PRGF -Endoret Technology BTI Implant systems. Scientific Dossier. Prince Felipe Award for Technological Innovation
|
|
|
- Michael Rodgers
- 10 years ago
- Views:
Transcription
1 BTI Implant systems Scientific Dossier Prince Felipe Award for Technological Innovation
2
3 Introduction Introduction This scientific dossier summarises the series of indexed international articles published over the last 15 years on the range of products and technologies developed by BTI Biotechnology Institute. It highlights the vast amount of scientific evidence that backs the biosafety and effectiveness of plasma rich in growth factors (PRGF -Endoret ) in many fields of medicine, with a particular focus on oral and maxillofacial surgery and oral implantology. This autologous technology has revolutionised the field of personalised regenerative medicine, as with the patient's blood we can obtain different therapeutic formulations rich in growth factors, the application of which encourages healing and tissue regeneration, reducing pain and inflammation. Many publications show the predictability and safety of BTI dental implants and of the surgical techniques (sinus elevation, split, biological drilling, etc) developed under a biological philosophy by Dr. Eduardo Anitua. This dossier also reviews the therapeutic potential of PRGF -Endoret in other fields of medicine in which our research team has been a pioneer at a worldwide level: orthopaedic surgery, treatment of chronic ulcers and facial regeneration, among others.
4 What are growth factors and how do they act? Growth factors are a set of substances that carry out an important function in intercellular communication. They carry out a large number of biological functions among which cellular proliferation is important, though they also decisively affect cellular survival, migration, differentiation and even apoptosis. Growth factors carry out their function at very low concentrations in body fluids and tissues, in the region of pico or nanograms. They act by binding to receptors located on the cell membrane that transmit the signal from the exterior to the interior of the cell, through the coupling of different protein kinases that are phosphorylated and which regulate a signalling cascade that ends up with the activation of one or more genes.
5 Growth factors are a set of substances that are fundamental for communication between cells. BTI Biotechnology Institute S.L.
6 How can tissues be regenerated? The process of tissue regeneration includes a complex set of biological events controlled by the action and synergy of a cocktail of growth factors. There are three agents involved in tissue regeneration: the cellular component, a combination of multiple biological mediators that include growth factors and cytokines among others and a matrix or scaffold that gives the new tissue under construction support. After an injury or tissue damage, they are activated and coordinate a large number of intercellular or intracellular paths with the aim of restoring the integrity of the tissue and its hemostasis. Growth factors are also necessary to promote angiogenesis or the formation of blood vessels that will supply oxygen and nutrients to the damaged tissue. Another fundamental aspect to be considered in the regeneration of a tissue is the development of a scaffold that acts as a provisional extracellular matrix and therefore houses the cells as well as locally presenting the biochemical, physical and structural signals that allow the anchorage of the cellular motility machinery. Werner S, Grose R. Regulation of wound healing by growth factors and cytokines. Physiol. Rev. 2003;83:
7 BTI Biotechnology Institute S.L. The tissue regeneration process is based on the combination of cells, growth factors and a matrix or Scaffold. Orive BIOGRAPHY: G, Anitua * Anitua E, et al. E, Biomaterials Sánchez M, Nurden for promoting AT, Nurden brain P, protection, Orive G, Andía repair I. New and insights regeneration. into and Nat Rev novel Neurosci. applications 2009;9: for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
8 PRGF -Endoret : A new concept in personalised regenerative medicine Over the last 15 years, the detailed study of platelets, of biological mediators contained in them and of the formulations aimed at allowing the administration and therapeutic use of growth factors and autologous biomaterials has allowed significant progress and has greatly increased the versatility and therapeutic possibilities of Plasma Rich in Growth Factors (PRGF -Endoret ) technology. PRGF -Endoret technology is based on the preparation of platelet-rich 100% autologous plasma the application of which to damaged tissue areas speeds up the regeneration of a large number of tissues without any adverse effects. Plasma rich in growth factors (PRGF - Endoret ) is a personalised technology that has revolutionised the field of regenerative medicine. This article, published in one of the most prestigious journals in the field of biotechnology, summarises the most important clinical results obtained with PRGF -Endoret. Its application over the last decade has extended to many fields of medicine, from oral and maxillofacial surgery to dermatology, cosmetics, orthopaedic surgery and sports medicine, and more recently to ophthalmology. Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol. 2006;24:
9 BTI Biotechnology Institute S.L.
10 How is PRGF -Endoret obtained? The set of therapeutic formulations of PRGF -Endoret are obtained by means of a simple protocol based on a tiny volume of the patient's blood. The blood is centrifuged (580g) in 9 ml citrated tubes during 8 minutes allowing the separation of red and white blood cells from the platelet-rich plasma. The two fractions of PRGF -Endoret are separated from the rest of the blood components by means of the plasma transfer device (PTD). Later, and prior to its therapeutic application, the fractions of PRGF -Endoret are activated with calcium chloride, leading to a series of therapeutic formulations. The process to obtain PRGF -Endoret is simple and easily reproducible. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua E. Plasma rich in growth factors: preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants. 1999;14:
11 BTI Biotechnology Institute S.L.
12 Versatility of PRGF -Endoret This article, published in of the most important scientific journals in the field of biomaterials, focuses on the enormous versatility that PRGF -Endoret technology offers, as by using the patient's blood we can obtain up to 4 biocompatible formulations: a. PRGF -Endoret supernatant: used to cultivate primary cells and stem cells in the laboratory, it is also the base of a new collyrium for treating a large number of pathologies of the occular surface. b. Liquid PRGF -Endoret : Ideal for infiltrations in skin, musculoskeletal system tissues, TMJ, etc. It is the perfect tool to bioactivate dental implants and prostheses of all types with the aim of accelerating their osseointegration. c. PRGF -Endoret clot or scaffold : Ideal to fill in defects and promote tissue regeneration: post-extraction, treatment of ulcers, tissue engineering, etc. d. Fibrin membrane: due to its hemostatic properties it is the best biomaterial to seal defects and stimulate epithelisation. Anitua E, Sánchez M, Orive G, Andía I. The potential impact of the preparation rich in growth factors (PRGF) in different medical fields. Biomaterials. 2007;28:
13 a b BTI Biotechnology Institute S.L. c d The versatility of PRGF -Endoret technology allows you to obtain up to 4 autologous formulations. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
14 Why does PRGF -Endoret work? The biological activity of the different formulations obtained with PRGF -Endoret technology is based on two fundamental pillars. On the one hand, the content in plasma and in particular platelet growth factors whose action regulates the main processes involved in tissue regeneration. the most important in the field of pharmacology, talks about the therapeutic potential of PRGF -Endoret technology and in particular describes how the perfect synergy between growth factors and fibrin is a key aspect when explaining the clinical results obtained with this autologous technology. On the other, the fibrin matrix, which is used as a provisional structure to house the cells and control the release kinetics of the growth factors present in PRGF -Endoret. Anitua E, Sánchez M, Orive G, Andia I. Delivering growth factors for therapeutics. Trends Pharmacol Sci. 2008;29:37-41 This article published in the prestigious journal Trends in Pharmacological Science, BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
15 BTI Biotechnology Institute S.L.
16 What makes PRGF -Endoret different to other platelet-rich plasmas? PRGF -Endoret is the first 100% autologous platelet-rich plasma to be described in literature worldwide. It is, likewise, a pioneering technology in translational regenerative medicine. Over 15 years of research, added to its exclusive properties, make PRGF -Endoret a unique technique. PRGF -Endoret is prepared with small volumes of the patient's blood and does not require the use of thrombin or chemical agents for its activation. Unlike other products, it does not include white blood cells (leukocytes) in its composition, which gives it more effective anti-inflammatory properties. It is the most versatile technology, as its multiple formulations offer a large number of therapeutic applications. In short, as shown by the series of letters to the editor published during recent years, we can define PRGF -Endoret as a platelet-rich autologous plasma whose effectiveness and safety have been widely proven. However, it is important to remember that not all platelet-rich plasmas are PRGF -Endoret. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video.
17 Anitua E, Sánchez M, Orive G, Andía I. Shedding light in the controversial terminology for platelet rich products. J Biomed Mater Res A. 2009;90: Sánchez M, Anitua E, Andia I. Poor standardization in platelet-rich therapies hampers advancement. Arthroscopy. 2010;26: Anitua E, Sánchez M, Orive G. The importance of understanding what is platelet-rich growth factor (PRGF) and what is not. J Shoulder Elbow Surg. 2011;20: Anitua E, Sánchez M, Prado R, Orive G. Plasma rich in growth factors: the pioneering autologous technology for tissue regeneration. J Biomed Mater Res A. 2011;97:536. BTI Biotechnology Institute S.L. Anitua E, Sánchez M, Prado R, Orive G. The P makes the difference in plasma rich in growth factors (PRGF) technology. Platelets. 2011;22: BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
18 The pillars of PRGF -Endoret : growth factors PRGF -Endoret contains a cocktail of autologous growth factors that proceed from both the plasma and the platelets. In fact, the platelets have a complex storage system in the form of intracellular granules that allow them to transport a large number of biologically active molecules. According to some authors, this list of proteins and peptides can come close to 500 molecules. Alpha (α) granules are the most abundant as there are around 40 to 80 alpha granules per platelet, but they are also the ones with the greatest retention capacity. In addition, they contain a series of antibacterial proteins that are generically called thrombocidines and which are lethal for a large variety of bacterial species. However, it is important to remember that the plasma contains important growth factors and that the combination of the plasma and platelet factors is a key element in the biological action of PRGF -Endoret. Anitua E, Andia I, Ardanza B, Nurden P, Nurden AT. Autologous platelets as a source of proteins for healing and tissue regeneration. Thromb Haemost. 2004;91:4-15.
