Table of Contents Error! Bookmark not defined.
|
|
|
- Stephany Agatha Copeland
- 10 years ago
- Views:
Transcription
1 Table of Contents EKG TRACING...1 Figure 1 - EKG Tracing... Error! Bookmark not defined. STEP Rate... 1 Figure 2 - Determining the Rate... 1 Step Rhythm... 2 Figure 3 - Determining the Rhythm Source... 2 Step Axis... 2 Figure 4 - The Limb and Augmented Leads in relation to the body... 3 Figure 4 - Computing the Axis... 4 Figure 5 - All limb and augmented leads... 4 STEP Precordial Leads... 5 Figure 6 - The Precordial Leads... 5 STEP Hypertrophy... 5 Figure 7 - Biphasic P-Waves... 6 Figure 8 - RVH... 6 Figure 9 - LVH... 7 STEP Blocks... 7 Figure 10 - AV-Block... 7 STEP Ischemia, Infarct and Injury... 9 Transmural Ischemia... 9 Sub-Endocardial Ischemia Figure 19 - ST-Segment Depression in subendocardial ischemia Step Miscellaneous...11 Ventricular Fibrillation Tachycardia Sinus Tachycardia Digitalis Toxicity Figure 22 - Digitalis Toxicity Hyperkalemia Figure 23 - Peaked-T Waves consistent with Hyperkalemia CREDITS...15 Authors...15 Henry Feldman Mariano Rey, MD Other Contributors...15 Daniel Fisher, MD
2 EKG Tracing Please refer to the EKG tracing below if you are not familiar with the labeling of the EKG waveforms. Step 1 Figure 1- EKG Tracing Rate The first step is to determine the RATE, which can be eyeballed by the following technique. Locate the QRS (the big spike) complex that is closest to a dark vertical line. Then count either forward or backwards to the next QRS complex. For each dark vertical line you pass, select the next number off the mnemonic " " to estimate the rate in beats per minute (BPM). In other words if you pass 2 lines before the next QRS, the heart rate (HR) would be less than 150. Remember that this is merely an estimate. You should use real measurements to determine the exact HR (for precise measurement: each large box represents 200msec and small boxes represent 40msec). As an example of using the mnemonic, in the segment of the EKG below, start at the QRS that lines up with the vertical line at "0". Now counting back each vertical line to the previous EKG " " we notice the HR to be slightly less than 100 (probably around 90-95). Figure 2 - Determining the Rate 1
3 Step 2 Rhythm Next we need to determine the RHYTHM both its source and its regularity. The prime concern is whether the source of the rhythm is the SA node (sino-atrial) or an ectopic pacemaker. To determine whether the source of the rhythm is "sinus" or an ectopic rhythm, you need to look at the relationship of the P-wave, if present, to the QRS-complex. If there is a P wave before each QRS and the P is in the same direction as the QRS, the rhythm can be said to be sinus. For instance note in the EKG segment below that there is a P-wave before each QRS (highlighted in blue) and that it is pointing up as is the QRS segment. Figure 3 - Determining the Rhythm Source Also look at the quality and quantity of P-waves before each QRS. There should only be one P-wave before each QRS. The P-wave should be in only one direction, and not biphasic (except for leads V1 and V2). It should also be closer than 200ms to the QRS. The shape of the P-wave should also be gently rounded and not peaked. Step 3 Axis Next we need to determine the AXIS of the EKG tracing. To do this we need to understand the basic 6 leads and their geometry. The EKG waveform comes from a measurement of surface voltages between 2 leads. A wave that is travelling towards the positive (+) lead will inscribe an upwards deflection of the EKG; conversely a wave traveling away from the positive lead will inscribe a downward deflection. Waves that are traveling at a 90 degree angle to a particular lead will create no deflection and is called an isoelectric lead. As an example in the pictures below, a wave travelling from the head to the feet would be shown as an upwards deflection in AVF, since it is going towards the AVF+ lead. The axis is the sum of the vectors, produced by the ekg leads, to produce a single electrical vector. Remember that a positive signal in Lead-I means that the signal is going right to left; this produces a vector, which if we take all the leads, we can sum. This summed vector should in general be pointing the same direction (down-left) for a normal heart; this makes sense if we think of the electrical conduction system of the heart which sends a signal from the SA node (top right) to the purkinje fibers (bottom left). Don't worry if you still don't get it, we'll give you a visual example further down the page. There are six basic leads discussed below and 6 precordial leads which will be discussed later. The basic leads consist of leads I, II and III and the augmented leads AVR, AVL and AVF. These are present on the basic 3-lead monitors and also on the 12-lead EKG machines. They consist of leads on 2
4 the left and right shoulders and one on the left side of the abdomen (although conceptually they are on the wrists and above the ankle; hence their name "limb leads"). A ground lead is placed on the right ankle. Figure 4 - The Limb and Augmented Leads in relation to the body You will notice that leads I, II and III form the sides of an equilateral triangle, while AVR, AVL and AVF bisect the vertices of the triangle. The easiest way to figure out the axis is to draw a normal X-Y graph and fill in the quadrants that are represented by each lead with a positive deflection. 3
