Thoracoscopy in Pleural Malignant Mesothelioma
|
|
|
- Austen Walton
- 10 years ago
- Views:
Transcription
1 Diagnostic and Therapeutic Endoscopy, 1997, Vol. 3, pp Reprints available directly from the publisher Photocopying permitted by license only (C) 1997 OPA (Overseas Publishers Association) Amsterdam B.V. Published in The Netherlands by Harwood Academic Publishers Printed in Singapore Thoracoscopy in Pleural Malignant Mesothelioma Diagnosis G. F. TASSI, G. P. MARCHETTI, F. FATTIBENE and P. L. CHIODERA* Division ofpneumology and *Service ofpathologic Anatomy, Valle Camonica Hospital, 25040, Esine (Brescia), Italy (Received 6 June 1996; revised 9 July 1996; in finalform 7 August 1996) On the basis of our personal experience in 70 cases (66 pleural effusions) observed during the period January January 1996 we are here illustrating and discussing the diagnostic role of thoracoscopy in malignant pleural mesothelioma. A histological diagnosis was achieved in 94.2% of cases. The endoscopic appearance was clearly neoplastic (masses, nodules) in 53 patients (75.7%) and simply inflammatory in 17 pachypleuritis in 13 (18.6%) and of diffuse hyperemia in 3 (5.7%). In all cases fluid cytology (diagnostic yield: 18.5%) and needle biopsy (diagnostic yield 17.1%) were performed. The extension of pleural involvement (endoscopic staging according to Boutin) was also determined. In 16 patients (22.8%) a parietal and diaphragmatic involvement (stage la) was found. In 40 patients (57.2%) an associated visceral invasion (stage Ib). In 14 cases (20%) a diffuse parietal, visceral and mediastinal extension (stage II). The exam has always been well tolerated with few immediate complications: subcutaneous emphysema (4 cases) and some negligeable parietal bleeding (2 cases). Keywords: pleural mesothelioma, diagnosis, thoracoscopy, pleural effusion INTRODUCTION There are still considerable difficulties in the diagnosis of pleural mesothelioma, both because of its aspecific clinical manifestations and because of the limited sensitivity of traditional X-rays and of computed axial tomography. Fluid cytology and needle biopsy have only partially improved chances of identifying the pathology (Whitaker and Shikin 1984; Leong et al. 1992). Thoracoscopy however, which has become a much more widely used method in recent years, in expert hands allows a correct diagnosis to be made in nearly all cases, thereby equalling the accuracy previously produced only by thoracot- Address of the corresponding author: Gianfranco Tassi MD, Divisione di Pneumologia, Ospedale di Valle Camonica, Esine (Brescia), Italy. 147
2 148 G.F. TASSI et al. omy (Boutin and Rey 1993). The procedure not only allows adequate and abundant tissue sampling for immunohistochemical staining which is essential for differential diagnosis from adenocarcinoma (Leong and Vernon-Roberts 1994) but also allows staging of the disease which is a useful prognostic factor and an important element in deciding therapy (Boutin et al. 1993). This report aims at illustrating and discussing the diagnostic role of thoracoscopy in mesothelioma on the basis of our experience in 70 cases. MATERIALS AND METHODS 70 cases of pleural malignant mesothelioma were diagnosed at thoracoscopy first in the Pneumology Division of the Spedali Civili in Brescia ( ) and then in the Pneumology Division of the Ospedale di Valle Camonica ( ) (Table I), between January 1984 and January During this period for diagnostic purposes in pleural disease of unknown etiologyb we carried out a total of 470 thoracoscopies so the disease was diagnosed in 14.9% of the diagnostic examinations. 49 of the patients were male (70%) and 21 were female (30%) with a M/F ratio of 2.3/1. Indications for thoracoscopy were pleural effusion in 66 patients (94.2%), while the existence of pleural thickening without exudation was the only anomaly found in 4 (5.8%). The right side was affected in 36 cases (51.4%), the left in 34 (48.6%), there were no bilateral cases. The average age was 61 years (min 41 yrs, max 84 yrs). Anamnesis for occupational exposure to asbes- TABLE Thoracoscopy in Pleural Mesothelioma Patients (n) 70 Patients aged < 60 a. (n) 28 Average age (yrs) 61.4 Pleural effusion (n) 66 Personal experience ( ) (M49; F21) (40%) (94.2%) tos was definitely positive in only 17 (24.2%) cases and negative or not clear in the