Urinary Incontinence Treatment
|
|
|
- Buddy Gallagher
- 10 years ago
- Views:
Transcription
1 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. M issouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois, Inc. WellCare Health Plans of New Jersey, Inc. WellCare Health Insurance of Arizona, Inc. WellCare of Florida, Inc. WellCare of Connecticut, Inc. WellCare of Georgia, Inc. WellCare of Kentucky, Inc. WellCare of Louisiana, Inc. WellCare of New York, Inc. WellCare of Ohio, Inc. WellCare of South Carolina, Inc. WellCare of Texas, Inc. WellCare Prescription Insurance, Inc. Urinary Incontinence Treatment Policy Number: Original Effective Date: 2/2/2009 Revised Date(s): 2/26/2010; 2/26/2011; 2/2/2012 DISCLAIMER The Clinical Coverage Guideline is intended to supplement certain standard WellCare benefit plans. The terms of a member s particular Benef it Plan, Ev idence of Cov erage, Certificate of Coverage, etc., may differ significantly from this Coverage Position. For example, a member s benefit plan may contain specif ic exclusions related to the topic addressed in this Clinical Coverage Guideline. When a conflict exists between the two documents, the Member s Benefit Plan always supersedes the inf ormation contained in the Clinical Coverage Guideline. Additionally, Clinical Coverage Guidelines relate exclusively t o the administration of health benefit plans and are NOT recommendations for treatment, nor should they be used as treatment guidelines. The application of the Clinical C overage Guideline is subject to the benef it determinations set forth by the Centers for Medicare and Medicaid Services (CMS) National and Local Coverage Determinations and state-specific Medicaid mandates, if any. Note: The lines of business (LOB) are subject to change without notice; consult for list of c urrent LOBs. APPLICATION STATEMENT The application of the Clinical Coverage Guideline is subject to the benefit determinations set f orth by the Centers f or Medicare and Medicaid Serv ices (CMS) National and Local Cov erage Determinations and state-specif ic Medicaid mandates, if any.
2 BACKGROUND Urinary incontinence is the involuntary loss of urine that is a social or hygienic problem. Urinary incontinence is categorized as transient, urge, stress, overflow, mixed, and functional. It affects at least 13 million Americans and is twice as common in women as in men. Urinary incontinence affects 10% to 52% of adult women and is severe in 3% to 17%. For noninstitutionalized persons aged 60 years or older, the prevalence ranges from 15% to 30%, and for nursing home residents, the prevalence is 50% or higher. The following are risk factors for the development of urinary incontinence in women, including childbirth, mode of delivery, pregnancy, increased parity, hysterectomy, recurrent urinary tract infections, and other gynecologic factors; gastrointestinal factors; medications such as diuretics, sedatives and beta-blockers; smoking; alcohol and caffeine use; presence of two or more chronic diseases such as chronic obstructive pulmonary disease (COPD), congestive heart failure (CHF), and diabetes; advanced age; white race; and high body mass index. Other causes of incontinence in both men and women include diseases that damage the cortical and subcortical inhibitory centers, such as dementia, Alzheimer s disease, normal pressure hydrocephalus, and multi-infarct disease from Hayes, 2006). Treatment options for urinary voiding disorders include: behavioral strategies, pharmacological interventions, temporary electrical stimulation, and reconstructive surgery. Usually, the less invasive, first- tier behavioral and pharmacological interventions are advised and are often combined with temporary electrical stimulation before irreversible, reconstructive surgery is considered as a treatment choice. Sacral Nerve Stimulation Sacral nerve stimulation (SNS) is currently intended for the treatment of intractable urinary urge incontinence, nonobstructive urinary retention, and urgency/frequency syndrome in adults. SNS is generally indicated in members who demonstrate at least 50% incontinence symptom relief during percutaneous test stimulation and who have failed or not tolerated more conservative treatments (e.g., behavioral strategies, pharmacological interventions). When the screening trial demonstrates successful results, permanent SNS system placement can be performed. The implantable pulse generator (IPG) is positioned surgically in the upper buttock region. Once the IPG is placed, it is then connected to an extension that passes underneath the skin to an electrical lead that has been placed through an incision over the lower back in contact with one side of the appropriate sacral nerve root, most often the S3 vertebra. Implantation is considered to be a reversible, minimally invasive procedure and is performed under general anesthesia. The IPG can be externally adjusted to optimal settings by a physician using a microprocessorbased console programmer. Members can operate a hand-held programmer to adjust levels of stimulation within physician-prescribed limits. The battery is expected to last approximately 7 9 years. When the battery loses power, another procedure is required to replace it. Pelvic Floor Electrical Stimulation Pelvic floor electrical stimulation can be performed in a clinical setting or at home. Electrodes can be placed either externally and internally; the treatment varies in stimulus frequency, stimulus intensity, treatment duration, number of sessions, and treatment days per week. During each treatment session, a frequency of 5 to 100 hertz (Hz) is used for 15 to 20 minutes once or twice daily. In most cases, vaginal, anal, and surface electrodes are used; removable electrodes are placed in the vagina or rectum (plug electrodes) or around the dorsum of the penis (butterfly electrodes). Electrodes may also be placed on the presacral skin to convey electrical impulses to the nerve roots that supply the pudendal and pelvic nerves to the bladder. In cases of urge incontinence, the objective of electrical stimulation is to reinforce the inhibitory system. Since these inhibitory neurons operate at low frequencies, stimulation is generally administered at 5 to 20 Hz. Electrical stimulation may also be transmitted percutaneously with surface electrodes to inhibit detrusor activity. Surface electrodes may be applied to the hamstring and quadriceps muscles of one or both legs. In these cases, electrical Clinical Coverage Guideline page 2
