The Circulatory System: Blood Chapter 18
|
|
|
- Octavia Ryan
- 7 years ago
- Views:
Transcription
1 The Circulatory System: Blood Chapter 18 Functions and properties of blood Plasma Blood cell production Erythrocytes Leukocytes Blood Types Hemostasis
2 Functions and Properties of Blood Functions in respiration, nutrition, waste elimination, thermoregulation, immune defense, water balance, electrolyte and ph balance Adults have 4-6 L of blood composed of: plasma, a clear extracellular fluid formed elements = blood cells and platelets Properties of blood: viscosity = resistance to flow osmolarity = concentration of dissolved particles
3 Hematocrit Centrifuge separates formed elements from plasma Hematocrit is the percent of total volume that is cells Normal hematocrit values Female: 37-48% Male: 45-53%
4 Plasma and Plasma Proteins Plasma is a mixture of proteins, enzymes, nutrients, wastes, hormones, and gases if allowed to clot, the liquid that remains is called serum 3 major categories of plasma proteins: albumins are the most abundant plasma protein contributes to viscosity and osmolarity and influences blood pressure, flow and fluid balance fibrinogen is precursor of fibrin threads that help form blood clots globulins (antibodies) provide immune system defenses alpha, beta and gamma globulins Albumens and fibrinogen plasma proteins are formed by the liver Globulins are antibodies produced by white blood cells called plasma cells
5 Plasma and Serum Blood to which an anticoagulant has been added will not clot. Blood cells will settle to the bottom of the tube leaving plasma at the top of the tube. Blood to which no anticoagulant has been added will clot. Blood cells get caught in the clot leave serum behind.
6 Non-protein Components of Plasma Nitrogenous compounds amino acids from dietary protein or tissue breakdown nitrogenous wastes (urea and ammonia) are toxic end products of catabolism that are normally removed from the blood by the kidneys Nutrients (glucose, vitamins, fats, minerals) Dissolved gases like O 2 and CO 2 are transported in plasma Many electrolytes (Na +, Cl +, K +, HCO 3-, Ca +2, and others) sodium makes up 90% of plasma cations accounting for more of the blood s osmolarity than any other solute
7 Formed Elements of Blood neutrophil eosinophil erythrocyte monocyte lymphocyte platelets basophil Formed Elements = Erythrocytes, Platelets, Leukocytes (neutrophil, eosinophil, basophil, monocyte, lymphocyte) Non-formed Elements = Plasma
8 Blood Cell Production (Hematopoiesis/Hemopoiesis) The following hematopoietic tissues produce blood cells: yolk sac of vertebrate embryos produce stem cells that colonize fetal bone marrow, liver, spleen lymph nodes and thymus liver stops producing blood cells at birth and the thymus stops at about age 10, but the other tissues continue to produce WBCs bone marrow contains stem cells that produce RBCs, WBCs and platelets Stem cells multiply continually and are pluripotent (capable of differentiating into multiple cell lines) Red bone marrow is active; yellow bone marrow is inactive and fatty Stem cells are stimulated by hormones including erythropoietin (EPO) from the kidney and the liver
9 amniotic sac yolk sac placenta
10 Stem Cells of Hematopoiesis
11 Erythrocytes (RBCs) Biconcave Disc-shaped cells 7.5 M diameter, 2.0 m thick at rim Flexible center allows folding so cells can pass through narrow capillaries More surface area than a simple disk facilitates diffusion rate of gasses in and out of the cell Major function of RBCs is gas transport Loses nucleus and most organelles during maturation resulting in increased surface area/volume ratio 33% of cytoplasm is hemoglobin (Hb) O 2 delivery to tissues and CO 2 transport back to lungs contains the enzyme, carbonic anhydrase (CA) that produces carbonic acid from CO 2 and water which plays an important role in gas transport and ph balance RBC count normal values men million RBCs/ L women million RBCs/ L
12 Erythrocytes on the tip of a Needle
13 Flexible center of erythrocytes allows folding so cells can pass through narrow capillaries. Capillaries are formed by cells called Endothelial Cells
14 Erythrocyte Production Erythropoiesis from stem cells in bone marrow produces 2.5 million RBCs/second. In response to erythropoietin (EPO), some stem cells develop into proerythroblasts which multiply and develop into erythroblasts. Erythroblasts multiply, synthesize hemoglobin and develop into normoblasts. Normoblasts synthesize more hemoglobin, discard their nucleus and develop into reticulocytes. Reticulocytes have a reticulated pattern of nuclear debris and a welldeveloped network of endoplasmic reticulum that was used for hemoglobin synthesis. a few reticulocytes enter the bloodstream before they fully mature into erythrocytes and can be 0.5% to 1.5% of the circulating RBCs Development from a stem cell to a RBC takes 3-5 days and involves: reduction in cell size, increase in cell number, synthesis of hemoglobin, loss of nucleus blood loss speeds up the process increasing reticulocyte count in circulating blood which is called a shift to the left
15
16 Erythrocyte Homeostasis Negative feedback control kidney and liver hypoxia EPO production bone marrow stimulation RBC count in 3-4 days Causes of Hypoxia low levels of atmospheric O 2 high elevation or altitude increase in exercise Endurance-trained athletes have RBC counts as high as 6.5 million/ l (normal range is 4-6 million) inhaling carbon monoxide hemorrhage
17 Nutritional Needs for Erythropoiesis Iron is key nutrient for erythropoiesis Iron is lost daily through urine, feces, and bleeding on average, men lose 0.9 mg/day and women lose 1.7 mg/day low absorption rate requires consumption of 5-20 mg/day dietary iron comes in 2 forms: ferric (Fe +3 ) and ferrous (Fe +2 ) stomach acid converts Fe +3 to absorbable Fe +2 gastroferritin from stomach binds Fe +2 and transports it to the intestines absorbed into blood & binds to transferrin to travel to bone marrow and liver liver binds surplus iron to apoferritin to create ferritin for storage erythrocytes use iron to make hemoglobin muscle uses iron to make myoglobin which stores O 2 all cells use iron to make cytochromes in mitochondria Other nutritional requirements include B 12, Folic Acid, Vitamin C and Copper (Cu is used as a cofactor for enzymes)
18 Iron Absorption, Transport & Storage
19 Hemoglobin Normal, adult hemoglobin (Hb A ) consists of 4 protein chains called globins (2 alpha chains and 2 beta chains). Each globin has a heme group which binds oxygen to ferrous ion (Fe +2 ). Each Hb molecule can carry four O 2 molecules. Fetal hemoglobin (Hb F ) has gamma instead of beta chains HbF has a higher affinity for O 2 than HbA enabling the fetus to extract O 2 from the mother s bloodstream
20 Erythrocytes and Hemoglobin RBC count and hemoglobin concentration determine the amount of oxygen the blood can carry. Hemoglobin concentration of whole blood: men 13-18g/dL women 12-16g/dL (dl = deciliter = 100ml) Why are values are lower in women? androgens that stimulate RBC production are lower in women women may have periodic menstrual loss of blood
21 Erythrocyte Disorders Polycythemia is an excess of RBCs primary polycythemia is due to cancer of erythropoietic cell line in the red bone marrow RBC count as high as 11 million/ L (normal range is 4-6 million / L) hematocrit of 80% secondary polycythemia can result from dehydration, high altitude, or physical conditioning RBC count of 8 million/ L Dangers of polycythemia increased blood viscosity can lead to embolism, stroke or heart failure
22 Anemia = Deficiency of RBCs or Hb Types of anemia iron-deficiency anemia hemorrhagic anemias from loss of blood hemolytic anemias from RBC destruction Effects of anemia tissue hypoxia and resulting necrosis low blood osmolarity and resulting tissue edema low blood viscosity and resulting increased heart rate
23 Sickle-Cell Disease
24 Sickle-Cell Disease Sickle-Cell is a hereditary defect in Hemoglobin (Hb S ) Recessive allele modifies hemoglobin structure Caused by a single amino acid substitution (valine is inserted in the protein where a glutamic acid should be) homozygous for Hb S have sickle-cell disease heterozygous for Hb S have sickle-cell trait but rarely have symptoms Most common in African Americans and people from Mediterranean region Implications of sickle-cell disease: Hb S turns to gel (polymerizes) at low oxygen concentrations causing cell elongation and inflexible sickle shape that is prone to lysis Sickle cells are sticky and agglutinate, blocking vessels, causing intense pain, kidney and heart failure, paralysis, and stroke chronic hypoxia activates hematopoietic tissue producing more deformed cells Hb S gene persists despite its harmful effects to the homozygous individual because it protects from malaria Hb S indigestible by malaria parasites
25 The ABO Group Your ABO blood type is determined by presence or absence of antigens (agglutinogens) A and/or B on RBCs blood type A has A antigens blood type B has B antigens blood type AB has both A and B antigens blood type O has neither antigen Frequency of blood types varies among populations, but in the USA, O is the most common and AB is the rarest.
