Contemporary Management of Malignant Pleural Mesothelioma
|
|
|
- Hortense Horn
- 8 years ago
- Views:
Transcription
1 Contemporary Management of Malignant Pleural Mesothelioma ERIC G. BUTCHART University Hospital of Wales, Cardiff, United Kingdom Key Words. Mesothelioma Surgery Radiotherapy Chemotherapy Immunology Gene therapy ABSTRACT The rapidly increasing incidence of malignant pleural mesothelioma underlines the urgency to achieve a consensus in the management of this tumor, which is biologically distinct from most other tumors. For patients with stage I tumors of epithelial type and good performance status, pleuropneumonectomy combined with chemotherapy and radiotherapy provides the best chance of prolonged survival, but further investigation is required to determine the optimum combination of adjuvant therapy. Debulking pleurectomy/decortication combined with adjuvant therapy is a worthwhile alternative for patients with more advanced disease, impaired performance status or tumors of less favorable histology (sarcomatous or biphasic). More clinical trials are urgently required to identify better adjuvant therapy for tumors containing sarcomatous elements. On currently available evidence, neither radiotherapy nor chemotherapy offer worthwhile prolonged disease control when used in isolation, although both have an important role as part of multimodality therapy. Hyperthermia may enhance the effect of both radiotherapy and chemotherapy, and newer radiosensitizing agents also need evaluating. Research into immunotherapy and gene therapy suggests that these newer approaches may have a place if tumor volume is small. In practice they will probably need to be combined with other therapeutic modalities, and further clinical trials are required. Consensus in mesothelioma management currently remains elusive but it seems clear that the way forward will involve striving for much earlier diagnosis, the use of multimodality therapy and collaboration between centers with special expertise in mesothelioma treatment to organize multicenter trials. The Oncologist 1999;4: There is no clear consensus on the treatment of malignant pleural mesothelioma, in contrast to the treatment of most other tumors. This is particularly unfortunate as the natural history of the tumor is one of rapid progression towards death within months of first symptoms if untreated [1, 2]. The need to find effective treatment is given added urgency by the dramatically increasing incidence of mesothelioma in most western countries, and this is expected to peak around the year 2020 [3]. It is estimated that mesothelioma deaths in men will double over the next 20 years [3]. The reasons for a lack of consensus in the management of mesothelioma are partly historical, partly related to the unique biology of the tumor and partly due to failure so far to find any single treatment or treatment combination which offers more than short-term tumor suppression in most patients. Historically, the very existence of a primary tumor of the pleura was disputed in the first half of this century [4] and, even when it became accepted as a distinct entity with a clear relationship to asbestos exposure in many patients [5], difficulties were still encountered in distinguishing the tumor from adenocarcinoma in many instances [6]. Until more sophisticated immunocytochemical techniques were developed to distinguish between epithelial mesothelioma and adenocarcinoma, there is no doubt that many cases treated as mesothelioma were, in fact, cases of secondary adenocarcinoma. This added to the confusion in the interpretation of the results of treatment. The biological behavior of mesothelioma is distinct from that of other solid tumors in that mesothelioma tends to grow in a sheet-like fashion, covering the surface of the parietal and then the visceral pleura; it shows little tendency to invade structures deep into the pleura in the early course of the disease, unless the pleura is breached by needles or Correspondence: Eric G. Butchart, M.D., Consultant Cardiothoracic Surgeon, University Hospital, Cardiff, CF4 4XW, Wales, UK. Telephone: ; Fax: ; egbutchart@aol.com Accepted for publication October 10, AlphaMed Press /99/$5.00/0 The Oncologist 1999;4:
2 Butchart 489 tubes, when it will spread readily along needle or tube tracks [7]. Part of the explanation for this unusual behavior appears to lie in the relative lack of proteases in comparison to other solid tumors [8]. In many instances the tumor appears to begin in a multifocal fashion resulting in scattered deposits of tumor with normal pleura intervening, suggesting either that a field change has occurred throughout the pleura, or that the tumor has metastasized locally within the pleural cavity [9]. Because the tumor is either broadly extensive on the pleural surface or multifocal at the time of detection, it does not lend itself to localized surgical excision. Surgical treatment aimed at complete resection therefore has to be much more extensive and is only suitable for a minority of patients (vide infra). Although much research work is in progress, more innovative approaches to treatment using immunotherapy or gene therapy have yet to make an impact [10]. Preliminary results suggest that they are unlikely to be effective alone and will probably need to be combined with conventional treatment. Further advances will only come from a better understanding of tumor biology [11, 12]. Meanwhile, the poor response to a wide variety of surgical approaches and conventional radiotherapy and chemotherapy, with a large number of different agents, continues to foster a rather nihilistic attitude toward the management of mesothelioma, and many chest physicians and oncologists recommend only palliative treatment to control recurrent pleural effusion [13]. Logically, selection of treatment should, as with other tumors, depend on histological type, tumor stage at the time of presentation and on the patient s performance status, particularly in relation to cardiac and respiratory function. HISTOLOGICAL TYPE Diffuse malignant pleural mesothelioma is classified by three histological types: pure epithelial (tubopapillary), pure mesenchymal (sarcomatous) or a mixture of the two (biphasic). Several series have demonstrated that pure epithelial mesothelioma is associated with a better prognosis [14-16] and that it responds better to radical surgery [14, 17]. Fortunately, epithelial mesothelioma is the most common histological type in most series. As with lung cancer treatment, it is likely that different approaches will be required for tumors of different histological type. TUMOR STAGING Several different staging classifications have been proposed for mesothelioma, the most recent and comprehensive being that proposed by the International Mesothelioma Interest Group (IMIG) based on the tumor/node/metastasis (TNM) system [18]. The IMIG staging system has been validated by Rusch and found to correlate well with prognosis Table 1. Butchart staging system [14] Stage 1 Tumor confined within the capsule of the parietal pleura, i.e. involving only ipsilateral pleura, lung, diaphragm, and external surface of pericardium within the pleural reflection. Stage II Tumor invading chest wall or mediastinal tissues or structures, e.g., esophagus, trachea, great vessels. Lymph node involvement within the chest. Stage III Tumor penetrating diaphragmatic muscle to involve peritoneum or the retroperitoneal space. Tumor penetrating pericardium to involve its internal surface or the heart. Involvement of the opposite pleura. Lymph node involvement outside the chest. Stage IV Distant blood-borne metastases. [16]. The first staging system, which the current author proposed in 1976 [14] (referred to subsequently in the literature as the Butchart staging system), still has the advantage of simplicity and relevance to prognosis and therapeutic options (Table 1); whereas the IMIG staging system (Table 2) may only be applied postoperatively or at autopsy, as it relies on histological criteria to differentiate one stage from another. It is therefore impossible to implement accurately in nonsurgical treatment regimes. In the Butchart staging system, stage I disease is tumor which has not invaded structures beyond the parietal pleura and has not metastasized to regional lymph nodes or beyond. Its relationship to prognosis, demonstrated first in 1976 on a relatively small number of patients undergoing radical surgery [14], has been confirmed most recently in a large series of 183 patients treated by pleuropneumonectomy and adjuvant therapy. In this series patients with negative resection margins and negative lymph nodes (Butchart stage I) had significantly better survival [17]. There is very little difference between the Butchart staging system and the IMIG system in the designation of stage I, except that in the IMIG system confluent visceral pleural tumor or extension of tumor into the paraenchyma of the lung places the tumor in stage II. However, in practice, scattered foci of visceral pleural tumor (IMIG stage I) very quickly coalesce to form confluent tumor, and in early disease it is very common to encounter a mixture of scattered foci in some areas and early confluence of some foci in others. Furthermore, once the visceral pleura is involved by tumor, parenchymal lung involvement is inevitable, as microscopic tumor spreads into the lung along the fibrous septa of the pulmonary lobules. More importantly, from a practical point of view, neither confluent visceral tumor nor parenchymal pulmonary invasion prejudice complete removal of tumor by pleuropneumonectomy.
