Utilization and Cost of Surgery for Lumbar Spinal Stenosis in a Commercially Insured Population
|
|
|
- Anna Patrick
- 10 years ago
- Views:
Transcription
1 Utilization and Cost of Surgery for Lumbar Spinal Stenosis in a Commercially Insured Population Prepared by Milliman, Inc. Kathryn Fitch, RN, MEd Principal and Healthcare Management Consultant Helen Blumen, MD, MBA Principal and Healthcare Management Consultant Tyler Engel, ASA, MAAA Associate Actuary Commissioned by Paradigm Spine, LLC Copyright 2015 Milliman. Inc.
2 TABLE OF CONTENTS EXECUTIVE SUMMARY 1 BACKGROUND 4 FINDINGS FROM COMMERCIAL CLAIM DATA ANALYSIS 5 DISCUSSION 11 APPENDIX A: METHODOLOGY 12 REFERENCES 18
3 EXECUTIVE SUMMARY Symptomatic lumbar spinal stenosis (LSS) is one of the most frequent indications for spinal surgery. Current evidence suggests that surgery for symptomatic LSS is more effective than nonoperative medical treatment when nonoperative treatment has failed to relieve symptoms after 6 months Surgical treatment of LSS typically includes decompression alone (laminectomy) or decompression with lumbar fusion. Similar clinical benefits with respect to pain, disability or walking ability have been reported in studies comparing decompression with lumbar fusion to decompression alone in the treatment of symptomatic LSS. 4 Decompression with lumbar fusion versus decompression alone for LSS results in similar reoperation/revision rates at 2 and 5 years post-surgery (for commercially insured members) and at 2 years post-surgery (for Medicare FFS beneficiaries) Higher rates of major complications, 30 day mortality and resource use have been reported following decompression with lumbar fusion compared to decompression alone This analysis was intended to quantify the frequency and cost of LSS related decompression and lumbar fusion surgeries in a commercially insured population as well as the portion of cases that had a decompression or lumbar fusion in the preceding 4 years. In addition, we modeled the cost impact of replacing a portion of lumbar fusion cases with decompression and use of an intralaminar lumbar stabilization (ILS) device. An ILS is a motionpreserving stabilization device for the lumbar spine, inserted during decompression surgery as an alternative to spinal fusion. Table 1 provides the number of all decompressions and lumbar fusions (LSS- and non LS- related) and the allowed cost per member per month ($PMPM) associated with these procedures. LSS-related decompressions cost $0.54 PMPM and account for 37% of lumbar decompressions while LSS-related lumbar fusions cost $2.13 PMPM and account for 50% of total lumbar fusions. The total $PMPM in 2013 for our denominator population was $ Table 1: 2013 Count and Cost of Lumbar Fusions and Decompressions Surgical Decompressions All (LSS- and non LSS- Related) LSS-related Only % Total that are LSS- Related Allowed $PMPM for All Allowed $PMPM for LSS-Related % Total Procedure $PMPM Contributed by LSS- Related 28,009 12,752 46% $1.45 $ % Lumbar Fusions 20,987 9,764 47% $4.25 $ % Total 48,996 22,516 46% $5.70 $ % Source: Milliman analysis of 2013 MarketScan commercial data. See methodology section of this report. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. Based on a 4 year longitudinal look back analysis, we identified 83% of the 2013 LSS related lumbar fusions and 90% of the LSS related decompressions as primary surgeries those having no claims for a decompression or lumbar fusion in the preceding 4 years. Table 2 shows the number, frequency, and cost of 2013 LSS related surgeries, split by whether the surgeries are primary or secondary. October
4 Table 2: Primary and Secondary Surgeries for Lumbar Spinal Stenosis LSS-related Spinal Procedure Type Surgical Decompressions Lumbar Fusions 2013 Procedure Count Frequency of Decompressions and Fusions in Preceding 4 years Count of 2013 by Number of Preceding Decompressions/ Fusions % of 2013 by Number of Preceding Decompressions/ Fusions Allowed $PMPM for 12,752 0 (primary) 11,463 90% $ (secondary) 1,289 10% $0.06 9,764 0 (primary) 8,113 83% $ (secondary) 1,651 17% $0.36 Total 22,516 22,516 $2.67 Source: Milliman analysis of MarketScan commercial data. See methodology section of this report. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. Using the assumptions in Table 3, we considered the potential cost impact of replacing a portion of LSS related primary lumbar fusions with the cost of a decompression and ILS device. Table 3: Cost Assumptions for Replacing a Portion of Lumbar Fusions with Decompression and ILS device Allowed Cost Based on MarketScan 2013 Analysis Average cost of a lumbar fusion $65,509 Average cost of a decompression without ILS device* $12,749 Average cost of ILS device** $7,000 Allowed $PMPM for primary lumbar fusions $1.77 Allowed total population $PMPM $ Source: Milliman analysis of 2013 MarketScan commercial data. See methodology section of this report. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. Primary fusion are those without fusion or decompression claims in prior 4 years. ILS: intralaminar stabilization device. Average cost of a lumbar fusion and decompression is based on the average cost of the combined primary and secondary cases for each surgery. * Fewer than 10 of the decompression cases had a claim for an ILS device. **Cost of ILS device was provided by Paradigm Spine, LLC. Based on the assumptions in Table 3, Table 4 provides the potential PMPM cost impact associated with 20%, 30% and 40% replacement of primary fusions with the cost of decompressions and ILS device. We assumed that there was no difference in post-operative costs when replacing lumbar fusions. We assumed no difference in the impact on revision/reoperations based on a 2015 published study reporting no statistically significant difference in 4 year revision/reoperation rates following LSS-related decompression with spinal fusion versus LSS-related decompression with an ILS device. 10 We assumed that the average cost of a decompression found in our MarketScan analysis accurately reflects a decompression that does not include ILS device costs, because we found that fewer than 10 decompressions in our analysis had a claim for an ILS device. Table 4: Potential Cost Impact of Replacement of Primary Fusions with Decompression and ILS Device 20% 30% Replacement Replacement Potential allowed $PMPM impact associated with replacing primary fusions with the cost of decompression and ILS device 40% Replacement ($0.25) ($0.37) ($0.49) Source: Milliman analysis of 2013 MarketScan commercial data. See methodology section of this report. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment Cost of decompressions and fusions for inpatient procedures include all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. Primary fusions are those without fusion or decompression claims in prior 4 years. ILS: intralaminar stabilization device. Average cost of a lumbar fusion and decompression is based on the average cost of the combined primary and secondary cases for each surgery. Fewer than 10 of the decompression cases had a claim for an ILS device. October
