sealant without sutures (occasionally sutures may be required). This can be performed via a mini-arthrotomy, a less invasive approach.
|
|
|
- Bryce Phillips
- 8 years ago
- Views:
Transcription
1 Rehabilitation guidelines for patients undergoing surgery for autologous chondrocyte implantation (ACI), matrix induced autologous chondrocyte implantation (MACI) and autologous matrix induced chondrogenesis (AMIC) of the knee At the RNOH our emphasis is on patient specific rehabilitation, which encourages recognition of those who may progress slower than others. We also want to encourage clinical reasoning. Milestone driven These are milestone driven guidelines designed to provide an equitable rehabilitation service to all our patients. They will also limit unnecessary visits to the outpatient clinic at RNOH by helping the patient and therapist to identify when a specialist review is required. Indications for surgery: Chondral and osteochondral defects of the knee Osteochondritis dissecans (spontaneous loss of a fragment of cartilage or bone and cartilage without trauma) Possible complications: Infection Bleeding Nerve damage Deep vein thrombosis Pulmonary embolism Persistent/recurrent pain Recurrent symptoms including locking, swelling, instability Failure of implant Persistent/recurrent joint crepitus Altered sensation in the knee post-operatively Surgical techniques: ACI technique: For this technique cells are harvested following arthroscopy and cultured. A periosteal flap is used or bilayer collagen membrane is sutured over the prepared cartilage defect, and the cell suspension is injected underneath. MACI technique: For this technique cells are harvested and cultured following arthroscopy using a collagen membrane matrix seeded with the cultured autologous chondrocytes. This cell-scaffold only requires fixing with a fibrin 1
2 sealant without sutures (occasionally sutures may be required). This can be performed via a mini-arthrotomy, a less invasive approach. AMIC technique: This technique is similar to microfracture but it involves using a collagen membrane to stabilise the microfracture clot, providing a more stable environment for new cartilage tissue formation. The membrane is attached with fibrin glue or sutures via an arthrotomy. Expected outcome: Improved function/mobility Reduced pain Full recovery may take up to twelve months Decreased joint clicking/ locking/ swelling/instability Pre-operatively Where possible the patient will be seen pre-operatively, and with consent, the following assessed: Current functional levels General health Social/work/hobbies Functional range of movement Balance/proprioception Gait/mobility, including walking aids, orthoses Post-operative expectations Patient information leaflet issued Post-operative management explained All ACTIVE trial patients will have completed a pre-operative assessment by the independent assessor. Post-operatively Always check the operation notes, and the post-operative instructions. Discuss any deviation from routine guidelines with the team concerned. Initial rehabilitation phase: in-patient stay (usually 0-3 days) Goals: To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise programme as appropriate 2
3 To understand self management/monitoring Restrictions: *Keep all patients in extension for 1 st week post-op* Patella / Trochlea grafts: o No range of movement exercises until 1 week post-op o Mobilise fully weight-bearing (FWB) with elbow crutches o Hinged knee brace locked in extension when weight-bearing for 4 weeks (can be unlocked for exercises to 45 degrees after 1 week) Femoral condyle grafts: o No range of movement exercises until 1 week post-op o Mobilise touch weight-bearing for 4 weeks, then partial weightbearing for a further 2 weeks o Knee brace locked in extension when weight-bearing for 1 week If sedentary employment, may be able to return to work from 2-4 weeks post-operatively, as long as provisions are made to elevate leg, and no complications Treatment: Pain-relief: ensure adequate analgesia Elevation: ensure elevating the leg with foot higher than waist Exercises: o Patella / Trochlea Teach static quads/gluts, co-contraction of quads/hamstrings o Femoral condyle Teach static quads/gluts, co-contraction of quads/hamstrings Education: teach how to monitor sensation, colour, circulation, temperature, swelling, and advise what to do if concerned. Teach protection, rest, icing, compression and elevation (PRICE) Mobility: ensure patient is independent with transfers and mobility, including stairs if necessary On discharge from the ward: Independent and safe mobilising, including stairs if appropriate Independent and safe with home exercise programme 3
