Adult Catheter Care & Infection Prevention Guide
|
|
|
- Gyles Snow
- 7 years ago
- Views:
Transcription
1 proudly presents the Adult Catheter Care & Infection Prevention Guide to accompany the interactive, educational program available at sponsored by assembled by March 17, Updated regularly.
2 This Adult Catheter Care and Infection Prevention Guide provides general information and is not intended to replace the advice of your clinician. Consumers are strongly advised to review the material with their clinician, especially recommended actions which may be different than your usual protocol. Although much of the information will be helpful for children, not all of it is applicable. Talk to your child s pediatric specialist for guidance. This guide was developed based on the latest guidelines from multiple professional organizations, as well as clinical practice at major HPN centers in the United States. It has been reviewed by leading clinicians from these centers, as well as the Oley Foundation s Medical & Research Director. A list of references is provided on page six. Credit for creating this guide, as well as the MY HPN Modules 1 & 2, goes to Oley Trustee Cheryl Thompson, PhD, RD, CNSD. Special thanks to Baxter Healthcare for underwriting MY HPN Module 2: Catheter-Associated Infections. Many thanks also to the patient and clinician volunteers who provided input on the project. Copyright 2010 The Oley Foundation. The Oley Foundation, 214 Hun Memorial, MC-28, Albany Medical Center, Albany, NY (800) 776-OLEY, (518) , FAX (518) bishopj@mail.amc.edu
3 Summary of Catheter-Associated Infections for Adult HPN Consumers Exit Site, Tunnel, and Port Pocket Infections Can occur at the Catheter exit site (where the catheter comes out from under the skin). Cuff or along the tract of a tunneled catheter. The cuff is a device under the skin that helps to prevent a tunneled catheter from slipping and bacteria from entering the bloodstream. The tunnel is the tract below the skin from the exit site to the point where the catheter enters the vein. Pocket around an implanted catheter port (also called a disc or Port-a-Cath ) that is placed completely under the skin. Causes Usually caused by germs on the skin (e.g. staphylococcus). May occur if: - There is a break in sterile technique when placing or accessing the catheter. - There is irritation from a suture (stitch) in the skin that anchors the catheter. - The exit site is inadequately cleaned/disinfected or a wet/soiled dressing is not replaced. Prevention Wash hands with liquid antibacterial soap for at least 15 seconds using friction before accessing the line; dry with a disposable towel. An alcohol-based gel or foam may be used if hands do not look dirty. Clean skin around the catheter exit site with 2% chlorhexidine in 70% alcohol for at least 30 seconds before replacing a sterile dressing. Allow to air dry. Scrub the hub (also called the injection cap), and rubber top of a medicine vial for at least 15 seconds before accessing. Some clinicians also recommend cleaning the hub after disconnecting. Change the dressing immediately if it becomes loose, damp or dirty; and routinely every 2 days (if gauze) or 7 days if clear dressing. Wash your hands before/after removing the old dressing. Avoid touching the exit site. Wear sterile gloves when placing a new dressing if advised to do so by your clinician. Ask your clinician about removing sutures if they remain after the exit site has healed (4-6 weeks) and/or if a sutureless system (i.e. commercial catheter-stabilization product, sterile tapes or surgical strips [such as Steri-Strips ] is an option. Note: Routine use of antimicrobial cream at the exit site is no longer recommended due to the potential to promote fungal infections and antimicrobial resistance. Symptoms/Signs Exit site infection: local redness*, drainage often with pus (that may only be on the dressing); firmness, swelling, warmer than usual skin temperature; tenderness within 2 cm (0.8 inch) of the catheter exit site. Usually not very painful or associated with a fever. Tunnel infection: redness, swelling, firmness, and moderate-severe pain > 2 cm (0.8 inch) from the catheter exit site along the tract of a tunneled catheter; drainage (often with pus) from the exit site; sometimes fever. If it involves the cuff, this may be felt under the skin. Pocket infection (implanted port): redness, tenderness, and/or firmness over the pocket; or a spontaneous opening may allow drainage of fluid with pus * A smaller area of redness can also be caused by irritation of a retained suture or movement of the catheter where it enters the skin this redness without infection is typically < ¼ inch (5-6 mm) in diameter. Immediate Call your clinician (or go to the ER) for fever >101 F (or prolonged/recurrent temperature 1 or action Treatment of catheter exit site infection Treatment of tunnel or port more degrees above normal), or shaking chills, or if the exit site has pus, redness or swelling. Antibiotics: antimicrobial ointment and/or oral/intravenous (IV) antibiotics. More frequent dressing changes (e.g. daily gauze dressing changes to remove drainage) Catheter removal is usually not necessary unless the infection is caused by certain germs that are difficult to treat; or does not go away (or comes back) after treatment with antibiotics; or the catheter cuff is visible at the exit site. The catheter is typically removed along with the use of oral or intravenous (IV) antibiotics. Oley Foundation (800) 776-OLEY, Updated page 1 of 6
