Neonatal respiratory distress including CPAP
|
|
|
- Reginald Dennis
- 7 years ago
- Views:
Transcription
1 Department of Health Neonatal respiratory distress including CPAP Clinical Guideline Presentation v minutes Towards your CPD Hours Great state. Great opportunity.
2 References: The Queensland Clinical Guideline Neonatal respiratory distress including CPAP is the primary reference for this package. Recommended citation: Queensland Clinical Guidelines. Neonatal respiratory distress including CPAP Clinical guideline education presentation I14.2-V2- R19 Queensland Health Disclaimer: This presentation is an implementation tool and should be used in conjunction with the published guideline. This information does not supersede or replace the guideline. Consult the guideline for further information and references. Feedback and contact details: M: GPO Box 48 Brisbane QLD 4001 E: URL: Funding: Queensland Clinical Guidelines is supported by the Clinical Access and Redesign Unit, Queensland Health. Copyright: State of Queensland (Queensland Health) 2014 This work is licensed under a Creative Commons Attribution Non-Commercial No Derivatives 3.0 Australia licence. In essence, you are free to copy and communicate the work in its current form for non-commercial purposes, as long as you attribute the Queensland Maternity and Neonatal Clinical Guidelines Program, Queensland Health and abide by the licence terms. You may not alter or adapt the work in any way. To view a copy of this licence, visit For further information contact Queensland Clinical Guidelines, RBWH Post Office, Herston Qld 4029, guidelines@health.qld.gov.au, phone (+61) For permissions beyond the scope of this licence contact: Intellectual Property Officer, Queensland Health, GPO Box 48, Brisbane Qld 4001, ip_officer@health.qld.gov.au, phone (07) Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 2
3 Abbreviations Abbreviation BGL CSCF CPAP CXR OGT PCO 2 RDS SpO 2 Term Blood glucose level Clinical services capability framework Continuous positive airway pressure Chest x-ray Oral gastric tube Partial pressure of carbon dioxide Respiratory distress syndrome Peripheral saturation of oxygen Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 3
4 Objectives Identify neonates requiring respiratory support following birth Diagnosis and management of respiratory distress Indications for transfer/retrieval Review the management principles for a neonate requiring CPAP Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 4
5 Signs of respiratory distress Tachypnoea (> 60 breaths/minute) Audible expiratory grunt Sternal, intercostal/lower costal recession Nasal flaring Cyanosis or O 2 requirement Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 5
6 Causes of respiratory distress Hyaline membrane disease Infection Group B streptococcal disease Retained fetal lung fluid Transient tachypnoea of the newborn (TTN) Aspiration meconium, blood or liquor Pneumothorax Congenital abnormalities Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 6
7 Oxygenation Give O 2 to maintain SpO % Continuously monitor: O 2 concentration SpO 2 preferably on right upper limb Respiration and heart rate Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 7
8 Blood cultures Collect blood cultures and full blood count Collect surface swabs if indicated Check blood culture results: At 24 hours Again at 48 hours If positive, contact higher level service to discuss duration of antibiotic therapy Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 8
9 Antibiotics Aim to commence within 30 minutes of diagnosis If no local policy, recommend: Penicillin 60 mg/kg/dose 12 hourly OR Ampicillin 50 mg/kg/dose 12 hourly AND Gentamicin 2.5mg/kg 30 weeks daily or if < 30 weeks every 36 hours Check Gentamicin level before 3 rd dose Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 9
10 Fluids Insert IV cannula and commence fluids 10% Dextrose at 60 ml/kg/day Consider umbilical venous catheter if IV difficult to achieve Small trophic feeds (2 ml/kg 3 hourly) may be started if stable and respirations comfortable Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 10
11 Chest x-ray To identify pathology - especially: Pneumothorax Congenital diaphragmatic hernia Chest masses Level 3 neonatal services Arrange review at Level 5 or Level 6 Nursery Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 11
12 Blood glucose Refer to Queensland Clinical Guideline: Newborn hypoglycaemia Aim for BGL 2.6 mmol/l or greater Treat BGL < 2.6 mmol/l Monitor 4 6 hourly for 24 hours or as indicated by BGL Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 12
13 Supportive care Maintain temperature Axillary C Skin C Minimal handling disturb only when absolutely necessary Blood gases not routinely required Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 13
14 Consultation and referral Level 2 and 3* - Contact a higher level service to discuss: Initiation of treatment If O 2 requirements reach 30% If O 2 need rapidly rises (>10% over 2 hours) If neonate < 35 weeks gestation Daily for ongoing advice and support Level 6 can be contacted by any level of service for advice *Nursery levels according to Clinical Services Capability Framework Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 14
