NROSCI/BIOSC 1070 and MSNBIO 2070 September 19 & 21, 2016 Cardiovascular 3 & 4: Mechanical Actions of the Heart and Determinants of Cardiac Output
|
|
|
- Maria Peters
- 7 years ago
- Views:
Transcription
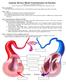
1 NROSCI/BIOSC 1070 and MSNBIO 2070 September 19 & 21, 2016 Cardiovascular 3 & 4: Mechanical Actions of the Heart and Determinants of Cardiac Output An essential component for the operation of the heart is the action of the valves. The valves insure that blood moves in only one direction. The opening and closing of the heart valves is controlled simply by the pressure gradients on the two sides of the valves. The two arteriovenous (AV) valves, the tricuspid and mitral valves, are comprised of flaps of connective tissue. On the ventricular side, the valves are attached to collagen cords called the cordae tendinae. The opposite ends of the cords are attached to the moundlike extensions of ventricular muscle called papillary muscles. The cordae tendinae prevent the flaps of the valve from getting stuck against the ventricular wall during ventricular filling and from being forced into the atria during ventricular systole. In contrast, the aortic and pulmonary semilunar valves have three cuplike leaflets that fill with blood, and which snap closed when backward pressure is placed on them. Special tethering such as the chordae tendinae are not required to insure that the semilunar valves close properly. The closing of the heart valves generates vibrations, which result in the heart sounds that physicians often monitor during examinations. The major heart sounds are commonly referred to as lub-dub. The softer lub is associated with closing of the tricuspid and mitral valves, and the dub comes from the closing of the semilunar valves. Careful assessment of the heart sounds can be done using a stethoscope; the procedure is referred to a auscultation. Through careful monitoring, two additional heart sounds are revealed. The third heart sound is associated with turbulent blood flow into the ventricle near the beginning of ventricular filling, and the fourth heart sound is produced by additional turbulent flow into the ventricle during atrial contraction. The heart sounds become abnormal if the valves are diseased. Two general types of abnormal heart sounds can be classified: a murmur and a gallop. Murmurs are heart sounds in addition to the four that are normally present, and gallops are augmented third or fourth heart sounds. Murmurs often occur when valves fail to close properly, producing regurgitation or movement of blood in the wrong direction. For example, if an AV valve does not close properly, blood will move from the ventricle into the atrium during systole. This turbulent movement of blood can be heard as an additional heart sound. Gallops often occur when the AV valves do not open properly or are narrowed (stenosed), resulting in excessive turbulence during movement of blood from the atria into the ventricles. Gallops can also occur when the ventricles are very stiff. 9/19/16 & 9/21/16 Page 1 Cardio 3-4
2 Clinical Notes: Echocardiography The beating heart can be imaged in real time using echocardiography. This technique employs ultrasound that is emitted from a piezoelectric crystal. The waves are reflected back to the crystal, and result in the production of electric impulses that are recorded. The characteristics of the reflected waves are dependent on the properties of the tissue that the waves pass through. A computer can interpret the electrical impulses generated by the vibrating pizoelectric crystal, and construct an image from these signals. There are three general placements for the echocardiograph transducer: Transthoracic echocardiogram (TTE), in which a transducer is moved over different locations on the chest or abdomen. Transesophageal echocardiogram (TEE), in which the transducer is passed down the esophagus to provide clearer pictures of the heart. Intracardiac echocardiogram, in which the transducer is inserted into the cardiac vessels. The following diagram shows two common planes imaged using transthoracic echocardiography: 9/19/16 & 9/21/16 Page 2 Cardio 3-4
3 Another way of describing the cardiac cycle is through a pressure-volume graph. Between points A and B in this graph, the ventricles are filling with blood. The AV valves open when the pressure in the atria exceeds that in the ventricles. After the AV valves open, ventricular pressure increases slightly as volume increases. At the end of this part of the cardiac cycle, the atria contract and the ventricles contain the maximal amount of blood that they will have during the cardiac cycle (end diastolic volume, shown at point B). Note that although end diastolic volume is typically about 135 ml, it can be more or less under certain conditions. For example, when heart rate is very high (and filling time is low), end diastolic volume often drops. When cardiac return increases, EDV also increases. In the next phase of the cardiac cycle, the ventricles begin to contract. Very rapidly, pressure in the ventricles exceeds that in the atria and the AV valves close. Subsequently, ventricular pressure increases but ventricular volume stays constant (hence, an isovolumetric contraction). When pressure in the ventricles is great enough, the semilunar valves open and blood is ejected into the aorta and pulmonary arteries (point C). Ventricular pressure continues to increase while ventricular volume drops. Eventually, the ventricles begin to relax, and the semilunar valves close. Note that ventricular volume is not zero at this time, but instead end-systolic volume is about 65 ml. This volume is variable, however, and can decrease if ventricular contractility increases. The ventricle then relaxes, but because the ventricular pressure exceeds atrial pressure the AV valves are closed. This is the isovolumetric relaxation phase of the cardiac cycle. When ventricular pressure drops below atrial pressure, the AV valves open and ventricular filling starts again. Note that if MAP increases, more pressure is needed in the left ventricle to open the aortic valve. Ejection fraction (EF) is defined as the fraction of end diastolic volume that is ejected out of the ventricle during each contraction. EF = SV/EDV If SV=70ml and EDV=135ml Then EF=70/135 or /19/16 & 9/21/16 Page 3 Cardio 3-4
4 Yet another means of depicting the cardiac cycle is shown above. This diagram includes both electrical and mechanical events that occur in the heart. Such a diagram is called the Wiggers diagram after the physiologist who first published it (Carl Wiggers). We have not discussed one pressure tracing in the Wigger s diagram: a recording of pressure in the left atrium. Three waves are evident: the a, c, and v waves. The a wave is caused by atrial contraction. The c wave is caused by ventricular contraction, and is due to 1) the small backflow of blood from the ventricle to the atrium when the mitral valve closes and 2) the bulging of the closed mitral valve backward into the atrium when ventricle pressure increases. The v wave is due to blood flowing from the veins into the atrium during ventricular contraction, which cannot leave because the mitral valve is shut. When the mitral valve opens, atrial pressure drops, demarking the peak of the v wave. It is important for you to understand the relationships between MAP, aortic valve opening, and end systolic volume. If total peripheral resistance increases, then the pressure in the left ventricle must increase more to open the aortic valve (since MAP is higher [MAP=CO*TPR], and the pressure in the left ventricle must exceed that in the aorta for the valve to open). In addition, the valve closes earlier when the ventricle begins to relax. As a consequence, stroke volume diminishes. 9/19/16 & 9/21/16 Page 4 Cardio 3-4
