Spinal Cord Injury and Skin Care
|
|
|
- Victoria Theodora Newton
- 7 years ago
- Views:
Transcription
1 Spinal Cord Injury and Skin Care What is a pressure sore? A pressure sore is also called a pressure ulcer, decubitus ulcer, decub or bedsore. When you have a pressure sore, you have an area of skin that is damaged due to a loss of blood flow to the area. Blood flow is necessary to keep skin healthy and skin dies if it does not get blood. Pressure sores can become infected and can be life threatening. What causes skin breakdown? Nerves send messages of pain to your brain to alert you to move so that you can relieve pressure, shift your weight or stay away from hot surfaces. With a spinal cord injury, these messages from the sensory nerves may not reach the brain. If there is no feeling you have no way of knowing that you have something pressing against your skin or that you have been in one position for too long. You can get a pressure sore by: Sitting for long periods of time without shifting weight. Lying too long without turning. Not having enough padding especially under bony areas like heels or bottom. Wearing clothes and shoes that fit too tightly. Sitting or lying on hard objects such as catheters, clamps, seams and buttons. Trauma such as abrasion, friction, bumps or falls. Shearing which is when the skin moves one way and the bone another. Tissue Under Pressure 1 May 2016
2 Risks for pressure sore development: Loss of muscle mass - paralysis causes muscles to shrink and decreases the protective cushion over the bone surfaces. Being underweight means you have less padding and overweight makes it harder for you to shift your weight to relieve pressure. Decreased circulation to the paralyzed limbs (due to lack of muscle movement), swelling in body parts that aren t moved frequently, smoking, diabetes, high blood pressure, high cholesterol, and illness. Other causes are o Aging causing more fragile skin o Scar tissue from previous skin breakdown o Spasticity causing your arms or legs to bump into an object o Temperature extremes - hot or cold o Alcohol or drug use, o Depression o Incontinence or sweating leading to excessive moisture o Or dry skin that becomes inflamed and infected Most pressure sores are preventable. How can you help to prevent pressure sores? Daily skin care with mild soap and warm water being sure to thoroughly rinse and dry. Be sure to keep the genital area and skin folds clean and dry. Pressure relief by moving or lifting yourself to take pressure off areas. Check your skin (or have your caregiver check your skin) at least 2 times per day. Look for changes in skin color, blisters, bruises, cracked or dry skin and feel for hardness, swelling or warmth which may be signs of skin breakdown. Pay special attention to the sacrum (lower back), coccyx (tailbone), heels, buttocks, hip, elbow, knee, ankle, toes and back of head. Pay attention to fingernails and toenails because an ingrown toenail may lead to an area that can easily become infected. If you notice a discolored area, stay off of it until the normal color returns. Develop a regular schedule for turning during the night. If you can t turn yourself, be sure that you are lifted rather than slid across sheets. Use pillows and foam pads under bony areas. Don t elevate the head of your bed (unless your doctor tells you to do it) because this can put too much pressure on your buttocks and lower back. 2 May 2016
3 Your health care provider may prescribe a special mattress if you are at the highest risk for pressure sore development. Immediately wash and dry skin if you have any leakage of urine or stool. Get a seating evaluation every 2 years or sooner if the condition of your skin changes. Be sure your wheelchair has the proper cushioning. Wear properly fitted clothing. Shoes should be 1-2 sizes longer and wider than your pre injury shoe size to allow for feet swelling during the day. Wear shoes with stiffer toes for protection in case you bump into objects with your feet. Don t carry anything in your back pockets. Drink plenty of water daily to be sure your body gets the fluids it needs. Eat a balanced diet to ensure proper nutrition and help the body to stay healthy. Avoid getting sunburned and be aware of any medications you are taking can make your skin burn easily. Avoid temperature extremes. Quit smoking. Stay as active as possible. When sitting in your wheelchair, do pressure reliefs every 15 to 30 minutes for at least 30 to 90 seconds. Do pressure reliefs when sitting in the car or on any other surface. If you can t do pressure relief by yourself, ask your caregiver to routinely move you and reduce pressure. How to do Pressure Reliefs or Weight Shifts The pressure relief technique that you use will depend on your injury, your type of wheelchair and how much movement and strength you have in your arms