ARVO 2016 Annual Meeting Abstracts
|
|
|
- Moris Barnett
- 9 years ago
- Views:
Transcription
1 222 AMD Imaging 2 Monday, May 02, :30 AM 10:15 AM Exhibit/Poster Hall Poster Session Program #/Board # Range: /C0062 C0092 Organizing Section: Retina Program Number: 1606 Poster Board Number: C0062 Prevalence and natural course of refractile drusen in eyes with intermediate age-related macular degeneration Akio Oishi 1, Maho Oishi 1, Sarah Thiele 1, Jennifer Nadal 2, Monika Fleckenstein 1, Frank G. Holz 1, Steffen Schmitz-Valckenberg 1. 1 Department of Ophthalmology, University of Bonn, Bonn, Germany; 2 Institute for Medical Biometry, Informatics and Epidemiology, University of Bonn, Bonn, Germany. Purpose: Refractile drusen represent a phenotypic feature in various stages of age-related macular degeneration (AMD). Aim of this analysis was to evaluate prevalence, natural course, and clinical significance of refractile druse associated with intermediate AMD in a prospective, longitudinal natural history study. Methods: Ninety-eight eyes of 98 subjects (mean age 73.1 ± 7.1 years) with intermediate AMD were included. At baseline and at each year, multimodal retinal imaging including infrared reflectance (IR), blue reflectance (BR), fundus autofluorescence, and optical coherence tomography (OCT) over a review period of up to 4 years was performed. Refractile drusen were identified in color fundus photographs and longitudinal changes of individual lesions were analyzed in different imaging modalities. Incidence of late atrophic and neovascular AMD was compared between eyes with and without refractile drusen. Results: Twenty of 98 eyes had refractile drusen at baseline with a total lesion number of 115. Lesions were bilateral in 14 subjects. Refractile drusen showed a hyperreflective appearance on IR (80.9%) and BR (93.9%). Corresponding hyperreflective material at the level of Bruch s membrane by OCT was noted in 33 %. Longitudinal observations revealed both spontaneous regression of refractile drusen (n = 10) as well as progression to geographic atrophy (n = 30) or exudative changes (n = 25). If refractile drusen were present at baseline, the development of central GA was more frequently observed as compared to eyes with no refractile drusen at baseline (9/15 vs 6/57, excluding patients who dropped out). The presence of refractile drusen resulted in similar rates for the incidence of choroidal neovascularization (3/15 vs 16/57). Conclusions: The results indicate that refractile drusen in eyes with intermediate AMD may represent a predictive marker for the progression towards GA rather than CNV. Expanded future natural history as well as interventional studies should record the presence of refractile drusen for further validation of these initial observations. Commercial Relationships: Akio Oishi, Novartis (R), Bayer (R), Alcon Japan (F); Maho Oishi, None; Sarah Thiele; Jennifer Nadal, None; Monika Fleckenstein, Heidelberg Engineering (R), US A1 pending (P), Bayer (R), Genentech (F), Optos (F), Merz (C), Novartis (R), Carl Zeiss Meditec (F), Genentech (R), Heidelberg Engineering (F); Frank G. Holz, Heidelberg Engineering (C), Genentech (C), Bayer Healthcare (C), Novartis (C), Allergan (C), Roche (C), Alcon (C); Steffen Schmitz-Valckenberg, Formycon (F), Optos (F), Bayer (R), Heidelberg Engineering (R), Alcon/Novartis (C), Genentech/Roche (F), Carl Zeiss Meditec AG (F), Bayer (F), Heidelberg Engineering (F), Alcon/Novartis (F), Allergan (F) Support: German Ministry of Education and Research (BMBF) Program Number: 1607 Poster Board Number: C0063 Qualitative and Quantitative Assessment of Type 1 Neovascularization in OCT-Angiography Alexandra Miere 1, Eliana Costanzo 2, Giuseppe Querques 3, Vittorio Capuano 1, Eric H. Souied 1. 1 Ophthalmology, Centre Hospitalier Intercommunal de Creteil, Créteil, France; 2 Ophthalmology, Second University of Naples, Naples, Italy; 3 Ophthalmology, University Scientific Institute San Raffaele, Milan, Italy. Purpose: To characterize the features of type 1 choroidal neovascularization (CNV) in optical coherence tomography angiography (OCTA) and qualitatively and quantitatively compare them with findings in indocyanine green angiography (ICGA). Methods: Treatment-naïve and treated patients diagnosed type 1 CNV were included in our study. All patients underwent multimodal imaging by fluorescein angiography (FA), ICGA, spectral domain (SD)-OCT, and OCTA. Lesion area, as well as vessel density were measured on choriocapillaris segmentation of OCTA and on ICGA middle and late frames. Results: Twenty eyes of 18 patients (12 treatment-naïve and 8 treated eyes) with a mean age 80.4 ± 8.2 were included. The mean visual acuity was 20/32. OCTA revealed a high flow neovascular network in the choriocapillaris segmentation in all study eyes in all eyes. A distinctive feeder vessel was present in 11/20 eyes (central feeder vessel in 8/20 eyes and lateral feeder vessel in 3/20 eyes, while in 9/20 eyes a feeder vessel could not be detected. Lesion size in OCTA images had a mean area of 2.18 mm 2 (± 1.97) and a mean vessel area of 1.17 mm 2 (± 1.01), while in ICGA the mean lesion size was 3.52 mm 2 (± 4.28) in the middle phase and 3.88 mm 2 (± 4.64) in the late phase images. A statistically significant difference between lesion size in OCTA and ICGA was detected in 17/20 eyes (p<0.005). Conclusions: Our results suggest and support the hypothesis that OCTA could show the actual minimal surface of type 1 CNV, because, as a dyeless examination, it is not influenced by leakage. Moreover, as a depth-enhanced, highly reproducible technique, OCTA is suitable for type 1 CNV localization and follow up. Commercial Relationships: Alexandra Miere, None; Eliana Costanzo, None; Giuseppe Querques, None; Vittorio Capuano, None; Eric H. Souied, None Program Number: 1608 Poster Board Number: C0064 OCT-Angiography Assessment Of CNV Evolution In Treated Exudative AMD: An Analysis Based On Activity Criteria Marco Lupidi 1, 2, Florence Coscas 2, 3, Fiore Tito 1, Carlo Cagini 1, Gabriel J. Coscas 2, 3. 1 Department of Biomedical and Surgical Sciences, Section of Ophthalmology, University of Perugia, Perugia, Italy; 2 Centre Ophtalmologique De L Odeon, Paris, France; 3 Centre Hospitalier Intercommunal de Créteil, Creteil, France. Purpose: To describe and analyze optical coherence tomography angiography (OCT-A) findings, based on Activity Criteria, in treatment-naive exudative AMD (eamd) before and after VEGF-trap intravitreal injections. Methods: Prospective case series of 60 eyes of 60 consecutive treatment naïve eamd patients (36 females, mean age 74.4 ± 6.2 years) diagnosed with different types of CNV (41 type I, 2 type II, 9 mixed type I-II, 3 type III, 5 AMD-related polyps) and evaluated by conventional multimodal imaging andspectralis OCT-A (Heidelberg Engineering, Heidelberg, Germany). A micro-structural analysis, based on 5 Activity Criteria (shape, branching pattern, presence of anastomoses, vessel s termini and presence of perilesional halo) was performed to achieve the treatment-induced changes in choroidal neovascularization (CNV)
2 morphology. The CNV area and greatest linear dimension (GLD) were measured along with the variation in subretinal and/or intraretinal fluid. Results: After treatment the morphological analysis of the CNV features on OCT-A showed, in the largest part of the lesions, a reduction in the visibility of tiny branching vessels, mainly present at the periphery of the lesion, of the anastomoses and small peripheral arcades. Moreover 95% of patients with initial exudative reaction on OCT, showed a decrease in the amount of fluid. Fifty-three (53) out of 60 patients demonstrated decreases in CNV GLD and area with an average reduction of 13% and 24% respectively. There was high (p< 0.05) inter-observer agreement both for morphological and quantitative OCT-A imaging analysis. Conclusions: OCT-A is a useful technology for non-invasive monitoring of the exudative AMD because both functional (blood flow) and morphological (fluid accumulation) information is provided from a single scan. Such monitoring, based on Activity Criteria and quantitative findings, may help in the diagnosis of CNV, guiding decisions for treatment, as well as in monitoring the evolution of CNV and its response to treatment. Commercial Relationships: Marco Lupidi, None; Florence Coscas, None; Fiore Tito, None; Carlo Cagini, None; Gabriel J. Coscas Program Number: 1609 Poster Board Number: C0065 Masked Assessment of Widefield En Face Swept Source OCT Imaging Versus Color, Autofluorescence, and Infrared Fundus Imaging for the Diagnosis of Reticular Pseudodrusen Karen B. Schaal 1, Andrew D. Legarreta 1, William J. Feuer 2, Giovanni Gregori 1, Qianqian Cheng 1, John E. Legarreta 1, Paul F. Stetson 3, Sophie Kubach 3, Philip J. Rosenfeld 1. 1 Ophthalmic Research, Basom Palmer Eye Institute, Key Biscayne, FL; 2 Biostatistics, University of Miami, Miami, FL; 3 Carl Zeiss Meditec, Dublin, CA. Purpose: To compare 12X12mm widefield en face swept source optical coherence tomography (SS-OCT) imaging with conventional color, autofluorescence, and infrared imaging for the detection of reticular pseudodrusen (RPD) in eyes with dry age-related macular degeneration (AMD). Methods: Patients with dry AMD were prospectively enrolled in an OCT imaging study at the Bascom Palmer Eye Institute. On the same day, all patients underwent color fundus imaging, fundus autofluorescence imaging, infrared reflectance imaging, and imaging with a prototype Zeiss 100kHz SS-OCT instrument (Carl Zeiss Meditec Inc., Dublin, CA) with a central wavelength of 1050nm. Two masked graders assessed the presence, absence, or uncertainty of RPD on the conventional images and separately on four different SS-OCT en face images. The four OCT images were the OCT fundus image (OFI), a sub-rpe slab image, and two 20 µm thick outer retinal slabs positioned µm and µm above the RPE. The OCT fundus image (OFI) and sub-rpe slab image were used to assess the presence of geographic atrophy, the outer retinal slab images were used to assess the presence of subretinal drusenoid deposits. The grading results between conventional imaging and SS- OCT en face imaging were compared, and questionable RPD cases were defined as absent RPD to simplify analysis. Since RPD could be detected using both imaging modalities, it was decided that the gold standard for the presence of RPD grading would be a positive reading with either SS-OCT or conventional imaging. Results: A total of 307 eyes (209 patients) were graded for the presence or absence of RPD based on SS-OCT and conventional imaging. The agreement between SS-OCT and multimodal imaging was 83%. The difference in RPD detection with either image modality was not statistically significant (p=0.21). The sensitivity of SS-OCT in RPD detection was 83%, and when using conventional imaging, the sensitivity was 75%. When using SS-OCT imaging alone, 10% of RPD cases would be missed, and when using conventional imaging alone, 14% or RPD cases would be missed. Conclusions: All four imaging modalities used together provided the best strategy for the detection of RPD. However, when using widefield en face SS-OCT slab imaging alone, the detection of RPD was at least as good as conventional imaging. Commercial Relationships: Karen B. Schaal, None; Andrew D. Legarreta, None; William J. Feuer, None; Giovanni Gregori, Carl Zeiss Meditec (P); Qianqian Cheng, None; John E. Legarreta, None; Paul F. Stetson, Carl Zeiss Meditec; Sophie Kubach; Philip J. Rosenfeld, Carl Zeiss Meditec (F), Carl Zeiss Meditec (R) Program Number: 1610 Poster Board Number: C0066 Choroidal and Outer Retinal OCT Features Preceding Development of Geographic Atrophy Eduardo A. Novais 1, 2, Ricardo N. Louzada 3, 2, Rachel E. Silver 5, Emily Cole 2, Giliann K. Collins 5, Eric M. Moult 4, Erin Wagner 5, Jay S. Duker 2, Daniela Ferrara 2, Johanna M. Seddon 5, 2. 1 Ophthalmology, Federal University of São Paulo (UNIFESP), São Paulo, Brazil; 2 Ophthalmology, New England Eye Center - Tufts University School of Medicine, Boston, MA; 3 Ophthalmology, Federal University of Goiás, Goiânia, Brazil; 4 MIT, Cambridge, MA; 5 Ophthalmic Epidemiology and Genetics Service, New England Eye Center - Tufts Medical Center, Boston, MA. Purpose: To evaluate parameters based on optical coherence tomography (OCT) that may be predictive of progression to geographic atrophy (GA) secondary to age-related macular degeneration (AMD). Methods: Retrospective review of SD-OCT imaging was conducted among subjects enrolled in ongoing studies of AMD. OCTs for subjects who progressed from intermediate AMD to GA (mean follow up: 2.8 years) after the baseline image (n=10), and agematched subjects with no AMD (n=10) were assessed. One eye per subject was evaluated: the eye that progressed to GA, and the eye with the highest quality images for controls. OCT images at baseline, annually, and last exam prior to GA development were systematically evaluated to identify potential prognostic factors in the vitreo-retinal interface, retina, and choroid. An algorithm assessing the light-todark ratio (LDR) between choroidal stromal area and choroidal vessel lumen was calculated. OCT parameters for progressors and controls were compared using Fisher s Exact and Welch s t-test. Associations between OCT parameters and the LDR were also assessed. Results: Among the choroidal features, irregularities in the choroidal vessels (thickening or thinning) were associated with progression to GA (P=0.02). Average sub-foveal choroidal thickness tended to be thinner in progressors compared to controls (188.4 μm vs μm, P=0.06). Choriocapillaris irregularity was significantly associated with the LDR (P=0.03). There was no difference in LDR between groups, suggesting that choroidal thinning associated with advanced AMD evolved with a preserved ratio between vessel lumen and choroidal stroma. Abnormal or disrupted outer neurosensory retinal parameters prior to signs of GA were noted for several features (P<0.0001): retinal thickness, external limiting membrane, ellipsoid zone, photoreceptor outer segments, and interdigitation zone. Conclusions: This systematic analysis revealed that the outer retina was markedly affected prior to onset of GA. Additional abnormalities in outer neurosensory retina and retinal pigment epithelium also
3 precede GA. Although there was a trend toward choroidal thinning, there was no difference in LDR. Female, age 65. A) baseline fundus; B) follow-up at 3 years with GA (dashed line); C) baseline OCT with subsidence of outer plexiform layer (yellow arrow); D) baseline LDR; E) follow-up OCT at 3 years with GA overlying the site of the large vessels (white arrows) Commercial Relationships: Eduardo A. Novais, None; Ricardo N. Louzada, None; Rachel E. Silver, None; Emily Cole, None; Giliann K. Collins; Eric M. Moult, None; Erin Wagner, None; Jay S. Duker, Allergan (C), Carl Zeiss Meditec (C), Eleven Biotherapeutics (S), Omeros (C), Topcon Medical Systems Inc. (C), OptoVue (C), CoDa Therapeutics (C), Alcon/Novartis (C), Lumenis (C); Daniela Ferrara, Genentech; Johanna M. Seddon, None Support: The Massachusetts Lions Eye Research Fund; Research to Prevent Blindness; and the Age-Related Macular Degeneration Research Fund, Ophthalmic Epidemiology and Genetics Service, Tufts Medical Center, Tufts University School of Medicine, Boston, MA. Program Number: 1611 Poster Board Number: C0067 Evaluation of automated drusen detection system for fundus photographs of patients with age-related macular degeneration Katia Delalibera Pacheco 1, 2, Yulia Wolfson 1, Philippe Burlina 1, 3, David E. Freund 3, Albert Feeny 3, Neil Joshi 3, Neil M. Bressler 1. 1 Retina Division, Wilmer Eye Institute, Johns Hopkins University School of Medicine, Baltimore, MD; 2 Retina Division, Brazilian Center of Vision, Brasilia, Brazil; 3 Applied Physics Laboratory, The Johns Hopkins University, Laurel, MD. Purpose: Evaluate an automated grading system for classifying agerelated macular degeneration (AMD) severity from fundus photos using a novel method developed at Johns Hopkins compared with human graders. Methods: Retinal images were analyzed to try to improve detection of people with earlier stages of AMD among individuals over age 50 who should be referred to eye care providers to monitor for onset of choroidal neovascularization (CNV). Using already digitized and de-identified images from the National Institutes of Health (NIH) database of fundus images from the Age-Related Eye Disease Study (AREDS) dbgap dataset, including images graded using 4 categories of: (1) no AMD, (2) early, (3) intermediate, or (4) advanced stage of AMD, per AREDS stages. In addition, differences between two operators grading and differences between manual grading (operator) and automated grading (machine) for the same set of images were compared. A two class problem was used; class 1 (AMD category 1 or 2) vs. class 2 (AMD category 3 or 4). Two independent graders reviewed and classified all images into these specific categories. Paired gradings were compared and percentage agreement using kappa statistics were calculated. Results: A subset of 917 images were evaluated. Agreement was almost perfect when comparing the first grader and AREDS (kappa = 0.87). For the second grader and AREDS, agreement was substantial (kappa = 0.74). When comparing machine versus AREDS, agreement was almost perfect (kappa = 0.85) and between the two graders it was substantial (kappa = 0.71). Conclusions: This study demonstrates the feasibility of humanmachine-based classification for automated AMD severity grading. Using one large public retinal image database, highly reproducible results were obtained when comparing manual and automated grading of severity of detected AMD. These techniques have the potential to provide individuals with automated grading of fundi to identify AMD or monitor those individuals with earlier stages of AMD for the onset of the more advanced stages when prompt treatment may be indicated to reduce the risk of blindness. Commercial Relationships: Katia Delalibera Pacheco, None; Yulia Wolfson, None; Philippe Burlina; David E. Freund, None; Albert Feeny, None; Neil Joshi, None; Neil M. Bressler, Novartis (F), Regeneron (F), Genentech/Roche (F), Bayer (F) Support: NIH Grant (R21 EY A1) and Johns Hopkins University Retina Division Research Grant Program Number: 1612 Poster Board Number: C0068 Changes in Clinical Appearance and Fundus Autofluorescence Associated with Drusen Regression in Intermediate Age-Related Macular Degeneration Aman Sharma, Sarah B. Sunshine, Alanna Tisdale, Emily Y. Chew, Wai T. Wong. National Eye Institute, National Institutes of Health, Bethesda, MD. Purpose: To assess short- and long-term clinical changes associated with drusen regression in eyes with intermediate age-related macular degeneration (AMD). Methods: Sixty participants aged 50 years and older with AMD in the Age-Related Eye Disease Study 2 (AREDS2) were evaluated for one or more areas of drusen regression > circle C1 in area from baseline to year 2. These eyes had been imaged with color fundus photography (CFP) and with modified fundus camera-based (mfc) in fundus autofluorescence (FAF) imaging at baseline, year two, and year five. Areas of drusen regression were graded on color fundus photographs, using AREDS grading protocol, and FAF images. Results: Forty-five eyes in 60 participants demonstrated drusen regression meeting criteria from baseline to year 2. One eye progressed to neovascular AMD and was excluded from analysis. In the remaining 44 eyes, areas of drusen regression on CFP at year 2 demonstrated no clinical abnormalities in 26/44 eyes (59%), developed new pigmentary changes in 15/44 eyes (34%), and developed new areas of atrophy in 3/44 eyes (7%). Drusen regression areas at year 2 were however associated with more prevalent local changes in FAF in 31/44 eyes (70%) (56% demonstrating decreased FAF, and 14% demonstrating increased FAF). At year 5, areas of drusen regression on CFP demonstrated clinical changes in 30/44 eyes (68%) with15/44 eyes (34%) demonstrating new pigmentary changes and 15/44 eyes (34%) demonstrating new atrophy from baseline. Drusen regression areas at year 5 were associated with local changes in FAF in 38/44 eyes (86%) (70% demonstrating increased FAF, and 16% demonstrating decreased FAF).