3 490 Contemporary Management of Malignant Pleural Mesothelioma Table 2. IMIG staging system [18] T1 T1a Tumor limited to the ipsilateral parietal pleura, including mediastinal and diaphragmatic pleura No involvement of the visceral pleura T1b Tumor involving the ipsilateral parietal pleura, including mediastinal and diaphragmatic pleura Scattered foci of tumor also involving the visceral pleura T2 Tumor involving each of the ipsilateral pleural surfaces (parietal, mediastinal, diaphragmatic, and visceral pleura) with at least one of the following features: involvement of diaphragmatic muscle confluent visceral pleural tumor (including the fissures) or extension of tumor from visceral pleural into the underlying pulmonary parenchyma T3 Describes locally advanced but potentially resectable tumor Tumor involving all of the ipsilateral pleural surfaces (parietal, mediastinal, diaphragmatic, and visceral pleural) with at least one of the following features: involvement of the endothoracic fascia extension into the mediastinal fat solitary, completely resectable focus of tumor extending into the soft tissues of the chest wall nontransmural involvement of the pericardium T4 Describes locally advanced technically unresectable tumor Tumor involving all of the ipsilateral pleural surfaces (parietal, mediastinal, diaphragmatic, and visceral) with at least one of the following features: diffuse extension or multifocal masses of tumor in the chest wall with or without associated rib destruction direct transdiaphragmatic extension of tumor to the peritoneum direct extension of tumor to the contralateral pleura direct extension of tumor to one or more mediastinal organs direct extension of tumor into the spine tumor extending through to the internal surface of the pericardium with or without a pericardial effusion; or tumor involving the myocardium N Lymph nodes NX Regional lymph nodes cannot be assessed N0 No regional lymph node metastases N1 Metastases in the ipsilateral bronchopulmonary or hilar lymph nodes N2 Metastases in the subcarinal or the ipsilateral mediastinal lymph nodes, including the ipsilateral internal mammary nodes N3 Metastases in the contralateral mediastinal, contralateral internal mammary, ipsilateral, or contralateral supraclavicular lymph nodes M Metastases MX Presence of distant metastases cannot be assessed M0 No distant metastasis M1 Distant metastasis present Stage Description Stage Description Stage Ia T1a N0 M0 Stage III Any T3 M0 Any N1 M0 Any N2 M0 Stage Ib T1b N0 M0 Stage IV Any T4 Any N3 Any M1 Stage II T2 N0 M0 More significant differences exist between the Butchart and the IMIG staging systems in the more advanced stages. In the IMIG system, any lymph node involvement places the tumor at least in stage III, whereas in the Butchart system,
4 Butchart 491 ipsilateral or mediastinal intrathoracic lymph node involvement is stage II. In the author s experience, truly contralateral intrathoracic nodal involvement is very unusual. The IMIG system adopts the same nomenclature for node status as the TNM classification for lung cancer, with hilar nodes being classified as N1 and mediastinal or internal mammary nodes classified as N2. With a tumor which begins in the parietal pleura, this is illogical, as internal mammary nodes are often involved before hilar nodes. Only mediastinal nodes may be sampled by mediastinoscopy and it is therefore not possible to accurately assess nodal status fully with this procedure prior to beginning treatment. It is possible, however, to sample all nodes using frozen section histology at the time of surgical exploration. In the Butchart staging system tumor is resectable, although with reduced prognosis, up to stage II, whereas in the IMIG system, tumor is deemed resectable up to stage III, while stage IV contains inoperable tumor, contralateral and extrathoracic nodal involvement and metastatic disease. Both staging systems have advantages and disadvantages. To avoid confusion, all further references to stage in this review article use the Butchart staging system. Readers may convert to the IMIG system if they wish by using Tables 1 and 2. The problem with all staging systems is that currently available imaging techniques do not reliably identify tumor stage, especially in early disease when tumor volume is relatively small. Because of potential staging inaccuracies, therapeutic regimes which do not involve surgical treatment are more difficult to evaluate. Gross chest wall involvement with rib destruction is easily identified on computerized tomography (CT) scan; but, at the other end of the spectrum, early chest wall involvement associated with minimal pleural thickening is sometimes impossible to detect with any imaging technique and can only be identified with certainty at operation, when the parietal pleura is stripped off the chest wall by blunt dissection. As with other tumors, the larger the tumor the more likely it is to have metastasized or invaded neighboring structures. Not surprisingly therefore, total tumor volume, as measured by three-dimensional CT, correlates with nodal status, overall staging, and survival [19]. However, autopsies on individual patients with tumors of epithelial type reveal that occasional patients die from extensive tumor bulk within the hemithorax, causing respiratory failure without any spread of tumor outside the confines of the parietal pleura or lymph node involvement [14]. Despite the effect of overall tumor bulk on prognosis in most patients, locally bulky disease does not necessarily predict local invasion at that site, in the author s experience. Hence local tumor thickness per se should not be taken as evidence of inoperability. Loss of fat planes between thickened pleura and underlying structures and tumor surrounding more than 50% of a mediastinal structure do, however, raise likelihood of involvement [20]. Thoracoscopy can provide information on the degree of parietal and visceral pleural involvement, but can provide no information on invasion of underlying structures. It therefore cannot reliably predict stage Ia or Ib according to the IMIG system. Diaphragmatic muscle involvement and eventual penetration to involve the peritoneal surface is particularly difficult to detect unless it is gross in extent. Magnetic resonance imaging (MRI) provides coronal and sagittal images in addition to axial images and hence offers slightly better assessment of diaphragmatic involvement than CT [20]. Laparoscopy has proved useful in detecting diaphragmatic penetration in equivocal cases [21]. Coronal MRI images provide better assessment of apical disease [22] spread into the fissures and bone invasion [23] than CT. MRI is also useful in distinguishing between benign and malignant pleural thickening [24]. PERFORMANCE STATUS A detailed assessment of performance status is an essential precursor to treatment planning, particularly if radical surgical treatment is contemplated. Pleuropneumonectomy is a major surgical procedure which is suitable only for very fit patients. Once the disease is established, lung function tests unfortunately provide little guidance on pulmonary reserve, as they are dominated by the effects of the pleural effusion and pulmonary restriction caused by tumor on the lung surface. Much better information is provided by a detailed history of premorbid exercise capacity and respiratory symptoms, coupled with CT assessment of the contralateral lung. Patients being considered for radical surgery should have a history of good exercise tolerance without dyspnea prior to developing mesothelioma and should be free of chronic bronchitis or asthma. The contralateral lung should be normal on CT; evidence of emphysema or asbestosis for example should preclude radical surgery. Cardiac assessment involves a detailed history and examination supplemented by exercise electrocardiogram and echocardiography. Radical surgery should only be contemplated in patients with normal cardiac function. Nutritional status is also important. Neither cachetic patients nor very obese patients are suitable for radical surgery. Renal function should be normal to reduce the risk of renal failure both postoperatively and following subsequent chemotherapy. Few patients over the age of 70 will be suitable for radical surgery unless exceptionally fit. CHOICE OF TREATMENT Given that no form of treatment currently available can reliably eradicate mesothelioma, it is important to have a full and open discussion with the patient and his or her family
5 492 Contemporary Management of Malignant Pleural Mesothelioma regarding treatment options. For patients who are very elderly, frail or compromised by other medical conditions or whose disease is at an advanced stage, there is little controversy: only palliative treatment or supportive care should be advised. However, for younger, fitter patients and particularly those with early disease, the choice of treatment is more controversial. Many patients will have difficulty accepting that the disease is incurable or that nothing can be done and will wish to explore all possible therapeutic options. Nowadays many patients access the medical literature via the internet and are already well informed at the first consultation. Ethical issues in relation to clinical trials also need to be taken into consideration given that the literature contains numerous phase II trials of various chemotherapeutic agents, either alone or in combination, which produce only short-term tumor regression in a minority of patients. Hopes should therefore not be falsely raised that a new drug in a forthcoming trial may cure or even control the disease. SURGICAL TREATMENT Surgery in mesothelioma can be radical, debulking or palliative. Radical surgery (pleuropneumonectomy) aims to eradicate all macroscopic disease and is therefore feasible only in stage I or early stage II disease (involved nodes or early localized chest wall invasion). All of the ipsilateral pleura, lung and pericardium are removed and, because diaphragmatic pleura cannot be separated from the diaphragmatic muscle for embryological reasons, it is necessary to remove the hemidiaphragm also as part of the procedure. Visualization of the diaphragm is facilitated by two levels of access to the chest through the same skin incision (Fig. 1) [7], although some surgeons use a single thoracotomy incision [17]. Debulking surgery involves parietal pleurectomy (leaving diaphragmatic pleura in place) and decortication of the lung (inevitably leaving some tumor on or in the lung in most cases) and is usually combined with other treatment modalities. Pleuropneumonectomy is a very major operation and in the author s view has no place as a debulking procedure, for example leaving the diaphragm in place with tumor covering it in the so-called modified pleuropneumonectomy procedure. Palliative surgery ranges from thoracoscopy and talc pleurodesis to more limited pleurectomy to achieve pleural symphysis [7]. Margin of clearance is an issue which continues to cause controversy. If pleuropneumonectomy has been used as a debulking procedure only, margins will clearly be positive. Even if it is used radically with curative intent in early disease, performing an extracapsular excision by staying outside the parietal pleura and resecting the diaphragm (Fig. 1), margins of clearance will be very small. The definition of negative resection margins depends on the criteria used by each pathologist and on the number and location of sites sampled on each specimen. Radical surgery is a major operation, suitable only for fit patients with normal cardiopulmonary function. In the past, pleuropneumonectomy has been condemned on the grounds of high mortality and morbidity and failure to achieve more than short to medium-term palliation. However, the results of pleuropneumonectomy in the literature need to be interpreted with caution. Many of the early reports in the literature were anecdotal accounts of two or three cases. Some authors summated the anecdotal reports of others and attempted to draw conclusions about the efficacy of the operation. In addition, Figure 1. Technique of pleuropneumonectomy. The diagram on the left shows the division of the diaphragm outside the pleural reflection, preserving the peritoneum. The middle diagram represents the division of the pericardium outside the pleural reflection. The diagram on the right shows the completion of the pneumonectomy intrapericardially and en bloc excision of mediastinal lymph nodes. ICS = intercostal space. The firm attachment of the parietal pleura to the diaphragm and pericardium is shown by the hatched lines. Reproduced with permission from [7].