and shoulders. Tilting and Reclining If you can t do independent pressure reliefs, you can use a power tilt wheelchair to regularly relieve pressure. Many wheelchairs have tilt, recline and elevating leg rests. It is very important that you receive proper training from your health care provider to be sure that you are getting enough pressure relief and are properly using these features. Tilt system wheelchairs allow for changing the angle orientation to the ground. Angle tilts of 25 and 65 degrees have been shown to provide adequate relief but 15 degrees or less does not provide adequate pressure relief. Recline system wheelchairs allow for a change in the seat to back angle while maintaining a constant seat angle with respect to the ground. Reclining affects the downward pressure (vertical) and horizontal pressure on the skin. Elevating leg rests allow for changes in the angles of the legs and or footrests in relation to the seat while extending the knee. Use of this feature while reclining can help reduce pressure. 3 May 2016
4 Leaning from Side to Side This helps relieve pressure over one buttock at a time. Lock the wheels on your wheelchair and swing one arm away from the wheelchair. Hold onto the remaining armrest and lean your body to the opposite side, taking the weight off one buttock for seconds. If you can t grasp the armrest with your hand, you may be able to hook your wrist behind the wheelchair push handle or back rest. To again sit upright, you may need to use the wheelchair push handle or armrest for assistance. Pushing up on the push rims of the wheels may also help in regaining an upright position. You may use a table or other stationery object to lean against for assistance. Be sure that the weight is completely off the opposite buttock and hold the position for seconds. Repeat on the other side. Leaning Forward This can be done alone or with assistance. Move your wheelchair so that the front casters are turned forward, and then lock the wheels of your wheelchair. Bend forward and bring your chest to your knees. This lifts the weight of your bottom from the wheelchair. Stay in this position for seconds. Return your body to the upright position. There are several techniques to regain an upright position depending on your equipment and the strength in your arms and trunk. You may: Place your hand on your knees to push up. Keep your hand on push handles and pull up. Place your hand against the front of the armrest and push up. Independent Push-ups This can be used by individuals who can extend their elbows and lift their body weight (people with an injury at C7 and below). Grip your arm rests with your hands and lift up completely off our seat for 60 seconds. Since this method could harm your rotator cuff (part of the shoulder joint), it should only be used if you are unable to complete the other techniques. Progression of Training Early in your training it may be difficult for you to shift your weight from the center of your chair. You may also find it difficult to regain an upright position after shifting your weight. If so, you may try the following techniques. Position and lock your chair next to a stationary object. Perform the side lean as instructed, but use the object to push up as you regain the upright position. Position and lock your chair in front of a table. Learn forward onto the table and use it to push back up. 4 May 2016
5 Alternate Techniques Below are some techniques that you can do and are less obvious. These can be done when you are out in the community without attracting attention. Cross one leg over the other and lean back to one side while holding your knee in position, lifting the weight off one buttock. Repeat using the other leg. Cross your leg by putting one ankle over the other knee and lean forward, lifting the weight off your buttock. Repeat using the other leg. Spend some time fixing your shoe laces, your feet, and the hem of your pants to achieve the same position as the forward lean technique. Lean against tables as you speak to friends. Building Skin Tolerance Skin tolerance is the amount of time that your skin can stand to be under pressure before damage starts to occur. The amount of time varies between people but regardless of your skin pressure tolerance, you still need to relieve pressure periodically. You need to move yourself every 15 to 30 minutes. Skin tolerance can change especially if you are sick, not eating well or have changes in the surface you are on or have changes in your posture. If any of these occur, remember to frequently inspect your skin. The increase in redness of your skin after applying pressure (the first sign of a pressure sore) and the amount of time it takes for the redness to fade will help you determine what your skin can tolerate. This will help you to determine how much time you need between pressure