5 There are some tricks to save you time, but first think about a normal EKG plot; in a normal EKG both leads I and AVF will be positive as the signal travels from the SA node (top right of the heart) to the tip of the ventricles (bottom left of the heart). This is a normal axis, and leads us to the rule of thumb, if I and AVF are positive the axis is normal. However, just because this is not the case does not mean that the axis is abnormal! (you need to look at more leads in this case) The normal axis actually allows the signal to travel up to 30 above the X axis and 30 to the left of the Y axis. Let's look at an example below and prove this. Figure 4 - Computing the Axis If the axis is not completely in the bottom left (the patient's left) quadrant (i.e. I and AVF are positive), it is simply a matter of using additional leads to determine the axis. Looking at the map of all the leads, we notice that almost 360 degrees of axis are covered. Use the same axis determination method you used with I and AVF. Figure 5 - All limb and augmented leads 4
6 Step 4 Precordial Leads Understanding the precordial leads and how they align with the heart is critical to understanding the EKG. First let's remember how the heart is located in the chest. Note that it sits flat above the diaphragm on the left side of the chest, and is pointed slightly to the left. This is important in understanding how the precordial leads correlate to the actual heart anatomy. We see below the precordial leads in their relationship to the heart and chest anatomy. Figure 6 - The Precordial Leads V1-V2 are over the right ventricle, while V4-V6 primarily are over the left ventricle. V3 is a transitional lead, and is approximately over the intraventricular septum, so it covers some of both ventricles. Remember that the bulk of the left ventricle is posterior, so feel free to create a V7 and V8 to get more information of the left ventricle. Step 5 Hypertrophy Hypertrophy is the increase in size of the myocytes in the myocardium, leading to thicker walls. It can be non-pathological, as in the case of people who frequently perform isometric exercise (lifting heavy weights, with the straining and Valsalva maneuver, produces an increased afterload). Extending this thought, we can see how hypertrophy can occur in the pathological sense by thinking about increased afterload on the heart as in individuals with high blood pressure which causes a left sided afterload increase. Left Sided afterload increases, such as systemic hypertension or aortic stenosis will cause the left ventricle (LV) to expand in response giving Left Ventricular Hypertrophy (LVH). 5
7 The right side of the heart can also experience afterload. Increased pressure in the pulmonary vessels will cause an increase in afterload (back-pressure) to the right ventricle (RV), leading to an increase in muscle mass of the RV to compensate, leading to Right Ventricular Hypertrophy (RVH). As the ventricles, the atria can also become hypertrophic (dilated), which is visualized as changes to the P-wave. The P-wave can become biphasic in bilateral atrial hypertrophy. The best place to look for Atrial Hypertrophy is in V1, which is mostly over the right atrium, but being the highest placed lead in the chest also gives left sided information as well). Below we see examples of Right and Left Atrial Hypertrophy showing as biphasic P-waves. Figure 7 - Biphasic P-Waves Next we need to examining the ventricles for evidence of hypertrophy there. Since increased muscle mass, logically yields to an increase in the signal (more channels - more current) we would expect to see changes in the QRS complex morphology. For Right Ventricular Hypertrophy we look at V1 (and less so in V2 and V3) and notice that there is a large R-wave (the normal V1 has a small R with a large S) Figure 8 - RVH This increased R height, will taper down, in V2 and V3. Remember that just because you find RVH doesn't mean that the left ventricle is also not hypertrophied, in which case you may not see the normal taper. In Left Ventricular Hypertrophy (LVH), you will have a large S wave in V1 and a large R wave in V5. The actual criteria, are to add the height of S in V1 and the height of R in V5 (in mm) and if the sum is greater than 35mm, then LVH is probable. For instance in the picture below, we measure the heights (23mm in V1 and 17mm in V5) which total greater than 35mm, so we meet a criterion for LVH. 6
8 Step 6 Figure 9 - LVH Blocks A block is an interruption of the normal flow of an electrical impulse traveling down from the SA node to the ventricles. The blocks can occur in the SA and AV nodes as well as in the bundles. SA Node Block consists of a failure of the SA node to transmit an impulse, and is usually seen as a complete pause of 1 beat (i.e. a "skipped beat"); if the pause lasts longer or the morphology of the P wave before and after the pause is different, it probably isn't SA block. This block can occur occasionally in normal patients, and should not necessarily be viewed as pathological. Here is an example of SA node block: Figure 10 - AV-Block AV Node Block is a block which delays the electrical impulse as it travels between the atria and the ventricles in the AV node. Since the P-wave represents the activity of the SA node, and the QRS