Unit 4 FIRST AID Lecture notes
|
|
|
- Tracy Hawkins
- 9 years ago
- Views:
Transcription
1 Unit 4 FIRST AID Lecture notes I. Emergency Procedures a. Most sports injuries do not result in life or death emergency situations, but when such situations do arise, prompt care is essential. b. Emergency care is defined as an unforeseen combination of circumstances and the resulting state that call for immediate action. c. Time becomes a critical factor and assistance to the athlete must be based on knowledge of what to do and how to do it. d. The prime concern of emergency aid is to maintain cardiovascular function, and indirectly, central nervous system function, since failure of any of these symptoms may lead to death. e. All sports programs must have an EMERGENCY PLAN that can be quickly and easily set in motion. The following issues should be addressed when developing an emergency plan: i. Know the location of the phones and emergency telephone numbers. ii. Know who is designated to make emergency telephone calls. Who has the key to gates or padlocks and who will open them? iii. Know the information to be given over the telephone. 1. Type of emergency situation. 2. Type of suspected emergency. 3. Present condition of the athlete. 4. Current assistance being given (for example, CPR or rescue breathing). 5. Location of telephone being used. 6. Exact location of emergency and how to enter facility. iv. A separate emergency plan is necessary for each sports field, court, or gymnasium. v. Make sure that each responsible person involved in the activity has be apprised of the emergency plan and that each person knows their responsibilities in the plan. II. Primary Survey a. A primary survey is that portion of the assessment concerned with evaluation of the basic life support mechanisms: AIRWAY, BREATHING, and CIRCULATION. These are referred to as the ABC s of life support. b. With most athletic injuries, a primary survey is completed easily and quickly. Critical life-support mechanisms can be evaluated almost immediately. For example, if an injured athlete is conscious and talking, one can assume that they are breathing and have a pulse. c. Time is of the most importance, so the primary evaluation must be done rapidly and accurately. Unit 4 First Aid 1 draft copy
2 d. During the primary survey, the examiner needs only to talk, feel, and observe. No diagnostic equipment is needed. Inquiries should be brief and pertinent, with no detailed questioning at this time. e. Four diagnostic signs should be observed. i. State of consciousness. ii. Respiration. iii. Skin color. iv. Pulse. f. The examiner must remain calm no matter what the situation may be. A calm attitude instills confidence in the athlete. g. A record of initial observations should be started. h. A thorough understanding of basic life-support procedures is necessary to the performance of a primary survey. i. Airway i. Anything that blocks the passage of air through the windpipe (trachea) into the lungs causes an airway obstruction. ii. The most common cause of airway obstruction is blockage of the opening by the tongue. This may occur when an athlete is unconscious. In this case, the tongue may fall toward the back of the throat and block the airway opening. iii. An obstructed airway is life-threatening and requires immediate attention. iv. Because the tongue is attached to the lower jaw, moving the lower jaw forward will usually lift the tongue away from the back of the throat and open the airway. This may be all that is required for breathing to resume spontaneously. v. The current recommended technique to open the airway is the head-tilt-chin-lift method. This maneuver is accomplished by tilting the head back with one hand and lifting the chin up gently with the other. With the athlete on their back, place the hand closest to the athlete s head on the forehead and apply firm backward pressure. At the same time, place the tips of your fingers under the lower jaw on the bony rim and lift the chin forward. Be careful when compressing the soft tissues under the chin because this could obstruct the airway. The chin should be lifted so that the teeth are almost brought together, however, avoid completely closing the mouth. vi. When a neck injury is suspected, movement of the cervical spine must be avoided. The jaw-thrust method can be used. vii. To relieve an airway obstruction caused by a foreign body, the examiner can use the Heimlich maneuver on a conscious athlete. 1. For the conscious victim, the Heimlich maneuver is applied until he or she is relieved or becomes unconscious. 2. Stand behind the athlete. Place both arms around the waist just above the hips and permit the athlete s head, arms, and upper trunk to hang forward. Unit 4 First Aid 2 draft copy
3 3. Grasp one fist with the other, placing the thumb side of the grasped fist in the center of the abdomen, clear of the rib cage. 4. Sharply and forcefully thrust the fists into the abdomen, inward and upward. Repeat the thrusts until the object is expelled, swallowed, or the athlete becomes unconscious. j. Breathing i. The term apnea refers to any temporary cessation of breathing. An athlete may stop breathing or be in respiratory arrest for a variety of reasons. The most common is airway obstruction. The airway may be obstructed by the tongue or a foreign object as explained above. Swelling in the throat caused by an allergic reaction, or tissue damage caused by a severe blow to the neck can also obstruct the airway. ii. Respiratory arrest may also result from cardiac arrest, poisons, drugs, or drowning. iii. Regardless of the cause, it is extremely important that the rescuer recognize the condition immediately. iv. The first priority is assessment and care of injuries involving an athlete s breathing is to establish an open airway. When the airway is opened, an athlete may begin to breath spontaneously. v. If it does not appear that breathing has begun after opening the airway, put your ear close to the athlete s mouth and nose. Look at the chest for any breathing movements. Listen for any exchange of air. Feel for breathing against your cheek or ear. vi. If the athlete is not breathing, appropriate techniques of artificial breathing must be initiated immediately. k. Circulation i. There are several reasons why an athlete s heart may stop beating, but should it occur, the exact cause is immaterial to the sports medicine professional. Of utmost importance is the recognition of cardiac arrest and the immediate initiation of emergency measures. ii. Circulation is assessed by palpating for a pulse. The carotid artery in the neck is the most commonly used artery to check for a pulse during an emergency situation. This is the main artery in the neck. The carotid artery is normally not obstructed by clothing or equipment and is easily accessible. Position yourself on one side of the athlete and place your index and middle fingers on the windpipe. Slide your fingers gently toward you. Press gently into the soft part of the neck next to the windpipe. The carotid pulse can be felt in the groove. Always feel for the carotid pulse on the side of the neck closest to you. iii. If the athlete does not have a pulse, appropriate emergency techniques of artificial circulation must be initiated immediately. Every sports medicine professional must be certified in Cardiopulmonary Resuscitation (CPR). Unit 4 First Aid 3 draft copy
4 III. IV. CPR Certification a. CPR certification must be done by a certified CPR instructor. Contact the Red Cross, American Heart Association or a local emergency response council or fire department for possible instructors. Secondary Survey a. Upon completing the primary survey and controlling any immediate lifethreatening problems, the secondary survey, which involves a more thorough examination of the athlete is conducted. This examination is a head-to-toe assessment to detect conditions that may not in themselves pose an immediate threat to life, but if left unrecognized and untreated, could become life threatening. b. This secondary survey should be completed before beginning stabilization and transport, if necessary, of the athlete. c. Injuries such as bleeding, spinal injury, and shock are examples of conditions that must be ruled out. i. Bleeding in order to detect bleeding, the examiner should do a quick scan from head to toe, lightly touching every part of the body, periodically checking their hands for blood. This should be done first and take only about 15 seconds. ii. Spinal injuries in order to detect spinal injuries, the examiner should gain a thorough history from the patient, including questions of what happened and how? Do they have neck or back pain? Do they have tingling and numbness in any extremity? Can they wiggle their fingers and toes? The examiner should also palpate the entire spine checking for deformity and tenderness. 1. If the athlete has any neck or back pain, the examiner should instruct the athlete to keep his/her head still and have another person hold the athlete s head still as a reminder. 2. The athlete should be placed on a backboard with a cervical collar on, and be immediately transported to a medical facility. iii. Shock in order to detect if someone is in shock, vital signs should be taken. Nail bed perfusion should be noted as well as the color of their skin and their responsiveness during the history taking process. 1. Pulse a normal pulse rate per minute for adults is between beats per minute and in children from beats per minute. A rapid but weak pulse could indicate shock. 2. Respiration the normal breathing rate per minute is approximately 12 breaths in adults and in children. Shallow breathing may indicate shock. 3. Blood pressure a normal blood pressure for adults is 120/80 mm Hg. A lowered blood pressure could indicate shock. Unit 4 First Aid 4 draft copy