26 Frequency of ABO Blood Groups Population O A B AB Cherokee, NC, USA 95% 4% 2% 0% Pawnee, OK, USA 58% 40% 3% 0% African-American, USA 51% 25% 19% 4% Caucasian, USA 46% 42% 9% 4% Eskimo, USA 47% 45% 6% 2% Nikappu, Japan 31% 38% 22% 9% Bengali, India 30% 26% 36% 7%
27 Agglutinins against the ABO Group Antibodies (agglutinins) against the A and B antigens appear 2-8 months after birth and reach a maximum concentration at 10 about years. you do not normally produce antibodies that would react against your own antigens (agglutinogens). each antibody can attach to several antigens at the same time causing agglutination (clumping) of red blood cells.
28 RBC antigens called agglutinogens A & B ABO Blood Types inherited combinations of proteins, glycoproteins and glycolipids on red blood cell membranes Plasma antibodies called agglutinins anti-a & B agglutinins are gamma globulins in blood plasma that recognize (stick to) foreign agglutinogens on RBCs responsible for RBC agglutination in mismatched blood transfusions
29 ABO Blood Types
30 Agglutination of Erythrocytes
31 ABO Blood Typing
32 Mismatched Transfusion Reaction Agglutinated RBCs block blood vessels and RBCs can rupture free Hb can block kidney tubules and cause death Universal donors and recipients AB called universal recipient since it lacks both antibody A and B; O called universal donor problem is donor s plasma may have antibodies against recipient s red blood cells solution is giving packed cells with minimum plasma
33 The Rh Group Rh or D agglutinogens were discovered in the Rhesus monkey in 1940, and then a similar system was found in humans.
34 The Rh Group Blood type is Rh+ if type D agglutinogens are present on RBCs Anti-D agglutinins are not normally present in blood and only form in Rh- individuals who are exposed to Rh+ blood: Rh- person gets a blood transfusion of Rh+ blood Rh- woman carrying an Rh+ fetus no problems result with either the first transfusion or the first pregnancy Hemolytic Disease of the Newborn (HDN or erythroblastosis fetalis) occurs if mother has formed anti-d antibodies and is pregnant with 2nd Rh+ child RhoGAM TM can be given to a pregnant woman with a fetal Rh incompatibility RhoGAM binds to fetal agglutinogens that get into in the mother s blood so her immune system will not mount an attack against the fetus during pregnancy
35 Hemolytic Disease of Newborn In the first pregnancy, some fetal Rh+ blood crosses into the mother and she slowly develops anti-d agglutinins In second pregnancy, the mother s antibodies can cross into the fetus and hemolyze the fetal blood causing severe anemia in the baby. Hemolyzed RBCs release hemoglobin which is converted to bilirubin. High bilirubin is toxic to the mother and child and can cause brain damage. Treat with transfusion or UV phototherapy to degrade bilirubin.
36 There is a dominant allele for the D antigen. The genetic pairs that can exist in humans are as follows: Genetic makeup Blood type + + Rh positive + - Rh positive - - Rh negative Parents' Possible allele Possible Rh Rh types combinations in the children Both & positive Both & or + - positive Both & or + - or - - positive or negative Both & negative One + & One & positive One + & One & or - - positive or negative
37 Frequency of Rh Blood Groups Population + - Cree, Quebec 98% 2% African-American, USA 85% 15% Caucasian, USA 85% 15% Eskimo, USA 100% 0% Bengali, India 95% 5%
38 Leukocytes (WBCs) 4,500-10,000 white blood cells/mcl (cells per microliter) Granulocytes contain specific granules eosinophils - pink-orange granules and bilobed nucleus (2-4%) basophils - abundant, dark violet granules (<1%) large U or S-shaped nucleus hidden by granules neutrophils - multilobed nucleus (60-70%) Very lightly stained reddish to violet granules in cytoplasm Agranulocytes contain no noticeable granules lymphocytes - round, uniform dark violet nucleus (25-33%) variable amounts of bluish cytoplasm (scanty to abundant) monocytes indented nucleus (3-8%) large cell with abundant cytoplasm
39 Granulocytes Neutrophils ( in bacterial infections) phagocytosis of bacteria releases antimicrobial chemicals Eosinophils ( in parasitic infections or allergies) phagocytosis of antigen-antibody complexes, allergens and inflammatory chemicals release enzymes that destroy parasites such as worms Basophils ( in inflammation or infection) secrete histamine (vasodilator) secrete heparin (anticoagulant)
40 Agranulocytes Lymphocytes ( in diverse infections and immune responses) destroy cancer cells, foreign cells, virally infected cells coordinate actions of other immune cells secrete antibodies and provide immune memory two groups: T-lymphocytes and B- lymphocytes Monocytes ( in viral infections and inflammation) mature into macrophages that consume (phagocytosis) pathogens and debris present antigens to activate other immune cells
41 Abnormalities of Leukocyte Count Leukopenia = low WBC count (<5000/ L) causes: radiation, poisons, infectious disease Leukocytosis = high WBC count (>10,000/ L) causes: infection, allergy and disease Leukemia = cancer of hemopoietic tissue myeloid (granulocyte) or lymphoid (lymphocyte) effects: patient subject to opportunistic infection, anemia and impaired clotting
42 Normal and Leukemia Blood Smears
43 Megakaryocytes and Platelets Megakaryocytes are bone marrow cells that repeatedly replicate their DNA without dividing megakaryocytes are gigantic cells (100 m diameter) with a huge nucleus megakaryocytes remain in the bone marrow Megakaryocytes release fragments that enter the bloodstream as platelets platelets live for about 10 days some platelets are stored in the spleen and can be released as needed
44 Megakaryocytes & Platelets
45 Science volume September 2007 p. 1689
46
47 Platelets Platelets are small fragments of megakaryocytes platelets are only 2-4 m diameter platelets contain granules used in clot formation platelets have pseudopods used for phagocytosis and clot retraction Normal Count: 130,000 to 400,000 platelets/ L Functions secrete clotting factors, growth factors for endothelial repair, and vasoconstrictors in broken vessels form temporary platelet plugs attract WBCs to sites of inflammation retract and eventually dissolve old blood clots
