Molina Dual Options MyCare Ohio Regional Molina MyCare Ohio Forum
|
|
|
- Patience Arnold
- 8 years ago
- Views:
Transcription
1 Molina Dual Options MyCare Ohio Regional Molina MyCare Ohio Forum
2 The Molina Mission Vision Statement Molina Healthcare is an innovative national health care leader, providing quality care and accessible services in an efficient and caring manner. Mission Statement Our mission is to provide quality health services to financially vulnerable families and individuals covered by government programs. Core Values We strive to be an exemplary organization. We care about the people we serve and advocate on their behalf. We provide quality service and remove barriers to health services. We are health care innovators and embrace change quickly. We respect each other and value ethical business practices. We are careful in the management of our financial resources and serve as prudent stewards of the public s funds.
3 Molina Healthcare of Ohio Serving since 2005 Medicaid Medicare MyCare Ohio Marketplace Lake Geauga Ashtabula Lucas Cuyahoga Trumbull Ottawa Fulton Erie Williams Lorain Portage Sandusky Summit Mahoning Wood Henry Huron Medina Defiance Seneca Columbiana Stark Hancock Ashland Wayne Paulding Putnam Crawford Wyandot Richland Carroll Jefferson Holmes Van Wert Allen Hardin Morrow Tuscarawas Marion Harrison Knox Auglaize Coshocton Mercer Union Logan Delaware Belmont Guernsey Shelby Licking Champaign Muskingum Miami Franklin Noble Monroe Darke Clark Madison Fairfield Perry Morgan Montgomery Pickaway Washington Preble Greene Hocking Fayette Athens Warren Butler Clinton Ross Vinton Meigs Hamilton Clermont Brown Highland Adams Pike Scioto Jackson Gallia Lawrence Began serving Ohio s Covered Families and Children Medicaid population Began serving Ohio s Aged, Blind or Disabled Medicaid population Awarded contract from Centers for Medicare and Medicaid Services to serve Medicare population Began offering Medicaid services statewide and for Children with Special Health Care Needs Began serving members through the Health Insurance Marketplace; Expanded service to Medicaid Adult Extension Population (childless adults and parents up to 138% FPL); Began serving beneficiaries eligible for both Medicaid and Medicare as part of MyCare Ohio. MHO Snapshot Membership: 337K Employees: 944 Statewide MHO Offices: 3 Provider Network PCP/Specialists: 25K Hospitals: 215 Ancillary Services: 5,782
4
5 My Care Ohio Eligibility Molina Dual Options MyCare Ohio is the name of Molina Healthcare s Medicare- Medicaid Plan (MMP) and is an option for consumers in the Central, West Central, and Southwest regions. Central: Franklin, Madison, Union, Delaware, and Pickaway West Central: Greene, Clark, and Montgomery Southwest: Butler, Warren, Clinton, Clermont, and Hamilton Consumers are eligible to join a MyCare Ohio managed care plan if: They are receiving full benefits from both Medicare and Medicaid They are 18 years of age or older They reside in a MyCare Ohio service region
6 Ohio MyCare Enrollment Medicare Passive Enrollment In 2014, members were only asked to choose or were passively enrolled into a MyCare Ohio plan to administer their Medicaid benefits. Effective Jan. 1, 2015, any member who did not actively choose to NOT participate in their MyCare Ohio plan for their Medicare benefits was passively enrolled. This means the plan assigned to members for their Medicaid benefits in 2014 is now also the plan administering their Medicare benefits. Members still have the right to opt-in or opt-out of the Medicare portion on a monthly basis. They will not have the option to opt-out of the Medicaid portion of MyCare Ohio. Members who wish to opt-out of the Medicare portion must call the Ohio Medicaid Consumer Hotline at (800) or for hearing impaired TTY (800) Any member who is newly eligible for MyCare Ohio after Jan. 1, 2015 who does not choose a plan will be automatically enrolled into one of the managed care plans for both their Medicaid and Medicare benefits.
7 Ohio MyCare Enrollment Medicare Passive Enrollment What are the benefits of having one plan for both Medicare and Medicaid from Molina Healthcare? The benefits of receiving Medicare and Medicaid from Molina Healthcare include: One ID card One point of contact to help you manage all of a member s health needs and assist in benefit explanation for both the Medicare and Medicaid benefits 24-Hour Nurse Advice Line and Behavioral Health Crisis Line Providers will only need to submit a single claim and it will be processed automatically under both the Medicare benefit and the Medicaid benefit. Providers will be able to speak to a single care manager regarding the care of the member. Molina Healthcare also offers value added benefits. For 2015, Molina Dual Options members will be eligible for: Supplemental transportation benefit (60 one-way trips) $20 per month allowance for over-the-counter items $0 copays on generic prescriptions Will the MyCare Ohio benefits be different than traditional Medicare? For Molina Dual Options members, Molina Healthcare will offer at minimum the same benefits as traditional Medicare Part A, Part B and Part D benefits. Molina Healthcare s prior authorization (PA) policies may be different from the Centers for Medicare and Medicaid Services (CMS) or the Ohio Department of Medicaid (ODM). Providers should review these PA rules before providing services to Molina Dual Options members.
8 Ohio MyCare Enrollment Passive Enrollment Split Billing Any member who changed from Medicaid Only (opt-out) to a full Medicare-Medicaid (opt-in) member with Molina Healthcare was given a new member ID number. If the member was passively enrolled, all claims with dates of service from Jan. 1, 2015 and after will need to be billed with the new member ID. All claims with a date of service prior to Jan. 1, 2015 will need to be billed with the member s Medicaid ID number. A claim cannot include a date range with both 2014 and 2015 dates of service if the member s ID number changed. Providers will need to bill two separate claims splitting the dates of service. This will hold true any time a member changes Medicare plans and receives a new member ID.
9 Claims Processing Region Counties Implementation date Number of claims Total Payments made % of denied claims % of claims paid within 30 days Central Southwest West Central Franklin, Union, Delaware, Madison, Pickaway Butler, Warren, Clinton, Hamilton, Clermont Montgomery Clarke, Greene July 1, ,628 $56,929, % 97.12% June 1, ,547 $81,640, % 96.21% July 1, ,904 $33,048, % 96.78% As of 1/26/2015
10 Member Benefits Molina Dual Options provides members with full Medicare Part A, Part B, and Part D as well as full Ohio Medicaid benefits. This includes, but is not limited to, the services listed here. In-patient Services Out-patient Services Rural Health Clinics (RHCS) and Federally Qualified Health Centers (FQHC) Physician Service (in office, home, hospital or elsewhere) Laboratory and X-Ray Services Family Planning Services and Supplies Home Health and Private Duty Nursing Services Podiatry Chiropractic Services DME Dental Services Vision Services Ambulance and Ambulette Services Nursing Facility Services Behavioral Health Services Home and Community-Based Waiver Services
11 Behavioral Health Molina Dual Options Behavioral Health Services may be billed by providers certified by the Department of Mental Health (ODMH) (PT 84) and Ohio Department of Mental Health & Addiction Services (ODMHAS) (PT 95) Alcohol and other Drug Treatment Service Ambulatory HCPCS/CPT Code Required Modifier Billing Increment Reportable In Detoxification H0014 HA or HF Day Whole Unit Assessment H0001 HA or HF Six Minutes.1,.2, etc. Case Management H0006 HA or HF Six Minutes.1,.2, etc. Crisis Intervention H0007 HA or HF Six Minutes.1,.2, etc. Group Counseling H0005 HA or HF 15 Minutes Whole Unit Individual Counseling H0004 HA or HF 15 Minutes Whole Unit Intensive Outpatient H0015 HA or HF Day Whole Unit Laboratory Urinalysis H0003 HA or HF Screen Whole Unit Medical/Somatic H0016 HA or HF Six Minutes.1,.2, etc. Methadone Administration H0020 HA or HF Dose Whole Unit Mental Health Service HCPCS/CPT Code Required Modifier Billing Increment Reportable In BH Counseling- Group H0004 HQ 15 Minutes Whole Unit BH Counseling- Individual H0004 HE or GT 15 Minutes Whole Unit CPST-Group H0036 HQ 15 Minutes Whole Unit CPST-Individual H0036 HE or GT 15 Minutes Whole Unit Crisis Intervention S9484 HE Six Minutes.1,.2, etc. Mental Health Assessment H0031 HE or GT Six Minutes.1,.2, etc. Partial Hospitalization S0201 HE Day Whole Unit Pharmacological Management HE, HQ or GT Six Minutes.1,.2, etc. Psychiatric Diagnostic Interview HE or GT Six Minutes.1,.2, etc.
12 Behavioral Health Prior Authorizations Most out-patient behavioral health services will not require a PA for Behavioral health services that do require a PA will be: Inpatient, residential treatment, partial hospitalization, day treatment Electroconvulsive therapy (ECT) Applied behavioral analysis (ABA) for treatment of autism spectrum disorder (ASD) Providers will need to fill out the Behavioral Health Outpatient Treatment Form and include the appropriate clinical information. The form is available online at
13 HCBS Waivers Assisted Living Waiver Program Medicaid-eligible individuals age 21 and older who require at least an intermediate level of care, are in a nursing facility, and are enrolled in PASSPORT, Choices, Ohio Home Care Waiver, or Transition Carve-Out Waivers. Choices Program Waiver Medicaid-eligible individuals who are age 60 and older who require at least an intermediate level of care and live in an approved service area. Home and Community-Based Services Waivers Medicaid-eligible individuals who would otherwise need to be in a nursing home, hospital, or facility for the mentally retarded and/or developmentally disabled. Home Choice Medicaid-eligible individuals living in a facility-based care setting for at least 90 days and moving into qualified housing. Transitions II Aging Carve-Out Waivers-eligible individuals age 60 or older with either intermediate level of care or skilled per the Ohio Administrative Code (OAC). Ohio Home Care Waiver Program Medicaid-eligible individuals who are younger than age 59 who require an intermediate or skilled level of care. PASSPORT Waiver Program Medicaid-eligible individuals who are age 60 or older, and require at least an intermediate level of care.
