Contents: POCT Program Massachusetts General Hospital - Pathology Service 55 Fruit Street, Boston, MA 02114
|
|
|
- Anthony Sims
- 9 years ago
- Views:
Transcription
1 Title: i-stat Operations and Testing Procedure Cross References: i-stat Operator Training Checklist i-stat INR Fingerstick Training and Assessment Record i-stat Competency Assessment 6-month and Annual i-stat Instrument Competency-Written Test i-stat Cartridge Temperature Storage Log i-stat Instrument Corrective Action Log i-stat Instrument Validation Log i-stat Record of Receipt-QC Documentation Log i-stat Training Guide MGH POCT Inter-Laboratory Correlation Procedure MGH POCT QC Storage Ordering and Documentation Guide POCT Proficiency Testing Procedure POCT Proficiency Testing Evaluation Worksheet i-stat CLEW update form POCT Program Massachusetts General Hospital - Pathology Service 55 Fruit Street, Boston, MA Contents: Purpose... 2 Scope... 2 Policy and Procedure Statement... 2 Proficiency Testing (For G3+, CG8+, CG4+, ACT, PT/INR and Troponin cartridges)... 2 Regulatory Requirements... 3 Competency Assessment... 3 Limitations/Interferences... 3 Test Kit/Supplies/Equipment... 6 Calibration... 7 Calibration Verification... 7 Electronic Quality Control... 7 Liquid Quality Control... 8 Barcode Scanning... 8 Calculations... 9 Reporting results... 9 Preventive Maintenance... 9 Instrument Replacement Policy Connectivity and LIS / HIS Down Time Procedure - OR Connectivity and LIS / HIS Down Time Procedure - Imaging Troubleshooting Alternative method References Reference Ranges ACT (Kaolin) Cartridge Procedure CG8+, CG4+, and G3+ Cartridges Procedure Creatinine Cartridge Procedure PT/INR Cartridge Procedure Troponin I Procedure Written By: Kim Gregory MT(ASCP) Date: 7/08 Nancy Toscano MT (ASCP) Date: 12/09 1
2 Purpose This document outlines policies and procedures pertaining to testing on the i-stat. In an effort to be concise, some information from the manufacturer s recommended procedure may be excluded. It is recommended that operators familiarize themselves with the manufacturer s product information that accompanies each package and their manual, if one exists. Scope Level of Personnel: All RN s, Catheterization lab techs, Perfusionists, Respiratory Therapists, Laboratory Technologists, and MD s who have successfully completed initial training and fulfilled the specific competency requirements for the complexity level of each cartridge. Testing Site: Clinical sites approved and on file with the Pathology service s POCT Division. Approved Cartridges: G3+, CG8+, CG4+, Creatinine, ACT (Kaolin), PT/INR, Troponin I Policy and Procedure Statement The i-stat is a portable clinical analyzer used in conjunction with i-stat cartridges to obtain definitive quantitative measurements of ACT, blood gas parameters, lactate, creatinine, PT/INR and Troponin I utilizing i-stat cartridges. The disposable cartridge contains all of the system s components (reagents, sensors, and waste container). Proficiency Testing (For G3+, CG8+, CG4+, ACT, PT/INR and Troponin cartridges) The College of American Pathologists (CAP) sends unknown samples to the laboratory for analysis several times per year. Results are submitted to the CAP within 10 days of survey receipt. If a site fails 2 out of 3 events or two consecutive events according to federal law, it may be required to discontinue testing. All Survey results are to be handled and reported in the same manner as clinical results following the directions on the CAP Survey package insert. The samples are not to be analyzed in duplicate unless clinical specimens are analyzed in duplicate. Actions or decisions must be documented. Participation must be random and not assigned to specific individuals. Successful participation may be used as demonstrating successful competency for that year. Upon receiving the survey: The POCT program will contact the participating departments regarding the survey and the timeline of the survey to be performed. The departments must be available within the period identified by POCT. The Key operators must make sure of the following: o Instruments are in good working order. o Randomly select staff to participate, but ensure that subsequent surveys are rotated among different staff (e.g. document in a log) o Maintain original CAP survey form with the results documented. o Maintain the signed Attestation form. o In addition, retain copies of above in the files of testing personnel. Once results are obtained, they should be given to the POCT Coordinators who will send them to CAP via mail, fax or electronic entry on the CAP website. Site Director and CLIA certificate Director or designees shall review survey results to assess performance and ensure compliance with the standard and comment. Scores of 100% minimally requires documentation of review by the Director or designee. Scores between 100% and 80% requires a comprehensive investigation and remedial action documented of unsuccessful challenges. Scores less than 80% requires a comprehensive investigation and documentation of remedial action of unsuccessful challenges. Scores of less than 80 percent may jeopardize a sites ability to continue to perform testing. Should a site fail proficiency, they will be required to immediately perform a comprehensive investigation and document remedial action. Operator re-training may be required. In order to avoid cessation of testing, a site failing a challenge will be expected to develop and implement a more aggressive plan for performance improvement 2
3 Each site is responsible for completing survey challenges when they arrive. Anticipated Survey Periods: AQ3 (Blood Gases), & PCARM (Cardiac Markers) WP3 (PT/INR) CT-1/CT5 (Activated Clotting Time) Product Receipt Evaluation receipt Product Receipt Evaluation receipt Product Receipt Evaluation receipt March April February March January February June July May June July August October November September October Regulatory Requirements I. Each testing site must have a documented quality control program, which is developed in collaboration with or has been approved by the MGH Pathology Service. II. All test results must be maintained in patient records with all required information for four years Required information: 1. Patient s name 2. Medical Record Number 3. Patient s gender 4. Patient s age or date of birth 5. Date & time test collected, performed and reported 6. Ordering Physician 7. Responsible physician (if not 6) 8. Reference or Target Range 9. Test Performed 10. Test units 11. Lab name III. Additional information that must be retained for four years: 1. Testing personnel records 2. Quality control results 3. Product information (i.e. serial number, lot numbers, expiration dates, etc.), information on quality control and any remedial action 4. QC charts, maintenance sheets, reference and critical ranges IV. Other 1. Universal precautions must be observed when handling any patient specimen. 2. A physician s order or standing order is required prior to performing test. 3. The Hospital Hand Hygiene policy must be adhered to at all times. V. Linearity/Calibration Verification The POCT program will perform and document linearity/calibration verification checks every six months for non - waived cartridges if applicable. Competency Assessment Testing personnel must demonstrate competency prior to direct patient testing. Refer to the individual cartridge procedures for specific competency requirements. All operators must read the procedure manual and complete the Operator Training Checklist after initial training and Competency Assessment Checklist after completing the competency assessment. Expired Operators: Operators that fail to meet competency requirements within 365 days will be locked out of the system. They will be required to undergo retraining and competency assessment according to above. Limitations/Interferences Interferences 3
4 An interferent is a substance, which, if present at significant levels in the blood specimen being analyzed, will produce an error in the result of the analyte being measured. For example, in the table below, β-hydroxybutyrate at sample concentration level of 16 mmol/l would decrease the measured sodium by 5 mmol/l. Analyte Interferent Details/Interferent Concentration/ ACT Incorrect handling Analyzer not maintained on a level surface during testing Effect on Analyte Result Results may be affected by >10% Exogenously added heparin, citrate, oxalate or EDTA Heparinized syringe Will interfere with results Creatinine Acetaminophen Ascorbate Bromide CO2 1 mmol/l mmol/l 100 mg/dl When Creat < 2mg/dL: pco2 >40 mmhg pco2 < 40 mmhg Increase ( )Creat by 0.25 mg/dl Increase ( )Creat by 0.7 mg/dl Increase ( )Creat by 0.8 mg/dl Increase ( )Creat by 6.9%/10 mmhg Decrease ( )Creat by 6.9%/10mmHg When Creat >2mg/dL: pco2 >40 mmhg pco2 < 40 mmhg Decrease ( )Creat by 3.7%/10mmHg Increase ( ) Creat by 3.7%/10mmHg Glucose (Cartridge) Creatine N-acetylcysteine Hydroxyurea Bromide PH Oxygen Hydroxyurea Thiocyanate 5 mg/dl 16.6mmol/L mmol/l (300 mg/dl) ph: per 0.1 ph units below 37 C ph: per 0.1 ph units above 37 C PO2 less than C 100 μmol/l 24 mmol/l (140 mg/dl) Increase( ) Creat by 0.20 mg/dl Increase( ) Creat by 0.4 mg/dl Use an alternative method to measure creatinine when patients have been administered hydroxyurea. Decrease ( ) glucose by 30 mg/dl Decrease ( ) glucose by 0.9 mg/dl (0.05 mmol/l) Increase ( ) glucose by 0.8 mg/dl (0.04 mmol/l) May decrease ( ) glucose Increase ( ) glucose 8 mg/dl (0.44 mmol/l) Decrease ( ) glucose by approx. 23% Analyte Interferent Details/Interferent Concentration Ionized Calcium Magnesium β-hydroxybutyrate Lactate Salicylate 1.0 mmol/l above normal 20 mmol/l 20 mmol/l 4.34 mmol/l Effect on Analyte Result Increase ( ) ica by 0.04 mmol/l Decrease ( ) ica by 0.1 mmol/l Decrease ( ) ica by 0.05 mmol/l Decrease ( ) ica by 0.1 mmol/l Lactate Bromide 25 mmol/l (200 mg/dl) Decrease ( ) lactate by 40% Cysteine 6.4 mmol/l (101 mg/dl) Decrease ( ) lactate by 11% Hydroxyurea Glycolic Acid 100 μmol/l Increase( ) Use alternative method to measure lactate Increase ( ) lactate 4
5 PCO2 PT/INR Propofol (Diprovan ) Thiopental Sodium Cubicin (daptomycin for injection) Chlorhexidine Gluconate Lupus Anticoagulant Antibodies For patients administered propofol or thiopental sodium, i-stat recommends the use of CG4+, CG8+, EG6+, and EG7+ cartridges, which are free from clinically significant interference at all relevant therapeutic doses. i-stat does not recommend the use of EC8+ cartridges for patients receiving propofol or thiopental sodium. This antibiotic has been found to cause a concentration-dependent false prolongation of prothrombin time (PT) and elevation of INR when using the i- STAT PT/INR test. It s recommended that an alternate testing method be used. The i-stat PT/INR test may report false prolongation of the prothrombin time (PT) and an elevation of the INR on samples contaminated with Chlorhexidine Gluconate. Sodium β-hydroxybutyrate Lactate Bromide 16 mmol/l (166 mg/dl) 20 mmol/l 37.5 mmol/l If the presence of lupus anticoagulant antibodies is known or suspected, use an alternate testing method. Decrease ( ) Na by 5 mmol/l Decrease ( ) Na by 5 mmol/l Increase ( ) Na by 5 mmol/l Troponin I Heparin 90 U/mL Decrease ( ) troponin by 20% Gross Hemolysis Rare Antibodies to troponin or its circulating complexes From traumatic draw or residual alcohol from drawing site Decrease ( ) troponin Samples from patients who have been exposed to animals or who have received therapeutic or diagnostic procedures employing immunoglobulins or reagents derived from immunoglobulins may contain antibodies, i.e. HAMA or other heterophile antibodies, which may interfere with immunoassays and produce erroneous results. While this product contains reagents that minimize the effect of these interferents, and QC algorithms designed to detect their effects, the possibility of interference causing erroneous results should be evaluated carefully in cases where there are inconsistencies in the clinical information. Results from the i-stat ctni assay should be considered in the context of the entirety of the available clinical information. 5
6 Test Kit/Supplies/Equipment Product Vendor Manufacturer # i-stat Liquid Controls: Level 1 Level 2 Level 3 Calibration Verification (4 ampoules each - levels 1 thru 5) i-stat 06F F F14-01 PeopleSoft # i-stat 06F CG8+ Cartridge i-stat 03P CG4+ Cartridge i-stat 03P G3+ Cartridge i-stat 03P Tests Creatinine Cartridge i-stat 03P Creatinine ACT Liquid Controls Level 1 Level 2 i-stat 06P P Na, K, ica, Glucose, ph, PCO2, PO2, lactate, Creatinine Na, K, ica, Glucose, ph, PCO2, PO2, Lactate Na, K, ica, Glucose, ph, PCO2, PO2, calculated parameters: TCO2, HCO3, BE, so2 Lactate, ph, PCO2, PO2, calculated parameters: TCO2, HCO3, BE, so2 ph, PCO2, PO2, calculated parameters: TCO2, HCO3, BE, so2 ACT (Kaolin) ACT (Kaolin) Cartridge i-stat 03P ACT (Kaolin) PT/INR Cartridge i-stat 03P PT/INR INR Liquid Controls Level 1 Level 2 i-stat 06P P PT/INR ctni Cartridge i-stat 03P Troponin I ctni Liquid Controls Level 1 Level 2 Level 3 Cardiac Markers ctni Calibration Verification Kit (3 levels x 2 each level) i-stat 06F F F Troponin I i-stat 06F Troponin I Electronic simulator i-stat 06F N/A Syringes 1 ml B&D Syringes 3 ml Portex Luerlock syringe Portex Storage requirement See individual cartridge procedure Store at 2-8ºC See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure See individual cartridge procedure < -18º C (-1º F), ctni Liquid Controls Room Temperature Room Temperature Room Temperature Room Temperature I-STAT1 9V NiMH Battery I- STAT 06F Room Temperature 6
7 Calibration Calibration is performed automatically as part of the test cycle on each cartridge type. Operator intervention is not necessary. Calibration Verification Calibration Verification (CAL VER) using the CAL VER solutions (low, medium, and high levels) on all non-waived analytes is required. (i.e. G3+, CG4+, CG8+, and Troponin I) CAL VER is performed: 1. On any new, or replacement device before clinically used 2. Every 6 months 3. As part of the troubleshooting process when controls reflect an unusual trend or are consistently out of range. Run each level once. i-stat analyzer must be docked after running the CAL VER solutions. POCT program will print out the reports from Precision web. Signed and approved by Medical director or designee. To perform CAL VER on i-stat: Press Menu. Press 3 to select Quality Tests. Press 3 to select CAL VER. If the Calibration Verification fails, the analyzer must be removed from use. Electronic Quality Control Electronic Simulators: The Electronic Simulator (both external and internal) is a quality control device for the analyzer. It simulates two levels of electrical signals that stress the analyzer s signal detection function both below and above measurement ranges. It provides an independent check on the ability of the analyzer to take accurate and sensitive measurements- of voltage, current and resistance from the cartridge. An analyzer will pass or fail this test depending on whether or not it measures these signals within specified limits. The Electronic Simulator will fail if high relative humidity interferes with the measurements, making separate recording of humidity unnecessary. A. Internal Electronic Simulator: The Internal Electronic Simulator runs every 8 hours for blood gases and for all the analytes every 24 hours. Inserting a cartridge triggers the internal simulator. When 8 hours has elapsed since the last Electronic Simulator test (internal or external), it will automatically perform the internal test before the sample is tested, adding about seconds to the testing cycle. 1. If it fails, the testing cycle stops and FAIL displays on the screen. Immediately rerun the cartridge in the same analyzer to confirm the FAIL. If the cartridge fails again rerun the cartridge in a different analyzer (if less than three minutes has lapsed from the time of cartridge filling.) If the cartridge fails in more than one analyzer, use a different cartridge. 2. If it passes, the cartridge cycle continues to completion and the user receives the test results. B. External Electronic Simulator: The External Electronic Simulator is a stable electronic device, which is inserted into the cartridge port of the analyzer as described above. It should be run when: 1. The analyzer has been dropped 2. Every six months 3. After major malfunction 4. Replacement analyzer received from i-stat To run external Simulator: Press the Menu key to access the Administration menu. Press the #3 for Quality test Press the #4 for Simulator 7