4 Initial rehabilitation phase: 1-6 weeks Goals: All exercises should be pain free Achieving range of movement within restrictions Restrictions: Patella/trochlea grafts: o Commence range of movement exercises 0-45 until week 4 o Mobilise fully weight-bearing with elbow crutches o Hinged knee brace locked in extension when weight-bearing for 4 weeks (can be unlocked for exercises to 45 degrees) Femoral condyle grafts: o Commence/progress range of movement as symptoms allow aiming for full range at 6 weeks o Mobilise touch weight-bearing for 4 weeks post-op, then partial weight-bearing for a further 2 weeks o Can then be weaned from brace at this stage as control allows Treatment: Advice/education: comprehensive education and instruction on restrictions and on carrying out activities of daily living (to avoid activities that can provoke excessive shear forces or impact) Posture advice/education Swelling management Gait re-education Stretches of tight structures as appropriate Mobility: ensure safely and independently mobile with/without walking aid Exercises: o Patella/trochlea grafts: Teach closed chain AROM/AAROM knee flexion and extension in lying/sitting, closed chain quads within 0-45 degrees range, static quads, co-contraction of quads/hamstrings o Femoral condyle grafts: 4
5 Teach closed chain AROM/AAROM knee flexion and extension in lying/sitting, open chain quads if pain allows, closed chain quads from 4 weeks (within range and within weight bearing restrictions), static quads, co-contraction of quads/hamstrings Low resistance isometric exercises Active exercises against gravity progressing to low resistance Patella mobilisations as appropriate Stationary cycling can be introduced from week 4 as long as resistance is minimal and there is sufficient ROM to complete a revolution without pain Manual therapy: o Soft tissue techniques as appropriate Hydrotherapy if appropriate Pacing advice as appropriate Milestones to progress to next phase: Achieving stated range of movement Pain free exercises Recovery rehabilitation phase: 6 weeks 12 weeks Goals: Optimise normal movement Improve strength and balance/proprioception Restrictions: Femoral condyle grafts: o Partial weight-bearing week 4-6 and FWB from week 6 The repair site is most vulnerable during the first 3 months after ACI/ MACI Avoid impact (i.e jogging, aerobics) as well as excessive loading and shearing forces All exercises should be pain free Treatment: Advice/education: Comprehensive education and instruction on restrictions and on carrying out activities of daily living (to avoid activities that can provoke excessive shear forces or impact) 5
6 Posture advice/education Swelling management Mobility: Ensure safely and independently mobile with/without walking aid Exercises o Controlled active range of movement (AROM) of the knee o Strengthening of muscles stabilising the knee including introduction of resistance and/or COG shift e.g resistance work with therabands/weights and duration. Progressive quadriceps, especially closed chain (depending on weight bearing status and comfort for femoral condyles) o Strengthening exercises of other muscle groups as appropriate. o Core stability work o Exercises to teach patient to find and maintain neutral extension in standing, avoiding hyper extension, with good control o Balance/proprioception work once appropriate, including double leg to single leg stand +/- eyes open/closed o Stretches of tight structures as appropriate, ensuring normal flexibility of quadriceps, hamstrings and calf muscles o Review lower limb biomechanics and kinetic chain. Address issues as appropriate o Biofeedback may be used if altered sequencing of muscles o Ensure mobility of patello-femoral joint o Incorporate functional dynamic test with the patient whilst working on proprioceptive control e.g descending stairs, gait and sit to stand Manual therapy: o Soft tissue techniques as appropriate o Joint mobilisations as appropriate Hydrotherapy if appropriate Pacing advice as appropriate Milestones to progress to next phase: Pain free exercises Mobilising independently Able to dynamically stabilise knee during single leg stand/squat (may take slightly longer with femoral condyles due to restricted weight bearing during first 6 weeks) 6