19 BTI Biotechnology Institute S.L. El PRGF -Endoret contains hundreds of molecules including plasma and platelet growth factors. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
20 Platelets and PRGF -Endoret In a couple of revision articles, our research team along with the Nurden Doctors from the Reference Centre for Platelet Disorders in France, have characterised the protein content of platelets in order to learn about the set of molecules present in PRGF -Endoret formulations. factor, EGF: epidermal growth factor or angiopoietin-1 among others. They release in parallel antibacterial molecules and specific growth factors that act on the mobilisation of progenitor cells from the bone marrow or from peripheral niches. Platelets release substances that promote tissue regeneration and which modulate both angiogenesis and inflammation. Important among other factors we have PDGF: plateletderived growth factor, TGF-ß: transforming growth factor ß, bfgf: basic fibroblast growth factor, VEGF: vascular endothelial growth Nurden AT, Nurden P, Sanchez M, Andia I, Anitua E. Platelets and wound healing. Front Biosci. 2008;13:
21 BTI Biotechnology Institute S.L. Platelets release growth factors responsible for coordinating the regenerative tissue response. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
22 The pillars of PRGF -Endoret : fibrin as a biomaterial Calcium acts as a cofactor in the activation process of PRGF -Endoret, which allows the conversion of the fibrinogen of the plasma into fibrin, generating a gel or clot with important biological functions. On the one hand, fibrin is an excellent matrix to maintain and house the cells, it acts as a provisional scaffold while the definitive tissue is regenerated and acts as a continuous growth factor release system. It is therefore a biocompatible and autologous sponge full of growth factors and cytokines that will permit a progressive release of them during several weeks. The fibrin obtained with PRGF -Endoret technology is probably the best biomaterial for encouraging tissue regeneration. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua E, Sanchez M, Nurden AT, Zalduendo M, de la Fuente M, Orive G, Azofra J, Andia I. Autologous fibrin matrices: a potential source of biological mediators that modulate tendon cell activities. J Biomed Mater Res A. 2006;77:
23 BTI Biotechnology Institute S.L. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
24 Biological and regenerative potential of PRGF -Endoret In over a decade of preclinical research, during which tens of cellular phenotypes were studied, we have managed to discover and understand the multiple biological functions that the set of therapeutic formulations of PRGF -Endoret carry out. The biological mediators of PRGF -Endoret stimulate and encourage such important processes for tissue regeneration as cellular proliferation and migration, chemotaxis (or the call from a distance for cells to go to the location of the injury), inflammation and the auto/paracrine synthesis of new molecules with biological activity. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua E, Sanchez M, Merayo-Lloves J, De la Fuente M, Muruzabal F, Orive G. Plasma rich in growth factors (PRGF-Endoret) stimulates proliferation and migration of primary keratocytes and conjunctival fibroblasts and inhibits and reverts TGF-beta1- Induced myodifferentiation. Invest Ophthalmol Vis Sci. 2011;52: Anitua E, Prado R, Orive G. Bilateral sinus elevation evaluating plasma rich in growth factors technology: a report of five cases. Clin Implant Dent Relat Res. 2012;14:51-60 Bendinelli P, Matteucci E, Dogliotti G, Corsi MM, Banfi G, Maroni P, Desiderio MA. Molecular basis of anti-inflammatory action of platelet-rich plasma on human chondrocytes: mechanisms of NF-κB inhibition via HGF. J Cell Physiol. 2012;225:
25 BTI Biotechnology Institute S.L.
26 PRGF -Endoret in the field of stem cells The growing interest in the range of biological options that PRGF -Endoret offers has even reached the field of stem cells. Stem or progenitor cells are characterised on the one hand by their unlimited capacity for proliferation, and on the other by the possibility of undergoing asymmetrical division (that is, self-renovation) maintaining their stemness while at the same time they can differentiate to diverse types of cells. There are different types of stem cells depending on their origin and their anatomical location. There is evidence that the content of biologically active agents in PRGF -Endoret affects the mobilisation, adhesion, proliferation, survival, activation and differentiation of mesenchymal stem cells and other subtypes of precursor cells. In addition, the cocktail of growth factors of PRGF -Endoret is an ideal resource for the cultivation and expansion of stem cells in the laboratory.
27 BTI Biotechnology Institute S.L. de Boer HC, Verseyden C, Ulfman LH, Zwaginga JJ, Bot I, Biessen EA, Rabelink TJ, van Zonneveld AJ. Fibrin and activated platelets cooperatively guide stem cells to a vascular injury and promote differentiation towards an endothelial cell phenotype. Arterioscler Thromb Vasc Biol. 2006;26: Kajikawa Y, Morihara T, Sakamoto H, Matsuda KI, Oshima Y, Yoshida A, Nagae M, Arai Y, Kawata M, Kubo T. Plateletrich plasma enhances the initial mobilization of circulation-derived cells for tendon healing. J Cell Physiol. 2008;215: Zhang J, Wang JH. Platelet-rich plasma releasate promotes differentiation of tendon stem cells into active tenocytes. Am J Sports Med. 2010;38: Cenni E, Avnet S, Fotia C, Salerno M, Baldini N. Platelet-rich plasma impairs osteoclast generation from human precursors of peripheral blood. J Orthop Res. 2010;28: Chen L, Dong SW, Liu JP, Tao X, Tang KL, Xu JZ. Synergy of tendon stem cells and platelet-rich plasma in tendon healing. J Orthop Res BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
28 Mechanism of action of PRGF -Endoret The use of growth factors and autologous fibrin for regenerative purposes represents a new approach to personalised medicine that a large number of patients could benefit from. In this paper, published in one of the most important journals of drug delivery, they discuss the mechanisms of action through which PRGF -Endoret produces its multiple therapeutic effects. Likewise, also important is the angiogenic action of the growth factors which is crucial to start regeneration. Last of all, though no less important, its anti-inflammatory and antibacterial properties are a key element. The stimulation of cell proliferation and migration along with the call to circulating cells to come to the location of the injury are basic aspects of the action of PRGF -Endoret. Anitua E, Orive G. Endogenous regenerative technology using plasma- and platelet-derived growth factors. J Control Release
29 BTI Biotechnology Institute S.L.
30 Bacteriostatic potential of PRGF -Endoret Our research team has proven that PRGF -Endoret presents bacteriostatic activity with a large number of bacterial and fungal strains. This is because the platelets contain a series of antibacterial proteins called thrombocidines. These proteins are part of a wider family known as defensins, and they are of a cationic nature, which will allow them to bind to and alter bacterial membranes. In addition to thrombocidines, platelets transport and release other antimicrobial peptides among which we should mention platelet factor 4, RANTES, tissue activating peptide 3, the basic protein of platelets, thymosin β-4, and fibrinopeptides A and B. In a recent paper we could see that the bacteriostatic potential of platelet-rich growth factors is due both to the antimicrobial peptides and to the fibrin, and not to the presence of leukocytes in their composition. In fact, the bacteriostatic effect of PRGF -Endoret is identical to that of a platelet and leukocyte-rich plasma. Another important conclusion of this study was to confirm how the inclusion of leukocytes notably alters the structure and uniformity of the fibrin matrix. Anitua E, Alonso R, Girbau C, Aguirre JJ, Muruzabal F, Orive G. Antibacterial effect of plasma rich in growth factors (PRGF) against Staphylococcus aureus and epidermidis strains. Clin Exp Dermatol
31 BTI Biotechnology Institute S.L. PRGF -Endoret presents bacteriostatic activity with a variety of bacterial strains. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
32 Therapeutic applications of PRGF -Endoret This revision article is a reference in international bibliography as it is the journal with the greatest scientific impact. It is about the therapeutic potential of plateletrich plasma, and in this specific case, PRGF - Endoret. This dossier summarises the preclinical and clinical scientific articles that endorse the biosafety and efficacy of PRGF -Endoret in many fields of medicine. The use of growth factors and autologous fibrin for regenerative purposes represents a new approach to personalised medicine that a large number of patients could benefit from. Anitua E, Sánchez M, Orive G. Potential of endogenous regenerative technology for in situ regenerative medicine. Adv Drug Deliv Rev. 2010;62:
33 BTI Biotechnology Institute S.L.
34 Field of Oral Surgery Introduction The versatility of PRGF -Endoret has allowed its use in the treatment of a wide range of clinical problems within the field of oral and maxillofacial surgery. An example of this is the following series of applications developed by our research team over the last two decades and summarised in the scientific dossier. From the treatment of the alveolus post-extraction to the use of this technology in gingival recessions or in the humectation of dental implants to encourage their osseointegration, the range of therapeutic possibilities is enormous. The possibility that PRGF -Endoret offers of working with a liquid formulation, with a three-dimensional matrix or a with retracted fibrin membrane drastically increases the number of therapeutic options and applications. We must not forget that thanks to its agglutinant properties, PRGF -Endoret technology is the perfect fellow traveller to prepare grafts, whether they are autologous bone, allogenic or any other biomaterial for bone regeneration.
35 BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
36 Surface bioactivation Preclinical Research In the late 90s Dr. Anitua developed a pioneering technique to humectate implants and bioactivate their surface with fibrin and autologous growth factors. In a simple procedure, the implants are soaked in freshly activated liquid PRGF- Endoret and in this way a fibrin membrane full of growth factors is generated that will encourage a faster osseointegration of the implants. The nano-rough surface of BTI implants is specially designed to boost the biological effects of PRGF -Endoret. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua EA. Enhancement of osseointegration by generating a dynamic implant surface. J Oral Implantol. 2006;32:72-76.
