regarding the early symptoms of spinal cord compression, and encouraged to notify such symptoms as soon as possible. Primary medical carers should also be aware of the risks of spinal cord compression and paraplegia and the importance of prompt action. Symptoms suggestive of spinal cord compression should be investigated in the absence of signs. If spinal cord compression is suspected, whether on symptomatic or clinical grounds, the investigation of choice is MRI scan 13. MRI is non-invasive and the precise level or levels of cord compression can be ascertained. If MRI is not available, then plain x-rays and CT myelogram should be used 14. Dexamethasone should be started on suspicion of spinal cord compression and whilst awaiting assessment 15. A randomised study has shown that the addition of high-dose dexamethasone to radiotherapy for spinal cord compression improves gait function after treatment 16. Patients presenting with suspected spinal cord compression should be reviewed as early as possible by a radiation oncologist and considered for review by an orthopaedic surgeon or neurosurgeon with an interest and expertise in spinal problems. A recently reported randomised trial compared decompressive surgical resection followed by radiotherapy with radiotherapy alone in patients with spinal cord compression caused by metastasis from a variety of tumour sites, of which lung was the most common 17. Patients randomised to surgery retained the ability to walk significantly longer than those treated with radiotherapy alone, although survival was not significantly different between the arms. Based on this study, surgery followed by radiotherapy should be considered the treatment of choice in most patients. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 165
181 Surgical intervention should also be considered in the following situations: solitary vertebral compression in a patient without previous diagnosis of malignancy pathological fracture or dislocation causing compression progressive disease while on radiotherapy or in previously irradiated site. When surgery is not considered appropriate, radiotherapy should be started immediately. Patients who are ambulatory and retain bladder or bowel function prior to the commencement of radiotherapy have the most favourable neurological outcome 12,18,19. KEY POINTS: Spinal cord compression is a medical emergency and urgent multidisciplinary management is advisable. Patients who are ambulatory and retain bladder or bowel function prior to the commencement of radiotherapy have the most favourable neurological outcome 12,18,19. Guidelines Management of Metastatic Spinal Cord Compression Dexamethasone should be started on suspicion of spinal cord compression and whilst awaiting assessment. Level of Evidence II III 3 Refs If spinal cord compression is suspected, whether on symptomatic or clinical grounds the investigation of choice is MRI scan. Surgery followed by radiotherapy is the treatment of choice for spinal cord compression. When surgery is not considered appropriate, radiotherapy should be started immediately. Radiotherapy is considered as effective as surgery in achieving symptomatic relief. III 3 13,14 II 17 III 3 12,18, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
182 8.4 BONE METASTASES A significant proportion of patients with metastatic lung cancer will have bony metastases. Most will be painful and some lead to pathological fracture (approximately 9%) 20. Symptoms suggestive of bone metastasis such as persistent, severe or unexplained bone pain, particularly worse at night and interfering with sleep, warrant investigation, initially with a plain x-ray. A radioisotope bone scan may help determine the extent and number of metastases. CT or MRI scans may be useful if doubt remains about the diagnosis. SOLITARY LESIONS It is important to ensure that a solitary lesion is a metastasis before treatment. In such cases the clinical situation of the patient (for example, a long disease-free interval after initial treatment for lung cancer) is important and the use of bone biopsy should not be excluded. If x-ray and bone scan suggest a solitary metastasis in the vertebrae, MRI should be performed. This may reveal that the lesion is not solitary or that it has characteristics of a metastasis. PATHOLOGICAL FRACTURES A pathological fracture may be the first presentation of a bony metastasis. It is most common in the proximal femur. Orthopaedic referral is required if: 50% of bone cortex is lost in a long bone; pain is present with over 50% of vertebral body destruction and/or pedicle destruction without collapse; moderate deformity and collapse is present 21. TREATMENT OF BONY METASTASES The treatment of bony metastases has two aims: to reduce pain and to reduce the risk of fracture particularly in long bones. The available treatments include radiotherapy, chemotherapy, bisphosphonates and internal fixation/replacement (as discussed below). Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 167
183 RADIOTHERAPY Palliative radiotherapy is a very important modality in the management of metastatic bone pain. Over 40% of patients can expect at least 50% pain relief at one month, and just under 30% can expect complete pain relief at one month 20. Various schedules of treatment are used and randomised studies have not shown a marked difference in pain relief from any particular schedule 22. The pathophysiology of bone pain from metastases and the mechanism of pain relief from radiotherapy are unclear 23. Recent trials have shown that 8Gy single fraction is as efficacious for pain relief as other schedules 22,24,25,26,27,28. Further trials may define those patients who would benefit from fractionated radiotherapy 22. The optimum schedule following elective pinning of lytic lesions has not been determined. Lesions in long bones should be assessed in conjunction with an orthopaedic surgeon and if the risk of fracture is considered high enough, then elective internal fixation is indicated. This should always be followed by radiation treatment 29. The aim of the radiation is not only to relieve the pain but also to cause tumour regression and subsequent healing. In patients who have widespread bony lesions consideration can be given to single fraction hemi-body radiation treatment. Doses of 8Gy to the lower hemi-body and 6Gy to the upper hemi-body are well tolerated with modern anti-emetics, and are able to give considerable relief with little morbidity provided blood counts are satisfactory 30,31. Systemic radiation therapy with bone-seeking radioisotopes may be helpful when there is a preponderance of sclerotic lesions, although the evidence on which this is based relates predominantly to patients with breast and prostate cancer 32. Guidelines Radiotherapy in Management of Skeletal Metastases Level of Evidence Refs Palliative radiotherapy remains the most effective single modality for the treatment of local metastatic bone pain. In the treatment of skeletal metastases trials have shown that 8Gy single fraction is as efficacious for pain relief as other schedules. In patients who have widespread bony lesions consideration can be given to single fraction hemibody radiation palliation. IV 20 II 22,24,25, 26,27,28 III Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
184 CHEMOTHERAPY Chemotherapy is worth considering in people with bone metastases, particularly those multifocal, symptomatic disease not controlled by simpler measures. This includes people with many symptomatic bone metastases, and people with coexisting visceral metastases that need immediate treatment (see chapter 5.5, p97). BISPHOSPHONATES Bisphosphonates like clodronate, palmidronate and zoledronate inhibit osteoclastic bone resorption and have an established role in the treatment of hypercalcaemia associated with malignancy. Bisphosphonates improve pain in people with symptomatic bone metastases from solid tumours including lung cancer 33,34,35. Bisphosphonates also reduce the incidence of skeletal events in people with multiple myeloma or bone metastases from breast cancer 33,36. A study recently reported in abstract form suggests that bisphosphonates may also reduce the rate of skeletal events in people with a range of solid tumours, including NSCLC 37. Bisphosphonates are generally well tolerated and the risk of serious side effects is low. The most common side effects of parenteral bisphosphonates are fever, flare of bone pain and myalgia in the 24 hours after infusion. Oral bisphosphonates may cause oesophogeal discomfort and irritation. Guideline Bisphosphonates in Management of Bone Metastases Level of Evidence Refs Bisphosphonates improve pain in people with symptomatic bone metastases from lung cancer. I 33,34,35 ORTHOPAEDIC MANAGEMENT Whilst radiotherapy can relieve bone pain when no significant mechanical failure has occurred, it is quite ineffective in circumstances in which a fracture in a weight-bearing bone has occurred or is inevitable. Orthopaedic management falls into three categories: prophylactic fixation of long bone deposits, where there is a risk of fracture stabilisation or reconstruction following pathological fracture decompression of the spinal cord and nerve roots, followed by stabilisation of the affected vertebra. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 169
185 MECHANISMS OF FRACTURE AND RISK ASSESSMENT As a general rule, when 50% of a cortex in a long bone has been destroyed fracture is likely 26. Prophylactic fixation should be performed prior to radiotherapy. Avulsion of the lesser tuberosity is an indication of imminent hip fracture. Any erosion of the femoral neck is an indication for prophylactic fixation. GENERAL PRINCIPLES FOR PROPHYLACTIC FIXATION ARE THAT: the procedure should provide immediate stability the surgeon must assume that the fracture will not unite the fixation should aim to last the lifetime of the patient Whatever implant is used should restore sufficient strength to allow immediate unsupported use. In the lower limb, this includes weight bearing. If the implant alone cannot satisfy these criteria, it might need supplementation by other material such as cement, bone substitutes or endoprostheses 38. Intramedullary nailing is indicated in fractures of the shaft of the femur, tibia or humerus. Osteosynthesis with a plate has only limited indications and should never be used in the lower limb. Cement, ceramic rings or one of the newer bone substitutes should be added to achieve immediate axial stability 29. Intramedullary nailing of femoral lesions is associated with a significant risk of intraoperative embolism and death. Unpublished data suggest a significant risk of acute oxygen desaturation during surgery. Such procedures need adequate monitoring and preventative measures. Non-weight bearing bones, such as ribs, fibula and much of the pelvis, can be safely treated with radiotherapy alone in most cases. The whole of the bone that has a metastasis should be imaged to ensure that the most appropriate fixation is used. Patients with multiple deposits should have all lesions at risk treated, if possible. This aids nursing care and the provision of radiotherapy. If the patient is in the terminal phase of their illness, the limb should be splinted and the limb made comfortable. 170 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
186 8.5 BRAIN METASTASES Cerebral metastases are common in lung cancer. The most common symptoms are focal neurological signs, headache, confusion, personality changes, nausea and vomiting. Diagnosis is made by history, physical examination and CT and/or MRI scan. There is a lot of non-randomised evidence that prognostic factors are of overwhelming importance in determining outcome in patients with intracranial metastatic disease and careful assessment of patients is therefore vital 39,40,41. It is important to distinguish true cerebral metastatic disease from meningeal disease or bony disease of the skull impinging on the brain or base of the skull causing cranial nerve damage, as treatment will differ. There is evidence that resection of a solitary intracranial metastasis followed by radiotherapy potentially results in increased local control and a longer disease-free survival than radiotherapy alone 40,42. It follows that patients presenting with an apparent solitary intracranial metastatic lesion should be staged to exclude extracranial metastatic disease, and the solitary nature of the brain metastasis confirmed with an MRI scan, if only a CT scan was performed to make the diagnosis. Stereotactic radiosurgery may be an alternative to surgical resection of a solitary brain metastasis 43,44 and has been shown to be of benefit in patients with two to four intracranial metastases, in addition to whole-brain radiotherapy 45. Metastases involving the cerebellum may require early intervention owing to their tendency to cause obstructive hydrocephalus and raise intracranial pressure. For this reason, these lesions are best managed with neurosurgical resection in patients who are fit enough. Radiotherapy on its own is not recommended. Cerebral metastatic disease is rarely a medical emergency but does require early diagnosis and evaluation. Radiotherapy to the whole brain has been an accepted standard of care for patients with brain metastases 46,47,48. At least four randomised trials carried out by the Radiotherapy Oncology Group (RTOG) in America, the Royal College of Radiologists in Britain and a French group compared different whole brain radiotherapy doses ranging from 10Gy in a single fraction to 40Gy in 20 fractions, and showed no differences in symptom response rates or times to disease progression according to dose/fractionation schedule 39,48,49,50. The overall response rate of symptoms of cerebral metastases to radiotherapy is around %, depending upon symptom type 39. The main side effect of radiotherapy to the whole brain is inevitable complete alopecia. Hair will usually regrow after a two to three month period although it may be less dense than previously. Other acute side effects include lethargy, nausea, vomiting, headaches and ataxia, which altogether occur in around 10% of patients 39. Dexamethasone is particularly useful in reducing cerebral oedema 51. Re-irradiation for progressive brain metastases may be considered in selected patients without progressive disease at other sites 52. Key point: The overall response rate of symptoms of cerebral metastases to radiotherapy is around %, depending upon symptom type 39. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 171
187 Guidelines Irradiation and Radiotherapy for Skeletal Metastases Level of Evidence Refs Radiotherapy is effective palliation for brain metastases from lung cancer. II 39,46,47,48 Resection of solitary cerebral metastases followed by radiotherapy potentially results in increased local control and a longer disease-free survival than radiotherapy alone. III 2 III 3 40,42 43 Stereotactic radiosurgery may be a suitable alternative to resection. Doses of whole brain radiotherapy ranging from 10Gy in a single fraction to 40Gy in 20 fractions have similar effectiveness in symptom palliation and times to disease progression. Shorter courses, for example 20Gy in five fractions, are recommended because of patient convenience. Re-irradiation for progressive brain metastases may be considered in selected patients without progressive disease at other sites. III 3 43, 44 II 39,48,49,50 IV 52 (This section on spinal cord compression, bony and brain metastases has been adapted with the permission of the National Breast Cancer Centre, from Management of Advanced Breast Cancer Clinical Practice Guidelines. NHMRC-NBCC Canberra, January 2001, pp 90 1.) References 1. A Medical Research Council (MRC) Randomised Trial of Palliative Radiotherapy With Two Fractions or a Single Fraction in Patients With Inoperable Non-Small Cell Lung Cancer (NSCLC) and Poor Performance Status. Br J Cancer 1992; 65: Rees GJ, Devrell CE, Barley VL, Newman HF. Palliative Radiotherapy for Lung Cancer: Two Versus Five Fractions. Clin Oncol (R Coll Radiol) 1997; 9(2): Inoperable Non-Small Cell Lung Cancer (NSCLC): A Medical Research Council Randomised Trial of Palliative Radiotherapy With Two Fractions or Ten Fractions. Br J Cancer 1991; 63: Macbeth FR, Bolger JJ, Hopwood P, Bleehen NM, Cartmell J, Girling DJ, Machin D, Stephens RJ, Bailey AJ. Randomized Trial of Palliative Two-Fraction Versus More Intensive 13-Fraction Radiotherapy for Patients With Inoperable Non-Small Cell Lung Cancer and Good Performance Status. Medical Research Council Lung Cancer Working Party. Clin Oncol (R Coll Radiol) 1996; 8(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
188 5. Randomized Study of Single Versus Fractionated Radiotherapy (RT) in the Palliation of Non-Small Cell Lung Cancer; NCIC CTG SC 15. Int J Radiat Oncol Biol Phys 2001; 51: Ball D, Smith J, Bishop J, Olver I, Davis S, O Brien P, Bernshaw D, Ryan G, Millward M. A Phase III Study of Radiotherapy With and Without Continuous-Infusion Fluorouracil As Palliation for Non-Small-Cell Lung Cancer. Br J Cancer 1997; 75(5): Stout R, Barber P, Burt P, Hopwood P, Swindell R, Hodgetts J, Lomax L. Clinical and Quality of Life Outcomes in the First United Kingdom Randomized Trial of Endobronchial Brachytherapy (Intraluminal Radiotherapy) Vs. External Beam Radiotherapy in the Palliative Treatment of Inoperable Non-Small Cell Lung Cancer. Radiother Oncol 2000; 56(3): Langendijk H, de Jong J, Tjwa M, Muller M, ten Velde G, Aaronson N, Lamers R, Slotman B, Wouters M. External Irradiation Versus External Irradiation Plus Endobronchial Brachytherapy in Inoperable Non-Small Cell Lung Cancer: a Prospective Randomized Study. Radiother Oncol 2001; 58(3): Ostler PJ, Clarke DP, Watkinson AF, Gaze MN. Superior Vena Cava Obstruction: a Modern Management Strategy. Clin Oncol (R Coll Radiol) 1997; 9(2): Rowell NP, Gleeson FV. Steroids, Radiotherapy, Chemotherapy and Stents for Superior Vena Caval Obstruction in Carcinoma of the Bronchus (Cochrane Review). Cochrane Database Syst Rev 2001; 4: CD Spiro SG, Shah S, Harper PG, Tobias JS, Geddes DM, Souhami RL. Treatment of Obstruction of the Superior Vena Cava by Combination Chemotherapy With and Without Irradiation in Small-Cell Carcinoma of the Bronchus. Thorax 1983; 38(7): Maranzano E, Latini P. Effectiveness of Radiation Therapy Without Surgery in Metastatic Spinal Cord Compression: Final Results From a Prospective Trial. Int J Radiat Oncol Biol Phys 1995; 32(4): Williams MP, Cherryman GR, Husband JE. Magnetic Resonance Imaging in Suspected Metastatic Spinal Cord Compression. Clin Radiol 1989; 40(3): Hoskin P. Radiotherapy in symptom management. Textbook of Palliative Medicine. Oxford, 1993: Cairncross JG, MacDonald DR. Central nervous system emergencies. Manual of Oncologic Therapeutics 1991/1992.J B Lippincott Company, Sorensen S, Helweg-Larsen S, Mouridsen H, Hansen HH. Effect of High-Dose Dexamethasone in Carcinomatous Metastatic Spinal Cord Compression Treated With Radiotherapy: a Randomised Trial. Eur J Cancer 1994; 30A(1): Patchell RA, Tibbs PA, Regine WF, Payne R, Saris S, Kryscio RJ, Young B. A randomised trial of direct decompressive surgical resection in the treatment of spinal cord compression caused by metastasis. Proc Am Soc Clin Oncol 22[1] Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 173
189 18. Turner S, Marosszeky B, Timms I, Boyages J. Malignant Spinal Cord Compression: a Prospective Evaluation. Int J Radiat Oncol Biol Phys 1993; 26(1): Findlay GF. Adverse Effects of the Management of Malignant Spinal Cord Compression. J Neurol Neurosurg Psychiatry 1984; 47(8): McQuay HJ. Radiotherapy for the palliation of painful bone metastases. Vol The Cochrane Database of Systematic Reviews. 21. DeWald RL, Bridwell KH, Prodromas C, Rodts MF. Reconstructive Spinal Surgery As Palliation for Metastatic Malignancies of the Spine. Spine 1985; 10(1): Nielsen OS, Bentzen SM, Sandberg E, Gadeberg CC, Timothy AR. Randomized Trial of Single Dose Versus Fractionated Palliative Radiotherapy of Bone Metastases. Radiother Oncol 1998; 47(3): Nielsen OS, Munro AJ, Tannock IF. Bone Metastases: Pathophysiology and Management Policy. J Clin Oncol 1991; 9(3): Gaze MN, Kelly CG, Kerr GR, Cull A, Cowie VJ, Gregor A, Howard GC, Rodger A. Pain Relief and Quality of Life Following Radiotherapy for Bone Metastases: a Randomised Trial of Two Fractionation Schedules. Radiother Oncol 1997; 45(2): Steenland E, Leer JW, van Houwelingen H, Post WJ, van den Hout WB, Kievit J, de Haes H, Martijn H, Oei B, Vonk E, van der Steen-Banasik E, Wiggenraad RG, Hoogenhout J, Warlam-Rodenhuis C, van Tienhoven G, Wanders R, Pomp J, van Reijn M, van M, I, Rutten E, Leer J, van Mierlo T. The Effect of a Single Fraction Compared to Multiple Fractions on Painful Bone Metastases: a Global Analysis of the Dutch Bone Metastasis Study. Radiother Oncol 1999; 52(2): British Association of Surgical Oncology Guidelines. The Management of Metastatic Bone Disease in the United Kingdom. The Breast Specialty Group of the British Association of Surgical Oncology. Eur J Surg Oncol 1999; 25(1): Madsen EL. Painful Bone Metastasis: Efficacy of Radiotherapy Assessed by the Patients: a Randomized Trial Comparing 4 Gy X 6 Versus 10 Gy X 2. Int J Radiat Oncol Biol Phys 1983; 9(12): Mithal NP, Needham PR, Hoskin PJ. Retreatment With Radiotherapy for Painful Bone Metastases. Int J Radiat Oncol Biol Phys 1994; 29(5): Korkala OL, Karaharju EO. Metastatic Fractures of Long Bones. Int Orthop 1991; 15(2): Bartelink H, Battermann J, Hart G. Half Body Irradiation. Int J Radiat Oncol Biol Phys 1980; 6(1): Salazar OM, Rubin P, Hendrickson FR, Komaki R, Poulter C, Newall J, Asbell SO, Mohiuddin M, Van Ess J. Single-Dose Half-Body Irradiation for Palliation of Multiple Bone Metastases From Solid Tumors. Final Radiation Therapy Oncology Group Report. Cancer 1986; 58(1): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
190 32. Serafini AN, Houston SJ, Resche I, Quick DP, Grund FM, Ell PJ, Bertrand A, Ahmann FR, Orihuela E, Reid RH, Lerski RA, Collier BD, McKillop JH, Purnell GL, Pecking AP, Thomas FD, Harrison KA. Palliation of Pain Associated With Metastatic Bone Cancer Using Samarium-153 Lexidronam: a Double-Blind Placebo-Controlled Clinical Trial. J Clin Oncol 1998; 16(4): Bloomfield DJ. Should Bisphosphonates Be Part of the Standard Therapy of Patients With Multiple Myeloma or Bone Metastases From Other Cancers? An Evidence- Based Review. J Clin Oncol 1998; 16(3): Ernst DS, Brasher P, Hagen N, Paterson AH, MacDonald RN, Bruera E. A Randomized, Controlled Trial of Intravenous Clodronate in Patients With Metastatic Bone Disease and Pain. J Pain Symptom Manage 1997; 13(6): Robertson AG, Reed NS, Ralston SH. Effect of Oral Clodronate on Metastatic Bone Pain: a Double-Blind, Placebo-Controlled Study. J Clin Oncol 1995; 13(9): Pavlakis N, Stockler M. Bisphosphonates for Breast Cancer. Cochrane Database Syst Rev 2002;(1): CD Rosen L, Gordon D, Tchekmedyian S, et al. Zoledronic acid (Zol) significantly reduces skeletal-related events (SREs) in patients with bone metastases from solid tumors. Proc Am Soc Clin Oncol Galasko CSB. Tumours of the musculoskeletal system: principle of management of metastatic diseases. Current Orthopaedics (2 edn).1988: Priestman TJ, Dunn J, Brada M, Rampling R, Baker PG. Final Results of the Royal College of Radiologists Trial Comparing Two Different Radiotherapy Schedules in the Treatment of Cerebral Metastases. Clin Oncol (R Coll Radiol) 1996; 8(5): Noordijk EM, Vecht CJ, Haaxma-Reiche H, Padberg GW, Voormolen JH, Hoekstra FH, Tans JT, Lambooij N, Metsaars JA, Wattendorff AR. The Choice of Treatment of Single Brain Metastasis Should Be Based on Extracranial Tumor Activity and Age. Int J Radiat Oncol Biol Phys 1994; 29(4): Gaspar L, Scott C, Rotman M, Asbell S, Phillips T, Wasserman T, McKenna WG, Byhardt R. Recursive Partitioning Analysis (RPA) of Prognostic Factors in Three Radiation Therapy Oncology Group (RTOG) Brain Metastases Trials. Int J Radiat Oncol Biol Phys 1997; 37(4): Patchell RA, Tibbs PA, Walsh JW, Dempsey RJ, Maruyama Y, Kryscio RJ, Markesbery WR, Macdonald JS, Young B. A Randomized Trial of Surgery in the Treatment of Single Metastases to the Brain. N Engl J Med 1990; 322(8): Flickinger JC, Kondziolka D, Lunsford LD, Coffey RJ, Goodman ML, Shaw EG, Hudgins WR, Weiner R, Harsh GR, Sneed PK. A Multi-Institutional Experience With Stereotactic Radiosurgery for Solitary Brain Metastasis. Int J Radiat Oncol Biol Phys 1994; 28(4): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 175
191 44. Auchter RM, Lamond JP, Alexander E, Buatti JM, Chappell R, Friedman WA, Kinsella TJ, Levin AB, Noyes WR, Schultz CJ, Loeffler JS, Mehta MP. A Multiinstitutional Outcome and Prognostic Factor Analysis of Radiosurgery for Resectable Single Brain Metastasis. Int J Radiat Oncol Biol Phys 1996; 35(1): Kondziolka D, et al. Stereotactic Radiosurgery Plus Whole Brain Radiotherapy Versus Radiotherapy Alone for Patients With Multiple Brain Metastases. Int J Radiat Oncol Biol Phys 1999; 45: Harwood AR, Simpson WJ. Radiation Therapy of Cerebral Metastases: A Randomised Propsective Clinical Trial. Int J Radiat Oncol Biol Phys 1977;(2): Chu FCG, Hilaris B. Value of Radiation Therapy in the Management of Intracranial Metastases. Cancer 1961;(14): Kurtz JM, Gelber R, Brady LW, Carella RJ, Cooper JS. The Palliation of Brain Metastases in a Favorable Patient Population: a Randomized Clinical Trial by the Radiation Therapy Oncology Group. Int J Radiat Oncol Biol Phys 1981; 7(7): Borgelt B, Gelber R, Kramer S, Brady LW, Chang CH, Davis LW, Perez CA, Hendrickson FR. The Palliation of Brain Metastases: Final Results of the First Two Studies by the Radiation Therapy Oncology Group. Int J Radiat Oncol Biol Phys 1980; 6(1): Haie-Meder C, Pellae-Cosset B, Laplanche A, Lagrange JL, Tuchais C, Nogues C, Arriagada R. Results of a Randomized Clinical Trial Comparing Two Radiation Schedules in the Palliative Treatment of Brain Metastases. Radiother Oncol 1993; 26(2): Hoskin PJ, Crow J, Ford HT. The Influence of Extent and Local Management on the Outcome of Radiotherapy for Brain Metastases. Int J Radiat Oncol Biol Phys 1990; 19(1): Wong WW, Schild SE, Sawyer TE, Shaw EG. Analysis of Outcome in Patients Reirradiated for Brain Metastases. Int J Radiat Oncol Biol Phys 1996; 34(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
192 9. ALTERNATIVE AND COMPLEMENTARY THERAPIES 9.1 General 9.2 Effectiveness, safety and cost Effectiveness Safety Cost 9.3 Discussing alternative therapies Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 177
193 9.1 GENERAL The term alternative therapies is used loosely to describe anything outside the orthodox circle of surgery, radiation and chemotherapy 1. It includes different approaches that operate on the hope that we can boost the immune system through a mind-body connection these range from visualisation to diet and prayer Most alternative therapies have not been tested in randomised clinical trials. Alternative therapies may involve some interference with conventional therapies and may cause harm. Some alternative therapies have been acknowledged by the medical profession as useful, and these are usually known as complementary therapies. The effect of other alternative therapies is unknown or may cause harm. Complementary therapies can work alongside conventional therapies, whereas alternative therapies may involve some tension or interference with conventional therapies. Educational and psychosocial care has been found to benefit adults with cancer in relation to alleviating anxiety, depression, mood, nausea, vomiting, pain and increasing knowledge. 3 Both relaxation and meditation are frequently and effectively used by general practitioners and palliative care teams. Guideline Educational and Psychosocial Care in Cancer Level of Evidence Refs Educational and psychosocial care has been found to benefit adults with cancer in relation to anxiety, depression, mood, nausea, vomiting, pain and knowledge. I 3 Alternative therapies, as they are referred to for the rest of this chapter, are used by many Australians. In a random sample of South Australians, 48.5% of respondents (reflecting the general population) had used at least one non-physicianprescribed alternative medicine during the past year, while 20.3% had visited at least one alternative practitioner 4. Looking specifically at people with cancer, Begbie et al found that 21.9% of people attending one of three NSW oncology clinics said they were using alternative therapies 5. Other studies, some overseas and some Australian, have found that 9 54% of adults with cancer 6,7,8,9,10 and 46% of children with cancer 11 use alternative therapies. Australians spent an estimated $309 million per year on alternative therapists and $621 million per year on alternative therapies in 1993, which far exceeds the patient contribution of $360 million to standard pharmaceuticals for 1992/93 3. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 179
194 The main reasons for using alternative therapies given in the Begbie et al study were: new source of hope (49% of users of alternative therapies) preference for natural therapy (40%) impression that it is a non-toxic therapy (37%) supportive alternative practitioner (29%) try something different (23%) greater personal involvement (14%). The main therapies used were: relaxation/meditation (59% of users of alternative therapies) diet therapy (57%) megavitamins (43%) positive imagery (44%) faith/spiritual healing (30%) naturopathy (27%) immune therapy (17%) homeopathy (16%) acupuncture (11%). Seventy-five percent of people using alternative therapies used more than one (median 3, range 1 8) 5. Even though there is no data examining specifically the use of alternative therapies in those with advanced lung cancer, there is no obvious reason why usage would not be similar to that of other people with cancer. There are three important issues to consider in the use of alternative therapies, as there are with mainstream therapies: effectiveness, safety and cost. 9.2 EFFECTIVENESS, SAFETY AND COST EFFECTIVENESS There is little evidence that alternative therapies are effective. Most have not been examined rigorously, and some of those that have been examined have not been found to be effective 12,13,14. In the USA, the National Institutes of Health have set up an Office of Alternative Medicine that aims to explore the merits of alternative therapies. Alternative therapies that concentrate on strengthening the mind-body relationship have been tested, and have been shown to be effective. For example, prayer is being tested in controlled 180 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
195 clinical trials and thus far has been shown to be effective 15. Laughter has also been effective for some individuals 16. Relaxation and meditation have been tested and shown to be valuable 17. Inhalation aromatherapy has been used in a placebo controlled blind randomised trial during radiotherapy in Australia. The aromatic oils were administered by inhalation during radiotherapy with the aim of reducing anxiety level. Patients underwent anxiety assessments before and following completion of treatment. There was no difference in test scores in the randomly assigned groups. The anxiety scores were significantly lower (p=0.04) at treatment completion in those having carrier oil only as against those treated in the fragrant arms of the trial 18. Guideline Aromatherapy and Anxiety in Radiotherapy Level of Evidence Refs Aromatherapy has not been shown to reduce anxiety in patients with cancer undergoing radiotherapy. II 18 In a recent initiative, the Federal Government has established a new unit to consider and evaluate complementary treatments 19. SAFETY Many alternative therapies requiring changes in diet should be safe, although when there is a danger of substantial weight loss, such diets should be avoided 6. Meditation and spiritual approaches appear to do no harm. However, most alternative therapies involving the consumption of substances have not been assessed for safety. Their content is uncontrolled and may be quite variable 20. They may be adulterated with corticosteroids or other active compounds 21. They may be intrinsically toxic 22. There have been reports of deaths from royal jelly 23, and hepatitis from chaparral tea 24, which is a herbal remedy for cancer used by Native Americans. There are concerns about the safety of megavitamins, particularly the fat-soluble vitamins 25,26. There is potential for high doses of vitamin A to cause headaches due to raised intracranial pressure 27. The safety of many other compounds, and their potential for cross-reactivity with standard therapies, is unknown. One problem that is known is the potential for those taking large doses of vitamin D or its derivatives to develop hypercalcaemia 28. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 181