3 stimulation is applied with pulse duration of 0.2 milliseconds (ms) and a frequency of 30 Hz. The hamstrings and quadriceps are stimulated alternately for 4 seconds each with an intervening 4-second duration in which no stimulation is applied. In another variation of the technique, an electrode is placed on the presacral skin over the S2/3/4 nerve roots and a second electrode is placed over the perineal skin. For stress incontinence, the goal of electrical stimulation is the activation of the motor neurons. In these cases, stimulation is generally administered at 20 to 50 Hz. For patients with mixed incontinence, the treatment sessions generally alternate between stimulation parameters for urge incontinence and stress incontinence (Hayes, 2006). Collagen Implant A collagen implant, which is injected into the submucosal tissues of the urethra and/or the bladder neck and into tissues adjacent to the urethra, is a prosthetic device used in the treatment of stress urinary incontinence resulting from intrinsic sphincter deficiency (ISD). ISD is a cause of stress urinary incontinence in which the urethral sphincter is unable to contract and generate sufficient resistance in the bladder, especially during stress maneuvers. Transurethral Radiofrequency Micro-Remodeling The Renessa System (Novasys Medical Inc.) consists of an RF generator and probe. The probe is inserted through the urethra into the bladder, and is anchored in the bladder outlet by inflation of a balloon at its tip. A series of 4 needles arranged concentrically around the probe shaft just beneath the balloon are deployed into the tissue after which pulses of RF energy lasting 60 to 90 seconds are administered. The RF energy raises the temperature in the vicinity of the needle tips to 65 C to 75 C. These temperatures are high enough to break down tissue proteins in the region of the needle tip but do not lead to tissue destruction. As these small lesions heal, the urethral tissue becomes firmer and less likely to open involuntarily under pressure. The process, which is also called microremodeling, is performed by a gynecologist or urologist, takes around 20 minutes, and has a recovery time of around 2 hours. The procedure has been carried out under conscious sedation, but preliminary data indicate it can also be performed in the office. The available evidence on the efficacy and safety of transurethral RF therapy with the Renessa system for treatment of SUI is very limited. Only two manufacturer-sponsored studies were identified that were conducted by a single group of researchers. There is some evidence of efficacy among patients with the most severe symptoms of SUI, but analysis and interpretation of the results is complicated by a high rate of placebo responses and lack of blinded assessment of outcomes. Moreover, there has been no evaluation of the long-term health outcomes or complications following this procedure, and it is unknown how it compares with alternative technologies. Further studies incorporating blinded assessment of objective outcomes and longer follow-up are needed to confirm the efficacy and safety of this procedure. POSITION STATEMENT 1) Sacral nerve stimulation is considered medically necessary and a covered benefit if ALL of the following criteria are met: Member has a diagnosis of urinary urge incontinence, non-obstructive urinary retention OR , , , Urinary Urgency-Frequency Syndrome; AND, The member has shown a documented positive response to a percutaneous trial of sacral stimulation*; AND, The member has not responded to conventional therapy, including documented behavioral, Clinical Coverage Guideline page 3
4 pharmacologic, and/or surgical corrective therapy. *Before a member is eligible for permanent implantation, the member must demonstrate a 50% or greater improvement through test stimulation. Improvement is measured through a voiding diary. 2) Non-implantable pelvic floor electrical stimulation is considered medically necessary if ALL of the following criteria are met: Member has a diagnosis of Stress and/or , Urinary Urge Incontinence; AND, Member is cognitively intact; AND, Member has failed a documented trial of pelvic muscle exercise (PME) training**. ** A failed trial of PME training is defined as no clinically significant improvement in urinary incontinence after completing 4 weeks of an ordered plan of pelvic muscle exercises designed to increase periurethral muscle strength. 3) Injectable urethral bulking agents (i.e., collagen) are considered medically necessary for members who: have not responded to conventional treatments; AND, have Iintrinsic Sphincter Deficiency (ISD) Injections of bulking agents have been shown to have NO clinical value in ANY of the following circumstances and, therefore, are NOT a covered benefit: Previous V15.3 Pelvic Radiation Therapy; OR, Unstable or Noncompliant Bladder; OR, Members with severe allergies manifested by a history of anaphylaxis, or history or presence of multiple severe allergies; OR, Members with an acute condition involving Cystitis, Urethritis, or Infection; OR, Members undergoing or planning to undergo desensitization injections to meat products. NOTE: Prior to collagen implant therapy, a skin test for collagen sensitivity must be administered and evaluated over a 4 week period. In male members, the evaluation must include a complete history and physical examination and a simple cystometrogram to determine that the bladder fills and stores properly. The member