remaining 53. All patients underwent pleural fluid cytology and closed pleural biopsy by Cope needle. The day before thoracoscopy, any pleural fluid present was aspirated and pneumothorax was then induced using a Morelli device; intrapleural pressures were determined which together with radioscopic control checked the degree of parenchymal collapse, according to our usual technique (Tassi and Marchetti 1993). The average amount of air insuttlated was ml, which gave a space of at least 5 cm between the lung and the chest wall. The actual thoracoscopy was always performed under local anesthesia (10-15 ml idocaine 2%), inserting Boutin s rigid thoracoscope (Wolf Co., Knittlingen, Germany) connected to a video camera for monitor viewing into the 5th -6th intercostal space on the midaxillary line using a single port. A second point of entry was necessary only in 4 cases in order to reach areas otherwise inaccessible. The entire pleural area was always explored and multiple biopsy samples (5-10) were taken both in any suspicious areas and in sites apparently without macroscopically evident lesions. In 3 patients with apparently normal visceral pleura and coexistent fibrohyaline parietal plaques, pleural biopsies were integrated with samples from the lung parenchyma using a coagulating forceps. At the end of the endoscopy, when indicated, poudrage was performed using an asbestos-free talc to induce symphysis (2.5-5 g): 29 patients were so treated. In all cases a chest tube for drainage (24-28 Fr) was inserted and left in place for an average of 3 days (min. a few hours, max 7 days). Since 1992, 39 patients have undergone local preventive radiotherapy days after the examination, with a total dose of 21 Gy over 3 days to a depth of 3 cm over an area between 50 and 100 cm 2 centered over each point of entry (Boutin et al. 1995).
3 THORACOSCOPY IN PLEURAL MALIGNANT MESOTHELIOMA DIAGNOSIS 149 RESULTS Exploration of the pleural cavity was straight forward in 59 patients (84-2%) since in these cases there were no adhesions, whereas in 11 patients (15.8%) complete exploration was made difficult; by the presence of adhesions which, even after lysis with forceps, sometimes partly hindered the procedure. However even in these cases the biopsies taken usually allowed a correct diagnosis to be made. Most of the lesions observed (Table II) were clearly neoplastic (Fig. 1): isolated nodules or multiple lesions (vegetations; masses; thickenings). Diffuse pachypleuritis was found less frequently (Fig. 2) and simple inflammation (Fig. 3) only rarely. Moreover the presence of fibrohyaline plaques with the characteristics of asbestotic plaques was noted in 13 patients (18.6%). Biopsy allowed the diagnosis of pleural malignant mesothelioma in 66 patients (94.2%) and also provided its histological classification (Table III) with a marked prevalence of epithelial type. In 2 cases in which biopsies were insufficient due to extensive adhesions which prevented a complete exploration of the cavity diagnosis was made after thoracotomy. In another 2 cases diagnosis was reached with a second thoracoscopy performed some months later due to the reappearance of the effusion. In all 3 patients submitted to forceps parenchymal biopsy we obtained a diagnosis of pulmonary asbestosis without complications using a coagulating forceps which insured the aerostasis of the lung therefore avoiding air leak. Inflammation Nodules Pachypleuritis Multiple lesions TABLE II Pleural Mesothelioma (n 70) Endoscopic pictures % 4(5.7) 17 (24.3) 13(18.6) 36 (51.4) FIGURE FIGURE 2 Thoracoscopy also allowed Boutin classification of the disease according to the degree of pleural involvement: in 16 cases (21.8%) only the parietal and diaphragmatic pleura were involved (stage Ia), 40 (57.2%) presented visceral invasion (stage Ib), and 14 (20%) massive invasion of all the pleural surfaces (stage II). Talc poudrage made in 29 cases achieved a permanent pleurodesis with no recurrence of effusion in 24 patients (83%). Thoracoscopy was always well tolerated and there were no major complications immediately after the procedure. Minor complications included subcutaneous emphysema in 4 patients (5.7%) and minor parietal bleeding in 2 (2.8%). Later complications included 3 (4.3%) cases of