5 When stroke volume diminishes, there is more blood left in the ventricle at the end of systole (end systolic volume increases). This increased volume is added to the volume transferred from the left atrium to left ventricle after the mitral valve opens. As a consequence, end diastolic volume increases. Thus, the next ventricular contraction is stronger due to the Frank-Starling effect. In essence, if TPR is high, then the heart must work harder and use more ATP to maintain constant cardiac output. Cardiac output is the amount of blood pumped from the ventricles per unit time. As mentioned in the first lecture, cardiac output at rest is about 5 L/min. This value is derived through the following calculation. The resting heart beats at about 70 times/min, and each ventricular ejection is about 70 ml (EDV-ESV). Thus, 70 beats/min * 0.07 L/beat = 4.9 L/min. You should be familiar with the formula to compute cardiac output, and how cardiac output relates to mean arterial pressure. MAP = CO * TPR MAP=(SV*HR) * TPR SV= Stroke Volume HR=Heart Rate MAP=((EDV-ESV)*HR) * TPR Cardiac output can be changed tremendously during some conditions. For example, during exercise it can rise from 5 L/min to 35 L/min. Let us consider how this happens. Obviously, an increase in stroke volume or heart rate can increase cardiac output. During the last lecture, we noted that intrinsic heart rate is actually beats/min, but is tonically suppressed to about 70 beats/minute by the parasympathetic nervous system. Thus, one way of increasing heart rate is by withdrawing parasympathetic drive on the heart. Heart rate can be increased further by the actions of the sympathetic nervous system. Recall that binding of NE or EPI to beta receptors on autorhythmic cells increases their firing rate, driving heart rate faster. Furthermore, the catecholamines enhance conduction through the AV node, bundle of His, and Purkinje fibers. However, there is an upward limit on heart rate. If the heart beats too rapidly, there is insufficient time for filling. This condition is called tachycardia. This begins to happen when heart rate exceeds ~170 beats/min. A limit on heart rate is imposed by the delay in conduction through the AV node as well as the long refractory period of myocardial cells. This limitation helps to insure that the heart will not beat too rapidly to effectively pump out blood. However, under certain pathological conditions tachycardia becomes so severe that circulatory collapse occurs. So, an increase in heart rate alone cannot explain the seven-fold increase in cardiac output that can occur during exercise. Stroke volume must also increase in order to amplify cardiac output. As noted in the last lecture, binding of catecholamines to beta-receptors on myocardial cells increases how powerfully they will contract. In other words, the sympathetic nervous system acts to enhance contractility. Obviously, increasing contractility tends to reduce end systolic volume, thereby increasing stroke volume. Any agent that increases cardiac contractility is called an inotropic agent. 9/19/16 & 9/21/16 Page 5 Cardio 3-4
6 Another way of enhancing stroke volume is to increase venous return (thereby increasing end diastolic volume). As noted previously, under physiological conditions the heart will pump out as much blood as it receives (the Frank-Starling Law of the Heart). This enhanced cardiac output during increased cardiac return is due to the fact that myocardial cells are stretched, which places their actin and myosin into a more efficient arrangement for contraction. In addition to mechanically affecting contraction strength by altering the relationship between the contractile proteins actin and myosin in cardiac muscle cells, stretch of a ventricle affects the sensitivity of the calcium-binding protein troponin for calcium. This heightened sensitivity increases the rate of cross-bridge attachment and detachment, and the amount of tension developed by the muscle fiber. These two adaptations result in a more intense ventricular contraction when the chamber s filling with blood increases. Thus, an increase in end diastolic volume insures that cardiac output will also increase. There are important limitations to consider in the relationships diagrammed above. When heart rate increases, there is a decrease in filling time for the ventricles, which tends to decrease stroke volume (Frank-Starling effect). However, this is offset by the Bowditch effect if increases in heart rate are only moderate. At heart rates > 140 bpm, filling time is so limited that cardiac output declines precipitously. There are also limits to ventricular filling. When the ventricle is full, pressure increases as more blood enters the ventricle. The pressure in the ventricle soon is equal to atrial pressure, such that there is no driving force for blood to enter the ventricle. 9/19/16 & 9/21/16 Page 6 Cardio 3-4
7 We previously noted for skeletal muscle that maximal tension is produced when the actin and myosin are in the optimal configuration for the myosin heads to interact with the actin active sites. If the skeletal muscle cell is crumpled too short or stretched too long, less tension is produced during contraction. A B C The length-tension relationship is even more pronounced in cardiac muscle than skeletal muscle. As noted in the graph to the right (brown line), small stretches of cardiac muscle cells results in a great increase in tension during contraction. An unfilled cardiac chamber is like example A above. Filling the chamber with blood stretches the myocytes so the arrangement of actin and myosin is like example B, which causes contractions to become stronger. In addition to mechanically affecting contraction strength by altering the relationship between the contractile proteins actin and myosin in cardiac muscle cells, stretch of a ventricle affects the sensitivity of the calcium-binding protein troponin for calcium. This heightened sensitivity increases the rate of cross-bridge attachment and detachment, and the amount of tension developed by the muscle fiber. As discussed in previous lectures, the parasympathetic nervous system has little affect on the contraction of ventricular cardiac muscle, although actions on atrial cardiac muscle have been demonstrated. The graph above also shows the changes in cardiac muscle tension during passive stretch (when the muscle is relaxed). Due to the presence of titin in cardiac muscle cells and collagen between the cells, as well as the interconnections between cells, tension is generated when cardiac muscle is stretched. This is important to remember when we discuss the stretch of a heart chamber and how that affects passive filling. Afterload is the mean tension produced by a chamber of the heart in order to eject blood. Another way of looking at afterload is the force that must be overcome to eject blood from the ventricle. A major factor contributing to afterload is aortic pressure: an increase in peripheral resistance increases afterload. As a consequence, the aortic valve closes earlier during the cardiac cycle, cardiac output is reduced, and end systolic volume increases. 9/19/16 & 9/21/16 Page 7 Cardio 3-4
