Gastric cancer surgery: Billroth I or Billroth II for distal gastrectomy?
|
|
|
- Lionel Chase
- 9 years ago
- Views:
Transcription
1 Gastric cancer surgery: Billroth I or Billroth II for distal gastrectomy? Chen M M*, B K Sah *, Yan M, Zhu Z G Department of general surgery, Rui Jin hospital. Shanghai Jiao Tong University, School of medicine. Shanghai Institute of Digestive Surgery, Shanghai, China Correspondence to Prof. Zhu Zheng Gang, department of general surgery, Rui Jin hospital. 197 Rui Jin Er road. Shanghai , China. Ph: ext Fax: [email protected] * Equal contributor: First Author Running head: Billroth I or Billroth II for distal gastrectomy?
2 Abstract Background: The selection of an anastomosis method after a distal gastrectomy is a highly debatable topic; however, the available documentation lacks the necessary research based on a comparison of early postoperative complications. This study was conducted to investigate the difference of early postoperative complications between Billroth I and Billroth II types of anastomosis for distal gastrectomies. Methods: A total of 809 patients who underwent distal gastrectomies for gastric cancer during four years were included in the study. The only study endpoint was analysis of in-patients postoperative complications. The risk adjusted complication rate was compared by POSSUM (Physiological and operative severity score for enumeration of morbidity and mortality) and the severity of complications was compared by Rui Jin Hospital classification of complication. Results: Complication rate of Billroth II type of anastomosis was almost double of that in Billroth I (P=0.000). Similarly, the risk adjusted complication rate was also higher in Billroth II group. More severe complications were observed and the postoperative duration was significantly longer in Billroth II type (P=0.000). Overall expenditure was significantly higher in Billroth II type (P=0.000). Conclusions: Billroth II method of anastomosis was associated with higher rate of early postoperative complications. Therefore, we conclude that the Billroth I method should be the first choice after a distal gastrectomy as long as the anatomic and oncological environment of an individual patient allows us to perform it. However more prospective studies should be designed to compare the overall surgical outcomes of both anastomosis methods. Key words: distal gastrectomy, postoperative complications, anastomosis, Billroth I
3 Background In the surgical approach for early and selective advanced gastric cancer, the gastrectomy with D2 lymphadenectomy was justified [1-5]. However the surgery procedures for gastric cancer vary from one to another unit. The extent of surgery for gastric cancer is highly heterogeneous. Certainly there are differences in morbidity rates associated with the different extents of surgery, even though they are all commonly denoted as radical resection [6-12]. Though postoperative complications and the mortality rate after gastric cancer surgery has significantly decreased over past years, it is still considered high [13-14]. The postoperative complication rate was higher with inexperienced surgeons than with experienced surgeons, and there was a considerable difference in early surgical outcomes among different centers [15-16]. Postoperative complications were inversely correlated with the volume of patients operated on in a surgical unit [17]; the same results were published for gastric cancer surgery [18]. There are many controversies over gastric cancer surgery, but there are comparatively fewer articles which are dedicated to early postoperative complications of gastric cancer surgery [ ].Therefore research on early postoperative complications may be beneficial to give reference points that can help to optimize the success of gastric cancer surgery. There were reports of the comparison of different types of the anastomosis method after a gastrectomy, however, these reports were basically focused on investigating the bile or enteric juice reflux into the gastric remnant and esophagus
4 following a gastrectomy. The majority of these reports advocated for Roux-en-Y Reconstruction and some for Billroth I (gastroduodenostomy) method of anastomosis. Billroth II (gastro-jejunostomy) method was not supported by the results of these tests [20-26]. In our clinical practice we observed that postoperative complications were higher in the Billroth II type of anastomosis, therefore we compared the early postoperative complications of patients with the Billroth I and Billroth II type of anastomosis. The POSSUM (physiological and operative severity score for the enumeration of morbidity and mortality) scoring system [27] was applied for the risk adjusted comparison of early postoperative complications between two groups. The POSSUM system was a valid system to evaluate the risk adjusted comparison of surgical outcomes in gastric cancer surgery [18-19]. First described in 1991 by Copeland et al, POSSUM was developed as an attempt to assess the quality of surgical care [27]. This scoring system produced assessments for morbidity and mortality rates which did not significantly differ from observed rates. For the development of POSSUM system, initially 62 individual factors were assessed by a multivariate discriminant analysis to reduce the number of variables. Finally, a 12-factor physiological score(age group, Cardiac status, ECG report, Respiratory status, Systolic blood pressure, Pulse rate, Glasgow coma scale, Hemoglobin, White cell count, Urea, Sodium, Potassium) and a 6-factor operative severity score (Operative complexity, Multiple procedures, Blood loss, Peritoneal contamination, Extent of malignant spread, Elective or emergency surgery) were
5 developed. Each of the factors were graded and scored exponentially as 1, 2, 4 or 8. Logistic regression analysis yielded statistically significant equations for morbidity. Although the higher the overall POSSUM score, the greater the risk of morbidity and mortality, individual scores do not directly reflect the percentage risk [27]. Methods The data were collected directly by the comprehensive review of the original records of all patients. A total of 809 patients who underwent radical or palliative distal gastrectomies for gastric cancer during four years was included in the study (Table 1). Any pathology other than that of the gastric cancer was excluded. Total gastrectomies and any type of palliative surgery (including exploratory laparotomy and gastro-jejunal anastomosis) other than gastrectomy were excluded. The median age of the patients was 58 years (range years). All the patients with early and resectable advanced gastric cancer (without significant distant metastases) underwent radical surgery (gastrectomies with D2 lymphadenectomy). Late stage gastric cancer patients underwent a palliative gastrectomy. Because of inadequate numbers of examined lymph nodes, we could not document all the pathological data according to the TNM classification. The only study endpoint was the analysis of in-patients postoperative complications. Complications were recorded according to the definitions mentioned in POSSUM [27]. However, there were a considerable number of complications which were not covered by its definitions. Therefore any undefined complication was recorded as innominate in this study, and details were provided in separate tables.