complex represents the activity of the ventricles, it makes sense that the P-R interval represents the delay through the AV node. The criteria for 1 AV node block is a PR interval greater than.2 seconds (200ms or 1 large box). Below we see an example of 1 AV node block. Figure 11-1 AV Block - PR Interval 200ms 2 AV Block is where there are more than 1 P-wave preceding each QRS complex. The P-waves are spaced in a regular rhythm, but there is no following ventricular response. We see this below where there is a 2:1 ratio of P-waves to each QRS. Note that other ratios do occur (3:1, 4:1, etc...) 2 AV Block with a 2:1 P-wave ratio 3 Block is a complete block of signals from the atria to the ventricles. As such we would expect complete dissociation between the timing of the P-waves and the QRS complexes. The P-waves will 7
9 be in a normal sinus rate, while the QRS's will be either in a nodal rhythm (60bpm) or a ventricular rhythm (30-40bpm). However, the key is the lack of synchronization between the two. The lack of synchronization is what determines whether you are in a 2 AV block with a greater than 1:1 ratio or 3 block. It is important to examine the morphology of the QRS complex; if it is a narrow complex, then the origin is likely to be nodal, while a wide complex is likely to be ventricular, although one should also take the rate into account. Below we see an example of 3 Block with a narrow QRS; note the dissociation between the P-wave rate and the QRS rate. Figure 12-3 Block Bundle Branch Blocks (BB) are blocks within the ventricular bundles, and normally consist of a left or right bundle branch block. You will often hear these erroneously referred to simply as a left or right "bundle", the "block" being superfluous. The blocks can be of the entire ventricular bundle or a fasicle of a given bundle. Here, we are simply going to introduce basic bundle blocks. The key to recognizing a bundle block is to find a R-R' wave; the 2 R waves per complex are really 2 superimposed QRS complexes from each of the ventricles firing separately but very close in time to each other. The criteria consist of a QRS wider than.12 seconds (3mm) and the 2 R waves. In a left bundle block, the left ventricular firing is delayed, while in right bundle block, the right ventricular firing is late. Below we see examples of Right and Left Bundle Branch Blocks. Note the R-R' complex repeating as well as the QRRS complex being wider than 3mm (.12sec). In the Right BBB, the R wave represents the Left Ventricular depolarization, while the R' wave represents the delayed right ventricular response. In the Left BBB, the R wave is the right ventricle and the R' is the left ventricle. Figure 13 - Right Bundle Branch Block (Lead V1) Figure 14 - Left Bundle Branch Block (lead V5) Remember to consider what precordial lead the block is presenting in; if the block morphology presents best in V1-V2, then it is a Right BBB, while a Left BBB pattern is best appreciated in leads V5-V6. Note: the axis will be hard, if not impossible, to accurately determine, as the ventricles are firing asynchronously with each other, altering the normal interventricular phasing. 8
10 Step 7 Ischemia, Infarct and Injury Cardiac Ischemia and infarctions are the most important acute EKG patterns to detect. We will deal with the life threatening arrhythmias, such as Asystole, V-Fib and V-Tach in the next section as they are radically different from normal EKG's, and should be handled separately. When a patient presents to the ER with chest pain, it is important first to immediately perform a complete EKG analysis with the preceding steps, unless a life-threatening rhythm is detected, along with the physical examination and clinical assessment of the patient. Ischemia is when blood flow to the myocardium is insufficient to maintain the metabolic demand of the myocytes. Ischemia can present with symptoms ranging from mild chest discomfort on exertion to the most severe form of ischemia, which results in the crushing chest pain of a infarction; Ischemia may also be silent. Figure 15 - The Range of Perfusion of the Myocardium Surprisingly, the QRS is not the most affected part of the EKG waveform in ventricular ischemia. The ST segment is most often affected in ischemic conditions. We will examine the 2 types of ST-segment changes: elevation and depression. These usually represent transmural ischemia and subendocardial ischemia respectively. Transmural Ischemia The hallmark of acute transmural ischemia (across the heart wall from endocardium to epicardium) is the elevation of the ST segment of the EKG. This is visualized by the ST-segment being raised above the isoelectric baseline. This is due to a higher (more positive) resting voltage of ischemic cells, which cause the ST-segment baseline to be more positive (an upwards deflection). This change in the ST segment is mostly localized in the lead most directly overlying the ischemic myocardial area. The etiology of transmural ischemia is the blood supply failing to feed the myocardium. This may lead to unstable angina, and should be taken very seriously, as this is the condition that progresses to an acute MI. As the ischemia becomes more extensive the ST segment elevation becomes more pronounced. The lead in which the ST elevation appears, allows you to accurately locate the ischemic or infarcted area of ventricular myocardium. If the elevation appears in inferior leads, this indicates an inferior ischemic/infarcted myocardium; the lateral leads, likewise indicate lateral wall ischemia/infarction. Figure 16 - ST-Segment Elevation 9