6 Butchart 493 interpretation of almost all series is hindered by one or more of the following factors: Lack of information on preoperative performance status. Lack of staging information, making it likely that some unsuitable tumors of advanced stage were submitted to surgery. Selection bias, with only more advanced disease being submitted to pleuropneumonectomy, early disease being treated with pleurectomy/decortication. Lack of precise histological typing and even confusion with secondary adenocarcinoma. Lack of detail about preoperative interventions such as tube drainage of effusion, thoracoscopy or open pleural biopsy, which could have seeded tumor into the chest wall. Varied surgical technique, with some techniques certain to leave residual tumor, e.g. failure to resect the affected hemidiaphragm. Lack of information about adjuvant therapy or varied adjuvant therapy. In recent years surgical mortality has fallen to a level similar to that of pneumonectomy for lung cancer in centers with a large experience of pleuropneumonectomy, and it has become apparent that pleuropneumonectomy combined with chemotherapy and radiotherapy extends survival in some categories of patients, particularly those with pure epithelial histological type and no lymph node involvement [17]. Sugarbaker and colleagues in Boston have done much to revive interest in radical surgery for mesothelioma in recent years [17]. For many years it has been apparent that pleuropneumonectomy alone could not eradicate the tumor, even in stage I, because of small margins of clearance and the risk of tumor seeding, and that it would be necessary to combine the operation with other treatment modalities [6]. The Boston group has used both chemotherapy and radiotherapy after pleuropneumonectomy. Unfortunately, because their protocol has changed at various times over the years and they have not disaggregated the data, it is impossible to determine which combination, if any, has been most successful. Prior to 1985, a combination of doxorubicin and cyclophosphamide was used; between 1985 and 1994 cisplatin was added to this regime; between 1995 and 1997 the regime was changed to carboplatin and paclitaxel. Throughout the period of analysis external radiation therapy was used in all patients to treat the hemithorax, mediastinum and areas of residual tumor or localized positive resection margins, but the radiation dose to the mediastinum in particular appears to have been higher in recent years [17]. A further change in protocol has now been made with the use of hyperthermic intrapleural cisplatin postoperatively [25]. In recent years the results achieved by Sugarbaker and colleagues have been better than those previously reported for any treatment combination in mesothelioma (particularly in certain subsets of patients) [17]. Despite their rather surprising previous finding that positive resection margins or residual local disease did not influence survival [26], in their most recently published results on a larger series of patients, they draw attention to positive resection margins, lymph node (N2) involvement and nonepithelial histology as adverse predictors of survival [17]. Patients with epithelial histology, negative resection margins and negative lymph nodes achieved 68% two-year and 46% five-year survival [17]. These results are extremely encouraging and, if confirmed by other investigators in well-designed trials, offer considerable promise for younger, fitter patients presenting with stage I epithelial histology. They also provide scope to combine trimodality therapy with other innovative forms of treatment in the hope of improving results still further. Intrapleural interleukin 2 (IL-2) for example is reported to have a 55% response rate in early disease [27]. Pretreatment with IL-2 would thus be an approach worth evaluating. Gene therapy, which is also discussed below, may similarly have a role either pre- or postoperatively. Based on currently available evidence, fit patients with stage I epithelial mesothelioma should be offered pleuropneumonectomy followed by chemotherapy and radiotherapy. But at present, it would appear that patients with sarcomatous histology or involved intrathoracic nodes will derive little benefit from trimodality therapy according to the protocols used by Sugarbaker and colleagues [17]. However until further trials have explored other chemotherapy regimes more targeted to sarcomatous tumors rather than epithelial tumors, it is probably too early to rule out this approach altogether in these patients. Debulking surgery (pleurectomy and decortication) in combination with radiation therapy, using intraoperative brachytherapy and postoperative external beam radiation, has been reported to extend survival [28]. The place of pleurectomy/decortication has been reviewed by Rusch [16, 29] contrasting the results to pleuropneumonectomy in a personal series [16]. Median survival was greater in the pleurectomy/decortication group, but patients undergoing pleuropneumonectomy had more advanced disease and in many cases did not receive any adjuvant therapy, unlike the pleurectomy/decortication group, rendering the comparison invalid. The pattern of recurrent disease differed between the two groups of patients, with local recurrence tending to occur after pleurectomy/decortication and distant metastases after pleuropneumonectomy [16]. The risk of local recurrence after
7 494 Contemporary Management of Malignant Pleural Mesothelioma debulking surgery was not diminished by adjuvant therapy [29]. Nevertheless it was concluded that this combination of therapy remained a useful form of treatment for patients whose medical condition precluded pleuropneumonectomy [29]. Although unlikely to eradicate the disease, debulking surgery has a place in abolishing pleural effusion, controlling symptoms such as chest wall pain and extending survival when combined with other treatment modalities. It can also be used as a surgical alternative in the patient who is found at operation for planned pleuropneumonectomy to be unsuitable for this procedure because of unexpected local invasion. Thus, in otherwise fit patients, a thoracotomy is rarely a wasted or unnecessary operation in early mesothelioma, at least in cases of epithelial type. Although the data in favor of pleuropneumonectomy are persuasive, at least for epithelial mesothelioma, the choice between pleuropneumonectomy and pleurectomy/decortication in stage I disease in patients fit enough for either procedure will only be put on a scientific basis by randomized trials of one surgical procedure or the other in combination with the same adjuvant therapy. Such trials have never been performed. Limited palliative surgery in the form of thoracoscopy and talc pleurodesis to eradicate effusion is useful in patients who cannot tolerate more extensive surgery. However, adhesion between visceral and parietal pleura can only be achieved if the underlying lung will expand sufficiently to meet the chest wall. Often a rind of tumor on the lung surface will prevent this from occurring. If this is the case, a limited thoracotomy and decortication of the affected area of lung may be successful [7]. An alternative approach would be the use of intrapleural chemotherapy or immunotherapy in an attempt to reduce the bulk of tumor on the lung surface. RADIOTHERAPY Radiotherapy as a primary isolated treatment for mesothelioma has so far been unsuccessful in extending survival [30], although it appears to confer benefit when combined with other forms of treatment [17]. In general, mesothelioma is regarded as relatively radioresistant, although mesothelioma cells grown in tissue culture from different patients have shown marked variation in their response to radiation, and it has been suggested that each patient s mesothelioma cells should be assessed for radiation sensitivity before beginning a course of radiotherapy [31]. The technique of external beam radiation is important in order to achieve good pleural dose distribution while sparing the underlying lung as much as possible and shielding the liver and stomach [32]. Different methods of fractionation of radiation treatment have been evaluated following previous surgery and chemotherapy in small numbers of patients with no one