8 1. Insert the simulator into the analyzer with the I facing up. (Do not touch the contact pads). Cartridge Locked is displayed indicating that the simulator should not be removed. DO NOT ATTEMPT TO REMOVE THE SIMULATOR WHILE THE Cartridge Locked MESSAGE IS DISPLAYED. AN ATTEMPT TO REMOVE FORCIBLY THE SIMULATOR DURING THIS CYCLE MAY DAMAGE THE ANALYZER. 2. If PASS is displayed on the analyzer screen, remove the simulator after the Cartridge, Locked message disappears from the display screen. 3. If FAIL is displayed on the analyzer screen: Repeat the procedure with the same Electronic Simulator. If PASS is displayed, use the analyzer as required. If FAIL is displayed, repeat the procedure with a different Electronic simulator, if available. a) If PASS is displayed with the second simulator, use the analyzer as required. b) If FAIL is displayed with the second Electronic simulator: (1) Do not analyze patient samples with the analyzer. (2) Transmit the result to Precision Web. (3) Record the failure in the Instrument Corrective Action Log, along with action taken. C. Thermal Probe Check i-stat analyzers contain a thermal control subsystem consisting of two thermal probes with thermistors and heating contact wires. When measurements are performed at a controlled temperature, the thermal probes in the analyzer contact the metalized area under the chips in the cartridge and maintain the temperature of the sensors and the fluids that come into contact with these sensors at the required temperature of 0.10C. The thermal probe check must be verified twice each year, after i-stat software update. Check the thermal probes as follows: Liquid Quality Control 1. If the analyzer and simulator have been stored separately in areas where the ambient temperature differs by more than 3C (5F), allow the simulator and analyzer to stand in the same place, out of drafts, for 30 minutes before inserting the simulator into the analyzer. Handle the simulator as little as possible to maintain its thermal uniformity and stability. 2. Insert the simulator into the analyzer. 3. When the results are displayed, press the period button and the difference between the thermal probes can be viewed on the analyzer s screen. (Acceptable: a value equal to or less that 0.1) If a FAIL message with t Quality Check Code, or a value greater than 0.1 displays repeat the procedure. Repeat the procedure if is displayed. Call Technical Support for repeated failures. 4. Documentation of results appears electronically in Precision Web under the test detail of the electronic simulator. 5. The results of the Thermal Probe Check for each analyzer are documented on the Thermal Probe Check Log. Liquid Quality Control must be performed: 1. On every analyzer prior to initial placement for patient testing 2. On every new lot number and every new shipment of cartridges 3. When there s a suspected cartridge or storage problem 4. On any back up analyzer placed in use before patient testing 5. On all cartridge/reagent types as well as all analytes. If the same analyte occurs on multiple cartridge/reagent types, it must be tested on every cartridge/reagent type 6. Monthly to check storage conditions of cartridges Note: Implementing a new or replacement device that uses Non-Waived Cartridges: i-stat is considered an option #1 device under CLIA. Point of care testing staff must run liquid controls daily for the first 10 days concurrently with EQC, both internal and external. If no QC failures occur then the analyzer is ready to use. Any failure will require further evaluation. Document results on i-stat Instrument Validation Log. Barcode Scanning To scan a barcode Hold the analyzer approximately 3-12 inches and at a 10 degree angle from the barcode to be scanned. Press and hold down the Scan key to start the barcode scanner. 8
9 When the analyzer accepts the barcode, it will beep in acknowledgment and automatically turn off the beam. The beam will also turn off after 3 seconds. You may view the data that scanned on the analyzer After viewing the data, release the Scan key. The meter contains a laser. DO NOT stare into the laser light or point it toward anyone. Calculations The i-stat analyzer contains a microprocessor that performs all calculations required for reporting results. Reporting results The handheld analyzer will display test results once the cartridge has been unlocked and the Cartridge Locked prompt disappears. Results display for 2 minutes. Recall results to the display screen by pressing the Menu key. For dark units where it is difficult to view the display, pressing and holding the 0 (zero) key will turn the backlight on. A. Suppressed Results The i-stat will not display results under three conditions: 1. Results outside of the system s reportable ranges are flagged with a < (less than) or > (greater than) indicating that the result is below the lower limit or above the upper limit of the reportable range respectively. See Analytical Range under Reference Ranges for these values. If a flag of < (less than) or > (greater than) occurs, SEND A SPECIMEN TO THE CLINICAL LABORATORY FOR ANALYSIS. Action: Follow unit protocol for critical results. 2. A result that is flagged with *** means that: a. There is an interfering substance in the sample. b. An individual sensor for that test has been compromised. c. This particular test is a calculated result that depends on the results of another test that has ***. d. The first time *** appears when a sample is tested, retest the sample using a new cartridge (certain tests such as ACTk and PT/INR require fresh samples). e. If *** appear again when the sample is tested a second time on the i-stat SEND A SPECIMEN TO THE CLINICAL LABORATORY FOR ANALYSIS. f. If *** reappears on multiple patient samples, call Point of Care Testing for assistance. 3. Results will not be reported if a test cycle has a problem with the sample, calibrant solution, sensors, mechanical, or electrical functions of the analyzer. Action: Take the action displayed with the message that identifies the problem. Refer to the i-stat system manual s troubleshooting section if necessary. Use a backup analyzer if necessary. B. Transmitting Results to the Electronic Medical Record 1. Place the analyzer in the Downloader. The Power light must be green and the blue proximity light will turn on automatically. When properly aligned, all unsent results will be automatically transmitted. The analyzer does NOT need to be turned on. The message Communication in progress is displayed. Verify that the display is turned off before removing from Downloader. 2. If unable to resolve data transmission issues, notify the Point of Care Testing Program. mghpoctcoordinators, pager: Preventive Maintenance A. Rechargeable battery: A nickel-metal-hydride (NiMH) rechargeable battery powers the analyzer. The battery recharges when the analyzer is placed in a Downloader/Recharger. The battery pack can also be removed from the analyzer and placed in the separate recharging compartment on the Downloader/Recharger. Full recharge from a discharged state takes approximately 40 hours. The analyzer will display Low Battery when battery recharge is needed. Spare batteries may be acquired from the POCT program staff. B. Disinfect exterior of analyzer between each patient with hospital-approved disinfectant, e.g. Sani wipe cloths or Virex 256. C. CLEW/JAMS software updates: Software updates performed twice per year re-establishes standardization values and incorporates refinements to the internal quality monitoring system. External Quality Control and the Thermal Probe Check are performed along with the CLEW update. The POCT Program will ensure CLEW updates are implemented prior to software expiration. 9
10 Instrument Replacement Policy A. The replacement instrument policy applies to the following situations: 1. Any malfunction of the instrument 2. Any new instrument 3. Any major maintenance B. The POCT program will perform the following before the replacement instrument is installed: 1. External Simulator (Refer to the procedure for external Simulator) 2. Thermal probe check (Refer to the procedure for Thermal probe check) 3. CAL VER (Refer to the procedure for performing CAL VER) 4. Liquid Quality control (Refer to the procedure for performing liquid controls) 5. Run liquid QC, internal QC and external simulator for 10 days (on analyzers used for non-waived testing) 6. Document all the results on the Instrument Validation Log 7. Inform the POCT sites regarding the replacement of the instrument. 8. All the reports must be approved and signed by the Medical Director or designee. Connectivity and LIS / HIS Down Time Procedure - OR 10
11 11
12 Connectivity and LIS / HIS Down Time Procedure - Imaging 12
13 Troubleshooting A. Analyzer: 1. No display: Either if the display screen remains blank, after a cartridge has been properly inserted or after the On/Off key has been pressed, the batteries should be replaced. 2. Cartridge Locked: Cartridge Locked appears on the screen during the testing cycle to indicate that the cartridge or simulator is locked in the analyzer and should not be removed. A cartridge or simulator must be removed only after the Cartridge Locked prompt disappears from the screen. Normally the analyzer will reset and release the cartridge after the testing cycle is completed. If the analyzer cannot reset, the Cartridge Locked prompt will remain on the screen. If this occurs, wait until the analyzer deactivates (display screen blank) and press the On/Off key. The analyzer will try to reset. If the Cartridge Locked prompt does not disappear, do not attempt to remove the cartridge. Contact the Point of Care Testing program: mghpoctcoordinators, pager: Low Battery: Recharge battery in Downloader/Recharge or swap with extra rechargeable battery. 4. Electronic simulator fail will appear if the analyzer has not successfully completed the electronic simulator test. Refer to ELECTRONIC QUALITY CONTROL section. 5. CLEW expiring, Upgrade required, Point of Care Testing would need to perform a software update. 6. Messages and Quality Check Codes: If a problem is detected during a testing cycle, the cycle will be stopped and a message box will appear on the screen. The messages will identify the code number. Refer to i-stat s technical bulletin(s) to determine the meaning of the code number and the suggested action. If the analyzer deactivates before the detected problem is addressed, the message box will reappear the next time the On/Off key is pressed. Document all problems on the Instrument Corrective Action Log and notify Point of Care Testing. Temperature out of Range error message: The analyzer must be moved to an area where the temperature is between C. Equilibration can take up to 30 minutes. Other error messages: Refer to the i-stat System Manual s Troubleshooting section for more information. 7. i-stat Dropped: Run simulator prior to patient testing. 8. Power Outage or Disaster scenario: Adaptors are available from the POCT program to allow i-stat to run on regular 9V batteries. Contact the POCT program for assistance. B. Cartridge: *** Instead of Results: 1. Test the patient specimen with a new cartridge. If *** reappears, send the sample to the Clinical Laboratory for analysis. The sample may contain a substance that interferes with the test. 2. If *** are obtained for the same test performed on an additional (different) patient, contact Point of Care Testing for assistance: mghpoctcoordinators, pager: (This problem may have been caused by improper cartridge storage). Technical support may be contacted 24 hours x 7 days at Alternative method Should the i-stat System become inoperable for any reason, specimens should be collected and submitted to the laboratory in accordance with the Laboratory Procedure Manual. References A. i-stat1 System Manual, i-stat Corporation, Princeton, N.J., 06/01/01. B. Gornall, A.G.: Applied biochemistry of clinical disorders, Chapter 6, Respiratory Disorders, p. 94, C. Gradwohl s Blood gas analysis and acid-base balance: Principles & Techniques, Chapter 17, p. 351, Fleisher & Schwartz. D. Pesce, A. and Kaplan, Methods in Clinical Chemistry, C.V. Mosby Co., St. Louis, MO, E. Tietz, Norbert W., Editor, Fundamentals of Clinical Chemistry, W.B. Saunders Co., Philadelphia, PA,
14 Reference Ranges The tested ranges are those ranges that were tested during functional sensitivity and linearity testing. Test Reference Range Critical Value Range (Approved by Med Poll Committee)* Analytical Range Calcium, ionized mmol/l <0.8 or >1.54 mmol/l PCO2 (arterial, venous, mix, capillary) mmhg ph (arterial, venous, mix, capillary) PO2 (arterial, venous, mix, capillary) mmhg Art: 14D, Art: Ven: Mix: Cap: Art: Ven: Mix: Cap: Art: 0-14 D: Art: >14 D: Mix: Ven: Cap: <20 or >75 mmhg, first only (within past 24 hours) <7.10 or >7.59 units, first only (within past 24 hours) <40 mmhg Glucose (Adult) mg/dl <50 or > Glucose, plasma (newborn) mg/dl <40 or >500 mg/dl Potassium Adult: mmol/l <1 mo: mmol/l <2.8 or >6.0 mmol/l 2-9 Sodium mmol/l <120 or >160 mmol/l Lactate mmol/l None TCO2 (calculated) HCO3 (calculated) Adult: mmol/l 14 days-1 yr: mmol/l <14 days: mmol/l > 1 year: mmol/l 14 days-1 yr: mmol/l 0-14 days: mmol/l <11.0 or >40.0 None BE (calculated) None None (-30) - (+30) SO2 (calculated) None None PT/INR PT sec (age 6 months to adult); PT-INR values for Warfarin Anti-Coag Therapy: Standard Intensity ; High Intensity EP Lab: Cardio aversion INR >2.0 All other EP procedures <3.5 Cath Lab: <1.5 Internal jugular approach <1.7 Femoral approach <2.0 Radial approach INR >5 POCT INR >5 Core Lab Troponin I Negative Borderline or positive samples reflex to the core laboratory for additional testing Creatinine mg/dl <10 yr: mg/dl None
15 *Clinical policy and Procedure Manual Laboratory Results: Guidelines for Retrieving and Reporting. Addressograph Patient Activated Clotting Time Target Ranges The Institution's Medical Staff believe Reference Ranges are not appropriate for Activated Clotting Time (ACT), instead Target Values or Ranges that vary with procedures, protocols. In some cases, physician clinical preferences may be appropriate. The following table provides guidelines that have been established by site Medical Directors and staff and is intended to take the place of Reference Ranges. ACT ranges are for heparin unless otherwise specified. Location Neuro-Radiology EP laboratory Respiratory: Catheterization Lab Cardiac Surgery: Qualifier or Description Target Range is patient-specific and subject to physician s discretion during the case. The Target Range is determined for each patient in the doctor s order. The Target Range is procedure and patient-specific. Interventional Catheterizations: Patients undergoing Diagnostic Catheterizations Target ranges may vary with procedure. Typical Target Range Used at MGH times the baseline value seconds seconds with an upper limit of 240 seconds (upper limit 230) for patients on platelet G2b-3a inhibitors and (upper limit 240) for patients off platelet G2b-3a inhibitors Patient will receive units heparin, regardless of ACT level. Baseline: seconds Therapeutic heparin drip: On Cardiopulmonary bypass regardless of the surgical procedure: Off Cardiopulmonary bypass CABG: Therapeutic bivalirudin for CPB: seconds (or control aptt seconds to convert to an ACT value) >450 seconds >400 seconds Initial ACT: >400 seconds To remain in the Medical Record Reviewed by: K Lewandrowski, MD Date: 2/2/10 15
16 ACT (Kaolin) Cartridge Procedure The Activated Clotting Time (ACT) is a measure of the time required for complete activation of the coagulation cascade. The endpoint is indicated by the conversion of a thrombin substrate other than fibrinogen and an electrochemical sensor is used to indicate that conversion. The ACT is primarily used to monitor a patient s state of anticoagulation due to heparin administered during a medical or surgical procedure (e.g. cardiac catheterization, renal dialysis, Percutaneous Transluminal Coronary Angioplasty). Specimen Collection Suitable Specimens for ACT: Fresh whole blood (venous or arterial) without anticoagulant collected in a plastic syringe properly labeled with the patient name, date of birth, or medical record number. If from an in-dwelling line, flush the line with 5 ml saline and discard the first 5 ml of blood or three to six dead space volumes of the catheter. Fresh whole blood (venous or arterial) collected in a plastic tube properly labeled with the patient name, date of birth, or medical record number without anticoagulant, clot activators, or serum separators. Device used to transfer sample to cartridge must be plastic. If a repeat measurement is needed, a fresh sample must be obtained Criteria for Specimen Rejection: Evidence of clotting Other sample types such as urine, CSF and pleural fluid Specimen collected in a glass syringe or tube or with anticoagulant of any kind NOTE: Avoid the Following Circumstances Drawing a specimen from an arm with an I.V Stasis (tourniquet left on longer than one minute before venipuncture) Extra muscle activity (fist pumping) Hemolysis (alcohol left over puncture site or a traumatic draw) Icing before filling cartridge Time delays before filling cartridge Reagent Storage Requirements Verification of Cartridge Storage Conditions during Shipment On receipt of new cartridges, verify that the transit temperatures were satisfactory using the fourwindow temperature indicator strip included with the cartridge boxes. Read the temperature strip immediately since it will change with exposure to room temperature. Record observations on the Record of Receipt that comes with each box and attach the receipt with strip in the space shown on the Record of Receipt /QC Documentation Log. Perform liquid QC on the cartridges and document results on the Record of Receipt /QC Documentation Log. A. Refrigerated Cartridges Store at 2-8 C. Do not allow cartridges to freeze. Verify that the cartridges stored in the refrigerator are all within the expiration date printed on the boxes. Do not use after expiration date. Verify that the refrigerator did not exceed the limits of 2 to 8 C (35 to 46 F). Record the temperature of refrigerator on temperature log sheet. Cartridges must remain in pouches until time of use. Do not use cartridge if pouch has been punctured. Individual cartridges may be used after standing five minutes at room temperature. An entire box of cartridges should stand at room temperature for one hour. Remedial Action: If the temperature is outside the range of 2 to 8 C (35 to 46 F), quarantine the cartridges in the storage refrigerator. Notify the Site Coordinator of the temperature failure. 16
