Endoscopic Management of Acute Lower Gastrointestinal Bleeding
|
|
|
- Rebecca Warner
- 10 years ago
- Views:
Transcription
1 American Journal of Gastroenterology ISSN C 2008 by Am. Coll. of Gastroenterology doi: /j x Published by Blackwell Publishing THE EXPERT S CORNER Endoscopic Management of Acute Lower Gastrointestinal Bleeding Louis M. Wong Kee Song, M.D., and Todd H. Baron, M.D. GI Bleeding Team, Division of Gastroenterology and Hepatology, Mayo Clinic, Rochester, Minnesota (Am J Gastroenterol 2008;103: ) INTRODUCTION Hemorrhage from the lower gastrointestinal (LGI) tract accounts for approximately 20% of all episodes of acute GI bleeding (1 3). Although prior descriptions of LGI hemorrhage have encompassed bleeding sources beyond the ligament of Treitz, small intestinal bleeding represents a distinct entity whose management algorithm has been redefined by the advent of capsule and double-balloon endoscopy. For the purpose of this article, we define acute LGI bleeding as the recent and sudden onset of overt hemorrhage (hematochezia or melena) originating from a source within the distal terminal ileum, colon, and/or rectum, and within potential reach of a colonoscope. Though general management principles will be outlined, this article will focus on the endoscopic approach and therapy for acute LGI bleeding. The approach described herein is derived primarily from our experience accumulated through the Mayo GI Bleeding Team practice. INITIAL EVALUATION AND TRIAGE Initial assessment of the patient presenting with presumed acute LGI bleeding consists of obtaining a focused history and physical examination, ordering the appropriate blood tests, assessing the severity of bleeding, providing the necessary resuscitative measures and blood transfusions, withholding particular drugs (i.e., anticoagulants, antiplatelets, nonsteroidal antiinflammatory drugs), correcting coagulation defects, and triaging the patient to the appropriate level of care (outpatient vs ward vs intensive care unit). Elements in the history can direct the assessment toward a cause of probable or high likelihood, such as postpolypectomy bleeding in a patient who recently underwent polypectomy, exacerbation of known inflammatory bowel disease, or ischemic colitis in a vasculopathic patient with sudden onset abdominal pain followed by bloody diarrhea. Although most overt LGI bleeding episodes will manifest as hematochezia (maroon-colored stools or fresh blood and clots per rectum), melenic stools may occur in the setting of bleeding from the cecum. Importantly, hematochezia associated with hemodynamic instability should prompt consideration for brisk bleeding from an upper gastrointestinal (UGI) source, particularly when risk factors such as a prior history of bleeding peptic ulcer or nonsteroidal antiinflammatory drug use are present. In the aforementioned circumstance, nasogastric tube (NGT) lavage is performed, and a positive or nondiagnostic (nonbilious, nonbloody) aspirate for blood prompts emergent upper endoscopy prior to performing colonoscopy. Although the return of a large amount of bile via NGT makes an UGI source unlikely, we would nevertheless perform an upper endoscopy in cases where a source is not identified at colonoscopy. The decision to manage in an outpatient setting or to admit to the intensive care unit (ICU) depends on several factors and sound clinical judgment. For example, a young, nonanemic patient with scant bleeding from suspected anorectal pathology (e.g., internal hemorrhoids) who is otherwise healthy can be managed as an outpatient. Conversely, a patient presenting with severe active bleeding (repetitive passage of 200 cc or more of bright red blood or blood clots), hemodynamic compromise (tachycardia, orthostasis, shock), >2 g/dl drop from baseline hemoglobin (Hgb), need for multiple transfusions (>2 units), supratherapeutic international normalized ratio (INR), perfusion-related complications (e.g., cardiac ischemia, dysrythmia), advanced age, and/or significant comorbid illnesses warrants admission to the ICU. A patient in whom bleeding seems to have stopped, as evidenced by cessation of or increasing interval between bowel movements, with stable vital signs and blood counts may be admitted to the hospital ward. Transfusion requirements should be individualized, but Hgb should be maintained at 10 g/dl in those with advanced age and comorbid conditions (e.g., coronary artery disease). Clotting derangements exacerbating bleeding should be corrected with fresh frozen plasma to an INR 2.0 and/or platelet transfusions to a platelet count 50,000. These thresholds also enable safer endoscopic evaluation and potential therapy. Patients with mechanical cardiac valves and/or recent metallic coronary stenting who need anticoagulation and/or antiplatelet therapy should be managed with the assistance of a cardiology specialist. Although there is no role for barium studies in the evaluation of acute LGI bleeding, plain abdominal X-rays and/or abdominal computed tomography scan may be obtained prior to colonoscopic evaluation depending on the clinical presentation and suspected etiology, as in ischemic or infectious/inflammatory colitis or suspected aortoenteric fistula, and support anticipated findings at subsequent colonoscopy. 1881
