Research Article. Abstract. Introduction
|
|
|
- Emily Lora Nicholson
- 8 years ago
- Views:
Transcription
1 Research Article Activation of Tumor-Associated Macrophages by the Vascular Disrupting Agent 5,6-Dimethylxanthenone-4-Acetic Acid Induces an Effective CD8 + T-Cell Mediated Antitumor Immune Response in Murine Models of Lung Cancer and Mesothelioma Arminder S. Jassar, 1 Eiji Suzuki, 1 Veena Kapoor, 1 Jing Sun, 1 Michael B. Silverberg, 1 Lumei Cheung, 1 Marie D. Burdick, 2 Robert M. Strieter, 2 Lai-Ming Ching, 3 Larry R. Kaiser, 1 and Steven M. Albelda 1 1 Thoracic Oncology Research Laboratory, University of Pennsylvania Medical School, Philadelphia, Pennsylvania; 2 Division of Pulmonary and Critical Care Medicine, Department of Medicine, University of California Los Angeles, Los Angeles, California; and 3 Auckland Cancer Society Research Centre, Faculty of Medical and Health Sciences, University of Auckland, Auckland, New Zealand Abstract 5,6-Dimethylxanthenone-4-acetic acid (DMXAA) is a small molecule in the flavanoid class that has antitumor activity thought to be due to ability to induce high local levels of tumor necrosis factor (TNF)-A that disrupt established blood vessels within tumors. The drug has completed phase 1 testing in humans and is currently in phase 2 trials in combination with chemotherapy. Although characterized as a vascular disrupting agent, there are some studies suggesting that DMXAA also has effects on the immune system that are important for its efficacy. The goal of this study was to carefully define the immune effects of DMXAA in a series of murine lung cancer and mesothelioma cell lines with varying immunologic characteristics. We show that DMXAA efficiently activated tumor-associated macrophages to release a variety of immunostimulatory cytokines and chemokines, including TNF-A; IFN-inducible protein-10; interleukin-6; macrophage inflammatory protein-2; monocyte chemotactic protein-1; and regulated on activation, normal T-cell expressed, and secreted. DMXAA treatment was highly effective in both small and large flank tumors. Animals cured of tumors by DMXAA generated a systemic memory response and were resistant to tumor cell rechallenge. DMXAA treatment led to initial tumor infiltration with macrophages that was followed by an influx of CD8 + T cells. These CD8 + T cells were required for antitumor efficacy because tumor inhibitory activity was lost in nude mice, mice depleted of CD8 + T cells, and perforin knockout mice, but not in CD4 + T-cell depleted mice. These data show that activation of tumor-associated macrophages by DMXAA is an efficient way to generate a CD8 + T-cell dependent antitumor immune response even in animals with relatively nonimmunogenic tumors. Given these properties, DMXAA might also be useful in boosting other forms of immunotherapy. (Cancer Res 2005; 65(24): ) Introduction Most clinically effective anticancer therapies are based on their ability to directly kill dividing tumor cells. However, therapies are Requests for reprints: Steven M. Albelda, Thoracic Oncology Research Laboratory, University of Pennsylvania Medical School, BRB II/III, 421 Curie Boulevard, Philadelphia, PA Phone: ; Fax: ; albelda@mail.med.upenn.edu. I2005 American Association for Cancer Research. doi: / can now being developed that target other cells within the tumor. Possible strategies for antitumor therapy include activating the tumor-associated macrophages (1 3) or targeting the tumor vasculature (4). Compared with the normal tissue beds, the vasculature in tumors exhibits an increased rate of proliferation, structural differences, and expression of unique genes and gene products (5). Tumor endothelium has been successfully targeted by drugs that inhibit angiogenesis. The efficacy of an antivascular endothelial growth factor (VEGF) antibody to inhibit tumor angiogenesis has recently been shown in colon and lung cancer (6, 7). Drugs classified as vascular disrupting agents have also been developed that can specifically affect established tumor vessels (8). Vascular disrupting agents are distinct from antiangiogenic agents in that they target existing tumor vessels rather than prevent growth of new vessels. One class of small molecule vascular disrupting agents under study are tubulin-depolymerizing agents, such as the Combretastatins (natural products from the African willow tree; ref. 9). Another group of drugs being investigated for their antivascular properties is the flavone acetic acid (FAA) derivatives (10). Flavanoids have a unique mechanism of action and are believed to exert their effects primarily by inducing localized release of TNF-a and other cytokines within tumor tissue. A more potent analogue of FAA, called 5,6-dimethylxanthenone-4-acetic acid (DMXAA), has been extensively studied (10, 11). Treatment of tumor-bearing mice with DMXAA results in a rapid reduction in tumor blood flow followed by tumor necrosis with only a rim of viable tumor tissue remaining by 24 hours. Despite these viable cancer cells, smaller tumors can be eradicated, although in larger tumors, cures are usually not achieved, perhaps because cells in this rim are capable of rapid proliferation. DMXAA is in early clinical trials and seems to be well tolerated, with some patients experiencing disease stability (12, 13), a reduction of tumor blood flow (12), and localized increases in TNF-a activity (10). Although flavanoids are classified as vascular disrupting agents, studies of mice treated with flavone acetic acid suggested that effects on the immune system were also important. This seems reasonable given their ability to both induce tumor necrosis and to stimulate an array of cytokines and chemokines. FAA was shown to activate natural killer cells, although this did not seem to mediate hemorrhagic necrosis (14, 15). However, the role of the acquired immune system in the effects of flavanoids remains uncertain. A central role for T cells Cancer Res 2005; 65: (24). December 15,
2 DMXAA Activates Tumor Macrophages and T Cells was suggested by Pratesi et al. (16) and Bibby et al. (17) who found that FAA lost much of its therapeutic effect when mouse tumor cells (CT26 or MAC26 colon cancer cells) were grown in nude or thymectomized mice versus syngeneic hosts despite the fact that hemorrhagic necrosis was still seen. This same group also saw no effect of DMXAA on MAC15A tumors grown in nude mice with good efficacy in syngeneic mice (18). In marked contrast, both DMXAA and FAA had good antitumor activity against mouse colon 38 tumor explants that were grown in nude mice, or thymectomized mice, although the percentage of cures were decreased compared with that in euthymic mice (19). Moreover, immunosuppression with high-dose cyclosporine only altered the time that that colon 38 tumor explants took to completely regress but did not reduce the number of complete regressions obtained with DMXAA (20). The specific role of T cells is also unclear. In the studies of Pratesi et al. (16), depletion of CD8 + T cells had no effect on efficacy, but antitumor activity was lost after depletion of CD4 + T cells. In contrast, studies examining the effects of FAA combined with interleukin (IL)-2 in the murine renal cell carcinoma (RENCA) model by Franco et al. (21) showed that depletion of CD4 + T cells had a partial effect on efficacy, whereas depletion of CD8 + T cells completely abrogated antitumor effects. Additionally, although both tumor graft tissue and host stromal tissue have been implicated as producers of cytokines in response to DMXAA, a clear cellular source has not been identified (22, 23). Thus, the role of the immune system in mediating the effects of DMXAA is not well defined. However, clarification of this question is important for a number of reasons. First, a more complete understanding of the mechanisms by which DMXAA exerts its affects could help target particular tumors that might be more amenable to therapy or in designing improved dosing schedules and treatment regimens. Second, if immune effects are induced, DMXAA could potentially be combined with a variety of other immune modulating therapies that could synergize with its activities. The goal of this study was to identify the key effector cells and carefully define the role of immune system in mediating the effects of DMXAA in a series of murine thoracic tumors with varying immunologic characteristics. We show that DMXAA efficiently activates tumor-associated macrophages to release a variety of immunostimulatory cytokines and chemokines. DMXAA treatment was highly effective in both small and large flank tumors, leading to initial tumor infiltration with macrophages followed by CD8 + T cells. These CD8 + T cells were required for antitumor efficacy because tumor inhibitory activity was lost in nude mice, mice depleted of CD8 + T cells, and perforin knockout mice but not in CD4 + T-cell-depleted mice. The ability of DMXAA to activate tumor macrophages and create a tumor microenvironment that is conducive to antitumor immune responses suggests that it could also be a useful adjunct to immunotherapy. Materials and Methods Cell lines. AB12 (a murine mesothelioma cell line; ref. 24) and L1C2 (a murine bronchoalveolar carcinoma cell line; ref. 25) are syngeneic to BALB/c mice. Lewis lung carcinoma (LLC) cells (syngeneic to C57/B6 mice) and the 2H-11 and H5V mouse endothelial cell lines were purchased from the American Type Culture Collection (ATCC, Manassas, VA). AB12, L1C2, LLC, 2H-11, and H5V cells were cultured and maintained in high-glucose DMEM (Mediatech, Washington, DC) supplemented with 10% fetal bovine serum (FBS), 2 mmol/l glutamine, 100 units/ml penicillin, and 100 Ag/mL streptomycin. The TC-1 cell line, derived from transformed primary lung epithelial cells of C57/B6 mice, was obtained from ATCC. TC-1 cells were cultured in RPMI 1640 supplemented with 10% FBS, 2 mmol/l glutamine, 100 units/ml penicillin, and 100 Ag/mL streptomycin. All cell lines were regularly tested and maintained negative for Mycoplasma spp. 5,6-Dimethylxanthenone-4-acetic acid. The sodium salt of DMXAA was synthesized at the Auckland Cancer Society Research Center (26). DMXAA was formulated in normal saline and administered by i.p. injections at a dose of 18 mg/kg in 200 AL saline. In vitro cell proliferation assay. To evaluate the direct antiproliferative effects of DMXAA, cells were seeded in 96-well plates at a density of cells per well. Twenty-four hours later, medium containing various concentrations of DMXAA was added. Survival of treated cells was compared with untreated cells 24 hours after addition of DMXAA using the MTS assay, a colorimetric test for the quantification of cell viability and proliferation (MTS Cell Proliferation Assay; Promega Corp., Madison, WI). Table 1. DMXAA up-regulates mrna for cytokines and chemokines in the tumors Cytokine/chemokine Experiment 1 (fold change F SE) Experiment 2 (fold change F SE) Average fold change IP F F RANTES 8.2 F F IL F F IFN-g 18.4 F F TNF-a 12.8 F F MIP-1a 5.6 F F MCP F F INOS 1.7 F F MIG 4.2 F F ICAM-I 2.3 F F NOTE: Flank L1C2 tumors were established by s.c. injection in mice. The mice were treated with DMXAA i.p. when the tumor size was f200 mm 3. Two hours later, tumors from control and DMXAA-treated mice were harvested and RNA was isolated. Semiquantitative analysis of gene expression was done using real-time RT-PCR. cdna concentrations from each pool were normalized using b-actin as a control gene. Relative level of expression of each of the selected genes ( fold change in DMXAA-treated versus control) was determined. Each sample was run in triplicate Cancer Res 2005; 65: (24). December 15, 2005
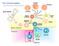