5 4. Body temperature a normal body temperature is 98.6 F. Temperature is measured with a thermometer. Changes in body temperature can be reflected in the skin. Cool, clammy and pale skin could indicate shock. 5. Pupils the pupils are extremely sensitive to situations affecting the nervous system. If one or both pupils are dilated, the athlete may be experiencing shock. The pupils response to light should also be noted. d. A total body survey (TBS) should then be conducted using the following format. i. The examiner should palpate the entire body noting any tenderness, deformity, or swelling. 1. Entire skull and facial bones. 2. Pupils equal size and normal reaction to light (head injury). 3. Fluid coming from the ears or nose (skull fracture). 4. Ask them to bite down with their teeth, check for pain and normal alignment (jaw fracture). 5. Cervical spine. 6. Clavicles, one at a time. 7. Sternum push down with side of hand. 8. Ribs push down and in from the sides. 9. Arms and hands one at a time, have athlete squeeze your fingers at the same time (neurological check). 10. Move one arm (if not injured) over the chest to be able to palpate the thoracic and lumbar spine. 11. Push on all four quadrants of the stomach (internal bleeding). 12. Pelvis push down and in (fracture). 13. Palpate each leg and foot separately; have the athlete push down and up with their feet against resistance (neurological check). 14. Take blood pressure, respiration rate, and pulse rate. ii. During the total body survey, the examiner should be gathering additional information about the injury and the athlete. V. After the TBS, the examiner can then do a more thorough assessment of the major complaint areas through a musculoskeletal evaluation (HIPS). Musculoskeletal Evaluation a. A logical process must be used to evaluate accurately the extent of musculoskeletal injuries. It is this part of the survey that usually comprises the largest portion of the total athletic injury assessment procedure. An ordered sequence of procedures is used to assess the nature, site, and severity of an athletic injury. b. When an injury occurs, early and accurate assessment is essential in developing an effective treatment and rehabilitation program. c. The importance of using a detailed and properly sequenced checklist in the assessment procedure cannot be overemphasized. By following a Unit 4 First Aid 5 draft copy
6 consistent pattern in your evaluation procedures, you are less likely to forget a procedure or miss an important detail. d. This evaluation can be divided into four basic steps. These can be easily remembered by the acronym HIPS, which stands for HISTORY, INSPECTION, PALPATION, and SPECIAL TESTS. e. Each step is important and should be carried out thoroughly and efficiently to accurately assess an athletic injury. Not all of the procedures discussed under each step of the HIPS evaluation will be carried out with each athletic injury. The nature, type, and severity of the injury will determine the evaluation techniques to be used. f. HISTORY i. Obtaining an accurate history of an injury is one of the most important steps in the secondary survey portion of the total athletic injury assessment process. Taking a history involves finding out as much information as possible about the actual injury and the circumstances surrounding its occurrence. This is accomplished by talking with the injured athlete or others who have observed the injury. Information gained in a thorough history can provide important clues in determining which structures may be injured and which assessment techniques will be appropriate as the examination continues. ii. Knowledge of the mechanism of common injuries is extremely important in determining the possible injuries of athletes. iii. When obtaining a history, the examiner should: 1. Be calm and reassuring. 2. Express questions that are simple and not leading. 3. Listen carefully to the athlete s complaints. iv. The main purpose of the history step is to find out as much information as possible about an injury and the circumstances surrounding its occurrence. v. Examples of questions: 1. Chief complaint and present problems? 2. How did the injury happen? Describe the mechanism of injury in detail. 3. If pain is present, its location, character, duration, variation, aggravation, intensity, radiation, and course? a. If possible, point to the painful area with one finger. b. Nerve pain tends to be sharp and/or burning. c. Bone pain is localized and piercing. d. Muscle pain is often dull, aching and referred to another area. e. Pain that subsides during activity usually indicates a chronic inflammation. f. Pain that increases in a joint throughout the day indicates a progressive increase in swelling. Unit 4 First Aid 6 draft copy
7 g. Is the pain increased or decreased by specific activities or stresses? 4. Has the problem occurred before? If so, when, and how was it treated? 5. How long have the symptoms been apparent? 6. Joint responses giving way, instability? 7. Any sounds at the time of injury? a. Sounds such as a snap, crack or pop at the time of injury often indicate bone breakage. b. Areas of the body that have abnormal amounts of fluid may produce sloshing sounds when gently palpated or moved. g. INSPECTION i. Along with gaining a knowledge and understanding of the athlete s major complaint from a history, a general inspection is also performed, often at the same time the history is taken. ii. This step is purely observational! iii. Look for any obvious bleeding, deformity, swelling, discoloration, or other signs of injury. iv. Note general body alignment and posture of the athlete. Is the athlete holding a body part or grasping some body area? v. If the athlete is moving around, note their functional abilities. Is the athlete using the injured part or protecting it? Are they limping? vi. Some athletes try to disguise or minimize the extent of their injury. Observing the athlete s face and eyes as they describe the injury may give further clues as to the extent of the pain. More pain may be reflected in the athlete s face than they may be willing to admit. vii. When inspecting an injury, clothing and equipment that may obscure the area should be removed. Consider the athlete s modesty in removing clothing and equipment. viii. Always compare the injured body part to the contralateral uninjured part and note any obvious differences. You must be aware of any pre-existing abnormalities in the uninjured body part cause by such things as congenital conditions or previous injuries. h. PALPATION i. Palpation means to touch and feel the injured area. After the history and observation steps, you can gain additional physical information concerning the injury by carefully palpating the affected body area. ii. The three types of structures that should be systematically palpated are Bones, Muscles, and Soft Tissue. iii. There are several important points to remember as you palpate an injured athlete: 1. Palpate in a tender manner to avoid unnecessary pain. If you cause the athlete unnecessary pain, they may become tense and uncooperative. Unit 4 First Aid 7 draft copy
8 2. To accurately palpate an injured area it should be as relaxed as possible. 3. The intensity or pressure used with each palpation maneuver can be increased depending upon the athlete s tolerance level and the severity of the injury. 4. It is good practice to begin palpating away from the injury site to encourage the athlete s cooperation and confidence. 5. It is important that you visualize the structures that are under your fingers as you palpate. Are you feeling approximately where ligaments, muscles and other structures should be? 6. Remember to compare the contralateral areas. iv. Pain is one of the most obvious and consistent symptoms of injury. It is especially important to locate areas that are most painful to touch. These are called areas of point tenderness and are usually found at the site of injury. v. Another physical sign that can be recognized by palpation is swelling. Swelling may be localized at the injury site or diffused over a larger area. The amount of swelling is usually related to the severity of injury. However, there are cases in which serious injuries produce very limited swelling and minor injuries cause severe and extensive swelling. vi. Additional information gained during palpation may be related to the temperature of the skin. Normal skin is moderately warm and dry. In palpating the site of an injury, any indication of an increase in skin temperature would suggest the occurrence of an inflammatory process. A decrease in skin temperature may be felt in areas of inadequate circulation. vii. Deformity is another physical sign that may be discovered during palpation. The cause may be a fracture, dislocation, or the tearing of soft tissue. i. SPECIAL TESTS i. The special tests section of the HIPS evaluation includes four areas: Range of Motion, Stress Tests, Neurological, and Circulatory. ii. Range of Motion three types of range of motion should be assessed: Active, Passive, and Resistive. 1. Active movement is movement that is performed solely by the patient and indicates three factors an ability and willingness to execute certain movements, muscular power, and range of active movement. Active movement may be normal, limited, or excessive. To initiate this type of movement, the athlete is asked to move the injured part through as full a range of motion as possible, and in all the ranges of motion at that joint. Note which movements, if any, cause pain and the amount and quality of pain that Unit 4 First Aid 8 draft copy