6 Severities of all complications were stratified according to Rui Jin Hospital Classification of Complication [14, 18-19]. Patients with multiple complications were grouped into the highest level of their respective complications, e.g. a patient with minor, moderate, and severe complications was categorized into the severe complication group (Table 2). Statistical analysis The statistical analysis was performed with the Statistical Package for Social Science (SPSS) version 13.0 for Windows (SPSS, Inc, Chicago, Illinois). A chi square test was used to compare the different types of complication rates between two groups. Non-parametric methods were used to test the data without normal distribution. A P-value of less than 0.05 was considered statistically significant. Formula for risk calculation in POSSUM Morbidity: ln R/1-R = (0.16 PS) + (0.19 OSS) Where R is predicted risk. PS and OSS stands for physiological score and operative severity score respectively. The exponential analysis method was used for prediction of morbidity rate [27]. After calculation of predicted morbidity, the observed-to-predicted operative morbidity ratio (O: E ratio) was calculated separately for Billroth I and Billroth II group. An O: E ratio less than one implies a performance that was better than expected, and a ratio greater than one indicates a performance that was worse than expected [18-19].
7 Results Details of complications according to the POSSUM criteria were summarized in table 3. The sum of the individual complications was not equal to the number of total complications. Multiple complications were possible in a single patient. There was a significant difference in the complication rate between groups of patients with Billroth I and Billroth II types of anastomosis (P=0.000). The complication rate of the Billroth II type of anastomosis was almost double of that in Billroth I. Incidence of different types of postoperative infection was significantly higher in the Billroth II type. The anastomotic leak and mortality rate were also higher in the Billroth II type, though there was no statistically significant difference in those observations. There was no significant difference of malignancy status between Billroth I and Billroth II group (p=0.316). But the complication rate was significantly higher in Billroth II than Billroth I group even after controlling the malignancy status (p<0.001). To control the effect of different type of resection on postoperative complication, we calculated the complication rate separately for radical and palliative resection. The complication rate of Billroth II was significantly higher than Billroth I in group of patients who underwent standard radical gastrectomy but not in the patients who underwent palliative gastrectomy (table 4). Moreover, the ratio of observed to estimated complication was 1.03 for the Billroth II group while it was only 0.74 in the Billroth I. This revealed that the surgical outcome was poorer in the Billroth II group. There were numerous innominate complications, and most of these
8 complications were accompanied by complications described in POSSUM (table 5). The majority of patients had pleural effusion and/ or seroperitoneum. Most of them were accompanied by a low fever but lacked a pathological diagnosis of infections. There were a substantial number of patients who had a persistent or relapsing fever of unknown origin. There were a number of patients who were clinically suspected to have a minor anastomotic leak but lacked any objective evidence to support it. Though these patients were settled by conservative treatments mainly nil per os, intravenous antibiotics and total paraenteral nutrition, these cases obviously increased the burden of the surgical ward. Other complications like pancreatic fistula, chyle leak and bleeding of the anastomosis site were rare. Almost all types of innominate complications were also higher in the Billroth II type. Among cases of innominate complications, some patients did not experience any complications described in POSSUM. These complications were recorded empirically and merged to calculate different levels of complication type according to Rui Jin Hospital classification of complications. There was significant difference in severity of complications between the two groups (P=0.000). More severe complications were observed in the Billroth II type (fig.1). All of the patients were categorized into three levels according to their postoperative stay at the hospital. There were significant differences in the postoperative duration between two groups of patients (P=0.000). About 85 percent of patients were discharged successfully in less than 15 days after a smooth recovery and removal of suture in the Billroth I type (fig.2). The postoperative duration was
9 significantly longer in the Billroth II type (P=0.000). Similarly, there was a significant difference in overall expenditure between the two types of anastomosis method (P=0.000). The median expenditure value in patients with Billroth II was RMB (Chinese currency) but it was only RMB for Billroth I (fig. 3) Discussion The comparison of surgical outcome is made more difficult due to a lack of standard definitions for complications and reliable auditing methods. Simply collecting outcome data alone is not sufficient to reflect treatment quality; because to compare postoperative complication data directly, the original populations must be identical. POSSUM has been proposed as a method for standardizing patient data, so direct comparisons of surgical outcomes can be made. However there are a number of complications (e.g., pancreatic or biliary leakage, chylus leakage, ileus, enteroplegia and pulmonary complications) that are not defined in POSSUM [18-19]. Although some of these complications seem to be minor, they can markedly extend the postoperative length of stay and treatment cost and should not be ignored. Therefore POSSUM may need some modifications to be appropriate for major surgical interventions. It was a well accepted truth that the extent of surgery, especially aggressive lymph node dissection, was useless to extend overall survival. Postoperative complications were significantly related with the extent of surgery, especially with the extent of lymph node dissection. This was even proven by Japanese surgeons who
10 reported in the New England Journal of Medicine [15, 28-30]. Therefore, gastric cancer surgery should be practiced only at experienced centers, and the extent of surgeries or procedures should be tailored to the competence of surgeons in this field [18]. It is imperative for non-specialized units to follow the experience of specialized units for gastric cancer surgery. The postoperative complication rate of our hospital was in the acceptable range. A majority of our patients had a smooth recovery, and postoperative mortality was not higher than previously reported data.. Our hospital, which deals with a high work volume, is a referral center for gastric cancer in China. Our hospital prefers the Billroth I method of anastomosis over the Billroth II method, and we seldom use the Roux-en-Y method after a distal gastrectomy. Our study suggests that the early postoperative complication rate is significantly lower in Billroth I group. Despite the fact that there was not standard follow-up data, the operative surgeons in our center feel that the long term patients satisfaction is also better with the Billroth I method. The Billroth I procedure is generally simpler to perform than other methods. It is considered to be more physiologically sound by preserving the continuity of the digestive tract with the duodenum and theoretically maintaining autocrine and paracrine signaling and feedback mechanisms[31-34]. Therefore the Billroth I type of anastomosis is superior to Billroth II. The major hurdle in selecting the Billroth I method is the anatomic and oncological environment of the tumor. If the tumor is more advanced and the location is more distal to the duodenum, it is difficult to perform the Billroth I anastomosis.