3 Cancer Research Figure 1. DMXAA up-regulates production of proinflammatory cytokines and chemokines in tumors. BALB/c mice with established L1C2 tumors were treated i.p. with either saline (Control) or 18 mg/kg DMXAA. A, tumors were harvested from control and DMXAA-treated mice (n = 3) and chopped into small pieces. Supernatants were collected 5 hours later and TNF-a levels were ascertained by ELISA and standardized to total protein levels. Columns, mean TNF-a (pg/ml/mg protein); bars, SE. B, to assess cytokine/chemokine levels within tumors, tumors (n = 6) were harvested 6 hours after i.p. injection of DMXAA, homogenized, and mediator levels were measured using a Luminex bead assay. Columns, fold change (DMXAA-treated versus control); bars, SE. *, P < 0.05, significantly different than controls. C, to identify the source of cytokines, tumors were harvested from L1C2-bearing (i) or TC-1-bearing (ii) mice (n = 6) and digested. Macrophages were isolated using CD11b magnetic beads and equal numbers were incubated with DMEM (Control) or DMXAA (10 Ag/mL) for 5 hours. TNF-a was measured in the supernatant by ELISA. Columns, average of two measurements done on cells aggregated from six mice each. Mice. Pathogen-free female BALB/c, BALB/c nude, and C57/B6 mice (6-8 weeks old) were purchased from Charles River Laboratories (Wilmington, MA). Perforin knockout mice on a C57/B6 background were obtained from Taconic Laboratories (Germantown, NY). Animals were housed in the animal facility at the Wistar Institute (Philadelphia, PA). The animal use committees of the Wistar Institute and University of Pennsylvania approved all protocols in compliance with the care and use of animals. Animal tumor models. To establish tumors, a single cell suspension of 10 6 tumor cells in 100 AL serum-free medium was injected s.c. into mice flanks. Tumors were measured twice weekly and volumes were estimated using the formula 3.14 [largest diameter (perpendicular diameter) 2 ]/6. Treatment was administered when tumors were f200 mm 3 in size and mice followed for tumor growth. Mice were sacrificed when the tumors became >10% body weight or the mice showed signs of distress. Real-time reverse transcription-pcr in tumors. To evaluate the effect of DMXAA on expression level of selected cytokine and chemokine mrnas in tumors, L1C2 tumors from control and DMXAA-treated mice were harvested 2, 4, 8, and 24 hours after DMXAA treatment and homogenized in TRIzol Reagent (Invitrogen, Carlsbad, CA). Three micrograms of RNA from the each tumor were reverse-transcribed using 0.5 Ag oligo(dt) (Promega), 10 mmol/l deoxynucleotide triphosphates (Clontech, Palo Alto, CA), and 1 unit of Powerscript Reverse Transcriptase in 5 First-Strand Buffer and 100 mmol/l DTT (Clontech) for 80 minutes at 42jC. Primers were designed using the protocol available in Sambrook and Russell (27). Primer sequences can be obtained from the authors upon request. Semiquantitative analysis of gene expression was done using a Cepheid Smart Cycler (Sunnyvale, CA) following the protocol of the manufacturer for SYBR green kit supplied by Roche. cdna concentrations from each pool were normalized using b-actin as a control gene. Relative level of expression of each of the selected genes ( fold change in DMXAA-treated versus control) was determined. Each sample was run in triplicate. The 2-hour time point was found to show maximal responses and the experiment was repeated at this time point (data presented for this time point only). Protein studies for cytokine and chemokine levels. The amount of TNF-a secreted by tumors activated by DMXAA was quantified using an ELISA kit to detect murine TNF-a according to the instructions of the manufacturer (BD OptEIA ELISA set, BD Biosciences PharMingen, San Diego, CA). Briefly, mice bearing L1C2 flank tumors were treated with DMXAA and tumors were harvested 2 and 21 hours later. These tumors were chopped into small pieces and immersed in serum-free DMEM containing 50 mg/l polymyxin B (Sigma-Aldrich, St. Louis, MO) in 48-well plates for a further 3 hours. The supernatant was then collected and tumors were weighed. Polymyxin was added because previous studies have shown that endotoxin contamination can stimulate DMXAA-mediated cytokine secretion (28). Note that there was no DMXAA in culture medium and the tumors were treated with DMXAA only in vivo. Preliminary studies showed Cancer Res 2005; 65: (24). December 15,
4 DMXAA Activates Tumor Macrophages and T Cells that the 5 hours (2 hours in vivo + 3 hours in culture medium) time point showed higher levels of TNF-a. Therefore, in replicate experiments, only this time point was used. The supernatants were spun at 14,000 rpm for 10 minutes and then aliquoted at 80jC until use. To compare changes in cytokine and chemokine mrna expression with protein levels within tumors, mice bearing L1C2 flank tumors were treated with DMXAA. After harvesting at 6, 24, and 48 hours, the tumors were sonicated for 30 seconds in 1 ml of complete buffer (50 ml PBS containing one tablet of antiprotease cocktail, Roche, Indianapolis, IN). Tissues were then spun at 3,000 rpm for 10 minutes and filtered through a 1.2 Am syringe filter unit. Total protein in each sample was determined. Mouse cytokine expression was measured using a multiplex Luminex bead assay system as previously described (29). Samples were incubated for 2 hours at room temperature with a mixture of anti-kc/cxcl1; IL-6; monocyte chemotactic protein-1 (MCP-1)/CCL2; ITAC/CXCL11; regulated on activation, normal T-cell expressed, and secreted (RANTES)/CCL5, macrophage inflammatory protein-2 (MIP-2)/CXCL2/3; and IFN-inducible protein-10 (IP-10)/CXCL10 beads in a 96-well plate. A mixture of the same panel of biotinylated antibodies was added to each well and the plate was incubated at room temperature for 1.5 hours. Streptavidin-phycoerythrin was added to the wells and the plate was incubated for 30 minutes. Next, 0.2% paraformaldehyde was added to the wells and the plate was read on a Luminex 100 IS instrument. The concentration of cytokines was determined from a standard curve assayed at the same time with known amounts of recombinant proteins. Data from the 6-hour time point showed maximal values and is presented here. Isolation of macrophages from tumors. L1C2 and TC-1 flank tumors were harvested from BALB/c and C57/B6 mice respectively, chopped, and digested with 1 mg/ml DNase I and 2 mg/ml collagenase type IV (Sigma, St. Louis, MO) at 37jC for 1 hour. Six to eight tumors were pooled together to obtain the required yield of cells. The resulting mixture was filtered and washed thrice in medium containing 50 mg/ l polymyxin B. Polymyxin B has no effect on the ability of DMXAA to induce TNF-a; however, because mouse macrophages are very sensitive to low amounts of lipopolysaccharide contamination, it was routinely included in experimental medium. Cells were sorted for macrophages using CD11b magnetic beads (Miltenyi Biotec, Inc., Auburn, CA) and a relatively pure population (f95%) of macrophages was obtained. Both CD11b-positive and CD11b-negative cells were collected and plated in 12- well plates at concentration of cells per well in 500 AL of control DMEM or medium containing DMXAA (10 Ag/mL). Cells were incubated for 5 hours at 37jC, supernatants were collected and frozen at 80jC until use. The TNF-a level in the supernatants were measured by ELISA. Immunohistochemical studies. Animals bearing flank tumors were treated with i.p. injections of DMXAA. Three mice were euthanized at different time points, tumors were harvested and immediately placed in Tissue-Tek OCT compound (Sakura Finetek USA, Inc., Torrance, CA) to be stored at 80jC. Five-micrometer sections were cut. Monoclonal antibodies against leukocytes (anti-cd45), macrophages (anti-cd11b), and CD8 + cells (anti-cd8) were obtained from BD Biosciences and immunohistochemical staining was done according to established protocols. Tumor cell infiltrate was quantified by counting the number of positively staining cells in multiple fields (>5) on multiple slides per high-powered (40) field. In vivo depletion of CD4 + and CD8 + T cells. To deplete CD4 + or CD8 + T cells, mice were injected i.p. with monoclonal antibodies purified from the anti-cd4 hybridoma GK1.5 or the anti-cd8 hybridoma , respectively (both obtained from ATCC). Mice were injected i.p. with 300 Ag of purified antibody in 200 AL of PBS. Antibody was administered 3 days and 1 day before tumor cell injection. Thereafter, a maintenance dose of 300 Ag was delivered every 6th day to ensure persistent depletion of targeted Figure 2. DMXAA has significant antitumor effects in murine mesothelioma and non small cell lung cancer tumors grown in syngeneic mice. Immunocompetent mice (five mice per group) with established LLC, L1C2, TC-1, and AB12 tumors were treated with DMXAA (18 mg/kg i.p.) when they were either relatively small ( mm 3 ; A and B) or larger ( mm 3 ; C and D). Tumor growth curves (A and C) or measured tumor volumes at 22 to 32 days after implantation (B and D) of both the small and the large LLC, L1C2, TC-1, and AB12 tumors were significantly smaller in the DMXAA-treated mice than in the control mice. Points and columns, mean volume (mm 3 ); bars, SE. *, P < Arrow, time of treatment with DMXAA Cancer Res 2005; 65: (24). December 15, 2005
5 Cancer Research Figure 3. DMXAA causes extensive tumor necrosis and a biphasic cellular influx into the tumor. A, wild-type mice. Mice bearing either LLC (A-B and E-P) or TC-1 (C-D) tumors were treated with DMXAA and tumors were harvested at 24 hours, 48 hours, and 7 days after treatment for histology and immunohistochemical studies. By H&E staining, both the LLC (A and B) and TC-1 (C and D) tumors showed presence of a significant areas of necrosis with peripheral sparing of tumor tissue at 24 hours after treatment (arrowheads). Immunohistochemical studies done in LLC tumors over a time course of 24 hours to 7 days showed a heavy infiltration of white cells (stained with anti-cd45 antibody) into tumor (E-H). Most of these cells were macrophages (stained with anti-cd11b; I-L). CD8 + T cells were scant in the tumors initially (M and N) but appear at the periphery of the tumor at day 3 (O, arrows) and infiltrate into the tumor by day 7 (P). B, CD8 + T-cell-depleted mice. LLC flank tumors were established in mice depleted of CD8 + T cells. These mice were treated with DMXAA and tumors were harvested 48 hours after treatment. H&E and immunohistochemical staining was done. Compared with controls (A), the DMXAA-treated tumors (B) showed the presence of large area of necrosis, which was sharply demarcated from a rim of viable tissue (arrowheads). CD11b immunostaining revealed a significant macrophage influx into the DMXAA-treated tumors (D) compared with the controls (C). lymphocyte population. For some experiments, the schedule for antibody administration varied with experimental goals; such variation has been described in Results. CD4 + and CD8 + lymphocyte depletion was confirmed by flow cytometry of splenic cell suspension (data not shown). Statistical analysis. Unless otherwise noted, data comparing differences between two groups were assessed using unpaired Student s t test. Multiple comparisons were made using ANOVA with appropriate post hoc testing. Differences were considered significant when P < Cancer Res 2005; 65: (24). December 15,