11 It is important to differentiate pathologic ST segment elevation from non-pathologic J-point elevation. J-point elevation is identified by an elevation of the terminal portion of the QRS which then dips back down towards the baseline before rising back up to the ST segment. This is opposed to the pathological ST-elevation which is visualized as the terminal portion of the QRS going directly up to the T-wave. Figure 17 - J-Point Elevation After the ischemia has progressed to an infarct, and the tissue has scarred, the EKG will show an inverted T wave. A pronounced Q-wave (not normally present) and loss of all or part of the R wave may also present. Sub-Endocardial Ischemia Figure 18 - Q-waves with Inverted T-Waves Let's look at the progression of ischemia in the subendocardium. Relative decreased flow in the subendocardial regions is a normal consequence of the squeezing of the myocardium, which compresses the blood supply to the endocardium during ventricular systole. However, this can also be a pathological condition, expressed in stable-angina. This is a condition where the myocardial demands exceed the coronary artery blood supply (unlike unstable angina which is a supply problem). This is represented on the EKG as ST-segment depression. With ischemia of the subendocardium the ischemic cells become more positive in their resting voltage (due to channel leakage) and this makes the subendocardium more positive; since the endocardium is further away from the precordial leads than the more negative mycardium we see this as a depression (see figure below).unlike elevation, the ST-segment depression is not localizable to a specific lead, but is seen in the leads with the tallest R waves, which are the inferior leads (II, III and AVF and leads V4-V6). Typically, stable angina will self-resolve, however, like elevation, the depression is increased as the myocardial demand increases. Below we see an example of ST-segment depression. Figure 19 - ST-Segment Depression in subendocardial ischemia 10
12 Step 8 Miscellaneous This section will deal with the miscellaneous rhythms that can present often as life threatening arrhythmias, however they don't fall into the simple categories outlined in the previous pages. Ventricular Fibrillation Ventricular Fibrillation (often called V-Fib) is the most life threatening arrhythmia, and is often the end rhythm before the asystole of death. The physiology of this rhythm, is a complete breakdown in the synchronization of the myocardial conduction system; different areas/cells/segments of the heart, are contracting and relaxing with no coordination with other parts. This random quivering results in a loss of cardiac output, resulting rapidly in death if untreated. The EKG pattern of V-Fib is recognized by a total lack of organized activity, ranging from course (large amplitude) to fine (close to asystole) in amplitude. The only "cure" for V-fib is electrical cardioversion (defibrillation). However, before cardioverting a patient, remember to assure yourself, that this is actual cardiac activity, and not an artifact of patient movement (such as a seizure, shivering or Parkinson's disease), electrical interference or other artifacts. Below are examples of course and fine V-Fib. Tachycardia Figure 20 - Course and Fine Ventricular Fibrillation Like any other heart rhythm the origin of the signal can be either atrial or ventricular. The source of a tachycardia, if ventricular, is always pathologic, while non-ventricular tachycardias can be thought of as "sinus" and supraventricular (SVT) rhythms, and may or may not be pathologic. Pathologic tachycardias can arise from multiple causes, such as an ectopic pacemaker cell which we call abnormal automaticity, from reentry around a non-conductive block and by "triggering" by an external source. 11
13 The most common cause of pathologic tachycardias and arrhythmias results from reentry. This is due to a signal splitting around a defect and one side of that split being conducted significantly slower than the other (see below). If the slow signal meet s the fast side ready to be depolarized it can cause both normal and retrograde depolarization. This can cause tachyarrhythmias due to the uncontrolled reentry. Figure 21 - Origin of reentrant arrhythmias Sinus Tachycardia This rhythm originates in the non-pathologic state from an increase in demand for cardiac output, which is successfully met by the heart and whose rhythm originates in the SA node. This is usually a remedy to a systemic process such as by hypovolemia, hypotension, hypoxia, nervousness, medications and exercise. Remember that if the rate is high enough, the P-wave can be obscured in the ST-segment, but is still present; this is an artifact of the EKG machine, and if you set the scanning rate higher, you can reduce this problem. Supraventricular Tachycardias Paroxysmal Atrial Tachycardia (PAT) This arrhythmia is seen with reentry in the atria. There is a circular conductive pathway in the atria, causing reentry to give a rapid tachycardia. There is a single ectopic pacemaker, which can even be the AV node itself. One feature often seen with this tachycardia will be inverted P-waves, due to the source being lower down in the atria. A diagnostic procedure that can be performed to separate this from sinus tachycardia is to do vagal maneuvers, and if the rhythm slows and then resumes after cessation of the maneuvers, sinus rhythm is present. If the rhythm terminates abruptly or there's no change, then it's PAT. Figure 22: Paroxysmal Atrial Tachycardia 12
