Major Depressive Disorder (MDD) Guideline Diagnostic Nomenclature for Clinical Depressive Conditions
|
|
|
- Phebe Stevenson
- 10 years ago
- Views:
Transcription
1 Major Depressive Disorder Major Depressive Disorder (MDD) Guideline Diagnostic omenclature for Clinical Depressive Conditions Conditions Diagnostic Criteria Duration Major Depression 5 of the following symptoms (must include either depressed mood or anhedonia): Depressed mood Loss of interest in most activities (anhedonia) Significant change in weight or appetite Insomnia or hypersomnia Decreased concentration Decreased energy Inappropriate guilt or feelings of worthlessness Psychomotor agitation or retardation Suicidal ideation 2 weeks Dysthymia Depression OS (ot Otherwise Specified) 3 or 4 of the symptoms listed above with the addition of feelings of hopelessness and the omission of suicidal ideation (must include depressed mood) Variables: all included disorders must cause clinically significant impairment in daily functioning but fail to meet classification for MDD or dysthymia (e.g., minor depression with 2 to 4 depressive symptoms) 2 years 2 weeks Reference: VA/DoD Clinical Practice Guideline for Management of Major Depressive Disorder (MDD), May 09 DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 ovember 2009
2 MDD Guideline Algorithm Page 1 Primary Care - Initial Assessment and Diagnosis 1 Patient age > 18 with suspected depression presenting to primary care? [A] Screening for MDD Brief assessment of initial presentation to assess for dangerousness [B] Unstable urgent condition? [C] Obtain relevant history, physical examination and lab tests [E] Obtain symptom score using PHQ-9 Determine and document DSM IV criteria for MDD [E] 4 Provide appropriate care or refer to stabilize and follow legal mandates [D] Over the past two weeks, how often have you been bothered by any of the following problems? 1. Little interest or pleasure in doing things 2. Feeling down, depressed, or hopeless. [A] Sidebar 1: Assessment - Medical history - Physical examination - Mental Status Exam - Relevant lab tests - Drug inventory (including over the counter and herbals) - Psychosocial history 7 Do medication(s) or 8 comorbid medical condition(s) contribute to symptoms? [F] Provide medical treatment and follow-up as indicated 9 Did depression symptoms resolve? 10 Continue medical follow-up as indicated DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 December 2003
3 MDD Guideline Algorithm Page 1 (Continued) Primary Care - Initial Assessment and Diagnosis Presumptive diagnosis of MDD? History of MDD? Are there symptoms of depression or functional impairment that do not meet DSM IV criteria for MDD? [H] Are there concerns aboiut funtional ability or patient s mental health? Provide psychoeducation for self management [I] 23 Repeat screening 22 Follow up within 20 annually 4-6 weeks 13 Follow-up and consider referral to mental health specialty Assess for manic or hypomanic symptoms or family history of bipollar disorder or other psychiatric comorbidities [G] Suspected bipolar disorder? Occurrence of other major mental illnesses Continue on Page 2 Initial Treatment 15 Consider management of Bipolar Disorder 17 Referral/consult to specialty care DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 ovember 2009
4 MDD Guideline Algorithm Page 2 Primary Care - Initial Treatment Patient with presumptive diagnosis or history of MDD, meets DSM-IV diagnostic criteria for MDD? Determine level of severity of MDD symptoms and functional impairment [J] Discuss treatment options and patient s preferences. Arrive at shared decision regarding treatment goals and plan [K] Sidebar 2: DSM-IV Diagnostic Criteria for MDD MDD diagnosis requires the presence of symptom 1, 2, or both; and at least 5 of 9 symptoms that persist for at least 2 weeks: 1. Depressed mood nearly every day for most of the day, based on self-report or observation of others 2. Marked reduction or loss of interest or pleasure in all or nearly all, activities for most of the day, nearly every day. 3. Significant non-dieting weight loss or weight gain (>5% change in body weight) 4. Insomnia or hypersomnia nearly every day 5. Psychomotor agitation or retardation (should be observable by others) 6. Fatigue/loss of energy nearly every day 7. Feelings of worthlessness or excessive/inappropriate guilt nearly every day 8. Diminished cognitive function (reduced ability to think or concentrate) nearly every day 9. Recurrent thoughts of death and/or suicide, suicide planning, or a suicide attempt DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 ovember 2009