reliefs. How do I know if I can increase my sitting time or time in one position? Building up skin tolerance is a gradual process but you can build skin tolerance by following these steps: Lie in one position for the amount of time directed by your health care provider Look at your skin. Touch the pink areas of your skin to see if they turn white. Stay off of the area until the pinkness or redness clears completely. If within minutes the redness or pinkness clears, you may increase your time between pressure reliefs or turning by 30 minutes. If the redness or pinkness does not clear in minutes, do not increase your time between pressure reliefs or turning. Recognizing and Treating Pressure Sores How Can I Tell If I Have a Pressure Sore? One of the first signs is a reddened, discolored or darkened area that may feel hard and warm to the touch. An African American s skin may look purple, bluish or shiny. If you remove pressure from the reddened area for minutes and the skin does not return to normal, a pressure sore has begun. Stay off of the area and follow the instructions below under Stage 1. Press on the red, pink or darkened area with your finger. The area should go white. Remove the pressure and the area should return to red, pink or a darkened color within 5 May 2016
6 a few seconds which indicates a good blood flow. If the area says white, the blood flow has been impaired and damage has begun. Dark skin may not have visible blanching even when healthy so it s important to look for other signs of damage like color changes or a feeling of hardness compared to surrounding areas. What you see at the skin s surface is often the smallest part of the sore. Don t be fooled into thinking that you only have a little problem. The pressure is usually from blood vessels under the skin being squeezed between the surface and bone so muscles and tissues near the bone suffer the greatest damage. Every pressure sore seen on the skin should be considered serious because of the probable damaged that has occurred under the skin. Stages of Pressure Sores Stage 1 Skin is not broken but is red or discolored or may show changes in hardness or temperature compared to surrounding areas. When the area is pressed, it remains red and doesn t lighten or turn white (blanch). The redness or color change does not fade within 30 minutes of removing pressure. A pressure sore at this stage can be reversed in about 3 days if all pressure is taken off the site. What to do Stay off the area and remove all pressure. Keep the area clean and dry; eat adequate calories high in protein, vitamins (especially A and C) and minerals (especially zinc). Increase the amount of water you normally drink and find and remove the cause. Inspect the area at least twice a day and call your health care provider if it is not gone in 2-3 days. Stage 2 The top layer of skin (epidermis) is broken creating a shallow open sore. The second layer of skin (dermis) may also be open. Drainage of fluid may be present. Healing time is usually three days to three weeks. 6 May 2016
7 What to do Get pressure off of the area and follow the steps outlined in Stage 1. See your health care provider right away. Stage 3 The wound extends through the second layer of skin (dermis) into the fatty subcutaneous (below the skin). Bone, tendons and muscles are not visible. Inspect the area for signs of infection which include: redness around the edge of the sore, pus, odor, fever, or greenish drainage from the sore and possible necrosis (black, dead tissue). Wounds at this stage often take 1 to 4 months to heal. What to do Get the pressure off the area and see your health care provider right away. Stage 3 wounds often need special wound care. You may also qualify for a special bed or pressure relieving mattress which can be ordered by your health care provider. Stage 4 This type of wound extends into the muscle and can extend as far down as the bone. Usually you will see a lot of dead tissue and drainage. There is a great chance of an infection. These wounds can take anywhere from 3 months to 2 years to heal. 7 May 2016
8 What to do Get pressure off of the area and call your health care provider right away. Surgery is frequently needed for this type of wound. Suspected deep tissue injury You may see a purple or maroon area of discolored skin that is not broken. You may also see a blood filled blister caused by damage to underlying soft tissue from pressure or shearing. This area may be surrounded by tissue that is painful, firm, mushy, boggy and warmer or cooler than nearby tissue. Deep tissue injury may be harder to identify in people who have darker skin tones. Progression may include a thin blister over a dark wound bed and the wound may evolve and become covered by a thin scab (eschar). The progression may be rapid and expose additional layers of tissue even