4 150 G.F. TASSI et al. TABLE IV Pleural Mesothelioma (n 70) Diagnostic means % Fluid cytology 13/70 (18.5) Pleural needle biopsy 12/70 (17.1 Thoracoscopic biopsy 66/70 (94.2) FIGURE 3 TABLE III Pleural Mesothelioma (n 70) Histological type % Epithelial 55 (78.6) Sarcomatous 5 (7.1) Mixed cell 7 (10) Other 3 (4.3) neoplastic invasion of the thoracic scar, all of them in the first 31 patients not treated by local radiotherapy. This no longer occurred in the remaing 39 who had a radiation therapy. DISCUSSION In recent years thoracoscopy has been enjoying a second youth and has become an invaluable method in the diagnosis of pleural effusions in general and mesothelioma in particular. In expert hands the examination is diagnostic in the vast majority of cases, reducing the need for exploratory thoracotomy which has higher morbidity and mortality (Weatherford et al. 1995). If we compare data regarding the sensitivity of the methods used before thoracoscopy the clear advantage of the latter is striking. Our experience (Table IV), similar in results to other large case studies, shows that mesothelioma can be diagnosed by thoracoscopy in 94% of cases: much higher than the 17/18% diagnostic yield of needle biopsy and fluid cytology. Even thoracoscopy does not however reach 100% sensitivity. The small percentage of false negatives present in all the studies is usually due to the presence of adhesions which cannot be divided endoscopically and which therefore prevent a complete exploration or the pleural cavity. It should be noted that this is usually the case when thoracoscopy is delayed too long and often eventually performed several months after the appearance of an effusion. It can therefore be supposed, and our experience confirms this, that a prompt use of the method in the investigation of pleurisies which have not been diagnosed with other means can further increase sensitivity. Clearly neoplastic lesions (vegetations; nodules; multiple lesions) were present in 75.7% of our cases showing that a generic diagnosis of malignancy at endoscopy is possible in most patients. However there can be more deceptive pictures of simple inflammation or of generic pachypleuritis (1/4 of our patients) and these cases emphasize the need for multiple biopsies from a wide range of sites. Asbestotic type fibrohyaline plaques (an irregular surface with a candle wax drop appearance), which we observed in 13 (18.6%) of our 70 patients are also useful for diagnosis: these plaques found together with clearly neoplastic lesions (nodules or masses) (Fig. 4) clearly point to a diagnosis of mesothelioma. In fact during our experience in neoplastic pleurisy in 400 thoracoscopies we have never found these plaques associated with other tumors. Another useful point to remember is that when fibrohyaline
5 THORACOSCOPY IN PLEURAL MALIGNANT MESOTHELIOMA DIAGNOSIS 151 FIGURE 4 plaques are found but occupational exposure has not been proved, lung biopsy with coagulating forceps can be performed during the same thoracoscopy session and under local anesthesia, thereby demonstrating an eventual asbestosis. We, like other authors (Rusch 1995), used thoracoscopic staging for therapeutic approach. In fact only fairly recently has it been discovered that mesothelioma which has invaded the visceral pleura after primitive involvement of the parietal and diaphragmatic pleura has a much worse prognosis and that in its early stages the disease may respond to an efficacious treatment (Astoul et al. 1993, Boutin et al. 1994). Therefore, latterly, 3 stage Ia patients were treated surgically with pleurectomy and 6 with intracavitary drugs (immunotherapy with gamma-interferon and chemotherapy with cisplatin) after the positioning of a device for intrapleural infusion. The number of patients treated is too small to be able to draw conclusions but we consider the clinical results of this approach to be encouraging. Obviously this treatment was possible only after thoracoscopy, once again underlining its usefulness in the modern clinical/ therapeutical management of pleural tumor. In the case of more extensive involvement (stages Ib and II) in patients with massive and recurrent effusions we performed talc poudrage which is still generally considered as the best technique of pleurodesis (Walker-Renard et al. 1994). Its complete efficacy in 83% of the cases avoided the need for painful thoracentesis which also exposes patients to the