then is asked to stand upright with a full bladder and to cough or otherwise exert abdominal pressure on his bladder. If the member leaks, the diagnosis of ISD is established. In female members, the evaluation must include a complete history and physical examination (including a pelvic exam) and a simple cystometrogram to rule out abnormalities of bladder compliance and abnormalities of urethral support. Following that determination, an abdominal leak point pressure (ALLP) test is performed. Leak point pressure, stated in cm H2O, is defined as the intra-abdominal pressure at which leakage occurs from the bladder (around a catheter) when the bladder has been filled with a minimum of 150 cc fluid. If the patient has an ALLP of less than 100 cm H2O, the diagnosis of ISD is established. Members whose incontinence does not improve with 5 injection procedures (5 separate treatment sessions) are considered treatment failures, and no further treatment of urinary incontinence by collagen implant is covered. Members who have a reoccurrence of incontinence following successful treatment with collagen implants in the past (e.g., 6-12 months previously) may benefit from additional treatment sessions. Coverage of additional sessions Clinical Coverage Guideline page 4
5 may be allowed but must be supported by medical justification. 4) Vaginal cones are considered medically necessary and a covered benefit if ALL of the following criteria are met: When used in combination with pelvic muscle exercises (Kegel s exercise); AND, Member has a diagnosis of or Simple (pure) Stress Urinary Incontinence 5) Pessary (bladder neck support prosthesis), a plastic device that fits into the vagina to help support the uterus and bladder, is considered medically necessary and a covered benefit if ALL of the following criteria are met: Member is female and has a diagnosis of Stressed or Mixed Urinary Incontinence 6) Tension-free vaginal tape procedures are considered medically necessary and a covered benefit if ALL of the following criteria are met: Member is female; AND, Has failed behavioral and pharmacological treatments; AND, Has a diagnosis of Stress Urinary Incontinence 7) Colposuspension and sling procedures are considered medically necessary and a covered benefit if ALL of the following criteria are met: Member has a diagnosis of or or Stress Urinary Incontinence; AND, Member is refractory to conservative management The following treatments for urinary incontinence are considered experimental and investigational and NOT a covered benefit: Transurethral radiofrequency micro-remodeling using the Renessa system (Novasys Medical Inc) Transvaginal radiofrequency bladder neck suspension Percutaneous tibial nerve stimulation Extracorporeal magnetic stimulation (Neocontrol System) Transurethral Macroplastique injection Transobturator tape procedure Implantable pelvic floor electrical stimulation CODING Covered CPT Codes when the above criteria has been met: Subcutaneous injection of filing material (e.g. collagen), 1 cc or less Subcutaneous injection of filing material (e.g. collagen), 1.1 to 5.0 cc Subcutaneous injection of filing material (e.g. collagen), 5.1 to 10.0 cc Subcutaneous injection of filing material (e.g. collagen), over 10.0 cc Endoscopic injection of implant material into the submucosal tissues of the urethra and/or bladder neck Anterior vesicourethropexy, or urethropexy (eg, Marshall-Marchetti-Krantz, Burch); simple Anterior vesicourethropexy, or urethropexy (eg, Marshall-Marchetti-Krantz, Burch); complicated (eg, secondary repair Laparoscopy, surgical; urethral suspension for stress incontinence Clinical Coverage Guideline page 5
6 51992 Laparoscopy, surgical; sling operation for stress incontinence (e.g., fascia or synthetic) Sling operation for correction of male urinary incontinence (e.g., fascia or synthetic) Removal or revision of sling for male urinary incontinence (e.g., fascia or synthetic) Insertion of tandem cuff (dual cuff) Insertion of inflatable urethral/bladder neck sphincter, including placement of pump, reservoir, and cuff Removal of inflatable urethral/bladder neck sphincter, including pump, reservoir, and cuff Removal and replacement of inflatable urethral/bladder neck sphincter including pump, reservoir, and cuff at the same operative session Removal and replacement of inflatable urethral/bladder neck sphincter including pump, reservoir, and cuff through an infected field at the same operative session including irrigation and debridement of infected tissue Repair of inflatable urethral/bladder neck sphincter, including pump, reservoir, and cuff Fitting and insertion of pessary or other intravaginal support device Removal or revision of sling for stress incontinence (e.g., fascia or synthetic) Sling operation for stress incontinence (e.g., fascia or synthetic) Application of surface (transcutaneous) neurostimulator Percutaneous implantation of neurostimulator electrodes; sacral nerve (transforaminal placement) Incision for implantation of neurostimulator electrodes; sacral nerve (transforaminal placement) Revision or removal of peripheral neurostimulator electrodes Electronic analysis of implanted neurostimulator pulse generator system (e.g., rate, pulse amplitude and duration, configuration of wave form, battery status, electrode selectability, output modulation, cycling, impedance and patient compliance measurements); simple or complex brain, spinal cord, or peripheral (i.e., cranial nerve, peripheral nerve, autonomic nerve, neuromuscular) neurostimulator pulse generator/transmitter, without reprogramming Electronic analysis of implanted neurostimulator pulse generator system (e.g., rate, pulse amplitude and duration, configuration of wave form, battery status, electrode selectability, output modulation, cycling, impedance and patient compliance measurements); simple spinal cord, or peripheral (i.e., peripheral nerve, autonomic nerve, neuromuscular) neurostimulator pulse generator/transmitter, with intraoperative