8 However, other factors can also contribute to afterload. For example, aortic valve stenosis also increase afterload. Note that increasing afterload produces a secondary increase in preload. The increased end systolic volume is added to normal venous return. This increase in preload activates the Frank- Starling mechanism to partially compensate for the reduction in stroke volume caused by the increase in afterload. The interaction between afterload and preload is utilized in the treatment following a heart attack, where the left ventricle in damaged. Vasodilator drugs are used to augment stroke volume by decreasing afterload, and at the same time, reduce ventricular preload. When arterial pressure is reduced, the ventricle can eject blood more rapidly, which increases the stroke volume and thereby decreases the end-systolic volume. Determinants of Cardiac Output Because less blood remains in the ventricle after systole, the ventricle will not fill to the same enddiastolic volume found before the afterload reduction. As a consequence, higher stroke volumes can be sustained by weaker ventricular contractions, diminishing the risk of congestive heart failure. Cardiac output is influenced both by factors intrinsic to the heart (heart rate and contractility) and factors extrinsic to the heart (preload and afterload). If afterload increases, then cardiac output drops unless heart rate and contractility also increase. If preload increases then cardiac output increases without any changes in heart rate and contractility. Hence Cardiac Output is dependent on the interactions between the cardiac and vascular components. Guyton and his colleagues conducted seminal experiments in the 1950s and 1960s to understand the interactions between the heart and the vasculature, and how they influence cardiac output. These interactions can be described through two equations that are plotted as the vascular function curve (sometimes called the venous return curve) and cardiac function curve. These curves consider the systemic circulation: a single pump and set of pipes. The vascular function curve determines how systemic venous pressure (P v ), which is the same as right atrial pressure, varies with changes in flow (Q) through the vasculature (or cardiac output). In other words, the vascular function curve considers how pressure in the circulation is affected by the vasculature. In contrast, the cardiac function curve considers how changes in systemic venous pressure (P v ) affects cardiac output. 9/19/16 & 9/21/16 Page 8 Cardio 3-4
9 This analysis is undoubtedly artificial, since it discounts the effects of factors such as gravity and skeletal muscle pumping on the cardiovascular system. However, it does provide some important insights, as noted below. The analysis makes the following assumptions: Q (R) Q Cardiac Output = Venous Return Central Venous Pressure = Right Atrial Pressure P v P a Using the model to understand differences in arterial and venous pressures As discussed in the first lecture, R = ΔP/Q (Ohm s Law) Thus, R=(P a P v )/Q (ΔP must be the difference between arterial and venous pressures) Assume that R = 20 mm Hg/L/min and Q = CO = 5 L/min Then, 20 mm Hg/L/min = (P a P v )/5 L/min 100 mm Hg = P a P v P a = 100 mm Hg + P v (in other words, P a is 100 mm Hg greater than P v ). Systemic Filling Pressure (P sf ) Normal Heart Stopped Q=5 L/min Q=0 L/min Pv=2 mm Hg Pa=102 mm Hg Pv=7 mm Hg Pa=7 mm Hg Guyton conducted experiments where the heart was transiently stopped in experimental animals. Immediately afterwards, pressures in the veins and arteries became equal. This pressure is known as systemic filling pressure (P sf ), which can be thought as the effective pressure head in the systemic circulation pushing the blood back into the heart. In mammals, P sf is approximately 7 mm Hg, which is much closer to normal venous pressure than to normal arterial pressure. Why is this the case? The answer relates to the fact that venous compliance is about 19 times higher than arterial compliance. The effects of vascular compliance on Psf can be determined quantitatively, as shown below. 9/19/16 & 9/21/16 Page 9 Cardio 3-4
10 During the first lecture, we learned that: ΔP = ΔV/C or C = ΔV/ΔP In the model: C a = ΔV a /ΔP a C v = ΔV v /ΔP v We also know that: C v =19C a or C v /C a = 19 When the heart is stopped, blood volume moves between the arterial and venous compartments, and the amount of blood moved is equal in the two compartments (the volume removed from one is placed in the other): ΔV a = ΔV v Hence: C a ΔP a = C v ΔP v C a ΔP a = 19C a ΔP v ΔP a = 19ΔP v In other words, the change in arterial pressure is much larger (19 times) than the change in venous pressure. The resulting pressure must be much closer to the original venous pressure. For example, if the original P a =102 mm Hg and the original P v =2 mm Hg, then: ΔP a = 102-X ΔP v = X-2 (102-X) = 19(X-2) (102-X)=19X X=19X 140=20X 7=X = P sf The Vascular Function or Venous Return Curve The vascular function curve is derived based on the notion that the volumes of blood moving between the arterial and venous compartments is equal: ΔV a = ΔV v. We have previously noted that: C = ΔV/ΔP so C a = ΔV a /ΔP a and C v = ΔV v /ΔP v Applying algebra: C a * ΔP a = ΔV a and C v * ΔP v = ΔV v C a * ΔP a = C v * ΔP v ΔP v /ΔP a = C a /C v We have also previously noted that: ΔP a = P a P sf and ΔP v = P v P sf And Ohm s law stipulates that: R = (P a P v )/Q 9/19/16 & 9/21/16 Page 10 Cardio 3-4
11 Using this information and applying algebra, the equations underlying the vascular function curve can be derived: " P v = P sf R*C %! a $ 'Q P a = P sf + R*C $ v # &Q # C a + C v & " C a + C v % This equation provides the relationship between: Cardiac Factors P v, venous pressure (same as right atrial pressure) Q, flow through the vascular system (same as venous return or cardiac output) and Vascular Factors R (peripheral resistance), C a, C v, and P sf. The graphical depiction of this equation is called the vascular function curve or venous return curve. This curve relates venous return (or cardiac output) to right atrial pressure. As right atrial (venous) pressure increases, venous return (or cardiac output) decreases and vice versa. When right atrial pressure equals P sf, venous return (or cardiac output) is zero, since there is no pressure difference to drive blood flow. Note that there is little additional venous return between a right atrial pressure of 0 mmhg and -8 mmhg (or any negative right atrial pressure). This is because the negative right atrial pressure tends to suck together the walls of the large veins near the heart, which limits any further increase in blood flow. The major concept to learn from the vascular function curve is the following: Right atrial pressure decreases as flow through the cardiovascular system (either venous return or cardiac output) increases. This relationship is determined by vascular properties (R, C a, C v, and P sf ). Resistance to Vascular Return Resistance to vascular return is essentially the resistance to movement of blood through the vasculature (essentially the same as total peripheral resistance, with the additional consideration of compliance of the vasculature). This value can be calculated using the model as follows: 9/19/16 & 9/21/16 Page 11 Cardio 3-4
12 " P v = P sf R*C % " a $ 'Q so P sf P v = R*C % a $ 'Q # C a + C v & # C a + C v & and (P sf P v ) Q " = R*C % a $ ' # C a + C v &! RVR = R*C $ a # & " C a + C v % so (P sf P v ) Q = RVR Note that vascular compliance has a major impact on retarding return of blood flow to the heart. Note that the slope of the linear portion of the vascular function curve is 1/RVR. Thus, for typical physiological values of P sf = 7 mm Hg, P v = 2 mm Hg, and Q = 5 L/min: (P sf P v ) Q = RVR (7 2 mmhg) 5 L/min =1 mmhg min/l The slope of the linear portion of the vascular function curve is 1/RVR. Hence, as RVR increases, the slope decreases. This means that a given change in right atrial (venous) pressure causes a smaller change in cardiac output (or venous return) at higher RVR. In addition, maximal cardiac output (or venous return) is lower when RVR is high. 9/19/16 & 9/21/16 Page 12 Cardio 3-4