risk of neoplastic seeding. Tolerance to the examination was very good, and there were no fatalities which further proves that thoracoscopy, if correctly performed, presents no particular risks or complications. We can therefore conclude that the role of thoracoscopy in mesothelioma nowadays is undeniably fundamental, both for diagnostic and therapeutic purposes, and it should be systematically utilized in all suspicious cases. References Whitaker, D., Shilkin, K. B.: Diagnosis of pleural mesothelioma in life: a practical approach. J. Pathol., 1984; 143: [2] Leong, A. S. Y., Stevens, C. T., Mukherjee, T. M.: Malignant mesothelioma: cytologic diagnosis with histologic, immunohistochemical and ultrastructural correlation. Semin. Diag. Pathol., 1992; 9: [3] Boutin, C., Rey, F.: Thoracoscopy in pleural malignant mesothelioma: a prospective study of 188 consecutive patients. Part 1: Diagnosis. Cancer, 1993; 72: [4] Leong, A. S.Y., Vernon-Roberts, E.: The immunohistochemistry of malignant mesothelioma. In: Rosen P. P. and Fechner R. E. (eds.): Pathology Annual Part 2. Appleton & Lange, Norwalk, [5] Boutin, C., Rey, F., Gouvemet, J. et al.: Thoracoscopy in pleural malignant mesothelioma: a prospective study of 188 consecutive patients. Part 2: Prognosis and staging. Cancer, 1993; 72: [6] Tassi, G. F., Marchetti, G. P.: Toracoscopia. Acram, Milano, [7] Boutin, C., Rey, F., Viallat, J. R.: Prevention of malignant seeding after invasive diagnostic procedure in patients with pleural mesothelioma, a randomized trial of local radiotherapy. Chest, 1995; 108: [8] Weatherford, D. A., Stephenson, J. E., Taylor, S. M. et al.: Thoracoscopy versus thoracotomy: indications and advantages. Am. Surg., 1995; 61: [9] Rusch, V. W.: A proposed new international TNM staging system for malignant pleural mesathelioma. Chest, 1995; 108: ] Astoul, P., Viallat, J. R., Laurent, J. C. et al." Intrapleural recombinant IL-2 passive immunotherapy for malignant pleural effusion. Chest, 1993; 103: Boutin, C., Nussbaum, E., Monnet, I. et al: Intrapleural treatment with recombinant gamma interferon in diffuse malignant mesothelioma. Cancer, 1994; 74: [12] Walker-Renard, P., Vaughan, L. M., Sahh, S. A.: Chemical pleurodesis for malignant pleural effusions. Ann. Intern. Med., 1994; 120:
6 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1. Jonathan C. Daniel 2. Kenneth S.
 PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
PET POSITIVE PLEURAL PLAQUES DECADES AFTER PLEURODESIS: MESOLTHELIOMA? Ellen A. Middleton 1 Jonathan C. Daniel 2 Kenneth S. Knox 1 Kathleen Williams 1 Departments of Medicine 1 and Surgery 2, University
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Surgeons Role in Symptom Management. A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND
 Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Surgeons Role in Symptom Management A/Prof Cliff K. C. Choong Consultant Thoracic Surgeon Latrobe Regional Hospital GIPPSLAND Conditions PLEURAL Pleural effusion Pneumothorax ENDOBRONCHIAL Haemoptysis
Therapy of pleural effusions Modern techniques
 Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
Therapy of pleural effusions Modern techniques Dr. Melanie Toffel Sugery of the chest Pleural effusion Ethiology In the normal pleural space there is a steady state in which there is a roughly equal rate
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines
 Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
Clinical cases in Malignant Pleural Mesothelioma: Adherence to the ESMO Clinical Practice Guidelines Wieneke Buikhuisen The Netherlands Cancer Institute Amsterdam The Netherlands Case (1) Male, 56 year
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3
 ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
ASBESTOS EXPOSURE AND SARCOMATOID MALIGNANT PLEURAL MESOTHELIOMA Gorantla Sambasivarao 1, Namballa Usharani 2, Tupakula Suresh Babu 3 HOW TO CITE THIS ARTICLE: Gorantla Sambasivarao, Namballa Usharani,
Malignant Mesothelioma
 Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Mesothelioma
 Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Principal Investigator: Valerie W. Rusch, MD, FACS, Chief, Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Protocol 1101-1088 Phase I study of intra-pleural administration of GL-ONC1 in patients with malignant pleural effusion: primary, metastases and mesothelioma Principal Investigator: Valerie W. Rusch, MD,