5 MDD Guideline Algorithm Page 2 (Continued) Primary Care - Initial Treatment 27 Is there indication for referral 28 to mental health specialty? [L] Initiate treatment strategies effective for depression [See sidebar 4] [M] Address psychosocial needs [] Refer to Mental Health Specialty Care SEVERIT Mild Sidebar 3: Indications for Referral to Mental Health - Unclear diagnosis - Evidence of psychotic features, past-mania or hypomania - Signs of comorbid psychiatric conditions - Unable to treat patient in primary care - eed for psychosocial interventions - Patient preference Sidebar 4: Initial Treatment Strategies for MDD PHQ-9 SCORE FUCTIOAL IMPAIRMET Mild IITIAL STRATEG Monotherapy-antidepressants or psychotherapy or, possibly combination 31 Schedule follow-up in 4-6 weeks Moderate Moderate Antidepressants or psychotherapy or, combination Continue on Page 3 Treatment Management and Follow-up Severe 20 Severe May start with antidepressants or psychotherapy but should prefer combination or multiple antidepressants Psychoeducation and self-management should be provided for all severity levels DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 ovember 2009
6 Major Depressive Disorder MDD Guideline Algorithm Page 3 Primary Care - Treatment Management and Follow-up Patient with a diagnosis of MDD on treatment Complete assessment (see sidebar 5) Review current medication Assess for dangerousness [O] Unstable or dangerous condition? [C] Is patient condition improving and current treatment strategy tolerable? [P] Provide appropriate care or refer to stabilize and follow legal mandates [D] 37 Continue current treatment strategy. Reassess by 4-6 weeks [Q] Full remission? [R] Sidebar 5: Assessment of Treatment Response - Symptoms severity (PHQ9) and risk for suicide - Tolerability to treatment (Adverse effects) - Adherence to treatment - Medical problems influencing recovery - Psychosocial barriers to therapy - Revaluate diagnosis and appropriate treatment Sidebar 6: Treatment Strategies Monotherapy (Psych. or Drugs) Combine psych and pharmacotherapy Complex psychopharmacology Somatic interventions Inpatient/residential Sidebar 7: Indication for Consultation or Referral to Mental Health Specialty Care - Primary care out of comfort zone - Complicated depression with comorbidity - Lack of resources - Treatment resistance - Patient request DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 ovember 2009
7 MDD Guideline Algorithm Page 3 (Continued) Primary Care - Treatment Management and Follow-up 44 Adjust/modify treatment: - Consider longer duration - Consider increasing dose - Consider augmentation - Consider switching to another agent - Consider modifying treatment strategy (See sidebar 6,7) [U] Continue treatment to prevent relapse [S] Sustained remission? 45 Schedule follow-up Relapse 41 Continue maintenance therapy in Primary Care [T] 42 Sustained remission? Recurrence 43 Return to Box 32 Screen annually DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 ovember 2009
8 MDD Guideline Algorithm ICD-9 and DSM-IV Codes ICD-9 Code Diagnosis DSM-IV Code Diagnosis 296.2x Major Depressive Disorder, Single Episode 296.2x Major Depressive Disorder, Single Episode 296.3x Major Depressive Disorder, Recurrent Episode 296.3x Major Depressive Disorder, Recurrent Dysthymic Disorder Dysthymic Disorder 311 Depressive Disorder, ot elsewhere classified 311 Depressive Disorder OS ICD-9 and DSM-IV 5th Digit Subclassification Codes: x in x 0 Unspecified 1 Mild 2 Moderate 3 Severe, o Psychotic Behavior 4 Severe, with Psychotic Behavior 5 In Partial or Unspecified Remission 6 Full Remission DHCC Clinicians Helpline: 1 (866) DS: PDH-CPG Tool Kit Pocket Cards Version 1.0 ovember 2009
MOLINA HEALTHCARE OF CALIFORNIA
 MOLINA HEALTHCARE OF CALIFORNIA MAJOR DEPRESSION IN ADULTS IN PRIMARY CARE HEALTH CARE GUIDELINE (ICSI) Health Care Guideline Twelfth Edition May 2009. The guideline was reviewed and adopted by the Molina
MOLINA HEALTHCARE OF CALIFORNIA MAJOR DEPRESSION IN ADULTS IN PRIMARY CARE HEALTH CARE GUIDELINE (ICSI) Health Care Guideline Twelfth Edition May 2009. The guideline was reviewed and adopted by the Molina
DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource
 E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
Depression Assessment & Treatment
 Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
Depre r s e sio i n o i n i a dults Yousuf Al Farsi
 Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
Depression Treatment Guide
 Depression Treatment Guide DSM V Criteria for Major Depressive Disorders A. Five (or more) of the following symptoms have been present during the same 2-week period and represent a change from previous
Depression Treatment Guide DSM V Criteria for Major Depressive Disorders A. Five (or more) of the following symptoms have been present during the same 2-week period and represent a change from previous
Feeling Moody? Major Depressive. Disorder. Is it just a bad mood or is it a disorder? Mood Disorders. www.seclairer.com S Eclairer 724-468-3999
 Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller
 Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
CHAPTER 5 MENTAL, BEHAVIOR AND NEURODEVELOPMENT DISORDERS (F01-F99) March 2014. 2014 MVP Health Care, Inc.