2 1882 Wong Kee Song and Baron Although colonoscopy is our initial test of choice for diagnosis and therapy, bleeding may rarely be so severe or massive, requiring emergent intervention and precluding its use. In this situation, prompt angiography with localization of the bleeding site and potential angiotherapy should be performed. Emergent surgery should be considered only as a last resort and is rarely needed to prevent death from exsanguination. However, the morbidity and mortality associated with blind subtotal colectomy is higher than segmental resection of a preoperatively identified bleeding site. A suggested algorithm for the evaluation of suspected acute LGI bleeding is presented in Figure 1. TIMING AND PREPARATION FOR COLONOSCOPY In patients with acute LGI bleeding necessitating hospitalization, we proceed with colonoscopic evaluation within hours of presentation. Although unprepped colonoscopy is performed by some, we believe the limited visibility, marginal benefit, and perceived increased risk for perforation from blind maneuvers through often sticky bloody material precludes this approach. In patients with active bleeding and need for urgent examination, the colon is rapidly purged with 4 6 L of a polyethylene glycol (PEG)-based solution given at a rate of1levery30minutes. The solution is given by NGT if the rate of administration is not tolerated by mouth. Unless contraindicated, the prokinetic drug metoclopramide (10 mg IV) is administered prior to the purge to hasten bowel transit and control nausea and vomiting. Colonoscopy can generally be performed within 1 2 hours upon completion of the preparation and the start of liquid discharge because dilution of blood and clots can be readily aspirated or washed away from view. Moreover, accumulation of fresh blood within the residual lavage solution enables localization of the colon segment within which active bleeding is occurring. In patients in whom bleeding seems to have stopped at the time of admission, the colon preparation can be administered in a standard and less hurried fashion, followed by colonoscopic evaluation on an elective basis the following day. COLONOSCOPIC PROCEDURE Examination We typically employ an adult colonoscope because the larger (3.7 mm) working channel facilitates clearing of blood, clots, Figure 1. Proposed algorithm for the evaluation of acute LGI bleeding. EGD = Esophagogastroduodenoscopy.
3 Acute Lower Gastrointestinal Bleeding 1883 and residual stool material, and enables passage of larger diameter hemostatic devices. The goal of the procedure is to identify a bleeding site and not cecal intubation per se. Meticulous examination, therefore, is performed both during insertion and withdrawal of the colonoscope because an intermittently bleeding lesion (e.g., diverticular or Dieulafoy) may only be identified during the insertion phase. Areas containing or accumulating fresh blood or clots are vigorously washed and examined as they are a potential harbinger of an underlying or adjacent bleeding site. Both syringe water flushes and a pedal-activated water jet irrigation device coupled to the endoscope are used for cleansing. The irrigation device is especially useful for removing adherent material from the mucosa and/or precisely pinpointing a bleeding site for targeted therapy (videoclip 1, Videoclips available online.) Examination under water immersion is also a useful technique to identify the nature and site of a bleeding lesion that is otherwise difficult to visualize (videoclip 2). Unless a definite bleeding colonic lesion is found or a specific lesion is sought (e.g., postpolypectomy bleeding), every attempt should be made to intubate the terminal ileum (TI). The presence of bilious, nonbloody fluid in the TI contrasting with fresh blood and clots in the right colon supports a colonic source of bleeding. Overview of Modalities for Hemostasis Endoscopic treatment modalities include injection, contact thermal coagulation, noncontact argon plasma coagulation, clipping, and banding. The use of one or a combination of these techniques depends on the site and features of the bleeding lesion(s), operator familiarity with the devices, and type of access to the bleeding site. General remarks regarding each of these techniques will be made, followed by our preferred endotherapeutic approach for specific LGI bleeding lesions. INJECTION THERAPY. Epinephrine injection works by volume tamponade of the bleeding vessel and transient vasoconstriction. We commonly inject a dilute epinephrine solution (1:10,000) to stop or slow active bleeding from a focal point prior to application of a more definitive therapy. We typically instill 1 3 ml of the solution per injection site, and one or more injections in and around the bleeding point are performed until hemostasis is achieved. For a nonbleeding visible vessel (NBVV), injections 1 3 mm away from (not directly into) the vessel should be performed. Similarly, epinephrine is injected around a dense adherent clot prior to clot removal performed via cold snare guillotine or with the tip of a thermal probe (videoclip 3). It is essential to avoid or minimize injection over the distal aspect of the lesion as creation of the submucosal bleb may lift the bleeding site away from view and compromise access to further therapy. Conversely, injection can be performed in a manner that improves lesion access to other therapies (videoclip 4). Although smallvolume injections ( 0.5 ml per injection; 2 ml total) of a desiccating agent (absolute ethanol) or a sclerosant (e.g., 5% ethalonamine oleate) can be effective at securing hemostasis, we almost never use these agents in the colon given the unpredictable depth of injury, increased risk for perforation, and availability of safer and equally effective alternatives. CONTACT THERMAL MODALITIES. The heater probe and bipolar electrocoagulation devices are most commonly used for coaptive (contact) coagulation of bleeding and nonbleeding visible vessels. Both modalities are similarly effective and the selection of a particular technique rests on operator familiarity and personal preference. The objective of coaptive coagulation in the thin-walled colon is to employ the least amount of power/energy and short duration of application so as to minimize the risk of perforation, while achieving the desired effect of tissue whitening