4 Conclusions: Drusen regression in intermediate AMD in the early phase (2 years) is associated with local changes in FAF patterns with relatively less prevalent changes in local clinical appearance. In the later phase (5 years), these areas progress to more pronounced changes in FAF and clinical appearance that reflect RPE disorganization and atrophy. These short and longer-term observations associate drusen regression with progressive stages of RPE change and degeneration in the context of intermediate AMD Commercial Relationships: Aman Sharma, None; Sarah B. Sunshine, None; Alanna Tisdale, None; Emily Y. Chew, None; Wai T. Wong, None Support: NEI Intramural Research Program Program Number: 1612a Poster Board Number: C0068a An Improved Method for Measuring Geographic Atrophy (GA) in patients with Age-related Macular Degeneration (AMD) Sarah B. Sunshine, Elvira Agron, Juliet Hartford, Frederick Ferris, Emily Y. Chew. National Eye Institute, National Institute of Health, Baltimore, MD. Purpose: Recent studies have utilized fundus auto-fluorescence (FAF) and color photography (CF) imaging to monitor progression of GA as an outcome variable. Grading of GA area has been done manually and using semi-automated techniques. However, these methods have led to difficulties with reproducibility and within person variance. Reduction in the variance in GA area measurements in clinical trials would increase power to assess treatment effects for AMD. Methods: One approach to minimizing the within person variance in estimating growth rates of GA is taking into account all possible information available at the time of estimating GA area. This includes simultaneous use of FAF and CF information for grading GA area at each time point. In addition, the grader can look at previous images and future images to make the best possible estimate of where the GA border is at each study visit. Notwithstanding the potential for bias, graders make the assumption that GA did not spontaneously resolve. Registering the images leads to concentrically expanding rings to depict the progression of GA over time, allowing for both estimates of GA area over time and estimates of growth rates along specific merridians. This approach has been applied to images obtained from study participants with GA and at least 4 years follow-up at two AREDS2 clincs. To date, 48 eyes (27 participants) with 4-8 years of imaging have been preliminarily evaluated using this methodology. Results: Sequential GA areas were obtained from baseline and annual imaging (FAF, CF). GA area was calculated from the grading of the images using side-by-side FAF and CF images and comparison with previous and follow-up images. The slope of the growth rate was calculated using regression analysis of the square root of the area over time (mm growth per year). Variance of the growth rate was calculated using this informed sequential grading process and was directly compared with independent single image grading over time. Preliminary analysis suggests an important reduction in within person variance. Conclusions: Using all information available on sequential visits appears to reduce the within person variance of GA growth rates. This approach will allow us to further elucidate the natural history of AMD and will allow clinical trials to more successfully characterize the effect of GA treatments. Commercial Relationships: Sarah B. Sunshine, None; Elvira Agron, None; Juliet Hartford, None; Frederick Ferris, None; Emily Y. Chew, None Program Number: 1613 Poster Board Number: C0069 The perimeter as predictor for the progression of geographic atrophy (GA) secondary to age-related macular degeneration (AMD) Maximilian Pfau 1, Moritz Lindner 1, Lukas Goerdt 1, Steffen Schmitz-Valckenberg 1, Srinivas R. Sadda 2, 3, Frank G. Holz 1, Monika Fleckenstein 1. 1 Department of Ophthalmology, University of Bonn, Bonn, Germany; 2 Doheny Eye Institute, UCLA, Los Angeles, CA; 3 Jules Stein Eye Institute, UCLA, Los Angeles, CA. Purpose: Natural history studies in geographic atrophy (GA) secondary to AMD show a high variability in rates of lesion progression over time. Previously identified prognostic markers include size of baseline GA, lesion circularity and FAF patterns. The aim of the current study was to evaluate the perimeter of the GA area at baseline as a prognostic marker for atrophy enlargement rates in a longitudinal natural history study. Methods: A total of 50 eyes of 42 patients (mean age 74.21±6.69) participating in the prospective natural history FAM- ( Fundus Autofluorescence imaging in Age-related Macular Degeneration, NCT ) and DSGA- ( Directional Spread in Geographic Atrophy, NCT ) studies were included in the analysis. Quantification of atrophy was performed based on fundus autofluorescence imaging and using the RegionFinder software (Heidelberg Engineering, Germany). The graded annotated images were transferred to ImageJ (Bethesda, Maryland, USA) to measure the area, circularity and perimeter of the lesions. Scaling-factors for the pixel-to-µm conversion were obtained from the HEYEX software (Heidelberg Engineering, Germany). Results: The area of atrophy was positively correlated to the area of upcoming expansion of the lesion (Spearman s rho 0.228, p=0.006). A higher correlation was observed between the area of upcoming expansion and the circularity (Spearman s rho , p<0.001) and the perimeter (Spearman s rho 0.456, p<0.001), respectively. Further analysis revealed that a decrease in circularity (during the previous interval) was followed by an increase of enlargement rate in the subsequent interval (p<0.05, Pearson s chi-squared test χ2). The circularity of atrophy was significantly decreased in eyes exhibiting the diffuse-trickling (DT) phenotype (0.117±0.118) compared to eyes exhibiting other phenotypes (0.344±0.229, p<0.001, Wilcoxon signed rank test). Eyes with the DT-phenotype exhibited a significantly faster enlargement rate than eyes with other FAF-phenotypes (2.98±0.86mm 2 versus 0.89±1.31mm 2, p<0.001). Conclusions: GA progression rates are correlated with the area, perimeter and circularity of the lesion. The findings indicate that spread of GA may be associated with the extent of damaged adjacent retinal pigment epithelium cells. Commercial Relationships: Maximilian Pfau; Moritz Lindner, Carl Zeiss Meditec (F), Carl Zeiss Meditec (I), Heidelberg Engineering (F), Optos (F), Alimera Sciences (R), Heidelberg Engineering (R), Genentech (F); Lukas Goerdt, Heidelberg Engineering (F), Carl Zeiss Meditec (F), Optos (F); Steffen Schmitz- Valckenberg, Heidelberg Engineering (R), Bayer HealthCare (F), Formycon (F), Optos (F), Allergan (F), Alcon/Novartis (F), Carl Zeiss Meditec (F), Heidelberg Engineering (F), Bayer HealthCare (R), Genentech/Roche (F), Alcon/Novartis (C); Srinivas R. Sadda, Optos (C), Allergan (C), Avalanche (C), Genetech (F), Stem Cells Inc. (C), Genetech (C), Optos (F), Iconic (C), Novartis (C), Thrombogenics (C), Regeneron (C), Bayer HealthCare (C), Allergan (F), Carl Zeiss Meditec (F); Frank G. Holz, Novartis (C), Bayer HealthCare (C), Merz (C), Roche (C), Allergan (F), Heidelberg Engineering (C), Novartis (F), Alcon (F), Alcon (C), Heidelberg Engineering (F), Carl Zeiss Meditec (F), Boehringer Ingelheim (C), Genentech (F), Bayer
5 ARVO 2016 Annual Meeting Abstracts HealthCare (F), Allergan (C), Heidelberg Engineering (R), Acucela (F), Optos (F), Acucela (C), Genentech (C); Monika Fleckenstein, Optos (F), Genentech (F), Heidelberg Engineering (R), Bayer HealthCare (R), Genentech (R), Carl Zeiss Meditec (F), Heidelberg Engineering (F), US (P), Merz (C), Novartis (R) Support: DFG Priority Program AMD Clinical Trial: NCT Program Number: 1614 Poster Board Number: C0070 OCTA detects flow alterations in the choriocapillaris underlying drusen in non-exudative age-related macular degeneration without geographic atrophy Eric M. Moult1, 2, Nadia K. Waheed3, Eduardo A. Novais4, 3, WooJhon Choi1, ByungKun Lee1, Emily Cole3, Chen D. Lu1, Philip J. Rosenfeld5, Jay S. Duker3, James G. Fujimoto1. 1Electrical Engineering and Computer Science, MIT, Cambridge, MA; 2 Health Sciences and Technology, Harvard-MIT, Cambridge, MA; 3 Ophthalmology, New England Eye Center - Tufts University School of Medicine, Boston, MA; 4Ophthalmology, Federal University of São Paulo / UNIFESPP, Rio de Janeiro, Brazil; 5Ophthalmology, Bascom Palmer Eye Institute - University of Miami Miller School of Medicine, Miami, FL. Purpose: The purpose of this study is to use en face optical coherence tomography angiography (OCTA) to investigate the flow characteristics of the choriocapillaris (CC) underlying drusen and to correlate these flow alterations with structural alterations of the retinal pigment epithelium (RPE) in patients with non-exudative age-related macular degeneration (AMD) without geographic atrophy (GA). Methods: OCTA imaging was performed using a 1050nm, 400kHz swept-source (SS)-OCT system in 35 eyes of 26 patients with nonexudative AMD without GA (77.5±9.0 years; 11 males; 15 females). CC flow alteration maps were constructed by binarizing en face OCTA CC slabs. Structural RPE alteration maps were constructed by binarizing sub-rpe slab projections. The spatial relationships between CC flow alterations and RPE alterations were then evaluated by overlaying these two alteration maps. Results: Figure 1 shows representative data suggesting a spatial relationship between RPE alterations and CC flow alterations. Some, but not all, drusen are associated with CC flow alteration. Conclusions: A combination of en face slab OCT structural maps and OCTA flow maps were used to associate structural alterations of the RPE to flow alterations of the CC. These observations confirm the mutualistic relationship between the RPE and the CC. Continuing work will investigate methods to quantitate these associations. Images from a 78 y/o Caucasian female with non-exudative AMD. (A) Color fundus photo showing large drusen associated with pigmentary changes. (B) Late stage FA showing hyperfluorescence due to drusen staining. (C) Red free photo showing drusen hypereflectivity; purple box indicates the 3mm x 3mm OCT field. (D) Enlargement of (C) corresponding to the OCT field. (E) OCTA projection of retinal vasculature. (F) OCT B-scan taken from the blue line in (E), showing a drusenoid pigment epithelial detachment; yellow-green lines demarcate the sub-rpe slab, shown in (H); yellow-orange lines demarcate intensity CC slab, shown in (I). (G) Unthresholded OCTA B-scan; yellow-orange lines, matching those in (F), demarcate the OCTA CC slab shown in (J). (K) Binarized subrpe slab; white indicates increased light penetration. (L) Binarized CC slab; black indicates CC alteration. (M) Semi-transparent overlay of (K) onto (L); red indicates increased light penetration. Scale bars: 1mm. Commercial Relationships: Eric M. Moult, None; Nadia K. Waheed, Iconic Therapeutics (C), Carl Zeiss Meditec Inc. (R), Optovue Inc. (R), ThromboGenics (C); Eduardo A. Novais, None; WooJhon Choi, None; ByungKun Lee, None; Emily Cole, None; Chen D. Lu, None; Philip J. Rosenfeld, Carl Zeiss Meditec Inc. (F); Jay S. Duker, Carl Zeiss Meditec Inc. (F), Optovue Inc. (F), Carl Zeiss Meditec Inc. (C), Optovue Inc. (C); James G. Fujimoto, Optovue Inc. (P), Carl Zeiss Meditec Inc. (P), Optovue Inc. (I) Support: R01-EY A, R44-EY02286, R01CA , FA , FA to access the versions of record.
6 ARVO 2016 Annual Meeting Abstracts Program Number: 1615 Poster Board Number: C0071 Monitoring treatment of retinal angiomatous proliferation by phase resolved Doppler OCT Mirjam E. Van Velthoven1, Jan H. de Jong1, Boy Braaf2, Maximilian Gräfe2, Sankha Amarakoon1, Koenraad A. Vermeer1, Suzanne Yzer1, Tom Missotten1, Johannes F. De Boer2. 1 Ophthalmology, Rotterdam Eye Hospital, Rotterdam, Netherlands; 2 VU University, Amsterdam, Netherlands. Purpose: In contrast to most conventional imaging techniques, Doppler OCT is able to provide depth-resolved information about intra- and transretinal blood flow non-invasively. We performed an exploratory prospective, observational cohort study to evaluate Doppler OCT for monitoring the effect of treatment in patients with retinal angiomatous proliferation (type 3 CNV). Methods: Twelve treatment-naïve patients were included, with a median age of 79 years (range 65-90). They were diagnosed with type 3 CNV based on fundus examination, fluorescein angiography and indocyanine-green angiography. Patients were additionally imaged with an experimental 1040 nm swept-source phase resolved Doppler OCT instrument before and after treatment. Patients were treated with either intravitreal bevacizumab or triamcinolone injection(s) with or without photodynamic therapy (PDT). Abnormal blood flow after treatment was defined as unchanged, decreased or absent. Results: Good quality Doppler OCT images before and after treatment could be obtained in 9 patients. After the first treatment series the type 3 CNV lesion was absent in 7 patients, in 1 patient the Doppler OCT depicted decreased flow in the lesion and 1 patient showed unchanged abnormal blood flow. Only in 1 out of 4 patients complete resolution was seen after a single bevacizumab injection. Combined therapy of bevacizumab with PDT showed complete resolution in 5 out of 5 patients (see figure). Conclusions: Doppler OCT is able to detect changes in abnormal blood flow after treatment of type 3 CNV. This type of imaging may become an important non-invasive monitoring tool for optimizing treatment strategies in type 3 CNV patients and possibly in other types of macular degeneration. Doppler en face (left) and tomogram (right) of abnormal intraretinal blood flow continuous to the sub-retinal pigment epithelial (RPE) region at the top of a pigment epithelial detachment (PED). The tomogram position is indicated by a red dotted line in the en face image (left). The Doppler flow information is superimposed in red over the grayscale structural OCT tomogram (right). Top: baseline. Middle: persisting abnormal flow after a single bevacizumab injection. Bottom: Resolution of abnormal flow after additional PDT treatment. The consecutive en face Doppler images (left) show gradual disappearance of the abnormal vascular network. Commercial Relationships: Mirjam E. Van Velthoven, Novartis Netherlands (R), Allergan Europe (R); Jan H. de Jong, None; Boy Braaf, None; Maximilian Gräfe, None; Sankha Amarakoon, None; Koenraad A. Vermeer, None; suzanne yzer, None; Tom Missotten, None; Johannes F. De Boer, Massachusetts General Hospital (P), Heidelberg Engineering (F) Program Number: 1616 Poster Board Number: C0072 Automatic versus manual segmentation of choroidal neovascularization lesions using optical coherence tomography Ruhella R. Hossain, Aishath R. Moosa, Nishal Patel. Ophthalmology, East Kent Hospitals University NHS Foundation Trust, London, United Kingdom. Purpose: Although fluorescein angiography is the current gold standard for diagnosing choroidal neovascularization (CNV), optical coherence tomography (OCT) segmentation software can identify the boundaries of the retinal pigment epithelium (RPE) changes and calculate the size of the CNV lesion. We hypothesize that 1) using surface area and volume as biomarkers for CNV lesions, OCT automatic segmentation is less accurate than manual segmentation both at diagnosis and after the third anti-vegf, Lucentis, injection; and 2) OCT automatic segmentation is an accurate diagnostic tool for measuring CNV lesions. to access the versions of record.