5 Increasing utilization and significant regional variation in rates of spinal fusion surgery have been reported over the past 25 years. A Dartmouth Atlas publication reported a 67% increase in the rate of spinal fusion surgery for LSS among Medicare FFS beneficiaries from 2001 to 2011 with the rate varying by a factor of more than fourteen across hospital referral regions. 11 A United Health Care commercial claim data analysis, based on a 25 million member population, reported an overall 41% increase in lumbar fusions for lumbar spine conditions (not limited to LSS) between 2004 and 2009 and regional variation in the rate of spinal fusion being 2.5 times as high in some regions compared to others. 12 An investigation by payers and employers for opportunities to impact these patterns appears warranted. This report was commissioned by Paradigm Spine, which manufactures Coflex, an intralaminar stabilization device indicated for use in decompression surgeries for LSS. One of the authors, Tyler Engel, is a member of the American Academy of Actuaries and meets its qualification standards for this communication. The findings reflect the research of the authors; Milliman does not intend to endorse any product or organization. If this report is reproduced, we ask that it be reproduced in its entirety, as pieces taken out of context can be misleading. As with any economic or actuarial analysis, it is not possible to capture all factors that may be significant. Because we present national average data, the findings should be interpreted carefully before they are applied to any particular situation. These results are based on analysis of Truven MarketScan commercial data for procedures performed in Different data sets, time periods and methodologies will produce different results. October
6 BACKGROUND Symptomatic lumbar spinal stenosis (LSS) is one of the most frequent indications for spinal surgery. LSS is a narrowing of the space within the vertebrae where spinal nerves pass, which can lead to intermittent neurogenic claudication pain in the leg that occurs during walking or standing and is relieved with sitting down or bending forward. LSS can be congenital or acquired, with the most common cause being acquired age-associated degeneration of the lumbar discs and facet joints. Radiographic CT diagnosed prevalence rates for acquired LSS were reported to be 20% (< 12mm) and 4% (< 10mm) in < 40 year olds and 42% (< 12mm) and 19% (< 10mm) in year olds, yet the majority of individuals were asymptomatic. 13 The management of LSS depends on the severity of the symptoms. For mild symptoms, nonoperative treatment with analgesics, physical therapy and exercises, and/or epidural steroid injections is recommended. For more severe symptomatic LSS where nonoperative treatment has failed, surgery is suggested. Decompression surgery is done to relieve pressure on impinged nerves in the spinal column, and decompression surgeries include partial or total laminectomy, hemilaminectomy, laminotomy and medical facetectomy. Insertion of an ILS device at the time of decompression as a motion preserving stabilization device became an option with FDA approval in October, Fusion, done in conjunction with decompression, joins two or more adjacent vertebrae to stabilize the spine and can be done with or without instrumentation. Current evidence suggests that spinal surgery for symptomatic LSS is more effective than nonoperative treatment, when nonoperative treatment has failed to relieve symptoms after 6 months Similar clinical benefits with respect to pain, disability or walking ability have been reported in studies comparing decompression with lumbar fusion to decompression alone in the treatment of symptomatic LSS. 4 Decompression with lumbar fusion versus decompression alone for LSS results in similar reoperation/revision rates at 2 and 5 years post- surgery (for commercially insured members) and at 2 years post-surgery (for Medicare fee-for-service beneficiaries) A 2015 clinical study reported no statistically significant difference in 4 year revision/reoperation rates following LSS related decompression with spinal fusion versus LSS related decompression with an ILS device. 10 Higher rates of major complications, 30 day mortality and resource use have been reported for decompression with lumbar fusion compared to decompression alone In this context, we analyzed the frequency and cost of LSS-related decompression and lumbar fusion surgeries in a commercially insured population as well as the portion of cases that had a decompression or lumbar fusion in the preceding 4 years. In addition, we calculated the potential cost impact of replacing a portion of primary lumbar spinal fusion surgeries with decompression and ILS. October
7 FINDINGS FROM COMMERCIAL CLAIM DATA ANALYSIS 2013 Snapshot analysis We used the 2013 Truven Health Analytics MarketScan (MarketScan) commercial data to identify the incidence and annual cost of LSS related spinal procedures including pain injections, epidural injections, decompressions and fusions (see methodology for details of identification criteria). Figure 1 provides demographic characteristics of the 22,968 members with an LSS-related spinal procedure. The majority of patients are older than 50, and men account for 53.2% of the patients having an LSS-related procedure. Figure 1: 2013 Demographics of Patients with an LSS Related Spinal Procedure Claim 14.0% % of Patietns Having an LSS- Related Spinal Procedure 12.0% 10.0% 8.0% 6.0% 4.0% 2.0% 5.2% 4.6% 4.0% 3.3% 2.3% 2.2% 1.1% 0.8% 1.0% 0.7% 6.7% 6.6% 9.4% 9.3% 12.1% 11.5% 10.2% 8.9% Male Female 0.0% years years years years years years years years years Age/Gender Source: Milliman analysis of 2013 MarketScan data. See methodology for identification of spinal procedures. Total number of patients with an LSSrelated spinal procedure=22,968. LSS-related procedures include pain injections, epidural steroid injections, decompressions and fusions. Table 5 provides summary data on the MarketScan 2013 denominator population meeting our standard inclusion criteria (see methodology), as well as the number and incidence rates of patients with an LSS related spinal procedure. Although our interest in this report is LSS related spinal procedures, we also provide incidence of all spinal decompressions and fusions (LSS and non LSS related) to provide context for the portion of total procedures that are LSS related. The counts in Table 5 reflect the number of members with the indicated procedure and do not reflect the count of procedures. October