and shallow cavitation. Although optimal treatment settings have not been firmly established in human trials, the following parameters for colonic applications have been found to be effective and relatively safe in our experience: 15 J for heater probe and W for bipolar; 2 3 s pulse duration; mild probe-tissue contact pressure. Several applications may be required to reach the treatment end point. The selection of the 7F or 10F bipolar or heat probes is dictated by the size of the bleeding point to be treated. Each probe enables water jet irrigation via a foot pedal for precise targeting and contact of the bleeding site with the probe. ARGON PLASMA COAGULATION. We typically reserve the use of argon plasma coagulation (APC) for the ablation of vascular ectasias, particularly when multiple or diffuse. In these situations, the noncontact approach and ease of use make APC more suitable than contact thermal techniques. The APC settings we use are W and 1 L/min argon flow rate, with 1 2 s pulses and tissue whitening as the end point. Although challenging at times, the APC probe should be fired at a distance of 1 3 mm from the target lesion. Inadvertent probe-tissue contact during activation may result in localized pneumatosis, which is immediately recognizable and often inconsequential. CLIPPING. Both reusable and single-use clipping devices are available. Although the use of the reusable device (Olympus America Inc., Center Valley, PA) is less costly and enables the selection of clips of different sizes, it requires a skillful assistant for clip loading and handling of the device. Moreover, the rotation capability of the device becomes erratic after several uses and time delay in clip reloading are disadvantageous if a short therapeutic window is available to control an actively bleeding lesion. In most situations, we employ the single-use clipping devices due to ease of use and expeditious application. We prefer the use of the Resolution clip (Boston Scientific, Natick, MA) with reopening capability or the rotatable QuickClip2Long (Olympus America Inc., Center Valley, PA) to that of the Triclip (Cook Medical Inc., Bloomington, IN). For the latter to work, the
4 1884 Wong Kee Song and Baron three-pronged configuration of the TriClip necessitates the lesion to be en face, which is not always achievable, and the thin pointy prongs may cheese wire through tissue during clip closure and aggravate or cause bleeding. Based upon results from animal studies (4,5), the duration of tissue anchoring and clip retention are longer for the Resolution clip compared with the QuickClip2, though in our experience, the clinical efficacy of the two clips appears to be comparable. When feasible, a tangential rather than perpendicular approach to the lesion and the application of suction prior to clip closure are maneuvers that allow the capture of more tissue between the two prongs. Both clips require enough soft tissue on either side of the prongs for adequate grasping. In circumstances with limited scope maneuverability and difficulty in accessing a particular lesion, the use of the QuickClip2 may be preferable as rotation of the clip may be the only maneuver that allows orientation of the clip in a favorable position. Clips work relatively well for pliable lesions that can be captured within the opened prongs (11 12 mm width span) and for mucosal defects that are less than cm in size. These defects can be closed by sequential application of clips in a zipper-like fashion. Clips are ineffective for treating a vessel within a large hard, fibrotic base and may actually precipitate torrential bleeding by causing trauma to the vessel. BANDING. Band ligation can be used for control of bleeding internal hemorrhoids or rectal varices and, in select circumstances, for treatment of focal and nonfibrotic bleeding colonic lesions that are < 2 cm in diameter. For example, we have used it for ligation of stigmata of diverticular bleeding that were otherwise difficult to access by other endoscopic means (Fig. 2). Caution with regard to the amount of tissue suctioned into the cap is warranted because of the potential for full-thickness tissue entrapment, necrosis, and resultant perforation. Management of Specific LGI Bleeding Lesions DIVERTICULAR BLEEDING. Diverticular bleeding is a common cause of acute LGI hemorrhage. Bleeding is arterial, occurring either at the neck or dome of the diverticulum. It is usually associated with painless hematochezia, although abdominal cramping may occur due to the cathartic effect of blood in the colon. Bleeding has usually stopped at the time of endoscopy although endotherapy is typically effective if an actively bleeding diverticulum or one with stigmata of recent hemorrhage is found. Our preferred approach is to use combination therapy of epinephrine injection that may evert the diverticulum for better access, followed by clipping of the vessel or the entire diverticular orifice (Fig. 3). If clipping is not feasible, contact thermal coagulation can be used cautiously, avoiding undue pressure particularly in the dome of the diverticular sac (videoclip 5). We also typically tattoo the offending diverticulum for future localization should rebleeding occur. Rarely, dense diverticular disease and a narrowed left-sided colonic lumen may impair clipping or thermal coagulation of a particular bleeding sigmoid diverticulum. In this instance, banding may be an option. Tattooing or placement of a clip adjacent to the culprit diverticulum will help localization of the latter during reinsertion of a dedicated upper endoscope equipped with the banding device, and the clip can serve as a marker for angiography should endotherapy fail. Figure 2. Banding of colonic diverticulum (A) with vessel exposure during suction through the cap (B). Postbanding appearance (C).