9 results. Note any restriction of limitation in the active motion. Compare the active range of motion to the uninjured side. 2. Passive movement is movement that is performed completely by the examiner. With the athlete relaxed, the body part is moved through as full a range of motion as possible. Passive movements are used to evaluate the integrity of the non-contractile tissues at the joint. As the part is moved, the examiner determines what is felt at the end of the movement or end feel. 3. Resistive movements are used to determine the status of a particular muscle or muscle group. The athlete is asked to contract the part as much as possible, while the examiner provides resistance. Low initial resistance against movements is gradually increased depending on the athlete s tolerance. Note the strength and site of pain at any point throughout the resisted range of motion. The following are some of the findings that resistive range of motion can provide: a. Weak and Painless possible third degree strain. b. Weak and Painful possible fracture at a joint site. c. Strong and Painful possible tear of a muscle or tendon. d. Strong and Pain Free no muscle injury. iii. Stress Tests iv. Special stress tests have been designed for almost every body region as a means of determining specific injuries. These stress tests are commonly used to determine ligament stability, muscle imbalance, tightness of specific structures, joint function, and integrity of structures. v. Neurological Exam 1. The neurological examination consists of reflex testing and sensation testing. 2. A deep tendon reflex is an involuntary contraction of a muscle in response to a tap on its tendon. Testing a reflex can provide an indication of the state of the nerve supplying that reflex. When evaluating reflexes, always test and compare each reflex bilaterally. Asymmetry between bilateral reflexes may indicate a loss or abnormality of nerve conduction and can be diminished, lost, or excessive. Common reflexes that should be checked are Biceps, Triceps, Patellar, and Achilles. 3. Testing for altered sensations is also an important part of the neurological exam. The examiner should run their hand or fingers over the skin of the injured area as well as the corresponding area on the uninjured side. Does the athlete feel any difference in sensation between the two sides? To Unit 4 First Aid 9 draft copy
10 test for pain, apply the sharp and dull points of a pin to the skin and note whether the athlete correctly perceives the stimulus. Abnormal responses to sensory testing include sensations that are decreased, absent, or increased. vi. Circulatory Exam 1. The circulatory exam includes three areas: Pulse, Blood Pressure, and Nail Bed Perfusion. 2. A pulse is defined as the alternate expansion and recoil of an artery caused by the intermittent ejection of blood from the heart. The pulse can be felt at numerous arteries throughout the body. Most commonly a pulse is taken at the carotid artery, brachial artery, radial artery, femoral artery, and at the dorsipedal site. It is important to take a pulse distal to the injury to determine if the extremity has sufficient circulation. If no pulse is found distal to a severe injury, a medical emergency exists. A normal adult pulse is beats per minute. 3. The athlete s blood pressure should be taken during the assessment process. Remember that a normal adult blood pressure is 120/80 mm Hg. j. Nail bed perfusion can also help to indicate circulatory problems. Squeezing the finger or toe nail bed distal to the injury site will blanch the nail (turn it white), and on release there should be a rapid return of a pink color. k. Decisions Made from a HIPS evaluation i. The examiner can make any of the following decisions after completing a thorough musculoskeletal examination: 1. The seriousness of the injury. 2. The type of first aid and immobilization. 3. Whether or not the injury warrants referral to a physician for further assessment. 4. The appropriate follow-through and treatment for this injury. l. Additional Information i. Injuries that are serious or need physician care should be referred for additional medical attention. If the examiner is unsure of the injury, the athlete should be referred for a physician s evaluation. ii. The physician is legally responsible for the diagnosis and course of treatment of an injured athlete. He or she may have to acquire additional information to make a final assessment. iii. X-rays an x-ray examination assists the physician in determining fractures and dislocations, or any other bone abnormality that may be present. iv. Arthroscope the fiber optic arthroscope is commonly used by orthopedic surgeons to view a joint and perform minor surgical procedures. The arthroscope is minimally invasive, and requires anesthesia and a small incision. Unit 4 First Aid 10 draft copy
11 v. Magnetic Resonance Imaging (MRI) MRI surrounds the body with powerful electromagnets, creating clear images of both soft tissue and bones, for accurate, non-invasive diagnosis of injuries and diseases. VI. Management of Acute Injuries a. The role the person providing first aid includes the prevention of further injury, reduction of pain, and stabilization of the injury. Also of importance is the control of bleeding and management of swelling, splinting, and handling and transportation of the injured athlete. b. Of major importance with musculoskeletal injuries in the initial control of bleeding, swelling, muscle spasm and pain. The acronym for this process is R-I-C-E (Rest, Ice, Compression, and Elevation). i. Rest 1. Rest is essential for many injuries. This can be achieved by immobilization of the injured body part, or the use of a cane or crutches. 2. Immobilization of an injury for the first 2-3 days after injury helps to ensure the healing of the wound without complication. Movement too early may increase bleeding, and possibly prolong recovery. ii. Ice 1. Cold, primarily ice in various forms is an effective first aid method. Cold reduces pain and muscle spasms. Cold is a stronger stimulus than pain from many minor injuries; therefore, the sensation of cold on an injury will override the feeling of pain. 2. Cold application also decreases swelling that occurs following an injury because it slows circulation by constricting blood vessels. 3. Prolonged application of cold can however, cause tissue damage. 4. Cold applied to a healthy athlete will feel uncomfortable. For best results, ice should be applied over a towel or other covering on the skin. Frostbite is a danger when cold is applied. A good rule of thumb is to apply a cold pack to a recent injury for a 20-minute period and repeat every 1-2 hours throughout the waking day. 5. Depending on the severity and site of the injury, cold may be applied intermittently for hours. If in doubt about the severity of any injury, it is best to extend the time RICE is applied. iii. Compression 1. Placing external pressure on an injury assists in decreasing blood flow to the site of the injury. Compression assists the Unit 4 First Aid 11 draft copy
12 body s healing process by reducing circulation to the area during the acute injury stage. 2. A compression wrap can also help support injured tissues and provide comfort to the athlete. Many types of compression are available. 3. An elastic wrap (Ace bandage) can provide the appropriate compression as can horseshoe pads combined with adhesive tape. Elastic wraps come in various sizes ranging from 2 to 6. The smaller the body part to be wrapped, the smaller and shorter the wrap required. 4. A compression elastic wrap should always be started distally, and should be wrapped toward the heart. The wrap should overlap itself by about _ its diameter. No gaps should be left as these would serve as an escape for swelling. The wrap should be stretched to about 70% of its maximum length to give adequate compression. Excessive pressure will not minimize swelling and will probably slow the healing process. 5. After any wrapping or taping, the athlete should be checked for comfort as well as signs of impaired circulation (numbness, tingling, discoloration, or loss of pulse). iv. Although cold is applied intermittently, compression should be maintained throughout the day. v. Elevation 1. Along with cold and compression, elevation reduces internal bleeding. By elevating the affected body part above the level of the heart, bleeding is reduced, and venous return is encouraged, further reducing swelling. Care must be taken that the elevated part is in a secure, supported and comfortable position. 2. Many studies now agree that elevation may be the best method of reducing swelling, even more than ice or compression. 3. Remember that for elevation to be effective, the injured body part must be above the level of the heart. vi. RICE Schedule 1. Evaluate the extent and severity of the injury. 2. Apply ice to the injury. 3. Hold ice pack firmly against the injury site with an elastic wrap. 4. Elevate the injured body part (when secure and stable) above the level of the heart. 5. After 20 minutes, remove the ice pack. 6. Reapply compression to the injured part. 7. Elevate the injured body part. Unit 4 First Aid 12 draft copy