196 There are also concerns about the knowledge base of alternative therapists. Some are well trained in their craft, but others are not. Most alternative therapists are not yet under state regulatory control. Potentially dangerous alternative therapies in those with advanced lung cancer include: taking calcium with or without vitamin D for bone disease, as this may exacerbate hypercalcaemia some diets recommended for treatment of cancer, such as the beetroot diet, the grape diet and the Gerson diet, as they may be nutritionally inadequate 29,30 the frequent use of enemas (such as coffee enemas or high colonic washouts), as they can cause electrolyte imbalances 31. COST It seems that many alternative therapies are inexpensive. In the study of Begbie et al, the median annual cost was $530. Almost two-thirds of women with advanced breast cancer using alternative therapies thought they were getting value for money. In the South Australian study, mean monthly expenditure on alternative therapies ranged from $1 $500, with a median of $10. Expenditure on alternative therapists was similar. However, some therapies are remarkably expensive, with one woman spending $20,000 per year on alternative treatments 5. Conventional therapies are effectively subsidised by governments, and most patients do not pay the full cost of treatments. With alternative therapies, they are required to pay the full cost. Those using alternative therapies should be advised to enquire about costs before embarking on a course of alternative therapies, as they should with standard therapies. 9.3 DISCUSSING ALTERNATIVE THERAPIES These three issues (effectiveness, safety and cost) need to be explored with all patients with advanced lung cancer who use alternative therapies. However, they can only be explored if the doctor is aware of the patient s use of such therapies. Begbie et al found that 40% of women with cancer using alternative therapies did not tell their doctors about them. Presumably, those people were either not asked, or chose not to tell their doctors. It can be assumed that a negative attitude emanating from medical practitioners about alternative therapies would inhibit frank discussion. Such inhibition would mean patients would not learn of the medical practitioner s support of, or concerns for, the way in which the alternative or complementary therapies may affect the conventional treatment patterns. 182 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
197 For many patients, feeling they can assume some control of the treatment of their disease is psychologically empowering. The physical problems that may arise from interference with conventional therapies may be attenuated by the strong psychological value of the alternative therapy. Conventional therapies often hold little hope of cure for patients, and it is understandable that patients will seek other solutions. Clinicians should also be aware that decisions to use alternative therapies might not be based on the same philosophical approach as that used by doctors. It is to everyone s advantage if patients are able to discuss alternative therapies openly, secure in the knowledge that they will continue to receive support and understanding from their doctors, whether or not those doctors agree with the therapy being used. Due to lack of information relating to cancer of the lung, this chapter has been largely unchanged from Clinical practice guidelines for the management of advanced breast cancer, with permission of The National Breast Cancer Centre. References 1. Batt.S. Patient no more: the politics of breast cancer. Melbourne: Spinifex Press, Love S, Lindsey K. Dr Susan Love s breast book.addison-wesley, Devine EC, Westlake SK. The Effects of Psychoeducational Care Provided to Adults With Cancer: Meta-Analysis of 116 Studies. Oncol Nurs Forum 1995; 22(9): MacLennan AH, Wilson DH, Taylor AW. Prevalence and Cost of Alternative Medicine in Australia. Lancet 1996; 347(9001): Begbie SD, Kerestes ZL, Bell DR. Patterns of Alternative Medicine Use by Cancer Patients. Med J Aust 1996; 165(10): Downer SM, Cody MM, McCluskey P, Wilson PD, Arnott SJ, Lister TA, Slevin ML. Pursuit and Practice of Complementary Therapies by Cancer Patients Receiving Conventional Treatment. BMJ 1994; 309(6947): Cassileth BR, Lusk EJ, Strouse TB, Bodenheimer BJ. Contemporary Unorthodox Treatments in Cancer Medicine. A Study of Patients, Treatments, and Practitioners. Ann Intern Med 1984; 101(1): Harris L, et al. Health information and the use of questionable treatments: a study of the American public, Washington DC: Department of Health and Human Services Lerner IJ, Kennedy BJ. The Prevalence of Questionable Methods of Cancer Treatment in the United States. CA Cancer J Clin 1992; 42(3): Miller MJ, Boyer MJ, Dunn SM. Why Do Australian Cancer Patients Use Unproven Treatments? Proc Am Soc Clin Oncol 1995; 22: 76. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 183
198 11. Sawyer MG, Gannoni AF, Toogood IR, Antoniou G, Rice M. The Use of Alternative Therapies by Children With Cancer. Med J Aust 1994; 160(6): Creagan ET, Moertel CG, O Fallon JR, Schutt AJ, O Connell MJ, Rubin J, Frytak S. Failure of High-Dose Vitamin C (Ascorbic Acid) Therapy to Benefit Patients With Advanced Cancer. A Controlled Trial. N Engl J Med 1979; 301(13): Moertel CG, Fleming TR, Creagan ET, Rubin J, O Connell MJ, Ames MM. High-Dose Vitamin C Versus Placebo in the Treatment of Patients With Advanced Cancer Who Have Had No Prior Chemotherapy. A Randomized Double-Blind Comparison. N Engl J Med 1985; 312(3): Moertel CG, Fleming TR, Rubin J, Kvols LK, Sarna G, Koch R, Currie VE, Young CW, Jones SE, Davignon JP. A Clinical Trial of Amygdalin (Laetrile) in the Treatment of Human Cancer. N Engl J Med 1982; 306(4): Dossey I. Healing words: the power of prayer. San Francisco: Harper, Cousins N. Anatomy of an illness. New York: Bantam Books, Baider L, Uziely B, De Nour AK. Progressive Muscle Relaxation and Guided Imagery in Cancer Patients. Gen Hosp Psychiatry 1994; 16(5): Graham PH, Browne L, Cox H, Graham J. Inhalation Aromatherapy During Radiotherapy: Results of a Placebo-Controlled Double-Blind Randomized Trial. J Clin Oncol 2003; 21(12): The Office of Complementary Medicines PO Box 100, Woden Australian Capital Territory 2606, ph; , fax: , Therapeutic Goods Administration, Department of Health and Aged Care. 20. Myers SP, Smith AJ. Cardioprotection and Garlic. Lancet 1997; 349(9045): Huxtable RJ. The Harmful Potential of Herbal and Other Plant Products. Drug Saf 1990; 5 Suppl 1: Pillans PI. Toxicity of Herbal Products. N Z Med J 1995; 108(1012): Adverse Drug Reactions Advisory Committee (ADRAC). Harmless Herbals? Adverse Drug Reaction Bulletin 1993; 12: Smith BC, Desmond PV. Acute Hepatitis Induced by Ingestion of the Herbal Medication Chaparral. Aust N Z J Med 1993; 23(5): Ragg M. The cancer prevention diet. Sydney: Pan MacMillan, Bowman BB, Kushner RF, Dawson SC, Levin B. Macrobiotic Diets for Cancer Treatment and Prevention. J Clin Oncol 1984; 2(6): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
199 27. Snodgrass SR. Vitamin Neurotoxicity. Mol Neurobiol 1992; 6(1): Koeffler HP, Hirji K, Itri L. 1,25-Dihydroxyvitamin D3: in Vivo and in Vitro Effects on Human Preleukemic and Leukemic Cells. Cancer Treat Rep 1985; 69(12): Boyle FM. Adverse Interaction of Herbal Medicine With Breast Cancer Treatment. Med J Aust 1997; 167(5): Shils ME, Hermann MG. Unproved Dietary Claims in the Treatment of Patients With Cancer. Bull N Y Acad Med 1982; 58(3): Eisele JW, Reay DT. Deaths Related to Coffee Enemas. JAMA 1980; 244(14): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 185
200 SECTION V ECONOMIC CONSIDERATIONS 10. COST-EFFECTIVENESS 10.1 Economic burden of lung cancer in Australia 10.2 Role of economic evidence in the development of the guidelines Smoking cessation and prevention Interventions provided by health care professionals Generic and personalised self-help material Nicotine replacement therapy (NRT) Mass media and other anti-smoking campaigns Intervention for hospitalised patients Other pharmacological therapies including bupropion Screening Initial assessment and follow-up Use of positron emission tomography in staging of NSCLC Treatment of NSCLC Follow-up after surgical management Chemotherapy for advanced (Stage IIIB & IV) NSCLC Radiotherapy and combination therapies Treatment of SCLC Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 187
201 10.1 ECONOMIC BURDEN OF LUNG CANCER IN AUSTRALIA In 1996 lung cancer was the second most common malignant cancer in males and fourth most common in females 1. Surgical resection provides curative therapy for early stage cancer, with five-year survival rates for early stage non-small cell lung cancer (NSCLC) ranging from 25% 67%. However, less than 20% of lung cancers are diagnosed when the cancer is still localized 2 and there are limited options for treatment of disseminated lung cancer. These factors have resulted in lung cancer being the most common cause of cancer death in males and the second most common in females 1. In NSW the five year relative survival rates for lung cancer was the lowest of any cancer, at 10% for males and 12% for females, between 1980 and The estimated burden of disease attributable to lung cancer in Australia is outlined in Table Years of Life Lost (YLL) due to lung cancer are considerably higher than Years Lost due to Disability (YLD). This reflects the fact that the burden of cancer is dominated by mortality rather than lengthy periods of disability 4. Table 1 10 Burden of disease attributable to lung cancer in Australia, Total Males Females Number Per cent Number Per cent Number Per cent Deaths YLL YLD DALY Abbreviations: YLL = Years of Life lost; YLD = Years Lost Due to Disability; DALY = Disability Adjusted Life Year The Australian Institute of Health and Welfare have estimated the costs of lung cancer at a macro level. In lung cancer was estimated to account for 5.6% of total health care system costs in Australia. It ranked fifth in terms of the most expensive cancers in Australia with total health care expenditure on lung cancer estimated at $107 million in (this estimate includes hospital, medical, pharmaceuticals, nursing home and allied health services, public health programs, research, other institutional and non-institutional and administration expenditure 4 ). Lung cancer ranks as the third most costly cancer for males aged and the fourth most costly cancer for males and females aged over Total treatment costs for per case of lung cancer were estimated at $ in , which ranks twelfth in terms of the most costly cancer to treat 5. However, there is relatively little micro-level information available in Australia about treatment patterns and resource use for lung cancer, particularly in terms of resource use by stage at diagnosis. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 189
202 10.2 ROLE OF ECONOMIC EVIDENCE IN THE DEVELOPMENT OF GUIDELINES The NHMRC has identified two main areas where economic evidence is important in the development of clinical practice guidelines: determination of which treatment alternatives are the most cost-effective determination of whether a proposed clinical practice guideline is cost-effective. In the development of these guidelines, the emphasis has been in the first instance on identifying those interventions for which there is evidence of effectiveness, before addressing questions of cost-effectiveness. There is limited evidence available within Australia to assess the costs and cost-effectiveness of alternatives for management of lung cancer. However, there is a range of international literature that provides information about the relative cost-effectiveness of alternatives, and this information can be used to inform the development of these guidelines. The approach taken in reviewing the economic evidence involved: identifying those areas where economic evidence is likely to be important identifying those areas where economic evaluation evidence is available reviewing and summarising the economic evaluation literature. However, it is important to note that international economic evaluation literature is limited in its relevance to Australia because of differences in cost structures and reimbursement arrangements, and because the comparator in international studies may not reflect current practice in Australia. A search was conducted using the databases Medline and Embase, covering the period Economic evaluation literature that pre-dates 1993 was considered to be of limited relevance because of changes in technology, cost structures and management practices. The key words included lung cancer, economic evaluation, cost-effectiveness analysis, cost benefit analysis, cost analysis and cost. Articles were included if they were economic evaluations, that is, if they involved comparison of alternative interventions in terms of costs and consequences. A supplementary search was undertaken to identify economic evaluations of smoking cessation interventions. Articles were classified into seven main areas: smoking cessation and prevention screening initial assessment and follow-up lung cancer imaging including the use of PET treatment of non-small cell lung cancer (NSCLC) treatment of small cell lung cancer (SCLC) radon exposure (environmental exposure)(see Appendix 5). These groupings reflected the main areas in which economic evaluation of interventions have been undertaken. 190 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
203 Articles were reviewed using the criteria recommended in the How to compare the costs and benefits: evaluation of the economic evidence 6. The shadow price criteria in this document were used as a basis for assessing the relative cost-effectiveness of interventions. That is, interventions that fall below the threshold of $ per life-year saved (LYS) are considered to be relatively cost-effective (good value for money) and can be recommended interventions that exceed a threshold of $ per LYS are considered not to be cost-effective and cannot be recommended without a strong justification interventions that fall between $ per LYS and $ per LYS require further consideration. However, assessment of overseas economic evaluations and even some Australian economic evaluations in these terms should be treated with some caution. Whether these costs and outcomes would be realised if the intervention were adopted in the Australian context depends upon a number of factors, but particularly on whether the comparator for the study reflects current practice in Australia. Cost-effectiveness results from studies are presented as reported in the relevant studies (that is, in the currency and time period as reported in the study), but also, for comparative purposes, converted to 2001 Australian dollars. Results in terms of 2001 Australian dollars are reported in parentheses. The conversion was undertaken using the OECD purchasing power parity estimates ( for the relevant year of the study to convert to Australian dollars for that year, then using the Australian Bureau of Statistics Health Price Index (weighted average of eight capital cities; ABS, 2002; Consumer Price Index Catalogue ) to convert the relevant costs to 2001 Australian dollars. Results in terms of 2001 Australian dollars are reported in parentheses below. However, in comparing across studies it should be noted that the results from different studies are not directly comparable. In particular, the scope of the studies may differ in terms of the range of costs and consequences considered, the perspective of the study and the choice of comparator. In addition, particularly for earlier studies, there may be important changes in cost structures and technology that limit comparability. The indicative cost-effectiveness estimates in 2001 Australian dollars should be treated as providing a guide to the likely cost-effectiveness of the interventions in the Australian setting, given the shadow prices suggested above. The findings of the literature review are summarised below. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 191
204 SMOKING CESSATION AND PREVENTION A number of studies have been undertaken to assess the cost-effectiveness of various smoking cessation interventions, including: nicotine replacement therapy and other pharmacological therapies information programs and Quit smoking campaigns delivered through various avenues (e.g. GP, pharmacist, community, media) counselling programs (e.g. group therapy and individual therapy) intervention on hospital admission. In general cost-effectiveness studies of smoking cessation do not directly assess the potential impacts on lung cancer morbidity and mortality, and many studies report results in terms of intermediate outcome measures such as additional quitters. This is partly because of the number of additional assumptions required to extrapolate from additional quitters/non-smokers to impact on morbidity and mortality. However, given the importance of smoking as a risk factor for lung cancer, it is valuable to consider the cost-effectiveness of interventions aimed at reducing or preventing smoking. In general, the cost-effectiveness research undertaken on smoking cessation and prevention indicates that smoking interventions represent good value for money. These results are primarily because of the relatively high level of benefits generated from the potential to avert years of life lost through reductions in morbidity and mortality, as well as because many of the interventions are relatively low cost compared with other health care interventions. Cost-effectiveness results do vary considerably between interventions. However, it is difficult to directly compare cost-effectiveness estimates across studies as estimates reflect not only the costs and effects of the alternative therapies but also different assumptions concerning the range of costs and benefits that are included in the evaluation. INTERVENTIONS PROVIDED BY HEALTH CARE PROFESSIONALS Smoking interventions can be delivered through a number of health care professionals including general practitioners, nurses, pharmacists and counsellors. There has been little cost-effectiveness research on this issue. Buck, Richmond et al 7 evaluated the costeffectiveness of a GP delivered smoking cessation intervention known as Smokescreen, which involves GP training. The cost-effectiveness of this intervention was estimated at $183 (A$208) per additional abstainer. Viney, Haas et al 8 compared a number of different strategies including a GP based brief advice intervention and a more structured intervention consisting of a number of sessions. The brief advice approach was found to be more cost-effective at $6 $41 per quitter ($A7 $50). Two studies have evaluated the cost-effectiveness of pharmacist intervention to assist smoking cessation. Cost-effectiveness estimates range from 300 (A$672) per one additional quit for pharmacists who were trained to provide more 192 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
205 appropriate information to people looking to stop smoking 9 to (A$1051) for a program which consisted of a contract between the pharmacist and patient and a series of counselling sessions over a 6 month period 10. Counsellors provide another avenue through which smoking interventions can be delivered. The Mayo Clinic Nicotine Dependence Center (USA) provides a counselling service, which consists of an initial consultation and the formulation of an individual treatment plan, which may include group therapy, inpatient program and/or pharmacologic therapy. Croghan, Offord et al 11 evaluated this program and estimated a net cost per life-year gained of $6828 (A$11 693). Prathiba, Tjeder et al 12 evaluated the cost-effectiveness of a counselling programme provided to hospital in-patients and out-patients. They estimated the cost per life-year saved from such a program at (A$667 $836), and the cost of an additional quit was valued at 851 (A$1671). These results indicate that appropriately trained health care professionals may be able to provide a cost-effective method through which to disseminate information on smoking cessation and/or conduct quit smoking campaigns. However, more evidence is needed to make a recommendation. GENERIC AND PERSONALISED SELF-HELP MATERIAL One study, by Lennox, Osman et al 13, was found to have looked at the cost-effectiveness of generic versus tailored self-help material. This study evaluated the impact of computer tailored and non-tailored smoking cessation letters and found that the tailored letter did not increase cessation rates over and above that of the non-tailored letter. However, it was found to be effective in promoting a shift towards smoking cessation. The costeffectiveness of the non-tailored letter (compared to no letter) was valued at 37 (A$49) per quitter, with the cost per life-year gained valued (A$67 $163). This study suggests that letter writing (either tailored or not tailored) is a cost-effective method of getting patients to quit smoking. However, non-tailored letter writing appears to be more cost-effective than tailored letter writing. NICOTINE REPLACEMENT THERAPY (NRT) Four studies were found which evaluated the cost-effectiveness of nicotine patches and one study evaluated the cost-effectiveness of Nicorette nasal spray. In all studies the incremental cost-effectiveness of nicotine patch or spray therapy was compared with (some form of) counselling alone. As outcome measures varied from study to study, the results have been set out in Table 2 10 (overleaf). In all studies nicotine replacement therapy, when used as an adjunct to counselling, was found to be a cost-effective intervention. Therefore, there appears to be support for recommending the use of nicotine replacement therapy in combination with counselling services. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 193
206 MASS MEDIA AND OTHER ANTI-SMOKING CAMPAIGNS Anti-smoking campaigns and media campaigns have taken many forms including mass media campaigns, community programs and work-site smoking cessation programs. Cost-effectiveness studies have been undertaken to evaluate a handful of these campaigns. Relative to other programs mass media campaigns appear to be relatively cost-effective. However, there is insufficient evidence to recommend one type of campaign over another. Table 2 10 Summary of NRT cost-effectiveness literature Study Study Comparator Unit of benefit country Akehurst and UK GP counselling alone Cost-effectiveness per quitter Piercy versus GP counselling is (A$8 264) and nicotine patch therapy Marginal cost per quitter was (A$3 365), marginal cost per death avoided (A$ ) and marginal cost per life-year gained (A$12 341). Akehurst and UK GP counselling alone Cost per life-year saved 1430 Piercy versus GP counselling (A$3 844). and nicotine nasal spray Fiscella and Franks USA GP counselling alone Cost of 1 additional lifetime quitter versus GP counselling $7 332 (A$10 745) and nicotine patch therapy Incremental cost-effectiveness ranged $4 930 $ (A$7 225 $14 718) per QALY for males and $4 955 $6 983 (A$7 262 $10 234) per female. Stapleton, Lowin UK GP counselling alone Incremental cost per life-year saved et al versus GP counselling range (A$775 $1 541). and nicotine patch therapy 194 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
207 Table 2 10 Summary of NRT cost-effectiveness literature (continued) Study Study Comparator Unit of benefit country Wasley, McNagny USA Counselling alone Average cost per life-year saved: et al versus GP counselling $965 $1 585 (A$1 414 $2 322) and nicotine patch for males; $1 634 $2 360 therapy (A$2 394 $3 459) for females Incremental cost per life-year saved: $1 796 $2 949 (A$2 632 $4 322) for males; $3040 $4 391 (A$4 455 $6 435) for females Table 3 10 Summary of mass media and other anti-smoking campaigns cost-effectiveness literature Study Study Intervention type Outcome country Mudde and Netherlands Mass media US$12 per quit (A$17). De Vries Ratcliffe, Cairns Scotland Mass media per quit (A$330 $724). et al Tillgren, Rosen Sweden Quit and win contest US$188 $1 222 (A$342 $2 223) et al per life-year saved. Stevens, UK Targeted campaign 105 (A$231) per life-year saved. Thorogood for high-risk group Estimates ranged et al (Turkish speaking (A$73 $861). groups in London) Tengs, Osgood USA National school based $4 900 $ et al education program (A$6 826 $ ) per quality adjusted life-year. Warner, Smith USA Firm health promotion $894 (A$1310) per life-year saved. et al program Estimates ranged $500 $2300 (A$733 $3370). Viney, Haas Australia Mass media $11 30 per quitter ($A13 36) et al Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 195
208 INTERVENTION FOR HOSPITALISED PATIENTS Two studies were found which attempted to evaluate the cost-effectiveness of a hospital based smoking cessation interventions. Meenan, Stevens et al 25 estimated that the incremental cost per incremental quit at $3697 (A$5975) and the incremental discounted life-year saved ranged between $1691 (A$2733) and $7444 (A$12 031). This study provides some evidence that smoking cessation interventions for hospital in-patients may be cost-effective. However, more evidence is required. OTHER PHARMACOLOGICAL THERAPIES INCLUDING BUPROPION Nielsen and Fiore 26 conducted a cost benefit analysis of bupropion, nicotine transdermal patch (NTP) and a combination of the two therapies. This study found that bupropion alone, with a net benefit estimated at $338 (A$428), had a greater net benefit than either NTP at $26 (A$33), combination therapy at $178 (A$226) or placebo at $258 (A$327). Johnson, Lucas et al 27 also compared the cost-effectiveness of NTP against bupropion SR, and found that, despite similar effectiveness levels, bupropion SR was more costeffective than NTP. The cost-effectiveness of bupropion hydrochloride as part of a health plan and work-site smoking cessation program was also evaluated and estimated to have a cost-benefit ratio of $1:4.10 $4.69 (A$1.30: ) 28. These studies indicate that bupropion is a cost-effective intervention for smoking cessation and may be more cost-effective than nicotine replacement therapy. However, the number of studies is limited. SCREENING The prevailing consensus appears to be that mass screening programs to detect lung cancer are of doubtful cost-effectiveness. This is largely driven by relatively low rates of detection accuracy of plain chest x-rays. Estimates of cost-effectiveness for mass screening with plain chest x-rays vary from $9000 (A$11 414) per undiscounted lifeyear gained 29 to $ (A$ ) 30 per life saved. These estimates would appear to provide some support for mass screening. The former study assumes an 18% reduction in mortality, based on extrapolation of staging data from four randomised controlled trials, and assuming a 100% participation rate in annual screening of male smokers aged However, the assumption of an 18% reduction in mortality is not adequately supported, given that trials on which the evidence was based did not show a mortality benefit. A further limitation is that consequences are not discounted. The latter study is a decision analytic model, with the detection rate based on results from a mass screening program in Japan. Both studies depend on the assumptions about detection rates, and the impact of early detection on survival. 196 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
209 The paucity of recent studies and the continued debate about whether plain x-rays are sensitive enough to detect lung cancer at a stage early enough to undertake curative treatment means that there does not appear to be strong support for recommending mass screening programs with plain x-rays on the basis of cost-effectiveness evidence. Recent technological advances, primarily the development of CT screening, have led to improvements in the sensitivity of screening. Marshall, Simpson 31,32 and Okamoto 33 have evaluated the cost-effectiveness of CT screening for lung cancer. Marshall, Simpson 32 developed a decision analytic model to examine the cost-effectiveness of annual lung cancer screening based on CT for a high-risk cohort aged 60 74, combining data from the ELCAP project and the SEER registry. The model assumes that screening will shift the stage distribution at diagnosis. Based on this the cost per life-year saved is $ ($A26 500), but in sensitivity analysis, this varied to $ ($A85 000) per LYS. The same authors have used similar data to examine the cost-effectiveness of one-time screening and have estimated that the cost per life-year saved ranges from $5940 ($A8275) for a very high-risk cohort (lung cancer prevalence of 2.7%) to $ ($A32 200) per life-year saved for a lower risk population of smokers. Okamoto 33 used a decision analytic model to examine the cost-effectiveness of CT screening compared with the current x-ray based screening in Japan, and concluded that while CT screening would be more expensive, it would also be more effective. Despite the fact that CT screening is more expensive than screening by plain x-rays, the preliminary evidence suggests that the improvements in detection provided by CT scanning may outweigh the additional costs, leading to better estimates of costeffectiveness for lung cancer screening. A major limitation of these studies is that the impact on mortality is based on extrapolation from screening results to a survival benefit. However, at this stage survival benefits from screening have not been demonstrated. Therefore, these cost-effectiveness estimates should be viewed with some caution as they are based on limited data on the effectiveness of CT screening, and may change with further evidence from randomised controlled trials. In general, the studies indicate that improvements in scanning technology that lead to better diagnostic accuracy (without parallel increases in cost) will improve the cost effectiveness of screening programs. For all screening programs, plain x-ray and CT, cost-effectiveness is significantly improved when screening is targeted at highrisk groups. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 197
210 Table 4 10 Summary of screening cost-effectiveness literature Study Study Screening type Unit of Benefit country Baba, Takahashi Japan Plain x-ray Cost of a life saved ~$ et al (A$ ). Caro, Klittich USA X-ray Cost-effectiveness of $9 000 et al (A$11 413) per undiscounted life-year gained or less than $ (A$25 364) per discounted life-year gained. Chirikos et al USA CT scan Incremental cost per life-year ratio $ (A$45 789) $ (A$ ). Marshall, Simpson USA CT scan High-risk cohort cost ~$ (A$26 469) per life-year saved. ($ $ [A$ $86 372]) Marshall, Simpson USA CT scan High-risk cohort one time screen is $5 940 (A$8 275) per life-year saved. General population $ (A$32 180) per life-year saved. INITIAL ASSESSMENT AND FOLLOW-UP There have been relatively few papers assessing the economic evidence for approaches to initial assessment of patients with suspected lung cancer. Raab, Hornberger et al 35 evaluated the cost-effectiveness of sputum cytology, when used as the first test preceding all other tests, in the diagnosis of lung cancer. Testing sputum cytology was found to be the dominant strategy as it lowered both medical costs and mortality risk. This study indicates that sputum cytology may provide a cost-effective option in the diagnosis of lung cancer. However, recommendations cannot be based on the findings on only one study. Therefore, this study can be taken as indicative of potential cost savings with further research required. The Canadian Lung Oncology Group 36 have investigated the costs and outcomes of investigation for mediastinal disease for patients with apparently operable lung cancer, comparing mediastinoscopy with CT. They concluded that CT is likely to produce the same number or fewer unnecessary thoracotomies, and be less costly. 198 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
211 In a more recent study, the Canadian Lung Oncology Group have also undertaken a randomised controlled trial and comparison of costs of a limited and a full investigation strategy prior to the final decision regarding surgery. In the limited strategy patients underwent CT of the chest and mediastinoscopy, and proceeded to thoracotomy if there was no evidence of major mediastinal disease on CT, mediastinoscopy or both. In the full investigation strategy, patients also underwent bone scintigraphy and CT of the chest, liver, adrenal glands and head after mediastinoscopy. Patients in the full investigation group were less likely to have a thoracotomy, but there was no significant difference in the relative risk of thoracotomy without cure between the two strategies. While the full investigation strategy had higher costs associated with professional fees, overall, the average cost of full investigation was lower than for the limited strategy, because of costs of hospital episodes avoided. However, the difference in costs was not significant 37. USE OF POSITRON EMISSION TOMOGRAPHY IN STAGING OF NSCLC A number of studies have used decision analytic models to evaluate the costeffectiveness of the use of Positron Emission Tomography (PET), in general FDG-PET, in staging and management of NSCLC. PET has been considered as both an adjunct and an alternative to conventional staging, which in most studies is assumed to be CT scanning. Most studies provide preliminary evidence to suggest that PET may be relatively cost-effective because of the potential to avoid unnecessary surgery through more accurate staging, and particularly through detection of disseminated disease. For example, Valk, Pounds et al 38 and von Schulthess, Steinert et al 39 both took a costminimisation approach and estimated that PET would be cost-saving as an adjunct or an alternative to conventional staging involving CT. However, neither study examines the impact on mortality, particularly the potential for PET to result in surgery avoided for potentially curable patients. Dietlein, Weber et al 40 and Scott, Shepherd et al 41 examined the relative cost-effectiveness of a number of different potential strategies for incorporating PET in staging of NSCLC. Dietlein, Weber et al 40 concluded that PET was likely to be cost-effective (143 EUR/LYS) for patients with normal sized mediastinal lymph nodes when used as an adjunct to conventional staging. The results of Scott, Shepherd et al 41, suggest that PET is less cost-effective, but may be good value for money under some strategies, particularly for patients who had no mediastinal lymph node involvement on CT. These results suggest that the cost-effectiveness of PET depends on how it is used in relation to conventional staging, and on the accuracy of the initial staging. The limitation of all the current cost-effectiveness analyses of PET is that they rely on estimates of sensitivity and specificity of PET based on relatively small case series rather than randomised controlled trials. Further, the relative cost-effectiveness of PET depends critically on the management decision made based on the PET results (that is, whether thoracotomy will be avoided, or whether the patient will have other Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 199