14 Waiver Coordinator and Care Management Council on Aging (COA) of Southwestern Ohio Central Ohio Area Agency on Aging Area Agency on Aging PSA2 National Church Residence (NCR) Assisted Care by Blackstone Molina Healthcare Southwest Region Central Region West Central Region Central Region Southwest, Central, West Central Southwest, Central, West Central Waiver Service Coordinator for members age 60 and over. Molina Healthcare will be the Waiver Service Coordinator for members under 60. Waiver Service Coordinator for members age 60 and over. Molina Healthcare will be the Waiver Service Coordinator for members under 60. Waiver Service Coordinator for members age 60 and over. Molina Healthcare will be the Waiver Service Coordinator for members under 60. Members who reside in permanent supportive housing managed by NCR may choose NCR as the waiver service coordinator in the Central Region. Waiver Service Coordinator for members age 60 and over. Molina Healthcare will be the Waiver Service Coordinator for members under 60. Waiver Service Coordinator for members under the age of 60. Molina Healthcare will be the Care Manager for all members with the exclusion of a member in a Health Home.
15 Care Management Contact Schedule Risk stratification level Intensive Minimum contact schedule First six months of enrollment in the risk stratification level (Note: Visit is an in-person contact.) 0-1 month: Two visits. Maximum of 15 days between visits. Month seven until conclusion of the demonstration (Note: Visit is an in-person contact) One visit each month. Maximum of 30 days between visits. 2-6 months: One visit each month. Maximum of 30 days between visits. Telephonic contact as needed. High Medium Low Monitoring 0-1 month: Two visits. Maximum of 15 days between visits. 2-3 months: One visit per month. Maximum of 30 days between visits. 4-6 months: Two visits in 90 days. Maximum of 45 days between visits. Telephonic contact as needed. 0-2 months: One visit. 3-6 months: Two visits. Maximum of 60 days between visits. Telephonic contact as needed. 0-4 months: One visit. 5-6 months: One telephonic contact. 0-6 months: One visit. Telephonic contact as needed. One visit every two months. Maximum of 60 days between visits. Monthly telephonic contact. One visit every three months. Maximum of 90 days between visits. Monthly telephonic contact. One visit every six months. Maximum of 180 days between visits. Quarterly telephonic contact. One visit per year. Semi-annual phone contact.
16 Self-Directed Care Through Morning Star Self-directed services allow participating individuals or their representatives decisionmaking authority and management over their waiver services. Self-directed services give individuals and their families more flexibility, control and responsibility for managing all aspects of the individual s care. Under self-directed care, an individual is the employer and can hire and/or fire a provider for violations of his or her contract. A Waiver Service Coordinator /Molina Care Manager will provide oversight to assist the individual with self-directed personal care. The individual also may choose an authorized representative to help with the day-to-day supervision of his or her service provider and to assist with employer-related tasks. A financial management agency, also known as a fiscal intermediary, will work with individuals to handle the taxes, payroll and worker s compensation responsibilities of being an employer. All self-directed care will be managed through Morning Star.
17 2015 Non-Emergent Transportation Logisticare: For distances greater than 30 miles one way, Logisticare will provide the transportation to Molina Dual Options MyCare Ohio Medicare-Medicaid Plan members. Note: It is important to have your patient(s) call two days in advance of the appointment to schedule the transportation. One additional passenger or escort is allowed to accompany the member if there is space availability. Logisticare does not cover door-to-door transportation. If this level of service is required, please use the Molina MyCare Ohio Medicaid Benefit Value-Added Benefits: New for 2015: Members of Molina Dual Options MyCare Ohio will receive a supplemental transportation benefit of 60 one-way trips at no cost to the member. Members of Molina MyCare Ohio Medicaid do not receive this value added benefit. Logisticare: (877) ; TTY (866) Molina Dual Options Member Services: (855) Molina MyCare Ohio Medicaid Member Services: (855)
18 2015 Non-Emergent Transportation Local County Department of Job and Family Services Non-Emergency Transportation (NET) program will need to be utilized by all members who qualify whether they are on a waiver, or not. If a waiver member is eligible for NET transportation, the member needs to use NET transportation through the county first, as waiver is always payer of last resort. If the member has not completed the application for NET transportation with the county, the Care Manager and Waiver Service Coordinators are to assist with getting the application completed for the member. While the application for NET transportation is pending approval and the member requires transportation, the Care Managers and Waiver Service Coordinators are able to approve waiver transportation on a case-by-case basis until the NET application is approved. Once the application is approved, the member must utilize NET transportation for all eligible rides. NET transportation applications are generally approved within one week of receiving the application at the county offices. If NET cannot meet our members needs, Molina Healthcare may approve the waiver covered benefits. Members may not self-refer for waiver benefits. All waiver services must be approved through Molina Care Managers.
19 2015 Non-Emergent Transportation Skilled Nursing Facility Transportation Molina Healthcare uses its contracted ambulance network and this transportation requires PA. If the facility uses a non-par company, they can direct this provider to call us for PA. If your current preferred vendor is non-par, you can direct them to the Non-par Contract Request Form at Covered services under state plan benefits for non-ambulatory members only: Ambulette/Wheelchair Transport Billing Code A0130 and S0209 No PA required for contracted providers Provider to call Molina Healthcare participating ambulance provider to schedule transportation Ambulance/Non-wheelchair Transport A0426, A0428, A0430, A0431 PA required Provider to call Molina Healthcare participating ambulance provider to schedule transportation Ambulance providers call Molina Healthcare for PA Eligibility dependent upon meeting criteria specified in OAC
20 2015 Non-Emergent Transportation Waiver transportation: During the transition of care period, supplemental transportation will continue to be an inclusive benefit for members on the following waivers of origin: Transitions II Aging Carve-Out Waiver Ohio Home Care Waiver PASSPORT Waiver When the transition of care period is over, all waiver eligible members will be enrolled in the MyCare Ohio combined waiver. At this point, waiver transportation will be determined on a case-by-case basis. Waiver transportation will be included in the waiver service plan that is authorized by the Waiver Service Coordinator/Molina Care Manager. Transportation services must be provided by a transportation provider certified by the Ohio Department of Aging to render this waiver service.
21 Transition of Care (TOC) Transition Requirements Physician Dialysis Treatment HCBS Waiver Beneficiaries 90-day transition for individuals identified for high-risk care management; 365 days for all others 90 days with same provider and level of service; and Comprehensive Plan of Care documents successful transition planning for new provider Non-Waiver Beneficiaries with LTC Needs (HH and PDN use) 90-day transition for individuals identified for high-risk care management; 365 days for all others 90 days with same provider and level of service; and Comprehensive Plan of Care documents successful transition planning for new provider NF Beneficiaries AL Beneficiaries 90-day transition for individuals identified for high-risk care management; 365 days for all others 90 days with same provider and level of service; and Comprehensive Plan of Care documents successful transition planning for new provider Beneficiaries not identified for LTC Services 90-day transition for individuals identified for high-risk care management; 365 days for all others 90 days with same provider and level of service; and Comprehensive Plan of Care documents successful transition planning for new provider
22 Transition of Care (Home Health) Transition Requirements HCBS Waiver Beneficiaries Non-Waiver Beneficiaries with LTC Needs (HH and PDN use) NF Beneficiaries AL Beneficiaries Beneficiaries not identified for LTC Services Medicaid Home Health and PDN Maintain service at current level and with current providers at current Medicaid reimbursement rates. Changes may not occur unless: Sustain existing service for 90 days and then review for medical necessity after an in-person assessment that includes provider observation For AL: Sustain existing service for 90 days and then review for medical necessity after an in-person assessment that includes provider observation N/A A significant change occurs as defined in OAC ; or Individuals express a desire to self-direct services; or After 365 days
23 Transition of Care (Waiver) Transition Requirements HCBS Waiver Beneficiaries Waiver Services Direct Care Personal Care Waiver Nursing Home Care Attendant Choice Home Care Attendant Maintain service at current level and with current providers at current Medicaid reimbursement rates. Plan initiated changes may not occur unless: A significant change occurs as defined in OAC ; or Individuals express a desire to self-direct services; or After 365 days. Out of Home Respite Enhanced Community Living Adult Day Health Services Social Work Counseling Independent Living Assistance Waiver Services All other Maintain service at current level for 365 days and existing service provider at existing rate for 90 days. Plan initiated change in service provider can only occur after an in-home assessment and plan for the transition to a new provider. 23
24 Prior Authorizations (PA) PA is a request for prospective review. It is designed to: Assist in benefit determination Prevent unanticipated denials of coverage Create a collaborative approach to determining the appropriate level of care for members receiving services Identify Care Management and Disease Management opportunities Improve coordination of care Requests for services on the Molina Healthcare Prior Authorization Guide are evaluated by licensed nurses and trained staff that have authority to approve services. Molina Healthcare will not retroactively approve PA services. All services must be requested prior to services being rendered.
25 PA Timeline Molina Healthcare recommends PAs be requested at least seven days prior to services being rendered. UM decision needed Standard (non-expedited) pre-service determination Urgent concurrent review Expedited initial determinations Reopening of adverse determination (additional information received) UM decision needed Routine (non-expedited) pre-service determinations Expedited/urgent determination Urgent concurrent review Molina Medicare/Molina Dual Options Timeliness Standards Decision time frame Within 14 calendar days of receipt of request Within 24 hours of receipt of the request Within 72 hours of receipt of request If meets CMS criteria (MCM Chapter ) for reopening Molina Medicaid Timeliness Standards (services not covered by Medicare) Decision time frame Within 14 calendar days of receipt of request Within 72 hours of receipt of request Within 24 hours of receipt of request
26 PA Timeline PA - Urgent vs. Standard Standards have been established by regulations to ensure a process for determining the urgency of a PA request for medical services. The CMS definition of an expedited PA request is when waiting the standard 14-day turnaround time would jeopardize a member s health or his or her ability to regain maximum function. PA requests for medical services should be marked Urgent following the guidelines listed above. If the clinical information submitted does not support a request as being Urgent, the request will be processed as a Standard request and processed within 14 calendar days. You can submit a PA by fax or by calling the Utilization Management (UM) department. For MyCare Ohio PA requests, please do not use the Molina E-portal. When checking to see if a service requires a PA we strongly recommend first viewing the service request form, then proceeding to verify if the specific CPT code requires a PA or is a non-covered service. The most up-to-date version of these items can be found under the forms section of the Molina Healthcare provider website at
27 Prior Authorizations *Please note: Molina Healthcare s PA requirements are different from ODM and CMS. Please check the pre-service request form and codified list to verify if a particular service requires a PA.