6 DMXAA Activates Tumor Macrophages and T Cells Results Murine tumor and tumor endothelial cell lines are relatively resistant to 5,6-dimethylxanthenone-4-acetic acid in vitro. Three murine lung cancer cell lines and one murine mesothelioma cell line were exposed to various concentrations of DMXAA to determine direct antiproliferative effects. The concentrations of DMXAA, which inhibited the proliferation of tumor cells by 50% compared with the control cells (IC 50 ) for L1C2, LLC, TC-1, and AB12 cell lines were 310, 285, 252, and 516 Ag/mL, respectively. DMXAA may cause tumor vascular disruption by directly acting on tumor endothelium (30), so we also checked the direct antiproliferative effect of DMXAA on the H5V and 2H11 tumor endothelial cell lines in vitro. The IC 50 of DMXAA for 2H11 cells was 665 Ag/mL and was >1,000 Ag/mL for H5V cells. Because administration of maximal dose of DMXAA to mice corresponds to a maximal free drug concentration of 9 Ag/mL in the plasma (31), it is unlikely that direct tumor or tumor endothelial cell killing plays a significant role in DMXAA activity in vivo. 5,6-Dimethylxanthenone-4-acetic acid markedly up-regulates mrna levels of proinflammatory and chemoattractant cytokines/chemokines in tumors. To confirm and extend previous work showing up-regulation of mrna for various cytokines in tumors in response to DMXAA (32), we did real-time reverse transcription-pcr (RT-PCR) studies on control and DMXAA-treated L1C2 tumors 2 hours after DMXAA administration using primers for several cytokines and chemokines. The mrnas for IP-10, RANTES, IL-6, IFN-g, TNF-a, MIP-1a, MCP-1, inos, Mig, and intercellular adhesion molecule (ICAM) were up-regulated between 73-fold and 2-fold (Table 1). 5,6-Dimethylxanthenone-4-acetic acid up-regulates production chemokines and cytokines in tumors. To ascertain if mrna up-regulation correlated with protein up-regulation, we evaluated the levels of some of the proteins secreted by tumors after treatment with DMXAA. We did ELISA to quantitate TNF-a secreted by tumors. L1C2 tumors treated with DMXAA showed TNF-a levels of 283 ng/g total protein compared with only 5 ng/g in the control tumors (56-fold increase; Fig. 1A). We also tested for up-regulation of other proteins in tumor homogenates using a Luminex bead assay and found that IP-10 (CXCL10), IL-6, KC (CXCL1), MIP-2 (CXCL2/3), MCP-1 (CCL2), and RANTES (CCL5) were significantly up-regulated (12 to 2 fold) in DMXAA-treated tumors (Fig. 1B). Macrophages are the major source of tumor necrosis factor-a in the tumors. To test the hypothesis that the major source of TNF-a in the tumors were macrophages, we isolated CD11b-positive and CD11b-negative cells from L1C2 and TC-1 flank tumors. Both the CD11b-positive and CD11b-negative cells were exposed to either DMEM or DMEM containing 10 Ag/mL DMXAA, a concentration previously shown to be optimal for in vitro studies with DMXAA (33). Supernatants were collected 5 hours later and TNF-a levels were determined by ELISA. The supernatants from CD11b-positive cells (macrophages) extracted from both the tumor cell types exposed to DMXAA showed very high levels of TNF-a (1,565 pg/ml from L1C2 tumors and 1,125 pg/ml from TC-1 tumors; Fig. 1C). The CD11b-negative cells secreted minimal amounts of TNF-a in the supernatant. These data show that the main cellular source of TNF-a is the tumorassociated macrophages and that DMXAA possesses the ability to trigger these macrophages to secrete TNF-a. 5,6-Dimethylxanthenone-4-acetic acid shows significant antitumor effects in AB12, L1C2, LLC, and TC-1 tumors grown in syngeneic mice. DMXAA has been shown to be highly effective in some cancer models. We evaluated the efficacy of DMXAA in our syngeneic lung cancer (LLC, TC-1, and L1C2) and mesothelioma (AB12) models. In small pilot experiments, a dose of 18 mg/kg was found to be optimal for our experiments (data not shown). Mice bearing flank tumors were treated with DMXAA when the average tumor size was between 120 and 300 mm 3. DMXAA was very effective in causing reduction in tumor size in all four cell lines. Cure rates of 100% (AB12), 80% (LLC), 100% (TC1), and 60% (L1C2) were obtained (Fig. 2A and B). To ascertain the dependency of tumor size on effectiveness of treatment, we treated large tumors (between 440 and 600 mm 3 ) with DMXAA. We found that even in large tumors, DMXAA was effective in restricting tumor growth. The average tumor size in the treated animals compared with controls was 49% (TC1), 36% (L1C2), and 38% (LLC; Fig. 2C and D). Grossly, DMXAA-treated tumors had a deep blue, congested appearance noticeable at 4 hours. Over the next 2 days, these tumors developed frank ulcers. In smaller tumors, this ulcer was later covered with a scab, which eventually fell off leaving behind intact skin with no residual tumor. In larger tumors, there was a macroscopically visible rim of viable tumor tissue surrounding the Table 2. Quantification of tumor cell infiltration after DMXAA treatment Cells per high power (40) field (mean F SE) Control 24 h post DMXAA 72 h post DMXAA 7 d post DMXAA CD11b + cells in wild-type mice 12.8 F F 8* 102 F 11* 159 F 14* CD11b + cells in CD8-depleted mice 19 F F 7* ND ND CD8 + cells in wild-type mice 14 F 8 ND ND 74 F 5* NOTE: Mice bearing LLC flank tumors were treated with DMXAA. Tumors were harvested and flash frozen at 24 hours, 72 hours, and 7 days after treatment. Frozen sections were cut and stained with antibodies against macrophages (CD11b) or T-cells (CD8). The number of positively staining cells per 40 high-power field (mean F SE) are shown. CD8 cells were not quantified in the 24- and 72-hour samples because the T-cell distribution was very inhomogeneous with cells only at the periphery of the tumors (see Fig. 3). CD11b cells were also measured in tumor-bearing mice depleted of CD8 T cells. CD8 depletion had no effect on macrophage accumulation. Abbreviation: ND, not determined. *P < 0.05 compared with control Cancer Res 2005; 65: (24). December 15, 2005
7 Cancer Research ulcer, which subsequently became thicker, and tumors began to regrow after a brief posttreatment growth arrest. 5,6-Dimethylxanthenone-4-acetic acid causes a biphasic influx of leukocytes into tumors. To assess the tumors microscopically, we did staining on tumor sections. Flank LLC tumor-bearing mice were treated with DMXAA and tumors harvested at 24, 48, and 72 hours and 7 days after treatment. H&E staining showed the presence of a large area of central necrosis with a diffuse infiltration of white cells into the tumor. A peripheral rim of intact tumor tissue was observed (Fig. 3A, A-D). Antibodies against CD45 (pan-wbc marker) showed that white cells infiltrated into the tumors at 24 hours and were present at 7 days after treatment (Fig. 3A, E-H). CD11b staining revealed that most of the infiltrating white cells were macrophages. Macrophage infiltration was significantly (P < 0.05) increased in these tumors 24 hours after DMXAA administration and remained elevated up to 7 days after treatment (Fig. 3A, I-L). Table 2 quantifies this infiltration by demonstrating the number of CD11b cells per high power field (40). There were very few CD8 + T cells at 24 and 48 hours after DMXAA treatment. The CD8 + cells began to appear, mostly at the periphery of the tumors, at 72 hours and were seen infiltrating into the tumors in significant numbers at 7 days posttreatment (P < 0.05 compared with baseline; Fig. 3A, M-P; Table 2). Tumors with the most prominent CD8 + T-cell infiltrates were smaller than the tumors without these infiltrates. These data show a shift, with time, in the spectrum of cell types involved in the antitumor effects: macrophages predominating the early posttreatment phase and CD8 + T cells being important in the later stages. Cured animals are resistant to tumor growth when rechallenged with same tumor type. Influx of CD8 + T cells into the tumors after DMXAA treatment suggested a role of the adaptive immune system in the process of tumor eradication. We, therefore, looked for generation of a memory response. Animals that were injected with flank tumors and were cured by DMXAA treatment were rechallenged with cells of same tumor cell type injected into the opposite flank. Naïve animals were injected at the same time and tumor growth compared between the two groups. The growth of tumors in the rechallenged animals was significantly inhibited when compared with the naïve controls. Whereas tumors were detected in all of the control animals, 0/5 AB12, 1/4 L1C2, and 0/8 LLC tumors grew in the rechallenged mice on day 14 after rechallenge. These data indicate generation of a systemic immune response that develops after treatment with DMXAA resulting in the rejection of rechallenge with tumor cells. Antitumor efficacy of 5,6-dimethylxanthenone-4-acetic acid is lost in immunodeficient mice. Prevention of tumor growth in rechallenged mice suggested that systemic immunity was generated in response to DMXAA treatment. Therefore, we studied the effects of DMXAA on tumors grown in mice lacking functional T-cells. L1C2, LLC, and TC1 flank tumors were grown in athymic nude mice and DMXAA was administered when the mean tumor volume was 270 to 386 mm 3. The efficacy of DMXAA was almost completely lost in these mice in all the three cell lines. As shown in Fig. 4A, B, andc, the average tumor volume in the treated group compared with control was 100%, 87%, and 91% in L1C2, LLC, and TC1 tumorbearing mice, respectively. These data show a crucial role for T-cellmediated immunity in mediating antitumor effects of DMXAA. CD8 + T lymphocytes mediate the antitumor effects of 5,6- dimethylxanthenone-4-acetic acid. To further identify the T-cell subset involved in mediating effects of DMXAA, we used antibodies to specifically deplete either CD8 + or CD4 + T lymphocytes. Flank tumors were studied in two cell lines, L1C2 (Fig. 4D) and LLC (Fig. 4E). Mice were treated with DMXAA when the mean tumor volume in the nondepleted mice was between 260 and 306 mm 3. In both cell lines, the antitumor effect of DMXAA was completely lost when the CD8 + T cells were depleted but was retained when the CD4 + T lymphocytes were depleted. These results show that CD8 + T lymphocytes are essential for the therapeutic effects of DMXAA. Cancer Res 2005; 65: (24). December 15,
8 DMXAA Activates Tumor Macrophages and T Cells Figure 4. A, antitumor effect of DMXAA is lost in immunodeficient mice. Treatment of immunocompetent mice with DMXAA with L1C2 flank tumors ledtomarkedgrowthinhibition.*,p < B, in contrast, treatment of BALB/c nude mice bearing established L1C2 tumors with DMXAA had virtually no effect on tumor growth. **, P >0.9.C, similarly, treatment of BALB/c nude mice with established LLC or TC-1 tumors (n = 5) with DMXAA had no significant antitumor effects compared with control tumors when measured at 21 or 22 days after tumor inoculation. #, P >0.1;##,P >0.4. D and E, L1C2 (D) and LLC (E) tumors were grown in the immunocompetent mice and mice that were depleted of either CD8 + or CD4 + T cells using monoclonal antibodies for the duration of the experiment (shaded column). Thesemicewerethendividedintocontrol(n = 5) or the treatment (DMXAA 18 mg/kg i.p.; n = 5 or 6) groups. Mean tumor volume in the DMXAA treatment group in the intact and CD4 + T-cell-depleted mice was significantly smaller than the control group for both the L1C2 (D) and LLC (E) tumors. *, P < 0.01; #, P < The treatment groups in the CD8 + T-cell-depleted mice were not significantly smaller than their respective controls. **, P = 0.46; ##, P = F, L1C2 tumors were established in immunocompetent mice. Mice were treated with DMXAA on day 12. At the same time, CD8 + T-cell depletion was commenced in selected mice (n = 5) and maintained through the further course of the experiment (shaded column). Although the tumors in the CD8 + T-cell-depleted mice were significantly smaller than the control group, there was only an initial brief growth delay in response to treatment after which the tumors began to regrow at almost the same rate as the controls. *, P < G, LLC tumors were established in perforin knockout (K.O.) mice and received either no treatment (n = 5) or treatment with 18 mg/kg DMXAA i.p. (n =5). Although the tumors in the treatment group were smaller than the control, DMXAA did not produce tumor cures and after an initial growth delay began to regrow at almost the same rate as the controls. *, P < Points and columns, mean volume; bars, SE. Arrow, time of treatment with DMXAA. Depletion of CD8 + T cells does not inhibit necrosis and macrophage influx into tumors. Possible explanations for loss of effect of DMXAA in CD8-depleted mice would be the absence of necrosis or limited migration of macrophages into tumor. To examine these hypotheses, flank LLC tumors were grown in mice in which CD8 + T cells had been depleted. These mice were treated with DMXAA and tumors were harvested 48 hours later for histologic studies. H&E staining revealed the presence of significant amounts of necrosis in treated mice (Fig. 3B, A and B). Immunohistochemical staining using the CD11b antibody showed increased infiltration of macrophages into tumors (Fig. 3B, C and D) similar in magnitude as seen in wild-type mice (Table 2). These data show that tumor necrosis and influx of macrophages can occur in the absence of circulating CD8 + T cells but are not sufficient to significantly inhibit tumor growth. CD8 + T lymphocytes are essential after administration of 5,6-dimethylxanthenone-4-acetic acid to produce tumor cures. To confirm that CD8 + T cells were involved in the antitumor response after the administration of DMXAA, we started CD8 + T cell depletion at the same time as DMXAA treatment. As shown in Fig. 4F, treatment with DMXAA in these animals results in an initial decrease in tumor size but tumors began to grow again and thereafter grew at the same rate as the control tumors. These data show that CD8 + T cells are not required in the early posttreatment phase but suggest a role of CD8 + cells in the late posttreatment phase. 