particular method found to have any advantage [33]. Radiotherapy is more effective if combined with radiosensitizing agents. Paclitaxel and carboplatin both have this property and may partly account for the improved results of trimodality therapy reported by Sugarbaker and colleagues referred to above [17]. Recently it has been reported that the angiogenesis inhibitor, angiostatin, a cleavage fragment of plasminogen, interacts with radiotherapy to create a synergistic effect in some tumors [34]. There are no reports of its use in mesothelioma yet, but it would appear to merit research in this tumor also. Hyperthermia is reported to enhance the effect of radiotherapy in mesothelioma, with higher response rates and fewer in-field recurrences [35]. Radiotherapy is useful in treating localized pain due to chest wall invasion [30, 36] although pain relief is often shortlived [37] with pain recurring after a median time interval of 69 days (range days) in one large series [35]. Radiotherapy is more effective in preventing seeding into the chest wall following thoracoscopy, needle aspiration and chest tube placement [38, 39]. Patients being considered for radical surgery should therefore undergo local radiotherapy to needle, tube or thoracoscopy tracks prior to definitive treatment, delaying at least one week before surgery to allow the full cytotoxic effect of the radiotherapy to occur. CHEMOTHERAPY The literature contains numerous reports of the use of various cytotoxic drugs as primary treatment for mesothelioma, given both systemically and intrapleurally. Although many produce a response in some patients, complete response is very unusual, and partial responses occur in less than one-third of patients in most series [40]. Recently somewhat higher response rates have been reported using a combination of methotrexate and vinblastine together with cisplatin in those patients able to tolerate the latter drug (53% response rate) [41] and using paclitaxel in combination with a platinum compound. In a small series paclitaxel and carboplatin produced a 57% response rate [42]. Experimentally in mice with mesothelioma, the combination of paclitaxel and cisplatin has been shown to be synergistic, producing higher response rates than either drug singly [43]. Similar synergism has been reported between paclitaxel and arginine butyrate on mesothelioma cells in tissue culture [44]. Continuous paclitaxel infusion during radiotherapy acts as a radiation sensitizer and is reported to be well tolerated [45]. An improved response occurs in many tumors using hyperthermic chemotherapy, as malignant cells are more susceptible to the cytotoxic effect of drugs at a higher temperature [46, 47]. Optimum enhancement occurs when heat and chemotherapy are given simultaneously [48]. Some drugs only exhibit an enhanced effect when the temperature reaches C (e.g., doxorubicin and bleomycin) but in others,
8 Butchart 495 such as cisplatin, the enhanced response is linear at temperatures from C. Good tolerance and improved pharmacokinetics have been reported in a small phase I study in pleural mesothelioma using intrapleural perfusion with cisplatin at 41.5 C in combination with pleurectomy/decortication or pleuropneumonectomy [49]. No phase II studies have been reported in pleural mesothelioma but encouraging shortterm results have been reported using hyperthermic cisplatin in peritoneal mesothelioma, with no short-term recurrence of disease in optimally debulked patients [50]. Sugarbaker and colleagues are now evaluating hyperthermic cisplatin both intrapleurally and intraperitoneally following pleuropneumonectomy in a phase I trial, using sodium thiosulphate to reduce systemic toxicity (personal communication). It is hoped that intraperitoneal hyperthermic cisplatin will reduce the risk of recurrent tumor in the peritoneal cavity. The chemotherapy is followed by radiation therapy, as in their previous protocol. So far the treatment combination has been well tolerated in more than 30 patients. Full results will be reported when the trial is complete. Many oncologists take the view that as chemotherapy alone produces little more than short-term tumor regression or stabilization with no prospect of cure, it is not justified to submit patients to the unpleasant side effects of these drugs for such a brief response. Certainly the ethical issues of entering patients into clinical trials to test new cytotoxic drugs or drug combinations need to be taken into consideration before patients are invited to participate. At present it appears that the most useful role of chemotherapy in mesothelioma is as part of bimodality or trimodality therapy in patients with early epithelial tumors (stage I or very limited stage II), perhaps in association with induced local hyperthermia. Unless more effective drugs can be found, it probably cannot be justified as isolated therapy in advanced disease (stage III or IV). IMMUNOTHERAPY The positive correlation between tumor infiltrating lymphocyte numbers and better prognosis in mesothelioma [51] underlines the importance of an immunological response to the tumor, and much research has been conducted into the basic immunology of mesothelioma in recent years in the hope that this would lead to new approaches to treatment [12, 52, 53]. One of the most important cytokines involved in determining tumor growth in mesothelioma is transforming growth factorbeta (TGF-β), a potent immunosuppressant, which inhibits the immune response to the tumor and which is produced in large quantities by many mesotheliomas [52]. This makes it an obvious target for therapy, but research work in this area has yet to translate into clinical success. Experimentally in mice, interferon-alpha (IFN-α) has been shown to suppress TGF-β mrna in mesothelioma cells but a significant therapeutic effect only occurred if treatment was commenced very early in the course of the disease, equivalent to mesothelioma in situ [54]. This accords with the poor response to IFN-α reported clinically in established disease [55, 56], even when combined with cytotoxic drug regimes [57-59]. Other immunological approaches to enhance the immune response to mesothelioma have been evaluated, involving either IL-2 or gamma-ifn. Neither systemic IL-2 nor direct intratumor injection of IL-2 (using a recombinant vaccinia virus expressing human IL-2) have been effective [60, 61]. In contrast, intrapleural IL-2 seems well tolerated and a 55% response rate has been reported in patients who were predominantly in stage I or II and predominantly of epithelial type. The median survival of responders and nonresponders was 28 months and 8 months, respectively (p < 0.01) and responders had 58% two-year survival and 41% three-year survival [27]. The same group also evaluated intrapleural gamma-ifn and found it less effective with an overall response rate of only 20%, although in stage I disease, the response rate was 45% [62]. Despite the low clinical response rate, intrapleural gamma-ifn has been shown to decrease intrapleural IL-6 concentrations produced by malignant cells and to cause activation of macrophages and cytotoxic T-lymphocytes [63]. GENE THERAPY Experimental studies in rodents have demonstrated that it is possible to transfer the herpes simplex thymidine kinase (HSVtk) gene to mesothelioma cells using an adenovirus vector, and subsequently treat with the antiviral drug ganciclovir to kill the mesothelioma cells, thereby eliminating tumor nodules [64]. This form of treatment is effective experimentally even when only a small percentage of mesothelioma cells is transduced, suggesting that there is an important bystander effect also [64, 65]. However, currently available viral vectors are less efficient at delivering genes to tumor cells interspersed in a dense, fibrous stroma, as in mesenchymal (sarcomatous) or mixed histology mesotheliomas [66]. Because of this problem and poor penetration of bulky tumor, it is likely that this type of gene therapy will need to be combined with either debulking or radical surgery. Following the experimental work in animals, trials have begun to evaluate gene therapy clinically [66]. A phase I clinical trial of recombinant adenovirus containing HSVtk gene injected intrapleurally followed by systemic treatment with ganciclovir for 14 days has revealed good tolerance of therapy but some side effects. These included fever, anemia, transient liver enzyme elevations and bullous skin eruptions in some patients. Gene transfer was documented in 11 out of 20 patients [67]. Since this initial report, a new adenoviral vector has been developed which appears to be as effective with less toxicity [68]. Phase II trials have yet to be reported. Studies of