37 BTI Biotechnology Institute S.L.
38 Surface bioactivation Preclinical Research In this study carried out with research animals the aim was to determine whether the humectation of the implant surfaces with PRGF -Endoret encouraged their osseointegration. To this end a total of 23 implants were inserted in the tibia/radius of 3 goats; 13 of them were previously humectated with PRGF -Endoret while the other 10 were not (control). 8 weeks later, a histomorphometric analysis was carried out on the bone biopsies of the sacrificed animals and we observed that the value of the bone-implant contact (BIC) was 51.28% in the animals humectated with PRGF -Endoret, as opposed to 21.89% in the implants that were not humectated, generating a significantly greater area in the former (p<0.01). These results prove how the humectation of implants with PRGF -Endoret encourages their faster osseointegration. Anitua E, Orive G, Pla R, Roman P, Serrano V, Andía I. The effects of PRGF on bone regeneration and on titanium implant osseointegration in goats: a histologic and histomorphometric study. J Biomed Mater Res A. 2009;91:
39 BTI Biotechnology Institute S.L. Humectation of BTI implants with PRGF -Endoret encourages faster osseointegration. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
40 Surface bioactivation Preclinical Research This new study carried out on research animals evaluated the effect of humectation of dental implants with PRGF -Endoret to encourage and accelerate their osseointegration. To this end 2 dogs were used in which 12 implants were inserted, 6 on each side of the mandible, humectating the implants of one side with PRGF -Endoret, and placing the implants of the opposite side without humectation (control). After 12 weeks, the implants were extracted along with the adjacent bone for a histologicalhistomorphometric analysis. The results showed that the implants humectated with PRGF -Endoret presented higher levels of BIC (bone-impant contact). We also observed higher values of trabecular bone thickness and bone maturity in the areas treated with PRGF -Endoret. Birang R, Tavakoli M, Shahabouei M, Torabi A, Dargahi A, Soolari A. Investigation of peri-implant bone healing using autologous plasma rich in growth factors in the canine mandible after 12 weeks: a pilot study. Open Dent J. 2011;5:
41 BTI Biotechnology Institute S.L. The aim of this study was to assess both the morphology and the composition of the interface formed by the implants activated with PRGF -Endoret. Both features are of capital importance for later regenerative events as both the morphology and the composition of the interface allow the modulation, among other aspects, of the balance between inflammation and regeneration around the implant. In this article we could see through electron, atomic and confocal microscopy that the bioactivation of implants with PRGF - Endoret generates a three-dimensional scaffold with a multitude of platelets, proteins and growth factors. In addition, the composition of the interface of the surfaces bioactivated with PRGF -Endoret is specific, containing platelet and protein elements different to those of other surfaces assessed. The specificity of both the morphology and the composition of the interfaces formed with implants bioactivated with PRGF - Endoret is very possibly the reason behind its beneficial clinical results. Tejero R, Rossbach P, Keller B, Anitua E, Reviakine I. Implant surfaces activated with plasma rich in growth factors: time of flight secondary ion mass spectrometry and principal component analysis study
42 The biological potential of PRGF -Endoret Preclinical Research In this laboratory test we analysed whether the new fraction F2 of PRGF -Endoret produces the same biological effect as the old fraction F3. To this end the potential was evaluated of the different formulations of PRGF -Endoret in the stimulation of different biological processes in human gingival fibroblasts, including the proliferation, migration and adhesión of fibroblasts, as well as the autocrine release of some angiogenic factors and components of the cellular matrix. The results observed showed that PRGF - Endoret significantly increased the cellular proliferation, migration and adhesion of gingival fibroblasts. These results showed how PRGF -Endoret is capable of promoting the regeneration of gingival connective tissue and highlighted the biological potential of the new fraction F2 of PRGF -Endoret. Anitua E, Troya M, Orive G. Plasma Rich in Growth Factors Promotes Gingival Tissue Regeneration by Stimulating Fibroblast Proliferation and Migration and by Blocking TGF-β1-Induced Myodifferentiation. J Periodontol
43 BTI Biotechnology Institute S.L. In another study carried out on human osteoblasts, again we saw the biological potential of the new fraction F2 of PRGF - Endoret and it was compared to the previous one, F3. To do so we evaluated: proliferation, migration, chemotaxis, autocrine secretion of growth factors and the production of components of the extracellular matrix. The results showed that the new F2 managed to increase the proliferation, migration and chemotaxis of the osteoblasts. In addition, the autocrine expression of two relevant pro-angiogenic factors: VEGF and HGF was significantly improved, and that of three osteoblastic activity markers: procollagen I (PC), osteocalcin (OC) and alkaline phosphatase (ALP). These results showed how the new fraction F2 of PRGF -Endoret stimulates some of the biological processes of the main cells responsible for bone regeneration and its effects are biologically comparable to the previous one, F3. Anitua E, Tejero R, Zalduendo MM, Orive G. Plasma Rich in Growth Factors Promotes Bone Tissue Regeneration by Stimulating Proliferation, Migration and Differentiation of Primary Human Osteoblasts
44 Biomechanical Studies Preclinical Research This biomechanical study was carried out with the aim of evaluating the influence of straight alignment versus distal offset on the bone stress distribution that the bone around the implant sustains. A mesial load of 200 N and a distal load of 230 N were applied to the prosthesis. These results showed that the fact that there is a limited offset (of up to 2.5 mm) of the prosthesis on the implant does not increase stress on the adjacent bone. The use of larger diameter implants will reduce even further the stress in the bone adjacent to the implant. A controlled offsetting of the implant on the prosthesis, in addition to allowing an optimal aesthetic restoration and reducing the emergence profile, does not increase bone stress and a possible risk of implant failure. Anitua E, Orive G. Finite element analysis of the influence of the offset placement of an implant-supported prosthesis on bone stress distribution. J Biomed Mater Res B Appl Biomater. 2009;89:
45 BTI Biotechnology Institute S.L. The aim of another biomechanical study was to evaluate the influence of the length, diameter and geometry of BTI implants on bone stress distribution. 3D finite element models were created and a load of 150 N was applied at an angle of 30 degrees. Different diameters (3.5 to 5.0 mm) and lengths (8.5 to 15 mm) were evaluated. The results showed that the effect of the implant diameter on bone stress distribution was more significant than the effect of the length or geometry. On the other hand the maximum stress was located around the implant neck and most of it in the bone adjacent to the first implant threads. According to the results observed, the use of greater diameter implants can be beneficial to reduce stress around the implant, meaning that the use of short implants with a greater diameter could be a reasonable alternative in locations where residual bone height is limited. Anitua E, Tapia R, Luzuriaga F, Orive G. Influence of implant length, diameter, and geometry on stress distribution: a finite element analysis. Int J Periodontics Restorative Dent. 2010;30:89-95.
46 Alveoluses Post- Extraction Clinical Research After the extraction of a tooth a healing and regeneration process starts for the tissues involved that will affect the final volume of alveolar bone and the structure of the ridge. An excessively traumatic extraction or an insufficient regeneration can lead to an excessive loss of bone tissue, a delay in the replacement of lost teeth with implants, may require invasive reconstruction techniques, or may generate a permanent defect without any possible correction. In order to modify this process favourably and to promote adequate regeneration, there are different therapeutic tools among which we could mention those aimed at isolating the defect and preventing the growth of conjunctive tissue towards its interior (membranes), materials susceptible of filling in the defect and substances with osteogenic and osteoconductor properties such as PRGF -Endoret.
47 The PRGF -Endoret clot is ideal for filling in the alveolus post-extraction and for releasing growth factors that promote its regeneration. BTI Biotechnology Institute S.L.
48 Alveoluses Post- Extraction Clinical Research This article is the first in scientific literature that describes the use of 100% autologous platelet-rich plasma in oral and maxillofacial surgery. The aim of this pioneering study was to evaluate the use of PRGF -Endoret in the regeneration of alveoluses post-extraction. To carry it out 20 patients were included who were randomly given PRGF -Endoret or the traditional treatment with suture. Biopsies were collected from 6 to 10 weeks after the extraction. The results showed that epithelisation was very good or excellent in the cases treated with PRGF -Endoret and normal in the control group. Regeneration was practically complete in 8 of the 10 cases. The biopsies of the areas treated with PRGF -Endoret showed mature compact bone with well organised trabeculae and normal morphology. In all the biopsies of the control group there was only connective tissue containing bone trabeculae, but in no cases mature bone. The results were significantly better when PRGF -Endoret was used and no adverse effects were observed. Anitua E.Plasma rich in growth factors: preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants. 1999;14:
49 BTI Biotechnology Institute S.L. This clinical study was focused on evaluating the clinical results of implants placed immediately in post-extraction sites using PRGF -Endoret as an adjuvant during surgery. A total of 30 patients were included in the study with chronic periapical lesions that required an extraction and a total of 61 implants were placed. Survival and bone loss were assessed 1 year after the implants were placed. The results after an average follow-up period of 18.5 months showed a survival rate of 98.4 %. Average bone loss was 0.41 mm. implants in alveoluses post-extraction can be considered an effective, safe and predictable treatment option in cases with periapical lesions. Del Fabbro M, Boggian C, Taschieri S. Immediate implant placement into fresh extraction sites with chronic periapical pathologic features combined with plasma rich in growth factors: preliminary results of single-cohort study. J Oral Maxillofac Surg. 2009;67: These results prove that the use of PRGF - Endoret for the immediate placement of
50 Alveoluses Post- Extraction Clinical Research The aim of this study was to describe and evaluate the use of PRGF -Endoret in the treatment of defects post-extraction. 14 patients were included who required the extraction of different teeth and in 7 of them PRGF -Endoret was applied while in the other 7 it was not, with this being used as the control group. After 11 to 14 weeks, the bone density was measured in the internal and external perimeter as well as in the centre of the defects using the BTI-Scan program. The results showed that bone density in the internal periphery and in the centre of the implant bed was significantly higher in the group treated with PRGF -Endoret with respect to the control group. Bone density was also higher in the external periphery, but without significant differences. As a result we can say that PRGF -Endoret promotes faster bone regeneration in alveoluses post-extraction. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua et al. Treatment of post-extraction defects using a novel clinical protocol: a case series study. Italian Oral Surgery. 2010;3:
51 1 st day Day 10 BTI Biotechnology Institute S.L. 3 months The application of PRGF -Endoret reduces inflammation and pain, accelerates the epithelisation of soft tissues and promotes bone regeneration. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
52 Alveoluses Post- Extraction Clinical Research The aim of this split-mouth study was to evaluate the efficacy of PRGF -Endoret in the regeneration of alveoluses post-extraction in impacted third molars. To this end the cytokines in the mucous tissues were analysed after the extraction with the application or not of PRGF -Endoret. Post-op pain and facial swelling were also assessed. The results showed that the inflammation parameters and the regeneration process of the lesion were all significantly better in the areas treated with PRGF -Endoret than in the control areas. On the other hand the post-op pain and facial swelling were less in the areas treated with PRGF -Endoret. In short, based on the results obtained it can be stated that PRGF -Endoret can be routinely used in the regeneration of impacted third molars. Mozzati M, Martinasso G, Pol R, Polastri C, Cristiano A, Muzio G, Canuto R. The impact of plasma rich in growth factors on clinical and biological factors involved in healing processes after third molar extraction. J Biomed Mater Res A. 2010;95:
53 BTI Biotechnology Institute S.L. This article describes a clinical case in which PRGF -Endoret was used to preserve the architecture of the soft tissues associated with an implant that was placed immediately after an extraction at the back of the superior maxilla. This procedure allowed a guided bone regeneration without the need to carry out vertical releasing incisions, presenting a good gingival outline in facial appearance after a single surgical phase. Rosano G, Taschieri S, Del Fabbro M. Immediate post-extraction implant placement using PRGF technology in maxillary premolar region: a new strategy for soft tissue management. J Oral Implantol
54 Horizontal and vertical bone regeneration Clinical Research In some situations, there is a lack of bone support due to an atrophy, trauma or surgical resection. As dental implants can only be placed if there is enough bone to be able to adequately stabilise them, the procedures for bone augmentation are an effective therapeutic option for these kinds of situations. In fact, in patients with long-term edentulous sites, even severe bone resorptions are frequently observed (both vertical and horizontal or combined defects). As a result, the use of additional techniques for bone augmentation is essential. Some of these techniques include the use of growth factors, osteogenic distraction, guided bone regeneration, the use of re-vascularised bone grafts and techniques such as ridge expansion or expanders or Split-Crest with ultrasonics. PRGF-ENDORET Technology
55 BTI Biotechnology Institute S.L. The aim of this study was to clinically evaluate the ridge expansion technique with ultrasonics called the Split-Crest technique, for the placement of dental implants in patients with narrow ridges. After at least 6 months after loading the implants, the state of the hard and soft tissues and the expansion achieved were evaluated, as well as the survival rate of the implants. 15 patients were included whose previous average ridge width was 4.29 mm and who received a total of 37 implants. PRGF - Endoret was applied during surgery to encourage tissue regeneration. The results showed that the state of the soft tissues was very good with adequate values of plaque index, bleeding and probing depth. The implant survival rate was 100 %. The average bone expansion achieved was 3.35 mm. These results showed how the Split- Crest technique with ultrasonics along with the application of PRGF -Endoret can be considered an effective and safe technique for bone expansion in narrow ridges. Anitua E, Begoña L, Orive G. Clinical Evaluation of Split-Crest Technique with Ultrasonic Bone Surgery for Narrow Ridge Expansion: Status of Soft and Hard Tissues and Implant Success. Clin Implant Dent Relat Res
56 Horizontal and vertical bone regeneration Clinical Research This article rescribes a new ridge expansion technique called the two-stage Split-Crest technique indicated for patients with severely resorbed ridges (3-4 mm). It consists of an expansion carried out in 2 consecutive stages using transitional implants. The implants used as transitional implants (2.5 and 3.0 mm diameter) were replaced from 5 to 7 months after their placement with others with a larger diameter. The state of the soft tissues was good with adequate probing depth values (average value was 3.06 mm). The average bone expansion achieved after the procedure was 8.49 mm apical and 7.10 mm occlusal. There were no implant failures during the follow-up period. These preliminary results prove the predictability and safety of the two-stage Split-Crest technique and its potential use in patients with severely resorbed ridges, as well as avoiding the use of other more aggressive techniques such as bone grafts. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua E, Begoña L, Orive G. Two-stage split-crest technique with ultrasonic bone surgery for controlled ridge expansion: a novel modified technique.oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112:
57 BTI Biotechnology Institute S.L. The new two-stage Split-Crest technique using transitional BTI implants allows an expansion of the ridge of 7-8 mm. Anitua E, Begoña L, Orive, G. Two-stage Split-crest technique with Ultra-sonic bone surgery for controlled ridge expansion: A modified technique and case series. Implant Dent
58 Horizontal and vertical bone regeneration Clinical Research The aim of this randomised clinical test was to evaluate the effectiveness of anorganic bovine bone in ridge expansion with a titanium mesh and to investigate the effect of PRGF -Endoret in preventing mesh exposure, given that it is a frequent complication in these procedures. 30 patients were included on whom a total of 43 ridge expansions were carried out. In 15 of them PRGF -Endoret was used to cover the titanium mesh, while it was not used in the rest (control) the 2 groups regarding the complications and bone formation. In the group treated with PRGF -Endoret there was no mesh exposure while in the control group there was an exposure rate of 28.5%. The radiological analysis showed that bone augmentation was higher in the group with PRGF -Endoret. On the other hand the implant survival rate was 100% in the group with PRGF -Endoret and 97.3% in the control group. After 6 months of evolution, the results showed significant differences between Torres J, et al. Platelet-rich plasma may prevent titanium-mesh exposure in alveolar ridge augmentation with anorganic bovine bone. J Clin Periodontol. 2010;37:
59 BTI Biotechnology Institute S.L. The aim of this randomised clinical trial was to evaluate the use of BTI motorised ridge expanders and to compare their results with those obtained by means of the lateral ridge expansion technique. 8 bilateral patients were included on whom the technique with expanders was applied to one side while on the other the lateral technique was used. The implants were placed 6 months later. The results showed significant differences in the bone expansion achieved with both techniques (1.5 mm with the motorised expanders and 1.2 mm with lateral expansion). These results showed the effectiveness of motorised expanders for the expansion of narrow ridges. In addition, the defects treated with expanders presented less bone width contraction during the first 6 months. Mazzocco F, Nart J, Cheung WS, Griffin TJ. Prospective evaluation of the use of motorized ridge expanders in guided bone regeneration for future implant sites. Int J Periodontics Restorative Dent. 2011;31:
60 Sinus elevation Clinical Research The insertion of implants in the posterior region of the superior maxilla is a difficult clinical procedure. Progressive horizontal and vertical bone resorption increases the sinus cavity while the maxillary sinus floor thickness is reduced. An absence of superior molars can even increase bone resorption, leading to the pneumatisation of the sinus due to an increased activity of osteoclasts in Schneider's membrane. These limitations can make it difficult to place an implant and can negatively affect the success of its osseointegration and the stability of the dental implants. The most frequently applied surgical procedure to reestablish an adequate bone volume and an adequate ridge height in the posterior region of the maxilla is an augmentation of the maxillary sinus. This technique involves the modification of the sinus cavity with the aim of generating sufficient bone volume within a space that used to be part of the sinus cavity.