5 Acute Lower Gastrointestinal Bleeding 1885 Figure 3. Clipping of bleeding diverticula targeting vessel (A and B) or closure of diverticular orifice (C and D). In most instances, a diagnosis of presumed diverticular bleeding is made by the presence of colonic diverticula and by ruling out other causes at colonoscopy. At the index colonoscopy, residual blood and clots are cleared as best possible to leave a clean colon. The patient is maintained on a clear liquid diet only and typically kept in hospital for 48 h because a sizeable proportion of patients, in our practice, tend to rebleed during this time interval. Should rebleeding occur during this time period, one should be committed to promptly repeating the endoscopic examination and without reprepping the colon. This strategy maximizes the potential to identify an actively bleeding site and perhaps identify a cutoff between bloody and nonbloody areas, hence localizing the bleeding source to within a segment of the colon. In patients with recurrent bleeding after two negative colonoscopic attempts, prompt angiography as close to the timing of bleeding may identify the bleeding site and allow for super-selective transcatheter embolization using particles such as microcoils or gelfoam pledgets. Empiric embolization is not recommended in the absence of bleeding given the risk of ischemic injury. We generally do not favor radionuclide bleeding scans prior to angiography given the often inaccurate localization of the bleeding site and missed opportunity to localize and treat the lesion at angiography due to the time delay in performing the bleeding scan. POSTPOLYPECTOMY BLEEDING. Postpolypectomy bleeding may be delayed up to 1 month after polypectomy. Risk factors include the removal of large sessile right-sided colon polyps as well as resumption of anticoagulation after polypectomy. Approximately 70% of patients stop bleeding spontaneously, as evidenced by decreasing frequency or cessation of stooling, and can be managed conservatively. Urgent colonoscopy should be performed in those passing frequent bloody bowel movements suggestive of active bleeding. Given that the location(s) of the polypectomy site(s) are known a priori, some endoscopists perform colonoscopy in an unprepped colon but we prefer to purge the colon to facilitate the examination and improve the field of view. When feasible, clipping of the bleeding point, with or without epinephrine injection, is our method of choice because it does not extend tissue injury as with thermal therapy (videoclip 3). Small polypectomy defects can be completely closed by placing clips in a zipper-like fashion. However, induration within an ulcer base may hamper placement of clips, though it does provide some measure of safety for contact thermal coagulation. ANGIODYSPLASIAS. Sporadic vascular ectasias (angiodysplasias) are more commonly found in the right colon and in the elderly. Although blood loss is typically occult,
6 1886 Wong Kee Song and Baron these lesions occasionally manifest as overt LGI bleeding with orthostasis, particularly in the commonly associated setting of anticoagulation or platelet dysfunction. Although endoscopic management of an actively bleeding angiodysplasia is straightforward, decision making may be more difficult in patients who have stopped bleeding and are found to have nonbleeding angiodysplasias as well as diverticula. This is not an uncommon occurrence because both conditions affect the same age group. In this situation, we typically ablate the angiodysplasias in the absence of another definite bleeding site. Contact and noncontact thermal techniques are effective at treating vascular ectasias; clipping is less than ideal for these lesions. Our preferred method of therapy is to ablate the vascular ectasias using APC due to its ease of use and more speedy application, especially when multiple lesions are present. Prior to APC, we partially collapse the lumen but keep the lesions in view. It is important to avoid thinning of the colonic wall with excessive air insufflation as this increases the risk for perforation during therapy. Although some recommend ablation of the arborizing blood vessels starting at the periphery, we typically target the center vessel of the angiodysplasia as ensuing coagulation and edema will efface the peripheral branches and limit the extent of coagulation needed. Also, for a very large angiodysplasia, a small amount of epinephrine injected next to the central vessel will often downsize the lesion and reduce the amount and area of coagulation needed for eradication. COLITIS. Several colitides can present with acute LGI bleeding, including inflammatory bowel disease, infectious colitis, and ischemic colitis. Features in the history, stool studies, and endoscopic assessment with biopsy typically lead to the definite diagnosis. Characteristic features of ischemic colitis include the presence of longitudinal ulcers with surrounding purplish, cyanotic mucosa as well as involvement of the watershed areas. In some cases, focal significant bleeding from an ulcerated area can be targeted for endoscopic therapy. NEOPLASMS. Primary and metastatic neoplasms can manifest with acute LGI bleeding. Occasionally, there is focal bleeding from the tumor that can be temporized with coagulation therapy but bleeding is generally slow and diffuse from tumor friability. Similar to colitis, the role of endoscopy is primarily diagnostic in this setting. RECTAL OUTLET BLEEDING. Rectal outlet bleeding is characterized by intermittent, low-volume hematochezia or blood clots mixed in stool and is caused by pathology such as internal hemorrhoids, fissures, and radiation proctopathy. Diagnosis is established by inspection of the external anal canal, anoscopy, and/or flexible endoscopy. Refractory hemorrhoidal bleeding is generally managed by a colorectal surgeon at our institution. Bleeding from radiation proctopathy is best managed with APC using short bursts of coagulation for superficial ablation of the radiation-induced telangiectasias (videoclip 6). It is important not to be overly aggressive and to avoid treatment-induced deep ulcerations given poor healing of these ulcers in a previously irradiated rectum. DIEULAFOY LESION. A bleeding Dieulafoy lesion is caused by an exposed artery arising within a minute mucosal defect and, unless actively bleeding, may be difficult to detect. When seen, we prefer combination therapy with epinephrine injection and either contact thermal coagulation or clipping for eradication. CONCLUSION Acute LGI bleeding presents a more complex diagnostic and therapeutic challenge than UGI bleeding. Colonoscopy remains the mainstay of diagnosis and therapy for acute LGI bleeding. For LGI bleeding lesions that are amenable to endoscopic therapy, the proper selection of hemostatic tools and methods of use usually result in a successful outcome. Reprint requests and correspondence: Louis M. Wong Kee Song, M.D., Mayo GI Bleeding Team, Division of Gastroenterology and Hepatology, Mayo Clinic, 200 1st Street S.W., Rochester, MN REFERENCES 1. Zuccaro G. Management of the adult patient with acute lower gastrointestinal bleeding. Am J Gastroenterol 1998;93: Eisen GM, Dominitz JA, Faigel DO, et al. An annotated algorithmic approach to acute lower gastrointestinal bleeding. Gastrointest Endosc 2001;53: Davila RE, Rajan E, Adler DG, et al. ASGE Guideline: The role of endoscopy in the patient with lower GI bleeding. Gastrointest Endosc 2005;62: Jensen DM, Machicado GA, Hirabayashi K. Randomized controlled study of 3 different types of hemoclips for hemostasis of bleeding canine acute gastric ulcers. Gastrointest Endosc 2006;64: Shin EJ, Ko CW, Magno P, et al. Comparative study of endoscopic clips: Duration of attachment at the site of clip application. Gastrointest Endosc 2007;66: CONFLICT OF INTEREST Guarantor of the article: Louis M. Wong Kee Song, M.D. Specific author contributions: Dr. Wong Kee Song: manuscript preparation and drafting; Dr. Baron: critical review of manuscript. Financial support: None. Potential competing interests: None.