7 Methods: Retrospective study of 10 macular degeneration patients diagnosed with CNV. Blinded observers, trained to detect RPE changes, manually delineated boundaries of CNV lesions using SDOCT (Topcon 2000) with drusen analysis before and after Lucentis injections. Caliber measurements were compared to automatic segmentation values. Statistical analysis was performed, taking into account inter-observer variability. Results: Automatic and manual segmentation measurements are similar in 1) retinal area and fovea center values both pre-and postinjection; and 2) retinal volume post-injection. Retinal volume preinjection was 1) similar between the two blinded observers; 2) varied between automatic measurements and observers in some patients; 3) underestimated for all patients in the automatic measurements. Overall, automatic segmentation detects a general reduction in CNV lesion size. Conclusions: OCT software detects CNV lesions and reports size reduction after the third Lucentis injection. OCT automatic segmentation using Topcon drusen analysis in this small cohort is an accurate diagnostic tool to measure CNV surface area and volume. OCT automatic segmentation versus manual segmentation of two blinded observers. Pre-injection measurements of A) Retinal area, B) Retinal volume, C) Centre of fovea. Post-injection measurements of D) Retinal area, E) Retinal volume, F) Centre of fovea. Commercial Relationships: Ruhella R. Hossain, None; Aishath R. Moosa, None; Nishal Patel, None Program Number: 1617 Poster Board Number: C0073 Influence of disease duration on choroidal neovascularization (CNV) microstructures in eyes with age-related macular degeneration (AMD) as assessed by optical coherence tomography angiography (OCTA) Reinhard Told, Andreas Pollreisz, Florian Sulzbacher, Stefan Sacu, Ursula Schmidt-Erfurth. Department of Ophthalmology, Medical University of Vienna, Vienna, Austria. Purpose: To compare AMD-CNV microstructures in untreated and treated eyes based on OCTA with disease duration. Methods: A total of 85 eyes of 85 consecutive patients with untreated or treated neovascular AMD (namd) (20 treatment naïve eyes, 65 eyes with previous anti-vegf treatment) were examined using the AngioVue OCTA system (Optovue, Fremont, CA) and evaluated based on CNV morphology by two independent graders. CNV was classified according to the following patterns: dense net (DN); vascular loop (VL); mixed (DN+VL). Further, CNV lesions were subcategorized based on vessel characteristics: branches with tiny capillaries; branches with single rare large vessels; anastomosis/ loops; peripheral arcade. Based on namd onset, patients were grouped into 4 cohorts: Group A (no history of previous namd); Group B (diagnosis within last 2 years); Group C (2-4 years); Group D (4-9 years). Results: In 10 (50%) treatment naïve and 40 (61%) previously treated eyes, CNV lesions were identified on OCTA. Groups A, B, C and D consisted of 20, 25, 25 and 15 eyes, respectively. The mean number of injections in groups B, C and D was 4.8±3.44, 14.6±8.83 and 23.8±7.5 (mean ± SD), respectively. Regarding main CNV types, DN could be observed in 21.1% of eyes in group A; 16% (C); 13.3% (D) and 8.3% (B); VL was most frequently present in group D (60%), followed by C (48%), A (21.1%) and B (12.5%). Mixed patterns were found in 16.7% of eyes in group B; 12% in C; 10.5% in A and 6.7% in D. The largest number of eyes with absent CNV lesions on OCTA was found in group B (62.5%), followed by A (47.4%), D (33.3%) and C (24%). Grading of subcategories revealed that group A contained the most tiny capillary branches (31.6%), while the majority of branches with single rare large vessels was found in groups C (66.7%) and D (60%). Anastomosis/loops were most often observed in groups D (53%) and C (48%). In 21.1% of eyes in group A, 13.3% in D and 8% in C peripheral arcades were identified, while none were observed in eyes of group B. Conclusions: In eyes with newly diagnosed namd, OCTA revealed specific microstructural CNV characteristics such as DN and branches with tiny capillaries. With disease duration and injection frequency vascular loop patterns and the presence of anastomosis/ loops within the CNV lesion increased. Commercial Relationships: Reinhard Told, None; Andreas Pollreisz, None; Florian Sulzbacher, None; Stefan Sacu, None; Ursula Schmidt-Erfurth, Boehringer (C), Bayer Healthcare (C), Alcon Lab. Inc. (C), Novartis (C) Clinical Trial: NCT Program Number: 1618 Poster Board Number: C0074 Histologically guided metrics for semi-automated analysis of fundus autofluorescence (FAF) in aging and age-related macular degeneration (AMD) Kenneth R. Sloan 1, 2, Anna V. Zarubina 2, Carrie Huisingh 2, Fazila Aseem 2, 3, Mark Clark 2, Gerald McGwin 2, 4, Yuhua Zhang 2, 5, Cynthia Owsley 2, Christine A. Curcio 2. 1 Department of Computer and Information Sciences, University of Alabama at Birmingham, Birmingham, AL; 2 Department of Ophthalmology, University of Alabama at Birmingham, Birmingham, AL; 3 School of Medicine, Wake Forest University, Winston-Salem, NC; 4 Department of Epidemiology, University of Alabama at Birmingham, Birmingham, AL; 5 Department of Biomedical Engineering, University of Alamaba at Birmingham, Birmingham, AL. Purpose: The retinal pigment epithelium (RPE) is the major signal source for blue FAF. New histology of human RPE in AMD revealed variable cell morphologies, layer thickening, and re-distribution and loss of AF granules [1-4]. Guided by these findings, we tested whether automated analysis of FAF intensity variation could elucidate RPE health in aging and early AMD. Methods: The Alabama Study of Early Age-Related Macular Degeneration prospectively tested functional biomarkers of incident AMD at 3 years [5]. Participants (n=544; 410 normal, 134 AMD, via AREDS 9-step scale) underwent multimodal imaging with FAF using a Spectralis without an internal AF reference [6]. In baseline and follow-up images, the vasculature and optic nerve head were masked
8 semi-automatically to reduce variability from non-af structures. In masked images, we computed standard deviation/ mean intensity (coefficient of variation, CV), previously used for Stargardt disease [7], within the ETDRS grid and sectors (central subfield, C1; inner ring, R3; outer ring; R6). Associations with age and AMD severity were examined by Spearman correlation coefficients (SCC). Changes in FAF metrics between baseline and follow-up were checked with general linear models. Results: Table 1 shows that at baseline, CV was positively and significantly associated with age in C1, R6, and the whole grid. There was a nominal association of CV with age in R3. CV was positively and significantly associated with AREDS grade in C1, R3, and the whole grid. Table 2 shows that at 3 years, CV increased significantly with time for the entire cohort, for the ETDRS grid and all sectors. Conclusions: In initial analyses of one histologically informed metric, we find that CV of FAF intensity in ETDRS sectors exhibits biologically plausible features suggestive of strong internal validity. These features include positive associations at baseline with age and AREDS grade, in a regionally specific manner (i.e., central 3 mm where Bruch s membrane lipids are prominent), and an overall increase, although small, over time. Other metrics are also under consideration. 1. Rudolf. Ophthalmology. 2013;120: Ach. IOVS. 2014;55: Ach. IOVS. 2015;56: Zanzottera. IOVS. 2015;56: Owsley. Ophthalmology. 2015; Delori. IOVS. 2011;52: Cideciyan. Hum Mol Genet. 2004;13:525. Commercial Relationships: Kenneth R. Sloan, Spouse - Novartis (C), Spouse - Janssen Cell Therapy (C), Spouse - Merck (C), Spouse - Genentech (C); Anna V. Zarubina, None; Carrie Huisingh, None; Fazila Aseem, None; Mark Clark, None; Gerald McGwin, None; Yuhua Zhang, None; Cynthia Owsley; Christine A. Curcio, Novartis (C), Merck (C), Genentech (C), Janssen Cell Therapy (C) Support: NIA R01AG04212; EyeSight Foundation of Alabama; Research to Prevent Blindness; NEI EY06109; R01EY Program Number: 1619 Poster Board Number: C0075 Accuracy, repeatability and reproducibility of a novel approach to quantify individual drusen in spectral-domain optical coherence tomography images Luis De Sisternes 1, Gowtham Jonna 2, Margaret Greven 4, Theodore Leng 4, Daniel Rubin 1, 3. 1 Radiology, Stanford University, Stanford, CA; 2 Ophthalmology, Albert Einstein College of Medicine, Bronx, NY; 3 Medicine (Biomedical Informatics Research), Stanford University, Stanford, CA; 4 Ophthalmology, Stanford University School of Medicine, Palo Alto, CA. Purpose: Drusen features in Spectral-Domain Optical Coherence Tomography (SD-OCT) have shown utility as biomarkers of age-related macular degeneration (AMD). We introduce a novel automated method to segment and quantify individual drusen in SD-OCT images, and evaluate the accuracy, repeatability and reproducibility of its measurements. Methods: Our method uses a smooth interpolation of the Retinal Pigment Epithelium (RPE) outer boundary to identify regions of substantial lifting in the inner RPE and inner-segment boundaries. Individual drusen are then differentiated by a Watershed transform and morphological refinements in the obtained lift map. Drusen properties are measured automatically from the segmentation results: number, area, volume, extent, slope, height, density and intensity within drusen. We evaluated our approach in 192 early and intermediate AMD eyes from 129 patients, analyzing segmentation accuracy by measuring overlap ratio (OR) with manual markings, and measurement repeatability and reproducibility by computing their mean percentage difference (PD) in repeated scan pairs, acquired twice using 200x200 and 512x128 macular scan protocols. Drusen area and volume repeatability for each protocol and reproducibility across the two protocols were also compared to Cirrus Review software results. Results: Our segmentation method produced segmentations of high accuracy, showing similar agreement with manual markings (0.72±0.09 OR) to measured intra- and inter-reader variability (0.78±0.09 and 0.77±0.09 OR, respectively). Automated drusen area and volume measurements displayed high repeatability (7.2% and 9.63% PD for 200x200 and 512x128 protocols, respectively) and reproducibility (7.37% PD), and were more stable across protocols than the Cirrus Review software (14.38% PD, with an excellent 3.32% PD in 200x200 protocol but a worse 22.91% PD in 512x128 protocol). Measurements of drusen slope and mean drusen intensity showed significant differences across protocols. Conclusions: Our method shows accurate segmentation results that are relatively stable in scans using the same protocol and also comparable across protocols, with the exception of drusen slope and mean intensity inside drusen due to intrinsic differences in the images. Cirrus quantification software shows a higher repeatability at the 200x200 protocol than using the 512x128 protocol. Commercial Relationships: Luis De Sisternes, None; Gowtham Jonna, None; Margaret Greven, None; Theodore Leng, None; Daniel Rubin, None Support: Spectrum Predictives and Diagnostics Accelerator (SPADA) innovation grant of Stanford University, part of the Clinical and Translational Science Award (CTSA) program, funded by the National Center for Advancing Translational Sciences (Grant UL1 TR001085) at the National Institutes of Health (NIH).
