PATIENT INFORMATION BOOKLET
|
|
|
- Janice Hodge
- 9 years ago
- Views:
Transcription
1 (060110) VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL END-STAGE AGE-RELATED MACULAR DEGENERATION PATIENT INFORMATION BOOKLET IMPORTANT INFORMATION This booklet will help you decide whether or not to have surgery to implant the Implantable Miniature Telescope (by Dr. Isaac Lipshitz) (intraocular telescope) in your eye to reduce the effects of your vision impairment from age-related macular degeneration. Please read the whole booklet. Discuss it thoroughly with your eye doctor, your surgeon, your family and your friends until you get answers to all your questions. You need to understand the risks and benefits of implanting the intraocular telescope before you decide to have the surgery. You and your doctor must both complete the Acceptance of Risk and Informed Decision Agreement before you can have the surgery. VisionCare Ophthalmic Technologies, Inc Saratoga Avenue, Suite 150 Saratoga, CA Phone: Fax:
2 PATIENT INFORMATION BOOKLET PAGE 1 OF 17 PATIENT INFORMATION BOOKLET VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) TABLE OF CONTENTS GLOSSARY... 3 INTRODUCTION... 5 Information about the Eye and Age-Related Macular Degeneration (AMD)... 5 What Does the Intraocular Telescope Do?... 6 How Does the Intraocular Telescope Work?... 6 ARE YOU A CANDIDATE FOR THE INTRAOCULAR TELESCOPE?... 6 ARE YOU SOMEONE WHO SHOULD NOT HAVE AN INTRAOCULAR TELESCOPE?... 7 CLINICAL STUDIES... 7 WHAT ARE THE RISKS OF THE INTRAOCULAR TELESCOPE?... 7 WHAT ARE THE BENEFITS OF THE INTRAOCULAR TELESCOPE?... 9 WHAT OTHER QUESTIONS SHOULD YOU CONSIDER BEFORE INTRAOCULAR TELESCOPE SURGERY? Is There a Way to See What Your Vision Will be Like With the Intraocular Telescope Before the Surgery to Help You Decide if the Intraocular Telescope May Work for You? Will You Need Training to Learn How to Use Your Intraocular Telescope? Are There Other Options You Could Use Instead of the Intraocular Telescope? What About Lucentis and Other Drugs? Can You Use Them Instead? WHAT TO EXPECT WITH THE SURGICAL PROCEDURE? Before the Surgery The Day of Surgery After the Surgery Will You Need Glasses after Implantation of the Intraocular Telescope? Will You Be Able to Drive after Implantation of the Intraocular Telescope? WHO SHOULD YOU TALK TO ABOUT YOUR QUESTIONS?... 12
3 PATIENT INFORMATION BOOKLET PAGE 2 OF 17 TABLE OF CONTENTS (CONTINUED) ACCEPTANCE OF RISK AND INFORMED DECISION AGREEMENT INFORMATION PATIENT ASSISTANCE INFORMATION INDEX ACCEPTANCE OF RISK AND INFORMED DECISION AGREEMENT... 15
4 PATIENT INFORMATION BOOKLET PAGE 3 OF 17 GLOSSARY Age-Related Macular Degeneration (AMD): an eye disease in older individuals that destroys sharp, central vision by damaging the retina. AMD makes it hard to read and recognize faces. Bilateral AMD: AMD in both eyes. Cataract: the natural lens of the eye becomes cloudy, causing hazy vision. Central vision: ability to see straight ahead for reading, recognizing faces, or seeing details. Contrast sensitivity: how well your eyes function in low light and how well you can distinguish one object from another or from the background. Cornea: the clear front portion of the eye. Corneal edema: swelling of the cornea that can make it cloudy and cause blurred vision. Corneal endothelial cells: layer of cells on the inside of the cornea that keeps the cornea healthy and transparent by controlling the amount of fluid in it; if you lose too many corneal endothelial cells due to eye surgery or disease, your cornea can become cloudy and cause blurred vision. Corneal transplant: replacement of your cornea with a new cornea from an organ donor. Depth perception: the ability to see in three dimensions and to identify how far away an object is. End-stage AMD: advanced AMD causing severe central vision loss that is not treatable by medication or laser surgery. External telescope: a hand-held or externally worn telescope used to magnify objects. Field of view: the angle of view from the center to the sides when looking forward, for example, 180 degrees of vision. Implantable Miniature Telescope ( intraocular telescope ): a very small telescope that is surgically implanted in the eye after removing the natural lens. An intraocular telescope magnifies images and is intended to improve central vision in patients with end-stage AMD. Intraocular: inside the eye. Intraocular lens (IOL): a very small lens implanted in the eye to replace a cloudy natural lens during cataract surgery.
5 PATIENT INFORMATION BOOKLET PAGE 4 OF 17 GLOSSARY (CONTINUED) Lens or Natural Lens: transparent structure inside the eye behind the iris that focuses light onto the retina to create an image. Macula: the central part of the retina at the back of the eye that is responsible for central vision. Peripheral vision: vision outside the center of gaze, on the sides. Profound vision impairment: vision 20/400 or worse. Retina: the light sensitive inner layer of the eye that is responsible for sight. Severe vision impairment: vision 20/160 to less than 20/400. Visual acuity: a measure of how well someone can see, for example, 20/20 or 20/200. Wet AMD: abnormal blood vessels under the retina that leak blood and fluid that cause damage to the retina.
6 PATIENT INFORMATION BOOKLET PAGE 5 OF 17 INTRODUCTION If you are thinking about having surgery to have the Implantable Miniature Telescope (by Dr. Isaac Lipshitz), also called the intraocular telescope, placed in your eye, please read this Patient Information Booklet carefully. You may want a friend or family member to read it to you. You may want to discuss it with your family and friends. You should ask questions of your eye doctor, your surgeon and the eye care professionals who work with your eye doctor and surgeon. Take all the time you need to thoroughly consider and understand the information and get all your questions answered. The intraocular telescope has potential benefits and potential risks. Only you can decide whether intraocular telescope surgery is a good option for improving your vision. Information about the Eye and Age-Related Macular Degeneration (AMD) The eye acts like a camera to focus light from outside the eye to form images or pictures on the surface of the retina. Light enters the eye through the cornea and lens which focus the light onto the retina. The macula is located in the center of the retina. The macula provides central vision. Central vision allows you to see objects clearly and to do common daily tasks such as reading and recognizing faces. AMD is a disease related to aging that gradually destroys the macula and therefore central vision. Figure 1 shows a picture of the inside of the eye. FIGURE 1 CROSS SECTION OF THE EYE
7 PATIENT INFORMATION BOOKLET PAGE 6 OF 17 What Does the Intraocular Telescope Do? The intraocular telescope is intended to improve distance and near vision in people who have lost central vision in both eyes because of end-stage AMD. The intraocular telescope is about the size of a pea and is surgically placed inside one eye. The implanted eye provides central vision. The other eye provides peripheral vision. A picture of the intraocular telescope is shown in Figure 2. FIGURE 2: IMPLANTABLE MINIATURE TELESCOPE (BY DR. ISAAC LIPSHITZ) How Does the Intraocular Telescope Work? When implanted in your eye, the intraocular telescope magnifies images and projects them onto a part of your retina that is healthy and can still see images. ARE YOU A CANDIDATE FOR THE INTRAOCULAR TELESCOPE? You are a candidate if you meet these criteria: You have end-stage AMD in both eyes. You are at least 75 years old. Your distance vision is no better than 20/160 but no worse than 20/800. You have cataract. You show improvement on an eye test chart using an external telescope. You agree to pre-surgery training with external telescopes with a low vision specialist long enough to make an informed decision. You agree to training with a low vision specialist after intraocular telescope surgery. You are informed of the intraocular telescope s risks and benefits. You understand and sign the Acceptance of Risk and Informed Decision Agreement for the intraocular telescope surgery.