61 a b BTI Biotechnology Institute S.L. c d The protocol consists of a) carrying out a complete osteotomy with surgical ultrasonics, b) filling in the sinus with a graft soaked in PRGF -Endoret, c) replacing the bone window and a fibrin membrane, and d) placing the implants months later. BIOGRAPHY: * Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006 May;24(5):
62 Sinus elevation Clinical Research This article describes the sinus elevation technique with the use of an osteotomy with ultrasonics. This is the first job that uses surgical ultrasonics. This technique offers important advantages over a conventional osteotomy that uses diamond tool bits. In addition, it reduces the risk of perforating Schneider's membrane. On the other hand it improves the vision and hygiene of the surgical area and provides a more conservative and controlled bone incision. The aim of this study was to evaluate a modified sinus elevation technique with osteotomes and the immediate placement of implants and the application of PRGF - Endoret. A total of 14 patients were included on whom this technique was carried out and the results showed that after an average follow-up period of 36 months, none of the implants failed and marginal bone loss after 1 year of load was 0.36 mm. All the treatments were successful. Torrella F, Pitarch J, Cabanes G, Anitua E. Ultrasonic ostectomy for the surgical approach of the maxillary sinus: a technical note. Int J Oral Maxillofac Implants. 1998;13: Taschieri S, Del Fabbro M. Postextraction osteotome sinus floor elevation technique using plasma-rich growth factors. Implant Dent. 2011;20:
63 BTI Biotechnology Institute S.L. The aim of this randomised clinical trial was to evaluate whether PRGF -Endoret improves the effectiveness of inorganic bovine bone in the sinus elevation technique. 87 patients were included on whom a total of 144 sinus elevations were carried out using biomaterial alone or in combination with PRGF -Endoret. A total of 286 implants were placed in the patients, who were monitored for 24 months. The results showed that the survival rate was higher in the implants placed using biomaterial + PRGF -Endoret. It should be noted that in patients with residual ridges of less that 4 mm, the implant survival rate was significantly higher in the areas treated with PRGF -Endoret (98.2 vs 90.7%). The histological and histomorphometric analysis revealed that the bone augmentation was significantly greater in the areas treated with PRGF -Endoret. These results showed that PRGF -Endoret can improve the osteoconductive properties of the biomaterial increasing the volume of new bone formed. Torres J, Tamimi F, Martinez PP, Alkhraisat MH, Linares R, Hernández G, Torres-Macho J, López-Cabarcos E. Effect of plateletrich plasma on sinus lifting: a randomized-controlled clinical trial. J Clin Periodontol. 2009;36:
64 Sinus elevation Clinical Research The aim of this study was to describe and evaluate the lateral sinus elevation technique with the application of PRGF -Endoret. 18 patients were included who received a total of 43 implants. All of them presented a residual bone height of 1-3 mm. The technique consisted of carrying out a vestibular osteotomy with ultrasonics, separating the window created and keeping it submerged in PRGF -Endoret. Once the elevation is carried out the window is replaced in its anatomical location and covered with autologous fibrin. After 6 months the samples of bone taken from the sinuses were evaluated. The results showed that after an average follow-up period of 13 months, the implant survival rate was 100%. These results showed that the lateral sinus elevation technique using PRGF -Endoret can be considered a safe, effective and predictable technique. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua E, Prado R, Orive G. A lateral approach for sinus elevation using PRGF technology. Clin Implant Dent Relat Res. 2009;11:23-31.
65 PRGF -Endoret Control BTI Biotechnology Institute S.L. Regenerative potential after 5 months and anti-inflammatory properties of PRGF -Endoret. The aim of this study was to evaluate the potential effect of PRGF -Endoret in the lateral approach for sinus elevation. 5 patients were included who required bilateral sinus elevations with a residual bone height of 1-3 mm. On one side PRGF - Endoret was used along with inorganic bovine bone, while only biomaterial was used on the other side. The use of PRGF -Endoret doubled the volume of the graft thanks to the action of the fibrin. Post-op pain and inflammation were greater on the control side (without PRGF -Endoret ). The areas treated with PRGF -Endoret presented a larger amount of new vital bone than those without. The immunohistochemistry of the biopsies revealed that the number of blood vessels per square millimetre of connective tissue was 116 vessels as opposed to 7 in the control areas. These results showed the therapeutic potential of PRGF -Endoret for reducing inflammation, increasing new bone formed and generating blood vessels in these sinus elevation procedures. Anitua E, Prado R, Orive G. Bilateral Sinus Elevation Evaluating Plasma Rich in Growth Factors Technology: A Report of Five Cases. Clin Implant Dent Relat Res
66 Bisphosphonate-related osteonecrosis of the jaw Clinical Research Biphosphonates are a group of drugs that reduce the rate of bone turnover, mainly through the inhibition of the action of osteoclasts, and they are administered both orally and intravenously in patients with oncological or rheumatic treatments. These drugs show calcium affinity and their mechanism of action at a cellular level includes the inhibition of the vascular endothelial growth factor (VEGF). Around the year 2003 the first cases of exposed bone that would not heal in the maxillofacial region in patients treated with intravenous biphosphonates were reported, meaning that this pathology was associated with the administration of biphosphonates and was identified as bisphosphonaterelated osteonecrosis of the jaw (BRONJ). The accumulated incidence of BRONJ has been estimated within a range of 8 to 12%, for IV administration and 0.7/100,000 people/year for oral administration. To date, the treatments available to prevent or treat BRONJ are very limited and the results obtained are not conclusive. Recently, the use of PRGF -Endoret has been proposed as part of a preventive and therapeutic approach. The hypothesis of the use of this autologous technology is based on the potential effects of the growth factors released in the osteoclasts and on angiogenesis.
67 BTI Biotechnology Institute S.L. This article describes the clinical case of a patient affected by BRONJ after being treated for several years with zoledronic acid (IV) and after a tooth extraction. Their symptomatology includes severe pain and hemimandibular paresthesia due to affectation of the dental nerve. The treatment consisted of surgical resection of the necrotic bone area combined with the application of PRGF -Endoret. improvement of the pain and paresthesia was observed. After a year, the patient had totally recovered sensitivity and the absence of necrotic bone was confirmed. These clinical results support the use of PRGF -Endoret as an adjuvant treatment for patients with BRONJ. One month after surgery, total closure of the ulcerous lesion in the mucous membrane was observed without the presence of necrotic bone. 6 months later, a significant Anitua et al.treatment of bisphosphonate-related osteonecrosis of the jaw (BRONJ) with plasma rich in growth factors (PRGF- ENDORET). J Cranio & Maxillofac Surg
68 Bisphosphonate-related osteonecrosis of the jaw Clinical Research The aim of this study was to describe and evaluate the use of PRGF -Endoret within the surgical tooth extraction protocol for patients in treatments with biphosphonate drugs and its role in the prevention of bisphosphonate-related osteonecrosis of the jaw (BRONJ). A total of 64 patients were included on whom a total of 220 extractions were carried out and in all of them PRGF - Endoret was applied to cover the defect and to encourage a correct regeneration of tissues. The patients were monitored for at least 4 months. Bisphosphonate-related osteonecrosis of the jaw only occurred in 5 post-extraction sites (2.27%). In the mandible, the cases of BRONJ were more frequent. The results of this study show that PRGF -Endoret is a possible alternative to prevent these lesions in patients in treatment with biphosphonates who have had dental extractions. Scoletta M, Arduino PG, Pol R, Arata V, Silvestri S, Chiecchio A, Mozzati M. Initial experience on the outcome of teeth extractions in intravenous bisphosphonate-treated patients: a cautionary report. J Oral Maxillofac Surg. 2011;69:
69 The aim of this study of case and control groups was to determine the role of PRGF -Endoret in the prevention of bisphosphonate-related osteonecrosis of the jaw in patients who took IV biphosphonates and who had dental extractions. The study included 100 patients, of whom 50 received PRGF -Endoret after the extraction while the rest did not receive PRGF -Endoret (control group). The patients were monitored for a period ranging between 24 and 60 months, carrying out annual checkups and scans. BRONJ was diagnosed in 2 patients and both were from the control group. Despite the small number of patients, these results may suggest that treatment of extractions with PRGF -Endoret may reduce the risk of developing BRONJ by these patients at risk receiving treatment with IV biphosphonates. Mozzati M, Arata V, Gallesio G, Carossa S. A dental extraction protocol with plasma rich in growth factors (PRGF) in patients on intravenous bisphosphonate therapy: a case-control study. Joint Bone Spine. 2011;78:648-9.