 CHAPTER 5 MENTAL, BEHAVIOR AND NEURODEVELOPMENT DISORDERS (F01-F99) March 2014 2014 MVP Health Care, Inc. CHAPTER 5 CHAPTER SPECIFIC CATEGORY CODE BLOCKS F01-F09 Mental disorders due to known physiological
CHAPTER 5 MENTAL, BEHAVIOR AND NEURODEVELOPMENT DISORDERS (F01-F99) March 2014 2014 MVP Health Care, Inc. CHAPTER 5 CHAPTER SPECIFIC CATEGORY CODE BLOCKS F01-F09 Mental disorders due to known physiological
Depression Flow Chart
 Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression Screening in Primary Care
 Depression Screening in Primary Care Toni Johnson, MD Kristen Palcisco, BA, MSN, APRN MetroHealth System Our Vision Make Greater Cleveland a healthier place to live and a better place to do business. 2
Depression Screening in Primary Care Toni Johnson, MD Kristen Palcisco, BA, MSN, APRN MetroHealth System Our Vision Make Greater Cleveland a healthier place to live and a better place to do business. 2
Depression, Mental Health and Native American Youth
 Depression, Mental Health and Native American Youth Aisha Mays, MD UCSF Department of Family And Community Medicine Native American Health Center Oakland, CA July 8, 2015 Presenter Disclosures No relationships
Depression, Mental Health and Native American Youth Aisha Mays, MD UCSF Department of Family And Community Medicine Native American Health Center Oakland, CA July 8, 2015 Presenter Disclosures No relationships
Update on guidelines on biological treatment of depressive disorder. Dr. Henry CHEUNG Psychiatrist in private practice
 Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Dr. Anna M. Acee, EdD, ANP-BC, PMHNP-BC Long Island University, Heilbrunn School of Nursing
 Dr. Anna M. Acee, EdD, ANP-BC, PMHNP-BC Long Island University, Heilbrunn School of Nursing Overview Depression is significantly higher among elderly adults receiving home healthcare, particularly among
Dr. Anna M. Acee, EdD, ANP-BC, PMHNP-BC Long Island University, Heilbrunn School of Nursing Overview Depression is significantly higher among elderly adults receiving home healthcare, particularly among
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION
 MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
Some helpful reminders on depression in children and young people. Maria Moldavsky Consultant Child and Adolescent Psychiatrist
 Some helpful reminders on depression in children and young people Maria Moldavsky Consultant Child and Adolescent Psychiatrist The clinical picture What art and my patients taught me Albert Durer (1471-1528)
Some helpful reminders on depression in children and young people Maria Moldavsky Consultant Child and Adolescent Psychiatrist The clinical picture What art and my patients taught me Albert Durer (1471-1528)
Depression Remission at Six Months Specifications 2014 (Follow-up Visits for 07/01/2012 to 06/30/2013 Index Contact Dates)
 Description Methodology Rationale Measurement Period A measure of the percentage of adults patients who have reached remission at six months (+/- 30 days) after being identified as having an initial PHQ-9
Description Methodology Rationale Measurement Period A measure of the percentage of adults patients who have reached remission at six months (+/- 30 days) after being identified as having an initial PHQ-9
Screening Tools and Interventions for Common Behavioral Health Disorders TXPEC-0772-13
 Screening Tools and Interventions for Common Behavioral Health Disorders TXPEC-0772-13 Screening Tools and Interventions for Common Behavioral Health Disorders Depression Depression is a potentially life-threatening
Screening Tools and Interventions for Common Behavioral Health Disorders TXPEC-0772-13 Screening Tools and Interventions for Common Behavioral Health Disorders Depression Depression is a potentially life-threatening
Psychosis Psychosis-substance use Bipolar Affective Disorder Programmes EASY JCEP EPISO Prodrome
 Dr. May Lam Assistant Professor, Department of Psychiatry, The University of Hong Kong Psychosis Psychosis-substance use Bipolar Affective Disorder Programmes EASY JCEP EPISO Prodrome a mental state in
Dr. May Lam Assistant Professor, Department of Psychiatry, The University of Hong Kong Psychosis Psychosis-substance use Bipolar Affective Disorder Programmes EASY JCEP EPISO Prodrome a mental state in
Part 1: Depression Screening in Primary Care
 Part 1: Depression Screening in Primary Care Toni Johnson, MD Kristen Palcisco, BA, MSN, APRN MetroHealth System Objectives Part 1: Improve ability to screen and diagnose Depression in Primary Care Increase
Part 1: Depression Screening in Primary Care Toni Johnson, MD Kristen Palcisco, BA, MSN, APRN MetroHealth System Objectives Part 1: Improve ability to screen and diagnose Depression in Primary Care Increase
PCORE Depression Post Survey
 PCORE Depression Post Survey 1. Please enter your UNI. 467 answered question 467 skipped question 0 2. Please fill in the name of institution you are working at for your Clerkship. 467 answered question
PCORE Depression Post Survey 1. Please enter your UNI. 467 answered question 467 skipped question 0 2. Please fill in the name of institution you are working at for your Clerkship. 467 answered question