8 PATIENT INFORMATION BOOKLET PAGE 7 OF 17 ARE YOU SOMEONE WHO SHOULD NOT HAVE AN INTRAOCULAR TELESCOPE? You should not have intraocular telescope surgery if: You have already had surgery in the same eye. You have poor peripheral vision in the other eye. You have uncontrolled glaucoma. You rub your eyes. Rubbing your eye after surgery could damage both the cornea and the intraocular telescope. Your eye doctor says you have a disease or condition that would make you a poor candidate. You should discuss your medical and vision history completely with your eye doctor. Only you, with the help of your eye doctor, surgeon, friends, and family, can decide whether to have the intraocular telescope implanted. If the potential benefits are more important to you than the risks, then you should ask your doctor if you are a good candidate for the intraocular telescope. If the risks seem greater to you than the potential benefits, you should let your doctor know that you do not want to have an intraocular telescope. CLINICAL STUDIES The following sections (What are the Risks of The Intraocular Telescope and What are the Benefits of the Intraocular Telescope) give the results of clinical studies of the intraocular telescope. 217 patients with vision impairment due to end-stage AMD in both eyes were studied at 28 U.S. centers to evaluate the safety and effectiveness of the intraocular telescope. Patients averaged 76 years of age, about half were female and half were male, and most were Caucasian. WHAT ARE THE RISKS OF THE INTRAOCULAR TELESCOPE? This section talks about the risks of having intraocular telescope surgery and about the risks of having the intraocular telescope during the 5 years after surgery. There may be other risks that were not detected in the studies, and the long-term risks of having the intraocular telescope more than 5 years are unknown. Surgery. After surgery has started, your surgeon may not be able to implant the intraocular telescope. If this happens, an intraocular lens (IOL) will be implanted instead. You will have all the risks of the surgery but without any of the benefits of the intraocular telescope. About 5% (1 out of 20) of patients had this problem. Corneal Edema. You may develop corneal edema, which is swelling of the cornea. Intraocular telescope surgery will cause you to lose some corneal endothelial cells immediately, and afterward you will continue to lose more cells over time than normally happens with aging. Once you lose corneal endothelial cells, they do not grow back.
9 PATIENT INFORMATION BOOKLET PAGE 8 OF 17 During the 5-year period after intraocular telescope surgery, about 12% of patients had very low corneal endothelial cell density, which can cause corneal edema to develop. Corneal edema is usually not painful except in very severe cases. If corneal edema is persistent (does not go away) and becomes bad enough to impair your vision, you may need a corneal transplant. It may also be necessary to remove the intraocular telescope during the corneal transplant surgery. Persistent corneal edema and persistent vision-impairing corneal edema are serious conditions that do not get better over time. Implanting the intraocular telescope in your eye will increase your risk of getting persistent corneal edema, which can progress to persistent vision-impairing corneal edema or the need for a corneal transplant. The risks of these events reported over a 5-year period of time are shown in Table 1. Persistent Corneal Edema TABLE 1 RISK OVER 5 YEARS Persistent Vision- Impairing Corneal Edema Corneal Transplant 9% 7% 4% Vision Loss. Your vision may get worse. The risk of losing more than 2 lines of vision on the eye chart was about 12% over the 5 years following intraocular telescope surgery. Also, 48% of patients in the study reported that their vision-related quality of life either stayed the same or got worse after intraocular telescope surgery. Removing the Intraocular Telescope. If you are unhappy with your vision after intraocular telescope surgery, you may want to have your eye surgeon remove the intraocular telescope. This requires another surgery with risks that are at least as high as the risks of the surgery to implant the intraocular telescope. The surgery to remove the intraocular telescope may cause additional loss of corneal endothelial cells, which may lead to corneal edema. During the 5-year period after intraocular telescope surgery, about 4% of patients had their intraocular telescope removed and replaced with an intraocular lens. Some Other Risks of Intraocular Telescope Surgery: double vision inability or difficulty controlling when to switch from using one eye to the other decreased peripheral vision in the eye with the intraocular telescope bleeding in the eye due to surgery infection inside the eye decrease in contrast sensitivity the need to surgically remove the intraocular telescope if it breaks inside your eye medical or visual complications dizziness or a queasy feeling
10 PATIENT INFORMATION BOOKLET PAGE 9 OF 17 changes in depth perception difficulty seeing in dim light difficulty seeing in bright light cloudy or blurred vision that makes it hard to see difference in speed of motion of the images in the two eyes, when the eyes are moved together. If you have intraocular telescope surgery, you should have a complete annual eye examination that includes checking your corneal endothelial cells. The annual examination will help you know whether any of the risks discussed in this section are happening to you. WHAT ARE THE BENEFITS OF THE INTRAOCULAR TELESCOPE? This section talks about the potential benefits of having intraocular telescope surgery. The intraocular telescope may improve your vision (the ability to see) and may improve your vision-related quality of life. Vision Improvement. Most patients implanted with the intraocular telescope had significant improvement in vision. At 1 and 2 years after surgery, about 75% of patients had an improvement in their distance visual acuity of 2-lines or more on the eye chart. A 2-line improvement would be from 20/200 to 20/125 or from 20/400 to 20/250. About 60% of patients improved their distance vision by 3-lines or more on the eye chart. About 40% of patients improved their vision by 4-lines or more. Improvements in distance and near vision were similar. There was a slight decline in visual acuity at 3 and 4 years after surgery. However, improvements in vision after intraocular telescope surgery are generally retained over time. Results beyond 5 years are unknown. Vision-Related Quality of Life Improvement. The majority (52%) of patients implanted with the intraocular telescope reported improvement in their vision-related quality of life. This means that they were more able to carry out activities that required distance or near vision. It also means they were more able to take part in social activities, and to independently carry out the activities of daily life. Other benefits include: Eye movements are normal with the intraocular telescope. Because the intraocular telescope is implanted inside your eye, whatever you are looking at can be followed with natural eye movements rather than by turning your head.
11 PATIENT INFORMATION BOOKLET PAGE 10 OF 17 WHAT OTHER QUESTIONS SHOULD YOU CONSIDER BEFORE INTRAOCULAR TELESCOPE SURGERY? Is There a Way to See What Your Vision Will Be Like With the Intraocular Telescope Before the Surgery to Help You to Decide if the Intraocular Telescope May Work for You? Yes. Before you decide whether to have intraocular telescope surgery, you will meet with low vision specialists to use an external telescope to see if your vision improves when using the external telescope. Using the external telescope will help you understand what it could be like to have an intraocular telescope in your eye. You will be asked to use the external telescope for as long as you need to see what the intraocular telescope will be like in your activities of daily living. You need to do this even if you have used external telescopes before. If you do not like your vision with the external telescope or your vision does not improve, you should not have the intraocular telescope implanted in your eye. Your eye doctor will recommend low vision specialists to you. The low vision specialists will check your vision. They will show you how to use the external telescope and help you understand what your vision will be like with the intraocular telescope implanted in your eye. The specialists will work with you to see whether or not you are able to adjust to the magnification to improve your vision. They will discuss your functional goals (what you want to be able to do) and evaluate them with you. Most people will need 2 to 4 meetings with the low vision specialists. The meetings will be about thirty minutes to an hour long. The external telescope will only determine if you will respond to magnification. Your ability to use the external telescope does not guarantee that you will be able to successfully use the intraocular telescope. Will You Need Training to Learn How to Use Your Intraocular Telescope? Yes. After you have surgery to implant your intraocular telescope, you will need to attend several training sessions with low vision specialists. The specialists will create a plan of care for you based on your individual situation and functional goals. The low vision specialists will work with you to teach you how to do your daily activities with your new intraocular telescope. Visits with the low vision specialists are important to getting the most benefit from your intraocular telescope. Each session will be thirty minutes to one hour long. Are There Other Options You Could Use Instead of the Intraocular Telescope? Yes. You can use handheld external telescopes, spectacle-mounted telescopes, or special magnifying eyeglasses instead of the intraocular telescope. You should discuss these options with your doctor. What About Lucentis and Other Drugs? Can You Use Them Instead? No. Lucentis is a medication used for earlier stages of AMD, called wet AMD. It is not used for your stage of AMD, which is called end-stage AMD. The intraocular telescope is intended to be used when Lucentis is no longer effective.