Malignant Mesothelioma Current Approaches to a Difficult Problem. Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Mesothelioma: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Diseases. Inflammations Non-inflammatory pleural effusions Pneumothorax Tumours
 Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
Asbestos and your lungs
 This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson
 Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Malignant Pleural Diseases Advances Clinicians Should Know F Gleeson The following relevant disclosures, conflicts of interest and/ or financial relationships exist related to this presentation: Consultant
Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement during Initial Diagnosis
 Case Reports in Pulmonology Volume 2015, Article ID 962504, 4 pages http://dx.doi.org/10.1155/2015/962504 Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement
Case Reports in Pulmonology Volume 2015, Article ID 962504, 4 pages http://dx.doi.org/10.1155/2015/962504 Case Report A Cause of Bilateral Chylothorax: A Case of Mesothelioma without Pleural Involvement
Sternotomy and removal of the tumor
 Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
Sternotomy and removal of the tumor All thymomas originate from epithelial thymic cells 4% of them consist of a pure population of epithelial cells Most have mixed populations of lymphoid cells to a
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
Malignant pleural mesothelioma: outcome of limited surgical management
 Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
Interactive Cardiovascular and Thoracic Surgery 2 (2003) 30 34 Institutional review Thoracic general Malignant pleural mesothelioma: outcome of limited surgical management Peter G. Phillips a, George Asimakopoulos
MesoPDT. Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI. Image Assisted Laser Therapy for Oncology
 MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
Research Article Frequency of Surgery in Black Patients with Malignant Pleural Mesothelioma
 Disease Markers Volume 2015, Article ID 282145, 5 pages http://dx.doi.org/10.1155/2015/282145 Research Article Frequency of Surgery in Black Patients with Malignant Pleural Mesothelioma Emanuela Taioli,
Disease Markers Volume 2015, Article ID 282145, 5 pages http://dx.doi.org/10.1155/2015/282145 Research Article Frequency of Surgery in Black Patients with Malignant Pleural Mesothelioma Emanuela Taioli,
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project
 INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
INTERNATIONAL ASSOCIATION FOR THE STUDY OF LUNG CANCER Prospective Mesothelioma Staging Project Data Forms and Fields in CRAB Electronic Data Capture System - Reduced Set - Pivotal data elements for developing
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Uses and Abuses of Pathology in Asbestos-exposed Populations
 Uses and Abuses of Pathology in Asbestos-exposed Populations Jerrold L. Abraham, MD Department of Pathology State University of New York Upstate Medical University Syracuse, NY, 13210 USA The term: Asbestosis,
Uses and Abuses of Pathology in Asbestos-exposed Populations Jerrold L. Abraham, MD Department of Pathology State University of New York Upstate Medical University Syracuse, NY, 13210 USA The term: Asbestosis,
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Survey of Mesothelioma Associated with Asbestos Exposure in Japan
 The research and development and the dissemination projects related to the 13 fields of occupational injuries and illnesses Survey of Mesothelioma Associated with Asbestos Exposure in Japan Clinical characteristics
The research and development and the dissemination projects related to the 13 fields of occupational injuries and illnesses Survey of Mesothelioma Associated with Asbestos Exposure in Japan Clinical characteristics
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Most cases of mesothelioma are caused by occupational
 Percutaneous Image-Guided Cutting Needle Biopsy of the Pleura in the Diagnosis of Malignant Mesothelioma* Rosie F. Adams, BM BCh; Winifred Gray, MB BS; Robert J. O. Davies, DM; and Fergus V. Gleeson, MB
Percutaneous Image-Guided Cutting Needle Biopsy of the Pleura in the Diagnosis of Malignant Mesothelioma* Rosie F. Adams, BM BCh; Winifred Gray, MB BS; Robert J. O. Davies, DM; and Fergus V. Gleeson, MB