48 Hemostasis 1) Vascular Spasm: Vasoconstriction reduces bleeding 2) Platelet Plug Formation: platelets adhere to exposed collagen fibers 3) Blood Clotting: RBCs and more platelets become enmeshed in fibrin threads
49 1) Vascular Spasm Prompt constriction of a broken blood vessel Triggers for a vascular spasm: some pain receptors directly innervate smooth muscle surrounding the blood vessel lasts only a few minutes injury to smooth muscle longer-lasting constriction platelets release serotonin which is a chemical vasoconstrictor
50 2) Platelet Plug Formation Normal endothelium is very smooth and is coated with prostacyclin (an ecosanoid that repels platelets) Broken vessel exposes rough surfaces of collagen Platelet plug formation: platelet pseudopods stick to damaged vessel and other platelets pseudopods contract and draw walls of vessel together forming a platelet plug platelets degranulate releasing a variety of substances serotonin is a vasoconstrictor thromboxane, an eicosanoid that promotes aggregation and degranulation of platelets and vessel vasoconstriction Positive feedback cycle is active until break in vessel is sealed
51 3) Blood Clotting (Coagulation) Clotting is the most effective defense against bleeding conversion of soluble plasma protein fibrinogen into insoluble fibrin threads that form the framework of a clot Clotting Factors are always present in the plasma and in tissues activating one factor will activate the next to form a reaction cascade Factors released by damaged blood vessel tissues cause the extrinsic cascade pathway to begin. Factors found only in the blood itself causes the intrinsic cascade pathway to begin (platelet degranulation). Both cascades normally occur together and lead to a fibrin clot.
52 Colorized scanning electron micrograph of a blood clot removed from the coronary artery of a patient with acute myocardial infarction showing he fibrin meshwork (brown) with trapped red blood cells and a cholesterol crystal (yellow). Science Vol 335 February 10, 2012
53 Coagulation Pathways Extrinsic Pathway Factors released by damaged tissues cause the extrinsic cascade pathway to begin which usually lasts about 15 seconds. Intrinsic Pathway Factors released by platelets start the intrinsic cascade pathway which usually lasts about 3-6 minutes. Calcium is required for both pathways.
54 Completion of Coagulation Both the intrinsic and extrinsic pathways lead to production of Factor X. Factor X produces key enzymes for activating Thrombin which converts soluble fibrinogen into an insoluble fibrin polymer. Thrombin also feeds back on the system to amplify its own production.
55 Coagulation Disorders Unwanted coagulations: Thrombosis = abnormal clotting in unbroken vessel most likely to occur in leg veins of inactive people clots can travel from veins to lungs producing a pulmonary embolism death can occur from hypoxia Embolism: abnormal clot traveling in a blood vessel Infarction, or tissue death, may occur if clot blocks blood supply to an organ Myocardial Infarction (MI) Stroke (brain clot or bleed) 650,000 Americans die annually of thromboembolisms
56 Clot Retraction and Dissolution Clot retraction occurs within 30 minutes pseudopods of platelets pull on fibers of fibrin which compacts the clot Platelet-derived growth factor is secreted by platelets and endothelial cells the growth factor is a mitotic stimulant for fibroblasts and smooth muscle that multiply and repair the damaged vessel Fibrinolysis or dissolution of a clot Fibrin is broken down by the enzyme plasmin Plasmin is produced by the intrinsic enzyme kallikrein and the extrinsic enzyme TPA (tissue plasminogen activator)
57 Blood Clot Dissolution Positive Feedback TPA Kallikrein in the plasma and TPA (tissue plasminogen activator) from damaged tissues quickly convert inactive plasminogen into plasmin Plasmin breaks down clots and promotes formation of more kallikrein
58 Dissolving Clots Streptokinase Enzyme made by the Streptococcus bacteria dissolves clots when administered intravenously. Relatively non-specific and digests many proteins. Tissue plasminogen activator (TPA) Specifically converts inactive plasminogen into the clot-dissolving enzyme plasmin Now produced by transgenic bacteria. Hementin Anticoagulant produced by the giant Amazon leech, Haementeria. Used to dissolve clots in cardiac patients. Now produced in transgenic bacteria.
59 Medicinal Leeches Removing Clots from a postsurgical hematoma
60 Prevention of Clots Platelet Repulsion: platelets do not adhere to prostacyclin-coating that normally lines blood vessels Thrombin Dilution: thrombin is normally diluted by circulating blood heart slowing, as during shock, can result in clot formation slow venous return in legs due to prolonged sitting can also result in clot formation Anticoagulants heparin secreted by basophils and mast cells during inflammatory response interferes with formation of clotting factors (prothrombin activator) Drugs like coumadin
61 Hemophilia Genetic lack of clotting factors hemophilia A is missing factor VIII (83% of cases) hemophilia B is missing factor IX (15% of cases) hemophilia C is missing factor XI (rare) Symptoms: physical exertion can cause bleeding and excruciating pain Treatments: transfusion of plasma or purified clotting factors factor VIII is now produced by transgenic bacteria
62 Normal Blood Values Adults have 4-6 L of blood Female Male Hematocrit: 37-48% 45-53% Hemoglobin: 12-16g/dL 13-18g/dL RBC count: million/ L million/ L WBC count: 4,500-10,000/ L neutrophils 60-70% eosinophils 2-4% basophils <1% lymphocytes 25-33% monocytes 3-8% platelet count: 130,000 to 400,000/ L
KEY CHAPTER 14: BLOOD OBJECTIVES. 1. Describe blood according to its tissue type and major functions.