13 The relative compliance of the venous and arterial vessels has a major impact on relative pressures in the two types of vessels, as illustrated in the graph to the left for different cardiac outputs. As we have discussed, C a ΔP a = C v ΔP v Let us assume that C v = 19C a, so C a ΔP a = 19C a ΔP v ΔP a = 19ΔP v At Q = 0, P v = P a = P sf = 7 mm Hg At Q = 5 L/min, P v = 2 mm Hg thus ΔP v = 5 mm Hg (= 7 2) A small change in circulatory blood volume results in a huge change in P sf, as reflected in the sharp steepness of the curve relating the two parameters. At a circulatory blood volume of 4 L, P sf is 0; this is the unstressed volume, which is insufficient to contribute to pressure because there is insufficient stretch of the vessel walls. Any additional volume inside the cardiovascular system above the unstressed volume is called the stressed volume. At a circulatory blood volume of 5 L, P sf = 7 mm Hg. If blood volume increases by 10%, P sf doubles! Changes in P sf produced by alterations in circulatory volume have a huge impact on cardiac output and venous return, as illustrated in the graph to the left. An increase in P sf causes the vascular function curve to shift upwards and to the right. Consequently, at a particular right atrial pressure, cardiac output and venous return are much larger. In other words, when circulatory blood volume increases, it is much easier for the heart to fill with blood, and cardiac output increases. 9/19/16 & 9/21/16 Page 13 Cardio 3-4
14 Cardiac Function Curve Now we will look at the effects of manipulating right atrial pressure on cardiac output. In essence, this approach measures the effects of changing preload on cardiac output and blood pressure, and produces the cardiac function curve. In the experiments we will be discussing, cardiac contractile state and heart rate are maintained constant, as is arterial pressure (afterload). The cardiac function curve is illustrated to the left. When right atrial pressure is low, cardiac output is 0, since there is too little blood in the cardiac chambers to generate pressure during systole. When right atrial pressure increases above ~4 mm Hg, cardiac output is maximum. This is because the ventricle fulls maximally, and thus cannot accommodate more blood (the factors that limit ventricle filling are discussed below). The cardiac function curves to the left show the effect of increasing heart rate on cardiac output. Modest increases in heart rate facilitate cardiac output, despite a shorter ventricular filling time, due to the Bowditch effect. However, large increases in heart rate shorten filling time so much that cardiac output plummets. 9/19/16 & 9/21/16 Page 14 Cardio 3-4
15 The cardiac output produced by a particular right atrial pressure is altered if the ventricle is hypereffective or hypoeffective. A hypereffective ventricle is present when sympathetic activity is high, or the ventricle is hypertrophied (the muscle mass has increased due to factors such as chronic exercise). In addition, the ventricle is hypereffective when afterload is low. A hypoeffective ventricle is present when there is no sympathetic stimulation, the ventricle is damaged, or afterload increases. It is possible to plot the vascular function and cardiac function curves on the same axes, as shown to the left. The two curves intersect at one point, called the equilibrium point. This point indicates the cardiac output, venous return, and right atrial pressure under this particular physiological condition. In the adjacent graph, point A shows the normal equilibrium point, when right atrial pressure is near 0 and cardiac output and venous return are near 5 L/min. The dashed line indicates the effect of increasing blood volume by 20%. The vascular function curve shifts but the cardiac function curve doesn t. Note that P sf increases to about 16 mm Hg, right atrial pressure is near 8 mm Hg, and cardiac output is ~13 L/min. Under most conditions, both the cardiac output and vascular function curves shift during a manipulation. For example, sympathetic nervous system activity causes the cardiac function curve to shift upwards and a bit to the left, while the vascular function curve shifts upwards and to the right, as illustrated below. These effects are due to the following actions of the sympathetic nervous system: 1) Increased cardiac contractility 2) Increased heart rate 3) Decreased venous compliance 4) Increased total peripheral resistance. Note that afterload increases during sympathetic stimulation, and this opposes a shift in the vascular function curve. Consequently, cardiac output just rises to 10 L/min during maximal sympathetic stimulation. 9/19/16 & 9/21/16 Page 15 Cardio 3-4
16 During exercise, the shift in the venous return curve is considerably different than during sympathetic stimulation. Why? First, afterload decreases as arterioles in skeletal muscle dilate (the mechanisms involved will be discussed in subsequent lectures). In addition, skeletal muscle pumping contributes to an increase in venous return. Cumulatively, these factors in addition to the actions of the sympathetic nervous system cause cardiac output to increase to ~20 L/min. Using the Pressure Volume Relationship to Understand Cardiac Dynamics We previously considered the functional pressure-volume curve, as shown on the left. Such curves can be used to determine a number of parameters regarding the cardiovascular system, and even to diagnose diseases. As such, it is important to understand these curves and the principles they reveal. The functional pressure-volume curve is shown in the area labeled by EW in the curve to the left (EW stands for external work, as discussed later in this lecture). The pressure-volume curves can also be used to describe all physiological events in the heart. The diastolic pressure curve is determined by filling the heart with progressively greater volumes of blood and then measuring the diastolic pressure immediately before ventricular contraction occurs, which is the end-diastolic pressure of the ventricle. Thus curve is often called the end diastolic pressure-volume relationship (EDPVR). 9/19/16 & 9/21/16 Page 16 Cardio 3-4
17 Until the volume of the noncontracting ventricle rises above about 150 ml, the diastolic pressure does not increase greatly. Therefore, up to this volume, blood can flow easily into the ventricle from the atrium. Above 150 ml, the ventricular diastolic pressure increases rapidly, partly because of fibrous tissue in the heart that will stretch no more and partly because the pericardium that surrounds the heart becomes filled nearly to its limit. The systolic pressure curve represents the maximal pressure that can be developed at a particular filling volume of the ventricle. During ventricular contraction, the systolic pressure increases even at low ventricular volumes and reaches a maximum at a ventricular volume of 150 to 170 ml. Then, as the volume increases still further, the systolic pressure actually decreases: at these great volumes, the actin and myosin filaments of the cardiac muscle fibers are pulled apart far enough that the strength of each cardiac fiber contraction becomes less than optimal. The systolic pressure curve is usually referred to as the end systolic pressure-volume relationship (ESPVR). Under physiological conditions, ESPVR is a line that intersects the upper left corner of the functional pressure volume curve. It is common for pressure-volume loops to be constructed from data collected