17 DO NOT USE the cartridges from this refrigerator. B. Room Temperature Cartridges: Cartridges at room temperature 18 to 30 C (64 to 86 F) are good for 14 days. Mark the room temperature expiration date on each cartridge. Do not return cartridges to the refrigerator once they have been at room temperature. Record the daily room temperature on temperature log sheet Return any cartridges that are beyond the 14-day room temperature stability to the site coordinator for tracking purposes. C. i-stat ACT Liquid Controls, Levels 1 and 2 Store at 2 to 8 C. Do not use after expiration date on box and ampoules. Record date and time removed from refrigeration. Control solutions may be stored at room temperature for up to 4 hours. If left out longer than 4 hours at room temperature, they should be discarded. Competency Assessment All operators must read the procedure manual and complete the Operator Training Checklist after initial training. The competency assessment process is done following initial training, after six months during the first year, then annually thereafter. Competency is assessed using six methods, examples of which are below: 1. Successful performance of routine patient testing, verified by direct observation 2. Supervisor monitoring of the recording and reporting of test results 3. Supervisor review of intermediate test results, QC, proficiency tests, and preventative maintenance performance 4. Successful performance of instrument maintenance function checks and calibration, verified by direct observation 5. Testing previously analyzed samples, proficiency testing samples, internal blind testing samples 6. Assessment of problem-solving skills Quality Control Prior to performing quality control, determine if additional preparation is required. Liquid Control preparation: ACT Coagulation Control Level 1 and Level 2 1. i-stat ACT controls are contained in 6-ml vials. Separate 6 ml vials contain 103 ml of calcium chloride solution for reconstitution. 2. Prior to testing, vials containing the lyophilized plasma and CaCl 2 reconstituting fluid should stand at room temperature for a minimum of 45 minutes. 3. Reconstitute only one level of control plasma at a time. CONTROL SOLUTIONS MUST BE USED IMMEDIATELY (less than 30 seconds) AFTER COMPLETING THE RECONSTITUTION AND MIXING STEPS. Pour the entire contents of the calcium chloride vial into the lyophilized human plasma control vial. 4. Allow the vial to sit at room temperature for 1 minute 5. Mix the contents by swirling gently for 1 minute, then inverting slowly for 30 seconds. 6. Visually inspect the control vial to ensure that the sample is fully reconstituted. If not, discard the reconstituted fluid and start over with fresh vials. 7. Using a plastic transfer pipette, plastic syringe, or plastic capillary tube with no anticoagulant, immediately transfer the solution from the vial into the ACT cartridge. NOTE: additional ACT cartridges may be tested with the remaining fluid if used within 30 seconds of complete reconstitution of the sample. Running the controls: 1. Put on gloves. 2. Press the On/Off key 3. Press the Menu key 4. Press 3 to select Quality Tests. NOTE: Always remember to analyze control materials in the Control pathway under the Quality Tests option of the i-stat 1 Analyzer Administration Menu. Do not analyze controls under the 17
18 Patient Test pathway. This must be done before inserting the test cartridge into the analyzer. The analyzer allows 15 minutes to insert the cartridge after the last keystroke. 5. Press 1 to select Control. 6. Press Scan to scan Operator ID 7. Press Scan to scan Control Lot number 8. Press Scan to scan the cartridge lot number from the box or manually enter the number using the keypad and press Enter. 9. Fill cartridge with the control (see below). Insert cartridge. 10. Enter 1 for i-stat Level 1. Enter 2 for i-stat Level Results will appear. At the bottom of one of the result pages, you will see 1- Test Options Select You will now have the following options: 1- Next level 2- Repeat level 3- History Control Evaluation: Using these options will allow you to continue your Quality Control testing without having to start again at the top of the QC menu. 1. Document results on the Record of Receipt /QC Documentation Log and compare results to the ranges to determine acceptability. 2. The operator performing the quality controls is responsible for evaluating the controls and performing any necessary corrective actions. If the results are out of range, corrective action must be documented on the Record of Receipt /QC Documentation Log. 3. If all results are within expected ranges, use the cartridges as needed. Transmit the results when finished. 4. The result statistics will be reviewed monthly by the Medical director or Designee. Quality Control Corrective Action: 1. If any liquid control result is unacceptable, patient testing can not be performed until the problem has been resolved. Use another analyzer or send the specimen to the Clinical Laboratory. 2. Repeat any out of range control, verifying that the control procedure above has been followed carefully. 3. Document all the results and corrective actions on Record of Receipt /QC Documentation Log. 4. If new control solutions fail a second time, analyzer, control solutions and cartridges should be pulled from use and the POCT program notified mghpoctcoordinators, pager: An investigation will be done to determine the cause of failure. Testing Procedure 1. Follow hand hygiene protocol and put on gloves. 2. Turn the analyzer on and press 2 for i-stat Cartridge. 3. Scan or enter the operator ID and patient CSN. Repeat if prompted. 4. Remove the cartridge from its pouch. Avoid touching the contact pads or exerting pressure over the calibrant pack in the center of the cartridge. 5. Following thorough mixing of the sample, direct the dispensing tip or capillary tube containing the blood into the sample well and dispense the sample until it reaches the fill mark on the cartridge and the well is about half full. 6. Close the cover over the sample well until it snaps into place. (Do not press over the sample well.) 7. Insert the cartridge into the cartridge port until it clicks into place. When using an ACT cartridge, the analyzer must remain horizontal during the testing cycle. 8. Select tests to be reported. 9. Enter additional parameters on the Chart page if required: Choose the number corresponding to the type of sample used when prompted at the Sample Type field. Press the key to return to the results page. 10. View results shown on the analyzer s display screen. 18
19 11. Remove the cartridge after Cartridge Locked message disappears. The analyzer is ready for the next test. 12. Remove gloves and perform hand hygiene. Documentation Dock meter after each test performed to transmit results. During network downtime, results are held in analyzer until they can be transmitted to patients electronic medical record. 19
20 CG8+, CG4+, and G3+ Cartridges Procedure The CG8+ cartridge is designed to directly measure glucose, sodium, potassium, ionized calcium, Hematocrit, ph, pco 2, and po 2, while calculating values for hemoglobin, TCO 2, HCO 3, BE and so 2. The CG4+ cartridge directly measures ph, pco 2, and po 2, and lactate and calculates values for TCO 2, HCO 3, BE and so 2. The G3+ is similar to the CG4+, except that lactate is not measured. Sodium, Potassium, Ionized Calcium, ph, and pco 2 These analytes are measured potentiometrically by ion-selective electrode. Concentrations are calculated from the measured potential through the Nernst equation. 1. Sodium and potassium test results are important in the diagnosis and treatment of patients suffering from hypertension, renal failure or impairment, cardiac distress, disorientation, dehydration, nausea and diarrhea. 2. Ionized calcium is the biologically active fraction of calcium. Through its role in a number of enzymatic reactions and in membrane transport mechanisms, ionized calcium is vitally important in blood coagulation, nerve conduction, and neuromuscular transmission and in muscle contraction. Measurements of ionized calcium may be particularly useful under these clinical conditions: transfusion of citrated blood, liver transplantation, open-heart surgery, neonatal hypocalcaemia, renal disease, hyperparathyroidism, malignancy, hypertension and pancreatitis. 3. ph is an index of the acidity or alkalinity of the blood. 4. pco 2, along with ph, is used to assess acid-base balance. pco 2 is the respiratory component of acid-base balance. pco 2 represents the balance between cellular production of CO 2 and ventilatory removal of CO 2. Causes of primary respiratory acidosis (increase in pco 2 ) are airway obstruction, sedatives and anesthetics, respiratory distress syndrome, and chronic obstructive pulmonary disease. Causes of primary metabolic acidosis are ketoacidosis, lactate acidosis and diarrhea. Causes of primary respiratory alkalosis (decrease in pco2) are hypoxia due to chronic heart failure, edema and neurological disorders, and mechanical hyperventilation. Causes of primary metabolic alkalosis are vomiting and antacid treatment. 5. po 2, a measurement of the pressure of oxygen dissolved in the blood, is measured amperometrically. The oxygen permeates through a gas permeable membrane from the sample into an internal electrolyte solution where it is reduced at the cathode. The oxygen reduction current is proportional to the dissolved oxygen concentration. Decreased po 2 may be caused by ventilation problems or by alteration in the flow of blood within the heart or lungs. 6. Glucose is measured amperometrically. Hydrogen peroxide, produced by the oxidation of glucose, is oxidized at an electrode to produce an electric current proportional to the glucose concentration. Glucose is the primary source of energy for the body and the only source of energy for brain tissue. Measurements of blood glucose levels are important for identification of both hypo- and hyperglycemia, as well as for managing patient treatment to maintain glucose within designated limits. 7. Lactate is measured amperometrically. The enzyme lactate oxidase, immobilized in the lactate biosensor, selectively converts lactate to pyruvate and hydrogen peroxide. The liberated hydrogen peroxide is oxidized by the platinum electrode to produce a current that is proportional to the sample concentration. Elevated levels of lactate are mainly found in conditions of hypoxia such as shock and hypovolumia; in conditions associated with diseases such as diabetes mellitus, neoplasia, and liver disease. (The i-stat will not be used for Hematocrit and/or hemoglobin determinations) Specimen Collection Suitable Specimens for Cartridges for Blood Gases, Electrolytes, and Chemistries: Fresh whole blood collected in a plain capillary collection tube or capillary collection tube balanced with heparin Fresh whole blood collected in a collection tube with lithium or sodium heparin. Fill tube to capacity Fresh whole blood collected in a plain plastic syringe or in a blood gas syringe. Criteria for Specimen Rejection: Evidence of clotting Specimens collected in vacuum tubes with anticoagulant other than lithium or sodium heparin Syringe for ph, PCO2 and PO2 with air bubbles in sample Incompletely filled vacuum tube for the measurement of ionized calcium 20
21 Other sample types such as urine, CSF and pleural fluid NOTE: Avoid the Following Circumstances Drawing a specimen from an arm with an I.V Stasis (tourniquet left on longer than one minute before venipuncture) Extra muscle activity (fist pumping) Hemolysis (alcohol left over puncture site or a traumatic draw) Icing before filling cartridge Time delays before filling cartridge Exposing the sample to air when measuring ph, PCO2 and PO2 Reagent Storage Requirements Verification of Cartridge Storage Conditions during Shipment On receipt of new cartridges, verify that the transit temperatures were satisfactory using the fourwindow temperature indicator strip included with the cartridge boxes. Read the temperature strip immediately since it will change with exposure to room temperature. Record observations on the Record of Receipt /QC Documentation Log that comes with each box and attach the receipt with strip, in the space shown on the log. Perform liquid QC on the cartridges and document results on the Record of Receipt /QC Documentation Log. A. Refrigerated cartridges Store at 2-8 C.Do not allow cartridges to freeze. Verify that the cartridges stored in the refrigerator are all within the expiration date printed on the boxes. Do not use after expiration date. Verify that the refrigerator did not exceed the limits of 2 to 8 C (35 to 46 F). Record the temperature of refrigerator on temperature log sheet. Cartridges must remain in pouches until time of use. Do not use cartridge if pouch has been punctured. Individual cartridges may be used after standing five minutes at room temperature. An entire box of cartridges should stand at room temperature for one Remedial Action: If the temperature is outside the range of 2 to 8 C (35 to 46 F), quarantine the cartridges in the storage refrigerator. Notify the Site Coordinator of the temperature failure. DO NOT USE the cartridges from this refrigerator. B. Room temperature cartridges: Cartridges at room temperature 18 to 30 C (64 to 86 F) are good for 2 months. Mark the room temperature expiration date on each cartridge. Do not return cartridges to the refrigerator once they have been at room temperature. Record the daily room temperature on temperature log sheet Return any cartridges that are beyond the 2 month room temperature stability to the site coordinator for tracking purposes. C. i-stat Aqueous Liquid Controls, Levels 1, 2 and 3 Store at 2 to 8 C. Do not use after expiration date on box and ampoules. Aqueous liquid controls used for oxygen measurement must stand at room temperature a minimum of 4 hours before use. Controls used for all other analytes must equilibrate for 30 minutes at room temperature. Record date and time removed from refrigeration. Aqueous liquid controls expire 5 days after removal from refrigeration. Competency Assessment All operators must read the procedure manual and complete the Operator Training Checklist after initial training. For ACT, Blood Gases, and Lactate, the competency assessment process is done following initial training, after 6 months during the first year, then annually thereafter. 21
22 Competency is assessed using six methods, examples of which are below: 1. Successful performance of routine patient testing, verified by direct observation 2. Supervisor monitoring of the recording and reporting of test results 3. Supervisor review of intermediate test results, QC, proficiency tests, and preventative maintenance performance 4. Successful performance of instrument maintenance function checks and calibration, verified by direct observation 5. Testing previously analyzed samples, proficiency testing samples, or internal blind testing samples. 6. Assessment of problem-solving skills Quality Control Prior to performing quality control, determine if additional preparation is required. i-stat Aqueous Liquid Controls: (For G3+, CG8+, CG4+) 1. Aqueous liquid controls require different temperature stabilization times depending on whether or not oxygen is to be measured. If oxygen is to be measured, equilibrate the ampoule for 4 hours. If not, equilibrate the ampoule for approximately 30 minutes at room temperature. 2. Hold the ampoule at the top, bottom (with forefinger and thumb), and shake times (about 10 seconds) to mix the solution. Tap the ampoule to restore the liquid to the bottom of the ampoule. 3. Open the ampoule by snapping off the tip. Protect fingers with gauze or use an ampoule breaker. 4. Immediately transfer control to syringe as follows: Use a clean 3 ml syringe. Replace attached needle with a 19-gauge blunt tip needle. 5. Aspirate the control from the ampoule into the syringe. Be careful that air is not drawn in with the liquid. Expel one or two drops of liquid before filling the cartridge. If desired, you may detach the blunt tip needle before filling the cartridge. 6. Immediately transfer the solution into a cartridge. 7. Immediately seal the cartridge and insert it into an analyzer. 8. Do not use the solution left in a syringe or ampoule for additional testing of cartridges that contain sensors for ionized calcium, ph, PCO 2, or PO 2. Open a new ampoule. Running the controls: 1. Put on gloves. 2. Press the On/Off key 3. Press the Menu key 4. Press 3 to select Quality Tests. NOTE: Always remember to analyze control materials in the Control pathway under the Quality Tests option of the i-stat 1 Analyzer Administration Menu. Do not analyze controls under the Patient Test pathway. This must be done before inserting the test cartridge into the analyzer. The analyzer allows 15 minutes to insert the cartridge after the last keystroke. 5. Press 1 to select Control. 6. Press Scan to scan Operator ID 7. Press Scan to scan Control Lot number 8. Press Scan to scan the cartridge lot number from the box or manually enter the number using the keypad and press Enter. 9. Fill cartridge with the control (see below). Insert cartridge. 10. Enter 1 for i-stat Level 1. Enter 2 for i-stat Level Results will appear. At the bottom of one of the result pages, you will see 1- Test Options Select You will now have the following options: 1- Next level 2- Repeat level 3- History Control Evaluation: Using these options will allow you to continue your Quality Control testing without having to start again at the top of the QC menu. 22