70 BTI implants Clinical Research The range of BTI implants presents a series of special and differential features. All of them have a surface treatment that gives them excellent humectability, thus obtaining a nanometric bioactive surface ideal in combination with PRGF -Endoret to shorten their osseointegration periods. On the other hand, their surface provides an excellent titanium-bone interface and maximum bone apposition is achieved with an increase of BIC (bone-implant contact). Its self-tapping apex with excellent advancing capacity and small apical surface avoids compressions and facilitates its directional control and placement in narrow ridges. Within the range of BTI implants, we should highlight the family of short ( 8.5 mm) and extra-short ( 6,5 mm) implants that have proven their high long-term predictability. Anitua E. Novel protocols for predictable implantology. Pract Proced Aesthet Dent. 2008;20:
71 This retrospective study with BTI implants was published in the journal with the greatest scientific impact in the field of dentistry. Its aim was to evaluate the long-term survival of BTI implants and to identify the possible risk factors associated with implant failures. A total of 5787 BTI implants of different diameters and lengths were included in the study. The results showed that the implant survival rate was 99.2%, 96.4% and 96.0% for the analysis based on the implant, on the surgery and on the patient, respectively. The risk factors that could be related to a higher implant failure rate were two-stage surgery and the use of special surgery-related techniques. These results attest to the predictability and safety of BTI's range of implants. Anitua E, Orive G, Aguirre JJ, Ardanza B, Andía I. 5-year clinical experience with BTI dental implants: risk factors for implant failure. J Clin Periodontol. 2008;35:
72 BTI implants Immediate load This study was carried out with the aim of describing the immediately loaded dental implant insertion technique and to evaluate the long-term survival, as well as the possible risk factors related to its failure. A total of 1139 implants were included and a survival rate of 99.3%, 96.8% and 96.9% was observed for the analysis based on the implant, on the surgery and on the patient, respectively. Only 5 of the implants failed during the follow-up period and no failure-related risk factors were found. These results showed the predictability of the immediate load technique described provided it is used with appropriate insertion torques and following strict clinical protocols. Anitua E, Orive G, Aguirre JJ, Andía I. Clinical outcome of immediately loaded dental implants bioactivated with plasma rich in growth factors: a 5-year retrospective study. J Periodontol. 2008;79:
73 Short implants Several years after starting the clinical use of short implants, the decision was made to carry out this study, the aim of which was to evaluate the long-term survival of short BTI implants ( 8.5 mm) in posterior areas of the superior maxilla and the mandible. A total of 532 implants placed in 293 patients were included. The results showed a survival rate of 99.2% and 98.7% for the analysis based on the implant and on the patient, respectively. Two of the implants failed due to different causes after an average follow-up period of 31 months. No risk factors related to the failure of the short implants could be identified. These results showed the high predictability of the use of short implants in posterior areas. Anitua E, Orive G, Aguirre JJ, Andía I. Five-year clinical evaluation of short dental implants placed in posterior areas: a retrospective study. J Periodontol. 2008;79:42-48.
74 BTI implants Short implants The aim of these studies was to evaluate the long-term survival (up to 8 years of followup) of short and extra-short BTI implants ( 8.5 mm) in posterior areas of the superior maxilla and the mandible. In the first of them, a total of 1287 short implants placed in 661 patients were included. The results showed a survival rate of 99.3% and 98.8% for the analysis based on the implant and on the patient, respectively. Nine of the implants failed due to different causes. No risk factors related to the failure of the short implants could be identified. ( 6,5) were also studied separately, showing survival rates of 97.9% and 97.1% for the implants and patients, respectively. These results showed that treatment with short and extra-short implants can be considered a safe and predictable technique if used following strict clinical protocols. In the second study the extra-short implants Anitua E, Orive G. Short implants in maxillae and mandibles: a retrospective study with 1 to 8 years of follow-up. J Periodontol. 2010;81:
75 a b BTI Biotechnology Institute S.L. c d Short and extra-short implants allow rehabilitations in atrophic ridges without having to resort to more aggressive techniques such as bone grafts. Anitua E. The Use of Short and Extra-Short BTI Implants In the Daily Clinical Practice. JIACD 2010;2:19-29.
76 BTI implants Short implants This study was carried out with the aim of evaluating the influence of an unfavourable crown/implant ratio ( 1) and other variables of the implant, be they surgical, prosthetic or biomechanical, on Marginal Bone Loss and on the survival of short implants in posterior areas. A total of 128 implants placed in 63 patients were evaluated. The average followup period was 22 months. The average C/I ratio of the implants was In 86 of them it was <2 and in 42 implants 2. The marginal bone loss observed was 0.35 mm during the first year post-load and 0.45 mm after the first year post-load. The implant and prosthesis survival rate was 100 %. The unfavourable C/I ratio did not show any relationship with the marginal bone loss of the implants. Of the remaining variables studied, the only one that showed a negative inflluence was the use of cantilevers in prosthetic rehabilitations. Anitua E, Begoña L, Piñas L, Orive, G. Impact of unfavorable crown-to-implant ratio on marginal bone loss and survival rates of short and extra-short implants placed in posterior regions
77 BTI Biotechnology Institute S.L. The aim of this study was to evaluate the influence of a very unfavourable crown/ implant ratio ( 2) and other variables, be they surgical, prosthetic or biomechanical, on Marginal Bone Loss and on the survival of short implants in posterior areas. A total of 42 implants placed in 28 patients were evaluated. The average follow-up period was 28 months. The average C/I ratio of the implants was The marginal bone loss observed was 0.38 mm and 0.24 mm mesial and distal, respectively. The implant and prosthesis survival rate was 100 %. The very unfavourable C/I ratio did not show any relationship with the marginal bone loss of the short implants in posterior areas. No relationship was found between the rest of the variables studied and marginal bone loss. Anitua E, Begoña L, Piñas L, Orive, G. Short and extra-short implants with a very unfavorable crown-to-implant ratio ( 2) in posterior regions. Influence on marginal bone loss and survival rate
78 BTI implants Narrow implants This study was carried out to evaluate the long-term survival and clinical effectiveness of narrow-diameter (2.5 and 3.0 mm) BTI Tiny implants in patients with an insufficient ridge (2.5 to 4.0 mm) to allow the placement of standard-diameter implants. 51 patients were included who received a total of 89 implants. The results showed a survival rate of 98.9% and 98.0% for the analysis based on the implant and on the patient, respectively. Only one implant failed 12 months after its placement. Average bone loss after 2 years of implant load was 1.26 mm. These results showed that 2.5 and 3.0 mm Tiny implants can be used effectively and safely for the treatment of narrow and severely resorbed ridges. Anitua E, Errazquin JM, de Pedro J, Barrio P, Begoña L, Orive G. Clinical evaluation of Tiny 2.5- and 3.0-mm narrow-diameter implants as definitive implants in different clinical situations: a retrospective cohort study. Eur J Oral Implantol. 2010;3:
79 The many clinical studies carried out with BTI implants prove their versatility, safety and predictability BTI Biotechnology Institute S.L.
80 BTI implants Implant explantation This article describes for the first time the concept of de-osseointegration of implants. For this purpose a new technique has been developed that uses the BTI Explantation Kit, which facilitates an easy and atraumatic explantation while keeping the walls of the alveolar bed intact to allow the placement of a new implant. In this study a total of 58 explantation cases of different implants were included using the BTI Explantation Kit. The removal torque varied between 80 and 200 Ncm. In 20 cases a new implant was placed. This article shows how the possibility of explanting dental implants atraumatically opens new doors in oral implantology. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua et al. Atraumatic Implant Explantation, is it Possible? Description of a Novel Technique and a Case Series Study JIACD. PRGF-ENDORET Technology
81 BTI Biotechnology Institute S.L. This study was carried out with the aim of describing and evaluating the new technique for the atraumatic explantation of implants. This new technique facilitates a fast explantation, keeping the alveolar bed walls intact and at the same time facilitating the insertion of a new implant during the same surgical operation. In this study 91 implants explanted from a total of 42 patients were included. The removal torques varied between 80 and 200 Ncm. In those cases where the implant removal torque exceeded 200 Ncm, 2-3 mm incisions were carried out with a set of atraumatic trephines to avoid excessively high torques. These results showed how the possibility of explanting implants atraumatically can be considered a viable alternative to replace failed implants. Anitua et al. A new approach for atraumatic implant explantation and immediate implant installation. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2012
82 BTI implants Antibiotic prophylaxis for implants The aim of this randomised clinical trial was to assess the need or not to administer an antibiotic prophylaxis with 2 g of oral amoxicillin one hour before the single dental implant insertion surgery to avoid post-op infections. 12 private centres which recruited a total of 105 patients took part. 52 patients received amoxicillin and 53 received a placebo. After 6 months, there were 6 infections and 2 implant failures in each group. No statistically significant differences were found for post-op infections, adverse events or implant failures between both groups. Observing the results of this study, antibiotic prophylaxis for single implants may not be necessary. DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. Anitua E, Aguirre JJ, Gorosabel A, Barrio P, Errazquin JM, Román P, Pla R, Carrete J, de Petro J, Orive G. A multicentre placebo-controlled randomised clinical trial of antibiotic prophylaxis for placement of single dental implants. Eur J Oral Implantol. 2009;2:
83 BTI Biotechnology Institute S.L. Biological drilling In this article, the aim was to describe and compare with the traditional drilling system a low-revolution drilling system ( r.p.m) that allows surgeons to obtain live autologous bone that can be associated with PRGF -Endoret to be used in bone grafts. Bone particles using both conventional techniques and the new low-revolution drillling system were collected and analysed under a microscope. The microscopic examination showed that the bone structure and the presence of live cells was preserved in all the samples collected with low-revolution drilling while these qualities were not maintained with conventional drilling. This new drilling technique can reduce damage to the host tissue and can be used to obtain a mass of live bone ideal for carrying out bone grafts associated with PRGF -Endoret. Anitua E, Carda C, Andia I. A novel drilling procedure and subsequent bone autograft preparation: a technical note. Int J Oral Maxillofac Implants. 2007;22:
84 Facial regeneration Aging is a multi-factorial process that is characterised by a progressive reduction of the functional capacity of all the body's tissues and organs, with the consequent loss of ability to adjust to environmental stimuli. It is a known fact that skin aging is produced by cellular or intercellular matrix degradation, reduced vascularisation, a dysfunction of skin annexes, fat atrophy and muscular atrophy or relaxation. These phenomena are fundamentally influenced by the inexorable passage of time and genetics, in addition to other factors such as sun exposure, diseases, nutrition, toxic habits, etc. The most evident signs of aging are wrinkles, dyschromias and ptosis, and other less evident ones, such as the texture, feel, colour, shine and brightness, which globally determine the final appearance of the skin. Today, and due to social pressure, increasing importance is given to our physical appearance, where it is considered acceptable and even necessary in more and more circles to struggle to maintain a youthful and healthy appearance. This growing aesthetic awareness means that the interest in developing new products to help us improve the appearance of our skin has increased.