if you receive optimal treatment. Unstageable An unstageable wound is one where there is full thickness tissue loss and the base of the ulcer is covered by slough (which is dead tissue separated from living tissue) of yellow, tan, gray, green or brown color and/or a scab of tan, brown or black color in the wound bed. Possible complications of pressure sores They can be life threatening! Infections can spread throughout the body to the blood, heart and bone. Amputations may be needed. You may need to be on prolonged bed rest that can keep you out of work, school and social activities for months. Autonomic dysreflexia (quick onset of excessively high blood pressure) can occur. You are at a higher risk of respiratory infections or urinary tract infections (UTIs) because you are less active. Treatment can be very costly related to lost wages and/or medical treatment. 8 May 2016
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Working together to prevent pressure ulcers (prevention and pressure-relieving devices)
 Working together to prevent pressure ulcers (prevention and pressure-relieving devices) Understanding NICE guidance information for people at risk of pressure ulcers, their carers, and the public Draft
Working together to prevent pressure ulcers (prevention and pressure-relieving devices) Understanding NICE guidance information for people at risk of pressure ulcers, their carers, and the public Draft
Pressure Ulcers. Occupational Therapy. This leaflet is for both yourself and Carers
 Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Preventing pressure ulcers
 Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Physiotherapy Database Exercises for people with Spinal Cord Injury
 Physiotherapy Database Exercises for people with Spinal Cord Injury Compiled by the physiotherapists associated with the following Sydney (Australian) spinal units : Last Generated on Mon Mar 29 16:57:20
Physiotherapy Database Exercises for people with Spinal Cord Injury Compiled by the physiotherapists associated with the following Sydney (Australian) spinal units : Last Generated on Mon Mar 29 16:57:20
Pressure Ulcers Assessing and Staging. Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010
 Pressure Ulcers Assessing and Staging Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010 Never Events: Pressure Ulcers Pressure Ulcer Codes: MD documentation of pressure ulcers determines
Pressure Ulcers Assessing and Staging Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010 Never Events: Pressure Ulcers Pressure Ulcer Codes: MD documentation of pressure ulcers determines
Position Statement: Pressure Ulcer Staging
 Position Statement: Pressure Ulcer Staging Statement of Position The Wound, Ostomy and Continence Nurses (WOCN) Society supports the use of the National Pressure Ulcer Advisory Panel Staging System (NPUAP).
Position Statement: Pressure Ulcer Staging Statement of Position The Wound, Ostomy and Continence Nurses (WOCN) Society supports the use of the National Pressure Ulcer Advisory Panel Staging System (NPUAP).
Pressure Sores (Decubitus Ulcers)
 Pressure Sores (Decubitus Ulcers) Judith Stevens, M.Ed. With thanks to Dr. Toni Benton, Jennifer Thorne-Lehman, Araceli Domingo for contributing resource information. Thanks to Ann Chase Stevens for sharing
Pressure Sores (Decubitus Ulcers) Judith Stevens, M.Ed. With thanks to Dr. Toni Benton, Jennifer Thorne-Lehman, Araceli Domingo for contributing resource information. Thanks to Ann Chase Stevens for sharing
Skin & Wound Care Prevention & Treatment. By Candy Houk, RN Skin & Wound Program Manager
 Skin & Wound Care Prevention & Treatment By Candy Houk, RN Skin & Wound Program Manager OBJECTIVES Classify Stage 1 and 2 pressure ulcers Recognize suspected Stage 3, 4, DTI, and unstageable pressure ulcers
Skin & Wound Care Prevention & Treatment By Candy Houk, RN Skin & Wound Program Manager OBJECTIVES Classify Stage 1 and 2 pressure ulcers Recognize suspected Stage 3, 4, DTI, and unstageable pressure ulcers
7/11/2011. Pressure Ulcers. Moisture-NOT Pressure. Wounds NOT Caused by Pressure
 Assessment and Documentation of Pressure Ulcers Jeri Ann Lundgren, RN, BSN, PHN, CWS, CWCN Pathway Health Services July 19, 2011 Training Objectives Describe etiologies of pressure ulcers Discuss how to
Assessment and Documentation of Pressure Ulcers Jeri Ann Lundgren, RN, BSN, PHN, CWS, CWCN Pathway Health Services July 19, 2011 Training Objectives Describe etiologies of pressure ulcers Discuss how to
Wound and Skin Assessment. Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center
 Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Pressure Ulcer Passport
 Pressure Ulcer Passport Information for patients This is a record of the treatment you are receiving for your pressure ulcer injury. Please bring it with you to all your healthcare appointments. This will