15 CPAP Continuous Positive Airway Pressure (CPAP) is the application of positive pressure to the airways of spontaneously breathing neonates throughout the respiratory cycle Manage in Level 4 nursery or above Resource requirements (human and equipment) as per CSCF Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 15
16 Benefits of CPAP Reduces O 2 requirements Reduces the work of breathing Reduces apnoea, bradycardia & episodes of O 2 desaturation Decreases need for ventilation Reduces risk of extubation failure Reduces the natural duration of RDS May prevent the need for transfer Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 16
17 Indications for CPAP Signs of respiratory distress O 2 requirement 30% to maintain SpO % Commence on CPAP if O 2 requirement < 30% and there are other significant signs of respiratory distress Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 17
18 Patient interface CPAP generator creates pressure in circuit Circuit for continuous flow of humidified gasses Interface device to connect to neonate s airway Bubble CPAP System Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 18
19 Patient interface Short binasal prong Hudson prongs Snorkel midline device Nasal mask Long nasopharyngeal tube Not routinely recommended Hudson Snorkel Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 19
20 Commencing CPAP Commence CPAP at 8 cm H 2 O Starting high and decreasing with improvement is preferable to starting low and increasing with deterioration Give O 2 to maintain SpO % Use gas flow at the lowest level that achieves desired pressure Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 20
21 Expected clinical course Acute disease normally lasts 1 3 days Signs of improvement in respiratory rate work of breathing (grunting, sternal/intercostal recession, nasal flaring) in O2 needs Improved CXR appearance/lung volume Improved blood gas (if measured) Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 21
22 Weaning CPAP Commence weaning when: SpO 2 consistently > 96% Grunting ceased/recession reduced Wean O 2 before pressure Wean to 21% then Pressure 1 cm every 2 4 hours until 5 cm H 2 O is reached Cease when stable in 21% and 5 cm H 2 O Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 22
23 Deterioration Signs of failure of CPAP delivery O 2 > 50% to maintain SpO % Rapid rise in O 2 requirement Respiratory acidosis (ph < 7.25) Recurrent apnoeic episodes Increased work of breathing Requires immediate medical assessment and CXR Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 23
24 Complications: Air Leaks Air leak syndromes (pneumothorax, pneumomediastinum, pneumopericardium, pulmonary interstitial emphysema (PIE)) Clinical signs: Increasing respiratory distress/ PCO 2 Oxygen desaturation Decreased air entry/asymmetrical chest movement or appearance Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 24
25 Pneumothorax Emergency management when neonate rapidly deteriorating: Needle thoracocentesis Intercostal catheter Refer to Appendix B in Guideline Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 25
26 Complications: Pressure injury Results from pressure of CPAP devices Source of discomfort, site for infection, long term functional and/or cosmetic sequelae Requires vigilant clinical surveillance to avoid pressure, traction, friction and moisture Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 26
27 Pressure injury prevention Measure and size interface for each neonate Position binasal prongs with 2 mm gap between horizontal section and nose No blanching of surrounding skin With cares inspect for signs of pressure injury Document presence/absence, location and extent of any injury Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 27
28 Complications: Other Abdominal distension - gas enters stomach and gastrointestinal tract Insert shortest available OGT, aspirate or free drainage Use size 8 FG - especially if large air aspirates or abdominal distension Use lowest flow of gas to achieve pressure Over inflation - excessive pressure can: Increase work of breathing Reduce cardiac output Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 28
29 Continuously: Monitoring Heart rate, Respiratory rate, SpO 2, PiO 2 Vigilant surveillance: Circuit integrity & equipment function, condensation Interface correctly positioned OGT position, Abdominal distension Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 29
30 Neonatal care Suction as required Cares 4 6 hourly with 1 2 staff Inspect for pressure injury with cares Aspirate OGT regularly Minimal handling Incorporate principles of developmental care Use a family centred approach Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 30
31 Prophylactic CPAP Not recommended Other therapies Humidified high flow nasal cannula Routine use instead of CPAP for acute lung disease is not recommended INSURE technique Routine use followed by CPAP not recommended for 32 weeks gestational age Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 31
32 Key Points Timely and appropriate management of respiratory distress improves outcomes Use the statewide guidelines to guide management Contact a higher level nursery for support and advice when necessary Involve the parents Queensland Clinical Guidelines: Neonatal respiratory distress including CPAP 32