11 This is because it is difficult to obtain tumor-free margins, and it may further increase the tension between anastomosis edges which may be associated with higher anastomotic leak. Interestingly enough, a higher rate of anastomotic leak was observed in the Billroth II group of this study. The overall complication rate was higher in the Billroth II group, especially the infectious complications. Intra-abdominal infection was also higher in the Billroth II group which may be the result of higher rate of postoperative pancreatitis and anastomotic leak. We trust the lower complication rate in Billroth I group may be attributed to its simplicity in terms of surgical insult and elimination of duodenal remnant which is very prone to rupture in case of distal obstruction or ileus. Also the early rupture of duodenal remnant induces peripancreatic abscess or intra-abdominal infection. However a well controlled prospective study is necessary to explore the potential factors behind the higher rate of infectious complications and anastomotic leaks. One can also argue that the difference in complication rate is simply the result of the inadequate surgical experience of the surgeon who prefers Billroth I against Billroth II, and better surgical outcome could be achieved in centers where the Billroth II is a preferred method. Though it was quite difficult to obtain a concrete answer for the choice of which anastomosis method should be preferred, the findings of this study at the very least demand further investigation into the potential causes of differences in surgical outcomes between the two different types of anastomosis. This necessitates integrative research to compare both the early and long-term aspects of the different
12 anastomosis methods. If the early postoperative outcome is better with the Billroth I method, it should be preferred for its simplicity and better physiological reconstruction. However the long-term patients satisfaction should also be taken into consideration, and operative surgeons should tailor the appropriate method in accordance with the prognosis of the tumor. The Roux-en-Y method of anastomosis was advocated by western authors [20-26] where the surgical work load was significantly lower than eastern countries like China, Korea and Japan. This method is not preferred in eastern countries including our center due to its complexity and lengthiness in comparison to the Billroth I method. Because of a higher rate of incidence of gastric cancer in the region, surgeons of a big hospital in eastern countries have to deal with a huge surgical work volume [14, 18]. Therefore it is wise to explore the simpler surgical methods for gastric cancer surgery which benefit both surgeons and patients. Conclusion The overall postoperative complication is still higher after gastric cancer surgery, though the severe complications and mortality rate are lower. The Billroth II method of anastomosis is associated with a higher rate of early postoperative complications. Therefore we conclude that the Billroth I method should be the first choice after a distal gastrectomy as long as the anatomic and oncological environment of the individual patient allows it. However more prospective studies should be designed to compare the overall surgical outcomes of both anastomosis methods.
13 Competing interests The authors declare that they have no competing interests. Authors' contributions CMM and BKS designed the study, collected the patients data and drafted the manuscript. YM and ZZG participated in the design of the study, assisted in drafting of the manuscript and performed the critical revision. All authors meet the criteria; they have read and approved the final manuscript. Acknowledgement The authors thank Shanghai Institute of Digestive Surgery for funding this research, computer engineer Mr. Dipendra Kumar Sah for designing a special POSSUM calculator and database program, the statistic bureau of Rui Jin hospital for providing records of patients, Dr. Li Chen, Yang Qiu Meng and Yao Xue Xin, for their support in interpretation of data.