28 Clinical Information Information generally required to support authorization decision making includes: Current (up to six months) adequate patient history related to the requested services Relevant physical examination that addresses the problem Relevant lab or radiology results to support the request (including previous MRI, CT lab or X-ray report/results) Relevant specialty consultation notes Any other information or data specific to the request Home health providers will need a current signed 485 and OASIS assessment. For a continuation of a certification period, Molina Healthcare will need the last two weeks of skilled nursing notes, aide notes, PT/OT notes, etc. Durable Medical Equipment (DME) providers will require a prescription (Rx), certain procedural terminology codes (if using a miscellaneous code, we need a description), diagnosis codes, clinical notes supporting Certificate of Medical Necessity (CMN) (if applicable), home evaluation (if applicable), and invoice pricing.
29 Nursing Facilities What is the process for Nursing Facility admission pre-certifications? The majority of pre-certifications will take place through the discharge planning process, when a member in need of post-acute nursing facility care is identified. Molina Healthcare s Care Review Clinicians will be in direct contact with the acute inpatient facilities, assisting with the discharge process and ensuring that medically necessary nursing facility admissions occur in a timely manner. These requests for nursing facility admissions are reviewed and a determination is rendered within 24 hours. In the event that a member is an emergent admit (i.e. direct admit from home or emergency room due to imminent safety risk) to a nursing facility after normal business hours, Molina Healthcare will accept notification from the nursing facility of the admission on the next business day. Please provide clinical information to support the admission. Who is responsible for calling in the request for the pre-certification? The Nursing Facility is responsible for contacting Molina Healthcare to get pre-certification. The hospital s discharge planner responsibility lies in working with Molina Healthcare to find a facility that will accept the member. The discharge planner needs to instruct the facility to call Molina Healthcare for the pre-certification.
30 Nursing Facilities Care Molina Dual Options member (Molina Healthcare administers both Medicare and Medicaid benefit) Bed Hold Days 30 days per calendar year under Medicaid benefit. No notification required. Hospice Notification only. Medical necessity review is not required with physician s order. Medicaid covers facility room and board. Readmit from acute hospital to skilled bed Readmit from acute hospital to custodial bed New admission - skilled New admission - custodial Currently admitted - status changes from skilled to custodial Currently admitted - status changes from custodial to skilled Authorization required Three-day stay requirement waived Notification only Authorizations entered for six-month periods Authorization required. Three-day stay requirement waived. Authorizations entered for seven-day periods. Notification only with authorizations entered for six-month periods Notification only if member is previously established long-term placement. If long-term placement has not been established, must notify assigned Care Manager so that a level of care (LOC) assessment can be completed. Custodial authorization will be entered for one month pending LOC assessment. Authorization required Authorizations entered for seven-day periods Molina MyCare Ohio Medicaid member (optout; Molina Healthcare administers only the Medicaid benefit) 30 days per calendar year under Medicaid benefit. No notification required. Notification only. Medical necessity review is not required with physician s order. Medicaid covers facility room and board. Notification only. No authorization required until 100 skilled Medicare days have been exhausted. Notification only Authorizations entered for six-month periods Notification only. No authorization required until 100 skilled Medicare days have been exhausted. Authorizations entered for seven-day periods Notification only with authorizations entered for six-month periods Notification only if member is previously established long-term placement. If long-term placement has not been established, must notify assigned Care Manager so that a level of care (LOC) assessment can be completed. Custodial authorization will be entered for one month pending LOC assessment. Notification only. No authorization required until 100 skilled Medicare days have been exhausted. Molina Healthcare Contact Person N/A Assigned Utilization Management (UM) Care Review Clinician Assigned UM Care Review Clinician Assigned Care Management (CM) Care Manager Assigned UM Care Review Clinician Assigned CM Care Manager Assigned UM Care Review Clinician / Assigned CM Care Manager (for non-ltc members) Assigned UM Care Review Clinician
31 Nursing Facilities Care Ancillary/Support services not included in per diem (nonhospice) Therapies (physical, occupational and/or speech) to be billed under Medicare Part B Molina Dual Options member (Molina Healthcare administers both Medicare and Medicaid benefit) Subject to Molina Healthcare s PA List (on website) Service provider will obtain PA directly from Molina Healthcare PA required after initial evaluation and six therapy sessions Molina MyCare Ohio Medicaid member (opt-out; Molina Healthcare administers only the Medicaid benefit) Medicare Primary Services - No PA with Molina Healthcare required. Molina Healthcare will adjudicate claims for secondary Medicaid benefit utilizing Medicare Explanation of Benefits (EOB). Medicaid Primary Services Refer to Molina Healthcare PA grid. No PA with Molina Healthcare required. Molina Healthcare will adjudicate claims for secondary Medicaid benefit utilizing Medicare EOB if Part B therapy cap has been reached. Molina Healthcare Contact Person Assigned UM Care Review Clinician for Molina Dual Options member Assigned UM Care Review Clinician New enrollee in MyCare Ohio while in facility (either skilled or custodial) Contact Molina Healthcare for PA/notification Contact Molina Healthcare for PA/notification Assigned UM Care Review Clinician
32 Nursing Facility Patient Liability What to do if the patient liability taken out was incorrect Patient liability is calculated by the County Department of Job and Family Services (CDJFS) and entered into the ODM enrollment system. Molina Healthcare uses the enrollment files from the state as the source for patient liability and not the amount billed on the claim. Due to a lag from when patient liability is updated by the county and entered in to the ODM enrollment system, Molina Healthcare may not yet have the correct patient liability amount for a given month. Nursing Facility and Hospice Providers If the incorrect patient liability amount has been applied to a claim, send the approved 9401 form with the nursing facility patient liability claims reconsideration form available at Upon receipt, Molina Healthcare will update the member record with the revised patient liability amount and reprocess all associated claims. Please use the following addresses/fax numbers to submit the spreadsheet. To comply with HIPAA, if you submit via , you must use secure . MHOClaimsReconsideration@MolinaHealthcare.com Fax: (800)
33 Nursing Facility Patient Liability
34 Provider Online Resources Provider Manuals Provider Online Directories Web Portal Preventative & Clinical Care Guidelines Prior Authorization Information Advanced Directives Claims Information Pharmacy Information HIPAA Fraud Waste and Abuse Information Frequently Used Forms Communications & Newsletters Member Rights & Responsibilities Contact Information
35 Electronic Funds Transfer & Remittance Advice Molina Healthcare has partnered with our payment vendor, FIS ProviderNet, for Electronic Funds Transfer (EFT) and Electronic Remittance Advice (ERA). Access to the ProviderNet portal is free to our participating providers and we encourage you to register after receiving your first check from Molina Healthcare. New ProviderNet User Registration: 1. Go to 2. Click Register. 3. Accept the Terms. 4. Verify your information BENEFITS Administrative rights to sign-up/manage your own EFT Account Ability to associate new providers within your organization to receive EFT/835s View/print/save PDF versions of your Explanation of Payment (EOP) Historical EOP search by various methods (i.e. claim number, member name) Ability to route files to your File Transfer Protocol (FTP) and/or associated Clearinghouse If you are associated with a Clearinghouse: 1. Go to Connectivity and click the Clearinghouses tab. 2. Select the Tax ID for which this clearinghouse applies. 3. Select a Clearinghouse (if applicable, enter your Trading Partner ID). 4. Select the file types you would like to send to this Clearinghouse and click Save. If you are a registered ProviderNet user: 1. Log in to ProviderNet and click Provider Info. 2. Click Add Payer and select Molina Healthcare from the payers list. 3. Enter recent check number associated with your primary Tax ID and Molina Healthcare. If you have questions regarding the actual registration process, please contact ProviderNet at: (877) or Provider.Services@fisglobal.com
36 Dual Options Provider Training Guides 36
37 Web Portal Use the Web Portal to verify member eligibility, check claims status, run a claims report, view HEDIS scores and PCP roster, and submit and check status of PAs. Web Portal:
38 Secure Messaging with Care Management Secure messaging is a new functionality that allows providers and members to communicate with Care Managers regarding elements of the Personal Health Record (PHR) including lab results, medications, allergies, and care plan. Providers and members can send messages to the Care Manager via Web Portal. Care Managers respond to the messages via Microsoft Outlook notification using new Customer Relationship Management (CRM) functionality.
39 Claims In accordance with 42 C.F.R , Molina Healthcare must pay 90 percent of all submitted clean claims within 30 days of the date of receipt and 99 percent of such claims within 90 days of the date of receipt. The clean pharmacy and non-pharmacy claims will be separately measured against the 30- and 90-day prompt pay standards. The prompt pay requirement applies to the processing of both electronic and paper claims for contracting and non-contracting providers by Molina Healthcare and delegated claims processing entities. These standards have to be met in order for Molina Healthcare to remain compliant with state requirements and ensure providers are paid timely.