from either experimental animals or human patients. In patients, a device that measures flow rates and pressures can be inserted via the femoral artery into the aorta and then the left ventricle to obtain the necessary data. It is also possible to obtain the volume of blood in the ventricle via echocardiography (although pressure must be measured invasively). As venous return varies spontaneously, many curves can be generated and plotted on the same axes. A line is then drawn connecting the upper left corner of each curve, which is ESPVR. The upper left corner of the functional pressure-volume curve represents aortic valve closure. Interestingly, the pressure at this point is generally near mean arterial pressure. Thus, ESPVR shows the mean arterial pressure generated at different ventricular volumes. The slope of ESPVR is dependent on the contractility of the ventricle. Under sympathetic stimulation, the slope becomes steeper, such that a particular ventricular volume the pressure is greater. By comparing a normal pressure-volume loop with one generated at the same end diastolic volume but under sympathetic stimulation, the changes in stroke volume resulting from the manipulation can be determined. 9/19/16 & 9/21/16 Page 17 Cardio 3-4
18 An increase in contractility has a complex effect on cardiac output. This is because mean arterial pressure (and thus afterload) increases along with the increase in cardiac output. Hence, an increase in contractility both facilitates and opposes an increase in cardiac output. As a result, the increase in cardiac output is relatively modest. Increased Afterload The graph to the left shows the effect of a selective increase in afterload (e.g., resulting from the administration of an alpha-receptor agonist) on cardiac output. Note that ventricular pressure must become much higher before the aortic valve opens, and the valve closes much earlier. Consequently, stroke volume is reduced appreciably. Increased Contractility Increased Afterload However, the effects of increased afterload on stroke volume are ameliorated when contractility increases along with the afterload, as shown in the graph to the left. In this example, stroke volume is identical in the normal state and in the state with combined increases in contractility and afterload. 9/19/16 & 9/21/16 Page 18 Cardio 3-4
19 Increased Preload An increase in preload results in more filling of the ventricle during diastole. Consequently, stroke volume increases in accordance with the additional filling, due to the Frank-Starling Law of the Heart. As noted in previous lectures, a variety of factors can contribute to an increase in preload. They include: 1. Decreased venous compliance (venoconstriction) 2. Decreased resistance to venous return (RVR) 3. Increased blood volume 4. Negative intrathoracic pressure 5. Decreased heart rate 6. Decreased ventricular stiffness 7. Supine posture 8. Increased skeletal muscle pumping Diagnosing Cardiovascular Disease Using the Pressure-Volume Relationship As noted earlier, the structural features of cardiac muscle (collagen, titin, interconnections of myocytes) cause tension (and thus pressure) to build in a ventricle as it fills with blood. The ventricle continues to fill as long as pressure in this chamber is lower than that in the connected atrium. Thus, changing the length-tension relationship (stiffness) for a ventricle can affect how much blood enters the chamber during diastole, and thus cardiac output. A number of medical conditions can result in restrictive cardiomyopathy, or scarring and stiffening of the left ventricle without a loss of contractility. This condition results in the EDPVR curve shifting upwards (dashed line is normal, solid line is during the disease state). As a result, pressure inside the ventricle increases quickly as fluid enters the chamber, and thus filling is limited before intraventricular pressure matches atrial pressure. Consequently, end-diastolic volume is reduced and stroke volume decreases. 9/19/16 & 9/21/16 Page 19 Cardio 3-4
20 The situation is even worse in many patients following a myocardial infarction. Damage to the cardiac muscle can result in both scarring of the ventricular wall and loss of contractility. As a result, stroke volume decreases appreciably (compare the dashed [normal] curve with the solid [disease state] curve in the diagram to the left. Energetics of cardiac contraction in the chamber. The area encompassed by the pressurevolume loop is defined as external work or stroke work, or the work performed by the ventricle to eject the stroke volume into the aorta. Stroke work can be estimated by the product of stroke volume and mean aortic pressure (SW = SV * MAP). In the graph to the left, the stroke work is the area labeled EW. The graph to the left also indicates the area that represents potential energy (PE). Potential energy is defined as the energy stored as a result of deformation of an elastic object. In the heart, the potential energy is the energy absorbed by the ventricular wall that does not result in a change in the pressure of the fluid The term pressure-volume area (PVA) refers to the sum of potential energy and external work. There is a highly linear correlation between the PVA and cardiac oxygen consumption per beat. This relationship holds true under a variety of loading and contractile conditions. This estimation of myocardial oxygen consumption (MVO 2 ) is used to study the coupling of mechanical work and the energy requirement of the heart in various disease states, such as diabetes, ventricular hypertrophy and heart failure. MVO 2 is also used in the calculation of cardiac efficiency, which is the ratio of cardiac stroke work to MVO 2 (Cardiac Efficiency = SW/MVO 2 ). 9/19/16 & 9/21/16 Page 20 Cardio 3-4
Note: The left and right sides of the heart must pump exactly the same volume of blood when averaged over a period of time
 page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 20: The Cardiovascular System: The Heart
 Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Lecture Outline. Cardiovascular Physiology. Cardiovascular System Function. Functional Anatomy of the Heart
 Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
Lecture Outline Cardiovascular Physiology Cardiac Output Controls & Blood Pressure Cardiovascular System Function Functional components of the cardiovascular system: Heart Blood Vessels Blood General functions
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
Starling s Law Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance
 Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance Just as the heart can initiate its own beat in the absence of any nervous or hormonal control, so also can the myocardium
Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance Just as the heart can initiate its own beat in the absence of any nervous or hormonal control, so also can the myocardium
Circulatory System Review
 Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Normal & Abnormal Intracardiac. Lancashire & South Cumbria Cardiac Network
 Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
Cardiovascular System
 Topics to Review Diffusion Skeletal muscle fiber (cell) anatomy Membrane potential and action potentials Action potential propagation Excitation-contraction coupling in skeletal muscle skeletal muscle
Topics to Review Diffusion Skeletal muscle fiber (cell) anatomy Membrane potential and action potentials Action potential propagation Excitation-contraction coupling in skeletal muscle skeletal muscle
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back
 Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Normal Intracardiac Pressures. Lancashire & South Cumbria Cardiac Network