8 Table 5: 2013 LSS-Related Spinal Procedure Member Count and Incidence Cohort Description Member Sample Size and Incidence Rate 2013 MarketScan Denominator Population for Snap Shot Analysis (age 0-64) 29,584,715 Number of year olds having a lumbar decompression surgery 26,888 Incidence of year olds having a lumbar decompression surgery 0.091% Number of year olds having an LSS-related lumbar decompression surgery 12,236 Incidence of year olds having an LSS-related lumbar decompression surgery 0.041% Number of year olds having a lumbar fusion surgery 20,408 Incidence of year olds having a lumbar fusion surgery 0.069% Number of year olds having an LSS-related lumbar fusion surgery 9,588 Incidence of year olds having an LSS-related lumbar fusion surgery 0.032% Number of year olds having an LSS-related spinal procedure (pain injections, epidural steroid injections, decompressions and fusions) Incidence of year olds having an LSS-related spinal procedure (pain injections, epidural steroid injections, decompressions and fusions) Source: Milliman analysis of 2013 MarketScan data. See methodology for identification of spinal procedures 22, % Some members had more than one procedure in 2013, and the total number of procedures is shown in Table 6. To calculate the contribution of LSS related spinal procedures to total population spend, we calculated a PMPM cost associated with each procedure based on all claim costs across each procedure type divided by the total population s member months. Cost of decompressions and fusions for inpatient procedures include all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. ILS device claims were identified in fewer than 10 decompression cases and were included in the average cost calculation of a decompression. For pain injections and epidural steroid injections, costs include all claim line allowed costs on the procedure claim. Table 6 provides the allowed PMPM cost as well as the utilization/1000 members and the average cost per procedure. The 2013 Denominator Population $PMPM was $ October
9 Table 6: 2013 Utilization and Cost of LSS-Related Spinal by Site of Service Spinal Procedure Type Site of Service Total Procedure Counts Average Allowed Cost per Procedure Utilization of each Procedure/ 1000 Members Allowed $PMPM for Pain Injections Outpatient 2,852 $1, $0.01 Epidural Steroid Injections Surgical Decompressions Surgical Decompressions Lumbar Fusions Lumbar Fusions Outpatient 18,607 $1, $0.06 Inpatient 3,740 $20, $0.26 Outpatient 9,012 $9, $0.28 All Surgical Decompressions 12,752 $12, $0.54 Inpatient 9,244 $67, $2.08 Outpatient 520 $27, $0.05 All Lumbar Fusions 9,764 $65, $2.13 Total 43, $2.75 Source: Milliman analysis of 2013 MarketScan data. See methodology for identification of spinal procedures. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. For pain injections and epidural steroid injections, cost include all claim line allowed costs on the procedure claim Table 7 compares the portion of LSS related lumbar fusions and decompressions to all lumbar fusions and decompressions on a procedure count basis and on a PMPM cost basis. The LSS related procedures account for 37% of the decompression $PMPM and 50% of the spinal fusion $PMPM. Table 7: Allowed 2013 $PMPM for Lumbar Fusions and Decompressions Surgical Decompressions All LSS related Only % Total that are LSS Related Allowed $PMPM for all Allowed $PMPM for LSS Related % Total Procedure $PMPM Contributed by LSS Related 28,009 12,752 46% $1.45 $ % Lumbar fusions 20,987 9,764 47% $4.25 $ % Total 48,996 22,516 46% $5.70 $ % Source: Milliman analysis of 2013 MarketScan data. See methodology for identification of LSS related lumbar fusion and decompression Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. October
10 Longitudinal Analysis We performed a longitudinal analysis in order to identify the portion of 2013 LSS related decompressions and fusions that were primary (no prior decompression or fusion in the 4 previous years) and secondary (1+ fusion or decompression in the prior 4 years). We performed a 4 year look back to identify the presence of prior decompressions and/or fusions. The look back required that the 2013 snapshot analysis members with decompressions and fusions have eligibility all months of This limited the 2013 starting denominator population to 6,006,693 and the number of decompressions to 3,393 and fusions to 2,608. Table 8 provides the incidence of 2013 decompressions and fusions that were primary and secondary based on the 4 year look back. In the 4 years prior to 2013 ( ), 10% of the patients undergoing decompressions in 2013 had a claim for at least one prior decompression or fusion, and 17% of the patients undergoing fusions in 2013 had a claim for at least one prior decompression or fusion. Table 8: 2013 LSS Related Spinal by Frequency of Decompression or Fusion in Prior 4 Years Distribution of Number of by 2013 LSS Related Number of Fusions in Decompressions in Total Preceding Number of Procedure Type Preceding 4 Years Preceding 4 Years Decompressions or Fusions % % Pain Injections % Epidural Steroid Injections Surgical Decompressions Lumbar Fusions % 0 0 4,095 83% % % % 0 0 3,050 90% % % % 0 0 2,167 83% % % % Total 11,798 Source: Milliman analysis of MarketScan data. See methodology for details of longitudinal analysis. October
11 Table 9 provides the years in which the previous decompressions and fusions occurred for those cases with prior decompression and fusions. For decompressions, the majority of the preceding decompressions and fusions occurred in the same or previous year; for fusions, the majority of previous procedures occurred in the same or previous 2 years. Table 9: Distribution of Prior Surgeries by Longitudinal Years 2013 LSS Related Procedure Type Surgical Decompressions Lumbar Fusions Number of Decompression / Fusions in Preceding 4 Years Total 2013 Year of Preceding Procedure ,050 N/A N/A N/A N/A N/A (6%) 28 (10%) 39 (13%) 70 (24%) 135 (47%) (15%) 8 (9%) 19 (22%) 29 (34%) 17 (20%) (13%) 8 (26%) 4 (13%) 6 (19%) 9 (29%) 0 2,167 N/A N/A N/A N/A N/A (13%) 55 (15%) 59 (16%) 99 (28%) 101 (28%) (8%) 35 (27%) 23 (17%) 35 (27%) 29 (22%) (24%) 10 (20%) 8 (16%) 10 (20%) 10 (20%) Source: Milliman analysis of MarketScan data. See methodology for details of longitudinal analysis. In Table 10, we applied the distribution of LSS related procedures identified as primary and secondary in the longitudinal analysis, to the 2013 snapshot analysis LSS related procedure counts. We calculated a $PMPM for each category of LSS related spinal procedures. The biggest contributor to LSS related spinal procedures was primary lumbar fusions (no prior decompression or fusion in preceding 4 years) with an amount of $1.77 PMPM. Table 10: Application of Longitudinal Analysis Primary and Secondary LSS Related Spinal Procedure Counts to 2013 Snapshot Analysis Count of 2013 Percentage of Number of by Decompressions Allowed LSS Related Spinal Number of by Number of Procedure and Fusions in $PMPM of Procedure Type Preceding Preceding Count Preceding 4 Decompressions Decompressions/ years / Fusions Fusions 2, ,012 71% $0.007 Pain Injections % $ % $ % $ , ,378 83% $0.053 Epidural Steroid 1 2,644 14% $0.009 Injections % $ % $0.000 Surgical Decompressions Lumbar Fusions 12, ,463 90% $ ,090 9% $ % $ % $ , ,113 83% $ ,344 14% $ % $ % $0.013 Total 43,975 43,975 $2.75 Source: Milliman analysis of 2013 MarketScan commercial data. See methodology section. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed cost (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. Primary fusion are those without fusion or decompression claims in prior 4 years. October