7 Intermediate rehabilitation phase: 12 weeks 6 months Goals: Optimise normal movement/control Grade IV-V muscle strength in operated leg Pain free exercises Treatment: Pain relief Advice/education Posture advice/education Mobility: progression of mobility and function Gait re-education Exercises: o Range of movement o Strengthening through range o Core stability work o Stretches of tight structures as appropriate o Review lower limb biomechanics and kinetic chain. Address issues as appropriate o Introduction of sports specific and occupation specific rehabilitation Balance/proprioception o Introduction of unstable base including use of uni/multidirectional wobble boards, trampet, gym ball and Dyna-cushion (progress with distractions including throwing, catching, reaching, turning) o Tie in core stability work o Progress from static to dynamic exercises as appropriate Introduce gym work including unrestricted static cycling, rowing, stepper Manual Therapy: o Soft tissue techniques as appropriate o Joint mobilisations as appropriate Hydrotherapy is appropriate Pacing advice as appropriate Milestones to progress to next phase: Able to dynamically stabilise the knee and be independently functional in everyday activities Failure to meet milestones: Refer back to team/discuss with team 7
8 Continue with outpatient physiotherapy if still progressing and appropriate goals Final rehabilitation phase: 6 months 1 year Goals: To be fit to return to high impact sports at 1 year if set as patient goal Hopping/changes of direction with good control Optimum balance/proprioception Establish long term maintenance programme Restrictions: From Month 9 may commence sport specific training and return to contact sport from 1 year post-op Treatment: Mobility/function: Progression of mobility and function, increasing dynamic control with sport specific training to functional goals Exercise: o Sports specific/functional exercises o Address any issues raised from patient return to activity o Functional dynamic work including running hopping and jumping (if sufficient dynamic stability) Return to low-impact activity/sports including light jogging on running machine, unlimited swimming Pacing advice Milestones for discharge: Good proprioceptive control dynamically Return to normal functional level Return to sports if set as patient goal 8
9 Failure to progress If a patient is failing to progress, then consider the following: Possible problem Action Swelling Ensure elevating leg regularly Use ice as appropriate if normal skin sensation and no contraindications Decrease amount of time on feet Pacing Use walking aids Circulatory exercises If decreases overnight, monitor closely If does not decrease over a few days, refer back to surgical team Pain Research has shown that the cartilage is continuing to heal for up to 3 years and this may account for slower progressing patients Decrease activity Ensure adequate analgesia Elevate regularly Decrease weight bearing and use walking aids as appropriate Pacing Modify exercise programme as appropriate. Should continue isometric work at all times If persists, refer back to surgical team Breakdown of wound e.g. Refer to surgical team inflammation, bleeding, infection Recurrent instability Refer back to surgical team Ensure exercises not too advanced for patient Address core stability Numbness/altered sensation Review immediate post-operative status if possible Ensure swelling under control If new onset or increasing refer back to surgical team If static, monitor closely, but inform surgical team and refer back if deteriorates or if concerned 9
10 Summary of evidence for physiotherapy guidelines A comprehensive literature search was carried out to identify research relating to rehabilitation following autologous chondrocyte Implantation of the knee and the ACTIVE trial. After reviewing the articles and information, the physiotherapy guidelines were produced on the best available evidence. ACTIVE trial protocol. Autologous chondrocyte transplantation/implantation versus existing treatments. (April 2008, Version 3.6.) Bailey A, Goodstone N, Roberts S et al (2003). Rehabilitation after oswestry autologous chondrocyte implantation: the OsCell protocol. Journal of sports rehabilitation. (12, ) Clare C et al (2005) Clinical and cost-effectiveness of autologous chondrocyte implantation for cartilage defects in knee joints: systematic review and economic evaluation. Health technology assessment (HTA) database, 98. Hambly K, Bobic V, Wondrasch B, Van Assche D, Marlovitis S (2006). Autologous chondrocyte implantation, postoperative care and rehabilitation. The american journal of sports medicine. (34, ) Knutsen G et al (2007), A randomized trial comparing autologous chondrocyte implantation with microfracture. The journal of bone and joint surgery. (89, ) Kreuz PC et al (2007), Importance of sports in cartilage regeneration after autologous chondrocyte implantation. The american journal of sports medicine. (35, ) Riegger-Krugh C et al (2008), Autologous chondrocyte implantation: current surgery and rehabilitation. Medicine and science in sports and exercise. (40 (2), ) The use of autologous chondrocyte implantation for the treatment of cartilage defects in knee joints, (2005). National institute for health and clinical excellence. Review of technology appraisal
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Milestone Driven. Team Contact Details