4 Catheter-Associated Bloodstream Infection (CABSI) Symptoms/signs Chills, shaking especially while infusing HPN or flushing the catheter Increased body temperature > 101 degrees Fahrenheit Low blood pressure; increased blood glucose; or glucose in urine Skin feels unusually warm and dry; or cool and moist Body aches, lethargy (i.e. less alert, less active) Causes Germs can grow at the catheter exit site (i.e. inadequate hand washing or not adequately cleaning the exit site) and then travel along the catheter into the blood. Germs can enter at the catheter injection hub (i.e. if not disinfected [cleaned] properly or by touch contamination when accessing the line); or multiply inside an occluded lumen. Spreading or seeding of germs from another source of infection inside your body (e.g. urinary tract infection, pneumonia, ileostomy/colostomy sites, etc.). Contaminated tubing or intravenous (IV) solution. Risk factors Multiple uses of the catheter (i.e. using the HPN lumen to draw blood or give other fluids) Increased contact with germs (e.g. from an ostomy, fistula, or wound drainage) Decreased immune function from certain medications or medical conditions Some types of catheters (e.g. non-tunneled; multi-lumen) or exit site locations (e.g. leg) Germs that grow in a biofilm layer on the tip of your catheter or at a thrombus (occlusion). Prevention IN ADDITION TO TIPS TO PREVENT LOCAL CATHETER INFECTION LISTED ABOVE: Discuss the most appropriate type of catheter and insertion site with your clinician. - Do not allow your HPN catheter to be used for other purposes (eg blood samples) unless absolutely necessary. - A single-lumen catheter is preferred to reduce risk of infection. Dedicate one lumen for HPN if you have a multiple-lumen catheter. Have an unneeded catheter removed. Change the HPN tubing (administration set) every 24 hours at home. Change the injection hub/cap every 7 days; or more frequently if blood is in the hub/cap. Do not infuse an HPN solution or additive if you think it may be contaminated (e.g. looks cloudy or something is floating in a clear solution, aseptic technique was not used to add an ingredient to HPN, product was not refrigerated as recommended). Be sure your catheter flushes easily since germs can grow at a thrombus (occlusion). Ask your clinician if you need antibiotics before a dental or medical procedure. Immediate Contact your clinician or go to the emergency room immediately if your temperature is action >101 degrees Fahrenheit (38 degrees Celsius), or you have shaking chills especially if this occurs while infusing IV fluids (such as HPN) or flushing the catheter. Ask your clinician in advance about other symptoms that warrant contacting them e.g. - if you have a decreased immune function, since you may not have the typical rise in temperature that other people have with an infection. - a prolonged (or recurrent) fever of one or more degrees above normal/baseline (e.g. that lasts more than 1 or 2 days) especially if you have other symptoms of infection such as Treatment of catheterassociated bloodstream infection (CABSI) body aches, feeling unusually tired, or increased glucose in blood or urine. IV antibiotics once blood cultures have been taken. Catheter removal may be necessary e.g. catheter tunnel or implanted port pocket infection; septic shock or complicated infection; blood cultures are positive for fungi or drug-resistant bacteria; the same microorganism causes infection again -- after previous treatment; or the consumer is pregnant. Antibiotic lock therapy may also be used in some cases e.g.: - to prevent infection if repeated CABSI despite always using aseptic technique, or the person is neutropenic (i.e. increased risk of infection due to low white blood cells). - to treat infection if it is thought to be from the spread of bacteria on the catheter hub; the microorganism is Staph. aureus, coagulase-negative staphylococci, or gram-negative bacilli; and there is not a catheter tunnel or implanted port pocket infection. Oley Foundation (800) 776-OLEY, Updated page 2 of 6
5 How You Can Help Prevent Catheter-Associated Infections (local and bloodstream) 1. Clean your work area before each use (i.e. before putting down your sterile barrier and supplies). Wash the area with 70% alcohol, antiseptic soap, or diluted bleach; and wipe with a clean paper towel. Work at a comfortable pace -- the risk of contamination increases if you rush. 2. Wash your hands before doing anything with your catheter or supplies. Wet hands and wrists with warm water. Scrub at least 15 seconds using liquid antibacterial soap (including under fingernails). Dry with a clean paper towel. Turn water off with the back of your wrist/elbow or paper towel. Anyone helping with your catheter must wash their hands this way as well. Wash your hands again if you touch your mouth, nose, or any unclean object. Ask your clinician about using an alcohol-based foam or gel if your hands have no visible dirt; find out specific products that are acceptable. - Apply foam/gel to palm of one hand (see label for the amount). - Cover entire surface of hands/fingers; and rub hands together until dry. 3. Avoid touch contamination. Only use sterile supplies when infusing your HPN or caring for your catheter. When piercing, opening, or connecting sterile items, allow only sterile surfaces to touch other sterile surfaces. Also, do not touch your catheter exit site with anything that is not sterile. - Some clinicians recommend sterile gloves when applying a new dressing or if you must touch the exit site. - Handle dressings only at the edges. 4. Scrub the hub for at least 15 seconds every time you access or flush the catheter. Scrub the injection hub/cap for at least 15 seconds before accessing the catheter (e.g. every time you infuse an IV fluid or flush the catheter). The friction is very important. Twist at least 10 times like juicing an orange. Also scrub the top of any medicine vial before accessing. Use 2% chlorhexidine solution in 70% alcohol, 70% alcohol or povidone-iodine. 5. Properly clean/disinfect the exit site during the dressing change. Wash your hands after removing the old dressing. Put on sterile gloves if recommended by your clinician. Wear a mask if you have an illness where you might cough near the exit site. - Do not routinely use antimicrobial ointments on the catheter exit site. Notify your clinician if you see any drainage, swelling or redness at the exit site. Use 2% chlorhexidine solution in 70% alcohol to clean the skin around your catheter exit site. - For most applicators, press sponge against skin and apply chlorhexadine solution using a back/forth and up/down scrub for at least 30 seconds. Do not wipe or blot. Allow to air dry completely (~ 2 minutes) before placing the dressing otherwise a rash may form. - If unable to use chlorhexidine (e.g. sensitivity or allergy), use 70% alcohol or povidone-iodine. 6. Cover the catheter exit site with a dressing as instructed by your clinician. Change your dressing routinely: gauze every 2 days; clear dressing every 7 days. Change your dressing immediately if it becomes damp, loose, or dirty; or moist from sweat. - Carry supplies to change the dressing when traveling. Use gauze dressing if the exit site is bleeding or oozing. Chlorhexidine-soaked (impregnated) dressings may help prevent contamination of the catheter exit site. Their use should be considered for adult consumers with non-tunneled catheters (e.g. PICC) who are at high risk for infection or if the infection rate is high despite using other strategies. Discuss the risks and benefits with your clinician. If you may have contaminated any supply, throw it out. Call your provider early to reorder supplies. Oley Foundation (800) 776-OLEY, Updated page 3 of 6