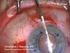
12 PATIENT INFORMATION BOOKLET PAGE 11 OF 17 WHAT TO EXPECT WITH THE SURGICAL PROCEDURE? Before the Surgery Before the surgery, your surgeon will get your medical history and check the health of both of your eyes. Tell your surgeon if you take any medication or have any allergies. Be sure to discuss all your questions with your surgeon before scheduling your surgery. Ask your surgeon if you should eat or drink right before the surgery. You should arrange for transportation to and from where you live. The Day of Surgery Surgery will be performed in an outpatient surgical setting. You should plan on 2 to 3 hours for surgical preparation, the surgery, and recovery period. You will remain awake during surgery. Your eye will be numbed at the beginning of the surgery so you will not feel any pain. You will get special eye drops to enlarge the pupil. Your eye will be held open with a special instrument, and an operating microscope will be placed in front of your eye. Your eye s natural lens will be removed. The intraocular telescope will then be implanted inside your eye in the same position where the natural lens was. The numbness will wear off after surgery. If your surgeon is unable to implant the intraocular telescope during surgery, your surgeon will implant an intraocular lens (IOL). After the Surgery After the intraocular telescope is implanted you will be provided with several types of eye drops to use at home. These eye drops will prevent infection and reduce redness, burning and swelling. You will be provided instructions on when to use the medications and how long to use them. Your surgeon may also give you a protective eye patch to use over the first few days (2 to 5 days) after your surgery. Your surgeon may tell you to limit certain activities for several weeks after the surgery. You will be asked to return for an eye exam one day after surgery, to make sure that you are recovering as expected. You should follow all of your surgeon s instructions. They are important. This includes using the eye medications and eye patch as your doctor directs. If you have a sudden worsening of your vision you should contact your doctor as soon as possible. You should expect improvement in central vision in the intraocular telescope implanted eye to occur over a period of time, from weeks to months. Do NOT RUB YOUR EYE after the intraocular telescope has been implanted inside your eye. You should not rub your eye for the rest of your life, not just in the immediate postoperative period. Rubbing your eye can damage the corneal endothelial cells. Damaging the corneal endothelial cells can lead to corneal edema and the need for a corneal transplant.
13 PATIENT INFORMATION BOOKLET PAGE 12 OF 17 Will You Need Glasses after Implantation of the Intraocular Telescope? Yes, you will probably need glasses to adjust both your distance and near vision. Will You Be Able to Drive after Implantation of the Intraocular Telescope? No. Even with both an intraocular telescope and glasses, you will not be able to drive a car. Your vision will not be good enough (20/40 in most states). WHO SHOULD YOU TALK TO ABOUT YOUR QUESTIONS? You should talk to your eye doctor, the surgeon to whom your eye doctor has referred you, the eye care professionals in their offices and your family and friends. This Patient Information Booklet provides you with information by asking and answering many questions about the intraocular telescope. In addition, here are a few questions you may want to ask your eye doctor, surgeon or other professionals: What are the benefits of the intraocular telescope for my end-stage AMD? What are the risks of the intraocular telescope? Are there other options for treating my end-stage AMD? What is the possibility that the intraocular telescope will not improve my central vision? What vision problems may happen with the intraocular telescope implanted in one eye? Do I have any conditions that would increase my risk of problems from intraocular telescope surgery? Will I be able to drive after getting the intraocular telescope? If I am not satisfied with the results after intraocular telescope surgery, will it be necessary for me to have another surgery to remove the intraocular telescope? Based on my age and the condition of my cornea, what is my risk of needing a corneal transplant in the future if I have intraocular telescope surgery? What could happen if I rub my eye after intraocular telescope surgery? Is the intraocular telescope fragile? Can it break in my eye? What would happen if the intraocular telescope breaks? How much will the surgery and follow-up cost? Will my health insurance cover this surgery? ACCEPTANCE OF RISK AND INFORMED DECISION AGREEMENT INFORMATION You will be given an Acceptance of Risk and Informed Decision Agreement for review and discussion with your eye surgeon. If you accept each risk and sign the Agreement, it means you have decided to have intraocular telescope surgery. You must complete the form by accepting each risk and sign the Agreement before you can have intraocular telescope surgery.
14 PATIENT INFORMATION BOOKLET PAGE 13 OF 17 PATIENT ASSISTANCE INFORMATION Your eye doctor will fill this in so you will know whom to contact if you have any questions about or problems with the intraocular telescope. EYE DOCTOR Name: Address: Telephone No: SURGEON IMPLANTING THE INTRAOCULAR TELESCOPE Name: Address: Telephone No: SURGERY LOCATION: Name: Address: Telephone No: VisionCare Ophthalmic Technologies, Inc Saratoga Avenue, Suite 150 Saratoga, CA Phone: Fax:
15 PATIENT INFORMATION BOOKLET PAGE 14 OF 17 INDEX A Age-related macular degeneration, AMD, 3, 5 Acceptance of Risk and Informed Decision Agreement, 6, 12, 15, 16, 17 J S Sensitivity, 3, 8 Severe vision impairment, 4 B Bilateral AMD, 3 Bleeding, 8 K T Training, 6, 10, 15, 16 C Cataract, 3, 6 Central vision, 3, 4, 5, 6, 11, 12, 15 Contrast sensitivity, 3, 8 Cornea, 3, 5, 7, 12 Corneal edema, 3, 7, 8, 11, 16 Corneal transplant, 3, 8, 11, 12, 16 L Lens, 3, 4, 5, 11 Lucentis, 10 Low vision specialist, 6, 10 U D Depth perception, 3, 9 Double vision, 8, 15 Drive, 12 E End-stage AMD, 3, 6, 7, 10, 12 External telescope, 3, 6, 10, 15, 17 M Macula, 4, 5 V Visual acuity, 4, 9 N Natural lens, 3, 4, 11 W Wet AMD, 4, 10 F Field of view, 3, 15 O X G P Peripheral vision, 4, 6, 7, 8, 15 Profound vision impairment, 4 Y H Q Quality of life, 8, 9 Z I Implantable Miniature Telescope or intraocular telescope, 3, 5, 6, 7, 8, 9, 10, 11, 12, 13, 15, 16, 17 Infection, 8, 11 Intraocular lens (IOL) 3, 7, 8, 9, 11, 16, 17 R Retina, 3, 4, 5, 6 Risk, 5, 6, 7, 8, 9, 12, 15,16, 17
16 PATIENT INFORMATION BOOKLET PAGE 15 OF 17 ACCEPTANCE OF RISK AND INFORMED DECISION AGREEMENT To the patient: This is the last step in deciding whether you want to have intraocular telescope surgery. This Agreement lists important risks of intraocular telescope surgery. Please review this Agreement carefully with your eye surgeon. You should sign this Agreement only if you are satisfied that each risk has been explained to you and you understand and accept each risk. If you accept each risk and sign the Agreement, it means you have decided to have intraocular telescope surgery. You must accept each risk and sign the Agreement before you can have intraocular telescope surgery. To the eye surgeon: Please review this Agreement carefully with your patient. For each item, initial if you are satisfied that the patient understands the item and has accepted it. Your signature confirms that the patient has completed and signed the Agreement. Patient Initials Physician Initials I understand that the intraocular telescope is implanted in only one eye. The eye with the intraocular telescope provides central vision. I will need to use my other eye for peripheral vision when I want to walk around. I used an external telescope to see if my vision would improve with magnification and it did. I find the vision acceptable. I had training in the use of an external telescope to see whether I can adjust to using one eye for central vision and the other eye for peripheral vision. I was able to do this with practice. I understand that my ability to use the external telescope does not guarantee that I will be able to successfully use the intraocular telescope. The field of view in the eye implanted with the intraocular telescope is restricted. I understand that I will lose peripheral vision in the eye implanted with the intraocular telescope and that I will need to rely on my other eye for peripheral vision. I understand that I may experience double vision after intraocular telescope surgery.