14 References 1. Sano T, Sasako M, Yamamoto S, et al. Gastric cancer surgery: Morbidity and mortality results from a prospective randomized controlled trial comparing D2 and extended para-aortic lymphadenectomy Japan Clinical Oncology Group Study J Clin Oncol 2004, 22: Swan R, Miner TJ. Current role of surgical therapy in gastric cancer. World J Gastroenterol 2006, 12: Kodera Y. The beginning of a new era: East meets West more comfortably regarding lymphadenectomy for gastric cancer Japan will finally drop the surgery-alone arm in its pursuit of a multimodal treatment strategy. Gastric Cancer 2007, 10: Roviello F, Marrelli D, Morgagni P, et al. Survival benefit of extended D2 lymphadenectomy in gastric cancer with involvement of second level lymph nodes: A longitudinal multicenter study. Ann Surg Oncol 2002, 9: Biffi R, Chiappa A, Luca F, et al. Extended lymph node dissection without routine splenopancreatectomy for treatment of gastric cancer: Low morbidity and mortality rates in a single center series of 250 patients. J Surg Oncol 2006, 93: Pedrazzani C, Marrelli D, Rampone B, et al. Postoperative complications and functional results after subtotal gastrectomy with Billroth II reconstruction for primary gastric cancer. Dig Dis Sci 2007, 52: Ichikura T, Chochi K, Sugasawa H. Modified radical lymphadenectomy (D1.5) for T2 3 gastric cancer. Arch Surg 2005, 390:
15 8. Lo SS, Wu CW, Shen KH, et al. Higher Morbidity and Mortality after Combined Total Gastrectomy and Pancreaticosplenectomy for Gastric Cancer. World J. Surg 2002, 26: Yasuda K, Shiraishi N, Adachi Y. Risk factors for complications following resections of large gastric cancer. Br J Surg 2001, 88: Marrelli D, Pedrazzani C, Neri A, et al. Complications after Extended (D2) and Super extended (D3) Lymphadenectomy for Gastric Cancer: Analysis of Potential Risk Factors. Ann Surg Oncol 2007, 14: Danielson H, Kokkola A, Kiviluoto T et al. Clinical outcome after D1 vs D2-3 gastrectomy for treatment of gastric cancer. Scand J Surg 2007, 96: Yonemura Y, Wu CC, Fukushima N, et al. Operative morbidity and mortality after D2 and D4 extended dissection for advanced gastric cancer: a prospective randomized trial conducted by Asian surgeons. Hepatogastroenterology 2006, 53: Hyung WJ, Kim SS, Choi WH, Cheong JH, Choi SH, Kim CB, Noh SH. Changes in Treatment Outcomes of Gastric Cancer Surgery Over 45 Years at A Single Institution. Yonsei Med J 2008, 49: Sah BK, Zhu ZG, Chen MM, Yan M, Yin HR, Lin YZ. Gastric Cancer Surgery and its Hazards: Post operative infection is the most important complication. Hepato-Gastroenterology 2008, 55: McCulloch P, Niita ME, Kazi H. Gastrectomy with extended lymphadenectomy for primary treatment of gastric cancer. Br J Surg 2005, 92:
16 Wu CW, Chang IS, Lo SS, Hsieh MC, Chen JH, Lui WY, Whang-Peng J. Complications Following D3 Gastrectomy: Post Hoc Analysis of a Randomized Trial.World J Surg 2006, 30: Irkmeyer JDB, Siewers AE, Finlayson EVA, et al. Hospital volume and surgical mortality in the United States. N Engl J Med 2002, 346: Sah BK, Zhu ZG, Chen MM, Xiang M, Chen J, Yan M, Lin YZ. Effect of surgical work volume on postoperative complication: superiority of specialized center in gastric cancer treatment. Langenbecks Arch Surg 2009, 394: Sah BK, Zhu ZG, Wang XY, Yang QM, Chen MM, Xiang M, Chen J, Yan M. Post-operative complications of gastric cancer surgery: female gender at high risk. Eur J Cancer Care 2009, 18: Nunobe S., Okaro A., Sasako M., M. Saka, Fukagawa T., Katai H., Sano T. Billroth 1 versus Roux-en-Y reconstructions: a quality-of-life survey at 5 years. Int J Clin Oncol 2007, 12: Fukuhara K., Osugi H., Takada N, Takemura M, Higashino M, Kinoshita H. Reconstructive Procedure after Distal Gastrectomy for Gastric Cancer that Best Prevents Duodenogastroesophageal Reflux. World J. Surg 2002, 26: Csendes A, Burgos AM, Smok G, Burdiles P, Braghetto I, Díaz JC. Latest results (12 21 years) of a prospective randomized study comparing Billroth II and Roux-en-Y anastomosis after a partial gastrectomy plus vagotomy in patients with duodenal ulcers. Ann Surg 2009, 249: Shinoto K, Ochiai T, Suzuki T, Okazumi S, Ozaki M. Effectiveness of
17 Roux-en-Y Reconstruction After Distal Gastrectomy Based on an Assessment of Biliary Kinetics. Surg Today 2003, 33: Kim BJ, O'Connell T. Gastroduodenostomy after gastric resection for cancer. Am Surg 1999, 65(10): Schweizer W, Blunschi T, Gertsch P, Blumgart LH. Postoperative course following stomach resection: a comparison of Billroth I, Billroth II and Roux-en-Y resection-reconstruction. Schweiz Med Wochenschr 1990, 120(14): Chan DC, Fan YM, Lin CK, Chen CJ, Chen CY, Chao YC. Roux-en-Y reconstruction after distal gastrectomy to reduce enterogastric reflux and helicobacter pylori infection. J Gastrointest Surg 2007, 11: Copeland GP, Jones D, Walters M. POSSUM: a scoring system for surgical audit. Br J Surg 1991, 78: Sasako M, Sano T, Yamamoto S, Kurokawa Y, Nashimoto A, Kurita A, Hiratsuka M, Tsujinaka T, Kinoshita T, Arai K, Yamamura Y, Okajima K. D2 Lymphadenectomy Alone or with Para-aortic Nodal Dissection for Gastric Cancer. N Engl J Med 2008, 359: Bonenkamp JJ, Hermans J, Sasako M, van de Velde CJH. Extended lymph-node dissection for gastric cancer. N Engl J Med 1999, 340: Wu CW, Chang IS, Lo SS, Hsieh MC, Chen JH, Lui WY, Whang-Peng J. Complications following D3 gastrectomy: post hoc analysis of a randomized trial. World J Surg 2006, 30:
18 31. Le Blanc-Louvry I, Ducrotte P, Peillon C, et al. Roux-en-Y limb motility after total or distal gastrectomy in symptomatic and asymptomatic patients. J Am Coll Surg 2000, 190: Le Blanc-Louvry I, Ducrotte P, Chayvialle JA, et al. Distal gastrectomy and Roux-Y limb in the rat: plasma motilin, pancreatic polypeptide concentrations, and duodenojejunal motility. Dig Dis Sci 2000, 45: Meyer BM, Werth BA, Beglinger C, et al. Role of cholecystokinin in regulation of gastrointestinal motor functions. Lancet 1989, II: van der Mijle HC, Beekhuis H, Bleichrodt RP, et al. Transit disorders of the gastric remnant and Roux limb after Roux-en-Y gastrojejunostomy: relation to symptomatology and vagotomy. Br J Surg 1993, 80:60 64
19 Figure legends Fig. 1 Severity level of overall complications Fig. 2 Postoperative duration at hospital Fig. 3 Difference of expenditure between two groups
20 Tables Table 1 Demographic data of the patients Details Number of patients Billroth I 626 Billroth II 183 Age group (years) Sex Male Female Type of resection Radical gastrectomy Palliative gastrectomy Malignancy Primary tumor Lymph node metastasis Distant metastasis 11 3 Automatic stapler No Yes Median value PS OSS * Including recurrent gastric cancer.