212 treatment such as chemotherapy, as an addition or alternative to thoracotomy) 42. Thus, it is important to assess the cost-effectiveness of PET in the local context and using evidence from randomised controlled trials. Two recent studies provide new evidence that will be critical in determining the value of PET in management of NSCLC. van Tineren, Hoekstra et al 43 have undertaken a randomised controlled trial of pre-operative assessment of patients with suspected Stage I-III NSCLC. Their results suggest that PET may avoid thoracotomy in 20% of patients. Although they have not as yet reported costeffectiveness analysis, these results suggest that PET may be relatively cost-effective. However, preliminary cost-effectiveness results from another randomised controlled trial and cost-effectiveness analysis 44 suggest that PET may not be cost-effective in management of Stage I II NSCLC. TREATMENT OF NON-SMALL CELL LUNG CANCER (NSCLC) There is relatively limited information about the cost-effectiveness of the range of treatments for non-small cell lung cancer, including the value of surgery for potentially operable disease, the appropriateness of adjuvant therapy and the appropriate choice of chemotherapy agent for disseminated cancer. FOLLOW UP AFTER SURGICAL MANAGEMENT There is very little information on cost-effectiveness of alternative follow-up strategies. Younes, Gross et al 45 compared the cost-effectiveness of a strict follow-up regime (consisting of strict visits, imaging and laboratory examinations) with infrequent visits. The study found that, for patients with resected NSCLC, the strict follow-up strategy was more expensive but did not lead to a significant difference in interval between recurrence. Gilbert, Reid et al 46 evaluated whether follow-up by a thoracic surgeon after cancer resection, as opposed to a GP, altered survival. The cost per recurrence detected by a thoracic surgeon was $4367 (A$5108) compared with $1105 (A$1293) for the cost per recurrence detected by a GP. No 5-year survival benefit for surgeon-detected recurrences was found. Therefore, follow-up via a GP was found to be relatively cost-effective. Similarly, Egermann, Jaeggi et al 47 examined the costs and outcomes of a strict protocol of regular follow-up for 10 years including clinic visits and chest radiography following resection for NSCLC, although it is not clear whether the comparator was no follow-up or a less frequent protocol. They concluded that the costs per life-year saved from the strict protocol were high. 200 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
213 CHEMOTHERAPY FOR ADVANCED (STAGE IIIB AND IV) NSCLC A number of studies evaluating different chemotherapy regimes for advanced NSCLC have been undertaken since 1995, although there is considerable overlap between studies in terms of the modelling approaches used and the trial and other data used to estimate effectiveness. The results are summarised in Table In general, these studies, particularly the review studies, provide evidence that chemotherapy provides a small survival and quality of life gain that is relatively cost-effective compared with supportive care 48. The majority of these studies provide evidence to suggest that the incremental cost-effectiveness of some chemotherapy regimes is less than $A per life-year gained, although cost-effectiveness estimates vary considerably. However, there is insufficient evidence at this stage to recommend one particular chemotherapy agent or regime over others on the basis of cost-effectiveness. However, it should be noted that these results are sensitive to the method of estimating or extrapolating survival and quality of life data from trials, to the chemotherapy regimes, to the relative costs of different chemotherapy regimes, and to the method of delivery of chemotherapy, with inpatient care being more costly than outpatient care. While the studies provide evidence to suggest that some chemotherapy regimes appear to be relatively more cost-effective than others, and in some instances cost-saving, extrapolating these results to the Australian context is not appropriate, as the relative cost-effectiveness is largely driven by the relative costs of the different chemotherapy regimes and modes of delivery, which can vary internationally. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 201
214 Table 5 10 Results of studies investigating costs and outcomes of alternative chemotherapy regimens Studies Study country Study questions Conclusions Palmer and Italy Comparison of 4 cisplatin regimens: No significant difference in survival Brandt G+P; MIP; E+P; NVB+P Based on $/tumour response, gemcitabine & cisplatin is more cost-effective Will, Berthelot Canada Comparisons of a range of chemo- VLB+P dominates BSC et al 2001 therapy regimes with best supportive Berthelot, Will care (BSC) including VLB+P; NVB; Incremental cost of chemotherapy compared with BSC ranges et al 51 NVB+P; PAX+P (3 doses); G from $1 900 $27 000/LYS ($A ); $2 658 $37 841/QALY ($A3 300 $46 300) At a threshold of $A30 000/QALY, preferred regime is NVB+P; for lower thresholds VLB+P is preferred, for higher, G is preferred; Results vary if outcome measure is LYS Koch, Johnson Germany Comparison of gemcitabine versus Gemcitabine has the potential to be cost saving et al ifosfamide/etoposide; assumes equal efficacy Billingham UK Comparison of MIC chemotherapy Chemotherapy more costly than palliative care. Incremental et al plus standard care versus palliative cost-effectiveness ratio of (A$31 333) per care alone. life-year gained. Clegg, Scott UK Comparison of a range of chemo- Incremental cost compared with BSC varied from et al therapy regimens with BSC: ($A8 633) for NVB to ($A98 360) for PAX. G; G+P; NVB; NVB+P; PAX; PAX+P various doses; DOC; DOC 2nd line At a threshold of $A30 000/LYS NVB; NVB+P; G; G+P; and PAX+P cost-effective Based on a review of 33 clinical trials and construction of a costing model 202 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
215 Table 5 10 Results of studies investigating costs and outcomes of alternative chemotherapy regimens (continued) Studies Study country Study questions Conclusions Annemans, The Netherlands, Comparison of paclitaxel & cisplatin Trial results show no difference in survival or quality of life Giaccone Belgium, Spain versus teniposide & cisplatin for et al and France advanced NSCLC PAX+P more expensive but additional responders Not clear that all costs were considered Smith, Hillner USA Comparison of three chemotherapy Incremental $/LYS ranged from $ (NVB+P versus et al regimes: NVB; NVB+P; VIN+P VIN+P) $ (VIN+P versus NVB alone) Hillner and Smith ($A $33 000) ; Evans and Le Canada Comparison of chemotherapy regimes NVB alone; NVB+P (delivered in outpatient setting); VLB+P Chevalier with BSC: NVB alone, NVP+P; VIN+P; and VP-16-P are dominant. Evans VP-16-P; VLB+P Cost per LYS for other therapies less than $A Evans , Canada Comparison of gemcitabine with Incremental $/LYS BSC Incremental $/LYS $630 $ depending on assumptions and numbers of cycles ($A854 $22 007) Earle and Evans Canada Comparison of PAC+P with standard Incremental $/LYS $ $ based on trial E+P for advanced NSCLC protocol ($A $ ) Outpatient protocol incremental $/LYS ($A33 000) Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 203
216 Table 5 10 Results of studies investigating costs and outcomes of alternative chemotherapy regimens (continued) Studies Study country Study questions Conclusions Leighl, Shepherd Canada Comparison of 2nd line docetaxel Incremental $/LYS ranged from $ $ et al with BSC based on the TAX 317 trial ($A ), but results were sensitive to changes in survival estimates, increasing to $ ($A ) Sacristan, Spain Comparison of G+P with E+P No differences in survival were found; Gem+P was lower cost Kennedy-Martin and had higher response rate and longer time to progress Preferred on a cost-minimisation basis Ramsey, USA Comparison of NVP+P with PAX+P No difference in survival or cancer related quality of life; Moinpour et al NVB+P less costly; preferred on a cost-minimisation basis Earle and Evans Canada Comparison of PAC alone with BSC Incremental Cost per LYS varied from $4 778 $ depending on assumptions ($A6 428 $28 986) Rubio-Terres, Spain Comparison of DOC+P; PAX+P; No difference in survival Tisaire et al PAX+C Doc+P less costly; preferred on cost-minimisation basis POHEM is a population health micro-simulation model developed by Statistics Canada, which is used to evaluate interventions. The lung cancer model was developed in collaboration with oncologists at the Ottawa Regional Cancer Centre (ORCC). Abbreviations: BSC: best supportive care; DOC: docetaxel; DOC+P: docetaxel & cisplatin; E+P: etoposide & cisplatin ; G: gemcitabine; G+P: gemcitabine & cisplatin; MIC: ; MIP: mitomycin, ifosfamide & cisplatin; NVB: vinorelbine; NVB +P: vinorelbine & cisplatin; NVP+P: ; PAX: paclitaxel; PAX+C: paclitaxel & carboplatin; PAX+P: paclitaxel & cisplatin ; T+P: teniposide & cisplatin ; VIN+P: vindesine & cisplatin; VLB+P: vinblastine & cisplatin; VP-16-P 204 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
217 RADIOTHERAPY AND COMBINATION THERAPIES Coy, Schaafsma et al 68 has estimated the incremental cost per LYS and cost per QALY for high dose palliative radiotherapy for advanced NSCLC compared with BSC to be $ per LYS ($A13 500) and $ per QALY ($A18 900). However, this study was not based on trial data and the results were sensitive to assumptions about cost and survival benefit. Evans, Will et al 69 have used the Canadian POHEM model to examine the costeffectiveness of combined modality interventions (pre and post operative chemotherapy and pre and post operative chemotherapy and radiotherapy) for Stage III NSCLC. They estimate that the cost per LYS ranges from $3 348 $ ($A ) for Stages IIIA and IIIB cancer, and may be lower with outpatient therapy. However, again, these results are not based on trial data and are sensitive to estimates of cost and survival gain. TREATMENT OF SMALL CELL LUNG CANCER (SCLC) The cost-effectiveness literature with regards to the treatment of small cell lung cancer is sparse, with only 5 articles located. Four studies evaluated alternative chemotherapy options including: pre emptive administration of G-CSF for patients treated with conventional myelosuppressive cytotoxic chemotherapy, routine use of granulocyte colony stimulating factor, cisplatin in combination with either etoposide or etoposide phosphate, and oral versus intravenous etoposide. A further study on the effectiveness of prophylactic cranial irradiation was also reviewed. As each study tackles a different treatment question it is difficult to draw conclusions or make any recommendations from the available literature. At best, these studies provide an initial indication of possible cost-effectiveness for certain treatment options. References 1. Australian Institute of Health and Welfare., Australasian Association of Cancer Registries: Cancer in Australia Canberra, Australian Institute of Health and Welfare; Australasian Association of Cancer Registries, Goumas C, O Connell D, Smith D, et al: Lung Cancer in NSW in 1973 to Supramaniam R, Smith DP, Coates MS, et al: Survival from cancer in New South Wales 1980 to Mathers C, Vos T, Stevenson C, et al: The burden of disease and injury in Australia. Canberra, Australian Institute of Health and Welfare, Mathers C, Australian Institute of Health and Welfare: Health system costs of cancer in Australia : an analysis of costs, service use, incidence and mortality by type of cancer. Canberra, Australian Institute of Health and Welfare, NHMRC: How to compare the costs and benefits: evaluation of the economic evidence Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 205
218 7. Buck DJ, Richmond RL, Mendelsohn CP: Cost-effectiveness analysis of a family physician delivered smoking cessation program. Preventive Medicine 31:641 8, Viney R, Haas M, Seymour J: Seeing through the smoke: using economic evaluation to allocate health promotion resources to prevent smoking. Health Promotion Journal of Australia 6:7 15, Sinclair HK, Silcock J, Bond CM, et al: The cost-effectiveness of intensive pharmaceutical intervention in assisting people to stop smoking. International Journal of Pharmacy Practice 7: , Crealey GE, McElnay JC, Maguire TA, et al: Costs and effects associated with a community pharmacy-based smoking-cessation programme. Pharmacoeconomics 14:323 33, Croghan IT, Offord KP, Evans RW, et al: Cost-effectiveness of treating nicotine dependence: the Mayo Clinic experience. Mayo Clinic Proceedings 72:917 24, Prathiba BV, Tjeder S, Phillips C, et al: A smoking cessation counsellor: should every hospital have one? Journal of the Royal Society of Health 118:356 9, Lennox AS, Osman LM, Reiter E, et al: Cost-effectiveness of computer tailored and non-tailored smoking cessation letters in general practice: randomised controlled trial. BMJ 322:1396, Akehurst RL, Piercy J: Cost-effectiveness of the use of transdermal Nicorette patches relative to GP counselling and nicotine gum in the prevention of smoking-related diseases. British Journal of Medical Economics 7: , Akehurst R, Piercy J: Cost-effectiveness of the use of Nicorette nasal spray to assist quitting smoking among heavy smokers. British Journal of Medical Economics 7: , Fiscella K, Franks P: Cost-effectiveness of the transdermal nicotine patch as an adjunct to physicians smoking cessation counselling. [see comments.]. JAMA 275: , Stapleton JA, Lowin A, Russell MA: Prescription of transdermal nicotine patches for smoking cessation in general practice: evaluation of cost-effectiveness. Lancet 354:210 5, Wasley MA, McNagny SE, Phillips VL, et al: The cost-effectiveness of the nicotine transdermal patch for smoking cessation. Preventive Medicine 26:264 70, Mudde AN, De Vries H: The reach and effectiveness of a national mass media-led smoking cessation campaign in The Netherlands. American Journal of Public Health 89:346 50, Ratcliffe J, Cairns J, Platt S: Cost effectiveness of a mass media-led anti-smoking campaign in Scotland. Tobacco Control 6:104 10, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
219 21. Tillgren P, Rosen M, Haglund BJ, et al: Cost-effectiveness of a tobacco quit and win contest in Sweden. Health Policy 26:43 53, Stevens W, Thorogood M, Kayikki S: Cost-effectiveness of a community antismoking campaign targeted at a high risk group in London. Health Promotion International 17:43 50, Tengs TO, Osgood ND, Chen LL: The cost-effectiveness of intensive national schoolbased anti-tobacco education: results from the tobacco policy model. Preventive Medicine 33:558 70, Warner KE, Smith RJ, Smith DG, et al: Health and economic implications of a worksite smoking-cessation program: a simulation analysis. Journal of Occupational & Environmental Medicine 38:981 92, Meenan RT, Stevens VJ, Hornbrook MC, et al: Cost-effectiveness of a hospital-based smoking cessation intervention. Medical Care 36:670 8, Nielsen K, Fiore MC: Cost-benefit analysis of sustained-release bupropion, nicotine patch, or both for smoking cessation. Preventive Medicine 30:209 16, Johnson CD, Lucas LM, Uchishiba MA: Efficacy and cost-effectiveness analysis of NRT patches vs. once-daily bupropion SR: A retrospective chart review. Journal of Pharmacy Technology 17: , Halpern MT, Khan ZM, Young TL, et al: Economic model of sustained-release bupropion hydrochloride in health plan and work site smoking-cessation programs. [erratum appears in Am J Health Syst Pharm 2000 Oct 1;57(19):1803.]. American Journal of Health-System Pharmacy 57:1421 9, Caro JJ, Klittich WS, Strauss G: Could chest X-ray screening for lung cancer be cost-effective? Cancer 89:2502 5, Baba Y, Takahashi M, Tominguchi S, et al: Cost-effectiveness decision analysis of mass screening for lung cancer. Academic Radiology 5 Suppl 2:344 6, Marshall D, Simpson KN, Earle CC, et al: Potential cost-effectiveness of one-time screening for lung cancer (LC) in a high risk cohort. Lung Cancer 32:227 36, Marshall D, Simpson KN, Earle CC, et al: Economic decision analysis model of screening for lung cancer. European Journal of Cancer 37: , Okamoto N: Cost-effectiveness of lung cancer screening in Japan. Cancer 89: , Chirikos TN, Hazelton T, Tockman M, et al: Screening for lung cancer with CT: a preliminary cost-effectiveness analysis. Chest 121: , Raab SS, Hornberger J, Raffin T: The importance of sputum cytology in the diagnosis of lung cancer: a cost-effectiveness analysis. Chest 112:937 45, Canadian Lung Oncology Group: Investigation for mediastinal disease in patients with apparently operable lung cancer. Annals of Thoracic Surgery 60:1382 9, 1995 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 207
220 37. Investigating extrathoracic metastatic disease in patients with apparently operable lung cancer. The Canadian Lung Oncology Group. Ann.Thorac.Surg. 71: , Valk PE, Pounds TR, Tesar RD, et al: Cost-effectiveness of PET imaging in clinical oncology. Nuclear Medicine & Biology 23:737 43, von Schulthess GK, Steinert HC, Dummer R, et al: Cost-effectiveness of whole-body PET imaging in non-small cell lung cancer and malignant melanoma. Academic Radiology 5:300 2, Dietlein M, Weber K, Gandjour A, et al: Cost-effectiveness of FDG-PET for the management of potentially operable non-small cell lung cancer: priority for a PET-based strategy after nodal-negative CT results. European Journal of Nuclear Medicine 27: , Scott WJ, Shepherd J, Gambhir SS: Cost-effectiveness of FDG-PET for staging non-small cell lung cancer: a decision analysis. Annals of Thoracic Surgery 66: , Viney RC, Fulham MJ, McCaughan BC, et al: Evaluation of the role of positron emission tomography in oncology. Medical Journal of Australia 172:459, van Tinteren H, Hoekstra OS, Smit EF, et al: Effectiveness of positron emission tomography in the preoperative assessment of patients with suspected non-smallcell lung cancer: the PLUS multicentre randomised trial. The Lancet 359: , Boyer M, Viney R, Fulham M, et al: A randomised trial of conventional staging (CS) with or without positron emission tomography (PET) in patients with Stage 1 or 2 Non-Small Cell Lung Cancer Younes RN, Gross JL, Deheinzelin D: Follow-up in lung cancer: how often and for what purpose? Chest 115:1494 9, Gilbert S, Reid KR, Lam MY, et al: Who should follow up lung cancer patients after operation? Annals of Thoracic Surgery 69: , Egermann U, Jaeggi K, Habicht JM, et al: Regular follow-up after curative resection of nonsmall cell lung cancer: a real benefit for patients? European Respiratory Journal 19: , Clegg A, Scott DA, Hewitson P, et al: Clinical and cost effectiveness of paclitaxel, docetaxel, gemcitabine, and vinorelbine in non-small cell lung cancer: a systematic review. Thorax 57:20 8, Palmer AJ, Brandt A: The cost-effectiveness of four cisplatin-containing chemotherapy regimens in the treatment of stages III B and IV non-small cell lung cancer: an Italian perspective. Monaldi Archives for Chest Disease 51:279 88, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
221 50. Will BP, Berthelot JM, Nobrega KM, et al: Canada s Population Health Model (POHEM): a tool for performing economic evaluations of cancer control interventions. European Journal of Cancer 37: , Berthelot JM, Will BP, Evans WK, et al: Decision framework for chemotherapeutic interventions for metastatic non-small-cell lung cancer. Journal of the National Cancer Institute 92:1321 9, Koch P, Johnson N, van Schaik J, et al: Gemcitabine: clinical and economic impact in inoperable non-small cell lung cancer. Anti-Cancer Drugs 6 Suppl 6:49 54, Billingham LJ, Bathers S, Burton A, et al: Patterns, costs and cost-effectiveness of care in a trial of chemotherapy for advanced non-small cell lung cancer. Lung Cancer 37: , Annemans L, Giaccone G, Vergnenegre A: The cost-effectiveness of paclitaxel (Taxol) + cisplatin is similar to that of teniposide + cisplatin in advanced non-small cell lung cancer: a multicountry analysis. Anti-Cancer Drugs 10:605 15, Smith TJ, Hillner BE, Neighbors DM, et al: Economic evaluation of a randomized clinical trial comparing vinorelbine, vinorelbine plus cisplatin, and vindesine plus cisplatin for non-small-cell lung cancer. Journal of Clinical Oncology 13: , Hillner BE, Smith TJ: Cost-effectiveness analysis of three regimens using vinorelbine (Navelbine) for non-small cell lung cancer. Seminars in Oncology 23:25 30, Hillner BE, Smith TJ: Overview of economic analysis of Le Chevalier Vinorelbine Study. Oncology (Huntington) 12:14 6, Evans WK, Le Chevalier T: The cost-effectiveness of navelbine alone or in combination with cisplatin in comparison to other chemotherapy regimens and best supportive care in stage IV non-small cell lung cancer. European Journal of Cancer 32A: , Evans WK: Cost-effectiveness of vinorelbine alone or vinorelbine plus cisplatin for stage IV NSCLC. Oncology (Huntington) 12:18 25, Evans WK: An estimate of the cost effectiveness of gemcitabine in stage IV non-small cell lung cancer. Seminars in Oncology 23:82 9, Evans WK: Cost-effectiveness of gemcitabine in stage IV non-small cell lung cancer: an estimate using the Population Health Model lung cancer module. Seminars in Oncology 24:7 56, Earle CC, Evans WK: Cost-effectiveness of paclitaxel plus cisplatin in advanced non-small-cell lung cancer. British Journal of Cancer 80: , Leighl NB, Shepherd FA, Kwong R, et al: Economic analysis of the TAX 317 trial: Docetaxel versus best supportive care as second-line therapy of advanced non-small-cell lung cancer. Journal of Clinical Oncology 20: , 2002 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 209
222 64. Sacristan JA, Kennedy-Martin T, Rosell R, et al: Economic evaluation in a randomized phase III clinical trial comparing gemcitabine/cisplatin and etoposide/ cisplatin in non-small cell lung cancer. Lung Cancer 28:97 107, Ramsey SD, Moinpour CM, Lovato LC, et al: Economic analysis of vinorelbine plus cisplatin versus paclitaxel plus carboplatin for advanced non-small-cell lung cancer. Journal of the National Cancer Institute 94:291 7, Earle CC, Evans WK: Management Issues for Stage IV Non-Small Cell Lung Cancer. Cancer Control 4: , Rubio-Terres C, Tisaire JL, Kobina S, et al: Cost-minimisation analysis of three regimens of chemotherapy (docetaxel-cisplatin, paclitaxel-cisplatin, paclitaxelcarboplatin) for advanced non-small-cell lung cancer. Lung Cancer 35:81 9, Coy P, Schaafsma J, Schofield JA: The cost-effectiveness and cost-utility of highdose palliative radiotherapy for advanced non-small-cell lung cancer. International Journal of Radiation Oncology, Biology, Physics 48: , Evans WK, Will BP, Berthelot JM, et al: Cost of combined modality interventions for stage III non-small-cell lung cancer. Journal of Clinical Oncology 15: , Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
223 APPENDICES Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 211
224 APPENDIX 1 TNM STAGING Source: UICC TNM Classification of Malignant Tumours Edited by LH Sobin and CH Wittekind, 6th Edition, Wiley-Liss LUNG TUMOURS INTRODUCTORY NOTES Each site is described under the following headings: Rules for classification with the procedures for assessing T, N and M categories; additional methods may be used when they enhance the accuracy of appraisal before treatment Anatomical subsites where appropriate Definition of the regional lymph nodes TNM Clinical classification ptnm Pathological classification G Histopathological grading where applicable Stage grouping Summary REGIONAL LYMPH NODES Direct extension of the primary tumour into lymph nodes is classified as lymph node metastasis. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 213
225 DISTANT METASTASIS The categories M1 and pm1 may be further specified according to the following notation: Pulmonary PUL Bone marrow MAR Osseous OSS Pleura PLE Hepatic HEP Peritoneum PER Brain BRA Adrenals ADR Lymph nodes LYM Skin SKI Others OTH R CLASSIFICATION The absence or presence of residual tumour after treatment is described by the symbol R. The definitions of the R classification are: RX Presence of residual tumour cannot be assessed R0 No residual tumour R1 Microscopic residual tumour R2 Macroscopic residual tumour 214 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
226 LUNG (ICD-0 C34) RULES FOR CLASSIFICATION The classification applies only to carcinomas. There should be histological confirmation of the disease and division of cases by histological type. The following are the procedures for assessing T, N and M categories: T categories Physical examination, imaging, endoscopy, and/or surgical exploration N categories Physical examination, imaging, endoscopy, and/or surgical exploration M categories Physical examination, imaging, and/or surgical exploration ANATOMICAL SUBSITES 1. Main bronchus (C34.0) 2. Upper lobe (C34.1) 3. Middle lobe (C34.2) 4. Lower lobe (C34.3) REGIONAL LYMPH NODES The regional lymph nodes are the intrathoracic, scalene and supraclavicular nodes. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 215
227 TNM CLINICAL CLASSIFICATION T - PRIMARY TUMOUR TX Primary tumour cannot be assessed, or tumour proven by the presence of malignant cells in sputum or bronchial washings but not visualised by imaging or bronchoscopy T0 No evidence of primary tumour Tis Carcinoma in situ T1 Tumour 3 cm or less in greatest dimension, surrounded by lung or visceral pleura, without bronchoscopic evidence of invasion more proximal than the lobar bronchus (ie., not in the main bronchus) 1 T2 Tumour with any of the following features of size or extent: More than 3 cm in greatest dimension Involves main bronchus, 2 cm or more distal to the carina Invades visceral pleura Associated with atelectasis or obstructive pneumonitis that extends to the hilar region but does not involve the entire lung T3 Tumour of any size that directly invades any of the following: chest wall (including superior sulcus tumours), diaphragm, mediastinal pleura, parietal pericardium; or tumour in the main bronchus less than 2 cm distal to the carina but without involvement of the carina; or associated atelectasis or obstructive pneumonitis of the entire lung T4 Tumour of any size that invades any of the following: mediastinum, heart, great vessels, trachea, oesophagus, vertebral body, carina; separate tumour nodule(s) in the same lobe; tumour with malignant pleural effusion 2 Notes: 1 The uncommon superficial spreading tumour of any size with its invasive component limited to the bronchial wall, which may extend proximal to the main bronchus, is also classified as T1. 2 Most pleural effusions with lung cancer are due to tumour. In a few patients, however, multiple cytopathological examinations of pleural fluid are negative for tumour, and the fluid is non-bloody and is not an exudate. Where these elements and clinical judgement dictate that the effusion is not related to the tumour, the effusion should be excluded as a staging element and the patient should be classified as T1, T2 or T Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
228 N REGIONAL LYMPH NODES NX N0 N1 N2 N3 Regional lymph nodes cannot be assessed No regional lymph node metastasis Metastasis in ipsilateral peribronchial and/or ipsilateral hilar lymph nodes and intrapulmonary nodes, including involvement by direct extension Metastasis in ipsilateral mediastinal and/or subcarinal lymph node(s) Metastasis in contralateral mediastinal, contralateral hilar, ipsilateral or contralateral scalene, or supraclavicular lymph node(s) M DISTANT METASTASIS MX M0 M1 Distant metastasis cannot be assessed No distant metastasis Distant metastasis, includes separate tumour nodule(s) in a different lobe (ipsilateral or contralateral) PTNM PATHOLOGICAL CLASSIFICATION The pt, pn, and pm categories correspond to the T, N, and M categories. pn0 Histological examination of hilar and mediastinal lymphadenectomy specimen(s) will ordinarily include 6 or more lymph nodes. If the lymph nodes are negative, but the number ordinarily examined is not met, classify as pn0. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 217
229 G HISTOPATHOLOGICAL GRADING GX Grade of differentiation cannot be assessed G1 Well differentiated G2 Moderately differentiated G3 Poorly differentiated G4 Undifferentiated STAGE GROUPING Occult carcinoma TX N0 M0 Stage 0 Tis N0 M0 Stage IA T1 N0 M0 Stage IB T2 N0 M0 Stage IIA T1 N1 M0 Stage IIB T2 N1 M0 T3 N0 M0 Stage IIIA T1, T2 N2 M0 T3 N1, N2 M0 Stage IIIB Any T N3 M0 T4 Any N M0 Stage IV Any T Any N M1 218 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
230 SUMMARY Lung TX T1 T2 T3 T4 N1 N2 N3 M1 Positive cytology only < 3 cm >3 cm, main bronchus >2 cm from carina, invades visceral pleura, partial atelectasis Chest wall, diaphragm, pericardium, mediastinal pleura, main bronchus <2 cm from carina, total atelectasis Mediastinum, heart, great vessels, carina, trachea, oesophagus, vertebra; separate nodules in same lobe, malignant pleural effusion Ipsilateral peribronchial, ipsilateral hilar Ipsilateral mediastinal, subcarinal Contralateral mediastinal or hilar, scalene or supraclavicular Includes separate nodule in different lobe Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 219
231 Reproduced from UICC TNM Supplement, 2nd Edition. A Commentary on Uniform Use. Edited by CH Wittekind, DE Henderson, RVP Hutter, LH Sobin. Wiley-Liss, 2002 LUNG RULES FOR CLASSIFICATION The classification applies to all types of carcinoma including small cell carcinoma. It does not apply to carcinoids. T Classification Summary Lung T1 < 3 cm T2 >3 cm, main bronchus > 2 cm from carina, invades visceral pleura, partial atelectasis T3 T4 Chest wall, diaphragm, pericardium, mediastinal pleura Main bronchus <2 cm from carina, total atelectasis Mediastinum, heart, great vessels, carina, trachea, oesophagus, vertebra; separate nodules in same node, malignant effusion 1. Tumour with local invasion of another lobe without tumour on the pleural surface should be classified as T2. 2. Invasion of phrenic nerve is classified as T3. 3. Vocal cord paralysis (resulting from invasion of the recurrent branch of the vagus nerve), superior vena caval obstruction or compression of the trachea or oesophagus is classified as T4. 4. T4 the great vessels are: Aorta Superior vena cava Inferior vena cava Main pulmonary artery (pulmonary trunk) Intrapericardial portions of the right and left pulmonary artery Intrapericardial portions of the superior and inferior right and left pulmonary veins Invasion of more distal branches does not qualify for classification as T Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
232 5. Direct extension to parietal pericardium is classified T3 and to visceral pericardium, T4. 6. Pleural effusion is classified as T4, unless there are multiple negative cytological examinations. 7. Tumour foci in the ipsilateral parietal and visceral pleura that are discontinuous from direct pleural invasion by the primary tumour are classified as T4. 8. Invasion of visceral pleura (T2) includes not only perforation of the mesothelium but also invasion of the lamina propria serosae. 9. Tumour extending to rib is classified as T Pericardial effusion is classified the same as pleural effusion. 11. Multiple tumours of the same histological type in the same lobe is T4, but in different lobes is M Multiple tumours of different histological type in the same lobe or in different lobes should be classified as T1-4 (m). M Classification Discontinuous tumours outside the parietal pleura in the chest wall or in the diaphragm are classified as M1. Small Cell Carcinoma The TNM classification and stage grouping should be applied to small cell carcinoma. TNM is of significance for prognosis of small cell carcinoma [21], and has the advantage of providing a uniform detailed classification of tumour spread. The former categories limited and extensive for small cell carcinoma have been inconsistently defined and used. The category limited disease as used in Veterans Administration Lung Cancer Study Group system for classification of small cell carcinoma [15] corresponds to Stages I and III A to extensive disease to Stages III B ( extensive disease I ) and IV ( extensive disease II ). Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 221
233 APPENDIX 2 MODIFIED STAGING FOR SMALL CELL LUNG CANCER THE VETERANS ADMINISTRATION LUNG STUDY GROUP (VALG) CLASSIFICATION 1 LIMITED DISEASE (a) disease confined to one hemithorax, although local extensions may be present; (b) no extrathoracic metastases except for possible ipsilateral, supraclavicular nodes if they can be included in the same (radiotherapy) portal as the primary tumour; (c) primary tumour and regional nodes which can be adequately treated and totally encompassed in every (radiotherapy) portal. EXTENSIVE DISEASE Inoperable patients who cannot be classified as having limited disease. CONSENSUS REPORT OF THE INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER (IASLC) 2 LIMITED DISEASE Disease restricted to one hemithorax with regional lymph node metastases, including hilar, ipsilateral and contralateral mediastinal, and ipsilateral and contralateral supraclavicular nodes and should also include patients with ipsilateral pleural effusion independent of whether the cytology is positive or negative. 222 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
234 EXTENSIVE DISEASE All patients with sites of disease beyond the definition of limited disease. It is recommended that the IASLC revision of the VALG classification be used as it is independent of the subjective opinion of the radiation oncologist as to what can be adequately treated and totally encompassed. References 1. Zelen M. Keynote address on biostatistics and data retrieval. Cancer Chemotherapy Reports Part 3, : Stahel R, Aisner J, Ginsberg R, Havemann K, Hirsch F, Ihde D, Jassem J, Karrer K, Maurer H, van Houtte P, Osterlind K. Staging and prognostic factors in small cell lung cancer. Lung Cancer 1989; 5: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 223