85 PRGF -Endoret represents the first biological therapy for personalised medicine that has proved its effectiveness in facial regeneration and anti-aging. BTI Biotechnology Institute S.L.
86 Facial regeneration Clinical research In this randomised clinical trial the effectiveness and safety of PRGF -Endoret was evaluated in the cutaneous regeneration of aged skin, comparing it with hyaluronic acid. A total of 100 patients were included with evident external signs of aged skin and were randomly assigned treatment with PRGF - Endoret or with hyaluronic acid. The level of skin moisturisation, cutaneous concentration of fat and skin ph, the level of severity of the wrinkle and patient satisfaction were evaluated. The results showed that in both follow-up visits the skin moisturisation and ph values as well as the satisfaction rate were significantly higher in the group treated with PRGF - Endoret (p<0.05) than in the control group. On the other hand, the fat index drop after 3 months was significantly lower in both groups with respect to the baseline visit. These results support the application of PRGF -Endoret in the treatment of age-related skin aging, obtaining excellent mid and long-term results after its application.
87 BTI Biotechnology Institute S.L. Anitua E, Sánches M, Sarabia R, Sanz J, Aguirre JJ, Orive G. Eficacia y seguridad del PRGF (plasma rico en factores de crecimiento) en la regeneración cutánea facial. Ensayo clínico, randomizado y controlado con ácido hialurónico. Journal of the AECEP. 2011: DEMONSTRATION VIDEO Scan this code with your mobile phone to watch the video. before after
88 Publications Traumatology, orthopaedic surgery and sports medicine Revision articles Sánchez M, Anitua E, Orive G, Mujika I, Andia I. Platelet-rich therapies in the treatment of orthopaedic sport injuries. Sports Med. 2009;39: Engebretsen L, Steffen K, Alsousou J, Anitua E, Bachl N, Devilee R, Everts P, Hamilton B, Huard J, Jenoure P, Kelberine F, Kon E, Maffulli N, Matheson G, Mei-Dan O, Menetrey J, Philippon M, Randelli P, Schamasch P, Schwellnus M, Vernec A, Verrall G. IOC consensus paper on the use of plateletrich plasma in sports medicine. Br J Sports Med. 2010;44: Sánchez M, Anitua E, Lopez-Vidriero E, Andía I. The future: optimizing the healing environment in anterior cruciate ligament reconstruction. Sports Med Arthrosc. 2010;18: Andia I, Sanchez M, Maffulli N. Tendon healing and platelet-rich plasma therapies. Expert Opin Biol Ther. 2010;10: Mei-Dan O, Lippi G, Sánchez M, Andia I, Maffulli N. Autologous platelet-rich plasma: a revolution in soft tissue sports injury management? Phys Sportsmed. 2010;38: Andia I, Sánchez M, Maffulli N. Platelet rich plasma therapies for sports muscle injuries: any evidence behind clinical practice? Expert Opin Biol Ther. 2011;11: Andia I, Sánchez M, Maffulli N. Joint pathology and platelet-rich plasma therapies. Expert Opin Biol Ther. 2012;12:7-22. Preclinical Research Anitua E, Andía I, Sanchez M, Azofra J, del Mar Zalduendo M, de la Fuente M, Nurden P, Nurden AT. Autologous preparations rich in growth factors
89 BTI Biotechnology Institute S.L. promote proliferation and induce VEGF and HGF production by human tendon cells in culture. J Orthop Res. 2005;23: Anitua E, Sanchez M, Nurden AT, Zalduendo M, de la Fuente M, Orive G, Azofra J, Andia I. Autologous fibrin matrices: a potential source of biological mediators that modulate tendon cell activities. J Biomed Mater Res A. 2006;77: Sánchez M, Anitua E, Azofra J, Andía I, Padilla S, Mujika I. Comparison of surgically repaired Achilles tendon tears using platelet-rich fibrin matrices. Am J Sports Med. 2007;35: Anitua E, Sanchez M, Nurden AT, Zalduendo M, de la Fuente M, Azofra J, Andia I. Reciprocal actions of platelet-secreted TGF-beta1 on the production of VEGF and HGF by human tendon cells. Plast Reconstr Surg. 2007;119: Anitua E, Sánchez M, Nurden AT, Zalduendo MM, de la Fuente M, Azofra J, Andía I. Platelet-released growth factors enhance the secretion of hyaluronic acid and induce hepatocyte growth factor production by synovial fibroblasts from arthritic patients. Rheumatology (Oxford). 2007;46: Anitua E, Sánchez M, Zalduendo MM, de la Fuente M, Prado R, Orive G, Andía I. Fibroblastic response to treatment with different preparations rich in growth factors. Cell Prolif. 2009;42: Gallo I, Sáenz A, Artiñano E, Esquide J. Autologous platelet-rich plasma: effect on sternal healing in the sheep model. Interact Cardiovasc Thorac Surg. 2010;11: Anitua E, Sanchez M, De la Fuente M, Zalduendo MM, Orive G. Plasma rich in growth factors (PRGF-Endoret) stimulates tendon and synovial fibroblasts migration and improves the biological properties of hyaluronic acid. Knee Surg Sports Traumatol Arthrosc
90 Publications Traumatology, orthopaedic surgery and sports medicine Clinical Research Sánchez M, Azofra J, Aizpurúa B, Elorriaga R, Anitua E, Andía I. Aplicación de plasma autólogo rico en factores de crecimiento en cirugía artroscópica - Use of autologous plasma rich in growth factors in Arthroscopic surgery. Cuadernos de Artroscopia 2003;10: Sánchez M, Azofra J, Anitua E, Andía I, Padilla S, Santisteban J, Mujika I. Plasma rich in growth factors to treat an articular cartilage avulsion: a case report. Med Sci Sports Exerc. 2003;35: Sanchez M, Anitua E, Andia I. Application of Autologous Growth Factors on Skeletal Muscle Healing. 2nd World Congress on Regenerative Medicine, May 18-20, 2005, Leipzig, Germany Sánchez M, Anitua E, Azofra J, Aguirre JJ, Andia I. Intra-articular injection of an autologous preparation rich in growth factors for the treatment of knee OA: a retrospective cohort study. Clin Exp Rheumatol. 2008;26: Sánchez M, Anitua E, Cole A, Da Silva A, Azofra J, Andia I. Management of post-surgical Achilles tendon complications with a preparation rich in growth factors: A study of two-cases. Injury Extra. 2009;40: Jiménez-Martin A, Angulo-Gutiérrez J, González- Herranz J, Rodriguez-De La Cueva JM, Lara-Bullón J, Vázquez-Garcia R. Surgery of subacromial syndrome with application of plasma rich in growth factors. Int J Shoulder Surg. 2009;3: Anitua E, Sánchez M, de la Fuente M, Azofra J, Zalduendo M, Aguirre JJ, Andía I. Relationship between Investigative Biomarkers and Radiographic Grading in Patients with Knee Osteoarthritis. Int J Rheumatol. 2009;2009: Sanchez M, Anitua E, Cugat R, Azofra J, Guadilla J, Seijas R, Andia I. Nonunions treated with autologous preparation rich in growth factors. J Orthop
91 PRGF -Endoret has been a pioneer proving its effectiveness in the treatment of osteoarthritis and tendinopathies Trauma. 2009;23: Seijas R, Santana-Suarez RY, Garcia-Balletbo M, Cuscó X, Ares O, Cugat R. Delayed union of the clavicle treated with plasma rich in growth factors. Acta Orthop Belg. 2010;76: Sánchez M, Anitua E, Azofra J, Prado R, Muruzabal F, Andia I. Ligamentization of tendon grafts treated with an endogenous preparation rich in growth factors: gross morphology and histology. Arthroscopy. 2010;26: Mei-Dan O, Carmont M, Kots E, Barchilon V, Nyska M, Mann G. Early return to play following complete rupture of the medial collateral ligament of the elbow using preparation rich in growth factors: a case report. J Shoulder Elbow Surg. 2010;19:e1-e5. Wang-Saegusa A, Cugat R, Ares O, Seijas R, Cuscó X, Garcia-Balletbó M. Infiltration of plasma rich in growth factors for osteoarthritis of the knee shortterm effects on function and quality of life. Arch Orthop Trauma Surg. 2011;131: Sánchez M, Guadilla J, Fiz N, Andia I. Ultrasoundguided platelet-rich plasma injections for the treatment of osteoarthritis of the hip. Rheumatology (Oxford). 2012;51: Guadilla J, Fiz N, Andia I, Sánchez M. Arthroscopic management and platelet-rich plasma therapy for avascular necrosis of the hip. Knee Surg Sports Traumatol Arthrosc ;20: Mei-Dan O, Carmont MR, Laver L, Mann G, Maffulli N, Nyska M. Platelet-Rich Plasma or Hyaluronate in the Management of Osteochondral Lesions of the Talus. Am J Sports Med Filardo G, Kon E, Pereira Ruiz MT, Vaccaro F, Guitaldi R, Di Martino A, Cenacchi A, Fornasari PM, Marcacci M. Platelet-rich plasma intra-articular injections for cartilage degeneration and osteoarthritis: single- versus double-spinning approach. Knee Surg Sports Traumatol Arthrosc
92 Publications Dermatology Anitua E, Sánchez M, Nurden AT, Nurden P, Orive G, Andía I. New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol 2006;24: Anitua E, Sánchez M, Orive G, Andía I. The potential impact of the preparation rich in growth factors (PRGF) in different medical fields. Biomaterials 2007;28: Anitua E, Sánchez M, Orive G, Andia I. Delivering growth factors for therapeutics. Trends Pharmacol Sci. 2008;29:37-41 Anitua E, Sánchez M, Orive G. Potential of endogenous regenerative technology for in situ regenerative medicine. Adv Drug Deliv Rev 2010;62: Preclinical Research Molina-Miñano F, López-Jornet P, Camacho- Alonso F, Vicente-Ortega V. The use of plasma rich in growth factors on wound healing in the skin: experimental study in rabbits. Int Wound J. 2009;6: Clinical Research Anitua E, Aguirre JJ, Algorta J, Ayerdi E, Cabezas AI, Orive G, Andia I. Effectiveness of autologous preparation rich in growth factors for the treatment of chronic cutaneous ulcers. J Biomed Mater Res B Appl Biomater. 2008;84: Orcajo B, Muruzabal F, Isasmendi MC, Gutierrez N, Sánchez M, Orive G, Anitua E. The use of plasma rich in growth factors (PRGF-Endoret) in the treatment of a severe mal perforant ulcer in the foot of a person with diabetes. Diabetes Res Clin Pract. 2011;93:e65-e67. Aguirre JJ et al. Eficacia del PRGF en el tratamiento de las úlceras cutáneas secundarias a insuficiencia venosa: Ensayo clínico aleatorizado controlado con tratamiento convencional
93 BTI Biotechnology Institute S.L.
94
95
96 USA 1730 Walton Road Suite 110 Blue Bell, PA USA Tel: (12) Fax: (12) Cat Ed.2 - Rev.0 FEB2012 UK 870 The Crescent Colchester Business Park Colchester Essex CO49YQ United Kingdom Tel: (44) Fax: (44) [email protected] GERMANY Mannheimer Str Pforzheim Germany Tel: (49) Fax: (49) [email protected] ITALY Piazzale Piola, Milan Italy Tel: (39) Fax: (39) [email protected] BTI Biotechnology Institute San Antonio, 15 5º Vitoria-Gasteiz (Álava) SPAIN Tel: Fax: [email protected] MEXICO Ejercito Nacional Mexicano 351, 3A Col. Granada Delegación Miguel Hidalgo México DF CP Mexico Tel: (52) Fax: (52) [email protected] PORTUGAL Praça Mouzinho de Albuquerque, 113, 5º Porto PORTUGAL Tel: (351) Fax: (351) [email protected] BTI RESEARCH BIOTECHNOLOGY INSTITUTE SCAN THIS CODE with your mobile phone and to access all the information of BTI Biotechnology Institute.