Pressure Ulcer Passport Information for patients This is a record of the treatment you are receiving for your pressure ulcer injury. Please bring it with you to all your healthcare appointments. This will
OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers
 OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers Presented by: Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director, OASIS Competency Institute 243 King Street, Suite 246 Northampton,
OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers Presented by: Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director, OASIS Competency Institute 243 King Street, Suite 246 Northampton,
How To Stage A Pressure Ulcer
 WOCN Society Position Statement: Pressure Ulcer Staging Originated By: Wound Committee Date Completed: 1996 Reviewed/Revised: July 2006 Revised: August 2007 Reviewed/Revised: April 2011 Definition of Pressure
WOCN Society Position Statement: Pressure Ulcer Staging Originated By: Wound Committee Date Completed: 1996 Reviewed/Revised: July 2006 Revised: August 2007 Reviewed/Revised: April 2011 Definition of Pressure
Instructions for Wearing your Scoliosis Brace
 Instructions for Wearing your Scoliosis Brace modified from Boston Scoliosis Brace course instruction manual, presented by NOPCP and Children s Hospital Medical Center, Boston, MA Goal: This requires:
Instructions for Wearing your Scoliosis Brace modified from Boston Scoliosis Brace course instruction manual, presented by NOPCP and Children s Hospital Medical Center, Boston, MA Goal: This requires:
Anyone who has difficulty moving can get a pressure sore. But you are more likely to get one if you:
 Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
Treat Your Feet: Foot care for people with diabetes
 Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Routine For: OT - General Guidelines/Energy Conservation (Caregiver)
 GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
Pressure Ulcers in Neonatal Patients. Rene Amaya, MD Pediatric Specialists of Houston Infectious Disease/Wound Care
 Pressure Ulcers in Neonatal Patients Rene Amaya, MD Pediatric Specialists of Houston Infectious Disease/Wound Care Objectives Review skin anatomy and understand why neonatal skin is at increased risk for
Pressure Ulcers in Neonatal Patients Rene Amaya, MD Pediatric Specialists of Houston Infectious Disease/Wound Care Objectives Review skin anatomy and understand why neonatal skin is at increased risk for
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
How does Diabetes Effect the Feet
 How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
Inservice: Wound Care and Dressings. Friday, June 26, 2009. A. Closed Wounds tissue is injured but skin is not BROKEN
 f Inservice: Wound Care and Dressings Friday, June 26, 2009 WOUNDS: Are injuries of the skin and underlying subcutaneous tissues and muscles (Nursing Manual by Lippincott) Are disruptions in the integrity
f Inservice: Wound Care and Dressings Friday, June 26, 2009 WOUNDS: Are injuries of the skin and underlying subcutaneous tissues and muscles (Nursing Manual by Lippincott) Are disruptions in the integrity
Preventing Pressure Ulcers and Assisting With Wound Care
 Preventing Pressure Ulcers and Assisting With Wound Care C H A P T E R 19 A nursing assistant makes an occupied bed. Providing clean, wrinkle-free linens is just one way that nursing assistants help to
Preventing Pressure Ulcers and Assisting With Wound Care C H A P T E R 19 A nursing assistant makes an occupied bed. Providing clean, wrinkle-free linens is just one way that nursing assistants help to
For Deep Pressure Massage
 T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
Coccydynia. (Coccyx Pain) Information for patients. Outpatients Physiotherapy Tel: 01473 703312
 Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
PATIENT TEACHING GUIDE: Wound Care Handbook
 PATIENT TEACHING GUIDE: Wound Care Handbook PATIENT TEACHING GUIDE: WOUND CARE Design by Mariscal Design, Illustrations by Lysa Hawke. The Wound Care Self Care Guide was written and prepared by: Barbara
PATIENT TEACHING GUIDE: Wound Care Handbook PATIENT TEACHING GUIDE: WOUND CARE Design by Mariscal Design, Illustrations by Lysa Hawke. The Wound Care Self Care Guide was written and prepared by: Barbara
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Wound Classification Name That Wound Sheridan, WY June 8 th 2013
 Initial Wound Care Consult Sheridan, WY June 8 th, 2013 History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed
Initial Wound Care Consult Sheridan, WY June 8 th, 2013 History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed
Community home-based prevention of disability due to lymphatic filariasis
 Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
THE PRINCIPLES & PRACTICES ASSOCIATED WITH CARING FOR THE SKIN OF A SPINAL CORD INJURED PATIENT