 Normal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform display
Normal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform display
Human Anatomy & Physiology II with Dr. Hubley
 Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Cardiovascular Physiology
 Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Milwaukee School of Engineering Gerrits@msoe.edu. Case Study: Factors that Affect Blood Pressure Instructor Version
 Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
THE HEART Dr. Ali Ebneshahidi
 THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School
 Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
MECHANICAL PROPERTIES OF THE HEART AND ITS INTERACTION WITH THE VASCULAR SYSTEM. November 11, 2002
 Cardiac Physiology Page 1 of 23 MECHANICAL PROPERTIES OF THE HEART AND ITS INTERACTION WITH THE VASCULAR SYSTEM Daniel Burkhoff MD PhD, Associate Professor of Medicine, Columbia University November 11,
Cardiac Physiology Page 1 of 23 MECHANICAL PROPERTIES OF THE HEART AND ITS INTERACTION WITH THE VASCULAR SYSTEM Daniel Burkhoff MD PhD, Associate Professor of Medicine, Columbia University November 11,
Introduction to CV Pathophysiology. Introduction to Cardiovascular Pathophysiology
 Introduction to CV Pathophysiology Munther K. Homoud, MD Tufts-New England Medical Center Spring 2008 Introduction to Cardiovascular Pathophysiology 1. Basic Anatomy 2. Excitation Contraction Coupling
Introduction to CV Pathophysiology Munther K. Homoud, MD Tufts-New England Medical Center Spring 2008 Introduction to Cardiovascular Pathophysiology 1. Basic Anatomy 2. Excitation Contraction Coupling
Functions of Blood System. Blood Cells
 Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Sign up to receive ATOTW weekly email worldanaesthesia@mac.com
 INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
INTRODUCTION TO CARDIOVASCULAR PHYSIOLOGY ANAESTHESIA TUTORIAL OF THE WEEK 125 16 TH MARCH 2009 Toby Elkington, Specialist Registrar Carl Gwinnutt, Consultant Department of Anaesthesia, Salford Royal NHS
Cardiovascular Biomechanics
 Cardiovascular Biomechanics Instructor Robin Shandas, Ph.D. Associate Professor of Pediatric Cardiology and Mechanical Engineering Robin.shandas@colorado.edu (303) 837-2586 (MWF) / (303) 492-0553 (T,Th)
Cardiovascular Biomechanics Instructor Robin Shandas, Ph.D. Associate Professor of Pediatric Cardiology and Mechanical Engineering Robin.shandas@colorado.edu (303) 837-2586 (MWF) / (303) 492-0553 (T,Th)
Blood Pressure. Blood Pressure (mm Hg) pressure exerted by blood against arterial walls. Blood Pressure. Blood Pressure
 Blood Pressure Blood Pressure (mm Hg) pressure exerted by blood against arterial walls Systolic pressure exerted on arteries during systole Diastolic pressure in arteries during diastole 120/80 Borderline
Blood Pressure Blood Pressure (mm Hg) pressure exerted by blood against arterial walls Systolic pressure exerted on arteries during systole Diastolic pressure in arteries during diastole 120/80 Borderline
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
How To Treat Heart Valve Disease
 The Valve Clinic at Baptist Health Madisonville The Valve Clinic at Baptist Health Madisonville Welcome to the Baptist Health Madisonville Valve Clinic at the Jack L. Hamman Heart & Vascular Center. We
The Valve Clinic at Baptist Health Madisonville The Valve Clinic at Baptist Health Madisonville Welcome to the Baptist Health Madisonville Valve Clinic at the Jack L. Hamman Heart & Vascular Center. We
Direct Arterial Blood Pressure Monitoring Angel M. Rivera CVT, VTS (ECC) Animal Emergency Center Glendale, WI March 2003
 Direct Arterial Blood Pressure Monitoring Angel M. Rivera CVT, VTS (ECC) Animal Emergency Center Glendale, WI March 2003 Introduction Direct measurement of arterial blood pressure is obtained via a peripheral
Direct Arterial Blood Pressure Monitoring Angel M. Rivera CVT, VTS (ECC) Animal Emergency Center Glendale, WI March 2003 Introduction Direct measurement of arterial blood pressure is obtained via a peripheral
Page 1. Introduction The blood vessels of the body form a closed delivery system that begins and ends at the heart.
 Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Fellow TEE Review Workshop Hemodynamic Calculations 2013. Director, Intraoperative TEE Program. Johns Hopkins School of Medicine
 Fellow TEE Review Workshop Hemodynamic Calculations 2013 Mary Beth Brady, MD, FASE Director, Intraoperative TEE Program Johns Hopkins School of Medicine At the conclusion of the workshop, the participants
Fellow TEE Review Workshop Hemodynamic Calculations 2013 Mary Beth Brady, MD, FASE Director, Intraoperative TEE Program Johns Hopkins School of Medicine At the conclusion of the workshop, the participants
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Heart Sounds & Murmurs
 Cardiovascular Physiology Heart Sounds & Murmurs Dr. Abeer A. Al-Masri MBBS, MSc, PhD Associate Professor Consultant Cardiovascular Physiologist Faculty of Medicine, KSU Detected over anterior chest wall
Cardiovascular Physiology Heart Sounds & Murmurs Dr. Abeer A. Al-Masri MBBS, MSc, PhD Associate Professor Consultant Cardiovascular Physiologist Faculty of Medicine, KSU Detected over anterior chest wall
Anaesthesia and Heart Failure
 Anaesthesia and Heart Failure Andrew Baldock, Specialist Registrar, Southampton University Hospitals NHS Trust E mail: ajbaldock@doctors.org.uk Self-assessment The following true/false questions may be
Anaesthesia and Heart Failure Andrew Baldock, Specialist Registrar, Southampton University Hospitals NHS Trust E mail: ajbaldock@doctors.org.uk Self-assessment The following true/false questions may be
Traumatic Cardiac Tamponade. Shane KF Seal 19 November 2003 POS
 Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
1 Congestive Heart Failure & its Pharmacological Management
 Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructor: Prof. Keith Baker 1 Congestive Heart Failure & its Pharmacological Management Keith Baker, M.D., Ph.D.
Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructor: Prof. Keith Baker 1 Congestive Heart Failure & its Pharmacological Management Keith Baker, M.D., Ph.D.
The Body s Transport System
 Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
PSIO 603/BME 511 1 Dr. Janis Burt February 19, 2007 MRB 422; 626-6833 jburt@u.arizona.edu. MUSCLE EXCITABILITY - Ventricle
 SIO 63/BME 511 1 Dr. Janis Burt February 19, 27 MRB 422; 626-6833 MUSCLE EXCITABILITY - Ventricle READING: Boron & Boulpaep pages: 483-57 OBJECTIVES: 1. Draw a picture of the heart in vertical (frontal
SIO 63/BME 511 1 Dr. Janis Burt February 19, 27 MRB 422; 626-6833 MUSCLE EXCITABILITY - Ventricle READING: Boron & Boulpaep pages: 483-57 OBJECTIVES: 1. Draw a picture of the heart in vertical (frontal
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Disease: Diagnosis & Treatment
 How I Treat Cardiology Peer Reviewed Heart Disease: Diagnosis & Treatment Amara Estrada, DVM, DACVIM (Cardiology) University of Florida Background Clinical heart disease is the stage of disease when a
How I Treat Cardiology Peer Reviewed Heart Disease: Diagnosis & Treatment Amara Estrada, DVM, DACVIM (Cardiology) University of Florida Background Clinical heart disease is the stage of disease when a
Factors Affecting Blood Pressure. Vessel Elasticity Blood Volume Cardiac Output
 Factors that Affect Pressure Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction pressure is affected by several factors:
Factors that Affect Pressure Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction pressure is affected by several factors:
To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes.