9 Program Number: 1620 Poster Board Number: C0076 Variability in fundus autofluorescence (FAF) intensity is locally and globally associated with rod-mediated dark adaptation (RMDA) delay in early age-related macular degeneration (AMD) Anna V. Zarubina 1, Carrie E. Huisingh 1, Fazila Aseem 1, 2, Gerald McGwin 1, 3, Mark Clark 1, Christine A. Curcio 1, Kenneth R. Sloan 1, 4, Cynthia Owsley 1. 1 Department of Ophthalmology, University of Alabama at Birmingham, Birmingham, AL; 2 School of Medicine, Wake Forest University, Winston-Salem, NC; 3 Department of Epidemiology, University of Alabama at Birmingham, Birmingham, AL; 4 Department of Computer and Information Sciences, University of Alabama at Birmingham, Birmingham, AL. Purpose: The retinal pigment epithelium (RPE) is the major signal source for blue FAF. Histology of human RPE in AMD reveals variable cell morphologies, layer thickening, and re-distribution and loss of autofluorescent granules. RMDA depends on RPE health, and RMDA delay is a risk factor for incident AMD. We examined the association between variability in FAF intensity and RMDA in eyes with and without AMD. Methods: FAF images of persons 60 years old enrolled in the ALSTAR study underwent semi-automated masking of the vasculature and optic disk to reduce variability associated with non-af structures. Coefficient of variation (CV) (standard deviation of intensity / mean intensity) was assessed within the ETDRS grid and its central (C1) and superior inner (S3) subfields. RMDA was assessed after an 83% photobleach with targets centered at 5 on superior vertical retinal meridian (in S3). Time (minutes) required for sensitivity recovery to 5.0 X 10-3 scotopic cd/m 2 was defined as the rod-intercept (RI). Measurements were repeated 3 years later. Spearman correlation coefficients (SCC) adjusting for age were used to assess the cross-sectional association between CV of FAF and RI and the change in measurements over time. Results: There were 544 eyes in the baseline cross-sectional analysis and 322 eyes in the follow-up analysis. At baseline age-adjusted SCC between FAF CV and RI in eyes in normal macular health in C1, S3, and the full ETDRS grid was 0.04 (p=0.39), 0.08 (p=0.10), and 0.08 (p=0.09) respectively. In eyes with early AMD, SCC was 0.07 (p=0.43), 0.19 (p=0.03), and 0.19 (p=0.03) in the same regions. The age-adjusted SCC between change in FAF CV and change in RI from baseline to 3-year follow-up in eyes in normal macular health in C1, S3 and the full ETDRS grid was (p=0.98), (p=0.71), and 0.03 (p=0.59), respectively. In eyes with AMD, the correlation was 0.29 (p=0.049), 0.32 (p=0.030), and 0.47 (p=0.0009) in the same regions. Conclusions: Increased FAF variability in early AMD is associated with slowing in RMDA, a previously identified risk factor for early AMD. In eyes with early AMD, increasing FAF variability over three years is associated with further slowing of RMDA. Semi-automated analysis of FAF may offer a novel approach for evaluating how RPE health impacts RMDA in aging and AMD. Commercial Relationships: Anna V. Zarubina, None; Carrie E. Huisingh, None; Fazila Aseem, None; Gerald McGwin, None; Mark Clark, None; Christine A. Curcio, Janssen Cell Therapy (C), Genentech (C), Merck (C), Novartis (C); Kenneth R. Sloan, spouse-merck (C), spouse-novartis (C), spouse- Janssen Cell Therapy (C), spouse-genentech (C); Cynthia Owsley, Genentech (F), the University of Alabama at Birmingham (P) Support: R01AG04212, R01EY06109; EyeSight Foundation of Alabama; Alfreda J. Schueler Trust; Research to Prevent Blindness Program Number: 1621 Poster Board Number: C0077 Choroidal Volume is Affected During Treatment for Neovascular AMD Alan J. Franklin. Retina Specialty Institute, Mobile, AL. Purpose: Current treatment for neovascular AMD, NVAMD, involves inhibition of vascular endothelial growth factor (VEGF), but little research exists concerning the extent of choroidal changes following therapy. Many groups have reported progressive RPE atrophy during anti-vegf treatment for neovascular AMD, and reduction of central choroidal thickness has been associated with progressive RPE atrophy. Our group and others have linked this reduction of central choroidal thickness to progressive atrophy associated with anti-angiogenic therapy for NVAMD. Therefore, in order to better delineate the affects of pathological neovascularization and the associated treatment with anti-vegf compounds, we sought to proceed with a retrospective clinical study to evaluate changes in choroidal volumes in this cohort of patients. Methods: Anti-VEGF treatments were controlled for by selecting patients exclusively undergoing anti-vegf therapies for neovascular AMD. Optical Computed Tomography (OCT) was utilized in conjunction with Heidleberg Eye software to attain average choroidal volumes from (n=24) patient eyes. Volumes were attained by drawing parallel lines across OCT imagery outlining both choroid-sclera junctions and Bruch s membrane for 40 images per left and right eye. Average posterior choroidal thickness and volumes (mm 3 ) were calculated by the software for 2 sets of measurements per eye. Each set selected was seperated by 6 month time spans between patient treatments. Measurements were performed by a masked observer. Results: Volume averages showed a 9/n=24, or 37.5% preference towards decreased choroidal volumes with a range of (-)1.09 mm 3 - (-)0.27 mm 3. Finally, 5/n=24, or 20.1% patients identified preference towards minimal change in volumes over the same inteval with a range of (-)0.01- (+)0.09. Both neovscularization and anti-vegf treatment diminished choroidal volume. Conclusions: Central choroidal thickness is diminished both at the onset of neovascular AMD, and further decreases during anti-vegf treatment compared to the fellow untreated eye. Choroidal volume is also significantly lowered. Thus, the altered mileu of pro-angiogenic cytokines associated with the onset of choroidal neovascularization attenuates choroidal thickness and volume. This observed loss of choroidal thickness and volume is worsened after anti-vegf therapy. Commercial Relationships: Alan J. Franklin, None Program Number: 1622 Poster Board Number: C0078 En-face versus 12-line radial spectral domain optical coherence tomography scan patterns for detection of neovascular agerelated macular degeneration pathology Murtaza K. Adam, Abtin Shahlaee, Jason Hsu. Wills Eye Hospital, Philadelphia, PA. Purpose: The 12-line spectral domain optical coherence tomography (SD-OCT) radial scan pattern has been shown to be equivalent to the 25-line raster scan pattern for the detection of fluid in neovascular age-related macular degeneration (namd), but no prior studies have compared either SD-OCT scan pattern to en-face OCT. The current study compares effectiveness of the auto-segmented en-face scan pattern to the 12-line radial SD-OCT scan pattern in detecting intraretinal, subretinal, and sub-retinal pigment epithelium (sub-rpe) fluid in namd. Methods: Retrospective, observational series of patients with namd imaged between November 2014 and October A total of 49 eyes that underwent both en-face OCT with superficial retinal, deep
10 retinal, and choriocapillaris auto-segmentation (Avanti; Optovue, Inc., Fremont, CA) and 12-line radial spectral domain OCT (SD- OCT) image acquisition scan patterns (Spectralis; Heidelberg Engineering, Heidelberg, Germany) were evaluated by two independent graders. The 12-line radial SD-OCT scan was considered the gold standard for fluid detection. Interobserver differences were evaluated by a third grader. Results: A total of 72 en-face and 12-line radial SD-OCT scans were interpreted (mean: 1.47 scans/eye). 41 scans (56.9%) had confirmed fluid on SD-OCT while 31 scans (43.1%) did not. The en-face scan pattern detected fluid in all but 10 scans (false negative rate = 24.3%; 95% CI %), resulting in a sensitivity of 75.6%. Conversely, the en-face scan pattern falsely detected fluid that was not actually present in all but 12 scans (false positive rate = 38.8%; 95% CI %), resulting in a specificity of 61.2%. The difference in fluid detection between scan patterns was statistically significant (P<0.05, McNemar test). Corroborating the en-face scan with a corresponding Avanti 3 x 3 mm, 304-line raster scan improved sensitivity and specificity of fluid detection to 87.8% and 90.3%, respectively. Conclusions: The en-face OCT scan protocol alone with autosegmentation is not as sensitive as the SD-OCT 12-line radial scan in detecting the presence of intraretinal, subretinal fluid, and sub-rpe fluid in namd. En-face scan findings should be corroborated with additional OCT scan protocols to guide clinical decision making. Commercial Relationships: Murtaza K. Adam, None; Abtin Shahlaee; Jason Hsu, None Support: 2015 Heed Fellowship Award Program Number: 1623 Poster Board Number: C0079 Simultaneous comparison of mouse laser-induced choroidal neovascularization histology with visible-light optical coherence tomography angiography Ronil Shah, Brian Soetikno, Ji Yi, Wenzhong Liu, Dimitra Skondra, Hao F. Zhang, Amani A. Fawzi. Northwestern University, Plano, TX. Purpose: Choroidal neovascularization (CNV) is the hallmark of neovascular AMD. We applied visible-light optical coherence tomography angiography (vis-octa) to longitudinally monitor laserinduced CNV in mice over the span of fourteen days after induction and compare our angiograms with post-mortem immunohistological stains. Methods: Twenty-five adult pigmented mice of mixed background were anesthetized and subjected to laser induced CNV following established protocols. Four lesions were created around the optic nerve. Laser shots that did not successfully rupture Bruch s membrane were excluded from analysis. To monitor the development and regression of the CNV lesion, retinal blood vessels were imaged in three dimensions with vis-octa from days 2 through 14 post laser injury. To compare ex vivo histology with the in vivo angiograms, we performed two sets of immunohistological stains to highlight mature and immature vessels. To highlight mature, perfused vessels, we performed intracardiac injection with isolectin B immediately before euthanasia. After euthanasia, the eyes were enucleated, fixed in paraformaldehyde, and to highlight all the endothelial cells in the area and, therefore, all the immature vessel sprouts, we stained the choroids with isolectin B The final double-stained choroids were imaged with confocal microscopy. Results: Comparing the in vivo images obtained from vis-octa (Figure A) to the ex vivo immunostained flat mount (Figure B) shows consistency between the two techniques. The vessels visualized by the vis-octa are representative of the vessels visualized via immunohistological staining of the flat mount. We compared measured areas of the CNV lesion between the vis-octa and immunostained images. From this, we found that vis-octa can reliably detect CNV at five days post laser-injury. Conclusions: Vis-OCTA of CNV correlates well with the true immunohistological morphology seen on choroidal flat mounts. Because the mouse laser induced CNV model is a widely accepted model for human neovascular AMD, vis-octa holds great promise for further study of the pathophysiology of CNV in rodents. A) Vis-OCTA of a CNV lesion Day 7 post laser induction colored by depth (see color bar). B) Ex vivo confocal microscopy of immunostained choroidal flat mount of the same CNV lesion. Arrows highlight same areas on both images. Scale bars: 100 um. Commercial Relationships: Ronil Shah, None; Brian Soetikno, None; Ji Yi, None; wenzhong Liu, None; Dimitra Skondra, None; Hao F. Zhang, None; Amani A. Fawzi, None Support: Research to Preventing Blindness, NY (Department of Ophthalmology, Northwestern University); NIH grants 1R01EY and 1DP3DK (H.F.Z. and A.A.F.), Macula Society Research Grant (A.A.F.) Program Number: 1624 Poster Board Number: C0080 Photoreceptor visibility surrounding different types of subretinal drusenoid deposits (SDD) revealed by adaptive optics scanning laser ophthalmoscopy (AOSLO) XIAOYU XU 2, 1, Xing Liu 1, Xiaolin Wang 2, Yuhua Zhang 2. 1 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University, Guangzhou, China; 2 Department of Ophthalmology, University of Alabama at Birmingham, Birmingham, AL. Purpose: To compare the microstructure of photoreceptors surrounding dot and ribbon SDD [PMID: ] using AOSLO. Methods: A total of 28 eyes of 14 patients with diagnosed age-related macular degeneration (AMD) and SDD were enrolled. SDD subtypes were determined and differentiated using color fundus photograph, infrared reflectance, autofluorescence images, and spectral-domain optical coherence tomography (SD-OCT). SDD were classified using an OCT-based 3-stage grading system. SDD lesions and surrounding photoreceptors were examined using AOSLO. The observation was repeated 3 times over 3.5 years. Results: Dot SDD were found in 22 eyes of 11 patients. Ribbon SDD were found in 2 eyes of 1 patient. Both forms were seen together in 4 eyes of 2 patients. For dot SDD at stage 3, AOSLO presented a typical pattern showing a central reflective core of the lesion material surrounded by a hyporeflective annulus. Photoreceptor mosaic was visible outside this SDD affected area. For ribbon SDD at the same stage, AOSLO revealed a similar lesion structure as that of the dot SDD. However, photoreceptors adjacent to the lesion were illegible.
11 Conclusions: The absence of photoreceptor mosaic in ribbon SDD may indicate degeneration in the photoreceptor outer segment and the interdigitation zone that impairs the waveguide property of the photoreceptors. Our study implied the possible differentiation of disease outcome and prognosis in different subtypes of SDD. Figure 1. Multimodal imaging of SDD. A-C are multimodal images of dot SDD. A. Discrete hypofluorescent spots in autofluorescence (AF) image of the macular. B. SD-OCT image taken through the green line in panel A. The ellipsoid zone (EZ) band was discernible in areas between SDD lesions. C. Typical en face appearance of SDD in AOSLO taken through the blue box in panel A. D-F are multimodal images of ribbon SDD. D. Interconnected hypofluorescent bands in AF image. E. SD-OCT image taken through the green line in panel D. The continuous accumulation of SDD material made the EZ band invisible. F. The AOSLO image taken through the blue box in panel D, no illegible photoreceptor mosaic adjacent to the SDD lesion was shown. Color arrowheads point to the corresponding SDD imaged in different imaging modalities. Commercial Relationships: XIAOYU XU, None; Xing Liu, None; Xiaolin Wang, None; Yuhua Zhang, None Support: NIH R01EY024378, P30 EY003039,and institutional support from Research to Prevent Blindness, EyeSight Foundation of Alabama, Buck Trust of Alabama, Science and Technology Planning Project of Guangdong Province, China, 2012B , Science and Technology Program of Guangzhou, China, 2013J , Fundamental Research Funds of the State Key Laboratory of Ophthalmology, China and International Program for Ph.D. Candidates, Sun Yat-Sen University, China. Program Number: 1625 Poster Board Number: C0081 Evaluating the Response of Type 1 Choroidal Neovasular Membrane in Neovascular Age-Related Macular Degeneration to Anti-VEGF Treatment by Optical Coherence Tomography- Angiography Ching J. Chen, Matt Olsen, Brian Tieu, Jordan Burnham. Ophthal & Visual Science, Univ of Mississippi Med Center, Jackson, MS. Purpose: To evaluate the response of Type 1 CNV in neovascular ARMD to anti-vegf treatment using OCT angiography (OCTA) Methods: Retrospective review of SSADA-based OCTA images from patients treated with anti-vegf for neovascular ARMD with type 1 CNV. Results: 37 eyes with type 1 CNV were treated with various anti- VEGF agents. Among them, 10 remained partially active; 7 were refractive to treatment; 10 were responsive with temporary inactivity; and 10 were quiescent for more than one year after treatment. The OCTA detected blood flow in all 37 treated CNVs. In partially active CNV, the size and vascular volume of the CNV varied. The size of the CNV was smaller in partially active and temporarily inactive CNVs compared to refractive CNVs. The CNV responded to anti- VEGF treatment by partial closure of peripheral vascular branches, but the central vascular trunk remained unaffected. Recurrent activity also involved mainly the peripheral branches. In refractive CNV, weekly OCTA showed no to minimal vascular responses. In quiescent CNV, flow change analysis showed a steady vascular flow pattern without changes. Conclusions: Blood flow was detected by OCTA in all treated CNVs regardless of their clinical response to anti-vegf treatment. The treatment goal for neovascular ARMD should not be a complete resolution of the CNV. Instead, the main aim may be turning an exudative type to a non-exudative CNV. The role of OCTA alone in the management of neovascular ARMD still needs further study. Commercial Relationships: Ching J. Chen, None; Matt Olsen; Brian Tieu, None; Jordan Burnham, None Program Number: 1626 Poster Board Number: C0082 Automated Detection of the Optic Disc in Fundus Autofluorescence Images of Age-Related Macular Degeneration Daniel Albertus 1, Kanishka T. Jayasundera 1, Chris Ranella 1, Matthew Johnson-Roberson 2. 1 Kellogg Eye Center, University of Michigan, Ann Arbor, MI; 2 Department of Naval Architecture & Marine Engineering and the Department of Electrical Engineering and Computer Science, University of Michigan, Ann Arbor, MI. Purpose: Current subjective analysis of fundus autofluorescence (FAF) images for age-related macular degeneration (AMD) is not ideal given new therapeutics which may be able to slow the progression of dry AMD. The detection of both hyper- and hypofluorescent regions of disease is challenging due to similarities between these areas and various normal FAF features including the optic disc. We show a reliable way of identifying the optic disc in a fully automatic manner in images from patients with AMD. Methods: Fundus autofluorescence (FAF) images from the Heidelberg Spectralis were first pre-processed, which includes correction for uneven illumination and contrast, followed by segmentation of the blood vessels. Next, a pixel-wise classification using Gabor wavelet responses and pixel intensity as features was carried out, followed by spatial clustering of the positively classified pixels to obtain distinct regions of interest. Region-wise classification was then carried out on these distinct clusters and the optic disc was identified based on surrounding vessel density and orientation as well as circle fit and relative size. Results: Optic disc detection was performed on 144 FAF images of patients with AMD. Of these 144 FAF images, 29 images were used for training whereby a human grader determined where the optic disc was on the image. The remaining 115 images were then used for testing of the algorithm which was successful in correctly identifying 86 (75%). Pixel wise the algorithm had a sensitivity of 97% and a specificity of 99% indicating that the algorithm was able to not only identify where the optic disc was but also accurately identify the specific pixels which represented it compared to the human grader. Conclusions: We present a method to automatically detect and segment optic discs in FAF images of patients with dry AMD. The proposed method takes advantage of vessel geometry outside the optic disc along with the geometry of the optic disc itself to refine