 NATIONAL SPINAL INJURIES CENTRE STOKE MANDEVILLE HOSPITAL HANDOUT PREPARED FOR PATIENTS, CARERS & COMMUNITY STAFF BY SPINAL OUTPATIENT SERVICES THE PRINCIPLES & PRACTICES ASSOCIATED WITH CARING FOR THE
NATIONAL SPINAL INJURIES CENTRE STOKE MANDEVILLE HOSPITAL HANDOUT PREPARED FOR PATIENTS, CARERS & COMMUNITY STAFF BY SPINAL OUTPATIENT SERVICES THE PRINCIPLES & PRACTICES ASSOCIATED WITH CARING FOR THE
Pressure Ulcers Risk Management and Treatment
 Pressure Ulcers Risk Management and Treatment Objectives State reasons why individuals initiate lawsuits. Define strategies to reduce the risk of litigation. Determine appropriate treatment for the patient.
Pressure Ulcers Risk Management and Treatment Objectives State reasons why individuals initiate lawsuits. Define strategies to reduce the risk of litigation. Determine appropriate treatment for the patient.
WHAT IS INCONTINENCE?
 CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
Spinal Cord Injury Education. Common Medical Problems Following Spinal Cord Injury
 Spinal Cord Injury Education Common Medical Problems Following Spinal Cord Injury Common Medical Complications After SCI, your body is vulnerable to various complications This presentation gives a brief
Spinal Cord Injury Education Common Medical Problems Following Spinal Cord Injury Common Medical Complications After SCI, your body is vulnerable to various complications This presentation gives a brief
How can DIABETES affect my FEET? Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Reducing Hospital. of Pressure Damage. Spread the Learning and celebrate the successes
 Reducing Hospital Acquired Pressure Ulcers Prevention & Management of Pressure Damage Spread the Learning and celebrate the successes Prevalence & Cost Prevalence ranges from 10% to 18% in the UK (Clark
Reducing Hospital Acquired Pressure Ulcers Prevention & Management of Pressure Damage Spread the Learning and celebrate the successes Prevalence & Cost Prevalence ranges from 10% to 18% in the UK (Clark
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Provided by the American Venous Forum: veinforum.org
 CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased.
 Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Safe Lifting and Carrying
 PART 1 Basic Lifts Proper lifting and handling will help protect against injury and make your job easier. It takes training and practice to do it right. The following are basic steps in safe lifting and
PART 1 Basic Lifts Proper lifting and handling will help protect against injury and make your job easier. It takes training and practice to do it right. The following are basic steps in safe lifting and
The Family Library. Understanding Diabetes
 The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
WOUND OSTOMY CONTINENCE NURSES SOCIETY GUIDANCE ON OASIS-C INTEGUMENTARY ITEMS
 Wound Ostomy Continence Nurses Society Guidance on OASIS-C Integumentary Items WOCN OASIS Taskforce Members: Ben Peirce (Chairperson), RN, BA, CWOCN, COS-C Dianne Mackey, BSN, RN, PHN, CWOCN Laurie McNichol,
Wound Ostomy Continence Nurses Society Guidance on OASIS-C Integumentary Items WOCN OASIS Taskforce Members: Ben Peirce (Chairperson), RN, BA, CWOCN, COS-C Dianne Mackey, BSN, RN, PHN, CWOCN Laurie McNichol,
Chapter. Some days I m so stiff. But even then, your firm yet gentle guidance always helps me move more easily. MOVING AND POSITIONING
 15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
Diabetes and your feet
 The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
HELPFUL HINTS FOR A HEALTHY BACK
 HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
FUNCTIONS OF THE SKIN
 FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
HOPE EXERCISE RECOVERY RESOURCES RELATIONSHIPS INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RELATIONSHIPS MOVEMENT. A Stroke Recovery Guide
 INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
PRESSURE ULCER GUIDELINES FOR TOPICAL TREATMENT
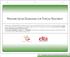 PRESSURE ULCER GUIDELINES FOR TOPICAL TREATMENT The following are suggested guidelines for treatment of pressure ulcers using products from Swiss-American Products, Inc. and are intended to supplement
PRESSURE ULCER GUIDELINES FOR TOPICAL TREATMENT The following are suggested guidelines for treatment of pressure ulcers using products from Swiss-American Products, Inc. and are intended to supplement
Individualized Care Plans Fully Developed
 Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Illinois Department of Public Health STATEMENT OF DEFICIENCIES AND PLAN OF CORRECTION. Statement of LICENSURE Violations
 (X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
(X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
SECTION 9. Mobility, positioning, and transfers. Moving after a stroke 9.1. Fatigue. Loss of sensation. Loss of motor function.