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS
 NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
A. All cells need oxygen and release carbon dioxide why?
 I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
Lothian Diabetes Handbook MANAGEMENT OF DIABETIC KETOACIDOSIS
 MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
NURSING SERVICES DEPARTMENT
 NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Neonatal resuscitation
 Neonatal resuscitation Document title: Neonatal resuscitation Publication date: October 2011 Document number: Document supplement Replaces document: Author: Audience: MN11.5-V2-R16 The document supplement
Neonatal resuscitation Document title: Neonatal resuscitation Publication date: October 2011 Document number: Document supplement Replaces document: Author: Audience: MN11.5-V2-R16 The document supplement
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NEONATAL INTENSIVE CARE UNIT: ADMISSION AND TRANSFER PROCEDURE AND ACUITY GUIDELINES Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE:
PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NEONATAL INTENSIVE CARE UNIT: ADMISSION AND TRANSFER PROCEDURE AND ACUITY GUIDELINES Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE:
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
Diabetic ketoacidosis in children and young people bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They
High-Frequency Oscillatory Ventilation
 High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
NHS FORTH VALLEY Chest Drain Insertion by Seldinger Method (Pigtail drains)
 NHS FORTH VALLEY Chest Drain Insertion by Seldinger Method (Pigtail drains) Date of First Issue 12/12/2012 Approved 12/12/2012 Current Issue Date 12/12/2012 Review Date 12/12/2014 Version 1 EQIA Yes 14/12/2012
NHS FORTH VALLEY Chest Drain Insertion by Seldinger Method (Pigtail drains) Date of First Issue 12/12/2012 Approved 12/12/2012 Current Issue Date 12/12/2012 Review Date 12/12/2014 Version 1 EQIA Yes 14/12/2012
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
CORD BLOOD COLLECTION / ANALYSIS- AT BIRTH
 WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Diabetic Ketoacidosis
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Diabetic Ketoacidosis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Diabetic Ketoacidosis Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Lung Cancer. Know how to stay strong
 Lung Cancer Know how to stay strong What is cancer? 2 Cancer is a disease when some cells in the body grow out of control Normal cells Your body has many tiny cells and keeps making new cells to keep you
Lung Cancer Know how to stay strong What is cancer? 2 Cancer is a disease when some cells in the body grow out of control Normal cells Your body has many tiny cells and keeps making new cells to keep you
CHEST TUBES AND CHEST DRAINAGE SYSTEMS
 CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
Hyperosmolar Non-Ketotic Diabetic State (HONK)
 Hyperosmolar Non-Ketotic Diabetic State (HONK) University Hospitals of Leicester NHS Trust Guidelines for Management of Acute Medical Emergencies Management is largely the same as for diabetic ketoacidosis
Hyperosmolar Non-Ketotic Diabetic State (HONK) University Hospitals of Leicester NHS Trust Guidelines for Management of Acute Medical Emergencies Management is largely the same as for diabetic ketoacidosis
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
 GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS
 ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
(C) AMBULANCE VICTORIA
 The Newborn Baby: Definitions and Contacts Newborn definition 'Newborn' refers to the first min to hours post birth. For the purpose of resuscitation, AV accepts up to the first 24 hours from birth in
The Newborn Baby: Definitions and Contacts Newborn definition 'Newborn' refers to the first min to hours post birth. For the purpose of resuscitation, AV accepts up to the first 24 hours from birth in
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Department of Health Commencing insulin therapy
 Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
Troubleshooting a Patient with a Chest Drain. A Simulation Workshop
 Troubleshooting a Patient with a Chest Drain. A Simulation Workshop Outline This is a simulation session that aims to improve skills at assessing a patient with a chest drain. It is undertaken using a
Troubleshooting a Patient with a Chest Drain. A Simulation Workshop Outline This is a simulation session that aims to improve skills at assessing a patient with a chest drain. It is undertaken using a
Neonatal Reference Guide
 Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Congenital Diaphragmatic Hernia. Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate
 Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN
 MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NRP Study Guide. This packet is intended for review only. Requirements to successfully complete NRP:
 This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
Mechanical Ventilation
 Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
NSQHS Standard 1 Governance
 NSQHS Standard 1 Governance How to use the Audit tools Governance Audit Tools Instructions The Health Service and Clinical Innovation Division, Patient Safety Unit, have developed audit tools for facilities
NSQHS Standard 1 Governance How to use the Audit tools Governance Audit Tools Instructions The Health Service and Clinical Innovation Division, Patient Safety Unit, have developed audit tools for facilities
CPT Pediatric Coding Updates 2009. The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009.
 CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
Respiratory failure and Oxygen Therapy
 Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
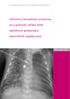 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
More detailed background information and references can be found at the end of this guideline
 Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY
 SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 13.8 THE RESUSCITATION OF THE NEWBORN INFANT IN SPECIAL CIRCUMSTANCES PREMATURITY Temperature management Very premature infants are at particular risk of hypothermia.
Common Conditions, Concerns, and Equipment in the NICU
 Common Conditions, Concerns, and Equipment in the NICU Babies in the NICU are carefully monitored because of their health risk. While the following is a comprehensive list of common conditions found in
Common Conditions, Concerns, and Equipment in the NICU Babies in the NICU are carefully monitored because of their health risk. While the following is a comprehensive list of common conditions found in
NHS FORTH VALLEY. Continuous Positive Airway Pressure (CPAP) Nursing Guidelines
 NHS FORTH VALLEY Continuous Positive Airway Pressure (CPAP) Nursing Guidelines Date of First Issue 10/06/2012 Approved 10/06/2012 Current Issue Date 26/11/2014 Review Date 26/11/2016 Version 1.1 EQIA Yes
NHS FORTH VALLEY Continuous Positive Airway Pressure (CPAP) Nursing Guidelines Date of First Issue 10/06/2012 Approved 10/06/2012 Current Issue Date 26/11/2014 Review Date 26/11/2016 Version 1.1 EQIA Yes
TRACHEOSTOMY TUBE PARTS
 Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD
 Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD This document describes the standard for clinical assessment, prescription, optimal management and follow-up of patients receiving domiciliary
Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD This document describes the standard for clinical assessment, prescription, optimal management and follow-up of patients receiving domiciliary
Milliman Guidelines NICU Levels*
 Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
MECHANICAL VENTILATION IN THE NEONATE
 Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz
 Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
From AARC Protocol Committee; Subcommittee Adult Critical Care Version 1.0a (Sept., 2003), Subcommittee Chair, Susan P. Pilbeam
 AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
a guide to understanding pierre robin sequence
 a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
ASSISTED VENTILATION IN NEONATES
 ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
2008 Coding Questions and Answers
 2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
Cord Blood Erythropoietin and Markers of Fetal Hypoxia
 July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
Airway Pressure Release Ventilation
 Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
The Fetal Treatment Program
 CONGENITAL LUNG LESIONS* The Fetal Treatment Program *This information is intended to supplement your consultation with members of the Fetal Treatment Program regarding your unborn child with a suspected
CONGENITAL LUNG LESIONS* The Fetal Treatment Program *This information is intended to supplement your consultation with members of the Fetal Treatment Program regarding your unborn child with a suspected
Respiratory Syncytial Virus (RSV)
 Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
Pediatric Respiratory System: Basic Anatomy & Physiology. Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City
 Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
DRG 475 Respiratory System Diagnosis with Ventilator Support. ICD-9-CM Coding Guidelines
 DRG 475 Respiratory System Diagnosis with Ventilator Support ICD-9-CM Coding G The below listed g are not inclusive. The coder should refer to the applicable Coding Clinic g for additional information.