or subsequent programming Electronic analysis of implanted neurostimulator pulse generator system (e.g., rate, pulse amplitude and duration, configuration of wave form, battery status, electrode selectability, output modulation, cycling, impedance and patient compliance measurements); complex brain, spinal cord, or peripheral (except cranial nerve) neurostimulator pulse generator/transmitter, with intraoperative or subsequent programming, first hour Electronic analysis of implanted neurostimulator pulse generator system (e.g., rate, pulse amplitude and duration, configuration of wave form, battery status, electrode selectability, output modulation, cycling, impedance and patient compliance measurements); complex spinal cord, or peripheral (except cranial nerve) neurostimulator pulse generator/transmitter, with intraoperative or subsequent programming, each additional 30 minutes after first hour Covered ICD-9-CM Procedure Codes when the above criteria has been met: Implantation or Replacement of Peripheral Neurostimulator Leads, i.e., Sacral Nerve Implantation of artificial urinary sphincter (AUS); i.e. urethral Levator muscle operation for urethrovesical suspension Injection of implant into urethra and/or bladder neck, i.e. Collagen implant Repair of Stress Incontinence NOS Insertion of other vaginal pessary Clinical Coverage Guideline page 6
7 Non Covered CPT Codes Transurethral radiofrequency micro-remodeling of the female bladder neck and proximal urethra for stress urinary incontinence Non Covered CPT Category III Codes 0193T Has been deleted effective 2011, to report use Covered HCPC Codes when the above criteria has been met: A4290 Sacral nerve stimulation test lead, each A4335 Incontinence Supply, miscellaneous (assign for Vaginal Cones, Tension Free Vaginal Tape as there are no specified codes to date) A4561 Pessary, rubber, any type A4562 Pessary, non-rubber, any type C1767 Generator, neurostimulator (implantable) C1771 Repair device, urinary, incontinence, with sling graft C1778 Lead, neurostimulator (implantable) C1787 Patient programmer, neurostimulator C1815 Prosthesis, urinary sphincter (implantable) C1816 Receiver and/or transmitter, neurostimulator (implantable) C1883 Adaptor/extension, pacing lead or neurostimulator lead (implantable) C1897 Lead, neurostimulator test kit (implantable) C2631 Repair device, urinary, incontinence, without sling graft E0740 Incontinence treatment system, pelvic floor stimulator, monitor, sensor and/or trainer L8603 Collagen Implant, Injectable bulking agent, urinary tract, 2.5 ml syringe, includes shipping and necessary supplies L8606 Synthetic implant, Injectable bulking agent, urinary tract, 1 ml syringe, includes shipping and necessary supplies L8680 Implantable neurostimulator electrode, each L8681 Patient programmer (external) for use with implantable programmable neurostimulator pulse generator L8682 Implantable neurostimulator radiofrequency receiver L8683 Radiofrequency transmitter (external) for use with implantable neurostimulator radiofrequency receiver L8684 Radiofrequency transmitter (external) for use with implantable sacral root neurostimulator receiver for bowel and bladder management, replacement L8685 Implantable neurostimulator pulse generator, single array, rechargeable, includes extension L8686 Implantable neurostimulator pulse generator, single array, non-rechargeable, includes extension L8687 Implantable neurostimulator pulse generator, dual array, rechargeable, include extension L8688 Implantable neurostimulator pulse generator, dual array, non-rechargeable, includes extension L8689 External recharging system for implanted neurostimulator, replacement only L8695 External recharging system for battery (external) for use with implantable neurostimulator Q3031 Collagen skin test S8270* Enuresis alarm, using auditory buzzer and/or vibration device *S- Codes are NON COVERED FOR MEDICARE Refer to HCPCS Level II Temporary National Codes Covered ICD-9-CM Diagnosis Codes when the above criteria has been met: ISD Intrinsic (Urethral) Sphincter Deficiency Female Stress Incontinence Retention of Urine, unspecified Urge incontinence Male Stress Incontinence Clinical Coverage Guideline page 7
8 Mixed incontinence (female) (male) Urinary Frequency *Current Procedural Terminology (CPT) 2012 American Medical Association: Chicago, IL. REFERENCES Peer Reviewed 1. Hayes Directory. (2008, September 18). Electrical percutaneous tibial nerve stimulation for urinary voiding dysfunction. Retrieved from 2. Hayes Directory. (2007, January 26). Transurethral radiofrequency micro-remodeling using the Renessa system (Novasys Medical Inc.) for female stress urinary incontinence. Retrieved from 3. Hayes Directory. (2006, March 31). Retrieved from Government Agencies, Professional and Medical Organizations 1. American Urological Association. (2009). Guideline for the surgical management of female stress urinary incontinence. Retrieved from 2. American Urological Association. (1997). Report on the surgical management of female stress urinary incontinence. 3. Centers for Medicare and Medicaid Services. (2006, June 19). National coverage determination for nonimplantable pelvic floor electrical stimulator (230.8). Retrieved from 4. Centers for Medicare and Medicaid Services. (2002, January 1). National coverage determination for sacral nerve stimulation for urinary incontinence (230.18). Retrieved from 5. Centers for Medicare and Medicaid Services. (1996, October 7). National coverage determination for incontinence control devices (230.10). Retrieved from HISTORY AND REVISIONS Date Action 2/2/2012 Approved by MPC. No changes. 12/1/2011 New template design approved by MPC. 2/26/2011 Approved by MPC. Clinical Coverage Guideline page 8
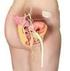
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide
 Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Normal bladder function requires a coordinated effort between the brain, spinal cord, and the bladder.