6 7. Replace catheter-related equipment on a regular schedule. Change HPN tubing (administration set) every 24 hours (ie use new tubing each day). Change injection hub/cap (and sutureless securement devices) every 7 days or as instructed by your clinician (e.g. change more frequently if there is blood in the hub/cap). 8. Never infuse any fluid through the catheter that you think might be contaminated. Do not use HPN if you see particles, the fluid is cloudy, or if there is a leak in the bag. Do not use any IV fluid if the beyond use (expiration) date has passed. Whenever possible, use single-dose containers/vials for HPN additives or medications. Do not combine the leftover content of single-use vials for later use. If a multidose vial is used, refrigerate after opening if recommended by the manufacturer. Scrub the rubber top of any container (e.g. multivitamins) with 70% alcohol before accessing it and only use a sterile needle/access device. Avoid touch contamination; throw away any unused portion if you think it might be contaminated (e.g. if the vial had been accessed before cleaning). Do not infuse HPN longer than 24 hours. 9. Make sure your catheter is flushing well because any clot in the catheter can be a gathering place for germs. A partially or completely blocked catheter can decrease your ability to infuse your medications as well as increase your risk of infection. Contact your clinician if you have any difficulty infusing your IV medications/fluids or HPN. 10. Secure your catheter to prevent accidental removal. Take steps to prevent catheter damage and be prepared if your catheter breaks. Loop and secure the catheter at all times (with a dressing or tape) to prevent pulling even if you are not using a dressing. Do not allow the catheter to dangle. Women should tuck excess catheter tubing under the strap of their bra. Keep a repair kit at home and take on trips in case a hole develops in a tunneled catheter. - Include alcohol-based gel/foam in case soap and water is not available to wash your hands. - Immediately clamp the catheter (between the catheter exit site and the hole). - Call your clinician and go to an emergency room or clinic. Bring your repair kit because, unfortunately, many emergency rooms do not have them. Ask your clinician about a sutureless securement device to reduce the risk of infection and accidental catheter migration/removal. 11. Showering is permitted but the catheter must be kept dry. For the first 30 days after catheter placement (or longer if the site hasn t healed), special precautions should be taken to reduce the risk of introducing germs into the catheter (e.g., protect the catheter and connecting device with a waterproof cover during the shower). The dressing needs to be changed if it becomes wet. Ask your clinician about the best way to care for your catheter when bathing or swimming. Some physicians permit only sponge bathing or showering for patients who have immune issues or experience frequent line infections. For additional information go to: Oley's Swimming with Home Parenteral and Enteral Nutrition If your HPN catheter is being replaced, discuss the options with your clinician so you can choose the catheter with the lowest risk of infection. A tunneled catheter is most commonly recommended for long-term HPN. An implanted catheter (port) or PICC may also be used. A single-lumen catheter is preferred (compared to multi-lumen) to reduce risk of infection. If you have a multi-lumen catheter, always use the same lumen for HPN. This should be labeled and should not be used for other purposes except in emergency situations. Your clinician should remove any catheter that is no longer needed. Oley Foundation (800) 776-OLEY, Updated page 4 of 6
7 General Information about Central Venous Catheters for Adult HPN Consumers The type of catheter and choice of vein depends on several factors including risks associated with the placement method, potential complications (thrombotic, infectious, mechanical), ease of site care, number of weekly infusions and anticipated duration of therapy. When a clinician places a central line, he/she should follow maximum barrier precautions: wearing a head cap, face mask, sterile body gown, and sterile gloves, and use a full size drape to cover the patient from head to toe.. Tunneled (cuffed) catheters are recommended for long-term home parenteral nutrition (HPN). General Information Comments Placement Tunneled catheters follow a tract under the skin before entering a central vein and have a cuff. They are the most common type of long-term HPN access. Often called by a brand name (eg Broviac, Groshong, Hickman ) or number of lumens (e.g. single, double or triple lumen). Lower rate of infection than non-tunneled catheters because 1) a cuff helps prevent germs from traveling along the catheter and 2) the catheter tract is a longer distance for germs to travel from the skin to vein. Under the skin, fibrin and collagen that form around the cuff help to secure the catheter in place. The cuff should be placed far enough from the exit site so that it doesn t work its way out with gentle tugging on the line associated with day-to-day use. Typically placed by a Surgeon or Interventional Radiologist. Expert opinion suggests the preferred vein for a tunneled catheter is the right internal jugular (neck) with an exit site on the chest wall; the next best is the left internal jugular, then subclavian (chest) veins. However, long-term HPN consumers that have thrombosed (clotted) neck and chest veins may need a