DRG 475 Respiratory System Diagnosis with Ventilator Support ICD-9-CM Coding G The below listed g are not inclusive. The coder should refer to the applicable Coding Clinic g for additional information.
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Applicant Information Sheet for MASS 45 Adult Oxygen: Initial Application and 4 Month Review
 , Queensland Health Applicant Information Sheet for Applicants should retain this section for their records Eligibility Administrative eligibility is dependent upon the applicant being a permanent Queensland
, Queensland Health Applicant Information Sheet for Applicants should retain this section for their records Eligibility Administrative eligibility is dependent upon the applicant being a permanent Queensland
Preemie Common Problems/Diseases
 Jaundice (Bilirubin) Jaundice is the yellow color to the skin that is often seen in the first few days after birth. The yellow color is due to bilirubin. Bilirubin is produced when red blood cells get
Jaundice (Bilirubin) Jaundice is the yellow color to the skin that is often seen in the first few days after birth. The yellow color is due to bilirubin. Bilirubin is produced when red blood cells get
Fetal Acid Base Status and Umbilical Cord Sampling. David Acker, MD
 Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
NRP 2012 Putting New Resuscitation Guidelines into Practice
 Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT
 CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT The 'DR ABCDE' approach to assessing an acutely unwell patient should be at the front of every junior doctor's mind whenever they get bleeped or asked to see
CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT The 'DR ABCDE' approach to assessing an acutely unwell patient should be at the front of every junior doctor's mind whenever they get bleeped or asked to see
Premature Infant Care
 Premature Infant Care Introduction A premature baby is born before the 37th week of pregnancy. Premature babies are also called preemies. Premature babies may have health problems because their organs
Premature Infant Care Introduction A premature baby is born before the 37th week of pregnancy. Premature babies are also called preemies. Premature babies may have health problems because their organs
ACID- BASE and ELECTROLYTE BALANCE. MGHS School of EMT-Paramedic Program 2011
 ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
MODULE. POSITIVE AIRWAY PRESSURE (PAP) Titrations
 MODULE POSITIVE AIRWAY PRESSURE (PAP) Titrations POSITIVE AIRWAY PRESSURE (PAP) TITRATIONS OBJECTIVES At the end of this module the student must be able to: Identify the standards of practice for administering
MODULE POSITIVE AIRWAY PRESSURE (PAP) Titrations POSITIVE AIRWAY PRESSURE (PAP) TITRATIONS OBJECTIVES At the end of this module the student must be able to: Identify the standards of practice for administering
Asthma in Infancy, Childhood and Adolescence. Presented by Frederick Lloyd, MD Palo Alto Medical Foundation Palo Alto, California
 Asthma in Infancy, Childhood and Adolescence Presented by Frederick Lloyd, MD Palo Alto Medical Foundation Palo Alto, California Major Health Problem in Childhood Afflicts 2.7 million children in the USA
Asthma in Infancy, Childhood and Adolescence Presented by Frederick Lloyd, MD Palo Alto Medical Foundation Palo Alto, California Major Health Problem in Childhood Afflicts 2.7 million children in the USA
The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2
 The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2 Ramalinga P. Reddy, M.D., MBA, FCCP Director, Children s Pulmonary & Sleep Center Mercy Children s Hospital
The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2 Ramalinga P. Reddy, M.D., MBA, FCCP Director, Children s Pulmonary & Sleep Center Mercy Children s Hospital
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Arterial Blood Gas Case Questions and Answers
 Arterial Blood Gas Case Questions and Answers In the space that follows you will find a series of cases that include arterial blood gases. Each case is then followed by an explanation of the acid-base
Arterial Blood Gas Case Questions and Answers In the space that follows you will find a series of cases that include arterial blood gases. Each case is then followed by an explanation of the acid-base
Over 660 Contact Hours of Online Continuing Nursing Education!