40 Claims Claims Submission Options 1. Submit paper claims directly to Molina Healthcare. 2. Clearinghouse (Emdeon) Emdeon is an outside vendor that is used by Molina Healthcare. When submitting Electronic Data Interchange (EDI) Claims (via a Clearinghouse) to Molina Healthcare, please utilize the payer ID. EDI or electronic claims get processed faster than paper claims. Providers can use any Clearinghouse of their choosing. Note that fees may apply. 3. Online submission through Web Portal Services at: Claims Address Molina Dual Options Claims P.O. Box Long Beach, CA EDI Claim Submission Issues Please call the EDI customer service line at (866) and/or submit an to EDI.Claims@molinahealthcare.com Emdeon Payer ID# Emdeon Telephone (877)
41 Claim Submission
42 Claims Customer Service The Corrected Claims form and Claims Reconsideration/Appeal form can be found on our website Participating providers have 120 days from the date of the original remittance advice to submit corrected claims and claim reconsiderations. The completed corrected claim and form may be mailed to: Molina Healthcare PO Box Long Beach, CA The competed reconsideration form and documentation can be faxed to: (800) or mailed to: Molina Healthcare of Ohio Attn: Provider Services PO Box Columbus, OH Corrections can be sent in an electronic format. In the 2300 Loop, the CLM segment (claim information), CLM05-3 (claim frequency type code) must indicate one of the following qualifier codes: 7 REPLACEMENT (Replacement of Prior Claim) 8 VOID (Void/Cancel of Prior Claim) The 2300 Loop, the REF segment (claim information), must include the original claim number issued to the claim being corrected. The original claim number can be found on the remittance advice. Corrected claim bill type for UB claims are billed in Loop 2300/CLM05-01.
43 Provider Bulletin In order to relay information regarding any system updates, a monthly Provider Bulletin is sent to Molina Healthcare s provider network. PA changes Updates to the pharmacy formulary The Provider Bulletin will include, but is not limited to: Provider training opportunities Changes in policies that could impact claim submission, billing procedures, or appeals Updates to the Molina Provider Web Portal Join Our Distribution List To receive this bulletin via , contact ProviderServices@MolinaHealthcare.com to send us your: group name, TIN, service location address, contact name, contact phone number, .
44 Contact Us DEPARTMENT NUMBER Care Management (855) Provider Services (855) Fax (866) Claims Inquiry Customer Service (855) Claims Reconsideration (855) Fax (800) Prior Authorization (855) Medicare Fax (866) Provider Web Portal Help (866) Member Services Molina Dual Options (Dual Benefits) Member Services Molina MyCare Ohio Medicaid (Medicaid Only ) (855) (855) Pharmacy (855) Fax: (888) Community Outreach (855) Fraud, Waste & Abuse Tip Line (866) Fax (877) Hour Nurse Advice Line MyCare Ohio (855) TTY Hour Nurse Advise Line Medicaid/Medicare/Marketplace Member Eligibility (800) (888) TTY (866) Member Services 8 a.m. to 8 p.m. Monday - Friday Provider Services 8 a.m. to 6 p.m. Monday Friday Waiver Providers: OHMyCareLTSS@MolinaHealthcare.com
45 Questions and Comments
2015 Outline of Medicare Supplement Coverage Cover Page (1 of 2) Plans A, F & N Basic Benefits:
 Anthem Blue Cross and Blue Shield Ohio Administrative Office: P.O. Box 659801, San Antonio, TX 78265 9101 Toll Free Telephone Number: 1-866-803-5169 Benefit Chart of Medicare Supplement Plans Sold for
Anthem Blue Cross and Blue Shield Ohio Administrative Office: P.O. Box 659801, San Antonio, TX 78265 9101 Toll Free Telephone Number: 1-866-803-5169 Benefit Chart of Medicare Supplement Plans Sold for
STATE PERFORMANCE MANAGEMENT FOR TREATMENT SERVICES
 STATE PERFORMANCE John R. Kasich, Governor Orman Hall, Director MANAGEMENT FOR TREATMENT SERVICES Understanding and Using the Information for the BH Leadership Group Meeting January 2012 Division of Planning,
STATE PERFORMANCE John R. Kasich, Governor Orman Hall, Director MANAGEMENT FOR TREATMENT SERVICES Understanding and Using the Information for the BH Leadership Group Meeting January 2012 Division of Planning,
***Proposed New Rule - June 2, 2016***
 5123:2-9-20 Home and community-based services - money management under the individual options and level one waivers. (A) Purpose This rule defines money management and sets forth provider qualifications,
5123:2-9-20 Home and community-based services - money management under the individual options and level one waivers. (A) Purpose This rule defines money management and sets forth provider qualifications,
Communities First Ohio -- Program Summary
 HOUSING FINANCE AGENCY/PROGRAM SPONSOR DESCRIPTION AVAILABLE MARKETS ELIGIBLE LENDERS Port of Greater Cincinnati Development Authority www.communitiesfirstohio.org The CommunitiesFirstOhio program provides
HOUSING FINANCE AGENCY/PROGRAM SPONSOR DESCRIPTION AVAILABLE MARKETS ELIGIBLE LENDERS Port of Greater Cincinnati Development Authority www.communitiesfirstohio.org The CommunitiesFirstOhio program provides
Ohio PREP Region 6 Quarterly Newsletter
 Ohio PREP Region 6 Quarterly Newsletter October 2015 Inside This Issue What is Ohio PREP 1 Goals of Ohio PREP 1 Agency Success 2 PREP Coalition 3 Upcoming PREP Training Workshops 3 Ohio PREP Regions 4
Ohio PREP Region 6 Quarterly Newsletter October 2015 Inside This Issue What is Ohio PREP 1 Goals of Ohio PREP 1 Agency Success 2 PREP Coalition 3 Upcoming PREP Training Workshops 3 Ohio PREP Regions 4
To begin your search, click the red button called Click here to search for Nursing Homes.
 NURSING HOME SEARCH To search for a nursing home, either click the link called Nursing Homes (including short-term rehabilitation) or use the red menu bar at the top for Nursing Homes. At any time during
NURSING HOME SEARCH To search for a nursing home, either click the link called Nursing Homes (including short-term rehabilitation) or use the red menu bar at the top for Nursing Homes. At any time during
FORMS 1099-MISC. James Driver Federal, State, and Local Government Specialist James.driver@irs.gov 859-244-2449
 FORMS 1099-MISC James Driver Federal, State, and Local Government Specialist James.driver@irs.gov 859-244-2449 1 What is a 1099-MISC information return? Form required to report payments for: Services or,
FORMS 1099-MISC James Driver Federal, State, and Local Government Specialist James.driver@irs.gov 859-244-2449 1 What is a 1099-MISC information return? Form required to report payments for: Services or,
Analysis of Proposed Tax Levies for Library Purposes
 Analysis of Proposed Tax Levies for Library Purposes March 2013 Prepared for the Ohio Library Council by Howard Fleeter & Associates 60 East Broad Street, Suite 350 Columbus, Ohio 43215 I. Overview This
Analysis of Proposed Tax Levies for Library Purposes March 2013 Prepared for the Ohio Library Council by Howard Fleeter & Associates 60 East Broad Street, Suite 350 Columbus, Ohio 43215 I. Overview This
Eligibility Molina Dual Options MyCare Ohio Medicare-Medicaid Plan Central West Central Southwest Southwest: West Central: Central:
 Molina Dual Options MyCare Ohio Transportation Benefit Provider Services Molina Healthcare June 2015 Eligibility Molina Dual Options MyCare Ohio Medicare-Medicaid Plan is a health plan that contracts with
Molina Dual Options MyCare Ohio Transportation Benefit Provider Services Molina Healthcare June 2015 Eligibility Molina Dual Options MyCare Ohio Medicare-Medicaid Plan is a health plan that contracts with
Molina Dual Options MyCare Ohio Medicare-Medicaid Plan FAQ s
 Molina Dual Options MyCare Ohio Medicare-Medicaid Plan FAQ s Coverage and Benefits Q: What is the Molina Dual Options MyCare Ohio Medicare-Medicaid Plan? A: Molina Dual Options is a health plan that contracts
Molina Dual Options MyCare Ohio Medicare-Medicaid Plan FAQ s Coverage and Benefits Q: What is the Molina Dual Options MyCare Ohio Medicare-Medicaid Plan? A: Molina Dual Options is a health plan that contracts
Molina Healthcare Dual Options Transportation Benefit 2014
 Molina Healthcare Dual Options Transportation Benefit 2014 Eligibility Dual Options (MMP) is the name of Molina s Medicare-Medicaid and will be an option for consumers in the Central, West Central, and
Molina Healthcare Dual Options Transportation Benefit 2014 Eligibility Dual Options (MMP) is the name of Molina s Medicare-Medicaid and will be an option for consumers in the Central, West Central, and
Ohio Legislative Service Commission
 Ohio Legislative Service Commission Fiscal Note & Local Impact Statement Todd A. Celmar Bill: Sub. H.B. 1 of the 130th G.A. Date: June 13, 2013 Status: As Passed by the Senate Sponsor: Rep. Derickson and
Ohio Legislative Service Commission Fiscal Note & Local Impact Statement Todd A. Celmar Bill: Sub. H.B. 1 of the 130th G.A. Date: June 13, 2013 Status: As Passed by the Senate Sponsor: Rep. Derickson and
The tangible personal property tax, which applies
 The tangible personal property tax, which applies to property used in business in Ohio, is gradually being phased out as part of a broader series of tax reforms enacted in 2005 by the General Assembly.
The tangible personal property tax, which applies to property used in business in Ohio, is gradually being phased out as part of a broader series of tax reforms enacted in 2005 by the General Assembly.