9 496 Contemporary Management of Malignant Pleural Mesothelioma gene transfer in malignant pleural effusions have revealed that chondroitin sulphates markedly inhibit gene transfer by interacting with the vector in solution. The authors suggest that drainage of the pleural effusion prior to treatment should allow more efficient gene transfer [69]. Another approach in gene therapy involves restoration of a gene product usually absent in mesothelioma cells. The gene product p16ikn4a can be re-expressed in mesothelioma cells following transfer with an adenovirus. Experimentally this has been shown to inhibit tumor formation, arrest tumor growth and diminish tumor size and spread [70]. Several other chromosomal losses have been identified in mesothelioma, suggesting that some may contain putative tumor suppressor genes [71-73]. The therapeutic possibilities of gene restoration therapy clearly need to be explored also. PHOTODYNAMIC THERAPY Photodynamic therapy involves administration of a tumor-localizing photosensitizing agent followed by activation of the agent by light of a wavelength specific to its absorption spectrum. The most commonly used photosensitizers are porphyrin-related compounds which bind to various cytoplasmic membranes within the cell. Light activation in the presence of molecular oxygen causes oxidative damage at the subcellular level, leading to cell death [74]. Cytotoxicity also occurs as the result of vascular damage, impaired blood supply and local hypoxia [75]. It is thought that a heightened immune response to the tumor may also be induced [76]. Experimental work with nude mice bearing human mesothelioma tumors has shown that mesothelioma is locally sensitive to photodynamic therapy. Various photosensitizing agents and light dosing regimes have been investigated [77-80], together with studies to define the optimum time interval between sensitizer administration and light activation [81]. Currently available technology limits effective light treatment penetration to about 1 cm [82], which means that intrapleural photodynamic therapy must be combined with debulking or radical surgery in most cases. The literature contains several anecdotal reports of small numbers of mesothelioma patients treated with photodynamic therapy in combination with various types of debulking surgery, and there are two reports from one center of a phase II study which yielded results inferior to other published surgical series in the literature [83, 84]. Only one phase III study has been reported [85]. This also showed no benefit for photodynamic therapy in terms of survival or local disease control in patients also treated with a combination of debulking surgery, cisplatin, IFN-α and tamoxifen [85]. Not only has photodynamic therapy proved to be ineffective clinically in trials reported to date, but there is also concern about its damaging effect on normal and healing tissues. Concern has been raised particularly about the risk of bronchopleural [84, 86] and esophagopleural [86-88] fistula, and in one series the combination of pleuropneumonectomy and intracavitary photodynamic therapy was associated with a mortality of 28.6% [84]. A small number of enthusiastic scientists and physicians continue to investigate photodynamic therapy in mesothelioma using newer technology and different photosensitizing agents in combination with various additional treatment modalities. Further trials are awaited with interest. However, on currently available evidence, it seems unlikely that this type of therapy will become part of the standard treatment for mesothelioma in the near future. PALLIATIVE THERAPY In patients whose performance status is poor or whose tumor has reached an advanced stage (III or IV), palliative therapy may have a role in helping to relieve the pain of chest wall involvement or the dyspnea due to recurrent pleural effusion. Radiotherapy has already been mentioned as a means of controlling chest wall pain. Strong opiates will almost certainly be required also, and in patients with intolerable pain, cordotomy may need to be considered. In patients with recurrent pleural effusion, thoracoscopy and instillation of talc can be useful to induce pleural adhesion [89], but only if the underlying lung is not so restricted by tumor on its surface that it will not expand sufficiently to reach the chest wall. If the lung has little or no tumor on its surface, outpatient management may be possible, using a small-bore catheter and a drainage bag in conjunction with sclerotherapy [90]. Pleuroperitoneal shunts are inadvisable as they risk seeding tumor into the peritoneal cavity. If the lung is restricted by tumor and recurrent effusions are troublesome, local treatment with chemotherapy, radiotherapy or immunotherapy may be worthwhile as a means of shrinking tumor on the lung surface sufficiently to allow re-expansion. However the natural history of advanced disease is that eventually the lung becomes fixed in a position midway between full expansion and complete collapse by contiguous tumor and progressive fluid formation ceases. It has been suggested on theoretical grounds that cytokine inhibitors may have a role in palliative therapy by helping to control pain and cytokine-mediated paraneoplastic effects such as cachexia, fever and the thrombophilia associated with thrombocytosis [52]. No clinical studies have been reported. FUTURE PROSPECTS In the past there has been a tendency to think of diffuse malignant pleural mesothelioma as one disease in therapeutic terms, irrespective of histological type and tumor stage. This does not happen with other tumors and is equally illogical and
10 Butchart 497 inappropriate in mesothelioma. As with other tumors, early diagnosis while the disease is still in stage I or even at an in situ stage must be the goal in order to maximize therapeutic options, particularly if immunotherapy or gene therapy is to be used. Patients with pure epithelial mesothelioma have a better prognosis and respond better to trimodality therapy. Stage I patients with epithelial mesothelioma who meet the fitness criteria described above should therefore be offered the option of radical surgery in combination with chemotherapy and radiotherapy. Further research is required to determine the optimum combination of these modalities in terms of timing of adjuvant therapy, individual drugs, use of hyperthermia and route of administration. The place of immunotherapy and gene therapy as adjunctive treatments also remains to be defined. For example, it may be possible to reduce tumor bulk and perhaps downstage the disease with immunotherapy prior to radical surgery, if treatment is started early enough. Gene therapy may have a role either preoperatively or in destroying the microscopic disease that remains after radical surgery. These and other combinations of treatment need to be tested in well-designed clinical trials, probably on a multicenter basis in order to enroll sufficient numbers of patients. Finding means to improve treatment for sarcomatous and mixed histology mesothelioma remains an even greater challenge. At present radical surgery does not seem worthwhile for these patients when combined with currently employed chemotherapy and radiotherapy. However, chemotherapy combinations used for treating other sarcomas need to be evaluated as adjunctive therapy before radical surgery is abandoned altogether as a treatment modality. Much remains to be learned about tumor biology and immunology and specifically why some tumors of apparently identical histology respond better to therapy than others. Ultimately the hope must be that development of tumor markers capable of identifying very early asymptomatic malignant change in patients at risk, coupled with the discovery of the fundamental cause of malignant transformation in mesothelial cells