12 Cost Impact of Replacing LSS-related Primary Lumbar Fusion by Decompression Plus ILS Device Our goal in this analysis was to consider the potential cost impact of replacing a portion of LSS-related primary lumbar fusions with decompression and intralaminar stabilization (ILS) device. Table 11 lists our cost assumptions, using the results of our 2013 MarketScan snapshot analysis. Table 11: Cost Assumptions for Replacing a Portion of Lumbar Fusions with Decompression and ILS device Allowed Cost Based on MarketScan 2013 Analysis Average cost of a lumbar fusion $65,509 Average cost of a decompression without ILS device* $12,749 Average cost of ILS device** $7,000 Allowed $PMPM for primary lumbar fusion $1.77 Allowed total population $PMPM $ Source: Milliman analysis of 2013 MarketScan commercial data. See methodology section. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed costs (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. Primary fusions are those without fusion or decompression claims in prior 4 years. ILS: intralaminar stabilization. Average cost of a lumbar fusion and decompression is based on the average cost of the combined primary and secondary cases for each surgery. *Fewer than 10 of the decompression cases had a claim for an ILS device. **Cost of ILS device was provided by Paradigm Spine, LLC. Based on the average cost assumptions in Table 11, we calculated the potential PMPM cost impact associated with 20%, 30% and 40% replacement of primary fusions with decompressions and an ILS device. The cost impact calculations assumes adding the cost of a $7,000 ILS device to each case. We assumed that there was no difference in post-operative costs for the different surgical options. We also assumed that there was no difference in the rate of revisions or reoperations for the different surgical options. This assumption is based on a 2015 clinical study reporting no statistically significant difference in 4 year revision/reoperation rates following LSS related decompression with spinal fusion versus LSS related decompression with an ILS device. 10 We did not consider any cost impact of adding an ILS device to 2013 primary decompressions. Table 12 shows the results of our calculations. We calculated a potential $0.25 to $0.49 PMPM lower cost with replacement of 20-40% of primary lumbar fusions with lumbar decompression and ILS devices. Table 12: Potential Cost Impact of Replacement of Primary Fusions with Decompression and ILS Device 20% Replacement 30% Replacement 40% Replacement Potential allowed $PMPM impact associated with replacing primary fusions with the cost of decompression and ILS device ($0.25) ($0.37) ($0.49) Source: Milliman analysis of 2013 MarketScan commercial data. See methodology section. Allowed cost includes the amount contracted by the payer with the provider, including the member s cost sharing payment. Cost of decompressions and fusions for inpatient procedures includes all allowed costs (facility and professional) from admission through discharge date and for outpatient procedures, all allowed costs on the day of the outpatient procedure. Primary fusion are those without fusion or decompression claims in prior 4 years. ILS: intralaminar stabilization device. Average cost of a lumbar fusion and decompression is based on the average cost of the combined primary and secondary cases for each surgery. Cost impact assumes adding the cost of ILS to each decompression ($7000) since fewer than 10 of the decompression cases had a claim for an ILS device. October
13 DISCUSSION The use of lumbar fusion surgery in the United States has increased significantly over the past 25 years. A retrospective cohort study using national sample administrative data from the Healthcare Cost and Utilization Project (HCUP) Nationwide Inpatient Sample from 1988 through 2001 reported a 220% increase in lumbar fusions for lumbar spine conditions (not limited to LSS) from 1990 to A Dartmouth Atlas publication reports a 67% increase in the rate of spinal fusion surgery for LSS among Medicare fee for service beneficiaries from 31.6/100,000 beneficiaries in 2001 to 52.7/100,000 beneficiaries in A United Health Care commercial claim data analysis, based on a 25 million member population, reported an overall 41% increase in lumbar fusions for lumbar spine conditions (not limited to LSS) between 2004 and 2009, increasing from a rate of 11.6/10,000 members to 16.4/10,000 members. Another Medicare analysis identified a 15 fold increase in complex fusions for LSS between 2002 and 2007 while the rate of simple fusions and decompressions fell. 8 There is also significant regional variation in the rate of spinal fusion. A Dartmouth Atlas publication reports the rate of spinal fusion surgery for LSS among Medicare fee for service beneficiaries varying by a factor of more than fourteen across hospital referral regions in A United Health Care commercial claim data analysis based on a 25 million member population, reported 2.5 times as high a rate of lumbar fusions for lumbar spine conditions (not limited to LSS) in some regions compared to others. 13 Our analysis identified LSS related primary lumbar spinal fusions (that is, lumbar spinal fusion that did not represent a reoperation, based on a 4 year lookback) contribute $1.77 PMPM of allowed costs for the commercially-insured population. We also identified a $0.25-$0.49 lower PMPM associated with replacing 20%-40% of the primary lumbar spinal fusions with surgical decompression and stabilization with an ILS device. Payers and employers may have an opportunity to favorably impact the cost of care for patients with LSS, without adversely affecting clinical outcomes. October
14 APPENDIX A: METHODOLOGY Data Source Truven Health Analytics MarketScan Commercial Claims Database The Truven Health Analytics MarketScan Commercial Claims Database (MarketScan) contains all paid claims generated by million commercially insured lives annually (depending on the year of data). The MarketScan database represents the inpatient and outpatient healthcare service use of individuals nationwide who are covered by the benefit plans of large employers, health plans, government, and public organizations. The data includes diagnosis codes, procedure codes, DRG codes, and NDC codes, along with site of service information and the amounts paid by commercial insurers. The MarketScan database links paid claims and encounter data to detailed patient information across sites and to types of providers. Patient identifiers are consistent over time, allowing for longitudinal studies. The annual medical database includes private sector health data from approximately 100 payers. We used the MarketScan data from Claim Data Analysis Step 1: Identified the 2013 denominator population The denominator population for the 2013 snapshot analysis included members with: At least one month of coverage in 2013 Prescription drug coverage Not covered by a capitated plan Not covered by Medicare Inclusive of employees and dependents Step 2: Identified all LSS related spinal procedures occurring in 2013 among year olds using the code list below. List of ICD9 Procedure and CPT/HCPCS codes used to identify LSS related spinal procedures Procedure Code Description Treatment/Procedure Type HCPCS Injection(s); single or multiple trigger point(s), 1 or 2 muscle(s) Other Pain Inject HCPCS Injection(s); single or multiple trigger point(s), 3 or more muscle(s) Other Pain Inject HCPCS Lateral lumbar spine fusion Fusion HCPCS Lateral thoracic/lumbar additional segment Fusion HCPCS Lumbar spine fusion Fusion HCPCS Additional spinal fusion Fusion HCPCS Presacral fusion w/ instrumentation L5-S1 Fusion HCPCS Lumbar spine fusion Fusion HCPCS Spine fusion extra segment Fusion HCPCS Lumbar spine fusion Fusion HCPCS Spine fusion extra segment Fusion HCPCS Lumbar spine fusion combined Fusion HCPCS Spine fusion extra segment Fusion October