5,6-Dimethylxanthenone-4-acetic acid effects were blunted in perforin knockout mice. The experiments above showed that CD8 + T cells were essential for the antitumor effect of DMXAA. CD8 + T cells can potentially act either via secreted cytokines or by direct cytolytic mechanisms, with perforin being one of the main mediators of the latter pathway. We, therefore, examined the antitumor effect of DMXAA in LLC flank tumors grown in perforindeficient mice. Mice were treated with DMXAA when the tumors were f200 mm 3 size. The tumor growth was slower in the treated animals compared with the control animals for the initial 4 to 5 days after treatment. Thereafter, the tumors in both the groups began to grow at similar rates (Fig. 4G). These data suggest that the role of CD8 + T cells in the later phase of the DMXAA response is perforin dependent. Discussion DMXAA has completed phase 1 clinical trials (12, 13) and a phase 2 trial has recently been initiated in combination with chemotherapy for patients with non small cell lung cancer. Because the mechanisms of action of DMXAA are still unclear, we studied the effects of DMXAA in murine models of thoracic cancers. Although DMXAA has been classified as a vascular disruptive agent causing TNF-a secretion and hemorrhagic necrosis in tumors, our data confirm other studies showing that the necrosis caused by DMXAA is not enough to produce tumor cures. In the tumor models that we studied, DMXAA does not produce its antitumor effects due to necrosis or by its direct antiproliferative actions but by generation of a potent antitumor immune response involving CD8 + T cells. This conclusion is supported by several pieces of data. First, treatment with DMXAA results in a delayed, but impressive intratumoral infiltrate of CD8 + T cells (Fig. 3; Table 2). Second, animals cured of their tumors after DMXAA treatment show immunity to tumor cell rechallenge. Third, antitumor efficacy of DMXAA is lost in nude and CD8 + T-cell-depleted mice despite the presence of hemorrhagic necrosis (Fig. 3B; ref. 4) Cancer Res 2005; 65: (24). December 15, 2005
9 Cancer Research We specifically wanted to study the effects of DMXAA on tumors with different levels of immunogenicity as defined by the inability of injected tumor cells to grow after previous vaccination of mice with irradiated cells. Using these variables, LLC cells were nonimmunogenic, TC-1 cells were intermediately immunogenic, and AB-12 and L1C2 cells were highly immunogenic (data not shown). Interestingly, even in the nonimmunogenic LLC tumors, the effect of DMXAA was completely dependent on CD8 + T cells. Our data showing lack of DMXAA effect in nude mice are similar to the studies of Pratesi et al. (16), Bibby et al. (17), and Law et al. (18); however, these investigators found that CD4 + T cells were required for FAA effects, not CD8 + T cells. Our data are consistent with the observations of Franco et al. (21) who showed an important CD8 + T-cell component to antitumor efficacy of FAA (in combination with IL-2) in a RENCA murine carcinoma model. Our findings differ from those that showed retention of activity of DMXAA against colon 38 tumors in nude mice (19). The reason for these differences is not known for certain but may relate to the specific tumor types studied. The mouse colon 38 tumor explant system may behave differently from the lung cancer and mesothelioma cell lines studied here. Our data support a model in which both the innate and adaptive immune systems are required for optimal antitumor effects, with an early effector phase driven by macrophages and a late effector phase driven by CD8 + T cells. Systemic administration of DMXAA rapidly activates CD11b + tumor-associated macrophages (within 2 hours) causing up-regulation of mrna for a variety of cytokines and chemokines, including IP10, RANTES, IL-6, IFN-g, TNF-a, MIP-1a, MCP-1, MIG (Table 1), as well as inducing the secretion of many of these proteins (documented for TNF-a, IP-10, IL-6, KC, MIP-2, MCP-1, and RANTES; Fig. 1). In in vitro studies, DMXAA did not induce tumor cells to chemoattract macrophages (data not shown). Based on previous studies (34), although not directly evaluated in this study, macrophage cytotoxicity for tumor cells is also likely enhanced. Histologic studies at early time points (24-48 hours) show the presence of large areas of necrosis within the treated tumors, with a peripheral rim of viable tumor tissue (Fig. 3). The tumors were found to be heavily infiltrated with leukocytes, the majority of which were macrophages. CD8 + T cells were rare in the tumors immediately after treatment but appeared in tumors f3 days posttreatment and infiltrated into tumors in significant numbers 1 week after DMXAA administration (Table 2). We postulate that this initial combination of vascular activation, tumor necrosis, and the presence of inflammatory cytokines and chemoattractants generates an immunostimulatory microenvironment that attracts an early monocyte (and possibly dendritic cell) infiltration into the tumor (Fig. 3), which, in turn, supports effective tumor antigen presentation and consequent generation of CD8 + CTLs. These CTLs subsequently infiltrate the tumor between days 3 and 7 post- DMXAA treatment (Fig. 3), causing tumor destruction. This effect can be blocked in the absence of perforin, suggesting involvement of direct cytolytic pathways in eradication of tumors by CD8 + T cells (Fig. 4G). Our model explains the presence of necrosis, but lack of tumorcures,innudemiceandthemicedepletedofcd8 + T cells.althoughwehavefocusedontheroleofcd8 + Tcellsin the effector phase of DMXAA treatment, they may also play a role in priming the tumor-associated macrophages. This idea is based on the observation that when CD8 + T cells were depleted just before treatment (compared with depleting CD8 cells before injecting tumor cells), there was an initial (3-4 day) delay in tumor growth (Fig. 4F) followedbyarapidregrowthof the tumor. This initial effect was not seen in nude mice or in mice depleted of CD8 + Tcellsatthetimeoftumorcellinjection (Fig. 4). We speculate that this initial effect may have been due to innate immune responses induced by the tumor-associated macrophages that have been primed by CD8 + T cells. This idea is supported by the presence of a similar partial antitumor effect seen in the perforin knockout mice, suggesting that the effects of CD8 + T cells in the pretreatment phase are perforinindependent and may be mediated by cytokine secretion. Experiments to examine the role of CD8 + T cells in priming phase are ongoing and will be reported separately. Interestingly, the CD8 + TcelleffectdoesnotrequireCD4 + Tcellhelpas complete tumor cures can be achieved even in the complete absence of CD4 + T cells. Although the role of CD8 + T cells was crucial for producing tumor cures, the fact that DMXAA primarily acts on tumorassociated macrophages highlights the potential key role of this cell type in initiating and maintaining adaptive antitumor immune responses. Two distinct phenotypes have been described for tumor macrophages (35). M1 macrophages produce TNF-a, nitric oxide, and antiangiogenic chemokines (like Mig and IP10) and inhibit tumor growth. M2 macrophages produce cytokines like IL-10, transforming growth factor-h, and VEGF that suppress T-cell activity and promote angiogenesis. Unfortunately, in most established mouse and human tumors, abundant numbers of the M2-phenotype macrophages are usually present (34). This immunosuppressive/angiogenic environment in the tumor is one of the major hurdles in developing efficacious immune therapies, which, if overcome, could potentially augment exogenous immune therapy. A recent study demonstrating synergistic effects with combination of the chemokine CCL-16 with an IL-10 receptor antibody and CpG supports this hypothesis and underscores the role of tumor-associated macrophage activation to overcome immune tolerance (3). DMXAA seems a highly effective way to convert M2 macrophages into cells with an M1 phenotype, as well as recruiting new macrophages that are immunostimulatory. Thus, properly stimulated macrophages generate an innate antitumor response that inhibits, rather than promotes, tumor growth. In addition to initiating effective antitumor immune responses, DMXAA may be a potential agent that can be combined with other forms of immunotherapy to generate synergistic effects. Treatment with DMXAA can markedly alter tumor microenvironment by switching macrophages into an activated phenotype and result in secretion of chemotactic cytokines that can traffic immunocytes to tumor. Additionally, an inflammatory milieu within the tumor may allow for more effective activation and function of these trafficked cells. Further, the necrosis induced within the tumors, in addition to reducing tumor burden, could also release tumor-specific antigens that could be presented by the antigen-presenting cells (dendritic cells and macrophages) to T cells, resulting in better activation of the adaptive immune system. Previous studies have shown that the combination of FAA with IL-2 enhanced the efficacy of FAA (36, 37). The antitumor efficacy of DMXAA was enhanced by the intratumoral injection of a plasmid encoding the costimulatory molecule B7.1 (CD80) followed by i.p. administration of DMXAA (38). ICAM-1 Cancer Res 2005; 65: (24). December 15,