Malignant Pleural Mesothelioma Diagnosed by Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration
 http://dx.doi.org/10.4046/trd.2013.74.2.74 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:74-78 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2013.74.2.74 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:74-78 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
Correspondence should be addressed to Heinz-Jakob Langen; [email protected]
 Radiology Research and Practice, Article ID 312846, 5 pages http://dx.doi.org/1.1155/214/312846 Research Article Performing Chest X-Rays at Inspiration in Uncooperative Children: The Effect of Exercises
Radiology Research and Practice, Article ID 312846, 5 pages http://dx.doi.org/1.1155/214/312846 Research Article Performing Chest X-Rays at Inspiration in Uncooperative Children: The Effect of Exercises
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
PRODYNOV. Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI. Image Assisted Laser Therapy for Oncology
 PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
American Thoracic Society
 American Thoracic Society Management of Malignant Pleural Effusions THIS OFFICIAL STATEMENT OF THE AMERICAN THORACIC SOCIETY WAS ADOPTED BY THE ATS BOARD OF DIRECTORS, MARCH 2000 CONTENTS Incidence Etiology
American Thoracic Society Management of Malignant Pleural Effusions THIS OFFICIAL STATEMENT OF THE AMERICAN THORACIC SOCIETY WAS ADOPTED BY THE ATS BOARD OF DIRECTORS, MARCH 2000 CONTENTS Incidence Etiology
What is Mesothelioma?
 What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
Screening, early referral and treatment for asbestos related cancer
 Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Screening, early referral and treatment for asbestos related cancer Marc de Perrot, MD, MSc, FRCSC Toronto Mesothelioma Research Program University of Toronto Asbestos related diseases Mesothelioma Lung
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Recommendations for the Reporting of Pleural Mesothelioma
 Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
Recommendations for the Reporting of Pleural Mesothelioma Association of Directors of Anatomic and Surgical Pathology * DOI: 10.1309/6A30YQHBMTHEJTEM It has been evident for decades that pathology reports
YOUR LUNG CANCER PATHOLOGY REPORT
 UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
CT findings in Differential Diagnosis between Tuberculous Pleurisy and Malignant Effusion
 CT findings in Differential Diagnosis between Tuberculous Pleurisy and Malignant Effusion Poster No.: E-0084 Congress: ESTI 2012 Type: Scientific Exhibit Authors: S. S. Shim, Y. Kim; Seoul/KR Keywords:
CT findings in Differential Diagnosis between Tuberculous Pleurisy and Malignant Effusion Poster No.: E-0084 Congress: ESTI 2012 Type: Scientific Exhibit Authors: S. S. Shim, Y. Kim; Seoul/KR Keywords:
Diagnostic Challenge. Department of Pathology,
 Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Mesothelioma and Asbestos
 CANCER INFORMATION FACTSHEET Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
CANCER INFORMATION FACTSHEET Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
How To Treat A Cancer With A Radical
 Management of mesothelioma [email protected] Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Management of mesothelioma [email protected] Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Malignant pleural mesothelioma P/D vs. EPP
 3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
Asbestos Related Diseases
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing
 Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing ASBESTOSIS November 2013 Bruce T. Bishop Lucy L. Brandon Willcox & Savage 440
Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing ASBESTOSIS November 2013 Bruce T. Bishop Lucy L. Brandon Willcox & Savage 440
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Pleural Mesotheliomas in Sprague-D~wley Rats by Erionite: First Experimental Evidence
 ENVIRONMENTAL RESEARCH 29, 238-244 (1982) Pleural Mesotheliomas in Sprague-D~wley Rats by Erionite: First Experimental Evidence CESARE MALTONI, FRANCO MINARDI, AND LEONILDO MORISI Institute oj Oncology,