Wherever you go... You ll feel safer with MedFlight Advantage
 Wherever you go... You ll feel safer with MedFlight Advantage YOUR FAMILY DE AN ADVANTAGE Industry leaders MedFlight, MedCare Ambulance and AirMed have joined forces to create a plan to protect you and
Wherever you go... You ll feel safer with MedFlight Advantage YOUR FAMILY DE AN ADVANTAGE Industry leaders MedFlight, MedCare Ambulance and AirMed have joined forces to create a plan to protect you and
Child Welfare System: Opportunities to Improve Coordination and Consistency in a Complex System April, 2013
 Child Welfare System: Opportunities to Improve Coordination and Consistency in a Complex System April, 2013 Part I. Introduction and Background The Public Children Services Agencies (PCSAs) are the county-level
Child Welfare System: Opportunities to Improve Coordination and Consistency in a Complex System April, 2013 Part I. Introduction and Background The Public Children Services Agencies (PCSAs) are the county-level
1-237 Adams *Adams $54,253 $0 Assistance Program ADAMS COUNTY TOTAL. $67,320 $24,944 Crime Victim Services 2-056 Allen *Allen Putnam $17,091 $205,346
 2014 Grant Allocations for Web Page 1 File County Counties SVAA VOCA Reach Out Inc. 1-102 Adams *Adams $13,067 $24,944 Adams Co. Prosecutor Victims 1-237 Adams *Adams $54,253 $0 Assistance ADAMS COUNTY
2014 Grant Allocations for Web Page 1 File County Counties SVAA VOCA Reach Out Inc. 1-102 Adams *Adams $13,067 $24,944 Adams Co. Prosecutor Victims 1-237 Adams *Adams $54,253 $0 Assistance ADAMS COUNTY
Induced Abortions in Ohio Ohio Department of Health OHIO 2013. An equal opportunity employer/provider
 OHIO 2013 Induced Abortions in Ohio Ohio Department of Health John Kasich, Governor Richard Hodges, Director of Health An equal opportunity employer/provider Induced Abortions in Ohio, 2013 Prepared by:
OHIO 2013 Induced Abortions in Ohio Ohio Department of Health John Kasich, Governor Richard Hodges, Director of Health An equal opportunity employer/provider Induced Abortions in Ohio, 2013 Prepared by:
MyCare Ohio Skilled Nursing Facility Orientation
 MyCare Ohio Skilled Nursing Facility Orientation Demonstration/Pilot Area Demonstration/Pilot Area 2 Health Plan Options Northwest Southwest West Central Central East Central Northeast Central Northeast
MyCare Ohio Skilled Nursing Facility Orientation Demonstration/Pilot Area Demonstration/Pilot Area 2 Health Plan Options Northwest Southwest West Central Central East Central Northeast Central Northeast
Ohio s Plug-In Electric Vehicle (PEV) Infrastructure Readiness Strategy. Joanna M. Pinkerton, PE Office of Jobs & Commerce
 Ohio s Plug-In Electric Vehicle (PEV) Infrastructure Readiness Strategy Joanna M. Pinkerton, PE Office of Jobs & Commerce Month June 26, 0, 2012 2011 Ohio s PEV Readiness Strategy Goal: To develop and
Ohio s Plug-In Electric Vehicle (PEV) Infrastructure Readiness Strategy Joanna M. Pinkerton, PE Office of Jobs & Commerce Month June 26, 0, 2012 2011 Ohio s PEV Readiness Strategy Goal: To develop and
Wherever you go... You ll feel safer with the MedFlight Advantage
 Wherever you go... You ll feel safer with the MedFlight Advantage YOUR FAMILY DESERVES AN ADVANTAGE Industry leaders MedFlight, MedCare Ambulance and AirMed have joined forces to create a plan to protect
Wherever you go... You ll feel safer with the MedFlight Advantage YOUR FAMILY DESERVES AN ADVANTAGE Industry leaders MedFlight, MedCare Ambulance and AirMed have joined forces to create a plan to protect
Dental Orientation. Molina Healthcare
 Dental Orientation Molina Healthcare Scion Provider Web Portal The Scion Electronic Outreach Team is calling all providers offices to provide information and help with registration. Some offices may receive
Dental Orientation Molina Healthcare Scion Provider Web Portal The Scion Electronic Outreach Team is calling all providers offices to provide information and help with registration. Some offices may receive
Metropolitan & Micropolitan Statistical Area Definitions in Ohio Based on 2000 Census Designations**
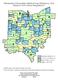 Metropolitan & Micropolitan Statistical Area Definitions in Ohio Based on 2000 Census Designations** * Statistical Areas in other states that include Ohio counties **Click on the letters or numbers to
Metropolitan & Micropolitan Statistical Area Definitions in Ohio Based on 2000 Census Designations** * Statistical Areas in other states that include Ohio counties **Click on the letters or numbers to
MI Health Link Program Nursing Facility Presentation June 3, 2015. Molina Healthcare of Michigan
 Program Nursing Facility Presentation June 3, 2015 Molina Healthcare of Michigan Headline Goes Here The Molina Story In 1980, the late Dr. C. David Molina, founded Molina Healthcare with a single clinic
Program Nursing Facility Presentation June 3, 2015 Molina Healthcare of Michigan Headline Goes Here The Molina Story In 1980, the late Dr. C. David Molina, founded Molina Healthcare with a single clinic
polymers & chemicals Partner with the Industry Leader
 polymers & chemicals Partner with the Industry Leader Quick Facts Employment 87,488 people Gross State Product (GSP) $13.7 billion Average Wages $56,461 Number of Firms 1,287 Rank in 2 nd 1 st the U.S.
polymers & chemicals Partner with the Industry Leader Quick Facts Employment 87,488 people Gross State Product (GSP) $13.7 billion Average Wages $56,461 Number of Firms 1,287 Rank in 2 nd 1 st the U.S.
Molina Healthcare of Ohio Nursing Facility Orientation Molina Dual Options MyCare Ohio 2014
 Molina Healthcare of Ohio Nursing Facility Orientation Molina Dual Options MyCare Ohio 2014 1 Eligibility Headline Goes Here Long Term Care (LTC) is the provision of medical, social, and personal care
Molina Healthcare of Ohio Nursing Facility Orientation Molina Dual Options MyCare Ohio 2014 1 Eligibility Headline Goes Here Long Term Care (LTC) is the provision of medical, social, and personal care
Evidence of Coverage:
 January 1 December 31, 2015 Evidence of Coverage: Your Medicare Health Benefits and Services and Prescription Drug Coverage as a Member of HealthSpan Medicare Standard (HMO) This booklet gives you the
January 1 December 31, 2015 Evidence of Coverage: Your Medicare Health Benefits and Services and Prescription Drug Coverage as a Member of HealthSpan Medicare Standard (HMO) This booklet gives you the
Molina Healthcare of Puerto Rico (MHPR) Non-Participating Provider Information
 Molina Healthcare of Puerto Rico (MHPR) Non-Participating Provider Information Please refer to Carta Normativa 15-0326 Re Transicion for details regarding the ASES-established Transition of Care and Reimbursement
Molina Healthcare of Puerto Rico (MHPR) Non-Participating Provider Information Please refer to Carta Normativa 15-0326 Re Transicion for details regarding the ASES-established Transition of Care and Reimbursement
Ohio Rapid Response Vendor List
 Rapid Response Vendor List AIG Financial Charles Betz 3455 Mill Run Drive, Suite 100 Hilliard Zip 43026 charles.betz@agla.com Phone (614)376-9205 Transition Center, Peer to Peer Support, Job Fair Counties
Rapid Response Vendor List AIG Financial Charles Betz 3455 Mill Run Drive, Suite 100 Hilliard Zip 43026 charles.betz@agla.com Phone (614)376-9205 Transition Center, Peer to Peer Support, Job Fair Counties
DIVISION OF PAROLE AND COMMUNITY SERVICES Parole Officer Assessment Packet
 DIVISION OF PAROLE AND COMMUNITY SERVICES Parole Officer Assessment Packet Requirements for Employment January 2007 Attached, you will find a map of the seven Adult Parole Authority Regions, the Parole
DIVISION OF PAROLE AND COMMUNITY SERVICES Parole Officer Assessment Packet Requirements for Employment January 2007 Attached, you will find a map of the seven Adult Parole Authority Regions, the Parole
How To Participate In The Well Sense Health Plan
 Well Sense Health Plan How We Do Business with Providers New Hampshire Health Protection Program August 2014 Agenda Working with Well Sense and our members Our partners Provider responsibilities Resources
Well Sense Health Plan How We Do Business with Providers New Hampshire Health Protection Program August 2014 Agenda Working with Well Sense and our members Our partners Provider responsibilities Resources
Ohio Air Quality 2011
 September 22 Ohio Air Quality 2 Division of Air Pollution Control John R. Kasich, Governor Mary Taylor, Lt. Governor Scott J. Nally, Director Blank Page 46 STATE OF OHIO AIR QUALITY CALENDAR YEAR 2 PREPARED
September 22 Ohio Air Quality 2 Division of Air Pollution Control John R. Kasich, Governor Mary Taylor, Lt. Governor Scott J. Nally, Director Blank Page 46 STATE OF OHIO AIR QUALITY CALENDAR YEAR 2 PREPARED
Behavioral Health Provider Training: Substance Abuse Treatment Updates
 Behavioral Health Provider Training: Substance Abuse Treatment Updates Agenda Laboratory Services Behavioral Health Claims Submission Process Targeted Case Management Utilization Management eservices Claims
Behavioral Health Provider Training: Substance Abuse Treatment Updates Agenda Laboratory Services Behavioral Health Claims Submission Process Targeted Case Management Utilization Management eservices Claims
What is the prior authorization process for Skilled Nursing Facility Admission?