15 Procedure Code HCPCS HCPCS Description Posterior non-segmental instrumentation (e.g., Harrington rod technique, pedicle fixation across 1 interspace, atlantoaxial transarticular screw fixation, sublaminar wiring at C1, facet screw fixation) (List separately in addition to code for primary procedure) Injection/infusion of neurolytic substance (e.g., alcohol, phenol, iced saline solutions), with or w/o other therapeutic substance; epidural, lumbar, sacral Treatment/Procedure Type Fusion HCPCS Inject spine lumbar/sacral Epidural HCPCS Injection(s), including indwelling catheter placement, continuous infusion or intermittent bolus Other Pain Inject Other Pain Inject HCPCS Remove spine lamina 1/2 lumbar Decompression HCPCS Remove spine lamina >2 lumbar Decompression HCPCS Low back disk surgery Decompression HCPCS Spinal disk surgery add-on Decompression HCPCS Laminotomy single lumbar Decompression HCPCS Laminotomy additional lumbar Decompression HCPCS Remove spine lamina 1 lumbar Decompression HCPCS Remove spinal lamina add-on Decompression HCPCS Decompress spinal cord lumbar Decompression HCPCS Decompress spine cord add-on Decompression HCPCS Injection, anesthetic agent; spinal accessory nerve Other Pain Inject HCPCS Injection foramen epidural cervical/thoracic Epidural HCPCS Injection foramen epidural add-on Epidural HCPCS Injection foramen epidural lumbar/sacral Epidural HCPCS Injection foramen epidural add-on Epidural HCPCS HCPCS HCPCS HCPCS Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with image guidance (fluoroscopy or CT), lumbar or sacral; single level Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with image guidance (fluoroscopy or CT), lumbar or sacral; second level (List separately in addition to code for primary procedure) Injection(s), diagnostic or therapeutic agent, paravertebral facet (zygapophyseal) joint (or nerves innervating that joint) with image guidance (fluoroscopy or CT), lumbar or sacral; third and any additional level(s) (List separately in addition to code for primary procedure Injection, anesthetic agent; lumbar or thoracic (paravertebral sympathetic) HCPCS Epidurography, radiological supervision and interpretation Epidural Other Pain Inject Other Pain Inject Other Pain Inject Other Pain Inject HCPCS 0171T Insertion of posterior spinous process distraction device, single level Decompression HCPCS 0172T Insertion of posterior spinous process distraction device, each additional level Decompression October
16 Procedure Code HCPCS HCPCS 0230T T Description Injection(s), anesthetic agent and/or steroid, transforaminal epidural, with us guidance, lumbar or sacral, single level Injection(s), anesthetic agent and/or steroid, transforaminal epidural, with us guidance, lumbar or sacral, each additional level Treatment/Procedure Type Epidural Epidural HCPCS 0275T Percutaneous laminotomy/laminectomy, lumbar Decompression HCPCS 0309T Arthrodesis, pre-sacral interbody technique, discectomy, lumbar, L4-5 interspace Fusion HCPCS C1821 Interspinous process distraction device (implantable) Decompression ICD-9 Proc reopening of laminectomy site Decompression ICD-9 Proc other exploration and decompression of spinal canal Decompression ICD-9 Proc anaesthesia inject-spin canal Epidural ICD-9 Proc spinal canal inject not elsewhere classified Epidural ICD-9 Proc excision/destruction intervertebral disc not otherwise specified Decompression ICD-9 Proc excision intervertebral disc Decompression ICD-9 Proc spinal fusion nos Fusion ICD-9 Proc dorsal/dorsal-lumbar anterior/anterior fusion anterior/anterior Fusion ICD-9 Proc dorsal/dorsal-lumbar fusion posterior/posterior Fusion ICD-9 Proc lumbar/lumbosacral fusion anterior/anterior Fusion ICD-9 Proc lumbar/lumbosacral fusion posterior/posterior Fusion ICD-9 Proc lumbar/lumbosacral fusion anterior/posterior Fusion ICD-9 Proc spinal refusion not otherwise specified Fusion ICD-9 Proc refusion dorsal/dorsal-lumbar anterior/anterior Fusion ICD-9 Proc refusion dorsal/dorsal-lumbar posterior/posterior Fusion ICD-9 Proc refusion lumbar/lumbosacral anterior/anterior Fusion ICD-9 Proc refusion lumbar/lumbosacral posterior/posterior Fusion ICD-9 Proc refusion lumbar/lumbosacral anterior/posterior Fusion ICD-9 Proc refusion of spine not elsewhere classified Fusion ICD-9 Proc ins spinal fusion device Fusion ICD-9 Proc insertion/replacement interspine device Decompression ICD-9 Proc revision interspine device Decompression ICD-9 Proc Insert/replace facet replacement device Decompression ICD-9 Proc rev facet replace device Decompression October
17 Step 3: Included only procedures that had: An LSS ICD-9 diagnosis code on the procedure claim: , , , OR an LSS associated DRG for the inpatient procedure and LSS coded on 1+ claim during 2013 see table below OR an LSS associated ICD-9 diagnosis code on the primary position of the outpatient procedure and LSS coded on 1+ claim during 2013 see table below Excluded all scoliosis cases identified as procedures coded with the following ICD-9 diagnosis codes in any position of the claim: , DRGs and Primary ICD-9 Diagnosis codes required for IP and OP without an LSS diagnosis coded on the procedure Procedure Code Description DRG 028 Spinal procedures w MCC DRG 029 Spinal procedures w CC or spinal neurostimulators DRG 030 Spinal procedures w/o CC/MCC DRG 453 Combined anterior/posterior spinal fusion w MCC DRG 454 Combined anterior/posterior spinal fusion w CC DRG 455 Combined anterior/posterior spinal fusion w/o CC/MCC DRG 456 Spinal fusion except cervical with spinal curvature/malignancy/infection or 9+ fusion w MCC DRG 457 Spinal fusion except cervical with spinal curvature/malignancy/infection or 9+ fusion w CC DRG 458 Spinal fusion except cervical with spinal curvature/malignancy/infection or 9+ fusion w/o CC/MCC DRG 459 Spinal fusion except cervical w MCC DRG 460 Spinal fusion except cervical w/o MCC DRG 052 Spinal disorders & injuries w CC/MCC DRG 053 Spinal disorders & injuries w/o CC/MCC DRG 490 Back & neck proc except spinal fusion w CC/MCC or disc device/neurostimulator DRG 491 Back & neck proc except spinal fusion w/o CC/MCC DRG 518 Back & Neck Proc Except Spinal Fusion W MCC Or Disc Device/Neurostimulator DRG 519 Back & Neck Proc Except Spinal Fusion W CC DRG 520 Back & Neck Proc Except Spinal Fusion W/O CC/MCC DRG 551 Medical back problems w MCC DRG 552 Medical back problems w/o MCC DRG 553 Bone diseases & arthropathies w MCC DRG 554 Bone diseases & arthropathies w/o MCC DRG 555 Signs & symptoms of musculoskeletal system & conn tissue w MCC October