23 1. Document results on the Record of Receipt /QC Documentation Log and compare results to the ranges to determine acceptability. 2. The operator performing the quality controls is responsible for evaluating the controls and performing any necessary corrective actions. If the results are out of range, corrective action must be documented on the Record of Receipt /QC Documentation Log. 3. If all results are within expected ranges, use the cartridges as needed. Transmit the results when finished. 4. The result statistics will be reviewed monthly by the Medical director or Designee. Quality Control Corrective Action: 1. If any liquid control result is unacceptable, patient testing can not be performed until the problem has been resolved. Use another analyzer or send the specimen to the Clinical Laboratory. 2. Repeat any out of range control, verifying that the control procedure above has been followed carefully. 3. Document all the results and corrective actions on the Record of Receipt /QC Documentation Log. 4. If new control solutions fail a second time, analyzer, control solutions and cartridges should be pulled from use and the POCT program notified - mghpoctcoordinators, pager: An investigation will be done to determine the cause of failure. Testing Procedure 1. Follow hand hygiene protocol and put on gloves. 2. Turn the analyzer on and press 2 for i-stat Cartridge. 3. Scan or enter the operator ID and patient s CSN. Repeat if prompted. 4. Remove the cartridge from its pouch. Avoid touching the contact pads or exerting pressure over the calibrant pack in the center of the cartridge. 5. Following thorough mixing of the sample, direct the dispensing tip or capillary tube containing the blood into the sample well and dispense the sample until it reaches the fill mark on the cartridge and the well is about half full. 6. Close the cover over the sample well until it snaps into place. (Do not press over the sample well.) 7. Insert the cartridge into the cartridge port until it clicks into place. When using an ACT cartridge, the analyzer must remain horizontal during the testing cycle. 8. Select tests to be reported. 9. Enter additional parameters on the Chart page if required: Choose the number corresponding to the type of sample used when prompted at the Sample Type field. Patient temperature can be entered as degrees Centigrade or Fahrenheit FIO 2 can be entered as the numbers of liters or as a percentage of oxygen a patient is receiving Press the key to return to the results page 10. View results shown on the analyzer s display screen. 11. Remove the cartridge after Cartridge Locked message disappears. The analyzer is ready for the next test. 12. Remove gloves and perform hand hygiene. Documentation Dock meter after each test performed to transmit results. During network downtime, results are held in analyzer until they can be transmitted to patients electronic medical record. 23
24 Creatinine Cartridge Procedure Creatinine is measured amperometrically. Hydrogen peroxide, which is produced through various enzymatic reactions within the cartridge, is oxidized at the platinum electrode to produce a current which is proportional to the sample creatinine concentration. Elevated levels of creatinine are mainly associated with abnormal renal function and occur whenever there is a significant reduction in glomerular filtration rate or when urine elimination is obstructed. Specimen Collection Suitable Specimens for measuring creatinine: Venous whole blood collected in a collection tube with lithium or sodium heparin. Fill tube to capacity Venous whole blood collected in a plain plastic syringe or in a blood gas syringe. Criteria for Specimen Rejection: Evidence of clotting Specimens collected in vacuum tubes with anticoagulant other than lithium or sodium heparin Other sample types such as urine, CSF and pleural fluid NOTE: Avoid the Following Circumstances Drawing a specimen from an arm with an I.V Stasis (tourniquet left on longer than one minute before venipuncture) Extra muscle activity (fist pumping) Hemolysis (alcohol left over puncture site or a traumatic draw) Icing before filling cartridge Time delays before filling cartridge Reagent Storage Requirements Verification of Cartridge Storage Conditions during Shipment On receipt of new cartridges, verify that the transit temperatures were satisfactory using the fourwindow temperature indicator strip included with the cartridge boxes. Read the temperature strip immediately since it will change with exposure to room temperature. Record observations on the Record of Receipt that comes with each box and attach the receipt, with strip, in the space shown on the Record of Receipt /QC Documentation Log. Perform liquid QC on the cartridges and document results on the Record of Receipt /QC Documentation Log. A. Refrigerated cartridges Store at 2-8 C. Do not allow cartridges to freeze. Verify that the cartridges stored in the refrigerator are all within the expiration date printed on the boxes. Do not use after expiration date. Verify that the refrigerator did not exceed the limits of 2 to 8 C (35 to 46 F). Record the temperature of refrigerator on temperature log sheet. Cartridges must remain in pouches until time of use. Do not use cartridge if pouch has been punctured. Individual cartridges may be used after standing five minutes at room temperature. An entire box of cartridges should stand at room temperature for one hour. Remedial Action: If the temperature is outside the range of 2 to 8 C (35 to 46 F), quarantine the cartridges in the storage refrigerator. Notify the Site Coordinator of the temperature failure. DO NOT USE the cartridges from this refrigerator. 24
25 B. Room temperature cartridges: Cartridges at room temperature 18 to 30 C (64 to 86 F) are good for 14 days. Mark the roomtemperature expiration date on each cartridge. Do not return cartridges to the refrigerator once they have been at room temperature. Record the daily room temperature on temperature log sheet Return any cartridges that are beyond the 14-day room temperature stability to the site coordinator for tracking purposes. C. i-stat Aqueous Liquid Controls, Levels 1 and 3 Store at 2 to 8 C. Do not use after expiration date on box and ampules. Aqueous liquid controls used for oxygen measurement must stand at room temperature a minimum of 4 hours before use. Controls used for all other analytes must equilibrate for 30 minutes at room temperature. Record date and time removed from refrigeration. Aqueous liquid controls expire 5 days after removal from refrigeration. Competency Assessment All operators must read the procedure manual and complete the Operator Training Checklist after initial training. Competency is assessed at orientation and annually using at least two of the following methods: 1. Performing a test on a blind specimen. 2. Supervisor observes performance of routine work. 3. Each user s quality control performance is monitored. 4. Written testing specific to the method. Quality Control Prior to performing quality control, determine if additional control material preparation is required. i-stat Aqueous Liquid Controls: (For Creat) 1. Aqueous liquid controls require different temperature stabilization times depending on whether or not oxygen is to be measured. If oxygen is to be measured, equilibrate the ampoule for 4 hours. If not, equilibrate the ampoule for approximately 30 minutes at room temperature. 2. Hold the ampoule at the top, bottom (with forefinger and thumb), and shake times (about 10 seconds) to mix the solution. Tap the ampoule to restore the liquid to the bottom of the ampoule. 3. Open the ampoule by snapping off the tip. Protect fingers with gauze or use an ampoule breaker. 4. Aspirate the control from the ampoule into a clean 3 ml syringe, until it is half full. 5. Expel three drops of liquid before filling the cartridge 6. Immediately transfer the solution into a cartridge. 7. Immediately seal the cartridge and insert it into an analyzer. Running the controls: 1. Put on gloves. 2. Press the On/Off key 3. Press the Menu key 4. Press 3 to select Quality Tests. NOTE: Always remember to analyze control materials in the Control pathway under the Quality Tests option of the i-stat 1 Analyzer Administration Menu. Do not analyze controls under the Patient Test pathway. This must be done before inserting the test cartridge into the analyzer. The analyzer allows 15 minutes to insert the cartridge after the last keystroke. 5. Press 1 to select Control. 6. Press Scan to scan Operator ID 7. Press Scan to scan Control Lot number 8. Press Scan to scan the cartridge lot number from the box or manually enter the number using the keypad and press Enter. 9. Fill cartridge with the control (see below). Insert cartridge. 10. Enter 1 for i-stat Level 1. Enter 3 for i-stat Level Results will appear. At the bottom of one of the result pages, you will see 1- Test Options Select 1. 25
26 12. You will now have the following options: 1- Next level 2- Repeat level 3- History Using these options will allow you to continue your Quality Control testing without having to start again at the top of the QC menu. Control Evaluation: 1. Document results on the Record of Receipt /QC Documentation Log and compare results to the ranges to determine acceptability. 2. The operator performing the quality controls is responsible for evaluating the controls and performing any necessary corrective actions. If the results are out of range, corrective action must be documented on the Record of Receipt /QC Documentation Log. 3. If all results are within expected ranges, use the cartridges as needed. Transmit the results when finished. 4. The result statistics will be reviewed monthly by the Medical director or Designee. Quality Control Corrective Action: 1. If any liquid control result is unacceptable, patient testing can not be performed until the problem has been resolved. Use another analyzer or send the specimen to the Clinical Laboratory. 2. Repeat any out of range control, verifying that the control procedure above has been followed carefully. 3. Document all the results and corrective actions on the Record of Receipt /QC Documentation Log 4. If new control solutions fail a second time, analyzer, control solutions and cartridges should be pulled from use and the POCT program notified mghpoctcoordinators, pager: An investigation will be done to determine the cause of failure. Testing Procedure Note: Use only VENOUS blood for Creatinine testing!! 1. Follow hand hygiene protocol and put on gloves. 2. Turn the analyzer on and press 2 for i-stat Cartridge. 3. Scan or enter the operator ID and patient CSN. Repeat if prompted. 4. Remove the cartridge from its pouch. Avoid touching the contact pads or exerting pressure over the calibrant pack in the center of the cartridge. 5. Following thorough mixing of the sample, direct the dispensing tip or capillary tube containing the blood into the sample well and dispense the sample until it reaches the fill mark on the cartridge and the well is about half full. 6. Close the cover over the sample well until it snaps into place. (Do not press over the sample well.) 7. Insert the cartridge into the cartridge port until it clicks into place. 8. Select tests to be reported. 9. Enter additional parameters on the Chart page if required: Choose the number corresponding to the type of sample used when prompted at the Sample Type field. Patient temperature can be entered as degrees Centigrade or Fahrenheit Press the key to return to the results page. 10. View results shown on the analyzer s display screen. 11. Remove the cartridge after Cartridge Locked message disappears. The analyzer is ready for the next test. 12. Remove gloves and perform hand hygiene. Documentation Dock meter after each test performed to transmit results. During network downtime, results are held in analyzer until they can be transmitted to patients electronic medical record. 26
27 PT/INR Cartridge Procedure The i-stat PT/INR test is a whole blood determination of the prothrombin time used for monitoring oral anticoagulant (warfarin) therapy. The test determines the time required for complete activation of the extrinsic pathway of the coagulation cascade when initiated (activated) with a thromboplastin. The PT/INR test result is reported as an International Normalized Ratio (INR) and, optionally, in seconds. The INR is the recommended method of result reporting for monitoring of oral anticoagulant therapy. Specimen Collection Suitable Specimens for PT/INR Fresh whole blood without anticoagulant collected in a plastic syringe or plastic evacuated tube without clot activators or serum separators. Device used to transfer sample to cartridge must be plastic. Fresh capillary whole blood dispensed directly into the cartridge from the finger Criteria for Specimen Rejection Evidence of clotting Specimens collected in glass syringes or tubes or with anticoagulant of any kind Other sample types such as urine, CSF, and pleural fluid NOTE: Avoid the Following Circumstances Drawing a specimen from an arm with an I.V. Stasis (tourniquet left on longer than one minute before venipuncture) Extra muscle activity (fist pumping) Hemolysis (alcohol left over puncture site, or a traumatic draw) Icing before filling cartridge Time delays before filling cartridge Reagent Storage Requirements Verification of Cartridge Storage Conditions during Shipment On receipt of new cartridges, verify that the transit temperatures were satisfactory using the fourwindow temperature indicator strip included with the cartridge boxes. Read the temperature strip immediately since it will change with exposure to room temperature. Record observations on the Record of Receipt that comes with each box and attach the receipt, with strip, in the space shown on the Record of Receipt /QC Documentation Log. Perform liquid QC on the cartridges and document results on the Record of Receipt /QC Documentation Log. A. Refrigerated cartridges Store at 2-8 C. Do not allow cartridges to freeze. Verify that the cartridges stored in the refrigerator are all within the expiration date printed on the boxes. Do not use after expiration date. Verify that the refrigerator did not exceed the limits of 2 to 8 C (35 to 46 F). Record the temperature of refrigerator on temperature log sheet. Cartridges must remain in pouches until time of use. Do not use cartridge if pouch has been punctured. Individual cartridges may be used after standing five minutes at room temperature. An entire box of cartridges should stand at room temperature for one hour. Remedial Action: If the temperature is outside the range of 2 to 8 C (35 to 46 F), quarantine the cartridges in the storage refrigerator. Notify the Site Coordinator of the temperature failure. DO NOT USE the cartridges from this refrigerator. 27
28 B. Room temperature cartridges: Cartridges at room temperature 18 to 30 C (64 to 86 F) are good for 14 days. Mark the roomtemperature expiration date on each cartridge. Do not return cartridges to the refrigerator once they have been at room temperature. Record the daily room temperature on temperature log sheet Return any cartridges that are beyond the 14-day room temperature stability to the site coordinator for tracking purposes. C. i-stat PT/INR Liquid Controls, Levels 1 and 2 Store at 2 to 8 C. Do not use after expiration date on box and ampoules. Record date and time removed from refrigeration. Control solutions may be stored at room temperature for up to 4 hours. If left out longer than 4 hours at room temperature, they should be discarded. Competency Assessment All operators must read the procedure manual and complete the Operator Training Checklist after initial training. For PT/INR, the competency assessment process is done following initial training, after 6 months during the first year, then annually thereafter. Competency is assessed using six methods, examples of which are below: 1. Successful performance of routine patient testing, verified by direct observation 2. Supervisor monitoring of the recording and reporting of test results 3. Supervisor review of intermediate test results, QC, proficiency tests, and preventative maintenance performance 4. Successful performance of instrument maintenance function checks and calibration, verified by direct observation 5. Testing previously analyzed samples, proficiency testing samples, or internal blind testing samples. 6. Assessment of problem-solving skills Quality Control Prior to performing quality control, determine if additional preparation is required. Liquid Control preparation: PT/INR Control Level 1 and Level 2 1. i-stat PT/INR controls are contained in 6-ml vials. Separate 6 ml vials contain 103 ml of calcium chloride solution for reconstitution. 2. Prior to testing, vials containing the lyophilized plasma and CaCl 2 reconstituting fluid should stand at room temperature for a minimum of 45 minutes. 3. Reconstitute only one level of control plasma at a time. CONTROL SOLUTIONS MUST BE USED IMMEDIATELY (less than 30 seconds) AFTER COMPLETING THE RECONSTITUTION AND MIXING STEPS. Pour the entire contents of the calcium chloride vial into the lyophilized human plasma control vial. 4. Allow the vial to sit at room temperature for 1 minute 5. Mix the contents by swirling gently for 1 minute, then inverting slowly for 30 seconds. 6. Visually inspect the control vial to ensure that the sample is fully reconstituted. If not, discard the reconstituted fluid and start over with fresh vials. 7. Using a plastic transfer pipette, plastic syringe, or plastic capillary tube with no anticoagulant, immediately transfer the solution from the vial into the PT/INR cartridge. NOTE: additional PT/INR cartridges may be tested with the remaining fluid if used within 30 seconds of complete reconstitution of the sample. Running the controls: 1. Put on gloves. 2. Press the On/Off key 3. Press the Menu key 4. Press 3 to select Quality Tests. NOTE: Always remember to analyze control materials in the Control pathway under the Quality Tests option of the i-stat 1 Analyzer Administration Menu. Do not analyze controls under the 28