 Circulatory system. Basic function: To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes. Not all organisms have a circulatory system -
Circulatory system. Basic function: To provide the body (cells) with oxygen, and remove CO 2. To provide the body (cells) with nutrients and remove wastes. Not all organisms have a circulatory system -
Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014
 Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014 Philip J. Bergmann Lab Objectives 1. To learn how blood flows through a dual circuit circulation with lungs. 2. To
Biol 111 Comparative & Human Anatomy Lab 9: Circulatory System of the Cat Spring 2014 Philip J. Bergmann Lab Objectives 1. To learn how blood flows through a dual circuit circulation with lungs. 2. To
Overview of the Cardiovascular System
 Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
Circulatory System and Blood
 Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
Heart Rate and Physical Fitness
 Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Edwards FloTrac Sensor & Edwards Vigileo Monitor. Measuring Continuous Cardiac Output with the FloTrac Sensor and Vigileo Monitor
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Measuring Continuous Cardiac Output with the FloTrac Sensor and Vigileo Monitor 1 Topics System Configuration Physiological Principles Pulse pressure relationship
Edwards FloTrac Sensor & Edwards Vigileo Monitor Measuring Continuous Cardiac Output with the FloTrac Sensor and Vigileo Monitor 1 Topics System Configuration Physiological Principles Pulse pressure relationship
Blood Vessels and Circulation
 13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
Workshop B: Essentials of Neonatal Cardiology and CHD Anthony C. Chang, MD, MBA, MPH CARDIAC INTENSIVE CARE
 SHUNT LESIONS NEONATAL : CONGENITAL CARDIAC MALFORMATIONS AND CARDIAC SURGERY ANTHONY C. CHANG, MD, MBA, MPH CHILDREN S HOSPITAL OF ORANGE COUNTY ATRIAL SEPTAL DEFECT LEFT TO RIGHT SHUNT INCREASED PULMONARY
SHUNT LESIONS NEONATAL : CONGENITAL CARDIAC MALFORMATIONS AND CARDIAC SURGERY ANTHONY C. CHANG, MD, MBA, MPH CHILDREN S HOSPITAL OF ORANGE COUNTY ATRIAL SEPTAL DEFECT LEFT TO RIGHT SHUNT INCREASED PULMONARY
Activity 4.2.3: EKG. Introduction. Equipment. Procedure
 Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
MICROGRAVITY EFFECTS ON HUMAN PHYSIOLOGY: CIRCULATORY SYSTEM
 National Aeronautics and Space Administration MICROGRAVITY EFFECTS ON HUMAN PHYSIOLOGY: CIRCULATORY SYSTEM Instructional Objectives Students will: analyze the effects of external stimuli on the physiological
National Aeronautics and Space Administration MICROGRAVITY EFFECTS ON HUMAN PHYSIOLOGY: CIRCULATORY SYSTEM Instructional Objectives Students will: analyze the effects of external stimuli on the physiological
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
RACE I Rapid Assessment by Cardiac Echo. Intensive Care Training Program Radboud University Medical Centre NIjmegen
 RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
Chapter 16: Circulation
 Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood?
 1 1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood? 2 The plan shows the blood system of a mammal. What does the part labelled X represent? A heart
1 1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood? 2 The plan shows the blood system of a mammal. What does the part labelled X represent? A heart
Electrocardiogram and Heart Sounds
 Electrocardiogram and Heart Sounds An introduction to the recording and analysis of electrocardiograms, and the sounds of the heart. Written by Staff of ADInstruments Introduction The beating of the heart
Electrocardiogram and Heart Sounds An introduction to the recording and analysis of electrocardiograms, and the sounds of the heart. Written by Staff of ADInstruments Introduction The beating of the heart
Heart Murmurs. Outline. Basic Pathophysiology
 Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
THE HEART AND CIRCULATION HENRY S. CABIN, M.D.
 CHAPTER 1 THE HEART AND CIRCULATION HENRY S. CABIN, M.D. INTRODUCTION The cardiovascular system is an elaborate network that performs two major tasks: It delivers oxygen and nutrients to body organs and
CHAPTER 1 THE HEART AND CIRCULATION HENRY S. CABIN, M.D. INTRODUCTION The cardiovascular system is an elaborate network that performs two major tasks: It delivers oxygen and nutrients to body organs and
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
Diagnostic and Therapeutic Procedures
 Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Blood vessels. transport blood throughout the body
 Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
CHAPTER XV PDL 101 HUMAN ANATOMY & PHYSIOLOGY. Ms. K. GOWRI. M.Pharm., Lecturer.
 CHAPTER XV PDL 101 HUMAN ANATOMY & PHYSIOLOGY Ms. K. GOWRI. M.Pharm., Lecturer. Types of Muscle Tissue Classified by location, appearance, and by the type of nervous system control or innervation. Skeletal
CHAPTER XV PDL 101 HUMAN ANATOMY & PHYSIOLOGY Ms. K. GOWRI. M.Pharm., Lecturer. Types of Muscle Tissue Classified by location, appearance, and by the type of nervous system control or innervation. Skeletal
Key Medical Terms Associated with the Cardiovascular System
 1 Key Medical Terms Associated with the Cardiovascular System Aneurysm: A thin, weakened section of the wall of an artery or vein that bulges outward, forming a balloon-like sac. Common causes are atherosclerosis,
1 Key Medical Terms Associated with the Cardiovascular System Aneurysm: A thin, weakened section of the wall of an artery or vein that bulges outward, forming a balloon-like sac. Common causes are atherosclerosis,
Dynamic Auscultation of Heart Sounds and Murmurs. Acknowledgement. Disclosures Real or Potential Conflicts of Interest
 Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
HEART MURMURS. Information Leaflet. Your Health. Our Priority.
 HEART MURMURS Information Leaflet Your Health. Our Priority. Page 2 of 5 What is a heart murmur? The first important thing to note is that a heart murmur is not a diagnosis or an illness and it does not
HEART MURMURS Information Leaflet Your Health. Our Priority. Page 2 of 5 What is a heart murmur? The first important thing to note is that a heart murmur is not a diagnosis or an illness and it does not
Common types of congenital heart defects
 Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Renal Blood Flow GFR. Glomerulus Fluid Flow and Forces. Renal Blood Flow (cont d)
 GFR Glomerular filtration rate: about 120 ml /minute (180 L a day) Decreases with age (about 10 ml/min for each decade over 40) GFR = Sum of the filtration of two million glomeruli Each glomerulus probably
GFR Glomerular filtration rate: about 120 ml /minute (180 L a day) Decreases with age (about 10 ml/min for each decade over 40) GFR = Sum of the filtration of two million glomeruli Each glomerulus probably
Provided by the American Venous Forum: veinforum.org
 CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
Chapter 19 Ci C r i cula l t a i t o i n
 Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Magnetic Resonance Quantitative Analysis. MRV MR Flow. Reliable analysis of heart and peripheral arteries in the clinical workflow
 Magnetic Resonance Quantitative Analysis MRV MR Flow Reliable analysis of heart and peripheral arteries in the clinical workflow CAAS MRV Functional Workflow Designed for imaging specialists, CAAS MRV
Magnetic Resonance Quantitative Analysis MRV MR Flow Reliable analysis of heart and peripheral arteries in the clinical workflow CAAS MRV Functional Workflow Designed for imaging specialists, CAAS MRV
Animal Systems: The Musculoskeletal System
 Animal Systems: The Musculoskeletal System Tissues, Organs, and Systems of Living Things Cells, Cell Division, and Animal Systems and Plant Systems Cell Specialization Human Systems The Digestive The Circulatory
Animal Systems: The Musculoskeletal System Tissues, Organs, and Systems of Living Things Cells, Cell Division, and Animal Systems and Plant Systems Cell Specialization Human Systems The Digestive The Circulatory
Auscultation of the Heart
 Review of Clinical Signs uscultation of the Heart Series Editor: Bernard Karnath, MD Bernard Karnath, MD William Thornton, MD uscultation of the heart can provide clues to the diagnosis of many cardiac
Review of Clinical Signs uscultation of the Heart Series Editor: Bernard Karnath, MD Bernard Karnath, MD William Thornton, MD uscultation of the heart can provide clues to the diagnosis of many cardiac
Carcinoid Hjärtsjukdom
 Carcinoid Hjärtsjukdom CARCINOID TUMORS 20/milj/år FORE-GUT 10% bronchial pancreatic gastric duodenal MID-GUT 70% 40% appendiceal jejunal 30% (6/m/år) ileal prox colonic HIND-GUT 20% distal colonic rectal
Carcinoid Hjärtsjukdom CARCINOID TUMORS 20/milj/år FORE-GUT 10% bronchial pancreatic gastric duodenal MID-GUT 70% 40% appendiceal jejunal 30% (6/m/år) ileal prox colonic HIND-GUT 20% distal colonic rectal
The EasySense unit can detect that the Smart Q Heart Rate Sensor is connected and the range it is set to.