7 Acute Lower Gastrointestinal Bleeding 1887 Supporting Information Additional Supporting Information may be found in the online version of this article: Videoclip 1: Precise identification of bleeding site with water jet device. Videoclip 2: Pinpointing bleeding site using water immersion technique. Videoclip 3: Postpolypectomy bleeding site with adherent clot treated with epinephrine injection and clipping. Videoclip 4: Improving lesion access for definitive therapy using sub-mucosal fluid injection. Videoclip 5: Active diverticular bleeding treated with epinephrine injection and bipolar electrocoagulation. Videoclip 6: Radiation proctopathy treated with argon plasma coagulation. Please note: Blackwell Publishing are not responsible for the content or functionality of any supporting materials supplied by the authors. Any queries (other than missing material) should be directed to the corresponding author for the article.
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD
 Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
Endoscopic Treatment of Bleeding Peptic Ulcers Panagiotis Katsinelos, MD, PhD Department of Endoscopy and Motility Unit G. Gennimatas General Hospital of Thessaloniki Endoscopic diagnosis for UGI bleeding
UGI Tract Hemorrhage. GI Tract Emergencies. UGI Hemorrhage. David D. Markowitz, MD. UGI tract hemorrhage Comorbid disease
 UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
UGI Tract Hemorrhage GI Tract Emergencies GI Hemorrhage David D. Markowitz, MD Associate Professor of Clinical Medicine Columbia University, College of Physicians & Surgeons Non variceal UGI hemorrhage
Surgical Management of GI Bleeding. VA Case Presentation. 0-24 hours 9/18/2012
 Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
Surgical Management of GI Bleeding Peter C. Wu, M.D. Associate Professor of Surgery Section of Surgical Oncology University of Washington Director, Cancer Telemedicine Program VA Puget Sound VA Case Presentation
Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding.
 Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding. Through innovation and continuous educational support, we offer a wide range
Hemostasis Solutions Boston Scientific is committed to improving patient care in the management of gastrointestinal bleeding. Through innovation and continuous educational support, we offer a wide range
HOW I DO IT Approach to lower gastrointestinal bleeding
 HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
HOW I DO IT Approach to lower gastrointestinal AUTHORSHIP How I do it: Roque Sáenz MD Eduardo Valdivieso MD, MSc The Latin-American Advanced Gastrointestinal Endoscopy Training Center Clínica Alemana,
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas
 Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
Endoscopic Doppler in the Management of Upper and Lower GI Bleeding: Case Studies & Atlas Presented By: Dennis M. Jensen, MD Professor of Medicine David Geffen School of Medicine at UCLA Associate Director,
ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding
 PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
PRACTICE GUIDELINES nature publishing group 1 ACG Clinical Guideline: Management of Patients With Acute Lower Gastrointestinal Bleeding Lisa L. Strate, MD, MPH, FACG1 and Ian M. Gralnek, MD, MSHS2 This
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
LOWER GASTROINTESTINAL BLEEDING GED/05/08
 LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
How to Effectively Code for Endoscopic Procedures in Gastroenterology
 How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
LOWER GI ENDOSCOPIES So why is CMS yanking our chain? General Concepts for all GI Endoscopy Procedures
 LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
HemoClip: Guidelines & Atlas
 HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
HemoClip: Guidelines & Atlas Cases presented by: Dennis M. Jensen, MD, CURE DDRC, UCLA & VA Medical Centers, and David Geffen School of Medicine at UCLA 1 Epi Injection and Hemoclipping of Chronic Gastric
Colonoscopy Data Collection Form
 Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Lower Gastrointestinal Bleeding Author: Burt Cagir, MD, FACS; Chief Editor: Julian Katz, MD
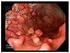 Lower Gastrointestinal Bleeding Author: Burt Cagir, MD, FACS; Chief Editor: Julian Katz, MD Reprinted with permission from Emedicine.com New users to emedicine.com will be required to register for free
Lower Gastrointestinal Bleeding Author: Burt Cagir, MD, FACS; Chief Editor: Julian Katz, MD Reprinted with permission from Emedicine.com New users to emedicine.com will be required to register for free
The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication.