10 DMXAA Activates Tumor Macrophages and T Cells immunogene therapy was similarly enhanced with DMXAA that was dependent on CD8 + and natural killer cells (39). We also have preliminary data to support the value of combining DMXAA with an antitumor vaccine. 4 In summary, we have shown a tumor-associated macrophage activator, DMXAA, that can induce strong CD8 + T-cell-mediated antitumor immune responses in both immunogenic and nonimmunogenic tumors and have implicated a role for both innate and adaptive immunity in the mechanism of the antitumor action of DMXAA. Initially, DMXAA activates tumor-associated macrophages to produce inflammatory cytokines and chemokines. These 4 In preparation. mediators lead to tumor necrosis and to the generation of CD8 + T cells that are critical mediators of the ultimate antitumor effects of DMXAA. Our data provides strong rationale for further studies involving the use of DMXAA to induce antitumor immune responses and the combination of DMXAA with other forms of immunotherapy. Acknowledgments Received 5/16/2005; revised 9/12/2005; accepted 9/28/2005. Grant support: National Cancer Institute grant PO1 CA The costs of publication of this article were defrayed in part by the payment of page charges. This article must therefore be hereby marked advertisement in accordance with 18 U.S.C. Section 1734 solely to indicate this fact. We thank Elliot Wakeam and Drs. Anil Vachani, Samuel Kim, and Rashmin Savani for their assistance. References 1. Fidler IJ. Therapy of cancer metastasis by systemic activation of macrophages. Adv Pharmacol 1994;30: Bingle L, Brown NJ, Lewis CE. The role of tumourassociated macrophages in tumour progression: implications for new anticancer therapies. J Pathol 2002;196: Guiducci C, Vicari AP, Sangaletti S, Trinchieri G, Colombo MP. Redirecting in vivo elicited tumor infiltrating macrophages and dendritic cells towards tumor rejection. Cancer Res 2005;65: Denekamp J. Vascular attack as a therapeutic strategy for cancer. Cancer Metastasis Rev 1990;9: St Croix B, Rago C, Velculescu V, et al. Genes expressed in human tumor endothelium. Science 2000; 289: Hadj Tahar A. Bevacizumab for advanced colorectal cancer. Issues Emerg Health Technol 2004;63: Herbst RS, Johnson DH, Mininberg E, et al. Phase I/II trial evaluating the anti-vascular endothelial growth factor monoclonal antibody bevacizumab in combination with the HER-1/epidermal growth factor receptor tyrosine kinase inhibitor erlotinib for patients with recurrent non-small-cell lung cancer. J Clin Oncol 2005; 23: Siemann DW, Chaplin DJ, Horsman MR. Vasculartargeting therapies for treatment of malignant disease. Cancer 2004;100: Tozer GM, Kanthou C, Parkins CS, Hill SA. The biology of the combretastatins as tumour vascular targeting agents. Int J Exp Pathol 2002;83: Baguley BC. Antivascular therapy of cancer: DMXAA. Lancet Oncol 2003;4: Baguley BC, Ching LM. DMXAA: an antivascular agent with multiple host responses. Int J Radiat Oncol Biol Phys 2002;54: Rustin GJ, Bradley C, Galbraith S, et al. 5,6- Dimethylxanthenone-4-acetic acid (DMXAA), a novel antivascular agent: phase I clinical and pharmacokinetic study. Br J Cancer 2003;88: Jameson MB, Thompson PI, Baguley BC, et al. Clinical aspects of a phase I trial of 5,6-dimethylxanthenone-4-acetic acid (DMXAA), a novel antivascular agent. Br J Cancer 2003;88: Ching LM, Baguley BC. Induction of natural killer cell activity by the antitumour compound flavone acetic acid (NSC ). Eur J Cancer Clin Oncol 1987;23: Hornung RL, Young HA, Urba WJ, Wiltrout RH. Immunomodulation of natural killer cell activity by flavone acetic acid: occurrence via induction of interferon a/h. J Natl Cancer Inst 1988;80: Pratesi G, Rodolfo M, Rovetta G, Parmiani G. Role of T cells and tumour necrosis factor in antitumour activity and toxicity of flavone acetic acid. Eur J Cancer 1990;26: Bibby MC, Phillips RM, Double JA, Pratesi G. Antitumour activity of flavone acetic acid (NSC ) in mice influence of immune status. Br J Cancer 1991;63: Laws AL, Matthew AM, Double JA, Bibby MC. Preclinical in vitro and in vivo activity of 5,6-dimethylxanthenone-4-acetic acid. Br J Cancer 1995;71: Ching LM, Joseph WR, Baguley BC. Antitumour responses to flavone-8-acetic acid and 5,6-dimethylxanthenone-4-acetic acid in immune deficient mice. Br J Cancer 1992;66: Pang JH, Cao Z, Joseph WR, Baguley BC, Ching LM. Antitumour activity of the novel immune modulator 5,6- dimethylxanthenone-4-acetic acid (DMXAA) in mice lacking the interferon-g receptor. Eur J Cancer 1998;34: Franco JL, Ghosh P, Wiltrout RH, et al. Partial degradation of T-cell signal transduction molecules by contaminating granulocytes during protein extraction of splenic T cells from tumor-bearing mice. Cancer Res 1995;55: Ching LM, Goldsmith D, Joseph WR, Korner H, Sedgwick JD, Baguley BC. Induction of intratumoral tumor necrosis factor (TNF) synthesis and hemorrhagic necrosis by 5,6-dimethylxanthenone-4-acetic acid (DMXAA) in TNF knockout mice. Cancer Res 1999;59: Joseph WR, Cao Z, Mountjoy KG, Marshall ES, Baguley BC, Ching LM. Stimulation of tumors to synthesize tumor necrosis factor-a in situ using 5,6- dimethylxanthenone-4-acetic acid: a novel approach to cancer therapy. Cancer Res 1999;59: Davis MR, Manning LS, Whitaker D, Garlepp MJ, Robinson BW. Establishment of a murine model of malignant mesothelioma. Int J Cancer 1992;52: Dubinett SM, Patrone L, Tobias J, Cochran AJ, Wen DR, McBride WH. Intratumoral interleukin-2 immunotherapy: activation of tumor-infiltrating and splenic lymphocytes in vivo. Cancer Immunol Immunother 1993;36: Rewcastle GW, Atwell GJ, Li ZA, Baguley BC, Denny WA. Potential antitumor agents. 61. Structure-activity relationships for in vivo colon 38 activity among disubstituted 9-oxo-9H-xanthene-4-acetic acids. J Med Chem 1991;34: Sambrook J, Russell D. Molecular cloning. A laboratory manual. 3rd ed. Cold Spring Harbor (NY): Cold Spring Harbor Laboratory Press; Philpott M, Ching LM, Baguley BC. The antitumour agent 5,6-dimethylxanthenone-4-acetic acid acts in vitro on human mononuclear cells as a co-stimulator with other inducers of tumour necrosis factor. Eur J Cancer 2001;37: Weber J, Sondak VK, Scotland R, et al. Granulocytemacrophage-colony-stimulating factor added to a multipeptide vaccine for resected Stage II melanoma. Cancer 2003;97: Ching LM, Cao Z, Kieda C, Zwain S, Jameson MB, Baguley BC. Induction of endothelial cell apoptosis by the antivascular agent 5,6-dimethylxanthenone-4-acetic acid. Br J Cancer 2002;86: Kestell P, Paxton JW, Rewcastle GW, Dunlop I, Baguley BC. Plasma disposition, metabolism and excretion of the experimental antitumour agent 5,6- dimethylxanthenone-4-acetic acid in the mouse, rat and rabbit. Cancer Chemother Pharmacol 1999;43: Cao Z, Baguley BC, Ching LM. Interferon-inducible protein 10 induction and inhibition of angiogenesis in vivo by the antitumor agent 5,6-dimethylxanthenone- 4-acetic acid (DMXAA). Cancer Res 2001;61: Wang LC, Reddy CB, Baguley BC, Kestell P, Sutherland R, Ching LM. Induction of tumour necrosis factor and interferon-g in cultured murine splenocytes by the antivascular agent DMXAA and its metabolites. Biochem Pharmacol 2004;67: Ching LM, Joseph WR, Baguley BC. Stimulation of macrophage tumouricidal activity by 5,6-dimethyl-xanthenone-4-acetic acid, a potent analogue of the antitumour agent flavone-8-acetic acid. Biochem Pharmacol 1992;44: Mantovani A, Sozzani S, Locati M, Allavena P, Sica A. Macrophage polarization: tumor-associated macrophages as a paradigm for polarized M2 mononuclear phagocytes. Trends Immunol 2002;23: Hornung RL, Back TC, Zaharko DS, Urba WJ, Longo DL, Wiltrout RH. Augmentation of natural killer activity, induction of IFN and development tumor immunity during the successful treatment of established murine renal cancer using flavone acetic acid and IL-2. J Immunol 1988;141: Futami H, Eader LA, Komschlies KL, et al. Flavone acetic acid directly induces expression of cytokine genes in mouse splenic leukocytes but not in human peripheral blood leukocytes. Cancer Res 1991;51: Kanwar JR, Kanwar RK, Pandey S, Ching LM, Krissansen GW. Vascular attack by 5,6-dimethylxanthenone-4-acetic acid combined with B7.1 (CD80)-mediated immunotherapy overcomes immune resistance and leads to the eradication of large tumors and multiple tumor foci. Cancer Res 2001;61: Kanwar JR, Berg RW, Yang Y, et al. Requirements for ICAM-1 immunogene therapy of lymphoma. Cancer Gene Ther 2003;10: Cancer Res 2005; 65: (24). December 15, 2005
Cancer and the immune system: can we beat cancer at its own game?
 Cancer and the immune system: can we beat cancer at its own game? Andrew R. Haas, MD, PhD Assistant Professor of Medicine University of Pennsylvania Medical Center Philadelphia, Pa Why can t immune
Cancer and the immune system: can we beat cancer at its own game? Andrew R. Haas, MD, PhD Assistant Professor of Medicine University of Pennsylvania Medical Center Philadelphia, Pa Why can t immune
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: adoptive_immunotherapy 11/1993 3/2016 3/2017 3/2016 Description of Procedure or Service The spontaneous regression
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: adoptive_immunotherapy 11/1993 3/2016 3/2017 3/2016 Description of Procedure or Service The spontaneous regression
Oncos Therapeutics: ONCOS THERAPEUTICS Personalized Cancer Immunotherapy. March 2015. Antti Vuolanto, COO and co-founder
 Oncos Therapeutics: Personalized Cancer Immunotherapy ONCOS THERAPEUTICS Personalized Cancer Immunotherapy March 2015 Antti Vuolanto, COO and co-founder 1 History of Oncos Therapeutics 2002 2007 2009 Research
Oncos Therapeutics: Personalized Cancer Immunotherapy ONCOS THERAPEUTICS Personalized Cancer Immunotherapy March 2015 Antti Vuolanto, COO and co-founder 1 History of Oncos Therapeutics 2002 2007 2009 Research
CONTENT. Chapter 1 Review of Literature. List of figures. List of tables
 Abstract Abbreviations List of figures CONTENT I-VI VII-VIII IX-XII List of tables XIII Chapter 1 Review of Literature 1. Vaccination against intracellular pathogens 1-34 1.1 Role of different immune responses
Abstract Abbreviations List of figures CONTENT I-VI VII-VIII IX-XII List of tables XIII Chapter 1 Review of Literature 1. Vaccination against intracellular pathogens 1-34 1.1 Role of different immune responses
The Need for a PARP in vivo Pharmacodynamic Assay
 The Need for a PARP in vivo Pharmacodynamic Assay Jay George, Ph.D., Chief Scientific Officer, Trevigen, Inc., Gaithersburg, MD For further infomation, please contact: William Booth, Ph.D. Tel: +44 (0)1235
The Need for a PARP in vivo Pharmacodynamic Assay Jay George, Ph.D., Chief Scientific Officer, Trevigen, Inc., Gaithersburg, MD For further infomation, please contact: William Booth, Ph.D. Tel: +44 (0)1235
CD22 Antigen Is Broadly Expressed on Lung Cancer Cells and Is a Target for Antibody-Based Therapy
 CD22 Antigen Is Broadly Expressed on Lung Cancer Cells and Is a Target for Antibody-Based Therapy Joseph M. Tuscano, Jason Kato, David Pearson, Chengyi Xiong, Laura Newell, Yunpeng Ma, David R. Gandara,
CD22 Antigen Is Broadly Expressed on Lung Cancer Cells and Is a Target for Antibody-Based Therapy Joseph M. Tuscano, Jason Kato, David Pearson, Chengyi Xiong, Laura Newell, Yunpeng Ma, David R. Gandara,
Gene Silencing Oligos (GSOs) Third Generation Antisense
 Gene Silencing Oligos (GSOs) Third Generation Antisense Walter R. Strapps, Ph.D. Executive Director, RNA Therapeutics Idera Pharmaceuticals Cambridge, MA NASDAQ: IDRA www.iderapharma.com Idera is a leader
Gene Silencing Oligos (GSOs) Third Generation Antisense Walter R. Strapps, Ph.D. Executive Director, RNA Therapeutics Idera Pharmaceuticals Cambridge, MA NASDAQ: IDRA www.iderapharma.com Idera is a leader
OPG-Fc inhibits ovariectomy-induced growth of disseminated breast cancer cells in bone.
 Title of the poster Authors Sheffield Cancer Research Centre University of Sheffield OPG-Fc inhibits ovariectomy-induced growth of disseminated breast cancer cells in bone. Dr Penelope Ottewell Background
Title of the poster Authors Sheffield Cancer Research Centre University of Sheffield OPG-Fc inhibits ovariectomy-induced growth of disseminated breast cancer cells in bone. Dr Penelope Ottewell Background
TABLE OF CONTENT. Page ACKNOWLEDGEMENTS. iii ENGLISH ABSTRACT THAI ABSTRACT. vii LIST OF TABLES LIST OF FIGURES. xvi ABBREVIATIONS.
 x TABLE OF CONTENT ACKNOWLEDGEMENTS ENGLISH ABSTRACT THAI ABSTRACT LIST OF TABLES LIST OF FIGURES ABBREVIATIONS iii iv vii xv xvi xviii CHAPTER I: INTRODUCTION 1.1 Statement of problems 1 1.2 Literature
x TABLE OF CONTENT ACKNOWLEDGEMENTS ENGLISH ABSTRACT THAI ABSTRACT LIST OF TABLES LIST OF FIGURES ABBREVIATIONS iii iv vii xv xvi xviii CHAPTER I: INTRODUCTION 1.1 Statement of problems 1 1.2 Literature
Use of Cyclooxygenase-2 Inhibition to Enhance the Efficacy of Immunotherapy
 [CANCER RESEARCH 63, 7845 7852, November 15, 2003] Use of Cyclooxygenase-2 Inhibition to Enhance the Efficacy of Immunotherapy Peter DeLong, Tomoyuki Tanaka, Robb Kruklitis, Adam C. Henry, Veena Kapoor,
[CANCER RESEARCH 63, 7845 7852, November 15, 2003] Use of Cyclooxygenase-2 Inhibition to Enhance the Efficacy of Immunotherapy Peter DeLong, Tomoyuki Tanaka, Robb Kruklitis, Adam C. Henry, Veena Kapoor,
NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY. Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds
 NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds CANCER IMMUNOTHERAPY - Breakthrough of the Year in Science magazine 2013.
NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds CANCER IMMUNOTHERAPY - Breakthrough of the Year in Science magazine 2013.