tunneled catheter in the femoral or saphenous vein. The exit site should be placed so that it is easy for the consumer to see and as far as possible from an infecting area such as an ostomy. For long-term HPN consumers, consider a standard-length silicone catheter with the cuff placed at least 2.5 cm from the exit site. Peripherally Inserted Central Catheters (PICC) General Information Comments Placement PICCs are typically used in the hospital or for short-term HPN. However, the use of PICCs for long-term HPN is becoming increasingly common. The exit site is on the arm (usually just above the bend at the elbow). As with other central catheters, the tip is placed in the distal superior vena cava (i.e. the main vein near your heart where the blood flows quickly). A PICC should not be confused with other catheters placed in the arm (e.g. peripheral or midline) that cannot be used for HPN. Short-term catheters such as a PICC are not tunneled (i.e. they do not have a long tract under the skin), and most do not have a cuff. Therefore, germs on the skin can be a major source of catheter-related bloodstream infection; and the catheter needs to be secured. For adult patients at high risk for infection, a chlorhexidine-soaked (impregnated) sponge can be placed over the exit site to reduce growth of bacteria. The sponge releases medication for 7 days if dry; however, it is less effective (and may cause skin irritation) if it becomes moist. Compared to other non-tunneled catheters placed at the neck or groin, the risk of infection may be lower because it is easier to keep the dressing clean/dry for a PICC placed in the arm. Further research is needed to assess risk of infection, and other complications (e.g. peripheral vein thrombophlebitis [inflammation of a vein], PICC-related thrombosis [clotting within the vein], and premature dislodgment). Typically placed by a Vascular Access/PICC team into a basilic, cephalic or brachial vein. Recent guidelines suggest using a commercial catheter-stabilization product, sterile tapes or surgical strips to secure a non-cuffed/non-tunneled catheter, rather than sutures. Ask your clinician about the best securement method to minimize catheter movement and contamination. A securement device is typically replaced every 7 days when the dressing is changed. Oley Foundation (800) 776-OLEY, Updated page 5 of 6
8 Implanted port catheters General Information Comments Placement Implanted port catheters (also called a Port or Port-a-Cath ) are commonly used for weekly/monthly access (e.g. chemotherapy). The port (or disc) of an implanted catheter is completely under the skin. An acceptable option for HPN especially if the consumer has not previously had catheterrelated bloodstream infections (because infection of the port requires surgical removal); and is willing to insert a needle into the port each time HPN is infused. Lowest risk of infection because the entire catheter is under the skin. Improved self-image; easier catheter-site care (no dressing is needed); safer for swimming. Typically placed into subclavian or internal jugular vein by General Surgery in an operating room. Minor surgery is required for catheter placement, repair or removal. Non-tunneled, non-cuffed catheters General Information Comments Placement Central Line Catheters Not Recommended for HPN Non-tunneled, non-cuffed catheters are intended for short-term use. They are not recommended for HPN due to high rates of infection, obstruction and dislocation. The catheter may be referred to by the vein insertion site (e.g. subclavian, internal jugular, or femoral catheter) or number of lumens. Account for the majority of catheter-related bloodstream infections. A non-tunneled catheter inserted in the subclavian vein is the safest, while the neck or groin is associated with the highest risk of infection. References: 1. Pittiruti M, Hamilton H, Biffi R, MacFie J, Pertkiewicz M. ESPEN Guidelines on Parenteral Nutrition: Central Venous Catheters (access, care, diagnosis and therapy of complications). Clinical Nutrition. 2009; 28: Available at: 2. Information adapted with permission from Morbidity and Mortality Weekly Report. August 9, 2002/Vol51/No.RR Steiger E. HPEN Working Group. Consensus statements regarding optimal management of home parenteral nutrition (HPN) access. JPEN J Parenter Enteral Nutr. 2006;30(1):S Staun, M, Pironi L, Bozzetti F et al. ESPEN Guidelines on Parenteral Nutrition: Home Parenteral Nutrition (HPN) in adult patients. Clinical Nutrition. 2009; 28: available at: 5. Howard L, Claunch C, McDowell R, Timchalk A: Five years of experience in patients receiving home nutrition support with implanted reservoir: A comparison with the external catheter. JPEN J Parent. Ent. Nutr. 1989;13: O Grady NP, Alexander M, Patchen Dellinger A, et al. CDC Guidelines for the prevention of intravascular catheter-related infections. In press. 7. Gillies D, Carr D, Frost J, O'Riordan E, Gunning R, O'Brien I. Gauze and tape and transparent polyurethane dressings for central venous catheters. Cochrane Database of Systematic Reviews 2003, Issue 3. Art. No.: CD DOI: / CD Worthington T, Elliott TS. Diagnosis of central venous catheter related infection in adult patients. J Infect. 2005; 51: Abstract available at: System2.PEntrez.Pubmed.Pubmed_ResultsPanel.Pubmed_RVDocSum&ordinalpos=7 9. Mermel LA, Allon M, Bouza E et al. Clinical practice guidelines for the diagnosis and management of intravascular catheterrelated infection: 2009 Update by the Infectious Diseases Society of America. Clinical Infectious Diseases. 2009; 49: Marschall J, Mermel LA, Classen D et al. Strategies to prevent central line-associated bloodstream infections in acute care hospitals. Infection Control and Hospital Epidemiology : S Oley Foundation (800) 776-OLEY, Updated page 6 of 6
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Peripherally Inserted Central Catheter (PICC) Patient Instructions
 Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
Vaxcel PICCs Valved and Non-Valved. A Patient s Guide
 Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
HICKMAN Catheter Care with a Needleless Connector
 HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Managing Your Non-Tunneled (Percutaneous) Catheter: PICC, SICC, and JCC. What is a PICC catheter?
 Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
PICC/Midclavicular/Midline Catheter
 47 PICC/Midclavicular/Midline Catheter Introduction- PICC/ MCV/ Midline You have a PICC/Midclavicular/Midline (peripherally inserted) catheter. This catheter should make receiving I.V. medicines or solutions
47 PICC/Midclavicular/Midline Catheter Introduction- PICC/ MCV/ Midline You have a PICC/Midclavicular/Midline (peripherally inserted) catheter. This catheter should make receiving I.V. medicines or solutions
Tunneled Central Venous Catheter (CVC) Placement
 PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
Section 4: Your Vascular Access. What is vascular access?
 Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Central Line-Associated Bloodstream Infection (CLABSI) Prevention. Basics of Infection Prevention 2-Day Mini-Course 2013
 Central Line-Associated Bloodstream Infection (CLABSI) Prevention Basics of Infection Prevention 2-Day Mini-Course 2013 2 Objectives Describe the etiology and epidemiology of central line associated bloodstream
Central Line-Associated Bloodstream Infection (CLABSI) Prevention Basics of Infection Prevention 2-Day Mini-Course 2013 2 Objectives Describe the etiology and epidemiology of central line associated bloodstream
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Policies & Procedures. I.D. Number: 1073
 Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
To maintain a port of entry to venous flow when all available peripheral ports have failed.
 I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
Central Venous Catheter Care For Haemodialysis
 Central Venous Catheter Care For Haemodialysis Information For Parents and Carers Haemodialysis Unit 01 878 4757 Main Hospital Number 01 878 4200 Central Venous Catheters We hope this booklet will help
Central Venous Catheter Care For Haemodialysis Information For Parents and Carers Haemodialysis Unit 01 878 4757 Main Hospital Number 01 878 4200 Central Venous Catheters We hope this booklet will help
Hemodialysis Access: What You Need to Know
 Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Care of your peripherally inserted central catheter
 Care of your peripherally inserted central catheter A guide for patients and their carers We care, we discover, we teach Contents What is a PICC?.... 1 How is it put in?.... 1 What are the benefits of
Care of your peripherally inserted central catheter A guide for patients and their carers We care, we discover, we teach Contents What is a PICC?.... 1 How is it put in?.... 1 What are the benefits of
Your Guide to Peritoneal Dialysis Module 3: Doing Peritoneal Dialysis at Home
 Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Peripherally Inserted Central Catheter (PICC)
 Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter. Peripherally-Inserted Central Catheter (PICC)
 Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter Peripherally-Inserted Central Catheter (PICC) Page 2 of 10 MC1482 Peripherally-Inserted Central Catheter Introduction A peripherally-inserted
Page 1 of 10 MC1482 Peripherally-Inserted Central Catheter Peripherally-Inserted Central Catheter (PICC) Page 2 of 10 MC1482 Peripherally-Inserted Central Catheter Introduction A peripherally-inserted
Management of Catheters Infectious Diseases Working Party/Nurses Group
 Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Going home with your Tunneled Catheter
 Going home with your Tunneled Catheter Your Tunneled Catheter was put in by on Interventional Radiologist Date Your Tunneled Catheter was put in at: McMaster University Medical Centre Hamilton General
Going home with your Tunneled Catheter Your Tunneled Catheter was put in by on Interventional Radiologist Date Your Tunneled Catheter was put in at: McMaster University Medical Centre Hamilton General
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO)
 A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
Are venous catheters safe in terms of blood tream infection? What should I know?
 Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Peripherally Inserted Central Venous Catheter (PICC) Invasive Devices Clinical Nurse Specialist Chief Nurse
 Peripherally Inserted Central Venous Catheter (PICC) Invasive Devices Clinical Nurse Specialist Chief Nurse This leaflet has been designed to give you important information about your condition / procedure,
Peripherally Inserted Central Venous Catheter (PICC) Invasive Devices Clinical Nurse Specialist Chief Nurse This leaflet has been designed to give you important information about your condition / procedure,
PICC Catheter for IV Therapy
 PICC Catheter for IV Therapy A Patient Guide for: PATIENT PICC A PICC is defined as a Peripherally Inserted Central Catheter. A PICC is a special IV Catheter. It is put in an arm vein and ends in a large
PICC Catheter for IV Therapy A Patient Guide for: PATIENT PICC A PICC is defined as a Peripherally Inserted Central Catheter. A PICC is a special IV Catheter. It is put in an arm vein and ends in a large
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC)
 Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HEMODIALYSIS ACCESS OPTIONS
 Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HEMODIALYSIS ACCESS OPTIONS What is a vascular access? A vascular access is a place on your body close to a vein and artery. This place
Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HEMODIALYSIS ACCESS OPTIONS What is a vascular access? A vascular access is a place on your body close to a vein and artery. This place
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
I. Questions for VAD slide program
 I. Questions for VAD slide program 1. The rate of central line associated blood stream infections (CLABSI) in the adult ICUs in Johns Hopkins Hospital is lower than the national average. 2. The mortality
I. Questions for VAD slide program 1. The rate of central line associated blood stream infections (CLABSI) in the adult ICUs in Johns Hopkins Hospital is lower than the national average. 2. The mortality
Peripherally Inserted Central Catheter
 Peripherally Inserted Central Catheter (PICC) by Patricia Griffin Kellicker, BSN En Español (Spanish Version) Definition A peripherally inserted central catheter is a long, thin tube that is inserted through
Peripherally Inserted Central Catheter (PICC) by Patricia Griffin Kellicker, BSN En Español (Spanish Version) Definition A peripherally inserted central catheter is a long, thin tube that is inserted through
Peripherally Inserted Central Catheter (PICC Line)
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home
 Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses
 Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
Flushing and Dressing a Peripherally Inserted Central Catheter (PICC Line): a Guide for Nurses Information for Nurses Introduction This information is for community nursing staffs who have been asked to
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
CATHETER for Hemodialysis
 CATHETER for Hemodialysis What You Need to Know to Stay Healthy with a Catheter One treatment choice for kidney failure is hemodialysis (HD). HD removes wastes and excess fluid from your blood. Your lifeline
CATHETER for Hemodialysis What You Need to Know to Stay Healthy with a Catheter One treatment choice for kidney failure is hemodialysis (HD). HD removes wastes and excess fluid from your blood. Your lifeline
Insertion of a Peripherally Inserted Central Catheter (PICC Line)
 Insertion of a Peripherally Inserted Central Catheter (PICC Line) Patient Information Introduction This booklet has been written to provide information to patients about to have a peripherally inserted
Insertion of a Peripherally Inserted Central Catheter (PICC Line) Patient Information Introduction This booklet has been written to provide information to patients about to have a peripherally inserted
Care of your central venous catheter A guide for patients and their carers. We care, we discover, we teach
 Care of your central venous catheter A guide for patients and their carers We care, we discover, we teach This booklet contains information about central venous catheters (CVC). These are sometimes called
Care of your central venous catheter A guide for patients and their carers We care, we discover, we teach This booklet contains information about central venous catheters (CVC). These are sometimes called
Going Home with a Urinary Catheter
 Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
PICC and Midline Catheters
 PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
1-800-862-2731 Administration of Meropenem For Child
 1 Drug Name: _Meropenem 1-800-862-2731 Administration of Meropenem For Child Dosage: milligrams every hours over 5 minutes Key Points: FLUSHING: Meropenem Heparin flush 1. Always wash your hands with an
1 Drug Name: _Meropenem 1-800-862-2731 Administration of Meropenem For Child Dosage: milligrams every hours over 5 minutes Key Points: FLUSHING: Meropenem Heparin flush 1. Always wash your hands with an
Renal Vascular Access Having a Fistula For Haemodialysis
 Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Central Venous Catheters for Veterinary Technicians
 Central Venous Catheters for Veterinary Technicians Erica Mattox, CVT, VTS (ECC) Central venous catheterization is passing a long catheter into a large vein, such as the jugular or caudal vena cava. This
Central Venous Catheters for Veterinary Technicians Erica Mattox, CVT, VTS (ECC) Central venous catheterization is passing a long catheter into a large vein, such as the jugular or caudal vena cava. This
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
I-140 Venipuncture for Blood Specimen Collection
 I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
Providing optimal care
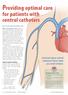 Providing optimal care for patients with central catheters By Ann Earhart, MSN, RN, ACNS-BC, CRNI WHEN REGISTERED NURSE Andrea arrives on shift for report, she learns that her patient, a 62-year-old male,
Providing optimal care for patients with central catheters By Ann Earhart, MSN, RN, ACNS-BC, CRNI WHEN REGISTERED NURSE Andrea arrives on shift for report, she learns that her patient, a 62-year-old male,
How to care for a Midline Catheter
 How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
MRSA. Living with. Acknowledgements. (Methicillin-Resistant Staphylococcus aureus)
 How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
Tunnelled haemodialysis catheter
 Liver, Renal & Surgery Tunnelled haemodialysis catheter Information for patients and carers This leaflet explains what a tunnelled haemodialysis catheter is and how it is put in. It also covers the risks
Liver, Renal & Surgery Tunnelled haemodialysis catheter Information for patients and carers This leaflet explains what a tunnelled haemodialysis catheter is and how it is put in. It also covers the risks
EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY. Methicillin-resistant Staph aureus: Management in the Outpatient Setting
 EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY Methicillin-resistant Staph aureus: Management in the Outpatient Setting Date Originated: Date Reviewed: Date Approved: Page 1 of Approved by: Department
EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY Methicillin-resistant Staph aureus: Management in the Outpatient Setting Date Originated: Date Reviewed: Date Approved: Page 1 of Approved by: Department
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Infection Prevention
 Infection Prevention Dear HSS Patient: The Hospital for Special Surgery is committed to patient safety and quality patient care and is proud to have achieved one of the lowest infection rates in New York
Infection Prevention Dear HSS Patient: The Hospital for Special Surgery is committed to patient safety and quality patient care and is proud to have achieved one of the lowest infection rates in New York
Community Nurse Referral Letter (Hickman Line Care)
 Community Nurse Referral Letter (Hickman Line Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a Hickman
Community Nurse Referral Letter (Hickman Line Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a Hickman
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g.