at the genetic level, will lead to gene therapy given early enough to restore normality to these cells. Diffuse malignant mesothelioma of the pleura should not be labeled as incurable until all possible treatment combinations have been properly evaluated in well-designed clinical trials. A collaborative approach involving basic scientists and oncologists, thoracic surgeons and physicians with experience in treating mesothelioma is essential. Because mesothelioma is still a relatively rare tumor despite its increasing frequency, treatment should ideally be concentrated in relatively few supraregional centers in order to maximize expertise, and allow innovative treatment combinations to be implemented with the greatest chance of success. Evaluation of new therapeutic approaches will be achieved more rapidly if these supraregional centers collaborate in multicenter trials. The nihilistic approach of simply waiting until the mesothelioma epidemic eventually begins to decline spontaneously in 20 or 30 years is untenable, in view of the hundreds of thousands of deaths which will result if no effective treatment is found [3]. REFERENCES 1 Elmes PC, Simpson MJC. The clinical aspects of mesothelioma. Q J Med 1976;45: Antman KH. Clinical presentation and natural history of benign and malignant mesothelioma. Semin Oncol 1981;8: Peto J, Decarli A, La Vecchia C et al. The European mesothelioma epidemic. Br J Cancer 1999;79: Klemperer P, Rabin CB. Primary neoplasms of the pleura. A report of 5 cases. Arch Pathol 1931;11: Wagner JC, Sleggs CA, Marchand P. Diffuse pleural mesothelioma and asbestos exposure in the North Western Cape Province. Br J Ind Med 1960;17: Butchart EG, Gibbs AR. Pleural mesothelioma. Curr Opin Oncol 1990;2: Butchart EG. Surgery of mesothelioma of the pleura. In: Roth JA, Ruckdeschel JC, Weisenburger TH, eds. Thoracic Oncology. Philadelphia: WB Saunders, 1989: Wojtukiewicz MZ, Zacharski LR, Memoli VA et al. Absence of components of coagulation and fibrinolysis pathways in situ in mesothelioma. Thromb Res 1989;55: Craighead JE. Current pathogenetic concepts of diffuse malignant mesothelioma. Hum Pathol 1987;18: Kaiser LR. New therapies in the treatment of malignant pleural mesothelioma. Semin Thorac Cardiovasc Surg 1997;9: Pass HI. Contemporary approaches in the investigation and treatment of malignant pleural mesothelioma. Chest Surg Clin N Am 1994;4: Upham JW, Garlepp MJ, Musk AW et al. Malignant mesothelioma: new insights into tumour biology and immunology as a basis for new treatment approaches. Thorax 1995;50: Lewis RJ. Malignant pleural mesothelioma: a nonsurgical problem. In: Kittle CF, ed. Current Controversies in Thoracic Surgery. Philadelphia: WB Saunders, 1986: Butchart EG, Ashcroft T, Barnsley WC et al. Pleuropneumonectomy in the management of diffuse malignant mesothelioma of the pleura. Thorax 1976;31: Curran D, Sahmoud T, Therasse P et al. Prognostic factors in patients with pleural mesothelioma: the European Organisation
11 498 Contemporary Management of Malignant Pleural Mesothelioma for Research and Treatment of Cancer experience. J Clin Oncol 1998;16: Rusch VW, Venkatraman E. The importance of surgical staging in the treatment of malignant pleural mesothelioma. J Thorac Cardiovasc Surg 1996;111: Sugarbaker DJ, Flores RM, Jaklitsch MT et al. Resection margins, extrapleural nodal status and cell type determine postoperative long-term survival in trimodality therapy of malignant pleural mesothelioma: results in 183 patients. J Thorac Cardiovasc Surg 1999;117: International Mesothelioma Interest Group. A proposed new international TNM staging system for malignant pleural mesothelioma. Chest 1995;108: Pass HI, Temeck BK, Kranda K et al. Preoperative tumor volume is associated with outcome in malignant pleural mesothelioma. J Thorac Cardiovasc Surg 1998;115: Patz EF, Shaffer K, Piwnica-Worms DR et al. Malignant pleural mesothelioma: value of CT and MR imaging in predicting resectability. Am J Radiol 1992;159: Conlon KC, Rusch VW, Gillern S. Laparoscopy: an important tool in the staging of malignant pleural mesothelioma. Ann Surg Oncol 1996;3: Gilron J, Richardi G, Fajadet P et al. New imaging modalities of mesothelioma (CT versus MRI). Eur Respir J 1994;7(suppl 18):131s. 23 Knuuttila A, Halme M, Kivisaari L et al. The clinical importance of magnetic resonance imaging versus computed tomography in malignant pleural mesothelioma. Lung Cancer 1998;22: Boraschi P, Neri S, Braccini G et al. Magnetic resonance appearance of asbestos-related benign and malignant pleural diseases. Scand J Work Environ Health 1999;25: Sugarbaker DJ. Extrapleural pneumonectomy is the procedure of choice for early stage malignant mesothelioma. American Association for Thoracic Surgery, 79th annual meeting, April Sugarbaker DJ, Garcia JP, Richards WG et al. Extrapleural pneumonectomy in the multimodality therapy of malignant pleural pleural mesothelioma. Ann Surg 1996;224: Astiyk O, Picat-Joossen D, Viallat JR et al. Intrapleural administration of interleukin-2 for the treatment of patients with malignant pleural mesothelioma: a Phase II study. Cancer 1998;83: Hilaris BS, Nori D, Kwong E et al. Pleurectomy and intraoperative brachytherapy and postoperative radiation in the treatment of malignant pleural mesothelioma. Int J Radiat Oncol Biol Phys 1984;10: Rusch VW. Pleurectomy/decortication in the setting of multimodality treatment for diffuse malignant pleural mesothelioma. Semin Thorac Cardiovasc Surg 1997;9: Ball DL, Cruickshank DG. The treatment of malignant mesothelioma of the pleura: review of a 5-year experience with special reference to radiotherapy. Am J Clin Oncol 1990;13: Häkkinen AM, Laasonen A, Linnainmaa K et al. Radiosensitivity of mesothelioma cell lines. Acta Oncol 1996;35: Kutcher GJ, Kestler C, Greenblatt D et al. Technique for external beam treatment for mesothelioma. Int J Radiat Oncol Biol Phys 1987;13: Holsti LR, Pyrhonen S, Kajanti M et al. Altered fractionation of hemithorax irradiation for pleural mesothelioma and failure patterns after treatment. Acta Oncol 1997;36: Mauceri HJ, Hanna NN, Beckett MA et al. Combined effects of angiostatin and ionising radiation in antitumour therapy. Nature 1998;394: De Graaf-Strukowska L, van der Zee J, van Putten W et al. Factors influencing the outcome of radiotherapy in malignant mesothelioma of the pleura a single-institution experience with 189 patients. Int J Radiat Oncol Biol Phys 1999;43: Davis SR, Tan L, Ball DL. Radiotherapy in the treatment of malignant mesothelioma of the pleura, with special reference to its use in palliation. Australas Radiol 1994;38: Bissett D, Macbeth FR, Cram I. The role of palliative radiotherapy in malignant mesothelioma. Clin Oncol 1991;3: Low EM, Khoury GG, Matthews AW et al. Prevention of tumour seeding following thoracoscopy in mesothelioma by prophylactic radiotherapy. Clin Oncol 1995;7: Boutin C, Rey F, Viallat JR. Prevention of malignant seeding after invasive diagnostic procedures in patients with pleural mesothelioma. A randomized trial of local radiotherapy. Chest 1995;108: Ryan CW, Herndon J, Vogelzang NJ. A review of chemotherapy trials for malignant mesothelioma. Chest 1998;113:66S-73S. 41 Hunt KJ, Longton G, Williams MA et al. Treatment of malignant mesothelioma with methotrexate and vinblastine, with or without platinum chemotherapy. Chest 1996;109: Hoffman KR. Paclitaxel and carboplatin combination chemotherapy is an effective palliative treatment for malignant mesothelioma. Proc Annu Meet Am Soc Clin Oncol 1996;15:A Chahinian AP, Mandeli JP, Gluck H et al. Effectiveness of cisplatin, paclitaxel, and suramin against human malignant mesothelioma xenografts in athymic nude mice. J Surg Oncol 1998;67: Emri S, Koc Y, O Brien MC et al. Taxol and arginine butyrate exert additive antiproliferative effects on human mesothelioma cells. Proc Annu Meet Am Soc Clin Oncol 1994;13:A Herscher LL, Hahn SM, Kroog G et al. Phase I study of paclitaxel as a radiation sensitizer in the treatment of mesothelioma and non-small-cell lung cancer. J Clin Oncol 1998;16: Galen P. Hyperthermia and chemotherapy. Adv Exp Med Biol 1990;267: Miller RC, Richards M, Baird C et al. Interaction of hyperthermia and chemotherapy agents; cell lethality and oncogenic potential. Int J Hyperthermia 1994;10:89-99.