 SECTION 9 Mobility, positioning, and transfers Section overview This section looks at: Moving after a stroke Assisting with mobility Positioning Managing the affected limb Transfers Wheelchair use Walking
SECTION 9 Mobility, positioning, and transfers Section overview This section looks at: Moving after a stroke Assisting with mobility Positioning Managing the affected limb Transfers Wheelchair use Walking
about Why You Should Know Melanoma
 about Why You Should Know Melanoma Why You Should Know about Melanoma Each year, more than 3 million Americans are diagnosed with skin cancer. This is the most common form of cancer. Of these, more than
about Why You Should Know Melanoma Why You Should Know about Melanoma Each year, more than 3 million Americans are diagnosed with skin cancer. This is the most common form of cancer. Of these, more than
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Exercises for older people
 Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
SECTION M: SKIN CONDITIONS. M0100: Determination of Pressure Ulcer Risk. Item Rationale Health-related Quality of Life.
 SECTION M: SKIN CONDITIONS Intent: The items in this section document the risk, presence, appearance, and change of pressure ulcers. This section also notes other skin ulcers, wounds, or lesions, and documents
SECTION M: SKIN CONDITIONS Intent: The items in this section document the risk, presence, appearance, and change of pressure ulcers. This section also notes other skin ulcers, wounds, or lesions, and documents
PATIENT HANDBOOK AND JOURNAL POST SURGERY
 PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
Oxford University Hospitals. NHS Trust. Hand & Plastics Physiotherapy Department Flexor Tendon Repair. Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Flexor Tendon Repair Information for patients Introduction You have had surgery to repair one or more of the tendons in your
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Flexor Tendon Repair Information for patients Introduction You have had surgery to repair one or more of the tendons in your
KINESIOLOGY TAPING GUIDE
 KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
Diabetic Foot Ulcers and Pressure Ulcers. Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences
 Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
Going home after an AV Fistula or AV Graft
 Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
Wound, Ostomy and Continence Nurses Society s Guidance on OASIS-C1 Integumentary Items: Best Practice for Clinicians
 Wound, Ostomy and Continence Nurses Society s Guidance on OASIS-C1 Integumentary Items: Best Practice for Clinicians Acknowledgments Wound, Ostomy and Continence Nurses Society s Guidance on OASIS-C1 Integumentary
Wound, Ostomy and Continence Nurses Society s Guidance on OASIS-C1 Integumentary Items: Best Practice for Clinicians Acknowledgments Wound, Ostomy and Continence Nurses Society s Guidance on OASIS-C1 Integumentary
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
SCI Rehab. Stages of Pressure Sores. Prevention of Pressure Sores Develop due to pressure on skin, lack of blood supply, tissue death.
 SCI Rehab Basics of Bowel and Bladder Management, Skin Protection, Bathroom DME, Positioning, and Transfers SCI Rehab 101 Rehab Education Basics Skin, Bladder, Bowel Skin Protection and Pressure Sore Prevention!
SCI Rehab Basics of Bowel and Bladder Management, Skin Protection, Bathroom DME, Positioning, and Transfers SCI Rehab 101 Rehab Education Basics Skin, Bladder, Bowel Skin Protection and Pressure Sore Prevention!