21 Table 2 Rui Jin Hospital classification of complications Minor Infection: Superficial wound infection, deep infection *, chest infection *, urinary infection, septicemia, pyrexia of unknown origin * Miscellaneous: Superficial wound dehiscence, wound hemorrhage, impaired renal function *, deep venous thrombosis *, Hypotension. Moderate Infection: Deep infection, chest infection, pyrexia of unknown origin. Miscellaneous: deep wound dehiscence, impaired renal function, deep venous thrombosis Innominate Severe Systemic: Cardiac failure, Respiratory failure, pulmonary embolus, Hypotension. Death Surgical: Deep hemorrhage, deep infection, anastomotic leak Innominate: complications with postop stay >30days *(postop 15 days), (postop>15 days), (Requiring laparotomy) Except innominate, the definition for all complications was adopted from POSSUM.
22 Table 3 Detail of complications Complications Billroth I Billroth II P value Number of patients Overall complication 126(20.1) 68(37.2) Hemorrhage Deep 3(0.5) 2(1.1) NS Wound dehiscence Superficial 2(0.3) 2(1.1) NS Deep 4 0 NS Anastomotic leak 8(1.3) 6(3.3) NS Infection Wound 2(0.3) 2(1.1) NS Deep 17(2.7) 19(10.4) PUO * 82(13.1) 36(19.7) Chest 17(2.7) 15(8.2) UTI 2(0.3) 3(1.6) NS Multiple 10(1.6) 10(5.5) System failure Renal 7(1.1) 4(2.2) NS Respiratory 2(0.3) 2(1.1) NS Cardiac 2(0.3) 1(0.5) NS Hypotension 2(0.3) 1(0.5) NS DVT 0 1(0.5) NS Death 1(0.2) 2(1.1) NS *pyrexia of unknown origin, urinary tract infection, deep venous thrombosis
23 Table 4 Complication rate between Billroth I and Billroth II reconstruction Complication P value Gastrectomy Reconstruction No Yes Radical Billroth I 483(80.6) 116(19.4) <0.001 Billroth II 99(61.9) 61(38.1) Palliative Billroth I 17(63.0) 10(37.0) NS Billroth II 16(69.6) 7(30.4)
24 Table 5 Innominate complications Complications Billroth I Billroth II P value Pleural effusion 26(4.4) 14(7.7) NS Consistent fever of unknown reason 55(8.8) 26(14.2) Seroperitoneum 27(4.3) 22(12.0) Gastro or enteroplegia 19(3.0) 14(7.7) Pancreatitis 1(0.2) 9(4.9) Central vein catheter infection 6(1.0) 2(1.1) NS Anastomosis site or upper GI bleeding 1(0.2) 4(2.2) Chyle leak 1(0.2) 1(0.5) NS Pancreatic fistula 0 1(0.5) NS
25 Appendix Definitions of morbidity in POSSUM system by Copeland et al 1. Hemorrhage: Wound hemorrhage: local haematoma requiring evacuation. Deep hemorrhage: postoperative bleeding requiring re-exploration. 2. Chest infection: production of purulent sputum with positive bacteriological cultures, with or without chest radiography changes or pyrexia, or consolidation seen on chest radiograph. 3. Wound infection: wound cellulitis or the discharge of purulent exudates. 4. Urinary infection: the presence of > 10 5 bacteria / ml with the presence of white cells in the urine, in previously clear urine. 5. Deep infection: the presence of an intra-abdominal collection confirmed clinically or radiologically. 6. Septicemia: positive blood culture. 7. Pyrexia of unknown origin: any temperature above 37 C for more than 24 h occurring after the original pyrexia following surgery (if present) had settled, for which no obvious cause could be found 8. Wound dehiscence: superficial or deep wound breakdown. 9. Deep venous thrombosis and pulmonary embolus: when suspected, confirmed radiologically by venography or ventilation/ perfusion scanning or diagnosed at post mortem. 10. Cardiac failure: symptoms or signs of left ventricular or congestive cardiac failure which required an alteration from preoperative therapeutic measures.
26 11. Impaired renal function: arbitrarily defined as an increase in blood urea of > 5 mmol / l from preoperative levels. 12. Hypotension: a fall in systolic blood pressure below 90 mmhg for more than 2 H as determined by sphygmomanometer or arterial pressure transducer measurement. 13. Respiratory failure: respiratory difficulty requiring emergency ventilation. 14. Anastomotic leak: discharge of bowel content via the drain, wound or abnormal orifice.