18 Procedure Code Description DRG 556 Signs & symptoms of musculoskeletal system & conn tissue w/o MCC DRG 559 Aftercare, musculoskeletal system & connective tissue w MCC DRG 560 Aftercare, musculoskeletal system & connective tissue w CC DRG 561 Aftercare, musculoskeletal system & connective tissue w/o CC/MCC DRG 856 Postoperative or post-traumatic infections w O.R. proc w MCC DRG 857 Postoperative or post-traumatic infections w O.R. proc w CC DRG 858 Postoperative or post-traumatic infections w O.R. proc w/o CC/MCC DRG 862 Postoperative & post-traumatic infections w MCC DRG 863 Postoperative & post-traumatic infections w/o MCC ICD-9 Diag acute postop pain not elsewhere classified ICD-9 Diag acute pain not elsewhere classified ICD-9 Diag chronic postop pain not elsewhere classified ICD-9 Diag chronic pain not elsewhere classified ICD-9 Diag chronic pain syndrome ICD-9 Diag cauda equina syndrome not otherwise specified ICD-9 Diag neurogenic bladder ICD-9 Diag lumbosacral plexus lesion ICD-9 Diag lumbosacral root lesion not elsewhere classified ICD-9 Diag sciatic nerve lesion ICD-9 Diag spondylopathy in other diseases ICD-9 Diag lumbosacral spondylosis ICD-9 Diag Spondylopathy with compression of lumbar spinal cord ICD-9 Diag spinal disorders not elsewhere classified ICD-9 Diag spondylosis not otherwise specified w/o myelopathy ICD-9 Diag spondylosis not otherwise specified w myelopathy ICD-9 Diag lumbar disc displacement ICD-9 Diag disc displacement not otherwise specified ICD-9 Diag lumbar/lumbosacral disc degeneration ICD-9 Diag disc degeneration not otherwise specified ICD-9 Diag disc disease w myelopathy not otherwise specified ICD-9 Diag lumbar disc disease w myelopathy ICD-9 Diag postlaminectomy syndrome not otherwise specified ICD-9 Diag postlaminectomy syndrome-lumbar ICD-9 Diag disc disease not elsewhere classified/not otherwise specified-unspecified ICD-9 Diag disc disease not elsewhere classified c/nos-lumbar ICD-9 Diag spinal stenosis not otherwise specified ICD-9 Diag spinal stenosis, lumbar wo claudication ICD-9 Diag spin stenosis, lumbar w claudication ICD-9 Diag lumbago October
19 Procedure Code Description ICD-9 Diag sciatica ICD-9 Diag lumbosacral neuritis not otherwise specified ICD-9 Diag backache not otherwise specified ICD-9 Diag disorders of sacrum ICD-9 Diag other back symptoms ICD-9 Diag back disorder not otherwise specified ICD-9 Diag postlaminectomy kyphosis ICD-9 Diag postlaminectomy lordosis ICD-9 Diag other postsurgery lordosis ICD-9 Diag lumbosacral spondylolysis ICD-9 Diag spondylolisthesis ICD-9 Diag V57.89 rehabilitation proc not elsewhere classified ICD-9 Diag V57.9 rehabilitation procedure not otherwise specified ICD-9 Diag V58.78 aftercare surgery musculoskeletal system not elsewhere classified Step 4: Calculated costs We identified site of service of LSS related procedures using POS codes 21 for inpatient and 11, 22, 24 for outpatient. All costs from admission through discharge date are included in the cost of an inpatient LSS related decompression and fusion. All costs on the day of an outpatient procedure are included in the cost of an outpatient LSS related decompression and fusion. We calculated the average cost of decompression and fusion using the weighted average of the inpatient and outpatient cases. The average cost of an LSS related outpatient pain injection and epidural treatment reflect all claim line cost for each pain injection and epidural claim. To calculate a $PMPM cost associated with each procedure, we added the claim cost of all procedures and divided by the total member months of the denominator population. October
20 REFERENCES 1 Kovacs FM, Urrutia G, Alarcon JD. Surgery versus conservative treatment for symptomatic lumbar spinal stenosis: a systematic review of randomized controlled trials. Spine. 2011;36:E May S, Comer C. Is surgery more effective than non-surgical treatment for spinal stenosis, and which non-surgical treatment is more effective? A systematic review. Physiotherapy. 2013;99: Weinstein JN, Tosteson TD, Lurie JD et.al. Surgical versus non-surgical therapy for lumbar spinal stenosis. N Eng J Med. 2008;358: Machado GC, Ferreira PH, Harris IA et al. Effectiveness of surgery for lumbar spinal stenosis: A systematic review and meta-analysis. PLos ONE. 2015;10: Lad SP, Huang KT, Bagley JH et. al. Disparities in the outcomes of lumbar spinal stenosis surgery based on insurance status. Spine. 2013;38: Shivanand PL, Babu R, Ugiliweneza B et.al. Surgery for spinal stenosis: long term reoperation rates, health care cost and impact of instrumentation. Spine. 2014; 39: Deyo RA, Martin BJ, Ching A et.al. Interspinous spacers compared to decompression or fusion for lumbar stenosis: complications and repeat operations in the Medicare population. Spine. 2013; 38: Deyo RA, Mirza SK, Martin BI et. al. Trends, major medical complications and charges associated with surgery for lumbar spinal stenosis in older adults. JAMA. 2010;303: Katz JN, Lipson SJ, Lew RA et.al. Lumbar laminectomy alone or with instrumented or noninstrumented arthrodesis in degenerative lumbar spinal stenosis. Patient selection, costs, surgical outcomes. Spine. 1997;22: Bae HW, Lauryssen C, Maislin G et. al. Therapeutic sustainability and durability of Coflex interlaminar stabilization after decompression for lumbar spinal stenosis: a four year assessment. Int J Spine Surg May 11;9: Martin BI, Tosteson AN, Lurie JD et.al. Variation in the care of surgical conditions: spinal stenosis, A Dartmouth Atlas of Health Care Series. The Dartmouth Institute for Health Policy and Clinical Practice Accessed at: 12 Pannell WC, Savin DD, Scott TP et. al. Trends in the surgical treatment of lumbar spine disease in the United States. The Spine Journal. 2015;15: Kalichman L, Cole R, Kim DH et.al. Spinal stenosis prevalence and association with symptoms: The Framingham Study. Spine.2009;9: Deyo RA, Gray DT, Kreuter W. et. al. United States trends in lumbar fusion surgery for degenerative conditions. Spine. 2005;30: October
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
Neck and Back Pain in VA Incidence and Prevalence in VA Users
 Neck and Back Pain in VA Incidence and Prevalence in VA Users Spotlight on Pain Management: Patsi Sinnott, PT, PhD, MPH Sharon Dally, MS, Tigran Avoundjian, MPH, Jody Trafton, PhD, Todd Wagner, PhD Dec.
Neck and Back Pain in VA Incidence and Prevalence in VA Users Spotlight on Pain Management: Patsi Sinnott, PT, PhD, MPH Sharon Dally, MS, Tigran Avoundjian, MPH, Jody Trafton, PhD, Todd Wagner, PhD Dec.
Coding and Payment Guide for Anesthesia Services. An essential coding, billing, and reimbursement resource for anesthesiology and pain management
 Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
Coding and Payment Guide for Anesthesia Services An essential coding, billing, and reimbursement resource for anesthesiology and pain management 2011 Contents Introduction...1 Coding Systems... 1 Claim
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Motion Preservation. Hansen Yuan, MD President, Spine Arthroplasty Society
 Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
Motion Preservation Procedure Codes Hansen Yuan, MD President, Spine Arthroplasty Society Who are we? The Spine Arthroplasty Society (SAS) is a group of medical and associated specialists devoted to the
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015
 Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis:
 Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Lumbar Spinal Stenosis Materclass: Surgical management of lumbar spinal stenosis: Presented By: Michelle Emsley Senior Spinal In-Patient Physiotherapist Learning objectives Indications Evidence Post operative
Cooled RF Systems. Cooled RF Systems. Reimbursement Guide
 Kimberly-Clark* Reimbursement Guide Kimberly-Clark * Pain Management Cooled RF Systems Reimbursement Guide Table of Contents Introduction... 3 Disc Biacuplasty (TransDiscal* System)... 5 SInergy* System...