14 Multifocal Atrial Tachycardia (MAT) This arrhythmia is seen with an ectopic pacemaker somewhere in the atria. The abnormal pacemaker cell, has stopped responding to the overdrive pacing from the sinus node. This causes there to be 2 or more asynchronous pacemakers for the heart. The hallmark of this form of SVT is the 2 or more P-wave morphologies you see; one P-wave from each pacemaker. Surprisingly this rhythm can often be broken by exercise or sinus-tachycardia; the reason for this, is that although the end result of MAT is tachycardia, each of the pacemakers is not tachycardia, it is the sum of their rates that produces the tachycardia. In exercise or other excitatory states, the sinus node will overdrive pace the ectopic cells. Figure 23 - Multifocal Atrial Tachycardia Red=sinus node, Blue=ectopic Ventricular Tachycardia When the rhythm originates in the ventricles, the intrinsic rate or automaticity is below 60 bpm. This can be seen in idioventricular rhythms when the SA or AV node are not the functioning pacemaker of the heart. However, when there is ischemic, infarcted or necrotic conductive tissue around the bundles, there can be a reentry of the downward propagating depolarization, that causes the signal to repeat itself. This causes the very fast rate, as seen in Ventricular Tachycardia (often called V-tach) ; this can be a life threatening condition. The hallmark of ventricular rhythms is the wide QRS complex. Below we see an example of V-Tach, with a ventricular rate of 150bpm. Digitalis Toxicity Figure 24 - Ventricular Tachycardia Digitalis is a very old cardiac drug derived from the Foxglove plant, used in slowing conduction through the AV node, usually in controlling the ventricular rate of atrial fibrillation. It is usually given in cases of atrial fibrillation. Overdoses of digitalis (either in the form of Digoxin or Digitoxin) can have effects ranging from mild 1 AV block to junctional rhythms through fatal arrhythmias. The primary mechanism of action of digitalis is to suppress the Na-K-ATPase pump; this causes the membrane potential to be more positive, allowing for easier reaching of threshold, leading to action potentials. This creates a situation where it is easy to get spontaneous action potentials, leading to arrhythmias. The most noticeable change to the EKG is the "swooping" ST-segment depression. You also may see extended PR intervals or 1 block, although this alone is indistinguishable from primary 1 AV Block. This will also be exacerbated by hyponatremia or hyperkalemia due to the failure of the ATPase pump to reestablish a membrane potential. Below we see an example of the swooping ST-segment. 13
15 Hyperkalemia Figure 25 - Digitalis Toxicity Potassium (K) is one of the 2 ions that make up the bulk of the ion-based membrane potential of cardiac cells (both myocytes and conduction cells). An imbalance of potassium can create a life threatening situation which must be corrected immediately. The most prominent feature of an EKG of a hyperkalemic patient is the peaked-t wave. The other feature of the hyperkalemic EKG is a stretching of entire waveform. Figure 26 - Peaked-T Waves consistent with Hyperkalemia 14
16 Credits Authors Henry Feldman Henry Feldman is a Medical Student in the Class of 2001 at the NYU School of Medicine. He is also a Massachusetts licensed EMT, a Nationally registered EMT as well as being ACLS certified. He is the webmaster for the NYU School of Medicine Student Organization Web Sites. He also produced all the artwork in this publication (except for the Ox-heart by Leonardo DaVinci). He is also an AHA CPR instructor. He can be reached at his [email protected] Mariano Rey, MD Mariano Rey, Class of 1976 at the NYU School of Medicine is the Director of the Bellevue Cardiac Clinic, Director of the NYU Cardiac Rehabilitation and Prevention Center, Director of the first-year Physiology Course, and is an associate professor of the NYU School of Medicine. He is also Director of Nuclear Cardiology and the Cardiac Stress Labratory. He can be reached at his [email protected] Other Contributors Daniel Fisher, MD Daniel Fisher, is a clinical instructor in the Department of Medicine, division of Cardiology. He is also the associate director of the Bellevue Stress Laboratory. He is also the Director of In-patient Services at the NYU Cardiac Rehabilitation and Prevention Center. He acted both as an editor and sounding board for parts of this publication. He can be reached at his [email protected] 15
BIPOLAR LIMB LEADS UNIPOLAR LIMB LEADS PRECORDIAL (UNIPOLAR) LEADS VIEW OF EACH LEAD INDICATIVE ECG CHANGES
 BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
ACLS Chapter 3 Rhythm Review Instructor Lesson Plan to Accompany ACLS Study Guide 3e
 ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Biology 347 General Physiology Lab Advanced Cardiac Functions ECG Leads and Einthoven s Triangle