Endogenous Regenerative Technology. oral surgery. www.bti-implant.us. Regenerative Medicine
 Endogenous Regenerative Technology oral surgery www.bti-implant.us Regenerative Medicine LEADER IN REGENERATIVE MEDICINE BTI Biotechnology Institute is a Spanish biomedicine company focused on the development
Endogenous Regenerative Technology oral surgery www.bti-implant.us Regenerative Medicine LEADER IN REGENERATIVE MEDICINE BTI Biotechnology Institute is a Spanish biomedicine company focused on the development
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
Bone augmentation procedure without wound closure
 THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
vitality meets bone volume around dental implants Straumann BoneCeramic
 vitality meets bone volume around dental implants Straumann BoneCeramic The vitality you need around your implants Bone volume restoration and preservation for the desired esthetic outcome Image by PD
vitality meets bone volume around dental implants Straumann BoneCeramic The vitality you need around your implants Bone volume restoration and preservation for the desired esthetic outcome Image by PD
The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review
 IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
Technology Breakthrough in Spinal Implants (Technical Insights)
 Technology Breakthrough in Spinal Implants (Technical Insights) Biomaterial innovations is a growth factor for spinal implant market June 2014 Table of Contents Section Page Number Executive Summary 4
Technology Breakthrough in Spinal Implants (Technical Insights) Biomaterial innovations is a growth factor for spinal implant market June 2014 Table of Contents Section Page Number Executive Summary 4
Dental Bone Grafting Options. A review of bone grafting options for patients needing more bone to place dental implants
 Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
Photofunctionalization
 Photofunctionalization One and only technology to overcome the biological aging of titanium Scientific brochure of photofunctionalization Volume 1, Issue 1, 2013 published by Global Network for Photofunctionalized
Photofunctionalization One and only technology to overcome the biological aging of titanium Scientific brochure of photofunctionalization Volume 1, Issue 1, 2013 published by Global Network for Photofunctionalized
INFUSE Bone Graft (rhbmp-2/acs)
 1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery. Consequences of tooth loss.
 Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Anatomic limitations in the maxilla provide challenges
 Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
chronos BOne VOid Filler Beta-Tricalcium Phosphate (b-tcp) bone graft substitute
 chronos BOne VOid Filler Beta-Tricalcium Phosphate (b-tcp) bone graft substitute chronos Bone Void Filler Osteoconductive Resorbable Synthetic chronos Granules and Preforms are synthetic, porous, osteoconductive,
chronos BOne VOid Filler Beta-Tricalcium Phosphate (b-tcp) bone graft substitute chronos Bone Void Filler Osteoconductive Resorbable Synthetic chronos Granules and Preforms are synthetic, porous, osteoconductive,
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Comparison of Peri-Implant Bone Loss
 Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan
 Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
San Diego Stem Cell Treatment Center Frequently Asked Questions
 San Diego Stem Cell Treatment Center Frequently Asked Questions What is a Stem Cell? A stem cell is basically any cell that can replicate and differentiate. This means the cell can not only multiply, but
San Diego Stem Cell Treatment Center Frequently Asked Questions What is a Stem Cell? A stem cell is basically any cell that can replicate and differentiate. This means the cell can not only multiply, but
Implants in your Laboratory: Abutment Design
 1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
Straumann Dental Implant System. Implant Selection Guide.
 Straumann Dental Implant System. Implant Selection Guide. STRAUMANN's IMPLANT PORTFOLIO The Straumann Dental Implant System offers two implant lines with diverse body and neck designs ranging from the
Straumann Dental Implant System. Implant Selection Guide. STRAUMANN's IMPLANT PORTFOLIO The Straumann Dental Implant System offers two implant lines with diverse body and neck designs ranging from the
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Ceramics on Implants Fixed Zirconium Dioxide-Based Restorations in the Rehabilitation of the Edentulous upper Jaw
 38 STARGET 1 I 11 ceramic restorations arne F. BOEcklER and MIcHaEl seitz Ceramics on Implants Fixed Zirconium Dioxide-Based Restorations in the Rehabilitation of the Edentulous upper Jaw Introduction
38 STARGET 1 I 11 ceramic restorations arne F. BOEcklER and MIcHaEl seitz Ceramics on Implants Fixed Zirconium Dioxide-Based Restorations in the Rehabilitation of the Edentulous upper Jaw Introduction
Dental Implant Options in Atrophic Jaws
 Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on Periodontology
 J Clin Periodontol 2008; 35 (Suppl. 8): 168 172 doi: 10.1111/j.1600-051X.2008.01268.x Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on
J Clin Periodontol 2008; 35 (Suppl. 8): 168 172 doi: 10.1111/j.1600-051X.2008.01268.x Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on
it will set at body temperature, and it will grow. UNIQUE FORMULATIONS
 BETTER BONE GRAFT FORMULATION. SUPERIOR BONE GRAFT HANDLING. When choosing a Demineralized Bone Matrix, remember that not all products are created equal. For excellent clinical performance and patient
BETTER BONE GRAFT FORMULATION. SUPERIOR BONE GRAFT HANDLING. When choosing a Demineralized Bone Matrix, remember that not all products are created equal. For excellent clinical performance and patient
The immediate post-extractional insertion of screw implants in dental practice
 VARIA The immediate post-extractional insertion of screw implants in dental practice Ioan Sîrbu, Emanuel Bratu, Mihai Sandulescu, Gabriela Tanase, Ion Popovici Bucuresti, Romania Summary This article presents
VARIA The immediate post-extractional insertion of screw implants in dental practice Ioan Sîrbu, Emanuel Bratu, Mihai Sandulescu, Gabriela Tanase, Ion Popovici Bucuresti, Romania Summary This article presents
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
CDT 2015 Code Change Summary New codes effective 1/1/2015
 CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
Biotechnology. Srivatsan Kidambi, Ph.D.
 Stem Stem Cell Cell Engineering-What, Biology and it Application Why, How?? to Biotechnology Srivatsan Kidambi, Ph.D. Assistant Professor Department of Chemical & Biomolecular Engineering University of
Stem Stem Cell Cell Engineering-What, Biology and it Application Why, How?? to Biotechnology Srivatsan Kidambi, Ph.D. Assistant Professor Department of Chemical & Biomolecular Engineering University of
MAIN LINE DENTAL IMPLANT CENTER
 1257 Lancaster Ave Berwyn, PA 19312 Tel: 610-722-5542 CHIUN-LIN (STEVEN), LIU D.D.S., D.M.D. School of Dental Medicine CURRICULUM VITAE Summer, 2012 Education: 1987-1993 D.D.S. Kaohsiung Medical University
1257 Lancaster Ave Berwyn, PA 19312 Tel: 610-722-5542 CHIUN-LIN (STEVEN), LIU D.D.S., D.M.D. School of Dental Medicine CURRICULUM VITAE Summer, 2012 Education: 1987-1993 D.D.S. Kaohsiung Medical University
Saudi Fellowship In Dental Implant (SF-DI)
 Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Bisphosphonate therapy. osteonecrosis of the jaw
 I overview Bisphosphonate therapy and osteonecrosis of the jaw Authors_Johannes D. Bähr, Prof. Dr Dr Peter Stoll & Dr Georg Bach, Germany _Introduction Fig. 1_Structural formula of pyrophosphate and basic
I overview Bisphosphonate therapy and osteonecrosis of the jaw Authors_Johannes D. Bähr, Prof. Dr Dr Peter Stoll & Dr Georg Bach, Germany _Introduction Fig. 1_Structural formula of pyrophosphate and basic
The SATURN implant by Cortex Dental Industries
 The SATURN implant by Cortex Dental Industries By Dr. Zvi Laster DMD W e P r o v e I t E v e r y D a y A case report using a newly designed implant specifically designed for immediate post-extraction loading
The SATURN implant by Cortex Dental Industries By Dr. Zvi Laster DMD W e P r o v e I t E v e r y D a y A case report using a newly designed implant specifically designed for immediate post-extraction loading
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Effets biologiques des facteurs de croissance sur la régénération musculaire
 Effets biologiques des facteurs de croissance sur la régénération musculaire Xavier Bigard (MD, PhD) Professeur Agrégé du Val-de-Grâce Institut de Recherche Biomédicale des Armées (IRBA) La Tronche (Grenoble)
Effets biologiques des facteurs de croissance sur la régénération musculaire Xavier Bigard (MD, PhD) Professeur Agrégé du Val-de-Grâce Institut de Recherche Biomédicale des Armées (IRBA) La Tronche (Grenoble)
Dental care and treatment for patients with head and neck cancer. Department of Restorative Dentistry Information for patients
 Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
BioHorizons Education Programme 2015
 BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
UNMH Oral and Maxillofacial Surgery Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All-on-4 treatment concept with NobelSpeedy Groovy
 All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
 BISPHOSPHONATE RELATED OSTEONECROSIS OF THE JAW (BRONJ) BISPHOSPHONATES AND WHAT HAPPENS TO BONE VINCENT E. DIFABIO, DDS, MS MEMBER OF THE COMMITTEE ON HEALTHCARE AND ADVOCACY FROM THE AMERICAN ASSOCIATION
BISPHOSPHONATE RELATED OSTEONECROSIS OF THE JAW (BRONJ) BISPHOSPHONATES AND WHAT HAPPENS TO BONE VINCENT E. DIFABIO, DDS, MS MEMBER OF THE COMMITTEE ON HEALTHCARE AND ADVOCACY FROM THE AMERICAN ASSOCIATION
Accelerated recovery of post-operative dental implant patients by means of pulsed shortwave (SWT) therapy: An Observational Study
 Bartolomeo Operti, MD and Dr Tiziano Tealdo Accelerated recovery of post-operative dental implant patients by means of pulsed shortwave (SWT) therapy: Bartolomeo Operti, MD Chief of Anesthesia Department
Bartolomeo Operti, MD and Dr Tiziano Tealdo Accelerated recovery of post-operative dental implant patients by means of pulsed shortwave (SWT) therapy: Bartolomeo Operti, MD Chief of Anesthesia Department
Tooth out what's next?