12 Butchart Storm FK. Clinical hyperthermia and chemotherapy. Radiol Clin North Am 1989;27: Ratto GB, Civalleri D, Esposito M et al. Pleural space perfusion with cisplatin in the multimodality treatment of malignant mesothelioma. J Thorac Cardiovasc Surg 1999;117: Ma GY, Bartlett DL, Reed E et al. Continuous hyperthermic peritoneal perfusion with cisplatin for the treatment of peritoneal mesothelioma. Cancer J Sci Am 1997;3: Leigh RA, Webster I. Lymphocytic infiltration of pleural mesothelioma and its significance for survival. S Afr Med J 1982;61: Bielefeldt-Ohmann H, Jarick AG, Fitzpatrick DR. Molecular pathobiology and immunology of malignant mesothelioma. J Pathol 1996;178: Donington JS, Mew DJ, Pass HI. Malignant pleural mesothelioma: newer aspects of carcinogenesis, molecular genetics, and prospects for future therapies. Surg Oncol 1995;4: Bielefeldt-Ohmann H, Fitzpatrick DR, Marzo AL et al. The potential for interferon-alpha therapy in mesothelioma. J Interferon Cytokine Res 1995;5: Ardizzoni A, Pennucci MC, Castagneto B et al. Recombinant interferon alpha-2b in the treatment of diffuse malignant pleural mesothelioma. Am J Clin Oncol 1994;17: Christmas TI, Manning LS, Garlepp MJ et al. Effect of interferon-alpha 2a on malignant mesothelioma. J Interferon Res 1993;13: Tansan S, Emri S, Selcuk T et al. Treatment of malignant pleural mesothelioma with cisplatin, mitomycin C and alpha interferon. Oncology 1994;51: Purohit A, Moreau L, Dietemann A et al. Weekly systemic combination of cisplatin and interferon alpha 2a in diffuse malignant pleural mesothelioma. Lung Cancer 1998;22: O Reilly EM, Ilson DH, Saltz LB et al. A phase II trial of interferon-alpha 2a and carboplatin in malignant mesothelioma. Cancer Invest 1999;17: Nano R, Capelli E, Civallero M et al. Effects of interleukin-2 for the treatment of malignant mesothelioma. Oncol Rep 1998;5: Robinson BW, Mukherjee SA, Davidson A et al. Cytokine gene therapy or infusion as treatment for solid human cancer. J Immunother 1998;21: Boutin C, Nussbaum E, Monnet I et al. Intrapleural treatment with recombinant gamma-interferon in early stage malignant pleural mesothelioma. Cancer 1994;74: Monti G, Jaurant MC, Monnet I et al. Intrapleural production of interleukin 6 during mesothelioma and its modulation by gamma-interferon treatment. Cancer Res 1994;54: Smythe WR, Hwang HC, Elshami AA et al. Treatment of experimental human mesothelioma using adenovirus transfer of the herpes simplex thymidine kinase gene. Ann Surg 1995;222: Escandi MC, van Someren GD, Vincent AJ et al. Gene therapy of experimental malignant mesothelioma using adenovirus vectors encoding the HSVtk gene. Gene Ther 1997;4: Sterman DH, Kaiser LR, Albelda SM. Gene therapy for malignant pleural mesothelioma. Hematol Oncol Clin North Am 1998;12: Sterman DH, Treat J, Litzky LA et al. Adenovirus-mediated herpes simplex virus thymidine kinase/ganciclovir gene therapy in patients with localized malignancy: results of a phase I clinical trial in malignant mesothelioma. Hum Gene Ther 1998;9: Lanuti M, Gao GP, Force SD et al. Evaluation of an E1E4- deleted adenovirus expressing the herpes simplex thymidine kinase suicide gene in cancer gene therapy. Hum Gene Ther 1999;10: Batra RK, Olsen JC, Hoganson DK et al. Retroviral gene transfer is inhibited by chondroitin sulfate proteoglycans/glycosaminoglycans in malignant pleural effusions. J Biol Chem 1997;272: Frizelle SP, Grim J, Zhou J et al. Re-expression of p16ink4a in mesothelioma cells results in cell cycle arrest, cell death, tumor suppression and tumor regression. Oncogene 1998;16: Balsara BR, Bell DW, Sonoda G et al. Comparative genomic hybridization and loss of heterozygosity analyses identify a common region of deletion at 15q in human malignant mesothelioma. Cancer Res 1999;59: Shivapurkar N, Virmani AK, Wistuba II et al. Deletions of chromosome 4 at multiple sites are frequent in malignant mesothelioma and small cell lung carcinoma. Clin Cancer Res 1999;5: Lee WC, Testa JR. Somatic genetic alterations in human malignant mesothelioma. Int J Oncol 1999;14: Oleinick NL, Evans HH. The photobiology of photodynamic therapy: cellular targets and mechanisms. Radiat Res 1998;150:146S-156S. 75 Fingar VH. Vascular effects of photodynamic therapy. J Clin Laser Med Surg 1996;14: Korbelik M. Induction of tumor immunity by photodynamic therapy. J Clin Laser Med Surg 1996;14: Feins RH, Hilf R, Ross H et al. Photodynamic therapy for human malignant mesothelioma in the nude mouse. J Surg Res 1990;49: Foster TH, Gibson SL, Raubertas RF. Response of Photofrinsensitised mesothelioma xenografts to photodynamic therapy with 514 nm light. Br J Cancer 1996;73: Ris HB, Giger A, Hof VI et al. Experimental assessment of photodynamic therapy with chlorins for malignant mesothelioma. Eur J Cardiothorac Surg 1997;12: Ris HB, Altermatt HJ, Stewart CM et al. Photodynamic therapy with m-tetrahydroxyphenylchlorin in vivo: optimization of the therapeutic index. Int J Cancer 1993;55: Ris HB, Altermatt HJ, Nachbur B et al. Effect of drug-light interval on photodynamic therapy with metatetrahydroxyphenylchlorin in malignant mesothelioma. Int J Cancer 1993;53:
13 500 Contemporary Management of Malignant Pleural Mesothelioma 82 Stewart F, Baas P, Star W. What does photodynamic therapy have to offer radiation oncologists (or their cancer patients)? Radiother Oncol 1998;48: Takita H, Mang TS, Loewen GM et al. Operation and intracavitary photodynamic therapy for malignant pleural mesothelioma: a phase II study. Ann Thorac Surg 1994;58: Moskal TL, Dougherty TJ, Urschel JD et al. Operation and photodynamic therapy for pleural mesothelioma: 6-year follow-up. Ann Thorac Surg 1998;66: Pass HI, Temeck BK, Kranda K et al. Phase III randomized trial of surgery with or without intraoperative photodynamic therapy and postoperative immunochemotherapy for malignant pleural mesothelioma. Ann Surg Oncol 1997;4: Pass HI, Delaney TF, Tochner Z et al. Intrapleural photodynamic therapy: results of a phase I trial. Ann Surg Oncol 1994;1: Leketich JD, Westkaemper J, Sommers KE et al. Bronchoesophagopleural fistula after photodynamic therapy for malignant mesothelioma. Ann Thorac Surg 1996;62: Temeck BK, Pass HI. Esophagopleural fistula: a complication of photodynamic therapy. South Med J 1995;88: Canto A, Guijarro R, Arnau A et al. Videothoracoscopy in the diagnosis and treatment of malignant pleural mesothelioma with associated pleural effusions. Thorac Cardiovasc Surg 1997;45: Patz EF. Malignant pleural effusions: recent advances and ambulatory sclerotherapy. Chest 1998;113:74S-77S.
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Malignant Mesothelioma Current Approaches to a Difficult Problem. Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Treatment of mesothelioma in Bloemfontein, South Africa
 European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
European Journal of Cardio-thoracic Surgery 24 (2003) 434 440 www.elsevier.com/locate/ejcts Treatment of mesothelioma in Bloemfontein, South Africa W.J. de Vries*, M.A. Long Cardiothoracic Department,
Malignant Mesothelioma
 Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Mesothelioma
 Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Recommendations for the Reporting of Pleural Mesothelioma
 Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Ahmed Farouk Abd El-Hafez, MD
 Presented By Ahmed Farouk Abd El-Hafez, MD Lecturer of Cardiothoracic Surgery Assiut University Asbestos exposure : amphibole fibers especially crocidolite asbestos Nonasbestos Causes : Silicate fibers
Presented By Ahmed Farouk Abd El-Hafez, MD Lecturer of Cardiothoracic Surgery Assiut University Asbestos exposure : amphibole fibers especially crocidolite asbestos Nonasbestos Causes : Silicate fibers
The Proposed New International TNM Staging System for Malignant Pleural Mesothelioma: Application to Imaging
 323.....:. #{149} :. #{149}..: #{149}. #{149}. :- : Received June 22, 1995; accepted after revision September 12, 1995. 1 Department of Radiology, Duke University Medical Center, Box 3808, Dunham, NC 2771
323.....:. #{149} :. #{149}..: #{149}. #{149}. :- : Received June 22, 1995; accepted after revision September 12, 1995. 1 Department of Radiology, Duke University Medical Center, Box 3808, Dunham, NC 2771
Sternotomy and removal of the tumor
 Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
Malignant pleural mesothelioma: outcome of limited surgical management
 Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Mesothelioma: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Post-operative intrapleural chemotherapy for mesothelioma
 Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE MESOTHELIOMA Lung Site Group Mesothelioma Date Guideline Created: April 2013 Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1.
MesoPDT. Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI. Image Assisted Laser Therapy for Oncology
 MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma
 Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma Based on AJCC/UICC TNM, 7th edition Protocol web posting date: February 1, 2011 Procedures Resection Authors
Protocol for the Examination of Specimens From Patients With Malignant Pleural Mesothelioma Based on AJCC/UICC TNM, 7th edition Protocol web posting date: February 1, 2011 Procedures Resection Authors
Principal Investigator: Valerie W. Rusch, MD, FACS, Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
People Living with Cancer
 Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Summary of treatment benefits
 Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
Risk Management Plan PEMETREXED Powder for concentrate for Solution for infusion Pemetrexed is also indicated as monotherapy for the maintenance treatment of locally advanced or metastatic non small cell
PRODYNOV. Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI. Image Assisted Laser Therapy for Oncology
 PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Surgery. Wedge resection only part of the lung, not. not a lobe, is removed. Cancer Council NSW
 The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
Smoking and misuse of certain pain medicines can affect the risk of developing renal cell cancer.
 Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
What is Mesothelioma?
 What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
Treatment of Mesothelioma with Radiotherapy
 41 Treatment of Mesothelioma with Radiotherapy Ryan P. Smith and Stephen M. Hahn General Principles of Radiation Therapy Radiation therapy is a therapeutic modality that uses ionizing radiation to treat
41 Treatment of Mesothelioma with Radiotherapy Ryan P. Smith and Stephen M. Hahn General Principles of Radiation Therapy Radiation therapy is a therapeutic modality that uses ionizing radiation to treat
MESOTHELIOMA. Not Just a Late Night Commercial. Graciela Hoal, RN, MSN, ACNP-BC
 MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma
 Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Round Table with Drs. Anne Tsao and Alex Farivar, Case 2: Mesothelioma I d like to welcome everyone, thanks for coming out to our lunch with experts. The faculty today are great people in the thoracic
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases
 Original Article Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases William G. Richards, PhD 1,2 ; John J. Godleski, MD 2,3 ; Beow Y.
Original Article Proposed Adjustments to Pathologic Staging of Epithelial Malignant Pleural Mesothelioma Based on Analysis of 354 Cases William G. Richards, PhD 1,2 ; John J. Godleski, MD 2,3 ; Beow Y.
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT
 1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy and Photodynamic Therapy
 CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.1.36 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:36-40 A Case of Advanced Malignant Pleural Mesothelioma Treatment with Chemotherapy
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
Screening, early referral and treatment for asbestos related cancer
 Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Diseases. Inflammations Non-inflammatory pleural effusions Pneumothorax Tumours
 Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
A succesfull case of HIPEC in a peritoneal mesothelioma patient
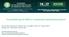 A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
Treatment of Malignant Pleural Mesothelioma: Is There a Benefit to Pleuropneumonectomy?
 55 Treatment of Malignant Pleural Mesothelioma: Is There a Benefit to Pleuropneumonectomy? Stacey Su, Michael T. Jaklitsch, and David J. Sugarbaker Malignant pleural mesothelioma (MPM) is a rare but highly
55 Treatment of Malignant Pleural Mesothelioma: Is There a Benefit to Pleuropneumonectomy? Stacey Su, Michael T. Jaklitsch, and David J. Sugarbaker Malignant pleural mesothelioma (MPM) is a rare but highly
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
How To Understand How Cancer Works
 Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Malignant Mesothelioma: an Update
 Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
How To Treat A Cancer With A Radical
 Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
The TV Series. www.healthybodyhealthymind.com INFORMATION TELEVISION NETWORK
 The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
Therapy of pleural effusions Modern techniques
 Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE
 Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Malignant Mesothelioma
 Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Columbia University Mesothelioma Applied Research Foundation - 2009 - www.curemeso.org. Mesothelioma Center www.mesocenter.org
 Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
General Rules SEER Summary Stage 2000. Objectives. What is Staging? 5/8/2014
 General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
Brain Cancer. This reference summary will help you understand how brain tumors are diagnosed and what options are available to treat them.
 Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline
 Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Evidence-based Series #7-14-2: Section 1 Surgical Management of Malignant Pleural Mesothelioma: A Clinical Practice Guideline D.E. Maziak, A. Gagliardi, A.E. Haynes, J.A. Mackay, W.K. Evans, and members
Surgical therapy of. who should be operated
 SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
SAMO Interdisciplinary Workshop on Chest Tumors Lucerne, 13th and 14th January 2012 Surgical therapy of mesothelioma, who should be operated Walter Weder MD Professor of Surgery University Hospital Zurich
B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC
 Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3
 ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
Malignant Mesothelioma
 Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
Malignant Mesothelioma What is malignant mesothelioma? Malignant mesothelioma is a cancer that starts in cells in the linings of certain parts of the body, especially in the linings of the chest or abdomen.
Malignant pleural mesothelioma P/D vs. EPP
 3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
Medullary Renal Cell Carcinoma Case Report
 Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
Bahrain Medical Bulletin, Vol. 27, No. 4, December 2005 Medullary Renal Cell Carcinoma Case Report Mohammed Abdulla Al-Tantawi MBBCH, CABS* Abdul Amir Issa MBBCH, CABS*** Mohammed Abdulla MBBCH, CABS**
Thoracoscopy in Pleural Malignant Mesothelioma
 Diagnostic and Therapeutic Endoscopy, 1997, Vol. 3, pp. 147-151 Reprints available directly from the publisher Photocopying permitted by license only (C) 1997 OPA (Overseas Publishers Association) Amsterdam
Diagnostic and Therapeutic Endoscopy, 1997, Vol. 3, pp. 147-151 Reprints available directly from the publisher Photocopying permitted by license only (C) 1997 OPA (Overseas Publishers Association) Amsterdam
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Brigham and Women s Hospital, Boston, MA, USA; 2 Verastem, Inc., Boston, MA, USA
 Determination of Biomarker Response in a Phase II Window of Opportunity Study of Defactinib (VS 6063), a Focal Adhesion Kinase (FAK) Inhibitor, in Patients with Resectable Malignant Pleural Mesothelioma
Determination of Biomarker Response in a Phase II Window of Opportunity Study of Defactinib (VS 6063), a Focal Adhesion Kinase (FAK) Inhibitor, in Patients with Resectable Malignant Pleural Mesothelioma
Photodynamic Therapy for Malignant Pleural Mesothelioma
 S-75 Photodynamic Therapy for Malignant Pleural Mesothelioma Presented by Joseph S. Friedberg, MD, University of Pennsylvania Health System, Philadelphia, Pennsylvania Abstract Surgery is the treatment
S-75 Photodynamic Therapy for Malignant Pleural Mesothelioma Presented by Joseph S. Friedberg, MD, University of Pennsylvania Health System, Philadelphia, Pennsylvania Abstract Surgery is the treatment
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
1 page Overview. CONCURRENT 1D, 1E, 1F Biology & Pathogenesis Multi-Modality Immunology 1
 1 page Overview 21 Oct Tuesday 1500 on REGISTRATION 1800 Welcome Reception & Cocktails at the Cape Town International Conference Centre (CTICC) 22 Oct Wednesday 0730 REGISTRATION 0830 OPENING 0900 PLENARY
1 page Overview 21 Oct Tuesday 1500 on REGISTRATION 1800 Welcome Reception & Cocktails at the Cape Town International Conference Centre (CTICC) 22 Oct Wednesday 0730 REGISTRATION 0830 OPENING 0900 PLENARY
How To Treat A Uterine Sarcoma
 EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition 2001 Uterus: Uterine Sarcomas Jeffrey L. Stern, MD Uterine sarcomas
EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition 2001 Uterus: Uterine Sarcomas Jeffrey L. Stern, MD Uterine sarcomas
Diagnosis and Prognosis of Pancreatic Cancer
 Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Understanding Your Surgical Options for Lung Cancer
 Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
Information Booklet for Patients Understanding Your Surgical Options for Lung Cancer Understanding Lung Cancer If you have just been diagnosed with lung cancer, this booklet will serve as an informational
Pre-workshop exercise
 Setting research priorities for mesothelioma workshop 10 th November 2014 Pre-workshop exercise Your individual ranking of unanswered questions about the diagnosis, treatment and care of mesothelioma Please
Setting research priorities for mesothelioma workshop 10 th November 2014 Pre-workshop exercise Your individual ranking of unanswered questions about the diagnosis, treatment and care of mesothelioma Please
Lung Cancer Treatment
 Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Plueral Malignancy: Radiologic-pathologic
 Plueral Malignancy: Radiologic-pathologic Correlation Ritu R. Gill, MD Pleural Malignancies: Radiologic-Pathologic Correlation Ritu R Gill MD Brigham and Women s Hospital Boston, Massachusetts Pleural
Plueral Malignancy: Radiologic-pathologic Correlation Ritu R. Gill, MD Pleural Malignancies: Radiologic-Pathologic Correlation Ritu R Gill MD Brigham and Women s Hospital Boston, Massachusetts Pleural