12 positive pixel classifications. Results validated the effectiveness of the technique on actual clinical FAF images despite the presence of geographic atrophy which mimics the appearance of the optic disc. The process leading up to optic disc detection including vessel segmentation, pixel-wise classification and circle fitting. Examples of the optic disc being positively identified despite the similar appearance to geographic atrophy. Commercial Relationships: Daniel Albertus, None; Kanishka T. Jayasundera, None; Chris Ranella; Matthew Johnson-Roberson, None Program Number: 1627 Poster Board Number: C0083 VCAM-1 targeted in vivo imaging of neovascular disease in preclinical model Md Imam Uddin 1, Stephanie Evans 1, Alexis Wong 2, David W. Wright 2, Ashwath Jayagopal 3, John S. Penn 1, 4. 1 Ophthalmology, Vanderbilt University School of Medicine, Nashville, TN; 2 Chemistry, Vanderbilt University, Nashville, TN; 3 Hoffmann-La Roche Ltd, Basel, Switzerland; 4 Department of Cell and Developmental Biology, Vanderbilt University, Nashville, TN. Purpose: Neovascularization is the major cause of vision loss in age-related macular degeneration (AMD) and other retinal diseases. Inflammatory biomarkers including vascular cell adhesion molecule 1 (VCAM-1) are overexpressed in endothelial cells correlating with AMD progression. In vivo imaging of VCAM-1 mrna may allow for the detection of early pathogenic events, be used to monitor disease progression, or allow for assessment of therapeutic response. To achieve this goal, we have developed hairpin DNA-functionalized gold nanoparticle (haunp) probes for the in vivo detection of VCAM-1 mrna expression in ocular tissues. Methods: Self-complementary, energy minimized DNAoligonucleotides were computationally designed to achieve hairpin loop secondary structures. The optimized DNA-oligonucleotides were each coupled to a near-infrared (NIR) dye and conjugated to spherical gold nanoparticles (haunp). To test the utility of the new haunp probes, adult C57B/6 mice received laser wounds to induce choroidal neovascularization (LCNV). The VCAM-1 mrna expression was assayed at days 0, 1, 2, 3, 6, 10 and 14 post-laser injury by qrt-pcr. The haunp probes were injected systemically or intraocularly in LCNV mice. In vivo imaging was performed using the Micron IV optical imaging system. The tissues were also examined ex vivo for specificity of the haunp probe. Scrambled oligonucleotide sequences were used as nonspecific control probes. Results: VCAM-1 mrna expression peaked at day 3 post-laser as determined by qrt-pcr analysis. At this time point, haunpdependent fluorescence enhancement clearly visualized the LCNV lesions with >30:1 signal to noise ratios as compared to adjacent non-injured tissues. VCAM-1 intravascular haunp-dependent fluorescence signal was minimal. The scrambled haunp probes were undetectable under the same image acquisition conditions. Conclusions: We have developed a targeted imaging probe for the detection of mrna expression in real time. In vivo imaging using this haunp probe in LCNV mice allowed high-resolution detection of VCAM-1 mrna expression localized to LCNV lesions. These probes may be easily adapted to transfection, knockdown or visualization of retinal gene expression in real time. The last of these has particularly strong implications for clinical application. Commercial Relationships: Md Imam Uddin, None; Stephanie Evans, None; Alexis Wong, None; David W. Wright; Ashwath Jayagopal, None; John S. Penn, None Program Number: 1628 Poster Board Number: C0084 Comparison of SD-OCT and OCT-Angiography Features in Presumed Choroidal Neovascularization in the AVATAR study Deepa Manjunath, Sunil K. Srivastava, Rishi P. Singh, Peter K. Kaiser, Aleksandra Rachitskaya, Justis P. Ehlers. Cleveland Clinic Foundation, Cleveland, OH. Purpose: Spectral domain optical coherence tomography (SD-OCT) is the current standard imaging modality for monitoring exudative activity secondary to choroidal neovascular tissue (CNV) in patients with macular disease. Optical coherence tomography angiography (OCT-A) is an emerging modality that allows direct visualization of flow within CNV vessels. It is not known how the detection of CNV by OCT-A compares with detection of choroidal neovascular exudation by SD-OCT. The purpose of this study was to evaluate the comparative features of the two modalities in eyes with presumed CNV. Methods: This was an IRB-approved prospective observational study examining OCT-A in eyes undergoing SD-OCT for macular disease, the AVATAR study. All patients were imaged with the Avanti RTVue XR HD (Optovue, Fremont, CA) and the Cirrus HD-OCT system (Zeiss, Oberkochen, Germany). The Avanti system was equipped with prototype SSADA algorithm software to generate segmented retinal OCT-A scans. Images were reviewed by a masked expert reviewer. SD-OCT scans were assessed for intraretinal fluid, subretinal fluid, subretinal hyperreflective material, and subretinal pigment epithelial
13 material. OCT-A scans were assessed for the presence or absence of CNV, defined as flow signal in the outer retina and/or abnormal vascular flow in the choroid. Results: A total of 81 eyes were imaged. Thirty-five eyes had subretinal and/or intraretinal fluid on SD-OCT while 46 were negative for fluid. Of the eyes with positive fluid on SD-OCT, 69% (24/35) had CNV on OCT-A, 14% (5/35) did not have CNV on OCT-A, and 17% (6/35) were indeterminate. Of the eyes with negative fluid on SD-OCT, 30% (14/46) had CNV on OCT-A, 50% (23/46) did not have CNV on OCT-A, and 20% (9/46) were indeterminate. Conclusions: OCT-A provides a unique opportunity for visualization of CNV in eyes with macular disease. OCT-A may predict active flow within CNV in the absence of exudative signs on SD-OCT. Further research is needed to better delineate the specific roles for OCT-A in the management of CNV. SD-OCT and OCT-angiography of eyes with presumed choroidal neovascularization (CNV). 3x3-mm OCT-A scans were segmented at the choriocapillaris. (a) Subretinal fluid on SD-OCT (arrows) corresponds to CNV on OCT-A. (b) Intraretinal fluid is positive on SD-OCT (arrows) but there is no CNV on OCT-A. (c) CNV can be seen on OCT-A but SD-OCT fluid is negative. Commercial Relationships: Deepa Manjunath; Sunil K. Srivastava, Carl Zeiss Meditec (C), Leica (C), Santen (C), Bausch and Lomb (C), Synergetics (P), Bausch and Lomb (F), Bioptigen (P), Allergan (F); Rishi P. Singh, Carl Zeiss Meditec (C); Peter K. Kaiser, Ophthotech (C), Novartis (C), Regeneron (C), Oraya (C), Genentech (C), Carl Zeiss Meditec (C), Bausch and Lomb (C), Alcon (C), Topcon (C), Ohr (C), Bayer (C); Aleksandra Rachitskaya, None; Justis P. Ehlers, Zeiss (C), Zeiss (F), Bioptigen/Leica (F), Bioptigen/Leica (C), Santen (C), Genentech (F), Bioptigen/Leica (P), Alcon (C), Synergetics (P), Thrombogenics (C), Regeneron (F), Thrombogenics (F) Support: NIH/NEI K23-EY A1; Ohio Department of Development TECH Program Number: 1629 Poster Board Number: C0085 Does fluorescein angiography add value in the management of suspected choroidal neovascularization? Prashant K. Parekh, Michael D. Abramoff. Ophthalmology, University of Iowa Hospitals and Clinics, Iowa City, IA. Purpose: Fluorescein angiography (FA) has long been the standard modality to diagnose and manage choroidal neovascularization (CNV). However, FA is costly, has a mortality of 1 per , and considerable morbidity from allergic reactions. Since the advent of anti-vegf therapy for CNV, optical coherence tomography (OCT), a non-invasive imaging method free of these disadvantages, is used extensively to manage CNV, while FA is primarily used to make the initial diagnosis. A recent study found the sensitivity and specificity of OCT compared to FFA in diagnosis of CNV to be 100 and 80.8%, respectively. We believe that FA alters management of patients that are initially suspected of having CNV in less than 10% of cases. If this hypothesis is confirmed, it would cast doubt on the clinical utility and cost-effectiveness of FA in diagnosing CNV, except in treatment failures and non-standard cases. Methods: After retrospective review of the clinical histories, FA, and OCT from 99 patients (99 eyes) who had an initial presentation of confirmed CNV and subsequent de-identification, three retina specialists masked to each other will review, in randomized order, the standardized brief initial clinical history, color fundus image, and OCT scan. They will then choose whether to manage each case by observation or anti-vegf injection (FA- arm). After rerandomization, corresponding early, mid, and late phase FA images will be added to each patient s case data, and the three experts will again choose from these 2 management options (FA+). For each expert, the case discordance (i.e., the percentage of cases where management differed between FA- and FA+) and inter-observer discordance (i.e., percentage of cases where all 3 experts differed) will be determined. Results: For one retina specialist, observation was recommended in 13.1% of cases while anti-vegf treatment was recommended in the remaining 86.9% for both FFA- and FFA+ groups. The case discordance was 13.1%. Inter-observer reliability, measured through kappa and intra-class correlation parameters, is pending based on the data from the other retina specialists. Conclusions: Based on the preliminary data, there is a suggestion that FA continues to have an important role in the management of CNV in standard cases; however, as more data is obtained from retina specialists, the discrepancy in management decisions may be further minimized. Commercial Relationships: Prashant K. Parekh, None; Michael D. Abramoff, None Program Number: 1630 Poster Board Number: C0086 RPE imaging with polarization-sensitive optical coherence tomography in healthy subjects and AMD patients Barry Cense 1, 2, Donald T. Miller 2, Ann E. Elsner 2. 1 Center for Optical Research and Education, Utsunomiya University, Utsunomiya, Japan; 2 School of Optometry, Indiana University, Bloomington, IN. Purpose: Morphological changes in the retina such as the appearance of drusen are routinely used to diagnose AMD. Polarization-sensitive optical coherence tomography (PS-OCT) can quantify optical properties of the retina which may help in the early diagnosis of AMD, prior to the formation of drusen.
14 Methods: Volumetric PS-OCT data sets acquired at 840 nm covering 15 by 15 centered at the fovea were obtained in 4.4 s. The retardance below the RPE, the degree of polarization uniformity (DOPU) and the standard deviation of the fast axis (STDVFA) in the RPE were quantified. Measurements were collected from a group of young healthy subjects (n = 10, age < 25 y), a group of ageing subjects (n = 10, age > 50 years) and patients with AMD in various stages (n = 5). Results: Low retardance signals (~ < 25 ), low STDVFA signals (<25 ), and DOPU values of ~0.5 were found in all young subjects. In all older subjects (age >50 years), a much higher retardance was found, with values up to 180. DOPU in the RPE was low (~0.35) and the STDVFA was similar to values found in the group of young subjects, indicating that deposits that scatter light were not sufficient to generate a signal different from what was measured in the younger group. In the AMD patients, retardance and DOPU values were similar to the young subjects. A considerable increase in STDVFA was measured (~35-40 ) in the RPE and also in the upper layers of the retina. Conclusions: Older subjects exhibit elevated phase retardation in BM, in sharp contrast to young healthy subjects and AMD patients who showed no such evidence. We propose that this signal is induced by accumulation of waste material or displacement of melanin in the RPE, which could have decreased the DOPU signal in the ageing subjects. In these cases, the polarization state changes more as a function of position across the fundus. In the AMD patients, the build up of debris below the RPE in drusen translates in an increased STDVFA signal. Commercial Relationships: Barry Cense, Indiana University, WO/2010/ (P), Massachusetts General Hospital, US 60/575,773 (P), Utsunomiya University, WO2013/ (P); Donald T. Miller, Indiana University, WO/2010/ (P); Ann E. Elsner, Aeon Imaging Program Number: 1631 Poster Board Number: C0087 Morphologic characteristics of the retina during drusen development in early and intermediate age-related macular degeneration Ferdinand G. Schlanitz, Magdalena Baratsits, Hrvoje Bogunovic, Alessio Montuoro, Stefan Sacu, Ursula Schmidt-Erfurth. Medical University of Vienna, Vienna, Austria. Purpose: The aim of this study was to investigate morphologic characteristics of the retina during drusen development in early and intermediate age-related macular degeneration (AMD) using spectraldomain optical coherence tomography (SD-OCT) images. Methods: 15 eyes with early or intermediate AMD were scanned using Spectralis SD-OCT (scanning area 20 x20, volume scan 1024x97) in a regular follow-up scheme every three months for at least one year. The standard EDTRS grid was centered on the fovea of the individual eyes and the drusen volume for each EDTRS-field was segmented by a software automatically. Two expert graders reviewed the each B-scans of the volume scans. The presence of pseudodrusen, RPE-migration, hyperreflective material inside drusen and vortexing of the internal retinal layers was noted, and the integrity of the RPE-layer as well as of the ELM and IS-OS-layer was evaluated and, if an atrophy/absence of one of those layers was observed, the area of absence was segmented manually. Results: 15 eyes were evaluated in this project. Progression of the drusen volume was observed in all eyes, as well as a spontaneous regression. Interestingly, drusen regression and progression can occur simultaneoulsy within different areas of the retina, and small distinct drusen regression events are often overrode by a much more substantial progression. During regression of drusen volume, as seen in the individual EDTRS-fields, migration of RPE cells was observed frequently (p<0.001), as well as vortexing of the internal retinal layers (p<0.001), hyperreflective material inside of drusen (p<0.001) and a beginning atrophy of the RPE layer as well as a dissolving ELM (p<0.05 and 0.01, resp.). However, only the development of hyperreflective material inside drusen seem to precede a drusen volume regression (p<0.001). Conclusions: Eyes in early AMD show a dynamic modeling of drusen, and progression as well as regression of drusen volume can occur simultaneously in the same eye. The evolving of certain characteristics are related to a regression of drusen volume, and further research might unveil their significance as biomarkers for progression of AMD. Commercial Relationships: Ferdinand G. Schlanitz, None; Magdalena Baratsits, None; Hrvoje Bogunovic, None; Alessio Montuoro, None; Stefan Sacu; Ursula Schmidt-Erfurth, Bayer (F), Boehringer (F), Allergan (F), Alcon (F) Program Number: 1632 Poster Board Number: C0088 Relationship of Pseudodrusen and Drusen Development in Agerelated Macular Degeneration Magdalena Baratsits, Ferdinand G. Schlanitz, Katharina Eibenberger, Alessio Montuoro, Stefan Sacu, Stefan Zotter, Bernhard Baumann, Michael Pircher, Christoph K. Hitzenberger, Ursula Schmidt-Erfurth. Medical University of Vienna, Vienna, Austria. Purpose: The aim of this study was to investigate the development of pseudodrusen (PD) and drusen in age-related macular degeneration (AMD) longitudinally by manual three-dimensional segmentation of polarization-sensitive OCT (PS-OCT) volume scans. Methods: 109 patients with early AMD were scanned using a widefield PS-OCT (scanning area 30 x30, volume scan 1024x250) in a regular follow-up scheme for at least one year. The collective was reviewed and patients with PD and drusen were selected for grading. The RPE and drusen were segmented by PS-OCT automatically. Two expert graders segmented manually every PD in the volume scan at baseline and at the follow-up visits. Hyperreflective material above the retinal pigment epithelium (RPE) and below the external limiting membrane (ELM) layer was defined and segmented as PD. Results: 15 eyes with PD were segmented manually by the graders. The mean volume at baseline was mm 3 for PD and 0.21mm 3 for drusen and at year one mm 3 for PD resp. 0.20mm 3 for drusen. The volume of PD significantly correlated with drusen volume (p<0.04), with eyes of large drusen volumes having lesser PD volume. During follow-up, development could be divided into three groups: Eyes in which both PD and drusen volumes increased over time, eyes with significant drusen regression and a concomitant growth of PD volume, and eyes with increasing drusen and regressing PD volumes. The largest growth rates were observed in the first group, whereas the other groups showed a concomitant uprising of pathomorphological signs such as a deteriorated RPE. No case of a simultaneous regression of both drusen and PD was observed. Conclusions: Due to the RPE-sensitivity of the PS-OCT, pseudodrusen could be segmented in a more reliable way than before. The development of PD and drusen volumes seems to be linked together, and the interactive relationships between those both pathomorphologic characteristics might give an insight on ongoing degenerative processes. Commercial Relationships: Magdalena Baratsits, None; Ferdinand G. Schlanitz, None; Katharina Eibenberger, None; Alessio Montuoro, None; Stefan Sacu, Askin (F), Bayer (F),