29 Patient Test pathway. This must be done before inserting the test cartridge into the analyzer. The analyzer allows 15 minutes to insert the cartridge after the last keystroke. 5. Press 1 to select Control. 6. Press Scan to scan Operator ID 7. Press Scan to scan Control Lot number 8. Press Scan to scan the cartridge lot number from the box or manually enter the number using 9. the keypad and press Enter. 10. Fill cartridge with the control (see below). Insert cartridge. 11. Enter 1 for i-stat Level 1. Enter 2 for i-stat Level Results will appear. At the bottom of one of the result pages, you will see 1- Test Options 13. Select You will now have the following options: 1- Next level 2- Repeat level 3- History Using these options will allow you to continue your Quality Control testing without having to start again at the top of the QC menu. Control Evaluation: 1. Document results on the Record of Receipt /QC Documentation Log and compare results to the ranges to determine acceptability. 2. The operator performing the quality controls is responsible for evaluating the controls and performing any necessary corrective actions. If the results are out of range, corrective action must be documented on the Record of Receipt /QC Documentation Log. 3. If all results are within expected ranges, use the cartridges as needed. Transmit the results when finished. 4. The result statistics will be reviewed monthly by the Medical director or Designee. Quality Control Corrective Action: 1. If any liquid control result is unacceptable, patient testing can not be performed until the problem has been resolved. Use another analyzer or send the specimen to the Clinical Laboratory. 2. Repeat any out of range control, verifying that the control procedure above has been followed carefully. 3. Document all the results and corrective actions on Record of Receipt /QC Documentation Log 4. If new control solutions fail a second time, analyzer, control solutions and cartridges should be pulled from use and the POCT program notified mghpoctcoordinators, pager: An investigation will be done to determine the cause of failure. Testing Procedure Caution: The i-stat PT/INR cartridge is designed to accept a sample between 20 and 45 micro liters. A single drop of blood from either a finger puncture or as formed at the tip of a syringe will typically be within this range. If a larger volume is delivered to the sample well, use caution when closing the cartridge as excess blood may be expelled from the cartridge. The i-stat PT/INR test can be performed using capillary or venous samples. Finger Stick: 1. Follow hand hygiene protocol and put on gloves. 2. Turn the analyzer on and press 2 for i-stat Cartridge. 3. Scan or enter the operator ID and patient CSN. Repeat if prompted. 4. Remove cartridge from foil pouch and place the cartridge on a flat surface Avoid touching the contact pads or exerting pressure over the calibrant pack in the center of the cartridge. 5. Prepare lancet device and set aside until needed. 6. Clean and prepare the finger to be sampled. Allow finger to dry thoroughly before sampling. 7. Prick the bottom side of the fingertip with the lancet device. 8. Gently squeeze the finger, developing a hanging drop of blood and perform the test with the first drop of blood. Avoid strong repetitive pressure ( milking ) as it may cause hemolysis or tissue fluid contamination of the specimen. 9. Touch the drop of blood against the bottom of the sample well. Once in contact with the sample well, the blood will be drawn into the cartridge. 29
30 10. Apply sample until it reaches the fill mark indicated on the cartridge. 11. Fold the sample closure over the sample well. 12. Press the rounded end of the closure until it snaps into place. 13. Insert the cartridge into the cartridge port until it clicks into place. When using a PT/INR cartridge, the analyzer must remain on a level, vibration-free surface with the display facing up during the testing cycle. 14. Select tests to be reported. 15. Enter additional parameters on the Chart page if required: Choose the number corresponding to the type of sample used when prompted at the Sample Type field. Patient temperature can be entered as degrees Centigrade or Fahrenheit FIO 2 can be entered as the numbers of liters or as a percentage of oxygen a patient is receiving Press the key to return to the results page 16. View results shown on the analyzer s display screen. 17. Remove the cartridge after Cartridge Locked message disappears. The analyzer is ready for the next test. 18. Remove gloves and perform hand hygiene. Venipuncture: Collection technique resulting in good blood flow must be used. The sample for testing should be drawn into a plastic collection device (either a plastic syringe or plastic evacuated tube). The collection device cannot contain anticoagulants such as heparin, EDTA, oxalate, or citrate. The collection device cannot contain clot activators or serum separators. If a second measurement is required, a fresh sample should be obtained. Note: Some experts recommend drawing and discarding a (venous) sample of at least 1.0 ml prior to drawing sample for coagulation testing. 1. Follow hand hygiene protocol and put on gloves. 2. Turn the analyzer on and press 2 for i-stat Cartridge. 3. Scan or enter the operator ID and patient CSN. Repeat if prompted. 4. Remove cartridge from foil pouch and place the cartridge on a flat surface Avoid touching the contact pads or exerting pressure over the calibrant pack in the center of the cartridge. 5. Apply sample until it reaches the fill mark indicated on the cartridge. 6. Fold the sample closure over the sample well. 7. Press the rounded end of the closure until it snaps into place. 8. Insert the cartridge into the cartridge port until it clicks into place. When using a PT/INR cartridge, the analyzer must remain on a level, vibration-free surface with the display facing up during the testing cycle. 9. Select tests to be reported. 10. Enter additional parameters on the Chart page if required: Choose the number corresponding to the type of sample used when prompted at the Sample Type field. Patient temperature can be entered as degrees Centigrade or Fahrenheit FIO 2 can be entered as the numbers of liters or as a percentage of oxygen a patient is receiving Press the key to return to the results page 11. View results shown on the analyzer s display screen. 12. Remove the cartridge after Cartridge Locked message disappears. The analyzer is ready for the next test. 13. Remove gloves and perform hand hygiene. Documentation 30
31 Dock meter after each test performed to transmit results. During network downtime, results are held in analyzer until they can be transmitted to patients electronic medical record. Troponin I Procedure The i-stat ctni test is an in vitro diagnostic test for the quantitative measurement of cardiac troponin I (ctni) in whole blood or plasma samples. Cardiac troponin I measurements can be used as an aid in the diagnosis and treatment of myocardial infarction and in the risk stratification of patients with acute coronary syndromes with respect to their relative risk of mortality. Elevated levels of cardiac-specific troponins convey prognostic information beyond that supplied by the patient s clinical signs and symptoms, the ECG at presentation, and the predischarge exercise test. In addition, the ability of ctni to be measured at the low-end of the concentration range allows therapeutic intervention to be considered at any elevation above the normal range Whole blood comes into contact with a sensor containing troponin-specific antibody and an enzyme conjugate specific to a separate portion of the ctni molecule. The ctni within the patient s sample becomes labeled with the conjugate and captured onto the eletrochemical sensor. A wash phase results in an enzymatic cleaving of the antibody/antigen/antibody sandwich, releasing a detectable electrochemical product. Specimen Collection 31
32 Suitable Specimens for Troponin I/cTnI Fresh heparinized whole blood or plasma samples collected in syringes or evacuated tubes containing lithium or sodium heparin. Collection tubes must be filled at least half full. Non heparinized whole blood samples tested within one minute of patient draw collected into a plastic syringe or plastic evacuated tube containing no additives. Criteria for Specimen Rejection Evidence of clotting The use of whole blood or plasma samples containing other anticoagulants such as EDTA, oxalate, and citrate will cause a in decreased ctni result. Other sample types such as urine, CSF, and pleural fluid Capillary tubes and direct skin punctures (e.g. fingersticks) should not be used with the ctni cartridge Samples should not be used unless the blood collection tube is filled at least half full NOTE: Avoid the Following Circumstances Drawing a specimen from an arm with an I.V Stasis (tourniquet left on longer than one minute before venipuncture) Extra muscle activity (fist pumping) Hemolysis (alcohol left over puncture site or a traumatic draw) Icing before filling cartridge Time delays before filling cartridge Reagent Storage Requirements Verification of Cartridge Storage Conditions during Shipment On receipt of new cartridges, verify that the transit temperatures were satisfactory using the fourwindow temperature indicator strip included with the cartridge boxes. Read the temperature strip immediately since it will change with exposure to room temperature. Record observations on the Record of Receipt that comes with each box and attach the receipt, with strip, in the space shown on the Record of Receipt /QC Documentation Log. Perform liquid QC on the cartridges and document results on the Record of Receipt /QC Documentation Log. A. Refrigerated cartridges Store at 2-8 C. Do not allow cartridges to freeze. Verify that the cartridges stored in the refrigerator are all within the expiration date printed on the boxes. Do not use after expiration date. Verify that the refrigerator did not exceed the limits of 2 to 8 C (35 to 46 F). Record the temperature of refrigerator on temperature log sheet. Cartridges must remain in pouches until time of use. Do not use cartridge if pouch has been punctured. Individual cartridges may be used after standing five minutes at room temperature. An entire box of cartridges should stand at room temperature for one hour. Remedial Action: If the temperature is outside the range of 2 to 8 C (35 to 46 F), quarantine the cartridges in the storage refrigerator. Notify the Site Coordinator of the temperature failure. DO NOT USE the cartridges from this refrigerator. B. Room temperature cartridges: Cartridges at room temperature 18 to 30 C (64 to 86 F) are good for 14 days. Mark the roomtemperature expiration date on each cartridge. Do not return cartridges to the refrigerator once they have been at room temperature. Record the daily room temperature on temperature log sheet Return any cartridges that are beyond the 14-day room temperature stability to the site coordinator for tracking purposes. C. i-stat Cardiac Marker Controls Levels 1, 2, and 3: Store at 18 C (-1 F) in a non-defrosting freezer. After thaw, the opened or 32
33 unopened vial is stable for 4 hours when capped and stored at 2-8 C (35-46 F). Do not re-freeze Competency Assessment All operators must read the procedure manual and complete the Operator Training Checklist after initial training. For ctni, the competency assessment process is done following initial training, after 6 months during the first year, then annually thereafter. Competency is assessed using six methods, examples of which are below: 1. Successful performance of routine patient testing, verified by direct observation 2. Supervisor monitoring of the recording and reporting of test results 3. Supervisor review of intermediate test results, QC, proficiency tests, and preventative maintenance performance 4. Successful performance of instrument maintenance function checks and calibration, verified by direct observation 5. Testing previously analyzed samples, proficiency testing samples, or internal blind testing samples. 6. Assessment of problem-solving skills Quality Control Prior to performing quality control, determine if additional preparation is required. Liquid Control preparation: ctni Control Level 1, 2, or Level 3 1. Remove vial from freezer and thaw at room temperature (18-30 C) for 15 minutes. 2. Thoroughly mix by gently swirling the bottle. Avoid foaming of the sample. Running the controls: 1. Put on gloves. 2. Press the On/Off key 3. Press the Menu key 4. Press 3 to select Quality Tests. NOTE: Always remember to analyze control materials in the Control pathway under the Quality Tests option of the i-stat 1 Analyzer Administration Menu. Do not analyze controls under the Patient Test pathway. This must be done before inserting the test cartridge into the analyzer. The analyzer allows 15 minutes to insert the cartridge after the last keystroke. 5. Press 1 to select Control. 6. Press Scan to scan Operator ID 7. Press Scan to scan Control Lot number 8. Press Scan to scan the cartridge lot number from the box or manually enter the number using 9. the keypad and press Enter. 10. Dispense a drop of sample directly from the vial into the i-stat ctni cartridge and seal the cartridge. Insert cartridge. 11. Enter 1 for i-stat Level 1. Enter 2 for i-stat Level 2, etc. 12. Results will appear. At the bottom of one of the result pages, you will see 1- Test Options 13. Select You will now have the following options: 4- Next level 5- Repeat level 6- History Using these options will allow you to continue your Quality Control testing without having to start again at the top of the QC menu. Control Evaluation: 1. Document results on the Record of Receipt /QC Documentation Log and compare results to the ranges to determine acceptability. 33
34 2. The operator performing the quality controls is responsible for evaluating the controls and performing any necessary corrective actions. If the results are out of range, corrective action must be documented on the Record of Receipt /QC Documentation Log. 3. If all results are within expected ranges, use the cartridges as needed. Transmit the results when finished. 4. The result statistics will be reviewed monthly by the Medical director or Designee. Quality Control Corrective Action: 1. If any liquid control result is unacceptable, patient testing can not be performed until the problem has been resolved. Use another analyzer or send the specimen to the Clinical Laboratory. 2. Repeat any out of range control, verifying that the control procedure above has been followed carefully. 3. Document all the results and corrective actions on Record of Receipt /QC Documentation Log 4. If new control solutions fail a second time, analyzer, control solutions and cartridges should be pulled from use and the POCT program notified mghpoctcoordinators, pager: An investigation will be done to determine the cause of failure Testing Procedure 1. Follow hand hygiene and put on gloves. 2. Turn the analyzer on and press 2 for i-stat Cartridge. 3. Scan or enter the operator ID and patient CSN. Repeat if prompted. 4. Remove the cartridge from its pouch. Avoid touching the contact pads or exerting pressure over the calibrant pack in the center of the cartridge. 5. Following thorough mixing of the sample, direct the dispensing tip or capillary tube containing the blood into the sample well and dispense the sample until it reaches the fill mark on the cartridge and the well is about half full. 6. Close the cover over the sample well until it snaps into place. (Do not press over the sample well.) 7. Insert the cartridge into the cartridge port until it clicks into place. 8. Select tests to be reported. 9. Enter additional parameters on the Chart page if required: Choose the number corresponding to the type of sample used when prompted at the Sample Type field. Patient temperature can be entered as degrees Centigrade or Fahrenheit 11. Press the key to return to the results page. 12. View results shown on the analyzer s display screen. 13. Remove the cartridge after Cartridge Locked message disappears. The analyzer is ready for the next test. 14. Remove gloves and perform hand hygiene. Documentation Dock meter after each test performed to transmit results. During network downtime, results are held in analyzer until they can be transmitted to patients electronic medical record 34
Procedure Manual for the i-stat System
 Procedure Manual for the i-stat System This Procedure Manual is intended to be a template for the Procedure Manual required by CLIA and laboratory accreditation bodies. This Procedure Manual should be
Procedure Manual for the i-stat System This Procedure Manual is intended to be a template for the Procedure Manual required by CLIA and laboratory accreditation bodies. This Procedure Manual should be
Title: Glucose Testing: StatStrip Glucose Meter Page 1 of 6
 Title: Glucose Testing: StatStrip Glucose Meter Page 1 of 6 CentraCare Health (CCH) adopts the following policy/procedure for: St. Cloud Hospital Original: 5/02 Minor Revision: Full Review: 1/15 Replaces:
Title: Glucose Testing: StatStrip Glucose Meter Page 1 of 6 CentraCare Health (CCH) adopts the following policy/procedure for: St. Cloud Hospital Original: 5/02 Minor Revision: Full Review: 1/15 Replaces:
User Guide. Quality Check Messages and Codes (continued) (01)00054749001286. Message Cause Action
 Quality Check Messages and Codes (continued) Message Cause Action i-stat Analyzer Error, Use Electronic Simulator Analyzer Error, See Manual No display Cartridge Locked does not disappear after test cycle
Quality Check Messages and Codes (continued) Message Cause Action i-stat Analyzer Error, Use Electronic Simulator Analyzer Error, See Manual No display Cartridge Locked does not disappear after test cycle
Contents. POCT Program Massachusetts General Hospital - Pathology Service 55 Fruit Street, Boston, MA 02114
 Title: DCA Vantage HgbA1C Procedure Cross References: DCA Vantage HgbA1C Training and Competency Assessment Record DCA Vantage Operator Training Checklist DCA Vantage Maintenance Log DCA Vantage Optical
Title: DCA Vantage HgbA1C Procedure Cross References: DCA Vantage HgbA1C Training and Competency Assessment Record DCA Vantage Operator Training Checklist DCA Vantage Maintenance Log DCA Vantage Optical
A Self-Study Packet for The Johns Hopkins Hospital Point-of-Care Testing Program copyright 2011 Johns Hopkins Hospital All rights reserved
 A Self-Study Packet for The Johns Hopkins Hospital Point-of-Care Testing Program copyright 2011 Johns Hopkins Hospital All rights reserved Overview and Objectives This module provides an introduction to
A Self-Study Packet for The Johns Hopkins Hospital Point-of-Care Testing Program copyright 2011 Johns Hopkins Hospital All rights reserved Overview and Objectives This module provides an introduction to
How To Test For Creatinine
 Creatinine is measured amperometrically. Creatinine is hydrolyzed to creatine in a reaction catalyzed by the enzyme creatinine amidohydrolase. Creatine is then hydrolyzed to sarcosine in a reaction catalyzed
Creatinine is measured amperometrically. Creatinine is hydrolyzed to creatine in a reaction catalyzed by the enzyme creatinine amidohydrolase. Creatine is then hydrolyzed to sarcosine in a reaction catalyzed
PROCEDURE NO. POC.514.01 LBH. Printed copies are for reference only. Please refer to the electronic copy for the latest version.