17 PATIENT INFORMATION BOOKLET PAGE 16 OF 17 ACCEPTANCE OF RISK AND INFORMED DECISION AGREEMENT (continued) Patient Initials Physician Initials I understand that if I have intraocular telescope surgery, I will need training to learn to use the intraocular telescope. I agree to attend such training. I understand that after intraocular telescope surgery, I will probably need glasses to adjust my near and distance vision. I understand there may be problems during surgery that may prevent my surgeon from implanting the intraocular telescope. If this happens, I understand that I may receive an intraocular lens (IOL) instead of the intraocular telescope. This means that I will have all the surgical risks, but I will not get the benefits of the intraocular telescope. I understand that instead of the intraocular telescope improving my vision, my vision could get worse. I understand that with the intraocular telescope implanted in my eye, my eye doctor may not be able to see parts of my eye or perform some procedures I may need in the future. I understand that having the intraocular telescope could cause corneal edema. This could happen at any time, even 5 or more years after my surgery, and require me to have corneal transplant surgery. If I have to have a corneal transplant, I understand that I may not be able to keep the intraocular telescope in my eye. My eye surgeon gave me the Patient Information Booklet on the intraocular telescope. I have had the chance to discuss the information in the Patient Information Booklet with my eye doctor, my eye surgeon, my family and my friends.
18 PATIENT INFORMATION BOOKLET PAGE 17 OF 17 ACCEPTANCE OF RISK AND INFORMED DECISION AGREEMENT (CONTINUED) I have had enough time to read and understand the information in the Patient Information Booklet. My eye doctor and eye surgeon have answered my questions. I have considered alternatives to the intraocular telescope such as external telescopes, spectacle mounted telescopes, and special magnifying eyeglasses. I choose to proceed with surgery to implant the intraocular telescope. Patient Name (Printed): Patient Signature: Date: Surgeon Name (Printed): Surgeon Signature: Date: Witness Name (Printed): Witness Signature: Date:
Patient Information Cataract surgery
 Patient Information Cataract surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Patient Information Cataract surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Eye Diseases. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com otf30101 Last reviewed: 05/21/2014 1
 Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
Patient information factsheet. Cataract surgery. Consent for cataract surgery
 Patient information factsheet Cataract surgery Consent for cataract surgery This leaflet gives you information that will help you decide whether to have cataract surgery. You might want to discuss it with
Patient information factsheet Cataract surgery Consent for cataract surgery This leaflet gives you information that will help you decide whether to have cataract surgery. You might want to discuss it with
CONSENT FORM. Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
BACKGROUND INFORMATION AND INFORMED CONSENT FOR CATARACT SURGERY AND IMPLANTATION OF AN INTRAOCULAR LENS
 OMNI EYE SPECIALISTS A Madison Street Company Proudly Owned by Employees Specializing in Medical and Surgical Care of the Eye 55 Madison St, Suite 355 Denver CO 80206 303-377-2020 800-GO-2-OMNI www.omnieye.com
OMNI EYE SPECIALISTS A Madison Street Company Proudly Owned by Employees Specializing in Medical and Surgical Care of the Eye 55 Madison St, Suite 355 Denver CO 80206 303-377-2020 800-GO-2-OMNI www.omnieye.com
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK)
 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
Alexandria Fairfax Sterling Leesburg 703-931-9100 703-573-8080 703-430-4400 703-858-3170
 DIABETIC RETINOPATHY www.theeyecenter.com This pamphlet has been written to help people with diabetic retinopathy and their families and friends better understand the disease. It describes the cause, symptoms,
DIABETIC RETINOPATHY www.theeyecenter.com This pamphlet has been written to help people with diabetic retinopathy and their families and friends better understand the disease. It describes the cause, symptoms,
Seeing Beyond the Symptoms
 Seeing Beyond the Symptoms Cataracts are one of the leading causes of vision impairment in the United States. 1 However, because cataracts form slowly and over a long period of time, many people suffer
Seeing Beyond the Symptoms Cataracts are one of the leading causes of vision impairment in the United States. 1 However, because cataracts form slowly and over a long period of time, many people suffer
Understanding cataract. The Eye Service at Barts Health
 Understanding cataract The Eye Service at Barts Health What is a cataract? If your doctor or optometrist/optician has told you that you have a cataract, do not be alarmed. Many people develop cataracts
Understanding cataract The Eye Service at Barts Health What is a cataract? If your doctor or optometrist/optician has told you that you have a cataract, do not be alarmed. Many people develop cataracts
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY
 INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
Avastin (Bevacizumab) Intravitreal Injection
 Avastin (Bevacizumab) Intravitreal Injection This handout describes how Avastin may be used to treat wet age related macular degeneration (AMD) or macular edema due to retinal vascular disease such as
Avastin (Bevacizumab) Intravitreal Injection This handout describes how Avastin may be used to treat wet age related macular degeneration (AMD) or macular edema due to retinal vascular disease such as
Explanation of the Procedure
 Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
Tucson Eye Care, PC. Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens
 Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Guide to Cataract Surgery
 Guide to Cataract Surgery According to Prevent Blindness America s Vision Problems in the U.S. report, more than 24 million Americans age 40 and older have cataract. By age 80, more than half of all Americans
Guide to Cataract Surgery According to Prevent Blindness America s Vision Problems in the U.S. report, more than 24 million Americans age 40 and older have cataract. By age 80, more than half of all Americans
How To Treat Eye Problems With A Laser
 1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
VISION LOSS EVERYTHING YOU WANTED TO KNOW BUT WERE AFRAID TO ASK!
 VISION LOSS EVERYTHING YOU WANTED TO KNOW BUT WERE AFRAID TO ASK! People with vision loss can continue to lead productive, dignified and fulfilling lives. We can help. What will I learn from this booklet?
VISION LOSS EVERYTHING YOU WANTED TO KNOW BUT WERE AFRAID TO ASK! People with vision loss can continue to lead productive, dignified and fulfilling lives. We can help. What will I learn from this booklet?
INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY
 INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
Descemet s Stripping Endothelial Keratoplasty (DSEK)
 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Laser Treatment for Diabetic Retinopathy
 Laser Treatment for Diabetic Retinopathy Your Questions Answered Patient Information Leaflet Diabetic Retinopathy and Laser An examination of your eyes has shown that your diabetes is affecting the back
Laser Treatment for Diabetic Retinopathy Your Questions Answered Patient Information Leaflet Diabetic Retinopathy and Laser An examination of your eyes has shown that your diabetes is affecting the back
Phaco-endoscopic cyclophotocoagulation (phaco-ecp)
 Ambulatory Care & Local Networks Phaco-endoscopic cyclophotocoagulation (phaco-ecp) Information for patients This leaflet answers some of the questions you may have about combined cataract and keyhole
Ambulatory Care & Local Networks Phaco-endoscopic cyclophotocoagulation (phaco-ecp) Information for patients This leaflet answers some of the questions you may have about combined cataract and keyhole
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Vitreo-Retinal and Macular Degeneration Frequently Asked Questions
 Vitreo-Retinal and Macular Degeneration Frequently Asked Questions What is a Vitreo-Retinal specialist? Retinal specialists are eye physicians and surgeons who focus on diseases in the back of the eye
Vitreo-Retinal and Macular Degeneration Frequently Asked Questions What is a Vitreo-Retinal specialist? Retinal specialists are eye physicians and surgeons who focus on diseases in the back of the eye
Get Your Eyes Examined
 1 Vision Changes You may notice vision changes with aging. Many changes are common and can often be corrected. As you get older, you are at higher risk of age-related eye diseases and conditions. Get Your
1 Vision Changes You may notice vision changes with aging. Many changes are common and can often be corrected. As you get older, you are at higher risk of age-related eye diseases and conditions. Get Your
Congratulations! You have just joined the thousands of people who are enjoying the benefits of laser vision correction.
 Dear Valued Patient, Thank you for choosing Shady Grove Ophthalmology for your laser vision correction procedure. Our excellent staff is committed to offering you the highest quality eye care using state
Dear Valued Patient, Thank you for choosing Shady Grove Ophthalmology for your laser vision correction procedure. Our excellent staff is committed to offering you the highest quality eye care using state
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
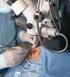 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
Glaucoma filtration surgery (Tube surgery)
 Oxford Eye Hospital Glaucoma filtration surgery (Tube surgery) Information for patients page 2 This leaflet gives you information that will help you decide whether to have glaucoma tube surgery. You might
Oxford Eye Hospital Glaucoma filtration surgery (Tube surgery) Information for patients page 2 This leaflet gives you information that will help you decide whether to have glaucoma tube surgery. You might
Physical and Mental Conditions Guidelines VISION CONDITIONS AND ACTIONS Page 5.4
 Physical and Mental Conditions Guidelines VISION CONDITIONS AND ACTIONS Page 5.4 AMBLYOPIA (Lazy Eye) A reduction in the acuteness of vision without apparent eye disease. This condition cannot be entirely
Physical and Mental Conditions Guidelines VISION CONDITIONS AND ACTIONS Page 5.4 AMBLYOPIA (Lazy Eye) A reduction in the acuteness of vision without apparent eye disease. This condition cannot be entirely
LASIK. Cornea. Iris. Vitreous
 LASIK Introduction LASIK surgery is a procedure that improves vision and can decrease or eliminate the need for eyeglasses or contact lenses. If you and your doctor decide that LASIK surgery is right for
LASIK Introduction LASIK surgery is a procedure that improves vision and can decrease or eliminate the need for eyeglasses or contact lenses. If you and your doctor decide that LASIK surgery is right for
Informed Consent for Refractive Lens Exchange (Clear Lens Replacement)
 Mark Packer, M.D. Informed Consent for Refractive Lens Exchange (Clear Lens Replacement) This surgery involves the removal of the natural lens of my eye, even though it is not a cataract. The natural lens
Mark Packer, M.D. Informed Consent for Refractive Lens Exchange (Clear Lens Replacement) This surgery involves the removal of the natural lens of my eye, even though it is not a cataract. The natural lens
WHAT IS A CATARACT, AND HOW IS IT TREATED?
 4089 TAMIAMI TRAIL NORTH SUITE A103 NAPLES, FL 34103 TELEPHONE (239) 262-2020 FAX (239) 435-1084 DOES THE PATIENT NEED OR WANT A TRANSLATOR, INTERPRETOR OR READER? YES NO TO THE PATIENT: You have the right,
4089 TAMIAMI TRAIL NORTH SUITE A103 NAPLES, FL 34103 TELEPHONE (239) 262-2020 FAX (239) 435-1084 DOES THE PATIENT NEED OR WANT A TRANSLATOR, INTERPRETOR OR READER? YES NO TO THE PATIENT: You have the right,
THE EYES IN MARFAN SYNDROME
 THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
Age-Related Eye Diseases and Conditions. See Well for a Lifetime
 Age-Related Eye Diseases and Conditions See Well for a Lifetime Vision Changes You may notice vision changes with aging. Many changes are common and can often be corrected. As you get older, you are at
Age-Related Eye Diseases and Conditions See Well for a Lifetime Vision Changes You may notice vision changes with aging. Many changes are common and can often be corrected. As you get older, you are at
TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM
 1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
Information about cataract surgery
 Information about cataract surgery Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information about cataract surgery Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Oregon Eye Specialists, PC YOUR GUIDE CATARACT SURGERY. Improving VISION. Improving LIFE.
 Oregon Eye Specialists, PC YOUR GUIDE TO CATARACT SURGERY Dinelli M. Monson, M.D. Comprehensive Ophthalmology Physician and Surgeon Tualatin Clinic: 19250 SW 65 th Ave, Ste 215 503.692.3630 Newberg Clinic:
Oregon Eye Specialists, PC YOUR GUIDE TO CATARACT SURGERY Dinelli M. Monson, M.D. Comprehensive Ophthalmology Physician and Surgeon Tualatin Clinic: 19250 SW 65 th Ave, Ste 215 503.692.3630 Newberg Clinic:
Cataract Surgery Patient Information
 Cataract Patient Information 1. Within the human eye, there is a normal structure called the lens. In youth, this lens is clear, and light rays pass through and are focused by this lens as well as the
Cataract Patient Information 1. Within the human eye, there is a normal structure called the lens. In youth, this lens is clear, and light rays pass through and are focused by this lens as well as the
Consent for Bilateral Simultaneous Refractive Surgery PRK
 Consent for Bilateral Simultaneous Refractive Surgery PRK Please sign and return Patient Copy While many patients choose to have both eyes treated at the same surgical setting, there may be risks associated
Consent for Bilateral Simultaneous Refractive Surgery PRK Please sign and return Patient Copy While many patients choose to have both eyes treated at the same surgical setting, there may be risks associated
The LenSx Laser System. Discover the assurance of bladeless cataract surgery
 g/ 14. The LenSx Laser System Discover the assurance of bladeless cataract surgery Don t let cataracts limit your lifestyle If you or someone you care for has been diagnosed with cataracts, you re certainly
g/ 14. The LenSx Laser System Discover the assurance of bladeless cataract surgery Don t let cataracts limit your lifestyle If you or someone you care for has been diagnosed with cataracts, you re certainly
Informed Consent for Cataract Surgery and/or Implantation of an Intraocular Lens (IOL)
 Bruce H. Brumm, MD, PC 6751 North 72 nd Street, Ste 105 Omaha, NE 68122 (402) 572-2020 800-775-5909 www.brummeye.com Informed Consent for Cataract Surgery and/or Implantation of an Intraocular Lens (IOL)
Bruce H. Brumm, MD, PC 6751 North 72 nd Street, Ste 105 Omaha, NE 68122 (402) 572-2020 800-775-5909 www.brummeye.com Informed Consent for Cataract Surgery and/or Implantation of an Intraocular Lens (IOL)
Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical,
 sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
Glenn B. Cook, M.D., Ph.D. DIPLOMATE AMERICAN BOARD OF OPHTHALMOLOGY Coronado Eye Associates
 Glenn B. Cook, M.D., Ph.D. INFORMED CONSENT FOR CATARACT OPERATION AND/OR IMPLANTATION OF INTRAOCULAR LENS INTRODUCTION: RIGHT / LEFT This information is given to you so that you can make an informed decision
Glenn B. Cook, M.D., Ph.D. INFORMED CONSENT FOR CATARACT OPERATION AND/OR IMPLANTATION OF INTRAOCULAR LENS INTRODUCTION: RIGHT / LEFT This information is given to you so that you can make an informed decision
Frequently Asked Questions. Understanding Cataracts and Cataract Surgery
 Frequently Asked Questions Understanding Cataracts and Cataract Surgery What is a cataract? A cataract is an opacification or clouding of the lens of the eye. The normal lens is clear and allows light
Frequently Asked Questions Understanding Cataracts and Cataract Surgery What is a cataract? A cataract is an opacification or clouding of the lens of the eye. The normal lens is clear and allows light
Age- Related Macular Degeneration
 Age- Related Macular Degeneration Age-Related Macular Degeneration (AMD) is the leading cause of blindness in the United States. It is caused by damage to a localized area of the central retina called
Age- Related Macular Degeneration Age-Related Macular Degeneration (AMD) is the leading cause of blindness in the United States. It is caused by damage to a localized area of the central retina called
Your eyes deserve to see their best.