 KEY CHAPTER 14: BLOOD OBJECTIVES 1. Describe blood according to its tissue type and major functions. TISSUE TYPE? MAJOR FUNCTIONS connective Transport Maintenance of body temperature 2. Define the term
KEY CHAPTER 14: BLOOD OBJECTIVES 1. Describe blood according to its tissue type and major functions. TISSUE TYPE? MAJOR FUNCTIONS connective Transport Maintenance of body temperature 2. Define the term
BLOOD-Chp. Chp.. 6 What are the functions of blood? What is the composition of blood? 3 major types of plasma proteins
 6.1 Blood: An overview BLOOD-Chp Chp.. 6 What are the functions of blood? Transportation: oxygen, nutrients, wastes, carbon dioxide and hormones Defense: against invasion by pathogens Regulatory functions:
6.1 Blood: An overview BLOOD-Chp Chp.. 6 What are the functions of blood? Transportation: oxygen, nutrients, wastes, carbon dioxide and hormones Defense: against invasion by pathogens Regulatory functions:
Thibodeau: Anatomy and Physiology, 5/e. Chapter 17: Blood
 Thibodeau: Anatomy and Physiology, 5/e Chapter 17: Blood This chapter begins a new unit. In this unit, the first four chapters deal with transportation one of the body's vital functions. It is important
Thibodeau: Anatomy and Physiology, 5/e Chapter 17: Blood This chapter begins a new unit. In this unit, the first four chapters deal with transportation one of the body's vital functions. It is important
 Blood Sticky, opaque fluid with a metallic taste (Fe 2+ ) Varies from scarlet (P O2 = 100) to dark red (P O2 = 40) ph is between 7.35 and 7.45 Average volume in an adult is 5 L (7% of body weight) 2 L
Blood Sticky, opaque fluid with a metallic taste (Fe 2+ ) Varies from scarlet (P O2 = 100) to dark red (P O2 = 40) ph is between 7.35 and 7.45 Average volume in an adult is 5 L (7% of body weight) 2 L
Blood. Blood. Blood Composition. Blood Composition. Fractionation & Hemopoesis
 Blood Blood Chapter 19 Blood is a specialized fluid connective tissue that contains cells suspended in a fluid matrix Functions of blood include: Transport of dissolved gases, nutrients, hormones and metabolic
Blood Blood Chapter 19 Blood is a specialized fluid connective tissue that contains cells suspended in a fluid matrix Functions of blood include: Transport of dissolved gases, nutrients, hormones and metabolic
Cardiovascular System. Blood Components
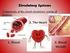 Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
Blood. Functions of Blood. Components of Blood. Transporting. Distributing body heat. A type of connective tissue. Formed elements.
 Blood Functions of Blood Transporting nutrients respiratory gases waste products Distributing body heat Components of Blood A type of connective tissue Formed elements Living blood cells Plasma Nonliving
Blood Functions of Blood Transporting nutrients respiratory gases waste products Distributing body heat Components of Blood A type of connective tissue Formed elements Living blood cells Plasma Nonliving
CHAPTER 14: CARDIOVASCULAR SYSTEM: BLOOD. 1. Describe blood according to its tissue type and major functions.
 OBJECTIVES: 1. Describe blood according to its tissue type and major functions. 2. Define the term hematology. 3. Name the average volume of blood in a human. 4. Name the two major components of blood
OBJECTIVES: 1. Describe blood according to its tissue type and major functions. 2. Define the term hematology. 3. Name the average volume of blood in a human. 4. Name the two major components of blood
Exercise 9: Blood. Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826.
 Exercise 9: Blood Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826. Blood Typing The membranes of human red blood cells (RBCs) contain a variety of cell surface proteins called
Exercise 9: Blood Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826. Blood Typing The membranes of human red blood cells (RBCs) contain a variety of cell surface proteins called
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 10 Blood. Short Answer. Figure 10.1
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 10 Blood Short Answer Figure 10.1 Using Figure 10.1, identify the following: 1) The neutrophil is indicated by letter. Answer: A Diff: 1 Page Ref:
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 10 Blood Short Answer Figure 10.1 Using Figure 10.1, identify the following: 1) The neutrophil is indicated by letter. Answer: A Diff: 1 Page Ref:
3. The Circulatory System
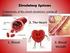 3. The Circulatory System A. Introduction B. Blood 1. Circulatory system transports water, electrolytes, hormones, enzymes, antibodies, cell, gases and nutrients to all cells and carries away metabolic
3. The Circulatory System A. Introduction B. Blood 1. Circulatory system transports water, electrolytes, hormones, enzymes, antibodies, cell, gases and nutrients to all cells and carries away metabolic
Chapter 18. Blood Types
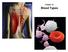 Chapter 18 Blood Types Blood Types blood types and transfusion compatibility are a matter of interactions between plasma proteins and erythrocytes Karl Landsteiner discovered blood types A, B and O in
Chapter 18 Blood Types Blood Types blood types and transfusion compatibility are a matter of interactions between plasma proteins and erythrocytes Karl Landsteiner discovered blood types A, B and O in
Please list four delivery functions of blood, two regulatory functions, and two protection functions. Delivery (distribution) functions
 Chapter 17 Blood Please list four delivery functions of blood, two regulatory functions, and two protection functions. Delivery (distribution) functions Names Period 1-3 - 2-4 - Regulatory functions 1-2
Chapter 17 Blood Please list four delivery functions of blood, two regulatory functions, and two protection functions. Delivery (distribution) functions Names Period 1-3 - 2-4 - Regulatory functions 1-2
Blood Questions. 8. A reduced ability to produce thrombin would cause the time required for blood clot formation to:
 Answer the first 40 items with: a. Increase b. Decrease c. Stay the same 1. An increase in plasma levels of erythropoietin will cause blood viscosity to: 2. The activation of plasminogen will cause the
Answer the first 40 items with: a. Increase b. Decrease c. Stay the same 1. An increase in plasma levels of erythropoietin will cause blood viscosity to: 2. The activation of plasminogen will cause the
Functions of Blood. Collects O 2 from lungs, nutrients from digestive tract, and waste products from tissues Helps maintain homeostasis
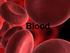 Blood Objectives Describe the functions of blood Describe blood plasma Explain the functions of red blood cells, white blood cells, and platelets Summarize the process of blood clotting What is Blood?
Blood Objectives Describe the functions of blood Describe blood plasma Explain the functions of red blood cells, white blood cells, and platelets Summarize the process of blood clotting What is Blood?