 Department Of Pathology POC.514.01- Blood Glucose Monitoring Accu-Chek Inform II Procedure-LBH Version# 1 Department PROCEDURE NO. PAGE NO. Point-of-Care Testing POC.514.01 LBH 1 OF 7 Printed copies are
Department Of Pathology POC.514.01- Blood Glucose Monitoring Accu-Chek Inform II Procedure-LBH Version# 1 Department PROCEDURE NO. PAGE NO. Point-of-Care Testing POC.514.01 LBH 1 OF 7 Printed copies are
Title: Fingerstick Glucose by Accu-Chek Inform
 Title: Fingerstick Glucose by Accu-Chek Inform Target Audience: This module is available to aid in assessing competency for all clinical staff who perform fingerstick glucose testing. Contents Instructions...
Title: Fingerstick Glucose by Accu-Chek Inform Target Audience: This module is available to aid in assessing competency for all clinical staff who perform fingerstick glucose testing. Contents Instructions...
Contents. Approved by: Kent Lewandrowski, M.D. 6/1/2005 Written/Updated by: Gino Pagnani Date: 4/3/09
 POCT Program Massachusetts General Hospital - Pathology Service 55 Fruit Street, Boston, MA 02114 Title: Hemoccult Sensa Fecal Occult Blood Procedure Cross References: Hemoccult Sensa Fecal Occult Blood
POCT Program Massachusetts General Hospital - Pathology Service 55 Fruit Street, Boston, MA 02114 Title: Hemoccult Sensa Fecal Occult Blood Procedure Cross References: Hemoccult Sensa Fecal Occult Blood
The Golden Rule of Specimen Collection: The Patient Test Result is Only as Good as the Sample We Get
 The Golden Rule of Specimen Collection: The Patient Test Result is Only as Good as the Sample We Get Jan Frerichs, MLS (ASCP) The University of Iowa [email protected] Importance of Phlebotomist
The Golden Rule of Specimen Collection: The Patient Test Result is Only as Good as the Sample We Get Jan Frerichs, MLS (ASCP) The University of Iowa [email protected] Importance of Phlebotomist
Inform II. Quick Reference Guide. for Healthcare Professionals BLOOD GLUCOSE MONITORING SYSTEM
 Inform II BLOOD GLUCOSE MONITORING SYSTEM Quick Reference Guide for Healthcare Professionals 2 Table of Contents Important... 4 General Information... 6 ACCU-CHEK Inform II Meter...10 How to Perform Patient
Inform II BLOOD GLUCOSE MONITORING SYSTEM Quick Reference Guide for Healthcare Professionals 2 Table of Contents Important... 4 General Information... 6 ACCU-CHEK Inform II Meter...10 How to Perform Patient
Quality Control of the Future: Risk Management and Individual Quality Control Plans (IQCPs)
 Quality Control of the Future: Risk Management and Individual Quality Control Plans (IQCPs) James H. Nichols, PhD, DABCC, FACB Professor of Pathology, Microbiology, and Immunology Medical Director, Clinical
Quality Control of the Future: Risk Management and Individual Quality Control Plans (IQCPs) James H. Nichols, PhD, DABCC, FACB Professor of Pathology, Microbiology, and Immunology Medical Director, Clinical
Biochemistry Validation Form
 Biochemistry Validation Form Method: Piccolo Xpress Chemistry 13 panel Manufacturer: Abaxis Cat no: 400-0029 CE marked: Yes: x No: Location of bench book: X:\Bio\Patricia\Piccollo Xpress evaluation (August
Biochemistry Validation Form Method: Piccolo Xpress Chemistry 13 panel Manufacturer: Abaxis Cat no: 400-0029 CE marked: Yes: x No: Location of bench book: X:\Bio\Patricia\Piccollo Xpress evaluation (August
Collection Guidelines for Routine & Special Coagulation Testing
 Revised May 2010 Collection Guidelines for Routine & Special Coagulation Testing Best samples come from peripheral stick with evacuated tube system 19 to 22 gauge needle (smaller or bigger could cause
Revised May 2010 Collection Guidelines for Routine & Special Coagulation Testing Best samples come from peripheral stick with evacuated tube system 19 to 22 gauge needle (smaller or bigger could cause
HEMATOCRIT/HCT AND CALCULATED HEMOGLOBIN/HB
 HEMATOCRIT/HCT AND CALCULATED HEMOGLOBIN/HB Hematocrit is determined conductometrically. The measured conductivity, after correction for electrolyte concentration, is inversely related to the hematocrit.
HEMATOCRIT/HCT AND CALCULATED HEMOGLOBIN/HB Hematocrit is determined conductometrically. The measured conductivity, after correction for electrolyte concentration, is inversely related to the hematocrit.
Hemoglobin Testing using the Data Management HemoCue Analyzer
 The Johns Hopkins Medical Institutions Hemoglobin Testing using the Data Management HemoCue Analyzer A Self-Study Packet for The Johns Hopkins Hospital Point-of-Care Testing Program Revision: 12/02 copyright
The Johns Hopkins Medical Institutions Hemoglobin Testing using the Data Management HemoCue Analyzer A Self-Study Packet for The Johns Hopkins Hospital Point-of-Care Testing Program Revision: 12/02 copyright
Chapter. Guaiac Screening CHAPTER 4: GUAIAC TESTING SCREENING FOR OCCULT BLOOD. Page 1 of 5 Guaiac 3-5-02.doc 6/24/2005
 Chapter 4 Guaiac Screening CHAPTER 4: GUAIAC TESTING SCREENING FOR OCCULT BLOOD Page 1 of 5 Guaiac 3-5-02.doc 6/24/2005 Procedure: Guaiac Testing Screening for Fecal Occult Blood POLICY: The stool occult
Chapter 4 Guaiac Screening CHAPTER 4: GUAIAC TESTING SCREENING FOR OCCULT BLOOD Page 1 of 5 Guaiac 3-5-02.doc 6/24/2005 Procedure: Guaiac Testing Screening for Fecal Occult Blood POLICY: The stool occult
Acid-Base Balance and the Anion Gap
 Acid-Base Balance and the Anion Gap 1. The body strives for electrical neutrality. a. Cations = Anions b. One of the cations is very special, H +, and its concentration is monitored and regulated very
Acid-Base Balance and the Anion Gap 1. The body strives for electrical neutrality. a. Cations = Anions b. One of the cations is very special, H +, and its concentration is monitored and regulated very
Eileen Whitehead 2010 East Lancashire HC NHS Trust
 Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
STANDARD OPERATING PROCEDURE FOR NOVA STAT STRIP CONNECTIVITY BLOOD GLUCOSE METERS FOR USE IN LEEDS NHS TRUST
 STANDARD OPERATING PROCEDURE FOR NOVA STAT STRIP CONNECTIVITY BLOOD GLUCOSE METERS FOR USE IN LEEDS NHS TRUST This Standard Operating Procedure explains the protocol for measuring blood glucose concentration
STANDARD OPERATING PROCEDURE FOR NOVA STAT STRIP CONNECTIVITY BLOOD GLUCOSE METERS FOR USE IN LEEDS NHS TRUST This Standard Operating Procedure explains the protocol for measuring blood glucose concentration
Textbook: Chapter 12 pages 351-353, Chapter 13 pages 385-388
 EXERCISE 11: BEDSIDE GLUCOSE TESTING Textbook: Chapter 12 pages 351-353, Chapter 13 pages 385-388 Skills: Objectives: 15 points 1. List the limitations of the bedside glucose test procedure. 2. State the
EXERCISE 11: BEDSIDE GLUCOSE TESTING Textbook: Chapter 12 pages 351-353, Chapter 13 pages 385-388 Skills: Objectives: 15 points 1. List the limitations of the bedside glucose test procedure. 2. State the
Introduction 1 The system 1 The meter 2 The display 3 The mode 3 The measurement 4 Coding the meter 4 How to obtain a drop of blood 6 Application of
 Introduction 1 The system 1 The meter 2 The display 3 The mode 3 The measurement 4 Coding the meter 4 How to obtain a drop of blood 6 Application of the blood 7 Procedure to test glucose 7 Procedure to
Introduction 1 The system 1 The meter 2 The display 3 The mode 3 The measurement 4 Coding the meter 4 How to obtain a drop of blood 6 Application of the blood 7 Procedure to test glucose 7 Procedure to
Reference Range: 0.5-1.6 mmol/l (arterial) 0.7-2.1 mmol/l (venous) CPT Code: 83605
 LACTIC ACID Fasting, arterial specimen preferred. Please note whether arterial or venous. 0.5 ml heparinized plasma. Green top or PST must be drawn, placed on ice, and spun within 15 minutes. Immediately
LACTIC ACID Fasting, arterial specimen preferred. Please note whether arterial or venous. 0.5 ml heparinized plasma. Green top or PST must be drawn, placed on ice, and spun within 15 minutes. Immediately
Quality Requirements of a Point of Care Testing Service
 Quality Requirements of a Point of Care Testing Service Adil I. Khan MSc, PhD Assistant Professor of Pathology Director of Point of Care Testing & Clinical Chemistry Laboratory, Temple University Episcopal
Quality Requirements of a Point of Care Testing Service Adil I. Khan MSc, PhD Assistant Professor of Pathology Director of Point of Care Testing & Clinical Chemistry Laboratory, Temple University Episcopal
Inc. Wuhan. Quantity Pre-coated, ready to use 96-well strip plate 1 Plate sealer for 96 wells 4 Standard (liquid) 2
 Uscn Life Science Inc. Wuhan Website: www.uscnk.com Phone: +86 27 84259552 Fax: +86 27 84259551 E-mail: [email protected] ELISA Kit for Human Prostaglandin E1(PG-E1) Instruction manual Cat. No.: E0904Hu
Uscn Life Science Inc. Wuhan Website: www.uscnk.com Phone: +86 27 84259552 Fax: +86 27 84259551 E-mail: [email protected] ELISA Kit for Human Prostaglandin E1(PG-E1) Instruction manual Cat. No.: E0904Hu
VENOUS BLOOD COLLECTION
 Venous Blood Collection p. 1 of 5 Johns Hopkins Medical Laboratories Department of Pathology Core Lab Clinical Services Zd7: Word: JHH Venous Blood Collection Procedure Signature Date Signature Date Written
Venous Blood Collection p. 1 of 5 Johns Hopkins Medical Laboratories Department of Pathology Core Lab Clinical Services Zd7: Word: JHH Venous Blood Collection Procedure Signature Date Signature Date Written
PROCEDURE COVERSHEET. Document Section: CHEMISTRY Author: JOANNE WONG Date Authored: JAN 2011. In Use Date: 2/1/2011 Discontinued Date:
 PROCEDURE COVERSHEET Procedure Title: ph (Urine, Body Fluid, Platelet Samples) Document Section: CHEMISTRY Author: JOANNE WONG Date Authored: JAN 2011 Laboratory Director: TED KURTZ, MD (PARNASSUS & CHINA
PROCEDURE COVERSHEET Procedure Title: ph (Urine, Body Fluid, Platelet Samples) Document Section: CHEMISTRY Author: JOANNE WONG Date Authored: JAN 2011 Laboratory Director: TED KURTZ, MD (PARNASSUS & CHINA
Onboard Quality Controls for the CoaguChek XS System
 Onboard Quality Controls for the CoaguChek XS System The new CoaguChek XS Anticoagulation Monitoring System incorporates a new onboard quality control system that eliminates the need for liquid controls
Onboard Quality Controls for the CoaguChek XS System The new CoaguChek XS Anticoagulation Monitoring System incorporates a new onboard quality control system that eliminates the need for liquid controls
STEP-BY-STEP INSTRUCTIONS FOR INVESTIGATIONAL USE. Rapid HCV Antibody Test FOR ORAQUICK RAPID HCV ANTIBODY TEST
 Before performing testing, all operators MUST read and become familiar with Universal Precautions for Prevention of Transmission of Human Immunodeficiency Virus, Hepatitis B Virus, and other Blood-borne
Before performing testing, all operators MUST read and become familiar with Universal Precautions for Prevention of Transmission of Human Immunodeficiency Virus, Hepatitis B Virus, and other Blood-borne
Rat Creatine Kinase MB isoenzyme,ck-mb ELISA Kit
 Rat Creatine Kinase MB isoenzyme,ck-mb ELISA Kit Catalog No: E0479r 96 Tests Operating instructions www.eiaab.com FOR RESEARCH USE ONLY; NOT FOR THERAPEUTIC OR DIAGNOSTIC APPLICATIONS! PLEASE READ THROUGH
Rat Creatine Kinase MB isoenzyme,ck-mb ELISA Kit Catalog No: E0479r 96 Tests Operating instructions www.eiaab.com FOR RESEARCH USE ONLY; NOT FOR THERAPEUTIC OR DIAGNOSTIC APPLICATIONS! PLEASE READ THROUGH
Abstract... i. Committee Membership... iii. Foreword... vii. 1 Scope... 1. 2 Introduction... 1. 3 Standard Precautions... 1. 4 Definitions...