 How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery.
 JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
How to Care for your Child s Indwelling Subcutaneous Catheter
 The Emily Center How to Care for your Child s Indwelling Subcutaneous Catheter Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #1054
The Emily Center How to Care for your Child s Indwelling Subcutaneous Catheter Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #1054
Infection control. Self-study course
 Infection control Self-study course Course objectives By the end of this course you will be able to: 1) Define a germ 2) Define the environment that a germ needs to live and grow 3) Explain the chain of
Infection control Self-study course Course objectives By the end of this course you will be able to: 1) Define a germ 2) Define the environment that a germ needs to live and grow 3) Explain the chain of
REMOVAL OF A PICC. Possible Cause Nursing Actions Prevention
 REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
How can you protect yourself from infections?
 How can you protect yourself from infections? Your Infection Prevention Guide www.esrdncc.org Table of Contents Preventing an infection is an important part of your kidney care...3 Things you can do...4
How can you protect yourself from infections? Your Infection Prevention Guide www.esrdncc.org Table of Contents Preventing an infection is an important part of your kidney care...3 Things you can do...4
Patient Information. PORT-A-CATH Implantable Venous Access Systems
 Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
Site Care of Your Central Venous Catheter Sterile
 Site Care of Your Central Venous Catheter Sterile Dressing Change Sterile Technique The skin surrounding your catheter s exit site must be kept clean, and a new sterile dressing should be applied on a
Site Care of Your Central Venous Catheter Sterile Dressing Change Sterile Technique The skin surrounding your catheter s exit site must be kept clean, and a new sterile dressing should be applied on a
VRE. Living with. Learning how to control the spread of Vancomycin-resistant enterococci (VRE)
 VRE Living with Learning how to control the spread of Vancomycin-resistant enterococci (VRE) CONTENTS IMPORTANT VRE is a serious infection that may become life-threatening if left untreated. If you or
VRE Living with Learning how to control the spread of Vancomycin-resistant enterococci (VRE) CONTENTS IMPORTANT VRE is a serious infection that may become life-threatening if left untreated. If you or
Understanding Your. Hemodialysis. Access Options
 Understanding Your Hemodialysis Access Options aakp American Association of Kidney Patients 3505 E. Frontage Road, Suite 315 Tampa, FL 33607 Toll-Free: 800-749-2257 Fax: 813-636-8122 www.aakp.org Overview
Understanding Your Hemodialysis Access Options aakp American Association of Kidney Patients 3505 E. Frontage Road, Suite 315 Tampa, FL 33607 Toll-Free: 800-749-2257 Fax: 813-636-8122 www.aakp.org Overview
Central venous catheters. Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95
 4 Central venous catheters Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95 CARE OF THE SITE Preparation Patient Equipment/Environment Nurse Explain the
4 Central venous catheters Care of the site 88 CVP measurement 90 Removal of CVC (non-tunnelled) 93 Care of long-term CVCs 95 CARE OF THE SITE Preparation Patient Equipment/Environment Nurse Explain the
Section 6: Your Hemodialysis Catheter
 Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Lifecath Midline. A Nurses Guide to Lifecath Midline
 Lifecath Midline A Nurses Guide to Lifecath Midline vygon@vygon.co.uk www.vygon.co.uk Lifecath Midline A Nurses Guide to Lifecath Midline This booklet provides guidance in the care and maintenance of Midline
Lifecath Midline A Nurses Guide to Lifecath Midline vygon@vygon.co.uk www.vygon.co.uk Lifecath Midline A Nurses Guide to Lifecath Midline This booklet provides guidance in the care and maintenance of Midline
Home Care for Your Wound Drain
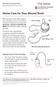 PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
Community Nurse Referral Letter (PICC Care)
 Community Nurse Referral Letter (PICC Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a PICC (Peripherally
Community Nurse Referral Letter (PICC Care) Name of nurse making the referral: Name Signature.. Date Ward.Tel 0845 1555 000 Ext. Dear Community Nurse The following patient requires care for a PICC (Peripherally
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Entity: Fairview Pharmacy Services Department: Fairview Home Infusion
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Entity: Fairview Pharmacy Services Department: Fairview Home Infusion
Living healthy with MRSA
 Stamford Health System Having MRSA means what? Living healthy with MRSA Discharge information for patients and families WASHING YOUR HANDS IS THE KEY!!! Staph aureus is a bacteria that lives on your skin
Stamford Health System Having MRSA means what? Living healthy with MRSA Discharge information for patients and families WASHING YOUR HANDS IS THE KEY!!! Staph aureus is a bacteria that lives on your skin
TREATMENT 1. Control bleeding by applying pressure over wound with Gauze Pads (Surgical Supply-4). 2. Contact Surgeon for laceration repair options.