15 Novartis (F), Allergan (F), Pharmaselect (F); Stefan Zotter, None; Bernhard Baumann, None; Michael Pircher, None; Christoph K. Hitzenberger, Canon (F); Ursula Schmidt-Erfurth, Bayer (F), Allergan (F), Alcon (F), Boehringer (F) Program Number: 1633 Poster Board Number: C0089 Computational analysis of spatial correspondence between intraretinal, subretinal and sub-rpe fluid in neovascular AMD Sophie Klimscha 1, Hrvoje Bogunovic 1, Thomas Schlegl 1, Ana-Maria Philip 1, Li Zhang 2, Michael D. Abramoff 2, Milan Sonka 2, Bianca Gerendas 1, Sebastian M. Waldstein 1, Ursula Schmidt-Erfurth 1. 1 Christian Doppler Laboratory for Ophthalmic Image Analysis, Vienna Reading Center, Department of Ophthalmology, Medical University Vienna, Vienna, Austria; 2 Department of Electrical and Computer Engineering, The University of Iowa, Iowa City, IA. Purpose: Evidence suggests that subretinal fluid (SRF) may be associated with favorable visual prognosis in the therapy of neovascular age-related macular degeneration (namd), while intraretinal cystoid fluid (IRC) correlates with poorer vision. The aim of this retrospective, cross-sectional study was to gain additional insight into structure-function correlation by analyzing the spatial correspondence between the main pathomorphologic components in namd, i.e., IRC, SRF and pigment-epithelial detachment (PED). We hypothesized that IRC occur mainly co-localized with PED, while SRF appears spatially anti-correlated with the other two components. Methods: SD-OCT volume scans (128 B-scans, 6x6mm) of 616 patients with treatment-naïve namd available at the Vienna Reading Center were included. IRC, SRF and PED were detected on a pervoxel basis using fully automated segmentation algorithms. For validation, IRC and SRF were segmented manually in a separate set of 38 patients. To quantify the spatial correspondence of IRC/SRF/ PED lesions, we calculated the percentages of IRC-, SRF-, or PEDaffected A-scans also affected by one or both of the respective other pathomorphologic components and reported the median across the population. Results: 78,848 OCT B-scans were analyzed automatically and 4,864 manually. Of the 6x6mm area covered by the SD-OCT scan, a mean of 9% was affected by IRC, 15% by SRF and 7% by PED. In the 616 automatically processed eyes, averaged spatial correspondence between the features was as follows: Of IRC-affected A-scans 16% presented with SRF, 36% with PED. Of SRF-affected A-scans 10% presented with IRC, 6% with PED. Of PED-affected A-scans 44% presented with IRC, 11% with SRF. In the 1-mm central foveal region, similar patterns were observed (Table 1). In the 38 manually segmented validation cases, consistent results were obtained (Table 1). Representative example cases are provided in Figure 1. Conclusions: In treatment-naïve namd, IRC most frequently appear above PED. In contrast, SRF appears spatially anti-correlated to PED and IRC. Thus, the positive effects of SRF on visual function may be attributed to a lower likelihood of concomitant IRC in the same area. Table 1
16 of which 4 progressed to GA and 3 to namd. The linear increase in transmission defects over time ranged from 2.5μm/mth to 221μm/mth with mean expansion of 58.4μm/mth (Standard deviation 65.9μm/ mth). Conclusions: Development of nga and GA in patients with unilateral neovascularisation is a relatively common phenomenon. Multi-modal imaging incorporating OCT features and AF significantly improves detection of the earliest changes. Commercial Relationships: Ruth E. Hogg; Rufino M. Silva, Pfizer (F), Roche (F); Giovanni Staurenghi, Pfizer (F), Roche (F); Chiara Rosina, None; Ana Rita Santos, None; Usha Chakravarthy, Roche (F), Pfizer (F) Support: Educational grant from Pfizer Inc. (A ). Figure 1: Automatically (a,b) and manually (c) segmented example cases Commercial Relationships: Sophie Klimscha, None; Hrvoje Bogunovic, None; Thomas Schlegl, None; Ana- Maria Philip, None; Li Zhang, None; Michael D. Abramoff; Milan Sonka, None; Bianca Gerendas, None; Sebastian M. Waldstein, Bayer Healthcare (C), Novartis (C); Ursula Schmidt-Erfurth, Novartis (C), Boehringer Ingelheim (C), Alcon (C), Bayer Healthcare (C) Support: Christian Doppler Research Society Program Number: 1634 Poster Board Number: C0090 Prevalent and incident geographic atrophy (GA) in fellow-eyes of patients with unilateral neovascular age-related macular degeneration (AMD) Ruth E. Hogg 1, Rufino M. Silva 2, Giovanni Staurenghi 3, Chiara Rosina 3, Ana Rita Santos 2, Usha Chakravarthy 1. 1 Centre for Experimental Medicine, Queen s University Belfast, Belfast, United Kingdom; 2 Association for Innovation and Biomedical Research on Light and Image, Ophthalmology Unit, Centro Hospitalar e Universitário Coimbra, and Faculty Medicine, University of Coimbra, Coimbre, Portugal; 3 Eye Clinic, Department of Clinical Science Luigi Sacco, Sacco Hospital, University of Milan, Milan, Italy. Purpose: To investigate the development of nascent or established geographic atrophy in the fellow eyes of patients with unilateral neovascular age-related macular degeneration using multi-modal imaging. Methods: Study sample: Study sample: 105 participants (53 males, 52 females) age years with unilateral advanced AMD from 3 Centres (Milan, Coimbra, Belfast) followed for a minimum of 12 months(mth). The study eye was the eye without advanced disease and imaged 6 monthly. Colour images were captured on the Topcon 50X fundus camera, red free (RF), autofluorescence (AF), infra-red (IR) and optical coherence tomography (OCT) on the Heidelberg Spectralis using standardised protocols. Established GA was defined as an area of reduced AF with well delineated margins and accompanied by loss of outer retinal layers on OCT. Nascent GA (nga) was said to be present when tomographic scans showed photoreceptor and or RPE loss with increased signal transmission. Expansion of areas of nga were measured on OCT and rates of progression calculated. Results: At baseline 87 study eyes had no evidence of either GA or nga, 5 had GA and nga and 6 nga only. In study eyes free of nga or GA at baseline, 9 (10.3%) developed nga during follow up Program Number: 1635 Poster Board Number: C0091 Comparison between Multimodal Imaging and OCT Angiography in the diagnosis of Age Related Choroidal Neovascularization Maurizio Mete 1, Antonio Peroglio Deiro 1, Massimo Guerriero 2, Grazia Pertile 1. 1 Ophthalmology, Ospedale Sacro Cuore Don Calabria, Negrar (VR), Italy; 2 Computer Science, University of Verona, Verona, Italy. Purpose: To assess inter- and intraobserver agreement between multimodal imaging (SD-OCT, fluorescein and indocyanine angiography) and OCT angiography for the diagnosis of Choroidal Neovascularization (CNV) in Age Related Macular Degeneration (AMD). Methods: Cross sectional study. Twenty-nine consecutive patients referred to our ophtalmologic department with a suspicious exudative AMD were studied by multimodal imaging (HRA Spectralis, Heidelberg Engenieering, Germany) and OCT Angiography (Optovue RTVue XR Avanti, Freemont, USA). The exams were performed in the same day. Two independent examiners reviewed the images. Cohen s K coefficient was calculated to evaluate the intra- and interobserver agreement for both techniques. Results: Twenty-nine consecutive patients were included (8 males, 21 females; mean age 73 years range 67-89). A good inter-observer agreement was observed (K =0.6568) for multimodal imaging and resulted statistically significant (P = ). Similar results were achieved also for OCT angiography (K=0.6778; P=0.0001). The intra-observer agreement between the two imaging techniques resulted optimal (K=0.8284); the area under the ROC curve was The analysis was repeated by another observer, who substantially replied the results. Conclusions: The gold standard technique for CNV diagnosis includes FA, ICGA and OCT. Usually they have to be considered together to reach the highest diagnostic power: nevertheless, achieving and analysing all the images could be extremely timeconsuming. OCT angiography is a new imaging tool that could allow obtaining angiographic-like images in a very quick time, with no need of dye injections. Our results showed that OCT angiography is a reliable tool for the diagnosis of CNV in AMD and may be considered as a substitute of conventional techniques, with both a substantial saving of time and a reduction of patient discomfort. Commercial Relationships: Maurizio Mete, None; Antonio Peroglio Deiro, None; Massimo Guerriero, None; Grazia Pertile, None
17 Program Number: 1636 Poster Board Number: C0092 Graph-based fluid segmentation from OCT images Ipek Oguz, Li Zhang, Andreas Wahle, Milan Sonka, Michael D. Abramoff. Ophthalmology, University of Iowa, Iowa City, IA. Purpose: Accurate and reproducible segmentation of fluid-filled regions from retinal OCT images is an important step allowing quantification of the disease status, longitudinal disease progression, and response to therapy in wet-pathology retinal diseases. However, segmentation of fluid-filled regions from OCT images is a challenging task due to their inhomogeneous appearance, the unpredictability of their number, size, location, and image appearance. Methods: We developed a knowledge-based approach that leverages a carefully designed cost function and graph-based segmentation techniques to provide a vendor-independent solution to this problem. The cost function reflects the known properties of the SEAD s (Symptomatic Exudate Associated Derangements) in a layer-specific manner. Retinal tissue characteristics are determined directly from the image, rather than enforcing a priori intensity models. We evaluate this approach on two publicly available datasets. The OPTIMA Cyst Segmentation Challenge training data consists of 15 AMD patients acquired with devices from 4 different vendors (Spectralis, Cirrus, Topcon, Nidek), with 49 to 128 B-scans per OCT volume. The DME dataset ( consists of 10 Spectralis scans with 61 B-scans each. Results: Compared to a previous machine-learning based approach, the absolute volume similarity error in the DME dataset was dramatically reduced from 81.3 ± 56.4% to 43.0 ± 37.4% (paired t-test, p << 0.01). Comparison to the first (second) manual rater resulted in 87% vs. 46.4% (75.2% vs. 39.5%) volume dissimilarity for the previous and new methods. Figs. 1 and 2 present qualitative results. Conclusions: The preliminary results are highly promising for robust vendor-independent segmentation of fluid-filled regions from OCT scans in exudative retinal diseases. Segmentation results in the OPTIMA dataset. Commercial Relationships: Ipek Oguz, None; Li Zhang, None; Andreas Wahle, None; Milan Sonka, University of Iowa (P); Michael D. Abramoff, IDx LLC (C), IDx LLC (I), University of Iowa (P) Support: National Institutes of Health grants R01 EY019112, R01 EY and R01 EB004640; the Department of Veterans Affairs, Arnold and Mabel Beckman Initiative for Macular Research. Segmentation results in the DME dataset.
ICG IMAGING FOR EXUDATIVE ARMD
 ICG IMAGING FOR EXUDATIVE ARMD MARK H. NELSON, MD MBA WINSTON-SALEM, NC ASRS INSTRUCTION COURSE AUGUST 24, 2011 FINANCIAL DISCLOSURE Novartis Pharmaceutics, Incorporated Consultant, Grant Recipient Heidelberg
ICG IMAGING FOR EXUDATIVE ARMD MARK H. NELSON, MD MBA WINSTON-SALEM, NC ASRS INSTRUCTION COURSE AUGUST 24, 2011 FINANCIAL DISCLOSURE Novartis Pharmaceutics, Incorporated Consultant, Grant Recipient Heidelberg
APRIL 8th 2016 Therapy
 APRIL 8th 2016 Therapy 09.00-10.00 SESSION 1: Age-related Macular Degeneration Moderators: S. Sadda, D. Sarraf, K. Bailey Freund, E. Souied 09.00-09.15 Prospective SD OCT Analysis of PED Associated with
APRIL 8th 2016 Therapy 09.00-10.00 SESSION 1: Age-related Macular Degeneration Moderators: S. Sadda, D. Sarraf, K. Bailey Freund, E. Souied 09.00-09.15 Prospective SD OCT Analysis of PED Associated with
Age- Related Macular Degeneration
 Age- Related Macular Degeneration Age-Related Macular Degeneration (AMD) is the leading cause of blindness in the United States. It is caused by damage to a localized area of the central retina called
Age- Related Macular Degeneration Age-Related Macular Degeneration (AMD) is the leading cause of blindness in the United States. It is caused by damage to a localized area of the central retina called
Retinal Imaging Biomarkers for Early Diagnosis of Alzheimer s Disease
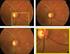 Retinal Imaging Biomarkers for Early Diagnosis of Alzheimer s Disease Eleonora (Nora) Lad, MD, PhD Assistant Professor of Ophthalmology, Vitreoretinal diseases Duke Center for Macular Diseases Duke University
Retinal Imaging Biomarkers for Early Diagnosis of Alzheimer s Disease Eleonora (Nora) Lad, MD, PhD Assistant Professor of Ophthalmology, Vitreoretinal diseases Duke Center for Macular Diseases Duke University
Trends in Ophthalmology a Market Perspective. Matthias Karl, Michael Kempe
 Trends in Ophthalmology a Market Perspective Matthias Karl, Michael Kempe 30.04.2013 Agenda 1 2 3 4 Role of Optical Technologies in Ophthalmology Demands of the Market - Trends in the Application Implications
Trends in Ophthalmology a Market Perspective Matthias Karl, Michael Kempe 30.04.2013 Agenda 1 2 3 4 Role of Optical Technologies in Ophthalmology Demands of the Market - Trends in the Application Implications
Angiogenesis, Exudation, and Degeneration 2015. February 7, 2015 Mandarin Oriental, Miami, Florida
 Angiogenesis, Exudation, and Degeneration 2015 February 7, 2015 Mandarin Oriental, Miami, Florida Program Directors: Philip J. Rosenfeld, MD, PhD and Harry W. Flynn, Jr., MD Course Associate Director:
Angiogenesis, Exudation, and Degeneration 2015 February 7, 2015 Mandarin Oriental, Miami, Florida Program Directors: Philip J. Rosenfeld, MD, PhD and Harry W. Flynn, Jr., MD Course Associate Director:
Optic Disc Drusen. Normal Enlarged view of Optic Disc. Lumpy Appearance of Optic Disc. Optic Disc Drusen With Drusen
 Optic Disc Drusen Your doctor has diagnosed you with optic disc drusen. Optic disc drusen are abnormal deposits of protein-like material in the optic disc the front part of the optic nerve. We do not know
Optic Disc Drusen Your doctor has diagnosed you with optic disc drusen. Optic disc drusen are abnormal deposits of protein-like material in the optic disc the front part of the optic nerve. We do not know
Angiogenesis, Exudation, and Degeneration 2016. February 6, 2016 Mandarin Oriental, Miami, FL
 Angiogenesis, Exudation, and Degeneration 2016 February 6, 2016 Mandarin Oriental, Miami, FL Program Directors: Philip J. Rosenfeld, MD, PhD and Harry W. Flynn, Jr., MD Course Associate Director: Carmen
Angiogenesis, Exudation, and Degeneration 2016 February 6, 2016 Mandarin Oriental, Miami, FL Program Directors: Philip J. Rosenfeld, MD, PhD and Harry W. Flynn, Jr., MD Course Associate Director: Carmen
Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling.
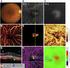 Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling. Robert Gizicki MD, Mohamed Haji, Flavio Rezende Retina Service, Hôpital Maisonneuve-Rosemont,
Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling. Robert Gizicki MD, Mohamed Haji, Flavio Rezende Retina Service, Hôpital Maisonneuve-Rosemont,
INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE DETAILED TABLE
 Proposed Disease Severity Level No apparent Mild Non- Proliferative Moderate Nonproliferative Severe Non- Proliferative Proliferative INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE
Proposed Disease Severity Level No apparent Mild Non- Proliferative Moderate Nonproliferative Severe Non- Proliferative Proliferative INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE
INFORMATION ON DARC: THE DIGITAL ANGIOGRAPHY READING CENTER
 INFORMATION ON DARC: THE DIGITAL ANGIOGRAPHY READING CENTER 1 DIGITAL ANGIOGRAPHY READING CENTER Chairman/Medical Director Jason S. Slakter, M.D. Clinical Professor of Ophthalmology NYU School of Medicine
INFORMATION ON DARC: THE DIGITAL ANGIOGRAPHY READING CENTER 1 DIGITAL ANGIOGRAPHY READING CENTER Chairman/Medical Director Jason S. Slakter, M.D. Clinical Professor of Ophthalmology NYU School of Medicine
We are on WHAT ARE THE RISK FACTORS FOR MACULAR DEGENERATION?
 We are on WHAT ARE THE RISK FACTORS FOR MACULAR DEGENERATION? Age Being 60 years of age and older Race Whites are much more likely to lose vision from AMD than Blacks Gender Women tend to be at greater
We are on WHAT ARE THE RISK FACTORS FOR MACULAR DEGENERATION? Age Being 60 years of age and older Race Whites are much more likely to lose vision from AMD than Blacks Gender Women tend to be at greater
Geographic Atrophy: The Advanced Form of Dry AMD
 Age-related macular degeneration (AMD) is a disease associated with aging that gradually destroys sharp, central vision. Central vision is needed for seeing objects clearly and for common daily tasks such
Age-related macular degeneration (AMD) is a disease associated with aging that gradually destroys sharp, central vision. Central vision is needed for seeing objects clearly and for common daily tasks such
Optic Nerve Imaging. Management of Glaucoma
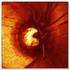 Optic Nerve Imaging in the Diagnosis and Management of Glaucoma Scott D. Smith, MD, MPH Associate Professor of Clinical Ophthalmology Director, Glaucoma Service Columbia University, New York, NY Glaucoma
Optic Nerve Imaging in the Diagnosis and Management of Glaucoma Scott D. Smith, MD, MPH Associate Professor of Clinical Ophthalmology Director, Glaucoma Service Columbia University, New York, NY Glaucoma
Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy
 Medical Care for the Elderly Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy JMAJ 46(1): 27 32, 2003 Shigehiko KITANO Professor, Department of Ophthalmology, Diabetes Center,
Medical Care for the Elderly Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy JMAJ 46(1): 27 32, 2003 Shigehiko KITANO Professor, Department of Ophthalmology, Diabetes Center,
NEW. CIRRUS HD-OCT 5000/500 Advancing Smart OCT. Imaging Applications: Anterior Segment Glaucoma Retina. International Version
 NEW CIRRUS HD-OCT 5000/500 Advancing Smart OCT Imaging Applications: Anterior Segment Glaucoma Retina International Version NEW PanoMap Analysis Wide-field structural damage assessment for glaucoma NEW
NEW CIRRUS HD-OCT 5000/500 Advancing Smart OCT Imaging Applications: Anterior Segment Glaucoma Retina International Version NEW PanoMap Analysis Wide-field structural damage assessment for glaucoma NEW
Diabetic Eye Screening Revised Grading Definitions
 Diabetic Eye Screening Revised Grading Definitions Version 1.3, 1 November 2012 To provide guidance on revised grading definitions for the NHS Diabetic Eye Screening Programme Project/Category Document
Diabetic Eye Screening Revised Grading Definitions Version 1.3, 1 November 2012 To provide guidance on revised grading definitions for the NHS Diabetic Eye Screening Programme Project/Category Document
Screening for Progressive Retinal Atrophy in Tibetan Terriers
 Screening for Progressive Retinal Atrophy in Tibetan Terriers What is PRA? Progressive retinal atrophy (PRA) is the name given to a group of conditions that are inherited and result in a progressive loss
Screening for Progressive Retinal Atrophy in Tibetan Terriers What is PRA? Progressive retinal atrophy (PRA) is the name given to a group of conditions that are inherited and result in a progressive loss
Vitreo-Retinal and Macular Degeneration Frequently Asked Questions
 Vitreo-Retinal and Macular Degeneration Frequently Asked Questions What is a Vitreo-Retinal specialist? Retinal specialists are eye physicians and surgeons who focus on diseases in the back of the eye
Vitreo-Retinal and Macular Degeneration Frequently Asked Questions What is a Vitreo-Retinal specialist? Retinal specialists are eye physicians and surgeons who focus on diseases in the back of the eye
Type 1 neovascularization with polypoidal lesions complicating dome shaped macula
 DOI 10.1186/s40942-015-0008-5 CASE REPORT Open Access Type 1 neovascularization with polypoidal lesions complicating dome shaped macula Jonathan Naysan 1,2,3,4, Kunal K Dansingani 1,2,5, Chandrakumar Balaratnasingam
DOI 10.1186/s40942-015-0008-5 CASE REPORT Open Access Type 1 neovascularization with polypoidal lesions complicating dome shaped macula Jonathan Naysan 1,2,3,4, Kunal K Dansingani 1,2,5, Chandrakumar Balaratnasingam
The Normative Database for the RTVue. Software version 4.0. Michael J. Sinai, PhD
 The Normative Database for the RTVue Software version 4.0 Michael J. Sinai, PhD Glaucoma is a multi-factorial optic neuropathy with characteristic structural changes and subsequent functional impairment.