27 Fig. 1 Severity level of overall complications 80.0% 78.75% Billroth I BillrothII 60.0% 59.56% Percent 40.0% 20.0% 21.86% 0.0% Null 8.63% 8.74% Minor 7.83% Moderate 4.79% Severe 9.84% Complications P=0.000 Figure 1
28 Fig. 2 Postoperative duration at hospital 100.0% Billroth I Billroth II 80.0% Percent 60.0% 40.0% 85.14% 62.84% 20.0% 30.6% 0.0% % % > % Postoperative days P=0.000 Figure 2
29 Fig. 3 Difference of expenditure between two groups Expenditure, RMB Billroth I Anastomosis type Billroth II P =0.000 Figure 3
30 Additional files provided with this submission: Additional file 1: Response to editor- revision 2.doc, 25K Additional file 2: Response to Reviewer 1 Prof.Shigefumi Yoshino- Revision 2.doc, 28K Additional file 3: Response to Reviewer 2 Prof. Motoki Ninomiya- Revision 2.doc, 28K Additional file 4: Response to Reviewer 3 Prof. Jianhui Cai- Revision 2.doc, 20K
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY. Dr. Shailesh V. Shrikhande
 PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
Evidence tabel Lokaal palliatieve behandelingen
 Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
The Royal Marsden. Surgery for Gastric and GE Junction Cancer: primary palliative where and when? William Allum
 The Royal Marsden Surgery for Gastric and GE Junction Cancer: primary palliative where and when? William Allum Any surgeon can cure Surgeon - dependent No surgeon can cure EMR D2 GASTRECTOMY H N SN. WEDGE
The Royal Marsden Surgery for Gastric and GE Junction Cancer: primary palliative where and when? William Allum Any surgeon can cure Surgeon - dependent No surgeon can cure EMR D2 GASTRECTOMY H N SN. WEDGE
The Whipple Procedure. Sally Hodges, Ph.D.(c) Given the length and difficulty of the procedure, regardless of the diagnosis, certain
 The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
How to treat early gastric cancer. Surgery
 How to treat early gastric cancer Surgery Mark I. van Berge Henegouwen Department of Surgery, AMC, Amsterdam Director upper GI surgical unit Academic Medical Center Upper GI surgery at AMC 100 oesophagectomies
How to treat early gastric cancer Surgery Mark I. van Berge Henegouwen Department of Surgery, AMC, Amsterdam Director upper GI surgical unit Academic Medical Center Upper GI surgery at AMC 100 oesophagectomies
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Cancer of the Cardia/GE Junction: Surgical Options
 Cancer of the Cardia/GE Junction: Surgical Options Michael A Smith, MD Associate Chief Thoracic Surgery Center for Thoracic Disease St Joseph s Hospital and Medical Center Phoenix, AZ Michael Smith, MD
Cancer of the Cardia/GE Junction: Surgical Options Michael A Smith, MD Associate Chief Thoracic Surgery Center for Thoracic Disease St Joseph s Hospital and Medical Center Phoenix, AZ Michael Smith, MD
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Open Ventral Hernia Repair
 Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
What is the Sleeve Gastrectomy?
 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Differences in type of comorbidity and complications in young and elderly
 Differences in type of comorbidity and complications in young and elderly 5.1 Relation between age, comorbidity, and complications in patients undergoing major surgery for head and neck cancer Peters TTA
Differences in type of comorbidity and complications in young and elderly 5.1 Relation between age, comorbidity, and complications in patients undergoing major surgery for head and neck cancer Peters TTA
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality. Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006
 The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
Survival analysis of 220 patients with completely resected stage II non small cell lung cancer
 窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
INTERVENTIONAL PROCEDURES PROGRAMME
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
Columbia University Mesothelioma Applied Research Foundation - 2009 - www.curemeso.org. Mesothelioma Center www.mesocenter.org
 Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
GIANT HERNIA REPAIR MY EXPERIENCE
 GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
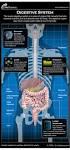 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Ching-Yao Yang, Yu-Wen Tien
 Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Historical Basis for Concern
 Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
The Role of Laparoscopy in Endometrial Cancer
 The Role of Laparoscopy in Endometrial Cancer Prof. Dr. Tugan BEŞE İstanbul University, Cerrahpaşa Medical Faculty Gynecologic Oncology Department Surgical staging in Endometrial Cancer Laparoscopic surgery
The Role of Laparoscopy in Endometrial Cancer Prof. Dr. Tugan BEŞE İstanbul University, Cerrahpaşa Medical Faculty Gynecologic Oncology Department Surgical staging in Endometrial Cancer Laparoscopic surgery
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of
 Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES.
 PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
Objectives. Preoperative Cardiac Risk Stratification for Noncardiac Surgery. History
 Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Stomach (Gastric) Cancer. Prof. M K Mahajan ACDT & RC Bathinda
 Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
Results of Surgery in a New Lung Institute in South Texas Focused on the Treatment of Lung Cancer
 Results of Surgery in a New Lung Institute in South Texas Focused on the Treatment of Lung Cancer Lung cancer accounts for 13% of all cancer diagnoses and is the leading cause of cancer death in both males
Results of Surgery in a New Lung Institute in South Texas Focused on the Treatment of Lung Cancer Lung cancer accounts for 13% of all cancer diagnoses and is the leading cause of cancer death in both males
The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx:
 James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
Peritoneal Surface Malignancies. Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA
 Peritoneal Surface Malignancies Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA Cancer dissemination routes Hematogenous metastases Lymphatic metastases Implants on peritoneal surfaces Surgically
Peritoneal Surface Malignancies Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA Cancer dissemination routes Hematogenous metastases Lymphatic metastases Implants on peritoneal surfaces Surgically
Kanıt: Klinik çalışmalarda ZYTIGA
 mkdpk de Sonunda Gerçek İlerleme! Kanıt: Klinik çalışmalarda ZYTIGA Dr. Sevil Bavbek 5. Türk Tıbbi Onkoloji Kongresi Mart 214, Antalya Endocrine therapies Adrenals Testis Abiraterone Orteronel Androgen
mkdpk de Sonunda Gerçek İlerleme! Kanıt: Klinik çalışmalarda ZYTIGA Dr. Sevil Bavbek 5. Türk Tıbbi Onkoloji Kongresi Mart 214, Antalya Endocrine therapies Adrenals Testis Abiraterone Orteronel Androgen
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Preoperative drainage is always indicated in malignant CBD strictures PRO. Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany
 Preoperative drainage is always indicated in malignant CBD strictures PRO Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany Background Jaundice is associated with high perioperative morbidity
Preoperative drainage is always indicated in malignant CBD strictures PRO Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany Background Jaundice is associated with high perioperative morbidity
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach
 Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
Demographics. MBSAQIP Case Number: IDN: ACS NSQIP Case Number:
 Demographics *LMRN: *DOB: / / *Gender: Male Female *Race: White Native Hawaiian/Other Pacific Islander Black or African American Asian American Indian or Alaska Native Unknown *Hispanic Ethnicity: Unknown
Demographics *LMRN: *DOB: / / *Gender: Male Female *Race: White Native Hawaiian/Other Pacific Islander Black or African American Asian American Indian or Alaska Native Unknown *Hispanic Ethnicity: Unknown
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
INFORMED CONSENT FOR POSSIBLE REMOVAL OF ADJUSTABLE GASTRIC BAND AND CONVERSION TO ROUX-EN-Y GASTRIC BYPASS SURGICAL PROCEDURE
 INFORMED CONSENT FOR POSSIBLE REMOVAL OF ADJUSTABLE GASTRIC BAND AND CONVERSION TO ROUX-EN-Y GASTRIC BYPASS SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand
INFORMED CONSENT FOR POSSIBLE REMOVAL OF ADJUSTABLE GASTRIC BAND AND CONVERSION TO ROUX-EN-Y GASTRIC BYPASS SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand
Guidelines for Management of Renal Cancer
 Guidelines for Management of Renal Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Section 5 updated bullets 5.3 and 5.4 Section 6 updated
Guidelines for Management of Renal Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Section 5 updated bullets 5.3 and 5.4 Section 6 updated
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE
 INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi
 Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
2016 Physician Quality Reporting System Data Collection Form: General Surgery (for patients aged 18 and older)
 2016 Physician Quality Reporting System Data Collection Form: General Surgery (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
2016 Physician Quality Reporting System Data Collection Form: General Surgery (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
Luis D. Carcorze Soto, MD PGY-3
 Luis D. Carcorze Soto, MD PGY-3 Peritoneal Surface Malignancies Peritoneum Patient Selection Operative Technique HIPEC EPIC Primary: Primary Peritoneal Carcinoma Malignant Peritoneal Mesothelioma Metastatic:
Luis D. Carcorze Soto, MD PGY-3 Peritoneal Surface Malignancies Peritoneum Patient Selection Operative Technique HIPEC EPIC Primary: Primary Peritoneal Carcinoma Malignant Peritoneal Mesothelioma Metastatic:
The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass
 ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
The Evolution of Bariatric Surgery. History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics
 The Evolution of Bariatric Surgery History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics It s a BIG Problem & it s Getting Worse Obesity is now a disease
The Evolution of Bariatric Surgery History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics It s a BIG Problem & it s Getting Worse Obesity is now a disease
Surgery for Advanced Gastric Cancer
 Surgery for Advanced Gastric Cancer Ken-ichi Mafune Introduction Ever since the first successful gastrectomy was performed by C. Billroth in 1881, surgery has been the only hope of cure for gastric cancer.
Surgery for Advanced Gastric Cancer Ken-ichi Mafune Introduction Ever since the first successful gastrectomy was performed by C. Billroth in 1881, surgery has been the only hope of cure for gastric cancer.
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Abstract Background Methods:
 Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Adjuvant Therapy Non Small Cell Lung Cancer. Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015
 Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Life Insurance Application Form
 Life Insurance Application Form INSTRUCTION To be completed by all applicants PERSONAL DETAILS Surname First name Middle name Sex Female Male Marital status (please tick) Single Married Other Current residential
Life Insurance Application Form INSTRUCTION To be completed by all applicants PERSONAL DETAILS Surname First name Middle name Sex Female Male Marital status (please tick) Single Married Other Current residential
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Gallstone Ileus. Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005
 Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
Oxford University Hospitals
 Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
CONTEMPORARY MANAGEMENT OF RENAL ANGIOMYOLIPOMA
 CONTEMPORARY MANAGEMENT OF RENAL ANGIOMYOLIPOMA Stephen A. Boorjian, MD Professor of Urology Vice Chair of Research Director, Urologic Oncology Fellowship Department of Urology Mayo Clinic, Rochester,
CONTEMPORARY MANAGEMENT OF RENAL ANGIOMYOLIPOMA Stephen A. Boorjian, MD Professor of Urology Vice Chair of Research Director, Urologic Oncology Fellowship Department of Urology Mayo Clinic, Rochester,
ONTARIO SUPERIOR COURT OF JUSTICE
 (PRECEDENT STATEMENT OF CLAIM C ) Court File No. ONTARIO SUPERIOR COURT OF JUSTICE BETWEEN: **************, *********** and ************* and Plaintiffs **********HOSPITAL, DR. *************, DR. **********,
(PRECEDENT STATEMENT OF CLAIM C ) Court File No. ONTARIO SUPERIOR COURT OF JUSTICE BETWEEN: **************, *********** and ************* and Plaintiffs **********HOSPITAL, DR. *************, DR. **********,
Bowel Preparation for Colon Resection. Eric Klein, M.D. SUNY Downstate Department of Surgery
 Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
Canine Lymphoma Frequently Asked Questions by Pet Owners
 Canine Lymphoma Frequently Asked Questions by Pet Owners What is lymphoma? The term lymphoma describes a diverse group of cancers in dogs that are derived from white blood cells called lymphocytes. Lymphocytes
Canine Lymphoma Frequently Asked Questions by Pet Owners What is lymphoma? The term lymphoma describes a diverse group of cancers in dogs that are derived from white blood cells called lymphocytes. Lymphocytes
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD
 SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery
 Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group
 Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group Lotte Holm Land MD, ph.d. Onkologisk Afd. R. OUH Kræft og komorbiditet - alle skal
Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group Lotte Holm Land MD, ph.d. Onkologisk Afd. R. OUH Kræft og komorbiditet - alle skal
Endoscopic therapy for obesity and complications of bariatric surgery
 Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
EMR Can anyone do this?