ENVIRONMENTAL RESEARCH 29, 238-244 (1982) Pleural Mesotheliomas in Sprague-D~wley Rats by Erionite: First Experimental Evidence CESARE MALTONI, FRANCO MINARDI, AND LEONILDO MORISI Institute oj Oncology,
Mesothelioma and Asbestos
 Cancer information factsheet Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
Cancer information factsheet Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Low-dose CT Imaging. Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital
 Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Malignant Mesothelioma Diagnosed by Bronchoscopic Biopsy
 CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.3.297 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:297-301 Malignant Mesothelioma Diagnosed by Bronchoscopic Biopsy Yeon-Hee Park,
CASE REPORT http://dx.doi.org/10.4046/trd.2015.78.3.297 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:297-301 Malignant Mesothelioma Diagnosed by Bronchoscopic Biopsy Yeon-Hee Park,
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium
 Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Asbestos Related Diseases. Asbestosis Mesothelioma Lung Cancer Pleural Disease. connecting raising awareness supporting advocating
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
MESOTHELIOMA. Not Just a Late Night Commercial. Graciela Hoal, RN, MSN, ACNP-BC
 MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
MESOTHELIOMA Not Just a Late Night Commercial Graciela Hoal, RN, MSN, ACNP-BC Saturday Session Thoracic Surgery Nurse Practitioner Greater Los Angeles Veteran Affairs Objectives Course Objectives: Discuss
Mesothelioma: Current Perspectives
 Refer to: Taylor RA, Johnson LP: : Current J>cr-, jpcclivej. West J Med 13 THEWESTEEN Journal of Medicine X'
Refer to: Taylor RA, Johnson LP: : Current J>cr-, jpcclivej. West J Med 13 THEWESTEEN Journal of Medicine X'
Evaluation and Management of the Breast Mass. Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003
 Evaluation and Management of the Breast Mass Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003 Common Presentations of Breast Disease Breast Mass Abnormal
Evaluation and Management of the Breast Mass Gary Dunnington,, M.D. Department of Surgery Internal Medicine Ambulatory Conference December 4, 2003 Common Presentations of Breast Disease Breast Mass Abnormal
INFLAMMATORY PLEURAL EFFUSION
 PLEURA- LESIONS LESIONS OF PLEURA Primary Intra pleural bacterial infections Neoplasm (mesothelioma) Secondary A complication of some underlying disease PLEURAL EFFUSION Common manifestation of both primary
PLEURA- LESIONS LESIONS OF PLEURA Primary Intra pleural bacterial infections Neoplasm (mesothelioma) Secondary A complication of some underlying disease PLEURAL EFFUSION Common manifestation of both primary
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
The diagnostic usefulness of tumour markers CEA and CA-125 in pleural effusion
 Malaysian J Path01 2002; 24(1) : 53-58 The diagnostic usefulness of tumour markers CEA and CA-125 in pleural effusion Pavai STHANESHWAR MD, Sook-Fan YAP FRCPath, FRCPA and Gita JAYARAM MDPath, MRCPath
Malaysian J Path01 2002; 24(1) : 53-58 The diagnostic usefulness of tumour markers CEA and CA-125 in pleural effusion Pavai STHANESHWAR MD, Sook-Fan YAP FRCPath, FRCPA and Gita JAYARAM MDPath, MRCPath
How To Understand How Cancer Works
 Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
A succesfull case of HIPEC in a peritoneal mesothelioma patient
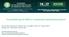 A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma
 The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
Malignant Pleural Mesothelioma. NCCN Guidelines for Patients
 Malignant Pleural Mesothelioma NCCN Guidelines for Patients Presented with support from the national law firm of Baron & Budd Also available at NCCN.com About this booklet Its purpose Learning that you
Malignant Pleural Mesothelioma NCCN Guidelines for Patients Presented with support from the national law firm of Baron & Budd Also available at NCCN.com About this booklet Its purpose Learning that you
PROTOCOL OF THE RITA DATA QUALITY STUDY
 PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
PROTOCOL OF THE RITA DATA QUALITY STUDY INTRODUCTION The RITA project is aimed at estimating the burden of rare malignant tumours in Italy using the population based cancer registries (CRs) data. One of
N26 Chest Tubes 5/9/2012
 Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