The Normative Database for the RTVue Software version 4.0 Michael J. Sinai, PhD Glaucoma is a multi-factorial optic neuropathy with characteristic structural changes and subsequent functional impairment.
An Informational Guide to CENTRAL RETINAL VEIN OCCLUSION
 Science of CRVO www.scienceofcrvo.org An Informational Guide to CENTRAL RETINAL VEIN OCCLUSION This brochure will guide you in understanding CRVO and the treatment options available to prevent vision loss.
Science of CRVO www.scienceofcrvo.org An Informational Guide to CENTRAL RETINAL VEIN OCCLUSION This brochure will guide you in understanding CRVO and the treatment options available to prevent vision loss.
Charles C Wykoff, David M Brown, Maria E Maldonado, Daniel E Croft. Clinical science
 Aflibercept treatment for patients with exudative age-related macular degeneration who were incomplete responders to multiple ranibizumab injections (TURF trial) Charles C Wykoff, David M Brown, Maria
Aflibercept treatment for patients with exudative age-related macular degeneration who were incomplete responders to multiple ranibizumab injections (TURF trial) Charles C Wykoff, David M Brown, Maria
MASTER OCT LECTURE OUTLINE Ophthalmic Photographers Society November 16, 2013 New Orleans, LA
 MASTER OCT LECTURE OUTLINE Ophthalmic Photographers Society November 16, 2013 New Orleans, LA Authors: James B Soque, CRA COA and Pamela A Weber, MD Island Retina Shirley, New York OPS COURSE SA 3 B Financial
MASTER OCT LECTURE OUTLINE Ophthalmic Photographers Society November 16, 2013 New Orleans, LA Authors: James B Soque, CRA COA and Pamela A Weber, MD Island Retina Shirley, New York OPS COURSE SA 3 B Financial
ACTVE INTERVENTIONAL CLINICAL TRIALS - 03/01/2015. Principal Investigator Study Title and Sponsor Study Description
 Cornea and External Disease Service Li, Jennifer A Prospective, Multicenter Post-Approval Study (PAS) of VisionCare s Implantable Miniature Telescope (by Dr. Isaac Lipshitz) in Patients with Bilateral
Cornea and External Disease Service Li, Jennifer A Prospective, Multicenter Post-Approval Study (PAS) of VisionCare s Implantable Miniature Telescope (by Dr. Isaac Lipshitz) in Patients with Bilateral
PATIENT INFORMATION BOOKLET
 (060110) VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL END-STAGE AGE-RELATED MACULAR
(060110) VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL END-STAGE AGE-RELATED MACULAR
EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE?
 24. Glaucoma: Imaging EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE? Chief Author: Dr. Amit porwal 1 Co-Authors: Dr. Kavita Porwal 2, Dr. Puja Rai 1 1. Choithram Netralaya,
24. Glaucoma: Imaging EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE? Chief Author: Dr. Amit porwal 1 Co-Authors: Dr. Kavita Porwal 2, Dr. Puja Rai 1 1. Choithram Netralaya,
Ohr Pharmaceutical Reports Fiscal Year 2015 Financial and Business Results
 December 10, 2015 Ohr Pharmaceutical Reports Fiscal Year 2015 Financial and Business Results OHR-102 Phase 3 Program in Wet-AMD to be Initiated Upon Completion of SPA; Enroll Patients in Q1 2016 Conference
December 10, 2015 Ohr Pharmaceutical Reports Fiscal Year 2015 Financial and Business Results OHR-102 Phase 3 Program in Wet-AMD to be Initiated Upon Completion of SPA; Enroll Patients in Q1 2016 Conference
SOCT Copernicus HR Specification
 Specification Light Source: SLED Central Wavelength: 850 nm Axial Resolution: 3 µm Transversal Resolution: 12-18 µm Scanning Speed: 52000 A-Scan per second A-Scan Resolution: 1024 points B-Scan Resolution:
Specification Light Source: SLED Central Wavelength: 850 nm Axial Resolution: 3 µm Transversal Resolution: 12-18 µm Scanning Speed: 52000 A-Scan per second A-Scan Resolution: 1024 points B-Scan Resolution:
Age-Related Macular Degeneration. K. Bailey Freund, M.D. James M. Klancnik, Jr., M.D. Lawrence A. Yannuzzi, M.D. Bruce Rosenthal, O.D.
 Age-Related Macular Degeneration K. Bailey Freund, M.D. James M. Klancnik, Jr., M.D. Lawrence A. Yannuzzi, M.D. Bruce Rosenthal, O.D. Contents Introduction 5 Anatomy of the Eye 6 The Eye 7 The Retina 9
Age-Related Macular Degeneration K. Bailey Freund, M.D. James M. Klancnik, Jr., M.D. Lawrence A. Yannuzzi, M.D. Bruce Rosenthal, O.D. Contents Introduction 5 Anatomy of the Eye 6 The Eye 7 The Retina 9
Measure of Confidence. Glaucoma Module Premium Edition
 Measure of Confidence Glaucoma Module Premium Edition The Changing Face of Glaucoma Practice Literature 1 Leske et al., Arch Ophthalmol 1997; 115:1051-1057 2 Doughty et al., Surv Ophthalmol 2000; 44:367-408
Measure of Confidence Glaucoma Module Premium Edition The Changing Face of Glaucoma Practice Literature 1 Leske et al., Arch Ophthalmol 1997; 115:1051-1057 2 Doughty et al., Surv Ophthalmol 2000; 44:367-408
Facts about diabetic macular oedema
 Patient information medical retina services Facts about diabetic macular oedema What is diabetic macular oedema? Diabetic eye disease is a leading cause of blindness registration among working age adults
Patient information medical retina services Facts about diabetic macular oedema What is diabetic macular oedema? Diabetic eye disease is a leading cause of blindness registration among working age adults
82 Gilbert Street, Adelaide, SA, 5000 82 Gilbert Street, Adelaide, SA, 5000 W +61 8 8104 5293 M +61 417 818 658 W +61 8 8104 5200 M +61 414 661 994
 ASX RELEASE Ellex Medical Lasers Limited (ASX:ELX) Adelaide, Australia Date: 14 September 2015 Release: Immediate Topic: Ellex releases first case study results for 2RT at major tradeshow Adelaide, Australia,
ASX RELEASE Ellex Medical Lasers Limited (ASX:ELX) Adelaide, Australia Date: 14 September 2015 Release: Immediate Topic: Ellex releases first case study results for 2RT at major tradeshow Adelaide, Australia,
Diabetes & blindness. due to DME BLINDNESS IN EUROPE
 Diabetes & blindness due to DME BLINDNESS IN EUROPE Blindness is a life-changing disability which puts a heavy strain on the daily lives of sufferers, their families, and society at large. Today, 284 million
Diabetes & blindness due to DME BLINDNESS IN EUROPE Blindness is a life-changing disability which puts a heavy strain on the daily lives of sufferers, their families, and society at large. Today, 284 million
Completed Clinical Research Trials Prema Abraham, M.D.
 Completed Clinical Research Trials Prema Abraham, M.D. AMD Studies 2010 Present Principal Investigator: A Phase 2, randomized, double-masked, controlled trial to establish the safety and efficacy of intravitreous
Completed Clinical Research Trials Prema Abraham, M.D. AMD Studies 2010 Present Principal Investigator: A Phase 2, randomized, double-masked, controlled trial to establish the safety and efficacy of intravitreous
imagespectrum ADVANCED DIGITAL IMAGE MANAGEMENT SYSTEM Get a Better Handle on the Big Picture.
 imagespectrum ADVANCED DIGITAL IMAGE MANAGEMENT SYSTEM Get a Better Handle on the Big Picture. imagespectrum Securely streamline your practice WORKFLOW WITH imagespectrum. imagespectrum enables eye care
imagespectrum ADVANCED DIGITAL IMAGE MANAGEMENT SYSTEM Get a Better Handle on the Big Picture. imagespectrum Securely streamline your practice WORKFLOW WITH imagespectrum. imagespectrum enables eye care
Assessing the Accuracy of the Technology-based Eye Care Services (TECS) Protocol to a Standard Clinical Ophthalmic Exam
 Assessing the Accuracy of the Technology-based Eye Care Services (TECS) Protocol to a Standard Clinical Ophthalmic Exam Introduction: As patients age, they are more at risk to lose vision. Routine eye
Assessing the Accuracy of the Technology-based Eye Care Services (TECS) Protocol to a Standard Clinical Ophthalmic Exam Introduction: As patients age, they are more at risk to lose vision. Routine eye
When a Macular Hole Is Not A Macular Hole. Contents. OCT Anatomy. Vitreomacular Traction 3/1/2012
 When a Macular Hole Is Not A Macular Hole Salil Shukla, MD Omni Eye Specialists Spring Symposium March 3, 2012 Contents Vitreomacular Traction Epiretinal Membrane Lamellar Hole Macular Hole (Myopic macular
When a Macular Hole Is Not A Macular Hole Salil Shukla, MD Omni Eye Specialists Spring Symposium March 3, 2012 Contents Vitreomacular Traction Epiretinal Membrane Lamellar Hole Macular Hole (Myopic macular
IR Conference Call on EYLEA (aflibercept) Injection in Diabetic Macular Edema. September 28, 2013
 IR Conference Call on EYLEA (aflibercept) Injection in Diabetic Macular Edema September 28, 2013 Safe Harbor Statement This presentation includes forward-looking statements that involve risks and uncertainties
IR Conference Call on EYLEA (aflibercept) Injection in Diabetic Macular Edema September 28, 2013 Safe Harbor Statement This presentation includes forward-looking statements that involve risks and uncertainties
DIABETIC RETINOPATHY. Diabetes mellitus is an abnormality of the blood glucose metabolism due to altered
 DIABETIC RETINOPATHY Diabetes mellitus Diabetes mellitus is an abnormality of the blood glucose metabolism due to altered insulin production or activity. There are two types diabetes mellitus- Insulin
DIABETIC RETINOPATHY Diabetes mellitus Diabetes mellitus is an abnormality of the blood glucose metabolism due to altered insulin production or activity. There are two types diabetes mellitus- Insulin
FDA approves Lucentis (ranibizumab injection) for treatment of diabetic macular edema
 Media Release Basel, 13 August 2012 FDA approves Lucentis (ranibizumab injection) for treatment of diabetic macular edema First major treatment advance in more than 25 years for sight-threatening condition
Media Release Basel, 13 August 2012 FDA approves Lucentis (ranibizumab injection) for treatment of diabetic macular edema First major treatment advance in more than 25 years for sight-threatening condition
Scanners and How to Use Them
 Written by Jonathan Sachs Copyright 1996-1999 Digital Light & Color Introduction A scanner is a device that converts images to a digital file you can use with your computer. There are many different types
Written by Jonathan Sachs Copyright 1996-1999 Digital Light & Color Introduction A scanner is a device that converts images to a digital file you can use with your computer. There are many different types
ICOP 2011 OXFORD UK REPORT ON THE INTERNATIONAL CONFERENCE ON OPHTHALMIC PHOTOGRAPHY 2011
 ICOP 2011 OXFORD UK REPORT ON THE INTERNATIONAL CONFERENCE ON OPHTHALMIC PHOTOGRAPHY 2011 Report compiled by: Rahila Bashir and the MEDICAL IMAGING UK Ltd conference team On September the 22 nd we saw
ICOP 2011 OXFORD UK REPORT ON THE INTERNATIONAL CONFERENCE ON OPHTHALMIC PHOTOGRAPHY 2011 Report compiled by: Rahila Bashir and the MEDICAL IMAGING UK Ltd conference team On September the 22 nd we saw
Title:Clinical and Optic Coherence Tomography Findings of Focal Choroidal Excavation in Chinese Patients
 Author's response to reviews Title:Clinical and Optic Coherence Tomography Findings of Focal Choroidal Excavation in Chinese Patients Authors: Jie Guo ([email protected]) Lu Zhong ([email protected]) Chunhui
Author's response to reviews Title:Clinical and Optic Coherence Tomography Findings of Focal Choroidal Excavation in Chinese Patients Authors: Jie Guo ([email protected]) Lu Zhong ([email protected]) Chunhui
Eye Diseases. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com otf30101 Last reviewed: 05/21/2014 1
 Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
Genetic Testing for Macular Degeneration
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
The Nurse/Technician Role Within the Emerging Ophthalmic Technology - OCTs/B-Scan
 The Nurse/Technician Role Within the Emerging Ophthalmic Technology - OCTs/B-Scan Margie V. Wilson, COMT Chief Clinical Supervisor UCSD Shiley Eye Center Thanks, Carol! Unfortunately. I have not financial
The Nurse/Technician Role Within the Emerging Ophthalmic Technology - OCTs/B-Scan Margie V. Wilson, COMT Chief Clinical Supervisor UCSD Shiley Eye Center Thanks, Carol! Unfortunately. I have not financial
Diabetic macular edema (DME) is the primary cause of
 Retina Fully Software for Retinal Thickness in Eyes With Diabetic Macular Edema From Images Acquired by Cirrus and Spectralis Systems Joo Yong Lee, 1,2 Stephanie J. Chiu, 3 Pratul P. Srinivasan, 3 Joseph
Retina Fully Software for Retinal Thickness in Eyes With Diabetic Macular Edema From Images Acquired by Cirrus and Spectralis Systems Joo Yong Lee, 1,2 Stephanie J. Chiu, 3 Pratul P. Srinivasan, 3 Joseph
OPTICAL COHERENCE TOMOGRAPHY (OCT) IS AN
 Thickness Profiles of Retinal Layers by Optical Coherence Tomography Image Segmentation AHMET MURAT BAGCI, MAHNAZ SHAHIDI, RASHID ANSARI, MICHAEL BLAIR, NORMAN PAUL BLAIR, AND RUTH ZELKHA PURPOSE: To report
Thickness Profiles of Retinal Layers by Optical Coherence Tomography Image Segmentation AHMET MURAT BAGCI, MAHNAZ SHAHIDI, RASHID ANSARI, MICHAEL BLAIR, NORMAN PAUL BLAIR, AND RUTH ZELKHA PURPOSE: To report
Blood Vessel Classification into Arteries and Veins in Retinal Images
 Blood Vessel Classification into Arteries and Veins in Retinal Images Claudia Kondermann and Daniel Kondermann a and Michelle Yan b a Interdisciplinary Center for Scientific Computing (IWR), University
Blood Vessel Classification into Arteries and Veins in Retinal Images Claudia Kondermann and Daniel Kondermann a and Michelle Yan b a Interdisciplinary Center for Scientific Computing (IWR), University
Angiogenesis, Exudation, and Degeneration 2014. February 8, 2014 Mandarin Oriental, Miami, Florida
 Angiogenesis, Exudation, and Degeneration 2014 February 8, 2014 Mandarin Oriental, Miami, Florida Program Directors: Philip J. Rosenfeld, MD, PhD and Harry W. Flynn, Jr., MD Course Associate Director:
Angiogenesis, Exudation, and Degeneration 2014 February 8, 2014 Mandarin Oriental, Miami, Florida Program Directors: Philip J. Rosenfeld, MD, PhD and Harry W. Flynn, Jr., MD Course Associate Director:
16th ESASO Retina Academy Programme
 16th ESASO Retina Academy Programme 23 25 June 2016, Estoril, Portugal THURSDAY, 23 JUNE 2016 14:00 Registration opens Congress hall 14:00 17:30 Poster Hanging 14:00 IMAGING WORKSHOP Room B Imaging Companies
16th ESASO Retina Academy Programme 23 25 June 2016, Estoril, Portugal THURSDAY, 23 JUNE 2016 14:00 Registration opens Congress hall 14:00 17:30 Poster Hanging 14:00 IMAGING WORKSHOP Room B Imaging Companies
ALLEN Mouse Brain Atlas
 TECHNICAL WHITE PAPER: QUALITY CONTROL STANDARDS FOR HIGH-THROUGHPUT RNA IN SITU HYBRIDIZATION DATA GENERATION Consistent data quality and internal reproducibility are critical concerns for high-throughput
TECHNICAL WHITE PAPER: QUALITY CONTROL STANDARDS FOR HIGH-THROUGHPUT RNA IN SITU HYBRIDIZATION DATA GENERATION Consistent data quality and internal reproducibility are critical concerns for high-throughput
Doppler. Doppler. Doppler shift. Doppler Frequency. Doppler shift. Doppler shift. Chapter 19
 Doppler Doppler Chapter 19 A moving train with a trumpet player holding the same tone for a very long time travels from your left to your right. The tone changes relative the motion of you (receiver) and
Doppler Doppler Chapter 19 A moving train with a trumpet player holding the same tone for a very long time travels from your left to your right. The tone changes relative the motion of you (receiver) and
Application of Automated Data Collection to Surface-Enhanced Raman Scattering (SERS)
 Application Note: 52020 Application of Automated Data Collection to Surface-Enhanced Raman Scattering (SERS) Timothy O. Deschaines, Ph.D., Thermo Fisher Scientific, Madison, WI, USA Key Words Array Automation
Application Note: 52020 Application of Automated Data Collection to Surface-Enhanced Raman Scattering (SERS) Timothy O. Deschaines, Ph.D., Thermo Fisher Scientific, Madison, WI, USA Key Words Array Automation
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION
 NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
Alexandria Fairfax Sterling Leesburg 703-931-9100 703-573-8080 703-430-4400 703-858-3170
 DIABETIC RETINOPATHY www.theeyecenter.com This pamphlet has been written to help people with diabetic retinopathy and their families and friends better understand the disease. It describes the cause, symptoms,
DIABETIC RETINOPATHY www.theeyecenter.com This pamphlet has been written to help people with diabetic retinopathy and their families and friends better understand the disease. It describes the cause, symptoms,
Advances in retinal implant technology
 Advances in retinal implant technology Andrew Kuznetsov Freiburg i.br. 3 May 2012 Rhine-Waal University of Applied Sciences, Emmerich Strategies electronic implants (top-down) subretinal implants epiretinal
Advances in retinal implant technology Andrew Kuznetsov Freiburg i.br. 3 May 2012 Rhine-Waal University of Applied Sciences, Emmerich Strategies electronic implants (top-down) subretinal implants epiretinal
Study of the Human Eye Working Principle: An impressive high angular resolution system with simple array detectors
 Study of the Human Eye Working Principle: An impressive high angular resolution system with simple array detectors Diego Betancourt and Carlos del Río Antenna Group, Public University of Navarra, Campus
Study of the Human Eye Working Principle: An impressive high angular resolution system with simple array detectors Diego Betancourt and Carlos del Río Antenna Group, Public University of Navarra, Campus
CR-2 AF and CR-2 PLUS AF Non-Mydriatic cameras. Designed for the highest possible image quality. See the smallest details, don t miss pathology.