 Vol. 27 No. 26 Replaces H3-A5 Vol. 23 No. 32 Procedures for the Collection of Diagnostic Blood Specimens by Venipuncture; Approved Standard Sixth Edition This document provides procedures for the collection
Vol. 27 No. 26 Replaces H3-A5 Vol. 23 No. 32 Procedures for the Collection of Diagnostic Blood Specimens by Venipuncture; Approved Standard Sixth Edition This document provides procedures for the collection
CAP Point of Care Checklist Frequently Asked Questions Roger D. Klein, MD Sheldon Campbell, MD, PhD Peter J. Howanitz, MD
 CAP Point of Care Checklist Frequently Asked Questions Roger D. Klein, MD Sheldon Campbell, MD, PhD Peter J. Howanitz, MD TABLE OF CONTENTS Introduction Applicability General Topics Proficiency Testing
CAP Point of Care Checklist Frequently Asked Questions Roger D. Klein, MD Sheldon Campbell, MD, PhD Peter J. Howanitz, MD TABLE OF CONTENTS Introduction Applicability General Topics Proficiency Testing
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!!
 Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Preface. Preface. A Healthcare professional should be contacted when Customer Service is not available.
 Preface Preface Thank you for selecting the GE100 Monitoring System. This manual provides all the information you need to operate this product for accurate test results. Please read the entire manual before
Preface Preface Thank you for selecting the GE100 Monitoring System. This manual provides all the information you need to operate this product for accurate test results. Please read the entire manual before
IgM ELISA. For the quantitative determination of IgM in human serum and plasma. For Research Use Only. Not For Use In Diagnostic Procedures.
 IgM ELISA For the quantitative determination of IgM in human serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Please read carefully due to Critical Changes, e.g., Calibrator
IgM ELISA For the quantitative determination of IgM in human serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Please read carefully due to Critical Changes, e.g., Calibrator
CoaguChek System. XS Plus. User Manual
 CoaguChek System XS Plus User Manual The contents of this manual, including all graphics and photographs, are the property of Roche Diagnostics. No part of this document may be reproduced or transmitted
CoaguChek System XS Plus User Manual The contents of this manual, including all graphics and photographs, are the property of Roche Diagnostics. No part of this document may be reproduced or transmitted
ACID- BASE and ELECTROLYTE BALANCE. MGHS School of EMT-Paramedic Program 2011
 ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
I-140 Venipuncture for Blood Specimen Collection
 I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
Arterial Blood Gas Case Questions and Answers
 Arterial Blood Gas Case Questions and Answers In the space that follows you will find a series of cases that include arterial blood gases. Each case is then followed by an explanation of the acid-base
Arterial Blood Gas Case Questions and Answers In the space that follows you will find a series of cases that include arterial blood gases. Each case is then followed by an explanation of the acid-base
2010 Laboratory Accreditation Program Audioconference. Accreditation Requirements for Waived Vs. Non-waived Tests
 2010 Laboratory Accreditation Program Audioconference Accreditation Requirements for Waived Vs. Non-waived Tests Objectives: After participating in this audioconference you will be able to: Define the
2010 Laboratory Accreditation Program Audioconference Accreditation Requirements for Waived Vs. Non-waived Tests Objectives: After participating in this audioconference you will be able to: Define the
FDA Public Hearing on Clinical Accuracy Requirements for Point of Care Blood Glucose Meters (BGMs)
 FDA Public Hearing on Clinical Accuracy Requirements for Point of Care Blood Glucose Meters (BGMs) Barriers to Overcoming Interferences and Limitations Alan T. Cariski, MD, JD, and Mike Flis, AdvaMed BGM
FDA Public Hearing on Clinical Accuracy Requirements for Point of Care Blood Glucose Meters (BGMs) Barriers to Overcoming Interferences and Limitations Alan T. Cariski, MD, JD, and Mike Flis, AdvaMed BGM
Contents. Abstract... i. Committee Membership... iii. Foreword... vii. 1 Scope... 1. 2 Introduction... 1. 3 Standard Precautions...
 Vol. 28 No. 20 Replaces H47-A Vol. 16 No. 3 One-Stage Prothrombin Time (PT) Test and Activated Partial Thromboplastin Time (APTT) Test; Approved Guideline Second Edition This document provides guidelines
Vol. 28 No. 20 Replaces H47-A Vol. 16 No. 3 One-Stage Prothrombin Time (PT) Test and Activated Partial Thromboplastin Time (APTT) Test; Approved Guideline Second Edition This document provides guidelines
Interpretation of Laboratory Values
 Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Mouse IgM ELISA. Cat. No. KT-407 K-ASSAY. For the quantitative determination of IgM in mouse biological samples. For Research Use Only. 1 Rev.
 K-ASSAY Mouse IgM ELISA For the quantitative determination of IgM in mouse biological samples Cat. No. KT-407 For Research Use Only. 1 Rev. 072309 K-ASSAY PRODUCT INFORMATION Mouse IgM ELISA Cat. No. KT-407
K-ASSAY Mouse IgM ELISA For the quantitative determination of IgM in mouse biological samples Cat. No. KT-407 For Research Use Only. 1 Rev. 072309 K-ASSAY PRODUCT INFORMATION Mouse IgM ELISA Cat. No. KT-407
Managing POCT: Trying to Control Testing in an Out-of-Control Environment. William Clarke, PhD, MBA, DABCC Johns Hopkins School of Medicine 3/24/11
 Managing POCT: Trying to Control Testing in an Out-of-Control Environment William Clarke, PhD, MBA, DABCC Johns Hopkins School of Medicine 3/24/11 Learning Objectives Participants should be able to: Discuss
Managing POCT: Trying to Control Testing in an Out-of-Control Environment William Clarke, PhD, MBA, DABCC Johns Hopkins School of Medicine 3/24/11 Learning Objectives Participants should be able to: Discuss
TOTAL PROTEIN FIBRINOGEN
 UNIT: Proteins 16tproteins.wpd Task Determination of Total Protein, Albumin and Globulins Objectives Upon completion of this exercise, the student will be able to: 1. Explain the ratio of albumin and globulin
UNIT: Proteins 16tproteins.wpd Task Determination of Total Protein, Albumin and Globulins Objectives Upon completion of this exercise, the student will be able to: 1. Explain the ratio of albumin and globulin
Central Line Blood Draw
 Central Line Blood Draw Welcome to the Central Line dressing blood draw refresher. Please use the navigation below to advance to the next page. The Central Line blood draw module is also available as a
Central Line Blood Draw Welcome to the Central Line dressing blood draw refresher. Please use the navigation below to advance to the next page. The Central Line blood draw module is also available as a
Lead Testing and On Site Calibration for Water Testing Detection Range: 2 100ppb
 Document: AND Lead 100 7 2013 Lead Testing and On Site Calibration for Water Testing Detection Range: 2 100ppb July, 2013 Edition 1 ANDalyze, Inc., 2012. All rights reserved. Printed in USA. Table of Contents
Document: AND Lead 100 7 2013 Lead Testing and On Site Calibration for Water Testing Detection Range: 2 100ppb July, 2013 Edition 1 ANDalyze, Inc., 2012. All rights reserved. Printed in USA. Table of Contents
Medications or therapeutic solutions may be injected directly into the bloodstream
 Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
MANITOBA PATIENT SERVICE CENTRE STANDARDS
 MANITOBA PATIENT SERVICE CENTRE STANDARDS February 2015 INTRODUCTION These Standards are derived from Z316.7-12 and are approved by the Council of the College of Physicians and Surgeons of Manitoba. These
MANITOBA PATIENT SERVICE CENTRE STANDARDS February 2015 INTRODUCTION These Standards are derived from Z316.7-12 and are approved by the Council of the College of Physicians and Surgeons of Manitoba. These
Chapter 14 Urinalysis, Body Fluids and Other Specimens. Objectives:
 EXERCISE 15: CHEMICAL EXAMINATION OF URINE Textbook: Skill: Chapter 14 Urinalysis, Body Fluids and Other Specimens 15 points Objectives: 1. Name 10 routine chemical tests performed on urine and list a
EXERCISE 15: CHEMICAL EXAMINATION OF URINE Textbook: Skill: Chapter 14 Urinalysis, Body Fluids and Other Specimens 15 points Objectives: 1. Name 10 routine chemical tests performed on urine and list a
Creatine Kinase (CK) Enzymatic Assay Kit Manual Catalog #: 3460-07
 Creatine Kinase (CK) Enzymatic Assay Kit Manual Catalog #: 3460-07 TABLE OF CONTENTS GENERAL INFORMATION... 2 Product Description... 2 Procedure Overview... 2 Kit Contents, Storage and Shelf Life... 3
Creatine Kinase (CK) Enzymatic Assay Kit Manual Catalog #: 3460-07 TABLE OF CONTENTS GENERAL INFORMATION... 2 Product Description... 2 Procedure Overview... 2 Kit Contents, Storage and Shelf Life... 3
Urinalysis Compliance Tools. POCC Webinar January 19, 2011 Dr. Susan Selgren
 Urinalysis Compliance Tools POCC Webinar January 19, 2011 Dr. Susan Selgren Learning Objectives Be able to review and improve upon a laboratory plan for compliance including: Competency Documentation Proficiency
Urinalysis Compliance Tools POCC Webinar January 19, 2011 Dr. Susan Selgren Learning Objectives Be able to review and improve upon a laboratory plan for compliance including: Competency Documentation Proficiency
Planning: Patient Goals and Expected Outcomes The patient will: Remain free of unusual bleeding Maintain effective tissue perfusion Implementation
 Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Portex Arterial Blood Sampling Kits
 Portex Arterial Blood Sampling Kits Safe Application. Simple Activation. Consistent Results. Portex Arterial Blood Sampling Kits > Compatible with Multi-parameter Analyzers > Balanced Heparin Provides
Portex Arterial Blood Sampling Kits Safe Application. Simple Activation. Consistent Results. Portex Arterial Blood Sampling Kits > Compatible with Multi-parameter Analyzers > Balanced Heparin Provides
510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY
 A. 510(k) Number: K092353 510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY B. Purpose for Submission: This is a new 510k application for a new indication for the MONOLISA Anti-HAV IgM EIA
A. 510(k) Number: K092353 510(k) SUBSTANTIAL EQUIVALENCE DETERMINATION DECISION SUMMARY B. Purpose for Submission: This is a new 510k application for a new indication for the MONOLISA Anti-HAV IgM EIA
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO)
 A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
Hemostasis analyzer system
 Hemostasis analyzer system Providing fast, actionable results to help you reduce risks, complications and costs Get the whole picture with TEG Hemostasis analyzer system For more than forty years, hospitals
Hemostasis analyzer system Providing fast, actionable results to help you reduce risks, complications and costs Get the whole picture with TEG Hemostasis analyzer system For more than forty years, hospitals
OneStep Fecal Occult Blood RapiDip InstaTest. Cat # 13020-1
 CORTEZ DIAGNOSTICS, INC. 23961 Craftsman Road, Suite D/E/F, Calabasas, CA 91302 USA Tel: (818) 591-3030 Fax: (818) 591-8383 E-mail: [email protected] Web site: www.rapidtest.com See external label
CORTEZ DIAGNOSTICS, INC. 23961 Craftsman Road, Suite D/E/F, Calabasas, CA 91302 USA Tel: (818) 591-3030 Fax: (818) 591-8383 E-mail: [email protected] Web site: www.rapidtest.com See external label
Lab 2. Spectrophotometric Measurement of Glucose
 Lab 2 Spectrophotometric Measurement of Glucose Objectives 1. Learn how to use a spectrophotometer. 2. Produce a glucose standard curve. 3. Perform a glucose assay. Safety Precautions Glucose Color Reagent
Lab 2 Spectrophotometric Measurement of Glucose Objectives 1. Learn how to use a spectrophotometer. 2. Produce a glucose standard curve. 3. Perform a glucose assay. Safety Precautions Glucose Color Reagent
Ammonia (plasma, blood)
 Ammonia (plasma, blood) 1 Name and description of analyte 1.1 Name of analyte Ammonia 1.2 Alternative names None 1.3 NLMC code 1.4 Description of analyte Ammonia has the formula NH 3. At physiological
Ammonia (plasma, blood) 1 Name and description of analyte 1.1 Name of analyte Ammonia 1.2 Alternative names None 1.3 NLMC code 1.4 Description of analyte Ammonia has the formula NH 3. At physiological
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins)
 Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
Jeopardy Topics: THE CLOT STOPS HERE (anticoagulants) SUGAR, SUGAR, HOW D YOU GET SO HIGH (insulins) I HEAR YA KNOCKING BUT YOU CAN T COME IN (electrolytes) TAKE MY BREATH AWAY (Opiates-morphine) OUT WITH
Radiation Sciences Nuclear Medicine Technology Program Hot Lab Log Book (Material)
 Radiation Sciences Nuclear Medicine Technology Program Hot Lab Log Book (Material) Table of Content Receiving a Radioactive Package Constancy Test Daily Survey Weekly Wipes Accuracy Test Linearity Geometric
Radiation Sciences Nuclear Medicine Technology Program Hot Lab Log Book (Material) Table of Content Receiving a Radioactive Package Constancy Test Daily Survey Weekly Wipes Accuracy Test Linearity Geometric
General. What is a laboratory test? What is a waived test?