Objectives Chapter 17
 17 Blood Objectives Chapter 17 1. Describe the composition and physical characteristics of whole blood. Explain why it is classified as a connective tissue. This is an all inclusive question and covers
17 Blood Objectives Chapter 17 1. Describe the composition and physical characteristics of whole blood. Explain why it is classified as a connective tissue. This is an all inclusive question and covers
37 2 Blood and the Lymphatic System Slide 1 of 34
 1 of 34 Blood is a connective tissue that contains both dissolved substances and specialized cells. 2 of 34 The functions of blood include: collecting oxygen from the lungs, nutrients from the digestive
1 of 34 Blood is a connective tissue that contains both dissolved substances and specialized cells. 2 of 34 The functions of blood include: collecting oxygen from the lungs, nutrients from the digestive
BLOOD Dr. Ali Ebneshahidi
 BLOOD Dr. Ali Ebneshahidi Functions of blood 1. Transport of substances: like Oxygen, CO2, nutrients, waste, heat, and hormones. 2. Protection: maintenance of normal Ph, normal body fluid volume, hemostasis,
BLOOD Dr. Ali Ebneshahidi Functions of blood 1. Transport of substances: like Oxygen, CO2, nutrients, waste, heat, and hormones. 2. Protection: maintenance of normal Ph, normal body fluid volume, hemostasis,
Blood & Hematology. The human body is made up mostly of water; ~60-65% (40 L)
 Blood & Hematology The human body is made up mostly of water; ~60-65% (40 L) Body s transport system plays key role in balancing fluids in the body s compartments river of life Marieb strictly speaking,
Blood & Hematology The human body is made up mostly of water; ~60-65% (40 L) Body s transport system plays key role in balancing fluids in the body s compartments river of life Marieb strictly speaking,
Components of Blood. Hematocrit 55% plasma 45% cells 99% RBCs < 1% WBCs and platelets. Blood Plasma
 The Cardiovascular System: The Blood Fluids of the Body Cells of the body are serviced by 2 fluids blood composed of plasma and a variety of cells transports nutrients and wastes interstitial fluid bathes
The Cardiovascular System: The Blood Fluids of the Body Cells of the body are serviced by 2 fluids blood composed of plasma and a variety of cells transports nutrients and wastes interstitial fluid bathes
LAB: Blood Exploration
 Name: Period: Date: LAB: Blood Exploration Introduction A liquid called plasma makes up about half (55%) of the content of blood. Plasma contains proteins that help blood to clot, transport substances
Name: Period: Date: LAB: Blood Exploration Introduction A liquid called plasma makes up about half (55%) of the content of blood. Plasma contains proteins that help blood to clot, transport substances
ABO-Rh Blood Typing With Synthetic Blood
 70-0101 ABO-Rh Blood Typing With Synthetic Blood Teacher s Manual World-Class Support for Science & Math The ability to type blood is an invaluable tool in the fields of medicine and criminology. Using
70-0101 ABO-Rh Blood Typing With Synthetic Blood Teacher s Manual World-Class Support for Science & Math The ability to type blood is an invaluable tool in the fields of medicine and criminology. Using
BIOLOGY 12 - CHAPTER 11 - BLOOD - CHAPTER NOTES
 BIOLOGY 12 - CHAPTER 11 - BLOOD - CHAPTER NOTES Facts Human beings are approximately 70% WATER by body weight. o Most of this water is within cells, while a smaller amount is found within: o Tissue fluid
BIOLOGY 12 - CHAPTER 11 - BLOOD - CHAPTER NOTES Facts Human beings are approximately 70% WATER by body weight. o Most of this water is within cells, while a smaller amount is found within: o Tissue fluid
A.L. Wafa a sameer 2014 Circulatory system / Physiology. Physiology of blood
 Red Blood Cells (Erythrocytes) Physiology of blood E rythrocytes : are the most abundant cells of the blood and are necessary for the delivery of oxygen to the tissues. The major function of red blood
Red Blood Cells (Erythrocytes) Physiology of blood E rythrocytes : are the most abundant cells of the blood and are necessary for the delivery of oxygen to the tissues. The major function of red blood
Human Anatomy & Physiology II with Dr. Hubley
 Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
Human Anatomy & Physiology II with Dr. Hubley Exam #1 Name: Instructions This exam consists of 40 multiple-choice questions. Each multiple-choice question answered correctly is worth one point, and the
UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM
 BIOLOGY - 2201 UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM What happens to your body as you run? Breathing, heart rate, temperature, muscle pain, thirsty... Homeotasis Homeostasis is the process of maintaining
BIOLOGY - 2201 UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM What happens to your body as you run? Breathing, heart rate, temperature, muscle pain, thirsty... Homeotasis Homeostasis is the process of maintaining
ABO-Rh Blood Typing Using Neo/BLOOD
 ABO-Rh Blood Typing Using Neo/BLOOD Objectives Determine the ABO and Rh blood type of unknown simulated blood samples. Prepare a simulated blood smear. Examine a prepared blood smear under the microscope
ABO-Rh Blood Typing Using Neo/BLOOD Objectives Determine the ABO and Rh blood type of unknown simulated blood samples. Prepare a simulated blood smear. Examine a prepared blood smear under the microscope
What Does My Bone Marrow Do?
 What Does My Bone Marrow Do? the myelodysplastic syndromes foundation, inc. Illustrations by Kirk Moldoff Published by The Myelodysplastic Syndromes Foundation, Inc. First Edition, 2009. 2012. Table of
What Does My Bone Marrow Do? the myelodysplastic syndromes foundation, inc. Illustrations by Kirk Moldoff Published by The Myelodysplastic Syndromes Foundation, Inc. First Edition, 2009. 2012. Table of
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer
 Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Collect and label sample according to standard protocols. Gently invert tube 8-10 times immediately after draw. DO NOT SHAKE. Do not centrifuge.
 Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
whole blood consists of two main elements: the formed elements
 bloodc components TERI JUNGE, CST/CFA whole blood consists of two main elements: the formed elements and the liquid element. The formed elements are cell fragments and cells, known as corpuscles, which
bloodc components TERI JUNGE, CST/CFA whole blood consists of two main elements: the formed elements and the liquid element. The formed elements are cell fragments and cells, known as corpuscles, which
12.1: The Function of Circulation page 478
 12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
Chapter 16: Circulation
 Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Phlebotomy Handbook Blood Collection Essentials Seventh Edition
 Phlebotomy Handbook Blood Collection Essentials Seventh Edition Diana Garza Kathleen Becan-McBride Chapter Four The Cardiovascular System Introduction Circulatory system is a transport system. Contributes
Phlebotomy Handbook Blood Collection Essentials Seventh Edition Diana Garza Kathleen Becan-McBride Chapter Four The Cardiovascular System Introduction Circulatory system is a transport system. Contributes
Bio Factsheet January 1999 Number 36
 January 1999 Number 36 Structure & of lood and Lymph This Factsheet summarises 1. The structure and function of blood plasma, red blood cells and white blood cells. 2. The formation of lymph and tissue
January 1999 Number 36 Structure & of lood and Lymph This Factsheet summarises 1. The structure and function of blood plasma, red blood cells and white blood cells. 2. The formation of lymph and tissue
2161-1 - Page 1. Name: 1) Choose the disease that is most closely related to the given phrase. Questions 10 and 11 refer to the following:
 Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
White Blood Cells (WBCs) or Leukocytes
 Lec.5 Z.H.Al-Zubaydi Medical Physiology White Blood Cells (WBCs) or Leukocytes Although leukocytes are far less numerous than red blood cells, they are important to body defense against disease. On average,
Lec.5 Z.H.Al-Zubaydi Medical Physiology White Blood Cells (WBCs) or Leukocytes Although leukocytes are far less numerous than red blood cells, they are important to body defense against disease. On average,
A&P 2 Blood Lab Guide In-Lab Exercises
 A&P 2 Blood Lab Guide In-Lab Exercises Have someone in your group read the following out loud, while the others read along: In this "Lab Guide", we will be looking at the blood and some common blood tests.
A&P 2 Blood Lab Guide In-Lab Exercises Have someone in your group read the following out loud, while the others read along: In this "Lab Guide", we will be looking at the blood and some common blood tests.
CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT
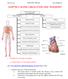 CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT BLOOD CIRCULATION AND TRANSPORT HUMAN BEING PLANTS Function of heart Wilting Structure of heart Blood vessels: characteristics and functions Transpiration: function
CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT BLOOD CIRCULATION AND TRANSPORT HUMAN BEING PLANTS Function of heart Wilting Structure of heart Blood vessels: characteristics and functions Transpiration: function
Platelet Review July 2012. Thomas S. Kickler M.D. Johns Hopkins University School of Medicine
 Platelet Review July 2012 Thomas S. Kickler M.D. Johns Hopkins University School of Medicine Hemostasis Hemostasis is the process that leads to the stopping of bleeding Hemostasis involves blood vessels,
Platelet Review July 2012 Thomas S. Kickler M.D. Johns Hopkins University School of Medicine Hemostasis Hemostasis is the process that leads to the stopping of bleeding Hemostasis involves blood vessels,
Name (print) Name (signature) Period. (Total 30 points)
 AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI
 Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI Overview of Hematology, http://www.nu.edu.sa/userfiles/mhmorsy/h
Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI Overview of Hematology, http://www.nu.edu.sa/userfiles/mhmorsy/h
Blood, Lymphatic and Immune Systems
 Component 3-Terminology in Healthcare and Public Health Settings Unit 4-Blood, Lymphatic and Immune Systems This material was developed by The University of Alabama at Birmingham, funded by the Department
Component 3-Terminology in Healthcare and Public Health Settings Unit 4-Blood, Lymphatic and Immune Systems This material was developed by The University of Alabama at Birmingham, funded by the Department
Hepatitis C. Laboratory Tests and Hepatitis C
 Hepatitis C Laboratory Tests and Hepatitis C If you have hepatitis C, your doctor will use laboratory tests to check your health. This handout will help you understand what the major tests are and what
Hepatitis C Laboratory Tests and Hepatitis C If you have hepatitis C, your doctor will use laboratory tests to check your health. This handout will help you understand what the major tests are and what
Haematology what does your blood test mean?
 Haematology what does your blood test mean? This document provides some reading material to be used in preparation for the Haematology what does your blood test mean? workshop at RMIT s Experience Health
Haematology what does your blood test mean? This document provides some reading material to be used in preparation for the Haematology what does your blood test mean? workshop at RMIT s Experience Health
Laboratory 12 Blood Cells
 Laboratory 12 Blood Cells Objectives: Identify microscopically each of the following: erythrocytes (red blood cells or RBCs), the five types of leukocytes (white blood cells or WBCs), and thrombocytes
Laboratory 12 Blood Cells Objectives: Identify microscopically each of the following: erythrocytes (red blood cells or RBCs), the five types of leukocytes (white blood cells or WBCs), and thrombocytes
Chapter 19 Ci C r i cula l t a i t o i n
 Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Chapter 19 Circulation A closed system Circulatory System Consisting of Heart, Arteries, Veins, Capillaries, Blood & the Lymphatic system Blood Make up The blood is made up of Plasma and three main types
Figure 14.2 Overview of Innate and Adaptive Immunity
 I M M U N I T Y Innate (inborn) Immunity does not distinguish one pathogen from another Figure 14.2 Overview of Innate and Adaptive Immunity Our first line of defense includes physical and chemical barriers
I M M U N I T Y Innate (inborn) Immunity does not distinguish one pathogen from another Figure 14.2 Overview of Innate and Adaptive Immunity Our first line of defense includes physical and chemical barriers
The Immune System. 2 Types of Defense Mechanisms. Lines of Defense. Line of Defense. Lines of Defense
 The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
Inflammation and Healing. Review of Normal Defenses. Review of Normal Capillary Exchange. BIO 375 Pathophysiology
 Inflammation and Healing BIO 375 Pathophysiology Review of Normal Defenses Review of Normal Capillary Exchange 1 Inflammation Inflammation is a biochemical and cellular process that occurs in vascularized
Inflammation and Healing BIO 375 Pathophysiology Review of Normal Defenses Review of Normal Capillary Exchange 1 Inflammation Inflammation is a biochemical and cellular process that occurs in vascularized
Just as a plumbing system carries water through a series of
 37 2 Blood and the Lymphatic System Just as a plumbing system carries water through a series of pipes to different parts of a house, the circulatory system carries blood through a series of blood vessels
37 2 Blood and the Lymphatic System Just as a plumbing system carries water through a series of pipes to different parts of a house, the circulatory system carries blood through a series of blood vessels
serum protein and A/ G ratio
 serum protein and A/ G ratio Blood plasma contains at least 125 individual proteins. Serum ( as contrasted with plasma) is deficient in those coagulation protein which are consumed during the process of
serum protein and A/ G ratio Blood plasma contains at least 125 individual proteins. Serum ( as contrasted with plasma) is deficient in those coagulation protein which are consumed during the process of
Functions of Blood System. Blood Cells
 Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Lymph capillaries, Lymphatic collecting vessels, Valves, Lymph Duct, Lymph node, Vein
 WLHS/A&P/Oppelt Name Lymphatic System Practice 1. Figure 12-1 provides an overview of the lymphatic vessels. First color code the following structures. Color code in Figure 12-1 Heart Veins Lymphatic vessels/lymph
WLHS/A&P/Oppelt Name Lymphatic System Practice 1. Figure 12-1 provides an overview of the lymphatic vessels. First color code the following structures. Color code in Figure 12-1 Heart Veins Lymphatic vessels/lymph
Reproductive System & Development: Practice Questions #1
 Reproductive System & Development: Practice Questions #1 1. Which two glands in the diagram produce gametes? A. glands A and B B. glands B and E C. glands C and F D. glands E and F 2. Base your answer
Reproductive System & Development: Practice Questions #1 1. Which two glands in the diagram produce gametes? A. glands A and B B. glands B and E C. glands C and F D. glands E and F 2. Base your answer
Blood & Marrow Transplant Glossary. Pediatric Blood and Marrow Transplant Program Patient Guide
 Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Circulatory System Review
 Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
CHAPTER 10 BLOOD GROUPS: ABO AND Rh
 CHAPTER 10 BLOOD GROUPS: ABO AND Rh The success of human blood transfusions requires compatibility for the two major blood group antigen systems, namely ABO and Rh. The ABO system is defined by two red
CHAPTER 10 BLOOD GROUPS: ABO AND Rh The success of human blood transfusions requires compatibility for the two major blood group antigen systems, namely ABO and Rh. The ABO system is defined by two red
The Circulatory System. Chapter 17 Lesson 1
 The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
The Immune System: A Tutorial
 The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types:
 Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
Physiology and Anatomy of Blood
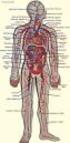 Physiology and Anatomy of Blood Prepared by An-Najah National University Faculty of Medicine and Health Sciences Department of Biomedical Sciences Disclosure The material and the illustrations are adopted
Physiology and Anatomy of Blood Prepared by An-Najah National University Faculty of Medicine and Health Sciences Department of Biomedical Sciences Disclosure The material and the illustrations are adopted
Structures of Proteins. Primary structure - amino acid sequence
 Structures of Proteins Primary structure - amino acid sequence Secondary structure chain of covalently linked amino acids folds into regularly repeating structures. Secondary structure is the result of
Structures of Proteins Primary structure - amino acid sequence Secondary structure chain of covalently linked amino acids folds into regularly repeating structures. Secondary structure is the result of
ANIMALS FORM & FUNCTION BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES. Animals Form & Function Activity #4 page 1
 AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
Blood Transfusion. There are three types of blood cells: Red blood cells. White blood cells. Platelets.
 Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Blood Transfusion Introduction Blood transfusions can save lives. Every second, someone in the world needs a blood transfusion. Blood transfusions can replace the blood lost from a serious injury or surgery.
Blood Physiology. Practical 4. Contents. Practical tasks. Erythrocytes The blood types
 Blood Physiology Practical 4 Contents Erythrocytes The blood types Practical tasks Determination of blood groups of the ABO system Determination of the Rhesus system (Rh factor) The cross matching test
Blood Physiology Practical 4 Contents Erythrocytes The blood types Practical tasks Determination of blood groups of the ABO system Determination of the Rhesus system (Rh factor) The cross matching test
Welcome to Human Anatomy & Physiology Z333
 Welcome to Human Anatomy & Physiology Z333 Instructor: Office: E-Mail: Phone: Office Hours: Mike LeMaster 2025 Cordley Hall lemastem@bcc.orst.edu 737-3705 (Zoology office) MWF 3:00-4:00 pm or by appointment
Welcome to Human Anatomy & Physiology Z333 Instructor: Office: E-Mail: Phone: Office Hours: Mike LeMaster 2025 Cordley Hall lemastem@bcc.orst.edu 737-3705 (Zoology office) MWF 3:00-4:00 pm or by appointment
Interpretation of Laboratory Values
 Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
10. T and B cells are types of a. endocrine cells. c. lymphocytes. b. platelets. d. complement cells.
 Virus and Immune System Review Directions: Write your answers on a separate piece of paper. 1. Why does a cut in the skin threaten the body s nonspecific defenses against disease? a. If a cut bleeds, disease-fighting
Virus and Immune System Review Directions: Write your answers on a separate piece of paper. 1. Why does a cut in the skin threaten the body s nonspecific defenses against disease? a. If a cut bleeds, disease-fighting
MCHENRY WESTERN LAKE COUNTY EMS SYSTEM OPTIONAL CE ADVANCED LEVEL (EMTP, PHRN, ECRN) August 2013. Anticoagulants
 MCHENRY WESTERN LAKE COUNTY EMS SYSTEM OPTIONAL CE ADVANCED LEVEL (EMTP, PHRN, ECRN) August 2013 Anticoagulants Anticoagulants are agents that prevent the formation of blood clots. Before we can talk about
MCHENRY WESTERN LAKE COUNTY EMS SYSTEM OPTIONAL CE ADVANCED LEVEL (EMTP, PHRN, ECRN) August 2013 Anticoagulants Anticoagulants are agents that prevent the formation of blood clots. Before we can talk about
Before continuing, try to answer the following questions. The answers can be found at the end of the article.
 BLOOD PHYSIOLOGY PART 1 ANAESTHESIA TUTORIAL OF THE WEEK 222 9 TH May 2011 Dr Karen Hayes Royal Devon and Exeter NHS Foundation Trust Correspondence: to kmhayes@hotmail.co.uk QUESTIONS Before continuing,
BLOOD PHYSIOLOGY PART 1 ANAESTHESIA TUTORIAL OF THE WEEK 222 9 TH May 2011 Dr Karen Hayes Royal Devon and Exeter NHS Foundation Trust Correspondence: to kmhayes@hotmail.co.uk QUESTIONS Before continuing,
Chapter 16: Innate Immunity
 Chapter 16: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity The Body s Defenses The body has 2 types of defense
Chapter 16: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity The Body s Defenses The body has 2 types of defense
Blood Transfusion. Red Blood Cells White Blood Cells Platelets
 Blood Transfusion Introduction Blood transfusions are very common. Each year, almost 5 million Americans need a blood transfusion. Blood transfusions are given to replace blood lost during surgery or serious
Blood Transfusion Introduction Blood transfusions are very common. Each year, almost 5 million Americans need a blood transfusion. Blood transfusions are given to replace blood lost during surgery or serious
MANAGING ANEMIA. When You Have Kidney Disease or Kidney Failure. www.kidney.org
 MANAGING ANEMIA When You Have Kidney Disease or Kidney Failure www.kidney.org About the Information in this Booklet Did you know that the National Kidney Foundation (NKF) offers guidelines and commentaries
MANAGING ANEMIA When You Have Kidney Disease or Kidney Failure www.kidney.org About the Information in this Booklet Did you know that the National Kidney Foundation (NKF) offers guidelines and commentaries
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
FLUID AND BLOOD THERAPY
 FLUID AND BLOOD THERAPY PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain fluid and blood therapy in the interfacility transfer environment
FLUID AND BLOOD THERAPY PURPOSE To familiarize and acquaint the transfer Paramedic with the skills and knowledge necessary to adequately maintain fluid and blood therapy in the interfacility transfer environment
The Immune System and Disease
 Chapter 40 The Immune System and Disease Section 40 1 Infectious Disease (pages 1029 1033) This section describes the causes of disease and explains how infectious diseases are transmitted Introduction
Chapter 40 The Immune System and Disease Section 40 1 Infectious Disease (pages 1029 1033) This section describes the causes of disease and explains how infectious diseases are transmitted Introduction
Direct Antiglobulin Test (DAT)
 Exercise 8 Exercise 9 Direct Antiglobulin Test (DAT) Elution Study Task Aim Introduction To perform the DAT and elution procedure with correct interpretation of results. To perform with 100% accuracy the
Exercise 8 Exercise 9 Direct Antiglobulin Test (DAT) Elution Study Task Aim Introduction To perform the DAT and elution procedure with correct interpretation of results. To perform with 100% accuracy the
BLOOD GROUP ANTIGENS AND ANTIBODIES
 BLOOD GROUP ANTIGENS AND ANTIBODIES Over 20 blood group systems having approximately 400 blood group antigens are currently recognised. The ABO and Rhesus (Rh) blood group systems are of major clinical
BLOOD GROUP ANTIGENS AND ANTIBODIES Over 20 blood group systems having approximately 400 blood group antigens are currently recognised. The ABO and Rhesus (Rh) blood group systems are of major clinical
Granulocytes vs. Agranulocytes
 Leukocytes are white blood cells (AKA colorless (non-pigmented) blood cells). (Much) smaller in number than RBCs. Unlike RBCs, there are several different types of WBCs. All contain a visible nucleus.
Leukocytes are white blood cells (AKA colorless (non-pigmented) blood cells). (Much) smaller in number than RBCs. Unlike RBCs, there are several different types of WBCs. All contain a visible nucleus.