VA/DoD Clinical Practice Guideline (CPG) for Management of Major Depressive Disorder (MDD) and Clinical Support Toolkit (MDD Tool Kit)
 VA/DoD Clinical Practice Guideline (CPG) for Management of Major Depressive Disorder (MDD) and Clinical Support Toolkit (MDD Tool Kit) [Version 1] June 27, 2012 2345 Crystal DriveCrystal Park 4, Suite
VA/DoD Clinical Practice Guideline (CPG) for Management of Major Depressive Disorder (MDD) and Clinical Support Toolkit (MDD Tool Kit) [Version 1] June 27, 2012 2345 Crystal DriveCrystal Park 4, Suite
Depression: Facility Assessment Checklists
 Depression: Facility Assessment Checklists A facility system assessment is a starting point for a quality improvement project. The checklists included in this booklet will be most useful if you take a
Depression: Facility Assessment Checklists A facility system assessment is a starting point for a quality improvement project. The checklists included in this booklet will be most useful if you take a
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå. aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí=
 `çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
Managing depression after stroke. Presented by Maree Hackett
 Managing depression after stroke Presented by Maree Hackett After stroke Physical changes We can see these Depression Emotionalism Anxiety Confusion Communication problems What is depression? Category
Managing depression after stroke Presented by Maree Hackett After stroke Physical changes We can see these Depression Emotionalism Anxiety Confusion Communication problems What is depression? Category
CLINICAL PRACTICE GUIDELINES. Depression
 CLINICAL PRACTICE GUIDELINES Depression MOH Clinical Practice Guidelines 6/2011 3 1 Published by Ministry of Health, Singapore 16 College Road, College of Medicine Building Singapore 169854 Printed by
CLINICAL PRACTICE GUIDELINES Depression MOH Clinical Practice Guidelines 6/2011 3 1 Published by Ministry of Health, Singapore 16 College Road, College of Medicine Building Singapore 169854 Printed by
Bipolar disorders: Changes from DSM IV TR to DSM 5
 Bipolar disorders: Changes from DSM IV TR to DSM 5 M. Amin Esmaeili, MD, MPH Iranian Research Center for HIV/AIDS (IRCHA) Iranian National Center for Addiction Studies (INCAS) Mood disorders committee
Bipolar disorders: Changes from DSM IV TR to DSM 5 M. Amin Esmaeili, MD, MPH Iranian Research Center for HIV/AIDS (IRCHA) Iranian National Center for Addiction Studies (INCAS) Mood disorders committee
B i p o l a r D i s o r d e r
 B i p o l a r D i s o r d e r Professor Ian Jones Director National Centre for Mental Health www.ncmh.info @ncmh_wales /WalesMentalHealth 029 2074 4392 [email protected] Robert Schumann 1810-1856 Schumann's
B i p o l a r D i s o r d e r Professor Ian Jones Director National Centre for Mental Health www.ncmh.info @ncmh_wales /WalesMentalHealth 029 2074 4392 [email protected] Robert Schumann 1810-1856 Schumann's
Bipolar Disorders. Poll Question
 Bipolar Disorders American Counseling Association DSM-V Webinar Series July 10, 2013 Dr. Todd F. Lewis, Ph.D., LPC, NCC The University of North Carolina at Greensboro Poll Question Who are you? Clinical
Bipolar Disorders American Counseling Association DSM-V Webinar Series July 10, 2013 Dr. Todd F. Lewis, Ph.D., LPC, NCC The University of North Carolina at Greensboro Poll Question Who are you? Clinical
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
Addiction Billing. Kimber Debelak, CMC, CMOM, CMIS Director, Recovery Pathways
 Addiction Billing Kimber Debelak, CMC, CMOM, CMIS Director, Recovery Pathways Objectives Provide overview of addiction billing contrasting E&M vs. behavioral health codes Present system changes in ICD-9
Addiction Billing Kimber Debelak, CMC, CMOM, CMIS Director, Recovery Pathways Objectives Provide overview of addiction billing contrasting E&M vs. behavioral health codes Present system changes in ICD-9
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90
 Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
Depression in adults with a chronic physical health problem
 Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression and its Treatment in Older Adults. Gregory A. Hinrichsen, Ph.D. Geropsychologist New York City
 Depression and its Treatment in Older Adults Gregory A. Hinrichsen, Ph.D. Geropsychologist New York City What is Depression? Everyday use of the word Clinically significant depressive symptoms : more severe,
Depression and its Treatment in Older Adults Gregory A. Hinrichsen, Ph.D. Geropsychologist New York City What is Depression? Everyday use of the word Clinically significant depressive symptoms : more severe,
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Welcome New Employees. Clinical Aspects of Mental Health, Developmental Disabilities, Addictive Diseases & Co-Occurring Disorders
 Welcome New Employees Clinical Aspects of Mental Health, Developmental Disabilities, Addictive Diseases & Co-Occurring Disorders After this presentation, you will be able to: Understand the term Serious