The role of IBV proteins in protection: cellular immune responses. COST meeting WG2 + WG3 Budapest, Hungary, 2015
 The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
Immunotherapy Concept Turned Reality
 Authored by: Jennifer Dolan Fox, PhD VirtualScopics Inc. jennifer_fox@virtualscopics.com +1 585 249 6231 Immunotherapy Concept Turned Reality Introduction While using the body s own immune system as a
Authored by: Jennifer Dolan Fox, PhD VirtualScopics Inc. jennifer_fox@virtualscopics.com +1 585 249 6231 Immunotherapy Concept Turned Reality Introduction While using the body s own immune system as a
a Phase 2 prostate cancer clinical trial is ongoing. Table 2: Squalamine vs Standard-of-care literature
 PRODUCT FACT SHEET Spring 2007 MISSION STATEMENT Genaera Corporation is a biopharmaceutical company with a focus on metabolic and respiratory diseases. The compounds in the Genaera pipeline address signal
PRODUCT FACT SHEET Spring 2007 MISSION STATEMENT Genaera Corporation is a biopharmaceutical company with a focus on metabolic and respiratory diseases. The compounds in the Genaera pipeline address signal
Fighting the Battles: Conducting a Clinical Assay
 Fighting the Battles: Conducting a Clinical Assay 6 Vocabulary: In Vitro: studies in biology that are conducted using components of an organism that have been isolated from their usual biological surroundings
Fighting the Battles: Conducting a Clinical Assay 6 Vocabulary: In Vitro: studies in biology that are conducted using components of an organism that have been isolated from their usual biological surroundings
Human CD4+T Cell Care Manual
 Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
Human CD4+T Cell Care Manual INSTRUCTION MANUAL ZBM0067.02 SHIPPING CONDITIONS Human CD4+T Cells, cryopreserved Cryopreserved human CD4+T cells are shipped on dry ice and should be stored in liquid nitrogen
Mouse IFN-gamma ELISpot Kit
 Page 1 of 8 Mouse IFN-gamma ELISpot Kit Without Plates With Plates With Sterile Plates Quantity Catalog Nos. 862.031.001 862.031.001P 862.031.001S 1 x 96 tests 862.031.005 862.031.005P 862.031.005S 5 x
Page 1 of 8 Mouse IFN-gamma ELISpot Kit Without Plates With Plates With Sterile Plates Quantity Catalog Nos. 862.031.001 862.031.001P 862.031.001S 1 x 96 tests 862.031.005 862.031.005P 862.031.005S 5 x
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency Evaluation of Medicines for Human Use London, 10 October 2007 Doc. Ref. COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON POTENCY TESTING OF CELL BASED IMMUNOTHERAPY
European Medicines Agency Evaluation of Medicines for Human Use London, 10 October 2007 Doc. Ref. COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON POTENCY TESTING OF CELL BASED IMMUNOTHERAPY
TITLE: Treatment of Prostate Cancer with a DBP-MAF-Vitamin D Complex to Target Angiogenesis and Tumorigenesis
 AD AWARD NUMBER: W81XWH-04-1-0010 TITLE: Treatment of Prostate Cancer with a DBP-MAF-Vitamin D Complex to Target Angiogenesis and Tumorigenesis PRINCIPAL INVESTIGATOR: Michael W. Fannon, Ph.D. CONTRACTING
AD AWARD NUMBER: W81XWH-04-1-0010 TITLE: Treatment of Prostate Cancer with a DBP-MAF-Vitamin D Complex to Target Angiogenesis and Tumorigenesis PRINCIPAL INVESTIGATOR: Michael W. Fannon, Ph.D. CONTRACTING
CONTRACTING ORGANIZATION: University of Alabama at Birmingham Birmingham, AL 35294
 AD Award Number: W81XWH-08-1-0030 TITLE: Regulation of Prostate Cancer Bone Metastasis by DKK1 PRINCIPAL INVESTIGATOR: Gregory A. Clines, M.D., Ph.D. CONTRACTING ORGANIZATION: University of Alabama at
AD Award Number: W81XWH-08-1-0030 TITLE: Regulation of Prostate Cancer Bone Metastasis by DKK1 PRINCIPAL INVESTIGATOR: Gregory A. Clines, M.D., Ph.D. CONTRACTING ORGANIZATION: University of Alabama at
Basics of Immunology
 Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
Basics of Immunology 2 Basics of Immunology What is the immune system? Biological mechanism for identifying and destroying pathogens within a larger organism. Pathogens: agents that cause disease Bacteria,
Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159. Date Submitted: 12-11-09
 Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159 Investigator: Institution: Carol Wyatt Kansas State University Date Submitted: 12-11-09 Industry summary: Effective circovirus vaccines
Title: Mapping T cell epitopes in PCV2 capsid protein - NPB #08-159 Investigator: Institution: Carol Wyatt Kansas State University Date Submitted: 12-11-09 Industry summary: Effective circovirus vaccines
ELISA BIO 110 Lab 1. Immunity and Disease
 ELISA BIO 110 Lab 1 Immunity and Disease Introduction The principal role of the mammalian immune response is to contain infectious disease agents. This response is mediated by several cellular and molecular
ELISA BIO 110 Lab 1 Immunity and Disease Introduction The principal role of the mammalian immune response is to contain infectious disease agents. This response is mediated by several cellular and molecular
Drug Development Services
 Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
Drug Development Services USING BLOOD AND BONE MARROW PRIMARY CELL SYSTEMS Clinically Relevant In Vitro Assays Broad Spectrum of Drug Classes Multi-Species Platforms Enhancing Drug Development through
Application Note No. 2 / July 2012. Quantitative Assessment of Cell Quality, Viability and Proliferation. System
 Application Note No. 2 / July 2012 Quantitative Assessment of Cell Quality, Viability and Proliferation System Quantitative Assessment of Cell Quality, Viability and Proliferation Introduction In vitro
Application Note No. 2 / July 2012 Quantitative Assessment of Cell Quality, Viability and Proliferation System Quantitative Assessment of Cell Quality, Viability and Proliferation Introduction In vitro
Predictive Biomarkers for Tumor Immunotherapy: Are we ready for clinical implementation? Howard L. Kaufman Rush University
 Predictive Biomarkers for Tumor Immunotherapy: Are we ready for clinical implementation? Howard L. Kaufman Rush University Changing Paradigms in Cancer Treatment Potential Uses of Biomarkers Adverse event
Predictive Biomarkers for Tumor Immunotherapy: Are we ready for clinical implementation? Howard L. Kaufman Rush University Changing Paradigms in Cancer Treatment Potential Uses of Biomarkers Adverse event
2.1.2 Characterization of antiviral effect of cytokine expression on HBV replication in transduced mouse hepatocytes line
 i 1 INTRODUCTION 1.1 Human Hepatitis B virus (HBV) 1 1.1.1 Pathogenesis of Hepatitis B 1 1.1.2 Genome organization of HBV 3 1.1.3 Structure of HBV virion 5 1.1.4 HBV life cycle 5 1.1.5 Experimental models
i 1 INTRODUCTION 1.1 Human Hepatitis B virus (HBV) 1 1.1.1 Pathogenesis of Hepatitis B 1 1.1.2 Genome organization of HBV 3 1.1.3 Structure of HBV virion 5 1.1.4 HBV life cycle 5 1.1.5 Experimental models
Making the switch to a safer CAR-T cell therapy
 Making the switch to a safer CAR-T cell therapy HaemaLogiX 2015 Technical Journal Club May 24 th 2016 Christina Müller - chimeric antigen receptor = CAR - CAR T cells are generated by lentiviral transduction
Making the switch to a safer CAR-T cell therapy HaemaLogiX 2015 Technical Journal Club May 24 th 2016 Christina Müller - chimeric antigen receptor = CAR - CAR T cells are generated by lentiviral transduction
LEUKEMIA LYMPHOMA MYELOMA Advances in Clinical Trials
 LEUKEMIA LYMPHOMA MYELOMA Advances in Clinical Trials OUR FOCUS ABOUT emerging treatments Presentation for: Judith E. Karp, MD Advancements for Acute Myelogenous Leukemia Supported by an unrestricted educational
LEUKEMIA LYMPHOMA MYELOMA Advances in Clinical Trials OUR FOCUS ABOUT emerging treatments Presentation for: Judith E. Karp, MD Advancements for Acute Myelogenous Leukemia Supported by an unrestricted educational
Dendritic Cells: A Basic Review *last updated May 2003
 *last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
*last updated May 2003 Prepared by: Eric Wieder, PhD MD Anderson Cancer Center Houston, TX USA What is a dendritic cell? Dendritic cells are antigen-presenting cells (APCs) which play a critical role in
ELITE Custom Antibody Services
 ELITE Custom Antibody Services ELITE Custom Antibody Services Experience, confidence, and understanding As a manufacturer and service provider, we have the experience, confidence, and understanding to
ELITE Custom Antibody Services ELITE Custom Antibody Services Experience, confidence, and understanding As a manufacturer and service provider, we have the experience, confidence, and understanding to
10 th EADO Congress Vilnius, 7-10 May 2014. Ipilimumab update. Michele Maio
 10 th EADO Congress Vilnius, 7-10 May 2014 Ipilimumab update Michele Maio Medical Oncology and Immunotherapy, Department of Oncology University Hospital of Siena, Istituto Toscano Tumori SIENA, ITALY Evolving
10 th EADO Congress Vilnius, 7-10 May 2014 Ipilimumab update Michele Maio Medical Oncology and Immunotherapy, Department of Oncology University Hospital of Siena, Istituto Toscano Tumori SIENA, ITALY Evolving
The immune system. Bone marrow. Thymus. Spleen. Bone marrow. NK cell. B-cell. T-cell. Basophil Neutrophil. Eosinophil. Myeloid progenitor
 The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
Additional file 1. Progress of phase II clinical trials of Panagen
 Additional file 1. Progress of phase II clinical trials of Panagen Documentation Phase II clinical trial of preparation Panagen was performed in compliance with the following documentation: Approval of
Additional file 1. Progress of phase II clinical trials of Panagen Documentation Phase II clinical trial of preparation Panagen was performed in compliance with the following documentation: Approval of
How To Treat Mesothelioma With A Tumor Stem Cell Inhibitor
 FAK INHIBITOR DEFACTINIB (VS-6063) TARGETS MESOTHELIOMA CANCER STEM CELLS Rationale for maintenance therapy after conventional therapy Jonathan Pachter, Ph.D. Vice President of Research, Verastem, Inc.
FAK INHIBITOR DEFACTINIB (VS-6063) TARGETS MESOTHELIOMA CANCER STEM CELLS Rationale for maintenance therapy after conventional therapy Jonathan Pachter, Ph.D. Vice President of Research, Verastem, Inc.
MULTIPLE MYELOMA. Dr Malkit S Riyat. MBChB, FRCPath(UK) Consultant Haematologist
 MULTIPLE MYELOMA Dr Malkit S Riyat MBChB, FRCPath(UK) Consultant Haematologist Multiple myeloma is an incurable malignancy that arises from postgerminal centre, somatically hypermutated B cells.
MULTIPLE MYELOMA Dr Malkit S Riyat MBChB, FRCPath(UK) Consultant Haematologist Multiple myeloma is an incurable malignancy that arises from postgerminal centre, somatically hypermutated B cells.
Activation and effector functions of HMI
 Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma
 Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma David E. Szymkowski Senior Director, Biotherapeutics Proteins by Design 1960s...1980s...2000s... Where are the bispecific antibody drugs? J Exp.
Anti-CD38 anti-cd3 bispecific antibody in multiple myeloma David E. Szymkowski Senior Director, Biotherapeutics Proteins by Design 1960s...1980s...2000s... Where are the bispecific antibody drugs? J Exp.
ALPHA (TNFa) IN OBESITY
 THE ROLE OF TUMOUR NECROSIS FACTOR ALPHA (TNFa) IN OBESITY Alison Mary Morris, B.Sc (Hons) A thesis submitted to Adelaide University for the degree of Doctor of Philosophy Department of Physiology Adelaide
THE ROLE OF TUMOUR NECROSIS FACTOR ALPHA (TNFa) IN OBESITY Alison Mary Morris, B.Sc (Hons) A thesis submitted to Adelaide University for the degree of Doctor of Philosophy Department of Physiology Adelaide
An Introduction To Immunotherapy And The Promise Of Tissue Phenomics
 An Introduction To Immunotherapy And The Promise Of Tissue Phenomics INSIDE: n The Potential of Immunotherapy n Towards an Understanding of Immunotherapy n Current Approaches to Immunotherapy n The Immunotherapy
An Introduction To Immunotherapy And The Promise Of Tissue Phenomics INSIDE: n The Potential of Immunotherapy n Towards an Understanding of Immunotherapy n Current Approaches to Immunotherapy n The Immunotherapy
OKT3. ~ The first mouse monoclonal antibody. used in clinical practice in the field of transplantation ~
 g944202 潘 怡 心 OKT3 ~ The first mouse monoclonal antibody used in clinical practice in the field of transplantation ~ As everybody knows, OKT3 is the first mouse monoclonal antibody produced for the treatment
g944202 潘 怡 心 OKT3 ~ The first mouse monoclonal antibody used in clinical practice in the field of transplantation ~ As everybody knows, OKT3 is the first mouse monoclonal antibody produced for the treatment
A disease and antibody biology approach to antibody drug discovery
 A disease and antibody biology approach to antibody drug discovery Björn Frendéus, PhD VP, Preclinical research Presenter: Björn Frendéus Date: 2011-11-08 1 Antibodies have revolutionized Cancer Treatment!