235 APPENDIX 3 PERFORMANCE STATUS CRITERIA OF THE EASTERN COOPERATIVE ONCOLOGY GROUP (ECOG) 1 Performance status 0 Performance status 1 Performance status 2 Performance status 3 Performance status 4 Fully active, able to carry on all pre-disease activities without restriction. Ambulatory but restricted in physically strenuous activity. Able to carry out light work or sedentary work e.g. light housework, office work. Ambulatory and capable of all self-care but unable to carry out any work activities. Up and about at least 50% of waking hours. Capable of only limited self-care, confined to bed or chair at least 50% of waking hours. Unable to carry on any self-care, totally confined to bed or chair. Reference 1. Oken MM, Creech RH, Tormey DC. Toxicity and response criteria of the Eastern Cooperative Oncology Group. American Journal of Clinical Oncology 1982; 5: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
236 APPENDIX 4 SYSTEMIC THERAPY FOR NON-SMALL CELL LUNG CANCER AN AFTERWORD Guidelines for managing lung cancer are by nature limited to what is known at a particular time, while new information becomes available continuously. In particular, new studies evaluating systemic treatments are increasingly being reported, and are likely to increase as new understandings of cancer biology are translated into new therapeutic targets. What follows is a survey of new randomised studies reported in the last 18 months that are likely to impact on systemic therapy options for treating non-small cell lung cancer. This is not a systematic review of all studies published or presented in this time, and does not replace any of the guidelines. No such new information likely to alter current management of small cell lung cancer has been reported. 1. NEW THERAPEUTIC AGENTS Gefitinib is an orally active inhibitor of the epidermal growth factor (EGFR) receptor signalling pathway. In two large (210 and 216 patients) randomised Phase II studies in non-small cell lung cancer patients whose disease had progressed after or failed to respond to systemic chemotherapy, gefitinib produced response rates of 18% and 12% and higher rates of reported improvement in patients symptoms 1,2. Although these were randomised studies, they did not have a control arm receiving supportive care alone or alternative chemotherapy. Two randomised, double-blind Phase III studies totalling over 2,000 patients with mainly stage IV disease comparing first-line chemotherapy with or without gefitinib showed no benefit from its use in this setting 3,4. Currently (August 2003) gefitinib is licensed in Australia. Until further comparative studies are available, it should not replace currently approved first or second line chemotherapy. Bronchioloalveolar cell carcinoma appears particularly dependent on EGFR signalling. Gefitinib has shown very promising activity in this subtype 5, and may become the systemic treatment of choice for this usually resistant condition. A similar drug acting on the same pathway, erlotinib, also has shown activity in non-small cell lung cancer, particularly bronchioloalveolar cell subtype 6,7. Pemetrexed, a novel antifolate drug, has been compared to a currently approved second-line drug, docetaxel, in a Phase III study of 571 patients with advanced nonsmall cell lung cancer who had received prior chemotherapy. Response rates, time to progression of disease, and survival were not significantly different but pemetrexed resulted in significantly less haematological toxicity and resultant hospitalisations for complications of neutropenia 8. Pemetrexed thus appears a reasonable alternative to docetaxel as second line chemotherapy, but is not currently approved in Australia for non-small cell lung cancer. No studies evaluating it as part of first-line chemotherapy have been reported yet. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 225
237 2. FIRST-LINE COMBINATIONS No new combinations have emerged as superior to those in the guidelines. Metaanalyses have been reported examining the role of platinum versus non-platinum combinations and the optimal number of drugs 9,10. These analyses were based on published trial data and did not consider unpublished trials or individual patient data. The results of these meta-analyses support the use of two drug platinum containing combinations as first-line chemotherapy with single agents, three drug combinations, and non-platinum combinations remaining the subject of further clinical trials. More Phase III trials are now available evaluating the combination of gemcitabine and carboplatin showing better survival that single-agent gemcitabine and older platinum based regimens 11,12. Carboplatin and gemcitabine can now be considered an alternative first line regimen to those in the guidelines. A large Phase III trial has confirmed the role of docetaxel/platinum combinations in first-line chemotherapy CHEMOTHERAPY WITH SURGERY AND/OR RADIATION THERAPY Longer follow-up has confirmed the benefit of concurrent platinum-based chemotherapy and radiation therapy for good performance status patients with unresected stage III non-small cell lung cancer. The 4-year survival was 21% with concurrent treatment and 12% with sequential treatment with no significant increase in long-term side effects 14. Many Phase II studies have examined different drug combinations with radical irradiation but no new combination has yet been reported in a Phase III study. For good performance status patients with stage IIIA (pn2) disease, a trial of 392 patients compared two different treatment approaches induction chemotherapy concurrently with moderate-dose radiation followed by surgical resection or concurrent radical radiation with chemotherapy and no surgery 15. Initial results did not demonstrate either approach to be clearly superior to the other with better long-term disease control in the surgery arm being counterbalanced by higher treatment related mortality. Currently, either arm of this trial is appropriate until longer term results are available The large (355 patient) French study of neoadjuvant chemotherapy has confirmed the benefit of this treatment in operable stage I (not T1N0) IIIA non-small cell lung cancer showing 5-year survival of 41% with neoadjuvant chemotherapy and surgery and 32% with surgery alone 16. However two recently reported adjuvant chemotherapy trials have been inconsistent. Following surgery for stage I-IIIA disease, 1206 patients were randomised to 3 cycles of platinum-based chemotherapy or observation. No differences in recurrence rate or survival were observed 17. However in another trial of very similar design, 1867 patients received 3 4 cycles of platinum based chemotherapy or observation and the chemotherapy group had statistically significantly improved disease-free and overall survival. In this trial, the 5-year survival rate was 45% with adjuvant chemotherapy and 40% with surgery alone 18. Further trials of adjuvant chemotherapy are expected to report results in the next months. 226 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
238 References 1. Fukuoka M, Yano S, Giaccone G, et al. Multi-institutional randomized Phase II trial of gefitinib for previously treated patients with advanced non-small cell lung cancer. J Clin Oncol, 21: , Kris MG, Natale RB, Herbst RS, et al. A Phase II trial of ZD1839 (Iressa) in advanced non-small cell lung cancer (NSCLC) patients who had failed platinum- and docetaxel-based regimens (IDEAL 2). Proc Am Soc Clin Oncol, 21:292a, 2002 (abst). 3. Giaccone G, Johnson DH, Manegold C, et al. A Phase III clinical trial of ZD1839 (Iressa) in combination with gemcitabine and cisplatin in chemotherapy-naïve patients with advanced non-small cell lung cancer (INTACT 1). 4. Johnson DH, Herbst R, Giaccone G, et al. ZD1839 (Iressa) in combination with paclitaxel & carboplatin in chemotherapy-naïve patients with advanced non-small cell lung cancer (NSCLC): Results from a Phase III clinical trial (INTACT 2). 5. West HL, Franklin WA, Gemerlock P, et al. ZD1839 (Iressa) in advanced bronchioloalveolar carcinoma (BAC): A preliminary report of SWOG S0126. Lung Cancer 41(suppl 2):S56, 2003 (abst). 6. Perez-Solar R, Chachoua A, Huberman M, et al. Final results from a Phase II study or erlotinib (Tarceva) monotherapy in patients with advanced non-small cell lung cancer following failure of platinum-based chemotherapy. Lung Cancer 41(suppl 2):S246, 2003 (abst). 7. Patel JD, Miller VA, Kris MG, et al. Encouraging activity and durable reponses demonstrated by the epidermal growth factor receptor-tyrosine kinase inhibitor, erlotinib (Tarceva, OSI774), in patients with advanced bronchioloalveolar cell carcinoma. Lung Cancer 41(suppl 2):S56, 2003 (abst). 8. Shepherd FA, Pereira JR, von Pawel J, et al. A Phase III study of pemetrexed vs docetaxel in patients with advanced non-small cell lung cancer (NSCLC) who were previously treated with chemotherapy. Lung Cancer 41(suppl 2):S4, 2003 (abst). 9. Delbaldo C, Syz N, Michiels S, Le Chevalier T, Pignon, J-P. Adding a second or a third drug to a chemotherapy regimen in patients with advanced non-small cell lung carcinoma (NSCLC): A meta-analysis of the literature. Proc Am Soc Clin Oncol, 22:623, 2003 (abst). 10. D Addario G, Pintille M, Cerny T, Feld R, Leighl NB, Shepherd FA. Platinum-based versus non-platinum-based chemotherapy in advanced non-small cell lung cancer (NSCLC): A meta-analysis of the published literature. Lung Cancer 41(suppl 2):S68, 2003 (abst). Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 227
239 11. Rudd RM, Gower NH, James LE, et al. Phase III randomised comparison of gemcitabine and carboplatin (GC) with mitomycin, ifosfamide and cisplatin (MIP) in advanced non-small cell lung cancer (NSCLC). Proc Am Soc Clin Oncol, 21:292a, 2002 (abst). 12. Senderholm C. Gemcitabine compared with gemcitabine plus carboplatin in advanced non-small cell lung cancer (NSCLC): A Phase III study by the Swedish Lung Cancer Study Group (SLUSG). Proc Am Soc Clin Oncol, 21:291a, 2002 (abst). 13. Fossella F, Pereira JR, von Pawel J, et al. Randomized, multinational, Phase III study of docetaxel plus platinum combinations versus vinorelbine plus cisplatin for advanced non-small cell lung cancer: The TX326 study group. J Clin Oncol, 21:xxx, Curran WJ, Scott CB, Langer CJ, Komaki R, et al. Long-term benefit is observed in a Phase III comparison of sequential vs concurrent chemo-radiation for patients with unresected stage III NSCLC: RTOG Proc Am Soc Clin Oncol, 22:621, 2003 (abst). 15. Albain KS, Scott CB, Rusch VR, et al. Phase III comparison of concurrent chemotherapy plus radiotherapy (CT/RT) and CT/RT followed by surgical resection for stage IIIA(pN2) non-small cell lung cancer (NSCLC): Initial results from intergroup trial Proc Am Soc Clin Oncol, 22:621, 2003 (abst). 16. Depierre A, Westeel V, Milleron B, et al. 5-year results of the French randomized study comparing preoperative chemotherapy followed by surgery and primary surgery in resectable stage 1 (except T1N0), II and IIIA non-small cell lung cancer. Lung Cancer 41(suppl 2):S62, 2003 (abst). 17. Tonato M. Final report of the Adjuvant Lung Project Italy (ALPI): an Italian/EORTC- LCG randomised trial of adjuvant chemotherapy in completely resected non-small cell lung cancer. Proc Am Soc Clin Oncol, 21:290a, 2002 (abst). 18. Le Chevalier T. Results of the randomized International Adjuvant Lung Cancer Trial (IALT): cisplatin-based chemotherapy (CT) vs no CT in 1867 patients with resected non-small cell lung cancer. Proc Am Soc Clin Oncol, 23:2, 2003 (abst). 228 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
240 APPENDIX 5 ASBESTOS AND OTHER ENVIRONMENTAL CARCINOGENS Asbestos Dose-response relationships for asbestos-related lung cancer Lung cancer and other occupational carcinogens Silica and silicosis Radiation Radon Uranium Metals Arsenic Beryllium Cadmium Chromium Haematite Nickel Tin mining Man-made mineral fibres (MMMF) Polycyclic aromatic hydrocarbons (PAH) and other environmental pollutants PAH Diesel exhaust fumes (DEF) Cooking oil vapours Occupations associated with increased risks for lung cancer Scar cancer of the lung Diffuse interstitial fibrosis and lung cancer Pulmonary emphysema and other forms of obstructive airways disease Adenomatous hyperplasia as a precursor for adenocarcinoma of the lung Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 229
241 There is little doubt that lung cancer related to inhalation of occupational carcinogens is under-recognised across industrialised societies. There are several reasons for this under-recognition: one is that the lung cancer burden across industrialised nations is overwhelmingly attributable to tobacco smoking that physicians may look no further for an explanation for lung cancer among their patients 1. Although some occupational lung cancers, notably asbestos-related or silica-related lung cancer, may occur in association with other disorders induced by the same occupational factor (for example asbestos-related pleural plaques, asbestosis or silicosis), which may point to the specific carcinogen in some patients (but by no means all), occupational lung cancer per se has no clinical or pathological features that allow its recognition as distinct from the general background of lung cancer in society. It follows that identification of occupational lung cancer is critically dependent upon a systematic and detailed job history. About 1 5% of the workforce is exposed to carcinogens in the workplace, and about 75% of all occupational cancers affect the lungs and pleura. From the lung cancer to mesothelioma ratio and data from overseas, one can estimate that about lung cancers related in part to asbestos exposure occur each year in Australia and about 300 cases related in part to exposure to other lung carcinogens. Steenland et al 2 estimated that approximately men and women develop lung cancer each year in the United States because of past exposure to occupational carcinogens, and more than half of these lung cancers are related to asbestos. These authors considered the estimates to be conservative, because (i) the analysis was restricted to confirmed carcinogens only, discounting occupations with excess lung cancer risk but for which the specific carcinogens remained unidentified, and (ii) the estimated numbers of workers exposed was probably too low. In 1992, Teschke and Barroetavena 3 reported that for the years , about 0.15% to 0.76% of incident cases of lung cancer were compensated across British Columbia, Saskatchewan and Ontario in Canada. In comparison, the estimated population-attributable risk percentage (PAR%) for lung cancer across the same three provinces was 3 17%. Asbestos was the agent listed for 36% of the lung cancer claims. Teschke and Barroetavena 3 concluded that accepted claims for lung cancer were lower by a factor of four or more than the lowest PAR% estimates from epidemiological studies in the US and Britain, suggesting under-reporting of occupational lung cancer. ASBESTOS About 4 12% of lung cancers in industrialised societies can be attributed in part to occupational exposure to asbestos 4,5,6,7. From mesothelioma estimates in Peto et al 8, one can predict that about lung cancer deaths are likely to occur in six nations of Western Europe (Britain, France, Germany, Italy, The Netherlands and Switzerland) over the next 35 years if a lung cancer:mesothelioma ratio of 1:1 holds, and at a ratio of 2:1, the estimate climbs to Tossavainen 4 estimates that about asbestos-related lung cancers and mesotheliomas occur each year across North America, Australia, and seven nations in Western Europe and Scandinavia (combined population ~ ). 230 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
242 The number of officially registered deaths from asbestos-induced diseases in the United Kingdom for the years included mesotheliomas (males = ; females = 2 701) and lung cancers: a lung cancer to mesothelioma ratio of about 0.1:1. This ratio has shown only minor variation over the years in figures published by the Health & Safety Commisssion 1, but an Office of Population Censuses (OPCS) / Health Safety Executive (HSE) document 9 published in 1995 reported that asbestos exposure caused about equal numbers of excess deaths from lung cancer (~200) and mesothelioma (183) for the period , a ratio of 1.09:1. In a study of cancer mortality among about asbestos factory workers in east London followed for over 30 years since first exposure 10, the excess lung cancer to mesothelioma ratio was 1.55:1. The analogous ratio in Germany for 1998 was 1.24:1 after introduction in 1992 of the 25 fibres/ml-years exposure standard for compensation of asbestos-related lung cancer (747 lung cancers; 602 mesotheliomas). Lung cancers also appear to be under-represented among asbestos-related diseases compensated in New South Wales (NSW) in Australia. For example, the 1998 Report of the NSW Dust Diseases Board lists the following determinations among claims during : 96 mesotheliomas in comparison to 9 asbestos induced carcinomas of the lung : a lung cancer:mesothelioma ratio of 0.09:1 (for disablement); the certificates for death comprised 104 mesotheliomas versus 14 lung cancers, a ratio of 0.13:1. Predictions for asbestos-related disorders in Australia (population ~ ) for the years include about cases of lung cancer (range to ) 11,12. Most asbestos-related lung cancers are attributable to the combined effects of asbestos and tobacco smoke, so that it is necessary to allow for cigarette smoking in comparable reference populations not exposed to asbestos in order to estimate the excess number of asbestos-attributable lung cancers. In this respect, the synergy between tobacco smoke and asbestos has been studied more extensively than the analogous synergy between tobacco smoke and other occupational/environmental carcinogens (eg, radiation). In different studies the interaction between asbestos and tobacco smoke for lung cancer induction varies from more than additive to supra-multiplicative, but the relationship approximates a multiplicative model for insulation workers 13,14. The greater carcinogenicity of the amphiboles for the mesothelium in comparison to chrysotile may not extend so clearly to the induction of lung cancer 14,15, although an extensive review published in reached the conclusion that the amphiboles are substantially more potent for lung cancer induction than chrysotile (as for mesothelioma). Occupational lung cancers are neoplasms of long latency 14. Two studies that calculated the latency time from the time of first asbestos exposure to the diagnosis of the lung cancer reported mean lag-times of about 35 years and 44 years respectively 17,18. For workers producing asbestos-containing insulation materials, of whom 77% were employed for <2 years, Nicholson et al 19 observed a significantly elevated relative risk for lung cancer that occurred within 10 years and thereafter remained constant throughout the period of observation. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 231
243 Lung cancer phenotype has no value in either proving or disproving a relationship to asbestos 14,20 (or other occupational carcinogens). Roggli and Sanders 21 found that adenocarcinomas predominated among 234 asbestos-associated lung cancers, for three groups delineated (ie. Asbestosis, plaque only and no plaque/no asbestosis groups), with no significant difference in the distribution of the histological types of cancer between the three groups. (In this respect, adenocarcinoma is now also the most frequent histological type of lung cancer unrelated to asbestos.) There seems to be no significant difference in the proportion of peripheral versus central cancers in subjects exposed to asbestos, in comparison to those who were not 14. A predominance of lower lobe carcinomas among asbestos-exposed workers has been recorded in several studies, with an upper lobe to lower lobe ratio that varied from 1:1.5 to 1: Other investigators found no difference in the lobar distribution of lung cancer in such workers: Lee et al 20 and Roggli and Sanders 21 found that lung cancers in asbestos-exposed individuals were located most often in the upper lobe, in a ratio of up to 3:1 21. DOSE-RESPONSE RELATIONSHIPS FOR ASBESTOS-RELATED LUNG CANCER In most studies, a direct and linear relationship has been demonstrated between relative risk for lung cancer (RR LCA ) and cumulative exposure to asbestos, including chrysotile and the amphiboles, expressed as: RR LCA = 1 + K L + E where E is cumulative asbestos exposure, expressed as fibres/ml-years (fibre-years), and K L is the industry-specific slope of the relationship expressed as the increase in the excess risk (RR LCA 1.0) per one fibre-year of exposure. In this respect, a 1991 consensus paper 22 reviewed five government-sponsored reports that described 15 cohort studies and accepted that RR LCA is proportional to cumulative exposure. The value of K L varies across cohorts, from ( % per fibre-year) in miners and for friction products manufacture, to (0.3 9% per fibre-year) in cohorts of asbestos, asbestos cement, asbestos textile, and insulation workers. Positive estimates for K L have been obtained in all studies, but some are based on a small number of cases or deaths, and some authorities have suggested an average value of K L = 0.01 independent of fibre type after exclusion of chrysotile miners because of their substantially lower RR LCA per unit exposure corresponding to an increase of 1% in RR LCA for each fibre-year of exposure. An extensive review by Hodgson and Darnton 16 reported similar doseresponse values for amphiboles (crocidolite and amosite), but lower values for mixed exposures (with a summary increase in risk of 0.47% per fibre/ml-year of exposure), however, this review was based on 17 cohort studies and did not include data and estimates for case-referent studies. 232 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
244 The linearity of the dose-response relationship between asbestos and lung cancer risk has been questioned 16 especially whether linearity is maintained at low exposures because there are no systematic observational data for exposure levels under 1.0 fibre/ml 23. However, there is no clear proof that the relationship is non-linear at low exposures and at present the linear model is employed by most occupational health authorities for risk estimates. Recently, a case-referent study from Sweden 24,25 found that the relationship between cigarette smoke and asbestos approximated an additive model at low asbestos exposures and that the risk per fibre/ml-year was higher than predicted by linear extrapolation from high dose exposures (14% per fibre/ml-year). Several reviews published between 1991 and 2000 have supported the cumulative exposure model for lung cancer risk as a consequence of asbestos exposure 14,16,26,27,28,29,30, with no clearly delineated threshold 16 and with no requirement for asbestosis or diffuse pleural fibrosis as a pre-requisite for attribution of lung cancer to asbestos 31 : Criteria for compensation of asbestos-related lung cancer and approaches to apportionment of the relative contributions of asbestos and cigarette smoke to lung cancer induction are discussed elsewhere 14,30,31,32,33,34,35,36,37. LUNG CANCER AND OTHER OCCUPATIONAL CARCINOGENS Apart from asbestos, those substances/processes designated by the International Agency for Research on Cancer (IARC) as probable or definite human lung carcinogens include the following: acrylonitrile, aluminium production, arsenic and certain arsenical compounds, beryllium and its compounds, bis(chloromethyl) ether and chloromethyl ether, cadmium and its compounds, chromium and its compounds, coal gasification, coke production, diesel exhausts, formaldehyde, glass manufacture, iron and steel founding, mustard gas, nickel, non-arsenical pesticides, radon, silica, soot, sulphuric acid mist, talc containing asbestos fibres, and underground haematite mining 38,39,40,41,42,43,44. Detailed consideration of these agents lies beyond the scope of this document and the interested reader is referred to relevant reviews (eg, see Dubrow and Wegman 45, Morabia et al 46, Harrington and Levy 47, Hayes 48, Steenland et al 2, and Christiani 49 ). Analysis of the dose-response relationship for many of these factors is confounded by co-existent other lung carcinogens (eg, tobacco smoke, asbestos, silica/silicosis, or radon 24, 50, 51 ). The interactive effects between such carcinogens and tobacco smoke are discussed at length in a World Health Organization/International Programme on Chemical Safety (WHO/IPCS) monograph published in Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 233
245 SILICA AND SILICOSIS An increased risk of lung cancer has been reported for patients with silicosis An estimate of the relative risk for silicotics with average smoking is about 3.4 (~1.7 for those with no history of smoking) 14. From an analysis of 15 cohort and case-control studies on silicotics, Steenland et al 60 derived a summary relative risk of 2.80 (CI = ); in a further analysis of 16 studies with high exposures to silica and without confounding exposures, these authors found a moderate excess risk of lung cancer (RR = 1.33; CI = ). De Klerk and Musk 57 found that an award of compensation for silicosis conferred an immediate and constant relative risk of 1.6 for lung cancer. There has long been debate over whether the increased risk of lung cancer with silica exposure is restricted to those with silicosis or whether the increase in risk is a reflection of high cumulative exposure per se 14,59. An industry-funded cohort mortality study on North American industrial sand workers 63,64,65 found that lung cancer risk was quite strongly related to cumulative exposure 64, but in the absence of chest radiographs a link between silicosis and lung cancer risk could not be addressed. RADIATION RADON Radon ( 222 Rn) is a gaseous product formed during the decay from uranium ( 238 U) to stable lead 2. Radon has a half-life of 3.8 days and decays into short-lived radioactive isotopes of bismuth, polonium and lead, known as radon progeny or radon daughters. The daughters represent metal ions that adhere to particles suspended in the air, and their decay is accompanied by the production of α-particles. Exposure to radon progeny is usually measured in working levels (WL) and cumulative exposure is expressed as WL-months (WLM); 1.0 WL is any combination of progeny that releases 1.3 x 10 5 MeV; alternatively, exposure to radon can be expressed as picocuries per litre (pci/l) 2. One pci/l is about equivalent to WLM and the standard in the US for radon exposure in mines is 4 WLM/year 2. Occupational exposures to radon can occur during mining for uranium and other metals (see following discussion) and in the processing of ores and radioactive materials. Radon is one likely causative factor for the 10 15% of lung cancers that occur among non-smokers. Radon appears to be of particular significance in geographic regions other than Australia 74,76,77, related to well-insulated airtight homes in cold climates, and with basements where the radon gas tends to accumulate 78 (in the US, radon measuring devices are available in the market place). The association between radon and lung cancer appears to be well founded 2,24,79,80,81,82 and epidemiological studies have shown an increased risk of lung cancer with increasing exposures to radon or its decay products. For miners, the excess relative risk for lung cancer is about 1 2% per WLM Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
246 There is also evidence of synergy between radon decay products and cigarette smoke 83. However, the exact risks to the general population from radon daughters have been the subject of some dispute. There is also some evidence of a possible association between Thorotrast (also an α-particle emitter) and small-cell carcinoma of lung 84. URANIUM Lung cancer has also been recorded among Navajo uranium miners 69,85. In this group, there appears to be synergy between the uranium mining and cigarette consumption, but the median cigarette consumption was small (about 1 3 cigarettes daily). Lung cancer is also recorded among other cohorts of uranium miners, for example in the former Czechoslovakia 66,70,86 and the former East Germany 68,72,74,87, and in workers involved in uranium processing 88,89. The risk factor among uranium miners is also α-particle emission from radon daughters. MilliSieverts are now used as the radiation unit for uranium mines, although WLM were used in the past. METALS ARSENIC Epidemiological studies on copper smelter workers clearly demonstrate that inorganic arsenic is a human lung carcinogen 49 ; inorganic arsenic is a constituent of most copper ores, and also lead and zinc ores to a lesser extent 2,49, and the workers are potentially exposed to arsenic trioxide released during the smelting process. Copper smelter workers have shown a clear dose-response relationship between the standardized mortality ratio for lung cancer and cumulative arsenic exposure expressed as mg/m 3 -years 49,90. The interactive effect with tobacco smoking appeared to be additive rather than multiplicative 49. In an analysis of six studies on arsenic and lung cancer, Steenland et al 2 calculated a combined relative risk for lung cancer of 3.69 (CI = ), with a clear doseresponse effect, but they commented that lung cancer risk is primarily a consequence of past high exposures. BERYLLIUM Exposure to beryllium occurs mainly in mining and refining, and in the manufacture of ceramics and electronic and aerospace equipment. According to NIOSH estimates, about workers were exposed to beryllium in the US during the 1980s 2, and a high proportion of those so exposed showed evidence of impairment of pulmonary function, presumably as a consequence of berylliosis. (In contrast, berylliosis appears to be virtually unknown in Australia.) From an analysis of the Beryllium Case Registry in the US, Steenland and Ward 91 reported a lung cancer SMR of 2.00 (CI = ) and in a later study, Ward et al 92 reported a lung cancer SMR of 1.24 (CI = ), from analysis of 9,225 workers across seven beryllium plants in Ohio and Pennsylvania 2. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 235
247 CADMIUM Cadmium is used mainly for electroplating, as a component of electrodes in batteries, and in alloys 2. Exposure is usually by inhalation. A study on a US plant where cadmium oxide and sulphide and metal were recovered from wastes from lead and zinc smelters showed a lung cancer relative risk of 1.49 (CI = ); a dose-response effect was observed and the lung cancer relative risk was significant for workers with the highest exposures (RR = 2.72; CI = ) 2. CHROMIUM There have been more than 50 studies on lung cancer among chromium workers: Steenland et al 2 estimate the overall relative risk for lung cancer across these studies to be 2.78 (CI = ) (see also Sorahan 93 ). The chromium in most of its compounds is in the trivalent (CrIII) or hexavalent state (CrVI); CrVI induces cancer in experimental animals, but CrIII does not. HAEMATITE An excess risk of lung cancer has also been reported among Chinese haematite miners (SMR = 370) 94, but silica, radon and arsenic represent confounding factors for evaluation of the risk among iron ore miners, especially for those who worked underground 94. NICKEL A 1990 IARC 95 report on nickel carcinogenesis found that the rate of lung and nasal cancer was significantly increased among workers at nickel refineries 96,97. Steenland et al 2 estimated the combined relative risk to be 1.56 (CI = ). Studies of nickel alloy workers and stainless steel welders have not demonstrated a consistently increased number of lung cancer deaths 98,99. There is evidence that different nickel compounds confer different risks for lung cancer; although nickel carbonyl is responsible for almost all cases of acute nickel toxicity, there are few data to indicate that metallic nickel increases the risk of cancer, and the indentity of the compound(s) responsible for the increased risk of lung cancer remains unclear 100,101. TIN MINING A high incidence of lung cancer has been reported among tin miners in Yunnan, China 51. Exposures in the mines appear to be complex and to include arsenic, radon progeny and silica. After adjustment for arsenic, age, year of starting work and tobacco smoking, subjects with the highest radon exposure had an odds ratio of 9.5, and risk increased with the duration of exposure. When adjustments were carried out for tobacco use and radon exposure, workers with the highest arsenic exposure had a relative risk of lung cancer of In another group in Guangxi province, investigators found a synergistic effect between cigarette smoking and measures of occupational exposure Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
248 MAN-MADE MINERAL FIBRES (MMMF) An elevated standardised mortality ratio for lung cancer has been reported in cohorts of workers involved in the production of MMMF (including rockwool/slagwool), notably in the early technological phases 102,103, when other carcinogens were also present in the workplace (arsenic, asbestos, and polycyclic aromatic hydrocarbons) and quantitative data on tobacco smoking and airborne fibre concentrations were lacking. It is, thus, not possible to ascertain whether the risk of lung cancer was related to the MMMFs themselves. Rödelsperger et al 104 found that asbestos was a confounding factor for assessment of the carcinogencity of MMMFs. The carcinogenicity of MMMFs and other fibrous and non-fibrous substitutes for asbestos has been reviewed in detail elsewhere 15. The appears to be no convincing evidence that inhaled fibreglass is carcinogenic in humans. POLYCYCLIC AROMATIC HYDROCARBONS (PAH) AND OTHER ENVIRONMENTAL POLLUTANTS PAH PAH are produced mainly by pyrolysis or incomplete combustion of organic substances and they comprise the major sub-group of this family of compounds 49. Occupational settings that involve potential exposure to PAH include aluminium production, iron and steel foundry work, coke production and coal gasification. Ash from fuel combustion and diesel exhaust fumes also contains PAH. Accordingly, occupational exposures to PAH are common, and it has been estimated that over two million workers were exposed to PAH worldwide in the mid-1980s 49. Epidemiological studies have demonstrated an elevated risk of lung cancer among workers involved in the production of coke, with a relative risk of about 15. Other studies have shown smaller but still elevated risk of lung cancer of about DIESEL EXHAUST FUMES Diesel exhaust is a complex mixture of gas-phase and particulate-phase chemicals that include substances known to be genotoxic or carcinogenic, including polycyclic aromatic hydrocarbons. Multiple studies over the years have returned conflicting data on whether inhaled diesel exhaust fumes (DEF) are carcinogenic in humans , but there appears to be increasing evidence that DEF does increase the risk of lung cancer 105,108,109,115,117,118,119. There seems to be an interactive synergy between DEF and cigarette smoke for lung cancer risk: in a study of Swedish dock workers, Emmelin 109 found an odds ratio of 1.6 (for medium DEF exposure) and 2.9 for high DEF exposures among non-smokers; for the smokers, the respective odds ratios were 10.7 and In a meta-analysis of studies on DEF, Lipsett and Campleman 117 estimated the pooled smoking-adjusted lung cancer risk from DEF to be In a detailed case-referent Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 237