Welcome New Employees Clinical Aspects of Mental Health, Developmental Disabilities, Addictive Diseases & Co-Occurring Disorders After this presentation, you will be able to: Understand the term Serious
Guide for family and friends of people affected by bipolar disorders. www.douglas.qc.ca
 Guide for family and friends of people affected by bipolar disorders www.douglas.qc.ca This guide is intended for families, friends and other people who are interested in understanding the different aspects
Guide for family and friends of people affected by bipolar disorders www.douglas.qc.ca This guide is intended for families, friends and other people who are interested in understanding the different aspects
Presently, there are no means of preventing bipolar disorder. However, there are ways of preventing future episodes: 1
 What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
Depression. The treatment and management of depression in adults. This is a partial update of NICE clinical guideline 23
 Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
TEEN MARIJUANA USE WORSENS DEPRESSION
 TEEN MARIJUANA USE WORSENS DEPRESSION An Analysis of Recent Data Shows Self-Medicating Could Actually Make Things Worse Millions of American teens* report experiencing weeks of hopelessness and loss of
TEEN MARIJUANA USE WORSENS DEPRESSION An Analysis of Recent Data Shows Self-Medicating Could Actually Make Things Worse Millions of American teens* report experiencing weeks of hopelessness and loss of
3/17/2014. Pediatric Bipolar Disorder
 Pediatric Bipolar Disorder 1 Highlighted Topics 1. Review the current DSM-5 definition and criteria for bipolar disorder 2. Highlight major historical developments in the scientific understanding of bipolar
Pediatric Bipolar Disorder 1 Highlighted Topics 1. Review the current DSM-5 definition and criteria for bipolar disorder 2. Highlight major historical developments in the scientific understanding of bipolar
The Clinical Presentation of Mood Disorders. Bob Boland MD
 The Clinical Presentation of Mood Disorders. Bob Boland MD 1 The Clinical Presentation of Mood Disorders 2 Concentrating On Depression Major Depression Mania Bipolar Disorder (Manic-Depression) For the
The Clinical Presentation of Mood Disorders. Bob Boland MD 1 The Clinical Presentation of Mood Disorders 2 Concentrating On Depression Major Depression Mania Bipolar Disorder (Manic-Depression) For the
Bipolar and related disorders and depressive disorders in DSM-5
 Should be cited as: Psychiatr. Pol. 2014; 48(2): 245 260 PL ISSN 0033-2674 www.psychiatriapolska.pl Bipolar and related disorders and depressive disorders in DSM-5 Dorota Łojko, Aleksandra Suwalska, Janusz
Should be cited as: Psychiatr. Pol. 2014; 48(2): 245 260 PL ISSN 0033-2674 www.psychiatriapolska.pl Bipolar and related disorders and depressive disorders in DSM-5 Dorota Łojko, Aleksandra Suwalska, Janusz
Schizoaffective disorder
 Schizoaffective disorder Dr.Varunee Mekareeya,M.D.,FRCPsychT Schizoaffective disorder is a psychiatric disorder that affects about 0.5 to 0.8 percent of the population. It is characterized by disordered
Schizoaffective disorder Dr.Varunee Mekareeya,M.D.,FRCPsychT Schizoaffective disorder is a psychiatric disorder that affects about 0.5 to 0.8 percent of the population. It is characterized by disordered
Major Depressive Disorders Questions submitted for consideration by workshop participants
 Major Depressive Disorders Questions submitted for consideration by workshop participants Prioritizing Comparative Effectiveness Research Questions: PCORI Stakeholder Workshops June 9, 2015 Patient-Centered
Major Depressive Disorders Questions submitted for consideration by workshop participants Prioritizing Comparative Effectiveness Research Questions: PCORI Stakeholder Workshops June 9, 2015 Patient-Centered
Washington State Regional Support Network (RSN)
 Access to Care Standards 11/25/03 Eligibility Requirements for Authorization of Services for Medicaid Adults & Medicaid Older Adults Please note: The following standards reflect the most restrictive authorization
Access to Care Standards 11/25/03 Eligibility Requirements for Authorization of Services for Medicaid Adults & Medicaid Older Adults Please note: The following standards reflect the most restrictive authorization
LEVEL I SA: OUTPATIENT INDIVIDUAL THERAPY - Adult
 LEVEL I SA: OUTPATIENT INDIVIDUAL THERAPY - Adult Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance-Related Disorders of the American
LEVEL I SA: OUTPATIENT INDIVIDUAL THERAPY - Adult Definition The following is based on the Adult Criteria of the Patient Placement Criteria for the Treatment of Substance-Related Disorders of the American
Adolescent Depression. Danielle Bradshaw, DO Diplomate of the American Board of Psychiatry and Neurology Adult and Child/Adolescent Psychiatry
 Adolescent Depression Danielle Bradshaw, DO Diplomate of the American Board of Psychiatry and Neurology Adult and Child/Adolescent Psychiatry Adolescence When does it start? When does it end? Characteristics:
Adolescent Depression Danielle Bradshaw, DO Diplomate of the American Board of Psychiatry and Neurology Adult and Child/Adolescent Psychiatry Adolescence When does it start? When does it end? Characteristics:
Improving the Recognition and Treatment of Bipolar Depression
 Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
Overview, Epidemiology, and the DSM-5 Criteria for Gambling Disorder
 Overview, Epidemiology, and the DSM-5 Criteria for Gambling Disorder Peter E. Nathan, Ph.D. Professor of Psychology and Public Health Emeritus University of Iowa Behavioral Health is Essential to Health
Overview, Epidemiology, and the DSM-5 Criteria for Gambling Disorder Peter E. Nathan, Ph.D. Professor of Psychology and Public Health Emeritus University of Iowa Behavioral Health is Essential to Health
ENTITLEMENT ELIGIBILITY GUIDELINE
 ENTITLEMENT ELIGIBILITY GUIDELINE BIPOLAR DISORDERS MPC 00608 ICD-9 296.0, 296.1, 296.4, 296.5, 296.6, 296.7, 296.8, 301.13 ICD-10 F30, F31, F34.0 DEFINITION BIPOLAR DISORDERS Bipolar Disorders include:
ENTITLEMENT ELIGIBILITY GUIDELINE BIPOLAR DISORDERS MPC 00608 ICD-9 296.0, 296.1, 296.4, 296.5, 296.6, 296.7, 296.8, 301.13 ICD-10 F30, F31, F34.0 DEFINITION BIPOLAR DISORDERS Bipolar Disorders include:
309.28 F43.22 Adjustment disorder with mixed anxiety and depressed mood Adjustment disorder with disturbance of conduct
 Description ICD-9-CM Code ICD-10-CM Code Adjustment reaction with adjustment disorder with depressed mood 309.0 F43.21 Adjustment disorder with depressed mood Adjustment disorder with anxiety 309.24 F43.22
Description ICD-9-CM Code ICD-10-CM Code Adjustment reaction with adjustment disorder with depressed mood 309.0 F43.21 Adjustment disorder with depressed mood Adjustment disorder with anxiety 309.24 F43.22
How to Recognize Depression and Its Related Mood and Emotional Disorders
 How to Recognize Depression and Its Related Mood and Emotional Disorders Dr. David H. Brendel Depression s Devastating Toll on the Individual Reduces or eliminates pleasure and jo Compromises and destroys
How to Recognize Depression and Its Related Mood and Emotional Disorders Dr. David H. Brendel Depression s Devastating Toll on the Individual Reduces or eliminates pleasure and jo Compromises and destroys
INPATIENT SERVICES. Inpatient Mental Health Services (Adult/Child/Adolescent)
 INPATIENT SERVICES Inpatient Mental Health Services (Adult/Child/Adolescent) Acute Inpatient Mental Health Services represent the most intensive level of psychiatric care and is delivered in a licensed
INPATIENT SERVICES Inpatient Mental Health Services (Adult/Child/Adolescent) Acute Inpatient Mental Health Services represent the most intensive level of psychiatric care and is delivered in a licensed
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Children s Community Health Plan INTENSIVE IN-HOME MENTAL HEALTH / SUBSTANCE ABUSE SERVICES ASSESSMENT AND RECOVERY / TREATMENT PLAN ATTACHMENT
 Children s Community Health Plan INTENSIVE IN-HOME MENTAL HEALTH / SUBSTANCE ABUSE SERVICES ASSESSMENT AND RECOVERY / TREATMENT PLAN ATTACHMENT Please fax with CCHP prior authorization form to 608-252-0853
Children s Community Health Plan INTENSIVE IN-HOME MENTAL HEALTH / SUBSTANCE ABUSE SERVICES ASSESSMENT AND RECOVERY / TREATMENT PLAN ATTACHMENT Please fax with CCHP prior authorization form to 608-252-0853
FACT SHEET 4. Bipolar Disorder. What Is Bipolar Disorder?
 FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
Behavioral Health Policy Phototherapy Light for the Treatment of Seasonal Affective (SAD) and Other Depressive Disorders
 Behavioral Health Policy Phototherapy Light for the Treatment of Seasonal Affective (SAD) and Other Depressive Disorders Table of Contents Policy: Commercial Coding Information Information Pertaining to
Behavioral Health Policy Phototherapy Light for the Treatment of Seasonal Affective (SAD) and Other Depressive Disorders Table of Contents Policy: Commercial Coding Information Information Pertaining to
Depression in the Elderly: Recognition, Diagnosis, and Treatment
 Depression in the Elderly: Recognition, Diagnosis, and Treatment LOUIS A. CANCELLARO, PhD, MD, EFAC Psych Professor Emeritus and Interim Chair ETSU Department of Psychiatry & Behavioral Sciences Diagnosis
Depression in the Elderly: Recognition, Diagnosis, and Treatment LOUIS A. CANCELLARO, PhD, MD, EFAC Psych Professor Emeritus and Interim Chair ETSU Department of Psychiatry & Behavioral Sciences Diagnosis
Assessment of depression in adults in primary care
 Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
When You Are More Than Down in the Dumps Depression in Older Adults
 When You Are More Than Down in the Dumps Depression in Older Adults Revised by M. Smith (2006) from K.C. Buckwalter & M. Smith (1993), When You Are More Than Down in the Dumps : Depression in the Elderly,
When You Are More Than Down in the Dumps Depression in Older Adults Revised by M. Smith (2006) from K.C. Buckwalter & M. Smith (1993), When You Are More Than Down in the Dumps : Depression in the Elderly,
Dual Diagnosis Nursing Care: Treating the Patient with Co-Occurring Addiction & Mental Health Disorders. Deborah Koivula R.N.