 .. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
.. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
surg urin Surgery: Urinary System 1
 Surgery: Urinary System 1 This section contains information to assist providers in billing for surgical procedures related to the urinary system. Extracorporeal Shock Wave Lithotripsy Medi-Cal covers Extracorporeal
Surgery: Urinary System 1 This section contains information to assist providers in billing for surgical procedures related to the urinary system. Extracorporeal Shock Wave Lithotripsy Medi-Cal covers Extracorporeal
Urinary Incontinence in Women. Susan Hingle, M.D. Department of Medicine
 Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
URINARY INCONTINENCE
 URINARY INCONTINENCE What is urinary incontinence? Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only a few drops when you cough or sneeze to entirely
URINARY INCONTINENCE What is urinary incontinence? Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only a few drops when you cough or sneeze to entirely
Moda Health Medical Necessity Criteria
 Page 1 of 8 Approved: Neal Mills, MD Date: 03/23/2016 Description: A number of procedures have been investigated for the treatment of urinary incontinence, including pelvic floor muscle exercises, behavioral
Page 1 of 8 Approved: Neal Mills, MD Date: 03/23/2016 Description: A number of procedures have been investigated for the treatment of urinary incontinence, including pelvic floor muscle exercises, behavioral
Urinary Incontinence. Types
 Urinary Incontinence Leakage of urine is called urinary incontinence. It is a common problem in women. Some women occasionally leak small amounts of urine. At other times, leakage of urine is frequent
Urinary Incontinence Leakage of urine is called urinary incontinence. It is a common problem in women. Some women occasionally leak small amounts of urine. At other times, leakage of urine is frequent
Urinary Incontinence. Anatomy and Terminology Overview. Moeen Abu-Sitta, MD, FACOG, FACS
 Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006
 Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006 What treatment options are available for a woman with stress urinary incontinence (SUI)? Behavioral therapy, medication, pessary,
Stress Urinary Incontinence: Treatment Manisha Patel, MD April 10, 2006 What treatment options are available for a woman with stress urinary incontinence (SUI)? Behavioral therapy, medication, pessary,
Urinary Incontinence FAQ Sheet
 Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
URINARY INCONTINENCE CASE PRESENTATION #1. Urinary Incontinence - History 2014/10/07. Structure of the Female Lower Urinary Tract
 Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Bladder pressure 2014/10/07 Structure of the Female Lower Urinary Tract Ureter URINARY INCONTINENCE Clinical Clerkship Lecture Series Outer peritoneal coat Detrusor smooth muscle Mucosa Trigone Proximal
Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Overactive Bladder (OAB)
 Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Female Urinary Disorders and Pelvic Organ Prolapse
 Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
FEMALE INCONTINENCE REVIEW
 200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
URINARY INCONTINENCE IN WOMEN
 URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse
 Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
Regain Control of Your Active Life Treatment Options for Incontinence and Pelvic Organ Prolapse Nearly one quarter of all women in the United States have some sort of pelvic floor disorder such as urinary
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Becoming knowledgeable about urinary incontinence Uterus Normal Pelvic Anatomy
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Becoming knowledgeable about urinary incontinence Uterus Normal Pelvic Anatomy
symptoms of Incontinence
 Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
National Coverage Determination. Vagus Nerve Stimulation (VNS)
 National Coverage Determination Vagus Nerve Stimulation (VNS) Number NEURO-004 Contractor Name Wisconsin Physicians Service Insurance Corporation AMA CPT Copyright Statement CPT codes, descriptions and
National Coverage Determination Vagus Nerve Stimulation (VNS) Number NEURO-004 Contractor Name Wisconsin Physicians Service Insurance Corporation AMA CPT Copyright Statement CPT codes, descriptions and
National Medical Policy
 National Medical Policy Subject: Urinary Incontinence Devices and Treatments Policy Number: NMP215 Effective Date*: March 2005 Updated: October 2015 This National Medical Policy is subject to the terms
National Medical Policy Subject: Urinary Incontinence Devices and Treatments Policy Number: NMP215 Effective Date*: March 2005 Updated: October 2015 This National Medical Policy is subject to the terms
1 in 3 women experience Stress Urinary Incontinence.
 A PATIENT S GUIDE 1 in 3 women experience Stress Urinary Incontinence. It s time to talk about SUI Get the facts. This Patient s Guide is intended as a public resource on the issue of Stress Urinary Incontinence
A PATIENT S GUIDE 1 in 3 women experience Stress Urinary Incontinence. It s time to talk about SUI Get the facts. This Patient s Guide is intended as a public resource on the issue of Stress Urinary Incontinence
SOGC Recommendations for Urinary Incontinence
 The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
The quality of evidence is rated, and recommendations are made using the criteria described by the Canadian Task Force on Preventive Health Care. Clinical Practice Guidelines: The Evaluation of Stress
Urinary Incontinence Dr. Leffler
 Urinary Incontinence Dr. Leffler The involuntary loss of urine at socially unacceptable times occurs in both women and men, but more commonly in women. It has multiple, far-reaching effects on daily activities,
Urinary Incontinence Dr. Leffler The involuntary loss of urine at socially unacceptable times occurs in both women and men, but more commonly in women. It has multiple, far-reaching effects on daily activities,
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Patient. Frequently Asked Questions. Transvaginal Surgical Mesh for Pelvic Organ Prolapse
 Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Coverage and Authorization Services is available to respond to your coding questions toll-free at 800-292-2903.
 For Urinary Control Commonly Billed Codes October 2010 Medtronic provides this information for your convenience only. It is not intended as a recommendation regarding clinical practice. It is the responsibility
For Urinary Control Commonly Billed Codes October 2010 Medtronic provides this information for your convenience only. It is not intended as a recommendation regarding clinical practice. It is the responsibility
Sacral Nerve Neuromodulation/Stimulation
 MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Sacral Nerve Neuromodulation/Stimulation Number 7.01.69 Effective
MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Sacral Nerve Neuromodulation/Stimulation Number 7.01.69 Effective
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use.