 Your eyes deserve to see their best. Your Choice for the Best Quality of Vision Correction STAAR Surgical s Visian ICL has a proven track record of providing improved quality of vision. When compared to
Your eyes deserve to see their best. Your Choice for the Best Quality of Vision Correction STAAR Surgical s Visian ICL has a proven track record of providing improved quality of vision. When compared to
Cataracts. Cataract and Primary Eye Care Service...215-928-3041. Main Number...215-928-3000. Physician Referral...1-877-AT-WILLS 1-877-289-4557
 Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
LASIK. What is LASIK? Eye Words to Know. Who is a good candidate for LASIK?
 2014 2015 LASIK What is LASIK? LASIK (laser in situ keratomileusis) is a type of refractive surgery. This kind of surgery uses a laser to treat vision problems caused by refractive errors. You have a refractive
2014 2015 LASIK What is LASIK? LASIK (laser in situ keratomileusis) is a type of refractive surgery. This kind of surgery uses a laser to treat vision problems caused by refractive errors. You have a refractive
Your eyes deserve to see their best.
 Your eyes deserve to see their best. The Implantable Collamer Lens Your Choice for the Best Quality of Vision Correction STAAR Surgical s Visian ICL has a proven track record of providing improved quality
Your eyes deserve to see their best. The Implantable Collamer Lens Your Choice for the Best Quality of Vision Correction STAAR Surgical s Visian ICL has a proven track record of providing improved quality
Discover the assurance of bladeless cataract surgery. The LenSx Laser System. Important Product Information for the LenSx Laser
 The LenSx Laser System Important Product Information for the LenSx Laser CAUTION: The LenSx Laser is restricted by law to the sale and use by, or on the order of, a physician. DESCRIPTION: The LenSx Laser
The LenSx Laser System Important Product Information for the LenSx Laser CAUTION: The LenSx Laser is restricted by law to the sale and use by, or on the order of, a physician. DESCRIPTION: The LenSx Laser
INFORMED CONSENT FOR CATARACT AND LENS IMPLANT SURGERY
 INFORMED CONSENT FOR CATARACT AND LENS IMPLANT SURGERY 1. GENERAL INFORMATION This information is given to you to help you make an informed decision about having cataract and/or lens implant surgery. Once
INFORMED CONSENT FOR CATARACT AND LENS IMPLANT SURGERY 1. GENERAL INFORMATION This information is given to you to help you make an informed decision about having cataract and/or lens implant surgery. Once
Informed Consent For Cataract Surgery And/Or Implantation of an Intraocular Lens
 Informed Consent For Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is given to you so that you can make an informed decision about having eye surgery. Take as
Informed Consent For Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is given to you so that you can make an informed decision about having eye surgery. Take as
Cataract and Cataract Surgery
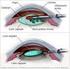 What is a cataract? A cataract is a cloudy area in the lens of your eye. The lens is located just behind the iris (coloured part of the eye). The lens helps to focus light entering the eye to give a clear
What is a cataract? A cataract is a cloudy area in the lens of your eye. The lens is located just behind the iris (coloured part of the eye). The lens helps to focus light entering the eye to give a clear
Information for patients attending appointments at King s College Hospital only
 Ambulatory Care & Local Networks Laser iridotomy Information for patients attending appointments at King s College Hospital only This leaflet answers some of the questions you may have about having laser
Ambulatory Care & Local Networks Laser iridotomy Information for patients attending appointments at King s College Hospital only This leaflet answers some of the questions you may have about having laser
National AMD & Low Vision Awareness Month- February 2016. Dr. Karuna Milind. Wellness Dept., Health India TPA.
 National AMD & Low Vision Awareness Month- February 2016. Dr. Karuna Milind. Wellness Dept., Health India TPA. February is National AMD and Low Vision Awareness Month. Age-related macular degeneration
National AMD & Low Vision Awareness Month- February 2016. Dr. Karuna Milind. Wellness Dept., Health India TPA. February is National AMD and Low Vision Awareness Month. Age-related macular degeneration
Information About Your Day Care Cataract Operation
 Information for patients Information About Your Day Care Cataract Operation Please read this booklet carefully. It contains important information to help you plan for your forthcoming operation. Please
Information for patients Information About Your Day Care Cataract Operation Please read this booklet carefully. It contains important information to help you plan for your forthcoming operation. Please
The Eye Care Center of New Jersey 108 Broughton Avenue Bloomfield, NJ 07003
 The Eye Care Center of New Jersey 108 Broughton Avenue Bloomfield, NJ 07003 Dear Patient, Welcome to The Eye Care Center of New Jersey! It means a great deal to us that you have chosen us to serve as your
The Eye Care Center of New Jersey 108 Broughton Avenue Bloomfield, NJ 07003 Dear Patient, Welcome to The Eye Care Center of New Jersey! It means a great deal to us that you have chosen us to serve as your
Preparing for laser treatment for diabetic retinopathy and maculopathy
 Preparing for laser treatment for diabetic retinopathy and maculopathy This leaflet sets out to answer the questions people with diabetic retinopathy commonly ask about laser treatment. You might want
Preparing for laser treatment for diabetic retinopathy and maculopathy This leaflet sets out to answer the questions people with diabetic retinopathy commonly ask about laser treatment. You might want
Which eye conditions can avastin injections be used for?