Kimberly-Clark* Reimbursement Guide Kimberly-Clark * Pain Management Cooled RF Systems Reimbursement Guide Table of Contents Introduction... 3 Disc Biacuplasty (TransDiscal* System)... 5 SInergy* System...
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT. Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE
 CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: [email protected] Fax: 303-703-1572
CODING SHEETS CHRONIC INTRACTABLE PAIN MANAGEMENT Effective January 1, 2011 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: [email protected] Fax: 303-703-1572
Procedure. 2 29827 $ 3,560 $ 1,476 Arthroscopy, shoulder, surgical; with rotator cuff repair 5.5% 241.1%
 Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
CPT Changes in Spine 2012
 CPT Changes in Spine 2012 Are you prepared? Presented by Barbara Cataletto, MBA, CPC Disclaimer The following presentations are not to be considered a replacement for the Current Procedural Terminology
CPT Changes in Spine 2012 Are you prepared? Presented by Barbara Cataletto, MBA, CPC Disclaimer The following presentations are not to be considered a replacement for the Current Procedural Terminology
https://www.laserspineinstitute.com/back_problems/foraminal_stenosis/e...
 Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
Questions? Call toll free 1-866-249-1627 Contact us today. We're here for you seven days a week. MRI Review Consultation Live help Call 1-866-249-1627 Chat Live Home Laser Spine Institute Laser Spine Institute's
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010
 Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
Presented by Zoran Maric, M.D. Orthopaedic Spine Surgeon May 22, 2010 1 cervical area thoracic area lumbar area sacrum coccyx Mayfield Clinic 2 3 4 5 Zoran Maric, MD Spine Surgery Procedures How to Document
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
MEDICAL POLICY No. 91591-R2 LUMBAR LAMINECTOMY Including Discectomy or Microdiscectomy, Foraminotomy, Laminotomy
 LUMBAR LAMINECTOMY Effective Date: June 4, 2015 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15 Date Of Origin: April 13, 2011 Status: Current Note: The prior authorization requirement was removed effective
LUMBAR LAMINECTOMY Effective Date: June 4, 2015 Review Dates: 4/11, 4/12, 4/13, 5/14, 5/15 Date Of Origin: April 13, 2011 Status: Current Note: The prior authorization requirement was removed effective
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Low Back Pain (LBP) Prevalence. Low Back Pain (LBP) Prevalence. Lumbar Fusion: Where is the Evidence?
 15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
CODING SHEETS CHRONIC INTRACTABLE SPASTICITY. Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE
 CODING SHEETS CHRONIC INTRACTABLE SPASTICITY Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: [email protected] Fax: 303-703-1572 CODMAN
CODING SHEETS CHRONIC INTRACTABLE SPASTICITY Effective January 1, 2009 CODMAN 3000 NEUROMODULATION AND ONCOLOGY REIMBURSEMENT HOTLINE Phone: 800-609-1108 Email: [email protected] Fax: 303-703-1572 CODMAN
How To Write An Icd10
 Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
Reimbursement Overview Supporting Adjunctive Use of the coflex-f Implant During Lumbar Fusion Procedures
 Interlaminar Technology Reimbursement Overview Supporting Adjunctive Use of the coflex-f Implant During Lumbar Fusion Procedures Coding Recommendations Overview Implant Description & Device Type Differentiation
Interlaminar Technology Reimbursement Overview Supporting Adjunctive Use of the coflex-f Implant During Lumbar Fusion Procedures Coding Recommendations Overview Implant Description & Device Type Differentiation
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
CMS Imaging Efficiency Measures Included in Hospital Outpatient Quality Data Reporting Program (HOP QDRP) 2009
 CMS Imaging Efficiency Measures Included in Hospital Outpatient Quality Data Reporting Program (HOP QDRP) 2009 OP 8: MRI LUMBAR SPINE FOR LOW BACK PAIN Measure Description: This measure estimates the percentage
CMS Imaging Efficiency Measures Included in Hospital Outpatient Quality Data Reporting Program (HOP QDRP) 2009 OP 8: MRI LUMBAR SPINE FOR LOW BACK PAIN Measure Description: This measure estimates the percentage
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
Interspinous Fixation (Fusion) Devices Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Interspinous Fixation (Fusion) Devices Lumbar Spine
Alaska Workers Compensation Fee Schedule Comparative Survey
 Alaska Workers Compensation Fee Comparative Survey As part of the Division s analysis of workers compensation medical costs in Alaska, we asked the National Council on Compensation Insurance (NCCI) to
Alaska Workers Compensation Fee Comparative Survey As part of the Division s analysis of workers compensation medical costs in Alaska, we asked the National Council on Compensation Insurance (NCCI) to
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Lumbar Spinal Stenosis
 Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Issued and entered this _6th_ day of October 2010 by Ken Ross Commissioner ORDER I PROCEDURAL BACKGROUND
 STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation In the matter of XXXXX Petitioner
Hitting a Nerve: The Triggers of Sciatica. Bruce Tranmer MD FRCS FACS
 Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Physician Coding and Payment Guide 2015
 Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
Targeted Drug Delivery Physician Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party sources and is subject
Spinal Surgery Clinical Coverage Policy No: 1A-30 Revised Date: DRAFT Table of Contents
 Clinical Coverage Policy No: 1A-30 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligible Recipients... 2 2.1 General Provisions... 2 2.2 EPSDT Special
Clinical Coverage Policy No: 1A-30 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligible Recipients... 2 2.1 General Provisions... 2 2.2 EPSDT Special
OUTLINE. Anatomy Approach to LBP Discogenic LBP. Treatment. Herniated Nucleus Pulposus Annular Tear. Non-Surgical Surgical
 DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA
 LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011
 1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
Overview Anatomy of the spinal canal What is spinal stenosis? > 1
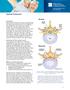 Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
Major Depressive Disorder:
 Major Depressive Disorder: An Actuarial Commercial Claim Data Analysis July 2013 Prepared by: Milliman, Inc. NY Kate Fitch RN, MEd Kosuke Iwasaki FIAJ, MAAA, MBA This report was commissioned by Takeda
Major Depressive Disorder: An Actuarial Commercial Claim Data Analysis July 2013 Prepared by: Milliman, Inc. NY Kate Fitch RN, MEd Kosuke Iwasaki FIAJ, MAAA, MBA This report was commissioned by Takeda
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705)
 Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD
Local Coverage Determination (LCD): Spinal Cord Stimulation (Dorsal Column Stimulation) (L34705) Contractor Information Contractor Name Novitas Solutions, Inc. LCD Information Document Information LCD
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary?