HUMAN ANATOMY & PHYSIOLOGY MAINTENANCE 30
 Curriculum Development In the Fairfield Public Schools FAIRFIELD PUBLIC SCHOOLS FAIRFIELD, CONNECTICUT HUMAN ANATOMY & PHYSIOLOGY MAINTENANCE 30 Board of Education Approved 05/22/2007 HUMAN ANATOMY & PHYSIOLOGY
Curriculum Development In the Fairfield Public Schools FAIRFIELD PUBLIC SCHOOLS FAIRFIELD, CONNECTICUT HUMAN ANATOMY & PHYSIOLOGY MAINTENANCE 30 Board of Education Approved 05/22/2007 HUMAN ANATOMY & PHYSIOLOGY
Immunity. Humans have three types of immunity innate, adaptive, and passive: Innate Immunity
 Immunity Humans have three types of immunity innate, adaptive, and passive: Innate Immunity Everyone is born with innate (or natural) immunity, a type of general protection. Many of the germs that affect
Immunity Humans have three types of immunity innate, adaptive, and passive: Innate Immunity Everyone is born with innate (or natural) immunity, a type of general protection. Many of the germs that affect
Liver Function Essay
 Liver Function Essay Name: Quindoline Ntui Date: April 20, 2009 Professor: Dr. Danil Hammoudi Class: Anatomy and Physiology 2 Liver function The human body consist of many highly organize part working
Liver Function Essay Name: Quindoline Ntui Date: April 20, 2009 Professor: Dr. Danil Hammoudi Class: Anatomy and Physiology 2 Liver function The human body consist of many highly organize part working
Cells, tissues and organs
 Chapter 8: Cells, tissues and organs Cells: building blocks of life Living things are made of cells. Many of the chemical reactions that keep organisms alive (metabolic functions) take place in cells.
Chapter 8: Cells, tissues and organs Cells: building blocks of life Living things are made of cells. Many of the chemical reactions that keep organisms alive (metabolic functions) take place in cells.
Keystone Review Practice Test Module A Cells and Cell Processes. 1. Which characteristic is shared by all prokaryotes and eukaryotes?
 Keystone Review Practice Test Module A Cells and Cell Processes 1. Which characteristic is shared by all prokaryotes and eukaryotes? a. Ability to store hereditary information b. Use of organelles to control
Keystone Review Practice Test Module A Cells and Cell Processes 1. Which characteristic is shared by all prokaryotes and eukaryotes? a. Ability to store hereditary information b. Use of organelles to control
Blood Plasma 4. Define blood plasma and list the components and their functions.
 Blood Objectives Overview: Blood Composition and Functions 1. Describe the components of blood and their relative proportions. Define the blood hematocrit. 2. List the physical characteristics of blood.
Blood Objectives Overview: Blood Composition and Functions 1. Describe the components of blood and their relative proportions. Define the blood hematocrit. 2. List the physical characteristics of blood.
TOTAL PROTEIN FIBRINOGEN
 UNIT: Proteins 16tproteins.wpd Task Determination of Total Protein, Albumin and Globulins Objectives Upon completion of this exercise, the student will be able to: 1. Explain the ratio of albumin and globulin
UNIT: Proteins 16tproteins.wpd Task Determination of Total Protein, Albumin and Globulins Objectives Upon completion of this exercise, the student will be able to: 1. Explain the ratio of albumin and globulin
Supplemental Material CBE Life Sciences Education. Su et al.
 Supplemental Material CBE Life Sciences Education Su et al. APPENDIX Human Body's Immune System Test This test consists of 31 questions, with only 1 answer to be selected for each question. Please select
Supplemental Material CBE Life Sciences Education Su et al. APPENDIX Human Body's Immune System Test This test consists of 31 questions, with only 1 answer to be selected for each question. Please select
The Lymphatic System. Dr. Naim Kittana, PhD
 The Lymphatic System Dr. Naim Kittana, PhD 1 Disclosure The material and the illustrations are adopted from the textbook Human Anatomy and Physiology / Ninth edition/ Eliane N. Marieb 2013 Dr. Naim Kittana,
The Lymphatic System Dr. Naim Kittana, PhD 1 Disclosure The material and the illustrations are adopted from the textbook Human Anatomy and Physiology / Ninth edition/ Eliane N. Marieb 2013 Dr. Naim Kittana,
Microbiology AN INTRODUCTION EIGHTH EDITION
 TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
Safe Blood and Blood Products
 Safe Blood and Blood Products Module 3 Blood Group Serology Safe Blood and Blood Products Module 3 Blood Group Serology Conversion of electronic files for the website edition was supported by Cooperative
Safe Blood and Blood Products Module 3 Blood Group Serology Safe Blood and Blood Products Module 3 Blood Group Serology Conversion of electronic files for the website edition was supported by Cooperative
Immune System Memory Game
 Immune System Memory Game Recommended Age: 12 years old Time: 45 minutes Everyday our bodies come in contact with millions of tiny organisms and particles that could potentially make us sick. Despite this,
Immune System Memory Game Recommended Age: 12 years old Time: 45 minutes Everyday our bodies come in contact with millions of tiny organisms and particles that could potentially make us sick. Despite this,
Visual Acuity. Hearing. Height and Weight. Blood Pressure MEASURED VALUE
 TEST ITEM DESCRIPTION STANDARD LEVEL Standard level varies among different examination methods. Please check with your medical facility about normal level. MEASURED VALUE Visual Acuity You look at rings
TEST ITEM DESCRIPTION STANDARD LEVEL Standard level varies among different examination methods. Please check with your medical facility about normal level. MEASURED VALUE Visual Acuity You look at rings
Lab 02: Blood Cytology (20 points)
 Pierce College Putman/Biol 242 Name: Lab 02: Blood Cytology (20 points) Reference: Marieb & Mitchell 9 th Ed: 29A (Activities 1, 2, 3, 4, 7); 10 th Ed: Exercise 29 (Activities 1, 2, 3, 4, 7). Pierce College
Pierce College Putman/Biol 242 Name: Lab 02: Blood Cytology (20 points) Reference: Marieb & Mitchell 9 th Ed: 29A (Activities 1, 2, 3, 4, 7); 10 th Ed: Exercise 29 (Activities 1, 2, 3, 4, 7). Pierce College
The chemical reactions inside cells are controlled by enzymes. Cells may be specialised to carry out a particular function.
 12.1 What are animals and plants built from? All living things are made up of cells. The structures of different types of cells are related to their functions. to relate the structure of different types
12.1 What are animals and plants built from? All living things are made up of cells. The structures of different types of cells are related to their functions. to relate the structure of different types
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS
 Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
RAD 223. Radiography physiology. Lecture Notes. First lecture: Cell and Tissue
 RAD 223 Radiography physiology Lecture Notes First lecture: Cell and Tissue Physiology: the word physiology derived from a Greek word for study of nature. It is the study of how the body and its part work
RAD 223 Radiography physiology Lecture Notes First lecture: Cell and Tissue Physiology: the word physiology derived from a Greek word for study of nature. It is the study of how the body and its part work
33.1 The Circulatory System
 33.1 The Circulatory System Lesson Objectives Identify the functions of the human circulatory system. Describe the structure of the heart and explain how it pumps blood through the body. Name three types
33.1 The Circulatory System Lesson Objectives Identify the functions of the human circulatory system. Describe the structure of the heart and explain how it pumps blood through the body. Name three types
VPM 152. INFLAMMATION: Chemical Mediators
 General Pathology VPM 152 INFLAMMATION: Chemical Mediators CHEMICAL MEDIATORS OF INFLAMMATION Definition: any messenger that acts on blood vessels, inflammatory cells or other cells to contribute to an
General Pathology VPM 152 INFLAMMATION: Chemical Mediators CHEMICAL MEDIATORS OF INFLAMMATION Definition: any messenger that acts on blood vessels, inflammatory cells or other cells to contribute to an