 REHABILITATION GUIDELINES FOR PATIENTS UNDERGOING A UNICONDYLAR KNEE REPLACEMENT (UKR) PATELLOFEMORAL JOINT REPLACEMENT (PFJR) OR TOTAL KNEE REPLACEMENT (TKR) At The RNOH our emphasis is on patient specific
REHABILITATION GUIDELINES FOR PATIENTS UNDERGOING A UNICONDYLAR KNEE REPLACEMENT (UKR) PATELLOFEMORAL JOINT REPLACEMENT (PFJR) OR TOTAL KNEE REPLACEMENT (TKR) At The RNOH our emphasis is on patient specific
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
Rehabilitation Guidelines for Autologous Chondrocyte Implantation. Ashley Conlin, PT, DPT, SCS, CSCS
 Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
ChondroCelect Rehabilitation Program
 ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI MR GREG CRIAG MR IAN COLLIER DECEMBER, 2004 INTRODUCTION Anterior cruciate ligament reconstruction
AN ACCELERATED REHABILITATION PROGRAMME FOR ENDOSCOPIC ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI MR GREG CRIAG MR IAN COLLIER DECEMBER, 2004 INTRODUCTION Anterior cruciate ligament reconstruction
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle
 A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
Post Surgery Rehabilitation Program for Knee Arthroscopy
 Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
ACL Non-Operative Protocol
 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
Hip Arthroscopy Post-operative Rehabilitation Protocol
 Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
Steps to Success: A Guide to Knee Rehabilitation
 Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction
 Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Cincinnati Sportsmedicine and Orthopaedic Center
 Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities
 Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees
 Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Ankle Stabilisation Procedure
 Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY
 PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
After Hip Arthroscopy
 After Hip Arthroscopy On your road to recovery... Rehabilitation is essential to help you return to an active life and reach your personal goals. This booklet provides goals, activities and milestones
After Hip Arthroscopy On your road to recovery... Rehabilitation is essential to help you return to an active life and reach your personal goals. This booklet provides goals, activities and milestones
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair
 Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
Rehabilitation Guidelines for Post-Operative Shoulder Instability Repair Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon
 Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon Knee Arthroscopy Physical Therapy Protocol This rehabilitation
Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon Knee Arthroscopy Physical Therapy Protocol This rehabilitation
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY
 B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
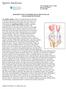 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL
 REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL Michael M. Reinold, PT, ATC Kevin E. Wilk, PT Jeffrey R. Dugas, MD E. Lyle Cain, MD Scott D. Gillogly, MD The following has
REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL Michael M. Reinold, PT, ATC Kevin E. Wilk, PT Jeffrey R. Dugas, MD E. Lyle Cain, MD Scott D. Gillogly, MD The following has
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Post Surgery Rehabilitation Program
 Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Rehabilitation Programme following Hip Arthroscopy
 Rehabilitation Programme following Hip Arthroscopy Updated May 2010 Hip Arthroscopy Patient information and rehabilitation programme: The Hip Joint The hip is a ball-and-socket joint and is the largest
Rehabilitation Programme following Hip Arthroscopy Updated May 2010 Hip Arthroscopy Patient information and rehabilitation programme: The Hip Joint The hip is a ball-and-socket joint and is the largest
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
28. APPENDIX G: REHABILITATION PROCEDURE. Rehabilitation procedure
 Frobell BR, Lohmander LS, Roos HP, Roos EM: Surgical vs. Non- Surgical Treatment of ACL-injuries A Randomized study. Draft date 2001-08-31, version 10 Page: 52 28. APPENDIX G: REHABILITATION PROCEDURE
Frobell BR, Lohmander LS, Roos HP, Roos EM: Surgical vs. Non- Surgical Treatment of ACL-injuries A Randomized study. Draft date 2001-08-31, version 10 Page: 52 28. APPENDIX G: REHABILITATION PROCEDURE
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1
 Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Frequently Asked Questions following Anterior Cruciate Ligament Reconstruction Surgery 1 Will my knee be normal after surgery and recovery? Unfortunately, even with an ACL reconstructive procedure, it