 What is avastin? Avastin is a drug that is licensed for the treatment of a certain type of colorectal cancer but can also be used to treat certain eye conditions by being injected into the eye. Although
What is avastin? Avastin is a drug that is licensed for the treatment of a certain type of colorectal cancer but can also be used to treat certain eye conditions by being injected into the eye. Although
Cataracts & Cataract surgery
 Cataracts & Cataract surgery Normal Vision What is a cataract? Light passes through the cornea-the curved, clear front surface of the eye. It then passes through the pupil and the lens. The curved surface
Cataracts & Cataract surgery Normal Vision What is a cataract? Light passes through the cornea-the curved, clear front surface of the eye. It then passes through the pupil and the lens. The curved surface
Facts about diabetic macular oedema
 Patient information medical retina services Facts about diabetic macular oedema What is diabetic macular oedema? Diabetic eye disease is a leading cause of blindness registration among working age adults
Patient information medical retina services Facts about diabetic macular oedema What is diabetic macular oedema? Diabetic eye disease is a leading cause of blindness registration among working age adults
INFORMED CONSENT FOR LASIK SURGERY
 IMPORTANT: READ EVERY WORD! This information is to help you make an informed decision about having laser assisted in-situ keratomileusis (LASIK) surgery to treat your nearsightedness, farsightedness and/or
IMPORTANT: READ EVERY WORD! This information is to help you make an informed decision about having laser assisted in-situ keratomileusis (LASIK) surgery to treat your nearsightedness, farsightedness and/or
I have read and understood this page. Patient Initials
 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) AND ADVANCE SURFACE ABLATION (ASA) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) AND ADVANCE SURFACE ABLATION (ASA) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding
Your Prescription for a New Beginning
 Your Prescription for a New Beginning Now is the time to stop letting poor vision stand in between you and life's most meaningful moments. Surgeons at TLC Laser Eye Centers specialize in the latest vision
Your Prescription for a New Beginning Now is the time to stop letting poor vision stand in between you and life's most meaningful moments. Surgeons at TLC Laser Eye Centers specialize in the latest vision
Informed Consent for Refractive Lens Exchange (Clear Lens Replacement)
 Drs. Fine, Hoffman and Packer, LLC PHYSICIANS AND SURGEONS, EyeMDs OPHTHALMOLOGY I. Howard Fine, M.D. Richard S. Hoffman, M.D. Mark Packer, M.D. 1550 Oak Street, Suite 5 www.finemd.com Eugene, OR 97401-7701
Drs. Fine, Hoffman and Packer, LLC PHYSICIANS AND SURGEONS, EyeMDs OPHTHALMOLOGY I. Howard Fine, M.D. Richard S. Hoffman, M.D. Mark Packer, M.D. 1550 Oak Street, Suite 5 www.finemd.com Eugene, OR 97401-7701
Glaucoma filtration surgery (Trabeculectomy)
 Oxford Eye Hospital Glaucoma filtration surgery (Trabeculectomy) Information for patients This leaflet gives you information that will help you decide whether to have glaucoma surgery. You might want to
Oxford Eye Hospital Glaucoma filtration surgery (Trabeculectomy) Information for patients This leaflet gives you information that will help you decide whether to have glaucoma surgery. You might want to
The Visian ICL Advantages
 The Visian ICL Advantages Many vision correction procedures promise an improved level of vision, but few vision correction alternatives offer the quality and features found with the Visian ICL. These include:
The Visian ICL Advantages Many vision correction procedures promise an improved level of vision, but few vision correction alternatives offer the quality and features found with the Visian ICL. These include:
OMNI EYE SPECIALISTS. The Intraocular Lens
 OMNI EYE SPECIALISTS Intraocular Lens Options In Cataract Surgery Or Refractive Lens Exchange Surgery Your decision to have vision surgery is important and the doctors at Omni Eye Specialists will explain
OMNI EYE SPECIALISTS Intraocular Lens Options In Cataract Surgery Or Refractive Lens Exchange Surgery Your decision to have vision surgery is important and the doctors at Omni Eye Specialists will explain
LASIK and Refractive Surgery. Laser and Lens Vision Correction Options
 LASIK and Refractive Surgery Laser and Lens Vision Correction Options For over 30 years, The Eye Institute of Utah has been giving people vision for life... Dr. Andrew Lyle, vision pioneer and founder
LASIK and Refractive Surgery Laser and Lens Vision Correction Options For over 30 years, The Eye Institute of Utah has been giving people vision for life... Dr. Andrew Lyle, vision pioneer and founder
Advanced Eyecare of Orange County Kim Doan, M.D. Eye Physician & Surgeon
 Advanced Eyecare of Orange County Kim Doan, M.D. Eye Physician & Surgeon Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that
Advanced Eyecare of Orange County Kim Doan, M.D. Eye Physician & Surgeon Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that
Refractive errors are caused by an imperfectly shaped eyeball, cornea or lens, and are of three basic types:
 Tips on Lasik Eye Surgery If you re tired of wearing glasses or contact lenses, you may be considering Lasik eye surgery one of the newest procedures to correct vision problems. Before you sign up for
Tips on Lasik Eye Surgery If you re tired of wearing glasses or contact lenses, you may be considering Lasik eye surgery one of the newest procedures to correct vision problems. Before you sign up for
Macular Hole. James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D.
 Macular Hole James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D. (804) 285-5300 or (804) 287-4200 www.vaeye.com Macular Hole In order to maintain
Macular Hole James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D. (804) 285-5300 or (804) 287-4200 www.vaeye.com Macular Hole In order to maintain
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
PATIENT CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 INTRODUCTION: You have been diagnosed with myopia (nearsightedness) or hyperopia (farsightedness) with or without astigmatism, or astigmatism alone. Myopia is a result of light entering the eye and focusing
INTRODUCTION: You have been diagnosed with myopia (nearsightedness) or hyperopia (farsightedness) with or without astigmatism, or astigmatism alone. Myopia is a result of light entering the eye and focusing
How To Know If You Can See Without Glasses Or Contact Lense After Lasik
 The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 Drs. Fine, Hoffman and Packer, LLC PHYSICIANS AND SURGEONS, EyeMDs OPHTHALMOLOGY I. Howard Fine, M.D. Richard S. Hoffman, M.D. Mark Packer, M.D. 1550 Oak Street, Suite 5 www.finemd.com Eugene, OR 97401-7701
Drs. Fine, Hoffman and Packer, LLC PHYSICIANS AND SURGEONS, EyeMDs OPHTHALMOLOGY I. Howard Fine, M.D. Richard S. Hoffman, M.D. Mark Packer, M.D. 1550 Oak Street, Suite 5 www.finemd.com Eugene, OR 97401-7701
INFORMED CONSENT TO HAVE LASIK
 A Division of Scott & Christie and Associates INFORMED CONSENT TO HAVE LASIK This information is to help you make an informed decision about having Laser Assisted Intrastromal Keratomileusis (LASIK), an
A Division of Scott & Christie and Associates INFORMED CONSENT TO HAVE LASIK This information is to help you make an informed decision about having Laser Assisted Intrastromal Keratomileusis (LASIK), an
Oxford Eye Hospital. Vitrectomy. Information for patients
 Oxford Eye Hospital Vitrectomy Information for patients What is a Vitrectomy The vitreous humour is normally a clear, transparent jelly-like substance inside the eye. It lies behind the iris (the coloured
Oxford Eye Hospital Vitrectomy Information for patients What is a Vitrectomy The vitreous humour is normally a clear, transparent jelly-like substance inside the eye. It lies behind the iris (the coloured
Welcome to the Verisyse Seminar
 Patient Seminar Welcome to the Verisyse Seminar Today we ll answer some of the most common questions about the Verisyse Phakic Intraocular Lens (IOL) including: Who is a candidate How the procedure is
Patient Seminar Welcome to the Verisyse Seminar Today we ll answer some of the most common questions about the Verisyse Phakic Intraocular Lens (IOL) including: Who is a candidate How the procedure is
There may be no symptoms at first. Eye problems can. You can help prevent eye problems. Just because you have
 Keeping your eyes healthy when you have diabetes Oregon Diabetes Resource Bank Handouts to help people with diabetes If you have diabetes, here are things you need to know: 1 2 3 Having diabetes makes
Keeping your eyes healthy when you have diabetes Oregon Diabetes Resource Bank Handouts to help people with diabetes If you have diabetes, here are things you need to know: 1 2 3 Having diabetes makes
LASIK & Refractive Surgery
 LASIK & Refractive Surgery LASIK PRK ICL RLE Monovision + + + For over 30 years, The Eye Institute of Utah has been giving people vision for life... The Eye Institute of Utah was the first medical facility
LASIK & Refractive Surgery LASIK PRK ICL RLE Monovision + + + For over 30 years, The Eye Institute of Utah has been giving people vision for life... The Eye Institute of Utah was the first medical facility
This booklet has been designed to give you all the information you need to undergo cataract surgery.