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Do you sit at a desk all day? Does your 9 to 5 leave no time for structured exercise..?
 Do you sit at a desk all day? Does your 9 to 5 leave no time for structured exercise..? Staying healthy at work is easier than you might think: Try building the following desk based exercises into your
Do you sit at a desk all day? Does your 9 to 5 leave no time for structured exercise..? Staying healthy at work is easier than you might think: Try building the following desk based exercises into your
Throughout this reference summary, you will find out what massage therapy is, its benefits, risks, and what to expect during and after a massage.
 Massage Therapy Introduction Massage therapy is the manipulation of the soft tissues of the body, including the skin, tendons, muscles and connective tissue by a professional, for relaxation or to enhance
Massage Therapy Introduction Massage therapy is the manipulation of the soft tissues of the body, including the skin, tendons, muscles and connective tissue by a professional, for relaxation or to enhance
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS:
 LESSON TOPIC: AVERAGE TIME: BACK INJURY PREVENTION 30 Minutes INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS: a. Handout #1
LESSON TOPIC: AVERAGE TIME: BACK INJURY PREVENTION 30 Minutes INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS: a. Handout #1
Strength Training HEALTHY BONES, HEALTHY HEART
 Strength Training HEALTHY BONES, HEALTHY HEART No matter what your age, strength training can improve your bone health and your balance. As we age, our bones lose both tissue and strength. This condition
Strength Training HEALTHY BONES, HEALTHY HEART No matter what your age, strength training can improve your bone health and your balance. As we age, our bones lose both tissue and strength. This condition
Surgery for breast cancer in men
 Surgery for breast cancer in men This information is an extract from the booklet Understanding breast cancer in men. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Surgery for breast cancer in men This information is an extract from the booklet Understanding breast cancer in men. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Hemodialysis Access: What You Need to Know
 Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
THERAPEUTIC USE OF HEAT AND COLD
 THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Pressure Injury Prevention and Management Policy
 Pressure Injury Prevention and Management Policy Owner (initiating the document): Dr Amanda Ling Contact name and number: Rachel Dennis (Ph: 9222 2197) Version: 1.5 Approved by: Professor Bryant Stokes,
Pressure Injury Prevention and Management Policy Owner (initiating the document): Dr Amanda Ling Contact name and number: Rachel Dennis (Ph: 9222 2197) Version: 1.5 Approved by: Professor Bryant Stokes,
FROZEN SHOULDER OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU. Frozen Shoulder FROZEN SHOULDER
 OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
Heel pain and Plantar fasciitis
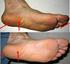 A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
MEDICATION GUIDE COUMADIN (COU-ma-din) (warfarin sodium)
 MEDICATION GUIDE COUMADIN (COU-ma-din) (warfarin sodium) Read this Medication Guide before you start taking COUMADIN (warfarin sodium) and each time you get a refill. There may be new information. This
MEDICATION GUIDE COUMADIN (COU-ma-din) (warfarin sodium) Read this Medication Guide before you start taking COUMADIN (warfarin sodium) and each time you get a refill. There may be new information. This
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Exercise After Breast Surgery. Post Mastectomy Therapy
 Exercise After Breast Surgery Post Mastectomy Therapy Dear Patient, Breast cancer is a journey and you have made it this far successfully. This booklet will help you continue your journey to recovery.
Exercise After Breast Surgery Post Mastectomy Therapy Dear Patient, Breast cancer is a journey and you have made it this far successfully. This booklet will help you continue your journey to recovery.
Fact sheet Exercises for older adults undergoing rehabilitation
 Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
LESSON OVERVIEW. Objectives: By the end of the lesson, the Lay Health Worker will be able to:
 Objectives: LESSON OVERVIEW By the end of the lesson, the Lay Health Worker will be able to: 1. Describe what arthritis is in general terms. 2. Identify common myths and beliefs about arthritis that may
Objectives: LESSON OVERVIEW By the end of the lesson, the Lay Health Worker will be able to: 1. Describe what arthritis is in general terms. 2. Identify common myths and beliefs about arthritis that may