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Baker Rehab Group HomeCare Rehab and Nursing LLC
 Baker Rehab Group HomeCare Rehab and Nursing LLC Introduction So it s time for a joint replacement... Are you worried about the surgery? Are you wondering about the pre and post surgical process? Do you
Baker Rehab Group HomeCare Rehab and Nursing LLC Introduction So it s time for a joint replacement... Are you worried about the surgery? Are you wondering about the pre and post surgical process? Do you
Rehabilitation Guidelines for Post-Operative Stiff Shoulder
 Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Rehabilitation Guidelines for Post-Operative Stiff Shoulder Please note that this is advisory information only. Your experiences may differ from those described. A fully qualified Physiotherapist must
Physiotherapy in Rheumatoid Arthritis. Information for patients Gina Wall Senior Physiotherapist
 Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Meniscus Repair Rehabilitation Dr. Walter R. Lowe
 Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Copeland Surface Replacement Arthroplasty (Hannan Mullett)
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Cartilage Repair Center
 Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol Phase I: Healing Phase (0-2 Weeks) Goal: Protect Incision, Reduce Inflammation, Allow Tissues to Heal, and Rest Wound Care: Keep Incision covered with sealed dressing
Hip Arthroscopy Rehabilitation Protocol Phase I: Healing Phase (0-2 Weeks) Goal: Protect Incision, Reduce Inflammation, Allow Tissues to Heal, and Rest Wound Care: Keep Incision covered with sealed dressing
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
www.noc.nhs.uk ACL Reconstruction Information for Patients Delivering Excellence Hip and Knee service
 www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
Ankle Arthroscopy and Follow-Up Physiotherapy
 Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
A patient s s guide to: Arthroscopy of the Hip
 A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
ChondroCelect Rehabilitation Guide for patellar and trochlear articular cartilage repair
 Chester Knee Clinic & Cartilage Repair Centre @ Nuffield Health, The Grosvenor Hospital Chester Consultant Orthopaedic Knee Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre @ Nuffield Health, The Grosvenor Hospital Chester Consultant Orthopaedic Knee Surgeon: Vladimir Bobic, MD, FRCSEd www.kneeclinic.info office@kneeclinic.info
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
Patella Realignment Tibial Tuberosity Transfer with Lateral Release
 Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
Rehabilitation After ACL Reconstruction
 CENTRE PERTH ORTHOPAEDIC & SPORTS MEDICINE Rehabilitation After ACL Reconstruction Dr Keith Holt Philosophy of Rehabilitation Rehabilitation, as it applies to the recovery period from Orthopaedic Surgery,
CENTRE PERTH ORTHOPAEDIC & SPORTS MEDICINE Rehabilitation After ACL Reconstruction Dr Keith Holt Philosophy of Rehabilitation Rehabilitation, as it applies to the recovery period from Orthopaedic Surgery,
ACL Rehabilitation Pathway. Expediating Safe Return to Optimum Performance. www.sportssurgeryclinic.com
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries ACL Rehabilitation Pathway Expediating Safe Return to Optimum Performance www.sportssurgeryclinic.com Contents Introduction...
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries ACL Rehabilitation Pathway Expediating Safe Return to Optimum Performance www.sportssurgeryclinic.com Contents Introduction...
RNOH Physiotherapy Department Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department Rehabilitation guidelines for patients undergoing spinal surgery Please note that this is advisory information only. Your experiences may differ from those described. All
RNOH Physiotherapy Department Rehabilitation guidelines for patients undergoing spinal surgery Please note that this is advisory information only. Your experiences may differ from those described. All
ANKLE STRENGTHENING INTRODUCTION EXERCISES SAFETY
 ANKLE STRENGTHENING INTRODUCTION Welcome to your Ankle Strengthening exercise program. The exercises in the program are designed to improve your ankle strength, fitness, balance and dynamic control. The
ANKLE STRENGTHENING INTRODUCTION Welcome to your Ankle Strengthening exercise program. The exercises in the program are designed to improve your ankle strength, fitness, balance and dynamic control. The
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes
 Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
When is Hip Arthroscopy recommended?
 HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