13 8. Reapply the ice pack in 1 to 2 hours, and depending on the degree of injury, continue this rotation until injury resolution has taken place and healing has begun. 9. Keep the injured body part elevated above the level of the heart. VII. Emergency Splinting a. Sometimes it is difficult to tell whether an injury is a fracture, dislocation, sprain, or strain. Since you cannot always be sure which of these an injured athlete may have, always care for it as a fracture. When in doubt, splint. b. Any suspected fracture should always be splinted before the athlete is moved. Transporting a person with a fracture without proper immobilization can result in increased injury to the athlete, and shock. It is possible that a mishandled fracture could cause death. c. Splinting is the process of immobilizing a body part. Any material that can immobilize a fractured bone can be used (rolled up newspaper, magazines, and pieces of wood). d. The purposes of splinting are: i. To immobilize a possibly fractured part of the body. ii. To lessen pain. iii. To prevent further damage to soft tissues. iv. To reduce the risk of serious bleeding. v. To reduce the possibility of loss of circulation in the injured part. vi. To prevent closed fractures from becoming open ones. e. The basic principles of splinting are: i. Splint only if you can do it without causing more pain and discomfort to the victim. ii. Splint an injury in the position you find it. iii. Apply the splint so that it immobilizes the fractured bone as well as the joints above and below the fracture. iv. Check the circulation before and after splinting. v. If at all possible, do not move the athlete until they have been splinted. f. If there are no splinting supplies available, splint the broken part to another part of the body. For example, a broken arm can be splinted to the chest, and a fractured leg can be splinted to the other, uninjured leg. g. Fractures of the ankle or leg require immobilization of the foot and knee. Any fracture involving the knee, thigh, or hip needs splinting of all the lower limb joints and one side of the trunk. h. Fractures around the shoulder complex are immobilized by a sling and swathe bandage, with the upper limb bound to the body securely. Upper arm and elbow fractures must be splinted, with immobilization effected in a straight-arm position. Lower arm and wrist fractures should be splinted in a position of forearm flexion and should be supported by a sling. Hand Unit 4 First Aid 13 draft copy
14 and finger dislocations and fractures should be splinted with tongue depressors, gauze rolls, or aluminum splints. i. Injury of the head, neck, and back are serious and difficult to care for. Once a head, neck, and/or back injury has been recognized, an ambulance should be immediately summoned. Primary emergency care involves maintaining normal breathing, treating for shock, and keeping the athlete quiet and in the position found until medical assistance arrives. Any movement of the athlete should include a backboard. This stabilization must be maintained throughout transportation, and through any hospital procedures, until the injury is cleared. VIII. Crutches a. When an athlete has a lower limb injury, weight bearing may be contraindicated. Situations of this type call for the use of a crutch or a cane. b. Very often, an athlete is assigned one of these aids without proper fitting or instruction in their use. An improper fit and usage can place abnormal stresses on various body parts. Constant pressure of the body weight on the crutch s axillary pads can be painful. This pressure on the nerves and blood vessels in the area can lead to temporary or even permanent numbness in the hands. Faulty mechanics in the use of crutches or canes could produce chronic low back and/or hip strain. c. For a correct fit the athlete should wear low-heeled shoes and stand with good posture and the feet close together. d. The crutch length is determined by first placing the tip 4 inches from the outer margin of the shoe and 2 inches in front of the shoe. The crutch can be adjusted to the athlete s height. e. The underarm crutch brace should be positioned 1 inch (two-finger widths) below the anterior folds of the axilla (armpit). Next, the hand brace is adjusted so that it is even with the athlete s hand and the elbow is flexed at approximately a degree angle. f. Many elements of crutch walking correspond with walking. The technique commonly used in sports injuries is the tripod method. In this method, the athlete swings through the crutches without making any surface contact with the injured limbs or by partially bearing weight with the injured limb. g. The following crutch walking sequence should be used: i. The athlete stands on one foot with the affected foot completely elevated or partially bearing weight. ii. Placing the crutch tips inches ahead of the feet, the athlete leans forward, straightens the elbows, pulls the upper crosspiece firmly against the side of the chest, and swings or steps between the stationary crutches. iii. After moving through, the athlete recovers the crutches and again places the tips forward. Unit 4 First Aid 14 draft copy
15 h. Once the athlete is able to move effectively on a level surface, negotiating stairs should be taught. As with level crutch walking, a tripod is maintained on stairs. i. In going upstairs, the unaffected support leg moves up one step while the body weight is supported by the hands. The full weight of the body is transferred to the support leg, followed by moving the crutch tips and affected leg to the step. ii. In going downstairs, the crutch tips and the affected leg move down one step followed by the support leg. If a handrail is available, both crutches can be held by the outside hand, and a similar pattern is followed as with the crutch on each side. IX. Head and Neck Injuries a. The following steps should be followed when stabilizing an athlete with a head, neck, and/or back injury: i. Establish whether the athlete is breathing and has a pulse. ii. Secure a spine board for transportation of the athlete. iii. Place all extremities in axial alignment. iv. Rolling the athlete over (if they are lying prone) requires four to five persons. The neck must be stabilized and must not be moved from its original position. Each person is responsible for one of the athlete s body segments. v. Place the spine board close to the side of the athlete. vi. The athlete should be rolled on to the board as one unit. vii. On the board, the athlete s head and neck should continue to be stabilized. viii. Do not remove the helmet (if wearing one) but the facemask can be cut away for possible CPR. ix. Secure the athlete to the spine board. x. If the athlete is face up, the athlete should be lifted straight up as a unit while the spine board is slid underneath. The athlete is slowly lowered straight down onto the board. The head and neck should be stabilized throughout the entire maneuver. X. Control of Bleeding a. Bleeding or hemorrhage refers to the loss of blood from arteries, capillaries or veins. Bleeding may be internal or external. Loss of blood may initially cause weakness and progress to shock and death if the bleeding is not controlled. b. There are three types of bleeding: i. Arterial loss of blood from an artery which carries oxygenated blood from the heart through the body. The blood spurts with each heartbeat and is bright red. Arterial bleeding is usually severe and hard to control and needs immediate attention. ii. Venous loss of blood from a vein which carries deoxygenated blood from the body back to the heart. It has a steady flow which Unit 4 First Aid 15 draft copy
16 can be heavy and the color is dark red. Venous bleeding is easier to control than arterial bleeding. iii. Capillary loss of blood from capillaries which are the smallest blood vessels. The blood flow is usually slow and steady. The threat of infection is greater than with arterial or venous bleeding. c. The average adult has 6 liters of blood circulating through their body at any one time. The acute loss of 10% of the circulatory blood volume (600 ml) may be critical. d. External bleeding is bleeding that can be seen coming from a wound. Some examples are bleeding from abrasions, incisions, lacerations, puncture wounds, amputations, open fractures, or nosebleeds. e. There are several methods for controlling bleeding. In most cases bleeding stops naturally after 6-10 minutes because of the body s clotting mechanism. However, sometimes the damaged vessels may be too large that clots cannot block them. f. The purposes of first aid for external bleeding are: i. Stop the bleeding. ii. Prevent infection. iii. Prevent shock. g. To control bleeding: i. Apply direct, local pressure on the wound with a dressing. Pressure stops the physical flow of blood and permits normal blood clotting to occur. A dressing is a clean covering placed over the wound that protects it and helps control the bleeding by absorbing the blood and allowing it to clot. Once you put a dressing on a wound, do not remove it. If bleeding continues, add new dressings on top of the old ones. The less a bleeding wound is disturbed, the better the chances of stopping the bleeding. ii. If a fracture is not suspected, elevate the wound above the level of the heart and continue to apply direct pressure. iii. If the bleeding still has not stopped, the next step is to apply pressure at a pressure point. Pressure points are over the major pulse points of the body. Because most wounds are supplied by more than one major artery, compression of a major artery rarely stops bleeding completely from a wound distal to the artery. Pressure point control can aid temporarily in the control of severe bleeding, but it should not be the primary or sole method of bleeding control. Continue to apply direct pressure and elevate the wound. iv. The final step to control bleeding is to apply a pressure bandage. A bandage is used to hold a dressing in place, restrain movement, and help stop bleeding. Apply pressure while wrapping the bandage over the dressing to keep pressure on the wound and slow the bleeding. Take the pulse and examine the fingertips or toes in the injured limb after wrapping the bandage to make sure the bandage is not too tight that it slows or stops circulation. Unit 4 First Aid 16 draft copy