 Captivator II Single-Use Snares The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare
Captivator II Single-Use Snares The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare
Evolution of Barrett s esophagus
 Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Captivator II. Single-Use Snares
 Captivator II Single-Use Snares Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare line
Captivator II Single-Use Snares Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare line
Clinical question: what is the role of colonoscopy in the diagnosis of ischemic colitis?
 Clinical question: what is the role of colonoscopy in the diagnosis of ischemic colitis? Filtered resources,, which appraise the quality of studies and often make recommendations for practice, include
Clinical question: what is the role of colonoscopy in the diagnosis of ischemic colitis? Filtered resources,, which appraise the quality of studies and often make recommendations for practice, include
Post-DDW OAG Course - Therapeutic Endoscopy
 Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
Learning Luncheon 7: Endoscopic Mucosal Resection: When, Where and How?
 Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
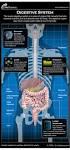 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
TEST QUESTIONS GASTROINTESTINAL BLEEDING
 TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
TEST QUESTIONS GASTROINTESTINAL BLEEDING QUESTION 1. The most frequent cause of UGI bleeding is: A. Esophageal varices B. Peptic ulcer disease C. Angiomata D. Mallory Weiss tear E. Gastritis The recommended
ESD for colorectal lesions I am in favour. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
Flexible sigmoidoscopy the procedure explained Please bring this booklet with you
 Flexible sigmoidoscopy the procedure explained Please bring this booklet with you Exceptional healthcare, personally delivered Introduction You have been advised by your GP or hospital doctor to have an
Flexible sigmoidoscopy the procedure explained Please bring this booklet with you Exceptional healthcare, personally delivered Introduction You have been advised by your GP or hospital doctor to have an
ERBEJET 2. The versatility of waterjet surgery: ERBEJET 2 with hybrid instruments WATERJET SURGERY
 ERBEJET 2 The versatility of waterjet surgery: ERBEJET 2 with hybrid instruments WATERJET SURGERY Gentle interventions in surgery and endoscopy Waterjet surgery with hybrid technology Waterjet surgery
ERBEJET 2 The versatility of waterjet surgery: ERBEJET 2 with hybrid instruments WATERJET SURGERY Gentle interventions in surgery and endoscopy Waterjet surgery with hybrid technology Waterjet surgery
These parameters cannot, at the present time, be determined by non-invasive imaging techniques.
 Endoscopic Mucosal Resection for Upper Gastrointestinal Lesions Kenneth K. Wang, M.D. Chairman, WEO Publication and Guidelines Committee Professor of Medicine, Mayo Clinic Rochester, Minnesota Upper gastrointestinal
Endoscopic Mucosal Resection for Upper Gastrointestinal Lesions Kenneth K. Wang, M.D. Chairman, WEO Publication and Guidelines Committee Professor of Medicine, Mayo Clinic Rochester, Minnesota Upper gastrointestinal
2016 Quick Reference Coding Chart
 43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D.
 Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Vikram S. Kumar Gillian Lieberman, MD. September 2002. Lower GI Bleeds. Vikram Sheel Kumar, Harvard Medical School Year III Gillian Lieberman, MD
 September 2002 Lower GI Bleeds Vikram Sheel Kumar, Harvard Medical School Year III Index Case maroon/bright red: think lower GI bleed Mr. X, 78 years old, presents w/ maroon stool and eighteen hours of
September 2002 Lower GI Bleeds Vikram Sheel Kumar, Harvard Medical School Year III Index Case maroon/bright red: think lower GI bleed Mr. X, 78 years old, presents w/ maroon stool and eighteen hours of
Acute Gastrointestinal Bleeding
 EMERGENCY MEDICINE BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Bobbie Lewis EDITOR Robert Litchkofski ASSISTANT EDITOR Melissa Frederick
EMERGENCY MEDICINE BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Bobbie Lewis EDITOR Robert Litchkofski ASSISTANT EDITOR Melissa Frederick
Captivator EMR Device
 Device Clinical Article and Abstract Summary Endoscopic Mucosal Bergman et al: EMR Training Tips Bergman et al: EMR Learning Curve ASGE: EMR & ESD Guidelines Bergman et al: Captivator EMR vs Cook Duette
Device Clinical Article and Abstract Summary Endoscopic Mucosal Bergman et al: EMR Training Tips Bergman et al: EMR Learning Curve ASGE: EMR & ESD Guidelines Bergman et al: Captivator EMR vs Cook Duette
Direct Current Therapy for Treatment of Hemorrhoids
 Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Acute lower gastrointestinal bleeding (LGIB) is distinct clinically from upper
 Gastroenterol Clin N Am 34 (2005) 665 678 GASTROENTEROLOGY CLINICS OF NORTH AMERICA Lower Gastrointestinal Bleeding Management Bryan T. Green, MD a, *, Don C. Rockey, MD b a Division of Gastroenterology,
Gastroenterol Clin N Am 34 (2005) 665 678 GASTROENTEROLOGY CLINICS OF NORTH AMERICA Lower Gastrointestinal Bleeding Management Bryan T. Green, MD a, *, Don C. Rockey, MD b a Division of Gastroenterology,
Designed by Endoscopists, Refined by Nurses & Techs An Intuitive Endoscopic Electrosurgical Platform
 Designed by Endoscopists, Refined by Nurses & Techs An Intuitive Endoscopic Electrosurgical Platform Energizing Therapeutic Endoscopy For Over 20 Years From the 1988 introduction of Argon and through a
Designed by Endoscopists, Refined by Nurses & Techs An Intuitive Endoscopic Electrosurgical Platform Energizing Therapeutic Endoscopy For Over 20 Years From the 1988 introduction of Argon and through a
Patients who fail to bring a driver/someone to stay with them for the night will have their procedure cancelled immediately.
 Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial
 Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Combined epinephrine and bipolar probe coagulation vs. bipolar probe coagulation alone for bleeding peptic ulcer: a randomized, controlled trial Maria Antonia Bianco, MD, Gianluca Rotondano, MD, Riccardo
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
Patient information on endoscopic mucosal resection (EMR) (Endoscopic removal of polyps) Your questions answered
 Patient information on endoscopic mucosal resection (EMR) (Endoscopic removal of polyps) Your questions answered Page 1 of 7 Contents What is a colonic polyp Page 3 What is an endoscopic mucosal resection
Patient information on endoscopic mucosal resection (EMR) (Endoscopic removal of polyps) Your questions answered Page 1 of 7 Contents What is a colonic polyp Page 3 What is an endoscopic mucosal resection
Emergencies in Post- Bariatric Surgery Patients
 Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Colon and Rectal Cancer
 Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
A PATIENT S GUIDE TO ABLATION THERAPY
 A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
A PATIENT S GUIDE TO ABLATION THERAPY THE DIVISION OF VASCULAR/INTERVENTIONAL RADIOLOGY THE ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL Treatment options for patients with cancer continue to expand, providing
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR)
 HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
Ischemia and Infarction
 Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
SAGES 2015 Flexible Endoscopy Course for Fellows
 Goals and Objectives: At the end of the course, the MIS fellow will be familiar with GI endoscopes, towers, and the instruments used for endoscopy and endoscopic surgery. The fellow will also be able to
Goals and Objectives: At the end of the course, the MIS fellow will be familiar with GI endoscopes, towers, and the instruments used for endoscopy and endoscopic surgery. The fellow will also be able to
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role. Lillian Khalil, BSN, RN Volunteers of America, Chesapeake
 Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Figure 2: Recurrent chest pain of suspected esophageal origin
 Figure 2: Recurrent chest pain of suspected esophageal origin 1 patient with chest pain of suspected esophageal origin 2 history and physical exam. suggestive of n-esophageal etiology? 3 evaluate and treat
Figure 2: Recurrent chest pain of suspected esophageal origin 1 patient with chest pain of suspected esophageal origin 2 history and physical exam. suggestive of n-esophageal etiology? 3 evaluate and treat
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy. Case Series
 ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
Management of the new antiplatelets and anticoagulants
 Management of the new antiplatelets and anticoagulants Session No.: 1 Name: C. Boustiere, T Ponchon Guidelines : Anti-thrombotic agents and digestive endoscopy 2006 : French guideline (SFED) 2007 : Japanese
Management of the new antiplatelets and anticoagulants Session No.: 1 Name: C. Boustiere, T Ponchon Guidelines : Anti-thrombotic agents and digestive endoscopy 2006 : French guideline (SFED) 2007 : Japanese
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
Please read the instructions 6 days before your colonoscopy.
 979-776-8440 Please read the instructions 6 days before your colonoscopy. COLONOSCOPY MIRALAX PREP SIX DAYS BEFORE THE COLONOSCOPY - Stop iron medications 6 days before your colonoscopy. - Stop taking
979-776-8440 Please read the instructions 6 days before your colonoscopy. COLONOSCOPY MIRALAX PREP SIX DAYS BEFORE THE COLONOSCOPY - Stop iron medications 6 days before your colonoscopy. - Stop taking
ENDOSCOPIC ULTRASOUND (EUS)
 ENDOSCOPIC ULTRASOUND (EUS) What you need to know before your procedure Your Doctor has decided that an EUS is necessary for further evaluation and treatment of your condition. This information sheet has
ENDOSCOPIC ULTRASOUND (EUS) What you need to know before your procedure Your Doctor has decided that an EUS is necessary for further evaluation and treatment of your condition. This information sheet has
Lower gastrointestinal bleeding in the elderly
 Online Submissions: http://www.wjgnet.com/1948-5190office [email protected] doi:10.4253/wjge.v2.i5.147 World J Gastrointest Endosc 2010 May 16; 2(5): 147-154 ISSN 1948-5190 (online) 2010 Baishideng. All
Online Submissions: http://www.wjgnet.com/1948-5190office [email protected] doi:10.4253/wjge.v2.i5.147 World J Gastrointest Endosc 2010 May 16; 2(5): 147-154 ISSN 1948-5190 (online) 2010 Baishideng. All
SIGN. Management of acute upper and lower gastrointestinal bleeding. September 2008. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 105 Management of acute upper and lower gastrointestinal bleeding A national clinical
Developing an endoscopic mucosal resection service in a district general hospital
 RESEARCH Developing an endoscopic mucosal resection service in a district general hospital Chris A Lamb, 1 Jamie A Barbour 2 1 Institute of Cellular Medicine, Newcastle University, The Medical School,
RESEARCH Developing an endoscopic mucosal resection service in a district general hospital Chris A Lamb, 1 Jamie A Barbour 2 1 Institute of Cellular Medicine, Newcastle University, The Medical School,
2015 CPT coding changes will have mixed effects on payment for general surgeons
 CPT coding changes will have mixed effects on payment for general surgeons 17 by Linda Barney, MD, FACS, and Mark T. Savarise, MD, FACS JAN BULLETIN American College of Surgeons 18 Significant changes
CPT coding changes will have mixed effects on payment for general surgeons 17 by Linda Barney, MD, FACS, and Mark T. Savarise, MD, FACS JAN BULLETIN American College of Surgeons 18 Significant changes
Peptic Ulcer. Anatomy The stomach is a hollow organ. It is located in the upper abdomen, under the ribs.
 Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
Peptic Ulcer Introduction A peptic ulcer is a sore in the lining of your stomach or duodenum. The duodenum is the first part of your small intestine. Peptic ulcers may also develop in the esophagus. Nearly
2015 Medicare Physician Fee Schedule Putting the Pieces Together for GI Colleen M. Schmitt, MD, MHA, FASGE ASGE President
 2015 Medicare Physician Fee Schedule Putting the Pieces Together for GI Colleen M. Schmitt, MD, MHA, FASGE ASGE President Glenn D. Littenberg, MD, MACP Chair, ASGE Practice Management Committee and CPT
2015 Medicare Physician Fee Schedule Putting the Pieces Together for GI Colleen M. Schmitt, MD, MHA, FASGE ASGE President Glenn D. Littenberg, MD, MACP Chair, ASGE Practice Management Committee and CPT
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Case Presentation: Diminutive polyps. Siwan Thomas-Gibson St. Marks Hospital London UK
 Case Presentation: Diminutive polyps Siwan Thomas-Gibson St. Marks Hospital London UK Case History 65 year old gentleman Bowel cancer screening FOBT positive No bowel symptoms No family history Smoker
Case Presentation: Diminutive polyps Siwan Thomas-Gibson St. Marks Hospital London UK Case History 65 year old gentleman Bowel cancer screening FOBT positive No bowel symptoms No family history Smoker
POEM Procedure for. Esophageal Achalasia
 POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
GASTRO-INTESTINAL BLEEDING
 Introduction Site of Bleeding History Physical Examination Laboratory Tests Investigation Treatment References Introduction Gastrointestinal bleeding is an uncommon but important sign in paediatric patients.
Introduction Site of Bleeding History Physical Examination Laboratory Tests Investigation Treatment References Introduction Gastrointestinal bleeding is an uncommon but important sign in paediatric patients.
Colorectal Cancer Care A Cancer Care Map for Patients
 Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Endo Conference: Large Polypectomy & EMR
 Endo Conference: Large Polypectomy & EMR Dr. Whang Feb 3, 2015 VOGELGRAM: genetic pathway of colorectal cancer & genes affected by point mutations Outline I. Baseline Colonoscopy II. Colon Polyps III.
Endo Conference: Large Polypectomy & EMR Dr. Whang Feb 3, 2015 VOGELGRAM: genetic pathway of colorectal cancer & genes affected by point mutations Outline I. Baseline Colonoscopy II. Colon Polyps III.
Common Pathology Diagnoses: ICD-9 to ICD-10 Mapping
 PERFORMANCE THAT MATTERS NUMBER OF CODES 14,000 69,000 ICD-9 DIAGNOSIS CODES ICD-10 DIAGNOSIS CODES CODE STRUCTURE ICD-9-CM CODE FORMAT ICD-10-CM CODE FORMAT X X X X X X X X X X X X CATEGORY ETIOLOGY,
PERFORMANCE THAT MATTERS NUMBER OF CODES 14,000 69,000 ICD-9 DIAGNOSIS CODES ICD-10 DIAGNOSIS CODES CODE STRUCTURE ICD-9-CM CODE FORMAT ICD-10-CM CODE FORMAT X X X X X X X X X X X X CATEGORY ETIOLOGY,
Endoscopic therapy for obesity and complications of bariatric surgery
 Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
EVIDENCE BASED TREATMENT OF CROHN S DISEASE. Dr E Ndabaneze
 EVIDENCE BASED TREATMENT OF CROHN S DISEASE Dr E Ndabaneze PLAN 1. Case presentation 2. Topic on Evidence based Treatment of Crohn s disease - Introduction pathology aetiology - Treatment - concept of
EVIDENCE BASED TREATMENT OF CROHN S DISEASE Dr E Ndabaneze PLAN 1. Case presentation 2. Topic on Evidence based Treatment of Crohn s disease - Introduction pathology aetiology - Treatment - concept of
Colorectal Cancer Screening
 Colorectal Cancer Screening Introduction Colorectal cancer (cancer of the large intestine) is the second most common cause of death from cancer in the United States, after lung cancer. However, colorectal
Colorectal Cancer Screening Introduction Colorectal cancer (cancer of the large intestine) is the second most common cause of death from cancer in the United States, after lung cancer. However, colorectal