 Biology 347 General Physiology Lab Advanced Cardiac Functions ECG Leads and Einthoven s Triangle Objectives Students will record a six-lead ECG from a resting subject and determine the QRS axis of the
Biology 347 General Physiology Lab Advanced Cardiac Functions ECG Leads and Einthoven s Triangle Objectives Students will record a six-lead ECG from a resting subject and determine the QRS axis of the
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
RAPID INTERPRETATION OF. EKG s
 Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Electrophysiology Introduction, Basics. The Myocardial Cell. Chapter 1- Thaler
 Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
Understanding the Electrocardiogram. David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem
 Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed
 Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
ST Segment Elevation Nothing is ever as hard (or easy) as it looks
 ST Segment Elevation Nothing is ever as hard (or easy) as it looks Cameron Guild, MD Division of Cardiology University of Mississippi Medical Center February 17, 2012 Objectives 1. Describe the electrical
ST Segment Elevation Nothing is ever as hard (or easy) as it looks Cameron Guild, MD Division of Cardiology University of Mississippi Medical Center February 17, 2012 Objectives 1. Describe the electrical
An ECG Primer. Quick Look. I saw it, but I did not realize it. Elizabeth Peabody
 4 An ECG Primer Quick Look Cardiac Monitoring System - p. 64 ECG Paper - p. 73 Lead Polarity and Vectors - p. 77 Basic ECG Components - p. 79 Heart Rate and Pulse Rate - p. 91 Summary - p. 94 Chapter Quiz
4 An ECG Primer Quick Look Cardiac Monitoring System - p. 64 ECG Paper - p. 73 Lead Polarity and Vectors - p. 77 Basic ECG Components - p. 79 Heart Rate and Pulse Rate - p. 91 Summary - p. 94 Chapter Quiz
Interpreting AV (Heart) Blocks: Breaking Down the Mystery
 Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
Activity 4.2.3: EKG. Introduction. Equipment. Procedure
 Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Systematic Approach to 12 Lead EKG Interpretation
 Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
VCA Veterinary Specialty Center of Seattle
 An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
How to read the ECG in athletes: distinguishing normal form abnormal
 How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
The Basics of 12 Lead EKG s
 EMS Solutions Presents The Basics of 12 Lead EKG s NOTICE: You DO NOT Have the Right to Reprint or Resell this Publication. However, you MAY give this report away, provided you do not change or alter the
EMS Solutions Presents The Basics of 12 Lead EKG s NOTICE: You DO NOT Have the Right to Reprint or Resell this Publication. However, you MAY give this report away, provided you do not change or alter the
Electrocardiography Review and the Normal EKG Response to Exercise
 Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
the basics Perfect Heart Institue, Piyavate Hospital
 ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Objectives. The ECG in Pulmonary and Congenital Heart Disease. Lead II P-Wave Amplitude during COPD Exacerbation and after Treatment (50 pts.
 The ECG in Pulmonary and Congenital Heart Disease Gabriel Gregoratos, MD Objectives Review the pathophysiology and ECG signs of pulmonary dysfunction Review the ECG findings in patients with: COPD (chronic
The ECG in Pulmonary and Congenital Heart Disease Gabriel Gregoratos, MD Objectives Review the pathophysiology and ECG signs of pulmonary dysfunction Review the ECG findings in patients with: COPD (chronic
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams
 Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Evaluation copy. Analyzing the Heart with EKG. Computer
 Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
ECG made extra easy. medics.cc
 ElectroCardioGraphyraphy ECG made extra easy Overview Objectives for this tutorial What is an ECG? Overview of performing electrocardiography on a patient Simple physiology Interpreting the ECG Objectives
ElectroCardioGraphyraphy ECG made extra easy Overview Objectives for this tutorial What is an ECG? Overview of performing electrocardiography on a patient Simple physiology Interpreting the ECG Objectives
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
Basic Cardiac Rhythms Identification and Response
 Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
ECG Measurments and Interpretation Programs
 ECG Measurments and Interpretation Programs Physician s Guide Distributed by Welch Allyn 4341 State Street Road, PO Box 220 Skaneateles Falls, NY 13153-0220 www.welchallyn.com Sales and Service information:
ECG Measurments and Interpretation Programs Physician s Guide Distributed by Welch Allyn 4341 State Street Road, PO Box 220 Skaneateles Falls, NY 13153-0220 www.welchallyn.com Sales and Service information:
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
School of Health Sciences
 School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
Copyright 2006 Blaufuss Multimedia. All rights reserved. Page 1
 Copyright 2006 Blaufuss Multimedia. All rights reserved. Page 1 002 Sinus Rhythm, atrial rate 90 Mobitz II AVB, Ventricular rate 50 Left Atrial Enlargement Left Ventricular Hypertrophy RBBB a) Long R-R
Copyright 2006 Blaufuss Multimedia. All rights reserved. Page 1 002 Sinus Rhythm, atrial rate 90 Mobitz II AVB, Ventricular rate 50 Left Atrial Enlargement Left Ventricular Hypertrophy RBBB a) Long R-R