17 v. The use of a tourniquet to stop bleeding is rarely necessary. Tourniquets, if they are used improperly, can crush the soft tissue of an injured extremity and cause permanent damage to nerves and blood vessels. Application of a tourniquet will not be discussed further. h. Infection can develop within hours or days of any injury. i. The signs and symptoms of infection are: 1. Pain or tenderness at the wound. 2. Redness, heat, or swelling at the wound. 3. Pus beneath the skin or in the wound. 4. Red streaks leading away from the wound. ii. An infection can cause a person to feel ill. iii. If any of these signs or symptoms develops, the victim should seek immediate medical help. iv. To reduce the threat of infection, wear gloves or wash your hands before caring for a wound. Wash minor wounds that are not bleeding severely with soap and water before applying the dressing. Do not try to clean major wounds that are bleeding severely, since this will cause additional bleeding. i. A nosebleed is a common injury in sports. i. A person may lose enough blood in a nosebleed to cause shock. ii. The blood seen coming from the nose may represent only a small amount of the total loss, since much blood passes down the throat into the stomach as the athlete swallows. A person who swallows a large amount of blood may become nauseated and may vomit. iii. The following techniques are successful in stopping most nosebleeds: 1. Apply pressure by pinching the nostrils together. 2. Keep the athlete in a sitting position with the head tilted forward whenever possible so that the blood trickling down the back of the throat will not be aspirated into the lungs. 3. Keep the athlete quiet. Anxiety will tend to increase the blood pressure and the nosebleed will worsen. 4. Apply ice over the nose. Local cooling is helpful in controlling bleeding. iv. If these measures fail to control the nosebleed, the athlete should be transported promptly to the emergency room. An athlete who suffers from frequent nosebleeds should be evaluated by a physician to determine the cause of the nosebleeds so that appropriate treatment may be initiated. j. Although, not usually visible, internal bleeding can be very serious. The athlete with severe internal bleeding may go into shock before the loss of blood is realized. A bruise or contusion indicates bleeding into the soft tissues and may be seen after a slight or severe injury. i. Internal bleeding can result from crushing injuries, punctures, injuries from blunt objects, tears in internal organs and blood Unit 4 First Aid 17 draft copy
18 vessels, bruised tissues, and fractured bones. If the victim is not properly checked, internal bleeding may go unnoticed. ii. Signs and symptoms of internal bleeding include: 1. Bruised, swollen, or rigid abdomen. 2. Bruises on chest or signs of fractured ribs. 3. Blood in vomit. 4. Wounds that have penetrated the chest or abdomen. 5. Fractures of the pelvis. 6. Abnormal pulse and difficult breathing. 7. Cool, moist skin. iii. There is little one can do in the field to control internal bleeding. If the sports medicine professional suspects internal bleeding based on the mechanism of injury or the athlete s signs and symptoms, basic life support should be provided and the athlete should be transported to the emergency room immediately. XI. Shock a. The first hour after a severe injury is the most important. A major problem occurring within this time frame is shock. Once shock reaches a certain dangerous level, the victim cannot be saved. b. Shock is the failure of the cardiovascular system to keep adequate blood circulating to the vital organs of the body (such as the brain, heart, and lungs). Shock develops as a result of the body s attempts to correct damage from severe injury. c. Lack of adequate blood flow to the brain and the spinal cord for more than 4-6 minutes will result in permanent damage. Permanent damage to the kidneys will result after 45 minutes. The heart requires constant blood flow or it will not function properly. No part of the body can exist without adequate blood flow for an indefinite period of time. d. Shock can be caused by bleeding, poisoning, insect bites and stings, snakebites, electrical shock, burns, severe injuries, psychological trauma, heart attack, and other medical conditions. e. The following signs and symptoms are common to all forms of shock: i. Nausea and vomiting. ii. Restlessness and anxiety. iii. Weak, rapid pulse. iv. Low blood pressure (systolic pressure is usually below 90 mm Hg.) v. Cold, wet, clammy skin. vi. Profuse sweating. vii. Paleness that changes to cyanosis. viii. Shallow, labored, rapid, or irregular gasping respirations. ix. Dull, lusterless eyes with dilated pupils. x. Drowsiness and sluggishness. xi. Loss of consciousness in cases of rapidly developing or severe shock. Unit 4 First Aid 18 draft copy
19 f. Any athlete who exhibits any of the signs or symptoms of shock should be immediately transported to a medical facility. While in the process of arranging transportation, the following measures should be taken: i. Monitor airway, breathing, and circulation. ii. Place the athlete on their back and elevate the feet and legs 8-12 inches (if no head/neck injuries or leg fractures are suspected). iii. If you suspect the athlete has a head/neck injury, keep them lying flat and wait for EMS. iv. Prevent loss of body heat by putting blankets over and under the person. Do not overheat the athlete. It is better than the athlete be cool than too warm. v. Accurately record the athlete s pulse, blood pressure, and other vital signs. Maintain a record of them at 5-minute intervals. vi. Do not give the individual anything to eat or drink. XII. Seizures a. Seizures are very common occurrences, but they are not completely understood. When seizures recur, and there are no underlying causes that can be treated directly, a person is said to have epilepsy. Epilepsy refers to any of the disorders caused by abnormal focus of electrical activity in the brain that produces seizures. b. A seizure or convulsion is characterized by generalized, uncoordinated muscular activity and changes in the level of consciousness which last for variable periods of time. Seizures can vary in form from severe convulsions to simply blacking out for a few seconds. A state of sleepiness or unconsciousness follows the seizure. c. Not all seizures are caused by epilepsy. They may occur as a result of a recent or old brain injury, a brain tumor, infection, fever, diabetes, or simply a genetic predisposition. d. Seizures are generally classified according to the degree and location of abnormal activity in the brain. e. Some individuals have an aura (sensation) before the onset of a seizure. Auras can be sound and vision hallucinations, a strange taste in the mouth, abdominal pain, numbness, or a sense of urgency to move to safety. f. A person having a seizure cannot control it. g. The first important step in the management of a seizure is to protect the athlete from accidentally inflicting self-injury. i. The athlete should be helped to lie down on the ground away from danger. ii. The athlete s head, arms, and legs should be protected, but not rigidly restrained. iii. Clothing should be loosened. iv. Nothing should be forced into the athlete s mouth. h. Following a seizure, the muscles relax. Check the athlete s airway, breathing, and circulation. A person recovering from a seizure is likely to Unit 4 First Aid 19 draft copy
20 be drowsy and disoriented. They need rest and reassurance. Stay with them until they are fully conscious and aware of the surroundings. Also look for any injuries that may have occurred during the seizures. i. If you know the athlete has epilepsy, it is usually not necessary to call EMS unless: i. The seizure lasts longer than a few minutes. ii. Another seizure begins soon after the first. iii. The athlete does not regain consciousness after the jerking movements have stopped. j. EMS should be called when someone having a seizure also: i. Is pregnant. ii. Carries identification as a diabetic. iii. Appears to be injured. iv. Is in the water and has swallowed large amounts of water. k. Epileptic s participation in sports has been controversial over the years. Most experts now agree that epileptics should not be restricted from participating in physical exercise. When epileptics do participate in sports, proper seizure control is mandatory, as is supervision during sports participation. The responsibility of determining whether an epileptic child can participate in sports is a joint responsibility of parents, physician and child. XIII. Other Soft Tissue Injuries a. Blisters a blister usually forms when heat generated by the skin rubbing against a hard or rough surface causes the layers of skin to separate. Fluid then accumulates between the layers. i. Those athletes who use their hands extensively to use implements such as a bat, racket, club, or bar are prone to blisters. Feet are also prone to blistering when they are forced to slide back and forth within a shoe that is making sudden changes of position. ii. The athlete will experience feeling a hot spot, a sharp, burning sensation as the blister is formed. Blister prevention is of the most importance. iii. Once developed, blisters can be a real problem for the athlete. Leave the blister intact. If the blister is already open or torn, keep the blister clean to avoid infection. A sterile dressing should be placed over the blister. b. Contusions a contusion is the bruising and destruction of soft tissue cells as the result of a direct blow. Blood vessels are broken, causing internal bleeding. As a result of the bleeding and leakage of cellular fluids, swelling results. Discoloration of the skin (a bruise) often accompanies the contusion. i. Untreated and unprotected contusions can lead to a more serious condition. ii. Treatment includes cold, compression, elevation, and the use of padding for protection. Unit 4 First Aid 20 draft copy