 General What is a laboratory test? What is a waived test? Laboratory tests are medical procedures that involve testing samples of blood, urine, or other tissues or substances from the body. Information
General What is a laboratory test? What is a waived test? Laboratory tests are medical procedures that involve testing samples of blood, urine, or other tissues or substances from the body. Information
Cold Agglutination Titer detecting Cold Reacting Antibodies
 Objectives: Cold Agglutination Titer detecting Cold Reacting Antibodies 1. Perform a serial dilution to determine the amount of cold reacting antibody present in a patient specimen with the results obtained
Objectives: Cold Agglutination Titer detecting Cold Reacting Antibodies 1. Perform a serial dilution to determine the amount of cold reacting antibody present in a patient specimen with the results obtained
Unaccredited Point-of-Care Laboratory Testing Guideline for Physicians
 Unaccredited Point-of-Care Laboratory Testing Guideline for Physicians Prepared by the Advisory Committee on Laboratory Medicine College of Physicians & Surgeons of Alberta Serving the Public by guiding
Unaccredited Point-of-Care Laboratory Testing Guideline for Physicians Prepared by the Advisory Committee on Laboratory Medicine College of Physicians & Surgeons of Alberta Serving the Public by guiding
Human Free Testosterone(F-TESTO) ELISA Kit
 Human Free Testosterone(F-TESTO) ELISA Kit Catalog Number. MBS700040 For the quantitative determination of human free testosterone(f-testo) concentrations in serum, plasma. This package insert must be
Human Free Testosterone(F-TESTO) ELISA Kit Catalog Number. MBS700040 For the quantitative determination of human free testosterone(f-testo) concentrations in serum, plasma. This package insert must be
Basic Lessons in Laboratory Quality Control
 Bio-Rad Laboratories QC education Basic Lessons in Laboratory Quality Control QC Workbook Basic Lessons in Laboratory Quality Control Written by Greg Cooper, CLS, MHA Manager of Clinical Standards and
Bio-Rad Laboratories QC education Basic Lessons in Laboratory Quality Control QC Workbook Basic Lessons in Laboratory Quality Control Written by Greg Cooper, CLS, MHA Manager of Clinical Standards and
URINE DIPSTICK Multistix 10SG
 The Johns Hopkins Hospital Point-of-Care Testing Program URINE DIPSTICK Multistix 10SG Operator Competency Only operators who have completed a defined training program and can demonstrate competence will
The Johns Hopkins Hospital Point-of-Care Testing Program URINE DIPSTICK Multistix 10SG Operator Competency Only operators who have completed a defined training program and can demonstrate competence will
USING CLSI GUIDELINES TO PERFORM METHOD EVALUATION STUDIES IN YOUR LABORATORY
 USING CLSI GUIDELINES TO PERFORM METHOD EVALUATION STUDIES IN YOUR LABORATORY Breakout Session 3B Tuesday, May 1 8:30 10 am James Blackwood, MS, CLSI David D. Koch, PhD, FACB, DABCC, Pathology & Laboratory
USING CLSI GUIDELINES TO PERFORM METHOD EVALUATION STUDIES IN YOUR LABORATORY Breakout Session 3B Tuesday, May 1 8:30 10 am James Blackwood, MS, CLSI David D. Koch, PhD, FACB, DABCC, Pathology & Laboratory
All Acute Care Hospitals and End-Stage Renal Disease Clinics. Subject: Billing and Claim Completion Guidelines for Renal Dialysis Services
 Indiana Health Coverage Programs P R O V I D E R B U L L E T I N BT200223 MAY 29, 2002 To: All Acute Care Hospitals and End-Stage Renal Disease Clinics Subject: Billing and Claim Completion Guidelines
Indiana Health Coverage Programs P R O V I D E R B U L L E T I N BT200223 MAY 29, 2002 To: All Acute Care Hospitals and End-Stage Renal Disease Clinics Subject: Billing and Claim Completion Guidelines
How Does a Doctor Test for AIDS?
 Edvo-Kit #S-70 How Does a Doctor Test for AIDS? S-70 Experiment Objective: The Human Immunodefi ciency Virus (HIV) is an infectious agent that causes Acquired Immunodefi ciency Syndrome (AIDS) in humans.
Edvo-Kit #S-70 How Does a Doctor Test for AIDS? S-70 Experiment Objective: The Human Immunodefi ciency Virus (HIV) is an infectious agent that causes Acquired Immunodefi ciency Syndrome (AIDS) in humans.
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home
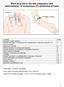 Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
ArtisanLink Staining System is an automated special stains slide
 Technical Tips Tips on using the ArtisanLink Special Staining System Jamie Nowacek, BS, HT(ASCP) CM, QIHC, PMP Dako North America, Inc. Carpinteria, CA, USA ArtisanLink Staining System is an automated
Technical Tips Tips on using the ArtisanLink Special Staining System Jamie Nowacek, BS, HT(ASCP) CM, QIHC, PMP Dako North America, Inc. Carpinteria, CA, USA ArtisanLink Staining System is an automated
The Control of ph and Oxidation Reduction Potential (ORP) in Cooling Tower Applications By Charles T. Johnson, Walchem Corporation
 The Control of ph and Oxidation Reduction Potential (ORP) in Cooling Tower Applications By Charles T. Johnson, Walchem Corporation Introduction The importance of keeping cooling tower water in proper chemical
The Control of ph and Oxidation Reduction Potential (ORP) in Cooling Tower Applications By Charles T. Johnson, Walchem Corporation Introduction The importance of keeping cooling tower water in proper chemical
CK-MB TEST CARD 004A302
 A rapid test for the qualitative detection of CK-MB in whole blood, serum or plasma. For professional in vitro diagnostic use only. INTENDED USE The CK-MB test card is a rapid chromatographic immunoassay
A rapid test for the qualitative detection of CK-MB in whole blood, serum or plasma. For professional in vitro diagnostic use only. INTENDED USE The CK-MB test card is a rapid chromatographic immunoassay
PRINCIPLE. REF 442635 (200 tests/cartridge) REF 476836 (400 tests/cartridge) ANNUAL REVIEW Reviewed by: Date. Date INTENDED USE
 SYNCHRON System(s) Chemistry Information Sheet Copyright 2010 Beckman Coulter, Inc. Creatine Kinase REF 442635 (200 tests/cartridge) REF 476836 (400 tests/cartridge) For In Vitro Diagnostic Use ANNUAL
SYNCHRON System(s) Chemistry Information Sheet Copyright 2010 Beckman Coulter, Inc. Creatine Kinase REF 442635 (200 tests/cartridge) REF 476836 (400 tests/cartridge) For In Vitro Diagnostic Use ANNUAL
digital fever alert ear thermometer suitable from birth instruction manual
 digital fever alert ear thermometer suitable from birth instruction manual digital fever alert ear thermometer instruction manual Please read these instructions carefully before using the thermometer and
digital fever alert ear thermometer suitable from birth instruction manual digital fever alert ear thermometer instruction manual Please read these instructions carefully before using the thermometer and
How to Verify Performance Specifications
 How to Verify Performance Specifications VERIFICATION OF PERFORMANCE SPECIFICATIONS In 2003, the Centers for Medicare and Medicaid Services (CMS) updated the CLIA 88 regulations. As a result of the updated
How to Verify Performance Specifications VERIFICATION OF PERFORMANCE SPECIFICATIONS In 2003, the Centers for Medicare and Medicaid Services (CMS) updated the CLIA 88 regulations. As a result of the updated
Dissolved Oxygen Sensors
 Instruction Sheet PN 51A-HxDO/rev.F June 2008 Models Hx438 and Gx448 Dissolved Oxygen Sensors For additional information, please refer to the Instruction Manuals CD shipped with this product, or visit
Instruction Sheet PN 51A-HxDO/rev.F June 2008 Models Hx438 and Gx448 Dissolved Oxygen Sensors For additional information, please refer to the Instruction Manuals CD shipped with this product, or visit
Direct Measurement Method Method 8157 0 to 20.0 mg/l (or 0 to 200% saturation) O 2 Clark-type Amperometric Sensor
 Oxygen, Dissolved DOC316.53.01241 Direct Measurement Method Method 8157 0 to 20.0 mg/l (or 0 to 200% saturation) O 2 Clark-type Amperometric Sensor Scope and application: For water, wastewater and process
Oxygen, Dissolved DOC316.53.01241 Direct Measurement Method Method 8157 0 to 20.0 mg/l (or 0 to 200% saturation) O 2 Clark-type Amperometric Sensor Scope and application: For water, wastewater and process
Homeostasis. The body must maintain a delicate balance of acids and bases.
 Homeostasis The body must maintain a delicate balance of acids and bases. Metabolic and respiratory processes must work together to keep hydrogen ion (H+) levels normal and stable. ph of Blood The ph of
Homeostasis The body must maintain a delicate balance of acids and bases. Metabolic and respiratory processes must work together to keep hydrogen ion (H+) levels normal and stable. ph of Blood The ph of
Blood Glucose Monitoring: The Facts about Accuracy
 Blood Glucose Monitoring: The Facts about Accuracy Summary The purpose of this document is to provide the facts about the accuracy of self-monitoring of blood glucose (SMBG) systems. Accuracy can be defined
Blood Glucose Monitoring: The Facts about Accuracy Summary The purpose of this document is to provide the facts about the accuracy of self-monitoring of blood glucose (SMBG) systems. Accuracy can be defined
The Determination of an Equilibrium Constant
 The Determination of an Equilibrium Constant Computer 10 Chemical reactions occur to reach a state of equilibrium. The equilibrium state can be characterized by quantitatively defining its equilibrium
The Determination of an Equilibrium Constant Computer 10 Chemical reactions occur to reach a state of equilibrium. The equilibrium state can be characterized by quantitatively defining its equilibrium
ACID-BASE TITRATIONS: DETERMINATION OF CARBONATE BY TITRATION WITH HYDROCHLORIC ACID BACKGROUND
 #3. Acid - Base Titrations 27 EXPERIMENT 3. ACID-BASE TITRATIONS: DETERMINATION OF CARBONATE BY TITRATION WITH HYDROCHLORIC ACID BACKGROUND Carbonate Equilibria In this experiment a solution of hydrochloric
#3. Acid - Base Titrations 27 EXPERIMENT 3. ACID-BASE TITRATIONS: DETERMINATION OF CARBONATE BY TITRATION WITH HYDROCHLORIC ACID BACKGROUND Carbonate Equilibria In this experiment a solution of hydrochloric
Intravenous Fluid Selection
 BENNMC03_0131186116.qxd 3/9/05 18:24 Page 20 seema Seema-3:Desktop Folder:PQ731: CHAPTER 3 Intravenous Fluid Selection LEARNING OBJECTIVES By the end of this chapter, you should be able to: Describe and
BENNMC03_0131186116.qxd 3/9/05 18:24 Page 20 seema Seema-3:Desktop Folder:PQ731: CHAPTER 3 Intravenous Fluid Selection LEARNING OBJECTIVES By the end of this chapter, you should be able to: Describe and
METHODS OF VITAMIN ANALYSIS
 METHODS OF VITAMIN ANALYSIS Specimen requirements; Fasting plasma or serum Lithium Heparin is the anticoagulant of choice for vitamins such as; thiamine, riboflavin, retinol, tocopherols & cholecalciferol
METHODS OF VITAMIN ANALYSIS Specimen requirements; Fasting plasma or serum Lithium Heparin is the anticoagulant of choice for vitamins such as; thiamine, riboflavin, retinol, tocopherols & cholecalciferol
UNIVERSITY OF CONNECTICUT HEALTH CENTER CORRECTIONAL MANAGED HEALTH CARE POLICY AND PROCEDURES FOR USE WITHIN THE CONNECTICUT DEPARTMENT OF CORRECTION
 UNIVERSITY OF CONNECTICUT HEALTH CENTER CORRECTIONAL MANAGED HEALTH CARE POLICY AND PROCEDURES FOR USE WITHIN THE CONNECTICUT DEPARTMENT OF CORRECTION NUMBER: P 1.01 Page 1 of 1 PATIENT SAFETY SYSTEM/PSS:
UNIVERSITY OF CONNECTICUT HEALTH CENTER CORRECTIONAL MANAGED HEALTH CARE POLICY AND PROCEDURES FOR USE WITHIN THE CONNECTICUT DEPARTMENT OF CORRECTION NUMBER: P 1.01 Page 1 of 1 PATIENT SAFETY SYSTEM/PSS:
For In Vitro Diagnostic Use
 SYNCHRON System(s) Chemistry Information Sheet Creatine Kinase REF (200 tests/cartridge) 442635 REF (400 tests/cartridge) 476836 For In Vitro Diagnostic Use ANNUAL REVIEW Reviewed by: Reviewed by: Date
SYNCHRON System(s) Chemistry Information Sheet Creatine Kinase REF (200 tests/cartridge) 442635 REF (400 tests/cartridge) 476836 For In Vitro Diagnostic Use ANNUAL REVIEW Reviewed by: Reviewed by: Date
Vaginal ph Test (ph Hydrion TM Paper 4.5-7.5)
 University of California, San Francisco Department of Laboratory Medicine San Francisco General Hospital 1001 Potrero Avenue, San Francisco CA 94110 Clinical Laboratory Eberhard Fiebig, M.D., Director
University of California, San Francisco Department of Laboratory Medicine San Francisco General Hospital 1001 Potrero Avenue, San Francisco CA 94110 Clinical Laboratory Eberhard Fiebig, M.D., Director
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Mouse Creatine Kinase MB isoenzyme (CKMB) ELISA
 KAMIYA BIOMEDICAL COMPANY Mouse Creatine Kinase MB isoenzyme (CKMB) ELISA For the quantitative determination of mouse CKMB in serum, plasma, cell culture fluid and other biological fluids Cat. No. KT-57681
KAMIYA BIOMEDICAL COMPANY Mouse Creatine Kinase MB isoenzyme (CKMB) ELISA For the quantitative determination of mouse CKMB in serum, plasma, cell culture fluid and other biological fluids Cat. No. KT-57681
Content Sheet 7-1: Overview of Quality Control for Quantitative Tests
 Content Sheet 7-1: Overview of Quality Control for Quantitative Tests Role in quality management system Quality Control (QC) is a component of process control, and is a major element of the quality management
Content Sheet 7-1: Overview of Quality Control for Quantitative Tests Role in quality management system Quality Control (QC) is a component of process control, and is a major element of the quality management
Milwaukee USER MANUAL
 Milwaukee USER MANUAL PORTABLE DISSOLVED OXYGEN METER MODEL: MW600 Smart DO Meter PROBE PREPARATION: The meter is supplied with a 9V battery. Slide off the battery compartment cover on the back of the
Milwaukee USER MANUAL PORTABLE DISSOLVED OXYGEN METER MODEL: MW600 Smart DO Meter PROBE PREPARATION: The meter is supplied with a 9V battery. Slide off the battery compartment cover on the back of the
ACID-BASE BALANCE AND ACID-BASE DISORDERS. I. Concept of Balance A. Determination of Acid-Base status 1. Specimens used - what they represent
 ACID-BASE BALANCE AND ACID-BASE DISORDERS I. Concept of Balance A. Determination of Acid-Base status 1. Specimens used - what they represent II. Electrolyte Composition of Body Fluids A. Extracellular
ACID-BASE BALANCE AND ACID-BASE DISORDERS I. Concept of Balance A. Determination of Acid-Base status 1. Specimens used - what they represent II. Electrolyte Composition of Body Fluids A. Extracellular
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
6 Easy Steps to ABG Analysis
 6 Easy Steps to ABG Analysis E-Booklet David W. Woodruff, MSN, RN- BC, CNS, CMSRN, CEN 571 Ledge Road, Macedonia, OH 44056 Telephone (800) 990-2629 Fax (800) 990-2585 1997-2012 Ed4Nurses, Inc. All rights
6 Easy Steps to ABG Analysis E-Booklet David W. Woodruff, MSN, RN- BC, CNS, CMSRN, CEN 571 Ledge Road, Macedonia, OH 44056 Telephone (800) 990-2629 Fax (800) 990-2585 1997-2012 Ed4Nurses, Inc. All rights
EXERCISE 5: ERYTHROCYTES SEDIMENTATION RATE - ESR, SED RATE
 EXERCISE 5: ERYTHROCYTES SEDIMENTATION RATE - ESR, SED RATE Textbook: Skills: None 10 points Objectives: 1. State the principle of the Erythrocytes Sedimentation Rate - ESR. 2. List two factors which may
EXERCISE 5: ERYTHROCYTES SEDIMENTATION RATE - ESR, SED RATE Textbook: Skills: None 10 points Objectives: 1. State the principle of the Erythrocytes Sedimentation Rate - ESR. 2. List two factors which may
Canine creatine kinase MB isoenzyme (CK-MB)ELISA Kit
 Canine creatine kinase MB isoenzyme (CK-MB)ELISA Kit Catalog No. CSB-E15852c (96T) This immunoassay kit allows for the in vitro quantitative determination of canine CK-MB concentrations in serum and plasma.
Canine creatine kinase MB isoenzyme (CK-MB)ELISA Kit Catalog No. CSB-E15852c (96T) This immunoassay kit allows for the in vitro quantitative determination of canine CK-MB concentrations in serum and plasma.