 Page 1 of 8 pages NOTE Contact Surgeon before giving any medication marked with an asterisk. In an emergency or during Loss of Signal, begin appropriate treatment; then call Surgeon as soon as possible.
Page 1 of 8 pages NOTE Contact Surgeon before giving any medication marked with an asterisk. In an emergency or during Loss of Signal, begin appropriate treatment; then call Surgeon as soon as possible.
Peripherally Inserted Central Catheter (PICC)
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Peripherally Inserted Central Catheter (PICC) Intravenous Therapy What is a PICC? A PICC is a very fine flexible tube measuring
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Peripherally Inserted Central Catheter (PICC) Intravenous Therapy What is a PICC? A PICC is a very fine flexible tube measuring
PICC Dressing Change
 PICC Dressing Change Gather materials: Non-sterile gloves (one pair) Alcohol pads to remove old dressing (as needed) Sterile dressing change kit:(mask, gloves, 2x2" gauze pads, drape, Steri-Strips, chlorhexidine,
PICC Dressing Change Gather materials: Non-sterile gloves (one pair) Alcohol pads to remove old dressing (as needed) Sterile dressing change kit:(mask, gloves, 2x2" gauze pads, drape, Steri-Strips, chlorhexidine,
Insertion of a Central Catheter (Hickman/Groshong Catheter)
 Insertion of a Central Catheter (Hickman/Groshong Catheter) Patient Information Introduction This booklet has been written to provide information to patients about to have a central catheter inserted in
Insertion of a Central Catheter (Hickman/Groshong Catheter) Patient Information Introduction This booklet has been written to provide information to patients about to have a central catheter inserted in
The temporary haemodialysis catheter
 The temporary haemodialysis catheter Department of Renal Medicine Patient Information Leaflet Introduction The information in this booklet is for: People have renal failure and who require urgent haemodialysis.
The temporary haemodialysis catheter Department of Renal Medicine Patient Information Leaflet Introduction The information in this booklet is for: People have renal failure and who require urgent haemodialysis.
What Is. Norovirus? Learning how to control the spread of norovirus. Web Sites
 Web Sites Centers for Disease Control and Prevention (CDC) http://www.cdc.gov/norovirus/index.html Your Local Health Department http://www.azdhs.gov/diro/lhliaison/countymap.htm What Is Ocument dn Norovirus?
Web Sites Centers for Disease Control and Prevention (CDC) http://www.cdc.gov/norovirus/index.html Your Local Health Department http://www.azdhs.gov/diro/lhliaison/countymap.htm What Is Ocument dn Norovirus?
Going home after an AV Fistula or AV Graft
 Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
Caring for Your PleurX Pleural Catheter
 Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Information for patients and nurses
 Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Living with MRSA. Things to remember about living with MRSA: This is really serious. I need to do something about this now!
 Things to remember about living with MRSA: 1. Wash your hands often. 2. Take care of yourself: Eat right, exercise, quit smoking, and avoid stress. 3. Take good care of your skin. 4. Keep skin infections
Things to remember about living with MRSA: 1. Wash your hands often. 2. Take care of yourself: Eat right, exercise, quit smoking, and avoid stress. 3. Take good care of your skin. 4. Keep skin infections
Learning About MRSA. 6 How is MRSA treated? 7 When should I seek medical care?
 IMPORTANT MRSA is a serious infection that can become life-threatening if left untreated. If you or someone in your family has been diagnosed with MRSA, there are steps you need to take now to avoid spreading
IMPORTANT MRSA is a serious infection that can become life-threatening if left untreated. If you or someone in your family has been diagnosed with MRSA, there are steps you need to take now to avoid spreading
BARD MEDICAL DIVISION UROLOGICAL DRAINAGE. Foley Catheter Care & Maintenance. Patient Education Guide
 BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
Tony Melendez Version 2013 LINES, TUBES, PORTS, WHAT TO DO WITH THEM
 Tony Melendez Version 2013 LINES, TUBES, PORTS, WHAT TO DO WITH THEM Discusion of the following PICC Line Hickman Cath Chest Tubes PICC s & Midlines Classic PICC Line A PICC line is essentially a narrow
Tony Melendez Version 2013 LINES, TUBES, PORTS, WHAT TO DO WITH THEM Discusion of the following PICC Line Hickman Cath Chest Tubes PICC s & Midlines Classic PICC Line A PICC line is essentially a narrow