Interpreting a rhythm strip
 3 Interpreting a rhythm strip Just the facts In this chapter, you ll learn: the components of an ECG complex and their significance and variations techniques for calculating the rate and rhythm of an ECG
3 Interpreting a rhythm strip Just the facts In this chapter, you ll learn: the components of an ECG complex and their significance and variations techniques for calculating the rate and rhythm of an ECG
Lecture Outline. Cardiovascular Physiology. Cardiovascular System Function. Functional Anatomy of the Heart
 Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
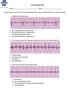 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Chapter 20: The Cardiovascular System: The Heart
 Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
The Electrocardiogram (ECG)
 The Electrocardiogram (ECG) Preparation for RWM Lab Experiment The first ECG was measured by Augustus Désiré Waller in 1887 using Lippmann's capillary electrometer. Recorded ECG: http://www.youtube.com/watch_popup?v=q0jmfivadue&vq=large
The Electrocardiogram (ECG) Preparation for RWM Lab Experiment The first ECG was measured by Augustus Désiré Waller in 1887 using Lippmann's capillary electrometer. Recorded ECG: http://www.youtube.com/watch_popup?v=q0jmfivadue&vq=large
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
ECG INTERPRETATION MANUAL
 Lancashire & South Cumbria Cardiac Network ECG INTERPRETATION MANUAL THE ABNORMAL ECG Lancashire And South Cumbria Cardiac Physiologist Training Manual AV NODAL BLOCKS (HEART BLOCKS) Disturbances of intra
Lancashire & South Cumbria Cardiac Network ECG INTERPRETATION MANUAL THE ABNORMAL ECG Lancashire And South Cumbria Cardiac Physiologist Training Manual AV NODAL BLOCKS (HEART BLOCKS) Disturbances of intra
Monitoring EKG. Evaluation copy
 Monitoring EKG Computer 28 An electrocardiogram, or EKG, is a graphical recording of the electrical events occurring within the heart. A typical EKG tracing consists of five identifiable deflections. Each
Monitoring EKG Computer 28 An electrocardiogram, or EKG, is a graphical recording of the electrical events occurring within the heart. A typical EKG tracing consists of five identifiable deflections. Each
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Banner Staff Service ECG Study Guide
 Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School
 Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
The abbreviation EKG, for electrocardiogram,
 CLIN PEDIATR OnlineFirst, published on January 28, 2010 as doi:10.1177/0009922809336206 Simplified Pediatric Electrocardiogram Interpretation Clinical Pediatrics Volume XX Number X Month XXXX xx-xx 2009
CLIN PEDIATR OnlineFirst, published on January 28, 2010 as doi:10.1177/0009922809336206 Simplified Pediatric Electrocardiogram Interpretation Clinical Pediatrics Volume XX Number X Month XXXX xx-xx 2009
Tips and Tricks to Demystify 12 Lead ECG Interpretation
 Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
22 Arrhythmias. C. Scharf and F. Duru. Siegenthaler, Differential Diagnosis in Internal Medicine (ISBN9783131421418), 2007 Georg Thieme Verlag
 22 22 Arrhythmias C. Scharf and F. Duru 22 712 Arrhythmias 22.1 Differential Diagnosis of Arrhythmias 714 Medical History 714 Clinical Examination 714 Electrocardiogram (ECG) 715 Additional Tools for the
22 22 Arrhythmias C. Scharf and F. Duru 22 712 Arrhythmias 22.1 Differential Diagnosis of Arrhythmias 714 Medical History 714 Clinical Examination 714 Electrocardiogram (ECG) 715 Additional Tools for the
Electrophysiology Daymar College. Lisa H. Young, RN, BSN, MAE 2011
 Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Basics of EKG Interpretation: A Programmed Study - Barbara Ritter Ed.D, FNP
 Basics of EKG Interpretation: A Programmed Study - Barbara Ritter Ed.D, FNP Acknowledgement is given to Leslie K. Muma, MS, RN, NP for assistance in preparation of this learning module. Description The
Basics of EKG Interpretation: A Programmed Study - Barbara Ritter Ed.D, FNP Acknowledgement is given to Leslie K. Muma, MS, RN, NP for assistance in preparation of this learning module. Description The
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
EKG Abnormalities. I. Early repolarization abnormality:
 I. Early repolarization abnormality: EKG Abnormalities A. A normal variant. Early repolarization is most often seen in healthy young adults. Look for ST elevation, tall QRS voltage, "fishhook" deformity
I. Early repolarization abnormality: EKG Abnormalities A. A normal variant. Early repolarization is most often seen in healthy young adults. Look for ST elevation, tall QRS voltage, "fishhook" deformity
Signal-averaged electrocardiography late potentials
 SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
Ischemia and Infarction
 Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Welcome to Vibrationdata
 Welcome to Vibrationdata Acoustics Shock Vibration Signal Processing December 2004 Newsletter Ni hao Feature Articles One of my goals is to measure a wide variety of oscillating signals. In some sense,
Welcome to Vibrationdata Acoustics Shock Vibration Signal Processing December 2004 Newsletter Ni hao Feature Articles One of my goals is to measure a wide variety of oscillating signals. In some sense,