 Dual Diagnosis Nursing Care: Treating the Patient with Co-Occurring Addiction & Mental Health Disorders. Deborah Koivula R.N. Webinar Overview & Objectives I. Review current trends in co-occurring disorders
Dual Diagnosis Nursing Care: Treating the Patient with Co-Occurring Addiction & Mental Health Disorders. Deborah Koivula R.N. Webinar Overview & Objectives I. Review current trends in co-occurring disorders
OUTPATIENT DAY SERVICES
 OUTPATIENT DAY SERVICES Intensive Outpatient Programs (IOP) Intensive Outpatient Programs (IOP) provide time limited, multidisciplinary, multimodal structured treatment in an outpatient setting. Such programs
OUTPATIENT DAY SERVICES Intensive Outpatient Programs (IOP) Intensive Outpatient Programs (IOP) provide time limited, multidisciplinary, multimodal structured treatment in an outpatient setting. Such programs
Bipolar Disorder. When people with bipolar disorder feel very happy and "up," they are also much more active than usual. This is called mania.
 Bipolar Disorder Introduction Bipolar disorder is a serious mental disorder. People who have bipolar disorder feel very happy and energized some days, and very sad and depressed on other days. Abnormal
Bipolar Disorder Introduction Bipolar disorder is a serious mental disorder. People who have bipolar disorder feel very happy and energized some days, and very sad and depressed on other days. Abnormal
Mental health issues in the elderly. January 28th 2008 Presented by Éric R. Thériault [email protected]
 Mental health issues in the elderly January 28th 2008 Presented by Éric R. Thériault [email protected] Cognitive Disorders Outline Dementia (294.xx) Dementia of the Alzheimer's Type (early and late
Mental health issues in the elderly January 28th 2008 Presented by Éric R. Thériault [email protected] Cognitive Disorders Outline Dementia (294.xx) Dementia of the Alzheimer's Type (early and late
Does Non-Suicidal Self-injury Mean Developing Borderline Personality Disorder? Dr Paul Wilkinson University of Cambridge
 Does Non-Suicidal Self-injury Mean Developing Borderline Personality Disorder? Dr Paul Wilkinson University of Cambridge If I see a patient who cuts themself, I just assume they have borderline personality
Does Non-Suicidal Self-injury Mean Developing Borderline Personality Disorder? Dr Paul Wilkinson University of Cambridge If I see a patient who cuts themself, I just assume they have borderline personality
Mood Disorders. What Are Mood Disorders? Unipolar vs. Bipolar
 Mood Disorders What Are Mood Disorders? In mood disorders, disturbances of mood are intense and persistent enough to be clearly maladaptive Key moods involved are mania and depression Encompasses both
Mood Disorders What Are Mood Disorders? In mood disorders, disturbances of mood are intense and persistent enough to be clearly maladaptive Key moods involved are mania and depression Encompasses both
Appendix B NMMCP Covered Services and Exceptions
 Acute Inpatient Hospitalization MH - Adult Definition An Acute Inpatient program is designed to provide medically necessary, intensive assessment, psychiatric treatment and support to individuals with
Acute Inpatient Hospitalization MH - Adult Definition An Acute Inpatient program is designed to provide medically necessary, intensive assessment, psychiatric treatment and support to individuals with
Symptoms of mania can include: 3
 Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Behavioral Health Best Practice Documentation
 Behavioral Health Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: DSM-5 and ICD-10 Codes Major Depressive Disorder Bipolar Disorder Eating
Behavioral Health Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: DSM-5 and ICD-10 Codes Major Depressive Disorder Bipolar Disorder Eating
TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management
 TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management WHY IS THIS IMPORTANT? Depression causes fluctuations in mood, low self esteem and loss of interest or pleasure in normally
TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management WHY IS THIS IMPORTANT? Depression causes fluctuations in mood, low self esteem and loss of interest or pleasure in normally
ICD-10-CM Provider Training Mini-Series. Session 6: Major Depressive Disorder (MDD)
 ICD-10-CM Provider Training Mini-Series Session 6: Major Depressive Disorder (MDD) Y0114_15_25800_I_005_09/15/2015 Disclaimer Welcome to the ICD-10-CM ( ICD-10 ) Provider Training Mini-Series! The ICD-10
ICD-10-CM Provider Training Mini-Series Session 6: Major Depressive Disorder (MDD) Y0114_15_25800_I_005_09/15/2015 Disclaimer Welcome to the ICD-10-CM ( ICD-10 ) Provider Training Mini-Series! The ICD-10
Treatment and management of depression in adults, including adults with a chronic physical health problem
 Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
How to Read the DSM-IV A Tutorial for Beginners
 How to Read the DSM-IV A Tutorial for Beginners By Dr. Robert Tippie, Ph.D. MARET Systems International Previously we explained the validity of pastors using the DSM-IV. In this article we will discuss
How to Read the DSM-IV A Tutorial for Beginners By Dr. Robert Tippie, Ph.D. MARET Systems International Previously we explained the validity of pastors using the DSM-IV. In this article we will discuss
IMR ISSUES, DECISIONS AND RATIONALES The Final Determination was based on decisions for the disputed items/services set forth below:
 Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Risk Adjustment Coding/Documentation Checklist