 CR-2 AF and CR-2 PLUS AF Non-Mydriatic cameras Designed for the highest possible image quality. See the smallest details, don t miss pathology. CR-2 AF Extremely compact and lightweight (just 15 kg) camera:
CR-2 AF and CR-2 PLUS AF Non-Mydriatic cameras Designed for the highest possible image quality. See the smallest details, don t miss pathology. CR-2 AF Extremely compact and lightweight (just 15 kg) camera:
PRODYNOV. Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI. Image Assisted Laser Therapy for Oncology
 PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
Introduction Houston Retina Associates
 1 2 Introduction This book was written by Houston Retina Associates to provide our patients with basic knowledge about retinal anatomy, an introduction to some of the diagnostic tests and treatments used
1 2 Introduction This book was written by Houston Retina Associates to provide our patients with basic knowledge about retinal anatomy, an introduction to some of the diagnostic tests and treatments used
Femto-LASIK. Pulsewidth: Ultrashort-pulse micro- machining can make sub- wavelength holes. micromachining
 All-laser laser LASIK (Femto( Femto-LASIK) Femto-LASIK 台 大 眼 科 王 一 中 IntraLase 2/1 Perfect Vision Ziemer (DaVinci) Carl Zeiss Meditec Pulsewidth: Femtosecond laser (Nd:Glass)) 153 nm (near infrared) Each
All-laser laser LASIK (Femto( Femto-LASIK) Femto-LASIK 台 大 眼 科 王 一 中 IntraLase 2/1 Perfect Vision Ziemer (DaVinci) Carl Zeiss Meditec Pulsewidth: Femtosecond laser (Nd:Glass)) 153 nm (near infrared) Each
UMHS-PUHSC JOINT INSTITUTE
 Imaging Biomarkers for Staging and Assessing Response to Therapy in Multiple Myeloma Qian Dong, MD. Radiology University of Michigan Wei Guo, MD. Orthopedic Oncology Peking University Second Hospital Team
Imaging Biomarkers for Staging and Assessing Response to Therapy in Multiple Myeloma Qian Dong, MD. Radiology University of Michigan Wei Guo, MD. Orthopedic Oncology Peking University Second Hospital Team
CLINICAL SCIENCES. Enhanced Depth Imaging Optical Coherence Tomography of Small Choroidal Melanoma
 CLINICAL SCIENCES Enhanced Depth Imaging Optical Coherence Tomography of Small Choroidal Melanoma Comparison With Choroidal Nevus Carol L. Shields, MD; Swathi Kaliki, MD; Duangnate Rojanaporn, MD; Sandor
CLINICAL SCIENCES Enhanced Depth Imaging Optical Coherence Tomography of Small Choroidal Melanoma Comparison With Choroidal Nevus Carol L. Shields, MD; Swathi Kaliki, MD; Duangnate Rojanaporn, MD; Sandor
An introduction to Optos
 An introduction to Optos Building The Retina Company Roy Davis, CEO Christine Soden, CFO 1 Forward-Looking Statements Certain statements made in this presentation are forward-looking statements. These
An introduction to Optos Building The Retina Company Roy Davis, CEO Christine Soden, CFO 1 Forward-Looking Statements Certain statements made in this presentation are forward-looking statements. These
Validation and Calibration. Definitions and Terminology
 Validation and Calibration Definitions and Terminology ACCEPTANCE CRITERIA: The specifications and acceptance/rejection criteria, such as acceptable quality level and unacceptable quality level, with an
Validation and Calibration Definitions and Terminology ACCEPTANCE CRITERIA: The specifications and acceptance/rejection criteria, such as acceptable quality level and unacceptable quality level, with an
Current Management of Retinal Vein Occlusion Robert A. Mittra, MD VRS Course 2015
 Central Retinal Vein Occlusion Hemi-Central Vein Occlusion Current Management of Retinal Vein Occlusion Robert A. Mittra, MD VRS Course 2015 Branch Retinal Vein Occlusion Ischemic vs. non-ischemic BRVO
Central Retinal Vein Occlusion Hemi-Central Vein Occlusion Current Management of Retinal Vein Occlusion Robert A. Mittra, MD VRS Course 2015 Branch Retinal Vein Occlusion Ischemic vs. non-ischemic BRVO
THE NEW ENGLAND OPHTHALMOLOGICAL SOCIETY FOR NURSING AND ALLIED HEALTH PERSONNEL. December 13, 2013 INNOVATIONS IN OPHTHALMIC CARE
 THE NEW ENGLAND OPHTHALMOLOGICAL SOCIETY THE 24 th ANNUAL OPHTHALMIC MEETING FOR NURSING AND ALLIED HEALTH PERSONNEL December 13, 2013 INNOVATIONS IN OPHTHALMIC CARE REGISTER HERE: http://www.neos-eyes.org/app/attendee/index.cfm?id=ljfco1v
THE NEW ENGLAND OPHTHALMOLOGICAL SOCIETY THE 24 th ANNUAL OPHTHALMIC MEETING FOR NURSING AND ALLIED HEALTH PERSONNEL December 13, 2013 INNOVATIONS IN OPHTHALMIC CARE REGISTER HERE: http://www.neos-eyes.org/app/attendee/index.cfm?id=ljfco1v
Clinical Applications of Optical Coherence Tomography in Ophthalmology
 11 Clinical Applications of Optical Coherence Tomography in Ophthalmology Upender K. Wali and Nadia Al Kharousi College of Medicine and Health Sciences, Sultan Qaboos University Oman In Ophthalmology,
11 Clinical Applications of Optical Coherence Tomography in Ophthalmology Upender K. Wali and Nadia Al Kharousi College of Medicine and Health Sciences, Sultan Qaboos University Oman In Ophthalmology,
Boomers and Disease Detection with OCT: Catalyst for Optometric Practice Growth
 Boomers and Disease Detection with OCT: Catalyst for Optometric Practice Growth COPE 38496-PD Michael Chaglasian, OD Boomers and Disease Detection with OCT: Catalyst for Optometric Practice Growth Disclosure:
Boomers and Disease Detection with OCT: Catalyst for Optometric Practice Growth COPE 38496-PD Michael Chaglasian, OD Boomers and Disease Detection with OCT: Catalyst for Optometric Practice Growth Disclosure:
The Long-term Effects of Laser Photocoagulation Treatment in Patients with Diabetic Retinopathy
 The Long-term Effects of Laser Photocoagulation Treatment in Patients with Diabetic Retinopathy The Early Treatment Diabetic Retinopathy Follow-up Study Emily Y. Chew, MD, 1 Frederick L. Ferris III, MD,
The Long-term Effects of Laser Photocoagulation Treatment in Patients with Diabetic Retinopathy The Early Treatment Diabetic Retinopathy Follow-up Study Emily Y. Chew, MD, 1 Frederick L. Ferris III, MD,
Processing the Image or Can you Believe what you see? Light and Color for Nonscientists PHYS 1230
 Processing the Image or Can you Believe what you see? Light and Color for Nonscientists PHYS 1230 Optical Illusions http://www.michaelbach.de/ot/mot_mib/index.html Vision We construct images unconsciously
Processing the Image or Can you Believe what you see? Light and Color for Nonscientists PHYS 1230 Optical Illusions http://www.michaelbach.de/ot/mot_mib/index.html Vision We construct images unconsciously
Fundus Photograph Reading Center
 Modified 7-Standard Field Digital Color Fundus Photography (7M-D) 8010 Excelsior Drive, Suite 100, Madison WI 53717 Telephone: (608) 410-0560 Fax: (608) 410-0566 Table of Contents 1. 7M-D Overview... 2
Modified 7-Standard Field Digital Color Fundus Photography (7M-D) 8010 Excelsior Drive, Suite 100, Madison WI 53717 Telephone: (608) 410-0560 Fax: (608) 410-0566 Table of Contents 1. 7M-D Overview... 2
Encoders for Linear Motors in the Electronics Industry
 Technical Information Encoders for Linear Motors in the Electronics Industry The semiconductor industry and automation technology increasingly require more precise and faster machines in order to satisfy
Technical Information Encoders for Linear Motors in the Electronics Industry The semiconductor industry and automation technology increasingly require more precise and faster machines in order to satisfy
Multi-slice Helical CT Scanning of the Chest
 Multi-slice Helical CT Scanning of the Chest Comparison of different low-dose acquisitions Lung cancer is the main cause of deaths due to cancer in human males and the incidence is constantly increasing.
Multi-slice Helical CT Scanning of the Chest Comparison of different low-dose acquisitions Lung cancer is the main cause of deaths due to cancer in human males and the incidence is constantly increasing.
Autonomous Diagnostic Imaging Performed by Untrained Operators using Augmented Reality as a Form of Just in Time Training
 Autonomous Diagnostic Imaging Performed by Untrained Operators using Augmented Reality as a Form of Just in Time Training PROPOSAL TEAM PI: David S. Martin, MS, Wyle Science, Technology, and Engineering
Autonomous Diagnostic Imaging Performed by Untrained Operators using Augmented Reality as a Form of Just in Time Training PROPOSAL TEAM PI: David S. Martin, MS, Wyle Science, Technology, and Engineering
Neuro imaging: looking with lasers in the brain
 Neuro imaging: looking with lasers in the brain Aim: To image life cells, label free, with cellular resolution in deep tissue Marloes Groot Vrije Universiteit Amsterdam Faculteit Exacte Wetenschappen Natuurkunde
Neuro imaging: looking with lasers in the brain Aim: To image life cells, label free, with cellular resolution in deep tissue Marloes Groot Vrije Universiteit Amsterdam Faculteit Exacte Wetenschappen Natuurkunde
Algebra 1 2008. Academic Content Standards Grade Eight and Grade Nine Ohio. Grade Eight. Number, Number Sense and Operations Standard
 Academic Content Standards Grade Eight and Grade Nine Ohio Algebra 1 2008 Grade Eight STANDARDS Number, Number Sense and Operations Standard Number and Number Systems 1. Use scientific notation to express
Academic Content Standards Grade Eight and Grade Nine Ohio Algebra 1 2008 Grade Eight STANDARDS Number, Number Sense and Operations Standard Number and Number Systems 1. Use scientific notation to express
In Proceedings of the Eleventh Conference on Biocybernetics and Biomedical Engineering, pages 842-846, Warsaw, Poland, December 2-4, 1999
 In Proceedings of the Eleventh Conference on Biocybernetics and Biomedical Engineering, pages 842-846, Warsaw, Poland, December 2-4, 1999 A Bayesian Network Model for Diagnosis of Liver Disorders Agnieszka
In Proceedings of the Eleventh Conference on Biocybernetics and Biomedical Engineering, pages 842-846, Warsaw, Poland, December 2-4, 1999 A Bayesian Network Model for Diagnosis of Liver Disorders Agnieszka
Essentials in Diagnostic Testing in the Retina Practice Riva Lee Asbell
 Essentials in Diagnostic Testing in the Retina Practice Riva Lee Asbell INTRODUCTION Coding and billing for diagnostic testing is a major part of ophthalmic practices in general, but more so in some of
Essentials in Diagnostic Testing in the Retina Practice Riva Lee Asbell INTRODUCTION Coding and billing for diagnostic testing is a major part of ophthalmic practices in general, but more so in some of
SHEEP EYE DISSECTION PROCEDURES
 SHEEP EYE DISSECTION PROCEDURES The anatomy of the human eye can be better shown and understood by the actual dissection of an eye. One eye of choice for dissection, that closely resembles the human eye,
SHEEP EYE DISSECTION PROCEDURES The anatomy of the human eye can be better shown and understood by the actual dissection of an eye. One eye of choice for dissection, that closely resembles the human eye,
NAVILAS Laser System Focal Laser Treatment for Diabetic Macular Edema - One Year Results of a Case Series
 Send Orders for Reprints to [email protected] 48 The Open Ophthalmology Journal, 2013, 7, 48-53 Open Access NAVILAS Laser System Focal Laser Treatment for Diabetic Macular Edema - One Year Results
Send Orders for Reprints to [email protected] 48 The Open Ophthalmology Journal, 2013, 7, 48-53 Open Access NAVILAS Laser System Focal Laser Treatment for Diabetic Macular Edema - One Year Results
Study Design and Statistical Analysis
 Study Design and Statistical Analysis Anny H Xiang, PhD Department of Preventive Medicine University of Southern California Outline Designing Clinical Research Studies Statistical Data Analysis Designing
Study Design and Statistical Analysis Anny H Xiang, PhD Department of Preventive Medicine University of Southern California Outline Designing Clinical Research Studies Statistical Data Analysis Designing
Research Methods & Experimental Design
 Research Methods & Experimental Design 16.422 Human Supervisory Control April 2004 Research Methods Qualitative vs. quantitative Understanding the relationship between objectives (research question) and
Research Methods & Experimental Design 16.422 Human Supervisory Control April 2004 Research Methods Qualitative vs. quantitative Understanding the relationship between objectives (research question) and
16th ESASO Retina Academy Programme
 16th ESASO Retina Academy Programme 23 25 June 2016, Estoril, Portugal THURSDAY, 23 JUNE 2016 14:00 Registration opens Congress hall 14:00 17:30 Poster display 14:00 17:30 IMAGING WORKSHOP Room B Technical
16th ESASO Retina Academy Programme 23 25 June 2016, Estoril, Portugal THURSDAY, 23 JUNE 2016 14:00 Registration opens Congress hall 14:00 17:30 Poster display 14:00 17:30 IMAGING WORKSHOP Room B Technical
II. DISTRIBUTIONS distribution normal distribution. standard scores
 Appendix D Basic Measurement And Statistics The following information was developed by Steven Rothke, PhD, Department of Psychology, Rehabilitation Institute of Chicago (RIC) and expanded by Mary F. Schmidt,
Appendix D Basic Measurement And Statistics The following information was developed by Steven Rothke, PhD, Department of Psychology, Rehabilitation Institute of Chicago (RIC) and expanded by Mary F. Schmidt,
A concise guide to Safety Glasses, the different standards and the effects of light on the eye. Contents. Links. Year of publication: 2010
 A concise guide to Safety Glasses, the different standards and the effects of light on the eye Year of publication: 2010 Produced by the leading supplier of Safety Glasses in the UK. All Rights Reserved.
A concise guide to Safety Glasses, the different standards and the effects of light on the eye Year of publication: 2010 Produced by the leading supplier of Safety Glasses in the UK. All Rights Reserved.
Care of the Patient with Age-Related Macular Degeneration
 OPTOMETRIC CLINICAL PRACTICE GUIDELINE Care of the Patient with Age-Related Macular Degeneration OPTOMETRY: THE PRIMARY EYE CARE PROFESSION Doctors of optometry are independent primary health care providers
OPTOMETRIC CLINICAL PRACTICE GUIDELINE Care of the Patient with Age-Related Macular Degeneration OPTOMETRY: THE PRIMARY EYE CARE PROFESSION Doctors of optometry are independent primary health care providers
Long-Term Outcomes of Flap Amputation After LASIK
 Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
Long-Term Outcomes of Flap Amputation After LASIK Priyanka Chhadva BS, Florence Cabot MD, Anat Galor MD, Sonia H. Yoo MD Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami
OHTAC Recommendation
 OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