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
2 ECG basics. Leads and planes. Leads. Planes. from different perspectives, which are called leads and planes.
 558302.qxp 3/14/12 10:47 PM Page 12 2 ECG basics One of the most valuable diagnostic tools available, an electrocardiogram (ECG) records the heart s electrical activity as waveforms. By interpreting these
558302.qxp 3/14/12 10:47 PM Page 12 2 ECG basics One of the most valuable diagnostic tools available, an electrocardiogram (ECG) records the heart s electrical activity as waveforms. By interpreting these
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
THE HEART Dr. Ali Ebneshahidi
 THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
ST Segment Monitoring. IntelliVue Patient Monitor and Information Center, Application Note
 ST Segment Monitoring ST/AR Algorithm IntelliVue Patient Monitor and Information Center, Application Note This application note describes principles and uses for continuous ST segment monitoring. It also
ST Segment Monitoring ST/AR Algorithm IntelliVue Patient Monitor and Information Center, Application Note This application note describes principles and uses for continuous ST segment monitoring. It also
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
Atrioventricular (AV) node ablation
 Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ
 «Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
Arrhythmia Monitoring Algorithm
 Arrhythmia Monitoring Algorithm Application Note Introduction The ST/AR (ST and Arrhythmia) algorithm is an ECG algorithm that the HeartStart MRx and XL+ monitor/defibrillators utilize for basic and cardiotach
Arrhythmia Monitoring Algorithm Application Note Introduction The ST/AR (ST and Arrhythmia) algorithm is an ECG algorithm that the HeartStart MRx and XL+ monitor/defibrillators utilize for basic and cardiotach
The new generation in ECG interpretation
 The new generation in ECG interpretation Philips DXL ECG Algorithm, Release PH100B The Philips DXL ECG Algorithm, developed by the Advanced Algorithm Research Center, uses sophisticated analytical methods
The new generation in ECG interpretation Philips DXL ECG Algorithm, Release PH100B The Philips DXL ECG Algorithm, developed by the Advanced Algorithm Research Center, uses sophisticated analytical methods
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD
 92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians
 Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Electrocardiogram and Heart Sounds
 Electrocardiogram and Heart Sounds An introduction to the recording and analysis of electrocardiograms, and the sounds of the heart. Written by Staff of ADInstruments Introduction The beating of the heart
Electrocardiogram and Heart Sounds An introduction to the recording and analysis of electrocardiograms, and the sounds of the heart. Written by Staff of ADInstruments Introduction The beating of the heart
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Feature Vector Selection for Automatic Classification of ECG Arrhythmias
 Feature Vector Selection for Automatic Classification of ECG Arrhythmias Ch.Venkanna 1, B. Raja Ganapathi 2 Assistant Professor, Dept. of ECE, G.V.P. College of Engineering (A), Madhurawada, A.P., India
Feature Vector Selection for Automatic Classification of ECG Arrhythmias Ch.Venkanna 1, B. Raja Ganapathi 2 Assistant Professor, Dept. of ECE, G.V.P. College of Engineering (A), Madhurawada, A.P., India
NHA Certified Clinical Medical Assistant (CCMA)
 NHA Certified Clinical Medical Assistant (CCMA) Detailed Test Plan 150 scored items, 20 pretest Exam Time: 2 hours 50 minutes # items 1. Patient Care 70 A. General Patient Care 53 1. Identify patients
NHA Certified Clinical Medical Assistant (CCMA) Detailed Test Plan 150 scored items, 20 pretest Exam Time: 2 hours 50 minutes # items 1. Patient Care 70 A. General Patient Care 53 1. Identify patients
Note: The left and right sides of the heart must pump exactly the same volume of blood when averaged over a period of time
 page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
The choice for quality ECG arrhythmia monitoring
 GE Healthcare EK-Pro The choice for quality ECG arrhythmia monitoring David A. Sitzman, MSEE. Mikko Kaski, MSAM. Ian Rowlandson, MSBE. Tarja Sivonen, RN. Olli Väisänen, MD, PhD. Clinical care environments
GE Healthcare EK-Pro The choice for quality ECG arrhythmia monitoring David A. Sitzman, MSEE. Mikko Kaski, MSAM. Ian Rowlandson, MSBE. Tarja Sivonen, RN. Olli Väisänen, MD, PhD. Clinical care environments