 Heart Rate Sensor Heart Rate Sensor (Product No PC-3147) Pulse rate Range: 0 to 200 bpm Resolution: 1 bpm Waveform Range: -2000 to 2000 mv Resolution: 1 mv Introduction The Smart Q Heart Rate Sensor monitors
Heart Rate Sensor Heart Rate Sensor (Product No PC-3147) Pulse rate Range: 0 to 200 bpm Resolution: 1 bpm Waveform Range: -2000 to 2000 mv Resolution: 1 mv Introduction The Smart Q Heart Rate Sensor monitors
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
Cardiovascular Responses to Exercise
 Cardiovascular Respiratory System Unit Chapter 13 Cardiovascular Responses to Exercise After studying the chapter, you should be able to Graph and explain the pattern of response for the major cardiovascular
Cardiovascular Respiratory System Unit Chapter 13 Cardiovascular Responses to Exercise After studying the chapter, you should be able to Graph and explain the pattern of response for the major cardiovascular
Gas Exchange Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.awl.
 Gas Exchange Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.awl.com/bc) Page 1. Introduction Oxygen and carbon dioxide diffuse between
Gas Exchange Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.awl.com/bc) Page 1. Introduction Oxygen and carbon dioxide diffuse between
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery
 Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
AgoraLink Agora for Life Science Technologies Linköpings Universitet Kurs i Fysiologisk mätteknik Biofluidflöden
 AgoraLink Agora for Life Science Technologies Linköpings Universitet Kurs i Fysiologisk mätteknik Biofluidflöden Fysiologisk mätteknik Anatomy of the heart The complex myocardium structure right ventricle
AgoraLink Agora for Life Science Technologies Linköpings Universitet Kurs i Fysiologisk mätteknik Biofluidflöden Fysiologisk mätteknik Anatomy of the heart The complex myocardium structure right ventricle
Understanding your child s heart Atrial septal defect
 Understanding your child s heart Atrial septal defect About this factsheet This factsheet is for the parents of babies and children who have an atrial septal defect (ASD). It explains, what an atrial septal
Understanding your child s heart Atrial septal defect About this factsheet This factsheet is for the parents of babies and children who have an atrial septal defect (ASD). It explains, what an atrial septal
What is echo? CHAPTER 1 1.1 BASIC NOTIONS. Ultrasound production and detection
 What is echo? CHAPTER 1 1.1 BASIC NOTIONS Echocardiography (echo) the use of ultrasound to examine the heart is a safe, powerful, non-invasive and painless technique. Echo is easy to understand as many
What is echo? CHAPTER 1 1.1 BASIC NOTIONS Echocardiography (echo) the use of ultrasound to examine the heart is a safe, powerful, non-invasive and painless technique. Echo is easy to understand as many
Cardiovascular System & Its Diseases. Lecture #4 Heart Failure & Cardiac Arrhythmias
 Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Responses to Static (Isometric) Exercise
 Responses to Static (Isometric) Exercise Suggestions for Teachers Background Static exercise involves the contraction of skeletal muscle without a change in muscle length, hence the alternative term, isometric
Responses to Static (Isometric) Exercise Suggestions for Teachers Background Static exercise involves the contraction of skeletal muscle without a change in muscle length, hence the alternative term, isometric
Cardiology. Anatomy and Physiology of the Heart.
 Cardiology Self Learning Package Module 1: Anatomy and Physiology of the Heart. Module 1: Anatomy and Physiology of the Heart Page 1 CONTENT Introduction Page 3 How to use the ECG Self Learning package.page
Cardiology Self Learning Package Module 1: Anatomy and Physiology of the Heart. Module 1: Anatomy and Physiology of the Heart Page 1 CONTENT Introduction Page 3 How to use the ECG Self Learning package.page
MEASURING AND RECORDING BLOOD PRESSURE
 MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity
 Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
INTRODUCTION TO EECP THERAPY
 INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
Questions FOETAL CIRCULATION ANAESTHESIA TUTORIAL OF THE WEEK 91 18 TH MAY 2008
 FOETAL CIRCULATION ANAESTHESIA TUTORIAL OF THE WEEK 91 18 TH MAY 2008 Dr. S. Mathieu, Specialist Registrar in Anaesthesia Dr. D. J. Dalgleish, Consultant Anaesthetist Royal Bournemouth and Christchurch
FOETAL CIRCULATION ANAESTHESIA TUTORIAL OF THE WEEK 91 18 TH MAY 2008 Dr. S. Mathieu, Specialist Registrar in Anaesthesia Dr. D. J. Dalgleish, Consultant Anaesthetist Royal Bournemouth and Christchurch
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM
 CHAPTER 6: THE CIRCULATORY SYSTEM THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM Most of the cells in the human body are not in direct contact with the external environment, so rely on the circulatory
CHAPTER 6: THE CIRCULATORY SYSTEM THE CIRCULATORY SYSTEM and the LYMPHATIC SYSTEM Most of the cells in the human body are not in direct contact with the external environment, so rely on the circulatory
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
Vtial sign #1: PULSE. Vital Signs: Assessment and Interpretation. Factors that influence pulse rate: Importance of Vital Signs
 Vital Signs: Assessment and Interpretation Elma I. LeDoux, MD, FACP, FACC Associate Professor of Medicine Vtial sign #1: PULSE Reflects heart rate (resting 60-90/min) Should be strong and regular Use 2
Vital Signs: Assessment and Interpretation Elma I. LeDoux, MD, FACP, FACC Associate Professor of Medicine Vtial sign #1: PULSE Reflects heart rate (resting 60-90/min) Should be strong and regular Use 2