 Eye Unit Cataract Surgery: This booklet has been designed to give you all the information you need to undergo cataract surgery. University Hospitals Coventry and Warwickshire is a teaching hospital and
Eye Unit Cataract Surgery: This booklet has been designed to give you all the information you need to undergo cataract surgery. University Hospitals Coventry and Warwickshire is a teaching hospital and
INFORMATION REGARDING DILATING EYE DROPS
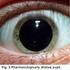 INFORMATION REGARDING DILATING EYE DROPS Dilating eye drops are used to dilate or enlarge the pupils of the eye to allow the doctor to get a better view of the inside of your eye. Dilating drops frequently
INFORMATION REGARDING DILATING EYE DROPS Dilating eye drops are used to dilate or enlarge the pupils of the eye to allow the doctor to get a better view of the inside of your eye. Dilating drops frequently
Stanger Hospital Eye Care Centre.
 Stanger Hospital Eye Care Centre. CATARACT SURGERY YOUR QUESTIONS ANSWERED YOUR QUESTIONS ANSWERED AFTER CATARACT SURGERY You are soon to be admitted to hospital to have your cataract removed. This booklet
Stanger Hospital Eye Care Centre. CATARACT SURGERY YOUR QUESTIONS ANSWERED YOUR QUESTIONS ANSWERED AFTER CATARACT SURGERY You are soon to be admitted to hospital to have your cataract removed. This booklet
IntraLase and LASIK: Risks and Complications
 No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
Keeping Your Eyes Healthy after Treatment for Childhood Cancer
 Keeping Your Eyes Healthy after Treatment for Childhood Cancer High doses of radiation to the brain, eye, or eye socket (orbit) during treatment for childhood cancer can have a long-lasting affect on the
Keeping Your Eyes Healthy after Treatment for Childhood Cancer High doses of radiation to the brain, eye, or eye socket (orbit) during treatment for childhood cancer can have a long-lasting affect on the
Informed Consent for Cataract Surgery or Clear Lens Extraction with Implantation of an Intraocular Lens
 Informed Consent for Cataract Surgery or Clear Lens Extraction with Implantation of an Intraocular Lens Please read the following pages carefully, and initial and sign where indicated. Please do not sign
Informed Consent for Cataract Surgery or Clear Lens Extraction with Implantation of an Intraocular Lens Please read the following pages carefully, and initial and sign where indicated. Please do not sign
Information For Consent For Cataract Surgery
 Information For Consent For Cataract Surgery Your Ophthalmologist has diagnosed you with a visually significant cataract. The following handout will explain your condition and give you the information
Information For Consent For Cataract Surgery Your Ophthalmologist has diagnosed you with a visually significant cataract. The following handout will explain your condition and give you the information
ACTVE INTERVENTIONAL CLINICAL TRIALS - 03/01/2015. Principal Investigator Study Title and Sponsor Study Description
 Cornea and External Disease Service Li, Jennifer A Prospective, Multicenter Post-Approval Study (PAS) of VisionCare s Implantable Miniature Telescope (by Dr. Isaac Lipshitz) in Patients with Bilateral
Cornea and External Disease Service Li, Jennifer A Prospective, Multicenter Post-Approval Study (PAS) of VisionCare s Implantable Miniature Telescope (by Dr. Isaac Lipshitz) in Patients with Bilateral
Informed Consent for Refractive Lens Exchange (Clear Lens Extraction)
 Informed Consent for Refractive Lens Exchange (Clear Lens Extraction) This form is designed to ensure that you have all the information you need to make a decision about whether or not you wish to undergo
Informed Consent for Refractive Lens Exchange (Clear Lens Extraction) This form is designed to ensure that you have all the information you need to make a decision about whether or not you wish to undergo
Trulign Toric Accommodating Intraocular Lenses PATIENT INFORMATION BROCHURE
 Trulign Toric Accommodating Intraocular Lenses PATIENT INFORMATION BROCHURE Table of Contents Page Glossary 2 Introducing Trulign Toric Accommodating IOL 5 What is a cataract 5 What is corneal astigmatism
Trulign Toric Accommodating Intraocular Lenses PATIENT INFORMATION BROCHURE Table of Contents Page Glossary 2 Introducing Trulign Toric Accommodating IOL 5 What is a cataract 5 What is corneal astigmatism
Visual Acuity, Impairments and Vision Insurance Plan Provisions. Stuart West Specialty Sales Manager Virginia CE Forum 2009 Course # 201718
 Visual Acuity, Impairments and Vision Insurance Plan Provisions Stuart West Specialty Sales Manager Virginia CE Forum 2009 Course # 201718 How Vision Works Light passes through the cornea & lens Light
Visual Acuity, Impairments and Vision Insurance Plan Provisions Stuart West Specialty Sales Manager Virginia CE Forum 2009 Course # 201718 How Vision Works Light passes through the cornea & lens Light
A PATIENT GUIDE TO EYE SURGERY
 A PATIENT GUIDE TO EYE SURGERY RISKS ASSOCIATED WITH SURGERY There is a one in 1000 or less than one percent chance that a cataract surgery patient will experience complications that lead to blindness
A PATIENT GUIDE TO EYE SURGERY RISKS ASSOCIATED WITH SURGERY There is a one in 1000 or less than one percent chance that a cataract surgery patient will experience complications that lead to blindness
LASER VISION CORRECTION SURGERY A GUIDE FOR PATIENTS. Professional care for your eye health
 LASER VISION CORRECTION SURGERY A GUIDE FOR PATIENTS Professional care for your eye health Contents About Dr John Males... 1 COMMON QUESTIONS How does an eye work?... 2 What is Myopia (short sightedness)...
LASER VISION CORRECTION SURGERY A GUIDE FOR PATIENTS Professional care for your eye health Contents About Dr John Males... 1 COMMON QUESTIONS How does an eye work?... 2 What is Myopia (short sightedness)...
Standard Single-Focus Lens Implant
 Standard Single-Focus Lens Implant These lenses are ideal for many cataract patients. The single-focus lens implants give patients the best possible clarity at one distance, either for far away, intermediate
Standard Single-Focus Lens Implant These lenses are ideal for many cataract patients. The single-focus lens implants give patients the best possible clarity at one distance, either for far away, intermediate
Color Vision Defects - Color Blindness
 Color Vision Defects - Color Blindness Introduction A color vision defect causes a person to see colors differently than most people. Color vision defects are sometimes called color blindness. There are
Color Vision Defects - Color Blindness Introduction A color vision defect causes a person to see colors differently than most people. Color vision defects are sometimes called color blindness. There are