 EMR Can anyone do this? Norio Fukami, MD University of Colorado Piecemeal resection? 1 Endoscopic mucosal resection (EMR) and Endoscopic submucosal dissection (ESD) Endoscopic removal of premalignant or
EMR Can anyone do this? Norio Fukami, MD University of Colorado Piecemeal resection? 1 Endoscopic mucosal resection (EMR) and Endoscopic submucosal dissection (ESD) Endoscopic removal of premalignant or
O. A. Khan, K. M. Reddy Department of Upper GI Surgery, St George s Hospital, London, UK
 BARIATRIC SURGERY: A MEDICOLEGAL PERSPECTIVE O. A. Khan, K. M. Reddy Department of Upper GI Surgery, St George s Hospital, London, UK Correspondence: Omar Khan, Department of Upper GI Surgery, St George
BARIATRIC SURGERY: A MEDICOLEGAL PERSPECTIVE O. A. Khan, K. M. Reddy Department of Upper GI Surgery, St George s Hospital, London, UK Correspondence: Omar Khan, Department of Upper GI Surgery, St George
COMMISSIONING. for ULTRA-RADICAL SURGERY ADVANCED OVARIAN CANCER
 COMMISSIONING for ULTRA-RADICAL SURGERY in ADVANCED OVARIAN CANCER WHY THIS MUST HAPPEN PERSPECTIVE COMMISSIONING FOR WHO, FOR WHAT? Biological Basis Surgical Basis International and national standards
COMMISSIONING for ULTRA-RADICAL SURGERY in ADVANCED OVARIAN CANCER WHY THIS MUST HAPPEN PERSPECTIVE COMMISSIONING FOR WHO, FOR WHAT? Biological Basis Surgical Basis International and national standards
Current Status and Perspectives of Radiation Therapy for Breast Cancer
 Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
SE5h, Sepsis Education.pdf. Surviving Sepsis
 Surviving Sepsis 1 Scope and Impact of the Problem: Severe sepsis is a major healthcare problem that affects millions of people around the world each year with an extremely high mortality rate of 30 to
Surviving Sepsis 1 Scope and Impact of the Problem: Severe sepsis is a major healthcare problem that affects millions of people around the world each year with an extremely high mortality rate of 30 to
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
The value of Modified Early Warning Score (MEWS) in surgical in-patients: a prospective observational study
 The Royal College of Surgeons of England GENERAL SURGERY doi 10.1308/003588406X130615 The value of Modified Early Warning Score (MEWS) in surgical in-patients: a prospective observational study J GARDNER-THORPE
The Royal College of Surgeons of England GENERAL SURGERY doi 10.1308/003588406X130615 The value of Modified Early Warning Score (MEWS) in surgical in-patients: a prospective observational study J GARDNER-THORPE
Surgical Management of Papillary Microcarcinoma 趙 子 傑 長 庚 紀 念 醫 院 林 口 總 院 一 般 外 科
 Surgical Management of Papillary Microcarcinoma 趙 子 傑 長 庚 紀 念 醫 院 林 口 總 院 一 般 外 科 Papillary microcarcinoma of thyroid Definition latent aberrant thyroid occult thyroid carcinoma latent papillary carcinoma)
Surgical Management of Papillary Microcarcinoma 趙 子 傑 長 庚 紀 念 醫 院 林 口 總 院 一 般 外 科 Papillary microcarcinoma of thyroid Definition latent aberrant thyroid occult thyroid carcinoma latent papillary carcinoma)
Whipple Procedure: A guide for patients and families UHN
 Whipple Procedure: A guide for patients and families UHN Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2014 University Health Network. All rights
Whipple Procedure: A guide for patients and families UHN Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2014 University Health Network. All rights
Why a loop and new approach makes sense!
 IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results
 Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Date: 06/06/2014 Our ref: 4496. I write in response to your request for information in relation to treatment for endometrial cancer in NHS Lothian.
 Lothian NHS Board Waverley Gate 2-4 Waterloo Place Edinburgh EH1 3EG Telephone 0131 536 9000 Fax 0131 536 9088 www.nhslothian.scot.nhs.uk Date: 06/06/2014 Our ref: 4496 Enquiries to: Bryony Pillath Extension:
Lothian NHS Board Waverley Gate 2-4 Waterloo Place Edinburgh EH1 3EG Telephone 0131 536 9000 Fax 0131 536 9088 www.nhslothian.scot.nhs.uk Date: 06/06/2014 Our ref: 4496 Enquiries to: Bryony Pillath Extension:
Clinical Practice Assessment Robotic surgery
 Clinical Practice Assessment Robotic surgery Background: Surgery is by nature invasive. Efforts have been made over time to reduce complications and the trauma inherently associated with surgery through
Clinical Practice Assessment Robotic surgery Background: Surgery is by nature invasive. Efforts have been made over time to reduce complications and the trauma inherently associated with surgery through
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