 Over 660 of Online Continuing Nursing Education! Choose from Four Great Series: Clinical Health Care Clinical & Continuing Education MedSenses AACN NetLearning is committed to providing you with the very
Over 660 of Online Continuing Nursing Education! Choose from Four Great Series: Clinical Health Care Clinical & Continuing Education MedSenses AACN NetLearning is committed to providing you with the very
COURSE SYLLABUS RC 223 CLINICAL-3
 COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
Statewide Anaesthesia and Perioperative Care Clinical Network (SWAPNET)
 Guideline [Optional heading here. Change font size to suit] Document Number # QH-GDL-395:2013 Statewide Anaesthesia and Perioperative Care Clinical Network (SWAPNET) Anaesthesia: non-bariatric surgery
Guideline [Optional heading here. Change font size to suit] Document Number # QH-GDL-395:2013 Statewide Anaesthesia and Perioperative Care Clinical Network (SWAPNET) Anaesthesia: non-bariatric surgery
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES. Appendix 5 166
 APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES Appendix 5 166 CORE CURRICULUM IN CHILD HEALTH This document is a guide for undergraduates, and summarises the key knowledge, skills and attitudes that it is
APPENDIX 5 MBCHB CURRENT LEARNING OBJECTIVES Appendix 5 166 CORE CURRICULUM IN CHILD HEALTH This document is a guide for undergraduates, and summarises the key knowledge, skills and attitudes that it is
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Chapter 2 - Anatomy & Physiology of the Respiratory System
 Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Mechanical Ventilators
 University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
Management of airway burns and inhalation injury PAEDIATRIC
 Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
The Complete list of NANDA Nursing Diagnosis for 2012-2014, with 16 new diagnoses. Below is the list of the 16 new NANDA Nursing Diagnoses
 The Complete list of NANDA Nursing Diagnosis for 2012-2014, with 16 new diagnoses. Below is the list of the 16 new NANDA Nursing Diagnoses 1. Risk for Ineffective Activity Planning 2. Risk for Adverse
The Complete list of NANDA Nursing Diagnosis for 2012-2014, with 16 new diagnoses. Below is the list of the 16 new NANDA Nursing Diagnoses 1. Risk for Ineffective Activity Planning 2. Risk for Adverse
NSQHS Standard 1 Governance
 NSQHS Standard 1 Governance Definitions sheet Governance Audit Tools Definitions Contents 1. Open Disclosure Program Page 1 2. ACUTE Clinical Record Audit Tools Page 2 -----------------------------------------------------------------------------------
NSQHS Standard 1 Governance Definitions sheet Governance Audit Tools Definitions Contents 1. Open Disclosure Program Page 1 2. ACUTE Clinical Record Audit Tools Page 2 -----------------------------------------------------------------------------------
Resuscitation of the baby at birth
 APPENDIX I Resuscitation of the baby at birth I.1 OBJECTIVES This will teach you: I.2 INTRODUCTION the important physiological differences in the newly born baby the equipment used for resuscitation at
APPENDIX I Resuscitation of the baby at birth I.1 OBJECTIVES This will teach you: I.2 INTRODUCTION the important physiological differences in the newly born baby the equipment used for resuscitation at
Protocols for Early Extubation After Cardiothoracic Surgery
 Protocols for Early Extubation After Cardiothoracic Surgery AATS / STS CT Critical Care Symposium April 27, 2014 Toronto, Ontario Nevin M. Katz, M.D. Johns Hopkins University Foundation for the Advancement
Protocols for Early Extubation After Cardiothoracic Surgery AATS / STS CT Critical Care Symposium April 27, 2014 Toronto, Ontario Nevin M. Katz, M.D. Johns Hopkins University Foundation for the Advancement
1.40 Prevention of Nosocomial Pneumonia
 1.40 Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare workers and contract healthcare
1.40 Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare workers and contract healthcare
11 Newborn Life Support
 11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