 Questions for my Doctor Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use. INDICATIONS: Coaptite Injectable Implant is indicated for soft
Questions for my Doctor Refer to Coaptite Injectable Implant Instructions for Use provided with product for complete instructions for use. INDICATIONS: Coaptite Injectable Implant is indicated for soft
Cardiac Rehabilitation CARDIAC REHABILITATION HS-091. Policy Number: HS-091. Original Effective Date: 3/16/2009
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. M issouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. M issouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
9/24/2015. Incontinence and Prolapse 2015 Primary Care Update CME Symposium. Objectives. Mark Memo, DO, FACS NEO Urology September 25-27
 Incontinence and Prolapse 2015 Primary Care Update CME Symposium Mark Memo, DO, FACS NEO Urology September 25-27 Objectives Incontinence Pelvic Organ Prolapse Vaginal Mesh Litigation 1 Urinary Incontinence
Incontinence and Prolapse 2015 Primary Care Update CME Symposium Mark Memo, DO, FACS NEO Urology September 25-27 Objectives Incontinence Pelvic Organ Prolapse Vaginal Mesh Litigation 1 Urinary Incontinence
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE
 VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE
 LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
AMS Sphincter 800 Urinary Prosthesis
 AMS Sphincter 800 Urinary Prosthesis AMS Sphincter 800 AMS Sphincter 800 AMS Sphincter 800 The device is implanted in the body and cannot be seen. The cuff can be placed at the bulbous urethra or at the
AMS Sphincter 800 Urinary Prosthesis AMS Sphincter 800 AMS Sphincter 800 AMS Sphincter 800 The device is implanted in the body and cannot be seen. The cuff can be placed at the bulbous urethra or at the
Stem Cell Transplantation
 Harmony Behavioral Health, Inc. Harmony Behavioral Health of Florida, Inc. Harmony Health Plan of Illinois, Inc. HealthEase of Florida, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance
Harmony Behavioral Health, Inc. Harmony Behavioral Health of Florida, Inc. Harmony Health Plan of Illinois, Inc. HealthEase of Florida, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
Do I Need to Have Surgery for Urinary Incontinence? What Kinds of Surgery Can Treat Stress Incontinence?
 Do I Need to Have Surgery for Urinary Incontinence? Excerpts from The Incontinence Solution: Answers for Women of All Ages, by William H. Parker, MD, Amy E. Rosenman, MD and Rachel Parker (Simon and Schuster,
Do I Need to Have Surgery for Urinary Incontinence? Excerpts from The Incontinence Solution: Answers for Women of All Ages, by William H. Parker, MD, Amy E. Rosenman, MD and Rachel Parker (Simon and Schuster,
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Male urinary incontinence (leakage of urine) you are not alone
 Male urinary incontinence (leakage of urine) you are not alone Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Male urinary incontinence (leakage of urine) you are not alone Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Liberty Pelvic Floor Stimulation
 Liberty Pelvic Floor Stimulation A logical first choice for treatment of urinary incontinence Liberty s simplified design exercises the correct muscles and is easy to use, therefore helping increase patient
Liberty Pelvic Floor Stimulation A logical first choice for treatment of urinary incontinence Liberty s simplified design exercises the correct muscles and is easy to use, therefore helping increase patient
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Sexuality after your Spinal Cord Injury
 Sexuality after your Spinal Cord Injury Introduction Spinal Cord Injury (SCI) affects to varying degrees the mechanics and sensations of sex and sexuality. Some people think that spinal injury means an
Sexuality after your Spinal Cord Injury Introduction Spinal Cord Injury (SCI) affects to varying degrees the mechanics and sensations of sex and sexuality. Some people think that spinal injury means an
Lifestyle changes. Pelvic floor muscle training
 Incontinence, urinary - Treatment Treating urinary incontinence The treatment you receive for urinary incontinence will depend on the type of incontinence you have and the severity of your symptoms. If
Incontinence, urinary - Treatment Treating urinary incontinence The treatment you receive for urinary incontinence will depend on the type of incontinence you have and the severity of your symptoms. If
Overactive bladder and urgency incontinence
 Overactive bladder and urgency incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing
Overactive bladder and urgency incontinence As a health care provider you can make a significant difference to the quality of life of patients like these by addressing urinary incontinence, introducing
Stress Urinary Incontinence
 Saint Mary s Hospital Gynaecology Service Warrell Unit Stress Urinary Incontinence Information for patients What is Stress Incontinence? Stress incontinence is a leakage of urine occurring on physical
Saint Mary s Hospital Gynaecology Service Warrell Unit Stress Urinary Incontinence Information for patients What is Stress Incontinence? Stress incontinence is a leakage of urine occurring on physical
Surgical Treatment for Female Stress Urinary. Continence. Consumer Education
 Surgical Treatment for Female Stress Urinary Incontinence By: Amy Rosenman, MD Geffen School of Medicine at UCLA Santa Monica, California Promoting Quality Continence Care through Consumer Education Always
Surgical Treatment for Female Stress Urinary Incontinence By: Amy Rosenman, MD Geffen School of Medicine at UCLA Santa Monica, California Promoting Quality Continence Care through Consumer Education Always
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline RECOMMENDATIONS 1 Conditional: Clinicians who are making
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline RECOMMENDATIONS 1 Conditional: Clinicians who are making
Management of Urinary Incontinence. Sheri J. Ross, BSc, DVM, PhD, Dipl. ACVIM (Internal Medicine)
 Management of Urinary Incontinence Sheri J. Ross, BSc, DVM, PhD, Dipl. ACVIM (Internal Medicine) Managing Urinary Incontinence Urinary incontinence is very prevalent among older animals. In this group
Management of Urinary Incontinence Sheri J. Ross, BSc, DVM, PhD, Dipl. ACVIM (Internal Medicine) Managing Urinary Incontinence Urinary incontinence is very prevalent among older animals. In this group
What you should know about Stress Urinary Incontinence
 Gynecare TVT Stop coping. Start living. What you should know about Stress Urinary Incontinence Have you ever leaked urine when you laughed, coughed or sneezed? You are not alone. Many women suffer from
Gynecare TVT Stop coping. Start living. What you should know about Stress Urinary Incontinence Have you ever leaked urine when you laughed, coughed or sneezed? You are not alone. Many women suffer from
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
GENUINE STRESS AND URGE INCONTINENCE PROTOCOL
 GENUINE STRESS AND URGE INCONTINENCE PROTOCOL Using the NeuroTrac ETSTM in combination of electrostimulation and EMG Biofeedback in the treatment of female urinary incontinence. Anna Pawlaczyk Specialist
GENUINE STRESS AND URGE INCONTINENCE PROTOCOL Using the NeuroTrac ETSTM in combination of electrostimulation and EMG Biofeedback in the treatment of female urinary incontinence. Anna Pawlaczyk Specialist
Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly. Prapa Pattrapornpisut 7 June 2012
 1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
Ask the Expert - Answers
 Ask the Expert - Answers Q. I had a hysterectomy four years ago. Since then, I have been experiencing progressively increasing urgency. I drink one XL cup of coffee per day but when I have to go, I have
Ask the Expert - Answers Q. I had a hysterectomy four years ago. Since then, I have been experiencing progressively increasing urgency. I drink one XL cup of coffee per day but when I have to go, I have
Urinary Incontinence
 Urinary Incontinence Q: What is urinary Urinary (YOOR-in-air-ee) incontinence (in-kahn-tih-nens) is when urine leaks out before you can get to a bathroom. If you have urinary incontinence, you re not alone.