249 analysis from Sweden, Gustavsson et al 24,25 found that for the highest quartile of cumulative exposure to diesel exhaust fumes versus no exposure, the relative risk of lung cancer was 1.63 (CI = ) and was 1.60 for other combustion products (CI = ). COOKING OIL VAPOURS Several studies have reported an increased risk of lung cancer among Chinese women who inhale volatile substances released from heated cooking oils, especially for nonsmokers with adenocarcinoma 120,121,122,123,124. Fumes from heated cooking oils contain different substances that are genotoxic, mutagenic and carcinogenic, including polycyclic aromatic hydrocarbons such as benzo[a]pyrene and dibenzanthracene The risk appears to be greatest with use of unrefined rapeseed oil for cooking. Zhong et al 122 recorded an odds ratio of 1.84 with use of rapeseed oil and an odds ratio of 2.38 according to the smokiness of the oil. Table 1 Non-asbestos occupational carcinogens for lung cancer Occupational carcinogen References Arsenic 2, 49, 90 Beryllium 2, 91, 92 Cadmium 2 Chromium, especially hexavalent chromium 2, 93 Cooking oils 120, 121, 122, 123, 124, 125, 126, 127, 128, 129, 130, 131, 132 Diesel exhaust fumes 105, 106, 107, 108, 109, 110, 111, 112, 113, 114, 115, 116, 117, 118, 119 Haematite 94 Man-made mineral fibres 15, 102, 103, 104 Nickel 148, 96, 97, 98, 99, 100, 101 Polycyclic aromatic hydrocarbons 49 Radon 2, 66, 67, 68, 69, 70, 71, 72, 73, 74, 75 Silica/silicosis 53, 54, 55, 56, 57, 58, 59, 60, 149, 62 Tin mining 49,51 Uranium 66, 68, 69, 70, 72, 74, 85, 86, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
250 OCCUPATIONS ASSOCIATED WITH INCREASED RISKS FOR LUNG CANCER In 1992, Morabia et al 133 reviewed multiple case-control studies that evaluated occupational risk factors for lung cancer, and they also carried out a multi-centre case-control study of 24 hospitals in nine metropolitan areas in the United States. They found that the following occupations had a significant increase in the risk of lung cancer independent of cigarette smoking: sheet metal workers and tinsmiths; crane-men, derrick-men, and hoist-men; heated-metal workers; construction labourers and electricians, and bookbinders and related printing trade workers. In all these occupations, the workers were exposed to known or suspected carcinogens that included asbestos, nickel, chromium, PAH and diesel exhaust fumes. Burns and Swanson 134 analysed incident lung cancer cases by occupation and industry groups and found an elevated risk of lung cancer in the following occupations: excavating and mining workers (OR = 4.01); furnace workers (OR = 3.11); armed services personnel (OR = 3.10); agricultural workers (OR = 2.05); mechanics (restricted to black males: OR = 4.16); painters (OR = 1.96); and drivers (OR = 1.88). Industries with an elevated risk of lung cancer included farming (OR = 2.21), mining (OR = 2.98), and primary ferrous metals manufacture (OR = 2.43). Five of the occupations found more often among lung cancer cases had probable exposure to diesel exhaust fumes. Other occupations with reported increased lung cancer relative risks include shoe manufacture and repairs. For some industries, the excess risk appears to be attributable to asbestos (eg, pulp and paper manufacture). For asbestos-related neoplasia, the main occupational groups at carcinogenic risk during the 1990s and beyond have been the end-users of asbestos-containing products, including building construction and demolition workers, insulation workers and shipyard workers 15. SCAR CANCER OF LUNG Although the literature does contain persuasive reports of lung cancers that appeared to develop in pre-existing scars, there is compelling evidence, based on the pattern of collapse and fibrosis in pulmonary scars and collagen fibre analysis, that the scar tissue in most scar cancers is secondary to the presence of the carcinoma a desmoplastic response to the tumour, analogous to the central desmoplasia of breast cancers 135,136,137,138. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 239
251 DIFFUSE INTERSTITIAL FIBROSIS AND LUNG CANCER Lung cancer is well recognised in patients with progressive systemic sclerosis (scleroderma) and other forms of diffuse interstitial fibrosis (DIF) that include usual interstitial pneumonia (UIP; cryptogenic fibrosing alveolitis) 14 : Turner-Warwick et al 139 reported the development of lung cancer in 12.9% of 155 patients with UIP followed to death. The relative risk for lung cancer was 14.1 in comparison to the general population of comparable age and gender, allowing for the length of follow-up for the UIP cohort. The relative risk for male smokers was 14.2 and was 6.7 for female smokers. The proportions of the histological types did not obviously differ from those found in patients without pulmonary fibrosis. (By way of comparison, a report from the same hospital on mortality in 155 cases of asbestosis revealed that lung cancer was present in 44%.) In a study from Japan, Nagai et al 140 reported lung cancer in 38% of patients with DIF who were smokers and in 11% of the same group who were non-smokers. Nonetheless, in this study 88% of the tumours were peripheral in distribution and the diagnosis in 27 out of 31 cases was established by transbronchial biopsy of lung (in limited samples of this type, there is a problem in distinguishing between genuine lung cancer and the reactive bronchiolo-alveolar epithelial proliferation that is an almost invariable accompaniment of DIF). In contrast, Wells and Mannino 141 found a 5% rate of association between DIF and lung cancer in the United States in comparison to 27% for asbestosis and lung cancer, as assessed from death certificates. In this respect, there is an extraordinary association between asbestosis and lung cancer, so that lung cancer occurs in about 25 45% of cases or more and is now the leading cause of death among asbestotics 14. Oksa et al 142 identified 11 lung cancers in 24 patients with progressive asbestosis (46%; standardized incidence rate SIR = 37), in comparison to 5/54 non-progressors (9%; SIR = 4.3). Mizushima and Kobayashi 143 reviewed 154 Japanese cases of lung cancer that occurred on a background of idiopathic DIF. These cancers were found predominantly in males (most were smokers). The histological types were the same as lung cancers among patients without interstitial fibrosis, except for a higher proportion of small cell carcinoma. The tumours were mainly peripheral and located in the lower lobes. However, in an autopsy and live case control study of Japanese IPF cases, Iwai et al 144 found that the IPF rate was twice as high among those whose occupations involved exposure to dusts and organic solvents than workers in other jobs. The live case-control study showed an relative risk of 1.34 for IPF among cadmium, chromium and lead metal production workers in comparison to the non-exposed. Some of the substances implicated in the IPF cases have also been implicated in lung carcinogenesis. 240 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
252 PULMONARY EMPHYSEMA AND OTHER FORMS OF OBSTRUCTIVE AIRWAYS DISEASE From case-control studies and analysis of lung cancers among lifelong non-smokers and former smokers, elevated lung cancer odds ratios have been found for emphysema, chronic bronchitis and asthma, after adjustment for active and passive smoking 145,133 (see Table 4 1). The risk was greater for squamous cell carcinoma and for diagnosis of these disorders at older ages. However, as discussed in an earlier section of this document, these findings were non-significant after adjustment for other variables and confounding factors 145,146. ADENOMATOUS HYPERPLASIA AS A PRECURSOR FOR ADENOCARCINOMA OF THE LUNG Foci of atypical adenomatous hyperplasia in lung tissue have been invoked as a precursor for peripheral adenocarcinoma (see Kerr 147 for an extensive review and references). These lesions take the form of small poorly circumscribed foci of thickening of alveolar septa with cuboidalisation or proliferation of the lining alveolar epithelial cells that show features of Clara cell or type II pneumocyte differentiation. Nuclear atypia and pleomorphism are usually mild in degree but some lesions display high-grade atypia (about 25 30%). The degree of atypia tends to increase with increasing size of the lesions. Some authorities set an upper size limit of 5 mm for these lesions and classify any similar lesion > 5 mm in diameter as adenocarcinoma. The reported frequency of atypical adenomatous hyperplasia is very variable and depend in part on the diligence with which these lesions are sought and on the presence or absence of other pathological changes in lung tissue (eg, emphysema or pneumonitis). These lesions are probably multiple in most cases, and they are seen most often in lung tissue resected for primary lung cancer (about % of cases) in comparison to lung tissue removed for other reasons (about %). Focal adenomatous hyperplasia is more strongly associated with adenocarcinoma than other histological types of lung cancer. The prevailing evidence indicates that these lesions are involved in a sequence from dysplasia/adenoma to carcinoma, and loss of heterozygosity, p53, c-erb-2 and k-ras mutations are described in these atypical foci. References 1. Health and Safety Commission (UK). Health and Safety Statistics 1998/99. London, HSE Books Steenland K, Loomis D, Shy C, Simonsen N. Review of Occupational Lung Carcinogens. Am J Ind Med 1996; 29(5): Teschke K, Barroetavena MC. Occupational Cancer in Canada: What Do We Know? CMAJ 1992; 147(10): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 241
253 4. Tossavainen A. Asbestos, asbestosis and cancer: exposure criteria for clinical diagnosis. People and Work Research Reports, vol 14. Helsinki, Finnish Institute of Occupational Health, 1997, van Loon AJ, Kant IJ, Swaen GM, Goldbohm RA, Kremer AM, van den Brandt PA. Occupational Exposure to Carcinogens and Risk of Lung Cancer: Results From The Netherlands Cohort Study. Occup Environ Med 1997; 54(11): Mandi A, Posgay M, Vadasz P, Major K, Rodelsperger K, Tossavainen A, Ungvary G, Woitowitz HJ, Galambos E, Nemeth L, Soltesz I, Egervary M, Boszormenyi NG. Role of Occupational Asbestos Exposure in Hungarian Lung Cancer Patients. Int Arch Occup Environ Health 2000; 73(8): Rodelsperger K, Mandi A, Tossavainen A, Bruckel B, Barbisan P, Woitowitz HJ. Inorganic Fibres in the Lung Tissue of Hungarian and German Lung Cancer Patients. Int Arch Occup Environ Health 2001; 74(2): Peto J, Decarli A, La Vecchia C, Levi F, Negri E. The European Mesothelioma Epidemic. Br J Cancer 1999; 79(3 4): Hutchings S, Jones J, Hodgson J. Asbestos related diseases. Drever, F. Occupational Health Decennial Supplement no. 10. London, Office of Population Censuses (OPCS), Health and Safety Executive (HSE), 1995, Berry G, Newhouse ML, Wagner JC. Mortality From All Cancers of Asbestos Factory Workers in East London Occup Environ Med 2000; 57(11): Winder C, Leigh J. Asbestos and Cancer: the worst is yet to come. Aust Safety News. August 1998, Comin CE, de Klerk NH, Henderson DW. Malignant Mesothelioma: Current Conundrums Over Risk Estimates and Whither Electron Microscopy for Diagnosis? Ultrastruct Pathol 1997; 21(4): Vainio H, Boffetta P. Mechanisms of the Combined Effect of Asbestos and Smoking in the Etiology of Lung Cancer. Scand J Work Environ Health 1994; 20(4): Henderson DW, de Klerk NH, Hammar S, et al. Asbestos and lung cancer: is it attributable to asbestosis, or to asbestos fiber burden? Corrin B (ed) Pathology of Lung Tumors. New York: Churchill Livingstone, 1997: World Trade Organization (WTO): European Communities - Measures Concerning Asbestos and Asbestos-containing Products Geneva, WTO ( 16. Hodgson JT, Darnton A. The Quantitative Risks of Mesothelioma and Lung Cancer in Relation to Asbestos Exposure. Ann Occup Hyg 2000; 44(8): Warnock ML, Isenberg W. Asbestos Burden and the Pathology of Lung Cancer. Chest 1986; 89(1): Hillerdal G. Pleural Plaques and Risk for Bronchial Carcinoma and Mesothelioma. A Prospective Study. Chest 1994; 105(1): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
254 19. Nicholson WJ, Perkel G, Selikoff IJ, Seidman H. Cancer from occupational asbestos exposure projections Peto R, Schneiderman M (eds) Quantification of Occupational Cancer. New York: Cold Spring Harbor Laboratory, 1981: Lee BW, Wain JC, Kelsey KT, Wiencke JK, Christiani DC. Association of Cigarette Smoking and Asbestos Exposure With Location and Histology of Lung Cancer. Am J Respir Crit Care Med 1998; 157(3 Pt 1): Roggli VL, Sanders LL. Asbestos Content of Lung Tissue and Carcinoma of the Lung: a Clinicopathologic Correlation and Mineral Fiber Analysis of 234 Cases. Ann Occup Hyg 2000; 44(2): Health Effects Institute Asbestos Research (HEI-AR). Asbestos in public commercial buildings: a literature review and synthesis of current knowledge. Cambridge, Massachusetts, HEIAR, Goldberg M. Asbestos and Risk of Cancer: Exposure-Effect Relationships for Occupationally Exposed Populations [Fr]. Rev Mal Respir 1999; 16(6 Pt 2): Gustavsson P, Jakobsson R, Nyberg F, Pershagen G, Jarup L, Scheele P. Occupational Exposure and Lung Cancer Risk: a Population-Based Case-Referent Study in Sweden. Am J Epidemiol 2000; 152(1): Gustavsson P, Nyberg F, Pershagen G, et al. Asbestos, diesel exhaust and interaction with smoking in a population-based case-referent study of lung cancer in Sweden. FP50, Singapore, International Commission on Occupational Health (ICOH 2000). 26. Henderson DW, Roggli VL, Shilkin KB, et al. Is asbestosis an obligate precursor for asbestos-induced lung cancer? Peters GA, Peters BJ, (eds). Sourcebook on Asbestos Diseases, vol 11. Charlottesville: Michie Company, 1995, pp Egilman D, Reinert A. Lung Cancer and Asbestos Exposure: Asbestosis Is Not Necessary. Am J Ind Med 1996; 30(4): Case BW, Dufresne A. Asbestos, Asbestosis, and Lung Cancer: Observations in Quebec Chrysotile Workers. Environ Health Perspect 1997; 105 Suppl 5: Billings CG, Howard P. Asbestos Exposure, Lung Cancer and Asbestosis. Monaldi Arch Chest Dis 2000; 55(2): Henderson DW, Leigh J. Asbestos and lung cancer: a selective up-date to the Helsiniki Criteria for individual attribution. People and Work Research Reports, vol 36. Helsinki, Finnish Institute for Occupational Health. 2000, 36: Consensus report: asbestos, asbestosis and cancer: the Helsinki criteria for diagnosis and attribution. Helsinki, Scand J Work Environ Health. 1997; 23: Chase GR, Kotin P, Crump K, Mitchell RS. Evaluation for Compensation of Asbestos- Exposed Individuals. II. Apportionment of Risk for Lung Cancer and Mesothelioma. J Occup Med 1985; 27(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 243
255 33. BK-report Faserjahre. Berufsgenossenschaftliche Hinweise zur Ermittlung der Kumulativen Asbestfaserstaub-Dosis am Arbeitsplatz (Faserjahre) und Bearbeitungshinweise zur Berufskrankheit Nr 4104 BKV (Lungenkrebs). Report on Occupational Diseases Fibre Years 1/1997. Sankt Augustin, Schriftenreihe des Hauptverbandes der gewerblichen Berufsgenossenschaften Leigh J, Berry G, de Klerk NH, Henderson DW. Asbestos-related lung cancer: apportionment of causation and damages to asbestos and tobacco smoke. Peters GA, Peters BJ (eds) Sourcebook on Asbestos Diseases, vol 13. Charlottesville: Michie Company, 1996: Baur X, Czuppon AB. Regulation and compensation of asbestos diseases in Germany. Peters GA, Peters BJ (eds). Sourcebook on Asbestos Diseases, vol. 15. Charlottesville: Lexis, 1997: Hindry M. Asbestos-related disease compensation in France. Peters GA, Peters BJ (eds) Sourcebook on Asbestos Diseases, vol. 16. Charlottesville: Lexis, 1997: Thimpont J, De Vuyst P. Occupational asbestos-related diseases in Belgium (epidemiological data and compensation criteria). Peters GA, Peters BJ (eds) Sourcebook on Asbestos Diseases, vol 17. Charlottesville: Lexis, 1998: IARC. Cadmium, nickel, some epoxides, miscellaneous industrial chemicals and general considerations on volatile anaesthetics Lyon, France, International Agency for Research on Cancer (IARC). 39. IARC. Monographs on the evaluation of carcinogenic risks to humans: chemicals and industrial processes associated with cancers in humans Lyon, France, IARC. 40. IARC. Some metals and metallic compounds. Monograph Lyon, France, International Agency for Research on Cancer (IARC). 41. IARC. Polynuclear aromatic compounds, part 3: industrial exposures in aluminium production, coal gasification, coke production and iron and steel founding. Monograph Lyon, France, International Agency for Research on Cancer (IARC). 42. IARC. Polynuclear aromatic compounds, part 4: bitumens, coal-tars and derived products, shale oils and soots. Monograph Lyon, France, International Agency for Research on Cancer (IARC). 43. IARC. Chromium, nickel and welding. Monograph Lyon, France, International Agency for Research on Cancer (IARC) 44. IARC. Beryllium, cadmium, mercury and exposures in the glass manufacturing industry. Monograph Lyon, France, IARC. 45. Dubrow R, Wegman DH. Setting Priorities for Occupational Cancer Research and Control: Synthesis of the Results of Occupational Disease Surveillance Studies. J Natl Cancer Inst 1983; 71(6): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
256 46. Morabia A, Markowitz S, Garibaldi K, Wynder EL. Lung Cancer and Occupation: Results of a Multicentre Case-Control Study. Br J Ind Med 1992; 49: Harrington JM, Levy LS. Lung Cancer. Parkes WR (ed) Occupational Lung Disorders (3rd edn). Oxford: Butterworth-Heinemann, 1994: Hayes RB. The Carcinogenicity of Metals in Humans. Cancer Causes Control 1997; 8(3): Christiani DC. Occupationally induced pulmonary malignancy (excluding asbestos-related cancers). Banks DE, Parker JE (eds) Occupational Lung Disease: an international perspective. London: Chapman & Hall, 1998: Boffetta P, Garcia-Gomez M, Pompe-Kirn V, Zaridze D, Bellander T, Bulbulyan M, Caballero JD, Ceccarelli F, Colin D, Dizdarevic T, Espanol S, Kobal A, Petrova N, Sallsten G, Merler E. Cancer Occurrence Among European Mercury Miners. Cancer Causes Control 1998; 9(6): Qiao YL, Taylor PR, Yao SX, Erozan YS, Luo XC, Barrett MJ, Yan QY, Giffen CA, Huang SQ, Maher MM, Forman MR, Tockman MS. Risk Factors and Early Detection of Lung Cancer in a Cohort of Chinese Tin Miners. Ann Epidemiol 1997; 7(8): Environmental Health Criteria 211: Health effects of interactions between tobacco use and exposure to other agents. Geneva, World Health Organisation (WHO)/ International Programme on Chemical Safety (IPCS), Amandus HE, Shy C, Castellan RM, et al. Silicosis and lung cancer in North Carolina dusty trades workers: a summary of findings San Francisco, Western Consortium for Public Health. Program Syllabus: Second International Symposium on Silica, Silicosis and Cancer, Goldsmith DF. Silica exposure and pulmonary cancer. Samet JM (ed) Epidemiology of Lung Cancer. New York: Marcel Dekker, 1994: Koskela R-S. Association of silica dust exposure with lung cancer and other diseases. Thesis: University of Tampere Goldsmith DF, Wagner GR, Saffiotti U, et al. Second International Symposium on Silica, Silicosis and Cancer. Scand J Work Environ Health 1995; suppl de Klerk NH, Musk AW. Silica, Compensated Silicosis, and Lung Cancer in Western Australian Goldminers. Occup Environ Med 1998; 55(4): McDonald JC. Silica and lung cancer. Castranova V, Vallyathan V, Wallace WE (eds) Silica and Silica-induced Lung Diseases. Boca Raton, Florida: CRC Press, 1996: Weill H, McDonald JC. Exposure to Crystalline Silica and Risk of Lung Cancer: the Epidemiological Evidence. Thorax 1996; 51(1): Steenland K, Stayner L. Silica, Asbestos, Man-Made Mineral Fibers, and Cancer. Cancer Causes Control 1997; 8(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 245
257 61. IARC. Silica, some silicates, coal dust and para-aramid fibrils. Lyon, France, International Agency for Research on Cancer (IARC) Honma K, Chiyotani K, Kimura K. Silicosis, Mixed Dust Pneumoconiosis, and Lung Cancer. Am J Ind Med 1997; 32(6): McDonald AD, McDonald JC, Rando RJ, Hughes JM, Weill H. Cohort Mortality Study of North American Industrial Sand Workers. I. Mortality From Lung Cancer, Silicosis and Other Causes. Ann Occup Hyg 2001; 45(3): Hughes JM, Weill H, Rando RJ, Shi R, McDonald AD, McDonald JC. Cohort Mortality Study of North American Industrial Sand Workers. II. Case-Referent Analysis of Lung Cancer and Silicosis Deaths. Ann Occup Hyg 2001; 45(3): Rando RJ, Shi R, Hughes JM, Weill H, McDonald AD, McDonald JC. Cohort Mortality Study of North American Industrial Sand Workers. III. Estimation of Past and Present Exposures to Respirable Crystalline Silica. Ann Occup Hyg 2001; 45(3): Sevc J, Tomasek L, Kunz E, Placek V, Chmelevsky D, Barclay D, Kellerer AM. A Survey of the Czechoslovak Follow-Up of Lung Cancer Mortality in Uranium Miners. Health Phys 1993; 64(4): Samet JM, Pathak DR, Morgan MV, Coultas DB, James DS, Hunt WC. Silicosis and Lung Cancer Risk in Underground Uranium Miners. Health Phys 1994; 66(4): Enderle GJ, Friedrich K. East German Uranium Miners (Wismut) Exposure Conditions and Health Consequences. Stem Cells 1995; 13 Suppl 1: Roscoe RJ, Deddens JA, Salvan A, Schnorr TM. Mortality Among Navajo Uranium Miners. Am J Public Health 1995; 85(4): Tomasek L, Darby SC. Recent Results From the Study of West Bohemian Uranium Miners Exposed to Radon and Its Progeny. Environ Health Perspect 1995; 103 Suppl 2: Finkelstein MM. Clinical Measures, Smoking, Radon Exposure, and Risk of Lung Cancer in Uranium Miners. Occup Environ Med 1996; 53(10): Bruske-Hohlfeld I, Mohner M, Wichmann HE. Predicted Number of Lung Cancer Cases in Germany Among Former Uranium Miners of the Wismut. Health Phys 1997; 72(1): Luebeck EG, Heidenreich WF, Hazelton WD, Paretzke HG, Moolgavkar SH. Biologically Based Analysis of the Data for the Colorado Uranium Miners Cohort: Age, Dose and Dose-Rate Effects. Radiat Res 1999; 152(4): Kreuzer M, Grosche B, Brachner A, Martignoni K, Schnelzer M, Schopka HJ, Bruske- Hohlfeld I, Wichmann HE, Burkart W. The German Uranium Miners Cohort Study: Feasibility and First Results. Radiat Res 1999; 152(6 Suppl): S56 S Gilliland FD, Hunt WC, Archer VE, Saccomanno G. Radon Progeny Exposure and Lung Cancer Risk Among Non-Smoking Uranium Miners. Health Phys 2000; 79(4): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
258 76. Yuan Y, Morishima H, Shen T, Koga T, Wei L, Sugahara T. Measurements of Rn-222, Rn-220 and Their Decay Products in the Environmental Air of the High Background Radiation Areas in Yangjiang, China. J Radiat Res (Tokyo) 2000; 41 Suppl: Kleinerman R, Wang Z, Lubin J, Zhang S, Metayer C, Brenner A. Lung Cancer and Indoor Air Pollution in Rural China. Ann Epidemiol 2000; 10(7): Ayotte P, Levesque B, Gauvin D, McGregor RG, Martel R, Gingras S, Walker WB, Letourneau EG. Indoor Exposure to 222Rn: a Public Health Perspective. Health Phys 1998; 75(3): Cooke TF. Indoor Air Pollutants. A Literature Review. Rev Environ Health 1991; 9(3): Piao CQ, Hei TK. The Biological Effectiveness of Radon Daughter Alpha Particles. I. Radon, Cigarette Smoke and Oncogenic Transformation. Carcinogenesis 1993; 14(3): Hei TK, Piao CQ, Willey JC, Thomas S, Hall EJ. Malignant Transformation of Human Bronchial Epithelial Cells by Radon-Simulated Alpha-Particles. Carcinogenesis 1994; 15(3): Tirmarche M. Radon and Cancer Risk: Epidemiological Studies After Occupational or Domestic Exposure [Fr]. Rev Epidemiol Sante Publique 1995; 43(5): Hampson SE, Andrews JA, Lee ME, Lichtenstein E, Barckley M. Radon and Cigarette Smoking: Perceptions of This Synergistic Health Risk. Health Psychol 2000; 19(3): Andersson M, Wallin H, Jonsson M, Nielsen LL, Visfeldt J, Vyberg M, Bennett WP, De Beneditti VM, Travis LB, Storm HH. Lung Carcinoma and Malignant Mesothelioma in Patients Exposed to Thorotrast: Incidence, Histology and P53 Status. Int J Cancer 1995; 63(3): Gilliland FD, Hunt WC, Pardilla M, Key CR. Uranium Mining and Lung Cancer Among Navajo Men in New Mexico and Arizona, 1969 to J Occup Environ Med 2000; 42(3): Tomasek L, Placek V. Radon Exposure and Lung Cancer Risk: Czech Cohort Study. Radiat Res 1999; 152(6 Suppl): S59 S Wesch H, Wiethege T, Spiethoff A, Wegener K, Muller KM, Mehlhorn J. German Uranium Miner Study-Historical Background and Available Histopathological Material. Radiat Res 1999; 152(6 Suppl): S48 S Dupree EA, Watkins JP, Ingle JN, Wallace PW, West CM, Tankersley WG. Uranium Dust Exposure and Lung Cancer Risk in Four Uranium Processing Operations. Epidemiology 1995; 6(4): Ritz B. Radiation Exposure and Cancer Mortality in Uranium Processing Workers. Epidemiology 1999; 10(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 247
259 90. Lee-Feldstein A. Cumulative Exposure to Arsenic and Its Relationship to Respiratory Cancer Among Copper Smelter Employees. J Occup Med 1986; 28(4): Steenland K, Ward E. Lung Cancer Incidence Among Patients With Beryllium Disease: a Cohort Mortality Study. J Natl Cancer Inst 1991; 83(19): Ward E, Okun A, Ruder A, Fingerhut M, Steenland K. A Mortality Study of Workers at Seven Beryllium Processing Plants. Am J Ind Med 1992; 22(6): Sorahan T, Burges DC, Hamilton L, Harrington JM. Lung Cancer Mortality in Nickel/Chromium Platers, Occup Environ Med 1998; 55(4): Christiani DC. Smoking and the Molecular Epidemiology of Lung Cancer. Clin Chest Med 2000; 21(1): 87 93, viii. 95. Chromium, nickel and welding Lyon, France, IARC. 96. Pedersen E, Hogetveit AC, Andersen A. Cancer of Respiratory Organs Among Workers at a Nickel Refinery in Norway. Int J Cancer 1973; 12(1): Kreyberg L. Lung Cancer in Workers in a Nickel Refinery. Br J Ind Med 1978; 35(2): Moulin JJ. A Meta-Analysis of Epidemiologic Studies of Lung Cancer in Welders. Scand J Work Environ Health 1997; 23(2): Moulin JJ, Clavel T, Roy D, Dananche B, Marquis N, Fevotte J, Fontana JM. Risk of Lung Cancer in Workers Producing Stainless Steel and Metallic Alloys. Int Arch Occup Environ Health 2000; 73(3): Oller AR, Costa M, Oberdorster G. Carcinogenicity Assessment of Selected Nickel Compounds. Toxicol Appl Pharmacol 1997; 143(1): Barceloux DG. Nickel. J Clin Toxicol 1999; 37(2): Enterline PE, Marsh GM, Henderson V, Callahan C. Mortality Update of a Cohort of U.S. Man-Made Mineral Fibre Workers. Ann Occup Hyg 1987; 31(4B): Simonato L, Fletcher AC, Cherrie J, Andersen A, Bertazzi PA, Charney N, Claude J, Dodgson J, Esteve J, Frentzel-Beyme R. Updating Lung Cancer Mortality Among a Cohort of Man-Made Mineral Fibre Production Workers in Seven European Countries. Cancer Lett 1986; 30(2): Rodelsperger K, Jockel K-H, Pohlabein H, et al. Asbestos and Man-Made Vitreous Fibres As Risk Factors for Diffuse Malignant Mesothelioma: Results From a German Hospital-Based Case-Control Study. Am J Ind Med 2001; 39: Garshick E, Schenker MB, Munoz A, Segal M, Smith TJ, Woskie SR, Hammond SK, Speizer FE. A Case-Control Study of Lung Cancer and Diesel Exhaust Exposure in Railroad Workers. Am Rev Respir Dis 1987; 135(6): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
260 106. Boffetta P, Stellman SD, Garfinkel L. Diesel Exhaust Exposure and Mortality Among Males in the American Cancer Society Prospective Study. Am J Ind Med 1988; 14(4): Boffetta P, Harris RE, Wynder EL. Diesel Exhaust Exposure and Lung Cancer Risk. Exp Pathol 1989; 37(1 4): Pepelko WE, Chen C. Quantitative Assessment of Cancer Risk From Exposure to Diesel Engine Emissions. Regul Toxicol Pharmacol 1993; 17(1): Emmelin A, Nystrom L, Wall S. Diesel Exhaust Exposure and Smoking: a Case- Referent Study of Lung Cancer Among Swedish Dock Workers. Epidemiology 1993; 4(3): Muscat JE. Carcinogenic Effects of Diesel Emissions and Lung Cancer: the Epidemiologic Evidence Is Not Causal. J Clin Epidemiol 1996; 49(8): Farmer PB. Diesel Fuel and Exhaust Emissions: Is There a Human Carcinogenic Risk? Lancet 1997; 350(9085): Cox LAJ. Does Diesel Exhaust Cause Human Lung Cancer? Risk Anal 1997; 17(6): Silverman DT. Is Diesel Exhaust a Human Lung Carcinogen? Epidemiology 1998; 9(1): Bhatia R, Lopipero P, Smith AH. Diesel Exhaust Exposure and Lung Cancer. Epidemiology 1998; 9(1): Steenland K, Deddens J, Stayner L. Diesel Exhaust and Lung Cancer in the Trucking Industry: Exposure-Response Analyses and Risk Assessment. Am J Ind Med 1998; 34(3): Bates DV. Diesel Exhaust and Lung Cancer. Epidemiology 1998; 9(4): Lipsett M, Campleman S. Occupational Exposure to Diesel Exhaust and Lung Cancer: a Meta-Analysis. Am J Public Health 1999; 89(7): Valberg PA, Watson AY. Comparative Mutagenic Dose of Ambient Diesel Engine Exhaust. Inhal Toxicol 1999; 11(3): Larkin EK, Smith TJ, Stayner L, Rosner B, Speizer FE, Garshick E. Diesel Exhaust Exposure and Lung Cancer: Adjustment for the Effect of Smoking in a Retrospective Cohort Study. Am J Ind Med 2000; 38(4): Gao YT, Blot WJ, Zheng W, Ershow AG, Hsu CW, Levin LI, Zhang R, Fraumeni JFJ. Lung Cancer Among Chinese Women. Int J Cancer 1987; 40(5): Wang TJ, Zhou BS, Shi JP. Lung Cancer in Nonsmoking Chinese Women: a Case-Control Study. Lung Cancer 1996; 14 Suppl 1: S93 S Zhong L, Goldberg MS, Gao YT, Jin F. Lung Cancer and Indoor Air Pollution Arising From Chinese-Style Cooking Among Nonsmoking Women Living in Shanghai, China. Epidemiology 1999; 10(5): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 249
261 123. Zhong L, Goldberg MS, Parent ME, Hanley JA. Risk of Developing Lung Cancer in Relation to Exposure to Fumes From Chinese-Style Cooking. Scand J Work Environ Health 1999; 25(4): Ko YC, Cheng LS, Lee CH, Huang JJ, Huang MS, Kao EL, Wang HZ, Lin HJ. Chinese Food Cooking and Lung Cancer in Women Nonsmokers. Am J Epidemiol 2000; 151(2): Chen H, Yang M, Ye S. A Study on Genotoxicity of Cooking Fumes From Rapeseed Oil. Biomed Environ Sci 1992; 5(3): Qu YH, Xu GX, Zhou JZ, Chen TD, Zhu LF, Shields PG, Wang HW, Gao YT. Genotoxicity of Heated Cooking Oil Vapors. Mutat Res 1992; 298(2): Li S, Pan D, Wang G. Analysis of Polycyclic Aromatic Hydrocarbons in Cooking Oil Fumes. Arch Environ Health 1994; 49(2): Pellizzari ED, Michael LC, Thomas KW, Shields PG, Harris C. Identification of 1,3-Butadiene, Benzene, and Other Volatile Organics From Wok Oil Emissions. J Expo Anal Environ Epidemiol 1995; 5(1): Chiang TA, Wu PF, Wang LF, Lee H, Lee CH, Ko YC. Mutagenicity and Polycyclic Aromatic Hydrocarbon Content of Fumes From Heated Cooking Oils Produced in Taiwan. Mutat Res 1997; 381(2): Wu PF, Chiang TA, Wang LF, Chang CS, Ko YC. Nitro-Polycyclic Aromatic Hydrocarbon Contents of Fumes From Heated Cooking Oils and Prevention of Mutagenicity by Catechin. Mutat Res 1998; 403(1 2): Wu PF, Chiang TA, Ko YC, Lee H. Genotoxicity of Fumes From Heated Cooking Oils Produced in Taiwan. Environ Res 1999; 80(2 Pt 1): Chiang TA, Wu PF, Ko YC. Identification of Carcinogens in Cooking Oil Fumes. Environ Res 1999; 81(1): Brownson RC, Alavanja MC. Previous Lung Disease and Lung Cancer Risk Among Women (United States). Cancer Causes Control 2000; 11(9): Burns PB, Swanson GM. The Occupational Cancer Incidence Surveillance Study (OCISS): Risk of Lung Cancer by Usual Occupation and Industry in the Detroit Metropolitan Area. Am J Ind Med 1991; 19(5): Madri JA, Carter D. Scar Cancers of the Lung: Origin and Significance. Hum Pathol 1984; 15(7): Kung IT, Lui IO, Loke SL, Khin MA, Mok CK, Lam WK, So SY. Pulmonary Scar Cancer. A Pathologic Reappraisal. Am J Surg Pathol 1985; 9(6): Barsky SH, Huang SJ, Bhuta S. The Extracellular Matrix of Pulmonary Scar Carcinomas Is Suggestive of a Desmoplastic Origin. Am J Pathol 1986; 124(3): Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
262 138. Kolin A, Koutoulakis T. Role of Arterial Occlusion in Pulmonary Scar Cancers. Hum Pathol 1988; 19(10): Turner-Warwick M, Lebowitz M, Burrows B, Johnson A. Cryptogenic Fibrosing Alveolitis and Lung Cancer. Thorax 1980; 35(7): Nagai A, Chiyotani A, Nakadate T, Konno K. Lung Cancer in Patients With Idiopathic Pulmonary Fibrosis. Tohoku J Exp Med 1992; 167(3): Wells C, Mannino DM. Pulmonary Fibrosis and Lung Cancer in the United States: Analysis of the Multiple Cause of Death Mortality Data, 1979 Through South Med J 1996; 89(5): Oksa P, Klockars M, Karjalainen A, Huuskonen MS, Vattulainen K, Pukkala E, Nordman H. Progression of Asbestosis Predicts Lung Cancer. Chest 1998; 113(6): Mizushima Y, Kobayashi M. Clinical Characteristics of Synchronous Multiple Lung Cancer Associated With Idiopathic Pulmonary Fibrosis. A Review of Japanese Cases. Chest 1995; 108(5): Iwai K, Mori T, Yamada N, Yamaguchi M, Hosoda Y. Idiopathic Pulmonary Fibrosis. Epidemiologic Approaches to Occupational Exposure. Am J Respir Crit Care Med 1994; 150(3): Mayne ST, Buenconsejo J, Janerich DT. Previous Lung Disease and Risk of Lung Cancer Among Men and Women Nonsmokers. Am J Epidemiol 1999; 149(1): Wu AH, Henderson BE, Pike MC, Yu MC. Smoking and Other Risk Factors for Lung Cancer in Women. J Natl Cancer Inst 1985; 74(4): Kerr KM. Adenomatous hyperplasia and the origin of peripheral adenocarcinoma of lung. Corrin B (ed) Pathology of Lung Tumours. New York: Churchill Livingstone, 1997: Chromium, nickel and welding Lyon, France, IARC Monographs on the evaluation of carcinogenic risks to humans vol 68. Silica, some silicates, coal dust and para-aramid fibrils Lyon, France, IARC. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 251