 Risk Adjustment Coding/Documentation Checklist The following list should be used to ensure that all member and diagnosis-related information is reported, and all the member s chronic conditions are documented
Risk Adjustment Coding/Documentation Checklist The following list should be used to ensure that all member and diagnosis-related information is reported, and all the member s chronic conditions are documented
1 Classification of Depression: Research and Diagnostic Criteria: DSM-IV and ICD-10
 1 1 Classification of Depression: Research and Diagnostic Criteria: DSM-IV and ICD-10 Alan M. Gruenberg, Reed D. Goldstein and Harold Alan Pincus Abstract This chapter shall address the classification
1 1 Classification of Depression: Research and Diagnostic Criteria: DSM-IV and ICD-10 Alan M. Gruenberg, Reed D. Goldstein and Harold Alan Pincus Abstract This chapter shall address the classification
Major Depressive Disorder: Evidence Based Practice
 Major Depressive Disorder: Evidence Based Practice 1) For the diagnosis of MDD, the symptoms must be present for at least a) 2 weeks b) 4 weeks c) 90 days d) 2 months 2) If a MDD episode persists for over
Major Depressive Disorder: Evidence Based Practice 1) For the diagnosis of MDD, the symptoms must be present for at least a) 2 weeks b) 4 weeks c) 90 days d) 2 months 2) If a MDD episode persists for over
See also www.thiswayup.org.au/clinic for an online treatment course.
 Depression What is depression? Depression is one of the common human emotional states. It is common to experience feelings of sadness and tiredness in response to life events, such as losses or disappointments.
Depression What is depression? Depression is one of the common human emotional states. It is common to experience feelings of sadness and tiredness in response to life events, such as losses or disappointments.
Worksite Depression Screening and Treatment: An Innovative, Integrated Program
 Photos placed in horizontal position with even amount of white space between photos and header Photos placed in horizontal position with even amount of white space between photos and header Worksite Depression
Photos placed in horizontal position with even amount of white space between photos and header Photos placed in horizontal position with even amount of white space between photos and header Worksite Depression
Eating Disorder Treatment Protocol
 Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5)
 The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) Cardwell C Nuckols, PhD [email protected] Cardwell C. Nuckols, PhD www.cnuckols.com SECTION I-BASICS DSM-5 Includes
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) Cardwell C Nuckols, PhD [email protected] Cardwell C. Nuckols, PhD www.cnuckols.com SECTION I-BASICS DSM-5 Includes
ICD-10 Update* Mental and Behavioral Health ICD-10-CM Codes Blue Cross Blue Shield of Michigan 2014
 ICD-10 Update* Mental and Behavioral Health ICD-10-CM Codes Blue Cross Blue Shield of Michigan 2014 *NOTE: The information in this document is not intended to impart legal advice. This overview is intended
ICD-10 Update* Mental and Behavioral Health ICD-10-CM Codes Blue Cross Blue Shield of Michigan 2014 *NOTE: The information in this document is not intended to impart legal advice. This overview is intended
SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS
 E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
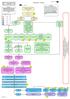 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
Intensive Residential Treatment Services -IRTS. Program Description
 Intensive Residential Treatment Services -IRTS Program Description A highly structured non-hospital based treatment setting that brings comprehensive and specialized diagnostic and treatment services to
Intensive Residential Treatment Services -IRTS Program Description A highly structured non-hospital based treatment setting that brings comprehensive and specialized diagnostic and treatment services to
POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm
 E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
Depression Support Resources: Telephonic/Care Management Follow-up
 Depression Support Resources: Telephonic/Care Management Follow-up Depression Support Resources: Telephonic/Care Management Follow-up Primary Care Toolkit September 2015 Page 29 Role of the Phone Clinician
Depression Support Resources: Telephonic/Care Management Follow-up Depression Support Resources: Telephonic/Care Management Follow-up Primary Care Toolkit September 2015 Page 29 Role of the Phone Clinician
Mental Health and Substance Abuse Reporting Requirements Section 425 of P.A. 154 of 2005
 Mental Health and Substance Abuse Reporting Requirements Section 425 of P.A. 154 of 2005 By April 1, 2006, the Department, in conjunction with the Department of Corrections, shall report the following
Mental Health and Substance Abuse Reporting Requirements Section 425 of P.A. 154 of 2005 By April 1, 2006, the Department, in conjunction with the Department of Corrections, shall report the following
CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS
 CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS Dept of Public Health Sciences February 6, 2015 Yeates Conwell, MD Dept of Psychiatry, University of Rochester Shulin Chen,
CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS Dept of Public Health Sciences February 6, 2015 Yeates Conwell, MD Dept of Psychiatry, University of Rochester Shulin Chen,