Urinary Incontinence Q: What is urinary Urinary (YOOR-in-air-ee) incontinence (in-kahn-tih-nens) is when urine leaks out before you can get to a bathroom. If you have urinary incontinence, you re not alone.
Canine Urinary Incontinence
 Urinary Incontinence in the Bitch Laurie Edge-Hughes, BScPT, MAnimSt, CAFCI, CCRT Urinary Incontinence = Involuntary leakage of urine during storage Micturation disorders (non-neurologic): 61% = Urethral
Urinary Incontinence in the Bitch Laurie Edge-Hughes, BScPT, MAnimSt, CAFCI, CCRT Urinary Incontinence = Involuntary leakage of urine during storage Micturation disorders (non-neurologic): 61% = Urethral
Treatments for Urinary Incontinence in Women
 Treatments for Urinary Incontinence in Women National Kidney and Urologic Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH
Treatments for Urinary Incontinence in Women National Kidney and Urologic Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH
1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE
 in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
THE MANAGEMENT OF URINARY INCONTINENCE WITHIN A STROKE UNIT POPULATION REENA DHAMI STROKE CNS EPSOM & ST.HELIER UNIVERSITY HOSPITALS
 THE MANAGEMENT OF URINARY INCONTINENCE WITHIN A STROKE UNIT POPULATION REENA DHAMI STROKE CNS EPSOM & ST.HELIER UNIVERSITY HOSPITALS Definition Urinary Incontinence is AN INABILITY TO HOLD URINE until
THE MANAGEMENT OF URINARY INCONTINENCE WITHIN A STROKE UNIT POPULATION REENA DHAMI STROKE CNS EPSOM & ST.HELIER UNIVERSITY HOSPITALS Definition Urinary Incontinence is AN INABILITY TO HOLD URINE until
MANAGEMENT OF SLING COMPLICATIONS IN FEMALES. Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida
 MANAGEMENT OF SLING COMPLICATIONS IN FEMALES Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida INTRODUCTION The traditional gold standard treatments for stress urinary
MANAGEMENT OF SLING COMPLICATIONS IN FEMALES Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida INTRODUCTION The traditional gold standard treatments for stress urinary
Urinary incontinence. The urinary system
 Urinary incontinence is defined as the involuntary loss of urine from the bladder. Although it is a common condition, most women who suffer from it do not seek help. It is thought that urinary incontinence
Urinary incontinence is defined as the involuntary loss of urine from the bladder. Although it is a common condition, most women who suffer from it do not seek help. It is thought that urinary incontinence
Neurostimulation: Orthopaedic Institute of Ohio 801 Medical Drive Lima, Ohio 45804 419-222-6622
 801 Medical Drive Lima, Ohio 45804 419-222-6622 Neurostimulation is the stimulation of the spinal cord by tiny electrical impulses. An implanted lead (a flexible insulated wire), which is powered by an
801 Medical Drive Lima, Ohio 45804 419-222-6622 Neurostimulation is the stimulation of the spinal cord by tiny electrical impulses. An implanted lead (a flexible insulated wire), which is powered by an
Dr Eva Fong. Urologist Auckland
 Dr Eva Fong Urologist Auckland Urinary incontinence: Treatment options GPCME 2013 Eva Fong Urologist Urinary incontinence Is not normal part of aging or childbearing We can make it better Urinary incontinence:
Dr Eva Fong Urologist Auckland Urinary incontinence: Treatment options GPCME 2013 Eva Fong Urologist Urinary incontinence Is not normal part of aging or childbearing We can make it better Urinary incontinence:
Long Term Acute Care Hospital: Criteria for Admission
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. M issouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. M issouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Transmittal 55 Date: MAY 5, 2006. SUBJECT: Changes Conforming to CR3648 for Therapy Services
 CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 55 Date: MAY 5, 2006 Change
CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 55 Date: MAY 5, 2006 Change
An operation for stress incontinence Tension-free Vaginal Tape (TVT)
 Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Female Urinary Incontinence
 Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. 1 Objectives Review the problem Feel confident
Female Urinary Incontinence Molly Heublein, MD Assistant Professor Clinical Medicine UCSF Women s Health Primary Care Disclosures I have nothing to disclose. 1 Objectives Review the problem Feel confident
INDEPENDENT REVIEW OF TRANSVAGINAL MESH IMPLANTS
 INDEPENDENT REVIEW OF TRANSVAGINAL MESH IMPLANTS Analysis of NHS information on surgery for stress urinary incontinence and pelvic organ prolapse in Scotland Contents 1 Introduction 1 Treatment for these
INDEPENDENT REVIEW OF TRANSVAGINAL MESH IMPLANTS Analysis of NHS information on surgery for stress urinary incontinence and pelvic organ prolapse in Scotland Contents 1 Introduction 1 Treatment for these
Urinary Continence. Second edition FAST FACTS. by Julian Shah and Gary Leach. Anatomy and physiology 7. Investigations and diagnosis 11
 FAST FACTS Urinary Continence Second edition Indispensable Guides to by Julian Shah and Gary Leach Clinical Practice Anatomy and physiology 7 Investigations and diagnosis 11 Detrusor instability 28 Primary
FAST FACTS Urinary Continence Second edition Indispensable Guides to by Julian Shah and Gary Leach Clinical Practice Anatomy and physiology 7 Investigations and diagnosis 11 Detrusor instability 28 Primary
Urinary Incontinence Definitions
 (AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
(AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
An illustrated guide to the management of incontinence.