 White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
Ambulatory Surgery Center Coding and Payment Guide 2015
 Targeted Drug Delivery Ambulatory Surgery Center Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party
Targeted Drug Delivery Ambulatory Surgery Center Coding and Payment Guide 2015 Flowonix Medical has compiled this coding information for your convenience. This information is gathered from third party
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Workers Compensation Medical Costs in NH Significantly Higher
 EMBARGOED: FOR RELEASE THURSDAY, MAY 22, 10 AM NOT FOR RELEASE UNTIL: May 22, 2014 Contact: Danielle Barrick, director of communications, (603) 271-7973, ext. 336, [email protected]; Deb Stone,
EMBARGOED: FOR RELEASE THURSDAY, MAY 22, 10 AM NOT FOR RELEASE UNTIL: May 22, 2014 Contact: Danielle Barrick, director of communications, (603) 271-7973, ext. 336, [email protected]; Deb Stone,
Patients with pain in the neck, arm, low back, or leg (sciatica) may benefit from ESI. Specifically, those with the following conditions:
 Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
COOLIEF* Cooled Radiofrequency Systems COOLIEF* COOLED RADIOFREQUENCY REIMBURSEMENT GUIDE
 COOLIEF* COOLED RADIOFREQUENCY REIMBURSEMENT GUIDE HALYARD* Pain Management Cooled RF Systems Reimbursement Guide Table of Contents Introduction... 3 COOLIEF* TRANSDICAL* Disc Biacuplasty Cooled Radiofrequency...
COOLIEF* COOLED RADIOFREQUENCY REIMBURSEMENT GUIDE HALYARD* Pain Management Cooled RF Systems Reimbursement Guide Table of Contents Introduction... 3 COOLIEF* TRANSDICAL* Disc Biacuplasty Cooled Radiofrequency...
Report therapeutic hip injection under fluoro with 20610 and 77002
 Report therapeutic hip injection under fluoro with 20610 and 77002 Use the following Q & A to determine how to bill imaging when you provide a hip injection. Question: How do you report an injection of
Report therapeutic hip injection under fluoro with 20610 and 77002 Use the following Q & A to determine how to bill imaging when you provide a hip injection. Question: How do you report an injection of
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Medicare Diagnosis By Dr. Ron Short, DC, MCS-P
 Medicare Diagnosis By Dr. Ron Short, DC, MCS-P Diagnosis o The diagnosis is one of two codes that you place on the CMS 1500 form when you submit a claim. o The diagnosis communicates the patient s condition
Medicare Diagnosis By Dr. Ron Short, DC, MCS-P Diagnosis o The diagnosis is one of two codes that you place on the CMS 1500 form when you submit a claim. o The diagnosis communicates the patient s condition
How to Overcome the 5 Biggest Reimbursement Challenges in Joint & Spine Coding
 How to Overcome the 5 Biggest Reimbursement Challenges in Joint & Spine Coding Presented by: Carolyn Neumann, CPC Senior Manager Coding and Coverage Access The opinions and codes denoted within are suggestions
How to Overcome the 5 Biggest Reimbursement Challenges in Joint & Spine Coding Presented by: Carolyn Neumann, CPC Senior Manager Coding and Coverage Access The opinions and codes denoted within are suggestions
Workers Compensation Insurance
 Workers Compensation Insurance New Hampshire Insurance Department Detailed Medical Cost Comparison The following exhibits compare the cost of Workers Compensation Medical services in New Hampshire to our
Workers Compensation Insurance New Hampshire Insurance Department Detailed Medical Cost Comparison The following exhibits compare the cost of Workers Compensation Medical services in New Hampshire to our
IP'Lumbar Spinal Stenosis
 A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
A Patient's G uide to IP'Lumbar Spinal Stenosis X*STOP Interspinous Process Decompression This patient information guide is made possible through cooperation between your physician and St. Francis Medical
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes.
 Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 07/24/2013 Comments: Policy Accepted during 2013 Annual Review with no changes. Title: Minimally Invasive,
Image-Guided Minimally Invasive Lumbar Decompression for Spinal Stenosis
 Image-Guided Minimally Invasive Lumbar Decompression for Spinal Stenosis Policy Number: 7.01.126 Last Review: 6/2015 Origination: 5/2010 Next Review: 6/2016 Policy Blue Cross and Blue Shield of Kansas
Image-Guided Minimally Invasive Lumbar Decompression for Spinal Stenosis Policy Number: 7.01.126 Last Review: 6/2015 Origination: 5/2010 Next Review: 6/2016 Policy Blue Cross and Blue Shield of Kansas
Aetna Injection Policy For Back Pain
 Aetna Injection Policy For Back Pain Number: 0016 Policy Aetna considers any of the following injections or procedures medically necessary for the treatment of back pain; provided, however, that only 1
Aetna Injection Policy For Back Pain Number: 0016 Policy Aetna considers any of the following injections or procedures medically necessary for the treatment of back pain; provided, however, that only 1
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
Surgical Treatment for Lumbar Spinal Stenosis Dynamic Interspinous Distraction Interlaminar Stabilization Implant - Coflex
 International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
International 31st Course For Percutaneous Endoscopic Spinal Surgery And Complementary Minimal Invasive Techniques Zurich, Switzerland January 24-25, 2013 Surgical Treatment for Lumbar Spinal Stenosis
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Cervical Stenosis & Myelopathy
 Cervical Stenosis & Myelopathy North American Spine Society Public Education Series What Are Cervical Stenosis and Myelopathy? The cervical spine (neck) is made up of a series of connected bones called
Cervical Stenosis & Myelopathy North American Spine Society Public Education Series What Are Cervical Stenosis and Myelopathy? The cervical spine (neck) is made up of a series of connected bones called
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Surgical Procedures of the Spine
 Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Degenerative Spine Solutions
 Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Imaged-Guided Minimally Invasive Lumbar Page 1 of 9 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Image-Guided Minimally Invasive Lumbar Professional Institutional
Imaged-Guided Minimally Invasive Lumbar Page 1 of 9 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Image-Guided Minimally Invasive Lumbar Professional Institutional
DUKE ORTHOPAEDIC SURGERY GOALS AND OBJECTIVES SPINE SERVICE
 GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University
 Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
MDC 1 DISEASES AND DISORDERS OF THE NERVOUS SYSTEM Implantation of chemotherapeutic agent Intracranial stents
 To assist the readers in identifying all changes that were made to the MS-DRGs as a result of comments, we developed the attached table that summaries those changes. MS-DRG Summary Table PRE-MDC Intestinal
To assist the readers in identifying all changes that were made to the MS-DRGs as a result of comments, we developed the attached table that summaries those changes. MS-DRG Summary Table PRE-MDC Intestinal
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Complications in Adult Deformity Surgery
 Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lower Back Pain. Introduction. Anatomy
 Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
The Surgical Spine. Sergio Rivero M.D.
 The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
Spine Surgery Coding: Don t Break Your Neck Trying to Figure It Out
 Spine Surgery Coding: Don t Break Your Neck Trying to Figure It Out Presented to: AAPC Annual Meeting Orlando, Florida April 15, 2013 Presented by: Kim Pollock, RN, MBA, CPC www.karenzupko.com Kim Pollock,
Spine Surgery Coding: Don t Break Your Neck Trying to Figure It Out Presented to: AAPC Annual Meeting Orlando, Florida April 15, 2013 Presented by: Kim Pollock, RN, MBA, CPC www.karenzupko.com Kim Pollock,