263 APPENDIX 6 NATIONAL TOBACCO STRATEGY ACTION PLAN An action plan under the National Drug Strategic Framework, the National Tobacco Strategy 1999 to (NTS) was endorsed by the Ministerial Council on Drug Strategy (MCDS) in June (see under Campaign Sites) The NTS comprises a range of tobacco control initiatives ultimately designed to improve the health of all Australians by eliminating or reducing their exposure to tobacco in all its forms. It emphasises a national collaborative approach to tobacco control issues, nominating a range of government, non government and community partnerships and links, under six main key strategy areas: strengthening community action promoting cessation of tobacco use reducing availability and supply of tobacco reducing tobacco promotion regulating tobacco reducing exposure to environmental tobacco smoke. While the overriding intention of the Strategy is to improve the health of all Australians, the following specific objectives support this goal: preventing uptake of tobacco use in non-smokers, especially children and young people reducing the number of users of tobacco products reducing the exposure of users to the harmful health consequences of tobacco products Reducing exposure to tobacco smoke. Initiatives implemented in the first 18 months of the NTS fall within the following areas: national tobacco campaigns indigenous tobacco control best practice in smoking cessation (see below) review of the national quitline sales to minors health warnings tobacco advertising bans nicotine regulation disclosure of cigarette ingredients environmental tobacco smoke. 252 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
264 Several initiatives in the strategy are particularly relevant to Medical Practitioners. One such project is a review of best practice in smoking cessation. The National Heart Foundation was commissioned in September 2000 to identify best practice in brief intervention for smoking cessation in a range of health care settings by professionals such as General Practitioners. This stage was completed in early The second stage of the project will build on the first to develop and promote the uptake of guidelines in smoking cessation. See also Smoking Cessation in chapter 2. Importantly, there is also considerable help and services available to smokers wishing to quit from state Cancer Council and QUIT. For health professionals, other Australian smoking control resources include key policy documents that provide a framework for tobacco control in Australia. They include: Miller M, Wood L Smoking cessation interventions: Review of evidence and implications for best practice in health care settings. National Tobacco Strategy 1999 to Occasional Paper. Canberra, Commonwealth of Australia. Commonwealth Department of Health and Ageing (CDHA) Priorities for Action in Cancer Control Commonwealth of Australia, Canberra, The Cancer Council Australia (TCCA) National Cancer Prevention Policy The Cancer Council Australia, Sydney. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 253
265 APPENDIX 7 LEVELS OF EVIDENCE FOR DIAGNOSTIC TESTS 1 I II Evidence obtained from at least one validating cohort study with good reference standards (+/- systematic review) or near 100% sensitivity and specificity of the diagnostic procedure. Evidence obtained from at least one exploratory cohort study with good reference standards (+/- systematic review) III Evidence obtained from non-consecutive study or without consistently applied reference standards (+/- systematic review) IV Evidence obtained from case-control study or with poor or non-independent reference standard Reference 1. Adapted from: Oxford Centre for Evidence-based medicine. Levels of evidence and grades of recommendation ( 254 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
266 APPENDIX 8 A MODEL FOR PATHOLOGY REPORTING OF LUNG CANCER NEPEAN HOSPITAL LUNG CANCER REPORTING PROTOCOL 1. Specimen type Pneumonectomy / lobectomy / segmentectomy / wedge resection 2. Topography R lung (RUL / RML / RLL) L lung (LUL / LLL) 3. Tumour location 4. Tumour size maximum diameter 5. Tumour type 6. Histological grade well / moderately / poorly differentiated undifferentiated 7. Vessel invasion absent / present if present state involvement of artery / vein / lymphatic if possible 8. Perineural invasion absent / present 9. Pleural involvement Pleura free of tumour Tumour abuts the visceral pleura but has not breached it Tumour has invaded through the visceral pleura Tumour has invaded through the parietal pleura 10. Bronchial resection margin free of tumour minimum distance between tumour and bronchial resection margin involved by in situ carcinoma percentage of circumference involved involved by invasive carcinoma mucosal or extramucosal (beyond bronchial cartilage) Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 255
267 11. Vascular resection margin free of tumour tumour thrombus present vessel wall involved by tumour 12. Other resection margins hilar soft tissue / others 13. Chest wall involvement of intercostal muscle / soft tissues / ribs tumour absent / present at inked resection margin 14. In situ carcinoma absent / present 15. Non-neoplastic lung 16. Lymph nodes site or level number of positive or tumour free / number received eg. 3/6 or 0/6 focal or extensive or complete involvement by tumour extracapsular spread (measure distance) Jenny Ma Wyatt Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
268 EXAMPLE OF REPORT USING NEPEAN HOSPITAL PROTOCOL 1. Specimen type: Lobectomy. 2. Topography: Right lung Right lower lobe. 3. Tumour location: Peripheral (subpleural). 4. Tumour size: 6cm in maximum diameter. 5. Tumour type: Squamous cell carcinoma. 6. Histological grade: Moderately differentiated. 7. Vessel invasion: Extensive invasion of pulmonary artery branches. 8. Perineural invasion: Absent. 9. Bronchial resection margin: Squamous cell carcinoma in situ involves approximately 30% of the circumference. 10. Vascular resection margin: Free of tumour. 11. Pleural involvement: The tumour has invaded through the parietal pleura. 12. Other resection margins: Free of tumour. 13. Chest wall: The tumour has invaded into intercostal muscle and soft tissues but not the ribs. The inked resection margin is free of tumour. 14. In situ carcinoma: Present (See 9). 15. Non-neoplastic lung: Areas of atelectasis but no evidence of tumour. 16. Lymph nodes: Peribronchial lymph nodes all show anthracosis and sinus histiocytosis but no evidence of tumour (0/7). Level 3 nodes one of three nodes shows focal involvement by tumour (1/3). This shows extracapsular spread of distance of 0.5mm. DIAGNOSIS: RIGHT LOWER LOBE OF LUNG (LOBECTOMY): SQUAMOUS CELL CARCINOMA SQUAMOUS CELL CARCINOMA IN SITU PRESENT AT BRONCHIAL RESECTION MARGIN CHEST WALL RESECTION MARGIN FREE OF TUMOUR TUMOUR PRESENT IN 1 OF 3 LEVEL THREE LYMPH NODES PERIBRONCHIAL LYMPH NODES FREE OF TUMOUR (0/7) Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 257
269 APPENDIX 9 MEMBERSHIP OF THE AUSTRALIAN CANCER NETWORK MANAGEMENT OF LUNG CANCER GUIDELINE WORKING PARTY A/Professor David Ball (Chairman) Dr Kate Brameld Dr Mary Brooksbank Dr Peter Cole Dr Sidney Davis Dr Kwun Fong Ms Ann Gillett-Dunn Professor Douglas Henderson Dr Mohammed Amjad Hussain A/Professor Louis Irving Professor David Kissane Dr W F Eddie Lau Professor Brian McCaughan Dr Michael Millward Dr Paul Mitchell Ms Ingrid Plueckhahn Emeritus Professor Tom Reeve Dr Karen Pedersen Ms Christine Vuletich Corresponding members: Dr Geoffrey Beadle Dr Michael Byrne Radiation Oncologist Epidemiologist Palliative Care Physician Thoracic Surgeon Radiation Oncologist Respiratory Physician Consumer Pathologist General Practitioner Respiratory Physician Psychiatrist Radiologist Thoracic Surgeon Medical Oncologist Medical Oncologist Oncology Nurse Convenor / ACN Senior Medical Advisor Review Coordinator / NCCI Senior Project Officer Manuscript Coordinator / ACN Executive Assistant Medical Oncologist Medical Oncologist 258 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
270 The Australian Cancer Network would also like to gratefully acknowledge: Lorraine Ivancic, Rosalie Viney and Philip Haywood of Centre Health Economics Research & Evaluation (CHERE), University of Technology, Sydney for their contribution of Chapter 10 - Cost effectiveness, Dr Renee Manser, Clinical Epidemiology and Health Services Evaluation Unit, The Royal Melbourne Hospital, for her contribution on Screening for lung cancer, Dr Jan Copeland, National Drug and Alcohol Centre UNSW, for review of segment on Cannabis and lung cancer, Dr Jenny Ma Wyatt for permission to incorporate Appendix 8 - A model for pathology reporting of lung cancer and to Ms Anna Takacs for assistance with editing. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 259
271 APPENDIX 10 SUBMISSIONS RECEIVED FOLLOWING PUBLIC CONSULTATION Submission No. 1 Dr Desmond Yip The Canberra Hospital Yamba Drive Garran ACT 2606 Tel: Fax: [email protected] 2 The Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG) Dr Ann Robertson Special Projects RANZCOG Albert Street East Melbourne VIC 3002 Tel: Fax: [email protected] 3 The Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG) Dr James Brodribb RANZCOG College House Albert Street East Melbourne VIC 3002 Tel: Fax: Dr Andrew Strickland Medical Oncologist 1332 Heatherton Road Noble Park VIC 3174 Tel: Fax: [email protected] 260 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
272 Submission No. 5 The Royal Australasian College of Surgeons (RACS) Dr Wendy Babidge Research and Administrative Manager ASERNIP-S PO Box 688 North Adelaide SA 5006 Tel: Fax: [email protected] 6 Dr Timothy Price Consultant Medical Oncologist Queen Elizabeth and Western Hospitals Woodville Road Woodville SA 5011 Fax: [email protected] 7 The Royal Australian and New Zealand College of Radiologists (RANZCR) Faculty of Radiation Oncology Dr Liz Kenny Dean Faculty of Radiation Oncology RANZCR Level 9 51 Druitt Street Sydney NSW 2000 Tel: Fax: [email protected] 8 AstraZeneca Pty Ltd Dr Glen Pater Director Medical and Regulatory Affairs AstraZeneca Pty Ltd Alma Road North Ryde NSW 2113 Tel: Fax: [email protected] Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 261
273 Submission No. 9 Dr Michael Byrne Head Department of Medical Oncology Sir Charles Gairdner Hospital Verdun Street Nedlands WA 6009 Tel: (08) Fax: (08) [email protected] 10 Dr Kwun Fong Department of Thoracic Medicine The Prince Charles Hospital Rode Road Chermside QLD 4032 Tel: Fax: [email protected] 11 The Thoracic Society of Australia and New Zealand (TSANZ) Dr Rayleen Bowman TSANZ 145 Macquarie Street Sydney NSW 2000 Tel: Fax: [email protected] 12 The Thoracic Society of Australia and New Zealand (TSANZ) Dr Jonathan Burdon President TSANZ 145 Macquarie Street Sydney NSW 2000 Tel: Fax: [email protected] 13 Dr Matthew Peters Senior Staff Specialist Department of Thoracic Medicine Concord Repatriation General Hospital Hospital Road Concord NSW 2137 Tel: (07) [email protected] 262 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
274 Submission No. 14 Dr Kate Brameld (Editorial Response) Research Associate Centre for Health Services Research School of Population Health The University of Western Australia Crawley WA 6009 Tel: Fax: The Medical Oncology Group of Australia (MOGA) Dr Nick Pavlakis Department of Medical Oncology Royal North Shore Hospital Pacific Highway St Leonards NSW 2065 Tel: Fax: National Cancer Control Initiative (NCCI) Professor Mark Elwood Director National Cancer Control Initiative 1 Rathdowne Street Carlton VIC 3053 Tel: Fax: [email protected] 17 Ms Ellen Kerrins Manager Cancer Prevention Unit The Cancer Council South Australia PO Box 929 Unley SA 5061 Tel: [email protected] Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 263
275 Submission No. 18 The Royal Australian College of General Practitioners (RACGP) Dr John Litt Senior Lecturer Department of General Practice Noarlunga Hospital Noarlunga Centre SA 5168 Tel: Fax: Professor RM Lowenthal Director of Medical Oncology Royal Hobart Hospital GPO Box 1061 L Hobart TAS 7001 Tel: Fax: Australian and New Zealand Society of Palliative Medicine (ANZSPM) Professor Michael Ashby McCulloch House Monash Medical Centre Clayotn VIC 3168 Tel: Fax: [email protected] 21 Dr Fiona Cameron Radiation Oncologist Sir Charles Gairdner Hospital Verdun Street Nedlands WA Ms Denise Sullivan Manager Policy and Tobacco Program Cancer Foundation of WA 46 Ventor Avenue West Perth WA 6005 Tel: Fax: [email protected] 264 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
276 Submission No. 23 South Western Sydney Area Health Service (SWSAHS) Professor Jeanette Ward Area Director South Western Sydney Area Health Service Locked Bag 7008 Liverpool NSW 1871 Tel: Fax: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 265
277 APPENDIX 11 GUIDELINE DEVELOPMENT PROCESS Clinical practice guidelines for the prevention, diagnosis and management of lung cancer have been prepared by the Australian Cancer Network (ACN) following the outline of National Health and Medical Research Council s (NHMRC) A guide to the development, implementation and evaluation of clinical practice guidelines (NHMRC Canberra 1999). The ACN Lung Cancer Working Party (see Appendix 9) under the Chairmanship of Associate Professor David Ball has co-ordinated the development of the guidelines. Lung cancer treatment is a challenge to multiple disciplines. Accordingly the Working Party was representative of Royal Colleges and specialty groups. It comprised representatives from all aspects of clinical practice, including epidemiology, thoracic medicine, thoracic surgery, pathology, medical and radiation oncology, psychosocial medicine, radiology, general practice, nursing, palliative care, medical economics and consumer advocacy. PURPOSE, SCOPE AND DEVELOPMENT PROCESS OF GUIDELINES The development of the guidelines was prompted by a number of factors as outlined in the Foreword, where the burden of lung cancer is highlighted and where it is recorded that a somewhat nihilistic attitude towards lung cancer had led to paucity of treatment, with further studies revealing a lack of accord or agreed approach to the management of patients with cancer of the lung. The prime reason to produce guidelines was to assist in education and improve practice and the quality of care provided by practitioners treating those with lung cancer in Australia. The general practitioner is usually the doctor of first contact, although each individual general practitioner may only see one, or at most, two lung cancer patients a year. It was an important principle to the Working Party that guidelines can improve consistency of care and of patient outcomes 1,2. References 1. Haines, A., Donald, A. Making better use of research findings. BMJ 1998: 317: (7150) Thomas, L.H., McCall, E., Cullem, N., Rousseau, N.,Souter, J., Sken, N. Effect of clinical guidelines in nursing midwifery and the therapies: a systematic review of evaluations. Qual Health Care 1998: 7: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
278 A specially formatted document will be prepared for general practitioners when the current document is accredited. The general practitioner document will provide sound guidance on referral to appropriate specialists. A consumer document will be developed at the same time. The Working Party was established with the approval and support of The Thoracic Society of Australia and New Zealand, The Australian Lung Foundation and the Royal Colleges. It first met in April 2000 in Melbourne. The aim of the Working Party was to develop guidelines to: Assist decision-making in the management of lung cancer Provide better understanding through education to all involved in the care of people with lung cancer Assess and assure the quality of care Improve clinical care Bring issues of cost-effectiveness into the public arena. Clinical practice guidelines provide a framework within which to apply clinical judgement and consider individual patient needs, while providing a milieu for interactive discussion for the patient. In providing such a background, the guidelines are not rigid procedural paths; rather their objective is to ensure that both clinicians and patients are clearly informed about the risks and benefits of the recommended interventions. It is acknowledged that some variations in clinical practice may reflect reasonable differences in clinical judgement, clinical situations and patient preferences and needs. The guidelines are based on key principles which underpin the NHMRC s recommendations for guideline development. These are: a focus on the improvement of patient outcomes a basis in the best available scientific evidence inclusion of statements concerning the strength of the recommendations and the adoption of a multidisciplinary approach that involves all stakeholders, including consumers. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 267
279 PROCESS EMPLOYED The Working Party approached the development of guidelines by setting itself five key tasks. Task 1. Identification of the known clinical problems and areas of uncertainty in each of the disciplines involved in lung cancer treatment. Task 2. Collection and review of scientific evidence, including meta-analyses, to identify the best and most appropriate practice for the various interventions in lung cancer treatment. Task 3. Collaboration of appropriate subgroups, to review and present special issues for the consideration of the full working group. Task 4. Development of a glossary of technical terms in relation to lung cancer, for incorporation in the practice guidelines. Task 5. A review and revision process following public consultation as required by NHMRC. The activity of the Working Party was conducted across Australia, with face-to-face meetings used primarily to identify the scope of the guidelines and to review out-ofsession activity. The final editing before submission to NHMRC was conducted by the Chair and an Executive Group from the Working Party. TASK 1 It was established that the guidelines should focus on recommendations that would improve the outcomes of patients with lung cancer and they would have a strong clinical emphasis. The Working Party considered it vitally important to distil the best elements of clinical management. To achieve this the Working Party was to consult widely with clinicians and to involve consumers to ensure that the resultant guidelines gained broad acceptance. TASK 2 Evidence was obtained through various avenues, including PubMed, Medline, CancerLit, Cochrane reviews and personal databases. Identified evidence was then exhaustively evaluated by the Working Party. Analysis of the reviewed literature elicited a number of principles that were incorporated in the guidelines. Each of the papers offered by members of the Working Party to support arguments was evaluated before being incorporated as a reference or rejected if it did not meet the specific criteria applied to the clinical area. 268 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
280 Since decisions may have to be made in the presence of low level published evidence, a number of recommendations are based on level IV evidence. For those recommendations for which level I IV evidence was lacking, conclusions were drawn from the considered opinion of clinical experts. The processes used in developing these guidelines were designed to ensure that, as far as possible, the recommendations reflect a consensus of those concerned with the treatment of lung cancer in Australia. The Working Party decided that it was important to give a clear indication in the guidelines as to the strength of the evidence for guidelines and key statements, and to provide references where appropriate. Relevant data that were not appropriate for developing guidelines were listed as key points. DESIGNATION OF LEVELS OF EVIDENCE I II III 1 III 2 III 3 IV Evidence obtained from a systematic review of all relevant randomised controlled trials. Evidence obtained from at least one properly designed randomised controlled trial. Evidence obtained from well-designed pseudo-randomised controlled trials (alternate allocation or some other method). Evidence obtained from comparative studies with concurrent controls and allocation not randomised (cohort studies), case-control studies, or interrupted time series with a control group. Evidence obtained from comparative studies with historical control, two or more single-arm studies, or interrupted time series without a parallel control group. Evidence obtained from case series, either post-test or pre-test and post-test. (In effect we listed all level III as III regardless of category.) These levels of evidence ratings have been adapted from US Preventive Services Task Force (1989), Guide to clinical preventive services: an assessment of the effectiveness of 169 interventions (ed M Fisher), Williams and Williams, Baltimore, Appendix A, p388. A guide to the development, implementation, and evaluation of clinical practice guidelines, NHMRC Canberra Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 269
281 TASK 3 During the initial development of these guidelines, the Working Party established clinical assessment subgroups. The leaders of these subgroups identified known clinical problems or issues in their respective fields and consulted more widely, before submitting manuscripts for the whole Working Party s discussions. This process allowed advancement of the clinical subgroup s input into the guidelines in the medical oncology, surgery and radiation oncology areas. Several presentations were made at Annual Meetings (2001, 2002) of The Thoracic Society of Australia and New Zealand, which led to further discussion and refinement of the manuscript. Problem areas were also discussed between Working Party members, their immediate colleagues and more widely in the impromptu clinical networks that strengthen clinical practice in Australia. The result is an agreed document in which the Working Party dealt with and resolved difficult issues. TASK 4 Members of the Working Party contributed to the compilation of a glossary of lung cancer terms, which forms an appendix to the clinical guidelines. It was based primarily on the Lung cancer guidelines for people with cancer, their families and friends, published by The Cancer Council Victoria (2000) and is used with their permission. TASK 5 The guidelines were sent to relevant experts, representatives of professional colleges and consumer representatives. Submissions were also received from others who responded to a public call for submissions by the ACN. Comments received were considered by a special committee chaired by Professor Robert Burton, and decisions to include or exclude comments were based on expert clinical judgement and whether the comments reasonably reflected best practice and the best available evidence. After revision the final drafts for each section were assembled, edited and approved by the Executive Review Group to forward to the NHMRC. Consumer representation was involved in all stages of guideline development. TARGET AUDIENCE The guidelines were developed to equip clinicians with recommendations for the optimal care of people with lung cancer. 270 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
282 COSTING ISSUES A review of the existing literature on cost-effectiveness of a variety of treatments was undertaken. IMPLEMENTATION AND DISSEMINATION The ACN is responsible for disseminating, implementing, evaluating and updating the guidelines. Evaluation and updating processes will be in accordance with NHMRC guidelines. The guidelines will also feature strongly in the accreditation and credentialing activity of the ACN. The implementation plan includes the following strategies: APPROVAL Guideline approval by NHMRC was given and the document will be circulated to relevant stakeholders as a critical first step to aid dissemination and implementation. DISSEMINATION The initial print run of 6,000 copies of the guidelines will be disseminated to relevant professional groups. Copies will also be made available to allied health organisations, state and territory health authorities, professional colleges and associations, public policy makers, health economists and professional journals. To assist electronic dissemination, the NHMRC and ACN have included the guidelines on their websites, enabling internet access. The availability of the guidelines will be advertised through the ACN newsletter, Wongi Yabber, which is published quarterly throughout the year, and distributed to professional colleges, ACN stakeholders and interest groups, including consumers and has a limited overseas circulation. Lastly, the guidelines have been promoted at a national seminar and a state seminar on lung cancer management, presentations at relevant professional meetings and conferences and submissions to professional journals. On 5 April 2003, the National Cancer Control Initiative held a meeting in Adelaide Improving the Management of Lung Cancer. The draft guidelines provided a substantial role in the discussion that took place. On 20 June 2003, The Cancer Council New South Wales held a meeting Implementing Multidisciplinary Care in Lung Cancer. Each attendee received a copy of the draft guidelines. The content featured significantly in presentations and small group activity. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 271
283 CONSULTATION / FEEDBACK Since acceptability of the guidelines by relevant stakeholders is a critical first step towards their implementation, consultation is an integral part of the implementation process. This is now an integral part of ACN s program on credentialing and accreditation. The guidelines were submitted to the NHMRC, following a public consultation process which was conducted by the ACN. EVALUATION AND UPDATING An essential part of the guideline development and implementation process is an evaluation of their effectiveness. An evaluation strategy will be drafted at the implementation stage and will include the collection of data to determine the impact of the guidelines on clinician behaviour and patient health outcomes. The guidelines reflect the best available knowledge at the time of their publication. However, as new evidence emerges from systematic reviews, they will require regular revision in order to maintain validity. The ACN proposes to investigate the most costeffective means of undertaking this. 272 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
284 APPENDIX 12 CONTACTS FOR HELP SERVICES Importantly, there are considerable help services available to smokers wishing to quit, including state Cancer Councils and QUIT. NATIONALLY QUITLINE Ph: CANCER HELPLINE The Cancer Helpline provides general information as well as information on local resources. This service can be accessed from anywhere in Australia for the cost of a local call, connecting to local cancer organisations: Ph: STATE AND TERRITORY CANCER ORGANISATIONS AND ASSOCIATED NUMBERS State and Territory Cancer Councils provide information and educational resources on all types of cancers. Some have lending libraries. Many cancer organisations have also developed their own publications about cancer and treatments. To find out about cancer support groups and other local services, State or Territory cancer organisations and the Cancer Helpline should be contacted. The Cancer Council ACT 159 Maribyrnong Avenue Kaleen ACT 2617 Ph: (02) Fax: (02) [email protected] Website: The Cancer Council New South Wales 153 Dowling St Woolloomooloo NSW 2011 Ph: (02) Fax: (02) [email protected] Website: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 273
285 The Cancer Council Northern Territory Casi House Unit Vanderlin Dr Casuarina NT 0810 Ph: (08) Fax: (08) [email protected] Website: The Cancer Council Tasmania 140 Bathurst St Hobart TAS 7000 Ph: (03) (03) Fax: (03) [email protected] Website: The Cancer Council Victoria 1 Rathdowne St Carlton South VlC 3053 Ph: (03) Fax: (03) [email protected] Website: The Cancer Council South Australia 202 Greenhill Rd Eastwood SA 5063 Ph: (08) Fax: (08) [email protected] Website: Cancer Foundation of Western Australia 46 Ventnor Ave West Perth WA 6005 Ph: (08) Fax: (08) [email protected] Website: Queensland Cancer Fund 553 Gregory Terrace Fortitude Valley QLD 4006 Ph: (07) Fax: (07) [email protected] Website: Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
286 LIST OF ABBREVIATIONS ATBC BSC CHART CT CXR DALY DIF ED ELCAP FDG-PET FNA G-CSF GM-CSF IARC LD LDH LYS M MRI N NCCI NHMRC NRT NSCLC OCA OR Alpha-tocopherol beta carotene Best supportive care Continuous hyperfractionated accelerated radiotherapy Computed tomography Chest x-ray Disability adjusted life year Diffuse interstitial fibrosis Extensive disease Early lung cancer action project Fluoro-deoxy glucose PET Fine needle aspiration Granulocyte colony stimulating factor Granulocyte-macrophage colony stimulating factor International Agency for Research on Cancer Limited disease Lactate dehydrogenase Life-year saved Metastases Magnetic resonance imaging Regional lymph nodes National Cancer Control Initiative National Health and Medical Research Council Nicotine replacement therapy Non-small cell lung cancer Vincristine, adriamycin and cyclophosphamide Odds ratio Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 275
287 PCI PE PET PI POHEM QALY QOL RR RRLCA RTC SCLC SMR SPN SVCO T TRT UICC VATS YLD YLL Prophylactic cranial irradiation Cisplatin with etoposide Positron emission tomography Cisplatin with irinotecan Population health model Quality adjusted life year Quality of life Relative risk Relative risk for lung cancer Randomised controlled trial Small cell lung cancer Standardised mortality rates Solitary pulmonary nodule Superior vena cava obstruction Primary tumour Thoracic radiotherapy International Union Against Cancer Video-assisted thoracoscopic techniques Years lost due to disability Years of life lost 276 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
288 GLOSSARY abdomen adenocarcinoma adjuvant chemotherapy advanced cancer alveoli anaesthetic asbestosis benign biopsy brachytherapy bronchi/ bronchioles bronchoscopy carcinoma cells The part of the body between the chest and hips, which contains the stomach, liver, intestines, bladder and kidneys. A type of lung cancer that starts in the bronchial glands that are found in the mucous membrane lining the airways. Chemotherapy that is used in a supplementary but not dominant therapy. Cancer that has metastasised and/or is unlikely to be cured. The tiny air sacs in the lungs; an adult has about 300 million. When air is breathed in, it goes via the airways to the alveoli, where oxygen is taken from them into the bloodstream. A drug that is taken to stop a person feeling pain during a medical procedure. A local anaesthetic numbs only a part of the body; a general anaesthetic causes a person to lose consciousness for a period of time. A slowly progressing lung disease caused by asbestos. It is not a cancer. Not cancerous. Benign cells are not able to spread like cancer cells. The removal of a small sample of tissue from the body, for examination under a microscope, to help diagnose a disease. A type of radiotherapy applicable to tumours which involves insertion of radioactive seeds directly into the tumour, which are retained (low dose brachytherapy). Another form is high dose brachytherapy, which involves treatment by temporary insertion of radioactive catheters into the tumour. Bronchi are the larger tubes that carry air in the lungs. Bronchioles are the tiny tubes that carry air to the outer parts of the lungs. An examination in which a tube is passed through the nose or the mouth into the lungs so that they can be examined for disease and some tissue sampled, if necessary. A cancer that arises in the tissue that lines the skin and internal organs of the body. The building blocks of the body. A human is made of millions of cells, which are adapted for different functions. Cells are able to reproduce themselves exactly, unless they are abnormal or damaged, as are cancer cells. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 277
289 chemotherapy chest cavity CT scanning diaphragm emphysema FNA FDG hamartoma helical (spiral) CT scanning large cell carcinoma lobectomy lobes lymphatic system lymph nodes The use of special (cytotoxic) drugs to treat cancer by killing cancer cells or slowing their growth. The area enclosed by the ribs, above the diaphragm. Computerised tomography is a technique for constructing pictures from cross sections of the body, by x-raying from many different angles the part of the body to be examined. A dome-like sheet of muscle that divides the chest cavity from the abdomen. It is used in breathing. A condition in which the alveoli of the lungs are enlarged and damaged, which reduces the lung s surface area, causing breathing difficulties. Fine needle aspiration is a procedure in which a fine needle is used to suck up a few cells from a tumour, for biopsy. Fluoro-deoxy glucose (see PET scanning) A benign local malformation resembling a neoplasm resulting from faulty development in an organ - frequently marked by one cell type. Patient moves continuously through a scanner without any stopping. The path of the beam through the patient is a continuous helix. A type of lung cancer that usually develops in the airways and is characterised by large rounded cells. A surgical operation to remove a lobe of a lung. The sections that make up the lungs the left lung has two lobes and the right lung, three. The lymphatic system is part of the immune system, which protects the body against invaders, like bacteria and parasites. The lymphatic system is a network of small lymph nodes connected by very thin lymph vessels, which branch into every part of the body. Also called lymph glands. Small, bean-shaped structures which form part of the lymphatic system. Lymph is the fluid that flows through this system and carries cells that help to fight disease and infection. The lymph nodes filter the lymph to remove bacteria and other harmful agents, such as cancer cells. 278 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