 An illustrated guide to the management of incontinence. 1 The problem of incontinence The ACA describes incontinence as an involuntary loss of urine and/or bowel motion. The amount can vary from slight
An illustrated guide to the management of incontinence. 1 The problem of incontinence The ACA describes incontinence as an involuntary loss of urine and/or bowel motion. The amount can vary from slight
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Learning Resource Guide. Understanding Incontinence. 2000 Prism Innovations, Inc. All Rights Reserved
 Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
A Physical Therapist s Perspective
 You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
You Can Do Something About INCONTINENCE A Physical Therapist s Perspective American Physical Therapy Association 1 You Can Do Something About Urinary Incontinence Incontinence, involuntary loss of bladder
Clinical Policy Bulletin: Urinary Incontinence
 Urinary Incontinence Page 1 of 57 Clinical Policy Bulletin: Urinary Incontinence Revised February 2015 Number: 0223 (Replaces CPBs 283, 324, and 470) Policy I. Aetna considers multi-channel urodynamic
Urinary Incontinence Page 1 of 57 Clinical Policy Bulletin: Urinary Incontinence Revised February 2015 Number: 0223 (Replaces CPBs 283, 324, and 470) Policy I. Aetna considers multi-channel urodynamic
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Lifestyle and Behavioral Changes Improving Urinary Urgency, Frequency and Urge Incontinence
 Lifestyle and Behavioral Changes Improving Urinary Urgency, Frequency and Urge Incontinence Manage your Fluid Intake: There is no scientific evidence that states we need eight 8 oz. glasses (64 oz.) of
Lifestyle and Behavioral Changes Improving Urinary Urgency, Frequency and Urge Incontinence Manage your Fluid Intake: There is no scientific evidence that states we need eight 8 oz. glasses (64 oz.) of
Primary Care Management Guidelines Female Urinary Incontinence. Overview of Lecture
 Primary Care Management Guidelines Female Urinary Incontinence Professor Don Wilson Department of Women s and Children s Health Dunedin School of Medicine University of Otago GP Teaching for Roy Morris,
Primary Care Management Guidelines Female Urinary Incontinence Professor Don Wilson Department of Women s and Children s Health Dunedin School of Medicine University of Otago GP Teaching for Roy Morris,
Urinary Incontinence. Causes of Incontinence. What s Happening?
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about her grandchildren and going to exercise classes with neighbors. But she s started to have
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about her grandchildren and going to exercise classes with neighbors. But she s started to have
Male Continence Training. AMS 800 Artificial Urinary Sphincter
 Male Continence Training AMS 800 Artificial Urinary Sphincter The AMS Sphincter 800 is the Gold Standard, time-tested surgical solution for control of moderate to severe stress urinary incontinence. Patient
Male Continence Training AMS 800 Artificial Urinary Sphincter The AMS Sphincter 800 is the Gold Standard, time-tested surgical solution for control of moderate to severe stress urinary incontinence. Patient
9/16/2013. Satisfying Solutions: Male Incontinence. Types of Incontinence. Men s Health Solutions for Erectile Dysfunction and Incontinence
 Men s Health Solutions for Erectile Dysfunction and Incontinence Dr. Karl J. Kreder and Dr. Brad A. Erickson Satisfying Solutions: Male Incontinence What is it? Male urinary incontinence is usually caused
Men s Health Solutions for Erectile Dysfunction and Incontinence Dr. Karl J. Kreder and Dr. Brad A. Erickson Satisfying Solutions: Male Incontinence What is it? Male urinary incontinence is usually caused
Management of Neurogenic Bladder Disorders
 Management of Neurogenic Bladder Disorders Andrea Staack, MD, PhD Pelvic Reconstructive Surgery, Urinary Incontinence & Female Urology Department of Urology Loma Linda University, CA What will you learn
Management of Neurogenic Bladder Disorders Andrea Staack, MD, PhD Pelvic Reconstructive Surgery, Urinary Incontinence & Female Urology Department of Urology Loma Linda University, CA What will you learn