 MyCare Long Term Care (LTC) Nursing Facility FAQs The nursing facility network is an essential part of the health care delivery system and we value your partnership. We appreciate the compassion you offer
MyCare Long Term Care (LTC) Nursing Facility FAQs The nursing facility network is an essential part of the health care delivery system and we value your partnership. We appreciate the compassion you offer
How To Contact Americigroup
 Mental Health Rehabilitative Services and Mental Health Targeted Case Management TXPEC-0870-14 1 Agenda Key contacts Eligibility Mental Health Rehabilitative services (MHR) and Mental Health Targeted (TCM)
Mental Health Rehabilitative Services and Mental Health Targeted Case Management TXPEC-0870-14 1 Agenda Key contacts Eligibility Mental Health Rehabilitative services (MHR) and Mental Health Targeted (TCM)
Mortgage Solutions for First-Time Homebuyers
 Mortgage Solutions for First-Time Homebuyers QUALIFIED MORTGAGES 2010 Dodd-Frank Wall Street Reform and Consumer Protection Act. Amends Regulation Z, Truth in Lending. Must prove the ability to repay the
Mortgage Solutions for First-Time Homebuyers QUALIFIED MORTGAGES 2010 Dodd-Frank Wall Street Reform and Consumer Protection Act. Amends Regulation Z, Truth in Lending. Must prove the ability to repay the
S.B. 236 126th General Assembly (As Introduced)
 Jennifer A. Parker Bill Analysis Legislative Service Commission S.B. 236 126th General Assembly (As Introduced) Sen. Carey BILL SUMMARY Implements the provisions of Section 2p, Article VIII of the Ohio
Jennifer A. Parker Bill Analysis Legislative Service Commission S.B. 236 126th General Assembly (As Introduced) Sen. Carey BILL SUMMARY Implements the provisions of Section 2p, Article VIII of the Ohio
CareSource MyCare Ohio (Medicare Medicaid Plan)
 CareSource MyCare Ohio (Medicare Medicaid Plan) What is MyCare Ohio? MyCare Ohio is the state of Ohio s Dual Demonstration. MyCare Ohio is a system of managed care plans selected to coordinate the physical,
CareSource MyCare Ohio (Medicare Medicaid Plan) What is MyCare Ohio? MyCare Ohio is the state of Ohio s Dual Demonstration. MyCare Ohio is a system of managed care plans selected to coordinate the physical,
Behavioral Health Provider Training: Program Overview & Helpful Information
 Behavioral Health Provider Training: Program Overview & Helpful Information Overview The Passport Behavioral Health Program provides members with access to a full continuum of recovery and resiliency focused
Behavioral Health Provider Training: Program Overview & Helpful Information Overview The Passport Behavioral Health Program provides members with access to a full continuum of recovery and resiliency focused
Quick Reference Guide
 Ohio Non-Participating Provider 2014 Physician, Health Care Professional, Facility and Ancillary Quick Reference Guide UHCCommunityPlan.com Important Phone Numbers Provider Services Department 800-600-9007
Ohio Non-Participating Provider 2014 Physician, Health Care Professional, Facility and Ancillary Quick Reference Guide UHCCommunityPlan.com Important Phone Numbers Provider Services Department 800-600-9007
2015 Summary of Benefits
 2015 Summary of Benefits Plans 003 and 004 H6298_14_027 accepted Summary of Benefits January 1, 2015 - December 31, 2015 This booklet gives you a summary of what we cover and what you pay. It doesn t list
2015 Summary of Benefits Plans 003 and 004 H6298_14_027 accepted Summary of Benefits January 1, 2015 - December 31, 2015 This booklet gives you a summary of what we cover and what you pay. It doesn t list
Ann E. Teske, PhD, RN, Associate Professor, Department of Nursing, Otterbein University Heather Reed, MA, Primary Care and Rural Health
 Ann E. Teske, PhD, RN, Associate Professor, Department of Nursing, Otterbein University Heather Reed, MA, Primary Care and Rural Health Administrator, Ohio Department of Health Exploratory Descriptive
Ann E. Teske, PhD, RN, Associate Professor, Department of Nursing, Otterbein University Heather Reed, MA, Primary Care and Rural Health Administrator, Ohio Department of Health Exploratory Descriptive
Section 9. Claims Claim Submission Molina Healthcare PO Box 22815 Long Beach, CA 90801
 Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Molina Healthcare of Ohio Provider Orientation - Medicaid
 Molina Healthcare of Ohio Provider Orientation - Medicaid Headline Goes Here Our Story In 1980, the late Dr. C. David Molina founded Molina Healthcare with a single clinic and a commitment to provide quality
Molina Healthcare of Ohio Provider Orientation - Medicaid Headline Goes Here Our Story In 1980, the late Dr. C. David Molina founded Molina Healthcare with a single clinic and a commitment to provide quality
Managed Care Organization and Provider Forum Region 3 June 24, 2013
 Managed Care Organization and Provider Forum Region 3 June 24, 2013 Humana Headquartered in Kentucky Fortune 100 company Leading national healthcare company 12 million medical members 8 million specialty
Managed Care Organization and Provider Forum Region 3 June 24, 2013 Humana Headquartered in Kentucky Fortune 100 company Leading national healthcare company 12 million medical members 8 million specialty
Third Quarter Updates Q3 2014
 Third Quarter Updates Q3 2014 0714.PR.P.PP. 2014 Agenda Claim Process Reminders and Updates Top Rejections Top Denials IHCP Updates Resources Claim Process Electronic submission MHS accepts TPL information
Third Quarter Updates Q3 2014 0714.PR.P.PP. 2014 Agenda Claim Process Reminders and Updates Top Rejections Top Denials IHCP Updates Resources Claim Process Electronic submission MHS accepts TPL information
Healthy Michigan MEMBER HANDBOOK
 Healthy Michigan MEMBER HANDBOOK 2014 The new name for Healthy 1 TABLE OF CONTENTS WELCOME TO HARBOR HEALTH PLAN.... 2 Who Is Harbor Health Plan?...3 How Do I Reach Member Services?...3 Is There A Website?....
Healthy Michigan MEMBER HANDBOOK 2014 The new name for Healthy 1 TABLE OF CONTENTS WELCOME TO HARBOR HEALTH PLAN.... 2 Who Is Harbor Health Plan?...3 How Do I Reach Member Services?...3 Is There A Website?....
Table of Contents. List of Figures and Tables
 Table of Contents Acknowledgements... 3 1.0 Executive Summary... 4 2.0 Introduction... 6 3.0 Methodology... 8 4.0 Results... 10 4.1 DS3 Services... 12 4.2 OC3 (155 Mbps) Services... 14 4.3 OC12 (622 Mbps)
Table of Contents Acknowledgements... 3 1.0 Executive Summary... 4 2.0 Introduction... 6 3.0 Methodology... 8 4.0 Results... 10 4.1 DS3 Services... 12 4.2 OC3 (155 Mbps) Services... 14 4.3 OC12 (622 Mbps)
LTC Monthly Claims Training How to Bill UB04 on Web Portal
 LTC Monthly Claims Training How to Bill UB04 on Web Portal Statewide Medicaid Managed Care: Key Components STATEWIDE MEDICAID MANAGED CARE PROGRAM MANAGED MEDICAL ASSISTANCE PROGRAM LONG-TERM CARE PROGRAM
LTC Monthly Claims Training How to Bill UB04 on Web Portal Statewide Medicaid Managed Care: Key Components STATEWIDE MEDICAID MANAGED CARE PROGRAM MANAGED MEDICAL ASSISTANCE PROGRAM LONG-TERM CARE PROGRAM
Section 6. Medical Management Program
 Section 6. Medical Management Program Introduction Molina Healthcare maintains a medical management program to ensure patient safety as well as detect and prevent fraud, waste and abuse in its programs.
Section 6. Medical Management Program Introduction Molina Healthcare maintains a medical management program to ensure patient safety as well as detect and prevent fraud, waste and abuse in its programs.
The RN & APRN Workforce in Ohio
 March 2015 Ohio Action Coalition The RN & APRN Workforce in Ohio An Overview of 2013 Licensure Renewal Data This analysis of the 2013 licensure renewal data was supported by funds from the State Implementation
March 2015 Ohio Action Coalition The RN & APRN Workforce in Ohio An Overview of 2013 Licensure Renewal Data This analysis of the 2013 licensure renewal data was supported by funds from the State Implementation
KanCare Billing and Payment
 JANUARY 2013 KMAP HCBS & NF BULLETIN 13021 KanCare Billing and Payment Kansas Department of Health and Environment, Division of Health Care Finance (KDHE-DHCF) and Kansas Department for Aging and Disability
JANUARY 2013 KMAP HCBS & NF BULLETIN 13021 KanCare Billing and Payment Kansas Department of Health and Environment, Division of Health Care Finance (KDHE-DHCF) and Kansas Department for Aging and Disability
Molina Healthcare of Ohio, Inc. PO Box 22712 Long Beach, CA 90801
 Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Community Mental Health Services (Provider Type 84)
 Ohio Department of Mental Health and Addiction Services (ODMS) MyCare Ohio Billing Guide For members who have Molina MyCare Ohio for both and, providers will only need to bill a single claim and it will
Ohio Department of Mental Health and Addiction Services (ODMS) MyCare Ohio Billing Guide For members who have Molina MyCare Ohio for both and, providers will only need to bill a single claim and it will
Ohio MHAS - SFY 2015 SAPT BG PASS-THRU GRANTS
 Allen Lima Urban Minority Alcohol Drug Abuse Outreach Program4256C UMADAOP UMADAOP 141,394 Lima-Urban Minority Alcohol Drug Abuse Outreach Prog. Inc. 4221F Womens Treatment 18,364 4224M Circle for Recovery
Allen Lima Urban Minority Alcohol Drug Abuse Outreach Program4256C UMADAOP UMADAOP 141,394 Lima-Urban Minority Alcohol Drug Abuse Outreach Prog. Inc. 4221F Womens Treatment 18,364 4224M Circle for Recovery
Frequently Asked Questions (FAQs) from December 2013 Behavioral Health Utilization Management Webinars
 Frequently Asked Questions (FAQs) from December 2013 Behavioral Health Utilization Management Webinars 1. In the past we did precertifications for Residential Treatment Centers (RTC). Will this change
Frequently Asked Questions (FAQs) from December 2013 Behavioral Health Utilization Management Webinars 1. In the past we did precertifications for Residential Treatment Centers (RTC). Will this change
CLAIM FORM REQUIREMENTS
 CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
H7833_150304MO01. Information for Care Providers about UnitedHealthcare Connected (Medicare- Medicaid Plan) in Harris County, Texas
 H7833_150304MO01 Information for Care Providers about UnitedHealthcare Connected (Medicare- Medicaid Plan) in Harris County, Texas Agenda Connecting Medicare and Medicaid Eligible Members Service Coordination
H7833_150304MO01 Information for Care Providers about UnitedHealthcare Connected (Medicare- Medicaid Plan) in Harris County, Texas Agenda Connecting Medicare and Medicaid Eligible Members Service Coordination
Ohio s Integrated Care Delivery System (ICDS) MyCare Ohio. (for HCBS Waiver providers) Ohio Department of Medicaid January 29, 2014
 Ohio s Integrated Care Delivery System (ICDS) MyCare Ohio (for HCBS Waiver providers) Ohio Department of Medicaid January 29, 2014 1 What is MyCare Ohio? New opportunities generated by the Affordable Care
Ohio s Integrated Care Delivery System (ICDS) MyCare Ohio (for HCBS Waiver providers) Ohio Department of Medicaid January 29, 2014 1 What is MyCare Ohio? New opportunities generated by the Affordable Care
SUMMARY OF BADGERCARE PLUS BENEFITS
 SUMMARY OF BADGERCARE PLUS BENEFITS Medical, mental health and substance abuse services Dental emergency NOT Pharmacy, chiropractic and dental services NOT 13 Ambulatory surgery centers Coverage of certain
SUMMARY OF BADGERCARE PLUS BENEFITS Medical, mental health and substance abuse services Dental emergency NOT Pharmacy, chiropractic and dental services NOT 13 Ambulatory surgery centers Coverage of certain
Enrollment Processing Center PO Box 659403 San Antonio, TX 78265-9403
 Enrollment Processing Center PO Box 659403 San Antonio, TX 78265-9403 Dear Friend: Thank you for considering us for your Medicare Advantage plan. I wish that I could sit down with you and go over all the
Enrollment Processing Center PO Box 659403 San Antonio, TX 78265-9403 Dear Friend: Thank you for considering us for your Medicare Advantage plan. I wish that I could sit down with you and go over all the
27. Will the plan pay for radiology done in the provider s office?... 10 28. How do providers request assistance with care management issues?...