290 MRI malignant mediastinum mesothelioma metastases neo-adjuvant non-small cell lung carcinoma odds ratio oesophagus palliative treatment peritoneum PET scan pleura pleural cavity A special imaging technique used to image internal structures of the body. It uses the influence of a large magnet to polarize hydrogen atoms in the tissues and then monitors the summation of the spinning energies within living cells. Images are very clear and are particularly good for soft tissue, brain and spinal cord, joints and abdomen. These scans may be used for detecting some cancers or for following their progress. Cancerous. Malignant cells can spread (metastasise) and can eventually cause death if they cannot be treated. The area in the chest cavity between the lungs. It contains the heart and large blood vessels, the oesophagus, the trachea and many lymph nodes. A rare cancer of the membranes around the lungs. Exposure to asbestos can cause mesothelioma. Also known as secondaries. Tumours or masses of cells that develop when cancer cells break away from the original (primary) cancer and are carried by the lymphatic and blood systems to other parts of the body. Chemotherapy that is administered before the dominant therapy, for example, radiotherapy/surgery. One of the two main groups of lung cancers. This group includes squamous cell carcinoma, adenocarcinoma, large cell carcinoma, bronchiolo-alveolar cell carcinoma and mesothelioma. The ratio of a part to the remainder. It is used to express the chance that a particular outcome will occur. The tube that carries food from the throat to the stomach. Treatment aimed at providing relief for symptoms without attempting to cure the disease. The lining of the abdomen. Positron emission tomography. A technique that is used to build up clear and detailed cross-section pictures of the body. The person is injected with a glucose solution containing a small amount of radioactive material. The PET scanner can see the radioactive substance. Damaged or cancerous cells show up as areas where the glucose solution is being used. Membranes that line the chest wall and cover the lungs. A space, normally empty, that lies between the two layers of the pleura. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 279
291 pleural effusion pneumonectomy primary cancer prognosis radiotherapy randomised controlled trial (RCT) rapid smoking recurrent cancer relative risk relative survival resection An abnormal accumulation of fluid in the pleural space. It may be asymptomatic or associated with chest pain, fever and coughing. A surgical operation to remove a whole lung. The original cancer. At some stage, cells from the primary cancer may break away and be carried to other parts of the body, where secondary cancers may form. An assessment of the course and likely outcome of a person s disease. The use of radiation, usually x-rays or gamma rays, to kill cancer cells or injure them so they cannot grow and multiply. Radiotherapy treatment can also harm normal cells, but they are able to repair themselves. A study or experiment where subjects are allocated at random to receive or not receive the treatment, procedure or intervention. The results for each group are compared. Generally held to be the most scientifically rigorous method of testing an hypothesis. Asking subjects to smoke at an increased rate (from the Cochrane database). The version of rapid smoking evaluated in most trials consists of asking subjects to take a puff every 6 or 10 seconds. They smoke for three minutes or until they either consume three cigarettes or feel unable to continue. After a period of rest this procedure is repeated two or three times. A cancer that grows from cells of a primary cancer that evaded treatment. Recurrent cancer may appear up to 20 years after the primary cancer was treated, depending on the type of cancer. The risk (of a disease or death) among those exposed to the risk compared to those who are not exposed to the risk. Relative survival analysis aims to quantify how long someone with a specific disease might survive when compared to the general population. The general population are matched to the disease cases by age, sex and year of diagnosis. Relative survival is thus the ratio of the proportion of survivors in the disease group to the proportion of survivors in a similar group of people without the disease. A relative survival of 100% would indicate that persons with disease do not die any more rapidly as they age than people without the disease whereas a result of less than 100% indicates that the disease is resulting in premature death, even when other causes of death have been accounted for. Surgical removal of a portion of any part of the body. 280 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
292 small cell carcinoma sputum sputum cytology test squamous cell carcinoma staging stent thoracocentesis tissue tissue biopsy A type of lung cancer that is strongly associated with cigarette smoking. It spreads early and causes few initial symptoms. Liquid coughed up from the lungs. Also known as phlegm. Examination of sputum under a microscope to look for cancer cells. A cancer found most commonly on skin, but also in inner linings of the body, for example, a lung. It forms in the squamous (scaly) epithelium. Investigations to find out how far a cancer has progressed. This is important in planning the best treatment. A tube made of metal or plastic that is inserted into a vessel or passage to keep it open and prevent closure when it is under pressure. A medical procedure to draw fluid or air from the chest, using a hollow needle. A collection of cells. Examination of tissue, which has been removed from the body, under a microscope so that any abnormalities in the cells can be seen. trachea (windpipe) The pipe through which air passes to reach the lungs. The trachea starts in the neck, immediately below the voice box (larynx), and descends a few centimetres into the chest before branching to form the two bronchi, one of which goes into each lung. tumour wedge resection A new or abnormal growth of tissue on or in the body. A surgical operation to remove a part of a lung, but not a complete lobe. This glossary was adapted from Lung Cancer: a guide for people with cancer, their families and friends, Anti-Cancer Council of Victoria, May 2000 with kind permission from The Cancer Council Victoria. Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 281
293 INDEX Note: Locator numbers in italic indicate a table or a figure. Guidelines are highlighted in bold for the convenience of users A acupuncture 180 guideline 145 and dyspnoea 143, 144 and pain management 148 and smoking cessation 26 adenocarcinoma 5, 11, 55, 241 see also non-small cell lung cancer aetiology 5 defined 5, 6 and diagnosis 34, 53 and environmental carcinogens 232, 238 incidence 5 pathogenesis 5 and survival rates 13 treatment 33 34, 56, 58 adenoma 55 56, 241 adenomatous hyperplasia 241 adrenal metastases 55, 57 cost-effectiveness of assessment 199 staging M stage assessment TNM category 214 aetiology 6 11 see also asbestos-related lung cancer; smoking; occupational lung cancer adenocarcinoma 5 and dietary fat 28 environmental carcinogens 10, genetic susceptibility 9 large cell carcinoma 6 medical radiation 9 previous lung disease 9 small cell lung cancer 5, 235 smoking 6 8 tobacco 6 8 cannabis 8 squamous cell carcinoma 5 Agency for Health Care Policy and Research 21 alcohol 29 alpha-carotene 28 alpha-tocopherol 29 Alpha-Tocopherol Beta Carotene (ATBC) trial 29 alternative therapies guidelines 26, 181 and complementary therapies 179 cost 179, 180 defined 179 discussion of effectiveness patient expenditure 179 rate of use 179 reasons for use 180 safety 179, 180, consumption of substances 181 and diet 181, 182 and enemas 182 and megavitamins 181 training of therapists 182 and smoking cessation 24, 26 acupuncture 26 effectiveness 26 exercise 26 hypnotherapy 26 therapies used 180 see also acupuncture aromatherapy 181 laughter 181 meditation 179, 180, 181 prayer relaxation 75, 143, 145, 148, 179, 180, 181 toxicity of substances Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
294 anticonvulsants guideline 150 and pain management 150 antidepressants 73 guidelines 73, 150 and pain management 150 and smoking cessation 24, 25 antioxidants 27 provitamin A carotenoids 27 vitamin C 27 vitamin E 27 selenium 27 anxiety see psychosocial support anxiolytics 24, 144 asbestos 10, amphiboles 231 chrysotile 231 asbestos exposure 10, see also asbestos-related lung cancer and cancer prevention 29, 30, 55 and case finding 31 and screening 34 interaction with other carcinogens 233, 237, 239 interaction with tobacco smoke 10, 29, 34, 231, 233 neoplasia, asbestos-related 239 as risk factor 30, 31, 230 risk/exposure relationship worker exposure 230, 232 asbestosis 10, 230, 232, 233, 240 asbestos-related lung cancer 10, , 239 see also occupational lung cancer death rate 231 and latency times 231 lobar distribution 232 rates of cancer risk/exposure relationship aspirin 29 asthma 145, 241 and lung cancer 9, 11 ATBC trial see Alpha-Tocopherol Beta Carotene trial atelectasis 147, 163 and T classification 53, 216, 219, 220 Australian Institute of Health and Welfare 189 aversion therapy 23 B berylliosis 235 beta-carotene 27, 28, 29, 30 guideline 31 and increased cancer risk 29, 31 Beta-Carotene and Retinol Efficacy Trial see CARET biological agents 106 biomarkers 32, bisphosphonates guideline 169 and bone metastases 167, 169 and hypercalcaemia 169 bone biopsy 167 scan 56 guideline 56 as site of metastases 55, 57 bone marrow as site of metastases 57 bone metastases 53, , 214 guidelines 147, 168, 169 diagnosis of 167 and hypercalcaemia 153 long-bone lesions and pain management 83, 147, 150, 168 guidelines 147 and radiotherapy 140, 148, 149 pathological fractures 167 and orthopaedic referral 167, 168 rate of 56, 167 and solitary lesions 167 and spinal cord compression 165 and staging Stage IV 83 symptoms 167 T stage involvement of vertebra 216, 219, 220 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 283
295 treatment of guidelines 168, 169 bisphosphonates 167, 169 chemotherapy 167, 169 internal fixation/replacement 167, 168 prophylactic fixation radiotherapy , 169, 170 dose 168 duration 168 and fractionated radiotherapy 168 following internal fixation 168 brain metastases 55, 57, 59, 97, guidelines 56, 127, 172 cost-effectiveness of assessment 199 imaging of 56, 171 and non-small cell lung cancer 83 and small cell lung cancer 57, 59, 119 staging M stage 55 stage IV 83 TNM category 214 treatment guidelines 172 chemotherapy 119 prophylactic cranial irradiation 119, 127 radiotherapy 171, 172 stereotactic radiosurgery 171, 172 surgery 83, 171 whole brain radiation 171, 172 British Thoracic Society Lung Cancer Guidelines 138 bronchiolo-alveolar cell carcinoma 53, 225 see also non-small cell carcinoma bronchitis, chronic 9, 11, 241 bronchoscopy guidelines 52, 61 accuracy 52 and central lesions 52 and follow-up 60 guidelines 61 fluorescence virtual 36 bronchus, main 215, 216 and T2 stage 216, 219, 220 and T3 stage 216, 219, 220 bullous lung disease 51 burden of disease 189, 189 economic cost 189 years of life lost (YLL) 189, 189 years lost due to disability (YLD) 189, 189 C calcification 50 see also solitary pulmonary nodule Canadian Lung Oncology Group The Cancer Council of NSW 71 Cancer Councils 75, 253 listed Cancer Helpline 273 cannabis 8 carcinogens 10, , 238 see also asbestos related lung cancer; occupational lung cancer; smoking arsenic 235, 238 interaction with tobacco smoke 235 relative risk 235 beryllium 235, 238 standardised mortality ratio (SMR) 235 cadmium 236, 238, 240 relative risk 236 chromium 236, 238, 239, 240 relative risk 236 cooking oil vapour 238, 238 diesel exhaust fumes , 238 haematite 233, 236, 238 interactions with other carcinogens 236 lead 240 man-made mineral fibres 237, 238 nickel 236, 238, 239 relative risk 236 toxicity 236 polycyclic aromatic hydrocarbons , 238 worker exposure 237 radon interactions with other carcinogens 233, 234, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
296 scar cancer 239 silica 234, 238 interactions with other carcinogens 233, 236 tin mining 236, 238 interactions with other carcinogens 236 relative risk 235 uranium 235, 238 millisieverts 235 worker exposure 230, 232, 237 CARET (Beta-Carotene and Retinol Efficacy Trial) 29 carina T stage involvement 216, 219, 220 carotenoids 27, 28 alpha-carotene 28 lycopene 28 case finding 31 CFA see cryptogenic fibrosing alveolitis CHART (continuous hyperfractionated accelerated radiotherapy) chemoprevention guideline 31 for lung cancer 29 and alcohol 29 alpha-tocopherol 29 ATBC 29 beta-carotene 29 CARET 29 for multiple cancers 29 aspirin 29 beta-carotene 29 for premalignancy 30 beta-carotene 30 etretinate 30 retinoids 30 for second primary lung cancers 30 isotretinoin 30 N-acetyl-cysteine 30, 31 retinyl palmitate 30, 31 chemoradiotherapy 83, 93, 164 see also chemotherapy; radiotherapy chemotherapy guidelines 90, 91, 94, 95, 100, 101, 104, 105, 106, 122, 123, 125, 127, 147, 165, 166 adjuvant 93 94, 226 guidelines 94, 95 and radiotherapy 94 and surgery 93 survival rates 93, 94, 95, 226 combination guidelines 101, 105 combined with radiotherapy 90 94, 120, 121, 126 surgery 226 compared with radiotherapy 84, 90, 91 surgery 92, 93, and cost-effectiveness 201, 205 of alternative regimens neo-adjuvant 94, 96 guidelines 95 and non-small cell lung cancer 91 advanced guidelines 100 management of 83, 84 and survival rates 84, 98, 99, 99, 100 treatment of 97, and pain management 147 guideline 150 and radiotherapy 90 94, 120, 121, 226 guideline 90, 91, 126 survival rate 90 second-line 102, 105, 125, 225 guidelines 106, 125 and small cell lung cancer 125 and small cell lung cancer 119 guidelines 105, 122, 123, 125, 127, 165 and surgery 226 and SVC obstruction 164, 165 and systemic therapy 98 99, 99, 225, 226 and toxicity 92, 121, 122, 123, 163, 225 of combination chemotherapy 100, 101, 102, 104, 120 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 285
297 of new agents 102, 103 for treatment of bone metastases 167, 169 brain metastases 119 dyspnoea 125 Stage I 53, 90, 226 Stage II 90, 226 Stage IIIA 95 Stage IIIB 97, 201 Stage IV 59, 97, 225 chemotherapy, combination guidelines 104, 105 benefits of new v old agents 102 combinations with platinum drugs 102 new non-platinum drugs 104 agents used 104 new platinum drugs agents used 100, 101, 102, 103 comparative trials , 103 and G-CSF 103 and performance status 100, 102 and quality of life 101, 103 survival rates 102, 103 optimal combinations triplet combinations 103 guidelines 104, 105 chest radiography see x-rays chest wall 53, 88, 145, 147 M classification 221 T stage involvement 53, 54, 85, 216, 219, 220, chronic obstructive pulmonary disease (COPD) 143, 148 cigarettes see smoking Cochrane Collaboration 164 Library 21 Tobacco Addiction Review Group 21 reviews 22, 23 combination chemotherapy see chemotherapy, combination community-based care 75 see also palliative care complementary therapies 179, 182 computed tomography (CT) 32, 33 35, 165 guidelines 35, 54, 55, 61 accuracy 35 guidelines 55 N stage T stage 54 adenocarcinoma and biomarkers 36 and bone metastases 167 and brain metastases 171 cost-effectiveness of 197, 198, 199 for diagnosis solitary pulmonary nodules Early Lung Cancer Action Project study 34, 35 false negative 35 false positive 35 and follow-up 60, low-dose helical 33 35, 36 National Cancer Control Initiative 35 and non-small cell lung cancer 54, guidelines 54, 55 squamous cell carcinoma and spinal cord compression 165 and solitary pulmonary nodules and x-rays 33 constipation 148, 149, guideline 151 and hypercalcaemia 153 prevention of 149, 151 rates of 141 treatment 149, guideline 151 continuous hyperfractionated accelerated radiotherapy (CHART) cooking oil vapour 238, 238 risk of cancer 238 COPD see chronic obstructive pulmonary disease cost effectiveness burden of disease 189, 189 and initial assessment 190, CT 198, 199 mediastinoscopy 198, 199 positron emission tomography (PET) 190, Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
298 sputum cytology 198 thoracotomy 199 screening 190, , 198 and CT 197, 198 mass screening 196 targeted 197, 198 and x-rays , 198 smoking cessation and prevention 190, , counselling programs 192, and follow-up 190, hospital admission 192, 196 information programs nicotine replacement therapy 192, 193, , 196 pharmacological therapies 192, 196 treatment of non-small cell lung cancer 190, 199, 200 advanced non-small cell lung cancer 201, alternative chemotherapy regimens 201, , 205 combined therapies 205 radiotherapy 205 surgery 199, 200 treatment of small cell lung cancer 190, 205 cough 51, 141, 142, guidelines 146 frequency of 141, 163 and haemoptysis 146 and non-small cell lung cancer 146 and quality of life 74, 145 treatment pharmacological radiotherapy 163 other 145 counselling 22, 23, 192, 193, guideline 145 cranial irradiation, prophylactic see prophylactic cranial irradiation cryptogenic fibrosing alveolitis (CFA) 240 D DEF see diesel exhaust fumes depression 73, guidelines 73 see also psychosocial support and antidepressants 73 coping attitude 73 predictors of 73 prevention of and psychotherapy 73 screening for 73, 74 detection see screening diagnosis 49 53, 147 guidelines 51, 52, 53, 54, 55, 59, 60 and bone metastases 167 and brain metastases 171 bullous lung disease 51 endobronchial lung tumours 52 and granulomatous disease 53 histological 5, 49, 53 guideline 55, 165 for non-small cell lung cancer 55 and SVC obstruction and TNM classification 215 and mediastinal masses 52 methods of bronchoscopy CT 49 51, 54, 55, 56 endobronchial ultrasound 52 fine needle aspiration biopsy magnetic resonance imaging 54, positron emission tomography 52 53, 54, 55, 56 sputum cytology 51 Wang needle samples 52 x-rays 49 51, 53 and peripheral lung lesions 52 and pneumonothorax 51 and solitary pulmonary nodules and spinal cord compression 165 and staging 53 diaphragm 53 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 287
299 M classification 221 T stage involvement 85, 216, 219, 220 diesel exhaust fumes (DEF) , 238 and tobacco smoke diet see nutrition diffuse interstitial fibrosis 240 distant metastasis 13, 32, 87 guideline 89 see also lymph node disease; individual sites; Stage IV categorised 214 M classification 217 see also M stage sites of 55, 57 adrenal 55, 57 bone 55, 57 brain 55, 57, 97 liver 55, 57 other 55, 56, 57, 85, 199 treatment guideline 89 chemotherapy 91, 97 radiotherapy 89 surgery 87 dysplasia 30, 151, 241 dyspnoea , 150 guidelines 145 and chemotherapy 125 defined 142 and palliative care 140, 141 and specialist nurse care 60 treatment guidelines 145 oxygen therapy 144 pharmacological , 145 radiotherapy 163 E Early Lung Cancer Action Project (ELCAP) 34, 35, 197 Eastern Cooperative Oncology Group (ECOG) 102 performance status criteria 224 ECOG see Eastern Cooperative Oncology Group EGFR see epidermal growth factor ELCAP see Early Lung Cancer Action Project emphysema 9, 11, 241 endobronchial tumours 52 environmental carcinogens see carcinogens environmental tobacco smoke 7 8, 8 and duration of smoking 7 8 EORTC see European Organization for Research and Treatment of Cancer epidermal growth factor (EGFR) 225 European Organization for Research and Treatment of Cancer (EORTC) 74, 91 EUROSCAN study 30 exercise 26 F false negative CT 35 positron emission tomography 55 and screening 31, 35 and sputum cytology 51 guideline 51 false positive CT 35 and granulomatous disease 53, 55 positron emission tomography 53, 55 guideline 55 and screening 31, 35 FAMCARE scale 151 fatigue 74, 142 and depression 73 management of 125, 141 rate of 141 and treatment 93, 125 febrile neutropenia 102, 103, 124 fine needle aspiration (FNA) 34 guideline 52 accuracy 52 and bullous lung disease 51 and pneumothorax 51 predictive value 51 fluorescence bronchoscopy fluoro-deoxy glucose PET (FDG-PET) see positron 288 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
300 emission tomography FNA see fine needle aspiration follow-up guidelines 61 see also patient support bronchoscopy 60, 61 CT 60, 61 positron emission tomography 60, 61 by specialist nurses 60 and tumour markers 60, 61 x-ray 60, 61 former smokers 6, 7, 29, 32, 241 fruit/vegetable intake 27, 28, 29 G G-CSF see granulocyte colony stimulating factor genetic markers 36 genetic susceptibility 9 GM-CSF see granulocyte macrophage colony stimulating factor granulocyte colony stimulating factor (G-CSF) 103, 124, 205 granulocyte macrophage colony stimulating factor (GM-CSF) 124 granulomatous disease 53, 55 see also tuberculosis great vessels listed 220 T stage involvement 216, 219, 220 H haemoptysis 141, 146 and radiotherapy 163 Health and Safety Commission 231 heart T stage involvement 216, 219, 220 helical CT see CT hilar node disease 86 see also lymph node metastases assessment 53, 54, 86 classification 84 ctnm 53 ptnm 217 TNM 216, 217, 219 diagnosis 53, 54 CT 54 magnetic resonance imaging 54 radiology 53 and small cell lung cancer, limited disease 222 and Stage II non-small cell lung cancer 85 staging 86 N stage 53, 54, 86, 217, 219 T stage 53, 86, 216 treatment surgery 84, 85, 86, 87 histology histopathological grading 218 non-small cell lung cancer 58, 88 small cell lung cancer 128 histoplasmosis 53 hospice care and palliative care 137, 138 symptom management 150, 151 hypercalcaemia 140, 153 and bisphosphonates 169 and non-small cell lung cancer 59, 97 symptoms treatment 154 and vitamin D 181, 182 hypnotherapy 26 hypoxaemia 144 I IARC (International Agency for Research on Cancer) 233 IASLC (International Association for the Study of Lung Cancer) 58 idiopathic pulmonary fibrosis (IPF) 240 immunostaining 36 immunotherapy 26 information provision guidelines 72, 74 and alternative therapies 182 and non-english speaking patients 71 and quality of life 71, 74 recommended approach 71 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 289
301 about support services 75 76, 151 International Agency for Research on Cancer see IARC 233 International Association for the Study of Lung Cancer (IASLC) 58 International Union Against Cancer see UICC interpreter services 71 interventions for smoking cessation see smoking cessation under prevention IPF see idiopathic pulmonary fibrosis J Japanese Lung Cancer Screening Study 84 L large cell carcinoma 6, 56 see also non-small cell lung cancer aetiology 6 pathogenesis 6 and T and N stages 55 and survival rates 13 levels of evidence 50, 254 life years saved (LYS) 191, 194, 205 liver 55, 57 cost-effectiveness of assessment 199 as site of metastases 55, 57 and pain management 147 TNM staging 55 lobar bronchus T classification 216 lobectomy 85 86, 87 guideline 86 and early stage NSCLC 85, 86 success of 85, 86 Lung Cancer Study Group 86 lymph nodes assessment 54, 86 87, 84 guideline 87 regional 215 lymph node metastasis 147 guideline 54 see also hilar, mediastinal, scalene and supraclavicular node disease defined 213, 222 listed 215 node size 34, 49, 51, 52, 87 guideline 54 and solitary pulmonary nodules 49 and staging 54, 86 retroperitoneal 57 staging N classification 217, 219 Stage I 86 TNM category 214 lymphadenectomy 87, 217 lymphangitis carcinomatosis 144 LYS see life years saved M M stage guidelines 56, 57 see also distant metastases assessment by CT 55 positron emission tomography 56, 57 assessment of adrenal metastases brain metastases 55 mediastinal node disease 219 non-small cell lung cancer classification assessment procedure 215 clinical classification 217 ptnm system 217 rules of classification 221 stage grouping 218 summary 219 MX stage clinical classification 217 M0 stage clinical classification 217 and occult metastases 55 stage grouping 218 M1 stage clinical classification 217, 219, 221 involvement of 290 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
302 chest wall 221 diaphragm 221 stage grouping 218 subcategories 214 magnetic resonance imaging (MRI) 54 guideline 166 accuracy 54 and bone metastases 167 and brain metastases 171 and lymph node metastases 54 and spinal cord compression 165, 166 and staging M stage T stage 54 main bronchus 215 T classification 216, 219, 220 malignant airway obstruction 147 management 147 man-made mineral fibres (MMMF) see mineral fibres, man-made marijuana see cannabis mediastinal node disease 198 guidelines 54, 55, 87 see also lymph node metastases and adenocarcinoma 55 assessment 54, 86 cost-effectiveness classification 84 ptnm 217 TNM 216, 217, 219 diagnosis CT 55, 198, 199 positron emission tomography 55, 199 radiology 53, 92 and large cell carcinoma 55 and pain management 147 and sampling 52, 86 guideline 87 and small cell lung cancer 57 limited disease 222 and Stage III non-small cell lung cancer 92 staging 55, 86, 199 M stage 219 N stage 53, 54, 86 87, 92, 217, 219 T stage 53, 86, 216, 219, 220 and squamous cell carcinoma 55 treatment surgery 84, 85, 86, 87 and vocal cord paralysis 153 mediastinal pleura T stage involvement 216, 219, 220 mediastinoscopy 164, as staging procedure 54, 84 mediastinum 53, 87 and T4 classification 216, 219, 220 medical radiation 9 meditation 179, 180, 181 mesothelioma mesothelium T classification 221 metaplasia 30 mineral fibres, man-made (MMMF) 237, 238 MMMF see mineral fibres, man-made MRI see magnetic resonance imaging N N stage 54 55, 85, 96, 226 guidelines 54 assessment by CT positron emission tomography 55 thoracotomy 54, 55 x-ray 53 assessment of hilar node disease 53, 54, 86, 217, 219 large cell carcinoma 55 mediastinal node disease 53, 54, 86 87, 92, 217, 219 non-small cell lung cancer 53, pleural effusion 53 classification 53, 221 assessment procedure 215 clinical classification 217 ptnm system 217 stage grouping 218 summary 219 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 291
303 and surgery 54, 87 NX clinical classification 217 N0 clinical classification 217 stage grouping 218 Stage I 85 Stage 1A 86 Stage II 85 N1 clinical classification 217, 219 involvement of ipsilateral hilar nodes 217, 219 ipsilateral peribronchial 217, 219 intrapulmonary nodes 217 lymph nodes 86, 87 stage grouping 218 Stage II 85 N2 clinical classification 217, 219 diagnosis 55 involvement of ipsilateral mediastinal lymph nodes 217, 219 lymph nodes 86, 87, 92 subcarinal lymph nodes 217, 219 stage grouping 218 Stage IIIA 96, 226 N3 clinical classification 217, 219 diagnosis 55 involvement of contralateral hilar nodes 219 contralateral mediastinal nodes 219 contralateral scalene nodes 219 contralateral supraclavicular nodes 219 stage grouping 218 National Cancer Control Initiative (NCCI) 35 National Cancer Institute (USA) 32 National Cancer Institute of Canada 163 National Strategy for Palliative Care 138 National Tobacco Strategy nausea guideline 179 and chemotherapy 103, 121 and hypercalcaemia 153 and pain management 149 and psychological support 74, 75, 179 guideline 179 as side effect of treatment 148, 149, 171 treatment of 149 NCCI (National Cancer Control Initiative) 35 neutropenia febrile 102, 103, 124 and systemic therapy 225 never smokers 6, 7, 30 nicotine replacement therapy (NRT) guideline 25 forms of 24 and other pharmacotherapy 24, 196 and smoking cessation 22 23, 24, 25 cost-effectiveness 192, 193, , 196 nodal assessment see lymph node assessment non-small cell lung cancer (NSCLC) 83 96, 147 guidelines 54, 55, 56, 57, 59, 85, 86, 87, 89, 90, 91, 92, 94, 95, 100, 101, 104, 106, 145 see also small cell lung cancer advanced (Stages IIIB IV) guidelines 100, 101, 104, 106 and alternative therapies 180, 182 and chemotherapy , 99, 101, 103, 203, 225 management of 74, 83, 97 defined 97 histology 58, 88 locoregional 88, 89 and radiotherapy 88, 89 lymph node assessment guideline 87 survival rates 86, 87 management by 83 96, 83 chemotherapy 83 palliation 83 radiotherapy 83 surgery 83, and metastases 292 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
304 see also distant metastases; individual sites adrenal bone 56, 169 brain 56 liver 55 rate of 55 modalities for investigation CT 54, guidelines 54 magnetic resonance imaging 54, positron emission tomography 54, 55, 56, 57 and other diseases 55, adenomas 55 56, 241 dyspnoea 141, 143 guideline 145 pericardial effusion 152, 153 pleural effusion 152 SVC obstruction 164 vocal cord paralysis 153 and prognostic factors guideline 59 Stage I 83 and cost-effectiveness of positron emission tomography 200 and lymph node assessment 87 and radiotherapy, postoperative 92 and surgery 84, 85 survival rates 84 85, 85 Stage II 83 and cost-effectiveness of positron emission tomography 200 and radiotherapy, postoperative 92 and surgery 84 survival rates 84 85, 85 Stages III 83 and cost-effectiveness of positron emission tomography 200 Stages IIIB and cost-effectiveness of treatment 201 Stage IV 83 and cost-effectiveness of treatment 201 and brain metastases 83 staging guidelines 54, ctnm 53 M stage N stage 53, ptnm 53 T stage 53, 54 TNM symptoms 141 treatment guidelines 85, 86, 87, 89, 90, 91, 92, 94, 95 biological agents 106 brachytherapy 163 chemotherapy 94, 105, 226 continuous hyperfractionated accelerated radiation therapy 90 radical chemoradiation 53 radiotherapy 84, 88, 89, 90, 205, 226 second-line chemotherapy surgery 53, 54, 84, 226 systemic therapy 98 99, 99, Non-Small Cell Lung Cancer Collaborative Group 93, 98 NRT see nicotine replacement therapy NSCLC see non-small cell lung cancer nurses and smoking cessation 22, 25, 27 specialist lung cancer 60, 138 nutrition 27 28, 139, 182 beta-cryptoxanthin 28 micronutrients 27 vegetable/fruit intake 27, 28, 29 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 293
305 O obstructive airways disease 241 see also emphysema obstructive pneumonitis and T classification 216 obstructive pulmonary disease, chronic (COPD) 143, 148 occupational lung cancer see also asbestos-related lung cancer; smoking carcinogens 233, 238, 240 asbestos cooking oil vapour 238, 238 diesel exhaust fumes , 238 metals , 238, 239 mineral fibres, man-made 237, 238 polycyclic aromatic hydrocarbons 237, 238 radiation , 238 silica 234, 238 occupations at risk 239, 240 odds ratios 239 worker exposure 230, 232, 237 oesophagitis 93 oesophagus T stage involvement 216, 219, 220 optical coherence tomography 36 orthopaedic management of bone metastases 169 internal fixation/replacement 167, 168 risk assessment 170 P PAH see polycyclic aromatic hydrocarbons pain clinics 150 pain control see pain management pain management , 151 guidelines 145, 147, 150 see also symptom management assessment 148 and bone metastases 83, 147, 150, 168 guidelines 147 rate of pain relief 168 and palliative care palliative care 49, 73, 137, guidelines 16, 75, 138, 145, 147, 151 for carers 137, 140 cost-effectiveness 151 defined 137 early referral 75, 139 guideline 75 forms of 119 pharmacological 148, 149, 150 and management of non-small cell lung cancer 83, 97 Stages IIIB and IV 83 outcomes 151 and pain management principles of 149 providers general practitioners 139 community services 138, 139 specialist respiratory nurses 138 specialist teams 138, 140, 141, 148 and quality of life 137 quality of dying 137 sites for acute hospital 140 inpatient hospices patient s residence symptom management bone metastases 170 constipation 149, cough 145 dyspnoea 140, 141, , 150 hypercalcaemia 153 malignant airway obstruction 147 pleural effusion 152 pericardial effusion vocal cord paralysis 153 palliative radiation see radiotherapy, palliative Pancoast syndrome 147 and pain management 147 parietal pericardium T stage involvement 216, 221 parietal pleura T stage involvement Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
306 ipsilateral 221 PAR% see population-attributable risk percentage passive smoking see environmental tobacco smoke pathological fracture and orthopaedic referral 167, 169 treatment of bisphosphonates 167, 169 chemotherapy 167, 169 internal fixation/replacement 167, 168 radiotherapy , 169 pathology reporting of lung cancer resections, standardised Nepean Hospital Lung Cancer Reporting Protocol example of report 257 patient support 71 72, guidelines 72, 73, 74, 75, , 179, 181 see also follow-up breaking bad news 71, 72 guideline 72 and death 75, 137, 138, 139, 146 information provision psychosocial support 73 75, 142, 143, 147, 181 guidelines 73, 75, 145, 150, 179, 181 social support PCI see prophylactic cranial irradiation performance status 49 guideline 59, 60, 89, 90, 100, 104, 106, 164 criteria (Eastern Cooperative Oncology Group) 224 and management of non-small cell lung cancer 83 Stages I III 90 as predictor of depression 73 prognostic factor for non-small cell lung cancer guideline 59 prognostic factor for small cell lung cancer 59 guideline 60 and treatments and chemotherapy 90, 98, 99, 100, 102 guidelines 90, 100, 104 combination therapies 90, 102 and radiotherapy 89, 90, 163 guideline 89, 90, 164 and second-line chemotherapy 105 guidelines 106 pericardial effusion 152, 153 management 153 T classification 221 treatment 152 pericardium T stage involvement parietal pleura 85 parietal pericardium 216, , 219, 220 peripheral lung lesions 51 guideline 52 diagnosis 52 peripheral tumours 36, 51 PET see positron emission tomography phrenic nerve T stage involvement 220 Physicians Health Study 29 PLCO (prostate, lung, colon and ovarian) study 32 pleural effusion 143, 152 guidelines 152, 153 management 152 and N stage 53 and small cell lung cancer 222 and Stage IIIB non-small cell lung cancer 97 and T classification 216, 219, 221 and T stage 53, 216, 219, 220, 221 pleural plaques 230 pneumonectomy 84, 85 pneumonitis 93, 241 pneumothorax 51 polycyclic aromatic hydrocarbons (PAH) , 238 worker exposure 237 population-attributable risk percentage (PAR%) 230 positron emission tomography (PET) 50, 52 53, 54 guideline 53, 55, 61 accuracy 50, 52 53, 55, 56, 57 cost-effectiveness 50, 52 managing non-small cell lung cancer 199, 200 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 295