21 c. Abrasions an abrasion is the scrapping away of the outer layers of the skin. Bleeding is limited due to the rupture of small veins and capillaries. Infection can occur. i. Initial management includes cleaning the wound and keeping it clean and dry. d. Lacerations a laceration is a jagged, irregular cut or tear in the soft tissues. The bleeding should be controlled and the wound should be cleaned. Apply a clean dressing and watch for signs of infection. XIV. Muscle, Tendon, and Ligament Injuries a. Strains a strain is a stretch, tear, or rip in a muscle or tendon. Most often a strain is produced by an abnormal muscular contraction. i. A strain may range from a minute separation of connective tissue and muscle fibers to a complete tendinous avulsion or muscle rupture. ii. Capillary and blood vessel hemorrhaging will result. iii. Strains are graded as first, second, or third degree injuries. 1. The first-degree strain is accompanied by local pain, which is increased by tension on the muscle, and a minor loss of strength. There is mild swelling, ecchymosis and local tenderness. 2. The second-degree strain is similar to a first-degree but has moderate signs and symptoms and impaired muscle function. 3. A third-degree strain has signs and symptoms that are severe, with a loss of muscle function and commonly a palpable defect in the muscle. iv. The muscles that have the highest incidence of strains in sports are the hamstrings group, gastrocnemius, quadriceps group, hip flexors, hip adductor group, spinalis group of the back, deltoid, and rotator cuff group of the shoulder. b. Tendinitis gradual onset of diffuse tenderness because of repeated micro-traumas and degenerative changes. Obvious signs of tendinitis are swelling and pain that move with the tendon. c. Sprains one of the most common and disabling injuries seen in sports. i. A sprain results from a traumatic twisting that results in stretching or total tearing of the stabilizing ligaments. ii. Sprains are also classified in three degrees of severity. 1. A first-degree sprain is characterized by some pain, minimum loss of function, mild point tenderness, little or no swelling, and no abnormal motion when tested. 2. With a second-degree sprain, there is pain, moderate loss of function, swelling, and in some cases, slight to moderate instability. 3. A third-degree or severe sprain is very painful, with major loss of function, marked instability, tenderness, and swelling. Unit 4 First Aid 21 draft copy
22 XV. Heat Illnesses a. High temperatures and elevated humidity can negatively impact athletic performance, adversely affect health, and even threaten life. While environmental heat problems most often strike football players, all athletes are susceptible. b. Exercise generates heat, which the body must dissipate. If too much heat is retained by the body, cells will literally cook and the athlete can die. The body cools itself mainly through the sweating mechanism; heat is carried away from the body as perspiration evaporates. i. There are approximately 2 million sweat glands in the human body. ii. Sweat production increases sharply with increasing temperature and may result in the loss of 2-8 liters of water in a 24-hour period. c. This cooling process can be interrupted in two ways: i. The humidity can be so high that sweat does not evaporate ii. The thermoregulatory system of the athlete can be disrupted, causing sweating to cease. d. It is important to prevent heat-related problems. This can be done by prehydration and re-hydration. Heavy fluid intake before, during, and after practices and games will help insure that athletes function effectively and safely. e. Aside from skin disorders such as sunburn, three specific heat illnesses or syndromes can result from thermal exposure. Each is normally caused by the same set of circumstances strenuous activity in a combination of hot and humid weather. i. Although the cause of these heat-related conditions is the same, each represents a different bodily reaction to excessive heat, with their own signs and symptoms and treatment procedures. ii. It is important to remember that heat cramps and heat exhaustion can lead to heat stroke. This is especially true when working with athletes. Athletes are more likely to continue working out or exercising even though symptoms may be developing. iii. Athletes in a sport such as football are required to wear heavy protective equipment and uniforms that cover much of the body and add to the problem of heat dissipation. iv. Athletes are also engaged in strenuous activity and may even be limited in the number of breaks, availability of water, and the intensity of the exercise sessions. All of these factors are important to the development of heat-related illnesses. v. Free intake of fluid during games and practice sessions should be encouraged, but large amounts at any one time should be avoided. f. Heat cramps i. Heat cramps are the least serious of the three heat illnesses. These cramps are painful spasms of skeletal muscles. Unit 4 First Aid 22 draft copy
23 ii. Heat cramps result from a fluid volume problem and can normally be prevented by providing unlimited amounts of water to athletes throughout activity in hot weather. iii. When heat cramps do occur, they normally accompany strenuous physical activity and profuse sweating in hot weather. iv. The most common muscles involved are the calf muscles or abdominal muscles, but any of the voluntary muscles can be affected. Heat cramps may be mild, with slight cramping, or they may be severe and incapacitating, with intense pain. v. Athletes suffering heat cramps are normally alert and oriented to their surroundings. The skin will be wet and warm as a result of excessive sweating. The body temperature, pulse, and respiratory rate should be normal or slightly elevated. vi. In most cases, heat cramps are not a serious problem and can be relived by slowly stretching the contracted muscle. The athlete should be encouraged to drink liquids. Many times the athlete will resume activity after alleviation of the muscle spasms, however, a severe episode of heat cramps may require the athlete to avoid further exertion for a longer period of time, possibly hours. vii. Conditioning and acclimatization to the heat also help reduce the incidence of heat cramps. viii. Should heat cramps frequently recur in the same athlete, additional assessment of specific causes is appropriate and medical referral may be necessary. Remember, athletes who suffer heat cramps should be closely observed as this condition may precipitate heat exhaustion or heat stroke. g. Heat exhaustion i. Heat exhaustion is the most common condition caused by exertion in hot weather. It is also known as heat prostration. ii. Heat exhaustion is characterized by profuse sweating, which makes the skin wet, cool, and clammy. The skin may appear pale or gray. The athlete also experiences a headache, weakness, dizziness, fatigue, nausea, alteration of consciousness, and possibly a loss of consciousness. iii. Heat exhaustion is normally not life threatening, but proper medical care is required. The athlete should be taken out of the hot environment and should lie on their back with the feet elevated. Remove as much equipment and uniform as possible. The body should be cooled by sponging or toweling the athlete with cool water. iv. If the athlete is conscious, allow them to drink cool fluids. The athlete should feel better in a short period of time. If symptoms persists or worsen, the athlete should be transported to a medical facility. v. Athletes suffering from heat exhaustion should be withheld from further activity for the remainder of that day and closely observed. Unit 4 First Aid 23 draft copy
24 h. Heat stroke i. Heat stroke is the least common of the heat-related illnesses, but is the most serious. ii. The body s sweating mechanism is shut off to conserve depleted fluid levels. The body temperature then rises rapidly to dangerous and possibly fatal levels. The body temperature may go over 106 F. iii. Heat stroke may develop suddenly or progress from heat cramps and/or heat exhaustion. iv. Heat stroke is a severe medical emergency. This condition must be recognized and treated immediately. v. Heat stroke is characterized by hot, dry skin and a rising temperature. The athlete s skin is reddened or flushed. The athlete is irritable, aggressive, emotionally unstable, hysterical, apathetic, and disoriented. As the temperature rises, the pulse becomes very rapid and strong and the blood pressure falls. Initially the athlete may experience headache, dizziness, and weakness, which are often followed by convulsions and unconsciousness. The athlete will not be sweating! vi. The immediate care for an athlete exhibiting the signs and symptoms of heat stroke is to reduce the body temperature as quickly as possible by any means available. This may include immersing the athlete in cold water, placing ice or cold towels around the body, or sponging the body with cool water. Remove clothing and equipment to prevent the retention of body heat. vii. The usual treatment for shock should also be administered, but cooling the body temperature to below 100 F is the priority. viii. If the athlete is conscious, allow them to drink cool water. Athletes suffering from heat stroke are critically ill and must be transported to an emergency room as quickly as possible. XVI. Cold Injuries a. Effects of cold i. When exposed to cold, the body attempts to increase internal heat production by increasing muscular activity, such as shivering, and by increasing the basal metabolic rate at which food stored within the body is burned. Heat loss is decreased by reducing the circulation of blood to the skin, muscles, and extremities. ii. Cold injury occurs in two ways. 1. The core temperature is maintained, but the temperature decreases in the skin, muscles, and extremities resulting in local injuries that include frostbite. 2. The core temperature and the temperature in the skin, muscles, and extremities both decrease, and all of the body processes slow down. This condition is known as hypothermia and may be fatal if not treated. Unit 4 First Aid 24 draft copy