A disease and antibody biology approach to antibody drug discovery Björn Frendéus, PhD VP, Preclinical research Presenter: Björn Frendéus Date: 2011-11-08 1 Antibodies have revolutionized Cancer Treatment!
International Symposium on Malignant Mesothelioma 2011 -- curemeso.org
 Measles virotherapy for malignant mesothelioma Manish R. Patel, D.O. Assistant Professor of Medicine University of Minnesota June 25, 2011 Medical Treatment of Mesothelioma Majority of patients are not
Measles virotherapy for malignant mesothelioma Manish R. Patel, D.O. Assistant Professor of Medicine University of Minnesota June 25, 2011 Medical Treatment of Mesothelioma Majority of patients are not
Effects of Herceptin on circulating tumor cells in HER2 positive early breast cancer
 Effects of Herceptin on circulating tumor cells in HER2 positive early breast cancer J.-L. Zhang, Q. Yao, J.-H. Chen,Y. Wang, H. Wang, Q. Fan, R. Ling, J. Yi and L. Wang Xijing Hospital Vascular Endocrine
Effects of Herceptin on circulating tumor cells in HER2 positive early breast cancer J.-L. Zhang, Q. Yao, J.-H. Chen,Y. Wang, H. Wang, Q. Fan, R. Ling, J. Yi and L. Wang Xijing Hospital Vascular Endocrine
Humoral response to therapeutic low-intensity pulsed ultrasound (LIPUS) treatment of rat maxillary socket after the removal of a molar tooth
 Humoral response to therapeutic low-intensity pulsed ultrasound (LIPUS) treatment of rat maxillary socket after the removal of a molar tooth Kouki Hidaka *1, Chihiro Miyamoto *2, Satoko Wada-Takahashi
Humoral response to therapeutic low-intensity pulsed ultrasound (LIPUS) treatment of rat maxillary socket after the removal of a molar tooth Kouki Hidaka *1, Chihiro Miyamoto *2, Satoko Wada-Takahashi
KMS-Specialist & Customized Biosimilar Service
 KMS-Specialist & Customized Biosimilar Service 1. Polyclonal Antibody Development Service KMS offering a variety of Polyclonal Antibody Services to fit your research and production needs. we develop polyclonal
KMS-Specialist & Customized Biosimilar Service 1. Polyclonal Antibody Development Service KMS offering a variety of Polyclonal Antibody Services to fit your research and production needs. we develop polyclonal
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Immuno-Oncology Model Application in the Preclinical Treatment Setting
 Immuno-Oncology Model Application in the Preclinical Treatment Setting Maryland Franklin, Ph.D. Senior Director, Scientific Development mfranklin@molecularimaging.com July 22, 2015 Tumor Models Conference
Immuno-Oncology Model Application in the Preclinical Treatment Setting Maryland Franklin, Ph.D. Senior Director, Scientific Development mfranklin@molecularimaging.com July 22, 2015 Tumor Models Conference
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center
 Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
CD3/TCR stimulation and surface detection Determination of specificity of intracellular detection of IL-7Rα by flow cytometry
 CD3/TCR stimulation and surface detection Stimulation of HPB-ALL cells with the anti-cd3 monoclonal antibody OKT3 was performed as described 3. In brief, antibody-coated plates were prepared by incubating
CD3/TCR stimulation and surface detection Stimulation of HPB-ALL cells with the anti-cd3 monoclonal antibody OKT3 was performed as described 3. In brief, antibody-coated plates were prepared by incubating
How To Use An Antibody
 GUIDELINES FOR THE PRODUCTION OF ANTIBODIES IN LABORATORY ANIMALS Table of Contents 1. Purpose 2. Choice of Species and Strain 3. Immunizing Antigen 4. Procedures for Polyclonal Antibody Production 5.
GUIDELINES FOR THE PRODUCTION OF ANTIBODIES IN LABORATORY ANIMALS Table of Contents 1. Purpose 2. Choice of Species and Strain 3. Immunizing Antigen 4. Procedures for Polyclonal Antibody Production 5.
Chapter 18: Applications of Immunology
 Chapter 18: Applications of Immunology 1. Vaccinations 2. Monoclonal vs Polyclonal Ab 3. Diagnostic Immunology 1. Vaccinations What is Vaccination? A method of inducing artificial immunity by exposing
Chapter 18: Applications of Immunology 1. Vaccinations 2. Monoclonal vs Polyclonal Ab 3. Diagnostic Immunology 1. Vaccinations What is Vaccination? A method of inducing artificial immunity by exposing
On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma
 On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma Uber die Entstehung von multinuklearen Reed-Sternberg Riesenzellen und die Rolle von CD4 T-Zellen
On the origin of giant multinuclear Reed-Sternberg cells and the role of CD4 T cells in Hodgkin lymphoma Uber die Entstehung von multinuklearen Reed-Sternberg Riesenzellen und die Rolle von CD4 T-Zellen
Cryoinjury of Breast Cancer Cells in Tissue Equivalent Constructs
 Cryoinjury of Breast Cancer Cells in Tissue Equivalent Constructs Bumsoo Han Department of Mechanical and Aerospace Engineering University of Texas at Arlington Cryosurgery Minimally invasive surgical
Cryoinjury of Breast Cancer Cells in Tissue Equivalent Constructs Bumsoo Han Department of Mechanical and Aerospace Engineering University of Texas at Arlington Cryosurgery Minimally invasive surgical
Supplemental Information. McBrayer et al. Supplemental Data
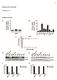 1 Supplemental Information McBrayer et al. Supplemental Data 2 Figure S1. Glucose consumption rates of MM cell lines exceed that of normal PBMC. (A) Normal PBMC isolated from three healthy donors were
1 Supplemental Information McBrayer et al. Supplemental Data 2 Figure S1. Glucose consumption rates of MM cell lines exceed that of normal PBMC. (A) Normal PBMC isolated from three healthy donors were
AAGPs TM Anti-Aging Glyco Peptides. Enhancing Cell, Tissue and Organ Integrity Molecular and biological attributes of lead AAGP molecule
 AAGPs TM Anti-Aging Glyco Peptides Enhancing Cell, Tissue and Organ Integrity Molecular and biological attributes of lead AAGP molecule 1 Acknowledgements This presentation was prepared by Dr. Samer Hussein
AAGPs TM Anti-Aging Glyco Peptides Enhancing Cell, Tissue and Organ Integrity Molecular and biological attributes of lead AAGP molecule 1 Acknowledgements This presentation was prepared by Dr. Samer Hussein
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland School of Medicine Baltimore, Md
 Major Advances in Cancer Prevention, Diagnosis and Treatment~ Why Mesothelioma Leads the Way H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland
Major Advances in Cancer Prevention, Diagnosis and Treatment~ Why Mesothelioma Leads the Way H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland
Enhancing Anti-Tumor Activity of Checkpoint Inhibition
 Enhancing Anti-Tumor Activity of Checkpoint Inhibition Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Laboratory of Tumor
Enhancing Anti-Tumor Activity of Checkpoint Inhibition Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Laboratory of Tumor
The Evaluation of Interferon-beta Levels in HPV-positive Cervical Cancer Cell Lines
 The Evaluation of Interferon-beta Levels in HPV-positive Cervical Cancer Cell Lines Olivia M. Ford and Jennifer T. Thomas, Ph.D. Human Papillomavirus (HPV) is the most common viral sexually transmitted
The Evaluation of Interferon-beta Levels in HPV-positive Cervical Cancer Cell Lines Olivia M. Ford and Jennifer T. Thomas, Ph.D. Human Papillomavirus (HPV) is the most common viral sexually transmitted
Biofocus Molecular Diagnostic Panel
 Biofocus Molecular Diagnostic Panel Dr. Lothar Prix Biofocus GmbH, Recklinghausen, Germany www.biofocus.de Molecular detection of infectious diseases Human & veterinary hereditary diseases / genetic predisposition
Biofocus Molecular Diagnostic Panel Dr. Lothar Prix Biofocus GmbH, Recklinghausen, Germany www.biofocus.de Molecular detection of infectious diseases Human & veterinary hereditary diseases / genetic predisposition
What is Cancer? Cancer is a genetic disease: Cancer typically involves a change in gene expression/function:
 Cancer is a genetic disease: Inherited cancer Sporadic cancer What is Cancer? Cancer typically involves a change in gene expression/function: Qualitative change Quantitative change Any cancer causing genetic
Cancer is a genetic disease: Inherited cancer Sporadic cancer What is Cancer? Cancer typically involves a change in gene expression/function: Qualitative change Quantitative change Any cancer causing genetic
Human Peripheral Blood Mononuclear Cell (PBMC) Manual
 Human Peripheral Blood Mononuclear Cell (PBMC) Manual INSTRUCTION MANUAL ZBM0063.04 SHIPPING CONDITIONS Human Peripheral Blood Mononuclear Cells, cryopreserved Cryopreserved human peripheral blood mononuclear
Human Peripheral Blood Mononuclear Cell (PBMC) Manual INSTRUCTION MANUAL ZBM0063.04 SHIPPING CONDITIONS Human Peripheral Blood Mononuclear Cells, cryopreserved Cryopreserved human peripheral blood mononuclear
SDS gel electrophoresis was performed using a 4% by 20% gradient gel 8. Quantification of Western blots was performed using Image J Processing and
 Supplemental Material: Western blot: SDS gel electrophoresis was performed using a 4% by 20% gradient gel 8. Quantification of Western blots was performed using Image J Processing and Analysis (NIH). Quantitative
Supplemental Material: Western blot: SDS gel electrophoresis was performed using a 4% by 20% gradient gel 8. Quantification of Western blots was performed using Image J Processing and Analysis (NIH). Quantitative
Mir-X mirna First-Strand Synthesis Kit User Manual
 User Manual Mir-X mirna First-Strand Synthesis Kit User Manual United States/Canada 800.662.2566 Asia Pacific +1.650.919.7300 Europe +33.(0)1.3904.6880 Japan +81.(0)77.543.6116 Clontech Laboratories, Inc.
User Manual Mir-X mirna First-Strand Synthesis Kit User Manual United States/Canada 800.662.2566 Asia Pacific +1.650.919.7300 Europe +33.(0)1.3904.6880 Japan +81.(0)77.543.6116 Clontech Laboratories, Inc.
MEDICAL BREAKTHROUGHS RESEARCH SUMMARY
 MEDICAL BREAKTHROUGHS RESEARCH SUMMARY TOPIC: Training the Body to Fight Melanoma REPORT: 3823 BACKGROUND: Melanoma is the most dangerous form of skin cancer that can be hard to treat and fatal if not
MEDICAL BREAKTHROUGHS RESEARCH SUMMARY TOPIC: Training the Body to Fight Melanoma REPORT: 3823 BACKGROUND: Melanoma is the most dangerous form of skin cancer that can be hard to treat and fatal if not
A Genetic Analysis of Rheumatoid Arthritis
 A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
Immune Checkpoint Blockade in Acute Myeloid Leukemia. Kinsey McCormick Hematology Fellow s Conference January 10, 2014
 Immune Checkpoint Blockade in Acute Myeloid Leukemia Kinsey McCormick Hematology Fellow s Conference January 10, 2014 Overview Overview of immune checkpoints Immune checkpoints as mechanism of immune evasion
Immune Checkpoint Blockade in Acute Myeloid Leukemia Kinsey McCormick Hematology Fellow s Conference January 10, 2014 Overview Overview of immune checkpoints Immune checkpoints as mechanism of immune evasion
2) Macrophages function to engulf and present antigen to other immune cells.
 Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Effectively Exploiting Big Data with Semantics
 Effectively Exploiting Big Data with Semantics Thomas C. Rindflesch, Ph.D. National Library of Medicine, National Institutes of Health Digital Government Institute s Government Big Data Conference, October
Effectively Exploiting Big Data with Semantics Thomas C. Rindflesch, Ph.D. National Library of Medicine, National Institutes of Health Digital Government Institute s Government Big Data Conference, October
MTT Cell Proliferation Assay
 ATCC 30-1010K Store at 4 C This product is intended for laboratory research purposes only. It is not intended for use in humans, animals or for diagnostics. Introduction Measurement of cell viability and
ATCC 30-1010K Store at 4 C This product is intended for laboratory research purposes only. It is not intended for use in humans, animals or for diagnostics. Introduction Measurement of cell viability and
Natalia Taborda Vanegas. Doc. Sci. Student Immunovirology Group Universidad de Antioquia
 Pathogenesis of Dengue Natalia Taborda Vanegas Doc. Sci. Student Immunovirology Group Universidad de Antioquia Infection process Epidermis keratinocytes Dermis Archives of Medical Research 36 (2005) 425
Pathogenesis of Dengue Natalia Taborda Vanegas Doc. Sci. Student Immunovirology Group Universidad de Antioquia Infection process Epidermis keratinocytes Dermis Archives of Medical Research 36 (2005) 425
Monoclonal Antibodies in Cancer. Ralph Schwall, PhD Associate Director, Translational Oncology Genentech, Inc.
 Monoclonal Antibodies in Cancer Ralph Schwall, PhD Associate Director, Translational Oncology Genentech, Inc. Disclaimer I had nothing to do with Herceptin Using lessons learned in new antibody projects
Monoclonal Antibodies in Cancer Ralph Schwall, PhD Associate Director, Translational Oncology Genentech, Inc. Disclaimer I had nothing to do with Herceptin Using lessons learned in new antibody projects
Hepatitis C Vaccines: Are we making progress?
 Hepatitis C Vaccines: Are we making progress? Second International Hepatitis Cure and Eradication Meeting. Vancouver November, 2015 Objectives: Review the need for a preventive vaccine in 2015. Identify
Hepatitis C Vaccines: Are we making progress? Second International Hepatitis Cure and Eradication Meeting. Vancouver November, 2015 Objectives: Review the need for a preventive vaccine in 2015. Identify
MALIGNANT PLEURAL FLUIDS AID MESOTHELIOMA CELL GROWTH AND PROPAGATION
 MALIGNANT PLEURAL FLUIDS AID MESOTHELIOMA CELL GROWTH AND PROPAGATION HUI MIN CHEAH PhD Candidate School of Medicine and Pharmacology University of Western Australia Lung Institute of Western Australia
MALIGNANT PLEURAL FLUIDS AID MESOTHELIOMA CELL GROWTH AND PROPAGATION HUI MIN CHEAH PhD Candidate School of Medicine and Pharmacology University of Western Australia Lung Institute of Western Australia
QUANTITATIVE RT-PCR. A = B (1+e) n. A=amplified products, B=input templates, n=cycle number, and e=amplification efficiency.
 QUANTITATIVE RT-PCR Application: Quantitative RT-PCR is used to quantify mrna in both relative and absolute terms. It can be applied for the quantification of mrna expressed from endogenous genes, and
QUANTITATIVE RT-PCR Application: Quantitative RT-PCR is used to quantify mrna in both relative and absolute terms. It can be applied for the quantification of mrna expressed from endogenous genes, and
CFSE Cell Division Assay Kit
 CFSE Cell Division Assay Kit Item No. 10009853 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 4 Precautions
CFSE Cell Division Assay Kit Item No. 10009853 Customer Service 800.364.9897 * Technical Support 888.526.5351 www.caymanchem.com TABLE OF CONTENTS GENERAL INFORMATION 3 Materials Supplied 4 Precautions
Welcome to the Launch of Biocon s Breakthrough Innovation. For Psoriasis. Treatment
 Welcome to the Launch of Biocon s Breakthrough Innovation For Psoriasis Treatment PRESS MEET Bangalore, August 10, 2013 Autoimmune Diseases are on the Rise Globally Autoimmune Disease Segment includes
Welcome to the Launch of Biocon s Breakthrough Innovation For Psoriasis Treatment PRESS MEET Bangalore, August 10, 2013 Autoimmune Diseases are on the Rise Globally Autoimmune Disease Segment includes
Evaluating the Efficiency of Targeted Designs for Randomized Clinical Trials
 Vol. 0, 6759 6763, October 5, 004 Clinical Cancer Research 6759 Perspective Evaluating the Efficiency of Targeted Designs for Randomized Clinical Trials Richard Simon and Aboubakar Maitournam Biometric
Vol. 0, 6759 6763, October 5, 004 Clinical Cancer Research 6759 Perspective Evaluating the Efficiency of Targeted Designs for Randomized Clinical Trials Richard Simon and Aboubakar Maitournam Biometric
Understanding the immune response to bacterial infections
 Understanding the immune response to bacterial infections A Ph.D. (SCIENCE) DISSERTATION SUBMITTED TO JADAVPUR UNIVERSITY SUSHIL KUMAR PATHAK DEPARTMENT OF CHEMISTRY BOSE INSTITUTE 2008 CONTENTS Page SUMMARY
Understanding the immune response to bacterial infections A Ph.D. (SCIENCE) DISSERTATION SUBMITTED TO JADAVPUR UNIVERSITY SUSHIL KUMAR PATHAK DEPARTMENT OF CHEMISTRY BOSE INSTITUTE 2008 CONTENTS Page SUMMARY
Basic Science in Medicine
 Medical Journal of th e Islamic Republic of Iran Volume 18 Number 3 Fall 1383 November 2004 Basic Science in Medicine ] EXPANSION OF HUMAN CORD BLOOD PRIMITIVE PROGENITORS IN SERUM-FREE MEDIA USING HUMAN
Medical Journal of th e Islamic Republic of Iran Volume 18 Number 3 Fall 1383 November 2004 Basic Science in Medicine ] EXPANSION OF HUMAN CORD BLOOD PRIMITIVE PROGENITORS IN SERUM-FREE MEDIA USING HUMAN
Amaxa Mouse T Cell Nucleofector Kit
 Amaxa Mouse T Cell Nucleofector Kit For T cells isolated from C57BL/6 & BALB/c mice Evaluated for murine T cells isolated from C57BL/6 & BALB/c mice This protocol is designed for murine lymphocytes or
Amaxa Mouse T Cell Nucleofector Kit For T cells isolated from C57BL/6 & BALB/c mice Evaluated for murine T cells isolated from C57BL/6 & BALB/c mice This protocol is designed for murine lymphocytes or
This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking
 Q1/2016 This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking statements involve risks and uncertainties
Q1/2016 This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking statements involve risks and uncertainties
treatments) worked by killing cancerous cells using chemo or radiotherapy. While these techniques can
 Shristi Pandey Genomics and Medicine Winter 2011 Prof. Doug Brutlag Chronic Myeloid Leukemia: A look into how genomics is changing the way we treat Cancer. Until the late 1990s, nearly all treatment methods
Shristi Pandey Genomics and Medicine Winter 2011 Prof. Doug Brutlag Chronic Myeloid Leukemia: A look into how genomics is changing the way we treat Cancer. Until the late 1990s, nearly all treatment methods
Bottle-neck Problems of Current Human Cancer Therapy
 International Conference on Human Cell, Tissue-based Products and Tissue Banks, Oct. 13-14,Taipei, Taiwan Autologous Dendritic Cell-based Immunotherapy of Glioblastoma Multiforme: Post-Phase-I Clinical
International Conference on Human Cell, Tissue-based Products and Tissue Banks, Oct. 13-14,Taipei, Taiwan Autologous Dendritic Cell-based Immunotherapy of Glioblastoma Multiforme: Post-Phase-I Clinical
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON THE PRE-CLINICAL EVALUATION OF ANTICANCER MEDICINAL PRODUCTS
 The European Agency for the Evaluation of Medicinal Products Human Medicines Evaluation Unit London, 23 July 1998 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON THE PRE-CLINICAL
The European Agency for the Evaluation of Medicinal Products Human Medicines Evaluation Unit London, 23 July 1998 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON THE PRE-CLINICAL
Uses of Flow Cytometry
 Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
Uses of Flow Cytometry 1. Multicolour analysis... 2 2. Cell Cycle and Proliferation... 3 a. Analysis of Cellular DNA Content... 4 b. Cell Proliferation Assays... 5 3. Immunology... 6 4. Apoptosis... 7
Avastin in breast cancer: Summary of clinical data
 Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Microbiology AN INTRODUCTION EIGHTH EDITION
 TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
T Cell Maturation,Activation and Differentiation
 T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma
 The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Name (print) Name (signature) Period. (Total 30 points)
 AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
Automation of Cell Staining Technical Information Bulletin
 Automation of Cell Staining Technical Information Bulletin Automation of Cell Staining Using the Biomek 4000 Laboratory Automation Workstation Amy N. Yoder, Sr. Development Scientist and Li Liu, Sr. Development
Automation of Cell Staining Technical Information Bulletin Automation of Cell Staining Using the Biomek 4000 Laboratory Automation Workstation Amy N. Yoder, Sr. Development Scientist and Li Liu, Sr. Development
THE CANCER STEM CELL INHIBITORS VS-6063 AND VS-5584 EXHIBIT SYNERGISTIC ANTICANCER ACTIVITY IN PRECLINICAL MODELS OF MESOTHELIOMA
 THE CANCER STEM CELL INHIBITORS VS-6063 AND VS-5584 EXHIBIT SYNERGISTIC ANTICANCER ACTIVITY IN PRECLINICAL MODELS OF MESOTHELIOMA Mitchell Keegan, Ph.D. Vice President of Development, Verastem, Inc. 1
THE CANCER STEM CELL INHIBITORS VS-6063 AND VS-5584 EXHIBIT SYNERGISTIC ANTICANCER ACTIVITY IN PRECLINICAL MODELS OF MESOTHELIOMA Mitchell Keegan, Ph.D. Vice President of Development, Verastem, Inc. 1
Notch 1 -dependent regulation of cell fate in colorectal cancer
 Notch 1 -dependent regulation of cell fate in colorectal cancer Referees: PD Dr. Tobias Dick Prof. Dr. Wilfried Roth http://d-nb.info/1057851272 CONTENTS Summary 1 Zusammenfassung 2 1 INTRODUCTION 3 1.1
Notch 1 -dependent regulation of cell fate in colorectal cancer Referees: PD Dr. Tobias Dick Prof. Dr. Wilfried Roth http://d-nb.info/1057851272 CONTENTS Summary 1 Zusammenfassung 2 1 INTRODUCTION 3 1.1
Custom Antibody Services
 prosci-inc.com Custom Antibody Services High Performance Antibodies and More Broad Antibody Catalog Extensive Antibody Services CUSTOM ANTIBODY SERVICES Established in 1998, ProSci Incorporated is a leading
prosci-inc.com Custom Antibody Services High Performance Antibodies and More Broad Antibody Catalog Extensive Antibody Services CUSTOM ANTIBODY SERVICES Established in 1998, ProSci Incorporated is a leading
User Manual. CelluLyser Lysis and cdna Synthesis Kit. Version 1.4 Oct 2012 From cells to cdna in one tube
 User Manual CelluLyser Lysis and cdna Synthesis Kit Version 1.4 Oct 2012 From cells to cdna in one tube CelluLyser Lysis and cdna Synthesis Kit Table of contents Introduction 4 Contents 5 Storage 5 Additionally
User Manual CelluLyser Lysis and cdna Synthesis Kit Version 1.4 Oct 2012 From cells to cdna in one tube CelluLyser Lysis and cdna Synthesis Kit Table of contents Introduction 4 Contents 5 Storage 5 Additionally
New Directions in Treatment of Ovarian Cancer. Amit M. Oza Princess Margaret Hospital University of Toronto
 New Directions in Treatment of Ovarian Cancer Amit M. Oza Princess Margaret Hospital University of Toronto Newly diagnosed: scenario Ist line Surgery chemotherapy Cure If can t cure can we turn into chronic
New Directions in Treatment of Ovarian Cancer Amit M. Oza Princess Margaret Hospital University of Toronto Newly diagnosed: scenario Ist line Surgery chemotherapy Cure If can t cure can we turn into chronic
Lipid Extraction Kit (Chloroform Free), Trial Size
 Product Manual Lipid Extraction Kit (Chloroform Free), Trial Size Catalog Number STA-612-T 10 preps FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Lipids are a diverse group of
Product Manual Lipid Extraction Kit (Chloroform Free), Trial Size Catalog Number STA-612-T 10 preps FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Lipids are a diverse group of