307 staging non-small cell lung cancer 56, false negative 55 false positive 53, 55 guideline 55 and follow-up 60 guideline 61 and granulomatous disease 53, 55 predictive value 53, 55 and staging M stage 56, 57 N stage T stage 54 predictive value fine needle aspiration biopsies 51 positron emission tomography 53, 55 prevention see also smoking cessation chemoprevention nutrition previous lung disease 9, 10, 11 relative risks 11 prognosis guidelines 59, 60 prognostic factors age 58, 59 albumin 58 performance status 58, 59 serum LDH 58, 59 sex 58, 59 weight loss 58, 59, 60 and non-small cell lung cancer and staging 59 TNM stage 58, 59 and small cell lung cancer guideline 60 and brain metastases 59 and staging 59 extensive disease 59, 60 limited disease 59, 60 progressive systemic sclerosis (scleroderma) 240 prophylactic cranial irradiation (PCI) 119, 127 guidelines 127 benefits 127 dose 127 side effects 74 and small cell lung cancer 119, 127, 205 survival rate 127 prostate, lung, colon and ovarian cancer screening (PLCO) study 32 provitamin A carotenoids see vitamin A psychiatry 75 see also psychological therapies psychological therapies guideline 73 benefits of 74 forms of delivery 74 modes of 74 relaxation-based therapies 75 see also relaxation for smoking cessation psychosocial support 73 75, 179 guidelines 73, 74, 75, 145, 150, 179, 181 and alternative therapies anxiety 73, guidelines 73, 145, 150 and dyspnoea 142, 143 and pain management 147 and carers 73, 137 depression 73, guideline 73 rate 73 predictors of 73 treatment guidelines 73, 75 antidepressants 73 palliative care 75 psychological ptnm 53, 217 Public Health Service (US) report 21 pulmonary disease, chronic obstructive (COPD) see chronic obstructive pulmonary disease pulmonary fibrosis 240 pulmonary nodule see solitary pulmonary nodule 296 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
308 Q QALY (Quality Adjusted Life-Years) and chemotherapy 228 cost-effectiveness of treatment 194, 228 and nicotine replacement therapy 194 and other therapies 205 Quality Adjusted Life-Years see QALY quality of life 35, 71, 74, 101, 139 guidelines 75 see also depression; pain management; psychosocial support and disease dyspnoea 142 non-small cell lung cancer 74, 97, 98, 99, 99, 100, 210, 227 small cell lung cancer 74 spinal cord compression 165, 166 and dying 136, 137, 140 and follow-up 60 and palliative care 75, 137, 139 and treatment side effects guidelines 75 chemotherapy 99, 99, 101, 102, 103, 122, 127, 201, oxygen therapy 148 prophylactic cranial irradiation 74, 127 psychological 74, 75 QUIT program 27, 253, 273 see also smoking cessation R R (residual tumour) classification 214 radiation (as carcinogen) , 238 radon , 238 exposure 234 risk 234 and tobacco smoke 235 uranium 235, 238 Radiation Therapy Oncology Group (RTOG) 89 radical chemoradiation 53 radiotherapy 88 93, 163 guidelines 89, 90, 91, 92, 126, 127, 147, 164, 166, 168, 172, 181 combined with chemotherapy 90 94, 120, 121, 226 surgery 92, 226 compared with chemotherapy 84, 90, 91 surgery 84, 88, 92 complications of 93 oesophagitis 93 pneumonitis 93 spinal cord injury 93 cost-effectiveness 205 dosage 89, 93, 163, 168 guidelines 89, 164, 172 hyperfractionated Radiation Therapy Oncology Group 89 duration 89 90, 163, 168 accelerated continuous hyperfractionated accelerated radiotherapy fractionated radiotherapy 168 and non-small cell lung cancer 84, 88, 89, 91 guideline 91 advanced 205 locoregional 88 management of 83, 84 and squamous cell carcinoma 88 and pain management 168 guidelines 147 palliative and small cell lung cancer guidelines 126, 127 limited disease 119 and Stage I 83, 92 and Stage II 83, 92, 226 and Stage III 92, 95 and Stage IIIA 83 and Stage IV 83 and stage of disease 90, 91 survival rates 84, 89, 90, 163, 226 toxicity 89, 120, 163 for treatment of guidelines 168, 172 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 297
309 bone metastases 140, 148, 149, , 169, 170 brain metastases 171, 172 haemoptysis pain 163 spinal cord compression 165, 166 squamous cell carcinoma 88, 90 Stage I 53, 90, 92, 226 Stage II 90, 92, 226 Stage IV 83 SVC obstruction 164 Veteran s Administration Lung Cancer Study Group 88 radiotherapy, palliative guidelines 164, 165, 168 multidisciplinary approach 165, 166 symptoms treated atelectasis 163 bone metastases 165, brain metastases 171 pathological fractures 167 solitary lesions 167 spinal cord compression SVC obstruction radon , 238 interactions with other carcinogens 233, 234, 236 referral 49, 150, 267 guidelines 49, 75 and multidisciplinary care 49 orthopaedic 167 to palliative care 139 for psychological care 49, 75 timing of 75, 139 relaxation 75, 148, 179, 180, 181 guideline 145 and dyspnoea 143, 145 respite care 75, 140 retinoids 30 see also beta-carotene ribs 170 T stage involvement 221 risk factors see also asbestos; carcinogens age 4, 7, 11 education 7, 9, 11 ethnicity 7, 9, 11 and general risk of cancer 7 8 genetic susceptibility 9 location of residence 4, 9 medical radiation 9 nutrition occupational exposures 7, 239, 240 see also occupational lung cancer previous lung disease, 9, 11 sex 3, 5, 7, 9 smoking 6, 7, 28 see also smoking environmental tobacco smoke 7 8, 8 Royal Australian and New Zealand College of Obstetricians and Gynaecologists 21 RTOG (Radiation Therapy Oncology Group) 89 S sarcoidosis 53 scalene lymph node 215 see also lymph node metastases and TNM classification 217, 219 SCLC see small cell lung cancer scleroderma (progressive systemic sclerosis) 240 screening 31, guideline 33 and case finding 31 Early Lung Cancer Action Project study 34, 35 false negative 31, 35 false positive 31, 35 Mayo Lung Project 32 methods of biomarkers 32, breath sample analysis 36 fine needle aspiration biopsies 34 fluorescence bronchoscopy genetic markers 36 helical CT 32, immunostaining 36 laser induced fluorescence endoscopy Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
310 optical coherence tomography 36 polymerase chain reaction assays 36 sputum cytology 32 33, 36 virtual bronchoscopy 36 x-ray 32, 33 past effects of 32 prostate, lung, colon and ovarian study 32 Surveillance, Epidemiology, and End Results program 32 second primary lung cancers 30, 60 SEER (Surveillance, Epidemiology, and End Results) program 32, 197 segmentectomy 85, 86 selenium 27 self-help guidelines 25 for smoking cessation 22, 23, 193 guidelines 25 and social support 75 silica 234, 238 see also carcinogens interactions with other carcinogens 233, 236 silica-related lung cancer 230, 233, 234 see also occupational lung cancer silicosis 230, 234, 238 interactions with other carcinogens 233, 234 and lung cancer risk 234 small cell lung cancer (SCLC) 5 6, , 240 guidelines 58, 60, 123, 125, 126, 127, 146 aetiology 5, 235 and cost-effectiveness of treatment 205 development of 52, 57 histology 128 management by stage 51, 119 extensive disease 119, 120, 121, 127 limited disease 119, 126 and other diseases SVC obstruction 164, 165 vocal cord paralysis 153 pathogenesis 5 rate of 57 staging extensive disease 56, 57 classification 221, 222, 223 limited disease 56 classification 221, 222 and TNM staging system 57, 221 survival rates 13, , 121, 122, 123, 124, symptom control 119 symptoms 141 treatment chemotherapy 57, , 125, 126 chemoradiotherapy 119 combination chemotherapy 119, 120, 121, 126 prophylactic cranial irradiation 119, 127 radiotherapy 57, 119, 120, 121, , 128 second-line chemotherapy 125 smoking 6 8 cannabis 8 environmental 7 8, 8 former smokers 6, 7, 29, 32, 241 never smokers 6, 7, 30 tobacco 6 8 and asbestos-related lung cancer 231, 233 interactions with other carcinogens 231, 233, 235, 236, 237 and pregnancy 21 and related diseases 22 and usual interstitial pneumonia 240 smoking cessation guidelines 25, 26 Cancer Councils 253 cost-effectiveness nicotine replacement therapy 192, 193 and Early Lung Cancer Action Project study 35 interventions acupuncture 25, 26 alternative therapies 25, 26 aversion therapy 23, 26 counselling programs 22, 23, 192, 193, exercise 25, 26 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 299
311 by general practitioners 22, 25, 27, 192, , 253 group therapy 22, 25, 27 by health care professionals 192, 253 hospital admission 25, 26, 192, 193 hypnotherapy 25, 26 immunotherapy 26 individual counselling 22, 25, 27 information programs mass media campaigns 194, 195 and National Tobacco Strategy nicotine replacement therapy 22 23, 24, 25, 193, , 196 by nurses 22, 25, 27 by pharmacists pharmacological therapies 24, 25, 27, 192 QUIT program 27, 253, 273 self-help 23, 25, 193 silver acetate 23 telephone counselling 23, 27 strategies to assist 25, 27 Smoking cessation clinical practice guidelines 21 SMR (Standardised Mortality Ratio) 235, 236, 237 social support solitary pulmonary nodule (SPN) calcification 50 malignancy rate 50 South Western Oncology Group (USA) (SWOG) 120, 121 Southeastern Cancer Study Group 120 spinal cord compression 93, guidelines 166 investigation methods CT 165 magnetic resonance imaging 165, 166 x-ray 165 management 166 orthopaedic referral 165, 169 treatment 97, 140 dexamethasone 165, 166 radiotherapy 165, 166 surgery 166 urgency 165, 166 spiral computed tomography see CT SPN see solitary pulmonary nodule sputum atypia 30 sputum cytology 32 33, 36, 51, 198 guidelines 33, 51 false negative 51 and screening squamous cell carcinoma 5, 52, 55, 58 see also non-small cell lung cancer aetiology 5 diagnosis by CT sputum cytology 51 and obstructive airways disease 241 pathogenesis 5 and survival rates 13 treatment of radiotherapy 88, 90 surgery 58 squamous metaplasia 30 Stage grouping 218 see also TNM staging small cell lung cancer extensive disease 221, 222, 223 limited disease 221, 222 Stage I 85 guidelines 85, 92 and chemotherapy 53, 90, 226 detection 30, 200 and lymph node assessment 86, 87 management 83 radiotherapy 53, 83, 90, 92, 226 guideline 92 survival 53, 92 and small cell lung cancer category 221 Stage grouping 218 and surgery 34, 53, 84 85, 85, 86, 226 survival rates 34, 53, 84, 85, 86 87, 226 and T stage 85, 86 Stage IA 86, 218 Stage IB 96, 218 Stage II Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
312 guideline 92 detection 200 management 83 N stage 85 Stage grouping 218 survival rates 84 85, 85, 226 T stage 85 and treatment guideline 92 chemotherapy 90, 226 radiotherapy 83, 90, 92, 226 surgery 53, 83, 84, 85, 226 Stage IIA 218 Stage IIB 218 Stage III 92 guideline 95 detection 200 management 83 Stage grouping 218 treatment 96, 226 chemotherapy 59, 91 combined 59, 90, 92 radiotherapy 92, 95 surgery 92, 226 Stage IIIA guideline 95 management of 83 N stage 96, 226 and small cell lung cancer category 221 Stage grouping 218 survival rates 94, 95, 226 treatment 95, 96, 226 chemotherapy 94, 95 radiotherapy 83 surgery 94, 95 Stage IIIB management of 83 and pleural effusion 97 and small cell lung cancer category 221 Stage grouping 218 treatment chemotherapy 97, 201 Stage IV and bone metastases 83 and brain metastases 83 management 83 and small cell lung cancer category 221 Stage grouping 218 treatment 201 chemotherapy 59, 97, 225 radiotherapy 83, 83 surgery 83 Stage 0 Stage grouping 218 staging guidelines 54, 56 and non-small cell lung cancer 53 57, and small cell lung cancer classification TNM system classification Standardised Mortality Ratio (SMR) 235, 236, 237 standardised pathology reporting of lung cancer resections Nepean Hospital Lung Cancer Reporting Protocol example of report 257 stereotactic radiosurgery 171, 172 guideline 172 subcarinal lymph node see also lymph node metastases and TNM classification 217, 219 superior sulcus tumour 54 T classification 216 superior vena cava (SVC) obstruction 164 guidelines 165 T classification 220 supraclavicular lymph nodes 215 see also lymph node metastases small cell lung cancer classification 222 TNM classification 217, 219 surgery guidelines 85, 86, 87, 92, 94, 95, 166, 172 combined with chemotherapy 226 radiotherapy 92, 226 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 301
313 compared with radiotherapy 84, 88, 92 surgery 92, 93, forms of guidelines 87, 172 lobectomy 85 86, 87 lymphadenectomy 87, 217 pneumonectomy 84, 85 segmentectomy 85, 86 thoracotomy 54, 55, 86, 147, and management of non-small cell lung cancer 53, 83, guidelines 85, 86, 87 lymph node assessment lymph node classification 84 survival rates 84 85, 85, 189, 226 and positron emission tomography 199 and Stage I 83, 84 85, 85, 86, 226 and Stage II 53, 83, 84, 85, 226 and Stage III 92, 226 and Stage IV 83 for treatment of bone metastases brain metastases 83, 171, 172 spinal cord compression Stage I 34, 53, 84 85, 85, 86, 226 Stage III 92, 226 Stage IIIA 94, 95 Surveillance, Epidemiology, and End Results (SEER) program 32, 197 SVC obstruction see superior vena cava obstruction SWOG (South Western Oncology Group) 120, 121 symptom control see symptom management symptom management 142, 151 see also pain management and chemotherapy 97, 98, 99, 99, 104, 122, 125 and palliative care 75, 137, 138, 140, 141 and palliative radiotherapy 164 of small cell lung cancer 119 of spinal cord compression 166 of SVC obstruction 164 systemic therapy 98 99, 99, see also chemotherapy T T stage 53, 87, 215 assessment 53 CT 54, 55 magnetic resonance imaging 54 positron emission tomography 54 x-ray 53 associated with atelectasis 216 mediastinum 216 obstructive pneumonitis 216 pleural effusion 216 superior sulcus tumour 216 classification , assessment procedure 215 clinical classification ptnm system 217 rules of classification stage grouping 218 summary 219 and surgery 54, 87 TX stage 216, 218, 219 T0 stage 216 Tis stage 216, 218 T1 stage 86, 219, 220 association with pleural effusion 216 clinical classification 216, 220 involvement of lobar bronchus 216 and N classification 53, 221 Stage I 85, 86 Stage II 85 stage grouping 218 T2 stage 219, 220 association with atelectasis 216, 219, 220 pleural effusion 216 obstructive pneumonitis Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
314 clinical classification 216, 220, 221 involvement of hilar region 216 main bronchus 216, 219, 220 visceral pleura 216, 219, 220, 221 and N classification 53, 221 Stage I 85 Stage II 85 stage grouping 218 T3 stage 216 association with atelectasis 216, 219, 220 obstructive pneumonitis 216 pleural effusion 216 superior sulcus tumours 216 clinical classification 216, 220 involvement of chest wall 85, 216, 219, 220 diaphragm 85, 216, 219, 220 main bronchus 216, 219, 220 mediastinal pleura 216, 219, 220 parietal pericardium 216, 221 parietal pleura 85 pericardium 85, 219, 220 phrenic nerve 220 rib 221 and N classification 221 Stage II 85 stage grouping 218 T4 stage 216 associated with malignant pleural effusion 216, 219, 220, 221 SVC obstruction 220 vocal cord paralysis 220 clinical classification 216, 220 involvement of carina 216, 219, 220 great vessels 216, 219, 220 heart 216, 219, 220 ipsilateral parietal pleura 221 mediastinum 219, 220 oesophagus 216, 219, 220 trachea 216, 219, 220 vertebra 216, 219, 220 visceral pericardium 221 and N classification 221 stage grouping 218 telephone counselling 23, 75 thoracotomy 86, 147, and N stage 54, 55 TNM staging guideline 59 see also Stage grouping assessment procedure 215 clinical classification ptnm system 217 rules of classification Stage grouping 218 summary 219 tobacco 6 8 see also smoking cessation and asbestos-related lung cancer 231, 233 interactions with other carcinogens 231, 233, 235, 236, 237 and pregnancy 21 and related diseases 22 and usual interstitial pneumonia 240 toxicity 181, 236 see also individual therapies genotoxicity 237, 238 haematological 102, 103, 225 neurotoxicity 121, 127 treatment at follow-up 60 trachea T stage involvement 216, 219, 220 Treating tobacco use and dependence 21 tuberculosis 50, 53 and risk of cancer 9, 11 tumour markers 60, 61 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer 303
315 U UICC (International Union Against Cancer) 58 UIP (usual interstitial pneumonia) 240 uranium 235, 238 and radon 234, 235 usual interstitial pneumonia (UIP) 240 V VALCSG see Veteran s Administration Lung Cancer Study Group VAS see visual analogue scale VATS see video-assisted thoracic techniques vegetable/fruit intake 27, 28, 29 vertebra see also bone metastases T stage involvement 216, 219, 220 Veteran s Administration Lung Cancer Study Group (VALCSG) 88, 221 classification 222 definitions extensive and limited disease 222, 223 video-assisted thoracoscopic techniques (VATS) 86 virtual bronchoscopy 36 visceral pericardium T stage involvement 221 visceral pleura T classification 216, 219, 220, 221 visual analogue scale (VAS) 142, 143 vitamin A 27, 181 vitamin C 27 vitamin D 181 and hypercalcaemia 181, 182 vitamin E 27, 29 vocal cord paralysis 153 T classification 220 treatment 153 volunteer support 75, 139 WLM (working level months) 234 Women s Health Study 29 working level months (WLM) 234 World Health Organization (WHO) 148 X x-rays 32, 50 guideline 61 assessment of T and N stages 53 cost-effectiveness , 198 and CT 33, 34, for diagnosis 49 51, 63 bone metastases 167 spinal cord compression 165 and follow-up 60, 61 for screening 32 33, 196 Y years lost due to disability (YLD) 189, 189 years of life lost (YLL) 189, 189 YLD see years lost due to disability YLL see years of life lost W weight loss 58, 59, 181 guideline 59 WHO see World Health Organization 304 Clinical practice guidelines for the prevention, diagnosis and management of lung cancer
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Radiotherapy in locally advanced & metastatic NSC lung cancer
 Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Lung cancer. A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment
 Lung cancer A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment Contents Contents 2 3 Section 1: Lung Cancer 4 i. Types of lung cancer 4 ii. Causes and risk factors 5 iii. Symptoms
Lung cancer A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment Contents Contents 2 3 Section 1: Lung Cancer 4 i. Types of lung cancer 4 ii. Causes and risk factors 5 iii. Symptoms
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Asbestos Related Diseases
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
This factsheet aims to outline the characteristics of some rare lung cancers, and highlight where each type of lung cancer may be different.
 There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Lung Cancer. Know how to stay strong
 Lung Cancer Know how to stay strong What is cancer? 2 Cancer is a disease when some cells in the body grow out of control Normal cells Your body has many tiny cells and keeps making new cells to keep you
Lung Cancer Know how to stay strong What is cancer? 2 Cancer is a disease when some cells in the body grow out of control Normal cells Your body has many tiny cells and keeps making new cells to keep you
Asbestos Related Diseases. Asbestosis Mesothelioma Lung Cancer Pleural Disease. connecting raising awareness supporting advocating
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
POLICY A. INDICATIONS
 Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
Lung Cancer & Mesothelioma 2011-2015
 Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
Lung Cancer & Mesothelioma 2011-2015 Annex G Mesothelioma 1. The vision for mesothelioma services is set out in the Mesothelioma Framework issued by DH on 26 February 2007 (supported by the British Thoracic
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
Guidance on competencies for management of Cancer Pain in adults
 Guidance on competencies for management of Cancer Pain in adults Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine B: Competencies for practitioners in Pain Medicine
Guidance on competencies for management of Cancer Pain in adults Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine B: Competencies for practitioners in Pain Medicine
Developing a model for peer support for patients with lung cancer. Final Report May 2008
 Developing a model for peer support for patients with lung cancer Final Report May 2008 Project Coordinator: Dr Linda Mileshkin Assistant Nurse Researcher: Allison Hatton Introduction Lung cancer is now
Developing a model for peer support for patients with lung cancer Final Report May 2008 Project Coordinator: Dr Linda Mileshkin Assistant Nurse Researcher: Allison Hatton Introduction Lung cancer is now
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
Please see the LUCADA data manual v3.1.3, available in the downloads section
 National Lung Cancer Audit Frequently Asked Questions What dataset should be used? Please see the LUCADA data manual v3.1.3, available in the downloads section What does LUCADA stand for? LUCADA stands
National Lung Cancer Audit Frequently Asked Questions What dataset should be used? Please see the LUCADA data manual v3.1.3, available in the downloads section What does LUCADA stand for? LUCADA stands
PRACTICE FRAMEWORK AND COMPETENCY STANDARDS FOR THE PROSTATE CANCER SPECIALIST NURSE
 PRACTICE FRAMEWORK AND COMPETENCY STANDARDS FOR THE PROSTATE CANCER SPECIALIST NURSE MARCH 2013 MONOGRAPHS IN PROSTATE CANCER OUR VISION, MISSION AND VALUES Prostate Cancer Foundation of Australia (PCFA)
PRACTICE FRAMEWORK AND COMPETENCY STANDARDS FOR THE PROSTATE CANCER SPECIALIST NURSE MARCH 2013 MONOGRAPHS IN PROSTATE CANCER OUR VISION, MISSION AND VALUES Prostate Cancer Foundation of Australia (PCFA)
Management of Non-Small Cell Lung Cancer Guide for General Practitioners
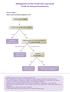 Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Management of n-small Cell Lung Cancer Guide for General Practitioners Clinical Stage I Cancer only in one lobe of lung and
Scottish Medicines Consortium
 Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Surgeons Role in Symptom Management. A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND
 Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
An Update on Lung Cancer Diagnosis
 An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
An Update on Lung Cancer Diagnosis Dr Michael Fanning MBBS FRACGP FRACP RESPIRATORY AND SLEEP PHYSICIAN Mater Medical Centre Outline Risk factors for lung cancer Screening for lung cancer Radiologic follow-up
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Cancer research in the Midland Region the prostate and bowel cancer projects
 Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Surgery. Wedge resection only part of the lung, not. not a lobe, is removed. Cancer Council NSW
 The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline
 Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline An ASCO Endorsement of Treatment of Small Cell Lung Cancer:
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline An ASCO Endorsement of Treatment of Small Cell Lung Cancer:
Lung cancer case study
 Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Therapeutic Goods Administration Orphan Drugs Program: Discussion paper
 Therapeutic Goods Administration Orphan Drugs Program: Discussion paper Submission from the Clinical Oncology Society of Australia and Cancer Council Australia March 2015 The Clinical Oncology Society
Therapeutic Goods Administration Orphan Drugs Program: Discussion paper Submission from the Clinical Oncology Society of Australia and Cancer Council Australia March 2015 The Clinical Oncology Society
Everolimus plus exemestane for second-line endocrine treatment of oestrogen receptor positive metastatic breast cancer
 LONDON CANCER NEWS DRUGS GROUP RAPID REVIEW Everolimus plus exemestane for second-line endocrine treatment of oestrogen receptor positive metastatic breast cancer Everolimus plus exemestane for second-line
LONDON CANCER NEWS DRUGS GROUP RAPID REVIEW Everolimus plus exemestane for second-line endocrine treatment of oestrogen receptor positive metastatic breast cancer Everolimus plus exemestane for second-line
Lung Cancer: More than meets the eye
 Lung Cancer Education Program November 23, 2013 Lung Cancer: More than meets the eye Shantanu Banerji MD, FRCPC Presenter Disclosure Faculty: Shantanu Banerji Relationships with commercial interests: Grants/Research
Lung Cancer Education Program November 23, 2013 Lung Cancer: More than meets the eye Shantanu Banerji MD, FRCPC Presenter Disclosure Faculty: Shantanu Banerji Relationships with commercial interests: Grants/Research
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group
 REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group In the 2002 edition of the ASCO meeting, a total of 315 abstracts in the field of respiratory
REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group In the 2002 edition of the ASCO meeting, a total of 315 abstracts in the field of respiratory
2015/16 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)-
 2015/16 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)- SECTION B PART 1 - SERVICE SPECIFICATION FOR LUNG CANCER Service specification
2015/16 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)- SECTION B PART 1 - SERVICE SPECIFICATION FOR LUNG CANCER Service specification
Understanding ductal carcinoma in situ (DCIS) and deciding about treatment
 Understanding ductal carcinoma in situ (DCIS) and deciding about treatment Developed by National Breast and Ovarian Cancer Centre Funded by the Australian Government Department of Health and Ageing Understanding
Understanding ductal carcinoma in situ (DCIS) and deciding about treatment Developed by National Breast and Ovarian Cancer Centre Funded by the Australian Government Department of Health and Ageing Understanding
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Lung Cancer Treatment
 Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Tricia Cox on 7/18/2012 at Oncology Center. Sarah Randolf. Female
 SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide
 What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
One out of every two men and one out of every three women will have some type of cancer at some point during their lifetime. 3
 1. What is cancer? 2. What causes cancer?. What causes cancer? 3. Can cancer be prevented? The Facts One out of every two men and one out of every three women will have some type of cancer at some point
1. What is cancer? 2. What causes cancer?. What causes cancer? 3. Can cancer be prevented? The Facts One out of every two men and one out of every three women will have some type of cancer at some point
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options
 Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Goals and Objectives: Breast Cancer Service Department of Radiation Oncology
 Goals and Objectives: Breast Cancer Service Department of Radiation Oncology The breast cancer service provides training in the diagnosis, management, treatment, and follow-up of breast malignancies, including
Goals and Objectives: Breast Cancer Service Department of Radiation Oncology The breast cancer service provides training in the diagnosis, management, treatment, and follow-up of breast malignancies, including
ductal carcinoma in situ (DCIS)
 Understanding ductal carcinoma in situ (DCIS) and deciding about treatment Understanding ductal carcinoma in situ (DCIS) and deciding about treatment Developed by National Breast and Ovarian Cancer Centre
Understanding ductal carcinoma in situ (DCIS) and deciding about treatment Understanding ductal carcinoma in situ (DCIS) and deciding about treatment Developed by National Breast and Ovarian Cancer Centre
a commitment in their practice to the roles and responsibilities of clinical oncologists X
 CLINICAL ONCOLOGY BLUEPRINT OF ASSESSMENT SYSTEM Good Medical Practice areas of curriculum - ST5 (Intermediate) Standards GMP criterion Workplace based assessment By the end of the third year of training
CLINICAL ONCOLOGY BLUEPRINT OF ASSESSMENT SYSTEM Good Medical Practice areas of curriculum - ST5 (Intermediate) Standards GMP criterion Workplace based assessment By the end of the third year of training
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Mesothelioma in Australia: Incidence (1982 to 2013) and Mortality (1997 to 2012)
 Mesothelioma in Australia: Incidence (1982 to 213) and Mortality (1997 to 212) 215 Disclaimer The information provided in this document can only assist you in the most general way. This document does not
Mesothelioma in Australia: Incidence (1982 to 213) and Mortality (1997 to 212) 215 Disclaimer The information provided in this document can only assist you in the most general way. This document does not
Lung cancer is not just one disease. There are two main types of lung cancer:
 1. What is lung cancer? 2. How common is lung cancer? 3. What are the risk factors for lung cancer? 4. What are the signs and symptoms of lung cancer? 5. How is lung cancer diagnosed? 6. What are the available
1. What is lung cancer? 2. How common is lung cancer? 3. What are the risk factors for lung cancer? 4. What are the signs and symptoms of lung cancer? 5. How is lung cancer diagnosed? 6. What are the available
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Lung cancer (non-small-cell)
 Patient information from the BMJ Group Lung cancer (non-small-cell) It can be devastating to find out that you or someone close to you has lung cancer. You will have to make some important decisions about
Patient information from the BMJ Group Lung cancer (non-small-cell) It can be devastating to find out that you or someone close to you has lung cancer. You will have to make some important decisions about
the standard of care 2009 5/1/2009 Mesothelioma: The standard of care take home messages PILC 2006 [email protected] Brussels, March 7, 2009
 Mesothelioma: The standard of care [email protected] Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
Mesothelioma: The standard of care [email protected] Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Stage I, II Non Small Cell Lung Cancer
 Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy) for Paediatric Cancer Treatment
 Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy) for Paediatric Cancer Treatment Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy)
Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy) for Paediatric Cancer Treatment Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Proton Beam Radiotherapy (High Energy)
The National Clinical Lung Cancer Audit (LUCADA)
 The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
The National Clinical Lung Cancer Audit (LUCADA) DATA MANUAL Title: Version: 3.1.5 Date: September 2013 LUCADA Lung Cancer Audit VERSION HISTORY Version Date Issued Brief Summary of Change Owner s Name
Adjuvant Therapy Non Small Cell Lung Cancer. Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015
 Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Primary Care Management of Colorectal Cancer
 Primary Care Management of Colorectal Cancer Dr. Dan Renouf, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Primary Care Management of Colorectal Cancer Survivors Daniel
Primary Care Management of Colorectal Cancer Dr. Dan Renouf, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Primary Care Management of Colorectal Cancer Survivors Daniel
RESEARCH EDUCATE ADVOCATE. Just Diagnosed with Melanoma Now What?
 RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
CLINICAL POLICY Department: Medical Management Document Name: Opdivo Reference Number: CP.PHAR.121 Effective Date: 07/15
 Page: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Page: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Malignant Mesothelioma
 Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Mesothelioma
 Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Cancer in Ireland 2013: Annual report of the National Cancer Registry
 Cancer in 2013: Annual report of the National Cancer Registry ABBREVIATIONS Acronyms 95% CI 95% confidence interval APC Annual percentage change ASR Age standardised rate (European standard population)
Cancer in 2013: Annual report of the National Cancer Registry ABBREVIATIONS Acronyms 95% CI 95% confidence interval APC Annual percentage change ASR Age standardised rate (European standard population)
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
PRIMARY LUNG CANCER TREATMENT
 PRIMARY LUNG CANCER TREATMENT Cancer Care Pathways Directorate Tailored Information in Cancer Care (TICC) Sir Anthony Mamo Oncology Centre December 2014 Contents About this booklet 1 Types of Lung Cancer
PRIMARY LUNG CANCER TREATMENT Cancer Care Pathways Directorate Tailored Information in Cancer Care (TICC) Sir Anthony Mamo Oncology Centre December 2014 Contents About this booklet 1 Types of Lung Cancer
Asbestos and your lungs
 This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
TREATING LUNG CANCER AT VA PITTSBURGH HEALTHCARE SYSTEM A HERO S GUIDE
 Providing the best in cancer care for Veterans TREATING LUNG CANCER AT VA PITTSBURGH HEALTHCARE SYSTEM A HERO S GUIDE VA Pittsburgh s state-of-the-art TomoTherapy machine, which delivers radiation to patients.
Providing the best in cancer care for Veterans TREATING LUNG CANCER AT VA PITTSBURGH HEALTHCARE SYSTEM A HERO S GUIDE VA Pittsburgh s state-of-the-art TomoTherapy machine, which delivers radiation to patients.
SMALL. 1-800-298-2436 LungCancerAlliance.org
 UNDERSTANDING Non- SMALL CELL LUNG CANCER 1-800-298-2436 LungCancerAlliance.org A guide for the patient I ANATOMY OF THE LUNGS The following image shows different parts that make up the lungs. Please use
UNDERSTANDING Non- SMALL CELL LUNG CANCER 1-800-298-2436 LungCancerAlliance.org A guide for the patient I ANATOMY OF THE LUNGS The following image shows different parts that make up the lungs. Please use
People Living with Cancer
 Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Medical Oncology. Rotation Goals & Objectives for rotating residents. General Objectives THE UNIVERSITY OF BRITISH COLUMBIA
 THE UNIVERSITY OF BRITISH COLUMBIA Department of Urologic Sciences Faculty of Medicine Gordon & Leslie Diamond Health Care Centre Level 6, 2775 Laurel Street Vancouver, BC, Canada V5Z 1M9 Tel: (604) 875-4301
THE UNIVERSITY OF BRITISH COLUMBIA Department of Urologic Sciences Faculty of Medicine Gordon & Leslie Diamond Health Care Centre Level 6, 2775 Laurel Street Vancouver, BC, Canada V5Z 1M9 Tel: (604) 875-4301