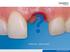 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANTS IN FOCUS. Endosseous dental implant restorations PLANNING FOR IMPLANT RESTORATIONS
 IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
STEM CELL FELLOWSHIP
 Module I: The Basic Principles of Stem Cells 1. Basics of Stem Cells a. Understanding the development of embryonic stem cells i. Embryonic stem cells ii. Embryonic germ cells iii. Differentiated stem cell
Module I: The Basic Principles of Stem Cells 1. Basics of Stem Cells a. Understanding the development of embryonic stem cells i. Embryonic stem cells ii. Embryonic germ cells iii. Differentiated stem cell
Inflammation and Healing. Review of Normal Defenses. Review of Normal Capillary Exchange. BIO 375 Pathophysiology
 Inflammation and Healing BIO 375 Pathophysiology Review of Normal Defenses Review of Normal Capillary Exchange 1 Inflammation Inflammation is a biochemical and cellular process that occurs in vascularized
Inflammation and Healing BIO 375 Pathophysiology Review of Normal Defenses Review of Normal Capillary Exchange 1 Inflammation Inflammation is a biochemical and cellular process that occurs in vascularized
The definitive implant restoration
 CASE REPORT Implant Bone Rings. One-Stage Three-Dimensional Bone Transplant Technique: A Case Report Mark R. Stevens, DDS 1 * Hany A. Emam, MS 2 Mahmoud E. L. Alaily, MS 3 Mohamed Sharawy, PhD 4 A variety
CASE REPORT Implant Bone Rings. One-Stage Three-Dimensional Bone Transplant Technique: A Case Report Mark R. Stevens, DDS 1 * Hany A. Emam, MS 2 Mahmoud E. L. Alaily, MS 3 Mohamed Sharawy, PhD 4 A variety
PowerLight LED Light Therapy. The FUTURE of corrective skin
 PowerLight LED Light Therapy The FUTURE of corrective skin care TODAY LED facial treatments Effective when used with correct protocols Non thermal stimulation of collagen Increases circulation and lymphatic
PowerLight LED Light Therapy The FUTURE of corrective skin care TODAY LED facial treatments Effective when used with correct protocols Non thermal stimulation of collagen Increases circulation and lymphatic
Rehabilitation of a complex case with zirconium dental implants
 Rehabilitation of a complex case with zirconium dental Authors_Dr Andrea Enrico Borgonovo, Dr Marcello Dolci, Dr Rachele Censi, Dr Oscar Arnaboldi, Dr Virna Vavassori & Prof Carlo Maiorana, Italy _Introduction
Rehabilitation of a complex case with zirconium dental Authors_Dr Andrea Enrico Borgonovo, Dr Marcello Dolci, Dr Rachele Censi, Dr Oscar Arnaboldi, Dr Virna Vavassori & Prof Carlo Maiorana, Italy _Introduction
Dental Implants - the tooth replacement solution
 Dental Implants - the tooth replacement solution Are missing teeth causing you to miss out on life? Missing teeth and loose dentures make too many people sit on the sidelines and let life pass them by.
Dental Implants - the tooth replacement solution Are missing teeth causing you to miss out on life? Missing teeth and loose dentures make too many people sit on the sidelines and let life pass them by.
Foundation Revolutionary Bone Augmentation Material. Thinking ahead. Focused on life. Regional Partner
 Foundation Revolutionary Bone Augmentation Material Thinking ahead. Focused on life. Regional Partner Stimulates New Bone Growth Foundation is a collagen-based, bone filling augmentation material for use
Foundation Revolutionary Bone Augmentation Material Thinking ahead. Focused on life. Regional Partner Stimulates New Bone Growth Foundation is a collagen-based, bone filling augmentation material for use
Zimmer Trabecular Metal Dental Implant
 Zimmer Trabecular Metal Dental Implant TRABECULAR METAL MATERIAL: Designed to Enhance Secondary Stability Through Bone Ingrowth. Artistic Rendering osseoincorporation TRABECULAR METAL MATERIAL Designed
Zimmer Trabecular Metal Dental Implant TRABECULAR METAL MATERIAL: Designed to Enhance Secondary Stability Through Bone Ingrowth. Artistic Rendering osseoincorporation TRABECULAR METAL MATERIAL Designed
Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial.
 Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial. Karaky AE, Sawair FA, Al-Karadsheh OA, Eimar HA, Algarugly SA, Baqain ZH. Eur J Oral Implantol. 2011 Spring;4(1):31-8.
Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial. Karaky AE, Sawair FA, Al-Karadsheh OA, Eimar HA, Algarugly SA, Baqain ZH. Eur J Oral Implantol. 2011 Spring;4(1):31-8.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
B978-0-443-06895-9.00005-8,
 B978-0-443-06895-9.00005-8, 00005 Chapter Restorative management 5 of dental implants 5.1 Basic implant terminology 133 5.2 Planning dental implants 134 5.3 Surgical phases 135 5.4 Provisional and definitive
B978-0-443-06895-9.00005-8, 00005 Chapter Restorative management 5 of dental implants 5.1 Basic implant terminology 133 5.2 Planning dental implants 134 5.3 Surgical phases 135 5.4 Provisional and definitive
Technological platforms
 Advitech Advitech is a life sciences & technology company Its mission is to discover and commercialize proprietary and evidence-based natural health products Focus on milk, whey and bovine colostrum R&D,
Advitech Advitech is a life sciences & technology company Its mission is to discover and commercialize proprietary and evidence-based natural health products Focus on milk, whey and bovine colostrum R&D,
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
The Very Best Reason. for Dental Implants. Gentle jawbone reconstruction with SonicWeld Rx
 The Very Best Reason for Dental Implants Gentle jawbone reconstruction with SonicWeld Rx There s a time where nothing can really hurt us It is the time where everything grows and thrives and even our teeth
The Very Best Reason for Dental Implants Gentle jawbone reconstruction with SonicWeld Rx There s a time where nothing can really hurt us It is the time where everything grows and thrives and even our teeth
DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI
 Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
Taking the Mystique out of Implant Dentistry. Dr. Michael Weinberg B.Sc., DDS, FICOI
 Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
Dental Implants in Edentulism
 Academy of Medicine, Singapore Dental Implants in Edentulism AMS-MOH Clinical Practice Guidelines 1/2012 Aug 2012 Levels of evidence and grades of recommendation Levels of evidence Level Type of Evidence
Academy of Medicine, Singapore Dental Implants in Edentulism AMS-MOH Clinical Practice Guidelines 1/2012 Aug 2012 Levels of evidence and grades of recommendation Levels of evidence Level Type of Evidence
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012
 PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
Immediate Molar Implant Placement: A Private Practice Clinical Investigation. Abstract
 Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
THE RESORBABLE MATRIX. Relax. Remaix. The membrane of choice for reliable bone and tissue regeneration
 THE RESORBABLE MATRIX Relax. Remaix. The membrane of choice for reliable bone and tissue regeneration Remaix properties Remaix is a resorbable barrier membrane for use in guided bone regeneration (GBR)
THE RESORBABLE MATRIX Relax. Remaix. The membrane of choice for reliable bone and tissue regeneration Remaix properties Remaix is a resorbable barrier membrane for use in guided bone regeneration (GBR)
Flapless Implant Surgery for Replacement of Posterior Teeth
 Course Number: 108.2 Flapless Implant Surgery for Replacement of Posterior Teeth Authored by J. Steven Cloyd, DDS Upon successful completion of this CE activity 1 CE credit hour may be awarded A Peer-Reviewed
Course Number: 108.2 Flapless Implant Surgery for Replacement of Posterior Teeth Authored by J. Steven Cloyd, DDS Upon successful completion of this CE activity 1 CE credit hour may be awarded A Peer-Reviewed
Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
THE CARTILAGE IMPLANT FOR BIOLOGICAL CARTILAGE REPAIR
 THE CARTILAGE IMPLANT FOR BIOLOGICAL CARTILAGE REPAIR 02/13 Content chondrotissue (p.4) Scientific Background (p.5) Preclinical Outcomes (p.6) Clinical Outcomes: MRI Evaluation (p.7) Clinical Outcomes:
THE CARTILAGE IMPLANT FOR BIOLOGICAL CARTILAGE REPAIR 02/13 Content chondrotissue (p.4) Scientific Background (p.5) Preclinical Outcomes (p.6) Clinical Outcomes: MRI Evaluation (p.7) Clinical Outcomes:
Osteoporosis Medicines and Jaw Problems
 Osteoporosis Medicines and Jaw Problems J. Michael Digney, D.D.S. Osteoporosis is a condition that affects over 10 million patients in this country, with the majority of those being post-menopausal women.
Osteoporosis Medicines and Jaw Problems J. Michael Digney, D.D.S. Osteoporosis is a condition that affects over 10 million patients in this country, with the majority of those being post-menopausal women.
Emdogain. The reliable solution for periodontal treatment.
 Emdogain The reliable solution for periodontal treatment. Straumann is the exclusive industrial partner of the ITI (International Team for Implantology) in the areas of research, development, and education.
Emdogain The reliable solution for periodontal treatment. Straumann is the exclusive industrial partner of the ITI (International Team for Implantology) in the areas of research, development, and education.
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
Prosthodontist s Perspective
 Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Retrospective study on the survival rate of IBS implant
 Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
Don t Let Life Pass You By Because Of Missing Teeth
 Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
Cross-sectional. Translate Lp3 after. Translate Lp3 after. Tipping Up3 after. ext Up2. ext Lp2. ext Lp2. Bur buc-ling with flap
 Table 2.1 Tooth movement following alveolar decortication injury is represented by 10 evidence-based, refereed, professional journal articles through to May 2013. All investigations include measurements
Table 2.1 Tooth movement following alveolar decortication injury is represented by 10 evidence-based, refereed, professional journal articles through to May 2013. All investigations include measurements
CAD/CAM technology supporting successful implant therapy
 CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Replacement of a single front tooth Surgical procedure and three-year results
 Case Report 10 2011 Replacement of a single front tooth Surgical procedure and three-year results Dr Peter Randelzhofer Munich, Germany Prosthetics Dr Peter Randelzhofer studied dentistry in Munich, Germany,
Case Report 10 2011 Replacement of a single front tooth Surgical procedure and three-year results Dr Peter Randelzhofer Munich, Germany Prosthetics Dr Peter Randelzhofer studied dentistry in Munich, Germany,
CHAPTER 10 RESTS AND PREPARATIONS. 4. Serve as a reference point for evaluating the fit of the framework to the teeth.
 CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
INFUSE Bone Graft Oral Maxillofacial Bone Grafting Procedures
 INFUSE Bone Graft Oral Maxillofacial Bone Grafting Procedures Dental Products Advisory Panel Committee Ed Chin, DPh Group Director, Regulatory Affairs Medtronic Spinal and Biologics 1 INFUSE Bone Graft
INFUSE Bone Graft Oral Maxillofacial Bone Grafting Procedures Dental Products Advisory Panel Committee Ed Chin, DPh Group Director, Regulatory Affairs Medtronic Spinal and Biologics 1 INFUSE Bone Graft