 Provider Q&A Contents 1. Who is Florida True Health?... 3 2. What is the new product name?... 3 3. Does the plan have a website?... 3 4. How will physicians be paid? (FFS or capitation)... 3 5. What clearing
Provider Q&A Contents 1. Who is Florida True Health?... 3 2. What is the new product name?... 3 3. Does the plan have a website?... 3 4. How will physicians be paid? (FFS or capitation)... 3 5. What clearing
Summary of Services and Cost Shares
 Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Grantee Telephone Program(s) Counties Served
 Grantee Telephone Program(s) Counties Served Adams Co. Chamber of Commerce P.O. Box 398 509 E. Main Street West Union, Ohio 45693 Contact: Deana Swayne deana@adamscountychamber.org ACEnet Ventures 94 Columbus
Grantee Telephone Program(s) Counties Served Adams Co. Chamber of Commerce P.O. Box 398 509 E. Main Street West Union, Ohio 45693 Contact: Deana Swayne deana@adamscountychamber.org ACEnet Ventures 94 Columbus
Provider Handbook Supplement for Blue Shield of California (BSC)
 Magellan Healthcare, Inc. * Provider Handbook Supplement for Blue Shield of California (BSC) *In California, Magellan does business as Human Affairs International of California, Inc. and/or Magellan Health
Magellan Healthcare, Inc. * Provider Handbook Supplement for Blue Shield of California (BSC) *In California, Magellan does business as Human Affairs International of California, Inc. and/or Magellan Health
Choose the Medicare Advantage Plan That s Right for You
 Choose the Medicare Advantage Plan That s Right for You Indiana University Health Plans is a Medicare Advantage organization with a Medicare contract. Other pharmacies/physicians/providers are available
Choose the Medicare Advantage Plan That s Right for You Indiana University Health Plans is a Medicare Advantage organization with a Medicare contract. Other pharmacies/physicians/providers are available
The Healthy Michigan Plan Handbook
 The Healthy Michigan Plan Handbook Introduction The Healthy Michigan Plan is a health care program through the Michigan Department of Community Health (MDCH). The Healthy Michigan Plan provides health
The Healthy Michigan Plan Handbook Introduction The Healthy Michigan Plan is a health care program through the Michigan Department of Community Health (MDCH). The Healthy Michigan Plan provides health
Claims and Billing Process. AHCCCS Provider Identification Number and NPI Number
 Claims and Billing Process AHCCCS Provider Identification Number and NPI Number All United Healthcare Community Plan providers requesting reimbursement for services must be properly registered with AHCCCS
Claims and Billing Process AHCCCS Provider Identification Number and NPI Number All United Healthcare Community Plan providers requesting reimbursement for services must be properly registered with AHCCCS
BadgerCare Plus and Wisconsin Medicaid Covered Services Comparison Chart
 and Wisconsin Covered Services Comparison Chart The covered services information in the following chart is provided as general information. Providers should refer to their service-specific publications
and Wisconsin Covered Services Comparison Chart The covered services information in the following chart is provided as general information. Providers should refer to their service-specific publications
Piedmont WellStar Medicare Choice (HMO) offered by Piedmont WellStar HealthPlans, Inc.
 Piedmont WellStar Medicare Choice (HMO) offered by Piedmont WellStar HealthPlans, Inc. Annual Notice of Changes for 2015 You are currently enrolled as a member of Piedmont WellStar Medicare Choice HMO.
Piedmont WellStar Medicare Choice (HMO) offered by Piedmont WellStar HealthPlans, Inc. Annual Notice of Changes for 2015 You are currently enrolled as a member of Piedmont WellStar Medicare Choice HMO.
Superior HealthPlan Hospital Training. SHP_2013158 Hospital Orientation Presentation
 Superior HealthPlan Hospital Training SHP_2013158 Hospital Orientation Presentation Introductions & Agenda Presenter Introductions About Superior HealthPlan Eligibility Medical Management CHIP Perinate
Superior HealthPlan Hospital Training SHP_2013158 Hospital Orientation Presentation Introductions & Agenda Presenter Introductions About Superior HealthPlan Eligibility Medical Management CHIP Perinate
Annual Notice of Changes/ Evidence of Coverage 2015
 Annual Notice of Changes/ Evidence of Coverage 2015 Indiana University Health Plans Medicare Select HMO 950 N. Meridian St., Suite 200 Indianapolis, IN 46204-1202 800.455.9776 TTY users call Relay Indiana
Annual Notice of Changes/ Evidence of Coverage 2015 Indiana University Health Plans Medicare Select HMO 950 N. Meridian St., Suite 200 Indianapolis, IN 46204-1202 800.455.9776 TTY users call Relay Indiana
Tribute Health Plan of Arkansas (HMO SNP), a Superior Select product.
 Tribute Health Plan of Arkansas (HMO SNP), a Superior Select product. Tribute Health Plan of Arkansas HMO SNP is a Health plan with a Medicare contract. Enrollment in Tribute Health Plan of Arkansas HMO
Tribute Health Plan of Arkansas (HMO SNP), a Superior Select product. Tribute Health Plan of Arkansas HMO SNP is a Health plan with a Medicare contract. Enrollment in Tribute Health Plan of Arkansas HMO
AETNA MEDICARE OPEN SM PLAN PROVIDER TERMS AND CONDITIONS OF PAYMENT
 AETNA MEDICARE OPEN SM PLAN PROVIDER TERMS AND CONDITIONS OF PAYMENT Table of Contents 1. Introduction 2. When a provider is deemed to accept Aetna Medicare Open Plan s terms and conditions 3. Provider
AETNA MEDICARE OPEN SM PLAN PROVIDER TERMS AND CONDITIONS OF PAYMENT Table of Contents 1. Introduction 2. When a provider is deemed to accept Aetna Medicare Open Plan s terms and conditions 3. Provider
Medical and Rx Claims Procedures
 This section of the Stryker Benefits Summary describes the procedures for filing a claim for medical and prescription drug benefits and how to appeal denied claims. Medical and Rx Benefits In-Network Providers
This section of the Stryker Benefits Summary describes the procedures for filing a claim for medical and prescription drug benefits and how to appeal denied claims. Medical and Rx Benefits In-Network Providers
Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide for American Medical Security Life Insurance Company
 Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide for American Medical Security Life Insurance Company Insureds 2009 Contents How to contact us... 2 Our claims process...
Physician, Health Care Professional, Facility and Ancillary Provider Administrative Guide for American Medical Security Life Insurance Company Insureds 2009 Contents How to contact us... 2 Our claims process...