25 iii. Body parts freeze when not enough heat is available to counteract external cold resulting in local injury. Predisposing factors include: 1. Inadequate insulation from cold and wind. 2. Restricted circulation because of tight clothing, especially footwear. 3. Fatigue. 4. Poor nutrition. 5. The use of alcohol. iv. The most commonly affected body parts are hands, feet, ears, and exposed parts of the face. All of these areas are located far from the heart and are normally subjected to rapid heat loss. v. Freezing temperatures affect the cells in the body in a predictable fashion. A cell is mostly water, which becomes cool and eventually freezes and is no longer able to function. The ice crystals that result then destroy the cell. b. Duration of the exposure, the temperature to which the skin has been exposed, and wind velocity are the three most important factors to consider when determining the severity of a local injury. c. Frostbite i. Frostbite usually involves the skin and the underlying superficial tissue. The affected person often does not notice it, and frequently a companion first perceives it. ii. The skin appears white and waxy and is firm to the touch, but the tissue beneath it is soft and resilient. iii. The person should be taken indoors, protected from the cold and subjected to slow, gentle warming. Effective warming techniques include the steady pressure of a warm hand, blowing warm breath, or holding the part in an armpit. For more serious frostbite, the body part can be placed in running cool water never hot water! iv. The affected area should not be rubbed with snow or by the hand. v. When the injured area thaws, it is first numb; then it turns blue or purple. Some swelling may also be seen. Blisters may form, and throbbing, aching, and burning may last for weeks in severe cases. The skin may remain permanently red, tender and sensitive to reexposure to cold, so these susceptible areas should receive extra protection. d. Hypothermia i. Severe body cooling, or hypothermia, can occur at temperatures well above freezing. It is usually caused by exposure to low or rapidly dropping temperatures, cold moisture, snow, or ice. ii. Hypothermia is aggravated by hunger, fatigue, and exertion, and may be associated with other local cold injuries like frostbite. iii. Generalized body cooling progresses through the following five states: 1. Shivering, which is the body s attempt to generate heat. Unit 4 First Aid 25 draft copy
26 2. Apathy, sleeplessness, listlessness, and indifference which may accompany rapid cooling of the body. 3. Unconsciousness, with a glassy stare, a very slow pulse rate, and slow respiratory rate. 4. Freezing of the extremities. 5. Death. iv. Shivering usually begins at a core temperature of 95 F and as the cooling process proceeds, clumsiness, fumbling, stumbling, falling, slow reactions, mental confusion, and difficulty in speaking follow. Death may occur within 2 hours of the onset of the first symptoms. v. Hypothermia is an acute, high priority, medical emergency and requires immediate transfer of the athlete to a medical facility. vi. The basic principles of emergency care are: 1. To prevent further heat loss by removing the athlete from the cold and wind, and replacing wet clothing. 2. To re-warm the athlete as rapidly and safely as possible by providing external heat in any way possible (hot water bottles, immersion in a tub of warm water, electric blankets, camp fires, or body heat from rescuers). 3. To be alert for complications. Shock and cardiac arrhythmias are commonly seen in serious cases. Vital signs must be monitored. Unit 4 First Aid 26 draft copy
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
5420-R STUDENT HEALTH SERVICES REGULATION NORTH COLONIE CENTRAL SCHOOLS NEWTONVILLE, NEW YORK Emergency Procedures and Approved First Aid Methods
 STUDENT HEALTH SERVICES REGULATION NORTH COLONIE CENTRAL SCHOOLS NEWTONVILLE, NEW YORK Emergency Procedures and Approved First Aid Methods EMERGENCY PROCEDURES Contact parents and cooperate with them in
STUDENT HEALTH SERVICES REGULATION NORTH COLONIE CENTRAL SCHOOLS NEWTONVILLE, NEW YORK Emergency Procedures and Approved First Aid Methods EMERGENCY PROCEDURES Contact parents and cooperate with them in
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Types of electrical injuries
 Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
12/5/2012. Introduction. Head, Neck, and Spine Injuries. Recognizing and Caring for Serious Head, Neck and Back Injuries
 Head, Neck, and Spine Injuries Identify the most common causes of head, neck and spinal injuries. List 10 situations that might indicate serious head, neck and spinal injuries. List the signals of head,
Head, Neck, and Spine Injuries Identify the most common causes of head, neck and spinal injuries. List 10 situations that might indicate serious head, neck and spinal injuries. List the signals of head,
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
FIRST AID FOR BASEBALL COACHES
 FIRST AID FOR BASEBALL COACHES Liability Issues. Do the right thing State provides qualified immunity Chapter 258 C, Section 13. Good Samaritan Law: No person who, in good faith, provides or obtains, or
FIRST AID FOR BASEBALL COACHES Liability Issues. Do the right thing State provides qualified immunity Chapter 258 C, Section 13. Good Samaritan Law: No person who, in good faith, provides or obtains, or
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
CHAPTER 1 DISASTER FIRST AID INTRODUCTION
 CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
WET, COUGHING AND COLD NEAR RIVER BANK STUNG BY BEE CAUSING ANAPHYLACTIC SHOCK TO WRIST
 GRIT IN EYE BROKEN LEG BONE WET, COUGHING AND COLD NEAR RIVER BANK STUNG BY BEE CAUSING ANAPHYLACTIC SHOCK HEART ATTACK SUFFERING FROM SHOCK CHOKING SEVERE BLEEDING TO WRIST HYPOTHERMIA ANGINA Localised
GRIT IN EYE BROKEN LEG BONE WET, COUGHING AND COLD NEAR RIVER BANK STUNG BY BEE CAUSING ANAPHYLACTIC SHOCK HEART ATTACK SUFFERING FROM SHOCK CHOKING SEVERE BLEEDING TO WRIST HYPOTHERMIA ANGINA Localised
MRC Medical Jeopardy Feud List of Treatments for Possible Injuries/Conditions
 List of Treatments for Possible Injuries/Conditions A. Apply cold compresses to affected area; elevate the area to reduce swelling and possible bleeding B. Apply direct pressure to wound area with sterile
List of Treatments for Possible Injuries/Conditions A. Apply cold compresses to affected area; elevate the area to reduce swelling and possible bleeding B. Apply direct pressure to wound area with sterile
First Aid Multiple Choice Test
 First Aid Multiple Choice Test Answer all 25 questions by circling the correct answer. This is an open-book test. Answers are contained in The Boy Scout Handbook. Patrol Troop 1. When making a 911 call,
First Aid Multiple Choice Test Answer all 25 questions by circling the correct answer. This is an open-book test. Answers are contained in The Boy Scout Handbook. Patrol Troop 1. When making a 911 call,
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Certified Athletic trainers should follow a 10-step process of evaluation for orthopedic injuries, which includes but is not limited to:
 Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Sports Injury Treatment
 Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Hand Injuries and Disorders
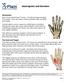 Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION. Airway must be open so oxygen can enter the body.
 CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION The Aims of First Aid The aims of first aid (the three Ps) are to: Preserve the casualty s life. Prevent
CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION The Aims of First Aid The aims of first aid (the three Ps) are to: Preserve the casualty s life. Prevent
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 715 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF HEMORRHAGE 1. PURPOSE: The management
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 715 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF HEMORRHAGE 1. PURPOSE: The management
Facial Sports Injuries
 Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Ankle Sprain. Information and Rehabilitation. Grade II. Grade I. Grade III
 514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
EYE, EAR, NOSE, and THROAT INJURIES
 T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
CHAPTER 32 QUIZ. Handout 32-1. Write the letter of the best answer in the space provided.
 Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Dressing and bandage
 Dressing and bandage Mihajlo Lojpur, M.D., Ph.D. INTRODUCTION The terms dressing and bandage are often used synonymously. In fact, the term dressing refers more correctly to the primary layer in contact
Dressing and bandage Mihajlo Lojpur, M.D., Ph.D. INTRODUCTION The terms dressing and bandage are often used synonymously. In fact, the term dressing refers more correctly to the primary layer in contact
Adult Choking and CPR Manual
 Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
CPR/First Aid. Lesson 12 Injuries to Muscles, Bones & Joints
 CPR/First Aid Lesson 12 Injuries to Muscles, Bones & Joints 1 Muscles Muscles are soft tissues. Your body has over 600 different muscles. Injuries to the brain, spinal cord or nerves can affect the muscles.
CPR/First Aid Lesson 12 Injuries to Muscles, Bones & Joints 1 Muscles Muscles are soft tissues. Your body has over 600 different muscles. Injuries to the brain, spinal cord or nerves can affect the muscles.
CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS
 CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS BRAIN INJURY Injury to the brain is one of the more serious outcomes that occur due to injury or illness. The first aider plays a major role in limiting damage
CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS BRAIN INJURY Injury to the brain is one of the more serious outcomes that occur due to injury or illness. The first aider plays a major role in limiting damage
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
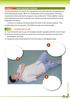 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
let s talk bleeds a bleed checklist for haemophilia patients
 let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CARDIAC REHABILITATION HOME EXERCISE ADVICE
 CARDIAC REHABILITATION HOME EXERCISE ADVICE Introduction Exercise is a very important as part of your rehabilitation and your future health. You will need to exercise at least three times per week, minimum,
CARDIAC REHABILITATION HOME EXERCISE ADVICE Introduction Exercise is a very important as part of your rehabilitation and your future health. You will need to exercise at least three times per week, minimum,
What Are Bursitis and Tendinitis?
 Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Contact your Doctor or Nurse for more information.
 A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
Preventing & Treating Low Back Pain
 Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Recent Injuries. www.physiofirst.org.uk
 Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Neck Injuries and Disorders
 Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Adult First Aid/CPR/AEd. Ready Reference
 Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
HELPFUL HINTS FOR A HEALTHY BACK
 HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
American Red Cross First Aid EXAMPLE ANSWER SHEET
 American Red Cross First Aid Exam A IMPORTANT: Read all instructions before beginning the exam. INSTRUCTIONS: Do not write on this exam. Mark all answers in pencil on the separate answer sheet as directed
American Red Cross First Aid Exam A IMPORTANT: Read all instructions before beginning the exam. INSTRUCTIONS: Do not write on this exam. Mark all answers in pencil on the separate answer sheet as directed
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
General Guidelines. Neck Stretch: Side. Neck Stretch: Forward. Shoulder Rolls. Side Stretch
 Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
o Understand the anatomy of the covered areas. This includes bony, muscular and ligamentous anatomy.
 COURSE TITLE Kin 505 Activities, Injuries Disease in the Larger Society On-Line offering Instructor Dr. John Miller [email protected] Course Description. Sports and exercise are a part of American society
COURSE TITLE Kin 505 Activities, Injuries Disease in the Larger Society On-Line offering Instructor Dr. John Miller [email protected] Course Description. Sports and exercise are a part of American society
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Reflex Physiology. Dr. Ali Ebneshahidi. 2009 Ebneshahidi
 Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS:
 LESSON TOPIC: AVERAGE TIME: BACK INJURY PREVENTION 30 Minutes INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS: a. Handout #1
LESSON TOPIC: AVERAGE TIME: BACK INJURY PREVENTION 30 Minutes INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS: a. Handout #1
2. (U4C2L3:F2) If your friend received a deep cut on her wrist, what would you do?
 Cadet Name: Date: 1. (U4C2L3:F1) Your friend receives a deep cut on her wrist while washing dishes. She asks for your help. How confident are you that you could provide appropriate aid? A) My friend is
Cadet Name: Date: 1. (U4C2L3:F1) Your friend receives a deep cut on her wrist while washing dishes. She asks for your help. How confident are you that you could provide appropriate aid? A) My friend is
FIRST AID TEST. 367 West Robles Ave Santa Rosa, CA 95407 707-206-9988. www.schoolbusing.com. Revised April 21, 2008 - 1 -
 FIRST AID TEST 367 West Robles Ave Santa Rosa, CA 95407 707-206-9988 www.schoolbusing.com Revised April 21, 2008-1 - West County Transportation Agency This test was developed to help school bus driver
FIRST AID TEST 367 West Robles Ave Santa Rosa, CA 95407 707-206-9988 www.schoolbusing.com Revised April 21, 2008-1 - West County Transportation Agency This test was developed to help school bus driver
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
For Deep Pressure Massage
 T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
Emergency Action Plans
 Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
RP0807 - PERFORM SPLINTING TECHNIQUES
 RP0807 - PERFORM SPLINTING TECHNIQUES TERMINAL LEARNING OBJECTIVE. 1. Without the aid of references, given a casualty and standard combat lifesaver medical equipment set, perform splinting techniques,
RP0807 - PERFORM SPLINTING TECHNIQUES TERMINAL LEARNING OBJECTIVE. 1. Without the aid of references, given a casualty and standard combat lifesaver medical equipment set, perform splinting techniques,
LEGAL PROTECTION. Good Samaritan Law RCW 4.24.300
 GOALS This course is designed to instruct coach very basic first aid techniques to protect the players under your guidance. This presentation only provides a brief overview of the issues that you may face
GOALS This course is designed to instruct coach very basic first aid techniques to protect the players under your guidance. This presentation only provides a brief overview of the issues that you may face
2 CHECKING AN INJURED OR ILL ATHLETE
 American Red Cross 2 CHECKING AN INJURED OR ILL ATHLETE ~~~'1'H ~.. 2 CHECKING AN INJURED OR III ATHLETE Checking the scene for safety and checking an injured or ill athlete is the first action to take,
American Red Cross 2 CHECKING AN INJURED OR ILL ATHLETE ~~~'1'H ~.. 2 CHECKING AN INJURED OR III ATHLETE Checking the scene for safety and checking an injured or ill athlete is the first action to take,
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
A small roller with a big effect. The mini roller for massaging, strengthening, stretching and warming up
 A small roller with a big effect The mini roller for massaging, strengthening, stretching and warming up Suva Preventative products P. O Box, 6002 Lucerne Enquiries Tel. 041 419 58 51 Orders www.suva.ch/waswo
A small roller with a big effect The mini roller for massaging, strengthening, stretching and warming up Suva Preventative products P. O Box, 6002 Lucerne Enquiries Tel. 041 419 58 51 Orders www.suva.ch/waswo
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES
 THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES I. THORACIC OUTLET SYNDROME TOS is a compression of nerves or blood vessels, or both, in the thoracic outlet region, which is the space between the collarbone
THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES I. THORACIC OUTLET SYNDROME TOS is a compression of nerves or blood vessels, or both, in the thoracic outlet region, which is the space between the collarbone
.org. Tennis Elbow (Lateral Epicondylitis) Anatomy. Cause
 Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Surgery for cervical disc prolapse or cervical osteophyte
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: [email protected]
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: [email protected]
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
How To Stretch Your Body
 Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS)
 SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
A Stretch-Break Program for Your Workplace! www.healthyworkplaceweek.ca
 www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
X-Plain Neck Exercises Reference Summary
 X-Plain Neck Exercises Reference Summary Introduction Exercising your neck can make it stronger, more flexible and reduce neck pain that is caused by stress and fatigue. This reference summary describes
X-Plain Neck Exercises Reference Summary Introduction Exercising your neck can make it stronger, more flexible and reduce neck pain that is caused by stress and fatigue. This reference summary describes
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