MyCare Ohio Assisted Living Provider Orientation & Training
 MyCare Ohio Assisted Living Provider Orientation & Training Opt IN Enrollees - Full duals with Buckeye Medicare and Medicaid benefits through Buckeye Medicare option to change plans monthly If member selects
MyCare Ohio Assisted Living Provider Orientation & Training Opt IN Enrollees - Full duals with Buckeye Medicare and Medicaid benefits through Buckeye Medicare option to change plans monthly If member selects
The Healthy Michigan Plan Handbook
 The Healthy Michigan Plan Handbook Introduction The Healthy Michigan Plan is a health care program through the Michigan Department of Community Health (MDCH). Eligibility for this program will be determined
The Healthy Michigan Plan Handbook Introduction The Healthy Michigan Plan is a health care program through the Michigan Department of Community Health (MDCH). Eligibility for this program will be determined
Handbook for Home Health Agencies
 Handbook for Home Health Agencies Chapter R-200 Policy and Procedures For Home Health Agencies Illinois Department of Public Aid CHAPTER R-200 Home Health Agency Services TABLE OF CONTENTS FOREWORD R-200
Handbook for Home Health Agencies Chapter R-200 Policy and Procedures For Home Health Agencies Illinois Department of Public Aid CHAPTER R-200 Home Health Agency Services TABLE OF CONTENTS FOREWORD R-200
New York. UnitedHealthcare Community Plan Claims System Migration Provider Quick Reference Guide. Complete Claims. Our Claims Process
 Our Claims Process Here are a few steps to ensure you receive prompt payment: 1 Review and copy both sides of the member s ID card. members receive an ID card containing information that helps you process
Our Claims Process Here are a few steps to ensure you receive prompt payment: 1 Review and copy both sides of the member s ID card. members receive an ID card containing information that helps you process
CHAPTER 7: UTILIZATION MANAGEMENT
 OVERVIEW The Plan s Utilization Management (UM) program is collaboration with providers to promote and document the appropriate use of health care resources. The program reflects the most current utilization
OVERVIEW The Plan s Utilization Management (UM) program is collaboration with providers to promote and document the appropriate use of health care resources. The program reflects the most current utilization
Your Medicare Health Benefits and Services and Prescription Drug Coverage as a Member of Molina Medicare Options Plus HMO SNP
 January 1 December 31, 2015 Evidence of Coverage: Your Medicare Health Benefits and Services and Prescription Drug Coverage as a Member of Molina Medicare Options Plus HMO SNP This booklet gives you the
January 1 December 31, 2015 Evidence of Coverage: Your Medicare Health Benefits and Services and Prescription Drug Coverage as a Member of Molina Medicare Options Plus HMO SNP This booklet gives you the
Medicare s 5-star rating system
 NOVEMBER 2012 Medicare s 5-star rating system Every year the Centers for Medicare & Medicaid Services (CMS) uses a star system to rate Medicare Advantage plans (with or without drug coverage) and Prescription
NOVEMBER 2012 Medicare s 5-star rating system Every year the Centers for Medicare & Medicaid Services (CMS) uses a star system to rate Medicare Advantage plans (with or without drug coverage) and Prescription
CLAIMS AND BILLING INSTRUCTIONAL MANUAL
 CLAIMS AND BILLING INSTRUCTIONAL MANUAL 2007 TABLE OF ONTENTS Paper Claims and Block Grant Submission Requirements... 3 State Requirements for Claims Turnaround Time... 12 Claims Appeal Process... 13 Third
CLAIMS AND BILLING INSTRUCTIONAL MANUAL 2007 TABLE OF ONTENTS Paper Claims and Block Grant Submission Requirements... 3 State Requirements for Claims Turnaround Time... 12 Claims Appeal Process... 13 Third
January 1, 2015 December 31, 2015 Summary of Benefits. Altius Advantra (HMO) H8649-003 80.06.361.1-UTWY A
 January, 205 December 3, 205 Summary of Benefits H8649-003 80.06.36.-UTWY A Y0022_205_H8649_003_UT_WYa Accepted /204 Summary of Benefits January, 205 December 3, 205 This booklet gives you a summary of
January, 205 December 3, 205 Summary of Benefits H8649-003 80.06.36.-UTWY A Y0022_205_H8649_003_UT_WYa Accepted /204 Summary of Benefits January, 205 December 3, 205 This booklet gives you a summary of
Commission on Minority Health
 MIH - Overview Commission on Minority Health More than 200 grants expected to be administered in FY - biennium Subsidies for Lupus Program remain steady at approximately $187,000 per year OVERVIEW The
MIH - Overview Commission on Minority Health More than 200 grants expected to be administered in FY - biennium Subsidies for Lupus Program remain steady at approximately $187,000 per year OVERVIEW The
How To Contact Us
 Molina Medicare Options Plus HMO SNP Member Services Method Member Services Contact Information CALL (800) 665-1029 Calls to this number are free. 7 days a week, 8 a.m. to 8 p.m., local time. Member Services
Molina Medicare Options Plus HMO SNP Member Services Method Member Services Contact Information CALL (800) 665-1029 Calls to this number are free. 7 days a week, 8 a.m. to 8 p.m., local time. Member Services
Ohio Occupational Therapy, Physical Therapy, and Athletic Trainers Board. Fiscal Year 2011 Annual Report
 Ohio Occupational Therapy, Physical Therapy, and Athletic Trainers Board Fiscal Year 2011 Annual Report Ohio Occupational Therapy, Physical Therapy, and Athletic Trainers Board 77 South High Street, 16
Ohio Occupational Therapy, Physical Therapy, and Athletic Trainers Board Fiscal Year 2011 Annual Report Ohio Occupational Therapy, Physical Therapy, and Athletic Trainers Board 77 South High Street, 16
A Regional Approach to Housing
 A Regional Approach to Housing Disability Housing Network Conference Presentation December 1, 2011 Goals for Today Define Regional Approach Review current regional approaches in Ohio Discuss efforts underway
A Regional Approach to Housing Disability Housing Network Conference Presentation December 1, 2011 Goals for Today Define Regional Approach Review current regional approaches in Ohio Discuss efforts underway
Molina Healthcare of Washington, Inc. Glossary GLOSSARY OF TERMS
 GLOSSARY OF TERMS Action The denial or limited Authorization of a requested service, including the type, level or provider of service; reduction, suspension, or termination of a previously authorized service;
GLOSSARY OF TERMS Action The denial or limited Authorization of a requested service, including the type, level or provider of service; reduction, suspension, or termination of a previously authorized service;
Workforce Analysis. Erie Lorain. Stark Richland. Coshocton Delaware. Muskingum Clark Madison. Noble Greene. Monroe Fayette.
 Workforce Analysis Williams Defiance Fulton Henry Putnam Lucas Wood Hancock Ottawa Sandusky Paulding Seneca Huron Medina Erie Lorain Cuyahoga Summit Lake Geauga Portage Ashtabula Trumbull Mahoning Van
Workforce Analysis Williams Defiance Fulton Henry Putnam Lucas Wood Hancock Ottawa Sandusky Paulding Seneca Huron Medina Erie Lorain Cuyahoga Summit Lake Geauga Portage Ashtabula Trumbull Mahoning Van
How To Manage Health Care Needs
 HEALTH MANAGEMENT CUP recognizes the importance of promoting effective health management and preventive care for conditions that are relevant to our populations, thereby improving health care outcomes.
HEALTH MANAGEMENT CUP recognizes the importance of promoting effective health management and preventive care for conditions that are relevant to our populations, thereby improving health care outcomes.
Choosing a Medicare Advantage plan you ll be confident in.
 Choosing a Medicare Advantage plan you ll be confident in. Indiana University Health Plans is a Medicare Advantage organization with a Medicare contract. Continued enrollment depends on the contract between
Choosing a Medicare Advantage plan you ll be confident in. Indiana University Health Plans is a Medicare Advantage organization with a Medicare contract. Continued enrollment depends on the contract between
Premera Blue Cross Medicare Advantage Provider Reference Manual
 Premera Blue Cross Medicare Advantage Provider Reference Manual Introduction to Premera Blue Cross Medicare Advantage Plans Premera Blue Cross offers Medicare Advantage (MA) plans in King, Pierce, Snohomish,
Premera Blue Cross Medicare Advantage Provider Reference Manual Introduction to Premera Blue Cross Medicare Advantage Plans Premera Blue Cross offers Medicare Advantage (MA) plans in King, Pierce, Snohomish,
Medicaid Substance Abuse Treatment Self-Referral Protocols Substance Abuse Improvement Initiative (SAII) January 1, 2010
 Medicaid Substance Abuse Treatment Self-Referral Protocols Substance Abuse Improvement Initiative (SAII) January 1, 2010 The Substance Abuse Improvement Initiative (SAII) allows Medicaid enrollees to select
Medicaid Substance Abuse Treatment Self-Referral Protocols Substance Abuse Improvement Initiative (SAII) January 1, 2010 The Substance Abuse Improvement Initiative (SAII) allows Medicaid enrollees to select
Quick Guide 2016. Peoples Health Choices 65 #14 (HMO) Jefferson, Orleans and Plaquemines parishes
 Quick Guide 2016 $0 mium* Plan Pre Peoples Health Choices 65 #14 (HMO) Jefferson, Orleans and Plaquemines parishes *You must continue to pay your Medicare Part B premium. H1961_PH16C65S1QG Accepted Thank
Quick Guide 2016 $0 mium* Plan Pre Peoples Health Choices 65 #14 (HMO) Jefferson, Orleans and Plaquemines parishes *You must continue to pay your Medicare Part B premium. H1961_PH16C65S1QG Accepted Thank
TIMEFRAME STANDARDS FOR UTILIZATION MANAGEMENT (UM) INITIAL DECISIONS
 ADMINISTRATIVE POLICY TIMEFRAME STANDARDS FOR UTILIZATION MANAGEMENT (UM) INITIAL DECISIONS Policy Number: ADMINISTRATIVE 088.15 T0 Effective Date: November 1, 2015 Table of Contents APPLICABLE LINES OF
ADMINISTRATIVE POLICY TIMEFRAME STANDARDS FOR UTILIZATION MANAGEMENT (UM) INITIAL DECISIONS Policy Number: ADMINISTRATIVE 088.15 T0 Effective Date: November 1, 2015 Table of Contents APPLICABLE LINES OF
NJ FamilyCare Expansion and Provider Enrollment FAQs
 NJ FamilyCare Expansion and Provider Enrollment FAQs Roxanne Kennedy MSW, LCSW Project Officer, Managed Behavioral Health Division of Medical Assistance and Health Service January 17, 2014 1 Expansion
NJ FamilyCare Expansion and Provider Enrollment FAQs Roxanne Kennedy MSW, LCSW Project Officer, Managed Behavioral Health Division of Medical Assistance and Health Service January 17, 2014 1 Expansion
Annual Notice of Changes for 2015
 Keystone 65 Select Medical-Only (HMO) offered by Independence Blue Cross Annual Notice of Changes for 2015 You are currently enrolled as a member of Keystone 65 Select Medical-Only. Next year, there will
Keystone 65 Select Medical-Only (HMO) offered by Independence Blue Cross Annual Notice of Changes for 2015 You are currently enrolled as a member of Keystone 65 Select Medical-Only. Next year, there will
Certain exceptions apply to Hospital Inpatient Confinement for childbirth as described below.
 Tennessee Applicable Policies PRECERTIFICATION Benefits payable for Hospital Inpatient Confinement Charges and confinement charges for services provided in an inpatient confinement facility will be reduced
Tennessee Applicable Policies PRECERTIFICATION Benefits payable for Hospital Inpatient Confinement Charges and confinement charges for services provided in an inpatient confinement facility will be reduced
State of Alabama Medicaid Agency
 Alabama Nursing Home Association (ANHA) Seminar SPONSORED BY: Senior Care Pharmacy & Gericare Medical Supply Playing by the Rules for the Medicaid Nursing Home Program and Conducting an Effective Medical
Alabama Nursing Home Association (ANHA) Seminar SPONSORED BY: Senior Care Pharmacy & Gericare Medical Supply Playing by the Rules for the Medicaid Nursing Home Program and Conducting an Effective Medical
